Abstract
The pathogenesis of recurrent aphthous ulceration (RAU) is unknown, although an abnormal immune reaction appears to be involved. RAU may result from oral epithelium damage caused by T cell-mediated immune response. To improve understanding of the role of T cells in RAU, the present study analyzed. the expression of T cell-related genes in oral ulcers from patients with RAU, as well as in healthy non-keratinized oral mucosa from aphthae-free volunteers. Biopsies from RAU patients and healthy individuals were analyzed using Human Th1-Th2-Th3 RT2 Profiler PCR Array and qRT-PCR that allowed to quantify the transcript levels of 86 genes related to T cell activation. We found that cells present in aphthous ulcers express a characteristic Th1-like gene profile. The majority of genes up-regulated in aphthous lesions such as IFN-γ, TNF, IL-15, IRF1, STAT-1 and STAT-4 were Th1-associated. Th2-realated genes were not overexpressed in RAU tissues, with the exception for CCR3. Th3- and Th17-related gene expression patterns were not demonstrated in RAU. These findings clearly reveal that aphthous ulcer formation is predominantly dependent on the activation of the Th1-type immune response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Recurrent aphthous ulcers (RAU) are the most common type of ulceration in oral cavity that affects about 20% of the world’s population (Rivera-Hidalgo et al. 2004). The pathogenesis of RAU is unknown, there is, however evidence for the involvement of genetic, immunological and infectious factors (Jurge et al. 2006). Recently, it was proposed that imbalance of the CD4+ Th1/Th2 immune response may contribute to loss of immune tolerance in oral mucosa causing inflammatory reaction and appearance of aphthae. Local and systemic predominance of Th1 cytokine production interferon (IFN)-γ, tumor necrosis factor (TNF), interleukin (IL)-2 and IL-12 in RAU have been reported in several studies (Albanidou-Farmaki et al. 2007; Buno et al. 1998; Dalghous et al. 2006; Lewkowicz et al. 2005; Natah et al. 2000). An increased Th1 activity in aphthous lesions has been confirmed by cDNA microarray study that revealed more intense expression of Th1-related genes (Borra et al. 2004). However, elevated levels of IL-4 and IL-5 were also demonstrated in RAU, while IL-10 production appeared to be unaffected or decreased (Buno et al. 1998; Dalghous et al. 2006; Lewkowicz et al. 2005). Recent report has also described the increased expression of chemokine RANTES and chemokine receptors CCR3 (linked with Th2 cells), CCR5 and CXCR3 (linked with Th1 cells) in aphthous ulcers (Dalghous et al. 2006). These findings together suggest a mixed Th1/Th2 response in RAU.
T helper cell subtypes, Th1 and Th2, originate from common naive precursor cells in response to antigen and cytokine stimulation. Th cells are functionally divided according to their cytokine profiles and type of mediated immune reaction. It is well recognized that disturbances in the balance between Th1 and Th2 responses can promote immune-mediated diseases. Enhanced Th2 response is involved in atopic diseases, such as asthma, whereas a dominating Th1 response is implicated in chronic autoimmune diseases, like type 1 diabetes or rheumatoid arthritis (Romagnani 1996). Recent studies have provided evidence for a third effector Th cell pathway, namely Th17, based on their production of IL-17 which is not produced by either Th1 or Th2 cells (Park et al. 2005). Th17 cells produce a range of other factors known to drive immune response, including TNF, IL-6, granulocyte–macrophage colony-stimulating factor, CXCL1 and CCL20 (Kikly et al. 2006). Proinflammatory Th17 cells appeared to be implicated in autoimmune tissue damage and had a dominant role in the induction of chronic autoimmune inflammation of the central nervous system and joints (Langrish et al. 2005).
Differentiation and expansion of CD4+ effector cells is tightly controlled by T regulatory cells. Several types of T CD4+ regulatory cells have been described including IL-10 producing T regulatory-1 (Tr1) cells, transforming growth factor (TGF)-β secreting Th3 cells and CD4+CD25+FOXP3+ regulatory cells. Tr1 cells exert their suppressive function mainly through IL-10 release that interferes with CD28 and inducible costimulator costimulatory signals (ICOS), and induces suppressor of cytokine signaling (SOCS) molecules (Taylor et al. 2007). Th3 regulatory cells are able to induce mucosal tolerance by migration to lymphoid tissues or target organs and suppression of immune responses through TGF-β release (Faria and Weiner 2006; Weiner 2001).
To better understand the mechanisms driving the pathogenesis of RAU, it is important to elucidate what is happening at the site of inflammation. Therefore, to address the relative contribution of different Th pathways in the pathogenesis of RAU, we evaluated the expression of genes that are associated with Th cell responses in oral ulcers form RAU patients, and for comparison, oral tissues from healthy individuals.
Materials and Methods
Patients and Samples
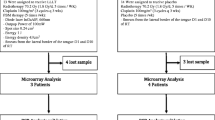
The study population consisted of 15 RAU patients (7 men, 8 women; mean age: 33.2 ± 5.24 years) who did not have any other systemic or inflammatory diseases and 12 healthy individuals, matched for age and sex (5 men, 7 women; mean age: 31.5 ± 6.35 years). A full blood cell count, red blood cell folate, serum levels of vitamin B12 and ferritin were performed to rule out a possible underlying haematological or gastrointestinal disorder. All RAU patients and controls, recruited from the outpatient clinic of the Department of Periodontology and Oral Medicine, Medical University (Lodz, Poland), were non-smokers and did not take any medication during the previous 2 months. The diagnosis of RAU was based on accepted clinical criteria (Porter and Scully 1999). All patients included in this study have been investigated in our clinic during previous episodes of ulceration that helped us to rule out a possible systemic cause. RAU patients had minor aphthous lesions that recurred at least one time per month during the six-month period prior to the study. Patients did not receive any treatment and their lesions healed spontaneously. Excisional mucosal biopsies were taken from healthy individuals and patients in the active stage of the disease (2–3 day-old ulcers). Normal non-keratinized lip or alveolar lining mucosa was taken during frenuloplasty or vestibuloplasty. Aphthous lesions were biopsied from the lip or buccal mucosa. The experimental protocol was approved by the Ethics Committee of Medical University of Lodz, and informed consent was obtained from all participants of the study.
RNA Isolation and cDNA Transcription
Total RNA was isolated from mucosal tissue with the use of Trisol (Invitrogen) and RNeasy Mini Kit (Qiagen, USA) according to the manufacturer’s instructions, and treated with RNase-free DNase I (Qiagen, USA) to remove contaminating genomic DNA. One μg of the total RNA was reverse transcribed to cDNA with random hexamers and M-MMLV reverse transcriptase using ReactionReady™ First Strand cDNA Syntesis Kit (SuperArray Bioscience Corporation, Frederick, USA).
Multiple Gene Profiling Microarray
Gene expression was analyzed using Human Th1-Th2-Th3 RT2 Profiler PCR Array (SuperArray, USA). cDNA was amplified in the presence of 84 specific primers (RefSeq accession numbers presented in Table 1), coated in 96-well microtiter plates on a Bio-Rad iCylcer® according to the following program: 95°C, 10 min (activation of HotStart DNA polymerase); 50 cycles of (95°C, 15 s; 60°C, 60 s). Separate samples from RAU individuals and controls were measured in a single run. We used RT2 Real-Time™ SYBR Green/PCR Master Mix (SuperArray, USA) that contains all of the reagents and buffers required for qRT-PCR. The mean expression levels of the following housekeeping genes were used for the normalization of the cDNA samples: hypoxanthine phosphoribosyltransferase 1, β-actin and glyceraldehyde-3-phosphate dehydrogenase.
Analysis of SOCS-3 mRNA Using Quantitative Real-Time RT-PCR
All the reagents were provided by SuperArray, USA. cDNA was amplified in the presence of specific primers for SOCS-3 (NM_003955.3) in 96-well microtiter plates on a Bio-Rad iCylcer® according the following program: 95°C, 15 min (activation of HotStart DNA polymerase); 50 cycles of (95°C, 30 s; 55°C, 30 s; and 72°C, 30 s). Separate samples from RAU individuals and controls were measured in triplicate. As a positive control cDNA synthesized from Human XpressRef™ Universal Reference Total RNA was used. Specificity of the reaction was checked by melting curve analysis, and relative expression of the genes was determined by the means of software program supplied by BioRad, USA.
Statistics
Data from real-time PCR were calculated using the ΔΔCt method and the PCR Array Data Analysis Template v3.0 (SuperArray, USA) as previously described (Hansel et al. 2008).
The fold differences in relative gene expression between normal oral mucosa and aphthous ulcers were calculated according to the formula:
where GOI is the gene of interest, HKG the housekeeping gene, C t the threshold cycle; RAU–aphthous ulcers; Normal–mucosa of healthy individuals. ΔΔC t is equal to ΔC t (RAU) − ΔC t (normal).
Statistical significance of differences among the groups was determined by the-Student’s t test (for normal distribution and equal variances), Cochran Q test (for normal distribution and unequal variances) or Wald-Wolfowitz runs test (for non parametric distribution), following calculation of the mean ± SD of each gene for both groups. The verification of normal distribution and analysis of variances were made using the Kolmogorov–Smirnov test and the Fisher’s test. p ≤ 0.05 was considered as the significant difference.
Results
The gene expression results identify one down-regulated and 28 up-regulated genes (p ≤ 0.05) in aphthous ulcers compared to healthy mucosa (Table 1). Further seven genes demonstrated at least a 3-fold difference in expression between aphthous tissue and normal tissue, but p values did not reach statistical significance. In this case, up-regulation was observed in five genes, while two genes appeared to be down-regulated in the aphthous ulcer samples.
A subset of eight genes represented chemokines and their receptors (Table 1). CCL7, CCR2 and CCR3 were significantly up-regulated (p < 0.001, p = 0.044 and p = 0.009 respectively). Further three genes demonstrated a non-significant difference of at least 3-fold: the genes for CCR4 and CCR5 were up-regulated, while CCL5 was down-regulated.
Another predominant functional group consisted of genes coding for cytokines, cytokine-related ligands, growth factors and their receptors. Significant up-regulation was observed in eight genes: TNF (p = 0.034), IFN-γ (p = 0.004), IL-6 (p = 0.047), IL-15 (p = 0.013), IL-18R (p = 0.045), INHBA (p = 0.027), CSF-2 (p < 0.001) and IRF1 (p = 0.032). Further, two genes demonstrated a non-significant up-regulation of at least 3-fold: IL-17α and IL-18.
A total of nine genes related to cell receptors and costimulatory molecules had significantly different level of expression in the aphthous ulcers than in the normal mucosa tissues, with eight genes showing up-regulation: CD4 (p = 0.034), CD40L (p = 0.045), CD80 (p = 0.033), CD86 (p = 0.017), ICOS (p = 0.040), CTLA-4 (p = 0.042), IGSF6 (p = 0.013) and Toll-like receptor (TLR)6 (p = 0.033) and one gene showing down-regulation: CD28 (p = 0.008). Additionally, the expression of CD27 mRNA was 5.6 times lower in ulcerative tissues, but the difference was not statistically significant.
A subset of 31 genes represented transcription factors and signaling molecules. Up-regulation was shown in nine genes: JAK2 (p = 0.028), LAT (p = 0.033), NFATC1 (p = 0.017), NFATC2IP (p = 0.007), PTPRC (p = 0.012), STAT1 (p = 0.016), STAT4 (p = 0.009), SOCS-1 (p = 0.021) and SOCS-3 (p = 0.012). We also demonstrated 3.1-fold up-regulation of T-bet, but the difference was not statistically significant.
Discussion
We have conducted a gene expression profiling using Th1-Th2-Th3 RT2 Profiler PCR Array to compare the relative expression of genes involved in Th cell responses in aphthous ulcers from RAU patients and non-keratinized mucosa from healthy individuals. Aside from analysis of Th1, Th2, Th3 and Th17-related genes, the PCR array allowed us to have an insight in wider aspects of immune regulation in RAU. Additionally, we performed a separate analysis of SOCS-3 mRNA expression to better determine immunoregulatory mechanisms that help to maintain a local and self-limited character of aphthous ulcers.
In this study we demonstrated that genes up-regulated in aphthous ulcers predominantly encoded factors associated with Th1 polarization such as IFN-γ and TNF. Elevated amounts of IFN-γ and TNF in RAU both at mRNA and protein were consequently demonstrated in previous studies (Albanidou-Farmaki et al. 2007; Buno et al. 1998; Dalghous et al. 2006; Lewkowicz et al. 2005; Natah et al. 2000). IFN-γ, primarily produced by Th1 lymphocytes and NK cells, not only stimulate cytotoxic immune responses, but also promotes Th1 cells differentiation and inhibit Th2 polarizations. The predominance of Th1 immune response is further confirmed by elevated levels of mRNA for transcriptional factors IRF1, STAT-1 and STAT-4. However, other Th1-related genes such as IL-2 or IL-12 were not up-regulated in our study, which is in dissonance with the previous investigation (Buno et al. 1998; Dalghous et al. 2006). These discrepancies may be explained by application of different techniques for cytokine measurement in our and other studies. Cytokines were detected at protein level using immunohistochemistry that refers to a percent of cytokine-positive cells (Dalghous et al. 2006), or at mRNA level using semi-quantitative southern blot analysis (Buno et al. 1998), while we determined mRNA levels using quantitative real-time PCR assay.
Activated Th1 lymphocytes promote cytotoxic immune response by stimulating CD8+ Tc cells and monocytes. Cytotoxity may be further supported by IL-6, IL-15 and CSF-2 that appeared to be up-regulated in aphthous ulcers. IL-15, which is mainly produced by dendritic cells (DCs) and monocytes/macrophages, is a strong inducer of NK cell differentiation. Thus, ulcer formation in RAU may result not only from Tc cell but also from NK cell cytotoxity. The importance of IL-15 in RAU pathogenesis is additionally supported by the recent findings showing an increased IL-15 serum level in RAU patients (Curnow et al. 2008).
In our study Th2-related genes were not up-regulated. No differences in IL-4, IL-5, IL-9, IL-10, IL-13, STAT-6, GATA-3, IRF4 or TNFSF4 mRNA expression were seen between RAU and healthy tissues. These findings are partially in agreement with the previous investigation. It was demonstrated that IL-4 and expression in RAU is comparable to healthy mucosa (Dalghous et al. 2006), or increased in aphthous ulcers (Buno et al. 1998). IL-10 expression was reported to be similar in RAU and healthy mucosa (Buno et al. 1998; Dalghous et al. 2006) or decreased in RAU (Miyamoto et al. 2008).
As Th3 cells are known for the production of large amounts of TGF-β, and their development is mainly dependent on TGF-β, we concluded based on the low expression of TGF-β mRNA that Th3 regulatory cells are not induced during inflammatory response in RAU. In spite of low TGF-β mRNA expression in RAU, we demonstrated other features of negative immune regulation such as elevated levels of CTLA-4, SOCS-1 and SOCS-3, and decreased levels of CD28 mRNA. Considering that aphthous biopsies were taken on the second or third day after formation of ulcers, activation of genes related to immune suppression was a surprising finding. The induction of suppressive mechanisms during an early immune response in aphthae may explain a self-limited character of aphthous ulcers that usually appear as small <1 cm lesions that heal within 7–10 days. However, it is not clear how the suppression is triggered. It is unlikely dependent on the action of CD4+CD25+ T regulatory cells, as our previous study showed that only one ulcer biopsy of eight was positive for FOXP3 mRNA (Lewkowicz et al. 2008).
Analysis of cytokine genes such as IL-17 and IL-23 that are associated with Th17 cell development and function showed their unchanged expression in RAU compared to normal tissue. Thus, Th17 cell population seems not to be involved in RAU-associated inflammatory response.
The majority of lymphocytes present in the aphthous ulcers are T CD4+ and CD8+ cells that are encountered in similar proportions (Dalghous et al. 2006). We have analyzed CD4 expression only in our study, and demonstrated its 27-fold up-regulation in aphthous ulcers. Analysis of gene expression for costimulatory molecules showed up-regulation of CD40L and ICOS that are present on activated lymphocytes. Additionally, increased expression of CD80, CD86 and IGSF6 in aphthous ulcers, costimulatory molecules that are related to DCs, may point out to the antigen uptake by DC and their maturation.
Lymphocyte migration from peripheral lymphoid tissue to the site of inflammation is possible due to expression of chemokine receptors and their ligands. CXCR3 (chemokine receptor for IP-10 and MIG) and CCR5 (chemokine receptor for MIP-1 and CCL5) are predominantly expressed on the surface of Th1 polarized T cells (Sallusto et al. 1998). Despite the evidence that the expression of CXCR3 and CCR5 is up-regulated in RAU on protein level (Dalghous et al. 2006), we failed to detect the considerable increase in mRNA expression of both CXCR3 and CCR5. Further, we demonstrated the increased expression of CCR2 and CCR3 (linked with Th2 cells) that was in agreement with the previous immunohistochemical study (Dalghous et al. 2006). We also found a 38-fold up-regulation of CCL7 that is among the most pleiotropic chemokines since it activates all major leukocyte classes by binding to CCR1, CCR2 and CCR3, and can be produced by different cell types, including fibroblasts, epithelial cells and monocytes (Menten et al. 1999, 2001). Our findings indicate the engagement of CCL7 and its receptors CCR2 and CCR3 in immune cell recruitment in RAU that unexpectedly highlights the role of Th2 cells. These findings might be explained by the stage at which the biopsy was taken. During the pre-ulcerative stage, the mRNA levels of CXCR3 and CCR5 might have been higher, as during this stage inflammatory cells start to migrate to the site of inflammation, while 2–3 days later the inflammatory response would subside. Therefore, transcription of CXCR3 and CCR5 will drop, while at protein level these receptors would still be detected. On the contrary, at the 2–3 day of ulcer Th2 cells may appear to attenuate the inflammatory reaction.
Another major observation made in our study is the significant up-regulation of TLR6 mRNA in RAU. TLRs are expressed by the variety of cells such as keratinocytes, fibroblasts, endothelial cells, DCs, macrophages, neutrophils (Miyake 2007). TLR6 is responsible for the recognition of different structures of Gram-positive bacteria that are abundant in the oral cavity and activation of Th1-like immune response (Nakao et al. 2005). Additionally, it seems that TLR6 overexpression did not only result from the bystander activation, as TLR4, that is responsible for the recognition of Gram-negative bacteria, was not up-regulated in RAU. Thus, we may speculate that overexpression of TLR6 in the oral mucosa may lead to excessive immune response towards commensals. Indeed, some previous studies suggested the role of Gram-positive bacteria in RAU pathogenesis (Hasan et al. 2002; Sun et al. 2002). More recently, an impaired signaling through TLR2 has been demonstrated in RAU patients which may inhibit Th2-type immune response and, in consequence, promote an abnormal Th1-type immune response (Borra et al. 2009).
In conclusion, we showed that Th1-associated genes are overexpressed in RAU in the absence of Th3- or Th17-type gene up-regulation. The role of Th2 cells in RAU pathogenesis remains unclear as the only increased marker of their presence demonstrated in our study was CCR3. The data also suggest that the acute inflammation in RAU is efficiently neutralized by simultaneous induction of anti-inflammatory response that promote resolution of inflammation and tissue healing. Further comparisons of the expression of most crucial T cell-related factors in aphthous ulcers using immunohistochemistry may reveal the specific pathways of the immune response that are responsible for ulcer formation.
References
Albanidou-Farmaki E, Markopoulos AK, Kalogerakou F et al (2007) Detection, enumeration and characterization of T helper cells secreting type 1 and type 2 cytokines in patients with recurrent aphthous stomatitis. Tohoku J Exp Med 212:101–105
Borra RC, Andrade PM, Silva ID et al (2004) The Th1/Th2 immune-type response of the recurrent aphthous ulceration analyzed by cDNA microarray. J Oral Pathol Med 33:140–146
Borra RC, de Mesquita Barros F, de Andrade Lotufo M et al (2009) Toll-like receptor activity in recurrent aphthous ulceration. J Oral Pathol Med 38:289–298
Buno IJ, Huff JC, Weston WL et al (1998) Elevated levels of interferon gamma, tumor necrosis factor alpha, interleukins 2, 4, and 5, but not interleukin 10, are present in recurrent aphthous stomatitis. Arch Dermatol 134:827–831
Curnow SJ, Pryce K, Modi N et al (2008) Serum cytokine profiles in Behçet’s disease: is there a role for IL-15 in pathogenesis? Immunol Lett 121:7–12
Dalghous AM, Freysdottir J, Fortune F (2006) Expression of cytokines, chemokines, and chemokine receptors in oral ulcers of patients with Behcet’s disease (BD) and recurrent aphthous stomatitis is Th1-associated, although Th2-association is also observed in patients with BD. Scand J Rheumatol 35:472–475
Faria AM, Weiner HL (2006) Oral tolerance: Therapeutic implications for autoimmune diseases. Clin Dev Immunol 13:143–157
Hansel NN, Cheadle C, Diette GB et al (2008) Analysis of CD4 + T-cell gene expression in allergic subjects using two different microarray platforms. Allergy 63:366–369
Hasan A, Shinnick T, Mizushima Y et al (2002) Defining a T-cell epitope within HSP 65 in recurrent aphthous stomatitis. Clin Exp Immunol 128:318–325
Jurge S, Kuffer R, Scully C et al (2006) Mucosal disease series. Number VI. Recurrent aphthous stomatitis. Oral Dis 12:1–21
Kikly K, Liu L, Na S et al (2006) The IL-23/Th17 axis: therapeutic target for autoimmune inflamation. Curr Opin Immunol 18:670–675
Langrish CL, Chen Y, Blumenschein WM et al (2005) IL-23 drives a pathogenic T cell population that induces autoimmune inflammation. J Exp Med 201:233–240
Lewkowicz N, Lewkowicz P, Banasik M et al (2005) Predominance of type 1 cytokines and decreased number of CD4+CD25+high T regulatory cells in peripheral blood of patients with recurrent aphthous ulcerations. Immunol Lett 99:57–62
Lewkowicz N, Lewkowicz P, Dzitko K et al (2008) Dysfunction of CD4+CD25high T regulatory cells in patients with recurrent aphthous stomatitis. J Oral Pathol Med 37:454–461
Menten P, Proost P, Struyf S et al (1999) Differential induction of monocyte chemotactic protein-3 in mononuclear leukocytes and fibroblasts by interferon-α/β and interferon-γ reveals MCP-3 heterogeneity. Eur J Immunol 29:678–685
Menten P, Wuyts A, Van Damme J (2001) Monocyte chemotactic protein-3. Eur Cytokine Netw 12:554–560
Miyake K (2007) Innate immune sensing of pathogens and danger signals by cell surface Toll-like receptors. Semin Immunol 19:3–10
Miyamoto NT, Borra RC, Abreu M et al (2008) Immune-expression of HSP27 and IL-10 in recurrent aphthous ulceration. J Oral Pathol Med 37:462–467
Nakao Y, Funami K, Kikkawa S et al (2005) Surface-expressed TLR6 participates in the recognition of diacylated lipopeptide and peptidoglycan in human cells. J Immunol 174:1566–1573
Natah S, Hayrinen-Immonen R, Heitanen J et al (2000) Immunolocalization of tumor necrosis factor-alpha expressing cells in recurrent aphthous ulcers lesions (RAU). J Oral Pathol Med 29:19–25
Park H, Li Z, Yang XO et al (2005) A distinct lineage of CD4 T cells regulates tissue inflammation by producing interleukin 17. Nat Immunol 6:1133–1141
Porter SR, Scully C (1999) Aphthous stomatitis: an overview of etiopathogenesis and management. Clin Exp Dermatol 16:235–243
Rivera-Hidalgo F, Shulman JD, Beach MM (2004) The association of tobacco and other factors with recurrent aphthous stomatitis in an US adult population. Oral Dis 10:335–345
Romagnani S (1996) Th1 and Th2 in human diseases. Clin Immunol Immunopathol 80(Pt 1):225–235
Sallusto F, Lenig D, Mackay CR et al (1998) Flexible programs of chemokine receptor expression on human polarized T helper 1 and 2 lymphocytes. J Exp Med 187:875–883
Sun A, Chia JS, Chiang CP (2002) Increased proliferative response of peripheral blood mononuclear cells and T cells to Streptococcus mutans and glucosyltransferase D antigens in the exacerbation stage of recurrent aphthous ulcerations. J Formos Med Assoc 101:560–566
Taylor A, Akdis M, Joss A et al (2007) IL-10 inhibits CD28 and ICOS costimulations of T cells via src homology 2 domain-containing protein tyrosine phosphatase 1. J Allergy Clin Immunol 120:76–83
Weiner HL (2001) Induction and mechanism of action of transforming growth factor-beta-secreting Th3 regulatory cells. Immunol Rev 182:207–214
Acknowledgments
We thank prof. Maciej Tarkowski for his help with the mRNA analysis. This work was supported by the grants of the Ministry of Science and Higher Education (Poland) N N402 445 33 and N N401 1569 33.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Lewkowicz, N., Kur, B., Kurnatowska, A. et al. Expression of Th1/Th2/Th3/Th17-Related Genes in Recurrent Aphthous Ulcers. Arch. Immunol. Ther. Exp. 59, 399 (2011). https://doi.org/10.1007/s00005-011-0134-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00005-011-0134-1