Abstract
Background
Studies addressing the anti-inflammatory properties of citrate dialysate enrolled patients in both hemodialysis (HD) and hemodiafiltration (HDF), the latter not adjusted for adequate convective exchange. This is a potential source of confounding in that HDF itself has anti-inflammatory effects regardless of the buffer, and optimal clinical outcomes are related to the amount of convection.
Methods
To distinguish the merits of the buffer from those of convection, we performed a 6-month, prospective, randomized, crossover AB-BA study. Comparisons were made during the 3-month study period of on-line HDF with standard dialysate containing three mmol of acetic acid (OL-HDFst) and the 3-month of OL-HDF with dialysate containing one mmol of citric acid (OL-HDFcit). Primary outcome measure of the study was interleukin-6 (IL-6). Klotho, high sensitivity C-reactive protein (hsCRP), fetuin and routine biochemical parameters were also analyzed.
Results
We analyzed 47 patients (mean age 64 years, range 27-84 years) enrolled in 10 participating Nephrology Units. Convective volumes were around 25 L/session with 90 percent of sessions > 20 L and ß2-microglobulin reduction rate 76% in both HDFs. Baseline median IL-6 values in OL-HDFst were 5.6 pg/ml (25:75 interquartile range IQR 2.9:10.6) and in OL-HDFcit 6.6 pg/ml (IQR 3.4:11.4 pg/ml). The difference was not statistically significant (p 0.88). IL-6 values were lower during OL-HDFcit than during OL-HDFst, both when analyzed as the median difference of overall IL-6 values (p 0.02) and as the median of pairwise differences between the baseline and the 3-month time points (p 0.03). The overall hsCRP values too, were lower during OL-HDFcit than during OL-HDFst (p 0.01). Klotho levels showed a time effect (p 0.02) and the increase was significant only during OL-HDFcit (p 0.01).
Conclusions
Citrate buffer modulated IL-6, hsCRP and Klotho levels during high volume OL-HDF. These results are not attributable to differences in the dialysis technology that was applied and may suggest a potential biological effect of citrate on CKD-associated inflammatory state. ClinicalTrials.gov identifier NCT02863016.
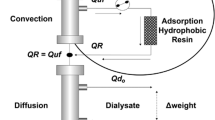
Graphic abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bicarbonate dialysate contains 3–4 mmol/L of acetate to stabilize the pH. As the patient’s pre-dialysis blood levels of this anion are usually lower than 0.1 mmol/L, during treatment the dialysate-blood gradient induces a strongly positive acetate mass balance and an increase in acetate plasma levels [1] with potentially negative effects on micro-inflammation [2]. Therefore, acetate-free dialysate may reduce the inflammatory status induced by extracorporeal treatments [1, 3].
Citric acid is an alternative dialysis buffer that is converted into its anion citrate in the body. The first clinical experience with citrate dialysate in chronic dialysis dates back to 20 years ago [4]. During the long time span since then, positive effects of citrate have been reported, particularly on anticoagulation and dialysis efficiency [5,6,7,8].
Moreover, citrate has clear anti-inflammatory properties in vitro [9, 10] and in various biological systems [11,12,13]. With regard to serum markers of inflammation, results are not so straightforward. Some studies found a reduction of beta2-microglobulin (ß2M) and/or high sensitivity C-reactive protein (hsCRP) and/or interleukin 6 (IL-6) [13,14,15,16,17], while others showed negative results [18,19,20]. Many of these studies bear methodological weaknesses such as short and not randomized study design and/or few retrieved data sets. Moreover, some studies enrolled both patients treated with hemodialysis (HD) and on-line hemodiafiltration (OL-HDF) performed both in pre- or post-dilution with inadequate convection volumes. This is a potential source of confounding in that OL-HDF may modulate micro-inflammation better than HD does [21,22,23,24,25] and, following the seminal paper by Maduell et al. [26], optimal clinical outcomes of OL-HDF are related to the amount of convection [27, 28]. Finally, long-term survival of dialysis patients treated with HD or HDF and citrate dialysate has recently been investigated in large retrospective studies [29,30,31], whose favorable results have been commented upon in an editorial [32]. Since inflammation is a powerful predictor of mortality, it is relevant to analyze the relationship between citrate and inflammation taking into account confounders, namely dialysis techniques.
In this prospective analysis, we aimed at assessing how the 3-month use of an acetate-free, 1 mmol citrate-dialysate would affect the inflammatory marker IL-6. Fetuin-A and Klotho, direct and indirect vascular calcification inhibitors, respectively, were also analyzed [33]. Comparisons were made in post-dilution OL-HDF pointing at convective exchanges as high as those suggested by current gold standards.
Methods
The Hephaestus study was a prospective, randomized, clinical study involving patients under dialysis treatment in Italy’s Tuscany and Piedmont regions. The study procedures adhere to the tenets of the Declaration of Helsinki. Each participant provided written informed consent and the ethics committee of the participating centers approved the study protocol. Based on the remarks of the ethics committee, the presence of randomization and cross-over made it necessary to change the study type from observational (as registered in clinicalTrials.gov) to interventional. Outcomes of the study were detailed and finalized, accordingly. The primary objective was to assess the effect of high volume citrate OL-HDF (OL-HDFcit) compared with standard high volume OL-HDF (OL-HDFst) on the inflammatory state of prevalent dialysis subjects. The primary outcome was the change in the inflammatory marker IL-6 in three months. This time span proved adequate to capture variations in circulating cytokines due to different dialysis techniques [21, 22]. Key outcome was also feasibility of obtaining optimal convective volumes and OL-HDF efficiency in removing small and medium molecules. A novel parameter of this study was the assessment of fetuin-A and Klotho during OL-HDFst vs. OL-HDFcit. Routine biochemistry, e.g., hsCRP, divalent ions and acid–base parameters were also analyzed.
Study design
This was a multicenter, cohort, prospective, 6-month randomized two-arm crossover study (AB or BA). After a 1-month run-in period in OL-HDF, patients were centrally randomized to two groups. AB group patients were treated with OL-HDFst for 3 months and then were transferred to OL-HDFcit for a further period of 3 months. BA group patients were treated in the reverse order. The dialysis technique was assigned with a 1:1 ratio by means of a computer-generated random list and randomization was stratified by dialysis centers.
Study population
We enrolled clinically stable patients aged > 18 years on dialysis treatment for at least 6 months. Internal vascular access (fistula or prosthesis) had to allow real blood flow of at least 250 ml/min and re-circulation below 10%. We excluded subjects with ongoing infections or recent hospitalizations or with clinically relevant residual renal function or with poor life expectancy due to metastatic cancer, severe cirrhosis and AIDS. Patients with an indwelling central venous catheter (CVC) were excluded due to CVC greater infectious risk than internal vascular access.
Treatment procedures
OL-HDFs were carried out with monitors provided with transmembrane pressure (TMP) biofeedback ultracontrol and with selectBag concentrates (Baxter International Inc., Medolla, Italy). Citrate acid concentrate contained 1 mmol of citric acid and 0 mmol of acetic acid; standard concentrate consisted of 3 mmol of acetic acid and 0 mmol of citrate. The nominal concentrations of other constituents of the dialysate (D) were Na 140, Cl 108-110, K 2-3, HCO3 32-34, Ca 1.5, Mg 0.5 mmol/l, glucose 1 gr/l. Two centers recruiting 10 patients utilized CaD 1.65 mmol/l.
Patients were treated with synthetic polyamide or polysulphone high-flux dialyzers. OL-HDFs were performed with ultrapure dialysis fluids, defined as bacterial count < 0.1 CFU/ml and endotoxin < 0.03 EU/ml according to the Italian guidelines [34]. The microbiological water quality of the dialysis fluid was regularly monitored. Anticoagulation was performed with low molecular weight heparin before treatment. All patients were on a thrice-weekly treatment schedule. Dialysis prescription aimed at obtaining convective exchanges > 20 lt/session. Besides citrate, participating centers did not have to change dialysis parameters before and after switching.
Study variables
Study variables were collected in the midweek dialysis session at baseline and thereafter in the middle and at the end of each AB or BA study period (e.g. 6, 12, 18 and 24-week time points). Monitor-derived parameters included effective treatment time, total processed blood, dialysate flow rate (Qd), total infusion (Qinf), early (20’) and hourly TMP, and eKTV (ionic dialysance). We obtained blood flow rate (Qb) by total processed blood and effective treatment time. Pre-post treatment body weight (BW) were also recorded. Patients’ age, anthropometric data and comorbidities were assessed using medical records and patient interviews at enrollment. Comorbidities were recorded using the Charlson Comorbidity Index (CCI). To account for the age effects, one point was added to the CCI score for each decade of life over the age of 50 [35]. Body mass index (BMI) was calculated as body weight/height2 (kg/m2). Pre-treatment hsCRP, ß2M, pH, bicarbonate (HCO3), ionized Calcium (Ca++), Phosphate (PO4), Magnesium (Mg), immunoreactive parathyroid hormone (iPTH), Alkaline Phosphatase (Alk Phos) and post-treatment activated partial thromboplastin time (aPTT) were performed locally by standard procedures. Pre-treatment serum IL-6, fetuin and klotho were centralized in the University of Piemonte Orientale (UPO) laboratory of physiology that was blind to the treatments. Commercially available ELISA kits were used for serum determination of IL-6 (Thermofisher Scientific, Waltham, MA), Fetuin (Cloud-Clone Corporation, Katy, TX) and soluble Klotho (IBL-America, Minneapolis, MN).
Statistics
Sample size estimation: the outcome variable considered for sample size estimation was IL-6. Assuming that in comparison with standard dialysate the citrate buffered dialysate would have reduced IL-6 by 20% over 3 months, we calculated that the inclusion of 45 patients would have conferred an 80% power to demonstrate a statistically significant reduction of IL-6 (α = 0.05, one-tailed test). To account for a 15% dropout rate, we included 53 subjects in the study.
To determine whether parameters were normally distributed, a Kolmogoroff-Smirnoff test was performed.
Accordingly, data were expressed as mean ± standard deviation (SD), median and 25:75 interquartile range (IQR) or as percent frequency (%). Between- and within-group comparisons were made by the Wilcoxon test, the T Test, repeated measures of ANOVA with Tukey–Kramer Multiple-Comparison Test or Chi Square Test, as appropriate. For all parameters, we compared the values obtained in OL-HDFst and OL-HDFcit; we analyzed trend by pairwise differences between the T2-T0 time points. For missing data, we used the average of the two closest values or the last observation carried forward method for imputation. Calculations were made using SPSS for Windows Version 25, Chicago, Illinois – US.
Results
During the calendar years 2016-2018, we enrolled 53 patients from 10 Italian regional dialysis centers, six in Tuscany and four in Piedmont. Randomization was effective, 27 patients were randomized to treatment sequence standard-citrate dialysate and 26 to treatment sequence citrate-standard dialysate. Period and carry-over effects were not significant so the patient differences between the two periods were used for analyses. Therefore, comparisons were made at baseline (T0), after 6 weeks (T1) and after 12 weeks (T2) in the 3 months of OL-HDFst and OL-HDFcit, respectively. Six patients (11% of the 53 enrolled) dropped out, five on OL-HDFst and one on OL-HDFcit. Reasons for dropping out in the OL-HDFst group were withdrawal of consent, transfer to another Center, non-fatal myocardial infarction (two) and thrombosis of vascular access. The patient on OL-HDFcit dropped out because of sepsis due to peripheral vascular disease.
Patients’ characteristics (Table 1)
The characteristics of the fully analyzed population (n 47) did not differ from the randomized one (n 53). Men made up a clear majority. The wide range of age (27–84 year) and weight (38-125 kg) of patients testifies that centers did not adopt restrictions on enrollment. Excluding age, Charlson comorbidity Index was 3.2 and 3.1 in the 2 populations, respectively, with dialytic state accounting for two points.
IL-6 (Fig. 1)
Baseline (T0) median IL-6 values were 5.6 pg/ml (IQR 2.9:10.6) and 6.6 pg/ml (IQR 3.4:11.4) in the OL-HDFst and OL-HDFcit allocation arms, respectively, and the difference was not significant (Wilcoxon, p 0.88). At time point T1 (6 weeks) and T2 (12 weeks) IL-6 values increased to 7.5 pg/ml (IQR 1.7:12.1) and to 7.0 pg/ml (IQR 2.3:11.2) during OL-HDFst, and decreased to 6.5 pg/ml (IQR 2.6:9.6) and 4.4 pg/ml (IQR 3.0:8.1) during OL-HDFcit. During the 3-month-study-period, IL-6 increased by 12% and decreased by 20% during OL-HDFst and OL-HDFcit, respectively. The median difference of overall IL-6 values during OL-HDFst and OL-HDFcit (-0.56 pg/ml, 95% Confidence Interval CI -1.05:-0.07) was significant (p 0.024), as it was (p 0.029) the median of pairwise differences between the T2-T0 time points (− 1.54 pg/ml, CI − 3.2:− 0.1).
Klotho (Fig. 2) and hsCRP
Baseline Klotho levels were 326 ± 235 pg/ml and 306 ± 240 pg/ml during OL-HDFst and OL-HDFcit, respectively, and the difference was not statistically significant (p 0.24). Values increased to 336 ± 252 pg/ml and 340 ± 227 pg/ml at time points T1 and T2 during OL-HDFst and to 326 ± 221 pg/ml and 352 ± 216 pg/ml during OL-HDFcit. The time effect by Anova was significant (p 0.015) and the increase was significant only during OL-HDFcit (T2-T0 comparison by Tukey, p 0.01). Unfortunately, we have hsCRP data from only 30 patients because not all centers routinely measured this parameter. The median hsCRP values were 1.68 mg/l (IQR 0.44:3.89) in OL-HDFst and 1.37 mg/l (0.45:2.78) in OL-HDFcit. The median difference − 0.3 (CI − 0.58:− 0.02) was highly significant by Wilcoxon (p 0.009).
Technical parameters (Table 2)
Regardless of the buffer, all dialysis Centers performed OL-HDFs according to the highest standards. Mean convection volumes were > 20 L in the overwhelming majority of treatments, compared to not particularly elevated average effective Qb values. Average TMPs were within the safe range at both the beginning and end treatments, as was percent filtration fraction. The end treatment aPTT was within the normal range in both procedures.
Dialysis efficiency (Table 3)
ß2 reduction rate was consistent in both treatments. However, serum ß2 pre-treatment values did not change. The efficiency for small molecule clearance was assessed by eKTV measured by monitor-derived ionic dialysance and did not vary among procedures.
Biochemistry (Tables 4 and 5)
Pre-treatment acid–base parameters and Ca++ values were not significantly different along the 3-month study period regardless of buffer (Table 4). The percentages of Ca++ values below 1 mmol/l were 7.1% of the 141 determinations performed in both standard and citrate OL-HDFs and only one Ca++ value was below 0.9 mmol/l during OL-HDFcit. There was a tendency to higher pre-treatment PO4 values and lower Mg values in OL-HDFcit in comparison with OL-HDFst. Fetuin and Alk Phos values did not change with time or between procedures. Although iPTH values were not significantly different along the 3-month study period regardless of buffer, there was a trend towards an increase in iPTH values in OL-HDFcit and a reduction in OL-HDFst. Dichotomizing the population according to the nominal CaD concentrations in OL-HDFcit (Table 5), Ca++ values were higher and iPTH values lower in the 10 patients on CaD 1.65 than in the 37 patients on CaD 1.5 mmol/l.
Discussion
In a dialysis population characterized by low-grade inflammation and in a 3-month time span, acetate-free, 1 mmol citrate OL-HDF achieved lower IL-6 values than standard bicarbonate 3 mmol acetate OL-HDF. The hsCRP trend corroborated the IL-6 results. Interestingly, the reduction of inflammatory markers is associated with an increase in Klotho in OL-HDFcit. Acid–base and laboratory parameters surrogate outcomes of mineral bone disease did not vary, particularly when dialysate Ca 1.65 mmol/l was used. These results are due to the use of citrate and not to differences in applied technology since both experimental and comparison OL-HDFs were performed at the highest quality levels.
The anti-inflammatory effect of citrate was investigated in manifold biological systems. Citrate induced minor polymorphonuclear and platelet degranulation with reduction of oxidized LDL [11], decreased glycoxidation and lipid peroxidation products [12], reduced cell-free mitochondrial DNA marker of cellular damage [13] and reduced intra-dialytic synthesis of Pentraxin-3, a marker of dialysis bio-incompatibility associated with cardiovascular diseases [19]. Moreover, we recently demonstrated that switching from acetate to citrate buffer reduces systemic inflammation and prevents the harmful effects of the adipokine chemerin, e.g., a uremic toxin known to induce vascular dysfunction by targeting both endothelial and vascular smooth muscle cells [17]. However, regarding inflammatory circulating molecules, some studies reported positive results [13,14,15,16,17], while others showed negative results [18,19,20]. The comparison between these studies is difficult due to differences in the study design, the dialysis technique and the target cytokine. In our RCT, we focused on IL-6 for a number of reasons. IL-6 is more predictive of hard clinical outcomes than the other routine laboratory-based measures of inflammation [36,37,38], it plays a pivotal role in the pathogenesis and progression of atherosclerosis [39] and it is implicated in the remodeling observed after myocardial infarction [40]. Moreover, a meta-analysis including more than 9000 patients demonstrated that circulating IL-6 levels are independently associated with a greater risk of cardiovascular mortality in the general elderly population [41]. In our study, IL-6 was measured at an external, qualified laboratory blinded to the procedures employed, and the trend of IL-6 in HDFs was evaluated by various statistical tests. These safeguards make us confident of the robustness of our results. As inflammation is among the surrogate markers of mortality, our data are in line with recent evidence on the safety of citrate on hard outcomes such as survival [29,30,31,32]. In this regard, it is interesting to note that in our study only one patient dropped out during OL-HDFcit, compared to five patients who did so during OL-HDFst. This result, however, is anecdotal because the study was not powered to investigate the clinical safety of citrate dialysate in the long run.
To assess the clinical role of citrate, the comparability of the dialysis techniques employed is also relevant. Some of the previous studies included patients on both HD and HDF [17, 19, 20], the latter employed in pre- and post re-infusion with inadequate amount of convection [20]. When only HDF was challenged, the infusion was in pre- [14] or in post-dilution without reporting the amount of convection [16]. These differences may well impact on results since, at variance with HD, HDF reduces systemic micro-inflammation [21,22,23,24,25] and only high convection volumes are associated with positive clinical outcomes [26,27,28]. Patient-related or dialysis center-related factors often prevent achieving the prescribed convection volumes [42]. In our study, average convective volume was particularly high, with 89% of treatments fulfilling the current gold standards [26,27,28]. Linked to high convection was a commensurate ß2 M reduction rate, which however did not result in pre-treatment lower values of ß2 M. These optimal outcomes are due to the excellent technical practices of the dialysis centers involved in this study. Mean TMP at 20’ is well within the range of recommendations and excludes significant albumin loss and dialyzer clotting at the beginning of treatment besetting treatment efficacy [43]. Accordingly, average session TMP profile is reassuring with a low percentage of TMP values at 240’ exceeding 300 mmHg. The achieved treatment time is superimposable to the set time, which excludes interruption of treatments due to technical problems. Unlike other studies [4, 5], we did not find higher dialysis efficiency for small molecules with citrate. In those studies, citrate was used in HD while we tested it in OL-HDF. The particularly high convection achieved may have obscured any advantages on KT/V, e.g., a parameter influenced by diffusion. Moreover, we measured KT/V by ionic dialysance, a method that yields lower results than measurements based on the urea distribution volume.
Regional citrate causes anticoagulation chelating Ca with a consequent reduction of the ionized fraction and potential hypocalcemia [44]. However, the small amount of citrate in the dialysate (0.65-1 mmol/l, as per manufacturer) is one-fifth of the standard concentration adopted in regional anticoagulation. We found higher serum Ca++ and lower iPTH values in citrate OL-HDF with CaD 1.65 than with CaD 1.5 (tab 5). Our results are in agreement with Molina et al. [16] and Perez-Garcia et al. data [45] and confirm the current trend of increasing CaD when using citrate dialysate. However, this recommendation did not enter in the routine of all HD centers. Indeed, the largest RCT to date published on citrate included both CaD 1.5 and 1.65 mmol/l (20). It is reasonable to hypothesize that the CaD of the citrate dialysate should be individualized based on the subject’s bone marker parameters. CaD 1.65 is suitable in subjects with serum Ca and PTH values in the low and high range of normality, respectively. Per contra, hypercalcemia or low serum iPTH levels or adynamic bone disease may benefit from lower CaD concentrations (32).
It should be pointed out that serum Ca++ and iPTH fluctuations are just two of the players in the field. It is a time-honored achievement that most body citrate is in the bone tissue, it is released during bone resorption, it binds calcium ions in organic fluids, thus counteracting calcium-phosphate precipitation in soft tissues [46]. Citrate may also take part in bone formation as it stabilizes the apatite nanocrystals in the bone [47]. While citrate is a low-molecular weight inhibitor of calcification, fetuin A and Klotho are high molecular weight direct and indirect inhibitors of systemic calcification, respectively [33]. However, both are pleotropic molecules with diverse, even contradictory effects on different systems, brought about by interaction with a variety of receptors [48]. The stable serum levels of fetuin, the significant increase in soluble Klotho and the reduction of inflammatory parameters that we herein observed in OL-HDFcit is just hypothesis-generating, and further studies specifically addressing the role of citrate on propensity to tissue calcification are needed. Klotho gene is mainly expressed in proximal and distal tubular epithelial cells and acts as a co-receptor for FGF-23 exerting a biological role on mineral metabolism and protection against vascular calcification. Moreover, Klotho deficiency has been associated with CKD progression and with the development of a pro-senescent phenotype characterized by accelerated vascular aging. In subjects with normal renal function, serum concentrations and vascular expression of Klotho were down-regulated in the presence of severe atherosclerotic lesions with a negative and significant correlation with inflammatory parameters such as TNF-alpha, IL-6 and IL-10 [49]. Similar data were also observed in patients with end stage renal disease [50]. Furthermore, in hemodialysis patients, lower Klotho levels are associated with a pro-inflammatory state and with increased cardiovascular/cerebrovascular events and mortality regardless of other established risk factors [51, 52]. Recent studies further corroborated the role of Klotho in CKD-related inflammation and premature aging. On one hand, pro-inflammatory factors are responsible for the activation of NF-kB, the intracellular master control of inflammatory response, oxidative stress and apoptosis. In turn, NF-kB activation down-regulates Klotho expression. On the other hand, the anti-inflammatory activity of Klotho may be at least in part ascribed to its negative regulation of NF-kB with its attendant decreased production of inflammatory mediators [53]. It was not the aim of this study to evaluate whether the inflammatory state generates Klotho or, on the contrary, if Klotho is mainly responsible for hampering inflammation. However, our results suggest that OL-HFDcit may modulate the inflammatory response of chronic uremic patients by increasing Klotho as well.
We acknowledge some limitations of our study: we did not evaluate heparin doses, hence, we cannot discriminate the anti-flogistic effect of citrate and heparin per se [54]. However, the superimposable end-treatment aPTT values make us confident that heparin regimens did not vary during either OL-HDFs, according to study protocol. Moreover, our study design prevents discriminating whether the anti-inflammatory effect of citric acid-based dialysate is due to the absence of acetate [1, 3] or to the presence of citrate as such. We should have compared citrate with other non-acetate buffers such as HCl. However, this latter dialysate was popular in the past but then its use gradually decreased.
In conclusion, notwithstanding the very high standards of both techniques tested in a population that did not show high levels of inflammation, OL-HDF citrate achieved lower serum levels of the pro-inflammatory marker IL-6 than the standard procedure. Moreover, OL-HDF citrate was associated with a significant increase in the anti-inflammatory and anti-aging molecule Klotho. These results are not attributable to differences in the dialysis technology that was applied and may suggest a potential biological effect of citrate on CKD-associated inflammatory state.
Change history
24 February 2021
A Correction to this paper has been published: https://doi.org/10.1007/s40620-021-01009-x
References
Pizzarelli F, Cerrai T, Dattolo P, Giuseppe F (2006) On-line haemodiafiltration with and without acetate. Nephrol Dial Transplant 21:1648–1651
Amore A, Cirina P, Mitola S et al (1997) Acetate intolerance is mediated by enhanced synthesis of nitric oxide by endothelial cells. J Am Soc Nephrol 8:1431–1436
Todeschini M, Macconi D, Garcia Fernandez N et al (2002) Effect of acetate-free biofiltration and bicarbonate hemodialysis on neutrophil activation. Am J Kidney Dis 40:783–793
Ahmad S, Callan R, Cole JJ, Blagg CR (2000) Dialysate made from dry chemicals using citric acid increases dialysis dose. Am J Kidney Dis 35:493–499
Kossmann RJ, Gonzales A, Callan R et al (2009) Increased efficiency of hemodialysis with citrate dialysate: a prospective controlled study. Clin J Am Soc Nephrol 4:1459–1464
Cheng YL, Yu AW, Tsang KY et al (2011) Anticoagulation during haemodialysis using a citrate-enriched dialysate: a feasibility study. Nephrol Dial Transplant 26:641–646
Aniort J, Petitclerc T, Créput C et al (2012) Safe use of citric acid based dialysate and heparin removal in postdilution online hemodiafiltration. Blood Purif 34:336–343
Sands JJ, Kotanko P, Segal JH et al (2012) Effects of citrate acid concentrate (citrasate®) on heparin N requirements and hemodialysis adequacy: a multicenter, prospective non-inferiority trial. Blood Purif 33:199–204
Bryland A, Wieslander A, Carlsson O et al (2012) Citrate treatment reduces endothelial death and inflammation under hyperglycaemic conditions. Diabetes & vascular disease research 9:42–51
Huang S, Sandholm K, Jonsson N et al (2015) Low concentrations of citrate reduce complement and granulocyte activation in vitro in human blood. Clin Kidney J 8:31–37
Gritters M, Grooteman MP, Schoorl M et al (2006) Citrate anticoagulation abolishes degranulation of polymorphonuclear cells and platelets and reduces oxidative stress during haemodialysis. Nephrol Dial Transplant 21:153–159
Masuda A, Hagiwara S, Tanimoto M et al (2012) Effects of Acetate-Free Citrate Dialysate on Glycoxidation and Lipid Peroxidation Products in Hemodialysis Patients. Nephron Extra 2:256–268
Su wong J, Da Rae K, Kyung Sook C et al (2019) Effects of Dialysate Acidification With Citrate Versus Acetate on Cell Damage, Uremic Toxin Levels, and Inflammation in Patients Receiving Maintenance Hemodialysis. Research Letter. Am J Kid Disease 73:432–434
Matsuyama K, Tomo T, Kadota J et al (2011) Acetate-free blood purification can improve nutritional status in hemodialysis patients. Journal Artif Organs 14:112–119
Panichi V, Fiaccadori E, Rosati A et al (2013) Post-Dilution on Line Haemodiafiltration with Citrate Dialysate: First Clinical Experience in Chronic Dialysis Patients. Sci World J. https://doi.org/10.1155/2013/703612
Molina Nuñez M, de Alarcón R, Roca S et al (2015) Citrate versus acetate-based dialysate in on-line haemodiafiltration. A prospective cross-over study. Blood Purif 39:181–187
Dellepiane S, Medica D, Guarena C et al (2019) Citrate anion improves chronic dialysis efficacy, reduces systemic inflammation and prevents Chemerin-mediated microvascular injury. Sci Rep 23(9):10622
Kuragano T, Kida A, Furuta M et al (2012) Effects of acetate free citrate-containing dialysate on metabolic acidosis, anemia, and malnutrition in hemodialysis patients. Artif Organs 2012(36):282–290
Grundström G, Christensson A, Alquist M et al (2013) Replacement of acetate with citrate in dialysis fluid: a randomized clinical trial of short term safety and fluid biocompatibility. BMC Nephrol 14:216
Schmitz M, Loke O, Fach B et al (2016) Effects of citrate dialysate in chronic dialysis: a multicentre randomized crossover study. Nephrol Dial Transplant 31:1327–1334
Canaud B, Wizemann V, Pizzarelli F et al (2001) Cellular interleukin-1 receptor antagonist production in patients receiving on-line haemodiafiltration therapy. Nephrol Dial Transplant 16:2181–2187
Carracedo J, Merino A, Nogueras S et al (2006) On-line hemodiafiltration reduces the proinflammatory CD14 + CD16 + monocyte-derived dendritic cells: a prospective, crossover study. J Am Soc Nephrol 17:2315–2321
Ramirez R, Carracedo J, Merino A et al (2007) Microinflammation induces endothelial damage in hemodialysis patients: the role of convective transport. Kidney Int 72:108–113
Panichi V, Rizza GM, Paoletti S et al (2008) Chronic inflammation and mortality in haemodialysis: effect of different renal replacement therapies. Results from the RISCAVID study. Nephrol Dial Transplant 23: 2337–2343
den Hoedt CH, Bots ML, Grooteman MPC et al (2014) for the CONTRAST Investigators. Online hemodiafiltration reduces systemic inflammation compared to low-flux hemodialysis. Kidney International 86: 423–432
Maduell F, Moreso F, Pons M et al (2013) High-efficiency postdilution online hemodiafiltration reduces all-cause mortality in hemodialysis patients. J Am Soc Nephrol 24:487–497
Davenport A, Peters SA, Bots ML et al (2016) Higher convection volume exchange with online hemodiafiltration is associated with survival advantage for dialysis patients: the effect of adjustment for body size. Kidney Int 89: 193–199
Peters SA, Bots ML, Canaud B et al (2016) Haemodiafiltration and mortality in end-stage kidney disease patients: a pooled individual participant data analysis from four randomized controlled trials. Nephrol Dial Transplant 31:978–984
Jacky Potier J, Dolley-Hitze T, Hamel D et al (2020) Long-term effects of citric acid-based bicarbonate haemodialysis on patient outcomes: a survival propensity score–matched study in western France. Nehprol Dial Transplant 35:1228–1236
Neri L, Bellocchio F, Kircelli F et al (2020) Long term mortality risk associated with citric acid based and acetic acid based bicarbonate hemodialysis: a historical cohort propensity score matched study in a large, multicenter, population-based study. Nephrol Dial Transplant 35:1237–1244
Couchoud C, Hannedouche T, Bauwens M et al (2020) Impact of the dialysate acid component on haemodialysis mortality rates. Nephrol Dial Transplant 35:1244–1249
Pizzarelli F, Basile C (2020) The Gordian knot of the long-term safety of dialysate citrate: is there really a concern about patient hard outcomes? Nehprol Dial Transplant 35:1090–1094
Villa-Bellosta R. New insights into endogenous mechanisms of protection against arterial calcification. Review article. Atherosclerosis, https://doi.org/10.1016/j.atherosclerosis.2020.03.007
Alloatti S, Bolasco P, Canavese C et al (2005) Italian Society of Nephrology Guidelines on water and solutions for dialysis. G Ital Nefrol 22:246–273
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis 40:373–383
Panichi V, Maggiore U, Taccola D et al (2004) Interleukin-6 is a stronger predictor of total and cardiovascular mortality than C-reactive protein in haemodialysis patients. Nephrol Dial Transplant 19:1154–1160
Pachaly MA, do Nascimento MM, Suliman ME et al (2008) Interleukin-6 is a better predictor of mortality as compared to C-reactive protein, homocysteine, pentosidine and advanced oxidation protein products in hemodialysis patients. Blood Purif 26:204–210
Desai AA, Nissenson A, Chertow GM et al (2009) The relationship between laboratory-based outcome measures and mortality in end-stage renal disease: a systematic review. Hemodialysis international 13:347–359
Ridker PM (2016) From C-Reactive Protein to Interleukin-6 to Interleukin-1: moving Upstream To Identify Novel Targets for Atheroprotection. Circ Res 118:145–156
Huang M et al (2015) Role of interleukin-6 in regulation of immune responses to remodelling after myocardial infarction. Heart Fail Rev 20:25–38
Li H et al (2017) Circulating interleukin-6 levels and cardiovascular and all-cause mortality in the elderly population: a meta-analysis. Arch Gerontol Geriatr 73:257–262
Lars Penne E, van der Weerd NC, Bots ML et al (2009) on behalf of the CONTRAST investigators. Patient- and treatment-related determinants of convective volume in post-dilution haemodiafiltration in clinical practice. Nephrol Dial Transplant 24:3493–3499
Pedrini LA, Cozzi G, Faranna P et al (2006) Transmembrane pressure modulation in high-volume mixed hemodiafiltration to optimize efficiency and minimize protein loss. Kidney Int 69:573–579
Fiaccadori E, Pistolesi V, Mariano F et al (2015) Regional citrate anticoagulation for renal replacement therapies in patients with acute kidney injury: a position statement of the Work Group ‘‘Renal Replacement Therapies in Critically Ill Patients’’ of the Italian Society of Nephrology. J Nephrol 28:151–164
Perez-Garcia R, Albalate M, Sequera P et al (2017) Calcium mass balance with citrate dialysate is lower than with acetate. Nefrologia 37:109–110
Dixon TF, Perkins HR (1952) Citric acid and bone metabolism. Biochem J 52:260–265
Hu YY, Rawal A, Schmidt-Rohr K (2010) Strongly bound citrate stabilizes the apatite nanocrystals in bone. Proc Natl Acad Sci USA 107:22425–22429
Rutsch F, Nitschke Y, Terkeltaub R (2011) Genetics in Arterial Calcification Pieces of a Puzzle and Cogs in a Wheel. Reviews. Circulation Research 109:578–592
Martín-Núñez E, Donate-Correa J, López-Castillo Á (2017) Soluble levels and endogenous vascular gene expression of KLOTHO are related to inflammation in human atherosclerotic disease. Clin Sci 131:2601–2609
Yu L, Kang L, Ren XZ et al (2018) Circulating α-Klotho Levels in Hemodialysis Patients and Their Relationship to Atherosclerosis. Kidney Blood Press Res. 43:1174–1182
Memmos E, Sarafidis P, Pateinakis P et al (2019) Soluble Klotho is associated with mortality and cardiovascular events in hemodialysis. BMC Nephrol. 20:217
Wei H, Li H, Song X, Du X, Cai Y, Li C, Dong L, Dong J (2019) Serum klotho: a potential predictor of cerebrovascular disease in hemodialysis patients. BMC Nephrol. 20:63
Zou D, Wu W, He Y et al (2018) The role of klotho in chronic kidney disease. BMC Nephrol. 19:285
Lavainne F, Meffray E, Pepper RJ et al (2014) Heparin use during dialysis sessions induces an increase in the antiangiogenic factor soluble Flt1. Nephrol Dial Transplant 29:1225–1231
Acknowledgements
Hephaestus Study Group: Alessia Scatena, Nephrology and Dialysis Unit, Versilia Hospital, Lido di Camaiore. Erika Biassoli, Nephrology and Dialysis Unit, ASL Nordovest Massa Carrara. Nadia Sami, Nephrology and Dialysis Unit, ASL Nordovest Massa Carrara. Giancarlo Betti, Nephrology and Dialysis Unit, ASL Nordovest Massa Carrara. Elvira Mancini, Nephrology and Dialysis Unit ASL VCO, Verbano Cusio Ossola. Ragazzoni Elena, Nephrology and Dialysis Unit, Borgomanero hospital, ASL NO Novara, Borgomanero, Italy Battista Michele, Nephrology and Dialysis Unit, Borgomanero hospital, ASL NO Novara, Borgomanero, Italy.
Funding
None.
Author information
Authors and Affiliations
Consortia
Contributions
PF designed the study, analyzed data and drafted the manuscript with CV and PV; FG and MV revised it critically; TA and DPC performed the statistical analysis; FA and GE carried out the centralized biochemical measurements; MM, FG, GC, CA, BM, CS, CA, QA, FO, DL coordinated the trial at the Center level. All authors approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose and they have no conflicts of interest to declare that are relevant to the content of this article.
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original article has been updated: Due to conclusion update.
Rights and permissions
About this article
Cite this article
Pizzarelli, F., Cantaluppi, V., Panichi, V. et al. Citrate high volume on-line hemodiafiltration modulates serum Interleukin-6 and Klotho levels: the multicenter randomized controlled study “Hephaestus”. J Nephrol 34, 1701–1710 (2021). https://doi.org/10.1007/s40620-020-00943-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-020-00943-6