Abstract
Because nitric oxide could play an important role in the pathogenesis of migraine (suggested by experimental, neuropathological, biochemical, and pharmacological data), and a recent meta-analysis showed an association between the single-nucleotide polymorphism (SNP) rs2070744 in the endothelial nitric oxide synthase (eNOS or NOS3) gene (chromosome 7q36.1) and the risk for migraine in Caucasians, we attempted to replicate the possible association between this SNP and the and the risk for migraine in the Caucasian Spanish population. The frequencies for the NOS3 rs2070744 genotypes and allelic variants were assessed in 283 migraine patients and 287 healthy controls with a TaqMan-based qPCR Assay. The putative influence on genotype frequency of age at onset of migraine attacks, gender, family history of migraine, absence or presence of aura, and triggering of migraine attacks by ethanol, were also analyzed. The frequencies of NOS3 rs2070744 genotypes and allelic variants were not associated with the risk for migraine (OR [95%] CI for the minor allele = 0.91 [0.72–1.15]) and were not influenced by age at onset of migraine, gender, presence of aura, or triggering of migraine attacks by ethanol. NOS3 rs2070744CC genotypes were significantly more frequent in patients with a family history of migraine. NOS3 rs2070744 SNP is not associated with the risk for migraine in Caucasian Spanish people although it might be related to family history.
Similar content being viewed by others
Introduction
Migraine is one of the most frequent neurological disorders, affecting between 10 and 18% of the population with a higher incidence in women than in men (2–3/1). Both, migraines without aura (MWoA) and with aura (MWA) show a high frequency of positive family history, ranging from 50 to 70%, and it is well known that the risk for both MWoA and MWA is increased in subjects with first-degree parents affected by this disease. However, migraine genetics is not well established to date. In patients with familial hemiplegic migraine, several genes such as CACNA1A, ATP1A2, and SCN1A have been identified as causative [1]. A recent meta-analysis of 22 hypothesis-free genome-wide association studies involving migraine patients (n = 59,764) and healthy controls (n = 316,078) identified 38 susceptibility loci for migraine [2]. During the last 20 years, there have been reported a substantial number of hypothesis-driven case-control association studies trying to establish a possible relationship between genetic variants in many candidate genes and the risk for migraine, leading to variable and inconsistent results, but a detailed description of these studies is out of the scope of the present report.
Nitric oxide (NO) has many important biological functions, which include the inhibition of platelet aggregation, the maintaining of the arterial vasodilatory tone, actions on neurotransmission processes, antitumor and antimicrobial activities, and mediation of macrophage cytotoxicity [3]. In addition, depending on its redox form, NO can act as a reactive free radical or have neuroprotective effects through N-methyl-D-aspartate glutamatergic receptor blockade [3]. The synthesis of NO from l-arginine is mediated by the three isoforms of NO synthase (NOS): neuronal NOS (nNOS or NOS1), inducible NOS (iNOS or NOS2), and endothelial NOS (eNOS or NOS3).
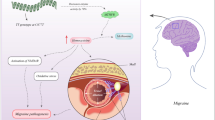
It is well known that NO has important implications in the pathophysiology of migraine, which are supported by many experimental, biochemical, neuropathological, and pharmacological data, involving mainly, but not exclusively, NOS1 (revised in [4, 5]). Several studies have addressed the possible association of certain allelic variants in NOS genes with the risk for migraine [4, 6,7,8,9,10,11,12,13,14,15,16,17,18,19] with variable results (revised in [4]).
NOS3 or eNOS gene (chromosome 7q36.1; gene identity 4846, MIM 163729) encodes the protein eNOS (http://www.ncbi.nlm.nih.gov/gene/4846). Two studies have shown an association between the NOS3 rs2070744 single-nucleotide polymorphism (SNP) and the risk for migraine [17, 19], while others failed to find this association [8, 13, 15, 18]. A recent meta-analysis showed an increased risk for migraine in carriers of the rs2070744CC genotype in Caucasian populations, and a lack of association in non-Caucasian populations and in the whole series [20].
In this replication study, we investigated the possible association between the rs2070744 and the risk for migraine in Caucasian Spanish people. We also studied, as a secondary analysis, the possible influence of this SNP in age at onset of migraine, gender, positive family history of migraine, the presence or absence of aura in migraineurs, and in the triggering of migraine attacks by alcohol.
Patients and methods
Patients and controls
The demographic data of the 283 patients fulfilling standardized diagnostic criteria for migraine (none of them suffered from other headache types) [21] and the 287 age- and gender-matched controls (who did not have either personal or familial positive history of migraine and did not suffer from other headache types) who participated in this study are summarized in Table 1. Migraine patients were recruited in the general neurologic clinics of three university hospitals during the periods between September 2006–September 2007 and June 2017–February 2019. Many of these patients were involved in other case-control genetic association studies published by our group [4, 22,23,24,25,26,27,28,29]. Details of the recruitment of both migraine patients and healthy controls were described elsewhere [28].
Ethical aspects
The principles of the Declaration of Helsinki were applied. All the participants were included in the study after written informed consent. The study protocol was approved by the Ethics Committees of the University Hospital “Príncipe de Asturias” (Alcalá de Henares, Madrid, Spain), University Hospital “Infanta Cristina” (Badajoz, Spain), and Hospital La Mancha-Centro (Alcázar de San Juan, Ciudad Real, Spain).
Genotyping of rs2070744 variants
Genotyping was performed in genomic DNA obtained from venous blood samples of participants using specific TaqMan probes for the rs2070744 SNP (C__15903863_10, Life Technologies, Alcobendas, Madrid, Spain). Full details of the procedure were described elsewhere [4].
Statistical analysis
Statistical analyses were done by using the SPSS 15.0 for Windows (SPSS Inc., Chicago, IL, USA). The Hardy–Weinberg equilibrium was confirmed, both in patients and in controls, by using the online program https://ihg.gsf.de/cgi-bin/hw/hwa1.pl. The chi-square test (or the Fisher’s exact test where appropriate) was used for assessing intergroup comparison values (both between the whole series of migraine patients and controls and between migraine patients and controls considering each gender separately). The 95% confidence intervals and the negative predictive values [30] were also calculated.
The sample size was determined from the allele frequencies observed for healthy individuals by using a genetic model that analyzed the minor allele frequency with an odds ratio (OR) value = 1.5 (α = 0.05). The statistical power (two-tailed association) for rs2070744 variant alleles, according to the sample size of this study, was 92.6%.
The genotype and allelic frequencies between subgroups of migraine patients according to the age at onset of migraine attacks (≤16 years vs. ≥16 years), negativity vs. positivity of family history of migraine, absence or presence of aura, and triggering or non triggering migraine attacks with alcohol were well calculated by using the chi-square test or the Fisher’s exact test when appropriate as well. The comparison of mean age at onset of migraine attacks between the three genotypes of rs2070744 SNP was done with a T-test for independent samples.
Results
The frequencies of rs2070744 genotypes and allelic variants were in Hardy–Weinberg’s equilibrium both in migraine patients and in healthy controls groups, did not differ significantly between the two groups (Table 2), and were not influenced by gender (Table 3) and age at onset of migraine (Table 4), and were similar in patients diagnosed with MWA than in those with MWoA (Table 4), and in migraine patients in which ethanol triggered migraine attacks than in those in which ethanol did not trigger migraine attacks (Table 5). The OR (95% CI; P) values obtained using the dominant and recessive models for the risk of developing migraine were 1.07 (0.75–1.52; 0.700) and 0.80 (0.49–1.29; 0.359), respectively. Armitage test for trend with the number of variant alleles indicated an OR equal to 0.9, with a P value = 0.414.
The frequencies of rs2070744CC genotype and rs2070744C allele were significantly higher in patients with a positive family history of migraine compared with those without a family history of this disease (Table 4). Mean ± SD age at onset of migraine was similar in migraine patients with rs2070744CC, CT, and TT genotypes (Table 6).
The OR (95% CI; P) values obtained using the dominant and recessive models for the comparison regarding family history positivity were 0.65 (0.37–1.16; 0.147) and 3.36 (1.20–9.44; 0.017), respectively. Armitage test for trend with the number of variant alleles indicated an OR value equal to 1.73, with a P value = 0.026.
Discussion
NOS3 rs2070744 SNP could affect NOS3 expression, which is related with endothelial dysfunction [31, 32]. NOS3 rs2070744 SNP has been associated with increased risk of coronary artery disease [33,34,35], essential hypertension [36], diabetes mellitus [34], diabetic nephropathy [34], diabetic retinopathy [37], cancer [38], periodontal disease [39], preeclampsia [40], normal tension glaucoma [41], psoriasis [42], multiple sclerosis [43], hypoxic-ischemic encephalopathy [44], delayed cerebral ischemia following aneurismal subarachnoid hemorrhage [45], and the power athletic status [46,47,48]. A population-based study in USA showed association between NOS3 rs2070744 and increased risk for stroke [49], while a case-control association study in Turkish did not find that association [50]. Finally, Gao et al. [51] describe decreased risk for immunoglobulin A nephropathy (in interaction with NOS3 rs1799983) in Chinese.
Despite NO could play an important role in the pathogenesis of migraine, as it was suggested by many previous data [4], to date it is not well established the possible contribution of polymorphisms in the NOS genes with the risk of developing this disease. Together with the description of increased risk for migraine described in Caucasian individuals carrying the NOS3 rs2070744CC genotype in a recent meta-analysis [20], Gonçalves et al. [15] described interaction between NOS3 rs743506 and NOS2 rs2297518 SNPs in the risk for migraine, and Güler et al. [18] a higher NOS3 rs1799983TT genotype frequency in migraine patients who had a headache duration of longer than 24 h compared with patients who had migraine of shorter duration. These data should suggest a possible association between NOS3 genes and migraine.
In contrast with the results of the previously mentioned meta-analysis describing a modest increase in the risk for migraine related with the NOS3 rs2070744CC genotype in Caucasians (435 migraine patients vs. 345 controls; OR [95% CI] = 1.62 [1.03–2.56] compared with TT + TC genotypes) [20], in the present study, involving Caucasian Spanish people, we failed to find any association between NOS3 rs2070744 variants with the risk for migraine, both analyzing the frequency of the different genotypes of this SNP under dominant, recessive of allelic models. Moreover, the pooled data of the present study with those of Caucasian series in the previously reported meta-analysis showed a lack of association of rs2070744 SNP as well (718 migraine patients vs. 632 controls; OR [95% CI] = 1.16 [0.86–1.57], P = 0.334). In addition, a secondary analysis failed to show any relationship between NOS3 rs2070744 variants and the age at onset of migraine, gender, presence or absence of aura, or provocation of migraine attacks by ethanol. However, we found an association between rs2070744CC genotype and rs2070744C alleles with the positivity of family history of migraine, but the statistical significance of this finding was not enough strong.
The relatively low sample size of the migraine patient and control cohorts involved in the current study (although it should be adequate to detect ORs of 1.5, it could be insufficient to detect more modest associations) should be considered as its main limitation. Taking into account the limitations of the present study, and in contrast with a previous meta-analysis [20], NOS3 rs2070744 variants are apparently unrelated with the risk of migraine in the Caucasian Spanish people. The fact that this particular SNP showed a lack of association with the risk of developing migraine in the population analyzed in the present study does not preclude the possibility of an association between other SNPs in the NOS3 gene and a modification in the risk for this disease.
References
Mateos V, Pareja JA, Pascual J. Tratado de cefaleas. Madrid: Luzán 5 S.A. Ediciones; 2009.
Gormley P, Anttila V, Winsvold BS, Palta P, Esko T, Pers TH, et al. Meta-analysis of 375,000 individuals identifies 38 susceptibility loci for migraine. Nat Genet. 2016;48:856–66.
Molina JA, Jiménez-Jiménez FJ, Ortí-Pareja M, Navarro JA. The role of nitric oxide in neurodegeneration: potential for pharmacological intervention. Drugs Aging. 1998;12:251–9.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, García-Albea E, et al. Neuronal nitric oxide synthase (nNOS, NOS1) rs693534 and rs7977109 variants and risk for migraine. Headache. 2015;55:1209–17.
Pradhan AA, Bertels Z, Akerman S. Targeted nitric oxide synthase inhibitors for migraine. Neurotherapeutics. 2018;15:391–401.
Griffiths LR, Nyholt DR, Curtain RP, Goadsby PJ, Brimage PJ. Migraine association and linkage studies of an endothelial nitric oxide synthase (NOS3) gene polymorphism. Neurology. 1997;49:614–7.
Lea RA, Curtain RP, Shepherd AG, Brimage PJ, Griffiths LR. No evidence for involvement of the human inducible nitric oxide synthase (iNOS) gene in susceptibility to typical migraine. Am J Med Genet. 2001;105:110–3.
Logan JF, Chakravarthy U, Hughes AE, Patterson CC, Jackson JA, Rankin SJ. Evidence for association of endothelial nitric oxide synthase gene in subjects with glaucoma and a history of migraine. Investig Ophthalmol Vis Sci. 2005;46:3221–6.
Borroni B, Rao R, Liberini P, Venturelli E, Cossandi M, Archetti S, et al. Endothelial nitric oxide synthase (Glu298Asp) polymorphism is an independent risk factor for migraine with aura. Headache. 2006;46:1575–9.
Toriello M, Oterino A, Pascual J, Castillo J, Colás R, Alonso-Arranz A, et al. Lack of association of endothelial nitric oxide synthase polymorphisms and migraine. Headache. 2008;48:1115–9.
Schürks M, Kurth T, Buring JE, Zee RY. A candidate gene association study of 77 polymorphisms in migraine. J Pain. 2009;10:759–66.
Jia S, Ni J, Chen S, Jiang Y, Dong W, Gao Y. Association of the pentanucleotide repeat polymorphism in NOS2 promoter region with susceptibility to migraine in a Chinese population. DNA Cell Biol. 2011;30:117–22.
Gonçalves FM, Martins-Oliveira A, Speciali JG, Luizon MR, Izidoro-Toledo TC, Silva PS, et al. Endothelial nitric oxide synthase haplotypes associated with aura in patients with migraine. DNA Cell Biol. 2011;30:363–9.
de OS, Mansur T, Gonçalves FM, Martins-Oliveira A, Speciali JG, Dach F, et al. Inducible nitric oxide synthase haplotype associated with migraine and aura. Mol Cell Biochem. 2012;364:303–8.
Gonçalves FM, Luizon MR, Speciali JG, Martins-Oliveira A, Dach F, Tanus-Santos JE. Interaction among nitric oxide (NO)-related genes in migraine susceptibility. Mol Cell Biochem. 2012;370:183–9.
Alaşehirli B, Akçalı A, Demiryürek AT, Özel A, Erdal ME, Neyal M. Lack of association between the C276T polymorphism of the neuronal nitric oxide synthase gene and migraine. Int J Neurosci. 2013;123:50–4.
Eröz R, Bahadir A, Dikici S, Tasdemir S. Association of endothelial nitric oxide synthase gene polymorphisms (894G/T, -786T/C, G10T) and clinical findings in patients with migraine. Neuromolecular Med. 2014;16:587–93.
Güler S, Gürkan H, Tozkir H, Turan N, Çelik Y. An investigation of the relationship between the eNOS gene polymorphism and diagnosed migraine. Balk J Med Genet. 2015;17:49–59.
Zakerjafari M, Dehkordi FF, Yaghoubi H. Evaluation of NOS3 T-C 786 gene polymorphism in Iranian patients affected by migraine and normal individuals. Adv Biores. 2016;7:16–9.
Dong H, Wang ZH, Dong B, Hu YN, Zhao HY. Endothelial nitric oxide synthase (-786T>C) polymorphism and migraine susceptibility: a meta-analysis. Medicine. 2018;97:e12241.
Headache Classification Committee of the International Headache Society. The International classification of headache disorders, 2nd ed. Cephalalgia. 2004;24(Suppl.1):1–160.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Agúndez JA, et al. Histamine-N-methyl transferase polymorphism and risk for migraine. Headache. 2008;48:1343–8.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Agúndez JA, et al. Alcohol dehydrogenase 2 genotype and risk for migraine. Headache. 2010;50:85–91.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Agúndez JA, et al. Dopamine receptor 3 (DRD3) polymorphism and risk for migraine. Eur J Neurol. 2010;17:1220–3.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Agúndez JA, et al. Paraoxonase 1 (PON 1) polymorphisms and risk for migraine. J Neurol. 2010;257:1482–5.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Agúndez JA, et al. SLC1A2 rs3794087 variant and risk for migraine. J Neurol Sci. 2014;338:92–5.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Ayuso P, Navacerrada F, et al. Diamine oxidasers10156191 and rs2052129 variants are associated with the risk for migraine. Headache. 2015;55:276–86.
García-Martín E, Martínez C, Serrador M, Alonso-Navarro H, Navacerrada F, Esguevillas G, et al. Gamma-aminobutyric acid (Gaba) receptors Rho (Gabrr) gene polymorphisms and risk for migraine. Headache. 2017;57:1118–35.
García-Martín E, Esguevillas G, Serrador M, Alonso-Navarro H, Navacerrada F, Amo G, et al. Gamma-aminobutyric acid (GABA) receptors GABRA4, GABRE, and GABRQ gene polymorphisms and risk for migraine. J Neural Transm. 2018;125:689–98.
Altman DG, Bland JM. Diagnostic tests 2: predictive values. Brit Med J. 1994;309:102.
Napoli C, Ignarro LJ. Nitric oxide and atherosclerosis. Nitric Oxide. 2001;5:88–97.
Napoli C, de Nigris F, Williams-Ignarro S, Pignalosa O, Sica V, Ignarro LJ. Nitric oxide and atherosclerosis: an update. Nitric Oxide. 2006;15:265–79.
Kong XZ, Zhang ZY, Wei LH, Li R, Yu J. The endothelial nitric oxide synthase gene T-786C polymorphism increases myocardial infarction risk: a meta-analysis. Med Sci Monit. 2017;23:759–66.
Dong J, Ping Y, Wang Y, Zhang Y. The roles of endothelial nitric oxide synthase gene polymorphisms in diabetes mellitus and its associated vascular complications: a systematic review and meta-analysis. Endocrine. 2018;62:412–22.
Li X, Lin Y, Zhang R. Associations between endothelial nitric oxide synthase gene polymorphisms and the risk of coronary artery disease: a systematic review and meta-analysis of 132 case-control studies. Eur J Prev Cardiol. 2019;26:160–70.
Gamil S, Erdmann J, Abdalrahman IB, Mohamed AO. Association of NOS3 gene polymorphisms with essential hypertension in Sudanese patients: a case control study. BMC Med Genet. 2017;18:128.
Midani F, Ben Amor Z, El Afrit MA, Kallel A, Feki M, Soualmia H. The role of genetic variants (rs869109213 and rs2070744) of the eNOS gene and BglII in the α2 subunit of the α2β1 integrin gene in diabetic retinopathy in a Tunisian population. Semin Ophthalmol. 2019;34:365–74.
Nan J, Liu Y, Xu C, Ge D. Effects of eNOS gene polymorphisms on individual susceptibility to cancer: a meta-analysis. Nitric Oxide. 2019;84:1–6.
Mazurek-Mochol M, Kozak M, Sawczuk M, Maciejewska A, Malinowski D, Safranow K, et al. Nos3 gene Rs1799983 and Rs2070744 polymorphisms in patients with periodontal disease. Folia Biol. 2018;64:59–64.
Zhou L, Hui X, Yuan H, Liu Y, Wang Y. Combination of genetic markers and age effectively facilitates the identification of people with high risk of preeclampsia in the Han Chinese population. Biomed Res Int. 2018;2018:4808046.
Jeoung JW, Kim DM, Oh S, Lee JS, Park SS, Kim JY. The relation between endothelial nitric oxide synthase polymorphisms and normal tension glaucoma. J Glaucoma. 2017;26:1030–5.
Coto-Segura P, Coto E, Mas-Vidal A, Morales B, Alvarez V, Díaz M, et al. Influence of endothelial nitric oxide synthase polymorphisms in psoriasis risk. Arch Dermatol Res. 2011;303:445–9.
Heidari MM, Khatami M, Tahamtan Y. Molecular analysis of rs2070744 and rs1799983 polymorphisms of NOS3 gene in Iranian patients with multiple sclerosis. Basic Clin Neurosci. 2017;8:279–84.
Wu Y, Zhu Z, Fang X, Yin L, Liu Y, Xu S, et al. The association between NOS3 gene polymorphisms and hypoxic-ischemic encephalopathy susceptibility and symptoms in Chinese Han population. Biomed Res Int. 2016;2016:1957374.
Hendrix P, Foreman PM, Harrigan MR, Fisher WS 3rd, Vyas NA, Lipsky RH, et al. Endothelial nitric oxide synthase polymorphism is associated with delayed cerebral ischemia following aneurysmal subarachnoid hemorrhage. World Neurosurg. 2017;101:514–9.
Gómez-Gallego F, Ruiz JR, Buxens A, Artieda M, Arteta D, Santiago C, et al. The -786 T/C polymorphism in the NOS3 gene is associated with elite performance in power sports. Eur J Appl Physiol. 2009;107:565–9.
Zmijewski P, Cięszczyk P, Ahmetov II, Gronek P, Lulińska-Kuklik E, Dornowski M, et al. The NOS3 G894T (rs1799983) and -786T/C (rs2070744) polymorphisms are associated with elite swimmer status. Biol Sport. 2018;35:313–9.
Weyerstraß J, Stewart K, Wesselius A, Zeegers M. Nine genetic polymorphisms associated with power athlete status – a meta-analysis. J Sci Med Sport. 2018;21:213–20.
Fan AZ, Fang J, Yesupriya A, Chang MH, Kilmer G, House M, et al. Gene polymorphisms in association with self-reported stroke in US adults. Appl Clin Genet. 2010;3:23–28.
Anlıaçık SÖ, Tokgöz S, Zamani AG, Yıldırım MS, İyisoy MS. Investigation of the relationship between ischemic stroke and endothelial nitric oxide synthase gene polymorphisms [G894T, intron 4 VNTR and T786C]. Turk J Med Sci. 2019;49:589–94.
Gao J, Wang M, Wei L, Niu D, Wei J, Ou Y, et al. The endothelial nitric oxide synthase gene polymorphism is associated with the susceptibility to immunoglobulin a nephropathy in Chinese population. Kidney Blood Press Res. 2017;42:608–16.
Acknowledgements
This work was supported in part by grants RETICS RD16/0006/0004 (ARADyAL), PI15/00303, and PI18/00540 from Fondo de Investigación Sanitaria, Instituto de Salud Carlos III, Madrid, Spain, and GR18145 and IB16170 from Junta de Extremadura, Mérida, Spain. Partially funded with FEDER funds.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
García-Martín, E., Navarro-Muñoz, S., Rodriguez, C. et al. Association between endothelial nitric oxide synthase (NOS3) rs2070744 and the risk for migraine. Pharmacogenomics J 20, 426–432 (2020). https://doi.org/10.1038/s41397-019-0133-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41397-019-0133-x
- Springer Nature Limited
This article is cited by
-
Oxidative Stress and Migraine
Molecular Neurobiology (2024)
-
A Comprehensive Investigation of Risk Association Between the -786 T > C, + 884 G > A, VNTR, rs743506, rs3918226 of eNOS and Susceptibility of Migraine: A Updated Meta-Analysis Utilizing Trial Sequential Analysis
Journal of Molecular Neuroscience (2023)
-
Endothelial nitric oxide synthase (NOS3) rs2070744 polymorphism and risk for multiple sclerosis
Journal of Neural Transmission (2020)