Abstract
Non-alcoholic fatty liver disease (NAFLD) is a substantial contributor to liver-related morbidity worldwide, and yet, there are no standard, universal pharmacologic therapies approved for this indication. The aim of this systematic review and meta-analysis is to evaluate the effectiveness of SGLT-2 inhibitors in improving hepatic steatosis and hepatic fibrosis in patients with NAFLD. An extensive electronic database search was done to identify studies published from inception until December 2023, without any language restrictions. All randomized controlled trials (RCT) that evaluated the use of SGLT-2 inhibitors for patients with NAFLD, regardless of diabetes mellitus status, were included. The Cochrane Risk of Bias 2.0 tool was used to assess the risk of bias of each study included. Evidence from all studies were synthesized as mean differences for continuous data, and as risk ratio for dichotomous outcomes. An inverse variance or Mantel–Haenszel test was used in conjunction with a random-effects meta-analysis model, where necessary. 18 eligible RCTs involving 1330 participants were analyzed, all of which had risk of bias ranging from low to some concerns. Significant difference in means was observed for controlled attenuation parameter (6 trials, n = 372; MD: − 10.59 dB/m, 95% CI [− 18.25, − 2.92], p = 0.007, I2 = 0%); L/S ratio (3 trials, n = 163; MD: 0.11, 95% CI [0.01, 0.21], p = 0.04, I2 = 78%); LSM (7 trials, n = 447; MD: − 0.67 kPa, 95% CI [− 1.19, − 0.16], p = 0.010, I2 = 69%); MRI-PDFF (5 trials, n = 330; MD: − 2.61%, 95% CI [− 5.05, − 0.17], p = 0.04, I2 = 78%), and FIB-4 index (10 trials, n = 648; MD: − 0.12, 95% CI [− 0.21, − 0.04], p = 0.005, I2 = 16%) after SGLT-2 inhibitor treatment as compared to controls. In conclusion, the use of SGLT-2 inhibitors may lead to slight improvement of hepatic steatosis and/or fibrosis as compared to controls in patients with NAFLD and Type 2 diabetes mellitus based on imaging and histopathology biomarkers with low to moderate certainty of evidence.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Non-alcoholic fatty liver disease (NAFLD) is a major cause of liver-related morbidity globally, with prevalence rates as high as 30%1, and steadily increasing number of cases, from 391.2 million in 1990 to 882.1 million in 20172.
It appears to be associated with one or more components of the metabolic syndrome, which include hypertension, dyslipidemia, obesity, and Type 2 diabetes mellitus and insulin resistance1,3. Although its pathogenesis has not yet been completely established, growing evidence shows that insulin resistance and dysregulation in lipid metabolism play huge roles in the development of hepatic steatosis. High fat diet, insulin resistance, obesity, dysregulated peripheral lipolysis, and other potential risk factors lead to increased entry of free fatty acids into the liver, which places hepatocytes under a ‘lipotoxic’ condition4. The accumulation of triacylglycerol in the hepatocyte cytoplasm presents histologically as steatosis. With the constant, repeated micro-hepatic injury, endoplasmic reticulum stress and mitochondrial dysfunction now arise. This then leads to lobular inflammation, cellular apoptosis, and hepatic fibrosis over time4.
If neglected, this treatable condition can lead to various severe consequences, such as advanced cirrhosis, hepatocellular cancer, and potentially cardiovascular morbidity5 and mortality6,7. Considering the prognostic consequences of NAFLD, effective therapy is warranted to prevent disease progression. Aside from weight loss and lifestyle modifications, pharmacologic treatments remain limited. In line with this, the role of a novel oral hypoglycemic agent called sodium–glucose cotransporter 2 (SGLT-2) inhibitor on the treatment of NAFLD has recently been investigated in various animal studies done on rodents models8,9,10 and human clinical trials11,12, with potential positive effects.
In a real-world study of 56 patients with NAFLD and Type 2 diabetes mellitus who received SGLT-2 inhibitors for 48 weeks, there were statistically significant decreases in both controlled attenuation parameter (CAP) from 312 dB/m at baseline to 280 dB/m at week 48, and liver stiffness measurement (LSM) from 9.1 kPa at baseline to 6.7 kPa at week 4811. Additionally, the SGLT-2 inhibitor group showed statistically significant reductions in body weight, alanine transaminase (ALT), uric acid, and Fibrosis-4 (FIB-4) index at week 48 in comparison to the non-SGLT-2 inhibitor group that received other oral hypoglycemic medications using the 1:1 propensity-score matched analysis11. Moreover, a meta-analysis of 10 randomized controlled trials with 573 participants showed that use of SGLT-2 inhibitors yielded statistically significant reductions in the levels of ALT, aspartate transaminase (AST), liver proton density fat fraction (MRI-PDFF), visceral fat mass area, and subcutaneous fat areas12.
The impetus for this systematic review and meta-analysis is to give a more precise estimate of effect and address variations with use of SGLT-2 inhibitors in the treatment of NAFLD to help guide clinical practice guideline development, with a renewed focus on the use of imaging and histopathology outcome measures as found in the up-to-date randomized controlled trials.
The objective of this meta-analysis is to evaluate the effectiveness of sodium–glucose cotransporter-2 (SGLT-2) inhibitors in improving hepatic steatosis and hepatic fibrosis using imaging biomarkers and histopathology in patients with non-alcoholic fatty liver disease.
Methodology
This present study was conducted in accordance with preferred reporting items for systematic review (PRISMA) guidelines13 (See also Supplementary Table S1).
Eligibility criteria
Studies were selected based on the following inclusion criteria: (1) randomized-controlled trials, regardless of blinding status, that include studies examining adult participants more than or equal to 18 years of age with diagnosed non-alcoholic fatty liver disease irrespective of other comorbidities with or without diabetes mellitus, obese or non-obese; (2) use of SGLT-2 inhibitors in the active experimental group and not restricted to a particular sub-type, dosage, frequency or duration; (3) for the comparators, studies with placebo or the usual standard of care as relevant controls.
Non-randomized clinical trials, cohort studies, case control studies or cross-sectional studies were excluded. There were no limitations regarding the type of setting and length of follow-up.
The primary outcomes included the controlled attenuation parameter (CAP) which is a method used to measure the degree of ultrasound attenuation by hepatic fat at the central frequency of FibroScan®. The CAP value is expressed in dB/m. The next primary outcome was the liver stiffness measurement (LSM) which refers to the non-invasive quantification of liver stiffness by transient elastography using FibroScan®. The LSM value is expressed as kilopascal or kPa. Another primary outcome of interest is the proportion of patients with at least one point improvement or one-stage reduction in the histological scores with respect to hepatic steatosis, hepatocellular ballooning, lobular inflammation, and fibrosis after treatment.
The secondary outcomes include the Fibrosis-4 (FIB-4) index which is a non-invasive scoring system from several laboratory tests that can predict significant hepatic fibrosis patients. It includes age (years), AST level (U/L), platelet count (109/L) and ALT (U/L). Other imaging biomarkers of hepatic steatosis included in this study were the liver-spleen attenuation ratio as quantified by computed tomography, and the magnetic resonance imaging derived proton-density-fat-fraction (MRI-PDFF) which enables a quantitative assessment of liver fat over the entire liver.
Information sources
Two independent reviewers (A.M.O.L., and J.A.P.) performed a comprehensive electronic database search via PUBMED14, Cochrane Central Register of Controlled Trials15, Embase16 and ACP Journal Club17, published from inception to 29 December 2023. Other unpublished trials and study registries were also sought after by scanning the ClinicalTrials.gov, ISRCTN Register, EU Clinical Trials Register and WHO ICTRP. The planned literature search was not restricted to the English language or publication date filter.
Search strategy
The MEDLINE search strategy entered at PubMED database14 was the use of the following terms: ((((((((((SGLT-2 inhibitor) OR (dapagliflozin)) OR (empagliflozin)) OR (ipragliflozin)) OR (tofogliflozin)) OR (canagliflozin)) OR (licogliflozin)) OR (luseogliflozin)) OR (ertugliflozin)) AND (non-alcoholic fatty liver disease)) OR (NAFLD) with filters for randomized controlled trial. These search terms were also similarly adapted for use with other electronic bibliographic databases15,16,17. We also attempted to look for other related articles that were not identified by electronic searches.
Selection process
Literature search results were imported to EPPI-Reviewer Version 4.14.2.0 for data management to facilitate the screening process18. Two independent reviewers (A.M.O.L, and J.A.P.) identified potentially eligible studies through screening of titles and abstracts, and assessed if these met the inclusion criteria. Any duplicate records of the same report were removed. For any disagreements between the authors, consensus of which articles to screen for full text were resolved by discussion. Subsequently, two researchers (A.M.O.L, and J.A.P.) independently screened full-text articles and scrutinized their eligibility. Again, any disagreements over the eligibility of the studies were resolved by consensus.
Data collection process
Two reviewers (A.M.O.L, and J.A.P.) independently extracted data from every report with the use of a standardized data collection form. The retrieved data were then compared. Any disagreements or discrepancies during the data collection process were resolved by reviewing the data again, and through a consensus discussion. A.M.O.L entered the data into Cochrane’s RevMan Web19, and again double checked for its completeness and accuracy. For missing data or unclear information, the reviewers attempted to correspond with the study investigators through their respective official email addresses.
Data items
We collected the following data from each included study: title and first author with citation details, study design, study location, total study duration, type and number of participants, study inclusion and exclusion criteria, baseline patient characteristics, detailed description of the intervention and control (type of drug used, dosage, frequency, duration of treatment), the outcome of interest and results.
Study risk of bias assessment
Two independent reviewers (A.M.O.L, and J.A.P.) assessed the risk of bias in included studies using the Cochrane Risk of Bias 2.0 (RoB 2.0) tool20. The domains in RoB 2.0 include bias arising from the randomization process; bias due to deviations from intended interventions; bias due to missing outcome data; bias in measurement of the outcome; and bias in selection of the reported result. The judgment of overall risk-of-bias were subdivided into “low risk of bias”, “some concerns” or “high risk of bias.”20. Any discrepancies in risk assessment were settled through constructive discussions between authors.
Effect measures
We used the unstandardized mean differences at 95% confidence interval for continuous data given the same measurement scales to assess outcomes. Additionally, we utilized the final measurement outcomes rather than the change-from-baseline outcomes as the latter was not reported in most of the studies and considering the difficulty to measure the outcomes precisely coupled with the skewness of the distribution21, hence the former was selected. For dichotomous data, we calculated the risk ratio (RR) and their 95% confidence interval.
Synthesis methods
To decide which studies were eligible for each synthesis, structured approaches were done with tabulation and coding of the main characteristics of the population, intervention, and outcomes. The intervention component of each study was coded along two dimensions namely SGLT-2 inhibitor only or SGLT-2 inhibitor plus another drug. The comparison group was likewise categorized into placebo only or standard of treatment, pioglitazone, ursodeoxycholic acid, tenegliptin, glimepiride, liraglutide, metformin, and metformin plus pioglitazone.
During the data synthesis, we noticed some continuous data presented as median and interquartile range. In this scenario, if the respective corresponding author cannot be contacted, we convert the study data into the estimated mean and standard deviation using the R-package ‘estmeansd 0.2.1’ for which was primarily referenced from the Mcgrath et al.22 2020 DEPRESsion Screening Data (DEPRESSD) Collaboration. There were also a few study data highlighted as mean and standard error (SE) for which it was converted to standard deviation (SD) using Revman Web by Cochrane19 and computed as SE multiplied by the square root of the sample size. In cases where there is no available information on variability measures, we did not exclude the studies from the meta-analysis. Instead, we imputed the missing data by getting the average standard deviations (SD) from other studies in the same meta-analysis.
To synthesize results, a meta-analysis of effect estimates was done using the Revman Web by Cochrane19. The random-effects meta-analysis model was chosen under the assumption that the true intervention effects are related through a distribution. The choice of this model was based on the clinical and methodological diversity of the included studies, and the concern for small-study effects. For continuous data, the inverse variance statistical method was used; while for dichotomous outcomes, the Mantel–Haenszel method was employed in consideration for some studies with small sample sizes and/or lower event rates21.
Heterogeneity among studies was identified in terms of clinical, methodological, and statistical factors. For statistical heterogeneity, assessment was done using the I2 statistics, with an interpretation of I2 value of 30–60% representing moderate heterogeneity, 50–90% indicating substantial heterogeneity, and 75–100% interpreted as considerable heterogeneity21. Whenever significant heterogeneity was detected, we proceeded with sensitivity analysis by omitting studies that are judged to be at high risk of bias, or excluding studies that are deemed ineligible such as unpublished data, inadequate sample sizes, substantial variances in patient characteristics, methodology or intervention21.
Reporting bias assessment
Funnel plot asymmetry was assessed for meta-analysis with at least 10 studies. It was interpreted by visual inspection and statistical tests using Egger regression and Begg & Mazumdar rank correlation. Additionally, assessment for selective outcome reporting or selective non-reporting of results was completed by directly examining if a study protocol/register is available prior to the published study, and if the outcomes stated in the protocol are concurrent with the published report. If a protocol was unavailable, we then compared the outcomes reported in the methods and results section of the published paper.
Certainty assessment
Two independent reviewers (A.M.O.L. and J.A.P.) evaluated the certainty of evidence for each outcome using the Grades of Recommendation, Assessment, Development and Evaluation Working Group (GRADE)23 approach. The rating criteria for considering lowering or raising the certainty of evidence was dependent on these factors, which consisted of risk of bias, inconsistency, indirectness, imprecision, publication bias, large effect, dose response and other plausible confounding bias. We utilized the online GRADEpro23 to generate the summary of findings table together with the footnotes as rationale for up-grade or down-grade the certainty of evidence.
Results
Study selection
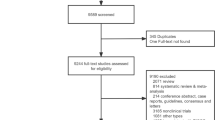
In the initial database search, we found a total of 1089 potential records (see Fig. 1). After eliminating the duplicates, we proceeded with screening the 854 records, from which we reviewed 37 full-text articles, and finally, we included 18 randomized-controlled studies24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41. Also, we comprehensively searched the references and other documents which cited these studies. However, no additional articles that fulfilled inclusion criteria were found in these searches.
We excluded 19 studies from our review because of the following reasons: Population criteria was not met in seven studies; there were no imaging/pathologic markers of steatosis or fibrosis or outcome of interest in six studies; SGLT-2 inhibitor was not used in one study; there were secondary publications of three included studies; there was incomplete data in one study; and there was still ongoing recruitment/trial in one study.
Study characteristics
Across 18 trials, a total of 1330 participants were included, with 631 in the SGLT-2 inhibitor group and 657 in the control group. No major differences in baseline characteristics were identified among the included studies. The mean age of participants ranged from 43.8 to 65.0 years in the SGLT-2i group and 41.8–65.6 years in the control group. All studies enrolled patients with non-alcoholic fatty liver disease based on ultrasonography24,27,29,32,35,36,37,40, computed tomography32,33,35, magnetic resonance imaging28,34, fatty liver index26, or pre-treatment biopsy findings30,38,39. Subsequently, two out of 18 studies excluded Type 2 diabetes mellitus in their eligibility criteria37,40. Empagliflozin, dapagliflozin, tofogliflozin, luseogliflozin, licogliflozin and ipragliflozin were the studied sodium-glucose cotransporter-2 inhibitors for the experimental group; whereas the control group had varied medications used including pioglitazone, metformin, glimepiride, tenegliptin, liraglutide, placebo or the usual standard of care. Lifestyle modifications and anti-diabetic drugs (including metformin, DPP4-inhibitors, sulfonylureas, and insulin) without any SGLT-2 inhibitors, pioglitazone or GLP-1 agonist, comprise the usual standard of care for Type 2 diabetes mellitus, which was used by three studies as control34,36,38. The course of treatment ranged from 12 to 72 weeks depending on the included trial. Other in-depth characteristics of included studies were presented in Table 1 and in the Supplementary Tables S2–S4 online.
Risk of bias in studies
The risk of bias of individual trials were assessed using the RoB 2.0 tool20. A summary of these assessments is provided in Table 2. Overall, most of the included studies (16/18) presented some concerns for risk of bias, while two studies were assessed as having low risk of bias.
Results of individual studies
For study results, see Figs. 2, 3, 4, 5, 6 and 7 which present the summary statistics for each of the individual studies, and the pooled effect estimates with their confidence intervals using Forest plots. The risk of bias judgments was also displayed beside the plot to consider the limitations of interpreting the findings.
Results of syntheses
Effect on hepatic steatosis
Controlled attenuation parameter (CAP)
Six randomized controlled trials (RCTs)24,29,31,36,37,39, including a combined total of 372 patients, compared the mean difference in controlled attenuation parameter (CAP) among non-alcoholic fatty liver patients given SGLT-2 inhibitor or the control intervention (see Fig. 2a). Each study utilized the transient liver elastography via FibroScan® to measure the controlled attenuation parameter as assessment for liver fat content. Five of the trials had some concerns for bias overall, owing to the lack of information on allocation concealment and/or use of per-protocol analysis. Empagliflozin was administered in two of the trials24,37, while ipragliflozin, tofogliflozin, and dapagliflozin were used in other trials as the active experimental group. For the control group, the medication given in each study slightly varies. Four trials were given standard of treatment for Type 2 diabetes mellitus, including one study receiving glimepiride39, metformin only31, respectively; the latter as combined metformin and pioglitazone29; whereas the other remaining two studies were given placebo24,37. After combining the results, the pooled mean difference in the reduction of CAP scores after randomly assigning to SGLT-2 inhibitor treatment versus the other comparators was (MD: − 10.59 dB/m, 95% CI [− 18.25, − 2.92], p = 0.007, I2 = 0%, moderate certainty of evidence).
(a) Forest plot of comparison: summary of mean difference in controlled attenuation parameter (CAP) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. (b) Forest plot of comparison [Sensitivity analysis, Taheri 2020 excluded]: summary of mean difference in controlled attenuation parameter (CAP) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control.
On sensitivity analysis, the study by Taheri et al.37 was excluded as the sample population criteria did not include NAFLD patients with Type 2 diabetes mellitus (see Fig. 2b). As compared with the previous pooled result, findings showed a higher mean difference in the reduction of CAP scores (MD: − 13.77 dB/m, 95% CI [− 23.00, − 4.55], p = 0.003, I2 = 0%, moderate certainty of evidence).
Liver-to-spleen attenuation (L/S) ratio
Only three studies32,33,35 measured the degree of fatty liver using L/S ratio on CT tomography during the study period (see Fig. 3). The liver-to-spleen attenuation ratio was calculated as the average liver attenuation at the region of interest divided by the average spleen attenuation using the unenhanced CT tomography. In total, 80 patients received SGLT-2 inhibitors and 83 patients received the control intervention. One trial35 was assessed to have low risk of bias while the remaining two32,33 had some concerns for bias due to lack of information on allocation concealment or blinding of the outcome assessor. The results showed that the SGLT-2 inhibitors significantly increased the L/S ratio by weighted mean difference (0.11, 95% CI [0.01, 0.21], p = 0.04, I2 = 78%, low certainty of evidence) compared to the control group.
Forest plot of comparison: summary of mean difference in liver-to-spleen attenuation (L/S) ratio post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Shibuya 2018 median and interquartile range study data converted to mean and SD using R-package ‘estmeansd 0.2.1’.
Liver proton density fat fraction (PDFF)
Five clinical trials27,28,30,34,41 provided data on the liver proton density fat fraction (PDFF) using magnetic resonance imaging (see Fig. 4a). A total of 175 cases and 155 controls had measured the MRI-PDFF (%) over the study period. The types of SGLT-2 inhibitors used include empagliflozin, dapagliflozin, licogliflozin, and tofogliflozin. The control intervention group consisted of placebo or standard of treatment for Type 2 diabetes mellitus other than SGLT-2 inhibitor, or pioglitazone treatment. Most of the studies presented some concerns for bias due to deviations from intended interventions with use of per-protocol analysis, and one trial34 lacked details on the concealment of the allocation sequence. The meta-analysis showed a trend towards a reduction in the liver proton density fat fraction at the end of treatment (MD: − 2.61%, 95% CI [− 5.05, − 0.17], p = 0.04, I2 = 78%, low certainty of evidence). In the sensitivity analysis, the study by Yoneda et al.41 was excluded owing to its control group being given pioglitazone, which is a medication shown to have some evidence in the treatment of NAFLD. On the other hand, the other trials consisted of placebo or standard of treatment groups. Results showed a consistent finding in the difference in means in the liver proton density fat fraction between SGLT-2 inhibitors and control with note of a decrease in heterogeneity (MD: − 3.65%, 95% CI [− 5.55, − 1.75], p = 0.0002, I2 = 59%, low certainty of evidence) (see Fig. 4b).
(a) Forest plot of comparison: summary of mean difference in liver proton density fat fraction (PDFF) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Harrison 2022 study—standard deviation derived from standard error calculated by Revman. **Ericksson 2018 and Harrison 2022 study measured as change-from-baseline scores. (b) Forest plot of comparison [Sensitivity analysis, Yoneda 2021 excluded]: summary of mean difference in liver proton density fat fraction (PDFF) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Harrison 2022 study—standard deviation derived from standard error calculated by Revman. **Ericksson 2018 and Harrison 2022 study measured as change-from-baseline score.
Effect on hepatic fibrosis
Liver stiffness measurement (LSM)
Analysis on the effect of SGLT-2 inhibitors versus control on the decrease in liver stiffness measurement (LSM) using meta-analysis is provided in Fig. 5a. Across seven randomized controlled trials (RCTs)24,26,31,36,37,39,41, a total of 227 patients in the SGLT-2 group, and 220 patients in the control group were included. Only one trial37 excluded Type 2 diabetes mellitus in the non-alcoholic fatty liver disease population. All trials measured LSM using transient liver elastography or FibroScan® except for one trial40 which used magnetic resonance elastography (MRE). Two studies24,37 used empagliflozin as the SGLT-2 inhibitor while the other two trials39,41 received tofogliflozin, and the remaining ones had dapagliflozin31,36, or dapagliflozin plus liraglutide as intervention26. The control groups were given other standard Type 2 diabetes mellitus treatments excluding SGLT-2 inhibitor, or placebo with moderate intensity physical activity and standard dietary advice only37. Results showed that the SGLT-2 inhibitors slightly decrease the LSM level by mean difference (− 0.67 kPa, 95% CI [− 1.19, − 0.16], p = 0.010, I2 = 69%, low certainty of evidence) compared to comparators. After performing a sensitivity analysis for which the study by Taheri et al.37 was excluded due to its non-inclusion of Type 2 diabetes mellitus population, a trend was observed towards a moderate reduction in the LSM level with further decrease in heterogeneity (MD: − 0.87 kPa, 95% CI [− 1.30, − 0.44], p < 0.0001, I2 = 37%, low certainty of evidence) (see Fig. 5b).
(a) Forest plot of comparison: summary of mean difference in liver stiffness measurement (LSM) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Takeshita 2022 measured as change-from-baseline scores. (b) Forest plot of comparison [Sensitivity analysis, Taheri 2020 excluded]: summary of mean difference in liver stiffness measurement (LSM) post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Takeshita 2022 measured as change-from-baseline scores.
Fibrosis-4 index (FIB-4)
The FIB-4 index is a simple and valuable non-invasive tool in estimating the risk of liver fibrosis. The compiled studies calculated it using the following formula: FIB-4 index = (Age [years] × AST [U/L])/(platelet [109/L] × ALT [U/L]). The mean baseline FIB-4 index across 10 studies24,25,27,28,29,37,39,40,41 ranges from 0.775 to 1.50 in SGLT-2 group, and 0.826–2.12 in the control group. Almost all studies have some concern for bias except for one study24 with low risk of bias. The pooled estimate demonstrated that SGLT-2 inhibitor treatment significantly decreased the FIB-4 index as compared to control (MD: − 0.12, 95% CI [− 0.21, − 0.04], p = 0.005, I2 = 16%, moderate certainty of evidence) (see Fig. 6).
Forest plot of comparison: summary of mean difference in FIB-4 index post-treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. *Takeshita 2022 median and interquartile range study data converted to mean and SD using R-package ‘estmeansd 0.2.1’.**Harrison 2022 with imputed standard deviation.
Effect on histopathology (steatosis, hepatocellular ballooning, lobular inflammation, liver fibrosis)
Only two trials39,40 histologically evaluated all biopsied specimens at baseline and post-treatment at 48 and 72 weeks respectively with a combined total of 41 patients in the SGLT-2 group and 45 patients in the control group. The biopsied liver tissues were scored for hepatic steatosis, hepatocellular ballooning, and lobular inflammation using the NAFLD activity score (NAS)42 while the liver fibrosis was classified according to Brunt et al.43 criteria. The pathological outcomes for each category were summarized separately in Fig. 7a–d. In the meta-analysis, the SGLT-2 inhibitor group was noted to have a higher likelihood of having at least a one-score or one-stage reduction after treatment than the control group with respect to hepatocellular ballooning (RR: 2.19, 95% CI [1.22, 3.94], p = 0.009, I2 = 0%, moderate certainty of evidence) and liver fibrosis (RR: 2.29, 95% CI [1.12, 4.68], p = 0.02, I2 = 33%, moderate certainty of evidence). There were no significant differences identified between the two groups with respect to the changes in steatosis or lobular inflammation.
(a) Forest plot of comparison: summary of one-score or one-stage reduction in hepatic steatosis after treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. (b) Forest plot of comparison: summary of one-score or one-stage reduction in hepatocellular ballooning after treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. (c) Forest plot of comparison: summary of one-score or one-stage reduction in lobular inflammation after treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control. (d) Forest plot of comparison: Summary of one-score or one-stage reduction in liver fibrosis after treatment in patients with NAFLD randomized to either SGLT-2 inhibitor or control.
Reporting biases in syntheses
The funnel plot for Fig. 8 shows no evidence for publication bias. Egger’s test for a regression intercept gave a p-value of 0.129, while Begg and Mazumdar’s test for rank correlation gave a p-value of 0.655, indicating no publication bias.
All outcomes were found to be stated in their respective protocols and reported in the final publication reports. Hence, no selective outcome reporting was identified.
Certainty of evidence
Using the GRADE approach23, these outcomes, which consist of CAP, FIB-4 index, one-score reduction in hepatic steatosis and fibrosis, were noted to have moderate certainty of evidence. Others were designated as having low certainty of evidence given the inconsistency of results and imprecision which downgraded the evidence level. Other detailed summaries of findings were presented in Table 3, with footnotes explaining judgments.
Discussion
The efficacy of SGLT-2 inhibitors in treating hepatic steatosis and fibrosis utilizing several imaging biomarkers and histopathology in patients with non-alcoholic fatty liver disease was investigated in this systematic review and meta-analysis of sixteen randomized controlled trials.
Consolidating the findings above, this meta-analysis found significant mean differences in CAP, L/S ratio, and MRI-PDFF after treatment, favoring the effect of SGLT-2 inhibitor over that of control especially in NAFLD patients.
These translate to a probable or slight positive effect on hepatic steatosis. In contrast, no significant differences were identified between the two groups with regards to the changes in steatosis or lobular inflammation on biopsy post-treatment. Nonetheless, interpretation of such findings in the latter appears to be inconclusive given the small number of studies.
With regards to hepatic fibrosis, there was a slight reduction in the LSM and FIB-4 index with use of SGLT-2 inhibitors in comparison to controls among non-alcoholic fatty liver patients with Type 2 diabetes mellitus. This was also confirmed histologically with the meta-analysis results showing at least a one-stage reduction in the treatment group with respect to hepatocellular ballooning and liver fibrosis.
Overall, our findings appear to be in line with those of other earlier systematic reviews and meta-analyses studies which also investigated the effects of SGLT-2 medications on NAFLD patients. A systematic review of four RCTs and four observational studies done by Raj et al.44 reported favorable effects of SGLT-2 inhibitors on the level of liver enzymes, liver fat, and fibrosis in patients with NAFLD. Similar positive effects of SGLT-2 inhibitors on liver enzyme and fat levels were also seen in individuals with NAFLD, according to a comprehensive evaluation of seven systematic reviews conducted by Shao et al.45.
A meta-analysis of four randomized trials evaluating liver fat content (LFC) using MRI by Coelho et al.46 (2020) showed a decrease in hepatic steatosis with the use of SGLT-2 inhibitors (MD: − 3.39%, 95% CI [− 6.01, − 0.77], p = 0.01, I2 = 89%). Moreover, a meta-analysis of two trials by Xing et al.47 reported a reduction in MRI-PDFF with the treatment of SGLT-2 inhibitors (MD: − 2.07%, 95% CI [− 3.86, − 0.28], p = 0.02, I2 = 10%). Another meta-analysis of two to four trials done by Song et al.48 revealed concordant findings, showing significant reduction in the level of liver controlled attenuation parameter (CAP) (MD: 0.29, 95% CI [− 26.95 to − 13.64], p < 0.00001, I2 = 0%), MRI-PDFF (MD:1.97, 95% CI [− 3.49 to − 0.45], p = 0.01, I2 = 11%), NAFLD score (MD: 0.55, 95% CI [1.04 to − 0.05], p = 0.03, I2 = 0%), fatty liver index (FLI) (MD: 11.21, 95% CI [− 16.53 to − 5.89], p < 0.0001, I2 = 0%), FIB‐4 index (MD: 0.25, 95% CI [− 0.39 to − 0.11], p = 0.0007, I2 = 10%), and increase in L/S ratio (MD: 0.16, 95% CI [0.10–0.22], p < 0.00001, I2 = 49%) with SGLT-2 inhibitor use.
In contrast, the meta-analysis done by Amjad et al.49 showed no statistically significant difference in fibrosis regression utilizing FIB-4 score (SMD = − 0.12, 95% CI: − 0.41 to 0.1, p = 0.994, I2 = 0%) and hepatic steatosis by using MRI-PDFF (SMD = − 0.31, 95% CI: –0.68 to 0.07, p = 0.502, I2 = 0%) between SGLT-2 inhibitors versus controls. However, it must be noted that this study only analyzed a total of three trials for both outcomes with inclusion of non-NAFLD population in one of the trials.
Despite the relevant findings in this meta-analysis, there were still some limitations in the evidence included in the review. We identified a few eligible studies with small sample sizes and inadequate power, leading to imprecise estimates. Also, most of the included studies had some concerns for risk of bias due to allocation concealment issues, use of per-protocol analysis, or missing results which partially affected the certainty (or confidence) in the body of evidence. Likewise, moderate to substantial statistical heterogeneity (I2 > 50%) was observed in some of the analysis which can be explained partially by variability in the studied participants, interventions and control used, in addition to the duration of treatment. Methodologically, different studies have diverse trial design methods (i.e., 1:1, 1:1:1, 2:1; double-blinded, open-label, and sample size differences) and quality which may reflect also in the heterogeneity measures. In terms of applicability to specific ethnic populations, majority of the studies included were conducted within Asia, with many subjects coming from Japan or China. The limited racial diversity within the study population may hence slightly affect the generalizability of the findings of this study.
Nonetheless, this updated meta-analysis was conducted in a comprehensive manner with an adequate number of databases searched by more than one reviewer to screen and extract data. Authors of the studies included were also contacted for completion and clarification of any missing information. The PRISMA guide & checklist13, and the Risk of bias 2.0 tool20 were likewise followed for transparency and completeness in reporting of the systematic review. Moreover, the certainty of evidence was presented using the GRADE approach23, which may assist physicians in the clinical decision-making process together with the patients.
As to implications for practice and policy, the positive evidence from this meta-analysis considers the use of SGLT-2 inhibitors for the treatment of Type 2 diabetes mellitus with an obese profile in the setting of concomitant non-alcoholic fatty liver disease.
The addition of SGLT-2 inhibitors to the usual management of dietary and lifestyle modifications in Type 2 diabetic patients with NAFLD may potentially prevent disease progression and the various complications that accompany the disease. Until now, there has been no standard clinically approved pharmacologic treatments for NAFLD. However, there is some growing evidence on the efficacy of other anti-diabetic medications including pioglitazone and GLP-1 agonists in its management. Although some studies included in this meta-analysis opted to compare the effects of SGLT-2 inhibitors with standard treatments not known to have any effects on NAFLD, some used pioglitazone50 or liraglutide51 as its control, which may slightly affect the positive magnitude of the results. Nevertheless, as a whole, the results of this meta-analysis remain useful in the clinical setting, thus providing an alternative treatment for those who have contraindications to the use of either pioglitazone or GLP-1 agonists.
Current standards of care in the management of Type 2 diabetes mellitus focus on the goal of cardiorenal risk reduction in high-risk patients on top of achievement and maintenance of glycemic and weight control52. Given the growing prevalence of NAFLD and its complications, it may be warranted to further discuss NAFLD in conversations highlighting the list of potential therapies beyond screening measures.
In the context of implications for future research, more randomized controlled trials are needed with (1) larger sample sizes to improve precision; (2) enrollment of a wider range of ethnic populations; (3) study objectives evaluating superiority or efficacy over placebo or standard of care (not only equivalence trials); and (4) use of intention-to-treat analysis in generating results to address bias due to deviations from intended interventions.
Conclusion
The pooled meta-analysis suggests that sodium-glucose cotransporter 2 inhibitors slightly improve hepatic steatosis and fibrosis as compared to controls in adult patients with non-alcoholic fatty liver disease and Type 2 diabetes mellitus with low to moderate certainty of evidence.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request. The protocol was registered at the International Prospective Register of Systematic Reviews (PROSPERO) with the following ID number: CRD42022306396. All information provided in the protocol remained the same and no additional amendments were created.
References
Younossi, Z. M. et al. Global epidemiology of nonalcoholic fatty liver disease—meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 64, 73–84 (2016).
Ge, X., Zheng, L., Wang, M., Du, Y. & Jiang, J. Prevalence trends in non-alcoholic fatty liver disease at the global, regional and National Levels, 1990–2017: A population-based observational study. BMJ Open 10, 8 (2020).
Younossi, Z. M. et al. The Global Epidemiology of NAFLD and Nash in patients with type 2 diabetes: A systematic review and meta-analysis. J. Hepatol. 71, 793–801 (2019).
Li, X. & Wang, H. Multiple organs involved in the pathogenesis of non-alcoholic fatty liver disease. Cell Biosci. 10, 1 (2020).
Adams, L. A., Anstee, Q. M., Tilg, H. & Targher, G. Non-alcoholic fatty liver disease and its relationship with cardiovascular disease and other extrahepatic diseases. Gut 66, 1138–1153 (2017).
Adams, L. A. et al. The natural history of nonalcoholic fatty liver disease: A population-based Cohort Study. Gastroenterology 129, 113–121 (2005).
Söderberg, C. et al. Decreased survival of subjects with elevated liver function tests during a 28-year follow-up. Hepatology 51, 595–602 (2009).
Jojima, T. et al. Empagliflozin (an SGLT2 inhibitor), alone or in combination with linagliptin (a DPP-4 inhibitor), prevents steatohepatitis in a novel mouse model of non-alcoholic steatohepatitis and diabetes. Diabetol. Metabol. Syndrome 8, 1 (2016).
Komiya, C. et al. Ipragliflozin improves hepatic steatosis in obese mice and liver dysfunction in type 2 diabetic patients irrespective of body weight reduction. PLOS ONE 11, 3 (2016).
Tahara, A. & Takasu, T. SGLT2 inhibitor ipragliflozin alone and combined with pioglitazone prevents progression of nonalcoholic steatohepatitis in a type 2 diabetes rodent model. Physiol. Rep. 7, 22 (2019).
Arai, T. et al. Effect of sodium-glucose cotransporter 2 inhibitor in patients with non-alcoholic fatty liver disease and type 2 diabetes mellitus: A propensity score-matched analysis of real-world data. Therapeut. Adv. Endocrinol. Metabol. 12, 204201882110002 (2021).
Wei, Q., Xu, X., Guo, L., Li, J. & Li, L. Effect of SGLT2 inhibitors on type 2 diabetes mellitus with non-alcoholic fatty liver disease: A meta-analysis of randomized controlled trials. Front. Endocrinol. 12, 256 (2021).
Page, M. J. et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 1456 (2021).
Advanced search results—PUBMED. National Center for Biotechnology Information (2023, accessed 29 Dec 2023). https://pubmed.ncbi.nlm.nih.gov/advanced/.
Search manager: Cochrane Library. Search Manager|Cochrane Library (2023, accessed 29 Dec 2023).https://www.cochranelibrary.com/advanced-search/search-manager.
Embase. (2023, accessed 29 Dec 2023). https://www.embase.com/landing?status=yellow.
American College of Physicians—Advanced Search (2023, accessed 29 Dec 2023). https://www.acpjournals.org/search/advanced.
EPPI-Reviewer4 (V.4.14.2.0) [Computer program]. Evidence for Policy and Practice Information and Co-ordinating Centre. https://eppi.ioe.ac.uk/cms/Default.aspx?tabid=2914 (2022).
Review Manager Web (RevMan Web) [Computer program]. The Cochrane Collaboration. https://revman.cochrane.org (2022).
Sterne, J. A. et al. Rob 2: A revised tool for assessing risk of bias in randomised trials. BMJ 2019, 4898 (2019).
Higgins, J. P. et al. Cochrane Handbook for Systematic Reviews of Interventions (Cochrane Collaboration, 2019).
McGrath, S. et al. Estimating the sample mean and standard deviation from commonly reported quantiles in meta-analysis. Stat. Methods Med. Res. 29, 2520–2537 (2020).
GRADEpro GDT: GRADEpro Guideline Development Tool [Computer program]. Hamilton (ON): McMaster University (developed by Evidence Prime). https://www.gradepro.org (2022).
Chehrehgosha, H. et al. Empagliflozin improves liver steatosis and fibrosis in patients with non-alcoholic fatty liver disease and type 2 diabetes: A randomized, double-blind, placebo-controlled clinical trial. Diabetes Therapy 12, 843–861 (2021).
Cho, K. Y. et al. Favorable effect of sodium–glucose cotransporter 2 inhibitor, dapagliflozin, on non-alcoholic fatty liver disease compared with pioglitazone. J. Diabetes Investig. 12, 1272–1277 (2020).
Chu, Y., Wang, D. & Lyu, Z. Effects of dapagliflozin combine with liraglutide on inflammatory factors, glucolipid metabolism and liver function in patients with type 2 diabetes combined with non-alcoholic fatty liver disease. Evalu. Anal. Drug-Use Hospit. China 9, 1067–1067 (2022).
Elhini, S. H. et al. The impact of an SGLT2 inhibitor versus ursodeoxycholic acid on liver steatosis in diabetic patients. Pharmaceuticals 15, 1516 (2022).
Eriksson, J. W. et al. Effects of dapagliflozin and N-3 carboxylic acids on non-alcoholic fatty liver disease in people with type 2 diabetes: A double-blind randomised placebo-controlled study. Diabetologia 61, 1923–1934 (2018).
Han, E., Lee, Y., Lee, B.-W., Kang, E. S. & Cha, B.-S. Ipragliflozin additively ameliorates non-alcoholic fatty liver disease in patients with type 2 diabetes controlled with metformin and pioglitazone: A 24-week randomized controlled trial. J. Clin. Med. 9, 259 (2020).
Harrison, S. A. et al. Licogliflozin for nonalcoholic steatohepatitis: A randomized, double-blind, placebo-controlled, phase 2A study. Nat. Med. 28, 1432–1438 (2022).
Hu, C. L., Wang, Y. C., Xi, Y. & Yao, X. M. Dapagliflozin therapy curative effect observation on nonalcoholic fatty liver disease in patients with type 2 diabetes mellitus. Indian J. Pharmaceut. Sci. 82, 169 (2020).
Ito, D. et al. Comparison of ipragliflozin and pioglitazone effects on nonalcoholic fatty liver disease in patients with type 2 diabetes: A randomized, 24-week, open-label, active-controlled trial. Diabetes Care 40, 1364–1372 (2017).
Kinoshita, T. et al. Comparison of the effects of three kinds of glucose-lowering drugs on non-alcoholic fatty liver disease in patients with type 2 diabetes: A randomized, open-label, three-ARM, active control study. J. Diabetes Investig. 11, 1612–1622 (2020).
Kuchay, M. S. et al. Effect of empagliflozin on liver fat in patients with type 2 diabetes and nonalcoholic fatty liver disease: A randomized controlled trial (E-LIFT trial). Diabetes Care 41, 1801–1808 (2018).
Shibuya, T. et al. Luseogliflozin improves liver fat deposition compared to metformin in type 2 diabetes patients with non-alcoholic fatty liver disease: A prospective randomized controlled pilot study. Diabetes Obes. Metabol. 20, 438–442 (2017).
Shimizu, M. et al. Evaluation of the effects of Dapagliflozin, a sodium-glucose co-transporter-2 inhibitor, on hepatic steatosis and fibrosis using transient elastography in patients with type 2 diabetes and non-alcoholic fatty liver disease. Diabetes Obes. Metabol. 21, 285–292 (2018).
Taheri, H. et al. Effect of empagliflozin on liver steatosis and fibrosis in patients with non-alcoholic fatty liver disease without diabetes: A randomized, double-blind, placebo-controlled trial. Adv. Therapy 37, 4697–4708 (2020).
Takahashi, H. et al. Ipragliflozin improves the hepatic outcomes of patients with diabetes with NAFLD. Hepatol. Commun. 6, 120–132 (2021).
Takeshita, Y. et al. Comparison of Tofogliflozin and glimepiride effects on nonalcoholic fatty liver disease in participants with type 2 diabetes: A randomized, 48-week, open-label, active-controlled trial. Diabetes Care 45, 2064–2075 (2022).
Tobita, H. et al. Comparison of dapagliflozin and teneligliptin in nonalcoholic fatty liver disease patients without type 2 diabetes mellitus: A prospective randomized study. J. Clin. Biochem. Nutr. 68, 173–180 (2021).
Yoneda, M. et al. Comparing the effects of tofogliflozin and pioglitazone in non-alcoholic fatty liver disease patients with type 2 diabetes mellitus (topind study): A randomized prospective open-label controlled trial. BMJ Open Diabetes Res. Care 9, 1 (2021).
Kleiner, D. E. et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41, 1313–1321 (2005).
Brunt, E. M., Janney, C. G., Di Bisceglie, A. M., Neuschwander-Tetri, B. A. & Bacon, B. R. Nonalcoholic steatohepatitis: A proposal for grading and staging the histological lesions. Am. J. Gastroenterol. 94, 2467–2474 (1999).
Raj, H. et al. SGLT-2 inhibitors in non-alcoholic fatty liver disease patients with type 2 diabetes mellitus: A systematic review. World J. Diabetes 10, 114–132 (2019).
Shao, S.-C., Kuo, L.-T., Chien, R.-N., Hung, M.-J. & Lai, E.C.-C. SGLT2 inhibitors in patients with type 2 diabetes with non-alcoholic fatty liver diseases: An umbrella review of Systematic Reviews. BMJ Open Diabetes Res. Care 8, 2 (2020).
dos Coelho, F. et al. Effects of sodium-glucose co-transporter 2 inhibitors on liver parameters and steatosis: A meta-analysis of randomized clinical trials. Diabetes/Metabol. Res. Rev. 37, 6 (2020).
Xing, B. et al. Effects of sodium–glucose cotransporter 2 inhibitors on non-alcoholic fatty liver disease in patients with type 2 diabetes: A meta-analysis of randomized controlled trials. J. Diabetes Investig. 11, 1238–1247 (2020).
Song, T. et al. Meta-analysis of the effect of sodium–glucose cotransporter 2 inhibitors on hepatic fibrosis in patients with type 2 diabetes mellitus complicated with non-alcoholic fatty liver disease. Hepatol. Res. 51, 641–651 (2021).
Amjad, W. et al. Sodium-glucose cotransporter-2 inhibitors improve liver enzymes in patients with co-existing non-alcoholic fatty liver disease: A systematic review and metanalysis. Gastroenterol. Rev. 17, 288–300 (2022).
Lian, J. & Fu, J. Pioglitazone for NAFLD patients with prediabetes or type 2 diabetes mellitus: A meta-analysis. Front. Endocrinol. 12, 145 (2021).
Patel-Chavez, C., Cusi, K. & Kadiyala, S. The emerging role of glucagon-like peptide-1 receptor agonists for the management of NAFLD. J. Clin. Endocrinol. Metabol. 107, 29–38 (2021).
ElSayed, N. A. et al. pharmacologic approaches to glycemic treatment: Standards of care in diabetes—2023. Diabetes Care 46, 140 (2022).
Funding
None of the authors received any external funding, grants, salaries, benefits, or services from a third party for any piece of submitted work.
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the manuscript. A.M.O.L. conceived and designed the whole study. A.M.O.L., and J.A.T. went through the rigorous data collection process: performed search strategies, screened for titles and abstracts, and full-screened articles, appraised quality of papers, and extracted data of eligible studies. A.M.O.L. was responsible for data synthesis, analysis, and management, respectively. A.M.O.L. wrote the initial protocol, while for the final manuscript and abstract, both A.M.O.L. and J.A.T. were involved. All authors read, edited, proofread, and approved the final paper to be submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ong Lopez, A.M.C., Pajimna, J.A.T. Efficacy of sodium glucose cotransporter 2 inhibitors on hepatic fibrosis and steatosis in non-alcoholic fatty liver disease: an updated systematic review and meta-analysis. Sci Rep 14, 2122 (2024). https://doi.org/10.1038/s41598-024-52603-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-52603-5
- Springer Nature Limited