Abstract
Biliary tract cancer, or cholangiocarcinoma, has a poor prognosis. Resection is the only curative treatment, but only a minority of patients are eligible. Chemotherapy and γ-irradiation are merely palliative, as they are unable to remove the malignancy completely. The chicken anemia virus-derived protein apoptin induces apoptosis in a wide range of human tumor cells and is not hindered by mutations inactivating p53 or by overexpression of Bcl-2, changes known to frustrate chemotherapy and radiation therapy. We examined whether apoptin kills human biliary tract cancer cells. Expression of apoptin by means of plasmids caused extensive cell death in three independent cholangiocarcinoma cell lines, CC-LP, CC-SW, and Mz-ChA-1, regardless of their oncogenic mutations, which included inactivated p16 and p53 and the disruption of the transforming growth factor β signaling pathway. In vitro delivery of apoptin by an adenoviral vector completely eradicated cholangiocarcinoma cells. Moreover, coexpression of the broad-spectrum caspase inhibitor p35 with apoptin only delayed the induced cell death. Changes in nuclear morphology still occurred early after transfection, and nuclei eventually disintegrated, suggesting that apoptin-induced cell death in these cells is not blocked by mutations in either the initiation or execution phase of apoptosis. The efficient induction of cell death by apoptin in cholangiocarcinoma cell lines makes apoptin an attractive candidate for molecular therapy of biliary tract cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Malignancies of the biliary tract give rise to high morbidity and mortality. These cholangiocarcinomas can be cured by surgery, but only in a minority of cases. Resection is particularly difficult due to dissemination of the tumor into different bile ducts [1]. At the time of diagnosis only one-half of the patients are resectable, but even then the 5-year survival rate is only around 25% [2, 3, 4]. Palliating the effects of biliary obstruction by endoscopic stenting is therefore often the only therapeutic possibility [5], especially since chemotherapy and γ-irradiation are not effective against cholangiocarcinoma [3, 6, 7]. During carcinogenesis cells acquire traits that enable them to proliferate uncontrollably. Among others, this comprises disabling fail-safe mechanisms that normal cells have to control growth, one of which is the induction of apoptosis [8, 9, 10, 11]. Paradoxically it is precisely this suicide program that cancer therapies such as chemotherapy and radiation employ to induce cell death. Thus, often tumor cells have obtained antiapoptotic changes rendering them resistant to conventional therapy [8, 12, 13]. Consequently, successful treatment of cholangiocarcinoma should be based on an agent that is not hindered by these features.
This study investigated whether the viral protein apoptin is a potential antitumor agent for cholangiocarcinoma. Apoptin efficiently induces apoptosis in a wide range of human tumor cell lines, including osteosarcoma, breast carcinoma, lymphoma, and hepatoma [14, 15]. Apoptin-induced apoptosis in human tumor cells was characterized by morphological changes in nuclear DNA by means of 2,4-diamino-2-phenylindole (DAPI) staining [15] and/or the presence of DNA strand breaks by analysis of DNA-laddering [16] and with the aid of terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling assay [17], by cytochrome c release and/or drop in mitochondrial potential [15]. Interestingly, there seem to be no known mutations in tumor cells that inhibit apoptin-induced apoptosis. For instance, nonfunctional p53 and overexpression of Bcl-2, characteristics known to inhibit apoptosis induced by chemotherapy, do not inactivate apoptin [16, 18, 19, 20]. In addition to its potent proapoptotic properties, apoptin exhibits remarkable tumor-specificity [21, 22] which renders apoptin suitable for nontargeted or systemic therapy. As a first step to determine whether apoptin might be useful against cholangiocarcinoma we analyzed whether biliary tract cancer cell lines are indeed sensitive to apoptin. Here we show that apoptin induces robust apoptosis in several cholangiocarcinoma cell lines in vitro, and moreover that replication-deficient adenoviruses expressing apoptin constitute an effective means to kill these cells.
Experimental procedures
Cells and cell culture
The cholangiocarcinoma cell lines CC-LP [23], CC-SW [23], and Mz-ChA-1 [24] and adenovirus producer cell lines PER.C6 [25] and 911 [26] were grown in Dulbecco’s modified Eagle’s medium (DMEM) supplemented with 10% fetal calf serum, 100 U/ml penicillin, and 100 µg/ml streptomycin (Life Technologies, Rockville, Md., USA) in a 5% CO2 atmosphere at 37°C. CC-LP and CC-SW cells were a kind gift from dr. T. Whiteside (Pittsburgh Cancer Institute, Pittsburgh, Pa., USA) and the Mz-Cha-1 cells from Dr. J. G. Fitz (University of Colorado, Denver, Colo., USA). For immunofluorescence cells were grown on glass microscope slides.
Plasmids and transfection
Expression plasmid pCMV-VP3 contains CAV DNA sequences encoding apoptin (nt 427–868) under control of the cytomegalovirus (CMV) enhancer/promoter [20]. pCMV-desmin encodes desmin, a component of type II intermediate filaments and was used as a negative control for the induction of apoptosis [27], pCMV-neo is the empty vector control [20]. The subcloning of the cDNA of p35 in pCMV has been described previously [15]. pAdApt-VP3 was generated by ligation of the apoptin-BamH1 fragment from pCMV-VP3 into the adenoviral transfer vector pAdApt constructed by IntroGene (now Crucell Holland BV). The plasmids pOLXALuc and pXALuc [28] were transfected to investigate whether the cell lines express functional p53. Expression plasmid pOLXALuc contains the luciferase gene under control of a part of the human HLA-1 promotor. This promoter contains a CAAT and TATA box in addition to a response element, which is activated by wild-type p53. pXALuc also contains the luciferase gene, but lacks the p53 response element. The plasmid pCMV-p53 encodes wild-type p53 under control of the CMV promoter [28].
Plasmid DNA was purified by centrifugation in a cesium chloride (CsCl) gradient and transfection was carried out by complexing with Fugene 6 transfection reagent according to the manufacturer’s protocol (Boehringer-Mannheim, Almere, The Netherlands). In cotransfections pCMV-p35 or pCMV-neo was used in threefold excess to the plasmid encoding the protein that was stained by immunefluorescence (apoptin or desmin). The DNA:Fugene ratio was 1:3 in all cases.
Indirect immunofluorescence and DAPI staining
Indirect immunofluorescence was performed as described previously [29]. To demonstrate the presence of apoptin and establish its cellular localization in transfected cells the cells were fixed with 80% acetone. The indirect immunofluorescence assay was performed with hybridoma culture supernatant containing the mouse monoclonal antibody 111.3 for apoptin and with a 100-fold dilution of monoclonal antibody 33 (Monosan, Uden, The Netherlands) for desmin. Fluorescein-isothiocyanate labeled goat anti-mouse antibody (Jackson Immunoresearch, West Grove Pa., USA) was used as second antibody. Nuclear DNA was stained with 1 µg/ml DAPI in 2% 1, 4 diazabicyclo-[2,2,2]-octane in glycerol/0.1 M Tris HCl pH 8.0.
Adenovirus production and infection
A replication-deficient adenoviral vector lacking the E1 region and expressing apoptin under the regulation of the CMV promoter was generated by cotransfecting near-confluent monolayers of PER.C6 cells with pAdApt-vp3 (GenBank M73260) and the AlfII-ITR fragment of adenovirus type 5 (nt 3534–35935). When cytopathic effects occurred, cells were harvested and lysed by freeze-thawing and the subsequent viral supernatant was serially diluted on PER.C6 cells. Individual clones were tested for apoptin expression by immunofluorescence and for the absence of replication-competent adenovirus by PCR as described [17]. The recombinant adenoviral vector AdCMVLacZ carries the Escherichia coli LacZ gene expressing β-galactosidase under control of the CMV promoter [30].
Large-scale production of adenovirus was performed according to Fallaux et al. [26]. Briefly, PER.C6 helper cells were infected with approximately 5 plaque-forming units per cell in a small volume of DMEM containing 2% horse serum (heat-inactivated at 56°C for 30 min). After a 2-h incubation DMEM/10% fetal calf serum was added to each flask. After 48 h later the detaching cells were harvested and collected in phosphate-buffered solution/2% horse serum. Viruses were isolated from the producer cells by freeze/thawing, purified by CsCl gradient centrifugation and dialysis against a sucrose-containing buffer. Viral titers were determined by plaque assays essentially as described by Graham and Prevec [31]. Briefly, adenovirus stocks were serially diluted in DMEM/2% horse serum and added to near-confluent 911 cells in six-well plates. After 2 h of incubation at 37°C/5% CO2 the medium was replaced by agar-containing culture medium. Plaques were scored on day 5–7 after infection.
Cholangiocarcinoma cells were counted and plated 4–6 h prior to infection. At the time of infection the appropriate number of infectious viral particles per cell (multiplicity of infection, MOI) was added in a small volume of DMEM/2% horse serum. After a 2-h incubation the volume was increased to regular levels with DMEM/10% fetal calf serum. This virus-containing medium was replaced the following day with DMEM/10% fetal calf serum.
Western blotting
Subconfluent monolayers of the various human tumor cell lines were lysed in RB lysis buffer (50 mM Tris HCl pH 7.4, 50 mM NaCl, 0.5% Doc, 2% NP40, 0.2% sodium dodecyl sulfate, and protease inhibitors). Samples were subjected to electrophoresis on a 15% polyacrylamide sodium dodecyl sulfate gel, followed by transfer to Immobilon P membranes (Millipore, Bedford, Mass., USA). After blocking in milk buffer (5% milk in Tris-buffered saline with 0.2% Tween buffer) the membranes were incubated with the mouse monoclonal antibody DO-1 for the detection of p53 (Santa Cruz Biotechnology, Santa Cruz, Calif., USA; dilution 1:500). The membranes were washed with Tris-buffered saline plus Tween buffer, and p53 was detected with horseradish peroxidase conjugated goat anti-mouse IgG (Sigma) as secondary antibody, followed by enhanced chemiluminescence according to the manufacturer’s instructions (Amersham, UK).
Luciferase assay
Forty hours after transfection the cells were lysed in 1× luciferase assay buffer (125 mM Tris-phosphate-pH 7.8, 10 mM dithiothreitol, 10 mM EDTA, 50% glycerol and 1% Triton α-100). After addition of the Luciferase Assay Substrate (Promega, Madison, Wis., USA) according to the manufacturer’s protocol, luciferase activity was measured in a Luminometer (Lumat LB 9501).
Giemsa staining
For detection of the number of attached cells CC-LP cells were washed twice with phosphate-buffered solution 3 days after infection and air-dried. Cells were subsequently fixed in methanol/acetic acid (3:1) for 15 min at room temperature. Cells were incubated in 3% Giemsa (Merck, Darmstadt, Germany), 1 mM Na2HPO4, pH 7.0 solution for 30 min. After staining the cells were washed four times with deionized water and allowed to air-dry.
Results
Apoptin induces cell death in cholangiocarcinoma cell lines
To determine whether chemoresistant cholangiocarcinoma-derived cell lines are sensitive to apoptosis induction by apoptin we analyzed three cell lines CC-SW [23], CC-LP [23], and Mz-ChA-1 [24]. Several oncogenic mutations have been described for these cell lines, including hypermethylation of the p16 promoter in CC-LP [32] and the disruption of the transforming growth factor (TGF) β signaling pathway in Mz-Cha-1 [33].
To examine the p53-status of the cholangiocarcinoma cell lines whole-cell lysates were subjected to western blot analysis. As seen in Fig. 1A, CC-LP cells did not express full-length p53, whereas CC-SW and Mz-Cha-1 cells expressed more p53 than the control cell line HepG2 expressing normal levels of functional p53, which could be indicative of the expression of non-functional p53 [34].
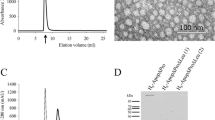
p53 expression and function in cholangiocarcinoma cell lines. A Whole-cell lysates of the cholangiocarcinoma cell lines were analyzed by western blotting using the p53-specific antibody DO-1. Lysates from the hepatoma cell lines HepG2 (exhibiting wild-type p53 expression) and Hep3b (lacking p53 expression) were used as reference. B Cholangiocarcinoma cells were cotransfected with the empty vector pCMV-neo and a construct containing the luciferase reporter gene under the control of a promoter either lacking (pXALuc, open bars, X) or containing (pOLXALuc, striped bars, O) p53 response elements, or were cotransfected with plasmid pCMV-p53 encoding wild-type p53 and pXALuc (gray bars, XP) or with pCMV-p53 and pOLXALuc (black bars, OP). The osteosarcoma cell lines U2OS and Saos-2 were used as references for functional and nonfunctional p53, respectively
To obtain more insight in the activity of p53 in these cholangiocarcinoma cell lines a luciferase reporter construct was used with a p53 response element in the promoter. As a control the identical construct without the p53 response element was used. Transfection of these constructs in the cholangiocarcinoma cell lines demonstrated that none of the lines expressed functional p53 in comparison to the luciferase activation by the endogenous wild-type p53 of the U2OS cell line (Fig. 1B). The p53-negative cell line Saos-2 showed some luciferase activation, which might be due to binding of p63 and/or p73 to the p53 response element [35]. As an additional control a plasmid encoding wild-type p53 was cotransfected with the luciferase reporter construct to demonstrate that when functional p53 is indeed present luciferase is expressed in the examined cholangiocarcinoma cell lines. This was the case for all cell lines except CC-LP, suggesting that in these cells p53 is rapidly degraded, as would be in line with our western blot results.
The three cholangiocarcinoma cell lines were transfected with plasmids encoding apoptin or desmin, a structural protein of muscle cells, as a non-apoptosis-inducing negative control. Several days after transfection cells were fixed and analyzed by indirect immunofluorescence using specific antibodies for either apoptin or desmin and by DAPI staining to detect apoptotic DNA fragmentation (Fig. 2A). Two days after transfection the percentage of apoptotic nuclei among apoptin-positive cells was already considerably increased compared to desmin-positive cells. Several days later apoptin induced up to 90% cell death in apoptin positive cells in all three lines (Fig. 2B). These data demonstrate that regardless of the molecular alterations that characterize these tumor cell lines, they are nevertheless equally sensitive to induction of apoptosis by apoptin.
Apoptin induces cell death in three cholangiocarcinoma cell lines. A Plasmids encoding apoptin and desmin were transfected into CC-LP, CC-SW and Mz-ChA-1 cells. Expression was visualized by indirect immunofluorescence (IFA, left panels). Representative images are shown from CC-SW cells expressing desmin (top) and apoptin (bottom), but results were similar in CC-LP and Mz-ChA-1 cells. Apoptotic morphology was determined by DAPI staining (right panels). B Percentage of apoptotic nuclei in apoptin-transfected (black bars) or desmin-transfected (white bars) cholangiocarcinoma cell lines (SW CC-SW; LP CC-LP; Mz Mz-ChA-1) measured on several days after transfection
Antitumor effect of apoptin expressed by an adenoviral vector
Next we examined whether cholangiocarcinoma cells can be efficiently killed by apoptin delivered by an adenoviral vector system, which is known to transduce cholangiocarcinoma cells efficiently [36, 37]. For this we used a replication-deficient adenovirus vector expressing apoptin or the LacZ gene as a negative control and transduced CC-LP cells at an MOI of 10. Apoptosis in transgene positive cells was scored by nuclear morphology 2, 3, or 5 days after infection (Fig. 3A). Five days after infection up to 80% of the cells expressing apoptin had died, compared to only 10% of the LacZ-positive cells. Using this MOI, approximately 25% of the cells was transduced by the adenovirus, indicating that higher virus titers are needed to kill all the tumor cells. Therefore we used an increasing dose of viral vector to infect CC-LP cells and analyzed the cells by Giemsa staining 3 days later. As shown in Fig. 3B, the number of cells retrieved dramatically decreased with increasing doses of virus expressing apoptin until no cells were left, while with the same or even higher doses of control virus, the cells remained unaffected. Similar results were obtained in cell viability assays using the WST-1 method (data not shown), in which mitochondrial dehydrogenase activity of viable cells was measured. These data indicate that adenoviral vectors efficiently infect CC-LP cells, and moreover that when apoptin is efficiently transduced to cholangiocarcinoma cells, they can all be eliminated.
Expression of apoptin by adenovirus vectors efficiently kills CC-LP cells. A CC-LP cells were infected with a replication-deficient adenoviral vector expressing apoptin (Ad-apoptin) or a marker protein β-galactosidase (Ad-LacZ) using a multiplicity of infection (MOI) of 10. Percentage of apoptotic nuclei in Ad-apoptin (black bars) or Ad-LacZ (white bars) transduced cells was measured on several days after infection. B CC-LP cells were infected with an increasing MOI indicated by the number next to each well using either Ad-LacZ or Ad-apoptin. Surviving cells were visualized by Giemsa staining
Apoptin-induced cell death is delayed but not abrogated by inhibition of caspases
The three cholangiocarcinoma cell lines tested here were equally sensitive to apoptin induced cell death, regardless of their oncogenic mutations (Fig. 2B). To study in more detail the possible effects of antiapoptotic changes on apoptin’s ability to kill cholangiocarcinoma cells we artificially introduced caspase inhibitor p35, a protein derived from baculovirus, which blocks both initiator and execution caspases [38]. Previously we have shown that p35 can inhibit p53 and apoptin-induced apoptosis in human osteosarcoma cells [15]. Preliminary data indicated that p35 also negatively interferes with FADD-induced apoptosis in CC-LP cells [39] (data not shown).
The percentage of morphologically apoptotic CC-LP cells containing apoptin was significantly reduced for each time point when p35 was coexpressed (Fig. 4A). This shows that cell death caused by apoptin in cholangiocarcinoma occurs at least in part via the activation of caspases and thus uses these components of the apoptotic machinery of the cell as it does in osteosarcoma [15]. Although coexpression of p35 and apoptin resulted in the detection of fewer apoptotic nuclei than expression of apoptin alone, many nonapoptotic cells still displayed changes in nuclear morphology, including slight condensation of DNA (Fig. 4B). No similar changes were observed in cells coexpressing p35 and desmin. Furthermore, 4 days after transfection, the percentage of cells expressing apoptin and exhibiting apoptotic morphology increased substantially above background. Thus even when downstream caspases are blocked by p35, in addition to already existing lesions in the apoptotic pathway apoptin is still able to kill, albeit with some delay.
Effects of the caspase inhibitor p35 on apoptin-induced cell death. A Induction of apoptosis by apoptin (black bars) in CC-LP cells is delayed by coexpression of p35 (striped bars). Desmin (white bars) constitutes a non-apoptosis-inducing control and thus represents transfection toxicity; coexpression of p35 has no effect in this case (stippled bars). B Coexpression of desmin and p35 does not lead to altered nuclear morphology (a+b). When apoptin is coexpressed with p35, the overall number of apoptotic cells is reduced but the nonapoptotic cells show changes in nuclear morphology (c+d and e+f). Approximately one-half of the cells expressing apoptin and p35 still undergo apoptosis 4 days after transfection (g+h)
Discussion
This study shows that apoptin could be a candidate for treatment of cholangiocarcinoma as cholangiocarcinoma-derived cell lines can effectively be killed by apoptin. Cholangiocarcinomas have been shown to harbor multiple antiapoptotic mutations, including p53 inactivation and upregulated Bcl-XL [32, 38], lesions that often lead to drug resistance [8, 12]. Importantly, the three independent cholangiocarcinoma cell lines tested here were equally sensitive to apoptin-induced apoptosis, including CC-LP cells, which had failed to respond to chemotherapy in vivo.
Evidently cell death is more efficient when caspases cleave crucial substrates such as PARP and Bid and activate DNases, thus disabling several components of the cell simultaneously, including those involved in metabolism and compromising DNA integrity [40]. However, even when caspases were blocked by a broad-spectrum inhibitor such as p35, the cells containing apoptin still died, although the process was delayed. The delay of cell death rather than complete blockage of apoptin-induced apoptosis by p35 has been observed previously in osteosarcoma cells [15], where in addition to slight changes in nuclear morphology also cytochrome c release from mitochondria still occurred. Furthermore, several groups have reported that caspase inhibition after an apoptotic insult leads to loss of clonogenicity [41, 42]. Thus in cholangiocarcinoma, as in osteosarcoma, mutations in both the decision and execution phase of apoptosis are not likely to confer resistance to apoptin.
The therapeutic window of an anticancer agent is determined not only by its potency but also by its toxicity to healthy surrounding tissues. Notably, it was demonstrated that human primary hepatocytes are refractory to apoptin when injected as a recombinant protein in vitro [22]. In addition, no hepatotoxicity was observed after intravenous administration of an adenoviral vector expressing apoptin in rats [17]. In the future the sensitivity of primary cholangiocytes to apoptin will need to be assessed. Due to technical difficulties in obtaining sufficient numbers of viable cholangiocytes and their limited culture time this question can be best addressed in vivo. For this the effect of Ad-apoptin on synoviocytes can be studied in mice by retrograde biliary infusion of the virus, resulting in transduction of biliary epithelial cells and hepatocytes [43]. To study the effect on cholangiocarcinoma in vivo, the golden Syrian hamster, which has a bile acid profile similar to that of humans, can be used as an experimental model [44]. The adenoviral vector described in this paper, in which apoptin expression is controlled by the CMV promoter, would be suitable for these kinds of experiments [43]. If apoptin indeed shows the same specificity for cholangiocarcinoma compared to cholangiocytes as has been demonstrated, for instance, in tumorigenic fibroblasts and keratinocytes compared to their normal counterparts [21], apoptin may be applicable in treating cholangiocarcinoma as well.
The tumor-selectivity of apoptin renders it suitable for systemic therapy, which in the case of nonresectable cholangiocarcinoma would be preferable. Alternatively, semiregional treatment by occlusion of the bile ducts would also be a possibility. In any case the major prerequisite at the moment is a suitable vector to deliver the apoptin gene. In this study we show that adenoviral transduction of apoptin is an effective method of introducing apoptin into cholangiocarcinoma cells in vitro, a procedure that subsequently causes the elimination of all tumor cells. Others have also reported that cholangiocarcinoma cells can be efficiently transduced by adenovirus [36, 37], indicating that at least enough receptor molecules are present. We have shown that replication-deficient adenovirus vectors expressing apoptin have significant antitumor effects against xenografted hepatoma, in some cases leading to complete regression [30].
In conclusion, the lack of efficient treatment for cholangiocarcinoma warrants the evaluation of alternative treatments. We propose that apoptin could be a potential candidate, as it is highly effective in killing several cholangiocarcinoma cell lines, in spite of multiple antiapoptotic alterations.
Abbreviations
- CMV :
-
Cytomegalovirus
- DAPI :
-
2,4-Diamino-2-phenylindole
- DMEM :
-
Dulbecco’s modified Eagle’s medium
- MOI :
-
Multiplicity of infection
References
De Groen PC, Gores GJ, laRusso NF, Gunderson LL, Nagorney DM (1999) Biliary tract cancers. N Engl J Med 341:1368–1378
Byrnes V, Afdhal N (2002) Cholangiocarcinoma of the hepatic hilum (klatskin tumor). Curr Treat Options Gastroenterol 5:87–94
Kawarada Y, Yamagiwa K, Das BC (2002) Analysis of the relationships between clinicopathologic factors and survival time in intrahepatic cholangiocarcinoma. Am J Surg 183:679–685
Valverde A, Bonhomme N, Farges O, Sauvanet A, Flejou JF, Belghiti J (1999) Resection of intrahepatic cholangiocarcinoma: a Western experience. J Hepatobiliary Pancreat Surg 6:122–127
Cheng JL, Bruno MJ, Bergman JJ, Rauws EA, Tytgat GN, Huibregtse K (2002) Endoscopic palliation of patients with biliary obstruction caused by nonresectable hilar cholangiocarcinoma: efficacy of self-expandable metallic Wallstents. Gastrointest Endosc 56:33–39
Crane CH, Macdonald KO, Vauthey JN, Yehuda P, Brown T, Curley S, Wong A, Delclos M, Charnsangavej C, Janjan NA (2002) Limitations of conventional doses of chemoradiation for unresectable biliary cancer. Int J Radiat Oncol Biol Phys 53:969–974
Price P (2001) Cholangiocarcinoma and the role of radiation and chemotherapy. Hepatogastroenterology 48:51–52
Dive C (1997) Avoidance of apoptosis as a mechanism of drug resistance. J Intern Med Suppl 740:139–145
Hannun YA (1997) Apoptosis and the dilemma of cancer chemotherapy. Blood 89:1845–1853
Makin G, Dive C (2001) Apoptosis and cancer chemotherapy. Trends Cell Biol 11:S22–S26
Hanahan D, Weinberg RA (2000) The hallmarks of cancer. Cell 100:57–70
Aas T, Borresen AL, Geisler S, Smith-Sorensen B, Johnsen H, Varhaug JE, Akslen LA, Lonning PE (1996) Specific p53 mutations are associated with de novo resistance to doxorubicin in breast cancer patients. Nat Med 2:811–814
Findley HW, Gu L, Yeager AM, Zhou M (1997) Expression and regulation of Bcl-2, Bcl-xl, and Bax correlate with p53 status and sensitivity to apoptosis in childhood acute lymphoblastic leukemia. Blood 89:2986–2993
Noteborn MHM, Danen-van Oorschot AAAM, Van der Eb AJ (1998) The apoptin gene of chicken anemia virus in the induction of apoptosis in human tumorigenic cells and in gene therapy of cancer. Gene Ther Mol Biol 1:399–406
Danen-van Oorschot AAAM, Van der Eb AJ, Noteborn MHM (2000) The chicken anemia virus-derived protein apoptin requires activation of caspases for induction of apoptosis in human tumor cells. J Virol 74:7072–7078
Zhuang SM, Shvarts A, Jochemsen AG, van Oorschot AA, van der Eb AJ, Noteborn MHM (1995) Differential sensitivity to Ad5 E1B-21kD and Bcl-2 proteins of apoptin-induced versus p53-induced apoptosis. Carcinogenesis 16:2939–2944
Pietersen AM, van der Eb MM, Rademaker HJ, van den Wollenberg DJ, Rabelink MJ, Kuppen PJ, van Dierendonck JH, van Ormondt H, Masman D, van de Velde CJ, van der Eb AJ, Hoeben RC, Noteborn MH (1999) Specific tumor-cell killing with adenovirus vectors containing the apoptin gene. Gene Ther 6:882–892
Danen-van Oorschot AAAM, van der Eb AJ, Noteborn MHM (1999) Bcl-2 stimulates apoptin-induced apoptosis. Adv Exp Med Biol 457:245–249
Danen-van Oorschot AAAM, Zhang Y, Erkeland SJ, Fischer DF, van der Eb AJ, Noteborn MHM (1999) The effect of Bcl-2 on apoptin in ‘normal’ vs transformed human cells. Leukemia 13 [Suppl 1]:S75–S77
Zhuang SM, Shvarts A, van Ormondt H, Jochemsen AG, van der Eb AJ, Noteborn MHM (1995) Apoptin, a protein derived from chicken anemia virus, induces p53-independent apoptosis in human osteosarcoma cells. Cancer Res 55:486–489
Danen-van Oorschot AAAM, Fischer DF, Grimbergen JM, Klein B, Zhuang S, Falkenburg JH, Backendorf C, Quax PH, van der Eb AJ, Noteborn MHM (1997) Apoptin induces apoptosis in human transformed and malignant cells but not in normal cells. Proc Natl Acad Sci U S A 94:5843–5847
Zhang Y-H, Leliveld SR, Kooistra K, Molenaar C, Rohn JL, Tanke HJ, Abrahams JP, Noteborn MHM (2003) Recombinant apoptin multimers kill tumor cells but are nontoxic and epitope-shielded in a normal-cell-specific fashion. Exp Cell Res 289:36–46
Shimizu Y, Demetris AJ, Gollin SM, Storto PD, Bedford HM, Altarac S, Iwatsuki S, Herberman RB, Whiteside TL (1992) Two new human cholangiocarcinoma cell lines and their cytogenetics and responses to growth factors, hormones, cytokines or immunologic effector cells. Int J Cancer 52:252–260
Knuth A, Gabbert H, Dippold W, Klein O, Sachsse W, Bitter-Suermann D, Prellwitz W, Meyer zum Buschenfelde KH (1985) Biliary adenocarcinoma. Characterisation of three new human tumor cell lines. J Hepatol 1:579–596
Fallaux FJ, Bout A, van der Velde I, van den Wollenberg DJ, Hehir KM, Keegan J, Auger C, Cramer SJ, van Ormondt H, van der Eb AJ, Valerio D, Hoeben RC (1998) New helper cells and matched early region 1-deleted adenovirus vectors prevent generation of replication-competent adenoviruses. Hum Gene Ther 9:1909–1917
Fallaux FJ, Kranenburg O, Cramer SJ, Houweling A, van Ormondt H, Hoeben RC, van der Eb AJ (1996) Characterization of 911: a new helper cell line for the titration and propagation of early region 1-deleted adenoviral vectors. Hum Gene Ther 7:215–222
Menke AL, Shvarts A, Riteco N, van Ham RC, van der Eb AJ, Jochemsen AG (1997) Wilms’ tumor 1-KTS isoforms induce p53-independent apoptosis that can be partially rescued by expression of the epidermal growth factor receptor or the insulin receptor. Cancer Res 57:1353–1363
Steegenga WT, Van Laar T, Shvarts A, Terleth C, Van der Eb AJ, Jochemsen AG (1995) Distinct modulation of p53 activity in transcription and cell cycle regulation by the large (54 kDa) and the small (21 kDa) adenovirus E1B proteins. Virology 212:543–554
van den Heuvel SJ, van Laar T, Kast WM, Melief CJ, Zantema A, van der Eb AJ (1990) Association between the cellular p53 and the adenovirus 5 E1B-55kd proteins reduces the oncogenicity of Ad-transformed cells. EMBO J 9:2621–2629
Eb MM van der, Pietersen AM, Speetjens FM, Kuppen PJ, van de Velde CJ, Noteborn MH, Hoeben RC (2002) Gene therapy with apoptin induces regression of xenografted human hepatomas. Cancer Gene Ther 9:53–61
Graham FL, Prevec L (1995) Methods for construction of adenovirus vectors. Mol Biotechnol 3:207–220
Caca K, Feisthammel J, Klee K, Tannapfel A, Witzigmann H, Wittekind C, Mossner J, Berr F (2002) Inactivation of the INK4a/ARF locus and p53 in sporadic extrahepatic bile duct cancers and bile tract cancer cell lines. Int J Cancer 97:481–488
Yazumi S, Ko K, Watanabe N, Shinohara H, Yoshikawa K, Chiba T, Takahashi R (2000) Disrupted transforming growth factor-beta signaling and deregulated growth in human biliary tract cancer cells. Int J Cancer 86:782–789
Okuda K, Nakanuma Y, Miyazaki M (2002) Cholangiocarcinoma: recent progress. II Molecular pathology and treatment. J Gastroenterol Hepatol 17:1056–1063
Moll UM, Erster, S, Zaika A (2001) p53, p63 and p73–slos, alliances and feuds among family members. Biochim Biophys Acta 1552:47–59
Pederson LC, Vickers SM, Buchsbaum DJ, Kancharla SR, Mayo MS, Curiel DT, Stackhouse MA (1998) Combined cytosine deaminase expression, 5-fluorocytosine exposure, and radiotherapy increases cytotoxicity to cholangiocarcinoma cells. J Gastrointest Surg 2:283–291
Pederson LC, Buchsbaum DJ, Vickers SM, Kancharla SR, Mayo MS, Curiel DT, Stackhouse MA (1997) Molecular chemotherapy combined with radiation therapy enhances killing of cholangiocarcinoma cells in vitro and in vivo. Cancer Res 57:4325–4332
Zhou Q, Krebs JF, Snipas SJ, Price A, Alnemri ES, Tomaselli KJ, Salvesen GS (1998) Interaction of the baculovirus anti-apoptotic protein p35 with caspases. Specificity, kinetics, and characterization of the caspase/p35 complex. Biochemistry 37:10757–10765
Stennicke HR, Ryan CA, Salvesen GS (2002) Reprieval from execution: the molecular basis of caspase inhibition. Trends Biochem Sci 27:94–101
Van Cruchten S, Van Den BW (2002) Morphological and biochemical aspects of apoptosis, oncosis and necrosis. Anat Histol Embryol 31:214–223
Hirsch T, Marchetti P, Susin SA, Dallaporta B, Zamzami N, Marzo I, Geuskens M, Kroemer G (1997) The apoptosis-necrosis paradox. Apoptogenic proteases activated after mitochondrial permeability transition determine the mode of cell death. Oncogene 15:1573–1581
McCarthy NJ, Whyte MK, Gilbert CS, Evan GI (1997) Inhibition of Ced-3/ICE-related proteases does not prevent cell death induced by oncogenes, DNA damage, or the Bcl-2 homologue Bak. J Cell Biol 136:215–227
Peeters MJ, Patijn GA, Lieber A, Meuse L, Kay MA (1996) Adenovirus-mediated hepatic gene transfer in mice: comparison of intravascular and biliary administration. Hum Gene Ther 7:1693–1699
Cheifetz RE, Davis NL, Owen DA (1996) An animal model of benign bile-duct stricture, sclerosing cholangitis and cholangiocarcinoma and the role of epiderma growth factor receptor in ductal proliferation. Can J Surg 39:193–197
Acknowledgements
We thank Piter Bosma (Amsterdam Medical Center) for stimulating discussions and Aart-Gerrit Jochemsen (Leiden University Medical Center) for helpful advise and for the kind donation of the vectors pOLXALuc and pXAluc.
Author information
Authors and Affiliations
Corresponding author
Additional information
A.M. Pietersen and S.A. Rutjes contributed equally to this manuscript
Rights and permissions
About this article
Cite this article
Pietersen, A.M., Rutjes, S.A., van Tongeren, J. et al. The tumor-selective viral protein apoptin effectively kills human biliary tract cancer cells. J Mol Med 82, 56–63 (2004). https://doi.org/10.1007/s00109-003-0486-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-003-0486-z