Abstract
D-cycloserine (DCS) and amantadine (AMA) act as partial NMDA receptor (R) agonist and antagonist, respectively. In the present study, we compared the effects of DCS and AMA on dopamine D2/3R binding in the brain of adult rats in relation to motor behavior. D2/3R binding was determined with small animal SPECT in baseline and after challenge with DCS (20 mg/kg) or AMA (40 mg/kg) with [123I]IBZM as radioligand. Immediately post-challenge, motor/exploratory behavior was assessed for 30 min in an open field. The regional binding potentials (ratios of the specifically bound compartments to the cerebellar reference region) were computed in baseline and post-challenge. DCS increased D2/3R binding in nucleus accumbens, substantia nigra/ventral tegmental area, thalamus, frontal, motor and parietal cortex as well as anterodorsal and posterior hippocampus, whereas AMA decreased D2/3R binding in nucleus accumbens, caudateputamen and thalamus. After DCS, ambulation and head-shoulder motility were decreased, while sitting was increased compared to vehicle and AMA. Moreover, DCS increased rearing relative to AMA. The regional elevations of D2/3R binding after DCS reflect a reduction of available dopamine throughout the mesolimbocortical system. In contrast, the reductions of D2/3R binding after AMA indicate increased dopamine in nucleus accumbens, caudateputamen and thalamus. Findings imply that, after DCS, nigrostriatal and mesolimbic dopamine levels are directly related to motor/exploratory activity, whereas an inverse relationship may be inferred for AMA.
Similar content being viewed by others
Introduction
D-cycloserine (DCS; D-4-amino-isoaxazolidinon) and amantadine (AMA; 1-amino-adamantane) act as N-methyl-D-aspartate (NMDA) receptor (R) agonist and antagonist, respectively. DCS binds with high affinity to the glycineB NMDAR subunit1 (inhibition constant [Ki] = 2.33 ± 0.29 μM2), and has proven beneficial for the treatment of psychiatric conditions, including schizophrenia3, major depressive disorder4, anxiety disorder5,6 and autism7. AMA binds to the phencyclidine NMDAR (Ki = 10 μM8) and to the opiate σ1R (Ki = 20 μM9). It is mainly applied for the treatment of L-DOPA induced dyskinesia and psychiatric symptoms of Parkinson’s disease10, but may also ameliorate major depressive disorder11, traumatic brain injury12, refractory electrical status epilepticus13 and multiple sclerosis fatigue14.
In rats, DCS (3 and 15 mg/kg i.p.15; 12 mg/kg i.p.16; 0.3 or 3 mg/kg i.p.17) had no effect on spontaneous locomotor activity15,16,17 or grooming17. After higher DCS doses (≥65 mg/kg perorally [p.o.]), however, motor activity reportedly was “slightly depresssed”18.
In contrast, AMA (40 or 80 mg/kg i.p.19; 50 or 100 mg/kg s.c.20; 100 mg/kg i.p.21) elevated locomotor activity immediately post-injection with the highest increase after 60 min19. A lower dose (20 mg/kg i.p.) was ineffective, whereas a higher dose (160 mg/kg i.p.) induced a depression of motor behavior19.
In vitro, DCS (10 μM) induced a significant elevation of dopamine (DA) efflux in rat striatal slices22, whereas systemic application of DCS (3 mg/kg i.p.) yielded “a slight but non-significant increase” of striatal DA23. Moreover, systemic DCS (30 mg/kg i.p.18; 300 mg/kg i.p.24) augmented γ-amino butyric acid (GABA) in the whole mouse brain, which was related to a decrease of GABA transaminase (GABA-T) levels. DCS (15 mg/kg i.p.25; 30 or 100 mg/kg i.p.18), furthermore, decreased glutamate (GLU) efflux in the rat amygdala25 and in the mouse whole brain18. Interestingly, however, no effect was produced in the rat frontal cortex (FC; 50 or 100 mg/kg i.p.26).
In rats, systemic AMA (100 mg/kg i.p.) augmented striatal acetylcholine (ACh) and nigral and striatal GABA, starting immediately post-injection21. Increases of striatal DA and serotonin (5-HT) concentrations were detectable, but not significant22. Also Maj et al.19 observed no effect on striatal DA after application of lower AMA doses (10 to 80 mg/kg i.p.). Other scientific groups, however, reported a significant augmentation of striatal DA after systemic AMA (40 mg/kg s.c.27; 46 or 92 mg/kg i.p.28; 100 mg/kg i.p.29), also starting immediately post-injection29. Likewise, intrastriatal infusion of AMA (0.1 mM or 1 mM) elevated the striatal release of both DA and GLU29.
After systemic DCS, so far, no in vivo imaging studies of D2R-like binding have been performed on either humans or rats. After chronic treatment with AMA (200 mg/day for at least 10 days), two in vivo imaging studies of striatal D2R-like binding have been conducted on Parkinsonian patients, using [11C]raclopride as radioligand30,31. Both studies reported a significant elevation of striatal D2R-like binding, implying that, at least in Parkinsonian patients, AMA did not increase synaptic DA to an extent sufficient to effect a detecable competition with the exogenous radioligand. Contrarily, in our previous study on healthy rats32, AMA challenge with 40 mg/kg i.p. reduced D2R-like binding in nucleus accumbens (NAC), caudateputamen (CP) and thalamus (THAL) relative to baseline, while 10 mg/kg diminished D2R-like binding in the anterodorsal HIPP (aHIPP).
In the present investigation, we assessed the effects of systemic DCS (20 mg/kg i.p.) on motor/exploratory behaviors and on D2R-like binding in regions of the rat nigrostriatal and mesolimbic systems, which are related to motor as well as cognitive and emotional functioning (NAC, CP, THAL, substantia nigra/ventral tegmental area [SN/VTA], FC, motor cortex [MC], parietal cortex [PC], aHIPP, posterior HIPP [pHIPP]) using small animal SPECT and MRI. For all of these areas, including those of HIPP and neocortex, autogradiography studies have confirmed the presence of D2R-like binding sites33,34,35. Effects of DCS on D2R-like binding were compared to our previous findings on the NMDAR antagonist AMA32.
Materials and Methods
Animals
Imaging studies of D2R-like binding sites were conducted on 38 adult male Wistar rats (ZETT, Heinrich-Heine University, Düsseldorf, Germany), weighing 397 ± 49 g (mean ± standard deviation [SD]; age: 3–4 months). The animals underwent morphological MRI, SPECT measurements in baseline and after injection of DCS or AMA, and behavioral testing after injection of DCS (20 mg/kg: n = 16) or AMA (40 mg/kg: n = 22). MRI and SPECT measurements in baseline and after pharmacological challenges were performed in randomized order and were separated by at least 3 days. Due to seizures or cardial arrest after the administation of the anaesthetic, 5 rats merely underwent behavioral measurements without subsequent D2R-like imaging. Behavioral data obtained after DCS and AMA were compared to the behavioral data obtained after vehicle (0.9% saline) in 16 further male rats of the same strain, age (3–4 months) and weight (418 ± 63 g). Behavioral data obtained after 40 mg/kg AMA and saline have been previously published32,36.
Rats were kept as previously described (e.g.32). The study was performed in accordance with the German Law on the Protection of Animals and the National Institutes of Health guide for the care and use of laboratory animals (NIH Publications No. 8023, revised 1978). The protocol was approved by the regional authority (Landesamt für Natur, Umwelt und Verbraucherschutz, Nordrhein-Westfalen, Recklinghausen, Germany).
MRI studies
After administration of ketamine hydrochloride (Ketavet®, Pharmacia GmbH, Erlangen, BRD; dose: 50 mg/kg i.p., concentration: 100 mg/ml) and xylazine hydrochloride (Rompun®, Bayer, Leverkusen, BRD; dose: 2.5 mg/kg i.p., concentration: 20 mg/ml), morphological imaging was performed with a dedicated small animal MRI (MRS3000 Pre-clinical MRI, 3.0 T, MR Solutions, Guildford, UK; spatial resolution: 0.25 × 0.25 × 0.69) as previously described32,37. Briefly, high-resolution images were obtained with a 3D fast low angle shot (FLASH) sequence38.
Drug treatment
Rats were administered either DCS (Sigma-Aldrich, Taufkirchen, Germany; molecular weight: 102.09 g/mol; dose: 20 mg/kg i.p., concentration: 20 mg/ml; n = 16), AMA hydrochloride (Sigma-Aldrich, Taufkirchen, Germany; molecular weight: 151.25 g/mol; dose: 40 mg/kg i.p., concentration: 40 mg/ml; n = 22) or vehicle (0.9% saline; B. Braun Melsungen AG, Melsungen, Germany; dose: 1 ml/kg i.p.; n = 16).
In former investigations, the doses of 20 mg/kg DCS39 and 40 mg/kg AMA19 were behaviorally active after systemic administration. Elevations of striatal DA were observed immediately after i.p. injection of DCS23 or AMA29. Therefore, behavioral measurements were started immediately after administration of either compound.
SPECT studies
D2R-like imaging in baseline and after challenge with DCS or AMA was conducted as previously described32,36,37,40. Also the employed small animal SPECT (“TierSPECT”; field of view: 90 mm; sensitivity: 22 for 123I; spatial resolution: 3.4 mm for 123I) employed in the present study was described in detail elsewhere41.
Upon anaesthesia with ketamine hydrochloride (dose: 100 mg/kg i.p., concentration: 100 mg/ml) and xylazine hydrochloride (dose: 5 mg/kg i.p., concentration: 20 mg/ml), [123I]S-3-iodo-N-(1-ethyl-2-pyrrolidinyl) methyl-2-hydroxy-6-methoxy benzamide ([123I]IBZM; GE Healthcare, München, Germany; activity: 27.9 ± 4.4 MBq, concentration: 3.4 × 10−9 g/ml, specific activity: > 74 TBq/mmol at reference time) was injected into the tail vein. This radioligand has a high affinity for binding sites of the D2R-like subtype (D2R: Ki = 1.6 nM, D3R: Ki = 2.2 nM42). Moreover, in investigatons with the “TierSPECT”, we have previously demonstrated its displaceability from the D2/3R binding site by endogenous DA (e.g.36). In both humans43 and rodents43,44, under various anaesthetics including ketamine44, specific binding of [123I]IBZM in the striatum reaches its maximum at about 40 min post-injection and remains stable for up to 2 h. This coincides with the time of maximum striatal DA concentrations after i.p. application of DCS (80 to 160 min post-challenge23) and AMA (60 to 90 min post-challenge29). In order to account for the respective time courses, data acquisition was started 45 min after radioligand administration (75 min post-challenge) and ended 105 min after radioligand application (135 min post-challenge).
Behavioral studies
Immediately after administration of DCS, AMA or saline, motor and exploratory behaviors were assessed in an open field (Phenotyper®, Noldus Information Technology, Wageningen, The Netherlands; dimensions: 45 × 45 × 56 cm) with EthoVision XT (Noldus Information Technology, Wageningen, The Netherlands) as previously described32,36,37,40. Durations (s) and frequencies (n) of ambulation, sitting (as a measure of “passive immobility”45), rearing, head-shoulder motility and grooming were rated in blocks of 5 min for a total of 30 min. Subsequent to behavioral tests, rats were anaesthetized as described above and injected [123I]IBZM.
Evaluation of SPECT imaging studies
D2/3R imaging data were evaluated with PMOD (version 3.5, PMOD Technologies Ltd., Zürich, Switzerland) as previously described32,37. Briefly, for each rat, SPECT and MR images were coregistered. Then, the MR image of each rat was coregistered with the Paxinos standard rat brain MRI46 provided by PMOD. The necessary mathematical transformations were used to re-import the SPECT image previously coregistered with the MRI. On the individual overlays of each rat brain SPECT with the Paxinos standard rat brain MRI volumes of interest (VOIs) were defined, as previously described32,37. Thereby, the maximum VOI diameters were either in the range of or beyond the spatial resolution of the employed small animal SPECT. Regional BPs were estimated according to the simplified reference tissue model47 by computing ratios of radioactivity counts obtained in the specifically-bound compartments (NAC, CP, THAL, SN/VTA, FC, MC, PC, aHIPP and pHIPP) to radioactivity counts in the cerebellar reference VOI.
Statistical analysis
D2/3R imaging studies
Distributions of both regional BPs and behavioral data were tested for normality with the non-parametric Kolmogorov-Smirnov test (α ≤ 0.05). Regional BPs were neither uniformly distributed in baseline, nor after DCS or AMA (0.002 ≤ p ≤ 0.200).
Medians and interquartile ranges (25-/75- and 5-/95-percentiles) of regional BPs were computed for both compounds. Moreover, percentual differences of BPs after DCS or AMA relative to baseline were calculated. Regional BPs were compared between baseline and challenge (20 mg/kg DCS or 40 mg/kg mg/kg AMA) with the non-parametric Wilcoxon signed rank test for paired samples (two-tailed, α ≤ 0.05).
Behavioral studies
Behavioral variables (duration and frequencies of ambulation, sitting, rearing, head-and-shoulder motility and grooming) were evaluated with two-way analyses of variance (ANOVAs) with the factors “time” (denoting the individual 5-min time bins) and “treatment” (denoting challenge with either 20 mg/kg DCS, 40 mg/kg AMA or saline). In the majority of comparisons over time bins and treatments, the Shapiro-Wilk normality test failed (p < 0.050). Post hoc pairwise comparisons between treatment groups were performed for each variable in the individual time bins with the Holm-Sidak test (overall α ≤ 0.05). Furthermore, Spearman rank correlation coefficients (r; α ≤ 0.05) were calculated for regional radioligand binding and behavioral parameters in the individual time frames (min 1–5, 6–10, 11–15, 16–20, 21–25 and 26–30).
Statistical analysis was performed with IBM SPSS Statistics 23 (IBM SPSS Software Germany, Ehningen, Germany). and SigmaStat (version 3.5, Systat Software Inc., Erkrath, Germany).
Results
D2/3R binding
Figures 1 and 2 show images of the Paxinos standard rat brain MRI atlas46 at different positions from Bregma together with the standard VOI templates provided by PMOD (left columns). The next columns show characteristic images of regional [123I]IBZM accumulations on coronal slices in baseline (middle) and after challenge (right) with 20 mg/kg DCS (Fig. 1) and 40 mg/kg AMA (Fig. 2), respectively, at the positions from Bregma depicted in the left columns48. Baseline and post-challenge scans after both treatments stem from the same rat.
Paxinos standard rat brain MRI and individual D2/3R SPECT in baseline and after challenge with the NMDAR agonist D-cycloserine (20 mg/kg i.p.) with [123I]IBZM as radioligand. Left columns: Paxinos standard rat brain MR images (Schiffer et al., 2006) at different positions from Bregma together with the standard VOI templates provided by PMOD. Middle columns: Series of coronal SPECT slices in a characteristic rat in baseline at the same positions from Bregma. Right columns: SPECT slices in the same rat after 20 mg/kg D-cycloserine at the same positions from Bregma. The increases of [123I]IBZM accumulation in nucleus accumbens (NAC), substantia nigra/ventral tegmental area (SN), thalamus (THAL), frontal cortex (FC), motor cortex (MC), parietal cortex (PC), anterodorsal hippocampus (aHIPP) and posterior hippocampus (pHIPP) are marked by white arrows. The presented rat also shows an increase of [123I]IBZM accumulation in the caudateputamen (CP) compared to baseline, which was not corroborated by the within-group comparison of D2/3R binding in baseline and post-challenge. SPECT images show binding potentials (BP). It is understood, that the calculation of BPs is only valid for regions with specific radioligand binding. Image algebra was performed with PMOD (version 3.5, PMOD Technologies Ltd., Zürich, Switzerland).
Paxinos standard rat brain MRI and individual D2/3R SPECT in baseline and after challenge with the NMDAR antagonist amantadine (40 mg/kg i.p.) with [123I]IBZM as radioligand. Left columns: Paxinos standard rat brain MR images (Schiffer et al., 2006) at different positions from Bregma together with the standard VOI templates provided by PMOD. Middle columns: Series of coronal SPECT slices in a characteristic rat in baseline at the same positions from Bregma. Right columns: SPECT slices in the same rat after 40 mg/kg amantadine at the same positions from Bregma. The reduction of [123I]IBZM accumulation in nucleus accumbens (NAC), caudateputamen (CP) and thalamus (THAL) are marked by white arrows. SPECT images show binding potentials (BP). It is understood, that the calculation of BPs is only valid for regions with specific radioligand binding. Image algebra was performed with PMOD (version 3.5, PMOD Technologies Ltd., Zürich, Switzerland). Further abbreviations (in alphabetical order): aHIPP), frontal cortex (FC), motor cortex (MC), parietal cortex (PC), posterior hippocampus (pHIPP), substantia nigra/ventral tegmental area (SN).
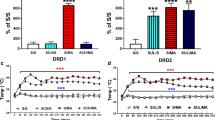
After 20 mg/kg DCS (Fig. 3), BPs were significantly augmented in NAC (+22%, p = 0.028), SN/VTA (+24%, p = 0.011), THAL (+10%, p = 0.046), FC (+19%, p = 0.033), MC (+41%, p = 0.007), PC (+25%, p = 0.016), aHIPP (+25%, p = 0.028) and pHIPP (+16%, p = 0.039) relative to baseline. No significant alteration was observed in the CP (p = 0.133).
Binding potentials in baseline (white) and after challenge with 20 mg/kg D-cycloserine (red). Rendered are medians and 25-/75- (boxes) and 9-/95-quartiles (whiskers). The circles represent the individual animals. For the paired comparisons, the respective p values are given (Wilcoxon signed rank test for paired samples, two-tailed, α = 0.05). Abbreviations (in alphabetical order): aHIPP, anterodorsal hippocampus; FC, frontal cortex; MC, motor cortex; PC, parietal cortex; pHIPP, posterior hippocampus; SN/VTA, substantia nigra/ventral tegmental area.
In contrast, the NMDAR antagonistic AMA (Fig. 4) induced significant reductions of the BP in NAC (−5%, p = 0.008), CP (−7%, p = 0.049) and THAL (−12%, p = 0.020) compared to baseline. No differences between 40 mg/kg AMA and baseline were observed in SN/VTA, FC, MC, PC, aHIPP and pHIPP (0.109 ≤ p ≤ 0.438).
Binding potentials in baseline (white) and after challenge with 40 mg/kg amantadine (blue). Rendered are medians and 25-/75- (boxes) and 9-/95-quartiles (whiskers). The circles represent the individual animals. For the paired comparisons, the respective p values are given (Wilcoxon signed rank test for paired samples, two-tailed, α = 0.05). Abbreviations (in alphabetical order): aHIPP, anterodorsal hippocampus; CP, caudateputamen; FC, frontal cortex; MC, motor cortex; NAC, nucleus accumbens; PC, parietal cortex; pHIPP, posterior hippocampus; SN/VTA, substantia nigra/ventral tegmental area; THAL, thalamus.
Motor and exploratory behaviors
For ambulation duration, the two-way ANOVAs yielded significant effects of “treatment” (p < 0.001), “time” (p < 0.001) and “treatment x time” (p = 0.005), whereas, for ambulation frequency, only effects of “time” (p < 0.001) and “treatment x time” (p = 0.001) were found. Both sitting duration and frequency yielded significant effects of “treatment” (p < 0.001, each), “time” (p < 0.001, each) and “treatment x time” (p < 0.001 and p = 0.014, respectively). This also held for rearing duration and frequency (“treatment”: p < 0.001, each; “time”: p < 0.001, each; “treatment x time”: p < 0.001, each), and for both duration and frequency of head-shoulder motility (“treatment”: p < 0.001, each; “time”: p = 0.041 and p < 0.001, respectively; “treatment x time”: p < 0.001, each). The analysis of grooming duration yielded significant effects of “treatment” (p < 0.001) and “time” (p < 0.001), whereas, for grooming frequency, significant effects of “time” (p = 0.002) and “treatment x time” (p = 0.013) were obtained.
After DCS, ambulation duration (min 1–5, 11–15 and 21–25; Fig. 5), rearing duration (min 11–15 and 21–25; Fig. 6), both duration (min 11–30) and frequency (min 1–5 and 11–25) of head-shoulder motility (Fig. 7) and grooming frequency (min 26–30; Fig. 8) were decreased compared to saline, while sitting duration (min 21–39; Fig. 9) and both rearing duration and frequency in min 1–5 (Fig. 6) were augmented.
Ambulation. Duration (s) and frequency (n) after vehicle (0.9% saline; white), 10 mg/10 D-cycloserine (red) and 40 mg/kg amantadine (blue). The figure shows box and whisker plots of median ambulation durations (A) and frequencies (B) in the individual 5-min time bins. 25-/75-percentiles are given in the boxes, while 5-/95-percentiles are represented by the whiskers. The circles represent the individual animals. The medians in each time bin are connected by black (saline), red (D-cycloserine) and blue lines (amantadine). Between-group differences were assessed using the Holm-Sidak test (two-tailed). Significant p values are given.
Rearing. Duration (s) and Frequency (n) after vehicle (0.9% saline, white), 10 mg/10 D-cycloserine (red) and 40 mg/kg amantadine (blue). The figure shows box and whisker plots of median rearing durations (A) and frequencies (B) in the individual 5-min time bins. 25-/75-percentiles are given in the boxes, while 5-/95-percentiles are represented by the whiskers. The circles represent the individual animals. The medians in each time bin are connected by black (saline), red (D-cycloserine) and blue lines (amantadine). Between-group differences were assessed using the Holm-Sidak test (two-tailed). Significant p values are given.
Head-shoulder motility. Duration (s) and Frequency (n) after vehicle (0.9% saline, white), 10 mg/10 D-cycloserine (red) and 40 mg/kg amantadine (blue). The figure shows box and whisker plots of the median durations (A) and frequencies (B) of head-shoulder motility during in the individual 5-min time bins. 25-/75-percentiles are given in the boxes, while 5-/95-percentiles are represented by the whiskers. The circles represent the individual animals. The medians in each time bin are connected by black (saline), red (D-cycloserine) and blue lines (amantadine). Between-group differences were assessed using the Holm-Sidak test (two-tailed). Significant p values are given.
Grooming. Duration (s) and Frequency (n) after vehicle (0.9% saline, white), 10 mg/10 D-cycloserine (red) and 40 mg/kg amantadine (blue). The figure shows box and whisker plots of the median durations (A) and frequencies (B) of grooming in the individual 5-min time bins. 25-/75-percentiles are given in the boxes, while 5-/95-percentiles are represented by the whiskers. The circles represent the individual animals. The medians in each time bin are connected by black (saline), red (D-cycloserine) and blue lines (amantadine). Between-group differences were assessed using the Holm-Sidak test (two-tailed). Significant p values are given.
Sitting. Duration (s) and frequency (n) after vehicle (0.9% saline; white), 10 mg/10 D-cycloserine (red) and 40 mg/kg amantadine (blue). The figure shows box and whisker plots of median sitting durations (A) and frequencies (B) in the individual 5-min time bins. 25-/75-percentiles are given in the boxes, while 5-/95-percentiles are represented by the whiskers. The circles represent the individual animals. The medians in each time bin are connected by black (saline), red (D-cycloserine) and blue lines (amantadine). Between-group differences were assessed using the Holm-Sidak test (two-tailed). Significant p values are given.
Correlation analysis revealed the following associations between behavioral parameters and regional D2/3R after 20 mg/kg DCS: lower sitting duration in min 1–5 ↔ higher D2/3R in MC (r = −0.517); lower sitting frequency in min 16–20 ↔ lower D2/3R in CP (r = 0.525), FC (r = 0.673) and MC (r = 0.567); lower rearing frequency in min 6–10 ↔ higher D2/3R in SN/VTA (r = −0.581); lower frequency of head-shoulder motility in min 1–5 ↔ higher D2/3R in NAC (r = −0.624), CP (r = −0.687), THAL (r = −0.536), SN/VTA (r = −0.551), FC (−0.504) and pHIPP (−0.608); lower grooming duration in min 6–10 ↔ lower D2/3R in MC (r = 0.590); lower grooming duration in min 26–30 ↔ higher D2/3R in NAC (r = −0.517) and lower grooming frequency in min 1–5 and 11–15 ↔ lower D2/3R in PC (r = 0.560) and pHIPP (r = 0.532), respectively.
After AMA, sitting frequency was increased from min 1–15, while sitting duration was decreased from min 21–30 (Fig. 9). Furthermore, duration and frequency (min 26–30, each; Fig. 7) of head-shoulder motility were elevated relative to saline, whereas ambulation duration (min 1–5 and 11–15; Fig. 5) and both rearing duration and frequency (min 1–15, each; Fig. 6) were reduced.
After 40 mg/kg AMA, the following associations between behavior and D2/3R were obtained: lower ambulation duration in min 1–5 and 11–15 ↔ lower D2/3R in SN/VTA (r = 0.561) and pHIPP (r = 0.603), respectively; lower ambulation frequency in min 1–5 ↔ lower D2/3R in NAC (r = 0.596), CP (r = 0.513), THAL (r = 0.498) and SN/VTA (r = 464); lower sitting duration in min 1–5 and 26–30 ↔ higher D2/3R in SN/VTA (r = −0.504) and pHIPP (r = −0.468), respectively; lower sitting frequency in min 6–10 ↔ higher D2/3R in NAC (r = 0.−606) and CP (r = −0.464); lower rearing duration in min 1–5 ↔ lower D2/3R in NAC (r = 0.521); lower rearing duration in min 21–25 ↔ higher D2/3R in THAL (r = −0.525); lower rearing frequency in min 21–25 ↔ higher D2/3R in THAL (r = −0.490); lower frequency of head-shoulder motility in min 1–5 and 11–15 ↔ lower D2/3R in NAC (r = 0.502), CP (r = 0.509), THAL (r = 0.598) and pHIPP (r = 0.604), respectively; lower grooming frequency in min 1–5, 6–10 and 11–15 ↔ lower D2/3R in NAC (r = 0.475 and 0.500), CP (r = 0.569) and PC (r = 0.550), respectively.
Comparison between NMDAR agonistic and antagonistic treatment yielded reduced ambulation duration (min 16–30; Fig. 5), sitting frequency (min 1–20; Fig. 9), duration of head-shoulder motilty (min 11–30; Fig. 7) and grooming frequency (min 21–30; Fig. 8) after DCS relative to AMA, while sitting duration was increased (min 16–30; Fig. 9). Moreover, after DCS, ambulation frequency was initially (min 1–5; Fig. 5) augmented compared to AMA, but declined in min 21–25. Similarly, the frequency of head-shoulder motility was initially (min 1–5; Fig. 7) elevated, but reduced from min 16–30.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. This article does not contain any studies with human participants performed by any of the authors.
Discussion
Challenge with the NMDAR agonist DCS in a dose of 20 mg/kg significantly increased D2/3R binding in NAC (+22%), SN/VTA (+24%), THAL (+10%), FC (+19%), MC (+41%), PC (+25%), aHIPP (+25%) and pHIPP (+16%), whereas challenge with the NMDAR antagonist AMA in a dose of 40 mg/kg reduced D2/3R binding in NAC (−5%), CP (−7%) and THAL (−12%).
In precedent studies on rats, systemic treatment with the DA precursor L-DOPA36, the DA reuptake inhibitor methylphenidate49, and the GABAAR agonist muscimol37,40 diminished [123]IBZM binding to the rat D2/3R. The augmentation of DA concentrations in the synaptic cleft is common to all of these compounds. Since [123]IBZM competes with endogenous DA molecules for D2/3R binding sites, the observed decreases of D2/3R binding may be conceived to reflect increased levels of synaptic DA50. Therefore, it may be surmised that, also in the present study, the AMA-induced regional reductions of D2/3R binding were due to elevated DA concentrations in these areas, whereas the observed regional increases of D2/3R binding after pre-treatment with DCS indicate reductions of available DA.
This is the first study, which assessed the effects of DCS on subcortical and neocortical DA in rats with a non-invasive in vivo imaging approach. Until now, the effect of DCS challenge on DA has only been studied in the rat CP, where either no effect23 or a significant elevation of DA efflux22 was observed. The latter is in contrast with our findings, which did not show an alteration of D2/3R binding in the CP after 20 mg/kg DCS. Likely reasons for this inconsistency are the differences in methods: firstly, we performed in vivo SPECT, while Bennett and Gronier22 assessed striatal homogenates with high pressure liquid chromatography; secondly, we administered DCS systemically, while Bennett and Gronier22 incubated striatal slices; and, thirdly, we used adult rats with a mean weight of 397 ± 49 g, while Bennett and Gronier22 employed adolesent animals, weighing between 250 and 350 g.
Also the effect of AMA on DA has only been studied in the rat CP. As detailed before32, our finding of elevated DA in the CP following administration of AMA is consistent with the results of Scatton et al.27, Quack et al.28 and Takahashi et al.29 also obtained after systemic AMA (40 and 100 mg/kg). It disagrees, however, with the findings of Maj et al.19 and Bak et al.21, who failed to detect alterations of striatal DA after 10 to 100 mg/kg. In all of these studies, either immature (110–150 g19) or adolescent (250–300 g21,27,28,29 rats were used, precluding age as relevant factor for the discrepancy of outcomes. All of these studies employed either invasive in vivo methods such as microdialysis28,29 or ex vivo methods such as spectrofluorometry19,21 and ion exchange chromatography of striatal preparations27. Scatton et al.27, however, sacrificed their rats 2 h post-challenge, whereas in the studies of Bak et al.21 and Maj et al.19 animals were killed only 1 h after systemic AMA. This indicates that a time of 1 h post-challenge may not be sufficient to induce detectable changes in neostriatal DA levels, at least if AMA action in living compartments is excluded by the chosen ex vivo approach.
Effects of the NMDAR agonistic DCS and the NMDAR antagonistic AMA on motor/exploratory parameters can be summarized as follows: (1) ambulation duration was decreased after both DCS (min 1–5, 11–15 and 21–25 and AMA (min 1–5 and 11–15), while ambulation frequency was unaltered after both treatments; (2) sitting duration was increased after DCS (min 21–30), but decreased after AMA (min 21–30), while sitting frequency was unaltered after DCS, but increased after AMA (min 1–15); (3) both rearing duration and frequency were initially increased after DCS (min 1–5, each) but decreased after AMA (min 1–15, each); (4) both duration (min 11–30) and frequency of head-shoulder motility (min 1–5 and 16–25) were decreased after DCS, but increased after AMA (min 16–30, each); and, finally, (5) grooming duration was unaltered after DCS and AMA, while grooming frequency was decreased after DCS (min 26–30) and unaltered after AMA. Moreover, comparisons between DCS and AMA revealed (1) decreased ambulation duration (min 16–30); (2) increased sitting duration (min 16–30), but decreased sitting frequency (min 1–20); (3) increased rearing duration and frequency (min 1–10, both); (4) decreased duration (min 11–30) and frequency of head-shoulder motility (min 16–30) and, finally, (5) decreased grooming frequency (min 21–30) after DCS relative to AMA. Thereby, interestingly, the frequencies of both ambulation and head-shoulder motility were elevated during the first 5 min post-injection relative to AMA.
The present result of significantly decreased ambulation after challenge with DCS compared to saline contradicts previous studies, which reported either no effect or merely a slight depression of spontaneous locomotor activity after systemic treatment with 0.3 to 65 mg/kg DCS15,16,17,18. Also the finding of decreased ambulation after challenge with AMA does not agree with previous fndings, showing an elevation of locomotor activity after systemic treatment with 40 to 100 mg/kg AMA19,20,21. Only the present finding of unaffected grooming duration confirms previous results obtained after 0.3 and 3 mg/kg DCS17.
Pharmacological effects on motor function in rodents are strongly dependent on age: the DA precursor L-DOPA, for instance, increased motor activity in neonatal (5 to 8 days old51) and immature rats (18 to 20 days old52) after doses of 12.5 to 50 mg/kg and 150 mg/kg, respectively, whereas motor activity was diminished in adult animals (25 to 30 days of age52). In the present study, rats were considerably older (approximately 4 months old and weighing 397 ± 49 g) compared to the other investigations on DCS and AMA, in which adolescent (250–300 g15; 250 ± 50 g16; 200–250 g17; 200 g18; 110–115 g19; 100–120 g20; average weight of 250 g21) animals were used. As a consequence, the present discrepancies may be accounted for by the difference of ages between samples in conjunction with NMDAR agonistic and antagonistic action on synaptic DA levels. The effects of DCS and AMA on both regional D2/3R binding and motor/exploratory parameters must be assessed in future investigations in rats of different ages in order to shed further light on this matter.
It is not surprising that the NMDAR agonist DCS and the NMDAR antagonist AMA exert opposite actions on D2/3R binding. Striking, however, are the differences in regional contributions: while AMA affects merely NAC, CP and THAL, DCS acts on the site of origin of DA fibers (SN/VTA) as well as on target regions of DAergic projections throughout the mesolimbic and nigrostriatal system (NAC, THAL, neocortex, HIPP) with the exception of the CP.
In rodents, DCS increased GABA efflux in the mouse whole brain18,24. Moreover, decreases of GLU levels were observed in the rat amygdala25 as well as in the mouse whole brain18, whereas no effect was detected in the rat FC26. This implies that overall alterations of GABAergic and GLUergic input to the nigrostriatal and mesolimbic target regions of ascending and descending fibers incurred a net decline of DA, reflected by the observed increases of D2R binding in NAC, SN/VTA, THAL, neocortex and HIPP.
As far as can be inferred from precedent investigations, the major difference between DCS and AMA action on cortical and subcortical DA levels is that GLU appears to be either unaffected or decreased by the former18,25,26 but increased by the latter29. As previously outlined in more detail32, it may be assumed that AMA (contrarily to DCS) increases GLUergic input to the target regions of corticostriatal and corticomesolimbic projections, thus augmenting DA efflux in CP, NAC and THAL. It may be hypothesized that these differences in GLUergic and DAergic activation are related to the observed behavioral differences, namely decreased rearing duration and frequency (min 1–10, each) and increased sitting frequency (min 1–20) after AMA compared to DCS. Moreover, also in the second half of the testing time, after AMA, exploration was primarily performed by the sitting animal merely moving its head and shoulders (min 11–30).
In the direct pathway (CP - pars reticulata of the SN/internal globus pallidus) DA disinhibits GABAergic neurons, incurring an activiation of the mesencephalic, diencephalic and brainstem motor centers, whereas, in the indirect pathway (CP - external globus pallidus/subthalamic nucleus - pars recticulata of the SN/internal globus pallidus), GABAergic neurons are inhibited by DA, resulting in a suppression of motor activity53. Moreover, the NAC with its afferents to the limbic system and its efferents to the GP acts as a limbic-motor interface, which is pivotal for the translation of emotional and motivational states into action54. Correlation analysis revealed that, after DCS, high sitting frequency (at 15 min post-challenge) predicted high D2/3R binding (and low DA) in CP, FC and MC (at 75 min post-challenge). Moreover, a low frequency of head-shoulder motility (immediately post-challenge) predicted high D2/3R binding (and low DA) in NAC, CP, THAL, SN/VTA, FC and pHIPP (at 75 min post-challenge). Contrarily, after AMA, a high sitting frequency (at 6 min post-challenge) predicted low D2/3R binding in NAC and CP (at 75 min post-challenge), whereas low durations and/or frequencies of ambulation and head-shoulder motility (immediately post-challenge) predicted low D2/3R binding in NAC, CP, THAL and SN/VTA (at 75 min post-challenge). This infers that after DCS and AMA, the altered levels of DA in the individual regions of the nigrostriatal and mesolimbic pathway within the first 15 min post-injection differentially affected motor neurons in conjunction with emotional/motivational states. Thereby, after DCS, lower regional DA concentrations produced the effect that rats were less able (and/or less “motivated”) to ambulate or explore their environment by head-shoulder movements, but more able (and/or more “motivated”) to exhibit rearing behavior. In contrast, after AMA, higher regional DA levels induced a general behavioral depression characterized by decreased rearing and increased sitting, while, consistently, exploration mainly consisted of head-and-shoulder movements. The question still remains to be solved, however, in as much the regional BPs (and DA levels) at the time of in vivo imaging correspond to the DA levels at the time of data acquisition in the open field. Future investigations are needed, in which behavior are assessed for a longer time than 30 min post-challenge. Moreover, regional D2/3R binding should be determined in different sets of animals at various times after [123I]IBZM application.
In the present study, findings may have been biased by the employment of the NMDAR antagonist ketamine as anaesthetic. Since ketamine has previously been shown to enhance DA release in rats (e.g.55,56,57), it can not be excluded that DA release elicited by ketamine actually reduced the amounts of visible regional D2/3 receptor binding after both DCS and AMA. Effects on neostriatal and/or ventrostriatal DA, however, are exerted by practically all known anaesthetics, including pentobarbital, propofol, halothane, chloral hydrate and isoflurane (for review see58). Therefore, we decided to maintain the usage of ketamine, which was employed in all our previous investigations. Since also this possible pitfall concerns the outcome of SPECT measurements both in baseline and post-challenge, the obtained BPs remain comparable between conditions.
Conclusion
Taken together, in adult rats, DCS increased D2/3R binding in NAC, SN/VTA, THAL, FC, MC, PC, aHIPP and pHIPP, whereas AMA decreased D2/3R binding in NAC, CP and THAL. The elevations of D2/3R binding after DCS reflect a reduction of available DA throughout the nigrostriatal and mesolimbic system, while the reductions of D2/3R binding after AMA indicate an increased availability of DA in NAC, CP and THAL. Findings imply a direct relationship between nigrostriatal and mesolimbic DA levels and motor/exploratory activity after DCS, but an inverse relationship after AMA.
References
Hood, W. F., Compton, R. P. & Monahan, J. P. D-cycloserine: a ligand for the N-mehyl-D-aspartate coupled glycine receptorhas partial agonist characteristics. Neurosci. Lett. 98, 91–95 (1989).
Monahan, J. B., Handelmann, G. E., Hood, W. F. & Cordi, A. A. D-cycloserine, a positive modulator of the N-methyl-D-aspartate receptor, enhances performance of learning tasks in rats. Pharmacol. Biochem. Behav. 34, 649–653 (1989).
Heresco-Levy, U., Javitt, D. C., Ermilov, M., Silipo, G. & Shimoni, J. Double-blind, placebo-controlled, crossover trial of D-cycloserine adjuvant therapy for treatment-resistant schizophrenia. Int. J. Neuropsychopharmacol. 1, 131–135 (1998).
Heresco-Levy, U. et al. A randomized add-on trial of high-dose D-cycloserine for treatment-resistant depression. Int. J. Neuropsychopharmacol. 16, 501–506 (2013).
Davis, M. NMDA receptors and fear extinction: implications for cognitive behavioral therapy. Dialogues Clin. Neurosci. 13, 463–474 (2011).
Tart, C. D. et al. Augmentation of exposure therapy with post-session administration of D-cycloserine. J. Psychiatr Res. 47, 168–174 (2013).
Posey, D. J. et al. A pilot study of D-cycloserine in subjects with autistic disorder. Am. J. Psychiatry. 161, 2115–2117 (2004).
Kornhuber, J., Bormann, J., Hübers, M., Rusche, K. & Riederer, P. Effects of the 1-amino-adamantanes at the MK-801-binding site of the NMDA-receptor-gated ion channel: a human postmortem brain study. Eur. J. Pharmacol. 206, 297–300 (1991).
Kornhuber, J., Schoppmeyer, K. & Riederer, P. Affinity of 1-aminoadamantanes for the sigma binding site in post-mortem human frontal cortex. Neurosci. Lett. 163, 129–131 (1993).
Vanle, B. et al. NMDA antagonists for treating the non-motor symptoms in Parkinson’s disease. Transl. Psychiatry. 8, 117 (2018).
Moryl, E., Danysz, W. & Quack, G. Potential antidepressive properties of amantadine, memantine and bifemelane. Pharmacol. Toxicol. 72, 394–397 (1993).
Spritzer, S. D. et al. Amantadine for patients with severe traumatic brain injury: a critically appraised topic. Neurologist. 19, 61–64 (2015).
Wilson, R. B., Eliyan, Y., Sankar, R. & Hussain, S. A. Amantadine: A new treatment for refractory electrical status epilepticus in sleep. Epilepsy Behav. 84, 74–78 (2018).
Shaygannejad, V., Janghorbani, M., Ashtari, F. & Zakeri, H. Comparison of the effect of aspirin and amantadine for the treatment of fatigue in multiple sclerosis: a randomized, blinded, crossover study. Neuro.l Res. 34, 854–858 (2012).
Herberg, L. J. & Rose, I. C. Effects of D-cycloserineand cycloleucine, ligands of the NMDA-associated strychnine-insensitive glycine site, on brain-stimulation reward and spontaneus locomotion. Pharmacol. Biochem. Behav. 36, 735–738 (1990).
Kretschmer, B. D., Zadow, B., Volz, T. L., Volz, L. & Schmidt, W. J. The contribution of the different binding sites of the N-methyl-D-aspartate (NMDA) receptor to the expression of behavior. J. Neural. Transm. Gen. Sect. 87, 23–35 (1992).
Dall’Olio, R., Rimondini, R. & Gandolfi, O. The NMDA positive modulator D-cycloserine inhibits dopamine-mediated behaviors in the rat. Neuropharmacology. 33, 55–59 (1994).
Polc, P. et al. L-cycloserine: behaviotal and biochemical effects after single and repeated administration to mice, rats and cats. Neuropharmacology 25, 411–418 (1986).
Maj, J., Sowińska, H. & Baran, L. The effect of amantadine on motor activity and catalepsy in rats. Psychopharmacologia. 24, 296–307 (1972).
Buus Lassen, J. The effect of amantadine and (+)-amphetamine on motility in rats after inhibition of monoamine synthesis and storage. Psychopharmacologia (Berl.). 29, 55–64 (1993).
Bak, I. J., Hassler, R., Kim, J. S. & Kataoka, K. Amantadine actions on acetylcholine and GABA in striatum and substantia nigra of rat in relation to behavioral changes. J. Neural Transm. 33, 45–61 (1972).
Bennett, S. & Gronier, B. Modulation of striatal dopamine release in vitro by agonists of the glycineB site of NMDA receptors; interaction with antipsychotics. Eur. J. Pharmacol. 527, 52–59 (2005).
Gandolfi, O., Rimondini, R. & Dall’Olio, R. D-cycloserine decreases both D1 and D2 dopamine receptors number and their function in rat brain. Pharmacol. Biochem. Behav. 48, 351–356 (1994).
Scotto, P., Monaco, P., Scardi, V. & Bonavita, V. Neurochemical studies with L-cycloserine, a central depressant agent. J. Neurochem. 10, 831–839 (1963).
Lehner, M. et al. The effects of midazolam and D-cycloserine on the release of glutamate and GABA in the basolateral amygdala of low and high anxiety rats during extinction trial of a conditioned fear test. Neurobiol. Learn. Mem. 94, 468–480 (2010).
Fujihira, T., Kanematsu, S., Umino, A., Yamamoto, N. & Nishikawa, T. Selective increase in the extracellular D-serine contents by D-cycloserine in the rat medial frontal cortex. Neurochem. Int. 51, 233–236 (2007).
Scatton, B., Cheramy, A., Besson, M. J. & Glowinski, J. Increased synthesis and release of dopamine in the striatum of the rat after amantadine treatment. Eur. J. Pharmacol. 13, 131–133 (1970).
Quack, G., Hesselink, M., Danysz, W. & Spanagel, R. Microdialysis studies with amantadine and memantine on pharmacokinetics and effects on dopamine turnover. J. Neural Transm. Suppl. 46, 97–105 (1995).
Takahashi, T., Yamashita, H., Zhang, Y. X. & Nakamura, S. Inhibitory effect of MK-801 on amantadine-induced dopamine release in the rat striatum. Brain Res. Bull. 41, 363–367 (1996).
Volonté, M. A. et al. A PET study with [11-C]raclopride in Parkinson’s disease: preliminary results on the effect of amantadine on the dopaminergic system. Neurol. Sci. 22, 107–108 (2001).
Moresco, R. M. et al. New perspectives on neurochemical effects of amantadine in the brain of parkinsonian patients: a PET - [(11)C]raclopride study. J Neural Transm. (Vienna). 109, 1265–1274 (2002).
Nikolaus, S., De Souza Silva, M.A., Huston, J. P., Antoch, G. & Müller, H. W. Amantadine enhances nigrostriatal and mesolimbic dopamine function in the rat brain in relation to motor and exploratory activity. Pharmacol. Biochem. Behav. 179, 156–170 (2019).
Bouthenet, M. L., Martres, M. P., Sales, N. & Schwartz, J. C. A detailed mapping of dopamine D-2 receptors in rat central nervous system by autoradiography with [125I]iodosulpride. Neuroscience. 20, 117–155 (1987).
Seeman, P. & Grigoriadis, D. Dopamine receptors in brain and periphery. Neurochem, Int. 10, 1–25 (1987).
Morelli, M., Mennini, T., Cagnotto, A., Toffano, G. & Di Chiara, G. Quantitative autoradiographical analysis of the age-related modulation of central dopamine D1 and D2 receptors. Neuroscience. 36, 403–410 (1990).
Nikolaus, S. et al. Relationship between L-DOPA-induced reduction in motor and exploratory activity and striatal dopamine D2 receptor binding in the rat. Front. Behav. Neurosci. 9, article 352 (2016).
Nikolaus, S. et al. GABAergic control of nigrostriatal and mesolimbic dopamine in the rat brain. Front. Behav. Neurosci. 12, article 38 (2018).
Haase, A., Frahm, J., Matthaei, D., Hänicke, W. & Merboldt, K. D. FLASH imaging. Rapid NMR imaging using low flip-angle pulses. J. Magn. Reson. 67, 258–266 (1986).
Zlomuzica, A., De Souza Silva, M. A., Huston, J. P. & Dere, E. NMDA receptor modulation by D-cycloserine promotes episodic-like memory in mice. Psychopharmacology (Berl). 193, 503–509 (2007).
Nikolaus, S. et al. GABAergic control of neostriatal dopamine D2 receptor binding and behaviors in the rat. Pharmacol. Biochem. Behav. 153, 76–87 (2017).
Schramm, N., Wirrwar, A., Sonnenberg, F. & Halling, H. Compact high resolution detector for small animal SPECT. IEEE Trans. Nucl. Sci. 47, 1163–1166 (2000).
Videbaek, C., Toska, K., Scheideler, M. A., Paulson, O. B. & Moos Knudsen, G. SPECT tracer [(123)I]IBZM has similar affinity to dopamine D2 and D3 receptors. Synapse. 38, 338–342 (2000).
Verhoeff, N. P. L. G. et al. In vitro and in vivo D2-dopamine receptor binding with ((123I)IBZM) in rat and human brain. Int. J. Rad. Appl. Instrum. B. 18, 837–846 (1991).
Jongen, C., de Bruin, K., Beekman, F. & Booij, J. SPECT imaging of D2 dopamine receptors and endogenous dopamine release in mice. Eur. J. Nucl. Med. Mol. Imaging. 35, 1692–1698 (2008).
Müller, C. P. et al. Cocaine-induced ‘active immobility’ and its modulation by the serotonin1A receptor. Behav. Pharmacol. 15, 481–493 (2004).
Schiffer, W. K. et al. Serial microPET measures of the metabolic reaction to a microdialysis probe implant. J. Neurosci. Methods. 155, 272–284 (2006).
Ichise, M., Meyer, J. H. & Yonekura, Y. An introduction to PET and SPECT neuroreceptor quantification models. J. Nucl, Med. 42, 755–763 (2001).
Paxinos, G. & Watson, C. The rat btain in stereotaxix coordinates. 7th edition. (Academic Press, Elesevier, Amsterdam, 2014).
Nikolaus, S. et al. [123I]Iodobenzamide binding to the rat dopamine D2 receptor in competition with haloperidol and endogenous dopamine – an in vivo imaging study with a dedicated small animal SPECT. Eur. J. Nucl. Med. Mol. Imaging. 32, 1305–1310 (2005).
Laruelle, M. Imaging synaptic neurotransmission with in vivo binding competition techniques: a critical review. J. Cereb. Blood Flow Metab. 20, 423–451 (2000).
McDevitt, J. T. & Setler, P. E. Differential effects of dopamine agonists in mature and immature rats. Eur. J. Pharmacol. 72, 69–75 (1981).
Grigoriadis, N., Simeonidou, C., Parashos, S. A., Alban, M. & Guiba-Tziampiri, O. Ontogenetic development of the locomotor response to levodopa in the rat. Pediatr. Neurol. 14, 41–45 (1996).
Grillner, S. & Robertson, B. The basal ganglia downstream control of brainstem motor centres–an evolutionarily conserved strategy. Curr. Opin. Neurobiol. 33, 47–52 (2015).
Mogenson, G. J., Jones, D. L. & Yim, C. Y. From motivation to action: functional interface between the limbic system and the motor system. Prog. Neurobiol. 14, 69–97 (1980).
Onoe, H. et al. Ketamine increases the striatal N-11C-methylspiperone binding in vivo: positron emission tomography study using conscious rhesus monkey. Brain Res. 663, 191–198 (1994).
Tsukada, H. et al. Ketamine decreased striatal [11C]raclopride binding with no alteration in static dopamine concentrations in the striatal extracellular fluid in the monkey brain: Multi-parametric PET studies combined with microdialysis analysis. Synapse. 37, 95–103 (2000).
Ohba, H., Harada, N., Nishiyama, S., Kakiuchi, T. & Tsukada, H. Ketamine/xylazine anesthesia alters [11C]MNPA binding to dopamine D2 receptors and response to methamphetamine challenge in monkey brain. Synapse. 63, 534–537 (2009).
Müller, C. P. et al. The in vivo neurochemistry of the brain during general anesthesia. J. Neurochem. 119, 419–446 (2011).
Acknowledgements
MAdSS was supported by a Heisenberg Fellowship SO 1032/5–1 and EU-FP7 (MC-ITN-“In-SENS”-ESR7 607616). JPH was supported by “Deutsche Forschungsgemeinschaft” (Grant: DFG HU 306/27-3).
Author information
Authors and Affiliations
Contributions
Experimental design: S.N., M.A.D.S.S., J.P.H., G.A. and H.W.M. Performance of imaging and behavioral studies: S.N., H.J.W., A.M.L. and F.W. Evaluation and statistical analysis: S.N. and M.B. Interpreation of findings: S.N., M.B., H.W.M. Writing and editing of the manuscript: S.N., H.J.W., A.M.L., F.W., M.B., C.A., E.M., H.H., J.P.H., G.A., H.W.M.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nikolaus, S., Wittsack, HJ., Wickrath, F. et al. Differential effects of D-cycloserine and amantadine on motor behavior and D2/3 receptor binding in the nigrostriatal and mesolimbic system of the adult rat. Sci Rep 9, 16128 (2019). https://doi.org/10.1038/s41598-019-52185-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-52185-7
- Springer Nature Limited