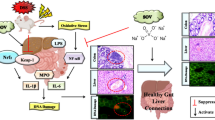
Abstract
Background
Ulcerative colitis is a chronic inflammatory condition in which the inflammatory response confined to the colon. There is a need to explore the new targets for UC such as Farnesoid X receptor and hydrogen sulfide pathway.
Methods
Wistar rats of either sex (200–250 g) were used. 2,4-Dinitrobenzene sulfonic acid (DNBS) (25 mg/rat) given by rectal route into the colon to induced symptoms of ulcerative colitis. Chenodeoxycholic acid (CDCA) (10 and 20 mg/kg) and sodium hydrogen sulfide (NaHS) (10 and 30 μmol/kg) and a inhibitor of cystathionine-γ-lyase enzyme (CSE) i.e. dl-propargylglycine (10 mg/kg) treatment given along with 2,4-dinitrobenzene sulfonic acid. The disease activity index was assessed by daily change in body weight and rectal bleed score and change in length of colon. Oxidative stress markers (reduced glutathione, malondialdehyde (MDA), nitrite, and catalase and myeloperoxidase enzyme activity), serum glutamic-oxaloacetic transaminase (SGOT) and serum glutamic pyruvic transaminase (SGPT) levels in blood serum, and cardiac hemodynamic were performed on last day.
Results
The administration of DNBS intra-rectally in rats produced loss of body weight and bloody diarrhea with significant increase in oxidative stress markers in the colon. CDCA (10 and 20 mg/kg) and NaHS (10 and 30 μmol/kg) significantly attenuated DNBS-induced UC in rats. The combination of CDCA (10 mg/kg) and NaHS (10 μmol/kg) showed synergetic effect whereas; dl-propargylglycine reversed the protective effect of CDCA.
Conclusion
The observed beneficial effects following CDCA may be due to its action through activation of CSE enzyme which leads to hydrogen sulfide generation.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Abbreviations
- 6E-CDCA:
-
6-ethyl chenodeoxycholic acid
- ALT:
-
alanine aminotransferase
- ANOVA:
-
analysis of variance
- AST:
-
aspartate aminotransferase
- CA:
-
cholic acid
- CDCA:
-
chenodeoxycholic acid
- CSE:
-
cystathionine-γ-lyase
- CaCl2:
-
calcium chloride
- CO2:
-
carbon dioxide
- DNBS:
-
2,4-dinitrobenzene sulfonic acid
- FXR:
-
Farnesoid X receptor
- GI:
-
gastrointestinal
- GSH:
-
glutathione
- H2O2:
-
hydrogen peroxide
- H2S:
-
hydrogen sulfide
- HOCl:
-
hypochlorous acid
- IBD:
-
inflammatory bowel disease
- IFN-γ:
-
interferon-γ
- IL:
-
interleukin
- iNOS:
-
inducible nitric oxide synthase
- KCl:
-
potassium chloride
- KH2PO4:
-
potassium hydrogen phosphate
- LPO:
-
lipid peroxidation
- LVEDP:
-
left ventricular end diastolic pressure
- MDA:
-
malondialdehyde
- MPO:
-
myeloperoxidase enzyme
- MgSO4:
-
magnesium sulfate
- NaCl:
-
sodium chloride
- NaHCO3:
-
sodium bicarbonate
- NaHS:
-
sodium hydrogen sulfide
- NO:
-
nitric oxide
- NSAID:
-
non steroidal anti-inflammatory drug ;O2oxygen
- PAG:
-
dl-propargylglycine
- SGOT:
-
serum glutamate oxaloacetate transaminase
- SGPT:
-
serum glutamate pyruvate transaminase
- TNBS:
-
2,4,6-trinitrobenzene sulfonic acid
- TNF-αtumor:
-
necrosis factor-α
- UC:
-
ulcerative colitis
References
Head KA, Jurenka JS. Inflammatory bowel disease Part 1: Ulcerative colitis – pathophysiology and conventional and alternative treatment options. Altern Med Rev 2003;8(3):247.
Rutgeerts P, Sandborn WJ, Feagan BG, Reinisch W, Olson A, Johanns J, et al. Infliximab for induction and maintenance therapy for ulcerative colitis. New Engl J Med 2005;353(23):2462–76.
Burisch J. Crohn’s disease and ulcerative colitis. Occurrence, course and prognosis during the first year of disease in a European population-based inception cohort. Dan Med J 2014;61(1):B4778.
Wallace JL, Le T, Carter L, Appleyard CB, Beck PL. Hapten-induced chronic colitis in the rat: alternatives to trinitrobenzene sulfonic acid. J Pharmacol Toxicol Methods 1995;33:237–9.
Goyal N, Rana A, Ahlawat A, Bijjem KRV, Kumar P. Animal models of inflammatory bowel disease: a review. Inflammopharmacology 2014;1–15.
Gadaleta RM, van Mil SW, Oldenburg B, Siersema PD, Klomp LW, van Erpecum KJ. Bile acids and their nuclear receptor FXR: relevance for hepatobiliary and gastrointestinal disease. BBA – Mol Cell Biol Lipids 2010;1801(7):683–92.
Vavassori P, Mencarelli A, Renga B, Distrutti E, Fiorucci S. The bile acid receptor FXR is a modulator of intestinal innate immunity. J Immunol 2009;183:6251–61.
Fiorucci S, Mencarelli A, Cipriani S, Renga B, Palladino G, Santucci L, et al. Activation of the Farnesoid-X receptor protects against gastrointestinal injury caused by non-steroidal anti-inflammatory drugs in mice. Br J Pharmacol 2011;164(8):1929–38.
Joshi SV, Vyas BA, Shah PD, Shah DR, Shah SA, Gandhi TR. Protective effect of aqueous extract of Oroxylum indicum Linn (root bark) against DNBS-induced colitis in rats. Indian J Pharmacol 2011;43(6):656.
Shifrin H, Nadler-Milbauer M, Shoham S, Weinstock M. Rivastigmine alleviates experimentally induced colitis in mice and rats by acting at central and peripheral sites to modulate immune responses. PLOS ONE 2013;8(2):e57668.
Wills ED. Mechanisms of lipid peroxide formation in animal tissues. Biochem J 1966;99:667–76.
Sastry KVH, Moudgal RP, Mohan J, Tyagi JS, Rao G. Spectrophotometric determination of serum nitrite and nitrate by copper–cadmium alloy. Anal Biochem 2002;306(1):79–82.
Ellman GL. Tissue sulfhydryl groups. Arch Biochem Biophys 1959;82(1):70–7.
Luck H. Catalase. In: Bergmeyer HU, editor. Methods of enzymatic analysis. New York: Academic Press; 1971. p. 885–93.
Langendorff O. Untersuchungen am iiberlebenden Saugetierherzen. Pflugers Archiv 1898;61:291–332.
Schirbel A, Fiocchi C. Inflammatory bowel disease: established and evolving considerations on its etiopathogenesis and therapy. J Dig Dis 2010;11:266–76.
Ordás I, Eckmann L, Talamini M, Baumgart DC, Sandborn WJ. Ulcerative colitis. Lancet 2012;380:1606–19.
Tran CD, Katsikeros R, Abimosleh SM. Current and Novel Treatments for Ulcerative Colitis. In: Shennak M, editor. Ulcerative Colitis from Genetics to Complications. InTech;ISBN: 2012978-953-307-853-3.https://doi.org/10.5772/25592.
Dothel G, Vasina V, Barbara G, Ponti FD. Animal models of chemically induced intestinal inflammation: predictivity and ethical issues. Pharmacol Ther 2013;139(1):71–86.
McCafferty DM. Peroxynitrite and inflammatory bowel disease. Gut 2000;46:436–9.
Wallace JL. Release of platelet-activating factor (PAF) and accelerated healing induced bya PAF antagonist in an animal model of chronic colitis. Can J Physiol Pharmacol 1988;66(4):422–5.
Cuzzocrea S, Mazzon E, Di Paola R, Patel NS, Genovese T, Muia C, et al. Erythropoietin reduces the development of experimental inflammatory bowel disease. J Pharmacol Exp Ther 2004;311(3):1272–80.
Xavier RJ, Podolsky DK. Unravelling the pathogenesis of inflammatory bowel disease. Nature 2007;448:427–34.
Gadaleta RM, van Erpecum KJ, Oldenburg B, Willemsen EC, Renooij W, Murzilli S, et al. Farnesoid X receptor activation inhibits inflammation and preserves the intestinal barrier in inflammatory bowel disease. Gut 2011. https://doi.org/10.1136/gut.2010.212159.
Wallace JL. Hydrogen sulfide-releasing anti-inflammatory drugs. Trends Pharmacol Sci 2007;28:501–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goyal, N., Rana, A., Bijjem, K.R.V. et al. Effect of chenodeoxycholic acid and sodium hydrogen sulfide in dinitro benzene sulfonic acid (DNBS) — Induced ulcerative colitis in rats. Pharmacol. Rep 67, 616–623 (2015). https://doi.org/10.1016/j.pharep.2014.12.018
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.pharep.2014.12.018