Abstract
Anticonvulsant hypersensitivity syndrome (AHS) is a rare and potentially fatal reaction that develops in susceptible patients following exposure to certain drugs, including aromatic anticonvulsants. Because of its ill-defined clinical picture and resemblance to other diseases, the diagnosis of AHS is often difficult and requires a safe and reliable diagnostic test. Other than systemic rechallenge, which is not always ethically permissible and has its own limitations, no reliable diagnostic test is available for this type of disorder. This systematic review attempts to evaluate the usefulness of the available in vitro tests in the diagnosis of AHS — namely, the lymphocyte transformation test (LTT) and the lymphocyte toxicity assay (LTA) — and to examine the different technical aspects of these tests that may contribute to their performance. We included studies in which aromatic anticonvulsant drugs were the likely causes of the hypersensitivity reaction and either the LTT or the LTA was used to aid the diagnosis of AHS. Analysis of original publications from 1950 to the last week of March 2009 and cited in PubMed, MEDLINE and EMBASE has revealed that there are numerous factors affecting the final result of the test, including the following: the timing of the test after exposure; the clinical manifestation of the reactions; the specific drug; and the test procedure and read-out system. In vitro diagnostic tests have the advantage over in vivo tests of being safe to use; however, in vitro tests for the diagnosis of AHS are not well standardized and their sensitivity and specificity are not yet determined. From the reviewed literature, the sensitivity of the LTT and the LTA seem to be around 70% and 90%, respectively, and the positive and negative predictive values of the tests in highly imputable cases are quite high. However, the lack of a gold-standard diagnostic test to prove drug culpability, along with the paucity of large-scale studies, precludes accurate determination of the epidemiological characteristics of these tests. It appears that without further understanding of the mechanisms underlying the pathophysiology of AHS, and how specific drugs and metabolites differentially affect these mechanisms, the development of more reliable tools for AHS diagnosis will be compromised. Consequently, in the absence of further research, the predictability of these tests will remain questionable and they are unlikely to be utilized on a large scale.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1. Background
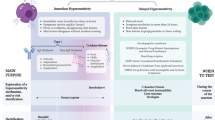
Anticonvulsant hypersensitivity syndrome (AHS), also known as drug hypersensitivity syndrome or drug rash with eosinophilia and systemic symptoms (DRESS), is a type B (‘bizarre’) adverse drug reaction (ADR) that develops in susceptible patients following exposure to certain drugs, including aromatic anticonvulsants (figure 1).[1,2] Although lacking a defined clinical picture, AHS is typically associated with the development of skin rash, fever, and internal organ dysfunction that may include blood discrasias, hepatitis, nephritis, myocarditis, thyroditis, and interstitial pneumonitis and encephalitis.[3] The pathophysiological mechanisms underlying AHS are not well understood; however, it is believed to be immune mediated in general and involve generation of electrophilic reactive metabolites that react covalently with macro-molecules to form immunogenic adducts able to activate the immune system.[4,5] The accurate incidence of AHS is unknown due to underreporting, but it has been estimated to range from 1 in 1000 to 1 in 10 000 in patients newly exposed to aromatic anticonvulsants.[6] While the disorder is rare, it is potentially fatal and represents a clinical dilemma to treating doctors. Diagnosis of AHS is challenging, as a reliable and safe diagnostic test is not available to confirm causality or identify the culprit drug. A number of in vivo and in vitro tests have been devised and used to aid the diagnosis of AHS.[7,8] These include skin tests (patch test, prick test, intradermal test), the lymphocyte transformation test (LTT) and the lymphocyte toxicity assay (LTA).[9] The use of patch tests in the diagnosis of AHS has been reviewed recently.[10] This systematic review is an attempt to evaluate the utility of in vitro tests used for the purpose of diagnosis of the T-cell-mediated type IV delayed AHS reactions. Other tests used for other types of allergic reactions (e.g. IgE measurement, radioallergosorbent test, basophil activation test) are not reviewed here.
In vitro diagnostic tests have the advantage over in vivo tests (patch test and rechallenge) of bearing no potential harm to patients. A number of in vitro diagnostic tests have been used to aid the diagnosis of delayed-type drug hypersensitivity reactions;[7,8,11–13] however, their true value is yet to be defined. Among these tests are those that utilize peripheral blood mononuclear cells (PBMCs) as target cells, including the LTT and the LTA. Unfortunately, these techniques require expensive equipment and sophisticated laboratories as well as specialized experience with biochemical and molecular methods, so only a few centers are sufficiently equipped to perform them. Hence, these methods, although successfully employed as research tools, have not been successfully translated into diagnostic tests.[14,15] The specific aims of the current systematic review are 4-fold: (i) to evaluate the use of LTT and LTA in the diagnosis of AHS; (ii) to describe the advantages and limitations of these tests; (iii) to discuss different technical aspects of both tests with the scope of possible improvement; and (iv) to identify potential future work to increase the diagnostic value of these tests. The overall objective of this review is to identify gaps that must be closed to allow these tests to become validated, mainstream diagnostic tools.
Leukocytes are present in peripheral blood at densities of 5–7 × 103 cells/mm3; 20–50% of these cells are lymphocytes, whereas 2×10% are monocytes. Lymphocytes are favored as a model for investigation of immune-mediated diseases because of their unique characteristics, which include that (i) they are easily obtained at adequate density; (ii) they play a key role in the immune system by orchestrating different elements of the immune response, and thus represent the state of the immune system in the specific patient; (iii) they are metabolically active and express most of the enzymes required for drug detoxication; and (iv) individual genetically based defects in the expression or activity of these detoxication enzymes are phenotypically expressed in lymphocytes.[1]
1.1 Isolation of Peripheral Blood Mononuclear Cells
Several methods have been used to isolate lymphocytes from heparinized whole blood, including the gelatine method, passage through glass wool or beads, and magnetic separation after cellular ingestion of carbonyl iron.[16] However, the most successful and currently most used method is that developed by Böyum.[17] This method involves centrifugation of diluted blood samples through a gradient of Ficoll®, a synthetic high-molecular-weight polymer of sucrose that is highly branched and has low intrinsic viscosity. This method permits recovery of 60% ± 20% of lymphocytes from original blood samples, with cell viability >90%. This technique allowed the use of isolated PMBCs in tests such as the LTT and LTA.
1.2 The Lymphocyte Transformation Test (LTT)
The in vitro lymphocyte transformation phenomenon was first described during the late 1950s. In short, human peripheral blood leukocytes (PBLs) differentiate in short-term primary cultures, forming plasts. This effect was later attributed to the presence of a constituent (phytohemagglutinin [PHA]) of a plant extract from red kidney beans (Phaseolus vulgaris) that is used to isolate blood peripheral leukocytes.[18] PHA causes erythrocytes to aggregate and sediment, allowing leukocytes to separate from whole blood preparations.[19,20] In a later report, Nowell[21] demonstrated that PHA also initiates mitotic activity (transformation) in cultured human leukocytes. To show that lymphocyte behavior in vitro has an immunological basis, Pearmain et al.[22] exposed PBLs isolated from both tuberculin-sensitive and -nonsensitive patients to tuberculin in vitro. Only PBLs from tuberculin-sensitive patients showed mitotic activity, whereas cells from patients not previously exposed to the antigen showed no mitosis.
One of the first reports of using the LTT for diagnosis of drug allergy was by Holland and Mauer,[23] who evaluated the effect of phenytoin on cultured lymphocytes isolated from patients sensitive to the drug and non-sensitive (control) subjects. In these experiments, PHA used as a positive control showed non-specific stimulation of all cells sampled, whereas phenytoin stimulated only the cells from phenytoin-sensitive patients.[23] When tested with peripheral lymphocytes isolated from a sulfadiazine-sensitive patient and incubated with the culprit drug in vitro, this effect was found to be concentration-dependent.[24] In 1966, Vischer[25] replaced the lengthy visual counting of mitotic figures from fixed slides with a faster and less subjective method by measuring radio-labeled thymidine incorporation into cellular DNA as a reflection of the rate of cell division. During the late 1960s and early 1970s, a great deal of work was done by Schellekens and colleagues[26–30] to optimize the in vitro lymphocyte transformation technique.
The terms ‘lymphocyte transformation test’ (LTT), ‘lymphocyte stimulation test’ (LST), and ‘lymphocyte proliferation test’ (LPT) are interchangeably used to describe this technique. The procedure includes incubation of PBMCs isolated from drug-hypersensitive patients with the incriminated agent at non-toxic concentrations and observation of any increase in the rate of cell proliferation measured by [3H]thymidine incorporation (figure 2). The increase in cell proliferation is expressed as a ratio between proliferation of cells incubated with and without the drug (vehicle alone; control). This ratio is defined as the stimulation index (SI) and it is calculated as follows (equation 1):
where [3H]thymidine uptake is expressed in counts per minute.
Cell cultures from drug-exposed and unexposed non-sensitive individuals are also used to confirm the specificity of a potential drug effect. The final result of the test depends on several factors such as the value of background cell proliferation and the type of the drug; however, an SI of >3 is always considered indicative of a positive reaction.[31] Other endpoints for measurement of T-cell activation, such as elevation of released cytokines (using an enzyme-linked immunosorbent assay [ELISA]), have been proposed and could be a more sensitive method for detection of T-cell activation than measurement of the rate of cell proliferation.[31,32] A recent technique based on staining of intracellular proteins with carboxyfluorescein succinimidyl ester (CFSE) has been used successfully to measure T-cell proliferation in vitro.[33,34] This fluorescent dye is used to non-specifically label intracellular proteins. In cell proliferation, the intensity of the fluorescent signal is progressively decreased as the stained proteins are divided during mitosis. An increase in the number of low-fluorescence cells indicates cell proliferation that can be measured by flow cytometry.[35,36]
The LTT has been used by some investigators for diagnosis of potential drug allergy cases for more than 20 years.[37] However, its value in diagnosis and prediction of AHS remains controversial.
1.3 The Lymphocyte Toxicity Assay (LTA)
Introduced by Spielberg and colleagues[1,38–41] in the 1980s, the LTA is an in vitro test that utilizes isolated PBMCs to investigate the mechanistic pathogenesis of idiosyncratic drug reactions. The test is based on the hypothesis that drug hypersensitivity develops as a result of imbalance between generation of toxic reactive metabolites (metabolic activation or toxication) and detoxication capacity that leads to accumulation of toxic metabolites (the ‘reactive metabolite’ hypo thesis).[4,42–44] In this test, lymphocytes are used not as immunogenic cells but rather as easy-to-obtain surrogate target cells.[41] The procedure for the test entails incubation of PBMCs isolated from the patient with the culprit drug in the presence of phenobarbital-induced mouse, rat, or rabbit liver microsomal 9000 × g supernatant fraction (S9), as a source of cytochrome P450 (CYP) mono-oxygenase activity.
CYP activity in the rodent (or sometimes human) liver preparation is hypothesized to oxidize drug to its active (cytotoxic) metabolite(s). Lymphocytes contain enzymes that are required for drug detoxication, including epoxide hydrolases and glutathione S-transferases, and any genetic defect in the function of these enzymes is phenotypically expressed in these cells. The percentage of cell death is then determined using different methods for assessing cell death (e.g. trypan blue exclusion or with a tetrazolium dye; for example, by the MTT [3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide] method [figure 3]). Cell death is assumed to reflect the vulnerability of the cells to the toxic effects of the drug, which is hypothesized to indicate the susceptibility of the patient to develop hypersensitivity reactions to the parent drug and its reactive metabolite(s), presumably via differences in detoxication capacity and immune processing.
Aromatic anticonvulsants are excellent examples of metabolically activated cytotoxicants, metabolized primarily by hepatic CYP isozymes into reactive electrophilic arene oxide metabolites.[5] These unstable and highly reactive intermediate metabolites are readily detoxified by epoxide hydrolase and/or glutathione S-transferase enzymes, usually to non-electrophilic products (dihydrodiols and S-glutathione conjugates, respectively).[45,46]
Although the same cell model (isolated PBMCs) is used in both types of assay, LTT and LTA are completely different approaches to the diagnosis of AHS. Whereas the former detects the in vivo immunological generation of drug-specific T lymphocytes used as a sign of hypersensitivity, the latter detects genetic defects that lead to accumulation of toxic metabolites, which are assumed to be a major factor in the etiology of drug hypersensitivity in addition to possible differences in cell death. Because the two tests use the same cell model and have similar nomenclature, it is not uncommon for individuals to confuse the LTT for the LTA or vice versa,[47] or to use different nomenclature to describe these tests.[2,48,49]
2. Research Methodology
In order to evaluate the clinical usefulness of these tests in diagnosis of AHS, we performed a systematic literature search using three major biomedical citation databases, PubMed, EMBASE and MEDLINE without any restriction on date from their commencement to the fourth week of May 2009.
2.1 Search Strategies
Search strategy I: the search was carried out using the key words ‘anticonvulsant’ and ‘antiepileptic’ in their singular, plural, and truncated forms. These terms were also mapped to their medical subject headings (MeSH) terms. We also searched for individual aromatic anticonvulsant drugs including ‘carbamazepine’, ‘phenytoin’, ‘phenobarbital’, ‘oxcarbazepine’, ‘primidone’, ‘lamotrigine’, ‘felbamate’, and ‘zonisamide’, both as key words and as MeSH terms when available, and the option ‘explode’ was used. The obtained results were combined using ‘or’.
Search strategy II: In parallel, we used as key words ‘lymphocyte toxicity assay’, ‘LTA’, ‘lymphocyte toxicity test’, ‘in vitro lymphocyte toxicity assay’, ‘in vitro lymphocyte toxicity test’, ‘lymphocyte transformation test’, ‘lymphocyte stimulation test’, ‘lymphocyte proliferation test’, ‘LTT’, ‘LST’, ‘LPT’, ‘drug-induced lymphocyte stimulation test’, and ‘DLST’. These terms were also mapped to their MeSH terms when available, and the option ‘explode’ was used.
We then combined the results of both searches (search strategies I and II) using ‘and’.
Retrieved publications were manually reviewed and the following selection criteria were applied: (i) original article written in English; (ii) study performed in human subjects; (iii) LTA or LTT used to diagnose AHS due to one or more aromatic anticonvulsant drug(s); and (iv) sufficient technical data for scientific evaluation.
Thirty-one articles from PubMed, 22 articles from MEDLINE, and 28 from EMBASE were found that met our selection criteria. The search results from the three databases were then combined and duplicates were removed. The final number of included articles from the three databases was 48. Thirty-six articles used the LTT and 12 used the LTA for the diagnosis of AHS (figure 4). Although single case reports were included in the review, none of these reports were used to calculate any of the tests’ epidemiological characteristics.
Flow chart of literature search and retrieval process. 1 The search strategies ‘Anticonvulsants’ and ‘LTA and LTT’ include all relevant medical subject headings and key words as described in section 2.1. AHS=anticonvulsant hypersensitivity syndrome; LTA=lymphocyte toxicity assay; LTT=lymphocyte transformation test.
3. Results
3.1 The LTT in the Diagnosis of Anticonvulsant Hypersensitivity Syndrome (AHS)
The use of the LTT in diagnosis of hypersensitivity to anticonvulsant drugs dates back to the early 1960s, but its use was almost always confined to experienced technicians in well equipped research centers, primarily for the purpose of investigating the mechanism of T-cell-mediated reactions rather than diagnosis of drug allergy.[14,15,50–53] In addition, because of its low laboratory-to-laboratory reproducibility[31,54] and difficulty in evaluating results,[31] this test cannot be described as user friendly and requires a great deal of experience for interpretation of results. For this reason, the test has not been translated into widespread clinical use. In fact, only a few research groups worldwide use this technique routinely.[31]
Table I summarizes data from original publications where the LTT has been used to investigate hypersensitivity reactions to anticonvulsants. Troost et al.[69] directly addressed the issue of LTT usefulness in AHS diagnosis They collected data from 65 patients who displayed a wide range of adverse effects of carbamazepine. They compared the performance of the patch test with the LTT and found that the LTT had a better positive predictive value than the patch test (40% and 20%, respectively). However, the inclusion criteria for the AHS cases were not well described and medical history was the only evidence that incriminated the drug. Furthermore, the low positive predictive value of the patch test for carbamazepine (20%) in this study may indicate that some of the cases that were included were not typical carbamazepine-induced hypersensitivity reactions. This is supported by the fact that only 23% of the included patients displayed systemic manifestations and that 92% of them had only some form of mild skin reaction as an adverse event.
In an attempt to determine the sensitivity and specificity of the LTT in the diagnosis of allergy to different drugs,[37] the files of 923 patients with possible hypersensitivity reactions to drugs were studied. These patients were classified based on their medical history, follow-up, and provocation tests into four groups where drug allergies were ‘definite,’ ‘probable,’ ‘less probable,’ or ‘negative’. One hundred cases were considered to have a very high probability of drug allergy, of which 78 had a positive LTT. Only 3 of these 100 cases were attributed to anticonvulsants (2 to carbamazepine and 1 to phenytoin). The two carbamazepine cases exhibited positive LTTs whereas for the phenytoin case, the LTT was negative. Although the chemistry of the drug in question appears to play a major role in determining the usefulness of the LTT, the overall specificity and sensitivity of this test in this study were found to be in the range of 85% and 76%, respectively. It is not known whether or not these numbers can be applied to anticonvulsant drugs. However, because many different factors are involved in determining the final result of the LTT as discussed below, one cannot generalize these figures to include all types of drugs taken under various conditions.
Numerous factors have been found to affect the predictive value of the LTT in the diagnosis of drug hypersensitivity reactions. These factors include the timing of the test in relation to the beginning of the reaction, the type of clinical manifestations caused by the drug, the nature of the suspected drug, and the test procedure itself.
3.1.1 Timing of the Test
Performing the LTT during an ADR may result in a high incidence of false-negative test results due to the high rate of spontaneous T-cell proliferation that does not respond to any additional in vitro stimulation (refractory period).[50,69,70] Houwerzijl et al.[79] demonstrated the relationship between the timing of the test and its outcome. Sequentially testing a number of patients with hypersensitivity reactions to carbamazepine, they showed that this refractory period may extend up to 11 weeks from the time of the adverse reaction. This effect may be due to impaired T-cell function, as the predominant T-cell mitogen, PHA, could not stimulate T cells during this period.[79] In contrast, Zakrzewska and Ivanyi[77] obtained positive results when performing LTT on six of nine patients within 2 weeks of the beginning of the adverse reaction. These authors attributed their results to the mild form of the adverse reactions (skin rash only) in their patients. In such cases, a shorter refractory period or no refractory period is expected because of the moderate degree of activation of T cells.
Although drug-specific T cells have been isolated from patients decades after the time of the reaction,[15] a positive LTT is not guaranteed if the test is performed later than 3–4 years after the reaction.[31] After remission from severe hypersensitivity drug reactions, the frequencies of circulating drug-specific T cells was estimated at between 1:250 and 1:5000 (from 1:2000 to 1:10000 for anticonvulsant drugs), and this rate does not appear to be affected by time. These frequencies were higher than the frequencies of T cells that recognize a full antigen such as tetanus toxoid.[15] It is well documented that circulating drug-specific T cells may last for years or even decades after the insult,[15,31,82] but the length of this period may vary considerably for reasons not yet understood.
In a recent study designed to investigate the effects of timing and the type of drug involved in adverse reactions on the utility of the LTT for diagnosis of drug hypersensitivity, Kano et al.[56] followed 12 patients experiencing different types of drug-induced hypersensitivity reactions (i.e. macula-papular eruption, Stevens-Johnson syndrome [SJS] and AHS or DRESS). Six patients developed AHS as a result of taking aromatic ring-containing anticonvulsants (phenytoin, carbamazepine, and phenobarbital). Only one of six patients showed a positive LTT when the tests were performed within 1 week of the onset of the reaction. However, all six patients gave positive LTT results when tested at a later time (ranging from 5 weeks to 1 year). Interestingly, patients with macula-papular eruption and SJS showed an opposite pattern where the SI levels decreased with time. In another study of one case of carbamazepine-induced hypersensitivity that involved pulmonary symptoms, fever, generalized maculopapular erythmatous skin eruptions, and eosinophilia, the LTT performed during the course of the reaction was positive (SI = 2.2). However, when the test was repeated 3 months after recovery, a negative result was obtained.[80]
In contrast, Wu et al.[14] did not find any association between the timing of the test and the strength of the response in a cohort of cases of hypersensitivity to carbamazepine. Specifically, testing a patient <1 month after the reaction resulted in a strongly positive LTT (SI up to 69.4). In the study, similar results were obtained when testing patients at 84 and 180 months after the event, similar to the results of Beeler et al.[15] at 4 and 19 months after the reaction. Houwerzijl et al.[79] showed that maximum SI values are obtained if the test is performed 10–20 weeks after the beginning of the reaction, after which the SI values start to decline over time.
It appears that during the course of the adverse reaction, drug-specific T lymphocytes go through three different stages:
-
1.
A highly reactive stage (very strong response) that shows spontaneous proliferation during which the cells do not respond to any additional in vitro stimulation.[31,56] This stage appears to last for the first 1–4 weeks after the adverse event, depending on the strength of the initial reaction.[79] Stronger reactions usually result in longer ‘refractory periods’ than weaker ones.
-
2.
An apparently long stage where drug-specific T cells can be detected in peripheral blood and are responsive to an in vitro stimulation (strong response). This stage starts at the remission of the reaction and may last for years and sometimes for decades.[31]
-
3.
A final stage, where no drug-specific T cells can be detected in peripheral blood (weak response). This does not mean that the patient is desensitized to the drug or is able to tolerate it. In fact, a severe reaction may develop again once the patient is exposed to the culprit agent.[15,31]
The so-called ‘refractory period’ has been attributed to two mechanisms: (i) the circulating peripheral T lymphocytes are at their maximum activation and do not respond to any further stimulation in the presence of the drug; and (ii) drug-specific T lymphocytes are selectively recruited to the affected target organs, leading to a deficiency of these cells in peripheral blood.[58,69,79] It has also been observed that PBMCs isolated from patients during the hypersensitivity episode are characterized by a high proliferation rate, presumably related to their recent exposure to the culprit drug (in vivo). These activated T cells cannot be further stimulated by exposure to the drug or PHA in vitro.
3.1.2 Clinical Manifestation of the Reactions
Hypersensitivity reactions to drugs can manifest in a wide range of distinct clinical symptoms, including morbilliforme or bullous exanthema, urticaria, involvement of other internal organs, fever, blood cell dyscrasia, hepatitis, nephritis, and interstitial lung disease.[61,83] Severe forms of AHS include erythema multiforme, SJS and toxic epidermal necrolysis (TEN).[84] Some of these reactions cannot be listed under any known classification of immune-mediated diseases. T-cell-mediated drug allergy can take different forms and utilize a variety of mechanisms, including activation of different clones of T cells and secretion of different types of mediators.[85] In some cases, such as in patients with drug-induced SJS, the proliferative response of the drug-specific T cells was found to be low despite the high level of secreted cytokines.[15] This can affect the ability of T-cell proliferation tests such as the LTT to detect low levels of circulating drug-specific T cells; however, in this particular context, measuring cytokine secretion as a readout system for T-cell activation can be more sensitive than the conventional LTT.[32]
A study by Neukomm et al.[61] did not find any correlation between the strength of the LTT result (SI) and the type of ADR, but showed positive LTT results for a wide variety of reactions including IgE-mediated reactions. It is quite unexpected that an in vitro test such as the LTT can give positive results in all cases where drug-induced reactions are attributed to different agents and mediated by distinct immunological mechanisms. For instance, haptens and pro-haptens such as β-lactam antibacterials require processing before they are able to activate T cells, whereas other drugs such as carbamazepine, lamotrigine, sulfamethoxazole, and their metabolites are thought to directly activate T cells through other mechanisms.[86–89]
Nevertheless, in most of the clinical syndromes associated with aromatic anticonvulsant use (e.g. generalized macula-papular exanthema, bullous reactions, multi-organ DRESS syndrome, etc.) the LTT is frequently positive.[31] As mentioned earlier, severe bullous reactions such as TEN rarely yield a positive LTT, and the reason behind this is unknown. Romano et al.[58] tested eight patients with a history of hypersensitivity reactions to carbamazepine (six patients with macula-papular exanthema, one with bullous exanthema, and one with SJS). All six cases with macula-papular exanthema yielded negative LTT results despite a positive patch test in four of them. The LTT was positive in the other two cases (bullous exanthema and SJS). The six macula-papular exanthema patients were tested within 2 years of the adverse reaction, whereas the bullous exanthema and SJS cases were tested 6 and 12 years later, respectively.[58]
The LTT detects circulating peripheral drug-specific T lymphocytes. Such aromatic anticonvulsant reactive T cells have been cloned and characterized in multiple previous studies.[14,15,51,53,57,90] If, for whatever reason, the pathophysiology of the disease does not involve a high frequency of circulating drug-specific T cells, the LTT will not confirm the diagnosis. The mediocre sensitivity of the LTT in the diagnosis of AHS (around 70%) has provoked uncertainty about the real pathophysiology of this disorder and whether it actually exists. There is increasing evidence of the heterogeneity of AHS reactions and that they might be mediated by distinct yet unidentified pathophysiology mechanisms.[43,44,91,92]
The mechanism or mechanisms by which isolated peripheral lymphocytes recognize the suspected drug are not well understood, as antigen processing does not seem to be required for T-cell activation in vitro. This can be partially explained by a relatively recently introduced paradigm, the ‘p-i’ concept. This term stands for ‘direct pharmacological interaction of drugs with immune receptors’ and assumes that a chemically inert drug can non-covalently interact with receptors on the immune cells and activate them without being a full antigen.[87] This interaction, which involves only T cells, may explain why drugs such as carbamazepine elicit only T-cell-mediated adverse effects, while haptens (β-lactam antibacterials) are able to cause all sorts of idiosyncratic reactions, including anaphylaxis. In fact, some investigators have found the LTT to be useless in the diagnosis of reactions such as pneumonia caused by minocycline, bucillamine, amoxicillin, and clindamycine[93–95] or hepatitis due to herbal medicines.[94] This is probably because these reactions were mediated by other mechanism(s). However, in cases with multiple organ involvement, including liver dysfunction, the LTT is more likely to yield positive results.[66] This suggests that several different immunological mechanisms underlie the apparent clinical manifestations.
3.1.3 The Specific Drug
The LTT has given positive results with most aromatic anticonvulsant drugs, including phenytoin, carbamazepine, oxcarbazepine, phenobarbital, lamotrigine, and zonisamide, with sensitivity ranging between 25% and 100%.[14,53,57,62,69,96] However, issues related to the chemistry and pharmacology of the tested drug may limit the outcome of the LTT. One such problem may be the solubility of the tested drug in the incubation medium. The majority of the lipophilic aromatic anticonvulsants are not water soluble and require solubilization in an organic solvent (e.g. dimethyl sulfoxide, ethanol, or propylene glycol). It is important to ensure that the final concentration of the solvent in the medium is not cytotoxic. In addition, some researchers have found that it is necessary to sonicate the drug solution to enhance its solubility.[56]
In addition, some drugs may cause non-specific activation or deactivation of PBMCs, resulting in false positive or false negative LTT results. Higher concentrations of carbamazepine or phenytoin cause cytotoxicity and kill PBMCs, an effect that may mask any expansion of lymphocytes, resulting in low SI levels (false negative). Therefore, it is essential to examine the effects of the used drug concentration on cells stimulated by the non-specific mitogen PHA.[31]
The effect of coadminstrated systemic corticosteroids on test results is controversial. Although some researchers state that systemic administration of more that 0.2mg/kg of prednisolone may interfere with the LTT,[31] others have found no such effect.[56]
3.1.4 Test Procedure and Read-Out System
The most evident pitfalls of this in vitro diagnostic test are its complicated procedure and lack of standardization.[31] Attempts to simplify the test procedure and improve its reproducibility have been described for decades;[32,34,37,55,77] however, the long-sought simple and reproducible LTT is not yet achievable. The common challenge among aromatic anticonvulsants is their need to be enzymatically activated to more reactive metabolites to elicit their presumed reactions.[42,49] This observation has led some researchers to use liver microsomes to increase the test sensitivity.[97] Others have also used ex vivo serum from healthy volunteers taking the drug.[74] However, these approaches did not improve the sensitivity of the test.
Another important aspect of the LTT is the read-out method. Traditionally, T-cell proliferation is measured by [3H]thymidine uptake, which has proven to be very reproducible. Other methods to detect T-cell activation, including measuring the synthesis and release of interleukin (IL)-5, IL-10, interferon-γ and CD69, have also been used and shown to improve the sensitivity of the test.[55,98] Others have also used increased secretion of soluble Fas ligand as a read-out or bio-marker and found this protein to be significantly increased in patients with carbamazepine-induced blistering diseases (SJS/TEN).[13,99] Granulysin is a cytolytic and proinflammatory protein secreted by activated cytotoxic T lymphocytes, natural killer (NK), and NK T cells.[100] It was shown to be a key mediator of keratinocyte apoptosis in severe bullous reactions and to be present in high concentrations in blister fluids in patients with carbamazepine- and phenytoin-induced SJS and TEN.[101] Expression of such mediators can be of clinical value in diagnosis or determining the prognosis of drug-induced bullous reactions.
3.2 The LTA in the Diagnosis of AHS
The use of the LTA in diagnosing AHS dates back to the early 1980s.[40] However, except for four major studies,[1,102–104] the lack of large-scale application is quite obvious (table II). Shear and Spielberg[1] studied 53 patients with a medical history suggesting AHS due to phenytoin, carbamazepine, or phenobarbital, as well as 49 unexposed healthy controls and 10 phenytoinexposed healthy controls. Symptoms included fever, skin rash (varying in severity from generalized exanthema to TEN), eosinophilia, atypical lymphocytosis, and internal organ involvement (liver, kidney, thyroid, or lung). The performance of the LTA as a diagnostic test in this cohort of patients was excellent, with only two false positives and one false negative result in patients with hypersensitivity reactions to phenobarbital. Naranjo et al.[104] tested 51 patients with highly likely diagnoses of AHS due to phenytoin, carbamazepine, or phenobarbital, and estimated the sensitivity and specificity of the LTA to be 99% and 75%, respectively. However, only eight drug-tolerant patients were included in the study, rendering precise determination of the specificity of the test impossible. On the other hand, the lack of a gold standard against which results of the LTA can be validated has always made these numbers merely an estimate.
In another study by Neuman et al.,[102] the LTA was used to diagnose AHS in 86 patients, 62 of whom developed an adverse reaction as a result of taking aromatic anticonvulsants. Although the inclusion criteria for the cases were not well defined, the sensitivity and specificity of the results of the LTA in the diagnosis of AHS were estimated to be 98% and 89%, respectively, and the positive and negative predictive values were found to be 90% and 64%, respectively. To evaluate cross-reactivity among old aromatic anticonvulsants (phenytoin, carbamazepine, and phenobarbital) and zonisamide, a new aromatic anticonvulsant, Neuman et al.[103] tested 20 aromatic anticonvulsant-hypersensitive patients and 20 aromatic anti-convulsant-tolerant patients, using the LTA. The tested patients had exhibited a broad spectrum of AHS manifestations, including fever, skin rash, internal organ involvement, SJS, and TEN). The authors estimated the sensitivity and specificity of the LTA in this cohort of patients to be 92.9% and 99.1, respectively.
In a technician-blinded, hospital-based controlled study, Dwivedi et al.[105] tested 11 patients with AHS due to phenytoin. Five patients had SJS, four had erythrodermic eruption, one had morbilliform eruption, and one had lichenoid eruption. The authors also tested 11 healthy and phenytoin-tolerant volunteers as controls. All 11 patients gave positive LTAs (the percentage of cell death ranged between 7% and 26% compared with 2.6% and 3.5% for controls). It is of note that in this study, cells from patients with a severe form of AHS (SJS) exhibited a higher percentage of cell death (12–26%) than those from patients with milder forms (7–13%); this was related to a greater deficiency in expression or effectiveness of detoxifying enzymes.
The LTA is simpler and has a less complicated procedure than the LTT, not requiring radioactive reagents. However, the sensitivity and specificity of the LTA in determining the culprit drug in AHS have not been extensively evaluated, mainly due to a lack of strict inclusion criteria in the reported cases. A systemic rechallenge could be definitive proof of drug culpability, but this is ethically unacceptable because of the possibility of danger to the patient.
3.2.1 Technical Considerations for the LTA
As outlined earlier, the basic principle of the LTA is to generate the presumed cytotoxic metabolite(s) of the suspected drug in vitro in the presence of the surrogate cell model, and to measure lymphocyte susceptibility to metabolite-induced cell death. This process depends largely on the test procedure and reagents used. Table III summarizes the different steps to be considered in optimizing the performance of the LTA.
For example, contamination of isolated PBMCs with platelets can affect lymphocyte function and activity in vitro[109,110] and may also modify the evaluation of cell death by the MTT method. Platelets have unusually high numbers of mitochondria (the source of the succinate dehydrogenase enzyme that converts MTT to blue formazan dye) and their presence in the medium can compromise the signal. We performed cell counting using flow cytometry of PBMC preparations freshly isolated using the Ficoll® method and found the ratio of platelets to lymphocytes after the second wash to be 100:140. These contaminated platelets are likely co-sedimented as a result of attachment to other cells. A number of methods have been introduced to prepare platelet-free PBMCs,[109,111–114] although this increases the cost and complexity of the test. On the other hand, the usage of platelets as a surrogate model in place of PBMCs could be advantageous, as platelets are easier to isolate and more abundant in peripheral blood than PBMCs. Platelets have been found to respond in the same way as PBMCs to different chemical insults, and platelets from drug-hypersensitive patients were found to be more susceptible to cell death induced by the suspected drug than platelets from healthy volunteers who had never been exposed to the drug (our unpublished data).
In addition, the in vitro metabolic activation system (liver microsomes) plays an important role in the success of the test, especially when testing drugs such as those aromatic anti-convulsants whose toxic metabolites are still unknown. Differences among species in terms of metabolic activation of drugs by CYP isozymes[115] and their relative levels of expression in untreated and induced microsomal systems should be considered when performing the LTA. The incubation conditions of the surrogate cells with the suspected drug and liver microsomes should be standardized. The pH value of the medium has a tremendous effect on the viability of PBMCs. We have found that a small variation in the washing buffer pH can result in a ~40% decrease in cell viability of isolated PBMCs (unpublished data); therefore, the pH should be adjusted to 7.2–7.4 just prior to performing the test. Other additives such as fetal bovine serum are also essential to the viability of the cells and should be standardized.
Cell death is the ultimate response of vulnerable cells exposed to the offending drug as an insult. However, it is a gross measure of the cellular and subcellular events that occur and may vary depending on the tested drug and the incubation conditions.[116] In this regard, cell death is unlikely to be the best endpoint to indicate cell response to a toxic insult. Finally, defining and obtaining the ultimate in vivo toxic metabolite(s) of the offending drugs and their direct in vitro testing will have a strong impact on the predictability of the results of the LTA, as the complicated metabolic activation step(s) will be eliminated. This has been proven to be true in testing patients who are hypersensitive to sulfonamides, where the reactive metabolites can be tested directly to assist in test validation.[117]
4. Discussion
AHS is a rare but potentially lethal disorder. One of the most challenging aspects of this disease is the difficulty of establishing a solid diagnosis in a timely manner.[2,8,118–121] Lack of a diagnosis or misdiagnosis may result in increased morbidity, increased mortality, and extended hospitalization.[122,123] Between 10% and 27% of patients with epilepsy discontinue their first antiepileptic drug because of the development of adverse reactions.[124] Aromatic anticonvulsant drugs such as phenytoin, carbamazepine, phenobarbital, and lamotrigine are linked to a relatively high risk of development of hypersensitivity reactions.[125] Carbamazepine was found to be the most common cause of severe forms of AHS (i.e. SJS and TEN).[126]
The diagnosis of AHS entails two main processes: first, establishing the diagnosis of the hypersensitivity reaction, usually from a series of clinically similar differential diagnoses; and secondly, identifying the culprit drug, potentially among a number of other concomitantly prescribed, innocent drugs. Numerous diagnostic tests are available and have been attempted for the diagnosis of drug hypersensitivity reactions; however, their epidemiological qualities are dependent on the type of reaction (immediate vs delayed reactions) and type of drug, and choosing the best test for a specific drug or drug class can be challenging.[7,8,37]
The LTT and LTA are two different approaches for AHS diagnosis and may complement each other as a battery of diagnostic tests that can also include in vivo tests such as the patch test and systemic rechallenge. The LTA may predict the susceptibility of patients to develop AHS based on a genetic deficiency in their cellular defense systems against toxic reactive drug metabolite(s), whereas the LTT may confirm the development of AHS by detecting peripherally circulating drug-specific T cells. It is evident that these tests lack standardization and large-scale validation to determine their appropriateness in terms of sensitivity and specificity in addition to positive and negative predictive values.[31,37,48]
The sensitivity and specificity of the LTT in the diagnosis of drug allergy have been estimated to range from 56% to 78% and from 85% to 93%, respectively, although these estimates are generally based on cases of allergy to β-lactam antibacterials and cannot be extended to other types of drugs.[37,82] In the diagnosis of AHS due to aromatic anticonvulsants, the LTT has frequently shown a sensitivity of between 71% and 100%[14,51,53,55,57,61,77,79] but this also ranges as low as 19–40%.[58,59,69,72] Estimates of specificity, however, seem to be quite good (close to 100%).[51,53] Nevertheless, one must always keep in mind that these estimates have been calculated in the absence of a diagnostic gold standard, which may explain the considerable variability in these numbers.
AHS has a broad range of clinical manifestations[127] reflecting differences in the underlying pathophysiology.[91,128] If the LTT is able to detect circulating drug-specific T cells, it is logical to expect that other non-T-cell-mediated reactions will not be detected using this approach. Ironically, the LTT gave positive results with IgE-mediated type I reactions, which also implies a role for T cells in these types of reactions.[61] In vitro tests detecting antigen-specific IgE antibodies are also available and might be expected to be more sensitive for these types of reactions.[8]
Reviewing publications on the use of the LTA as a diagnostic tool for AHS has revealed a range of sensitivity between 85% and 100% with well documented AHS cases, with satisfactory negative and positive predictive values. The LTA has also been shown to possess good sensitivity in cases involving AHS due to sulfonamides[117,129–131] and valproic acid.[132]
5. Conclusions
Analysis of peripheral blood lymphocytes has been a ‘promising’ diagnostic tool for AHS for several decades. It appears that without further understanding of the mechanisms underlying the pathophysiology of AHS and how specific drugs and metabolites differentially affect these mechanisms, the development of more reliable tools for AHS diagnosis will be compromised. Consequently, in the absence of further research, the predictability of these tests will remain questionable and they are unlikely to be utilized on a large scale.
References
Shear NH, Spielberg SP. Anticonvulsant hypersensitivity syndrome: in vitro assessment of risk. J Clin Invest 1988 Dec; 82(6): 1826–32
Zaccara G, Franciotta D, Perucca E. Idiosyncratic adverse reactions to antiepileptic drugs. Epilepsia 2007 Jul; 48(7): 1223–44
Peyriere H, Dereure O, Breton H, et al. Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist? Br J Dermatol 2006 Aug; 155(2): 422–8
Shapiro LE, Shear NH. Mechanisms of drug reactions: the metabolic track. Semin Cutan Med Surg 1996 Dec; 15(4): 217–27
Spielberg SP, Gordon GB, Blake DA, et al. Anticonvulsant toxicity in vitro: possible role of arene oxides. J Pharmacol Exp Ther 1981 May; 217(2): 386–9
Tennis P, Stern RS. Risk of serious cutaneous disorders after initiation of use of phenytoin, carbamazepine, or sodium valproate: a record linkage study. Neurology 1997 Aug; 49(2): 542–6
Primeau MN, Adkinson Jr NF. Recent advances in the diagnosis of drug allergy. Curr Opin Allergy Clin Immunol 2001 Aug; 1(4): 337–41
Romano A, Demoly P. Recent advances in the diagnosis of drug allergy. Curr Opin Allergy Clin Immunol 2007 Aug; 7(4): 299–303
Pourpak Z, Fazlollahi MR, Fattahi F. Understanding adverse drug reactions and drug allergies: principles, diagnosis and treatment aspects. Recent Pat Inflamm Allergy Drug Discov 2008; 2(1): 24–46
Elzagallaai AA, Knowles SR, Rieder MJ, et al. Patch testing for the diagnosis of anticonvulsant hypersensitivity syndrome: a systematic review. Drug Saf 2009; 32(5): 391–408
Naranjo CA, Shear NH, Lanctot KL. Advances in the diagnosis of adverse drug reactions. J Clin Pharmacol 1992 Oct; 32(10): 897–904
Beeler A, Pichler WJ. In vitro tests of T-cell-mediated drug hypersensitivity. In: Pichler WJ, editor. Drug hypersensitivity. Basel: Karger, 2007: 380–90
Lan CC, Wu CS, Tsai PC, et al. Diagnostic role of soluble fas ligand secretion by peripheral blood mononuclear cells from patients with previous drug-induced blistering disease: a pilot study. Acta Derm Venereol 2006; 86(3): 215–8
Wu Y, Sanderson JP, Farrell J, et al. Activation of T cells by carbamazepine and carbamazepine metabolites. J Allergy Clin Immunol 2006 Jul; 118(1): 233–41
Beeler A, Engler O, Gerber BO, et al. Long-lasting reactivity and high frequency of drug-specific T cells after severe systemic drug hypersensitivity reactions. J Allergy Clin Immunol 2006 Feb; 117(2): 455–62
Pentycross CR. Technique for lymphocyte transformation. J Clin Pathol 1968 Mar; 21(2): 175–8
Böyum A. Isolation of leucocytes from human blood: further observations. Methylcellulose, dextran, and Ficoll as erythrocyte aggregating agents. Scand J Clin Lab Invest Suppl 1968; 97: 31–50
Rigas DA, Osgood EE. Purification and properties of the phytohemagglutinin of Phaseolus vulgaris. J Biol Chem 1955 Feb; 212(2): 607–15
Minor AH, Burnett L. A method for obtaining living leukocytes from human peripheral blood by acceleration of erythrocyte sedimentation. Blood 1948 Jul; 3(7): 799–802
Li JG, Osgood EE. A method for the rapid separation of leukocytes and nucleated erythrocytes from blood of marrow with a phytohemagglutinin from red beans (Phaseolus vulgaris). Blood 1949 May; 4(5): 670–5
Nowell PC. Phytohemagglutinin: an initiator of mitosis in cultures of normal human leukocytes. Cancer Res 1960 May; 20: 462–6
Pearmain G, Lycette RR, Fitzgerald PH. Tuberculin-induced mitosis in peripheral blood leucocytes. Lancet 1963 Mar 23; 1(7282): 637–8
Holland P, Mauer AM. Drug-induced in-vitro stimulation of peripheral lymphocytes. Lancet 1964 Jun 20; 1(7347): 1368–9
Caron GA, Sarkany I. Lymphoblast transformation in sulphonamide sensitivity. Br J Dermatol 1965 Nov; 77(11): 556–60
Vischer TL. Lymphocyte cultures in drug hypersensitivity. Lancet 1966 Aug 27; 2(7461): 467–9
Leguit Jr P, Meinesz A, Zeijlemaker WP, et al. Immunological studies in burn patients: I. Lymphocyte transformation in vitro. Int Arch Allergy Appl Immunol 1973; 44(1): 101–21
Schellekens PT, Eijsvoogel VP. Lymphocyte transformation in vitro: I. Tissue culture conditions and quantitative measurements. Clin Exp Immunol 1968 Jul; 3(6): 571–84
Schellekens PT, Eijsvoogel VP. Lymphocyte transformation in vitro: III. Mechanism of stimulation in the mixed lymphocyte culture. Clin Exp Immunol 1970 Aug; 7(2): 229–39
Schellekens PT, Eijsvoogel VP. Lymphocyte transformation in vitro: IV. Recruitment in antigen-stimulated cultures. Clin Exp Immunol 1971 Feb; 8(2): 187–94
Schellekens PT, Vriesendorp B, Eijsvoogel VP, et al. Lymphocyte transformation in vitro: II. Mixed lymphocyte culture in relation to leucocyte antigens. Clin Exp Immunol 1970 Feb; 6(2): 241–54
Pichler WJ, Tilch J. The lymphocyte transformation test in the diagnosis of drug hypersensitivity. Allergy 2004 Aug; 59(8): 809–20
Sachs B, Erdmann S, Malte Baron J, et al. Determination of interleukin-5 secretion from drug-specific activated ex vivo peripheral blood mononuclear cells as a test system for the in vitro detection of drug sensitization. Clin Exp Allergy 2002 May; 32(5): 736–44
Turcanu V, Maleki SJ, Lack G. Characterization of lymphocyte responses to peanuts in normal children, peanut-allergic children, and allergic children who acquired tolerance to peanuts. J Clin Invest 2003 Apr; 111(7): 1065–72
Okumura A, Tsuge I, Kubota T, et al. Phenytoin desensitization monitored by antigen specific T cell response using carboxyfluorescein succinimidyl ester dilution assay. Eur J Paediatr Neurol 2007 Nov; 11(6): 385–8
Lyons AB. Analysing cell division in vivo and in vitro using flow cytometric measurement of CFSE dye dilution. J Immunol Methods 2000 Sep 21; 243(1–2): 147–54
Fulcher D, Wong S. Carboxyfluorescein succinimidyl ester-based pro-liferative assays for assessment of T cell function in the diagnostic laboratory. Immunol Cell Biol 1999 Dec; 77(6): 559–64
Nyfeler B, Pichler WJ. The lymphocyte transformation test for the diagnosis of drug allergy: sensitivity and specificity. Clin Exp Allergy 1997 Feb; 27(2): 175–81
Spielberg SP. In vitro assessment of pharmacogenetic susceptibility to toxic drug metabolites in humans. Fed Proc 1984 May 15; 43(8): 2308–13
Spielberg SP. In vitro analysis of idiosyncratic drug reactions. Clin Biochem 1986 Apr; 19(2): 142–4
Spielberg SP, Gordon GB, Blake DA, et al. Predisposition to phenytoin hepatotoxicity assessed in vitro. N Engl J Med 1981 Sep 24; 305(13): 722–7
Spielberg SP. Acetaminophen toxicity in human lymphocytes in vitro. J Pharmacol Exp Ther 1980 May; 213(2): 395–8
Knowles SR, Uetrecht J, Shear NH. Idiosyncratic drug reactions: the reactive metabolite syndromes. Lancet 2000 Nov 4; 356(9241): 1587–91
Uetrecht J. Idiosyncratic drug reactions: current understanding. Annu Rev Pharmacol Toxicol 2007; 47: 513–39
Uetrecht J. Idiosyncratic drug reactions: past, present, and future. Chem Res Toxicol 2008 Jan; 21 (1): 84-92
Kupfer A, Brilis GM, Watson JT, et al. A major pathway of mephenytoin metabolism in man: aromatic hydroxylation to p-hydroxymephenytoin. Drug Metab Dispos 1980 Jan-Feb; 8(1): 1–4
Lertratanangkoon K, Horning MG. Metabolism of carbamazepine. Drug Metab Dispos 1982 Jan–Feb; 10(1): 1–10
Karande S, Gogtay NJ, Kanchan S, et al. Anticonvulsant hypersensitivity syndrome to lamotrigine confirmed by lymphocyte stimulation in vitro. Indian J Med Sci 2006 Feb; 60(2): 59–63
Aberer W. Drug hypersensitivities: the need for standardization. Eur Ann Allergy Clin Immunol 2005 Jun; 37(6): 219–22
Wolkenstein P, Charue D, Laurent P, et al. Metabolic predisposition to cutaneous adverse drug reactions: role in toxic epidermal necrolysis caused by sulfonamides and anticonvulsants. Arch Dermatol 1995 May; 131(5): 544–51
Hari Y, Frutig-Schnyder K, Hurni M, et al. T cell involvement in cutaneous drug eruptions. Clin Exp Allergy 2001 Sep; 31(9): 1398–408
Naisbitt DJ, Farrell J, Wong G, et al. Characterization of drug-specific T cells in lamotrigine hypersensitivity. J Allergy Clin Immunol 2003 Jun; 111(6): 1393–403
Farrell J, Naisbitt DJ, Drummond NS, et al. Characterization of sulfamethoxazole and sulfamethoxazole metabolite-specific T-cell responses in animals and humans. J Pharmacol Exp Ther 2003 Jul; 306(1): 229–37
Naisbitt DJ, Britschgi M, Wong G, et al. Hypersensitivity reactions to carbamazepine: characterization of the specificity, phenotype, and cytokine profile of drug-specific T cell clones. Mol Pharmacol 2003 Mar; 63(3): 732–41
Berg PA, Becker EW. The lymphocyte transformation test: a debated method for the evaluation of drug allergic hepatic injury. J Hepatol 1995 Jan; 22(1): 115–8
Beeler A, Zaccaria L, Kawabata T, et al. CD69 upregulation on T cells as an in vitro marker for delayed-type drug hypersensitivity. Allergy 2008 Feb; 63(2): 181–8
Kano Y, Hirahara K, Mitsuyama Y, et al. Utility of the lymphocyte transformation test in the diagnosis of drug sensitivity: dependence on its timing and the type of drug eruption. Allergy 2007 Dec; 62(12): 1439–44
Tsuge I, Okumura A, Kondo Y, et al. Allergen-specific T-cell response in patients with phenytoin hypersensitivity: simultaneous analysis of proliferation and cytokine production by carboxyfluorescein succinimidyl ester (CFSE) dilution assay. Allergol Int 2007 Jun; 56(2): 149–55
Romano A, Pettinato R, Andriolo M, et al. Hypersensitivity to aromatic anticonvulsants: in vivo and in vitro cross-reactivity studies. Curr Pharm Des 2006; 12(26): 3373–81
Gex-Collet C, Helbling A, Pichler WJ. Multiple drug hypersensitivity: proof of multiple drug hypersensitivity by patch and lymphocyte transformation tests. J Investig Allergol Clin Immunol 2005; 15(4): 293–6
Aihara Y, Ito SI, Kobayashi Y, et al. Carbamazepine-induced hypersensitivity syndrome associated with transient hypogammaglobulinaemia and reactivation of human herpesvirus 6 infection demonstrated by real-time quantitative polymerase chain reaction. Br J Dermatol 2003 Jul; 149(1): 165–9
Neukomm CB, Yawalkar N, Helbling A, et al. T-cell reactions to drugs in distinct clinical manifestations of drug allergy. J Investig Allergol Clin Immunol 2001; 11(4): 275–84
Mutoh K, Hidaka Y, Hirose Y, et al. Possible induction of systemic lupus erythematosus by zonisamide. Pediatr Neurol 2001 Oct; 25(4): 340–3
Troger U, Brandt W, Rose W. Development of a pulmonary phenytoin-associated hypersensitivity reaction despite concomitant dexamethasone and prednisolone administration. Int J Clin Pharmacol Ther 2000 Sep; 38(9): 452–6
Troger U, Brandt W, Rose W. A very early onset of respiratory failure due to phenytoin-associated hypersensitivity syndrome and concomitant glucocorticoid administration [letter]. Intensive Care Med 2000 Feb; 26(2): 258
Chinen J, Piecuch S. Anticonvulsant hypersensitivity syndrome versus Kawasaki disease: a challenging clinical diagnosis with therapeutic implications. Clin Pediatr (Phila) 2000 Feb; 39(2): 109–11
Schaub N, Bircher AJ. Severe hypersensitivity syndrome to lamotrigine confirmed by lymphocyte stimulation in vitro. Allergy 2000 Feb; 55(2): 191–3
Brown KL, Henderson DC, Nadel S, et al. Carbamazepine hypersensitivity and the use of lymphocyte proliferation responses. Dev Med Child Neurol 1999 Apr; 41(4): 267–9
Sachs B, Ronnau AC, von Schmiedeberg S, et al. Lamotrigine-induced Stevens-Johnson syndrome: demonstration of specific lymphocyte reactivity in vitro. Dermatology 1997; 195(1): 60–4
Troost RJ, Van Parys JA, Hooijkaas H, et al. Allergy to carbamazepine: parallel in vivo and in vitro detection. Epilepsia 1996 Nov; 37(11): 1093–9
Okuyama R, Ichinohasama R, Tagami H. Carbamazepine induced erythroderma with systemic lymphadenopathy. J Dermatol 1996 Jul; 23(7): 489–94
Mauri-Hellweg D, Bettens F, Mauri D, et al. Activation of drug-specific CD4+ and CD8+ T cells in individuals allergic to sulfonamides, phenytoin, and carbamazepine. J Immunol 1995 Jul 1; 155(1): 462–72
Kimura M, Yoshino K, Maeoka Y, et al. Carbamazepine-induced throm-bocytopenia and carbamazepine-10,11-epoxide: a case report. Psychiatry Clin Neurosci 1995 Mar; 49(1): 69–70
Friedmann PS, Strickland I, Pirmohamed M, et al. Investigation of mechanisms in toxic epidermal necrolysis induced by carbamazepine. Arch Dermatol 1994 May; 130(5): 598–604
Maria VA, Pinto L, Victorino RM. Lymphocyte reactivity to ex-vivo drug antigens in drug-induced hepatitis. J Hepatol 1994 Aug; 21(2): 151–8
Takahashi N, Aizawa H, Takata S, et al. Acute interstitial pneumonitis induced by carbamazepine. Eur Respir J 1993 Oct; 6(9): 1409–11
Danno K, Kume M, Ohta M, et al. Erythroderma with generalized lymphadenopathy induced by phenytoin. J Dermatol 1989 Oct; 16(5): 392–6
Zakrzewska JM, Ivanyi L. In vitro lymphocyte proliferation by carbamazepine, carbamazepine-10, 11-epoxide, and oxcarbazepine in the diagnosis of drug-induced hypersensitivity. J Allergy Clin Immunol 1988 Jul; 82(1): 110–5
De Swert LF, Ceuppens JL, Teuwen D, et al. Acute interstitial pneumonitis and carbamazepine therapy. Acta Paediatr Scand 1984 Mar; 73(2): 285–8
Houwerzijl J, De Gast GC, Nater JP, et al. Lymphocyte-stimulation tests and patch tests to carbamazepine hypersensitivity. Clin Exp Immunol 1977 Aug; 29(2): 272–7
Cullinan SA, Bower GC. Acute pulmonary hypersensitivity to carbamazepine. Chest 1975 Oct; 68(4): 580–1
Virolainen M. Blast transformation in vivo and in vitro in carbamazepin hypersensitivity. Clin Exp Immunol 1971 Sep; 9(3): 429–35
Luque I, Leyva L, Jose Torres M, et al. In vitro T-cell responses to beta-lactam drugs in immediate and nonimmediate allergic reactions. Allergy 2001 Jul; 56(7): 611–8
Shepherd GM. Hypersensitivity reactions to drugs: evaluation and management. Mt Sinai J Med 2003 Mar; 70(2): 113–25
Sharma VK, Vatve M, Sawhney IM, et al. Clinical spectrum of drug rashes due to antiepileptics. J Assoc Physicians India 1998 Jul; 46(7): 595–7
Kuechler PC, Britschgi M, Schmid S, et al. Cytotoxic mechanisms in different forms of T-cell-mediated drug allergies. Allergy 2004 Jun; 59(6): 613–22
Posadas SJ, Pichler WJ. Delayed drug hypersensitivity reactions-new concepts. Clin Exp Allergy 2007 Jul; 37(7): 989–99
Pichler WJ, Beeler A, Keller M, et al. Pharmacological interaction of drugs with immune receptors: the p-i concept. Allergol Int 2006 Mar; 55(1): 17–25
Gerber BO, Pichler WJ. Noncovalent interactions of drugs with immune receptors may mediate drug-induced hypersensitivity reactions. AAPS J 2006; 8(1): E160–5
Gerber BO, Pichler WJ. The p-i concept: evidence and implications. In: Pichler WJ, editor. Drug hypersensitivity. Basel: Karger, 2007: 66–73
Hashizume H, Takigawa M, Tokura Y. Characterization of drug-specific T cells in phenobarbital-induced eruption. J Immunol 2002 May 15; 168(10): 5359–68
Naisbitt DJ, Pirmohamed M, Park BK. Immunological principles of T-cell-mediated adverse drug reactions in skin. Expert Opin Drug Saf 2007 Mar; 6(2): 109–24
Pichler WJ. Delayed drug hypersensitivity reactions. Ann Intern Med 2003 Oct 21; 139(8): 683–93
Matsuno O, Okubo T, Hiroshige S, et al. Drug-induced lymphocyte stimulation test is not useful for the diagnosis of drug-induced pneumonia. Tohoku J Exp Med 2007 May; 212(1): 49–53
Mantani N, Kogure T, Tamura J, et al. Lymphocyte transformation test for medicinal herbs yields false-positive results for first-visit patients. Clin Diagn Lab Immunol 2003 May; 10(3): 479–80
Ono E, Miyazaki E, Matsuno O, et al. Minocycline-induced acute eosino-philic pneumonia: controversial results of lymphocyte stimulation test and re-challenge test. Intern Med 2007; 46(9): 593–5
Wu Y, Farrell J, Pirmohamed M, et al. Generation and characterization of antigen-specific CD4+, CD8+, and CD4+CD8+ T-cell clones from patients with carbamazepine hypersensitivity. J Allergy Clin Immunol 2007 Apr; 119(4): 973–81
Sachs B, Erdmann S, Al-Masaoudi T, et al. In vitro drug allergy detection system incorporating human liver microsomes in chlorazepate-induced skin rash: drug-specific proliferation associated with interleukin-5 secretion. Br J Dermatol 2001 Feb; 144(2): 316–20
Merk HF. Diagnosis of drug hypersensitivity: lymphocyte transformation test and cytokines. Toxicology 2005 Apr 15; 209(2): 217–20
Abe R, Shimizu T, Shibaki A, et al. Toxic epidermal necrolysis and Stevens-Johnson syndrome are induced by soluble Fas ligand. Am J Pathol 2003 May; 162(5): 1515–20
Krensky AM, Clayberger C. Granulysin: a novel host defense molecule. Am J Transplant 2005 Aug; 5(8): 1789–92
Chung WH, Hung SI, Yang JY, et al. Granulysin is a key mediator for disseminated keratinocyte death in Stevens-Johnson syndrome and toxic epidermal necrolysis. Nat Med 2008 Dec; 14(12): 1343–50
Neuman MG, Malkiewicz IM, Shear NH. A novel lymphocyte toxicity assay to assess drug hypersensitivity syndromes. Clin Biochem 2000 Oct; 33(7): 517–24
Neuman MG, Shear NH, Malkiewicz IM, et al. Predicting possible zonisamide hypersensitivity syndrome. Exp Dermatol 2008 Dec; 17(12): 1045–51
Naranjo CA, Kwok MC, Lanctot KL, et al. Enhanced differential diagnosis of anticonvulsant hypersensitivity reactions by an integrated Bayesian and biochemical approach. Clin Pharmacol Ther 1994 Nov; 56(5): 564–75
Dwivedi R, Gogtay N, Kharkar V, et al. In-vitro lymphocyte toxicity to a phenytoin metabolite in phenytoin induced cutaneous adverse drug eruptions. Indian J Dermatol Venereol Leprol 2004 Jul–Aug; 70(4): 217–20
Bavdekar SB, Muranjan MN, Gogtay NJ, et al. Anticonvulsant hypersensitivity syndrome: lymphocyte toxicity assay for the confirmation of diagnosis and risk assessment. Ann Pharmacother 2004 Oct; 38(10): 1648–50
Gennis MA, Vemuri R, Burns EA, et al. Familial occurrence of hypersensitivity to phenytoin. Am J Med 1991 Dec; 91(6): 631–4
Pirmohamed M, Graham A, Roberts P, et al. Carbamazepine-hypersensitivity: assessment of clinical and in vitro chemical cross-reactivity with phenytoin and oxcarbazepine. Br J Clin Pharmacol 1991 Dec; 32(6): 741–9
Hewitt CW, Sawyer S, Beck PA, et al. A simple method for the isolation of platelet-free lymphocyte suspensions from rat whole blood. J Immunol Methods 1980; 36(3–4): 227–34
Rueda F, Marti F, Pinol G, et al. Artefactual low lymphocyte activity caused by platelet contamination in the mononuclear cell preparations. Am J Hematol 1989 Jun; 31(2): 126–7
Casale TB, Kaliner M. A rapid method for isolation of human mononuclear cells free of significant platelet contamination. J Immunol Methods 1982 Dec 30; 55(3): 347–53
Hurwitz RL, Schreinemachers D, Kersey JH. Elimination of platelets from mononuclear cell preparations using heat-killed yeast. Exp Hematol 1979 Feb; 7(2): 81–6
Lad PM, Easton J, Niedzin H, et al. A method for the preparation of mononuclear cells devoid of platelet contamination and its application to the evaluation of putative alpha-receptors in normal and asthmatic subjects. J Immunol Methods 1988 Jun 13; 110(2): 193–202
Shibusawa Y, Suzuki K, Kinoshita H, et al. Selective separation of human peripheral platelets, granulocytes and lymphocytes by surface affinity chromatography. J Chromatogr B Biomed Appl 1995 Apr 21; 666(2): 233–9
Martignoni M, Groothuis GM, de Kanter R. Species differences between mouse, rat, dog, monkey and human CYP-mediated drug metabolism, inhibition and induction. Expert Opin Drug Metab Toxicol 2006 Dec; 2(6): 875–94
Park BK, Pirmohamed M, Kitteringham NR. The role of cytochrome P450 enzymes in hepatic and extrahepatic human drug toxicity. Pharmacol Ther 1995; 68(3): 385–424
Rieder MJ, Uetrecht J, Shear NH, et al. Diagnosis of sulfonamide hypersensitivity reactions by in-vitro “rechallenge” with hydroxylamine metabolites. Ann Intern Med 1989 Feb 15; 110(4): 286–9
Ting TY. Anticonvulsant hypersensitivity syndrome: identification and management. Curr Treat Options Neurol 2007 Jul; 9(4): 243–8
Krauss G. Current understanding of delayed anticonvulsant hypersensitivity reactions. Epilepsy Curr 2006 Mar–Apr; 6(2): 33–7
Gogtay NJ, Bavdekar SB, Kshirsagar NA. Anticonvulsant hypersensitivity syndrome: a review. Expert Opin Drug Saf 2005 May; 4(3): 571–81
Bessmertny O, Pham T. Antiepileptic hypersensitivity syndrome: clinicians beware and be aware. Curr Allergy Asthma Rep 2002 Jan; 2(1): 34–9
Quinones MD, Valero C, Salcedo M, et al. Phenytoin hypersensitivity syndrome with fatal evolution. Allergy 1999 Jan; 54(1): 83–4
Huang LY, Liao WC, Chiou CC, et al. Fatal toxic epidermal necrolysis induced by carbamazepine treatment in a patient who previously had carbamazepine-induced Stevens-Johnson syndrome. J Formos Med Assoc 2007 Dec; 106(12): 1032–7
Kwan P, Brodie MJ. Effectiveness of first antiepileptic drug. Epilepsia 2001 Oct;42(10): 1255–60
Toledano R, Gil-Nagel A. Adverse effects of antiepileptic drugs. Semin Neurol 2008 Jul; 28(3): 317–27
Devi K, George S, Criton S, et al. Carbamazepine: the commonest cause of toxic epidermal necrolysis and Stevens-Johnson syndrome. A study of 7 years. Indian J Dermatol Venereol Leprol 2005 Sep–Oct; 71(5): 325–8
Mathews KP. Clinical spectrum of allergic and pseudoallergic drug reactions. J Allergy Clin Immunol 1984 Oct; 74 (4 Pt 2): 558–66
Leeder JS. Mechanisms of idiosyncratic hypersensitivity reactions to antiepileptic drugs. Epilepsia 1998; 39Suppl. 7: S8–16
Shear NH, Spielberg SP, Grant DM, et al. Differences in metabolism of sulfonamides predisposing to idiosyncratic toxicity. Ann Intern Med 1986 Aug; 105(2): 179–84
Lanctot KL, Ghajar BM, Shear NH, et al. Improving the diagnosis of hypersensitivity reactions associated with sulfonamides. J Clin Pharmacol 1994 Dec; 34(12): 1228–33
Neuman MG, Shear NH, Malkiewicz IM, et al. Immunopathogenesis of hypersensitivity syndrome reactions to sulfonamides. Transl Res 2007 May; 149(5): 243–53
Tabatabaei AR, Thies RL, Abbott FS. Assessing the mechanism of metabolism-dependent valproic acid-induced in vitro cytotoxicity. Chem Res Toxicol 1999 Apr; 12(4): 323–30
Acknowledgments
No sources of funding were used to assist in the preparation of this review. The authors have no conflicts of interest that are directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Elzagallaai, A.A., Knowles, S.R., Rieder, M.J. et al. In Vitro Testing for the Diagnosis of Anticonvulsant Hypersensitivity Syndrome. Mol Diag Ther 13, 313–330 (2009). https://doi.org/10.1007/BF03256336
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03256336