Abstract
There has been considerable progress over the last decade in the standardization of the acute kidney injury (AKI) definition with the publication of the RIFLE, AKIN, KDIGO and ERBP classification criteria. However, these classification criteria still rely on imperfect parameters such as serum creatinine and urinary output. The use of timed urine collections, kinetic eGFR (estimated glomerular filtration rate), real time measurement of GFR and direct measures of tubular damage can theoretically aid in a more timely diagnosis of AKI and improve patients’ outcome. There has been an extensive search for new biomarkers indicative of structural tubular damage but it remains controversial whether these new markers should be included in the current classification criteria. The use of these markers has also led to the creation of a new concept called subclinical AKI, a condition where there is an increase in biomarkers but without clinical AKI, defined as an increase in serum creatinine and/or a decrease in urinary output. In this review we provide a framework on how to critical appraise biomarker research and on how to position the concept of subclinical AKI. The evaluation of biomarker performance and the usefulness of the concept ‘subclinical AKI’ requires careful consideration of the context these biomarkers are used in (clinical versus research setting) and the goal we want to achieve (risk assessment versus prediction versus early diagnosis versus prognostication). It remains currently unknown whether an increase in biomarkers levels without functional repercussion is clinically relevant and whether including biomarkers in classification criteria will improve patients’ outcome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The development of consensus definitions by Acute Dialysis Quality Initiative (ADQI) in 2004 (RIFLE criteria) [1] The Acute Kidney Injury Network (AKIN) in 2007 (AKIN criteria) [2], KDIGO [3] and ERBP [4] was a major step forward in homogenizing the definition of acute kidney injury (AKI). A standardized definition is critical for comparing epidemiological studies and enrolling patients in clinical trials. The consensus criteria classify patients according to changes in serum creatinine (sCr) and urine output (UO) by acknowledging the equal importance of both small sCr increases and small decreases in UO within a certain time frame. However, using these criteria for AKI diagnosis is still subjected to limitations according to some authors [5], since changes in sCr and UO merely reflect functional changes and do not incorporate parameters that directly indicate tubular damage. Addition of postoperative UO measurements, also when collected during routine care on surgical hospital wards, substantially increases the apparent incidence of AKI and significantly changes the prognostic implications of AKI identification and staging, and this both on ICU as on hospital wards [6, 7]. sCr values are influenced by many non-renal determinants and both the generation rate and the distribution volume of creatinine are not stable in critically ill patients. An acute change in GFR after a renal insult does not result in an abrupt increase in sCr due to the time needed for creatinine to accumulate in the body [8] and it usually takes 24–36 h after a renal insult to reach a new steady state [9]. The delayed increase in sCr after a decline in GFR is seen especially in patients who simultaneously become fluid overloaded. Likewise, sCr does not immediately decrease when GFR improves [10]. Serial measurements of creatinine clearance provided more timely and accurate information on renal function compared to serial sCr measurements in critically ill patients [11].
The recognition of the limitations of sCr and UO has prompted research on new biomarkers possibly reflecting tubular structural damage. Based on these results members of the ADQI group proposed a reformulation of the diagnostic approach to AKI where not only markers of kidney function (e.g. changes in sCr and UO), but also markers of kidney damage should be incorporated. A subgroup of AKI patients was described who did not fulfil the classically used functional criteria for AKI diagnosis but showed elevated levels of new biomarkers presumably reflecting tubular injury, suggesting that these patients suffered from “subclinical AKI” [12].
This review explores in more detail the concept of subclinical AKI. To clarify reasoning, we will provide a thinking framework, as the role and value of all these concepts substantially depends on the setting and intention for which they are being used. Therefore, we tabulated several points of reflection to be taken into account regarding setting and aims in which this concept could be used (Table 1).
Original definition of subclinical AKI
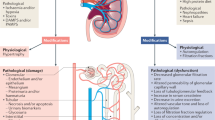
The initial paradigm identifies four clinically relevant groups based on the absence of signs of functional changes or damage (A), presence of signs of damage but without loss of function (B), presence of functional changes but without signs of damage (C) and signs of both damage and loss of function (D) [12,13,14] (Fig. 1).

(figure modified from Murray et al. [14])
Entities of acute kidney injury (AKI) syndrome by damage and dysfunction (or both). a No AKI. b AKI with tubular damage (biomarker-positivity) (subclinical AKI). c AKI with dysfunction (RIFLE/AKIN/KDIGO). d AKI with tubular damage (biomarker-positivity) and dysfunction (RIFLE/AKIN/KDIGO). Arrows indicate the potential progression from subclinical AKI (b) to AKI (d) and from hemodynamic AKI (c) to AKI (d)
According to the paradigm, renal damage is based on an increased urinary excretion of “injury” biomarkers while loss of function is based on an increase in sCr and/or a decrease in urinary output. Haase et al. [13] demonstrated that patients who were NGAL positive/sCr negative (group B) had similar lengths of ICU and hospital stay compared with those who were NGAL negative/sCr positive (group C), and these were significantly longer than those who were NGAL negative/sCr negative (group A). In addition, they more frequently received renal replacement therapy (RRT) and were more likely to experience patient mortality compared with patients without evidence of AKI (group A). Two subsequent prospective studies [15, 16] enrolling patients treated in an emergency department assessed the short-term prognostic relevance of biomarker based (subclinical) AKI. In the study by Nickolas, urinary (u) NGAL or uKIM-1 were elevated whereas sCr level was less than 1.4 mg/dl in 15% of patients. These patients were at increased risk of subsequent RRT and increased hospital mortality. In another multicenter study (N = 665) a subgroup of 29 patients (4.3%) were considered to have subclinical AKI (plasma NGAL positive/sCr negative) on admission at the emergency unit. These patients had significantly higher rates of clinical events for the combined endpoint of renal replacement therapy (RRT) or in-hospital mortality than the patients who were sCr negative/plasma NGAL negative [16]. Adult patients enrolled in the Translational Research in Biomarker Endpoints in AKI (TRIBE-AKI) without clinical AKI but within the highest versus 2 lowest tertiles of peak urinary IL-18 and KIM-1had worse long-term survival [17]. Renal transplant recipients who did not develop delayed graft function but had high perioperative urinary biomarker levels (NGAL and IL-18) had higher rates of poor graft outcomes at 1 year than those who developed delayed graft function but had below median levels of urinary biomarkers [18].
In a recent multicenter German study including 200 patients urinary biomarkers (NGAL, midkine, and interleukin 6) were identified as independent predictors of AKI post cardiac surgery [19]. Focusing on the NGAL data only, the majority of patients (66.8%) was classified as NGAL negative/RIFLE negative (ie, no renal injury), 21.1% as NGAL positive/RIFLE negative (ie, subclinical AKI), 4.5% as NGAL negative/RIFLE positive (ie, isolated functional AKI), and 7.5% as NGAL positive/RIFLE positive (ie, higher risk functional AKI). The odds ratios for the primary end point (need for acute RRT or in-hospital mortality), in NGAL positive/RIFLE negative patients (subclinical AKI) versus NGAL negative/RIFLE negative patients was 5.86 [95% CI 1.34–25.65 (P = .020)] and adjusted hazard ratio (HR), 7.18 [95% CI 1.52–33.93 (P = .013)]. These subclinical AKI patients had a 10-fold increase in in-hospital mortality compared with NGAL negative/RIFLE negative patients. Separation for long-term survival was found in biomarker positive versus negative patients independent of RIFLE status [20].
Other studies have investigated the frequency of “subclinical AKI” after nephrotoxic exposure. In a recent prospective observational cohort study, Kidney Injury Molecule-1 (KIM-1) and NGAL were used to identify aminoglycoside-induced nephrotoxicity in 158 children and young adults with cystic fibrosis [21]. The median peak fold-change during tobramycin exposure for KIM-1 was 2.28 (IQR 2.69) and 4.02 (IQR 7.29) for NGAL. Urine KIM-1 rises earlier and reaches a peak at 3–5 days, whereas NGAL rises later and reaches a peak at 9–11 days. None of these children developed AKI defined by the KDIGO criteria. According to the proposed definition these patients suffered thus from subclinical AKI during at least 2 weeks.
Non-steroidal anti-inflammatory drug administration was associated with a significant increase in urinary NGAL in children who did not develop clinical AKI following cardiopulmonary bypass surgery [22]. NGAL levels are also elevated following contrast administration in patients who do not develop a significant increase in sCr level [23, 24]. Based on the above discussed studies where biomarkers were measured concomitantly with sCr, at least two types of subclinical AKI seem to exist. First, subclinical AKI can be detected in patients who never develop “functional” AKI and where the biomarkers disappear after the exposure to the insult has stopped [21,22,23,24]. This type is often observed during the exposure to potentially nephrotoxic substances (aminoglycosides, NSAIDs, contrast media). The question can be raised whether in these clinical situations the increased levels biomarkers should not be considered more as markers of “exposure”, reflecting “renal handling of the xenobiotic” rather than of tubular damage. One could consider that the renal handling of many drugs imposes a stress to the tubular cells which, in case of overexposure, eventually can generate structural damage important enough to provoke frank nephrotoxic AKI. It is thus possible, but not yet proven, that some of these biomarkers are able to predict subsequent clinically relevant nephrotoxicity [25].
The second type of subclinical AKI is probably more frequent and exists only in the relatively short period that the sCr is not yet sufficiently elevated to fulfill the actually AKI KDIGO definition [13, 20]. The fact that the sCr is not yet elevated does not exclude that the GFR has not declined because of the existence of functional renal reserve (see below). However, as far as we know, the proportion of subclinical AKI patients that after a few days develop functionally based AKI versus those that never develop functional AKI is not known. To the best of our knowledge no differences in gender or race exist in the incidence or prognosis of “subclinical AKI”.
Hemodynamic AKI
In Fig. 1 hemodynamic AKI, formerly called “pre-renal” or “transient” AKI are represented by group C where functional loss (increased sCr to a level that meets the KDIGO definition) occurs in absence of detectable kidney damage, based on biomarkers. Transient AKI is a reversible state and presumably also reflects hemodynamic dysfunction. The hemodynamic changes occur as a “normal” renal physiologic response to a reduction in “absolute” extracellular volume or a reduction in “effective” circulating volume, like in heart failure and severe liver cirrhosis. It has been a matter of debate when exactly this prerenal AKI becomes intrinsic AKI [26,27,28], and it has been suggested they often do coexist in the same patient [29]. Transient AKI was not associated with substantial tubular injury as reflected by normal NGAL release [30], whereas an increased biomarker excretion was observed in more sustained AKI. Expression of renal genes is different in two murine models of AKI, one induced by severe extracellular fluid volume depletion (vAKI) and the other by ischemic injury (iAKI), but with comparable increases in sCr [31]. The genes induced by vAKI included those involved in metabolic, transport, and osmoregulatory pathways, which are essential to the normal response of the kidney to volume depletion, and this expression was reversed by volume repletion. By contrast, pathways upregulated in the iAKI model represented those genes involved in cell injury, death and inflammation. These data were further translated to humans suggesting that AKI caused by volume depletion and those by intrinsic AKI represent distinct molecular entities [32].
The role of renal functional reserve (RFR)
A “normal” sCr does not exclude a decline in GFR while a normal or even a supranormal GFR does not exclude kidney functional changes nor subclinical structural damage. When estimating renal function, the concept of renal functional reserve (RFR) should be taken into account. RFR is defined as the increase in GFR above basal fasting values which can be activated by stress, oral protein load, amino acid, dopamine, or glucagon infusion [33]. The increase in GFR indicates the capability of the kidneys to compensate temporarily for functional loss of part of the nephrons [34, 35].
The concept of RFR might be relevant when evaluating renal function in AKI. RFR may be activated in critically ill patients as evidenced by the finding of “supra-normal” GFR values when measured by daily 24-h creatinine clearances in patients on a ventilator and/or receiving vasopressors for hemodynamic support [34, 36,37,38]. As far as we know no data on urinary biomarkers exist in states of hyperfiltration in critically ill patients.
There are no data about the exact changes of RFR in AKI, but it may well be that in AKI, a part of RFR is activated and subsequently lost before the decline in GFR and an increase in sCr are noticeable. In these cases, the reduced GFR in some “injured” nephrons is compensated for by other non-injured functioning nephrons [34]. Interestingly, RFR measured after an acute protein load was recently explored to predict post cardiac surgery AKI in patients with “normal” resting GFR, (i.e. eGFR > 60 ml/min/1.73m2) the day before undergoing cardiac surgery [39]. Inadequate preoperative RFR was associated with a 10 fold increased risk for postoperative AKI. In the same study, levels of urinary cell cycle biomarkers [TIMP-2] × [IGFBP7] before the operation did not discriminate between the groups with and without postoperative AKI. However, [TIMP-2] × [IGFBP7] at post surgery ICU admission predicted AKI with an AUC of 0.87 (95% CI 0.79–0.84).
The role of “novel” biomarkers as indicators of structural renal damage
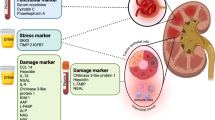
An ideal biomarker should be measurable from non-invasive sources and the test should be easy to perform with a rapid turnover and high reliability. The biomarker should be organ- specific, its levels should correlate with severity of damage and it should be able to pick up AKI in a stage when functional damage is not yet detectable (thus ‘subclinical AKI’). Different biomarkers have different windows of opportunities which makes it difficult to define optimal timing of their analysis after renal injury, especially when the exact moment of the renal insult is unknown [40].
Except for the setting or paediatric cardiovascular surgery, the performance of the “first” generation of the novel biomarkers is poor and adds little or nothing to a clinical model [40,41,42].
One of the explanations might be that biomarkers, besides markers of damage, are often influenced by comorbidities, and systemic inflammation [43,44,45,46].
Correlating biomarkers of structural damage with histological evidence of kidney injury is difficult because kidney biopsies are rarely performed in AKI. In addition, a clear correlation between severity of AKI and histological findings is often lacking and in both human or experimental septic AKI, there are no consistent renal histopathological changes at all [47]. In kidney biopsies performed in hospitalized deceased kidney donors at the time of organ procurement, change in sCr concentration during donor hospitalization performed extremely poor to diagnose AKI, and performance of urinary L-FABP, IL-18, KIM-1 or NGAL was not better. In donors who did not have sCr-based AKI (so-called subclinical AKI), NGAL concentrations were however higher with increasing severities of tubular injury on biopsy [48]. An increase in [TIMP-2] × [IGFBP7] has been considered as the earliest signal of cellular stress [49], because damaged renal epithelial cells activate cell stress responsive genes involved in cell cycle arrest immediately before S phase, and IGFBP7 and TIMP-2 are among the mediators of this process [50, 51].
However, recent experimental work [52] suggests that the urinary TIMP2 × IGFBP7 elevations in AKI-induced by renal ischemia are not due to stress-induced tubular cell gene transcription. Rather, increased glomerular damage, decreased tubular reabsorption, and urinary TIMP2 × IGFBP7 leakage seem to be the most likely mechanisms contributing to the elevated urinary levels.
A recent meta-analysis on urinary TIMP2 × IGFBP7 concluded there was significant heterogeneity among the included studies and that publication bias could not be excluded [53]. Cell cycle inhibitor levels are also influenced by several comorbidities, independent of kidney injury [54]. They can only be used as an add-on test to standard parameters and should thus not be used as a stand-alone test. Also, no data on its performance outside ICU setting are available [55, 56].
Only few studies have used biomarkers as a clinical decision tool and results have been conflicting. The PrevAKI trial [57] was a single-center randomized trial of 276 patients undergoing cardiac surgery with a [TIMP-2] × [IGFBP7] greater than 0.3 within 4 h of surgery. Patients were randomized to either standard care or an intervention group who received a targeted bundle of AKI-prevention strategies for 48 h postoperatively based on the recommendations of the Kidney Disease Improving Global Outcomes (KDIGO) guidelines [3]. A 17% absolute risk reduction in AKI at 72 h and 15% reduction in moderate to severe AKI (KDIGO stage II and III) was demonstrated with this intervention.
The BigpAK study [58] used a similar design and evaluated patients undergoing major elective noncardiac surgery with at least one risk factor for AKI. Patients with elevated [TIMP2] × [IGFBP7] greater than 0.3 postoperatively were randomly allocated to either standard care or application of the KDIGO AKI care bundle that included a nephrology consultation. This policy reduced AKI severity, postoperative creatinine increase, length of ICU, and hospital stay. However, it remains unclear if the use of biomarkers contributed to these relative improvements [59]. At present, there is a paucity of data on the possible outcome benefit using these markers to guide treatment of AKI and it remains unclear whether their use improves patient outcome. Their role in clinical practice remains thus unclear, whereas a potential role in research, be it to explore nephrotoxicity or to enrich trials, is a possibility (Table 1).
Estimation of real time GFR and sCr kinetics
Serial measurements of creatinine clearance provide more timely and accurate information on renal function compared to serial sCr measurements in critically ill patients [11]. An example of a series of consecutive 4 h creatinine clearances in one individual is given in Fig. 2 [60].

(figure modified from Pickering et al. [60])
Delayed increase in serum creatinine following a decrease in GFR as estimated by 4 h creatinine clearance. Open circles indicate the evolution of the measured 4 h creatinine clearance; the closed circles indicate the evolution of the sCr in an individual participating in the EARLY ARF trial (Endre et al. Kidney Int. 2010;77(11):1020–1030)
Several researchers have attempted to develop an equation allowing the calculation of GFR based on kinetic estimation (keGFR) to avoid incorrect interpretation of sCr under the non-steady state conditions of AKI [10, 61].
The kinetic GFR is derived from the initial sCr, the volume of distribution, the creatinine production rate, and the quantitative difference between consecutive sCr values over a given time period. As this calculated GFR is based on a mathematical model the method has inherent limitations that are related to the accuracy of the assumptions of the model. The most problematic issue is that the model assumes a constant creatinine production rate and more or less stable creatinine distribution volume. Also, the formula still requires the use of a baseline sCr value and GFR, obtained prior to the insult causing AKI, which is often not available. Although the baseline GFR can be estimated by back-calculation [1], this is known to be prone to errors [62]. Nevertheless, the kinetic equation can provide a more timely diagnosis of AKI and a better appreciation of the severity of AKI, whereas it can also detect renal recovery earlier. This could be helpful for clinicians, both for prognostication and drug dosing. The use of the kinetic eGFR has been validated in a number of recent independent clinical studies [63,64,65,66].
A point-of-care bedside fluorescence-based measured GFR (mGFR) assay has experimentally been developed for the rapid bedside measurement of GFR which is potentially applicable in AKI. Fluorescent conjugates of a small freely filterable reporter (inulin) and a large non-filterable marker (500 kDa dextran) are infused as a bolus, and the in vivo fluorescent signals in plasma are detected and quantified by a radiometric optical fiber system. The plasma volume is estimated by dilution of the large dextran molecule and the GFR is determined using a radiometric two-compartment method 60 min after injection. The GFR measured by this method presented excellent agreement with a concurrent 6-h iohexol-based GFR measurement [67]. The technique proved to be safe, rapid, accurate and reproducible at measuring GFR across a wide range of kidney functions [68].
Thus fully developed real-time transcutaneous or intravascular monitoring of GFR may prove to be an ideal bedside tool for risk stratification, early diagnosis, prognosis and therapy guidance, especially drug dosing, in AKI.
Conclusion
Current classification criteria for AKI rely on imperfect functional parameters such as serum creatinine and urinary output. The use of 4 h creatinine clearances, kinetic eGFR formulas and bedside real time GFR measurements can be helpful to pick up functional AKI and recovery in an earlier stage. The research on biomarkers resulted in the creation of a concept called ‘subclinical’ AKI. There is currently no hard evidence that the use of biomarkers for kidney damage improves patient outcomes. The potential role of the concept subclinical AKI depends upon the application and setting.
The day we will dispose of more reliable markers, including bedside “true” GFR measurements will probably make the need of a concept such as ‘subclinical AKI’ redundant.
References
Bellomo R, Ronco C, Kellum JA, Mehta RL, Palevsky P (2004) Acute renal failure—definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care 8(4):R204–R212
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG et al (2007) Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 11(2):1–8
Kidney disease (2012) Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney Int Suppl 2:1–138
Fliser D, Laville M, Covic A, Fouque D, Vanholder R, Juillard L et al (2012) A European Renal Best Practice (ERBP) position statement on the Kidney Disease Improving Global Outcomes (KDIGO) clinical practice guidelines on acute kidney injury: part 1: definitions, conservative management and contrast-induced nephropathy. Nephrol Dial Transplant 27(12):4263–4272
Thomas ME, Blaine C, Dawnay A, Devonald MA, Ftouh S, Laing C et al (2015) The definition of acute kidney injury and its use in practice. Kidney Int 87(1):62–73
Vanmassenhove J, Glorieux G, Hoste E, Dhondt A, Vanholder R, Van BW (2013) Urinary output and fractional excretion of sodium and urea as indicators of transient versus intrinsic acute kidney injury during early sepsis. Crit Care 17(5):1–10
Quan S, Pannu N, Wilson T, Ball C, Tan Z, Tonelli M et al (2016) Prognostic implications of adding urine output to serum creatinine measurements for staging of acute kidney injury after major surgery: a cohort study. Nephrol Dial Transplant 31(12):2049–2056
Endre ZH, Pickering JW, Walker RJ (2011) Clearance and beyond: the complementary roles of GFR measurement and injury biomarkers in acute kidney injury (AKI). Am J Physiol Renal Physiol 301(4):F697–F707
Waikar SS, Bonventre JV (2009) Creatinine kinetics and the definition of acute kidney injury. J Am Soc Nephrol 20(3):672–679
Chen S (2013) Retooling the creatinine clearance equation to estimate kinetic GFR when the plasma creatinine is changing acutely. J Am Soc Nephrol 24(6):877–888
Pickering JW, Frampton CM, Walker RJ, Shaw GM, Endre ZH (2012) Four hour creatinine clearance is better than plasma creatinine for monitoring renal function in critically ill patients. Crit Care (London England) 16(3):R107
Haase M, Kellum JA, Ronco C (2012) Subclinical AKI—an emerging syndrome with important consequences. Nat Rev Nephrol 8(12):735–739
Haase M, Devarajan P, Haase-Fielitz A, Bellomo R, Cruz DN, Wagener G et al (2011) The outcome of neutrophil gelatinase-associated lipocalin-positive subclinical acute kidney injury: a multicenter pooled analysis of prospective studies. J Am Coll Cardiol 57(17):1752–1761
Murray PT, Mehta RL, Shaw A, Ronco C, Endre Z, Kellum JA et al (2014) Potential use of biomarkers in acute kidney injury: report and summary of recommendations from the 10th Acute Dialysis Quality Initiative consensus conference. Kidney Int 85(3):513–521
Nickolas TL, Schmidt-Ott KM, Canetta P, Forster C, Singer E, Sise M et al (2012) Diagnostic and prognostic stratification in the emergency department using urinary biomarkers of nephron damage: a multicenter prospective cohort study. J Am Coll Cardiol 59(3):246–255
Di Somma S, Magrini L, De Berardinis B, Marino R, Ferri E, Moscatelli P et al (2013) Additive value of blood neutrophil gelatinase-associated lipocalin to clinical judgement in acute kidney injury diagnosis and mortality prediction in patients hospitalized from the emergency department. Crit Care (London England) 17(1):R29
Coca SG, Garg AX, Thiessen-Philbrook H, Koyner JL, Patel UD, Krumholz HM et al (2014) Urinary biomarkers of AKI and mortality 3 years after cardiac surgery. J Am Soc Nephrol 25(5):1063–1071
Hall IE, Doshi MD, Reese PP, Marcus RJ, Thiessen-Philbrook H, Parikh CR (2012) Association between peritransplant kidney injury biomarkers and 1-year allograft outcomes. Clin J Am Soc Nephrol 7(8):1224–1233
Anaya-Ayala JE, Ismail N, Reardon MJ, Peden EK (2012) Endovascular salvage of a right brachial artery-right atrium hemodialysis graft using a covered endoprosthesis. J Vasc Access 13(4):520–523
Albert C, Albert A, Kube J, Bellomo R, Wettersten N, Kuppe H et al (2018) Urinary biomarkers may provide prognostic information for subclinical acute kidney injury after cardiac surgery. J Thorac Cardiovasc Surg 155(6):2441–2452 e13
McWilliam SJ, Antoine DJ, Jorgensen AL, Smyth RL, Pirmohamed M (2018) Urinary biomarkers of aminoglycoside-induced nephrotoxicity in cystic fibrosis: kidney injury molecule-1 and neutrophil gelatinase-associated lipocalin. Science 8(1):5094
Nehus E, Kaddourah A, Bennett M, Pyles O, Devarajan P (2017) Subclinical kidney injury in children receiving nonsteroidal anti-inflammatory drugs after cardiac surgery. J Pediatr 189:175–180
Bachorzewska-Gajewska H, Malyszko J, Sitniewska E, Malyszko JS, Dobrzycki S (2006) Neutrophil-gelatinase-associated lipocalin and renal function after percutaneous coronary interventions. Am J Nephrol 26(3):287–292
Bachorzewska-Gajewska H, Malyszko J, Sitniewska E, Malyszko JS, Dobrzycki S (2007) Neutrophil gelatinase-associated lipocalin (NGAL) correlations with cystatin C, serum creatinine and eGFR in patients with normal serum creatinine undergoing coronary angiography. Nephrol Dial Transplant 22(1):295–296
Kane-Gill SL, Smithburger PL, Kashani K, Kellum JA, Frazee E (2017) Clinical relevance and predictive value of damage biomarkers of drug-induced kidney injury. Drug Saf 40(11):1049–1074
Bellomo R, Bagshaw S, Langenberg C, Ronco C (2007) Pre-renal azotemia: a flawed paradigm in critically ill septic patients? Contrib Nephrol 156:1–9
Parikh CR, Coca SG (2010) Acute kidney injury: defining prerenal azotemia in clinical practice and research. Nat Rev Nephrol 6(11):641–642
Belcher JM, Parikh CR (2011) Is it time to evolve past the prerenal azotemia versus acute tubular necrosis classification? Clin J Am Soc Nephrol 6(10):2332–2334
Schneider AG, Bellomo R (2013) Urinalysis and pre-renal acute kidney injury: time to move on. Crit Care (London, England) 17(3):141
Au V, Feit J, Barasch J, Sladen RN, Wagener G (2016) Urinary neutrophil gelatinase-associated lipocalin (NGAL) distinguishes sustained from transient acute kidney injury after general surgery. Kidney Int Rep 1(1):3–9
Xu K, Rosenstiel P, Paragas N, Hinze C, Gao X, Huai Shen T et al (2017) Unique transcriptional programs identify subtypes of AKI. J Am Soc Nephrol 28(6):1729–1740
Devarajan P (2017) Acute kidney injury: acute kidney injury: still misunderstood and misdiagnosed. Nat Rev Nephrol 13(3):137–138
Molitoris BA. Rethinking CKD, Evaluation (2017) Should we be quantifying basal or stimulated GFR to maximize precision and sensitivity? Am J Kidney Dis 69(5):675–683
Molitoris BA, Reilly ES (2016) Quantifying glomerular filtration rates in acute kidney injury: a requirement for translational success. Semin Nephrol 36(1):31–41
Bosch JP, Lew S, Glabman S, Lauer A (1986) Renal hemodynamic changes in humans. Response to protein loading in normal and diseased kidneys. Am J Med 81(5):809–815
Claus BO, Hoste EA, Colpaert K, Robays H, Decruyenaere J, De Waele JJ (2013) Augmented renal clearance is a common finding with worse clinical outcome in critically ill patients receiving antimicrobial therapy. J Crit Care 28(5):695–700
Udy AA, Baptista JP, Lim NL, Joynt GM, Jarrett P, Wockner L et al (2014) Augmented renal clearance in the ICU: results of a multicenter observational study of renal function in critically ill patients with normal plasma creatinine concentrations. Crit Care Med 42(3):520–527
Baptista JP, Udy AA, Sousa E, Pimentel J, Wang L, Roberts JA et al (2011) A comparison of estimates of glomerular filtration in critically ill patients with augmented renal clearance. Crit Care (London England) 15(3):R139
Husain-Syed F, Ferrari F, Sharma A, Danesi TH, Bezerra P, Lopez-Giacoman S et al (2018) Preoperative renal functional reserve predicts risk of acute kidney injury after cardiac operation. Ann Thorac Surg 105(4):1094–1101
Vanmassenhove J, Vanholder R, Nagler E, Van BW (2013) Urinary and serum biomarkers for the diagnosis of acute kidney injury: an in-depth review of the literature. Nephrol Dial Transplant 28(2):254–273
Lameire NH, Vanholder RC, Van Biesen WA (2011) How to use biomarkers efficiently in acute kidney injury. Kidney Int 79(10):1047–1050
Malhotra R, Siew ED (2017) Biomarkers for the early detection and prognosis of acute kidney injury. Clin J Am Soc Nephrol 12(1):149–173
Vanmassenhove J, Glorieux G, Lameire N, Hoste E, Dhondt A, Vanholder R et al (2015) Influence of severity of illness on neutrophil gelatinase-associated lipocalin performance as a marker of acute kidney injury: a prospective cohort study of patients with sepsis. BMC Nephrol 16:18
Giasson J, Li GH, Chen Y (2011) Neutrophil gelatinase-associated lipocalin (NGAL) as a new biomarker for non-acute kidney injury (AKI) diseases. Inflamm Allergy Drug Targets 10(4):272–282
Decavele AS, Dhondt L, De Buyzere ML, Delanghe JR (2011) Increased urinary neutrophil gelatinase associated lipocalin in urinary tract infections and leukocyturia. Clin Chem Lab Med 49(6):999–1003
Martensson J, Bellomo R (2014) The rise and fall of NGAL in acute kidney injury. Blood Purif 37(4):304–310
Langenberg C, Bagshaw SM, May CN, Bellomo R (2008) The histopathology of septic acute kidney injury: a systematic review. Crit Care 12(2):R38
Moledina DG, Hall IE, Thiessen-Philbrook H, Reese PP, Weng FL, Schroppel B et al (2017) Performance of serum creatinine and kidney injury biomarkers for diagnosing histologic acute tubular injury. Am J Kidney Dis 70(6):807–816
Kashani K, Al-Khafaji A, Ardiles T, Artigas A, Bagshaw SM, Bell M et al (2013) Discovery and validation of cell cycle arrest biomarkers in human acute kidney injury. Crit Care 17(1):R25
Ronco C (2016) Acute kidney injury: from clinical to molecular diagnosis. Crit Care (London England) 20(1):201
Ronco C (2016) Cell-cycle arrest biomarkers: the light at the end of the acute kidney injury tunnel. Nephrol Dial Transplant 31(1):3–5
Johnson ACM, Zager RA (2018) Mechanisms underlying increased TIMP2 and IGFBP7 urinary excretion in experimental AKI. J Am Soc Nephrol 29(8):2157–2167
Liu C, Lu X, Mao Z, Kang H, Liu H, Pan L et al (2017) The diagnostic accuracy of urinary [TIMP-2]·[IGFBP7] for acute kidney injury in adults: a PRISMA-compliant meta-analysis. Medicine (Baltimore) 96(27):e7484
Bell M, Larsson A, Venge P, Bellomo R, Martensson J (2015) Assessment of cell-cycle arrest biomarkers to predict early and delayed acute kidney injury. Dis Mark 2015:158658
Vijayan A, Faubel S, Askenazi DJ, Cerda J, Fissell WH, Heung M et al (2016) Clinical use of the urine biomarker [TIMP-2] × [IGFBP7] for acute kidney injury risk assessment. Am J Kidney Dis 68(1):19–28
Lameire N, Vanmassenhove J, Van Biesen W, Vanholder R (2016) The cell cycle biomarkers: promising research, but do not oversell them. Clin Kidney J 9(3):353–358
Meersch M, Schmidt C, Hoffmeier A, Van Aken H, Wempe C, Gerss J et al (2017) Prevention of cardiac surgery-associated AKI by implementing the KDIGO guidelines in high risk patients identified by biomarkers: the PrevAKI randomized controlled trial. Intensive Care Med 43(11):1551–1561
Gocze I, Jauch D, Gotz M, Kennedy P, Jung B, Zeman F et al (2018) Biomarker-guided intervention to prevent acute kidney injury after major surgery: the prospective randomized BigpAK study. Ann Surg 267(6):1013–1020
Singh AN, Kilambi R (2018) Biomarker-guided intervention to prevent AKI or KDIGO care bundle to prevent AKI in high-risk patients undergoing major surgery? Ann Surg 268(6):e67–e68
Pickering JW, Endre ZH (2012) Challenges facing early detection of acute kidney injury in the critically ill. World J Crit Care Med 1(3):61–66
Chen S (2018) Kinetic glomerular filtration rate in routine clinical practice-applications and possibilities. Adv Chronic Kidney Dis 25(1):105–14
Siew ED, Matheny ME, Ikizler TA, Lewis JB, Miller RA, Waitman LR et al (2010) Commonly used surrogates for baseline renal function affect the classification and prognosis of acute kidney injury. Kidney Int 77:536–542
Pianta TJ, Endre ZH, Pickering JW, Buckley NA, Peake PW (2015) Kinetic estimation of GFR improves prediction of dialysis and recovery after kidney transplantation. PLoS One 10(5):e0125669
Seelhammer TG, Maile MD, Heung M, Haft JW, Jewell ES, Engoren M (2016) Kinetic estimated glomerular filtration rate and acute kidney injury in cardiac surgery patients. J Crit Care 31(1):249–254
Dewitte A, Joannes-Boyau O, Sidobre C, Fleureau C, Bats ML, Derache P et al (2015) Kinetic eGFR and novel AKI biomarkers to predict renal recovery. Clin J Am Soc Nephrol 10(11):1900–1910
O’Sullivan ED, Doyle A (2017) The clinical utility of kinetic glomerular filtration rate. Clin Kidney J 10(2):202–208
Wang E, Meier DJ, Sandoval RM, Von Hendy-Willson VE, Pressler BM, Bunch RM et al (2012) A portable fiberoptic ratiometric fluorescence analyzer provides rapid point-of-care determination of glomerular filtration rate in large animals. Kidney Int 81(1):112–117
Rizk DV, Meier D, Sandoval RM, Chacana T, Reilly ES, Seegmiller JC et al (2018) A novel method for rapid bedside measurement of GFR. J Am Soc Nephrol 29(6):1609–1613
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interests to declare.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Vanmassenhove, J., Van Biesen, W., Vanholder, R. et al. Subclinical AKI: ready for primetime in clinical practice?. J Nephrol 32, 9–16 (2019). https://doi.org/10.1007/s40620-018-00566-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-018-00566-y