Abstract
Background
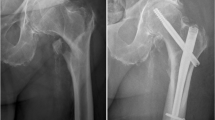
Intertrochanteric fragility fracture (IFF) treated with proximal femoral nail anti-rotation (PFNA) is associated with significant hidden blood loss and high blood transfusion rate. The purpose of the present study was to evaluate the efficacy and safety of tranexamic acid (TXA) in reducing blood loss in these patients.
Materials and Methods
Consecutive eligible patients were recruited and randomly assigned to a TXA group or a control group. The TXA group received 15 mg/kg body weight of TXA intravenously 15 min before incision and the same dose 3 h later. The control group received 100 mL of saline intravenously 15 min before incision. The efficacy outcomes included the total perioperative blood loss, postoperative transfusion rate, postoperative hemoglobin level, and length of the hospital stay. The safety outcomes were the incidence of thrombotic events and the mortality rate within 6 weeks after surgery.
Results
We had 44 patients in the TXA group and 46 patients in the control group for the final analysis. The TXA group had significantly lower total perioperative blood loss than the control group (384.5 ± 366.3 mL vs. 566.2 ± 361.5 mL; P < 0.020). Postoperative transfusion rate was 15.9% in the TXA group versus 36.9% in the control group (P = 0.024). Each group had one patient with postoperative deep venous thrombosis. In the control group, three patients had cerebral infarction, and one patient died within 6 weeks after the operation.
Conclusion
Intravenous TXA is effective in reducing total perioperative blood loss and transfusion rate in IFF treated with PFNA. No increased risk of thrombotic events was observed with the use of TXA; however, this study was underpowered for detecting this outcome. Further research is necessary before TXA can be recommended for high-risk patients.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Wei J, Wang J, Gao M, Wang M. Analysis of perioperative blood loss in treatment of senile hip fractures. Chin J Orthop Trauma 2015;17:104–7.
Hou GJ, Zhou F, Zhang ZS, Ji HQ, Tian Y. Analysis of the blood loss in perioperative period of femoral intertrochanteric fractures in old patients treated with different internal fixations. Beijing Da Xue Xue Bao Yi Xue Ban 2013;45:738–41.
Foss NB, Kehlet H. Hidden blood loss after surgery for hip fracture. J Bone Joint Surg Br 2006;88:1053–9.
Millar NL, Deakin AH, Millar LL, Kinnimonth AW, Picard F. Blood loss following total knee replacement in the morbidly obese: Effects of computer navigation. Knee 2011;18:108–12.
Smith GH, Tsang J, Molyneux SG, White TO. The hidden blood loss after hip fracture. Injury 2011;42:133–5.
Bao N, Zhou L, Cong Y, Guo T, Fan W, Chang Z, et al. Free fatty acids are responsible for the hidden blood loss in total hip and knee arthroplasty. Med Hypotheses 2013;81:104–7.
Piovella F, Wang CJ, Lu H, Lee K, Lee LH, Lee WC, et al. Deep-vein thrombosis rates after major orthopedic surgery in Asia. An epidemiological study based on postoperative screening with centrally adjudicated bilateral venography. J Thromb Haemost 2005;3:2664–70.
Lee SY, Ro du H, Chung CY, Lee KM, Kwon SS, Sung KH, et al. Incidence of deep vein thrombosis after major lower limb orthopedic surgery: Analysis of a nationwide claim registry. Yonsei Med J 2015;56:139–45.
Zhou XD, Tao LJ, Li J, Wu LD. Do we really need tranexamic acid in total hip arthroplasty? A meta-analysis of nineteen randomized controlled trials. Arch Orthop Trauma Surg 2013;133:1017–27.
Wu Q, Zhang HA, Liu SL, Meng T, Zhou X, Wang P, et al. Is tranexamic acid clinically effective and safe to prevent blood loss in total knee arthroplasty? A meta-analysis of 34 randomized controlled trials. Eur J Orthop Surg Traumatol 2015;25:525–41.
Sukeik M, Alshryda S, Haddad FS, Mason JM. Systematic review and meta-analysis of the use of tranexamic acid in total hip replacement. J Bone Joint Surg Br 2011;93:39–46.
Zufferey PJ, Miquet M, Quenet S, Martin P, Adam P, Albaladejo P, et al. Tranexamic acid in hip fracture surgery: A randomized controlled trial. Br J Anaesth 2010;104:23–30.
Nadler SB, Hidalgo JH, Bloch T. Prediction of blood volume in normal human adults. Surgery 1962;51:224–32.
Gross JB. Estimating allowable blood loss: Corrected for dilution. Anesthesiology 1983;58:277–80.
Roberts KC, Brox WT, Jevsevar DS, Sevarino K. Management of hip fractures in the elderly. J Am Acad Orthop Surg 2015;23:131–7.
Ng W, Jerath A, Wąsowicz M. Tranexamic acid: A clinical review. Anaesthesiol Intensive Ther 2015;47:339–50.
Jennings JD, Solarz MK, Haydel C. Application of tranexamic acid in trauma and orthopedic surgery. Orthop Clin North Am 2016;47:137–43.
Tang P, Hu F, Shen J, Zhang L, Zhang L. Proximal femoral nail antirotation versus hemiarthroplasty: A study for the treatment of intertrochanteric fractures. Injury 2012;43:876–81.
Mohib Y, Rashid RH, Ali M, Zubairi AJ, Umer M. Does tranexamic acid reduce blood transfusion following surgery for inter-trochanteric fracture? A randomized control trial. J Pak Med Assoc 2015;65:S17–20.
Vijay BS, Bedi V, Mitra S, Das B. Role of tranexamic acid in reducing postoperative blood loss and transfusion requirement in patients undergoing hip and femoral surgeries. Saudi J Anaesth 2013;7:29–32.
Sadeghi M, Mehr-Aein A. Does a single bolus dose of tranexamic acid reduce blood loss and transfusion requirements during hip fracture surgery? A prospective randomized double blind study in 67 patients. Acta Med Iran 2007;45:437–42.
Tengberg PT, Foss NB, Palm H, Kallemose T, Troelsen A. Tranexamic acid reduces blood loss in patients with extracapsular fractures of the hip: Results of a randomised controlled trial. Bone Joint J 2016;98-B: 747–53.
Farrow LS, Smith TO, Ashcroft GP, Myint PK. A systematic review of tranexamic acid in hip fracture surgery. Br J Clin Pharmacol 2016;82:1458–70.
Jimenez JJ, Iribarren JL, Lorente L, Rodriguez JM, Hernandez D, Nassar I, et al. Tranexamic acid attenuates inflammatory response in cardiopulmonary bypass surgery through blockade of fibrinolysis: A case control study followed by a randomized double-blind controlled trial. Crit Care 2007;11:R117.
Gillette BP, Maradit Kremers H, Duncan CM, Smith HM, Trousdale RT, Pagnano MW, et al. Economic impact of tranexamic acid in healthy patients undergoing primary total hip and knee arthroplasty. J Arthroplasty 2013;28:137–9.
Irisson E, Hémon Y, Pauly V, Parratte S, Argenson JN, Kerbaul F, et al. Tranexamic acid reduces blood loss and financial cost in primary total hip and knee replacement surgery. Orthop Traumatol Surg Res 2012;98:477–83.
Gillette BP, DeSimone LJ, Trousdale RT, Pagnano MW, Sierra RJ. Low risk of thromboembolic complications with tranexamic acid after primary total hip and knee arthroplasty. Clin Orthop Relat Res 2013;471:150–4.
Wu YG, Zeng Y, Yang TM, Si HB, Cao F, Shen B, et al. The efficacy and safety of combination of intravenous and topical tranexamic acid in revision hip arthroplasty: A Randomized, controlled trial. J Arthroplasty 2016;31:2548–53.
Formby PM, Pickett AM, Van Blarcum GS, Mack AW, Newman MT. The use of intravenous tranexamic acid in patients undergoing total hip or knee arthroplasty: A retrospective analysis at a single military institution. Mil Med 2015;180:1087–90.
Whiting DR, Gillette BP, Duncan C, Smith H, Pagnano MW, Sierra RJ, et al. Preliminary results suggest tranexamic acid is safe and effective in arthroplasty patients with severe comorbidities. Clin Orthop Relat Res 2014;472:66–72.
Roberts I, Perel P, Prieto-Merino D, Shakur H, Coats T, Hunt BJ, et al. Effect of tranexamic acid on mortality in patients with traumatic bleeding: Prespecified analysis of data from randomised controlled trial. BMJ 2012;345:e5839.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luo, X., He, S., Lin, Z. et al. Efficacy and Safety of Tranexamic Acid for Controlling Bleeding During Surgical Treatment of Intertrochanteric Fragility Fracture with Proximal Femoral Nail Anti-rotation: A Randomized Controlled Trial. JOIO 53, 263–269 (2019). https://doi.org/10.4103/ortho.IJOrtho_401_17
Published:
Issue Date:
DOI: https://doi.org/10.4103/ortho.IJOrtho_401_17