Abstract
Objective
Stable fixation of periprosthetic or periimplant fractures with an angular stable plate and early weight bearing as tolerated.
Indications
Periprosthetic femur fractures around the hip, Vancouver type B1 or C. Periprosthetic femur and tibia fractures around the knee. Periprosthetic fractures of the humerus. Periimplant fractures after intramedullary nailing.
Contraindications
Loosening of prosthesis. Local infection. Osteitis.
Surgical technique
Preoperative planning is recommended. After minimally invasive fracture reduction and preliminary fixation, submuscular insertion of a large fragment femoral titanium plate or a distal femur plate. The plate is fixed with locking head screws and/or regular cortical screws where possible. If stability is insufficient, one or two locking attachment plates (LAP) are mounted to the femoral plate around the stem of the prosthesis. After fixing the LAP to one of the locking holes of the femoral plate, 3.5 mm screws are used to connect the LAP to the cortical bone and/or cement mantle of the prosthesis.
Postoperative management
Weight bearing as tolerated starting on postoperative day 1 is suggested under supervision of a physiotherapist.
Results
In 6 patients with periprosthetic fractures and 2 patients with periimplant fractures, no surgical complications (e.g., wound infection or bleeding) were observed. The mean time to bony union was 14 weeks. No implant loosening of the locking attachment plate was observed. At the follow-up examination, all patients had reached their prefracture mobility level.
Zusammenfassung
Operationsziel
Erreichen einer belastungsstabilen Osteosynthese bei periprothetischen Frakturen mit stabilem Prothesenschaft durch eine weichteilschonende und biomechanisch überlegene Fixation auch im periprothetischen Bereich mit Hilfe einer speziellen „Locking Attachment Plate“ (LAP).
Indikationen
Periprothetische Oberschenkelfrakturen Typ Vancouver B1 oder C. Periprothetische Oberschenkel- oder Tibiafrakturen bei schaftgeführter Knieprothese. Periprothetische Oberarmfrakturen. Periimplantfrakturen nach intramedullärer Nagelung.
Kontraindikationen
Prothesenlockerung. Lokaler Infekt. Osteitis.
Operationstechnik
Anatomische Reposition der Fraktur und Halten mittels Klemmen; submuskuläres Einschieben der Platte und Schienen der gesamten Femurlänge; distale Plattenlöcher werden über Stichinzisionen besetzt; proximal etwa in der Mitte des Prothesenschafts Anschrauben der LAP in einem Plattenloch einer winkelstabilen Platte und Besetzen der LAP-Löcher mit 3,5-mm-Kleinfragmentkortikalisschrauben in der Femurkortikalis und/oder dem Zementmantel der Prothese. Die Femurplatte wird mit weiteren Schrauben im Bereich des Trochanter major gesichert.
Weiterbehandlung
Schmerzadaptierte Vollbelastung unter physiotherapeutischer Anleitung ab dem 1. postoperativen Tag.
Ergebnisse
Bei insgesamt 6 Patienten mit periprothetischen und 2 Patienten mit periimplantären Frakturen wurden keine Komplikationen beobachtet, die mit der Operation in Verbindung standen (z. B. Wundinfektionen oder Blutungen). Die mittlere Zeitspanne bis zur kallösen Überbrückung betrug 14 Wochen. In keinem Fall musste eine Lockerung der LAP festgestellt werden. Alle Patienten hatten zum Nachuntersuchungszeitpunkt ihren präoperativen funktionellen Status vor Fraktur wieder erreicht.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introductory remarks
Periprosthetic fractures are becoming more frequent [3, 4, 6]. Contributing to this situation are an increasing number of hip arthroplasties, the prevalence of osteoporosis, and an increasing life expectancy. The reported incidence varies between 0.1 and 18 % [7]. The Mayo Clinic Joint Replacement Database estimates the incidence of periprosthetic fracture after primary hip replacement with 1 % (238 of 23,980) and after revision hip prostheses with 4 % (252 of 6349) [2, 7].
There are numerous classifications for periprosthetic fractures. The Vancouver classification of Duncan and Masri [1] is used frequently and helps during decision-making concerning the appropriate treatment. It includes with the following: type A fractures at the level of the trochanter, type B fractures in the area of the stem, and type C fractures distal to the stem. Type B fractures are subdivided according to stable stem (B1), stem loosening (B2), and stem loosening with bone loss in B3 (Fig. 1).
Vancouver classification of periprosthetic fractures according to Duncan and Masri. a Fractures in the trochanteric region, b fractures in the stem region, c fractures distal to the tip of the stem. AG fractures of the greater trochanter, AL fractures of the lesser trochanter, B1 with the stem firmly in place, B2 with loose stem, B3 with bone defect present
While type A fractures rarely need surgical fixation, type B fractures are mainly treated operatively. If the prosthesis is loose (type B2) a revision of the prosthesis to a long stem prosthesis is necessary in most cases [6, 7]. Previous x-rays and/or CT scans are helpful to determine whether the stem is loose, but in some cases this can only be seen intraoperatively. Thus, it is recommended to be prepared for a change of the prosthetic stem.
Lindahl et al. [5] describes failure rates of 33.9 % for periprosthetic fractures fixed with plate osteosynthesis and 43.9 % for repair with only cerclage cables. These high rates suggest that new strategies are necessary to improve outcomes. The locking attachment plate (LAP; Synthes, Paoli, PA, USA; Bettlach, Switzerland) may be used with standard locking compression plates (LCP, DepuySynthes) and creates a stable construct with screw fixation around the stem. From a biomechanical point of view, screw–plate constructs provide greater stiffness compared to cable−plate constructs [8]. As an alternative, it has also been demonstrated that plates with polyaxial screws lead to high union rates in osteoporotic periprosthetic fractures [9].
Surgical principle and objective
Secure periprosthetic plate fixation by using the remaining cortex and/or the cement mantle around the femoral stem for screw anchorage. This avoids the use of cerclage wires and allows—in combination with a long splinting plate fixation—for immediate mobilization of the patient.
Advantages
-
The use of cerclage wires can be minimized or avoided
-
Better fixation of the plate adjacent to the prosthetic stem than with any other method
-
More than one locking attachment plate (LAP) can be used, if necessary
-
Biological osteosynthesis without compromise of the periosteal blood supply
-
Unlike cerclage wires or monocortical screws, the small fragment screws of the LAP maybe anchored in the surrounding cement
Disadvantages
-
Reduction of the fracture without a large exposure requires special minimally invasive surgical techniques and instruments
-
Longer image intensifier time than with open reduction should be anticipated
-
Higher costs in comparison to cerclage wires
Indications
-
Periprosthetic femur fractures around the hip, Vancouver type B1 or C
-
Periprosthetic femur and tibia fractures around the knee
-
Periprosthetic fractures of the humerus
-
Periimplant fractures after intramedullary nailing
Contraindications
-
Complete loosened prosthesis stem in a multifragmentary fracture situation
-
Bone stock and/or cement mantle not sufficient to anchor the screws
Patient information
-
General surgical risks
-
Missing bony healing and potential need for further interventions (e.g., bone grafting)
-
Potential need for transfusion of blood products
-
Implant or prosthesis loosening
-
Postoperative infection with other surgical interventions (prosthesis removal, prosthesis revision, or amputation)
-
Leg length discrepancy and rotational or angular malreduction
-
Secondary periprosthetic or periimplant fracture
-
No hardware removal is suggested
-
Immediate postoperative mobilization with full weight bearing
Preoperative work-up
-
Examination and documentation of the peripheral pulses and neurological findings
-
Assessment of the prefracture functional status of the patient (e.g., Barthel Index) and the mobility level (e.g., Parker Score) to estimate the functional outcome
-
X-ray films of the entire femur and knee joint, each at two orthogonal views
-
CT scan to assess the stability and wear of the prosthetic components especially of the shaft component and for precise determination of the fracture configuration
-
Pain treatment—according to the WHO Guidelines without NSAIDS in the elderly
-
Interdisciplinary assessment with an anesthesiologist and a geriatrician for scheduling the operation at an optimal time point, early assessment of potential complications, management of anticoagulation therapy, and preoperative fluid management
-
Preoperative planning for the measurement of the plate length, number and position of the screws and the LAP. In poor bone, it is recommended to use three to four bicortical screws on each fracture site in case of a fracture with good bone contact and four to five bicortical screws on each fracture site in case of a comminuted fracture.
-
Perioperative antibiotic prophylaxis for 48 h started at least 1 h prior to skin incision
-
Packed red blood cells and cell saver
-
Image intensifier
Instruments and implants
-
Basic surgical instruments
-
Minimally invasive reduction and plate insertion instruments (DepuySynthes)
-
LCP 4.5 curved
-
For proximal fractures, a flipped distal femur plate from the opposite side can also be used to have more fixation options around the stem posteriorly
-
Locking attachment plate (Synthes with 4 and with 8 holes)
-
Instruments for LCP bending
-
Small fragment locking set
-
Large fragment locking set
Anesthesia and positioning
-
General or spinal anesthesia
-
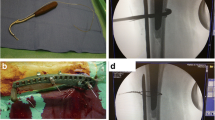
In lateral position, control of the fragments, reduction and fixation seems to be easier than in supine position. Alignment in all dimensions can be well controlled. It is important to check the visibility of the affected femur in both plains with the image intensifier before draping. To ease the lateral view, the contralateral leg must be angulated and the affected leg is supported by two pads (Fig. 2).
Surgical technique
Fig. 2, Fig. 3, Fig. 4, Fig. 5, Fig. 6, Fig. 7, Fig. 8, Fig. 9, Fig. 10, Fig. 11, Fig. 12, Fig. 13
In some cases, a closed reduction is not possible due to muscle interposition, hematoma or jammed periosteum. In these cases the fracture is localized by using the image intensifier and an approximately 5 cm skin incision is done directly there. After sharp dissection of the fascia, the fibers of the vastus lateralis muscle are carefully split (a) The periosteum is preserved as much as possible. In simple fracture situations the approximation of the pieces should be as close as possible by using clamps (b) in order to achieve good fracture healing. In multifragmentary fracture situations, a temporary cerclage wire can be used for fracture reduction in order to restore the correct length and rotation of the femur. The assistant has to pull and rotate the leg
The length of the plate is determined by preoperative measurement and checked under image intensifier. It is recommended to splint the whole bone in order to avoid further periimplant fractures. In each case, the plate must be contoured according to the shape of the greater trochanter and the lateral femoral condyle. The appropriate plate is then introduced into the submuscular plane using a plate holder (a). Alternatively, a guide sleeve attached to a locking hole can be used as a joystick to introduce to the plate (b)
Eight such cortices on each proximally and distally of the fracture site should be tamped with locking screws. At the proximal end it may be impossible to use locking screws due to the stem and in these cases nonlocking screws are placed dorsal to the stem (a). The distal ends of the plate are now fixed to the bone using locking screws. Optionally, a conventional screw can be used to align the plate to the bone (b). In the proximal part the screw lies particularly dorsally to the prosthesis stem. This positioning may permit placement of one or two 4.5 mm bicortical screws in the proximal femur
An appropriate distal plate fixation used with a long spanning plate construct in a proximal Type B1 fracture is shown. A bicortical locking screw is introduced in the distal part. At least 4 screws should be introduced to ensure sufficient stability. To distribute the mechanical stress over the plate length, one bicortical screw can be placed a few holes proximally
For proximal fixation of the plate, the locking attachment plate is used. An incision is made in the area of the stem. The fascia is sharply divided. Adequate exposure is created to implant the locking attachment plate (LAP). The conical screw is introduced with a star drive screwdriver into the selected locking hole. Then the upper part of the screw—a button-head screw—is inserted through the LAP into the conical screw. Ideally the LAP is bent before fixation onto the plate in order to align it to the bone
The locking attachment plate (a) is fixed to the plate (b). The plates are available with 4 or 8 holes for 3.5 mm locking head or 3.5 mm standard cortex screws. The usage of either the 4 or 8 holes plate is an individual decision, whereas in most of the cases a 4 hole plate can be used. Furthermore, the 8 hole plate is associated with more extensive soft tissue damage
Locking or standard screws are placed tangentially in the cortical bone and/or cement mantle around the prosthesis stem. A 2.8 mm drill is used for the angle-stable screw, alternatively a 2.5 mm drill is used to insert conventional 3.5 mm cortex screws. Most of the time the surgeon needs to “palpate” with the drill bit and the corridor for the screw is limited. Therefore, nonlocked screws are usually preferred. Drilling must be performed very carefully in order to avoid breakage of the drill bit. On the dorsal side of the femur, the linea aspera provides good bone stock for stable anchorage of the screws
The wounds are closed in layers. Suction drain is usually not necessary. The post-operative X-ray shows the anatomical reduction of the fracture with final implant position. The postoperative course was uneventful. After 1 year the fracture was well healed and the patient is still fully mobile at home with a walker
Special considerations
Special periprosthetic locking screws (a) with blunt tip can be used in the area around the stem (b). They are available in lengths of 8, 10, 12, 14, and 18 mm. Using an appropriate screw length is mandatory in order to avoid contact with or pushing upon the stem. This could result in splitting of the femoral cortex or also the creation of a galvanic battery resulting in corrosion of the femoral stem due to the dissimilar metals involved
Postoperative management
-
Wound dressing and elastic bandage are applied from foot to groin
-
Mobilization on the postoperative day 1 with the help of crutches or with the walking frame under the supervision of a physiotherapist
-
Weight bearing as tolerated is allowed
-
Application of a low molecular weight heparin for venous thromboembolism prophylaxis
-
X-ray assessment is made before discharge, after 6 weeks, 3 months, and 1 year
-
No planned implant removal
Errors, hazards, complications
-
Misplacement of the plate at the proximal femur: in case of tangential screw insertion there is no good fixation to the bone. If this is noticed intraoperatively the plate and screws should be replaced.
-
Refracture around the end of a proximally fixed plate around the stem of a hip prosthesis. A long plate should be used to splint the whole femur in order to avoid this.
-
Periimplant fracture after application of a plate that is too short: new osteosynthesis with longer plate.
-
Infection: follow the accepted rules for the treatment of infected implants
-
Iatrogenic fracture of the osteoporotic bone caused by vigorous use of the reduction clamps. Cerclage wires may help to fix this situation.
Results
From May 2009 to August 2010, 6 patients with periprosthetic fractures and 2 patients with periimplant fractures were treated with the above-described method in three trauma units. The mean age of the patients was 82 years and all were female. All periprosthetic fractures occurred in the femur; seven were located around a stable hip stem or revision hip stem and one around a stable revision knee stem. The mean time from prosthesis implantation to fracture was 12 years. The periimplant fractures were each around a PFNa and an ETN (both Synthes). Three cases are shown in Fig. 14, Fig. 15, and Fig. 16.
The mean time to follow-up was 13 months. We did not observe any surgical complications (wound infection, bleeding) in this case series. The mean time to bone healing was 14 weeks (callus formation). We did not observe any implant loosening of the locking attachment plate. At time of follow-up, 4 patients were walking independently, three with a walking frame, and one patient needed assistance from another person; all patients reached their prefracture mobility status.
References
Duncan CP, Masri BA (1995) Fractures of the femur after hip replacement. Instr Course Lect 44:293–304
Lee SR, Bostrom MP (2004) Periprosthetic fractures of the femur after total hip arthroplasty. Instr Course Lect 53:111–118
Lindahl H (2007) Epidemiology of periprosthetic femur fracture around a total hip arthroplasty. Injury 38:651–654
Lindahl H, Garellick G, Regner H et al (2006) Three hundred and twenty-one periprosthetic femoral fractures. J Bone Joint Surg Am 88:1215–1222
Lindahl H, Malchau H, Oden A, Garellick G (2006) Risk factors for failure after treatment of a periprosthetic fracture of the femur. J Bone Joint Surg Br 88:26–30
Masri BA, Meek RM, Duncan CP (2004) Periprosthetic fractures evaluation and treatment. Clin Orthop Relat Res 4:80–95
Pike J, Davidson D, Garbuz D et al (2009) Principles of treatment for periprosthetic femoral shaft fractures around well-fixed total hip arthroplasty. J Am Acad Orthop Surg 17:677–688
Lever JR, Zdero R, Nousiainen T et al (2010) The biomechanical analysis of three plating fixation systems for periprosthetic femoral fracture near the tip of a total hip arthroplasty. J Orthop Surg Res 5:45
Erhart JB, Grob K, Roderer G et al (2008) Treatment of periprosthetic femur fractures with non-contact bridging plate: a new angular stable implant. Arch Orthop Trauma Surg 128:409–416
Conflict of interest
On behalf of all authors, the corresponding author states that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kammerlander, C., Kates, S., Wagner, M. et al. Minimally invasive periprosthetic plate osteosynthesis using the locking attachment plate. Oper Orthop Traumatol 25, 398–410 (2013). https://doi.org/10.1007/s00064-011-0091-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00064-011-0091-1
Keywords
- Periprosthetic fracture
- Locking attachment plate
- Minimally invasive osteosynthesis
- Periprosthetic fractures
- Osteoporosis