Abstract
Background
High levels of Aβ in the cerebral cortex distinguish demented Alzheimer’s disease (AD) from nondemented elderly individuals, suggesting that decreased amyloid-beta (Aβ) peptide clearance from the brain is a key precipitating factor in AD.
Materials and Methods
The levels of Aβ in brain and plasma as well as apolipoprotein E (ApoE) in brain were investigated by enzyme-linked immunosorbent assay (ELISA) and Western blotting at various times during the life span of the APP23 transgenic (Tg) and control mice. Histochemistry and immunocytochemistry were used to assess the morphologic characteristics of the brain parenchymal and cerebrovascular amyloid deposits and the intracellular amyloid precursor protein (APP) deposits in the APP23 Tg mice.
Results
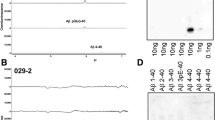
No significant differences were found in the plasma levels of Aβ between the APP23 Tg and control mice from 2–20 months of age. In contrast, soluble Aβ levels in the brain were continually elevated, increasing 4-fold at 2 months and 33-fold in the APP23 Tg mice at 20 months of age when compared to the control mice. Soluble Aβ42 was about 60% higher than Aβ40. In the APP23 Tg mice, insoluble Aβ40 remained at basal levels in the brain until 9 months and then rose to 680 µg/g cortex by 20 months. Insoluble Aβ40 was negligible in non-Tg mice at all ages. Insoluble Aβ42 in APP23 Tg mice rose to 60 µg/g cortex at 20 months, representing 24 times the control Aβ42 levels. Elevated levels of ApoE in the brain were observed in the APP23 Tg mice at 2 months of age, becoming substantially higher by 20 months. ApoE colocalized with Aβ in the plaques. Beta-amyloid precursor protein (βAPP) deposits were detected within the neuronal cytoplasm from 4 months of age onward. Amyloid angiopathy in the APP23 Tg mice increased markedly with age, being by far more severe than in the Tg2576 mice.
Conclusions
We suggest that the APP23 Tg mouse may develop an earlier blockage in Aβ clearance than the Tg2576 mice, resulting in a more severe accumulation of Aβ in the perivascular drainage pathways and in the brain. Both Tg mice reflect decreased Aβ elimination and as models for the amyloid cascade they are useful to study AD pathophysiology and therapy.







Similar content being viewed by others
References
Lue LF, Kuo YM, Roher AE, et al. (1999). Soluble amyloid beta peptide concentration as a predictor of synaptic change in Alzheimer’s disease. Am. J. Path. 155: 853–862.
McLean CA, Cherny RA, Fraser FW, et al. (1999). Soluble pool of Abeta amyloid as a determinant of severity of neurodegeneration in Alzheimer’s disease. Ann. Neurol. 46: 860–866.
Nicholson C, Sykova E. (1998). Extracellular space structure revealed by diffusion analysis. Trends Neurosci. 21: 207–215.
Cserr HF, Harling BC, Ichimura T, Knopf PM, Yamada S. (1990). Drainage of cerebral extracellular fluids into cervical lymph: An afferent limb in brain/immune system interactions. Fernstrom Foundation Series 14: 413–420.
Zhang ET, Richards HK, Kida S, Weller RO. (1992). Directional and compartmentalised drainage of interstitial fluid and cerebrospinal fluid from the rat brain. Acta Neuropathogica 83: 233–239.
Weller RO. (1998). Pathology of cerebrospinal fluid and interstitial fluid of the CNS: significance for Alzheimer disease, prion disorders and multiple sclerosis. J. Neuropathol. Exp. Neurol. 57: 885–894.
Vinters HV, Wang ZZ, Secor DL. (1996). Brain parenchymal and microvascular amyloid in Alzheimer’s disease. Brain Pathol. 6: 179–195.
Olafsson I, Thorsteinsson L, Jensson O. (1996). The molecular pathology of hereditary cystatin C amyloid angiopathy causing brain hemorrhage. Brain Pathol. 6: 121–126.
Ghetti B, Piccardo P, Frangione B, et al. (1996). Prion protein hereditary amyloidosis: Parenchymal and vascular. Semin. Virol. 7: 189–200.
Revesz T, Holton JL, Doshi B, Anderton BH, Scaravilli F, Plant GT. (1999). Cytoskeletal pathology in familial cerebral amyloid angiopathy (British type) with non-neuritic amyloid plaque formation. Acta Neuropathol. 97: 170–176.
Mead S, James-Galton M, Revesz T, et al. (2000). Familial British dementia with amyloid angiopathy: early clinical, neuropsychological and imaging findings. Brain 123: 975–991.
Weller RO, Massey A, Newman TA, Hutchings M, Kuo YM, Roher AE. (1998). Cerebral amyloid angiopathy: amyloid beta accumulates in putative interstitial fluid drainage pathways in Alzheimer’s disease. Am. J. Pathol. 153: 725–733.
Kuo YM, Kokjohn TA, Beach TG, et al. (2001). Comparative analysis of Aβ chemical structure and amyloid plaque morphology of APP23 transgenic mice. J. Biol. Chem. 276: 12991–12998.
Roses AD. (1996). Apolipoprotein E alleles as risk factors in Alzheimer’s disease. Annu. Rev. Med. 47: 387–400.
Kuo YM, Crawford F, Mullan M, et al. (2000). Elevated Aβ and apolipoprotein E in AβPP transgenic mice and its relationship to amyloid accumulation in Alzheimer’s disease. Mol. Med. 6: 430–439.
Holmquist L, Carlson K. (1977). Selective extraction of human serum very low density apolipoproteins with organic solvents. Biochem. Biophys. Acta 493: 400–409.
Dolphin PJ. (1980). Organic extraction and preparative isolectricfocusing of rat serum apolipoproteins. FEBS Lett. 117: 252–258.
Dolphin PJ, Wong L, Rubinstein D. (1978). A comparison of some immunological characteristics of very low density lipoproteins of normal and hypercholesterolemic rat sera. Can. J. Biochem. 56: 673–683.
Beach TG, Tago H, Nagai T, Kimura H, McGeer PL, McGeer EG. (1987). Perfusion-fixation of the human brain for immunohistochemistry: comparison with immersion-fixation. J. Neurosci. Meth. 19: 183–192.
Mehta PD, Dalton AJ, Mehta SP, Kim KS, Sersen EA, Wisniewski HM. (1998). Increased plasma amyloid Aβ protein 1–42 levels in Down syndrome. Neurosci. Lett. 241: 13–16.
Ishii T, Kametani F, Haga S, Sato M. (1989). The immunohistochemical demonstration of subsequences of the precursor of the amyloid A4 protein in senile plaques in Alzheimer’s disease. Neuropathol. Appl. Neurobiol. 15: 135–147.
Gouras GK, Tsai J, Naslund J, et al. (2000). Intraneuronal Aβ 42 accumulation in human brain. Am. J. Pathol. 156: 15–20.
Wilson CA, Doms RW, Lee VMY. (1999). Intracellular APP processing and Aβ production in Alzheimer’s disease. J. Neuropathol. Exp. Neurol. 58: 787–794.
Weller RO, Massey A, Kuo YM, Roher AE. (2000). Cerebral amyloid angiopathy: accumulation of A beta in interstitial fluid drainage pathways in Alzheimer’s disease. Ann. NY Acad. Sci. 903: 110–117.
Shinkai Y, Yoshimura M, Ito Y, et al. (1995). Amyloid betaproteins 1–40 and 1–42(43) in the soluble fraction of extra-and intracranial blood vessels. Ann. Neurol. 38: 421–428.
Zhang ET, Inman CBE, Weller RO. (1990). Interrelationships of the pia mater and the perivascular (Virchow-Robin) spaces in the human cerebrum. J. Anat. 170: 111–123.
Kida S, Pantazis A, Weller RO. (1993). CSF drains directly from the subarachnoid space into nasal lymphatics in the rat. Anatomy, histology and immunological significance. Neuropathol. Appl. Neurobiol. 19: 480–488.
Knopf PM, Cserr HF, Nolan SC, Wu TY, Harling-Berg CJ. (1995). Physiology and immunology of lymphatic drainage of interstitial and cerebrospinal fluid from the brain. Neuropathol. Appl. Neurobiol. 21: 175–180.
Cserr HF, DePasquale M, Harling-Berg CJ, Park JT, Knopf PM. (1992). Afferent and efferent arms of the humoral immune response to CSF-administered albumins in a rat model with normal blood-brain barrier permeability. J. Neuroimmunology 41: 195–202.
Phillips MJ, Needham M, Weller RO. (1997). Role of cervical lymph nodes in autoimmune encephalomyelitis in the Lewis rat. J. Pathol. 182: 457–464.
Calhoun ME, Burgermeister P, Phinney AL, et al. (1999). Neuronal overexpression of mutant amyloid precursor protein results in prominent deposition of cerebrovascular amyloid. Proc. Nat. Acad. Sci. U.S.A. 96: 14088–14093.
Winkler DT, Bondolfi L, Herzig MC, et al. (2001). Spontaneous hemorrhagic stroke in a mouse model of cerebral amyloid angiopathy. J. Neurosci. 21: 1619–1627.
Shinkai Y, Yoshimura M, Morishima-Kawashima M, et al. (1997). Amyloid beta-protein deposition in the leptomeninges and cerebral cortex. Ann. Neurol. 42: 899–908.
Guenette SY, Tanzi RE. (1999). Progress toward valid transgenic mouse models for Alzheimer’s disease. Neurobiol. Aging 20: 201–211.
Acknowledgments
This study was partially supported by The State of Arizona Alzheimer’s Disease Research Center and by the National Institutes of Health (AG-17490).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kuo, YM., Beach, T.G., Sue, L.I. et al. The Evolution of Aβ Peptide Burden in the APP23 Transgenic Mice: Implications for Aβ Deposition in Alzheimer Disease. Mol Med 7, 609–618 (2001). https://doi.org/10.1007/BF03401867
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03401867