Abstract
Introduction
The pathogenesis and clinical profiles of patients with pulmonary hypertension (PH) associated with interstitial lung disease (ILD-PH) are poorly understood. Whether and to what extent pulmonary arterial hypertension (PAH)-specific therapy improves hemodynamic and outcome in ILD-PH are also unknown.
Study Objective
This study aims to clarify the characteristics, clinical course and response to PAH-specific therapy of ILD and/or PH by enrolling three unique subsets: PAH, ILD-PH, and ILD.
Methods
The proposed study is a retrospective and prospective, multi-centre, observational cohort study of patients treated at any of three university hospitals in the Hokkaido region of Japan who have any one of the following: PAH; ILD-PH with or without PAH features; or ILD without PH. We aim to enrol 250 patients in total. For the retrospective observation period, data obtained after 1 January 2010, will be analysed, and the prospective observation period will be 1 year. We will compare the clinical data of patients with ILD-PH with those of patients with PAH and those of patients with ILD without PH in the real-world clinical setting. In addition, within the cohort of patients with ILD-PH, we will explore the subset with “ILD-PH with PAH features” and compare the response to PAH-specific therapy with that of PAH. The primary outcome will be the change in pulmonary vascular resistance from first treatment to follow-up in patients with PAH and ILD-PH with PAH features (excluding ILD-PH without PAH feature and ILD-no-PH for the primary outcome). The exploratory outcomes will include analyses of PH-associated biomarkers, right ventricular function and patient-reported outcomes.
Results
This is a protocol article and the results will be presented after data collection is completed.
Conclusion
The POPLAR study will provide data that help better understand the pathophysiology of ILD-PH and improve the quality of life and outcome of patients with PH and/or ILD.
Trial Registration
Japan Registry of Clinical Trials: jRCT1010230018.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Why carry out this study? |
The prognosis of pulmonary hypertension (PH) associated with interstitial lung disease (ILD) remains very poor. |
Limited data are available regarding the underlying mechanisms and association between treatment patterns and prognosis of ILD-associated PH and the safety/efficacy of PAH-specific therapy in the affected patients. |
What was learned from the study? |
The present retrospective and prospective study will improve current understanding of the responder/non-responder profile to PAH-specific therapy in patients with PAH and those with ILD-associated PH. |
The ILD with/without PH cohort in this study may help elucidate the pathogenesis and clinical course of PH in ILD. |
This study will provide data on pulmonary haemodynamics, pulmonary/cardiac imaging, patient-reported outcomes and biomarkers that are useful to improve treatment, quality of life and the prognosis of patients with ILD and PH, as well as those with ILD alone and PAH. |
Introduction
Pulmonary hypertension (PH) is a pathophysiological disorder characterized by mean pulmonary arterial pressure (mPAP) > 20 mmHg on right heart catheterization (RHC) [1] and is classified into groups 1–5 according to the aetiology. Some classes of PH are recognized as intractable diseases in Japan. Group 3 PH is defined as PH associated with lung disease and/or hypoxemia, such as interstitial lung disease (ILD) [1] (ILD-PH). ILD-PH is associated with reduced exercise capacity, the need for supplemental oxygen, poor quality of life and poor prognosis [2,3,4]. Pulmonary arterial hypertension (PAH) features in patients with group 3 ILD-PH have been reported, further complicating the condition. Several concepts, such as ‘PAH phenotype’, ‘out-of-proportion PH’ and “pulmonary vascular resistance (PVR) > 5 Wood Units (WU) as severe PH criteria”, have been proposed to describe this complicated condition, and these have become reflected in clinical practice guidelines [2, 5,6,7]. However, it remains unknown why PH develops in only a subset of patients with ILD. In addition, the natural course, response to pulmonary vasodilators and prognostic factors of ILD-PH are not well characterized.
Among the various subtypes of PH, ILD-PH is one of the most fatal conditions that patients and clinicians face because of the lack of effective treatments [8, 9]. Some trials have demonstrated no clinical benefit with pulmonary vasoactive drugs [10, 11], and poor haemodynamic response to a pulmonary vasodilator has also been reported in patients with ILD-PH [12]. However, several studies have obtained promising results with PAH-specific therapy [13,14,15]. Given the controversy around the effectiveness of PAH-specific therapy for ILD-PH and the lack of a definition for PAH features in ILD-PH, PAH-specific therapy is not indicated for ILD-PH in most countries. Currently, European Society of Cardiology (ESC)/European Respiratory Society (ERS) guidelines do not routinely recommend PAH medications in patients with ILD with non-severe PH [5], but PAH-specific treatment is available in several countries. In Japan, PAH-specific therapy is reimbursed for patients with “PAH with lung diseases” if the treatment decision can be adequately supported by the results of careful clinical assessments for PH patients with ILD complications. As a result, a considerable number of patients with ILD-PH have been receiving PAH-specific therapy in Japan and some other parts of the world.
A variety of biomarkers are used in the practice of ILD and PH. For example, KL6 and brain natriuretic peptide (BNP)/N-terminal pro-brain natriuretic peptide (NT-proBNP) are established biomarkers for the diagnosis and monitoring of ILD and PH, respectively [5, 16]. In addition, the development of other proteins and microRNAs related to inflammation or cell proliferation as new biomarkers is expected [17,18,19,20], although their clinical value has yet to be established. Alternatively, the clinical value of tools such as computed tomography (CT), cardiac magnetic resonance imaging (CMR) [21, 22], assessment of right ventricular (RV) function [23] and patient-reported outcomes (PROs) [24] have been reported in PAH and/or ILD. However, again, the clinical relevance of these modalities and indices remains to be elucidated for patients with ILD-PH.
Therefore, we aim to describe the differences in patient characteristics, clinical course and treatment response to PAH-specific therapy between patients with PAH and those with ILD-PH with PAH features in the real-world setting. In addition, by analysing biomarkers, CT/CMR images, RV function indices and PRO data, we aim to better characterize ILD-PH with or without PAH features, as compared with PAH and ILD without PH. This information will improve our understanding of the pathogenesis, early diagnosis and appropriate management of ILD with PH.
Methods
Study Design
The proposed study is a retrospective and prospective, multi-centre, observational study to be conducted in Hokkaido, Japan (Fig. 1). The study settings adopted a mixture of retrospective and prospective study due to our limited study scope in dealing with rare, intractable diseases; the enrolment of a large number of participants is expected to be difficult.
In the prospective recruitment period, participating sites will prospectively enrol patients when patients attend their regular visit in order to minimize selection bias. At each site, the participating physician will assess the patients to determine their eligibility for data collection. Enrolment will stop when the maximum number of patients in each group has been reached. After study entry, the patients will enter the 1-year observation period.
For prevalent patients, medical records will be retrospectively reviewed up to 1 January 2010, to identify the correct index dates for the first ILD diagnosis, first PH diagnosis, first PAH-specific therapy (endothelin receptor antagonists, phosphodiesterase type-5 inhibitors, soluble guanylate cyclase stimulators, prostaglandin I2 and prostaglandin I2 agonist) and first follow-up after PAH-specific therapy (3–6 months after drug therapy), as appropriate.
Figure 2 shows the study schema for prevalent and incident patients. The end of the study will be the last data collection point for the last participating patient. The total study duration, including prospective enrolment (1.5 years: from October 2023 through March 2025) and prospective observation (1 year from each patient’s enrolment: the prospective observation period of the last patient will end in March 2026), will be 2.5 years.
Study Objectives
The objectives of this study are: (1) to clarify the differences in haemodynamic response to PAH-specific therapy between patients with PAH and those with ILD-PH with PAH features; (2) to elucidate the characteristics of ILD-PH in terms of biomarker profile, CT and CMR images, RV function, PRO data and clinical course as compared with those of PAH or ILD without PH; and (3) to exploratory characterize the subset of ‘ILD-PH with PAH features’ using a tentative definition described below.
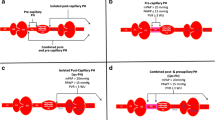
Regarding the first objective, it can be hypothesized that the response to PAH-specific therapy is poorer in ILD-PH than in PAH based on prior reports. Corte et al. reported that the PVR index decreased only slightly (− 1.1 WU from 13.9 WU/m2) in patients with ILD-PH treated with bosentan [12], whereas the same treatment reduced PVR by 16.8% in patients with PAH [25]. However, some small studies, including our previous study, have shown a favourable response to PAH-specific therapy in ILD-PH [14, 26]. Thus, in the present study, we aimed to assure that the vasodilatory effect of PAH-specific therapy is less in ILD-PH than in PAH. Regarding the second objective, abundant studies have reported the clinical values of biomarkers, CT/CMR and PRO analysis in PAH and ILD. However, most of these studies have targeted PAH or ILD alone, and limited data are available for ILD-PH. Thus, in the present study, we aim to identify clinical data that are specific to ILD-PH as compared with PAH or ILD alone, which may be useful for early diagnosis and better management of ILD-PH. Finally, using a tentative definition of “PAH feature”, we aim to identify distinct characteristics of this subset, for example in the biomarker profile, lung parenchyma/vascular morphology and RV morphology or function. In addition, using quantitative CT data and PVR, we are going to draw a scatter plot, as shown in Fig. 3, which will aid in identifying the subset of ILD-PH with PAH features.
Hypothesis. We hypothesize that patients with ILD-PH with PAH features will respond to PAH therapy and will demonstrate a greater improvement in key measures, such as PVR, than patients with ILD-PH without PAH features and those not on PAH therapy. We also hypothesize that the baseline characteristics will differ between patients with ILD-PH with and without PAH features, such as biomarker and imaging analysis results. HRCT High-resolution computed tomography, ILD interstitial lung disease, PAH pulmonary arterial hypertension, PH pulmonary hypertension, PVR pulmonary vascular resistance, WU wood units
Geographics and Study Population
This study will be conducted in Hokkaido, Japan (Fig. 1). The geographic advantages of this study are that: (1) patients with ILD-PH with PAH features in Japan are treated with PAH-specific therapy; (2) Hokkaido has centralized research sites for PH/PAH treatment (3 university hospitals); (3) all research sites have a homogeneous respiratory/cardiovascular collaboration platform for PH/PAH treatment; and (4) the probability of patients with PH/PAH visiting hospitals outside of Hokkaido is low. Study participants will be recruited from outpatients or inpatients treated at any of these three university hospitals for PAH, ILD-PH with PAH features, ILD-PH without PAH features or ILD-no PH (newly diagnosed [incident] or previously diagnosed before study entry [prevalent]).
Sample Size
The sample sizes for PAH and ILD-PH were planned at 70 and 90 patients, respectively, which were determined based on an estimation of eligible patient numbers from all participating sites. A comparable number of participants (n = 90) with ILD-no PH will be enrolled to support the exploratory analyses of ILD-PH versus ILD-no PH. In this study, no sample size calculations were performed because of the rarity of PAH and ILD-PH, particularly of newly diagnosed cases in the participating hospitals.
Inclusion and Exclusion Criteria
The inclusion criteria will be: (1) male or female patients aged ≥ 20 years at the time of initial PH or ILD diagnosis; (2) diagnosis of PAH, ILD-PH with or without PAH features, or ILD-no PH (incident or prevalent); (3) patients treated as outpatients or inpatients at any of the three sites where specialty care for ILD and PH is provided; and (4) patients who provided written informed consent to participate in the study. Patients diagnosed with PAH will be enrolled, including all subgroups (idiopathic PAH/heritable PAH, connective tissue disease [CTD]-PAH, congenital heart disease-PAH, portopulmonary hypertension, etc.). Patients diagnosed with ILD will be enrolled from the following subdivisions: idiopathic pulmonary fibrosis, idiopathic non-specific interstitial pneumonia, unclassifiable idiopathic interstitial pneumonia, chronic hypersensitivity pneumonitis, CTD-associated ILD and combined pulmonary fibrosis and emphysema. Comprehensive autoantibody test data will be collected and considered in the analysis of CTD-associated ILDs.
The exclusion criteria will be: (1) a diagnosis of group 2, 4, or 5 PH, including sarcoidosis PH; (2) a diagnosis of group 3 ILD-PH without PAH features in patients having received treatment for PAH before baseline; (3) a diagnosis of ILD that is expected to change rapidly, such as respiratory infection and drug-induced pneumonia; (4) first ILD or PH diagnosis before 1 January 2010; and (5) patient is deemed inappropriate for participation by the principal investigator.
Diagnosis
Pulmonary arterial hypertension will be diagnosed according to the following criteria: mPAP > 20 mmHg; pulmonary artery wedge pressure (PAWP) ≤ 15 mmHg; and PVR > 2 WU, in accordance with the 2022 ESC/ERS guidelines for PH diagnosis [5]. Limited ILD will be acceptable as a coexisting condition as PAH cohort in the study. The method described by Goh et al. [27] will be applied to ensure the correct classifications of PAH and ILD-PH, respectively. ILD-PH will be diagnosed according to the Guidance for Diagnosis and Treatment of Idiopathic Interstitial Pneumonia, third edition [28]. There is no established definition for ‘PAH features’; therefore, the presence or absence of PAH features will be concluded if all of the following criteria are met: (1) stable ILD on lung high-resolution CT (HRCT) and/or pulmonary function tests for at least 6 months; (2) progressive and severe PH, considered as such based on patients’ symptoms/signs, BNP/NT-proBNP, echocardiographic parameters and/or RHC data; and (3) treating physician’s judgment that PAH-specific therapy would be clinically beneficial. PVR > 5 WU will be not set as the criteria for PAH features in this study, taking into consideration the actual clinical practice at this time. Baseline PVR (whether the PVR is > 5 WU or < 5 WU) will be considered during data analysis. ILD-no PH will be defined as fulfilment of the ILD diagnostic criteria [28] and absence of PH, defined as an mPAP ≤ 20 mmHg according to RHC, or if RHC is not performed, a tricuspid regurgitant pressure gradient (TRPG) ≤ 31 mmHg on echocardiography and %DLCO (diffusing capacity of the lung for carbon monoxide) > 50% on pulmonary function testing [29]. The severity of lung parenchymal damage in ILD and whether each patient is considered to have “PAH feature” are determined by the patient’s physician as well as by the judgment at the time of data analysis by ≥ 2 independent pulmonologists assigned for this study. The determination will be based on CT evaluation according to Goh et al. [27].
Data Collection and Management
The primary data source will be participants’ medical records. Data collection for each participant will be considered to be complete if all data accumulated for 1 year from study entry have been collected. Only patients with complete information for a given assessment will be included in the analysis of that assessment; missing data of each participant in the collection items will not be imputed. A participant will be withdrawn from data collection if: (1) they request withdrawal or withdraw consent; (2) they are lost to follow-up; (3) the entire study is discontinued; or (4) the principal investigator considers it appropriate to withdraw the participant. In cases of death or loss to follow-up during the 1 year observation period, the data collected until death (including cause of death) or loss to follow-up will be analysed, unless consent is withdrawn. The monitors assigned to the study will review the medical records of all patients who participated in the study on site and will review the data on the case report forms to confirm eligibility.
Outcome Measures and Survey Items
The data collection schedules for prevalent and incident patients are shown in Tables 1 and 2, respectively. The primary outcome of interest will be the change in PVR from baseline (before the first treatment) to follow-up at 3–6 months, which will be compared between patients with PAH and patients with ILD-PH with PAH features.
The secondary outcomes of interest will be (from baseline to follow-up at 3–6 months): (1) change in mPAP (in patients with PAH and ILD-PH with PAH features); (2) changes in echocardiography parameters (TRPG, tricuspid annular plane systolic excursion, eccentricity index, RV end-systolic area) in patients with PAH and ILD-PH with PAH features; (3) changes in pulmonary function test-derived measures (forced vital capacity [FVC], forced expiratory volume in 1 s [FEV1], FEV1/FVC ratio, total lung capacity, DLCO, DLCO divided by alveolar volume) in patients with PAH and ILD-PH with PAH features; (4) changes in CMR-derived measures (RV ejection fraction, RV stroke volume, RV end-diastolic volume, RV end-systolic volume, RV mass) in incident patients with PAH and incident ILD-PH with PAH features; and (5) changes in CMR-derived and RHC-derived parameters (cardiac index, pulmonary arterial compliance, and indices of RV function and RV–pulmonary arterial coupling [end-systoilc elastance (Ees), stiffness constant, end-diastolic elastance (Eed) and Ees/Ea]) in incident patients with PAH and incident ILD-PH with PAH features. The methodology that will be used to calculate the indices of RV function and RV–pulmonary arterial coupling has been reported previously [30].
Other exploratory outcomes will be: (1) time to first clinical deterioration (defined by [1] all-cause death; [2] hospitalization related with ILD or PH; [3] addition or dose increase of medication for PAH; and [4] initiation or dose increase of steroid or immunosuppressant for ILD) during the 1-year prospective observation period (in patients with PAH, ILD-PH and ILD-no PH); (2) number and reason(s) for hospitalization(s)/death during the 1-year prospective observation period (in patients with PAH, ILD-PH and ILD-no PH, respectively); (3) change in health-related quality of life (according to the EmPHasis-10 questionnaire) from study entry to 1 year (in patients with PAH and ILD-PH, respectively); (4) change in other PROs (Short-Form Health Survey-36, King’s Brief ILD Questionnaire, Epworth Sleepiness Scale and Zung Self-Rating Depression Scale) from study entry to 1 year (in patients with PAH, ILD-PH and ILD-no PH) respectively; (5) change in echocardiography-derived measures from study entry to 1 year (in incident patients with PAH, ILD-PH and ILD-no PH, respectively); (6) change in RHC-derived and CMR-derived measures from study entry to 1 year (in incident patients with PAH and ILD-PH, respectively); and (7) biomarker analysis (including microRNA, blood tests, PH-related genetic analysis and imaging studies). In addition, when the participants are hospitalized or have died, the reason for the hospitalization or death will be specified as one of the following eight categories: 1, PH alone; 2, ILD alone; 3, single cause other than PH and ILD; 4, PH + ILD; 5, PH + α; 6, ILD + α; 7, PH + ILD + α; 8, unknown, based on the method reported previously [31, 32]. Note: α means any factor other than PH or ILD that contributed to hospitalization or death. The rationale for the decision to add or increase PAH medications and the validity of the clinical outcomes will be confirmed with other clinical data by ≥ 2 independent pulmonologists, as well as the independent judgment of the CT evaluation.
Drug classes, names, doses and start/end dates for PAH-specific therapies and concomitant medications will be collected. This drug information and treatment regimen (mono-, dual and triple therapy) will be used to analyse the effect on the endpoints in each cohort.
Statistical Analysis
Descriptive statistics will be summarized (mean ± standard deviation; median and quartiles; and absolute numbers with percentages, as appropriate). Clinical parameters (continuous variables) at baseline versus at follow-up will be compared using the paired t-test or Wilcoxon’s signed-rank test for each diagnostic group. Clinical parameters will be compared among the diagnostic groups using the analysis of covariance. The time to clinical deterioration will be analysed using the Kaplan–Meier method and the log-rank test to compare between patients with PAH and those with ILD-PH with PAH features, those with ILD-PH without PAH features and those with ILD-no PH. Multivariate Cox proportional hazard model will be used to identify factors associated with the PAH treatment response and other clinical outcomes. Subgroup analysis will be performed on variables related to disease types, treatment types/durations, disease stages and either incident or prevalent patients. P < 0.05 will be considered to be statistically significant.
Ethics/Ethical Approval
Written informed consent will be obtained from all participants, including the consent for publication of the study. The decision of patients to participate will not impact their standard of care, and the treatment decision will have been made prior to and independently of the patient’s inclusion. All aspects of treatment and clinical management will be in accordance with local clinical practice and applicable local regulations, and at the discretion of the participating (or treating) physician. The Hokkaido University Hospital Clinical Research Supervision Center Biomedical Research Ethics Review Board approved the study protocol (No. 023-0067) on 14 June 2023, and the study is registered in the Japan Registry of Clinical Trials (jRCT1010230018). The Asahikawa Medical University Research Ethics Committee approved the study protocol (No. C2315) on 31 July 2023 and the Sapporo Medical University Hospital Institutional Review Board approved the study protocol (No. 352-95) on 24 August 2023. The study will be performed in accordance with the principles of the Declaration of Helsinki and the Ethical Guidelines for Life Science and Medical Research Involving Human Patients (Notification No. 1 of the Ministry of Education, Culture, Sports, Science and Technology/Ministry of Health, Labour and Welfare/Ministry of Economy, Trade and Industry in 2021).
Discussion
This is the first study to describe and clarify the characteristics and clinical course of Japanese patients with ILD-PH with or without PAH features, PAH and ILD-no PH in the clinical practice setting. We expect this aim will be achieved by evaluating the inpatients and outpatients centralized at three research sites with a homogeneous respiratory/cardiovascular collaboration platform in Hokkaido, Japan.
Despite the high unmet medical need of ILD-PH, there is an insufficient understanding of the clinical profiles of patients with ILD-PH who may benefit from PAH therapy, as well as the degree of clinical benefit that may be achieved with PAH therapy. The reason for this are the lack of an established definition to determine which patients are eligible for PAH-specific therapy, as well as the lack of evidence on how best to treat these patients (e.g. type of treatment, single or combined regimens and when changes should be made to the treatment regimen). Notably, previous studies have shown inconsistent results for the efficacy of PAH-specific therapy in different ILD-PH populations [10, 11, 13,14,15, 38].
The proposed study will distinguish the differences between ILD-PH with PAH features, ILD-PH without PAH features, PAH and ILD-no PH in terms of characteristics, clinical course and treatment response, and unpick the predictors of a positive therapeutic response to PAH-specific therapy. The results will deepen current understanding of the diagnosis and treatment of patients with ILD-PH with PAH features and help identify patients who will benefit from PAH-specific therapy.
The second rationale for the proposed study is related to the fact that right heart morphology and dysfunction significantly affect PAH prognosis [33]. RV–pulmonary arterial coupling and RV-diastolic dysfunction are poor prognostic factors [34, 35]. Therefore, a better understanding of RV morphology and dysfunction may be important for improving PH prognosis. Few reports have addressed these issues in ILD-PH, with most studies to date conducted in PAH [34, 35]. Therefore, the proposed study provides an opportunity to expand current understanding of ILD-PH.
Considering the lack of robust evidence supporting the use of PAH therapy in patients with ILD-PH with and without PAH features, an observational study is considered more suitable than an interventional study. We will use three criteria to tentatively define PAH features: (1) stable ILD; (2) progressive PH; and (3) candidacy for PAH-approved drug treatment. However, the presence of PAH features is not binary (i.e. present or absent), as shown in Fig. 3; rather, it occurs gradually in patients with ILD. Although the definition of PAH features cannot be definitively established from the present study alone, the findings could contribute to establishing a definition for PAH features in the future.
Based on the prospective and retrospective data collection, factors associated with the onset and prognosis of PH may be identified from biomarkers, PH-related genetic analysis and imaging data in ILD. For example, genetic abnormalities, including bone morphogenetic protein receptor 2 (BMPR2) mutations, elevation of certain microRNAs and/or distinctive features on HRCT, may be identified as novel predictors of PH development/worsening in ILD. The investigation may also increase our knowledge of the optimal choice of PAH therapy for PAH with ILD.
Strengths and Limitations
The POPLAR study has various strengths (Fig. 4). First, the focus on patients with ILD-PH with PAH features treated with PAH-specific therapy is unique. In most of the world, PAH-specific therapy is not indicated for ILD-PH. However, in Japan, PAH-specific therapy is indicated for ‘PAH with lung diseases’ if the treatment decision can be adequately supported by careful clinical assessment [36, 37]. Therefore, a considerable number of patients with ILD-PH with PAH features receive PAH-specific therapy in the real-world setting in Japan. Second, geographic advantages may be noted in patient recruitment and data accumulation; Hokkaido is an island with three university hospitals that have a homogeneous respiratory/cardiovascular collaboration platform, allowing good patient coverage (Fig. 4). A homogeneous respiratory/cardiovascular collaboration platform is less common outside of Hokkaido. Thus, the availability of data from these patients provides a unique opportunity to examine this important clinical question in Hokkaido, Japan, and the findings could later be expanded to other countries and regions.
The proposed study also has some limitations. The target diseases are rare, so a retrospective/prospective study design will be adopted. Therefore, bias may exist in the retrospective data compared to data collected prospectively. Second, this study will be observational, and the treatment method is based on the clinical judgment of the physician and cannot be controlled. Third, the definition of “PAH feature” was arbitrary. However, there is no established criteria to accurately identify the subset with PAH feature in patients with ILD. Thus, we used tentative criteria that can be applied in the clinical practice. The validity of the PAH feature will be assessed by independent adjudicating physicians participating in this study, and the influence of definitional uncertainty will be avoided as much as possible. Finally, the number of patients will be limited, and the patient data may not be generalizable to all parts of Japan.
Conclusion
We expect to obtain evidence that could contribute to improve the quality of life and prognosis of patients with PH and ILD. The proposed study will help to clarify the characteristics, clinical course and response to PAH-specific therapy in patients with ILD-PH with PAH features and deepen the understanding of diagnosis and treatment in clinical practice.
Data Availability
This article is a design paper and does not currently include study data at this time. The corresponding author should be contacted for informationon study data availability.
References
Simonneau G, Montani D, Celermajer DS, et al. Haemodynamic definitions and updated clinical classification of pulmonary hypertension. Eur Respir J. 2019;53:1801913.
Nathan SD, Barbera JA, Gaine SP, et al. Pulmonary hypertension in chronic lung disease and hypoxia. Eur Respir J. 2019;53:1801914.
Andersen CU, Mellemkjær S, Hilberg O, et al. Pulmonary hypertension in interstitial lung disease: prevalence, prognosis and 6 min walk test. Respir Med. 2012;106:875–82.
King CS, Shlobin OA. The trouble with group 3 pulmonary hypertension in interstitial lung disease: dilemmas in diagnosis and the conundrum of treatment. Chest. 2020;158:1651–64.
Humbert M, Kovacs G, Hoeper MM, et al. 2022 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur Heart J. 2022;43:3618–731.
Chatterjee K, Tarawneh AR, Alam S. Out of proportion pulmonary hypertension in obstructive lung diseases. Curr Opin Pulm Med. 2018;24:161–72.
Caminati A, Cassandro R, Harari S. Pulmonary hypertension in chronic interstitial lung diseases. Eur Respir Rev. 2013;22:292–301.
Behr J. Inhaled treprostinil in pulmonary hypertension in the context of interstitial lung disease: a success, finally. Am J Respir Crit Care Med. 2022;205:144–5.
Tanabe N, Kumamaru H, Tamura Y, et al. Multi-institutional prospective cohort study of patients with pulmonary hypertension associated with respiratory diseases. Circ J. 2021;85:333–42.
Nathan SD, Behr J, Collard HR, et al. Riociguat for idiopathic interstitial pneumonia-associated pulmonary hypertension (RISE-IIP): a randomised, placebo-controlled phase 2b study. Lancet Respir Med. 2019;7:780–90.
Behr J, Nathan SD, Wuyts WA, et al. Efficacy and safety of sildenafil added to pirfenidone in patients with advanced idiopathic pulmonary fibrosis and risk of pulmonary hypertension: a double-blind, randomised, placebo-controlled, phase 2b trial. Lancet Respir Med. 2021;9:85–95.
Corte TJ, Keir GJ, Dimopoulos K, Howard L, Corris PA, Parfitt L, et al. Bosentan in pulmonary hypertension associated with fibrotic idiopathic interstitial pneumonia. Am J Respir Crit Care Med. 2014;190(2):208–17.
Waxman A, Restrepo Jaramillo R, Thenappan T, et al. Inhaled treprostinil in pulmonary hypertension due to interstitial lung disease. N Engl J Med. 2021;384:325–34.
Sato T, Tsujino I, Sugimoto A, et al. The effects of pulmonary vasodilating agents on right ventricular parameters in severe group 3 pulmonary hypertension: a pilot study. Pulm Circ. 2016;6:524–31.
Nathan SD, Flaherty KR, Glassberg MK, et al. A randomized, double-blind, placebo-controlled study of pulsed, inhaled nitric oxide in subjects at risk of pulmonary hypertension associated with pulmonary fibrosis. Chest. 2020;158:637–45.
Tomos I, Roussis I, Matthaiou AM, Dimakou K. Molecular and genetic biomarkers in idiopathic pulmonary fibrosis: where are we now? Biomedicines. 2023;11(10):2796.
Selimovic N, Bergh CH, Andersson B, Sakiniene E, Carlsten H, Rundqvist B. Growth factors and interleukin-6 across the lung circulation in pulmonary hypertension. Eur Respir J. 2009;34(3):662–8.
Fathimath Muneesa M, Shaikh SB, Jeena TM, Bhandary YP. Inflammatory mediators in various molecular pathways involved in the development of pulmonary fibrosis. Int Immunopharmacol. 2021;96: 107608.
Zhou G, Chen T, Raj JU. MicroRNAs in pulmonary arterial hypertension. Am J Respir Cell Mol Biol. 2015;52(2):139–51.
Li H, Zhao X, Shan H, Liang H. MicroRNAs in idiopathic pulmonary fibrosis: involvement in pathogenesis and potential use in diagnosis and therapeutics. Acta Pharm Sin B. 2016;6(6):531–9.
Mahammedi A, Oshmyansky A, Hassoun PM, Thiemann DR, Siegelman SS. Pulmonary artery measurements in pulmonary hypertension: the role of computed tomography. J Thorac Imaging. 2013;28(2):96–103.
Swift AJ, Capener D, Johns C, Hamilton N, Rothman A, Elliot C, et al. Magnetic resonance imaging in the prognostic evaluation of patients with pulmonary arterial hypertension. Am J Respir Crit Care Med. 2017;196(2):228–39.
Vanderpool RR, Hunter KS, Insel M, Garcia JGN, Bedrick EJ, Tedford RJ, et al. The right ventricular-pulmonary arterial coupling and diastolic function response to therapy in pulmonary arterial hypertension. Chest. 2022;161(4):1048–59.
Yorke J, Corris P, Gaine S, Gibbs JS, Kiely DG, Harries C, et al. emPHasis-10: development of a health-related quality of life measure in pulmonary hypertension. Eur Respir J. 2014;43(4):1106–13.
Galie N, Rubin L, Hoeper M, Jansa P, Al-Hiti H, Meyer G, et al. Treatment of patients with mildly symptomatic pulmonary arterial hypertension with bosentan (EARLY study): a double-blind, randomised controlled trial. Lancet. 2008;371(9630):2093–100.
Ghofrani HA, Wiedemann R, Rose F, Schermuly RT, Olschewski H, Weissmann N, et al. Sildenafil for treatment of lung fibrosis and pulmonary hypertension: a randomised controlled trial. Lancet. 2002;360(9337):895–900.
Goh NS, Desai SR, Veeraraghavan S, et al. Interstitial lung disease in systemic sclerosis: a simple staging system. Am J Respir Crit Care Med. 2008;177(11):1248–54.
Committee for the Guidelines for Diagnosis and Treatment of Diffuse Lung Disease, the Japanese Respiratory Society (2016) Guidance for Diagnosis and Treatment of Idiopathic Interstitial Pneumonia (third edition). Nankodo Co Ltd., Tokyo, 2016
Furukawa T, Kondoh Y, Taniguchi H, et al. A scoring system to predict the elevation of mean pulmonary arterial pressure in idiopathic pulmonary fibrosis. Eur Respir J. 2018;51:1701311.
Shima H, Nakaya T, Tsujino I, et al. Accuracy of Swan-Ganz catheterization-based assessment of right ventricular function: Validation study using high-fidelity micromanometry-derived values as reference. Pulm Circ. 2022;12: e12078.
Tonelli AR, Arelli V, Minai OA, Newman J, Bair N, Heresi GA, et al. Causes and circumstances of death in pulmonary arterial hypertension. Am J Respir Crit Care Med. 2013;188(3):365–9.
Nakamura J, Tsujino I, Ohira H, Nakaya T, Sugimoto A, Sato T, et al. Various factors contribute to death in patients with different types of pulmonary hypertension: a retrospective pilot study from a single tertiary center. Respir Investig. 2022;60:647–57.
Vonk Noordegraaf A, Chin KM, Haddad F, et al. Pathophysiology of the right ventricle and of the pulmonary circulation in pulmonary hypertension: an update. Eur Respir J. 2019;53:1801900.
Nakaya T, Tsujino I, Nakamura J, et al. Right ventricular pressure-volume loop produced with simultaneous application of three-dimensional echocardiography and high-fidelity micromanometry in a patient with pulmonary arterial hypertension. Echocardiography. 2021;38:805–7.
Nakaya T, Ohira H, Sato T, et al. Right ventriculo-pulmonary arterial uncoupling and poor outcomes in pulmonary arterial hypertension. Pulm Circ. 2020;10:2045894020957223.
Investigative Research Group on Intractable Respiratory Diseases and Pulmonary Hypertension Research Group. Pulmonary arterial hypertension (designated intractable disease 86). Date last updated: July 2022 https://www.nanbyou.or.jp/entry/253. Accessed 17 May 2023.
Kanatani Y, Tomita N, Sato Y, et al. National Registry of Intractable Diseases in Japan: present status and future prospects. Neurol Med Chir (Tokyo). 2017;57:1–7.
Raghu G, Behr J, Brown KK, ARTEMIS-IPF Investigators, et al. Treatment of idiopathic pulmonary fibrosis with ambrisentan: a parallel, randomized trial. Ann Intern Med. 2013;158:641–9.
Medical Writing/Editorial Assistance
The authors wish to thank Emily Woodhouse, PhD, of Edanz, Japan, for providing medical writing support, which was funded by Janssen Pharmaceutical K. K., Japan, through EMC K. K., Japan, in accordance with Good Publication Practice (GPP 2022) guidelines (https://www.ismpp.org/gpp-2022).
Funding
This study will be funded by Janssen Pharmaceutical K.K. who also funded the Rapid Service Fee.
Author information
Authors and Affiliations
Contributions
Ichizo Tsujino contributed to the original study concept. Ichizo Tsujino, Kazuki Kitahara, Junichi Omura, Toshiyuki Iwahori and Satoshi Konno contributed toward the overall concept, study protocol and methodology. All authors contributed towards the development of the manuscript. All authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript and have given their approval for the publication.
Corresponding author
Ethics declarations
Conflict of Interest
Ichizo Tsujino received lecture fees from Nippon Shinyaku Co. Ltd. and Janssen Pharmaceutical K.K., as well as funding for the endowed division from Mochida Pharmaceuticals K.K., Nippon Shinyaku Co. Ltd., Nippon Boehringer Ingelheim Co. Ltd., Medical System Network Co. Ltd., Kaneka Corp. and Takeyama Co. Ltd. Kazuki Kitahara, Junichi Omura and Toshiyuki Iwahori are employees of Janssen Pharmaceutical K.K. Toshiyuki Iwahori is a visiting Associate Professor at Shiga University of Medical Science and an advisor of Mizuta Seisakusho, Inc. Toshiyuki Iwahori received lecture fees from Shiga University of Medical Science and Yahad Club for Doctors Physicians in Israel as a visiting associate professor of Shiga University of Medical Science. Satoshi Konno received funding for the endowed division from Mochida Pharmaceuticals K.K., Nippon Shinyaku Co. Ltd., Nippon Boehringer Ingelheim Co. Ltd., Medical System Network Co. Ltd., Kaneka Corp. and Takeyama Co. Ltd.
Ethical Approval
Written informed consent will be obtained from all participants, including the consent for publication of the study. The decision of patients to participate will not impact their standard of care, and the treatment decision will have been made prior to and independently of the patient’s inclusion. All aspects of treatment and clinical management will be in accordance with local clinical practice and applicable local regulations, and at the discretion of the participating (or treating) physician. The Hokkaido University Hospital Clinical Research Supervision Center Biomedical Research Ethics Review Board approved the study protocol (No. 023-0067) on 14 June 2023, and the study is registered in the Japan Registry of Clinical Trials (jRCT1010230018). The Asahikawa Medical University Research Ethics Committee approved the study protocol (No. C2315) on 31 July 2023 and the Sapporo Medical University Hospital Institutional Review Board approved the study protocol (No. 352-95) on 24 August 2023. The study will be performed in accordance with the principles of the Declaration of Helsinki and the Ethical Guidelines for Life Science and Medical Research Involving Human Patients (Notification No. 1 of the Ministry of Education, Culture, Sports, Science and Technology/Ministry of Health, Labour and Welfare/Ministry of Economy, Trade and Industry in 2021).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Tsujino, I., Kitahara, K., Omura, J. et al. A PrOsPective Cohort Study on Interstitial Lung Disease-Associated Pulmonary Hypertension with a ParticulaR Focus on the Subset with Pulmonary Arterial Hypertension Features (POPLAR Study). Pulm Ther 10, 297–313 (2024). https://doi.org/10.1007/s41030-024-00264-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41030-024-00264-0