ABSTRACT
In the study, we developed a novel oral dosage form of Compound Danshen to resolve the problems of low bioavailability, disequilibrium in drug release, and stomach degradation of active components of Compound Danshen in conventional formulas. A colon-specific osmotic pump capsule (COPC) of Compound Danshen was prepared using a semipermeable shell with the core components. Using a single-factor method, we obtained the optimal formulation that consisted of Salvia miltiorrhiza extract, Panax notoginseng extract, Borneol, sodium chloride, polyethylene oxide wsr-N10, hydroxypropyl-β-cyclodextrin, and ludipress. Moreover, in vitro dissolution test showed simultaneous releases of active ingredients from Compound Danshen COPC over 12 h at pH 7.8, displaying zero-order release characteristics. The impetus of drug release mainly depended on the difference in osmotic pressure across the capsule shell. Next, scanning electron microscopy showed morphological changes in the capsule shell during the dissolution test. More importantly, pharmacokinetic study in beagle dogs indicated that relative bioavailability was 330.58% and retention time was greatly prolonged in Compound Danshen COPC, compared with those in marketed Compound Danshen tablet products. Finally, in vivo imaging studies in beagle dogs showed that COPC was stable in gastrointestinal tract and the drug was specifically released in the colon region.

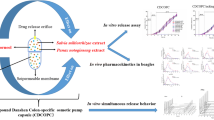
A colon-specific osmotic pump capsule (COPC) of Compound Danshen was developed and optimized to achieve simultaneous zero-order release of multiple active components of Compound Danshen in the colon. More importantly, the COPC have proved to improve the bioavailability and prolong the retention time of Compound Danshen, compared with those in a marketed product.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The Compound Danshen formula, a traditional Chinese medicine (TCM) recognized in the official Chinese Pharmacopoeia, is composed of Radix Salvia miltiorrhiza, Panax notoginseng, and Borneol (1). It has been extensively used to treat coronary heart diseases, angina pectoris, and hyperlipidemia (2,3,4).
To date, marketed Compound Danshen products, including Compound Danshen tablets (CDT) and Compound Danshen dripping pills (5), have a feature of frequent dosing. However, frequent dosing may lead to patient noncompliance, especially in elderly patients with sluggishness and memory degradation, and to potential fluctuation in blood drug concentration. To overcome this problem, many sustained-release systems have been developed. For instance, Compound Danshen sustained-release tablets and sustained-release capsules have been developed (6,7). These dosage forms are able to reduce dosing frequency and improve patient compliance by releasing the drug continuously. However, as the integrity of active ingredients is important to exert synergistic pharmacological effects (8), significant differences in solubility among the active ingredients, namely, from free water-soluble forms to practically water insoluble forms, cause a disparity in drug release among the above preparations, weakening the overall treatment outcome (9,10). Some studies, such as studies of Compound Danshen osmotic pump tablets, could achieve simultaneous release of Compound Danshen active ingredients in the gastrointestinal tract (11), but the active ingredients of P. notoginseng are easily hydrolyzed by gastric fluid into aglycones and sugars, resulting in low bioavailability and poor therapeutic effect (12,13). Therefore, it is important to develop a novel oral dosage form to address these limitations of conventional preparations.
Currently, several preparation methods are used to enhance the efficacy of Compound Danshen, among which the osmotic pump system (OPS) has attracted wide attention owing to the unique drug release mode and controllable drug release rate (14,15,16,17,18,19). The OPS, which exhibits sustained drug release driven by osmotic pressure, can improve patient compliance by reducing the frequency of drug administration. Moreover, the drug release behavior of OPS generally follows zero-order kinetics, and it is not affected by factors such as gastrointestinal motility, environmental pH, and food presence (20,21,22,23,24,25,26). In addition, several studies on OPS have shown that simultaneous release of different drugs can be achieved by adjusting the composition of the core components of the OPS (27,28). Moreover, the oral colon-specific drug delivery system (OCDDS) can directly deliver drugs to the colon and provide a mild environment with close to neutral pH, and thus, protecting acid- and enzyme-labile drugs (29,30,31). Furthermore, a longer transit time in the colon can prolong the residence of drugs in the body (32,33,34,35). Therefore, the combined use of OCDDS and OPS can overcome the limitations associated with the conventional Compound Danshen products.
In our previous study, we developed a colon-specific osmotic pump capsule (COPC) of P. notoginseng saponins, which was proved to achieve colon-specific and zero-order release, thus improving the bioavailability of P. notoginseng saponins. Based on this achievement, the great potential of COPC in Compound Danshen delivery has been confirmed. Therefore, in the present study, we used COPC for the delivery of a Chinese herbal compound that contains more complex components.
Materials and Methods
Materials
Radix S. miltiorrhiza extract was extracted in our laboratory (marker concentrations: 30.20 mg/g salvianolic acid B and 1.21 mg/g tanshinone IIA; lot number: 20161129). Panax notoginseng extract was also extracted in our laboratory (marker concentrations: 31.32 mg/g notoginsenoside R1, 54.26 mg/g ginsenoside Rg1, 51.37 mg/g ginsenoside Re, 57.01 mg/g ginsenoside Rb1, and 21.57 mg/g ginsenoside Rd.; lot number: 20161129). Borneol was purchased from Lifang Pharmacy (Anhui, China). Astragaloside, notoginsenoside R1, ginsenoside Rg1, ginsenoside Re, ginsenoside Rb1, ginsenoside Rd., salvianolic acid B, and tanshinone IIA were purchased from the National Institutes for Food and Drug Control (Beijing, China). Eudragit® S100 was gifted by Evonik Company (Essen, Germany). Cellulose acetate (CA) was obtained from Sinopharm Chemical Reagent Company (Shanghai, China). Hydroxypropyl-β-cyclodextrin (HP-β-CD) was obtained from Nanjing Otuo Funi Biotechnology Co., Ltd. (Jiangsu, China). Polyethylene glycol (PEO) with average molecular weights of 1 × 105 (PEO WSR N10), 2 × 105 (PEO WSR N80), and 9 × 105 (PEO WSR N1105) was obtained from Dow Chemical Company (Midland, MI, USA). Ludipress was received from BASF SE (Ludwigshafen, Germany). Acetone was obtained from Shanghai Pilot Chemical Company (Shanghai, China). Commercial Compound Danshen tablets (214 mg/tablet) were manufactured by Guangzhou Baiyunshan Hutchison Whampoa Chinese Medicine Co., Ltd. (Yunnan, China). The other chemicals were of analytical reagent grade.
Methods
Preparation of the COPC of Compound Danshen
The COPC was formulated and prepared as previously described (15). The shell of the COPC was prepared by the dip plastic method. Firstly, the coating solution was prepared by dissolving CA, PEG 6000, and Eudragit® S100 in a solvent mixture of acetone and water (9.5 mL/0.5 mL). The capsule mold was slowly dipped into the coating solution. Next, the mold was lifted up vertically and rotated three times. The above operations were repeated three times. The mold was dried at a temperature of 25°C and humidity of 60% for 2 h after the coating solution was evenly dispersed on the surface of the capsule mold. Afterward, the capsule was plucked out from the mold and trimmed by a capsule cutter machine. Finally, a 0.8-mm hole was drilled on the top of the capsule cap by a Lumonics Phase I laser (Tianjin Institute of Industrial Automation Instrument, Tianjin, China) and sealed with 15% (w/v) Eudragit® S100 solution.
The dosage of the COPC of Compound Danshen was selected based on the requirements of the Chinese Pharmacopoeia 2015 edition (ChP. 2015) for CDTs (not less than 0.2 mg of tanshinone IIA, 5 mg of salvianolic acid B, and 6 mg of a mixture of notoginsenoside R1, ginsenoside Rg1, ginsenoside Re, and ginsenoside Rb1 per tablet).
Firstly, Salvia miltiorrhiza extract (174 mg), Radix P. notoginseng extract (32 mg), borneolum (8 mg), and a specific amount of NaCl, penetration polymer, solubilizer, and ludipress were passed through a 100-mesh sieve individually and then uniformly mixed using a mortar and loaded into the body of capsules. The cap was nested on the body and the seam was sealed with a coating solution to prevent content leakage.
In Vitro Dissolution Test
To optimize the COPC formulation of Compound Danshen, a single-factor method was used to investigate influencing factors including the amount of NaCl, type and amount of suspending agent, as well as type and amount of solubilizer through in vitro dissolution test of different formulations. The details of the different COPC formulations are provided in Table I.
An in vitro dissolution test was carried out using a dissolution apparatus (AT 7smart; SOTAX Technology Co., Ltd., Switzerland) at 37.5°C ± 0.5°C with a rotation speed of 100 rpm and dissolution medium volume of 900 mL, according to the basket method in the Chinese Pharmacopoeia 2015 edition (ChP. 2015).
The dissolution test was performed in simulated gastric fluid (SGF, pH 1.0) for 2 h, followed by 3 h in phosphate buffer saline (PBS, pH 6.8), and finally for another 12 h in PBS (pH 7.8). The dissolution apparatus was set to withdraw 5 mL of sample at predetermined sampling times (2, 3, 5, 7, 9, 11, 13, 15, and 17 h) and replaced by the same volume of fresh dissolution medium. All samples were passed through a 0.45-μm membrane filter. The seven indicative components of Compound Danshen were simultaneously detected using the dual-wavelength method by ultra-performance liquid chromatography (the UPLC chromatogram is showed in Fig. 1). The detection wavelengths were 279 (for salvianolic acid B and tanshinone IIA) and 203 nm (for notoginsenoside R1 and ginsenoside Rg1, Rb1, Re, and Rd), and the cumulative release was calculated at each time point.
The similarity factor (ƒ2) is recommended by the FDA to evaluate the similarity among release curves of solid preparations, and the formula used to calculate it is as follows (36):
where Rt and Tt represent the release rate of the reference and test samples, respectively, and n is the sampling number. The ƒ2 ranges from 0 to 100. If ƒ2 is higher than 50, it indicates a better release profile similarity. If ƒ2 is less than 50, the release curves are not similar.
Evaluation of Drug Release Kinetics
The in vitro drug release kinetics was fitted with the zero-order, first-order, and Higuchi models. The coefficient of correlation was employed to evaluate the drug release kinetics of COPC Table II.
Influence of Differences in Capsule Internal and External Osmotic Pressure on Drug Release
The internal and external osmotic pressure difference of the COPC in the in vitro dissolution test was measured using an auto freezing point osmometer (Shanghai Medical University Instrument, Shanghai, China). Capsules of the same batch were obtained from the dissolution apparatus individually at the predetermined time intervals (2, 3, 5, 7, 9, 11, 13, 15, and 17 h). The capsules were carefully cut open. Twenty microliters of the liquid contents was diluted 100 times with the corresponding dissolution medium prior to the determination of osmotic pressure. Meanwhile, the osmotic pressure of the bulk dissolution medium at the same time point was also measured, and the difference between the osmotic pressures was calculated.
Scanning Electron Microscopy
Scanning electron microscopy was used to evaluate the surface and cross section of the shell of COPC before and after the in vitro dissolution test. The outer surface sample was prepared by cutting the COPC shell before and after the dissolution test and dried at 40°C for 2 h. Cross section sample was prepared by fracturing the capsule shell in liquid nitrogen to obtain complete a cross section and dried at 40°C for 2 h. The samples were studied under a scanning electron microscope (EVO18; Carl Zeiss, Germany) at a magnification power of 500 × and 10 k×. The accelerating voltage was 10 kV.
In Vivo Study in Beagle Dogs
The protocol of the animal experimental study was approved by the Anhui Medical University Animal Experimental Ethics Committee (Hefei, China). The beagle dogs used in the experiment were provided by the Experimental Animal Center of Anhui Medical University. Nine male beagle dogs (11 ± 2.5 kg) were randomly assigned to three groups (Groups A, B, and C) with three dogs per group. The dogs were fasted for 12 h before a single oral dose administration of three CDTs (Group A), three colon-specific capsules of Compound Danshen (S. miltiorrhiza extract, Radix P. notoginseng extract, and Borneol were loaded into the colon-specific capsule without optimized excipient, CC) (Group B), and three COPCs of Compound Danshen (Group C). Each group received the same oral dose containing 522 mg S. miltiorrhiza extract, 96 mg Radix P. notoginseng extract, and 24 mg Borneol with 200 mL of water via a feeding tube. The dogs had free access to food and drinking water throughout the study. About 3 ml of venous blood was sampled before drug administration and at the predetermined time intervals. It was then placed in heparinized tubes. The sampling time points were 0.5, 1, 1.5, 2, 2.5, 3, 4, 6, 8, 10, 12, 24, and 36 h for Group A; 2, 3, 5, 5.5, 6, 6.5, 7, 7.5, 9, 11, 13, 15, 17, 24, 30, and 36 h for Group B; and 2, 3, 5, 6, 7, 9, 11, 13, 15, 17, 24, 30, and 36 h for group C. The collected blood samples were centrifuged at 3000 rpm for 10 min, and then the upper plasma layer was collected and stored at −20°C. About 20 μL of the internal standard (methanol solution of astragaloside, 530 μg/mL), 150 μL of plasma, and 450 μL of acetonitrile were mixed and vortexed for 2 min. The mixture was centrifuged at 12,000 rpm for 10 min. The supernatant was separated and dried in a 40°C water bath. The residue after drying was reconstituted with 150 μL of methanol. The reconstituted sample was vortexed for 1 min and centrifuged for 10 min at 12,000 rpm. Finally, 4 μL of the supernatant was collected for the UPLC-MS/MS analysis (37).
UPLC-MS/MS Assay for the Seven Indicative Components of Compound Danshen
Ultra-performance liquid chromatography-electrospray tandem mass spectrometry (UPLC-MS/MS) analytical method was established to determine the seven indicative components of Compound Danshen in the plasma of beagle dogs. The UPLC-MS/MS apparatus comprised an Agilent 1290 UPLC system, a Triple QuadTM 4500 Mass Spectrometer (AB SCIEX Company, USA), an electrospray ionization source, and an autosampler.
The Waters ACQUITY UPLC® BEH C18 column (100 mm × 2.1 mm, 1.7 μm) was used. The mobile phases were 0.1% formic acid water (A) and acetonitrile (B) at the flow rate of 0.4 mL/min, and the column temperature was 40°C. A gradient elution was utilized with the following profile: 0–1.0 min, 70% A; 1.0–2.0 min, 60% A; 2.0–4.0 min, 51% A; 4.0–4.1 min, 52% A; 4.1–7.1 min, 15% A; 7.0–7.1 min, 30% A; and 7.1–8.0 min, 70% A. The ESI source and the positive ion mode were used, and the optimized mass spectrometry conditions were as follows: IV, 5500 V; TEM, 450°C; CUR, 35 psi; Gas 1, 65 psi; and Gas 2, 65 psi. The mass spectrometry multi-reaction monitoring (MRM) parameters of the seven active ingredients (namely, notoginsenoside R1, ginsenoside (Rg1, Re, Rb1, and Rd), salvianolic acid B, and tanshinone IIA) and IS (astragaloside) were optimized (Tables II and III).
Statistical Analysis
The DAS 2.0 pharmacokinetics software was used to calculate pharmacokinetics parameters. All data are expressed as mean ± standard deviation. The one-way analysis of variance was used to analyze the data.
In Vivo Imaging Studies
Multislice spiral CT (MSCT) was used to monitor the fate of the capsules in the gastrointestinal (GI) tract of beagle dogs. Three male beagle dogs (11 ± 2.5 kg) were provided by the Experimental Animal Center of Anhui Medical University. The nontoxic contrast agent barium sulfate was used to replace a part of the core components of the optimized COPC of Compound Danshen to track the location of the capsule and observe drug release in the GI of beagle dogs. The beagle dogs (11 ± 2.5 kg) were fasted for 12 h before the administration of the COPC loaded with barium sulfate with 200 mL of water via a feeding tube. MSCT images were captured at predetermined times (2, 6, and 9 h) to trace the capsule in vivo. MSCT imaging was carried out in 64-row 128-slice spiral CT (Siemens, Germany) by placing the beagle dogs in the prone position.
Results and Discussions
Effect of the Osmotic Agent on Drug Release
The osmotic pump capsules require a high osmotic pressure to release the drug. Generally, the drug itself cannot produce enough osmotic pressure to maintain a continuous and stable release profile. Therefore, it is necessary to add an osmotic agent to increase the osmotic pressure difference across the capsule shell. NaCl was selected as the osmotic agent, which can result in a high osmotic pressure at an equivalent amount than that of other osmotic agents. In this study, different amounts (80, 100, and 120 mg; Table I F1–F3) of NaCl were investigated to understand its effect on drug release (Fig. 2). An increased drug release rate and thorough release were achieved with a high amount of NaCl. Slow and incomplete release was observed with 80 mg NaCl, whereas 100 and 120 mg NaCl yielded complete drug release with a more consistent drug release rate in the former. Hence, the optimum amount of NaCl was selected as 100 mg.
Effect of Type and Amount of Suspending Agent on Drug Release
The powder of TCM extract, which contains polysaccharides, can easily adhere to the internal surface of the capsule shell during the dissolution test, hindering the release of the drug. Therefore, a suspending agent is used to enhance the dissolution rate and diffusion of water into the contents of the capsule. Three types of PEO (Table I F4–F6), namely, WSR N10, WSR N80, and WSR N1105, were utilized as a suspending agent in this study. The effect of various types of PEO on drug release is shown in Fig. 3a, b, and c. As the molecular weight of PEO increased, the viscosity increased, which slowed down water absorption, hydration rate, and drug release. Thus, WSR N10 was selected as the ideal suspending agent. The amount of WSR N10 was 20 mg (Fig. 3d), at which a more simultaneous release of multiple active ingredients was achieved.
Effect of Type and Amount of Solubilizer on Drug Release
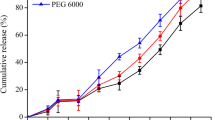
Compound Danshen contains multiple water-soluble components with different solubilities. As shown in Figs. 1 and 2, tanshinone IIA, a lipophilic component in S. miltiorrhiza, presented an incomplete and asynchronous release. In this study, four types of solubilizers were evaluated. The effect of the solubilizers on the release of tanshinone IIA is shown in Fig. 4a. The results revealed that HP-β-CD resulted in a drug release curve that best fitted to zero-order when compared with that of the other solubilizers. Meanwhile, tanshinone IIA and HP-β-CD could form an inclusion complex, which improved the release performance of the components (38). The amount of HP-β-CD was optimized to 20 mg to exhibit a zero-order release as shown in Fig. 4b, whereas 40 mg of HP-β-CD caused a burst release in 4–6 h.
Evaluation of the Optimal Formulation
The optimal formulation obtained using the single-factor method consists of NaCl 25%, PEO wsr-N10 5%, and HP-β-CD 5% (all presented in w/w of the core components). The formulation and preparation of the COPC shell were based on a previous study (12). The COPC of Compound Danshen was thereafter assembled using the optimized core and capsule shell for the in vitro release evaluation. As shown in Fig. 5c, cumulative release of the seven indicative components in artificial SGF (pH 1.0) and PBS (pH 6.8) was less than 10% of the labeled amount. However, in PBS of pH 7.8, the drug release rate was close to zero-order kinetics, and the release profiles of the seven indicative components were similar. Furthermore, the release curves of CDT, CC, and COPC were compared by measuring the accumulated release rate of the indicative components. Figure 5a shows that the release of components from the commercial tablet ended within 2 h and the release of notoginseng components and tanshinone IIA was low. This could be because the notoginseng components are decomposed in artificially simulated gastric fluid and that tanshinone IIA, as a fat-soluble component, has low solubility and dissolution rate in water. Besides, the release profiles of the indicative components from CDT were not similar. Contrary to that in the commercial tablets, the notoginseng components in CC presented a higher accumulative release due to the protection by the capsule from the artificially simulated gastric fluid. However, it still showed asynchronous release of different components. On the contrary, the COPC not only prevented the decomposition of notoginseng components but also yielded a simultaneous release of all the components.
Drug Release Kinetics
The release profiles of the indicative components were fitted to different models. Table II illustrates that the fitting coefficients of the seven indicative components were the highest when fitted to the zero-order model.
Drug Release Mechanism
In our previous studies, we focused on the effects of different factors on drug release from COPC and found that drug release from the COPC was not dependent on equipment type or agitation speed (15). The effect of osmotic pressure on OPS has been investigated by adjusting the osmotic pressure of the dissolution medium (18,19). This method is widely adopted, but it cannot assess the release mechanism of the osmotic system comprehensively and intuitively. In this study, a direct method that determines the osmotic pressure inside the capsule was used to investigate the relationship between osmotic gradient and drug release. Figure 6 illustrates that the osmotic pressure difference across the capsule shell showed a gradual increase during the first 7 h, which elucidated increasingly dissolved amount of water-soluble components within the capsule. The osmotic pressure difference gradually decreased with the release of the capsule contents. The release of the drug (with salvianolic acid B as an example shown in Fig. 5) was also faster during the first 7–9 h, in accordance with the higher osmotic pressure gradient across the capsule. These results further clarified the relationship between osmotic pressure and drug release from COPC.
Scanning Electron Microscopy
The outer surface and cross section of the capsule shell before and after the dissolution test were examined by scanning electron microscopy to observe the morphological changes in COPC shell during the dissolution test and to evaluate the mechanism of drug release from the COPC. Figure 7 shows that before dissolution, the outer surface of the capsule shell was smooth without any pores or cracks, and the cross section also showed a smooth surface without any cracks. Some depressions were observed on the surface at a magnification power of 10 k×, which might be due to the use of volatile solvent during the dipping process.
After the dissolution test, several pores were observed on the surface, while the capsule shell was still intact. Meanwhile, the cross section showed a series of depressions of varying depths across the shell, and a spongy porous structure was found at a magnification of 10 k×. It can be explained that the pore former was leached from the membrane gradually as the release experiment progressed, and pores through the capsule membrane were formed, which increased the osmotic pressure of the capsule gradually by allowing water to enter the capsule. This inference was also consistent with the results of the drug release mechanism test.
Pharmacokinetic Studies
Compound Danshen contains several chemical components, which would affect the release behavior of the active components. Thereby, seven indicative components were monitored during the pharmacokinetic studies. The UPLC-MS/MS method was used to evaluate their plasma drug concentration in beagle dogs due to the low concentrations of those components in the blood.
The seven indicative component concentration-time curves after oral administration of CDT, CC, and COPC in beagle dogs are illustrated in Fig. 8. It showed that CDT peaked in a short period but dropped abruptly compared with that of the other two groups. The CC group showed a 5-h delayed peak with slower decrease. However, the blood concentration of CC group also fluctuated greatly. Contrarily, the COPC group not only achieved longer delayed peak but also shows a wider peak, indicating a delayed and sustained drug release of COPC. The main pharmacokinetic parameters summarized in Table IV revealed that the Tmax of seven indicative component in COPC group was significantly prolonged and all around 11 h, suggesting a delayed and simultaneous releases from COPC. Moreover, the integrated MRT for COPC is 11.77 h versus 5.90 h and 8.02 h for CDT and CC group. More importantly, the AUC was significantly improved, the area under the curve (AUC0 → 36h) for COPC is 303.01 ng·h·mL−1, whereas CDT and CC are found to be 92.97 ng·h·mL−1 and 102.40 ng·h·mL−1. The relative bioavailability was 330.58% and 292.62% in comparison with that of CDT and CC (Table V). Furthermore, the unbroken COPCs were excreted from beagle dogs, which demonstrated that osmotic pump capsule did not disintegrate in vivo and that the drug was released gradually through the pores in the cap of the capsule.
In conclusion, the COPC could significantly improve the bioavailability of Compound Danshen compared with the market CDT. At the same time, compared with OCDDS system, the combination of OPS and OCDDS can improve the bioavailability of drugs and avoid the fluctuation of blood concentration.
In Vivo Imaging Studies
Currently, a variety of oral drug delivery systems has been applied to evaluate drug release of OCDDS in vivo (39,40,41). Multislice spiral CT scanning technology uses X-ray beam to obtain scanning trajectory spiral during information acquisition (42). This new scanning method considerably improves scanning efficacy and offers high value in the evaluation of OCDDS preparations in vivo.
In this study, MSCT scanning was used to evaluate the colon-specific characteristics of the capsule visually. Figure 9 shows the fate of the COPC in beagle dogs. Two hours after administration, an obvious highlight was found in the stomach in the frontal plane, whereas a complete capsule was observed in the transverse and sagittal planes. This suggests that the capsule was intact and stable in the hostile environment of the stomach without any drug leakage. Furthermore, the capsule reached the small intestine 6 h after administration, and an intact capsule was found in the transverse plane. Meanwhile, the highlights found in the frontal and sagittal planes were of an intact capsule shape, indicating that the capsule was still intact without drug leakage. At 9 h, the capsule was migrated toward the colon region and the drug was released from the capsule. The core components including barium sulfate in the capsule was released and distributed from the transverse colon to the descending colon.
Multislice spiral CT scanning of the colon-specific osmotic pump capsules in beagle dogs. 2 h, images of capsule in the stomach in the frontal plane (a), sagittal plane (b), and transverse plane (c). 6 h, images of capsule in the small intestine in the frontal plane (d), sagittal plane (e), and transverse plane (f). 9 h images of capsule in the colon in the frontal plane (g), sagittal plane (h), and transverse plane (i)
The results demonstrated that the capsule can direct drug release specifically in the colon region in vivo and this was consistent with the results of the in vitro dissolution test, providing an intuitive basis for the conclusions of pharmacokinetics study.
Conclusions
In the present study, a novel COPC of Compound Danshen was successfully developed and optimized to achieve simultaneous zero-order release of multiple active components of Compound Danshen in the colon. The drug release profiles showed a zero-order release of the seven active ingredients in Compound Danshen over 12 h at pH 7.8 through the pores in the capsule cap. The results also confirmed that the release was driven by the differential osmotic pressure gradient across the capsule shell and changes in the capsule shell were observed by scanning electron microscopy. The pharmacokinetics studies in beagle dogs after oral administration of CDT, CC, and COPC showed the significantly prolonged Tmax and MRT controlled-release effects of the COPC. The relative bioavailability of the seven indicative components was significantly increased to 330.58%, compared with that of the CDT. Furthermore, in vivo imaging studies showed that the osmotic pump capsule was stable in the GI tract and that it was able to deliver the drug specifically to the colon. In conclusion, we addressed the limitations associated with Compound Danshen using the COPC system. It presented a promising strategy to achieve simultaneous release of multiple active ingredients, therefore improving the bioavailability of other Chinese herbal compounds, which otherwise suffer from similar delivery issues that prevent their clinical usefulness.
References
Wang X, Morris-Natschke S, Lee K. New developments in the chemistry and biology of the bioactive constituents of Tanshen. Med Res Rev. 2007;27(1):133–48.
Shi M, Huang F, Deng C, Wang Y, Kai G. Bioactivities, biosynthesis and biotechnological production of phenolic acids in Salvia miltiorrhiza. Crit Rev Food Sci Nutr. 2018:1–12.
Cheng TO. Cardiovascular effects of Danshen. Int J Cardiol. 2007;121(1):9–22.
Li M, Li Q, Zhang C, Zhang N, Cui Z, Huang L, et al. An ethnopharmacological investigation of medicinal Salvia plants (Lamiaceae) in China. Acta Pharm Sin B. 2013;3(4):273–80.
Yan G, Zhu Z, Jin L, Chen J, Xie H, Miozzi J, et al. Study on the quality evaluation of compound Danshen preparations based on the xCELLigence real-time cell-based assay and Pharmacodynamic authentication. Molecules. 2018;23(9):2090.
Li Y, Zhang Y, Zhu C. Pharmacokinetics and correlation between in vitro release and in vivo absorption of bio-adhesive pellets of Panax notoginseng saponins. Chin J Nat Med. 2017;15(2):142–51.
Li D, Song HT, Chu Y, Chen DW, He ZG. Preparation of compound Danshen sustained-release Capsula by multiparticulate time-controlled release technology. Chin Tradit Herb Drugs. 2009;40:544–8.
Xian Z, Valentina R-N, Antony K, Dennis C, Chunguang L, Alan B, et al. Synergistic effects of Danshen (Salvia Miltiorrhizae Radix et Rhizoma) and Sanqi (Notoginseng Radix et Rhizoma) combination in angiogenesis behavior in EAhy 926 cells. Medicines. 2017;4(4):85.
Chunyan SU, Ming Q, Rahman K, Han T, Qin L. Salvia miltiorrhiza: traditional medicinal uses, chemistry, and pharmacology. Chin J Nat Med. 2015;13(3):163–82.
Shen Q, Li J, Zhang C, Wang P, Mohammed A, Ni S, et al. Panax notoginseng saponins reduce high-risk factors for thrombosis through peroxisome proliferator-activated receptor -γ pathway. Biomed Pharmacother. 2017;96:1163–9.
Xue L, Yuanbo LI, Guo D, Yin J, Liu Y, Hou S. Study on preparation and release mechanism of effervescent osmotic pump tablet of compound Danshen. China J Chin Mater Med. 2009;34(7):848–51.
Duan L, Xiong X, Hu J, Liu Y, Wang J. Efficacy and safety of oral Panax notoginseng saponins for unstable angina patients: a meta-analysis and systematic review. Phytomedicine. 2018;47(1):23–33.
Duan L, Xiong X, Hu J, Liu Y, Li J, Wang J. Panax notoginseng Saponins for treating coronary artery disease: a functional and mechanistic overview. Front Pharmacol. 2017;8:702.
Li X, Pan W, Nie S, Wu L. Studies on controlled release effervescent osmotic pump tablets from traditional Chinese medicine compound recipe. J Control Release. 2004;96(3):359–67.
Jin D, Wang B, Hu R, Su D, Chen J, Zhou H, et al. A novel Colon-specific osmotic pump capsule of Panax notoginseng Saponins (PNS): formulation, optimization, and in vitro-in vivo evaluation. AAPS PharmSciTech. 2018;19(5):2322–9.
Malaterre V, Ogorka J, Loggia N, Gurny R. Evaluation of the tablet Core factors influencing the release kinetics and the Loadability of push–pull osmotic systems. Drug Dev Ind Pharm. 2009;35(4):433–9.
Huang Y, Zhang S, Shen H, Li J, Gao C. Controlled release of the Nimodipine-loaded self-microemulsion osmotic pump capsules: development and characterization. AAPS PharmSciTech. 2018;19(3):1–12.
Xin T, Yang Z, Jing H, Zhang W, Gao Y, Yang X, et al. A time-released osmotic pump fabricated by compression-coated method: formulation screen, mechanism research and pharmacokinetic study. Asian J Pharm Sci. 2014;9(4):208–17.
Cheng L, Li T, Dong L, Wang X, Huo Q, Wang H, et al. Design and evaluation of bilayer pump tablet of Flurbiprofen solid dispersion for zero-order controlled delivery. J Pharm Sci. 2017;107(5):1434–42.
Cheng L, Gai X, Wen H, Liu D, Tang X, Wang Y, et al. Aqueous polymer dispersion coating used for osmotic pump tablets: membrane property investigation and IVIVC evaluation. AAPS PharmSciTech. 2017;19(1):1–9.
Theeuwes F. Elementary osmotic pump. J Pharm Sci. 1975;64(12):1987–91.
Hill A, Breyer S, Geissler S, Mier W, Haberkorn U, Weigandt M, et al. How do in-vitro release profiles of nanosuspensions from Alzet®; pumps correspond to the in-vivo situation? A case study on radiolabeled fenofibrate. J Control Release. 2013;168(1):77–87.
Rachna R, Teller RS, Mesquita PMM, Herold BC, Kiser PF. Osmotic pump tablets for delivery of antiretrovirals to the vaginal mucosa. Antivir Res. 2013;100(1):255–8.
Ali R, Walther M, Bodmeier R. Cellulose acetate butyrate: Ammonio methacrylate copolymer blends as a novel coating in osmotic tablets. AAPS PharmSciTech. 2017;19(1):1–7.
Elzahaby SA, Aboughaly MHH, Abdelbary G, Elgazayerly ON. Zero order release and bioavailability enhancement of poorly water soluble Vinpocetine from self-nanoemulsifying osmotic pump tablet. Pharm Dev Technol. 2018;23(9):900–10.
Defang O, Shufang N, Wei L, Hong G, Hui L, Weisan P. In vitro and in vivo evaluation of two extended release preparations of combination metformin and glipizide. Drug Dev Ind Pharm. 2005;31(7):677–85.
Qin C, He W, Zhu C, Wu M, Jin Z, Zhang Q, et al. Controlled release of metformin hydrochloride and repaglinide from sandwiched osmotic pump tablet. Int J Pharm. 2014;466:276–85.
Zhao S, Yu F, Liu N, Di Z, Yan K, Liu Y, et al. Synchronous delivery of felodipine and metoprolol tartrate using monolithic osmotic pump technology. Drug Dev Ind Pharm. 2016;42(1):1723–31.
Den Mooter GV, Kinget R. Oral colon-specific drug delivery: a review. Drug Deliv. 1995;2(2):81–93.
Singh A, Sharma A, Pooja, Anju. Novel approaches for colon targeted drug delivery system. J Med Vet Mycol. 2014;26(2):207–17.
Del Curto MD, Palugan L, Foppoli A, Zema L, Gazzaniga A, Maroni A. Erodible time-dependent Colon delivery systems with improved efficiency in delaying the onset of drug release. J Pharm Sci. 2014;103(11):3585–93.
Ding Y, Lin Q, Kan J. Development and characteristics nanoscale retrograded starch as an encapsulating agent for colon-specific drug delivery. Colloids surf., B. 2018;171(1):656–67.
Patel MM. Cutting-edge technologies in colon-targeted drug delivery systems. Expert Opin Drug Deliv. 2011;8(10):1247–58.
Lu L, Chen G, Qiu Y, Li M, Liu D, Hu D, et al. Nanoparticle-based oral delivery systems for colon targeting: principles and design strategies. Chin Sci Bull. 2016;61(9):670–81.
Banerjee A, Pathak S, Subramanium VD, Dharanivasan G, Verma RS. Strategies for targeted drug delivery in treatment of colon cancer: current trends and future perspectives. Drug Discov Today. 2017;22(8):1224–32.
Shah VP, Tsong Y, Sathe P, Liu J. In vitro dissolution profile comparison—statistics and analysis of the similarity factor, f2. Pharm Res. 1998;15(6):889–96.
Yang S, Zhang K, Lin X, Miao Y, Meng L, Chen W, et al. Pharmacokinetic comparisons of single herb extract of Fufang Danshen preparation with different combinations of its constituent herbs in rats. J Pharm Biomed Anal. 2012;67–68:77–85.
Wang L, Jiang X, Xu W, Li C. Complexation of tanshinone IIA with 2-hydroxypropyl-β-cyclodextrin: effect on aqueous solubility, dissolution rate, and intestinal absorption behavior in rats. Int J Pharm. 2007;341(1–2):58–67.
Li W, Shi CH, Sheng YL, Cui P, Zhao YQ, Zhang XR. In vitro dissolution and in vivo gamma scintigraphic evaluation of press-coated salbutamol sulfate tablets. Acta Pharma. 2013;63(4):545–51.
Lanjhiyana SK, Pranav B, Karthikeyan K, Sweety L, Muthu MS. Chitosan-sodium alginate blended polyelectrolyte complexes as potential multiparticulate carrier system: colon-targeted delivery and gamma scintigraphic imaging. Expert Opin Drug Deliv. 2013;10(1):5–15.
Celkan A, Acartürk F, Tuğcu-Demiröz F, Gökçora N, Akkaş BE, Güner LA. Gamma scintigraphic studies on guar gum-based compressed coated tablets for colonic delivery of theophylline in healthy volunteers. J Drug Delivery Sci Technol. 2016;32(1):31–7.
Liang X, Pauwels R, Jacobs R, Hassan B, Li L, Corpas L, et al. A comparative evaluation of cone beam computed tomography (CBCT) and multi-slice CT (MSCT): part I. on subjective image quality. Eur J Radiol. 2010;75(2):265–9.
Funding
This study was supported by the National Natural Science Foundation of China (No.81573615, No.81274100), the National Science and Technology Support Plan (Project No. 2012BAI26B03), and the Project of Scientific Research Fund of Anhui University of Chinese medicine (No.2017zryb002).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
CONFLICT OF INTEREST
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nie, X., Wang, B., Hu, R. et al. Development and Evaluation of Controlled and Simultaneous Release of Compound Danshen Based on a Novel Colon-Specific Osmotic Pump Capsule. AAPS PharmSciTech 21, 38 (2020). https://doi.org/10.1208/s12249-019-1603-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-019-1603-9