Abstract
Psychedelic-assisted psychotherapy gained considerable interest as a novel treatment strategy for fear-related mental disorders but the underlying mechanism remains poorly understood. The serotonin 2A (5-HT2A) receptor is a key target underlying the effects of psychedelics on emotional arousal but its role in fear processing remains controversial. Using the psychedelic 5-HT2A/5-HT2C receptor agonist 2,5-dimethoxy-4-iodoamphetamine (DOI) and 5-HT2A receptor knockout (KO) mice we investigated the effect of 5-HT2A receptor activation on emotional processing. We show that DOI administration did not impair performance in a spontaneous alternation task but reduced anxiety-like avoidance behavior in the elevated plus maze and elevated zero maze tasks. Moreover, we found that DOI did not block memory recall but diminished fear expression in a passive avoidance task. Likewise, DOI administration reduced fear expression in an auditory fear conditioning paradigm, while it did not affect retention of fear extinction when administered prior to extinction learning. The effect of DOI on fear expression was abolished in 5-HT2A receptor KO mice. Administration of DOI induced a significant increase of c-Fos expression in specific amygdalar nuclei. Moreover, local infusion of the 5-HT2A receptor antagonist M100907 into the amygdala reversed the effect of systemic administration of DOI on fear expression while local administration of DOI into the amygdala was sufficient to suppress fear expression. Our data demonstrate that activation of 5-HT2A receptors in the amygdala suppresses fear expression but provide no evidence for an effect on retention of fear extinction.
Similar content being viewed by others
Introduction
Post-traumatic stress disorder (PTSD) is a severe mental disorder, that can develop following exposure to a traumatic event [1], affecting between 1.3% and 12.2% of individuals during their lifetime [2]. Patients typically suffer from intrusive thoughts and re-experience the trauma, while suffering long-term changes in arousal, mood and cognition [1]. The first-line treatment for PTSD consists of trauma-focused psychotherapies, such as exposure-based therapy, and pharmacotherapy with selective serotonin reuptake inhibitors [3,4,5]. While psychotherapy typically yields greater effects than pharmacotherapy [4], dropout rates are high [6, 7] and up to 60–72% of patients fail to achieve full remission [3, 6]. This has been conceptualized as a failure of fear extinction, the process in which subjects learn that a past fearful experience no longer poses an acute threat [8]. This has led to an ongoing search for pharmacological agents that improve the tolerability and efficacy of psychotherapy, especially of drugs that improve extinction [9, 10].
Psychedelic-assisted psychotherapy gained considerable interest in the treatment of mental disorders [11,12,13,14,15] and 3,4-methylenedioxymethamphetamine (MDMA) has given promising clinical results in patients with PTSD [16, 17]. The main rationale behind MDMA-assisted psychotherapy is that it may reduce aversion to fear-provoking thoughts while promoting the extinction of fearful memories [15, 18, 19]. Fear extinction is the learning process by which exposure to fear-provoking cues reduces fear responses. As such, MDMA may influence memories associated with traumatic events in a clinical setting [20]. Preclinical studies indicate that MDMA suppresses fear expression during extinction training, but its effects on extinction learning remain unclear [21,22,23,24]. MDMA shares several properties with psychostimulants, and classic psychedelics such as psilocybin, lysergic acid dimethylamide (LSD), and dimethyltryptamine (DMT) [25]. MDMA stimulates norepinephrine, serotonin and dopamine release by reversing the activity of their transporters [26,27,28,29,30,31]. Interestingly, 5-HT2A receptor antagonism was shown to attenuate the effects of MDMA on emotional arousal in humans [18, 32, 33] and reversed the effect of MDMA on fear processing in rats [23].
While classic psychedelics were explored in psychodynamic therapies of trauma, no formal clinical trial has examined their therapeutic potential in the treatment of PTSD [15]. In preclinical studies, the psychedelics psilocybin and TCB-2 enhanced the acquisition of trace fear extinction in mice [34, 35]. However, the effect of these compounds on the retention of fear extinction remains unclear. Interestingly, a recent study showed that a single dose of DMT decreased fear expression during extinction training and improved the retention of extinction [36]. Moreover, while chronic intermittent administration of DMT did not affect fear expression, it enhanced extinction retention in rats [37]. However, given that besides the 5-HT2A receptor, most psychedelics, including DMT, also target other receptors such as the 5-HT1A receptor, the molecular targets that drive the effects of classic psychedelics on fear processing are not clearly established.
In the present study, we explored the effects of the psychedelic 5-HT2A/5-HT2C receptor agonist 2,5-dimethoxy-4-iodoamphetamine (DOI) in wild type and 5-HT2A receptor knockout (5-HT2A KO) mice to determine the impact of 5-HT2A receptor activation on anxiety and fear processing. We first studied the effects of DOI administration on exploratory behavior in a spontaneous alternation task, an elevated zero maze task and in an elevated plus maze task. Next, we determined the effects of DOI treatment on memory recall and fear expression in passive avoidance task. Finally, we studied the effects of DOI in an auditory fear conditioning paradigm. We used c-Fos analysis and local administration of the 5-HT2A receptor antagonist M100907 to identify key anatomical substrates for the observed effect of DOI. In line with the psychedelic-assisted psychotherapy model, we hypothesized that administration of DOI, at a dose that leads to robust activation of 5-HT2A receptors, would rapidly reduce anxiety-like behaviors and would improve the retention of fear extinction in mice.
Materials and methods
Animals
Male C57BL/6J wild type mice or 5-HT2A receptor KO mice on C57BL/6J background, aged 8–12 weeks at the time of testing, were group housed (2–4 per cage) and maintained on a 12/12 h day-night cycle under standard laboratory conditions with controlled temperature (20–24 °C) and humidity (30–60%). Food and water were available ad libitum. Mice were habituated to the housing facility for at least 1 week and to handling procedures on at least three consecutive days before starting the experiments. The experiments were performed between 9 a.m. and 5 p.m.. All procedures were in strict compliance with the animal use and care guidelines of Montpellier University (authorization A34-518/A34-172-13) and the guidelines of the Ethical Committee for Animal Experiments of the Vrije Universiteit Brussel (ECD 17-213-3 and 21-213-10).
Drugs and administration
Stock solutions of the 5-HT2A/5-HT2C agonist 2,5-Dimethoxy-4-iodoamphetamine hydrochloride (DOI, Tocris Bioscience) and the 5-HT2A receptor antagonist (R)-(+)-alpha-(2,3-Dimethoxyphenyl)-1-[2-(4-fluorophenyl)ethyl]-4-piperinemethanol (M100907, Tocris Bioscience) were prepared in 99.9% dimethylsulfoxide (DMSO; Sigma-Aldrich Chemicals) and stored at −20 °C. Working solutions were freshly prepared by diluting the stock solutions in sterile saline (0.9% NaCl, Baxter). We based these doses on previous studies showing robust effects on 5-HT2A receptors in mice [38, 39]. For intraperitoneal (i.p.) administration, DOI was diluted to a dose of 2 mg/kg for an injection volume of 10 ml/kg. The working solution contained 5% v/v DMSO in sterile saline and control mice received the same volume of 5% v/v DMSO in sterile saline. I.p. injections were carried out 30 min before the start of behavioral experiments. For targeted intracranial (i.c.) administrations, working solutions were prepared by diluting a stock solution to a final dose of 2.5 μg per site for DOI and 0.3 μg per site for M100907. Working solutions were adjusted to pH 5.5–6.5 and contained 20% DMSO. Control mice were injected with the same volume of 20% DMSO in sterile saline. Infusion needles (33G, PlasticsOne) with 0.5 mm protrusion (medial prefrontal cortex, mPFC) or 1 mm protrusion (amygdala) were inserted into each guide cannulae for i.c. administration. DOI and the corresponding vehicle (Veh) were infused at a flow rate of 0.5 μl/min for 1 min. M100907 and the corresponding Veh were infused at a flow rate of 1 μl/min for 1 min. The injector was left in the cannulae for 1 min after infusion to allow for diffusion of the compounds and to avoid back-flow. I.c. infusions were carried out 30 min before behavioral interventions and immediately prior to systemic administrations when relevant.
Stereotactic surgery
Cannula implantations were carried out as previously described [40]. Briefly, stainless steel guide cannulae (26 gauge, Plastics One) were implanted bilaterally above the medial prefrontal cortex (mPFC, coordinates: 2.00 mm anterior, 0.40 mm lateral, 2.00 mm ventral from bregma) or amygdala (coordinates: 1.80 mm posterior, 3.40 mm lateral, 3.90 mm ventral from bregma). Correct cannula placement was evaluated post-mortem, using a dissecting microscope and anatomical reference atlas [41]. Animals with misplaced or blocked cannulae were excluded from analysis.
Y-maze spontaneous alternation
The apparatus consisted of three enclosed arms (L × W × H: 30 × 6 × 15 cm). No intramaze cues were provided while extramaze cues were placed in the room. Mice were placed in a random arm of the maze and explored it for 5 min with all three arms open. Trials were recorded using an overhead camera and video files were scored manually by an observer blinded to treatment. The percentage alternation (i.e., the number of alternations divided by the total possible alternations and multiplied by 100) was used as a measure of spatial working memory and executive function [42, 43]. One alternation was counted when mice visited the three different arms consecutively. Immediate re-entries were discounted.
Elevated zero maze
We used a circle-shaped maze (Diameter: 100 cm) divided into four distinct areas and elevated to a height of 50 cm above the floor. These quadrants are two opened and two closed areas facing each other respectively without any intermediate space between each area. Mice were placed in the center of one of the open sections to freely explore the maze for a total duration of 5 min. Trials were recorded using an overhead camera and the exploration behavior of each mouse was scored by an observer blinded to treatment.
Elevated plus maze
The apparatus consisted of a plus-shaped maze with two opposite open (L × W: 23.5 × 8 cm) and enclosed arms (L × W × H: 23.5 × 8 × 20 cm high). The arms extended from a central platform (L × W: 8 × 8 cm) and the maze was elevated to a height of 50 cm above the floor. Each mouse was placed at the center of the maze and could freely explore it for a total duration of 10 min. Trials were recorded using an overhead camera and the behavior of mice was scored by an observer blinded to treatment. The time spent in open arms and the number of entries in both arms were recorded manually and expressed as a percentage of total time spent and total entries. Propensity of mice to explore the open arms was used as a measure of anxiety-like avoidance behavior.
Circular corridor
Horizontal and vertical activity were measured in a circular corridor (Imetronic, Pessac, France). Counts for horizontal activity were incremented by consecutive interruption of two adjacent beams placed at a height of 1 cm per 90° sector of the corridor (mice moving through one-quarter of the circular corridor) and counts for vertical activity (rearing) corresponding to interruption of beams placed at a height of 7.5 cm along the corridor (mice stretching upwards) were used as an additional measure for exploratory activity. Mice were habituated to handling and to the test apparatus before on three consecutive days before the actual experiment. In this habituation procedure mice were injected with saline (0.9% NaCl) 30 min before being placed in the activity box for a duration of 60 min. On the test day, mice were placed in the activity box 30 min after treatment with Veh or DOI and their activity was monitored for 10 min.
Passive avoidance
The procedure comprised training, short-term memory (STM) performed 60 min after the training, and long-term memory (LTM) performed 24 h after training. Mice were placed in a dark room for 30–180 min before the start of the experiments. The training sessions began by placing the mice in a brightly lit (700 lux) corridor (L × W × H: 50 × 10 × 40 cm Plexiglas walls), separated from a dark chamber (L × W × H: 10 × 10 × 40 cm) by a guillotine door. When mice entered the dark chamber, the door was shut followed by foot-shock (2 s, 0.6 mA) delivery. Training ended immediately after foot-shock delivery. STM and LTM lasted 5 min. STM and LTM sessions were identical to the training session, but no foot-shock was given in these trials. Latency to chamber entry was recorded for all mice. Additionally, the light corridor was divided into four areas (L1–L4) based on their distance from the dark chamber (L1: closest, L4: furthest). Mice began each session in the area of the corridor placed the furthest from the chamber (L4). Latency to explore, time spent in each area and freezing were quantified. Freezing time was expressed as a percentage of the total trial duration. An overhead camera recorded all trials and behavior was analyzed using an automated video monitoring system (Ethovision XT, Noldus).
Auditory fear conditioning
Auditory fear conditioning followed a previously described protocol with minor modifications [44]. Different context configurations were used for fear conditioning (context A: metal grid on black floor, gray walls, cleaned with 1% acetic acid between trials) and for fear extinction, extinction recall or fear recall tests (context B: white rubber floor, checkerboard-pattern walls, cleaned with 3% hospital antiseptic concentrate between trials). Each session began with 2 min habituation (Hab) to the context and ended with 1 min cool down. During conditioning, mice received 3 (moderate conditioning) or 5 (strong conditioning) pairings (60 s inter-stimulus interval: ITI) of the conditional stimulus (CS, 4 kHz, 80 dB, 30 s tone) co-terminating with a 0.6 mA (moderate conditioning) or 1.0 mA (strong conditioning) unconditional stimulus (US, 2 s, scrambled footshock). Fear extinction followed one day after conditioning and consisted of 40 CS presentations (5 s ITI) in context B. Extinction control mice were treated identically but were placed in a novel open field (30 × 30 × 30 cm Plexiglas walls) instead of context B and were not exposed to CS presentations. Efficacy of extinction was examined by exposing the animals to four CS presentations (60 s ITI) in context B, either one day after extinction training (early extinction recall) or 3 weeks after extinction training (late extinction recall). In experiments without fear extinction, fear recall was tested 1 day after fear conditioning by two CS presentations (60 s ITI). Freezing behavior was defined as a lack of detectable movements other than breathing for 1 s or more and was scored with an automated video monitoring system (Ethovision XT, Noldus: Figs. 1E–G, 2D, 3B, 4C, E) or load-cell coupler detection system (Freezing, Panlab: Figs. 2B, C, Fig. 4). We expressed freezing behavior as the percentage of time mice spent freezing relative to the total amount of time of Hab or CS presentation. Freezing behavior during Hab and ITI was not included in the statistical analysis but freezing during Hab was plotted for reference.
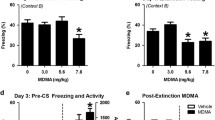
A Effect of DOI (nVeh = 13, nDOI = 10) on the number of alternations (p = 0.4528) and count of arm entries (p = 0.0146) in the Y-maze spontaneous alternation test. B Effect of DOI (nVeh = 11, nDOI = 11) on performance in the elevated zero maze: percentage of time spent in open zones (p = 0.0023) and count of zone entries (open zones: p < 0.0001; closed zones: p < 0.0001). C Effect of DOI (nVeh = 9, nDOI = 8) on performance in elevated plus maze: percentage of time spent in open arms (p = 0.0054) and count of arm entries (open arms: p = 0.0046; closed arms: p = 0.1501). D Effect of DOI (nVeh = 9, nDOI = 10) on activity of mice in the circular corridor apparatus: vertical activity (treatment: p = 0.4690; time: p = 0.5593; interaction: p = 0.8317), horizontal activity (treatment: p = 0.8823; time: p = 0.2521; interaction: p = 0.6075). E Schematic representation of the experimental design for passive avoidance testing in a light corridor and dark chamber setup. Areas of the light compartment were designated L1-L4 from closest to furthest away from the dark compartment. F Following training, none of the mice (nVeh = 17, nDOI = 16) entered the dark chamber. G Effect of DOI on freezing during the long-term memory test (p = 0.0001). H Effect of DOI on latency to enter areas of the brightly-lit corridor (treatment effect: p = 0.0571, area effect: p = 0.001; interaction: p = 0.0034). I Effect of DOI on time spent in areas of the brightly-lit corridor (treatment effect: p = 0.6559; area effect: p < 0.0001, interaction: p < 0.0001). Data are presented as mean values ± SEM (*p < 0.05; #p < 0.05; ##p < 0.01; ####p < 0.0001 vs. Veh group).
A Schematic representation of the experimental design for testing the effect of DOI on auditory fear extinction. B Effect of DOI on fear extinction following moderate conditioning in wild type mice (nVeh = 12, nDOI = 7). Fear conditioning: (CS effect: p < 0.0001; treatment effect: p = 0.5088; interaction: p = 0.8382). Fear extinction (CS effect: p = 0.0045; treatment effect: p = 0.0002; interaction: p = 0.3472). Early extinction recall (p = 0.7858). C Effect of DOI on fear extinction following moderate conditioning in 5-HT2A receptor KO mice (nVeh = 10, nDOI = 7). Fear conditioning (CS effect: p < 0.0001; treatment effect: p = 0.5650; interaction: p = 0.7400). Fear extinction: (CS effect: p < 0.0001; treatment effect: p = 0.3236; interaction: p = 0.0652). Early extinction recall (p = 0.7559). D Effect of treatment with Veh (V) or DOI (D) on fear extinction following strong conditioning in wild type mice (nVeh- = 13, nDOI- = 13, nVeh+ = 13, nDOI+ = 14). Fear conditioning (CS effect: p < 0.0001; group effect: p = 0.9984; interaction p = 0.9879). Fear extinction (CS effect: p < 0.0001; treatment effect: p < 0.0001; interaction: p < 0.0001). Early extinction recall (extinction effect: p = 0.0023; treatment effect: p = 0.8157; interaction: p = 0.2308). Late extinction recall (extinction effect: p = 0.5438; treatment effect: p = 0.3645; interaction: p = 0.4390). Data are presented as mean values ± SEM (*p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001 vs. Veh group).
A. Schematic representation of the experimental design for investigating the effect of DOI on c-Fos expression in mice subjected to fear conditioning. Regions examined: prelimbic (PL) and infralimbic (IL) cortices of the medial prefrontal cortex; lateral (LA), basolateral (BLA), lateral (CeL) and medial (CeM) division of the central amygdala. B Effect of DOI on freezing during fear memory recall (nVeh = nDOI = 7; p = 0.0001). C Effect of DOI on c-Fos expression during fear memory recall (treatment effect: p = 0.0017; region effect: p < 0.0001; interaction: p < 0.0001). D Effect of DOI on c-Fos expression in PV+ interneurons during fear memory recall (treatment effect: p = 0.2710; region effect: p < 0.0001; interaction: p = 0.006). PV+ neuron count (treatment effect: p = 0.1396; region effect: p < 0.0001; interaction: p = 0.2345). E Representative confocal microscopy images labeled for c-Fos (red) and PV (cyan). Scale bar = 200 μm. Data are presented as mean values ± SEM (*p < 0.05; **p < 0.01; ###p < 0.001. vs Veh group).
A Schematic representation of the experimental design used to investigate how 5-HT2A receptors expressed in discrete brain regions control freezing behavior during fear memory recall. B Cannula placement sites for infusion of M100907 (black) or the corresponding Veh (white) in the mPFC. C Modulation of freezing during fear memory recall by systemic DOI (2 mg/kg i.p.) and local infusion of M100907 (0.3 μg per injection site) or the corresponding Veh (nVeh = nDOI = 5; p = 0.4209). D Cannula placement sites for infusion of M100907 (black) or the corresponding Veh (white) in the amygdala. E Modulation of freezing during fear memory recall by systemic DOI (2 mg/kg i.p.) and local infusion of M100907 (0.3 μg per injection site) or the corresponding Veh into amygdala (nVeh/DOI = 6; nM100907/DOI = 4; p = 0.0216). F Cannula placement sites for infusion of DOI (black) or the corresponding Veh (white) in the amygdala. G Modulation of freezing during fear memory recall by local infusion of DOI (2.5 μg per injection site) or the corresponding Veh into the amygdala (nVeh = 6; nDOI = 4; p = 0.0003). Data are presented as mean values ± SEM (##p < 0.01, ###p < 0.001 vs Veh group).
Immunofluorescence and confocal microscopy
Tissue processing and image acquisition were carried out as previously described [45]. In brief, mice were anesthetized with sodium pentobarbital i.p. (200 mg/ml) and transcardially perfused with phosphate-buffered saline (PBS, Sigma-Aldrich) and ice-cold 4% paraformaldehyde (PFA, VWR Chemicals), 90 min after the behavioral procedure. 40 μm thick slices were prepared on a vibratome (Leica VT1000S, Leica Biosystems) and stored in anti-freeze solution (TBS solution (50 mM Tris, pH 7.6, Sigma-Aldrich, Germany) containing 30% glycerol (Millipore, Merck, Germany) and 30% ethylene glycol (VWR Chemicals, Belgium)) at −20 °C until further processing. Slices were rinsed and incubated with primary rabbit anti-c-Fos (1:500; #2250, Cell Signaling), mouse anti-parvalbumin (1:1000; #PV235, Swant) or rabbit anti-5-HT2A antibodies (1:100; #24288 ImmunoStar Inc.) followed by rinsing and incubation with secondary antibodies (Jackson ImmunoResearch Laboratories) as outlined in the Supplementary Methods. Confocal microscope images (Zeiss, Axio Observer with LSM 710-6NLO configuration, Zeiss International) were processed and analyzed with ImageJ software (v. 1.53b). Prefrontal cortex (coordinates: +2.0 mm anterior-posterior) and amygdala nuclei (−1.8 mm anterior-posterior) were manually marked after applying an automatic Li threshold algorithm using the channel corresponding to parvalbumin (PV) [41, 46]. Expression of c-Fos was analyzed using the Find Maxima ImageJ plugin, after preprocessing the images with a median filter [46, 47]. Cells expressing PV were counted manually. For quantitative image analysis, each data point corresponds to the mean result of 2–4 images per region per mouse.
Statistical analysis
Data were expressed as mean values ± SEM. Statistical analysis was performed using Graphpad Prism (v. 9.1.1). Threshold for statistical significance was set at alpha = 0.05. Data were analyzed by unpaired two-tailed t tests (with Welsch’s correction if the compared datasets had significantly different variations), or by two-way ANOVA, for independent and repeated measures (with Greenhouse-Geisser correction for interpretation of within-group effects [48] and Bonferroni adjustment for post-hoc analysis) as appropriate. The complete results of the statistical analysis can be found in the Supplementary Tables 1–7.
Results
DOI does not impair exploratory behavior and aversive memory recall but suppresses innate and conditioned anxiety-like avoidance behavior
We selected a dose of DOI (2 mg/kg i.p.) that was previously shown to induce a robust 5-HT2A-dependent head-twitch response in C57BL/6J mice [49]. DOI had no significant effect on spontaneous alternation (Fig. 1A, Supplementary Table 1; t(21) = 0.77, p = 0.4528), demonstrating intact executive performance, but increased exploratory activity in the Y-maze (Fig. 1A, Supplementary Table 1; t(21) = 2.27, p = 0.0146). In the elevated zero maze, DOI significantly increased the time spent in the open zones (t(20) = 6.01, p < 0.0001) and the overall number of zone entries (t(20) = 6.02, p < 0.0001). The configuration of elevated zero maze implies that an overall increase in activity results in an equivalent increase in open zone and closed zone entries (Fig. 1B; Supplementary Table 1; open zone: t(20) = 6.01, p < 0.0001; closed zone: t(20) = 5.99, p < 0.0001). In the elevated plus maze task, DOI increased open arm entries (Fig. 1C; Supplementary Table 1; t(15) = 3.33, p = 0.0046) and time spent in the open arms (Fig. 1C, Supplementary Table 1; t(15) = 3.25, p = 0.0054). Moreover, we observed no significant effect of DOI on the number of closed arm entries (Fig. 1C, Supplementary Table 1; t(15) = 1.52, p = 0.1501). We further investigated whether the observed increase in exploratory activity was the result of a psychostimulant-like hyperlocomotor effect. When mice were thoroughly habituated to a circular corridor, an experimental setup in which psychostimulants induce a clear hyperlocomotor response [50, 51], DOI had no significant effect on locomotor activity (Fig. 1D, Supplementary Table 1; treatment: F(1, 18) = 0.001, p = 0.97). This suggests that the effects of DOI on exploratory behavior are dependent on novelty and anxiogenic properties of the testing environment.
Importantly, in 5-HT2A KO mice, DOI did not affect spontaneous alternation or exploratory activity in the Y-maze and had no significant effect on anxiety-like behavior or exploratory activity in the elevated plus maze (Supplementary Fig. 1, Supplementary Table 1). In the passive avoidance task, mice were placed in a brightly lit corridor and trained to avoid an adjacent dark chamber (Fig. 1E). During the short-term memory test (STM), one hour after training, none of the mice entered the dark chamber (Fig. 1F). There were no significant differences between experimental groups in freezing behavior (Supplementary Table 1; t(31) = 0.68, p = 0.4992), the amount of time spent in different areas of the corridor (Supplementary Table 2; treatment: F(1, 31) = 1.436, p = 0.2685) or the latency to explore the areas closer to the chamber (Supplementary Table 2; treatment: F(1, 31) = 0.5855, p = 0.4500). This demonstrates effective randomization of mice. One day later, mice were injected with Veh or DOI and subjected to a long-term memory test (LTM). During LTM, none of the mice entered the dark chamber (Fig. 1F), demonstrating intact aversive memory recall. Interestingly, DOI significantly lowered freezing (Fig. 1G, Supplementary Table 1; t(20.19) = 5.20, p < 0.0001), decreased the latency to explore areas of the corridor closest to the dark chamber (Fig. 1H, Supplementary Table 2; treatment: F(1, 31) = 3.91, p = 0.0571, area: F(1.314, 40,73) = 14.08, p = 0.001, interaction: F(2, 62) = 6.22, p = 0.0034) and decreased time in the area furthest away from the dark chamber (Fig. 1I, Supplementary Table 2; treatment: F(1, 31) = 0.20, p = 0.6559, area: F(1.171, 36.29) = 416.4, p < 0.0001, interaction: F(3, 93) = 7.94, p < 0.0001). This shows that DOI decreases innate and conditioned anxiety-like avoidance behavior, while it does not disrupt aversive memory recall.
DOI suppresses conditioned freezing through activation of 5-HT2A receptors
We next investigated the effects of DOI (2 mg/kg i.p.) in an auditory fear conditioning paradigm. Following conditioning (day 1), mice were subjected to fear extinction training (day 2) and an early (day 30) and late (day 29) extinction recall test (Fig. 2A). Effective randomization was demonstrated by the lack of significant group differences during conditioning on the first day (Fig. 2, Supplementary Table 3). Mice received treatment before extinction training on day 2. In mice that underwent moderate conditioning (3 CS-US pairings at 0.6 mA), the administration of DOI before extinction training significantly reduced conditioned freezing in wild type mice (Fig. 2B, Supplementary Tables 3 and 4; treatment: F(1, 17) = 23.37, p = 0.0002) but not in 5-HT2A KO mice (Fig. 2C, Supplementary Tables 3 and 4; treatment: F(1, 16) = 1.037, p = 0.3236). During early extinction recall (day 3) we observed no significant treatment effect in wild type (Fig. 2B, Supplementary Table 3; t(17) = 0.28, p = 0.7858) or 5-HT2A receptor KO mice (Fig. 2C, Supplementary Table 3; t(16) = 0.32, p = 0.7559). This demonstrates that DOI had no significant effect on the extinction learning process. Given that potential beneficial effects of DOI on the retention of fear extinction may have been diminished by a floor effect, we carried out an additional experiment with strong conditioning (5 CS-US pairings at 1 mA), followed by an early extinction retrieval test one day after extinction training and a late extinction retrieval test 3 weeks after extinction training. In this experiment we included additional control groups of mice that that were treated identically but were placed in a novel open field without cue exposure following treatment rather than undergoing extinction training. The extinction training significantly reduced freezing in control mice during early extinction recall (Fig. 2D, Supplementary Table 3; extinction effect F(1, 51) = 10.35, p = 0.0023), but not during late extinction recall (Fig. 2D, Supplementary Table 3; extinction effect F(1, 51) = 0.3735, p = 0.5438). This demonstrates that while extinction training reduced cued fear expression one day later, this effect of extinction training was lost 3 weeks later. DOI significantly suppressed freezing during extinction training (Fig. 2D, Supplementary Tables 3 and 4; treatment: F(1, 27) = 49.29, p < 0.0001). In extinction control mice that were placed in an open field, we observed a significant effect of DOI on exploratory activity, measured by traveled distance (Supplementary Fig. 2, Supplementary Table 3; treatment effect: F(1, 24) = 15.89, p = 0.0005). We found no significant differences, between mice treated with DOI and their respective Veh controls during the early (Fig. 2D, Supplementary Table 3; treatment effect: F(1, 51) = 0.05487, p = 0.8157) or late (Fig. 2D, Supplementary Table 3, treatment effect: F(1, 51) = 0.8373, p = 0.3645) extinction recall sessions. Taken together, our data demonstrate that DOI does not affect the retention of auditory fear extinction.
DOI increases c-Fos expression in the amygdala upon auditory fear memory recall
To identify potential brain regions involved in the observed effects on fear expression, we administered DOI (2 mg/kg i.p.) or Veh before fear recall (Fig. 3A) and sacrificed mice 90 min later for analysis of c-Fos expression used as a proxy for neuronal activity [52]. We focused our analysis on brain regions expressing 5-HT2A receptors (Supplementary Fig. 3) and involved in auditory fear conditioning [53], namely the prelimbic and infralimbic subregions of the mPFC and the lateral amygdala (LA), basolateral amygdala, lateral (CeL) and medial (CeM) division of the central amygdala. As expected, DOI suppressed conditioned freezing (Fig. 3B, Supplementary Table 5; t(12) = 5.46, p = 0.0001). DOI also induced an overall increase in c-Fos expression (Fig. 3C, Supplementary Table 5; treatment: F(1, 12) = 16.28, p = 0.0017) and post-hoc analysis (Supplementary Table 6) revealed a significant increase in the LA (Fig. 3C; t(9.747) = 4.89; p = 0.0041) and CeL (Fig. 3C; t(7.735) = 3.70; p = 0.0383). Activation of 5-HT2A receptors was previously reported to increase firing of PV interneurons in the amygdala, suggesting a potential mechanism through which 5-HT2A receptor activation may suppress fear expression [54, 55]. Further analysis (Supplementary Tables 5 and 6) showed that the number of PV+ per mm2 was dependent on the examined region (F(2.436, 29.55) = 37.01, p < 0.0001) while no significant treatment or interaction was noted. Analysis of c-Fos expression in PV+ interneurons (Fig. 3D, Supplementary Tables 5 and 6) showed no significant treatment effect (F(1, 12) = 1.33, p = 0.2710), but significant regional differences (F(2.314, 27.77) = 25.79, p < 0.0001) and a significant treatment by region interaction (F(3, 36) = 4.88, p = 0.0060). This suggests that DOI may increase c-Fos expression in PV+ interneurons in some brain regions, but this was not confirmed in post-hoc analysis (Supplementary Table 6) given the low number of co-labeled cells (Fig. 3D, E). When DOI was administered to naive mice or to mice that were previously subjected to fear conditioning but that did not undergo auditory fear memory recall, a similar pattern of c-Fos expression was observed (Supplementary Fig. 4; Supplementary Table 5). Interestingly, in these experiments where mice did not show fear expression, DOI-induced changes in c-Fos expression in the CeL did not reach statistical significance (Supplementary Fig. 4; Supplementary Table 6).
5-HT2A receptors in the amygdala drive the effect of DOI on conditioned freezing
To further investigate the neuroanatomical substrate for the observed effect of DOI on conditioned freezing, we carried out an experiment where we administered DOI (2 mg/kg i.p.) systemically and the selective 5-HT2A receptor antagonist M100907 (0.3 μg per injection site) [54] or Veh locally either in the mPFC or the amygdala 30 min before fear recall (Fig. 4, Supplementary Fig. 5, Supplementary Table 7). Low freezing following DOI administration was not significantly affected when M100907 was infused into the mPFC (Fig. 4B, C; t(8) = 0.85, p = 0.4209) but was reversed when M100907 was delivered into the amygdala (Fig. 4D, E; t(4.030) = 3.40, p = 0.0216). Finally, we demonstrate that local infusion (Fig. 4F) of DOI (2.5 μg per injection site) into the amygdala 30 min before fear recall significantly suppressed freezing (Fig. 4G; t(18) = 4.47, p = 0.0003).
Discussion
We found that the psychedelic 5-HT2A/5-HT2C receptor agonist DOI decreased anxiety-like avoidance behaviour in the elevated plus maze and conditioned passive avoidance tasks. In addition, DOI suppressed conditioned freezing during extinction training without significant effects on the retention of extinction. The effect of DOI on conditioned freezing was mediated by activation of 5-HT2A receptors in the amygdala.
We found no evidence for impaired execution of the spontaneous alternation task following the administration of DOI at the selected dose. While other studies have found effects of DOI on executive functions in a similar task in rats [56, 57] and on spontaneous alternation in mice [58], these effects appear to be dependent on serotoninergic tone and activation of 5-HT2C receptors by the high DOI doses [58]. Consistent with this notion, the selective 5-HT2A receptor agonist 25CN-NBOH did not affect spontaneous alternation in mice but restored deficits induced by the 5-HT1A receptor agonist 8-OH-DPAT [58]. Similarly, spontaneous alternation impairments induced by the non-selective 5-HT receptor agonist meta-chlorophenylpiperazine (mCPP) were reversed by the 5-HT2C receptor antagonist SB242084 but not by the 5-HT2A receptor antagonist M100907 in rats [59].
We found a significant increase in Y-maze exploration, confirming previous observations [58]. We also found a significant increase in activity in the elevated plus maze and zero maze tasks. While DOI decreases open field exploration in rats [60,61,62,63] it appears to have dose-dependent effects in mice, with lower doses (up to 1 mg/kg) increasing exploration through activation of 5-HT2A receptors and higher doses (from 10 mg/kg) decreasing exploration through 5-HT2C receptors [64]. In previously conditioned mice, we also observed a significant increase in open field exploration after administration of DOI. In contrast, we found no significant effect of DOI on locomotor activity in mice that were extensively habituated to a circular corridor. We, therefore, propose that the observed increase in activity reflects decreased anxiety and increased novelty-dependent exploratory drive rather than a psychostimulant-like hyperlocomotor effect. Indeed, we found that DOI administration selectively increased the fraction of time mice spent in the open arms of the elevated plus maze or in the open sections of the elevated zero maze. This indicates an anxiolytic effect. Our observations are in agreement with previous literature showing that DOI decreases anxiety-like avoidance behavior in naive mice and rats [65, 66]. These effects are dose-dependent, with 5-HT2A receptor-dependent anxiolytic effects for lower doses of DOI and potential 5-HT2C-dependent anxiogenic effects for higher doses of DOI [65]. In contrast with these anxiolytic effects of DOI in the elevated plus maze and in other behavioral tests [67], psychostimulants such as amphetamine increase locomotor activity in the open field test but reduce open arm entries and exploration in the elevated plus maze test [68,69,70].
The notion that DOI reduces anxiety-like avoidance behavior was further confirmed in the passive avoidance task. Surprisingly, we found that DOI had no effect on aversive memory retention, given that none of the mice entered the compartment where they previously received a shock. Nevertheless, DOI significantly increased exploratory behavior and suppressed conditioned freezing. In the auditory fear conditioning paradigm, we also found that DOI suppressed conditioned freezing. While a previous study suggested that stimulation of 5-HT2A receptors may facilitate the acquisition auditory fear extinction, retention of extinction was not investigated [37]. Contrary to our initial hypothesis, we found no significant effect on the retention of fear extinction at early or late time points. Importantly, activation of 5-HT2A receptors in the amygdala is necessary and sufficient to recapitulate the effects of systemic administration of DOI on conditioned freezing behavior. The fact that nuclei of the amygdala are well established neural hubs orchestrating aversive behaviors such as freezing [71], further supports the notion that the effect of DOI on conditioned freezing reflects suppression of fear expression rather than a non-specific hyper-locomotor effect. Taken together, our findings indicate that 5-HT2A activation by the psychedelic DOI suppressed fear expression without significant effects on the retention of fear extinction.
Systemic administration of DOI in naive mice elicits an increase in c-Fos expression in diverse brain regions including the mPFC and the amygdala. While this effect may also occur in cells and brain regions that do not express the 5-HT2A receptor [72, 73], the c-Fos expression pattern was largely congruent with that of the widely distributed 5-HT2A receptor (Supplementary Fig. 3). In mice that were subjected to fear conditioning, the administration of DOI prior to fear memory recall only significantly increased c-Fos expression in the LA and CeL. We propose that 5-HT2A receptors in the LA may be a critical target through which psychedelics affect fear expression. Indeed, local antagonism of 5-HT2A receptors in the amygdala reversed the effect of systemic DOI administration on fear expression. Corroborating this observation, direct infusion of DOI into the amygdala similarly suppressed fear expression. Given that we observed no 5-HT2A expression in the CeL, changes in c-Fos expression in this brain area may indeed reflect altered fear expression following administration of DOI rather than a direct effect of DOI on cells in the CeL. Interestingly, a previous study found that reduced 5-HT2A receptor signaling in PV interneurons in the amygdala may drive stress-induced changes in GABAergic transmission and behavior [55]. However, we found no significant effects of DOI on c-Fos expression in PV interneurons. This may be due to the low number of PV interneurons in the amygdala and relatively small group sizes. Further experiments, in which the effects of DOI on c-Fos expression in discrete neuronal populations are compared directly between mice that express fear and mice that do not, may further help to unravel the cellular basis for the effects of DOI on fear expression. Importantly, 5-HT2A receptors expressed in other brain regions, such as the ventral hippocampus or periaqueductal gray matter may contribute to the anxiolytic effects of DOI [74, 75], while direct activation of 5-HT2A receptors in the BNST was recently reported to increase conditioned freezing behavior [76]. This suggests that activation of 5-HT2A receptors in different brain areas may have different effects on defensive behaviors. Moreover, the effects of psychedelics may depend on the activity state of 5-HT2A receptors in discrete brain areas. Nevertheless, in agreement with our findings, the psychedelic 5-HT2A/5-HT2C receptor agonists TCB-2, 2CN-NBOH, and psilocybin were all shown to reduce conditioned freezing when administered systemically in mice [34, 35].
To the best of our knowledge, no formal clinical trials have presently investigated classic psychedelics in PTSD. However, psilocybin and LSD showed promising effects in cancer-related depression and anxiety [77,78,79,80,81]. Interestingly, psilocybin reduced threat-induced modulation of amygdala connectivity in healthy volunteers [82]. Similarly, LSD suppressed amygdala reactivity to fearful stimuli [78] and impaired fear recognition in healthy volunteers [83]. This suggests that classic psychedelics affect fear processing and may be useful for treating fear-related disorders such as PTSD. Few studies have directly investigated the role of 5-HT2A receptors in the putative effects of psychedelics on fear extinction. Recently, DMT, a psychedelic 5-HT2A/5-HT1A agonist, was shown to facilitate auditory fear extinction in rats [36]. However, 5-HT1A receptors may have contributed to this effect of DMT given that 5-HT1A receptor activation was previously shown to reduce auditory fear expression and to facilitate fear extinction in rodents [84,85,86,87]. Interestingly, activation of 5-HT2A receptors may induce delayed improvement in the acquisition of contextual fear extinction through long-term epigenetic and synaptic plasticity [88]. Together, this suggests that 5-HT2A receptors are a key target for the acute effects of psychedelics on fear expression, but other receptors or delayed mechanisms may contribute to effects of psychedelics on fear extinction.
It was recently proposed that the clinical effect of MDMA-assisted psychotherapy for PTSD treatment may result from reduction of fear during fearful memories [15, 17, 18] or from enhanced extinction of fearful memories [20]. In line with this notion, MDMA was reported to suppress freezing during extinction training and to improve retention of fear extinction in mice [21, 22]. However, a recent study showed that while MDMA suppressed fear expression during extinction training, it interfered with the retention of extinction in rats [24]. Therefore, it remains unclear whether facilitation of extinction is the underlying mechanism of MDMA-assisted psychotherapy [20]. Moreover, it remains uncertain whether the psychedelic properties of MDMA are required for its therapeutic effects. While MDMA is not a classic psychedelic, many of its psychotropic effects involve 5-HT release and activation of 5-HT2A receptors [33, 89,90,91,92,93]. In this context, activation of 5-HT2A receptors may indeed be a mechanism through which MDMA modulates fear processing [23], consistent with our data demonstrating that direct 5-HT2A receptor activation by a psychedelic suppresses fear expression.
We conclude that the psychedelic DOI suppresses fear expression in mice through activation of amygdala 5-HT2A receptors while it has no significant effect on the retention of extinction. Our study is limited to a single administration of DOI, but it provides insight into the mechanism through which acute psychedelic effects may yield therapeutic outcomes for psychedelic-assisted psychotherapy. Indeed, if psychedelics suppress fear expression without impairing recall and extinction of fearful memories, this may enable psychotherapy in patients for whom the experience would otherwise be too aversive as described by a PTSD patient who underwent MDMA-assisted psychotherapy: “It allowed me to see my trauma without fear or hesitation and finally process things and move forward” [20].
References
Battle DE. Diagnostic and statistical manual of mental disorders (DSM). Codas. 2013;25:191–2.
Shalev A, Liberzon I, Marmar C. Post-traumatic stress disorder. N Engl J Med. 2017;376:2459–69.
Maria M, Steenkamp P. Psychotherapy for military-Related PTSD: a review of randomized clinical trials. JAMA. 2015;314:489–500.
Lee DJ, Schnitzlein CW, Wolf JP, Vythilingam M, Rasmusson AM, Hoge CW. Psychotherapy versus pharmacotherapy for posttraumatic stress disorder: systemic review and meta-analyses to determine first-line treatments. Depress Anxiety. 2016;33:792–806.
Hoskins M, Pearce J, Bethell A, Dankova L, Barbui C, Tol WA, et al. Pharmacotherapy for post-traumatic stress disorder: Systematic review and meta-analysis. Br J Psychiatry. 2015;206:93–100.
Bradley R, Greene J, Russ E, Dutra L, Westen D. A multidimensional meta-analysis of psychotherapy for PTSD. Am J Psychiatry. 2005;162:214–27.
Cipriani A, Williams T, Nikolakopoulou A, Salanti G, Chaimani A, Ipser J, et al. Comparative efficacy and acceptability of pharmacological treatments for post-traumatic stress disorder in adults: a network meta-analysis. Psychol Med. 2018;48:1975–84.
Milad MR, Quirk GJ. Fear extinction as a model for translational neuroscience: ten years of progress. Annu Rev Psychol. 2012;63:129.
Singewald N, Schmuckermair C, Whittle N, Holmes A, Ressler KJ. Pharmacology of cognitive enhancers for exposure-based therapy of fear, anxiety and trauma-related disorders. Pharm Ther. 2015;149:150–90.
Sartori SB, Singewald N. Novel pharmacological targets in drug development for the treatment of anxiety and anxiety-related disorders. Pharm Ther. 2019;204:107402.
Sessa B. Turn on and tune in to evidence-based psychedelic research. Lancet Psychiatry. 2015;2:10–2.
Mithoefer MC, Grob CS, Brewerton TD. Novel psychopharmacological therapies for psychiatric disorders: psilocybin and MDMA. Lancet. Psychiatry. 2016;3:481–8.
Kyzar EJ, Nichols CD, Gainetdinov RR, Nichols DE, Kalueff AV. Psychedelic drugs in biomedicine. Trends Pharm Sci. 2017;38:992–1005.
Reiff CM, Richman EE, Nemeroff CB, Carpenter LL, Widge AS, Rodriguez CI, et al. Psychedelics and psychedelic-assisted psychotherapy. Am J Psychiatry. 2020;177:391–410.
Krediet E, Bostoen T, Breeksema J, van Schagen A, Passie T, Vermetten E. Reviewing the potential of psychedelics for the treatment of PTSD. Int J Neuropsychopharmacol. 2020;23:385–400.
Feduccia AA, Jerome L, Yazar-Klosinski B, Emerson A, Mithoefer MC, Doblin R. Breakthrough for trauma treatment: safety and efficacy of MDMA-assisted psychotherapy compared to paroxetine and sertraline. Front Psychiatry. 2019;10:650.
Mitchell JM, Bogenschutz M, Lilienstein A, Harrison C, Kleiman S, Parker-Guilbert K, et al. MDMA-assisted therapy for severe PTSD: a randomized, double-blind, placebo-controlled phase 3 study. Nat Med. 2021;27:1025–33.
Liechti ME, Baumann C, Gamma A, Vollenweider FX. Acute psychological effects of 3,4-methylenedioxymethamphetamine (MDMA, “Ecstasy”) are attenuated by the serotonin uptake inhibitor citalopram. Neuropsychopharmacology. 2000;22:513–21.
Mithoefer MC, Mithoefer AT, Feduccia AA, Jerome L, Wagner M, Wymer J, et al. 3,4-methylenedioxymethamphetamine (MDMA)-assisted psychotherapy for post-traumatic stress disorder in military veterans, firefighters, and police officers: a randomised, double-blind, dose-response, phase 2 clinical trial. Lancet Psychiatry. 2018;5:486–97.
Feduccia AA, Mithoefer MC. MDMA-assisted psychotherapy for PTSD: are memory reconsolidation and fear extinction underlying mechanisms? Prog Neuro-Psychopharmacol Biol Psychiatry. 2018;84:221–8.
Young MB, Andero R, Ressler KJ, Howell LL. 3,4-Methylenedioxymethamphetamine facilitates fear extinction learning. Transl Psychiatry. 2015;5:e634.
Curry DW, Young MB, Tran AN, Daoud GE, Howell LL. Separating the agony from ecstasy: R(−)-3,4-methylenedioxymethamphetamine has prosocial and therapeutic-like effects without signs of neurotoxicity in mice. Neuropharmacology. 2018;128:196–206.
Young MB, Norrholm SD, Khoury LM, Jovanovic T, Rauch SAM, Reiff CM, et al. Inhibition of serotonin transporters disrupts the enhancement of fear memory extinction by 3,4-methylenedioxymethamphetamine (MDMA). Psychopharmacology. 2017;234:2883–95.
Hake HS, Davis JKP, Wood RR, Tanner MK, Loetz EC, Sanchez A, et al. 3,4-methylenedioxymethamphetamine (MDMA) impairs the extinction and reconsolidation of fear memory in rats. Physiol Behav. 2019;199:343–50.
Holze F, Vizeli P, Müller F, Ley L, Duerig R, Varghese N, et al. Distinct acute effects of LSD, MDMA, and d-amphetamine in healthy subjects. Neuropsychopharmacology. 2020;45:462–71.
Han DD, Gu HH. Comparison of the monoamine transporters from human and mouse in their sensitivities to psychostimulant drugs. BMC Pharmacol. 2006;6:6.
Verrico CD, Lynch L, Fahey MA, Fryer A-K, Miller GM, Madras BK. MDMA-induced impairment in primates: antagonism by a selective norepinephrine or serotonin, but not by a dopamine/norepinephrine transport inhibitor. J Psychopharmacol. 2008;22:187–202.
Trigo JM, Renoir T, Lanfumey L, Hamon M, Lesch K-P, Robledo P, et al. 3,4-Methylenedioxymethamphetamine self-administration is abolished in serotonin transporter knockout mice. Biol Psychiatry. 2007;62:669–79.
Hagino Y, Takamatsu Y, Yamamoto H, Iwamura T, Murphy DL, Uhl GR, et al. Effects of MDMA on extracellular dopamine and serotonin levels in mice lacking dopamine and/or serotonin transporters. Curr Neuropharmacol. 2011;9:91–5.
Rickli A, Kopf S, Hoener MC, Liechti ME. Pharmacological profile of novel psychoactive benzofurans. Br J Pharmacol. 2015;172:3412–25.
Doly S, Valjent E, Setola V, Callebert J, Hervé D, Launay J-M, et al. Serotonin 5-HT2B receptors are required for 3,4-methylenedioxymethamphetamine-induced hyperlocomotion and 5-HT release in vivo and in vitro. J Neurosci 2008;28:2933–40.
van Wel JHP, Kuypers KPC, Theunissen EL, Bosker WM, Bakker K, Ramaekers JG. Effects of acute MDMA intoxication on mood and impulsivity: role of the 5-HT2 and 5-HT1 receptors. PLoS One. 2012;7:e40187.
Kuypers KPC, de la Torre R, Farre M, Pizarro N, Xicota L, Ramaekers JG. MDMA-induced indifference to negative sounds is mediated by the 5-HT 2A receptor. Psychopharmacology. 2018;235:481–90.
Catlow BJ, Song S, Paredes DA, Kirstein CL, Sanchez-Ramos J. Effects of psilocybin on hippocampal neurogenesis and extinction of trace fear conditioning. Exp Brain Res. 2013;228:481–91.
Zhang G, Ásgeirsdóttir HN, Cohen SJ, Munchow AH, Barrera MP, Stackman RW. Stimulation of serotonin 2A receptors facilitates consolidation and extinction of fear memory in C57BL/6J mice. Neuropharmacology. 2013;64:403–13.
Cameron L, Benson CJ, Dunlap LE, Olson DE. Effects of N,N-dimethyltryptamine on rat behaviors relevant to anxiety and depression. ACS Chem Neurosci. 2018;9:1582–90.
Cameron L, Benson CJ, DeFelice BC, Fiehn O, Olson DE. Chronic, intermittent microdoses of the psychedelic N,N-dimethyltryptamine (DMT) produce positive effects on mood and anxiety in rodents. ACS Chem Neurosci. 2019;10:3261–70.
Winstanley CA, Chudasama Y, Dalley JW, Theobald DEH, Glennon JC, Robbins TW. Intra-prefrontal 8-OH-DPAT and M100907 improve visuospatial attention and decrease impulsivity on the five-choice serial reaction time task in rats. Psychopharmacology. 2003;167:304–14.
Darmani NA, Shaddy J, Gerdes CF. Differential ontogenesis of three DOI-induced behaviors in mice. Physiol Behav. 1996;60:1495–1500.
Pierre A, Van Schuerbeek A, Allaoui W, Van Laere S, Singewald N, Van Eeckhaut A, et al. Effects of ghrelin receptor activation on forebrain dopamine release, conditioned fear and fear extinction in C57BL/6J mice. J Neurochem. 8;154:389–403.
Paxinos G, Franklin KB. Paxinos and Franklin’s the mouse brain in stereotaxic coordinates. Academic Press; 2019.
De Bundel D, Schallier A, Loyens E, Fernando R, Miyashita H, Van Liefferinge J, et al. Loss of system xc− does not induce oxidative stress but decreases extracellular glutamate in hippocampus and influences spatial working memory and limbic seizure susceptibility. J Neurosci. 2011;31:5792–803.
Sarnyai Z, Sibille EL, Pavlides C, Fenster RJ, McEwen BS, Tóth M. Impaired hippocampal-dependent learning and functional abnormalities in the hippocampus in mice lacking serotonin1A receptors. Proc Natl Acad Sci USA. 2000;97:14731–6.
Zussy C, Gómez-Santacana X, Rovira X, De Bundel D, Ferrazzo S, Bosch D, et al. Dynamic modulation of inflammatory pain-related affective and sensory symptoms by optical control of amygdala metabotropic glutamate receptor 4. Mol Psychiatry. 2018;23:509–20.
Albertini G, Walrave L, Demuyser T, Massie A, De, Bundel D, et al. 6 Hz corneal kindling in mice triggers neurobehavioral comorbidities accompanied by relevant changes in c-Fos immunoreactivity throughout the brain. Epilepsia. 2018;59:67–78.
Schindelin J, Arganda-Carreras I, Frise E, Kaynig V, Longair M, Pietzsch T, et al. Fiji: an open-source platform for biological-image analysis. Nat Methods. 2012;9:676–82.
Wheeler A, Henriques R. Standard and super-resolution bioimaging data analysis: a primer. 312. Wiley Online Library; 2017.
Maxwell SE, Delaney HD, Kelley K. Designing experiments and analyzing data: a model comparison perspective. Routledge; 2017.
Canal CE, da Silva UBO, Gresch PJ, Watt EE, Sanders-Bush E, Airey DC. The serotonin 2C receptor potently modulates the head-twitch response in mice induced by a phenethylamine hallucinogen. Psychopharmacology. 2010;209:163–74.
De Bundel D, Gangarossa G, Biever A, Bonnefont X, Valjent E. Cognitive dysfunction, elevated anxiety, and reduced cocaine response in circadian clock-deficient cryptochrome knockout mice. Front Behav Neurosci. 2013;7:152.
Puighermanal E, Castell L, Esteve-Codina A, Melser S, Kaganovsky K, Zussy C, et al. Functional and molecular heterogeneity of D2R neurons along dorsal-ventral axis in the striatum. Nat Commun. 2020;11:1957.
Bullitt E. Expression of C-fos-like protein as a marker for neuronal activity following noxious stimulation in the rat. J Comp Neurol. 1990;296:517–30.
Marek R, Sun Y, Sah P. Neural circuits for a top-down control of fear and extinction. Psychopharmacology. 2019;236:313–20.
Bocchio M, Fucsina G, Oikonomidis L, McHugh SB, Bannerman DM, Sharp T, et al. Increased serotonin transporter expression reduces fear and recruitment of parvalbumin interneurons of the amygdala. Neuropsychopharmacology. 2015;40:3015–26.
Jiang X, Xing G, Yang C, Verma A, Zhang L, Li H. Stress impairs 5-HT2A receptor-mediated serotonergic facilitation of GABA release in juvenile rat basolateral amygdala. Neuropsychopharmacology. 2009;34:410–23.
Ruotsalainen S, MacDonald E, Koivisto E, Stefanski R, Haapalinna A, Riekkinen P, et al. 5 -HT1A Receptor agonist (8-OH-DPAT) and 5-HT2 receptor agonist (DOI) disrupt the non-cognitive performance of rats in a working memory task. J Psychopharmacol. 1998;12:177–85.
Hjorth S, Magnusson T. The 5-HT 1A receptor agonist, 8-OH-DPAT, preferentially activates cell body 5-HT autoreceptors in rat brain in vivo. Naunyn-Schmiedebergs Arch Pharmacol. 1988;338:463–71.
Odland AU, Jessen L, Kristensen JL, Fitzpatrick CM, Andreasen JT. The 5-hydroxytryptamine 2A receptor agonists DOI and 25CN-NBOH decrease marble burying and reverse 8-OH-DPAT-induced deficit in spontaneous alternation. Neuropharmacology. 2021;183:107838.
Papakosta V-M, Kalogerakou S, Kontis D, Anyfandi E, Theochari E, Boulougouris V, et al. 5-HT2C receptor involvement in the control of persistence in the Reinforced Spatial Alternation animal model of obsessive–compulsive disorder. Behav Brain Res. 2013;243:176–83.
Hameleers R, Blokland A, Steinbusch HWM, Visser-Vandewalle V, Temel Y. Hypomobility after DOI administration can be reversed by subthalamic nucleus deep brain stimulation. Behav Brain Res. 2007;185:65–7.
Krebs-Thomson K, Geyer MA. Evidence for a functional interaction between 5-HT1A and 5-HT2 receptors in rats. Psychopharmacology. 1998;140:69–74.
Wing LL, Tapson GS, Geyer MA. 5HT-2 mediation of acute behavioral effects of hallucinogens in rats. Psychopharmacology. 1990;100:417–25.
Mittman SM, Geyer MA. Dissociation of multiple effects of acute LSD on exploratory behavior in rats by ritanserin and propranolol. Psychopharmacology. 1991;105:69–76.
Halberstadt AL, van der Heijden I, Ruderman MA, Risbrough VB, Gingrich JA, Geyer MA, et al. 5-HT2A and 5-HT2C receptors exert opposing effects on locomotor activity in mice. Neuropsychopharmacology. 2009;34:1958–67.
Onaivi ES, Bishop-Robinson C, Darmani NA, Sanders-Bush E. Behavioral effects of (±)-1-(2,5-dimethoxy-4-iodophenyl)-2-aminopropane, (DOI) in the elevated plus-maze test. Life Sci. 1995;57:2455–66.
Nic Dhonnchadha BÁ, Hascoët M, Jolliet P, Bourin M. Evidence for a 5-HT2A receptor mode of action in the anxiolytic-like properties of DOI in mice. Behav Brain Res. 2003;147:175–84.
Ripoll N, Hascoët M, Bourin M. Implication of 5-HT2A subtype receptors in DOI activity in the four-plates test-retest paradigm in mice. Behav Brain Res. 2006;166:131–9.
Lapin IP. Anxiogenic effect of phenylethylamine and amphetamine in the elevated plus-maze in mice and its attenuation by ethanol. Pharm Biochem Behav. 1993;44:241–3.
Lin HQ, Burden PM, Christie MJ, Johnston GA. The anxiogenic-like and anxiolytic-like effects of MDMA on mice in the elevated plus-maze: a comparison with amphetamine. Pharm Biochem Behav. 1999;62:403–8.
Biala G, Kruk M. Effects of co-administration of bupropion and nicotine or D-amphetamine on the elevated plus maze test in mice. J Pharm Pharmacol. 2009;61:493–502.
LeDoux J. The amygdala. Curr Biol. 2007;17:R868–74.
Maćkowiak M, Chocyk A, Fijał K, Czyrak A, Wedzony K. c-Fos proteins, induced by the serotonin receptor agonist DOI, are not expressed in 5-HT2A positive cortical neurons. Brain Res Mol Brain Res. 1999;71:358–63.
Martin DA, Nichols CD. Psychedelics recruit multiple cellular types and produce complex transcriptional responses within the brain. EBioMedicine. 2016;11:262–77.
de Paula Soares V, Zangrossi H. Stimulation of 5-HT1A or 5-HT2A receptors in the ventrolateral periaqueductal gray causes anxiolytic-, but not panicolytic-like effect in rats. Behav Brain. 2009;197:178–85.
Petit-Demoulière B, Massé F, Cogrel N, Hascoët M, Bourin M. Brain structures implicated in the four-plate test in naïve and experienced Swiss mice using injection of diazepam and the 5-HT2A agonist DOI. Behav Brain Res. 2009;204:200–5.
Hessel M, Pape H-C, Seidenbecher T. Stimulation of 5-HT receptors in anterodorsal BNST guides fear to predictable and unpredictable threat. Eur Neuropsychopharmacol J Eur Coll Neuropsychopharmacol. 2020;39:56–69.
Gasser P, Kirchner K, Passie T. LSD-assisted psychotherapy for anxiety associated with a life-threatening disease: a qualitative study of acute and sustained subjective effects. J Psychopharmacol. 2014;29:57–68.
Goldberg SB, Pace BT, Nicholas CR, Raison CL, Hutson PR. The experimental effects of psilocybin on symptoms of anxiety and depression: a meta-analysis. Psychiatry Res. 2020;284:112749.
Ross S, Bossis A, Guss J, Agin-Liebes G, Malone T, Cohen B, et al. Rapid and sustained symptom reduction following psilocybin treatment for anxiety and depression in patients with life-threatening cancer: a randomized controlled trial. J Psychopharmacol. 2016;30:1165–80.
Griffiths RR, Johnson MW, Carducci MA, Umbricht A, Richards WA, Richards BD, et al. Psilocybin produces substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer: a randomized double-blind trial. J Psychopharmacol. 2016;30:1181–97.
Muttoni S, Ardissino M, John C. Classical psychedelics for the treatment of depression and anxiety: a systematic review. J Affect Disord. 2019;258:11–24.
Kraehenmann R, Schmidt A, Friston K, Preller KH, Seifritz E, Vollenweider FX. The mixed serotonin receptor agonist psilocybin reduces threat-induced modulation of amygdala connectivity. NeuroImage Clin. 2016;11:53–60.
Dolder PC, Schmid Y, Müller F, Borgwardt S, Liechti ME. LSD acutely impairs fear recognition and enhances emotional empathy and sociality. Neuropsychopharmacology. 2016;41:2638–46.
Risbrough VB, Brodkin JD, Geyer MA. GABA-A and 5-HT1A receptor agonists block expression of fear-potentiated startle in mice. Neuropsychopharmacology. 2003;28:654–63.
Zhao Y, Bijlsma EY, ter Heegde F, Verdouw MP, Garssen J, Newman-Tancredi A, et al. Activation of somatodendritic 5-HT 1A autoreceptors reduces the acquisition and expression of cued fear in the rat fear-potentiated startle test. Psychopharmacology. 2019;236:1171–85.
Wang C-C, Lin H-C, Chan Y-H, Gean P-W, Yang YK, Chen PS. 5-HT1A-receptor agonist modified amygdala activity and amygdala-associated social behavior in a valproate-induced rat autism model. Int J Neuropsychopharmacol. 2013;16:2027–39.
Koseki H, Matsumoto M, Togashi H, Miura Y, Fukushima K, Yoshioka M. Alteration of synaptic transmission in the hippocampal-mPFC pathway during extinction trials of context-dependent fear memory in juvenile rat stress models. Synapse. 2009;63:805–13.
de la Fuente Revenga M, Zhu B, Guevara CA, Naler LB, Saunders JM, Zhou Z, et al. Prolonged epigenomic and synaptic plasticity alterations following single exposure to a psychedelic in mice. Cell Rep. 2021;37:109836.
Padich RA, McCloskey TC, Kehne JH. 5-HT modulation of auditory and visual sensorimotor gating: II. Effects of the 5-HT 2A antagonist MDL 100,907 on disruption of sound and light prepulse inhibition produced by 5-HT agonists in Wistar rats. Psychopharmacology. 1996;124:107–16.
Orejarena MJ, Lanfumey L, Maldonado R, Robledo P. Involvement of 5-HT2A receptors in MDMA reinforcement and cue-induced reinstatement of MDMA-seeking behaviour. Int J Neuropsychopharmacol. 2011;14:927–40.
Kehne JH, Ketteler HJ, McCloskey TC, Sullivan CK, Dudley MW, Schmidt CJ. Effects of the selective 5-HT2A receptor antagonist MDL 100,907 on MDMA-induced locomotor stimulation in rats. Neuropsychopharmacology. 1996;15:116–24.
Herin DV, Liu S, Ullrich T, Rice KC, Cunningham KA. Role of the serotonin 5-HT 2A receptor in the hyperlocomotive and hyperthermic effects of (+)-3,4-methylenedioxymethamphetamine. Psychopharmacology. 2005;178:505–13.
Pitts EG, Minerva AR, Chandler EB, Kohn JN, Logun MT, Sulima A, et al. 3,4-Methylenedioxymethamphetamine increases affiliative behaviors in squirrel monkeys in a serotonin 2A receptor-dependent manner. Neuropsychopharmacology. 2017;42:1962–71.
Acknowledgements
We acknowledge the practical support of Wissal Allaoui, Gino De Smet, and Anke De Smet.
Funding
This work was supported by the Fund for Scientific Research Flanders (G023020N to DDB), by grants from CNRS, INSERM, University of Montpellier, iSITE MUSE and Fondation pour la Recherche Médicale (to PM, JB, and CB) and by INSERM, Fondation pour la Recherche Médicale (DEQ20160334919) and the French National Research Agency ANR (DOPAFEAR to EV).
Author information
Authors and Affiliations
Contributions
DDB., EV, and CB conceived the original idea. JB and PM contributed to conception of the study. DDB, EV, and BP designed the experiments. DDB, BP, SR, MS, and AVS carried out the experiments. DDB and BP analyzed the data. AP provided technical training and contributed to supervising the experiments. CB contributed essential materials. DDB and BP wrote the manuscript. All authors contributed to interpretation of the results and provided critical feedback on the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Pędzich, B.D., Rubens, S., Sekssaoui, M. et al. Effects of a psychedelic 5-HT2A receptor agonist on anxiety-related behavior and fear processing in mice. Neuropsychopharmacol. 47, 1304–1314 (2022). https://doi.org/10.1038/s41386-022-01324-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-022-01324-2
- Springer Nature Switzerland AG