Abstract
The sleep–wake cycle is a process regulated by multiple neurobiological mechanisms that in aberrant functioning provokes several sleep disturbances. Among the major categories of sleep disorders, insomnia represents one of the most reported in population. Pharmacological interventions aimed for treating this sleep disturbance include compounds such as antidepressants, antihistamines, sedative-hypnotics, among others. However, using pharmacological treatments increase undesirable side effects such as addiction to sleep-inducing drugs. Here, we review and summarize recent publications available in PubMed regarding the use of non-pharmacological/invasive means to control insomnia, including physical exercise and transcranial direct current stimulation (tDCS). Current data suggest that these two strategies efficiently manage insomnia, and in turn opens new approaches to develop therapeutical tools to diminish this pathology. Nevertheless, additional research is required to understand the neurobiological mechanism of action of physical exercise and tDCS in insomnia control.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Insomnia
The sleep–wake cycle displays abnormal features characterized and classified in multiple sleep disturbances. In this regard, the International Classification of the Sleep Disorders defines insomnia as a pathology characterized by difficulties in either initiating or maintaining sleep, waking up across the night or earlier than desired in the morning [1]. Epidemiological studies have reported that insomnia is one of the most sleep disturbances in population [2]. Despite that different pharmacological treatments have been developed for managing insomnia, including benzodiazepines, benzodiazepine-receptor agonists, etc. [3,4,5,6], further side effects are often reported. Here, we review and summarize recent findings available in PubMed regarding the positive effects of using non-pharmacological/invasive means for managing insomnia, including physical exercise and transcranial direct current stimulation (tDCS).
2 Non-pharmacological Interventions for Managing Insomnia
Several reports have suggested that cognitive-behavioral therapy (CBT), mind–body therapies (such as yoga), light therapy, acupressure, physical exercise, tDCS, among others are becoming emerging/non-pharmacological options for managing insomnia [7,8,9,10,11,12,13]. In the following sections, we present a general overview of some recent publications regarding the uses of physical exercise and tDCS to control insomnia. In-depth examination of the use of less well-supported approaches (CBT, yoga, light therapy, acupressure, among others) is beyond the scope of this review.
2.1 Physical Exercise
Based in definition of insomnia, several approaches—including physical exercise—have been suggested for managing this sleep disorder. For instance, Crönlein [14] states that further research should define a standardized definition of sleep quality and use this definition to determine the effects of exercise and other interventions. Whether a standard definition of sleep quality is available, several studies have examined the effects of physical exercise in insomnia [15,16,17,18]. In this regard, older subjects (55–65 years old) diagnosed with insomnia participated in physical exercise conditions (morning exercise). Under these circumstances, morning exercise diminished the insomnia by decreasing the number of sleep state transitions over the night. Similar results were observed on self-reported quality of sleep, by describing that individuals with a high fitness level, which was associated with regular physical activity and exercise, perceived higher sleep quality. In contrast, participants with a self-reported lack of physical activity evaluated their sleep quality as poor [17]. In line with this observation, the sleep quality of 5000 women over 10 years showed that subjects that had a higher level of physical activity reported lower risks of developing insomnia [18]. Other studies have indicated that prolonged time of daily physical activity significantly reduced the risk of insomnia [16]. In this regard, Dzierzewski et al. [19] found that moderate to vigorous physical activity influenced the subjective sleep quality.
The resulting effects of physical exercise in insomnia management are thought to be mediated by thermoregulation [20]. Sleep onset is associated with a decline in body temperature, which is increased if physical exercise is applied between 2 and 6 pm. In response, the mechanisms of heat dissipation are activated and sleep is improved. Thus, one would assume that heating the body leads to an improvement of sleep [21, 22].
In addition, a variety of factors that influence the effects of physical exercise in insomnia control, include intensity, type of physical exercise and timing. Several lines of evidence suggest that moderate-intensity physical aerobic exercise in the afternoon using a treadmill [running speed at 4 km/h (3-min warm-up) with increments of 0.5 km/h every minute up to voluntary exhaustion during 50 min], but not after high-intensity physical aerobic exercise (3 periods of 10 min of exercise on a treadmill alternating with 10 min of rest) or moderate resistance physical exercise (shoulder/chest/leg press, vertical traction, leg curl/extension, abdominal crunch, or lower back. Three sets of 10 repetitions with 90-s recovery intervals during 50 min), decreases insomnia [23]. However, contradictory findings are available. For instance, a study compared the effects of acute morning or evening aerobic step physical exercise in two subjective insomnia criteria: difficulty in initiating sleep and early morning awakening. Results showed that acute physical exercise in the morning decreased the difficulties for initiating sleep but subjective sleep quality did not change after the acute interventions [24, 25].
The role of physical exercise in insomnia control might engage functioning of hormones. It has been demonstrate that acute physical exercise is linked with insomnia symptoms via cortisol levels since the contents of this hormone have been found increased after acute high-intensity training [26, 27]. An elevated cortisol levels in the evening correlate with the number of bouts of nocturnal awakenings in insomnia patients [28]. However, chronic moderate aerobic exercise using treadmill with an initial velocity of 4 km/h, increasing speed by 0.5 km/h each minute until voluntary exhaustion (3 times/week/4 months) decreased the cortisol levels, reduced sleep onset latency, and significantly increased total sleep time [29]. Although the mechanisms that underlie the interrelation between physical exercise and hormones functioning remain to be fully characterized, it seems that physical exercise exerts control of insomnia.
An additional variable that influences the effects of physical exercise in insomnia control is the timing of the intervention since early morning awakening seems to be associated with an advanced core body temperature rhythm [30]. Other studies have demonstrated that chronic moderate to high-intensity physical exercise interventions (step aerobics exercise 3 times/week/10 weeks at an intensity of 75–85% of the heart rate reserve during 45 min) modified the circadian rhythm, which is related with melatonin levels of individuals [31]. Opposite findings have been described by showing that low-intensity/chronic physical exercise exerts negative effects on the secretion of melatonin [32]. Despite the current evidence describes the relationship among physical exercise and melatonin release [33, 34], further studies are needed to clarify the mechanism of action that implies the interrelation of these two variables.
Insomnia also has been associated with an impaired immune function, such as lower levels of immune cells [35, 36]. Thus, the relationship between immune system and physical exercise might explain the positive effects of physical exercise in insomnia management. Nehlsen-Cannarella et al. [37] examined the role of moderate physical exercise training on the immune response finding changes in immune system such as immunoglobulins and T-cell subpopulation after 6–15 weeks of training.
On the other hand, moderate aerobic exercise showed positive trends towards increased total sleep time and decreased of awakening during sleep time [38]. In addition, the effects of an aerobic physical exercise in older adults with mild sleep impairments have demonstrated that the 8-week long intervention of 2 aquatic exercise sessions of 60 min/week lead to significant benefits on the sleep onset latency and the sleep efficiency [39]. Similar findings have been reported in this regard. For example, randomized controlled trials with physical exercise training programmes between 10 and 16 weeks, consisting of moderate to vigorous aerobic or resistance training with a dataset of over 300 participants with sleeping problems, showed positive effects on sleep quality as well as a sleep latency reduction [40]. Moreover, Hartescu et al. [41], published the outcomes of a randomized controlled trial in which the insomniac participants were instructed to walk at moderate-intensity for at least 30 min/day/5 days/week over a period of 6 months. The results of this intervention reduced the severity of insomnia symptoms and a significantly elevated mood. Thus, greater insomnia symptoms predict greater improvements in mood state after physical exercise [42].
In overall, the available literature suggests that acute as well as moderate physical exercise controls insomnia [43, 44]. Moreover, it is worthy to mention that long-term moderate-intensity aerobic exercises have shown to be more effective in managing insomnia over a prolonged period of time [23, 45,46,47].
2.2 Transcranial Direct Current Stimulation for Insomnia
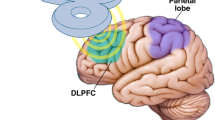
Transcranial direct current stimulation (tDCS) is a non-invasive brain stimulation technique that applies a low-intensity and continuous current that presumably induces cortical excitability changes [48]. tDCS has been used for multiple health purposes [48,49,50,51,52,53]. Regarding the use of tDCS in insomnia, the role of prefronto-thalamic-cerebellar circuit on cognitive dysfunctions and sleep quality in euthymic bipolar disorder (BD) patients have showed that tDCS (2 mA) for 20 min/day during 3 consecutive weeks applied to left dorsolateral prefrontal cortex (DLPFC) and right cerebellar cortex improved sleep [54]. It has been suggested that DLPFC and cerebellum play a relevant role in modulating sleep [55, 56]. Similar findings were reported by Galbiati et al. [57] since the effects of anodal tDCS applied to left DLPFC on arousal of patients with idiopathic hypersomnia during the 4 weeks/3 times/week reduced excessive daytime sleepiness. These results suggest that tDCS may modulate sleepiness in idiopathic patients [55,56,57].
Emerging research has demonstrated that application of slow oscillatory tDCS compared to sham-slow oscillatory tDCS decreased waking time [58,59,60]. These findings suggest a putative sleep-stabilizing role for slow oscillatory after tDCS in insomniacs [61, 62]. Despite the mechanism of action of tDCS in insomnia control remains to be described, it is thought that nitric oxide (NO) might be engaged in the control of insomnia. Recent evidence has shown that release of NO promotes sleep [63]. Following this idea, the gap junction permeability of neurons may be affect by NO, which in turn could activate sleep-related neurons that project to several areas of the central nervous system, including cerebral cortex [64]. Thus, it is suspected that slow oscillatory tDCS would increase NO production leading to sleep promotion. Nevertheless, future studies should be aimed to address this assumption. Besides, wider parameters for tDCS stimulation might be focus of further reports.
3 Conclusions
Insomnia is a sleep disorder reported in general population [1, 2]. Despite the wide spectrum of pharmacological options for treating insomnia [3,4,5,6, 65, 66], alternative non-pharmacological/invasive strategies for preventing and managing this sleep disturbance are emerging as an effective therapeutic option, including physical exercise as well as tDCS [7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47, 54,55,56,57, 60, 66,67,68] (Fig. 1).
In this regard, physical exercise controls insomnia in different approaches. For example, subjects with a high fitness level linked with physical activity and exercise, self-perceived higher sleep quality [16, 17]. In addition, moderate-intensity physical aerobic exercise in the afternoon using a treadmill, but not after high-intensity physical aerobic exercise (intense physical exercise in treadmill) or moderate resistance physical exercise (weightlifting), control insomnia [23]. On the other side, the use of tDCS for treating insomnia has limited exploration. Despite that few papers have been published in this regard, common findings have been described: application of tDCS to DLPFC and right cerebellar cortex decreases insomnia [54, 57]. Although the revised evidence suggests that physical exercise and tDCS manages insomnia [7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47, 54,55,56,57, 60,61,62,63,64,65,66,67,68], further studies should be aimed to verify if these two strategies fulfill international guidelines for managing insomnia, including the American Academy of Sleep Medicine or the European Sleep Research Society recommendations [3, 69, 70]. Likewise, as one can assume, timing, duration, and type of physical exercise displays different effectiveness in insomnia control. Same criteria for using tDCS by variables such as time, duration and intensity of stimulation. An additional issue to be addressed is the possible long-term effects of using physical exercise or tDCS in insomnia. Finally, the lack of data describing the mechanism of action of physical exercise or tDCS represents a gray area that needs to be addressed (Table 1).
References
American Academy of Sleep Medicine. International classification of sleep disorders: diagnostic coding manual, 3rd ed. Darien, IL, USA: American Academy of Sleep Medicine; 2014
Ancoli-Israel S, Roth T. Characteristics of insomnia in the United States: results of the 1991 National Sleep Foundation Survey. I. Sleep. 1999;22:S347–53.
Sateia MJ, Buysse DJ, Krystal AD, Neubauer DN, Heald JL. Clinical practice guideline for the pharmacologic treatment of chronic insomnia in adults: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2017;13:307–49.
Monti JM, Torterolo P, Perumal SRP. The effects of second generation antipsychotic drugs on sleep variables in healthy subjects and patients with schizophrenia. Sleep Med Rev. 2017;33:51–7.
Araújo T, Jarrin DC, Leanza Y, Vallières A, Morin CM. Qualitative studies of insomnia: current state of knowledge in the field. Sleep Med Rev. 2017;31:58–69.
Doufas AG, Panagiotou OA, Panousis P, Wong SS, Ioannidis JPA. Insomnia from drug treatments: evidence from meta-analyses of randomized trials and concordance with prescribing information. Mayo Clin Proc. 2017;92:72–87.
van Maanen A, Meijer AM, van der Heijden KB, Oort FJ. The effects of light therapy on sleep problems: a systematic review and meta-analysis. Sleep Med Rev. 2016;29:52–62.
Sadler P, McLaren S, Klein B, Jenkins M. Advancing cognitive behaviour therapy for older adults with comorbid insomnia and depression. Cogn Behav Ther. 2017;8:1–16.
Vitiello MV. Cognitive-behavioural therapy for insomnia is effective, safe and highly deployable. Evid Based Nurs. 2017;20:92.
van Maanen A, Meijer AM, Smits MG, van der Heijden KB, Oort FJ. Effects of melatonin and bright light treatment in childhood chronic sleep onset insomnia with late melatonin onset: a randomized controlled study. Sleep. 2017;40(2). https://doi.org/10.1093/sleep/zsw038.
Yeung WF, Ho FY, Chung KF, Zhang ZJ, Yu BY, Suen LK, Chan LY, Chen HY, Ho LM, Lao LX. Self-administered acupressure for insomnia disorder: a pilot randomized controlled trial. J Sleep Res. 2017 (In press).
Hayhoe S. Insomnia: can acupuncture help? Pain Manag. 2017;7:49–57.
Zhou ES, Gardiner P, Bertisch SM. Integrative medicine for insomnia. Med Clin North Am. 2017;101:865–79.
Crönlein T. Insomnia and obesity. Curr Opin Psychiatry. 2016;29:409–12.
Chen LJ, Steptoe A, Chen YH, Ku PW, Lin CH. Physical activity, smoking, and the incidence of clinically diagnosed insomnia. Sleep Med. 2017;30:189–94.
Morita Y, Sasai-Sakuma T, Inoue Y. Effects of acute morning and evening exercise on subjective and objective sleep quality in older individuals with insomnia. Sleep Med. 2017;34:200–8.
Gerber M, Brand S, Holsboer-Trachsler E, Pühse U. Fitness and exercise as correlates of sleep complaints: is it all in our minds? Med Sci Sports Exerc. 2010;42:893–901.
Spörndly-Nees S, Åsenlöf P, Lindberg E. High or increasing levels of physical activity protect women from future insomnia. Sleep Med. 2017;32:22–7.
Dzierzewski JM, Buman MP, Giacobbi PR, Roberts BL, Aiken-Morgan AT, Marsiske M, McCrae CS. Exercise and sleep in community-dwelling older adults: evidence for a reciprocal relationship. J Sleep Res. 2014;23:61–8.
Montgomery PI, Dennis J. Physical exercise for sleep problems in adults aged 60+. Cochrane Database Syst Rev. 2002;(4):CD003404. https://doi.org/10.1002/14651858.CD003404.
Horne JA, Staff LHE. Exercise and sleep: body-heating effects. Sleep. 1983;6:36–46.
Passos GS, Poyares DLR, Santana MG, Tufik S, Mello MT. Is exercise an alternative treatment for chronic insomnia? Clinics. 2012;67:653–60.
Passos GS, Poyares D, Santana MG, Tufik S, de Mello MT. Effect of chronic physical exercise on anxiety in patients with chronic primary insomnia. Sleep Med. 2009;10:S19.
Caspersen CJ, Powell KE, Christenson GM. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep. 1985;2:126–31.
Brand S, Kalak N, Gerber M, Kirov R, Pühse U, Holsboer-Trachsler E. High self-perceived exercise exertion before bedtime is associated with greater objectively assessed sleep efficiency. Sleep Med. 2014;15:1031–6.
Bonato M, La Torre A, Saresella M, Marventano I, Merati G, Vitale JA. Salivary cortisol concentration after high-intensity interval exercise: time of day and chronotype effect. Chronobiol Int. 2017;34:698–707.
Budde H, Machado S, Ribeiro P, Wegner M. The cortisol response to exercise in young adults. Front Behav Neurosci. 2015;9:13.
Chen G, Xia L, Wang F, Li X, Jiao C. Patients with chronic insomnia have selective impairments in memory that are modulated by cortisol. Psychophysiology. 2016;53:1567–76.
Passos GS, Poyares D, Santana MG, Teixeira AADS, Lira FS, Youngstedt SD, Santos RVT, Tufik S, De Mello MT. Exercise improves immune function, antidepressive response, and sleep quality in patients with chronic primary insomnia. Biomed Res Int. 2014;2014:1–7.
Lack LC, Gradisar M, Van Someren EJW, Wright HR, Lushington K. The relationship between insomnia and body temperatures. Sleep Med Rev. 2008;12:307–17.
Cai ZY, Chen KWC, Wen HJ. Effects of a group-based step aerobics training on sleep quality and melatonin levels in sleep-impaired postmenopausal women. J Strength Cond Res. 2014;28:2597–603.
Kim HJ, Kim DH. Effect of different exercise intensity on blood melatonin density in sleep disordered rats. J Korean Soc Phys Med. 2014;9:45–53.
Atkinson G, Edwards B, Reilly T, Waterhouse J. Exercise as a synchroniser of human circadian rhythms: an update and discussion of the methodological problems. Eur J Appl Physiol. 2007;99:331–41.
Escames G, Ozturk G, Baño-Otálora B, Pozo MJ, Madrid JA, Reiter RJ, Serrano E, Concepción M, Acuña-Castroviejo D. Exercise and melatonin in humans: reciprocal benefits. J Pineal Res. 2012;52:1–11.
Imeri L, Opp MR. How (and why) the immune system makes us sleep. Nat Rev Neurosci. 2009;10:199–210.
Cover H, Irwin M. Immunity and depression: insomnia, retardation, and reduction of natural killer cell activity. J Behav Med. 1994;17:217–23.
Nehlsen-Cannarella SL, Nieman DC, Balk-Lamberton AJ, Markoff PA, Chritton DB, Gusewitch G, Lee JW. The effects of moderate exercise training on immune response. Med Sci Sports Exerc. 1991;23:64–70.
Guilleminault C, Clerk A, Black J, Labanowski M, Pelayo R, Claman D. Nondrug treatment trials in psychophysiologic insomnia. Arch Intern Med. 1995;155:838–44.
Chen LJ, Fox KR, Ku PW, Chang YW. Effects of aquatic exercise on sleep in older adults with mild sleep impairment: a randomized controlled trial. Int J Behav Med. 2016;23:501–6.
Yang PY, Ho KH, Chen HC, Chien MY. Exercise training improves sleep quality in middle-aged and older adults with sleep problems: a systematic review. J Physiother. 2012;58:157–63.
Hartescu I, Morgan K, Stevinson CD. Increased physical activity improves sleep and mood outcomes in inactive people with insomnia: a randomized controlled trial. J Sleep Res. 2015;24:526–34.
Rouleau CR, Horsley KJ, Morse E, Aggarwal S, Bacon SL, Campbell TS. The Association between insomnia symptoms and mood changes during exercise among patients enrolled in cardiac rehabilitation. J Cardiopulm Rehabil Prev. 2015;35:409–16.
Kredlow MA, Capozzoli MC, Hearon BA, Calkins AW, Otto MW. The effects of physical activity on sleep: a meta-analytic review. J Behav Med. 2015;38:427–49.
Mendelson M, Borowik A, Michallet A, Perrin C, Monneret D, Faure P, Levy P, Pépin J, Wuyam B, Flore P. Sleep quality, sleep duration and physical activity in obese adolescents: effects of exercise training. Pediatr Obes. 2016;11:26–32.
Schmitt A, Falkai P. Aerobic exercise in major psychiatric disorders: promises and challenges. Eur Arch Psychiatry Clin Neurosci. 2017;267:93–4.
Reid KJ, Baron KG, Lu B, Naylor E, Wolfe L, Zee PC. Aerobic exercise improves self-reported sleep and quality of life in older adults with insomnia. Sleep Med. 2010;11:934–40.
Patel SR, Zhu X, Storfer-Isser A, Mehra R, Jenny NS, Tracy R, Redline S. Sleep duration and biomarkers of inflammation. Sleep. 2009;32:200–4.
Lattari E, Costa SS, Campos C, De Oliveira AJ, Machado S, Neto GAM. Can transcranial direct current stimulation on the dorsolateral prefrontal cortex improves balance and functional mobility in Parkinson’s disease? Neurosci Lett. 2017;63:6165–9.
Dondé C, Amad A, Nieto I, Brunoni AR, Neufeld NH, Bellivier F, Poulet E, Geoffroy PA. Transcranial direct-current stimulation (tDCS) for bipolar depression: a systematic review and meta-analysis. Prog Neuropsychopharmacol Biol Psychiatry. 2017;78:123–31.
Philip NS, Nelson BG, Frohlich F, Lim KO, Widge AS, Carpenter LL. Low-intensity transcranial current stimulation in psychiatry. Am J Psychiatry. 2017;174:628–39.
Göbel CH, Tronnier VM, Münte TF. Brain stimulation in obesity. Int J Obes. 2017 (In press).
ALHarbi MF, Armijo-Olivo S, Kim ES. Transcranial direct current stimulation (tDCS) to improve naming ability in post-stroke aphasia: a critical review. Behav Brain Res. 2017;332:7–15.
Weinberger AB, Green AE, Chrysikou EG. Using transcranial direct current stimulation to enhance creative cognition: interactions between task, polarity, and stimulation site. Front Hum Neurosci. 2017;11:246.
Minichino A, Bersani FS, Spagnoli F, Corrado A, De Michele F, Calò WK, Primavera M, Yang B, Bernabei L, Macrì F. Prefronto-cerebellar transcranial direct current stimulation improves sleep quality in euthymic bipolar patients: a brief report. Behav Neurol. 2014;2014:876521.
McKenna BS, Eyler LT. Overlapping prefrontal systems involved in cognitive and emotional processing in euthymic bipolar disorder and following sleep deprivation: a review of functional neuroimaging studies. Clin Psychol Rev. 2012;32:650–63.
DelRosso LM, Hoque R. The cerebellum and sleep. Neurol Clin. 2014;32:893–900.
Galbiati A, Abutalebi J, Iannaccone S, Borsa VM, Musteata S, Zucconi M, Giora E, Ferini-Strambi L. The effects of transcranial direct current stimulation (tDCS) on idiopathic hypersomnia: a pilot study. Arch Ital Biol. 2016;154:1–5.
de Sá AS, Campos C, Rocha NB, Yuan TF, Paes F, Arias-Carrión O, Carta MG, Nardi AE, Cheniaux E, Machado S. Neurobiology of bipolar disorder: abnormalities on cognitive and cortical functioning and biomarker levels. CNS Neurol Disord Targets. 2016;15:713–22.
Pedroso JL, Braga-Neto P, Felício AC, Aquino CCH, Prado LB, Prado GFD, Barsottini OGP. Sleep disorders in cerebellar ataxias. Arq Neuropsiquiatr. 2011;69:253–7.
Saebipour MR, Joghataei MT, Yoonessi A, Sadeghniiat-Haghighi K, Khalighinejad N, Khademi S. Slow oscillating transcranial direct current stimulation during sleep has a sleep-stabilizing effect in chronic insomnia: a pilot study. J Sleep Res. 2015;24:518–25.
Dang-Vu TT, Schabus M, Desseilles M, Albouy G, Boly M, Darsaud A, Gais S, Rauchs G, Sterpenich V, Vandewalle G. Spontaneous neural activity during human slow wave sleep. Proc Natl Acad Sci. 2008;105:15160–5.
Kaufmann C, Wehrle R, Wetter TC, Holsboer F, Auer DP, Pollmächer T, Czisch M. Brain activation and hypothalamic functional connectivity during human non-rapid eye movement sleep: an EEG/fMRI study. Brain. 2005;129:655–67.
Morairty SR, Dittrich L, Pasumarthi RK, Valladao D, Heiss JE, Gerashchenko D, Kilduff TS. A role for cortical nNOS/NK1 neurons in coupling homeostatic sleep drive to EEG slow wave activity. Proc Natl Acad Sci. 2013;110:20272–7.
Gerashchenko D, Wisor JP, Kilduff TS. Sleep-active cells in the cerebral cortex and their role in slow-wave activity. Sleep Biol Rhythms. 2011;9:71–7.
Maness DL, Khan M. Nonpharmacologic management of chronic insomnia. Am Fam Physician. 2015;92:1058–64.
Hollenbach D, Broker R, Herlehy S, Stuber K. Non-pharmacological interventions for sleep quality and insomnia during pregnancy: a systematic review. J Can Chiropr Assoc. 2013;57:260–70.
Dolezal BA, Neufeld EV, Boland DM, Martin JL, Cooper CB. Interrelationship between sleep and exercise: a systematic review. Adv Prev Med. 2017;2017:1364387.
Milne S, Elkins MR. Exercise as an alternative treatment for chronic insomnia (PEDro synthesis). Br J Sports Med. 2017;51:479–80.
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, Harrod CG. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2017;13:479–504.
Riemann D, Baglioni C, Bassetti C, Bjorvatn B, Dolenc Groselj L, Ellis JG, Espie CA, Garcia-Borreguero D, Gjerstad M, Gonçalves M, Hertenstein E, Jansson-Fröjmark M, Jennum PJ, Leger D, Nissen C, Parrino L, Paunio T, Pevernagie D, Verbraecken J, Weeß HG, Wichniak A, Zavalko I, Arnardottir ES, Deleanu OC, Strazisar B, Zoetmulder M, Spiegelhalder K. European guideline for the diagnosis and treatment of insomnia. J Sleep Res. 2017 (In press).
Funding
This work was supported by The University of California Institute for Mexico and the United States (UC MEXUS) and Consejo Nacional de Ciencia y Tecnología (CONACyT. Grant CN-17-19) and Escuela de Medicina, Universidad Anáhuac Mayab Grant (PresInvEMR2017) given to EM-R.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
All data reported in this paper are from public repositories.
Conflict of interest
Authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Higuera-Hernández, M.F., Reyes-Cuapio, E., Gutiérrez-Mendoza, M. et al. Alternative Strategies for Managing Insomnia: The Case of Physical Exercise and Transcranial Direct Current Stimulation. A Narrative Review. Sleep Vigilance 2, 39–44 (2018). https://doi.org/10.1007/s41782-018-0037-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41782-018-0037-x