Key Points
-
Recent research efforts have narrowed the gap between in vivo MRI and pathology with respect to multiple sclerosis (MS) lesion development and staging
-
Demyelinated lesions in marmoset experimental autoimmune encephalomyelitis (EAE) resemble their human counterparts far better than do lesions in rodent EAE models
-
Application of parallel MRI methods in MS and marmoset EAE facilitates interpretation of data collected in both conditions
-
The perivenular topography of inflammatory demyelinating lesions might facilitate the diagnostic work-up for MS
-
Smouldering lesions and meningeal inflammation are important features of chronic inflammation that should be targeted for in vivo imaging
Abstract
Over the past few decades, MRI-based visualization of demyelinated CNS lesions has become pivotal to the diagnosis and monitoring of multiple sclerosis (MS). In this Review, we outline current efforts to correlate imaging findings with the pathology of lesion development in MS, and the pitfalls that are being encountered in this research. Multimodal imaging at high and ultra-high magnetic field strengths is yielding biologically relevant insights into the pathophysiology of blood–brain barrier dynamics and both active and chronic inflammation, as well as mechanisms of lesion healing and remyelination. Here, we parallel the results in humans with advances in imaging of a primate model of MS — experimental autoimmune encephalomyelitis (EAE) in the common marmoset — in which demyelinated lesions resemble their human counterparts far more closely than do EAE lesions in the rodent. This approach holds promise for the identification of innovative biological markers, and for next-generation clinical trials that will focus more on tissue protection and repair.




Similar content being viewed by others
References
Filippi, M. et al. Association between pathological and MRI findings in multiple sclerosis. Lancet Neurol. 11, 349–360 (2012).
't Hart, B. A., van Kooyk, Y., Geurts, J. J. & Gran, B. The primate autoimmune encephalomyelitis model; a bridge between mouse and man. Ann. Clin. Transl. Neurol. 2, 581–593 (2015).
Maggi, P. et al. The formation of inflammatory demyelinated lesions in cerebral white matter. Ann. Neurol. 76, 594–608 (2014).
Guy, J. R. et al. Custom fit 3D-printed brain holders for comparison of histology with MRI in marmosets. J. Neurosci. Methods 257, 55–63 (2016).
Ransohoff, R. M. & Engelhardt, B. The anatomical and cellular basis of immune surveillance in the central nervous system. Nat. Rev. Immunol. 12, 623–635 (2012).
Bartholomäus, I. et al. Effector T cell interactions with meningeal vascular structures in nascent autoimmune CNS lesions. Nature 462, 94–98 (2009).
Lucchinetti, C. F. et al. Inflammatory cortical demyelination in early multiple sclerosis. N. Engl. J. Med. 365, 2188–2197 (2011).
Polman, C. H. et al. Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann. Neurol. 69, 292–302 (2011).
Filippi, M. et al. MRI criteria for the diagnosis of multiple sclerosis: MAGNIMS consensus guidelines. Lancet Neurol. 15, 292–303 (2016).
Rae-Grant, A. D., Wong, C., Bernatowicz, R. & Fox, R. J. Observations on the brain vasculature in multiple sclerosis: a historical perspective. Mult. Scler. Relat. Disord. 3, 156–162 (2014).
Tan, I. L. et al. MR venography of multiple sclerosis. AJNR Am. J. Neuroradiol. 21, 1039–1042 (2000).
Hammond, K. E. et al. Quantitative in vivo magnetic resonance imaging of multiple sclerosis at 7 Tesla with sensitivity to iron. Ann. Neurol. 64, 707–713 (2008).
Tallantyre, E. C. et al. Demonstrating the perivascular distribution of MS lesions in vivo with 7-Tesla MRI. Neurology 70, 2076–2078 (2008).
Sati, P., George, I. C., Shea, C. D., Gaitan, M. I. & Reich, D. S. FLAIR*: a combined MR contrast technique for visualizing white matter lesions and parenchymal veins. Radiology 265, 926–932 (2012).
Tallantyre, E. C. et al. Ultra-high-field imaging distinguishes MS lesions from asymptomatic white matter lesions. Neurology 76, 534–539 (2011).
Kau, T. et al. The 'central vein sign': is there a place for susceptibility weighted imaging in possible multiple sclerosis? Eur. Radiol. 23, 1956–1962 (2013).
Absinta, M. et al. Seven-tesla phase imaging of acute multiple sclerosis lesions: a new window into the inflammatory process. Ann. Neurol. 74, 669–678 (2013).
Absinta, M. et al. Direct MRI detection of impending plaque development in multiple sclerosis. Neurol. Neuroimmunol. Neuroinflamm. 2, e145 (2015).
Gaitan, M. I., de Alwis, M. P., Sati, P., Nair, G. & Reich, D. S. Multiple sclerosis shrinks intralesional, and enlarges extralesional, brain parenchymal veins. Neurology 80, 145–151 (2013).
Müller, K. et al. Detailing intra-lesional venous lumen shrinking in multiple sclerosis investigated by sFLAIR MRI at 7-T. J. Neurol. 261, 2032–2036 (2014).
Dal-Bianco, A. et al. Veins in plaques of multiple sclerosis patients — a longitudinal magnetic resonance imaging study at 7 Tesla. Eur. Radiol. 25, 2913–2920 (2015).
George, I. C. et al. Clinical 3-tesla FLAIR* MRI improves diagnostic accuracy in multiple sclerosis. Mult. Scler. http://dx.doi.org/10.1177/1352458515624975 (2016).
Lummel, N. et al. Presence of a central vein within white matter lesions on susceptibility weighted imaging: a specific finding for multiple sclerosis? Neuroradiology 53, 311–317 (2011).
Kilsdonk, I. D. et al. Improved differentiation between MS and vascular brain lesions using FLAIR* at 7 Tesla. Eur. Radiol. 24, 841–849 (2014).
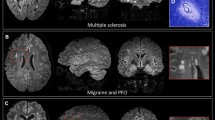
Solomon, A. J. et al. 'Central vessel sign' on 3T FLAIR* MRI for the differentiation of multiple sclerosis from migraine. Ann. Clin. Transl. Neurol. 3, 82–87 (2015).
Wuerfel, J. et al. Lesion morphology at 7 Tesla MRI differentiates Susac syndrome from multiple sclerosis. Mult. Scler. 18, 1592–1599 (2012).
Massacesi, L. et al. Active and passively induced experimental autoimmune encephalomyelitis in common marmosets: a new model for multiple sclerosis. Ann. Neurol. 37, 519–530 (1995).
Genain, C. P. & Hauser, S. L. Experimental allergic encephalomyelitis in the New World monkey Callithrix jacchus. Immunol. Rev. 183, 159–172 (2001).
Jagessar, S. A. et al. Autoimmunity against myelin oligodendrocyte glycoprotein is dispensable for the initiation although essential for the progression of chronic encephalomyelitis in common marmosets. J. Neuropathol. Exp. Neurol. 67, 326–340 (2008).
Jagessar, S. A., Dijkman, K., Dunham, J., 't Hart, B. A. & Kap, Y. S. Experimental autoimmune encephalomyelitis in marmosets. Methods Mol. Biol. 1304, 171–186 (2016).
Hart, B. A. et al. Histopathological characterization of magnetic resonance imaging-detectable brain white matter lesions in a primate model of multiple sclerosis: a correlative study in the experimental autoimmune encephalomyelitis model in common marmosets (Callithrix jacchus). Am. J. Pathol. 153, 649–663 (1998).
t Hart, B. A. et al. Modelling of multiple sclerosis: lessons learned in a non-human primate. Lancet Neurol. 3, 588–597 (2004).
Blezer, E. L., Bauer, J., Brok, H. P., Nicolay, K. & 't Hart, B. A. Quantitative MRI-pathology correlations of brain white matter lesions developing in a non-human primate model of multiple sclerosis. NMR Biomed. 20, 90–103 (2007).
Jordan, E. K. et al. Serial MR imaging of experimental autoimmune encephalomyelitis induced by human white matter or by chimeric myelin-basic and proteolipid protein in the common marmoset. AJNR Am. J. Neuroradiol. 20, 965–976 (1999).
Diem, R. et al. Autoimmune optic neuritis in the common marmoset monkey: comparison of visual evoked potentials with MRI and histopathology. Invest. Ophthalmol. Vis. Sci. 49, 3707–3714 (2008).
Boretius, S. et al. Monitoring of EAE onset and progression in the common marmoset monkey by sequential high-resolution 3D MRI. NMR Biomed. 19, 41–49 (2006).
Gaitan, M. I. et al. Perivenular brain lesions in a primate multiple sclerosis model at 7-tesla magnetic resonance imaging. Mult. Scler. 20, 64–71 (2014).
Henderson, A. P., Barnett, M. H., Parratt, J. D. & Prineas, J. W. Multiple sclerosis: distribution of inflammatory cells in newly forming lesions. Ann. Neurol. 66, 739–753 (2009).
Prineas, J. W. & Parratt, J. D. Oligodendrocytes and the early multiple sclerosis lesion. Ann. Neurol. 72, 18–31 (2012).
Lucchinetti, C. et al. Heterogeneity of multiple sclerosis lesions: implications for the pathogenesis of demyelination. Ann. Neurol. 47, 707–717 (2000).
Singh, S. et al. Microglial nodules in early multiple sclerosis white matter are associated with degenerating axons. Acta Neuropathol. 125, 595–608 (2013).
Peferoen, L. A. et al. Activation status of human microglia is dependent on lesion formation stage and remyelination in multiple sclerosis. J. Neuropathol. Exp. Neurol. 74, 48–63 (2015).
Nikic, I. et al. A reversible form of axon damage in experimental autoimmune encephalomyelitis and multiple sclerosis. Nat. Med. 17, 495–499 (2011).
Alvarez, J. I. et al. Focal disturbances in the blood–brain barrier are associated with formation of neuroinflammatory lesions. Neurobiol. Dis. 74, 14–24 (2014).
Filippi, M., Rocca, M. A., Martino, G., Horsfield, M. A. & Comi, G. Magnetization transfer changes in the normal appearing white matter precede the appearance of enhancing lesions in patients with multiple sclerosis. Ann. Neurol. 43, 809–814 (1998).
Goodkin, D. E. et al. A serial study of new MS lesions and the white matter from which they arise. Neurology 51, 1689–1697 (1998).
Werring, D. J. et al. The pathogenesis of lesions and normal-appearing white matter changes in multiple sclerosis: a serial diffusion MRI study. Brain 123, 1667–1676 (2000).
Eisele, P. et al. Reduced diffusion in a subset of acute MS lesions: a serial multiparametric MRI study. AJNR Am. J. Neuroradiol. 33, 1369–1373 (2012).
Tartaglia, M. C. et al. Choline is increased in pre-lesional normal appearing white matter in multiple sclerosis. J. Neurol. 249, 1382–1390 (2002).
Wuerfel, J. et al. Changes in cerebral perfusion precede plaque formation in multiple sclerosis: a longitudinal perfusion MRI study. Brain 127, 111–119 (2004).
Wiggermann, V. et al. Magnetic resonance frequency shifts during acute MS lesion formation. Neurology 81, 211–218 (2013).
Guttmann, C. R. et al. Multiple sclerosis lesion formation and early evolution revisited: a weekly high-resolution magnetic resonance imaging study. Mult. Scler. 22, 761–769 (2016).
Obermeier, B., Daneman, R. & Ransohoff, R. M. Development, maintenance and disruption of the blood–brain barrier. Nat. Med. 19, 1584–1596 (2013).
Vos, C. M. et al. Blood–brain barrier alterations in both focal and diffuse abnormalities on postmortem MRI in multiple sclerosis. Neurobiol. Dis. 20, 953–960 (2005).
Gay, D. & Esiri, M. Blood–brain barrier damage in acute multiple sclerosis plaques: an immunocytological study. Brain 114, 557–572 (1991).
Agrawal, S. M. et al. Extracellular matrix metalloproteinase inducer shows active perivascular cuffs in multiple sclerosis. Brain 136, 1760–1777 (2013).
Davalos, D. et al. Fibrinogen-induced perivascular microglial clustering is required for the development of axonal damage in neuroinflammation. Nat. Commun. 3, 1227 (2012).
Ryu, J. K. et al. Blood coagulation protein fibrinogen promotes autoimmunity and demyelination via chemokine release and antigen presentation. Nat. Commun. 6, 8164 (2015).
McFarland, H. F. et al. Using gadolinium-enhanced magnetic resonance imaging lesions to monitor disease activity in multiple sclerosis. Ann. Neurol. 32, 758–766 (1992).
Frank, J. A. et al. Serial contrast-enhanced magnetic resonance imaging in patients with early relapsing–remitting multiple sclerosis: implications for treatment trials. Ann. Neurol. 36, S86–S90 (1994).
Gaitan, M. I. et al. Evolution of the blood–brain barrier in newly forming multiple sclerosis lesions. Ann. Neurol. 70, 22–29 (2011).
Gaitan, M. I., Sati, P., Inati, S. J. & Reich, D. S. Initial investigation of the blood–brain barrier in MS lesions at 7 tesla. Mult. Scler. 19, 1068–1073 (2013).
Lassmann, H., Raine, C. S., Antel, J. & Prineas, J. W. Immunopathology of multiple sclerosis: report on an international meeting held at the Institute of Neurology of the University of Vienna. J. Neuroimmunol. 86, 213–217 (1998).
van der Valk, P. & De Groot, C. J. Staging of multiple sclerosis (MS) lesions: pathology of the time frame of MS. Neuropathol. Appl. Neurobiol. 26, 2–10 (2000).
Yamasaki, R. et al. Differential roles of microglia and monocytes in the inflamed central nervous system. J. Exp. Med. 211, 1533–1549 (2014).
Butovsky, O. et al. Identification of a unique TGF-β-dependent molecular and functional signature in microglia. Nat. Neurosci. 17, 131–143 (2014).
Miron, V. E. et al. M2 microglia and macrophages drive oligodendrocyte differentiation during CNS remyelination. Nat. Neurosci. 16, 1211–1218 (2013).
Lassmann, H., van Horssen, J. & Mahad, D. Progressive multiple sclerosis: pathology and pathogenesis. Nat. Rev. Neurol. 8, 647–656 (2012).
Hametner, S. et al. Iron and neurodegeneration in the multiple sclerosis brain. Ann. Neurol. 74, 848–861 (2013).
Stephenson, E., Nathoo, N., Mahjoub, Y., Dunn, J. F. & Yong, V. W. Iron in multiple sclerosis: roles in neurodegeneration and repair. Nat. Rev. Neurol. 10, 459–468 (2014).
Trapp, B. D. et al. Axonal transection in the lesions of multiple sclerosis. N. Engl. J. Med. 338, 278–285 (1998).
Dutta, R. et al. Mitochondrial dysfunction as a cause of axonal degeneration in multiple sclerosis patients. Ann. Neurol. 59, 478–489 (2006).
Laule, C. et al. Myelin water imaging in multiple sclerosis: quantitative correlations with histopathology. Mult. Scler. 12, 747–753 (2006).
Levesque, I. R. et al. Reproducibility of quantitative magnetization-transfer imaging parameters from repeated measurements. Magn. Reson. Med. 64, 391–400 (2010).
Sati, P. et al. Micro-compartment specific T2* relaxation in the brain. NeuroImage 77, 268–278 (2013).
Alonso-Ortiz, E., Levesque, I. R. & Pike, G. B. MRI-based myelin water imaging: a technical review. Magn. Reson. Med. 73, 70–81 (2015).
Yablonskiy, D. A., Luo, J., Sukstanskii, A. L., Iyer, A. & Cross, A. H. Biophysical mechanisms of MRI signal frequency contrast in multiple sclerosis. Proc. Natl Acad. Sci. USA 109, 14212–14217 (2012).
Mehta, V. et al. Iron is a sensitive biomarker for inflammation in multiple sclerosis lesions. PLoS ONE 8, e57573 (2013).
Chen, W. et al. Quantitative susceptibility mapping of multiple sclerosis lesions at various ages. Radiology 271, 183–192 (2014).
Shechter, R. & Schwartz, M. CNS sterile injury: just another wound healing? Trends Mol. Med. 19, 135–143 (2013).
Prineas, J. W., Barnard, R. O., Kwon, E. E., Sharer, L. R. & Cho, E. S. Multiple sclerosis: remyelination of nascent lesions. Ann. Neurol. 33, 137–151 (1993).
Raine, C. S. & Wu, E. Multiple sclerosis: remyelination in acute lesions. J. Neuropathol. Exp. Neurol. 52, 199–204 (1993).
Patrikios, P. et al. Remyelination is extensive in a subset of multiple sclerosis patients. Brain 129, 3165–3172 (2006).
Albert, M., Antel, J., Bruck, W. & Stadelmann, C. Extensive cortical remyelination in patients with chronic multiple sclerosis. Brain Pathol. 17, 129–138 (2007).
Bramow, S. et al. Demyelination versus remyelination in progressive multiple sclerosis. Brain 133, 2983–2998 (2010).
Chang, A., Tourtellotte, W. W., Rudick, R. & Trapp, B. D. Premyelinating oligodendrocytes in chronic lesions of multiple sclerosis. N. Engl. J. Med. 346, 165–173 (2002).
Kuhlmann, T. et al. Differentiation block of oligodendroglial progenitor cells as a cause for remyelination failure in chronic multiple sclerosis. Brain 131, 1749–1758 (2008).
Goldschmidt, T., Antel, J., König, F. B., Bruck, W. & Kuhlmann, T. Remyelination capacity of the MS brain decreases with disease chronicity. Neurology 72, 1914–1921 (2009).
Franklin, R. J. & Gallo, V. The translational biology of remyelination: past, present, and future. Glia 62, 1905–1915 (2014).
van Walderveen, M. A. et al. Histopathologic correlate of hypointense lesions on T1-weighted spin-echo MRI in multiple sclerosis. Neurology 50, 1282–1288 (1998).
van Waesberghe, J. H. et al. Axonal loss in multiple sclerosis lesions: magnetic resonance imaging insights into substrates of disability. Ann. Neurol. 46, 747–754 (1999).
Chen, J. T. et al. Magnetization transfer ratio evolution with demyelination and remyelination in multiple sclerosis lesions. Ann. Neurol. 63, 254–262 (2008).
Reich, D. S. et al. Sample-size calculations for short-term proof-of-concept studies of tissue protection and repair in multiple sclerosis lesions via conventional clinical imaging. Mult. Scler. 21, 1693–1704 (2015).
Lassmann, H. Review: the architecture of inflammatory demyelinating lesions: implications for studies on pathogenesis. Neuropathol. Appl. Neurobiol. 37, 698–710 (2011).
Frischer, J. M. et al. Clinical and pathological insights into the dynamic nature of the white matter multiple sclerosis plaque. Ann. Neurol. 78, 710–721 (2015).
Pitt, D. et al. Imaging cortical lesions in multiple sclerosis with ultra-high-field magnetic resonance imaging. Arch. Neurol. 67, 812–818 (2010).
Bagnato, F. et al. Tracking iron in multiple sclerosis: a combined imaging and histopathological study at 7 Tesla. Brain 134, 3602–3615 (2011).
Bian, W. et al. A serial in vivo 7T magnetic resonance phase imaging study of white matter lesions in multiple sclerosis. Mult. Scler. 19, 69–75 (2012).
Yao, B. et al. Chronic multiple sclerosis lesions: characterization with high-field-strength MR imaging. Radiology 262, 206–215 (2012).
Hagemeier, J. et al. Iron deposition in multiple sclerosis lesions measured by susceptibility-weighted imaging filtered phase: a case control study. J. Magn. Reson. Imaging 36, 73–83 (2012).
Absinta, M. et al. Poor outcome in MS lesions with persistent 7-tesla phase rim. J. Clin. Invest. http://dx.doi.org/10.1172/JCI86198 (2016).
Vellinga, M. M. et al. Pluriformity of inflammation in multiple sclerosis shown by ultra-small iron oxide particle enhancement. Brain 131, 800–807 (2008).
Tourdias, T. et al. Assessment of disease activity in multiple sclerosis phenotypes with combined gadolinium- and superparamagnetic iron oxide-enhanced MR imaging. Radiology 264, 225–233 (2012).
Maarouf, A. et al. Ultra-small superparamagnetic iron oxide enhancement is associated with higher loss of brain tissue structure in clinically isolated syndrome. Mult. Scler. http://dx.doi.org/10.1177/1352458515607649 (2015).
Dousset, V. et al. Comparison of ultrasmall particles of iron oxide (USPIO)-enhanced T2-weighted, conventional T2-weighted, and gadolinium-enhanced T1-weighted MR images in rats with experimental autoimmune encephalomyelitis. AJNR Am. J. Neuroradiol. 20, 223–227 (1999).
Berger, C., Hiestand, P., Kindler-Baumann, D., Rudin, M. & Rausch, M. Analysis of lesion development during acute inflammation and remission in a rat model of experimental autoimmune encephalomyelitis by visualization of macrophage infiltration, demyelination and blood–brain barrier damage. NMR Biomed. 19, 101–107 (2006).
Baeten, K. et al. Visualisation of the kinetics of macrophage infiltration during experimental autoimmune encephalomyelitis by magnetic resonance imaging. J. Neuroimmunol. 195, 1–6 (2008).
Lucchinetti, C. F., Bruck, W., Rodriguez, M. & Lassmann, H. Distinct patterns of multiple sclerosis pathology indicates heterogeneity on pathogenesis. Brain Pathol. 6, 259–274 (1996).
Metz, I. et al. Pathologic heterogeneity persists in early active multiple sclerosis lesions. Ann. Neurol. 75, 728–738 (2014).
Popescu, B. F., Bunyan, R. F., Parisi, J. E., Ransohoff, R. M. & Lucchinetti, C. F. A case of multiple sclerosis presenting with inflammatory cortical demyelination. Neurology 76, 1705–1710 (2011).
Kutzelnigg, A. et al. Cortical demyelination and diffuse white matter injury in multiple sclerosis. Brain 128, 2705–2712 (2005).
Peterson, J. W., Bo, L., Mork, S., Chang, A. & Trapp, B. D. Transected neurites, apoptotic neurons, and reduced inflammation in cortical multiple sclerosis lesions. Ann. Neurol. 50, 389–400 (2001).
Bo, L., Vedeler, C. A., Nyland, H., Trapp, B. D. & Mork, S. J. Intracortical multiple sclerosis lesions are not associated with increased lymphocyte infiltration. Mult. Scler. 9, 323–331 (2003).
Kooi, E. J., Strijbis, E. M., van der Valk, P. & Geurts, J. J. Heterogeneity of cortical lesions in multiple sclerosis: clinical and pathologic implications. Neurology 79, 1369–1376 (2012).
Chang, A. et al. Cortical remyelination: a new target for repair therapies in multiple sclerosis. Ann. Neurol. 72, 918–926 (2012).
Kidd, D. et al. Cortical lesions in multiple sclerosis. Brain 122, 17–26 (1999).
Fischer, M. T. et al. Disease-specific molecular events in cortical multiple sclerosis lesions. Brain 136, 1799–1815 (2013).
Magliozzi, R. et al. Meningeal B-cell follicles in secondary progressive multiple sclerosis associate with early onset of disease and severe cortical pathology. Brain 130, 1089–1104 (2007).
Magliozzi, R. et al. A Gradient of neuronal loss and meningeal inflammation in multiple sclerosis. Ann. Neurol. 68, 477–493 (2010).
Howell, O. W. et al. Meningeal inflammation is widespread and linked to cortical pathology in multiple sclerosis. Brain 134, 2755–2771 (2011).
Choi, S. R. et al. Meningeal inflammation plays a role in the pathology of primary progressive multiple sclerosis. Brain 135, 2925–2937 (2012).
Kuerten, S. et al. Tertiary lymphoid organ development coincides with determinant spreading of the myelin-specific T cell response. Acta Neuropathol. 124, 861–873 (2012).
Magliozzi, R. et al. B-cell enrichment and Epstein–Barr virus infection in inflammatory cortical lesions in secondary progressive multiple sclerosis. J. Neuropathol. Exp. Neurol. 72, 29–41 (2013).
Bo, L., Geurts, J. J., van der Valk, P., Polman, C. & Barkhof, F. Lack of correlation between cortical demyelination and white matter pathologic changes in multiple sclerosis. Arch. Neurol. 64, 76–80 (2007).
Calabrese, M. et al. Exploring the origins of grey matter damage in multiple sclerosis. Nat. Rev. Neurosci. 16, 147–158 (2015).
Geurts, J. J. et al. Cortical lesions in multiple sclerosis: combined postmortem MR imaging and histopathology. AJNR Am. J. Neuroradiol. 26, 572–577 (2005).
Schmierer, K. et al. High field (9.4 Tesla) magnetic resonance imaging of cortical grey matter lesions in multiple sclerosis. Brain 133, 858–867 (2010).
Seewann, A. et al. Postmortem verification of MS cortical lesion detection with 3D DIR. Neurology 78, 302–308 (2012).
Sethi, V. et al. Improved detection of cortical MS lesions with phase-sensitive inversion recovery MRI. J. Neurol. Neurosurg. Psychiatry 83, 877–882 (2012).
Mainero, C. et al. In vivo imaging of cortical pathology in multiple sclerosis using ultra-high field MRI. Neurology 73, 941–948 (2009).
Nielsen, A. S. et al. Contribution of cortical lesion subtypes at 7T MRI to physical and cognitive performance in MS. Neurology 81, 641–649 (2013).
Mainero, C. et al. A gradient in cortical pathology in multiple sclerosis by in vivo quantitative 7 T imaging. Brain 138, 932–945 (2015).
Abdel-Fahim, R. et al. Improved detection of focal cortical lesions using 7 T magnetisation transfer imaging in patients with multiple sclerosis. Mult. Scler. Relat. Disord. 3, 258–265 (2014).
Jonkman, L. E. et al. Ultra-high field MTR and qR2* differentiates subpial cortical lesions from normal-appearing gray matter in multiple sclerosis. Mult. Scler. http://dx.doi.org/10.1177/1352458515620499 (2015).
Calabrese, M. et al. Cortical lesions in primary progressive multiple sclerosis: a 2-year longitudinal MR study. Neurology 72, 1330–1336 (2009).
Calabrese, M. et al. Cortical lesions and atrophy associated with cognitive impairment in relapsing–remitting multiple sclerosis. Arch. Neurol. 66, 1144–1150 (2009).
Roosendaal, S. D. et al. Accumulation of cortical lesions in MS: relation with cognitive impairment. Mult. Scler. 15, 708–714 (2009).
Calabrese, M. et al. A 3-year magnetic resonance imaging study of cortical lesions in relapse-onset multiple sclerosis. Ann. Neurol. 67, 376–383 (2010).
Calabrese, M. et al. Cortical lesion load associates with progression of disability in multiple sclerosis. Brain 135, 2952–2961 (2012).
Absinta, M. et al. Gadolinium-based MRI characterization of leptomeningeal inflammation in multiple sclerosis. Neurology 85, 18–28 (2015).
Pomeroy, I. M., Matthews, P. M., Frank, J. A., Jordan, E. K. & Esiri, M. M. Demyelinated neocortical lesions in marmoset autoimmune encephalomyelitis mimic those in multiple sclerosis. Brain 128, 2713–2721 (2005).
Merkler, D. et al. Differential macrophage/microglia activation in neocortical EAE lesions in the marmoset monkey. Brain Pathol. 16, 117–123 (2006).
Pomeroy, I. M., Jordan, E. K., Frank, J. A., Matthews, P. M. & Esiri, M. M. Diffuse cortical atrophy in a marmoset model of multiple sclerosis. Neurosci. Lett. 437, 121–124 (2008).
Pomeroy, I. M., Jordan, E. K., Frank, J. A., Matthews, P. M. & Esiri, M. M. Focal and diffuse cortical degenerative changes in a marmoset model of multiple sclerosis. Mult. Scler. 16, 537–548 (2010).
Kramann, N. et al. Increased meningeal T and plasma cell infiltration is associated with early subpial cortical demyelination in common marmosets with experimental autoimmune encephalomyelitis. Brain Pathol. 25, 276–286 (2015).
Acknowledgements
The authors acknowledge financial support from the Intramural Research Program of the National Institute of Neurological Disorders and Stroke, USA. D.S.R. has received research support from Vertex Pharmaceuticals and the Myelin Repair Foundation. This funding is not a competing interest in the context of the current article.
Author information
Authors and Affiliations
Contributions
All authors researched data for the article, made substantial contributions to discussions of the content, wrote the article, and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information S1 (video)
Coronal 3 T FLAIR* images (combination of coregistered T2*-weighted magnitude and T2-weighted fluid-attenuation inversion recovery images) from a 33-year-old woman with relapsing–remitting multiple sclerosis. A prominent central vein can be seen in the majority of lesions. (MP4 12448 kb)
Supplementary information S2 (video)
Dynamic contrast enhancement MRI shows a centripetally enhancing lesion (red arrow) in an untreated 49-year-old woman with progressive multiple sclerosis and radiological relapses. (MP4 2009 kb)
Supplementary information S3 (video)
Dynamic contrast enhancement MRI of a new periventricular centripetally enhancing lesion in a 33-year-old man with relapsing–remitting multiple sclerosis. Over a 20 min period, contrast material progressively and completely fills the lesion. (MP4 5843 kb)
Rights and permissions
About this article
Cite this article
Absinta, M., Sati, P. & Reich, D. Advanced MRI and staging of multiple sclerosis lesions. Nat Rev Neurol 12, 358–368 (2016). https://doi.org/10.1038/nrneurol.2016.59
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2016.59
- Springer Nature Limited
This article is cited by
-
Imaging of brain barrier inflammation and brain fluid drainage in human neurological diseases
Cellular and Molecular Life Sciences (2024)
-
Meningeal inflammation as a driver of cortical grey matter pathology and clinical progression in multiple sclerosis
Nature Reviews Neurology (2023)
-
Glia Connect Inflammation and Neurodegeneration in Multiple Sclerosis
Neuroscience Bulletin (2023)
-
The role of glial cells in multiple sclerosis disease progression
Nature Reviews Neurology (2022)
-
Prognostic Markers in Multiple Sclerosis
Neuroscience and Behavioral Physiology (2022)