Abstract
Background
Limited research have examined predictors of illicit use of drugs and binge drinking among gay, bisexual, and other men who have sex with men (MSM) in Kazakhstan and Central Asia. This study examines earlier sexual debut as a risk factor for lifetime and recent substance use behaviors among MSM in Kazakhstan.
Methods
We conducted a secondary analysis of self-reported data from a NIDA-funded HIV prevention trial including 902 adult cisgender MSM in Kazakhstan who completed structured screening interviews. Logistic regression models were used to estimate associations between earlier sexual debut (ages 16 and older as the reference group) and lifetime and recent substance use, with covariance adjustment for sociodemographic characteristics.
Results
The majority of MSM in our sample reported lifetime binge drinking behavior (73%) and illicit use of drugs (65%). Participants with an earlier sexual debut before 13 years old had significantly higher odds of lifetime binge drinking and any illicit use of drugs (aOR = 2.3, 95%CI: 1.2–4.5; aOR = 3.0, 95%CI: 1.6–5.8). MSM who reported an earlier sexual debut between 13–15 years old had significantly higher odds of lifetime binge drinking and illicit use of any drugs (aOR = 1.6, 95%CI: 1.1–2.3; aOR = 1.6, 95%CI: 1.1–2.3); as well as recent binge drinking behavior (aOR = 1.6, 95%CI: 1.2–2.3).
Conclusion
Future research should examine pathways between earlier sexual experiences and substance use behaviors among sexually diverse populations. Earlier sexual experiences during childhood and adolescence may be relevant contextual information for interventions aimed at substance use risk prevention, treatment, and recovery among MSM populations.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Gay, bisexual, and other men who have sex with men (MSM) are a relatively understudied population in Kazakhstan and Central Asia, and limited research has examined how earlier sexual experiences during childhood and adolescence are related to HIV-risk factors, such as substance use, among MSM in Kazakhstan. MSM in Kazakhstan are navigating a recent rise in HIV incidence (UNAIDS, 2020), and substance use has been highlighted as a key possible driver of HIV disparities among MSM in Kazakhstan (ECOM, 2018; UNAIDS, 2020). Earlier age of first sexual activity, or earlier sexual debut, has been associated with substance use behaviors among sexually diverse populations globally, yet these factors have not been investigated among MSM in Kazakhstan (Cheung et al., 2014; Halkitis et al., 2021; Lowry et al., 2017).
Sexual Development and Sexual Debut Timing
Previous research have explored reports of heterosexual young people’s sexual debut, but relatively fewer studies have examined sexual and gender diverse people’s first partnered sexual experiences (Averett et al., 2014; Babin & Humphreys, 2021; Dion & Boislard, 2020). As young people sexually develop they often become curious about aspects of sexual activity—however, common forms of exploratory sexual behaviors can vary between developmental age groups (Wurtele & Kenny, 2011). For example, although partnered sexual intercourse is frequently reported among adolescents, these behaviors are rarely reported among children ages twelve and under (Hornor, 2004; Kellogg, 2010; Lindberg et al., 2021; Wurtele & Kenny, 2011); it is important to note that among pre-teenage children, reports of oral-genital, anal, and vaginal sex are often indicators of child sexual abuse (CSA) victimization as well as other forms of abuse and neglect (Hornor, 2004; Kellogg, 2010; Wurtele & Kenny, 2011). Although it is common for children and adolescents to develop curiosity about their own bodies, as well as other people’s bodies, earlier age of sexual debut is associated with higher risk behaviors including substance use (Clark et al., 2020; Wurtele & Kenny, 2011).
Earlier Sexual Debut and Substance Use
Substance use behaviors associated with earlier sexual debut have been mainly explored among adolescent heterosexual people in the USA, and fewer studies have examined sexually diverse and global populations (Cavazos-Rehg et al., 2009; Halkitis et al., 2021; Lowry et al., 2017; Outlaw et al., 2011; Xu et al., 2016).
In the general population, earlier sexual debut has been associated with substance use behaviors. A longitudinal study of Mexican-origin youth found that earlier sexual debut was associated with increased risk of long-term trends in substance use throughout adolescence (Clark et al., 2020). A study of adolescents in eight African countries found that young people who began having sex before 15 years old were more likely to report alcohol, tobacco, and illicit use of drugs (Peltzer, 2010). Among a sample of adolescents from six Caribbean countries, earlier sexual debut was associated with male gender and substance use (e.g., smoking and alcohol use) (Peltzer & Pengpid, 2015).
Among sexually diverse young people in the USA, earlier sexual debut before the age of 13 has been linked to drug-related risk behaviors including recent cigarette, alcohol, and marijuana use as well as lifetime use of prescription drugs, cocaine, methamphetamine, heroin, and injected drugs (Lowry et al., 2017). Specifically among US MSM, sexual debut before the age of 16 has been associated with lifetime drug use, particularly marijuana use (Outlaw et al., 2011). A qualitative study of non-gay identified (NGI) Latino men who have sex with men and women found that those who experienced a sexual debut between 13 and 20 years of age were more likely to be recruited into sex work as teenagers by drug-involved NGI peers (Finlinson et al., 2006). A longitudinal study of MSM in the Netherlands found that MSM with a higher behavioral risk score for HIV seroconversion were more likely to report an earlier sexual debut and increased frequency of substance use over time (Basten et al., 2018).
Earlier Sexual Debut, Risky Sexual Behavior, and Substance Use in Kazakhstan
Limited research has investigated the role or potential implications of earlier sexual debut among people in Kazakhstan. A nationally representative survey of adolescents in Kazakhstan found that approximately a third of young people were sexually active by their 18th birthday, and that the average age of sexual debut among sexually active adolescents was 16 years old (UNFPA, 2018). Among a study sample of medical students in Semey, Kazakhstan, men reported an earlier median age of sexual debut (16 years old) compared to women (18 years old) (Hansson et al., 2008). The difference in reported sexual debut by gender in this region may be a result of sociocultural double standards that encourages men’s heterosexual sexual behavior and stigmatizes women’s sexual behavior (Hansson et al., 2008). Information about sexual debut or earlier sexual behavior among sexually diverse people in Kazakhstan is limited and may be a result of broader issues around stigma against LGBTQ people (Hansson et al., 2008; Latypov et al., 2013).
Higher risk sexual behaviors (e.g., condomless sex with a partner) and substance use have been more widely investigated in Kazakhstan as a key factor underlying rising HIV prevalence (Jiwatram-Negrón et al., 2018; Marotta et al., 2018). Couple-based and intimate partner focused HIV prevention research among people in Kazakhstan have frequently focused on the role of risky sexual behavior in conjunction with injection drug use and other forms of substance use (El-Bassel et al., 2014; Gilbert et al., 2010; Marotta et al., 2018; Shaw et al., 2017). HIV prevention microfinance interventions have been implemented for women in Kazakhstan who engage in substance use and sex work (McCrimmon et al., 2018; Mergenova et al., 2019). Although substance use research with MSM in Kazakhstan is limited, one study based in Almaty found that condomless anal intercourse was significantly associated with non-injection drug use (Berry et al., 2012). Given evidence of associations between HIV-risk and substance use among MSM in Kazakhstan, and connections between substance use and sexual risk in other contexts, further insight into earlier sexual debut experiences among MSM in Kazakhstan is needed.
Study Aims
This study seeks to advance our understanding of the experiences of sexually diverse populations in Kazakhstan by examining whether earlier sexual debut is associated with an increased likelihood of substance use in a sample of MSM from three major cities. Specifically, we explore the prevalence of earlier sexual debut and whether earlier sexual debut is associated with recent and lifetime binge drinking behaviors and illicit use of drugs among MSM in this region.
Materials and Methods
Data Collection and Procedures
This study uses data obtained during the conduct of a NIDA-funded clinical trial of a behavioral intervention seeking to increase the engagement of MSM who use substances (i.e., binge drink, illicit use of drugs) in Kazakhstan in the HIV care continuum (see Paine et al., 2021). In the parent study, a stepped wedge design was used to test the intervention across three geographically disparate cities: Almaty, Nur-Sultan (formerly Astana), and Shymkent. The clinical trial commenced in 2018 with all cities in the “pre-implementation” phase. After pre-implementation, the “implementation” clinical trial phase was conducted in each city spaced six months apart. The data presented in this report utilized self-reported data collected during structured screening interviews conducted in Russian or Kazakh in Almaty, Nur-Sultan, and Shymkent that were completed between July 2018 and September 2021 (N = 902). All study procedures were approved by the Institutional Review Board (IRB) at Columbia University (Protocol # IRB—AAAQ7251) and the Local Ethical Committee at Farabi Kazakh National University (Protocol # IRB—A052).
Participants
Screened individuals were considered eligible for these analyses if they were 18 years and older, self-identified as a cisgender man, and reported having had consensual sex with a man.
Measures
Earlier Sexual Debut
Participants self-reported how old they were when they first had sex, which was characterized as their age of sexual debut. Due to the cultural relativity and subjectivity of what may be socially considered a normal age of sexual debut, earlier sexual debut was determined by the two lowest reported interquartile age groups in our MSM sample. Sexual debut was divided into three categories—those with a sexual debut before the age of 13 years old, between 13 and 15 years old, and 16 years and older with the former two categories indicating earlier sexual debut. The purpose of having two distinct earlier sexual debut categories was to recognize a possible difference in health behavior risk for those who experienced earlier sexual behavior prior to being a teenager (Hall et al., 2020). Additionally, the age of consent in Kazakhstan is 16 years old which coincides with our reference group (UNFPA, n.d.).
Substance Use
Participants were asked about recent (past 90 days) and lifetime binge drinking behavior as well as illicit use of drugs which included marijuana, heroin, other opioids, stimulants, cocaine, hallucinogens, inhalants, and club drugs. Any recent or lifetime illicit substance use was calculated using Boolean OR operators among all of the reported illicit drugs. Binge drinking was defined as consuming five or more drinks within a two-hour period (Courtney & Polich, 2009).
Covariates
The following population characteristics as covariates were included in all multivariable models: age; city (Almaty, Nur-Sultan, and Shymkent); marital status (single, married, no longer with a spouse, or “other”); highest educational attainment level (9th grade or less, high school or vocational, bachelor’s degree or more, or “other” category); employment (full time, part time, unemployed, or “other”); housing insecurity (past 6 months); self-reported HIV status (positive, negative, or unknown); self-reported sexual orientation (heterosexual, bisexual or gay, and other); and self-reported estimated income in Kazakhstan Tenge (KZT) per month for the prior 6 months. Income was transformed using log squared to reduce heteroscedasticity.
Statistical Analyses
For our descriptive analyses, we assessed the frequencies of population sociodemographic characteristics, and substance use, and age of sexual debut (see Tables 1, 2 and 3). For bivariate analyses, we used chi-square tests to evaluate any associations between earlier sexual debut and substance use behaviors. Finally, for the multivariable models, we used logistic regression to assess associations between earlier sexual debut and substance use while adjusting for age, city, marital status, education, employment, HIV-status, sexual orientation, and income (see Table 4).
Results
Sample Characteristics
Table 1 displays the population characteristics of the sample. Most of the men in our sample lived in Almaty (41%); about half had a college education or more (49%); and were 28 years old on average. The majority of participants worked full time (52%); were housing secure (91%); and had an average monthly income of approximately 140,000 KZT (about 300 USD) over the past 6 months. The majority of MSM in the sample reported being single (79%), HIV-negative (60%), and identified as gay, bisexual, or a sexual orientation other than heterosexual (97%). Approximately two-thirds (67%) of MSM participants were 16 years or older at the time of their sexual debut.
Substance Use
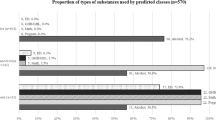
Table 2 displays descriptive statistics for substance use. The most frequently reported types of substance use were lifetime binge drinking (73%) and any use of illicit substances (65%), followed by lifetime marijuana use (48%) inhalants (34%). The same pattern occurred for reported substance use in the past 90 days, with the greatest reports of binge drinking (57%) and any illicit use of substances (28%), followed by marijuana (16%) and inhalant use (13%).
Associations Between Earlier Sexual Debut and Substance Use
Table 3 presents the distribution of the sample with respect to earlier sexual debut and substance use. Bivariate analyses indicated that earlier sexual debut was significantly associated with binge drinking and illicit drug use. Compared to participants reporting a sexual debut at age 16 or older, earlier sexual debut was associated with higher rates of ever binge drinking and using marijuana, heroin, opioids, stimulants, cocaine, club drugs, and any illicit drugs. Compared to sexual debut at 16 or older, earlier sexual debut was associated with higher rates of binge drinking and marijuana, heroin, opioid, stimulant, and any illicit drug use in the past 90 days.
Results from multivariable models are presented in Table 4. There was a significant relationship between earlier sexual debut and substance use. Compared to participants with a sexual debut of 16 years of age or older, those with sexual debuts before the age of 13 had significantly higher odds of ever reporting to binge drink, use marijuana, or any illicit drugs (aOR = 2.3, 95%CI: 1.2–4.5; aOR = 3.0, 95%CI: 1.7–5.4; aOR = 3.0, 95%CI: 1.6–5.8). MSM with sexual debuts between the ages of 13 and 15 years old had significantly higher odds of ever binge drinking, using marijuana, heroin, other opioids, stimulants, cocaine, club drugs, or any illicit drugs (aOR = 1.6, 95%CI: 1.1–2.3; aOR = 1.4, 95%CI: 1.0–2.0; aOR = 3.8, 95%CI: 1.8–8.2; aOR = 2.1, 95%CI: 1.1–3.7; aOR = 2.4, 95%CI: 1.5–3.8; aOR = 2.7, 95%CI: 1.3–5.5; aOR = 2.0, 95%CI: 1.2–3.4; aOR = 1.6, 95%CI: 1.1–2.3), as well as binge drinking, use marijuana, or stimulants in the past 90 days (aOR = 1.6, 95%CI: 1.2–2.3; aOR = 1.5, 95%CI: 1.0–2.3; aOR = 4.3, 95%CI: 2.1–8.8).
Discussion
In our final models of earlier sexual debut and substance use among MSM in Kazakhstan, we found significant associations between earlier sexual debut and binge drinking as well as illicit use of drugs. Although earlier sexual debut has been found to be a significant risk factor for other sexual risk behaviors among MSM in China, sexual debut has rarely been assessed as a risk factor for substance use among this minority population in Central Asia or Eastern Europe, limiting our knowledge of the broader connections between sexual behavior and substance use (Tang et al., 2020; Wirtz et al., 2013; Xu et al., 2016; Zou et al., 2016). Our present study suggests that earlier age of sexual onset is a relevant risk factor for a variety of substance use behaviors among MSM in Kazakhstan, warranting incorporation of age of sexual debut in future substance use research among sexually diverse populations.
Our findings make an important contribution to the current sexuality and substance use literature. Earlier sexual debut is often measured using one discrete age marker; however, we examined associations between average age of sexual debut (ages 16 and over) and two distinct age ranges of earlier sexual debut to account for variability between pre- and post-teenage sexual debuts and substance use risk (Lowry et al., 2017; Sawyer et al., 2018). Our findings support differentiating between earlier sexual debut groups. Although in our final models both earlier sexual debut categories were significantly associated with substance use risk compared to a sexual debut 16 years or older, MSM in the earliest sexual debut category (ages 12 and under) reported greater adjusted odd ratios of lifetime binge drinking, marijuana use, or any illicit substance. Due to concerns that sexual debut before 13 years old may be a result of CSA, future research should screen for CSA as a potential risk factor for substance use behaviors among MSM in Kazakhstan. These results suggest that age of sexual onset during earlier adolescence or childhood may be a particularly vulnerable time for sexual decision-making and identity formation that may result in higher-risk behaviors in the form of substance use.
Service needs that may be relevant for MSM in Kazakhstan could include additional clinical attention towards assessing and addressing potential CSA as well as voluntary or consensual sexual activity during earlier adolescence and childhood. Within Kazakhstan, adolescents have limited access to sexual and reproductive health information, particularly in the native Kazakh language, and sexual education among young people remains a taboo social topic (WHO, 2020). Our findings warrant an increase of sexual health resources for a wide range of young people—including children and adolescents—and reducing barriers to care for youth and MSM. Overall, further research is needed to better elucidate causal pathways between earlier sexual experiences among sexually diverse people and risky substance use behaviors.
Clinicians who provide HIV prevention services for MSM who use substances in Kazakhstan should consider incorporating sexual history screening questions that inquire about childhood and adolescent sexual experiences, particularly non-consensual sexual experiences during this developmental period. Within the broader literature, trauma-informed HIV prevention and treatment among MSM has been recognized as an important aspect of holistic care for MSM at high co-occurring risk of HIV and trauma (Brezing et al., 2015; Brown & Adeagbo, 2022; Sales et al., 2016). MSM at elevated risk of HIV-infection who use substances and have a history of CSA-victimization may need comprehensive healthcare services, such as HIV prevention resources (e.g., HIV testing, pre-exposure prophylaxis), substance use harm reduction services, and trauma-informed mental health resources. MSM who use substances and are at elevated risk of HIV infection may require a multipronged approach to clinical care that addresses complex co-occurring issues, such as substance use, HIV risk, and history of CSA victimization.
Limitations
This study had several limitations. Some of our models were limited by small proportions of participants using certain illicit substances, particularly recent illicit use of drugs. This study is not necessarily representative of MSM in Kazakhstan, and all participants were recruited from major cities in the region which does not capture rural MSM experiences. The earlier sexual debut question used was a relatively broad single question about age of first sexual activity that did not assess information about the sexual partner (e.g., the partner’s gender or age) and whether this experience was consensual or non-consensual. Additionally, the small number of participants reporting an earlier sexual debut before 13 years old (n = 75) may have limited our ability to capture associations between substance use risks and earlier sexual debut among the sample size of MSM. Although sexual debut presumably predates the majority of substance use behaviors reported by adults, our study is cross-sectional and is unable to assess temporal sequences. Lastly, social desirability bias may have influenced how participants self-reported socially sensitive behaviors, such as substance use and sexual behaviors during childhood or adolescence.
Conclusion
Sexual experiences during childhood and early adolescence are a potential risk factor for current and lifetime substance use among MSM in Kazakhstan. Earlier onset of sexual activity was significantly associated with lifetime marijuana, heroin, opioid, stimulant, cocaine, and club drug use as well as binge drinking and any illicit use of drugs. Earlier sexual debut also was significantly associated with recent binge drinking, marijuana, and stimulant use. Further research is needed to examine how consensual and non-consensual sexual experiences during childhood and adolescence are linked to risky substance use behaviors among men who have sex with men.
Availability of Data and Material
The dataset generated and/or analyzed during the current study is not publicly available.
References
Averett, P., Moore, A., & Price, L. (2014). Virginity definitions and meaning among the LGBT community. Journal of Gay & Lesbian Social Services, 26(3), 259–278. https://doi.org/10.1080/10538720.2014.924802
Babin, C., & Humphreys, T. (2021). Virginity beliefs in lesbian, gay, and bisexual individuals experiencing same- and different-sex “first” times. The Canadian Journal of Human Sexuality, 30(3), 397–409. https://doi.org/10.3138/cjhs.2021-0029
Basten, M., Heijne, J. C. M., Geskus, R., Den Daas, C., Kretzschmar, M., & Matser, A. (2018). Sexual risk behaviour trajectories among MSM at risk for HIV in Amsterdam, the Netherlands. AIDS (london, England), 32(9), 1185–1192. https://doi.org/10.1097/QAD.0000000000001803
Berry, M., Wirtz, A. L., Janayeva, A., Ragoza, V., Terlikbayeva, A., Amirov, B., Baral, S., & Beyrer, C. (2012). Risk factors for HIV and unprotected anal intercourse among men who have sex with men (MSM) in Almaty, Kazakhstan. PLoS ONE, 7(8), e43071. https://doi.org/10.1371/journal.pone.0043071
Brezing, C., Ferrara, M., & Freudenreich, O. (2015). The syndemic illness of HIV and trauma: Implications for a trauma-informed model of care. Psychosomatics, 56(2), 107–118.
Brown, M. J., & Adeagbo, O. (2022). Trauma-informed HIV care interventions: Towards a holistic approach. Current HIV/AIDS Reports, 19(3), 177–183.
Cavazos-Rehg, P. A., Krauss, M. J., Spitznagel, E. L., Schootman, M., Bucholz, K. K., Peipert, J. F., Sanders-Thompson, V., Cottler, L. B., & Bierut, L. J. (2009). Age of sexual debut among US adolescents. Contraception, 80(2), 158–162. https://doi.org/10.1016/j.contraception.2009.02.014
Cheung, D. H., Suharlim, C., Guadamuz, T. E., Lim, S. H., Koe, S., & Wei, C. (2014). Earlier anal sexarche and co-occurring sexual risk are associated with current HIV-related risk behaviors among an online sample of men who have sex with men in Asia. AIDS and Behavior, 18(12), 2423–2431. https://doi.org/10.1007/s10461-014-0821-0
Clark, D. A., Donnellan, M. B., Durbin, C. E., Nuttall, A. K., Hicks, B. M., & Robins, R. W. (2020). Sex, drugs, and early emerging risk: Examining the association between sexual debut and substance use across adolescence. PLoS ONE, 15(2), e0228432. https://doi.org/10.1371/journal.pone.0228432
Courtney, K. E., & Polich, J. (2009). Binge drinking in young adults: Data, definitions, and determinants. Psychological Bulletin, 135(1), 142–156. https://doi.org/10.1037/a0014414
Dion, L., & Boislard, M.-A. (2020). “Of course we had sex!”: A qualitative exploration of first sex among women who have sex with women. The Canadian Journal of Human Sexuality, 29(2), 249–261. https://doi.org/10.3138/cjhs.2020-0019
El-Bassel, N., Gilbert, L., Terlikbayeva, A., Beyrer, C., Wu, E., Chang, M., Hunt, T., Ismayilova, L., Shaw, S. A., Primbetova, S., Rozental, Y., Zhussupov, B., & Tukeyev, M. (2014). Effects of a couple-based intervention to reduce risks for HIV, HCV, and STIs among drug-involved heterosexual couples in Kazakhstan: A randomized controlled trial. Journal of Acquired Immune Deficiency Syndromes (1999), 67(2), 196–203. https://doi.org/10.1097/QAI.0000000000000277
Eurasian Coalition on Male Health: Brief on HIV among MSM in Kazakhstan (2018). Retrieved March 2022, from http://ecom.ngo
Finlinson, H. A., Colón, H. M., Robles, R. R., & Soto, M. (2006). Sexual identity formation and AIDS prevention: An exploratory study of non-gay-identified Puerto Rican MSM from Working Class Neighborhoods. AIDS and Behavior, 10(5), 531–539. https://doi.org/10.1007/s10461-006-9107-5
Gilbert, L., El-Bassel, N., Terlikbayeva, A., Rozental, Y., Chang, M., Brisson, A., Wu, E., & Bakpayev, M. (2010). Couple-based HIV prevention for injecting drug users in Kazakhstan: A pilot intervention study. Journal of Prevention & Intervention in the Community, 38(2), 162–176. https://doi.org/10.1080/10852351003640914
Halkitis, P. N., LoSchiavo, C., Martino, R. J., Cruz, B. M. D. L., Stults, C. B., & Krause, K. D. (2021). Age of sexual debut among young gay-identified sexual minority men: The P18 cohort study. The Journal of Sex Research, 58(5), 573–580. https://doi.org/10.1080/00224499.2020.1783505
Hall, C. D. X., Moran, K., Newcomb, M. E., & Mustanski, B. (2020). Age of occurrence and severity of childhood sexual abuse: Impacts on health outcomes in men who have sex with men and transgender women. The Journal of Sex Research, 56(6), 763–774. https://doi.org/10.1080/00224499.2020.1840497
Hansson, M., Stockfelt, L., Urazalin, M., Ahlm, C., & Andersson, R. (2008). HIV/AIDS awareness and risk behavior among students in Semey, Kazakhstan: A cross-sectional survey. BMC International Health and Human Rights, 8(1), 14. https://doi.org/10.1186/1472-698X-8-14
Hornor, G. (2004). Sexual behavior in children: Normal or not? Journal of Pediatric Health Care, 18(2), 57–64. https://doi.org/10.1016/S0891-5245(03)00154-8
Jiwatram-Negrón, T., Michalopoulos, L. M., & El-Bassel, N. (2018). The syndemic effect of injection drug use, intimate partner violence, and HIV on mental health among drug-involved women in Kazakhstan. Global Social Welfare, 5(2), 71–81. https://doi.org/10.1007/s40609-018-0112-1
Kellogg, N. D. (2010). Sexual behaviors in children: Evaluation and management. American Family Physician, 82(10), 1233–1238.
Latypov, A., Rhodes, T., & Reynolds, L. (2013). Prohibition, stigma and violence against men who have sex with men: Effects on HIV in Central Asia. Central Asian Survey, 32(1), 52–65. https://doi.org/10.1080/02634937.2013.768059
Lindberg, L. D., Firestein, L., & Beavin, C. (2021). Trends in U.S. adolescent sexual behavior and contraceptive use, 2006–2019. Contraception: X, 3, 100064. https://doi.org/10.1016/j.conx.2021.100064
Lowry, R., Dunville, R., Robin, L., & Kann, L. (2017). Early sexual debut and associated risk behaviors among sexual minority youth. American Journal of Preventive Medicine, 52(3), 379–384. https://doi.org/10.1016/j.amepre.2016.10.008
Marotta, P. L., Terlikbayeva, A., Gilbert, L., Hunt, T., Mandavia, A., Wu, E., & El-Bassel, N. (2018). Intimate relationships and patterns of drug and sexual risk behaviors among people who inject drugs in Kazakhstan: A latent class analysis. Drug and Alcohol Dependence, 192, 294–302. https://doi.org/10.1016/j.drugalcdep.2018.07.046
McCrimmon, T., Witte, S., Mergenova, G., Terlikbayeva, A., Primbetova, S., Kuskulov, A., Bellamy, S. L., & El-Bassel, N. (2018). Microfinance for women at high risk for HIV in Kazakhstan: Study protocol for a cluster-randomized controlled trial. Trials, 19(1), 187. https://doi.org/10.1186/s13063-018-2566-y
Mergenova, G., El-Bassel, N., McCrimmon, T., Terlikbayeva, A., Primbetova, S., Riedel, M., Kuskulov, A., Velez-Grau, C., & Witte, S. S. (2019). Project Nova: A combination HIV Prevention and Microfinance Intervention for women who engage in sex work and use drugs in Kazakhstan. AIDS and Behavior, 23(1), 1–14. https://doi.org/10.1007/s10461-018-2268-1
Outlaw, A. Y., Phillips, G. I., Hightow-Weidman, L. B., Fields, S. D., Hidalgo, J., Halpern-Felsher, B., & Green-Jones, M. (2011). Age of MSM sexual debut and risk factors: Results from a multisite study of racial/ethnic minority YMSM living with HIV. AIDS Patient Care and STDs, 25(Sup1), S23–S29. https://doi.org/10.1089/apc.2011.9879
Paine, E. A., Lee, Y. G., Vinogradov, V., Zhakupova, G., Hunt, T., Primbetova, S., Terlikbayeva, A., El-Bassel, N., & Wu, E. (2021). HIV stigma, homophobia, sexual and gender minority community connectedness and HIV testing among gay, bisexual, and other men and transgender people who have sex with men in Kazakhstan. AIDS and Behavior, 25(8), 2568–2577. https://doi.org/10.1007/s10461-021-03217-9
Peltzer, K. (2010). Early sexual debut and associated factors among in-school adolescents in eight African countries. Acta Paediatrica, 99(8), 1242–1247. https://doi.org/10.1111/j.1651-2227.2010.01874.x
Peltzer, K., & Pengpid, S. (2015). Early sexual debut and associated factors among in-school adolescents in six Caribbean countries. The West Indian Medical Journal, 64(4), 351–356. https://doi.org/10.7727/wimj.2014.025
Sales, J. M., Swartzendruber, A., & Phillips, A. L. (2016). Trauma-informed HIV prevention and treatment. Current HIV/AIDS Reports, 13, 374–382.
Sawyer, S. M., Azzopardi, P. S., Wickremarathne, D., & Patton, G. C. (2018). The age of adolescence. The Lancet Child & Adolescent Health, 2(3), 223–228. https://doi.org/10.1016/S2352-4642(18)30022-1
Shaw, S. A., Terlikbayeva, A., Famouri, L., Hunt, T., Gilbert, L., Rozental, Y., Primbetova, S., Chang, M., Ma, X., & El-Bassel, N. (2017). HIV testing and access to HIV medical care among people who inject drugs and their intimate partners in Kazakhstan. Journal of Substance Use, 22(1), 53–59. https://doi.org/10.3109/14659891.2016.1143046
Tang, W., Wang, Y., Huang, W., Wu, D., Yang, F., Xu, Y., Ong, J. J., Fu, H., Yang, B., Wang, C., Ma, W., Wei, C., & Tucker, J. D. (2020). Adolescent and non-consensual anal sexual debut among Chinese men who have sex with men: A cross-sectional study. BMC Infectious Diseases, 20(1), 732. https://doi.org/10.1186/s12879-020-05466-w
UNAIDS Data 2020 Report. (2020). 2020 Global AIDS update—Seizing the moment—Tackling entrenched inequalities to end epidemics. Geneva: UNAIDS. Retrieved March 8, 2022, from https://aids2020.unaids.org/report/
United Nations Population Fund. (2018). A summary of the sociological survey on the status of reproductive health of adolescents and young people aged 15–19, their sexual behavior and access to reproductive health services and information. New York, N.Y: UNFPA, United Nations Population Fund. Retrieved March 7, 2022, from https://kazakhstan.unfpa.org/en/publications/summary-sociological-survey-status-reproductive-health-adolescents-and-young-people
United Nations Population Fund Kazakhstan. (n.d.). Child marriage in Kazakhstan (summary). Almaty, Kazakhstan: UNFPA Kazakhstan. Retrieved March 7, 2022 from https://eeca.unfpa.org/sites/default/files/pub-pdf/unfpa%20kazakhstan%20summary.pdf
Wirtz, A. L., Kirey, A., Peryskina, A., Houdart, F., & Beyrer, C. (2013). Uncovering the epidemic of HIV among men who have sex with men in Central Asia. Drug and Alcohol Dependence, 132, S17–S24. https://doi.org/10.1016/j.drugalcdep.2013.06.031
World Health Organization. Regional Office for Europe. (2020). Assessment of sexual, reproductive, maternal, newborn, child and adolescent health in the context of universal health coverage in Kazakhstan. World Health Organization. Regional Office for Europe. Retrieved March 7, 2022, from https://apps.who.int/iris/handle/10665/331173
Wurtele, S., & Kenny, M. (2011). Normative sexuality development in childhood: Implications for developmental guidance and prevention of childhood sexual abuse. Journal of Multicultural Counseling and Development, 43, 1–24.
Xu, R., Dai, W., Zhao, G., Tu, D., Yang, L., Wang, F., Cai, Y., Lan, L., Tan, H., Liu, A., Feng, T., & Kaminga, A. C. (2016). Early sexual debut and HIV infection among men who have sex with men in Shenzhen, China. BioMed Research International, 2016, 1–8. https://doi.org/10.1155/2016/2987472
Zou, H., Xu, J., Hu, Q., Yu, Y., Fu, G., Wang, Z., Lu, L., Zhuang, M., Chen, X., Fu, J., Zhou, Z., Geng, W., Jiang, Y., & Shang, H. (2016). Decreasing age at first anal intercourse among men who have sex with men in China: A multicentre cross-sectional survey. Journal of the International AIDS Society, 19(1), 20792. https://doi.org/10.7448/IAS.19.1.20792
Acknowledgements
In addition to the co-authors, this work was only made possible by the research staff who showed tremendous dedication, skill, and sensitivity—Gassan Akhmedov, Karina Alipova, Farruh Aripov, Dilara Belkesheva, Daniyar Bekishev, Ferangiz Hazanova, Altynay Kambekova, Saltanat Kuskulova, Aitkul Nazarova, Syrim Omirbek, Olga Balabekova, Sultana Kali, Aidar Yelkeyev, Saida Yessenova, Valeria Davydova, and Aizhan Toleuova—and, most importantly, the time and trust given by the participants. The findings and conclusions in this report do not necessarily represent the views of NIDA, Columbia University, or the Global Health Research Center of Central Asia.
Funding
The data for this study were obtained as part of a study funded by the National Institute on Drug Abuse (NIDA; https://www.drugabuse.gov/), grant # R01DA040513. Additionally, Emily Allen Paine’s time was partly supported by a grant from NIMH (K01MH128117).
Author information
Authors and Affiliations
Contributions
CIL conceptualized the study, conducted the data analysis, and drafted the manuscript. EW, YGL, and EAP edited and reviewed the manuscript prior to submission. YGL, GM, VV, and GZ were responsible for the oversite of data collection. SP, AT, and EW collaborated on the design and oversite of the parent study. All authors had full access to the data, reviewed and edited the manuscript, and take responsibility for its integrity as well as the accuracy of the analysis.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The original trial was approved by both the institutional review board of Columbia University and The Local Ethical Committee et al.-Farabi Kazakh National University. Verbal informed consent was obtained from all participants; a waiver of written documentation of consent was obtained from the IRB because the research presented no more than minimal risk of harm to subjects. All procedures performed in studies involving human participants were in accordance with the ethical standards of the intuitional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors. The current data analysis for this manuscript was performed on completely de-identified data.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Laughney, C.I., Lee, Y.G., Mergenova, G. et al. Earlier Sexual Debut as a Risk Factor for Substance Use Among Men Who Have Sex with Men (MSM) in Kazakhstan. Glob Soc Welf 11, 225–232 (2024). https://doi.org/10.1007/s40609-023-00298-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40609-023-00298-3