Abstract
Excessive dietary salt intake can counteract the renoprotective effects of renin–angiotensin system (RAS) blockade in hypertensive patients with chronic kidney disease (CKD). In rodents, salt loading induces hypertension and renal damage by activating the mineralocorticoid receptor (MR) independently of plasma aldosterone levels. Thus, high salt-induced resistance to RAS blockade may be mediated by MR activation. To test this, a post hoc analysis of the Eplerenone Combination Versus Conventional Agents to Lower Blood Pressure on Urinary Antialbuminuric Treatment Effect (EVALUATE) trial was conducted. Thus, 304 non-diabetic hypertensive patients on RAS-blocking therapy were divided into tertiles according to salt intake (estimated 24-h urinary sodium excretion at baseline) and compared in terms of percent reduction in urinary albumin-to-creatinine ratio (UACR) at 52 weeks relative to baseline. The eplerenone-treated patients in the highest sodium excretion tertile exhibited significantly greater reduction in UACR than the placebo subjects in the same tertile (−22.5% vs. +21.8%, p = 0.02). This disparity was not observed in the lowest (−10.2% vs. −0.84%, p = 0.65) or middle (−19.5% vs. +9.5%, p = 0.22) tertiles. Similar systolic blood pressure changes were observed. In the whole cohort, reduction in UACR correlated positively with reduction in systolic blood pressure (r2 = 0.04, p = 0.02). These results support the hypothesis that excessive salt intake can enhance resistance to RAS blockade by activating MR. They also suggest that eplerenone plus RAS blockade may be effective for CKD in hypertensive patients, especially those with excessive salt intake.
Similar content being viewed by others
Introduction
The guideline-recommended treatment for patients with hypertension and chronic kidney disease (CKD) is blockade of the renin–angiotensin system (RAS) by using an angiotensin-converting enzyme inhibitor (ACEi) or an angiotensin-receptor blocker (ARB): this therapy is recommended because it not only has antihypertensive effects, it also has renoprotective effects [1,2,3]. However, albuminuria often persists in hypertensive patients with CKD despite RAS blockade. This is significant because these patients have the same risk of end-stage renal disease (ESRD) as hypertensive patients with CKD who are given placebo [4]. Therefore, hypertensive patients with CKD who exhibit residual albuminuria after RAS blockade require more aggressive treatment.
When combined with RAS blockade, mineralocorticoid receptor (MR) blockade provides additional renoprotective effects [5,6,7,8,9]. The results of the randomized, double-blind, placebo-controlled Eplerenone Combination Versus Conventional Agents to Lower Blood Pressure on Urinary Antialbuminuric Treatment Effect (EVALUATE) trial were recently reported [10]. This trial showed that a relatively low dose of the selective MR-blocker eplerenone significantly and safely reduced urinary albuminuria in non-diabetic hypertensive patients with albuminuria, independent of aldosterone levels [10].
Excessive dietary salt intake is a risk factor for the progression of CKD [11,12,13,14] and is thought to induce resistance to RAS blockade [11, 15, 16]. Several previous reports, including post hoc analyses of randomized controlled trials, showed that this effect of high dietary salt is mediated by suppressing the RAS inhibitor-induced decline in glomerular filtration ratio (GFR) [15, 16] and albuminuria [11]. Significantly, in rodents, dietary salt loading was found to potentiate MR signaling in the kidneys [17, 18]. These findings together suggest that excessive salt intake contributes to resistance to RAS blockade therapy by activating the MR pathway in the kidneys and that MR blockade will effectively suppress residual renal injury [18]. This hypothesis was tested by a post hoc analysis of patients in the EVALUATE trial.
Methods
Study design
A detailed description of the EVALUATE trial (UMIN000001803) has been published [10]. Briefly, this trial enrolled patients, aged 20–79 years, from 59 clinics and hospitals throughout Japan. All patients were hypertensive: systolic blood pressure (SBP) was 130–179 mmHg and/or diastolic blood pressure (DBP) was 80–99 mmHg. All patients had a pre-treatment urinary albumin-to-creatinine ratio (UACR) in the first morning void urine (a mean of three measurements on three consecutive pre-treatment visits) of 30–599 mg/g and an estimated GFR (eGFR) of ≥50 ml/min per 1.73 m2. In addition, all had received an ACEi and/or ARB for at least 8 weeks. The main exclusion criteria included hypertensive emergencies, hyperkalemia, diabetes, severe liver damage, severe heart failure, severe arrhythmia, angina, and myocardial infarction or cerebrovascular disease within 6 months before registration. Patients were randomized to treatment with eplerenone (50 mg/day) or placebo for 52 weeks, and continued to take the antihypertensive treatments they received at baseline. Antihypertensive agents (apart from an MR antagonist, ACEi, or ARB) were added during the study if the blood pressure was ≥130/80 mmHg. Patient follow-up visits occurred 4, 8, 16, 28, 40, and 52 weeks after study-drug initiation. Cuff blood pressure was measured and blood and first morning void urine samples were obtained at every visit. Urinary albumin, sodium, and creatinine concentrations were measured at the central laboratory. All other measurements were obtained in the clinic. Calculations of eGFR were based on the modification in diet in renal disease formula of the Japanese Society of Nephrology [19]. Twenty-four hours urinary sodium excretion (24-h UNa) was calculated from the sodium concentration in the morning void urine by using a previously reported formula [20]. UACR in the first void urine samples was also determined.
The primary outcome of this post hoc study was percent change in UACR at 52 weeks (or, in patients who discontinued, at the last visit) relative to baseline. The secondary outcomes were change in blood pressure, serum potassium, serum creatinine, eGFR, frequency of one or more episodes of severe hyperkalemia (defined as > 5.6 mEq/l) during the 52-week study period.
Statistical analyses
The patients were divided into tertiles based on estimated 24-h UNa at baseline. The eplerenone and placebo groups in each tertile were compared in terms of baseline demographic, clinical, and biochemical variables by using t-test with Welch’s correction, Mann–Whitney test, or Chi-squared test as appropriate. The exception related to the comparison of the two groups in each UNa tertile in terms of the frequency of hyperkalemia; for that, we used the Cochran–Mantel–Haenszel test. The correlation between two variables in a specified patient group was determined by using Pearson Product Moment Correlation Analysis. All analyses were two-sided, and the significance level was set at 0.05. All statistical analyses were performed by using JMP software version 11.2.1 (SAS Institute).
Results
Baseline demographic, clinical, and laboratory variables of the placebo and eplerenone groups in the tertiles
In total, 304 patients whose urinary albumin levels were measured at both baseline and the end of the study were enrolled in the study. These patients were grouped into tertiles according to their baseline estimated 24-h UNa: the cutoffs were at 189 and 235 mEq/day. Within each tertile, the eplerenone and placebo groups had similar baseline demographic, clinical, and biochemical characteristics, including blood pressure, eGFR, plasma renin activity, plasma aldosterone concentrations, and UACR. However, in the lowest tertile, the placebo group had a significantly higher baseline plasma aldosterone–renin ratio (ARR) than the eplerenone group (p = 0.05 after rounding) (Table 1).
Change in UACR relative at 52 weeks to baseline
Although the placebo groups of the tertiles received standard RAS blockade treatment, their percent change in UACR at the end of the trial relative to baseline tended to rise as salt intake increased: the percent change in UACR in the placebo groups of the lowest, middle, and highest tertiles rose from −0.8% to +9.5% to +21.8%, respectively (Fig. 1a, open bars). The opposite trend was observed for the eplerenone groups (Fig. 1a, closed bars). Comparison of eplerenone to placebo in each tertile showed that in the highest tertile, eplerenone associated with a significantly greater reduction in UACR at 52 weeks relative to baseline (−22.5% vs. +21.8%, p = 0.02). Smaller differences between eplerenone and placebo were observed for the middle (−19.5% vs. +9.5%) and lowest (−10.2% vs. −0.84%) tertiles; these differences did not achieve statistical significance (p = 0.22 and 0.65, respectively) (Fig. 1a; Supplementary Figure 1). These data are consistent with correlation analyses of all placebo- and eplerenone-treated patients in the cohort. Thus, the placebo-treated patients exhibited a positive correlation (r2 = 0.02, p = 0.09) between a change in UACR at 52 weeks relative to baseline and baseline 24-h UNa excretion, whereas the eplerenone-treated patients demonstrated a negative correlation (r2 = 0.00, p = 0.62) between these variables (Supplementary Figure 2).
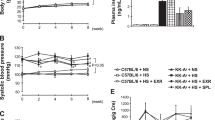
Change in a albumin-to-creatinine ratio (UACR) and b systolic and diastolic blood pressure at the end of the 52-week treatment period relative to baseline in the tertiles of estimated 24-h urinary sodium excretion. The eplerenone group is represented by closed bars and the placebo group by open bars. Error bars represent SDs. L lowest tertile, M middle tertile, H highest tertile, SBP systolic blood pressure, DBP diastolic blood pressure *p < 0.05 vs. placebo group, as determined by t-test with Welch’s correction
Change in blood pressure
Salt had a somewhat similar effect on blood pressure. Thus, as dietary salt levels rose in the tertiles, the ability of RAS blockade to control SBP tended to diminish from −11.0 to −8.9 to −5.3 mmHg. Adding eplerenone significantly augmented the SBP-controlling effect of the RAS blocker in these tertiles from −10.3 to −12.6 to −14.9 mmHg. The same effect was observed for DBP: in the placebo tertiles, DBP dropped from −6.6 to −4.3 to −2.3 mmHg, whereas in the eplerenone groups, DBP steadily improved from −6.3 to −8.1 to −9.2 mmHg. As a result, in the highest UNa tertile, the eplerenone group exhibited significantly greater improvements in SBP relative to baseline than the placebo group (−14.9 ± 3.2 vs. −5.3 ± 3.3 mmHg, p = 0.04). This was also observed for DBP (−9.2 ± 2.2 vs. −2.3 ± 2.3 mmHg, p = 0.03). However, the eplerenone and placebo groups in the middle tertile did not differ significantly in terms of improvement in SBP (−12.6 ± 1.9 vs. 8.9 ± 1.8 mmHg, p = 0.15) or DBP (−8.1 ± 1.4 vs. −4.3 ± 1.4 mmHg, p = 0.05). Similarly, the eplerenone and placebo groups in the lowest tertile did not differ significantly in terms of improvement in SBP (−10.3 ± 1.9 vs. −11.0 ± 2.1 mmHg, p = 0.78) or DBP (−6.3 ± 1.2 vs. −6.6 ± 1.3 mmHg, p = 0.87) (Fig. 1b; Supplementary Figure 3).
Correlation analyses showed that change in UACR and change in SBP did not correlate significantly in either the entire eplerenone group (r2 = 0.02, p = 0.11) or the entire placebo group (r2 = 0.02, p = 0.11). However, when the whole cohort was analyzed, a positive correlation was observed (r2 = 0.04, p = 0.02) (Supplementary Figure 4) [10].
Change in serum potassium
In the lowest tertile, the eplerenone group exhibited significantly greater increases in serum potassium at 52 weeks relative to baseline than the placebo group (0.12 vs. −0.05 mEq/l, p = 0.05). This significant difference was also observed in the middle tertile (0.21 vs. 0.05 mEq/l, p = 0.03). The eplerenone group in the highest tertile also tended to have greater increases in serum potassium (0.19 vs. 0.07 mEq/l) but this did not achieve statistical significance (p = 0.06) (Table 2).
The entire eplerenone group was significantly more likely to develop hyperkalemia (>5 mEq/l) during the study period than the entire placebo group (9.3% vs. 2.6%, p = 0.01). This tendency was also observed in the tertile groups: in the lowest, middle, and highest tertiles, the eplerenone group tended to be more likely to develop hyperkalemia than the placebo group (7.1% vs. 2.0%, p = 0.20; 9.8% vs. 3.8%, p = 0.21; and 10.9% vs. 2.0%, p = 0.05 [this was not significant before rounding], respectively) (Table 3). There were no cases of severe hyperkalemia (≧5.6 mEq/l).
Change in other renal variables
The eplerenone and placebo groups in each tertile did not differ in terms of change in serum creatinine concentrations at week 52 relative to baseline (Table 2). Moreover, while the eplerenone groups in the tertiles tended to have greater eGFR changes than the placebo groups, these differences did not achieve statistical significance (Table 2).
Discussion
This study showed that in non-diabetic hypertensive patients receiving standard RAS blockade therapy only, excessive dietary salt tended to increase albuminuria. This is consistent with previous reports [11, 15, 16]. The crucial observation of this study is that MR blockade in patients with CKD effectively suppressed this salt-induced albuminuria; thus MR blockade overcame salt-induced resistance to standard RAS blockade therapy. This in turn suggests that MR signal activation contributes to high salt-induced resistance to RAS blockade. It is generally thought that dietary salt normally suppresses the plasma level of aldosterone, which is the physiological ligand for MR in the kidney; this maintains blood pressure and fluid homeostasis. However, studies on rodent models show that in pathological conditions, while dietary salt continues to suppress plasma aldosterone levels, it also potentiates MR signaling in the kidneys by activating the small GTPase Rac1. This leads to hypertension and renal injury [17, 18, 21, 22]. This possibility is supported by the finding that eplerenone-associated reductions in UACR do not correlate with baseline plasma or urinary aldosterone concentrations [10].
Hemodynamic changes, especially changes in blood pressure, play major roles in reducing albuminuria [23]. In agreement with previous findings, our study showed that the reduction in UACR correlated positively with the reduction in SBP (Supplementary Figure 4). Notably, the reduction in UACR occurred during the early phase of the study (at 4 or 8 weeks). Thus, the early phase reduction in UACR may be due to hemodynamic rather than histological changes. That the beneficial effect of the MR blocker on albuminuria is mediated by hemodynamic change is supported by a sub-analysis of the TOPCAT study: this analysis showed that an MR blocker is beneficial in American heart failure patients and that this effect associated with a decrease in blood pressure. By contrast, Russian/Georgian patients with heart failure did not benefit from the MR-blocker treatment, nor did they exhibit a decrease in blood pressure [24]. Taken together, these findings suggest that the antihypertensive efficacy of eplerenone is shaped by the amount of salt intake and salt-induced MR activation contributes to the resistance of blood pressure to RAS blockade and the resulting albuminuria.
The results presented here also suggest that it is important to restrict dietary salt when treating CKD patients with RAS blockade therapy. While the study design did not permit us to evaluate the effect of salt restriction on resistance to RAS blockade [25], this notion is supported by the fact that when non-diabetic Japanese individuals with a higher baseline salt intake (≥240 mEq/day) were asked to restrict their salt intake for 1 year, their UACR dropped significantly [26]. Thus, there may be a causal relationship between dietary salt intake and albuminuria. Moreover, an intensive low salt diet reduced the albuminuria in non-diabetic hypertensive Korean patients who were treated with olmesartan [27]. Because the incidence of resistant hypertension in CKD patients with albuminuria is high [28], these findings suggest that MR blocker [29] as well as a low salt diet [30] may be effective treatments for resistant hypertension.
The daily salt intake of the cohort (as calculated from estimated 24-h UNa) was relatively high in this study. This high salt intake may be largely due to the local dietary habits in East Asia, where people are reported to have the highest salt intake in the world [31]. A recent nationwide study in Japan reported that the mean sodium excretion was 206.0 mEq/day in men and 173.9 mEq/day in women [32]. Moreover, a large-scale cohort study reported that the mean estimated 24-h UNa of the participants, 42% of whom were from China, was 214 mEq/day [33]. As a result, even the lowest tertile of our study cohort, who had 24-h UNa levels of ≤189 mEq/day, included subjects whose sodium excretion levels were higher than the global average (about 160 mEq/day) [34]. Nevertheless, the UACR in the lowest tertile did not worsen during the 52 weeks of treatment with standard RAS blockade (the change in UACR at 52 weeks relative to baseline was −0.8%). This suggests that consuming <189 mEq of salt per day will not influence the antialbuminuric effects of RAS blockade in this high salt-consuming population. However, it remains possible that the relatively high salt intake of the study population may have weakened the differences between the tertiles in terms of baseline plasma renin activity (PRA): this may have resulted in the loss of significant relationships between basal PRA and eplerenone-induced reduction of blood pressure or UACR.
Several other potential factors may affect the interpretation of our study results. First, the aforementioned TOPCAT sub-analysis showed that the beneficial effect of the MR blocker in the American heart failure patients also associated with increased serum potassium and creatinine concentrations [24]. In our study, the MR blockade also associated with increased serum potassium concentrations (but not serum creatinine concentrations). However, this association was only significant in the lowest and middle tertiles; the difference between the eplerenone and placebo groups in the highest tertile did not achieve statistical significance (Table 2). Therefore, it seems that serum potassium and creatinine concentrations played only limited roles in the ability of eplerenone to significantly reduce the UACR in the highest tertile. Second, in the lowest tertile, the placebo group had a higher baseline ARR than the eplerenone group. This suggests the possibility that this placebo group had a higher prevalence of subclinical primary aldosteronism. However, that may not affect the result because in that tertile, RAS blockade on its own did not differ significantly from RAS blockade plus MR blockade in terms of changing the UACR at 52 weeks. Third, the highest tertile group had a higher body weight than the lowest tertile (73.0 and 71.3 vs. 65.7 and 63.6 kg in the eplerenone and the placebo group, respectively) (Table 1). This is important because investigators have shown that the amount of daily salt intake increases proportionally with the incidence of obesity [35]. Moreover, obesity as well as metabolic syndrome often associates with salt-sensitive hypertension [36,37,38]. Thus, even though the tertiles did not differ significantly in terms of baseline plasma aldosterone levels, it remains possible that obesity-induced hyperaldosteronism may have elevated the plasma aldosterone levels in the highest tertile to some degree. It is also possible that the higher body weight of the highest tertile may also have influenced its response to eplerenone, because it has been reported that eplerenone more effectively reduces blood pressure and albuminuria in patients with metabolic syndrome [39]. In our study, however, body weight did not correlate significantly with either plasma aldosterone levels or the change in UACR at 52 weeks (data not shown).
This analysis also had several methodological limitations that are due to its post hoc, exploratory, and predefined design. First, change in UACR is a surrogate marker for ESRD. Thus, trials examining the effect of eplerenone on more representative endpoints of ESRD are warranted. In addition, 24-h UNa at baseline was calculated from spot urine. While this method is practical, its ability to precisely measure salt intake is limited [40]. Specifically, while the 24-h UNa estimate is highly reliable when it is in the range of 181.0–233.3 mEq/day, it is relatively less reliable in the lower range, where the formula tends to underestimate the 24-h UNa [20].
Finally, this study showed that combination therapy with 50 mg/day eplerenone and standard doses of RAS inhibitors was efficacious and safe for non-diabetic patients with CKD, albuminuria, an eGFR of 50 ml/min per 1.73 m2 or more, and especially high salt intake. However, such combination therapy in patients with diabetic nephropathy and/or renal insufficiency increases the risk of serious hyperkalemia. This is supported by the fact that the present study showed that the combination therapy significantly increased the plasma potassium levels, although it did not elevate the frequency of severe hyperkalemia. Future studies that evaluate the ability of MR antagonists to retard the progression of ESRD as well as reduce albuminuria and blood pressure in patients with diabetic kidney diseases are needed. Similar studies with patients with renal insufficiency (eGFR in the range of 30–60) and with Caucasian patients with low daily salt intake (100–150 mEq/day) are also warranted. Nevertheless, our study, together with the fact that a meta-analysis of the placebo-adjusted drug effects in 21 clinical trials showed that reducing residual albuminuria correlates positively with retarded progression to ESRD [41], suggests that MR blockade may help to improve the CKD prognosis of hypertensive patients with residual albuminuria who are being treated with standard RAS therapy, especially when resistance to RAS inhibitors associates with excessive salt intake.
Disclaimer
The corresponding author had full access to all of the data in the study and takes full responsibility for the integrity of the data and the accuracy of the data analysis.
References
Mancia G, Fagard R, Narkiewicz K, Redón J, Zanchetti A, Böhm M. et al. Task Force Members. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens. 2013;31:1281–357.
James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, Handler J, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA. 2014;311:507–20.
Shimamoto K, Ando K, Fujita T, Hasebe N, Higaki J, Horiuchi M, et al. Japanese Society of Hypertension Committee for Guidelines for the Management of Hypertension. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2014). Hypertens Res. 2014;37:253–390.
de Zeeuw D, Remuzzi G, Parving H-H, Keane WF, Zhang Z, Shahinfar S, et al. Proteinuria, a target for renoprotection in patients with type 2 diabetic nephropathy: lessons from RENAAL. Kidney Int. 2004;65:2309–20.
Sato A, Hayashi K, Naruse M, Saruta T. Effectiveness of aldosterone blockade in patients with diabetic nephropathy. Hypertension. 2003;41:64–68.
Epstein M, Williams GH, Weinberger M, Lewin A, Krause S, Mukherjee R, et al. Selective aldosterone blockade with eplerenone reduces albuminuria in patients with type 2 diabetes. Clin J Am Soc Nephrol. 2006;1:940–51.
Mehdi UF, Adams-Huet B, Raskin P, Vega GL, Toto RD. Addition of angiotensin receptor blockade or mineralocorticoid antagonism to maximal angiotensin-converting enzyme inhibition in diabetic nephropathy. J Am Soc Nephrol. 2009;20:2641–50.
Mavrakanas TA, Gariani K, Martin P-Y. Mineralocorticoid receptor blockade in addition to angiotensin converting enzyme inhibitor or angiotensin II receptor blocker treatment: an emerging paradigm in diabetic nephropathy: a systematic review. Eur J Intern Med. 2014;25:173–6.
Bakris GL, Agarwal R, Chan JC, Cooper ME, Gansevoort RT, Haller H. et al. Mineralocorticoid Receptor Antagonist Tolerability Study–Diabetic Nephropathy (ARTS-DN) Study Group. Effect of finerenone on albuminuria in patients with diabetic nephropathy: a randomized clinical trial. JAMA. 2015;314:884–94.
Ando K, Ohtsu H, Uchida S, Kaname S, Arakawa Y, Fujita T. et al. for the EVALUATE Study Group. Anti-albuminuric effect of the aldosterone blocker eplerenone in non-diabetic hypertensive patients with albuminuria: a double-blind, randomised, placebo-controlled trial. Lancet Diabetes Endocrinol. 2014;2:944–53.
Vegter S, Perna A, Postma MJ, Navis G, Remuzzi G, Ruggenenti P. Sodium intake, ACE inhibition, and progression to ESRD. J Am Soc Nephrol. 2012;23:165–73.
Engelen L, Soedamah-Muthu SS, Geleijnse JM, Toeller M, Chaturvedi N, Fuller JH, et al. Higher dietary salt intake is associated with microalbuminuria, but not with retinopathy in individuals with type 1 diabetes: the EURODIAB Prospective Complications Study. Diabetologia. 2014;57:2315–23.
Han SY, Hong JW, Noh JH, Kim D-J. Association of the estimated 24-h urinary sodium excretion with albuminuria in adult koreans: the 2011 Korea National Health and Nutrition Examination Survey. PLoS ONE. 2014;9:e109073.
McMahon EJ, Bauer JD, Hawley CM, Isbel NM, Stowasser M, Johnson DW, et al. A randomized trial of dietary sodium restriction in CKD. J Am Soc Nephrol. 2013;24:2096–103.
Heeg JE, de Jong PE, van der Hem GK, de Zeeuw D. Efficacy and variability of the antiproteinuric effect of ACE inhibition by lisinopril. Kidney Int. 1989;36:272–9.
Lambers Heerspink HJ, Holtkamp FA, Parving H-H, Navis GJ, Lewis JB, Ritz E, et al. Moderation of dietary sodium potentiates the renal and cardiovascular protective effects of angiotensin receptor blockers. Kidney Int. 2012;82:330–7.
Shibata S, Mu S, Kawarazaki H, Muraoka K, Ishizawa K-I, Yoshida S, et al. Rac1 GTPase in rodent kidneys is essential for salt-sensitive hypertension via a mineralocorticoid receptor-dependent pathway. J Clin Invest. 2011;121:3233–43.
Shibata S, Ishizawa K, Uchida S. Mineralocorticoid receptor as a therapeutic target in chronic kidney disease and hypertension. Hypertens Res. 2017;40:221–5.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K. et al. Collaborators developing the Japanese equation for estimated GFR.Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Tanaka T, Okamura T, Miura K, Kadowaki T, Ueshima H, Nakagawa H, et al. A simple method to estimate populational 24-h urinary sodium and potassium excretion using a casual urine specimen. J Hum Hypertens. 2002;16:97–103.
Shibata S, Nagase M, Yoshida S, Kawarazaki W, Kurihara H, Tanaka H, et al. Modification of mineralocorticoid receptor function by Rac1 GTPase: implication in proteinuric kidney disease. Nat Med. 2008;14:1370–6.
Nishimoto M, Fujita T. Renal mechanisms of salt-sensitive hypertension: contribution of two steroid receptor-associated pathways. Am J Phsiol Renal Physiol. 2015;308:F377–87.
Fotheringham J, Odudu A, McKane W, Ellam T. Modification of the relationship between blood pressure and renal albumin permeability by impaired excretory function and diabetes. Hypertension. 2015;65:510–6.
Pfeffer MA, Claggett B, Assmann SF, Boineau R, Anand IS, Clausell N, et al. Regional variation in patients and outcomes in the Treatment of Preserved Cardiac Function Heart Failure With an Aldosterone Antagonist (TOPCAT) trial. Circulation. 2015;131:34–42.
Ando K, Ohtsu H, Arakawa Y, Kubota K, Yamaguchi T, Nagase M. et al. Eplerenone combination Versus conventional Agents to Lower blood pressure on Urinary Antialbuminuric Treatment Effect Study Investigators. Rationale and design of the Eplerenone combination Versus conventional Agents to Lower blood pressure on Urinary Antialbuminuric Treatment Effect (EVALUATE) trial: a double-blinded randomized placebo-controlled trial to evaluate the antialbuminuric effects of an aldosterone blocker in hypertensive patients with albuminuria. Hypertens Res. 2010;33:616–21.
Suzuki K, Konta T, Takasaki S, Ikeda A, Ichikawa K, Sato H, et al. High variability of albuminuria in nondiabetic population: the Takahata Study. Clin Exp Nephrol. 2009;13:452–9.
Hwang JH, Chin HJ, Kim S, Kim DK, Kim S, Kim S, et al. Effects of intensive low-salt diet education on albuminuria among nondiabetic patients with hypertension treated with olmesartan: a single-blinded randomized, controlled trial. Clin J Am Soc Nephrol. 2014;9:2059–69.
Tanner RM, Calhoun DA, Bell EK, Bowling CB, Gutiérrez OM, Irvin MR, et al. Prevalence of apparent treatment-resistant hypertension among individuals with CKD. Clin J Am Soc Nephrol. 2013;8:1583–90.
Václavík J, Sedlák R, Plachy M, Navrátil K, Plásek J, Jarkovsky J, et al. Addition of spironolactone in patients with resistant arterial hypertension (ASPIRANT): a randomized, double-blind, placebo-controlled trial. Hypertension. 2011;57:1069–75.
Pimenta E, Gaddam KK, Oparil S, Aban I, Husain S, Dell’Italia LJ, et al. Effects of dietary sodium reduction on blood pressure in subjects with resistant hypertension: results from a randomized trial. Hypertension. 2009;54:475–81.
Powles J, Fahimi S, Micha R, Khatibzadeh S, Shi P, Ezzati M. et al.Global Burden of Diseases Nutrition and Chronic Diseases Expert Group (NutriCoDE) Global, regional and national sodium intakes in 1990 and 2010: a systematic analysis of 24 h urinary sodium excretion and dietary surveys worldwide. BMJ Open. 2013;3:e003733–e003733.
Asakura K, Uechi K, Sasaki Y, Masayasu S, Sasaki S. Estimation of sodium and potassium intakes assessed by two 24 h urine collections in healthy Japanese adults: a nationwide study. Br J Nutr. 2014;112:1195–205.
O’Donnell M, Mente A, Rangarajan S, McQueen MJ, Wang X, Liu L. et al. PURE Investigators. Urinary sodium and potassium excretion, mortality, and cardiovascular events. N Engl J Med. 2014;371:612–23.
McCarron DA, Kazaks AG, Geerling JC, Stern JS, Graudal NA. Normal range of human dietary sodium intake: a perspective based on 24-hour urinary sodium excretion worldwide. Am J Hypertens. 2013;26:1218–23.
Ma Y, He FJ, Macgregor GA. High salt intake: independent risk factor for obesity? Hypertension. 2015;66:843–9. https://doi.org/10.1161/HYPERTENSIONAHA.115.05948
Perschel FH, Schemer R, Seiler L, Reincke M, Deinum J, Maser-Gluth C, et al. Rapid screening test for primary hyperaldosteronism: ratio of plasma aldosterone to renin concentration determined by fully automated chemiluminescence immunoassays. Clin Chem. 2004;50:1650–5.
Nagase M, Fujita T. Mineralocorticoid receptor activation in obesity hypertension. Hypertens Res. 2009;32:649–57.
Ahmed AH, Gordon RD, Taylor P, Ward G, Pimenta E, Stowasser M, et al. Effect of atenolol on aldosterone/renin ratio calculated by both plasma renin activity and direct renin concentration in healthy male volunteers. J Clin Endocrinol Metab. 2010;95:3201–6.
Suzuki H, Shuto H, Shuto C, Ohara I, Inokuma S, Abe Y, et al. Eplerenone, an aldosterone blocker, is more effective in reducing blood pressure in patients with, than without, metabolic syndrome. Ther Adv Cardiovasc Dis. 2012;6:141–7.
Kawano Y, Tsuchihashi T, Matsuura H, Ando K, Fujita T, Ueshima H. et al.Working Group for Dietary Salt Reduction of the Japanese Society of Hypertension. Report of the Working Group for Dietary Salt Reduction of the Japanese Society of Hypertension: (2) Assessment of salt intake in the management of hypertension. Hypertens Res. 2007;30:887–93.
Lambers Heerspink HJ, Kröpelin TF, Hoekman J, de Zeeuw D, on behalf of the, Reducing Albuminuria as Surrogate Endpoint (REASSURE) Consortium. Drug-induced reduction in albuminuria is associated with subsequent renoprotection: a meta-analysis. J Am Soc Nephrol. 2014;26:2055–64.
Acknowledgements
T.F. was supported by JSPS KAKENHI Grant Number 15H05788. The EVALUATE study was sponsored by Pfizer.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors indicated no potential conflicts of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Nishimoto, M., Ohtsu, H., Marumo, T. et al. Mineralocorticoid receptor blockade suppresses dietary salt-induced ACEI/ARB-resistant albuminuria in non-diabetic hypertension: a sub-analysis of evaluate study. Hypertens Res 42, 514–521 (2019). https://doi.org/10.1038/s41440-018-0201-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-018-0201-7
- Springer Nature Singapore Pte Ltd.
Keywords
This article is cited by
-
Exploratory study on the relationship between urinary sodium/potassium ratio, salt intake, and the antihypertensive effect of esaxerenone: the ENaK Study
Hypertension Research (2024)
-
Aldosteron und Niere – eine komplexe Interaktion
Journal für Endokrinologie, Diabetologie und Stoffwechsel (2024)
-
Efficacy and safety of a low-sodium diet and spironolactone in patients with stage 1-3a chronic kidney disease: a pilot study
BMC Nephrology (2022)
-
Lysine-specific demethylase 1 as a corepressor of mineralocorticoid receptor
Hypertension Research (2022)
-
Antihypertensive Effect of Long-Term Monotherapy with Esaxerenone in Patients with Essential Hypertension: Relationship Between Baseline Urinary Sodium Excretion and Its Antihypertensive Effect
Advances in Therapy (2022)