Abstract
Human populations are exposed to a wide spectrum of environmental contaminants, some of which are considered reproductive toxins. The influence of such toxins on the male reproductive system has been investigated extensively in animal models, while epidemiological studies seek to understand the effect of human exposures. The basic tenant of epidemiological studies in male human reproduction is to infer how one or more substances alter the hormonal profile, seminal characteristics, or both. Determining if a substance alters semen quality may not always provide the underlying mechanism. The mechanisms by which toxins may alter human sperm and semen quality are typically examined as a function of hormonal changes and cellular damage. The possibility that more subtle epigenetic alterations underlie some of the reproductive changes has, until recently, received little attention. In this review, we discuss the roles of epigenetics in human spermatogenesis, while considering the impact of reproductive toxicants on the epigenome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The ubiquitous nature of industrial activities in developing and developed countries results in a continuous exposure to environmental contaminants. Constant exposure to environmental contaminants poses a potential risk to health. For example, these can include carcinogens, drugs, food additives, hydrocarbons, and pesticides. The long-term health effects of constant low-level exposure to contaminants, from both individual substances and mixtures, are often unknown. This is highlighted by the risk of such exposure to reproductive outcomes. Given the worldwide decline in sperm count [1] paralleling the increasing use of infertility services, such as assisted reproductive technologies (ARTs), detailed exploration of exposures to natural compounds (nutrition) and xenobiotics (environmental contaminants) on the human germline is necessary to understand how it may impact future generations.
The Human Male Reproductive System
The male reproductive system is a complex symphony of cell types orchestrated by Sertoli cells (SCs), Leydig cells (LCs), germ cells, and epididymal cells. Each is a critical member of spermatogenesis and essential to male fertility. The hypothalamic-pituitary-gonadal axis modulates the production of testosterone and spermatogenesis (reviewed in [2]), directly interacting with the male reproductive tract. As shown in Fig. 1a, this is comprised of testis, epididymis, and vas deferens, as well as a variety of accessory sex glands. Blood vessels permeate the interstitial space, providing oxygen and nutrients to the surrounding tissue. Leydig cells surrounding the blood vessels generate testosterone and other steroids necessary for the formation of a healthy male gamete through spermatogenesis. This process of differentiation guides the development of the male gamete, from stem cell to mature sperm, within seminiferous tubule. The SCs lining the tubule lend a degree of immune privilege by creating a blood-testis barrier (BTB) and preventing the immune system from viewing the germ cells as nonself, against which an immune response would be mounted. The SCs also serve to nourish the developing sperm, with progressive cell-cell interactions between the SC and developing sperm moving the maturing sperm from the basal to apical surface of the SC toward the lumen of the seminiferous tubule.
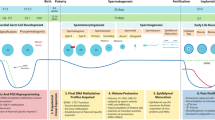
The human male reproductive system and epigenetic aspects of spermatozoa. a Structure and location of the human testis, epididymis, and vas deferens. Spermatogenesis occurs in the testis, with the resultant spermatozoa transited into the epididymis. The sperm undergo a maturation process while moving through the epididymis. Caudal sperm are moved into the vas deferens for collection prior to ejaculation. The process of sperm development in the testis occurs over approximately 69–80 days, while the movement of spermatozoa through the epididymis averages around 8 days. In total, a complete seminiferous cycle is completed in around 90 days. b A detailed cross section of the seminiferous tubule, the location of which is indicated with a red box in Fig. 1a. The intersistal space contains blood vessels and Leydig cells, while the seminiferous tubule is lined with Sertoli cells. Spermatogenic stem cells, located in the basement membrane of the tubule, are moved toward the apical surface of the Sertoli cell as spermatogenesis progresses. The blood-testis barrier is formed behind pachytene spermatocytes to protect the developing spermatocyte from the immune system. Adapted in part from [4•]
Human spermatogenesis occurs over a cycle of approximately 90 days, with 69–80 days of development within the seminiferous tubule and 8 days in the epididymis prior to ejaculation, as illustrated in Fig. 1a [3]. Spermatogenesis begins with the replication of type A (dark) (abbreviated Adark) spermatogonial stem cells (SSCs), which serve as a germ cell reservoir. Following asymmetric division, the undifferentiated Adark spermatogonia are located in the basal compartment of the seminiferous tubules, flanked by Sertoli cells. Upon commitment, Adark spermatogonia differentiate to type A (pale) (abbreviated Apale) spermatogonia. Apale spermatogonia replicate to form two type B spermatogonia, considered to be differentiated spermatogonia, which are translocated closer to the apical surface of the Sertoli cell. Type B spermatogonia differentiate into primary spermatocytes, which are then secured behind the blood-testes barrier established by Sertoli cell junctions [4•]. Primary spermatocytes undergo reductive divisions yielding haploid round spermatids, located near the apical surface of the seminiferous tubule. In turn, the round spermatid then undergoes a marked morphological transformation as the histone-packaged genome is primarily replaced by autosomal male-specific protamine proteins. As the round spermatid elongates, a residual body forms and the majority of the cytoplasm is shed as a cytoplasmic droplet, yielding a final head area of approximately 24 μm2 [5].
Sperm: More than Just a Genome
Sperm have been perceived as little more than a vessel that delivers the paternal genome to the oocyte. However, intense scrutiny over the past decades has revealed mature sperm to have a complex organization, marked by a highly specialized epigenome that is vastly different from that of a somatic cell. Where the somatic cell genome is organized by nucleosomes, comprised primarily of histone complexes, the sperm genome is primarily organized by protamines. Only a small fraction, approximately 15 %, of the DNA remains associated with histones in human sperm [6]. During spermatid maturation, specialized transition proteins, e.g., TNP1 and TNP2, act to displace histones. Protamines then associate with the freed chromatin, ultimately rendering protamine-bound DNA to be approximately 10 times more compact than histone-bound DNA. The mechanism by which histone-bound regions are designated to be maintained or replaced by protamines is yet unknown but in part may be decided by the underlying pattern of DNA methylation [7]. Using genome-wide strategies, regions of histone retention in mature sperm have been shown to be enriched at loci associated with embryonic development and repetitive elements, such as centromere repeats and retrotransposons [8–11].
Effect of Exposures on Sperm Parameters and Fertility
In mammalian systems, both in utero and post-natal environmental exposures can alter fertility through a variety of mechanisms. Tables 1 and 2 detail examples of work demonstrating that exposures to endocrine disruptors and other toxicants can act on many different cell types in the reproductive system or exhibit particular affinity for a select cell type. The cells that underlie human spermatogenesis originate in the first trimester of fetal life. Interruptions or changes to this process may lead to testicular dysfunction and infertility in the adult [12–15]. The establishment of the SSCs and Sertoli cells in utero [14–16], followed by their subsequent application in pubertal development and spermatogenesis, provides the opportunity for in utero exposure to impact adult reproductive health, reviewed in [17].
Leydig Cells
LCs serve as steroidogenesis factories, utilizing lipids to synthesize hormones, with testosterone production being critical for spermatogenesis and sexual health. As such, toxicity to LC populations can have a deleterious effect on spermatogenesis and seminal parameters. The importance of LC to spermatogenesis in vivo has been investigated through chemical ablation. The administration of ethane dimethanesulfonate (EDS) is an established method that specifically eliminates LCs [18], possibly through upregulation of glutathione synthesis in the LC [19]. Although LC populations eventually recover with time [20], their initial death is accompanied by a reduction in testosterone production [21, 22]. This androgen withdrawal results in apoptosis of the seminiferous epithelium [21], possibly through increased expression of the Fas ligand in germ cells [22]. Although LCs provide critical steroids to the testis, the presence of the LC itself, outside of testosterone production, may be dispensible in spermatogenic processes [22, 23].
Sertoli Cells
The SC is a complex cell responsible for maintaining the BTB and supporting germ cells during spermatogenesis. Factors involved in the differentiation and homeostasis of Sertoli cells, both in the fetus and adult, have been extensively scrutinized (reviewed in [24]). The importance of SCs to testicular health and germ cell differentiation has been examined in several different studies. Targeted ablation of SCs by diphtheria toxin in transgenic mice rapidly depletes all germ cell populations in the seminiferous tubule [25]. Disruption of Sertoli cell structure by toxins is well-documented and can result in decreased sperm parameters. Exposure of mice to perfluorooctane sulfonate (PFOS), considered a persistant organic pollutant (POP), decreases sperm count. Concomitantly, SC vacuolization, increased BTB permeability, and a reduction in junction proteins are also observed [26]. In cultured primary human SCs, acute cadmium (a toxic metal) and bisphenol A (BPA) exposure disrupts F-actin network dynamics and the localization of cell adhesion proteins [27].
Phthalates, esters of phthalic acid, are considered endocrine disruptors and ubiquitous environmental contaminants. It is well known that SCs are a major target of phthalates [28]. In addition to numerous studies on in utero phthalate exposure, the reproductive sequelae of prepubertal, pubertal, and adult phthalate exposure is a subject of active research [29–33]. Due to the marked response of rodent models to a plethora of phthalate compounds, rats and mice are typically employed to assess the reproductive impact of phthalate exposure [34, 35••]. Prenatal epidemiological exposure studies of di(2-ethylhexyl) phthalate (DEHP) in children suggest a negative correlation with progesterone (P4) and INSL3, products of LCs and inhibin B, a product of SCs [36]. However, physiological changes in phthalate-exposed SCs have not been demonstrated in vivo for humans. This is similar to that observed at high dose (2500 mg/kg bodyweight) DEHP post-natal exposure of marmosets [37]. Both human and primate (marmoset) studies have thus far failed to recapitulate the testicular damage seen in rodent models.
Spermatogenic Stem Cells
The SSC is the precursor to all spermatids. Therefore, damage to SSCs or loss of the population of SSC (Adark) spermatogonia can drastically impact sperm production, even to the point of azoospermia (absence of sperm in the ejaculate). SSCs rely on Sertoli cells for maintenance of the stem cell niche, as well as the signals for commitment to spermatogenesis. It is important to note that Sertoli cell health is equally vital for maintaining SSC populations as SSC health.
In rodent models and human disease, elimination of SSCs results in oligozoospermia (low sperm concentration) or azoospermia (absence of sperm in ejaculate). In humans, this is classified as Sertoli cell only syndrome (SCOS), also known as germ cell aplasia, and is characterized by the absence of germ cells in the seminiferous tubule. Due to their stem cell properties and high rate of division, SSCs are particularly vulnerable to cytotoxic insult. Radiation and agents used in cancer therapies are known to be gonadotoxic, affecting SSCs. For example, busulphan, a chemotherapeutic, can induce azoospermia in rodents and primates by ablating the population of SSCs [38, 39]. Patients receiving potent gonadotoxic chemotherapy, such as cyclophosphamide, an alkylating agent, are often counseled to undergo fertility preservation prior to treatment [40]. During chemotherapy, the suppression of spermatogenesis through hormonal therapy reduces SSC expansion and may reduce SSC damage, although the success of this approach in human trials has been mixed [41, 42].
Other, more ubiquitious toxins can also be detrimental to SSCs. For example, tobacco use is suspected to impact SSC proliferation. Despite a small sample size, maternal cigarette smoking has been significantly associated with a reduction in germ cells in first-trimester human embryonic gonads [43]. In utero exposure through maternal smoking has also been shown in rodents to deplete SSCs [44]. Post-natal exposure to cigarette smoke, at least in rats, also negatively affects SSC proliferation, an effect which may be mediated by antagonism of the aryl hydrocarbon receptor (AHR) [45, 46].
Spermatocytes
Spermatocytes are established within an intermediate transitioning stage of sperm development, during which a series of reductive divisions occurs. Depletion of spermatocytes, through immune attack, Sertoli cell dysfunction, DNA damage, or other insults, can result in the loss of a generation of sperm. 2-Methoxyethanol (ME), a solvent used as a de-icing agent, is known to primarily target pachetyne spermatocytes in mammals. In rodents and guinea pigs, ME administration is toxic to spermatocytes, resulting in the degeneration of the germ cells [47]. Acrylamide, formed by cooking starchy foods at high temperatures, can also impact spermatocytes through the formation of glycidamide-DNA adducts [48]. Chronic murine exposure to low-dose acrylamide similar to human dietary estimates (1 μg/kg bodyweight/day) over the course of 12 months produced germ cell DNA damage [49•]. Both the epididymis and germ cells express Cyp2e1, the enzyme that metabolizes acrylamide to the DNA adduct-forming glycidamide, making them a major target of acrylamide exposure [50, 51].
Spermatids
After spermatogenesis is complete, the maturing spermatids move from the seminiferous tubule into the epididymis, where they spend approximately 8 days completing maturation prior to entering the vas deferens in preparation for ejaculation [3]. As sperm mature during this transit, protamine compaction through the action of thiol peroxidases continues, proteins are glycosylated, and the spermatozoa are exposed to epididymal exosomes (epididymosomes), reviewed in [52•] and [53]. The period prior to and during compaction is primarily when the effects of environmental exposures may be felt and when biochemical processes gone awry take their toll. For example, dysregulation of the epididymis and/or the blood-epididymis barrier (BEB) that tightly regulates epididymal immune system activity [54], may result in a continual reduction in living sperm or sperm quality, potentially resulting in oligozoospermia, azoospermia, or necrospermia (immobile or dead sperm in ejaculate). Sperm autoimmunity, in which the male’s immune system generates anti-sperm antibodies, which are subsequently found in seminal fluid, can alter fertilization capacity. This is reflected in sperm motility as assessed by post-coital testing. It is inversely correlated with sperm antibodies, predictive of male autoimmunity [55].
As with SSCs, spermatids may also be sensitive to cigarette smoking [56, 57]. Alterations in epididymal proteins responsive to oxidative stress, endoplasmic stress, and glutathione production have been observed [57]. It is important to note that the excessive generation of reactive oxidative species (ROS) and the oxidative imbalance in the epididymis may be a pathophysiological mechanism of many different toxins and etiologies of disease. For example, testicular heat stress, such as is seen in patients with variocele and various murine models, can generate ROS, resulting in altered balance of ROS and antioxidant systems [58–60].
Characteristics of the Mammalian Sperm Epigenome
The epigenome of mammalian sperm is suspected to play a key role in the mechanism by which environmental exposures can alter fertility and produce intergenerational effects. A summary is briefly presented considering the contribution of DNA methylation, chromatin structure, and RNAs. Some of the primary contributions to our understanding in the field are highlighted below.
DNA Methylation
DNA methylation is catalyzed by methyltransferases that add a methyl group to DNA. In the case of cytosine methylation, the addition occurs on the 5′ carbon of the nucleotide base. Although DNA methylation can occur in the context of 5-hydroxymethylcytosine, 5-formylcytosine, and 5-carboxycytosine, the most commonly studied form is 5-methylcytosine [61]. 5-Methylcytosine has been studied extensively as general regulator of gene expression within the context of CpG methylation. The level of DNA methylation in the sperm genome, compared to somatic cells, is both altered and complex. Large-scale genomic sequencing has shown that mammalian sperm are primarily hypermethylated compared to other cell types [62, 63], a pattern which extends to zebrafish [64]. While the sperm genome is hypermethylated, as is seen in some classes of repeats [65, 66], hypomethylation occurs in developmental promoters [8], satellite repeats, and SVA retrotransposons [63]. Upon fertilization, the uniquely compacted sperm decondenses, essentially exploding as the paternal protamines are displaced and replaced by maternal histones [67]. Concomitantly, the paternal genome is actively and rapidly demethylated only to be followed by remethylation after the blastocyst stage. Even though the majority of the original paternal DNA methylation marks are removed [68], the knowledge of their parental origin is maintained in early embryogenesis as evidenced by the preservation of imprinted loci.
DNA methylation is not a static feature of the mammalian sperm genome. It can be modified in response to weight loss [69], exercise training [70], and environmental exposures, including exposure to BPA [71]. Males exposed to BPA present sperm with reduced LINE-1 (a repeat family) methylation [71]. Although epidemiological studies in humans have yet to provide a definitive link between the sperm methylome and offspring phenotype, rodent models have provided some clues. Locus-specific patterns of altered sperm methylation have been associated with metabolic alterations in the offspring after in utero undernourishment in mouse [72].
DNA Methylation and Fertility
The prognostic value of DNA methylation in infertility studies has yet to be shown. This is complicated by its variability between sperm with differing “quality” (i.e., high-quality vs low-quality sperm) [73]. However, Aston et al. suggest that a genome-wide analysis of sperm methylation can distinguish sperm of fertile and infertile individuals [74•]. Currently, it appears that DNA methylation changes are a consequence, not a cause, of poor spermatogenesis and spermatid aberrations.
Chromatin Structure and Fertility
As described above, the chromatin structure of sperm is vastly different from that of a somatic cell. The histone-protamine exchange that occurs during spermatogenesis is a key differentiative control point as the spermatid transitions to the mature spermatozoon. A protamine-bound genome is much more tightly packaged than its histone counterpart. This can serve to protect the paternal genome during epididymal transit and transition through the female reproductive tract. Protamine deficiency is associated with an increased incidence of abnormal sperm morphology [75, 76], and an aberrant protamine/histone ratio is associated with increased DNA damage in humans and in animal models [77, 78]. The latter can be assessed using the comet assay [79], sperm chromatin dispersion (SCD), DNA breakage detection-fluorescence in situ hybridization (DBD-FISH), or the TUNEL assay.
RNAs
The mammalian testis yields a complex transcriptome [80], which is echoed in the transcriptionally and essentially translationally silent sperm [81, 82•]. This reflects several different mechanisms that impair both transcription and translation. Notably, ribosomal RNA is largely fragmented, eliminating translation in the mature sperm [83]. Although the majority of spermatid RNAs are expunged as the residual body is shed during elongation, the mature sperm still contains a variety of RNA species. The transcripts that remain provide a record of past events during spematogenesis, before and after the last burst of transcription. The fate and purpose of the sperm RNAs in the zygote are unclear in humans [84], but in mouse models, functional transcripts can be transferred to and transcribed (or utilized) by the fertilized oocyte [85, 86••]. Whether spermatozoal RNAs are required for embryogenesis and/or implantation is still debated [87, 88].
Mature spermatozoa harbor a series of long RNAs, as well as a variety of small RNAs. The long RNAs consist of both coding and noncoding RNAs, in various states of fragmentation. It has been proposed that intact transcripts may represent those necessary for the final stages of spermatid elongation or intended for use in the zygote. Recently, they have been shown to serve as predictors of successful pregnancies in couples undergoing ART for idiopathic infertility (no known cause) [89•]. Small RNA species, which include transfer RNAs (tRNAs), microRNAs (miRNAs), and piwi-interacting RNAs (piRNAs), are generally referred to as small noncoding RNAs (sncRNAs) [90]. One of the best understood species of small RNAs is miRNAs, which function as regulatory RNAs through the DICER/DROSHA processing pathway. Subsequent base pairing with their target RNA leads to the degradation of the messenger RNA (mRNA) [91]. This is complemented by the action of piRNAs that can regulate retrotransposons [92], alter spermatid mRNA abundance [93], or may serve as part of assessing genome compatibility by consolidation/confrontation [84].
Transgenerational and Intergenerational Effects
The mammalian sperm epigenome is a putative mediator of intergenerational and transgenerational transmission of paternal environmental exposures. On one hand, intergenerational transmission is due to exposure of the germ cells to the agent, while on the other hand, transgenerational transmission propagates to future generations in the absence of continued exposure [Fig. 1, ref. 94••]. To some extent, these may be mediated through sperm RNAs. For example, the role of early life stress on sncRNAs in murine sperm has been examined, suggesting that seemingly unrelated cues can be transferred. Mice subjected to early life traumatic stress exhibited changes in the abundance of several spermatazoal miRNAs and piRNAs, in conjunction with behavioral and metabolic changes compared to an unstressed control. Progeny generated from injection of sperm RNA from the stressed fathers into embryos, compared to unstressed controls, exhibited similar behavior and metabolic patterns as the stressed fathers. This supports the notion that at least in mice, spermataozoal RNA populations can transmit the results of an early life stress to their progeny [95].
Paternal characteristics, such as obesity, may also influence offspring phenotype through sperm RNAs, as observed in a murine obesity model, which identified a range of differentially methylated miRNAs in sperm [96]. Interestingly, reductions in male obesity in humans have been shown to alter specific sperm RNAs [69], raising the possibility of intergenerational transmission of human obesity.
Exosomes/Exosomal RNA
While a portion of sperm RNAs are undoubtedly derived as the result of spermatogenesis, the transmission of paternal experiences, such as a neural signal, to sperm may come from a different source [97]. To address this possibility, soma-to-germline transmission of RNA in male mice was examined [98••]. In this study, an enhanced green fluorescent protein (EGFP)-expressing human melanoma cell line, xenografted into nude mice, was shown to release exosomes containing EGFP RNA into the blood. Sperm from the xenografted mice was subsequently shown to contain EGFP RNA, indicating that the germ cell can absorb exosomes and their contents [98••].
Sperm RNAs derived from extracellular sources may be acquired during epididymal maturation [86••, 99]. Compared to a control diet, mice fed a low-protein diet fathered offspring with altered hepatic metabolism. This was associated with a series of differentially abundant small sperm RNAs, specifically tRNA fragments and let-7 miRNAs. These RNAs, acquired by sperm from epididymal exosomes (epididysomes) during epididymal maturation, were capable of modulating zygotic expression of the genomic targets for the small RNAs [86••]. These results suggested that the sperm RNAs can be acquired from the epididymis and may be responsible for the offspring’s phenotype. In a complementary murine study, intergenerational transmission of a father’s high-fat diet through sperm RNA, specifically, transfer RNA-derived small RNAs, has been shown [100].
DNA Methylation/Epimutations
The evidence for diet-induced changes in sperm DNA methylation is contradictory, with both negative [101] and supportive studies [96]. Interestingly, paternal dietary folate does alter the sperm epigenome. The mechanism by which folate availability impacts the offspring’s susceptibility to birth defects may be through changes in histone methylation [102]. Perhaps this reflects a portion of the paternal histones that remain after fertilization. The apparent significance of the contribution of histones as compared to DNA methylation and paternal diet has been emphasized. It has been noted that the sperm histone composition in fathers fed a high-fat diet changes, although DNA methylation of several imprinted loci appears to remain static [103]. The suspected role of histone modifications may be well founded. In humans, the establishment of embryo constitutive heterochromatin may be directed by the placement of histone modifications in sperm [104].
Evidence of Toxins/Substances Which Alter the Sperm Epigenome
Each component of the sperm epigenome, presented above, has the potential to be modulated by intrinsic and extrinsic factors. Examples of epigenetic outcomes in the male reproductive system as a function of toxins and/or environmental exposures are summarized in Tables 1 and 2. The intergenerational studies described above have provided a basis to begin to understand the possible transgenerational effects of male environmental exposures. For example, several studies have shown striking intergenerational effects following murine in utero exposure to the fungicide vinclozolin. In a series of studies, fetal mice were exposed to vinclozolin during embryonic days 8–14, a period of gonadal sex determination. This transient exposure resulted in altered sperm and Sertoli cell DNA methylation of the F2 (grandchildren) of the exposed fetuses, indicating a transgenerational effect [105, 106]. In addition to the intergenerational effect, with an F1 (children of fathers exposed in utero) phenotype, a transgenerational inheritance is observed, with the F2 generation (grandchildren of fathers exposed in utero). Although the germ cells which become the F1 generation are exposed to the environmental insult during the in utero development of the F0 males, it is important to note that the gametes destined to become the F2 generation are never themselves exposed. Therefore, in transgenerational inheritance, a phenotype resulting from an exposure must be propagated through an epigenetic mechanism.
Another endocrine disruptor, DEHP, has also been shown to have multigenerational effects. F0 male mice, exposed to DEHP (500 mg/kg body weight/day) during embryonic days 7–14, exhibit a variety of reproductive phenotypes (e.g., delayed pubertal onset and decreased anogenital distance). Although the F1 and F2 progeny of exposed mice were largely normal, their seminiferous tubules were structurally altered and sperm counts reduced, which were attributed to reduced SSC proliferation in the exposed lines [107]. The primary animal models used to study paternal endocrine disruptor exposure epigenetic effects have employed in utero exposure. Comparatively, few studies have investigated the transgenerational or intergenerational effects of post-natal or adult exposure in animal models. However, one study using high DEHP exposure in weaned mice observed reduced sperm motility in the offspring of exposed males, indicating an intergenerational effect on reproductive tissues after post-natal exposure [108]. This collection of studies suggests that environmental exposure to endocrine disruptors can have robust intergenerational and transgenerational effects in mice. However, conclusive studies using exposure levels relevant to the human populations, as well as exposures at the various stages of germ cell development, as outlined in Fig. 1 of reference [17], are needed.
Conclusion
The above provides an inroad to the possible mechanisms by which environmental exposure, including reproductive toxicants, can impact seminal parameters and male fertility. Given that certain stimuli, such as obesity, endocrine disruptors, and other environmental agents, are becoming increasingly common, the mechanisms and physiological consequences of such exposures will continue to be discovered. Their mechanisms of action are likely to be mediated through the sperm epigenome, which is suspected to play a role in intergenerational inheritance of paternal environmental exposure. Within these bounds, the intergenerational sequelae stemming from toxin exposures will be resolved. Although much important work has been carried out in rodents, reliance on this physiological system currently constrains the inroads to the human male reproductive system. It is essential that we achieve a better understanding of the father’s contribution in producing healthy offspring.
Abbreviations
- BTB:
-
Blood-testis barrier
- BEB:
-
Blood-epididymis barrier
- LC:
-
Leydig cell
- SC:
-
Sertoli cell
- SSC:
-
Spermatogenic stem cell
- sncRNA:
-
Small noncoding RNAs
- BPA:
-
Bisphenol A
- DEHP:
-
Di(2-ethylhexyl) phthalate
- DBP:
-
Di-n-butyl phthalate
- e.d.:
-
Embryonic day
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Rolland M, Le Moal J, Wagner V, et al. Decline in semen concentration and morphology in a sample of 26 609 men close to general population between 1989 and 2005 in France. Human Reproduction (Oxford, England). 2013;28(2):462–70. doi:10.1093/humrep/des415.
Jin J-M, Yang W-X. Molecular regulation of hypothalamus–pituitary–gonads axis in males. Gene. 2014;551(1):15–25. doi:10.1016/j.gene.2014.08.048.
Amann RP. The cycle of the seminiferous epithelium in humans: a need to revisit? J Androl. 2008;29(5):469–87. doi:10.2164/jandrol.107.004655.
Hai Y, Hou J, Liu Y, et al. The roles and regulation of Sertoli cells in fate determinations of spermatogonial stem cells and spermatogenesis. Semin Cell Dev Biol. 2014;29:66–75. doi:10.1016/j.semcdb.2014.04.007 .A comprehensive review of the importance of SCs in reproductive health
Aziz N, Fear S, Taylor C, et al. Human sperm head morphometric distribution and its influence on human fertility. Fertil Steril. 1998;70(5):883–91. doi:10.1016/S0015-0282(98)00317-3.
Balhorn R. The protamine family of sperm nuclear proteins. Genome Biol. 2007;8(9):227. doi:10.1186/gb-2007-8-9-227.
Brunner AM, Nanni P, Mansuy IM. Epigenetic marking of sperm by post-translational modification of histones and protamines. Epigenetics & Chromatin. 2014;7:2. doi:10.1186/1756-8935-7-2.
Hammoud SS, Nix DA, Zhang H, et al. Distinctive chromatin in human sperm packages genes for embryo development. Nature. 2009;460(7254):473–8 .http://www.nature.com/nature/journal/v460/n7254/suppinfo/nature08162_S1.html.
Carone BR, Hung J-H, Hainer SJ, et al. High resolution mapping of chromatin packaging in mouse ES cells and sperm. Dev Cell. 2014;30(1):11–22. doi:10.1016/j.devcel.2014.05.024.
Samans B, Yang Y, Krebs S, et al. Uniformity of nucleosome preservation pattern in mammalian sperm and its connection to repetitive DNA elements. Dev Cell. 2014;30(1):23–35. doi:10.1016/j.devcel.2014.05.023.
Johnson GD, Jodar M, Pique-Regi R et al. Nuclease footprints in sperm project past and future chromatin regulatory events. Sci Rep. 2016;6:25864. doi:10.1038/srep25864.
Wakeling SI, Miles DC, Western PS. Identifying disruptors of male germ cell development by small molecule screening in ex vivo gonad cultures. BMC Research Notes. 2013;6:168. doi:10.1186/1756-0500-6-168.
Juul A, Almstrup K, Andersson A-M, et al. Possible fetal determinants of male infertility. Nat Rev Endocrinol. 2014;10(9):553–62. doi:10.1038/nrendo.2014.97.
Pitetti J-L, Calvel P, Zimmermann C, et al. An essential role for insulin and IGF1 receptors in regulating Sertoli cell proliferation, testis size, and FSH action in mice. Mol Endocrinol. 2013;27(5):814–27. doi:10.1210/me.2012-1258.
Jørgensen A, Nielsen JE, Perlman S, et al. Ex vivo culture of human fetal gonads: manipulation of meiosis signalling by retinoic acid treatment disrupts testis development. Hum Reprod. 2015;30(10):2351–63. doi:10.1093/humrep/dev194.
Altman E, Yango P, Moustafa R, et al. Characterization of human spermatogonial stem cell markers in fetal, pediatric, and adult testicular tissues. Reproduction (Cambridge, England). 2014;148(4):417–27. doi:10.1530/REP-14-0123.
Wu H, Hauser R, Krawetz SA, et al. Environmental susceptibility of the sperm epigenome during windows of male germ cell development. Current environmental health reports. 2015;2(4):356–66. doi:10.1007/s40572-015-0067-7.
Morris AJ, Taylor MF, Morris ID. Leydig cell apoptosis in response to ethane Dimethanesulphonate after both in vivo and in vitro treatment. J Androl. 1997;18(3):274–80. doi:10.1002/j.1939-4640.1997.tb01919.x.
Kelce WR, Zirkin BR. Mechanism by which ethane dimethanesulfonate kills adult rat leydig cells: involvement of intracellular glutathione. Toxicol Appl Pharmacol. 1993;120(1):80–8. doi:10.1006/taap.1993.1089.
Guo J, Zhou H, Su Z, et al. Comparison of cell types in the rat leydig cell lineage after ethane dimethanesulfonate treatment. Reproduction. 2013;145(4):371–80. doi:10.1530/rep-12-0465.
Woolveridge I, de Boer-Brouwer M, Taylor MF, et al. Apoptosis in the rat spermatogenic epithelium following androgen withdrawal: changes in apoptosis-related genes. Biol Reprod. 1999;60(2):461–70. doi:10.1095/biolreprod60.2.461.
Nandi S, Banerjee PP, Zirkin BR. Germ cell apoptosis in the testes of Sprague Dawley rats following testosterone withdrawal by ethane 1,2-dimethanesulfonate administration: relationship to Fas? Biol Reprod. 1999;61(1):70–5. doi:10.1095/biolreprod61.1.70.
Sharpe RM, Maddocks S, Kerr JB. Cell-cell interactions in the control of spermatogenesis as studied using leydig cell destruction and testosterone replacement. Am J Anat. 1990;188(1):3–20. doi:10.1002/aja.1001880103.
Tarulli GA, Stanton PG, Meachem SJ. Is the adult Sertoli cell terminally differentiated? Biol Reprod. 2012;87(1):13 . doi:10.1095/biolreprod.111.095091.1-1
Rebourcet D, O’Shaughnessy PJ, Monteiro A, et al. Sertoli cells maintain leydig cell number and peritubular Myoid cell activity in the adult mouse testis. PLoS One. 2014;9(8):e105687. doi:10.1371/journal.pone.0105687.
Qiu L, Zhang X, Zhang X, et al. Sertoli cell is a potential target for perfluorooctane sulfonate–induced reproductive dysfunction in male mice. Toxicol Sci. 2013;135(1):229–40. doi:10.1093/toxsci/kft129.
Xiao X, Mruk DD, Tang EI, et al. Environmental toxicants perturb human Sertoli cell adhesive function via changes in F-actin organization mediated by actin regulatory proteins. Hum Reprod. 2014;29(6):1279–91. doi:10.1093/humrep/deu011.
Mazaud-Guittot S. Dissecting the phthalate-induced Sertoli cell injury: the fragile balance of proteases and their inhibitors. Biol Reprod. 2011;85(6):1091–3. doi:10.1095/biolreprod.111.095976.
Desdoits-Lethimonier C, Albert O, Le Bizec B, et al. Human testis steroidogenesis is inhibited by phthalates. Hum Reprod. 2012;27(5):1451–9. doi:10.1093/humrep/des069.
Hauser R, Meeker JD, Singh NP, et al. DNA damage in human sperm is related to urinary levels of phthalate monoester and oxidative metabolites. Hum Reprod. 2007;22(3):688–95. doi:10.1093/humrep/del428.
Duty SM, Silva MJ, Barr DB, et al. Phthalate exposure and human semen parameters. Epidemiology. 2003;14(3):269–77. doi:10.1097/01.ede.0000059950.11836.16.
Zhang Y, Cao Y, Shi H, et al. Could exposure to phthalates speed up or delay pubertal onset and development? A 1.5-year follow-up of a school-based population. Environ Int. 2015;83:41–9. doi:10.1016/j.envint.2015.06.005.
Liu C, Qian P, Yang L et al. Pubertal exposure to di-(2-ethylhexyl)-phthalate inhibits G9a-mediated histone methylation during spermatogenesis in mice. Archives of Toxicology. 2015:1–15. doi:10.1007/s00204–015–1529-2.
Habert R, Muczynski V, Grisin T, et al. Concerns about the widespread use of rodent models for human risk assessments of endocrine disruptors. Reproduction (Cambridge, England). 2014;147(4):R119–R29. doi:10.1530/REP-13-0497.
Johnson KJ, Heger NE, Boekelheide K. Of mice and men (and rats): phthalate-induced fetal testis endocrine disruption is species-dependent. Toxicol Sci. 2012;129(2):235–48. doi:10.1093/toxsci/kfs206 .An overview of the use of rodent models in assessing phthalate-induced testicular dysgenesis syndrome
Araki A, Mitsui T, Miyashita C, et al. Association between maternal exposure to di(2-ethylhexyl) phthalate and reproductive hormone levels in fetal blood: the Hokkaido study on environment and children's health. PLoS One. 2014;9(10):e109039. doi:10.1371/journal.pone.0109039.
Tomonari Y, Kurata Y, David RM, et al. Effect of di(2-ethylhexyl) phthalate (DEHP) on genital organs from juvenile common marmosets: I. Morphological and biochemical investigation in 65-week toxicity study. J Toxic Environ Health A. 2006;69(17):1651–72. doi:10.1080/15287390600630054.
Levi M, Hasky N, Stemmer SM, et al. Anti-Müllerian hormone is a marker for chemotherapy-induced testicular toxicity. Endocrinology. 2015;156(10):3818–27. doi:10.1210/en.2015-1310.
Hermann BP, Sukhwani M, Lin C-C, et al. Characterization, cryopreservation and ablation of spermatogonial stem cells in adult rhesus macaques. Stem cells (Dayton, Ohio). 2007;25(9):2330–8. doi:10.1634/stemcells.2007-0143.
Gajjar R, Miller SD, Meyers KE, et al. Fertility preservation in patients receiving cyclophosphamide therapy for renal disease. Pediatr Nephrol. 2014;30(7):1099–106. doi:10.1007/s00467-014-2897-1.
Kangasniemi M, Wilson G, Huhtaniemi I, et al. Protection against procarbazine-induced testicular damage by GnRH-agonist and antiandrogen treatment in the rat. Endocrinology. 1995;136(8):3677–80. doi:10.1210/endo.136.8.7628410.
Kreuser ED, D. K, E. T. The role of LHRH-analogues in protecting gonadal functions during chemotherapy and irradiation. Eur Urol. 1993;23(1):157–63 .discussion 63-4
Mamsen LS, Lutterodt MC, Andersen EW, et al. Cigarette smoking during early pregnancy reduces the number of embryonic germ and somatic cells. Hum Reprod. 2010;25(11):2755–61. doi:10.1093/humrep/deq215.
Sobinoff AP, Sutherland JM, Beckett EL, et al. Damaging legacy: maternal cigarette smoking has long-term consequences for male offspring fertility. Hum Reprod. 2014;29(12):2719–35. doi:10.1093/humrep/deu235.
Audi SSSS. Effect of cigarette smoke on body weight, food intake and reproductive organs in adult albino rats. Indian J Exp Biol. 44(7):562–5.
Esakky P, Hansen DA, Drury AM, et al. Cigarette smoke condensate induces aryl hydrocarbon receptor-dependent changes in gene expression in spermatocytes. Reprod Toxicol. 2012;34(4):665–76. doi:10.1016/j.reprotox.2012.10.005.
Ku WW, Wine RN, Chae BY, et al. Spermatocyte toxicity of 2-methoxyethanol (ME) in rats and Guinea pigs: evidence for the induction of apoptosis. Toxicol Appl Pharmacol. 1995;134(1):100–10. doi:10.1006/taap.1995.1173.
Sams C, Jones K, Warren N, et al. Towards a biological monitoring guidance value for acrylamide. Toxicol Lett. 2015;237(1):30–7. doi:10.1016/j.toxlet.2015.05.018.
Nixon BJ, Stanger SJ, Nixon B, et al. Chronic exposure to acrylamide induces DNA damage in male germ cells of mice. Toxicol Sci. 2012;129(1):135–45. doi:10.1093/toxsci/kfs178 .This study demonstrates that chronic exposure at physiologically relevant doses of acrylamide , a potential human carcinogen , can alter sperm DNA integrity in mice
Nixon BJ, Katen AL, Stanger SJ, et al. Mouse spermatocytes express CYP2E1 and respond to acrylamide exposure. PLoS One. 2014;9(5):e94904. doi:10.1371/journal.pone.0094904.
DuTeaux SB, Hengel MJ, DeGroot DE, et al. Evidence for trichloroethylene Bioactivation and adduct formation in the rat epididymis and efferent ducts. Biol Reprod. 2003;69(3):771–9. doi:10.1095/biolreprod.102.014845.
Dacheux J-L, Dacheux F. New insights into epididymal function in relation to sperm maturation. Reproduction. 2014;147(2):R27–42. doi:10.1530/rep-13-0420 .A review of the influence of the epididymal proteins and environment on sperm maturation in preparation for fertilization
Sullivan R, Saez F. Epididymosomes, prostasomes, and liposomes: their roles in mammalian male reproductive physiology. Reproduction. 2013;146(1):R21–35. doi:10.1530/rep-13-0058.
Shum WW, Smith TB, Cortez-Retamozo V, et al. Epithelial basal cells are distinct from dendritic cells and macrophages in the mouse epididymis. Biol Reprod. 2014;90(5):90 . doi:10.1095/biolreprod.113.116681.1-10
Mathur SS. Sperm motility on postcoital testing correlates with male autoimmunity to sperm. Fertil Steril. 41(1):81–7.
Close CE, Roberts PL, Berger RE. Cigarettes, alcohol and marijuana are related to pyospermia in infertile men. J Urol. 1990;144(4):900–3.
Zhu Z, Xu W, Dai J, et al. The alteration of protein profile induced by cigarette smoking via oxidative stress in mice epididymis. Int J Biochem Cell Biol. 2013;45(3):571–82. doi:10.1016/j.biocel.2012.12.007.
Kaur S, Bansal MP. Protective role of dietary-supplemented selenium and vitamin E in heat-induced apoptosis and oxidative stress in mice testes. Andrologia. 2015;47(10):1109–19. doi:10.1111/and.12390.
Hendin BN, Kolettis PN, Sharma RK, et al. Varicocele is associated with elevated spermatozoal reactive oxygen species production and diminished seminal plasma antioxidant capacity. J Urol. 1999;161(6):1831–4. doi:10.1016/S0022-5347(05)68818-0.
KP N, SSR A, FF P, et al. Relationship of interleukin-6 with semen characteristics and oxidative stress in patients with varicocele. Urology. 2004;64(5):1010–3. doi:10.1016/j.urology.2004.05.045.
Plongthongkum N, Diep DH, Zhang K. Advances in the profiling of DNA modifications: cytosine methylation and beyond. Nat Rev Genet. 2014;15(10):647–61. doi:10.1038/nrg3772.
Hammoud Saher S, Low Diana HP, Yi C, et al. Chromatin and transcription transitions of mammalian adult germline stem cells and spermatogenesis. Cell Stem Cell. 2014;15(2):239–53. doi:10.1016/j.stem.2014.04.006.
Molaro A, Hodges E, Fang F, et al. Sperm methylation profiles reveal features of epigenetic inheritance and evolution in primates. Cell. 2011;146(6):1029–41. doi:10.1016/j.cell.2011.08.016.
Jiang L, Zhang J, Wang J-J, et al. Sperm, but not oocyte, DNA methylome is inherited by zebrafish early embryos. Cell. 2013;153(4):773–84. doi:10.1016/j.cell.2013.04.041.
Sigurdsson MI, Smith AV, Bjornsson HT, et al. Distribution of a marker of germline methylation differs between major families of transposon-derived repeats in the human genome. Gene. 2012;492(1):104–9. doi:10.1016/j.gene.2011.10.046.
Smith ZD, Chan MM, Mikkelsen TS, et al. A unique regulatory phase of DNA methylation in the early mammalian embryo. Nature. 2012;484(7394):339–44. doi:10.1038/nature10960.
Jones EL, Mudrak O, Zalensky AO. Kinetics of human male pronuclear development in a heterologous ICSI model. J Assist Reprod Genet. 2010;27(6):277–83. doi:10.1007/s10815-010-9402-y.
Messerschmidt DM, Knowles BB, Solter D. DNA methylation dynamics during epigenetic reprogramming in the germline and preimplantation embryos. Genes Dev. 2014;28(8):812–28. doi:10.1101/gad.234294.113.
Donkin I, Versteyhe S, Ingerslev Lars R, et al. Obesity and bariatric surgery drive epigenetic variation of spermatozoa in humans. Cell Metab. 2016;23:1–10. doi:10.1016/j.cmet.2015.11.004.
Denham J, O'Brien BJ, Harvey JT, et al. Genome-wide sperm DNA methylation changes after 3 months of exercise training in humans. Epigenomics. 2015;7(5):717–31. doi:10.2217/epi.15.29.
Miao M, Zhou X, Li Y, et al. LINE-1 hypomethylation in spermatozoa is associated with bisphenol a exposure. Andrologie. 2014;2(1):138–44. doi:10.1111/j.2047-2927.2013.00166.x.
Radford EJ, Ito M, Shi H, et al. In utero undernourishment perturbs the adult sperm methylome and is linked to metabolic disease transmission. Science (New York, NY). 2014;345(6198):1255903. doi:10.1126/science.1255903.
Jenkins TG, Aston KI, Trost C, et al. Intra-sample heterogeneity of sperm DNA methylation. Mol Hum Reprod. 2015;21(4):313–9. doi:10.1093/molehr/gau115.
Aston KI, Uren PJ, Jenkins TG, et al. Aberrant sperm DNA methylation predicts male fertility status and embryo quality. Fertil Steril. 2015;104(6):1388–97. doi:10.1016/j.fertnstert.2015.08.019 .e5. This study provides evidence that the sperm methylome can predict fertility and embryonic health
Utsuno H, Miyamoto T, Oka K, et al. Morphological alterations in protamine-deficient spermatozoa. Hum Reprod. 2014;29(11):2374–81. doi:10.1093/humrep/deu225.
Iranpour FG. Impact of sperm chromatin evaluation on fertilization rate in intracytoplasmic sperm injection. Adv Biol Res. 2014;3:229. doi:10.4103/2277-9175.145719.
Nili HA, Mozdarani H, Aleyasin A. Correlation of sperm DNA damage with protamine deficiency in Iranian subfertile men. Reprod BioMed Online. 2009;18(4):479–85. doi:10.1016/S1472-6483(10)60123-X.
Fortes MRS, Satake N, Corbet DH, et al. Sperm protamine deficiency correlates with sperm DNA damage in Bos indicus bulls. Andrologie. 2014;2(3):370–8. doi:10.1111/j.2047-2927.2014.00196.x.
Collins AR. Measuring oxidative damage to DNA and its repair with the comet assay. Biochim Biophys Acta Gen Subj. 2014;1840(2):794–800. doi:10.1016/j.bbagen.2013.04.022.
Soumillon M, Necsulea A, Weier M, et al. Cellular source and mechanisms of high transcriptome complexity in the mammalian testis. Cell Rep. 2013;3(6):2179–90. doi:10.1016/j.celrep.2013.05.031.
Sendler E, Johnson GD, Mao S, et al. Stability, delivery and functions of human sperm RNAs at fertilization. Nucleic Acids Res. 2013;41(7):4104–17. doi:10.1093/nar/gkt132.
Jodar M, Sendler E, Krawetz SA. The protein and transcript profiles of human semen. Cell Tissue Res. 2015;363(1):85–96. doi:10.1007/s00441-015-2237-1 .A review of the information that high-throughput technologies have revealed about the structure and function of sperm and seminal factors
Johnson GD, Sendler E, Lalancette C, et al. Cleavage of rRNA ensures translational cessation in sperm at fertilization. Mol Hum Reprod. 2011;17(12):721–6. doi:10.1093/molehr/gar054.
Jodar M, Selvaraju S, Sendler E, et al. The presence, role and clinical use of spermatozoal RNAs. Hum Reprod Update. 2013;19(6):604–24. doi:10.1093/humupd/dmt031.
Fang P, Zeng P, Wang Z, et al. Estimated diversity of messenger RNAs in each murine spermatozoa and their potential function during early zygotic development. Biol Reprod. 2014;90(5):94 . doi:10.1095/biolreprod.114.117788.1-11
Sharma U, Conine CC, Shea JM, et al. Biogenesis and function of tRNA fragments during sperm maturation and fertilization in mammals. Science. 2016;351(6271):391–6. doi:10.1126/science.aad6780 .This study demonstrates the importance of sperm RNAs obtained during epididymal transit on offspring development and health , in a mouse model
Liu W-M, Pang RTK, Chiu PCN, et al. Sperm-borne microRNA-34c is required for the first cleavage division in mouse. Proc Natl Acad Sci U S A. 2012;109(2):490–4. doi:10.1073/pnas.1110368109.
Yuan S, Tang C, Zhang Y, et al. Mir-34b/c and mir-449a/b/c are required for spermatogenesis, but not for the first cleavage division in mice. Biology Open. 2015;4(2):212–23. doi:10.1242/bio.201410959.
Jodar M, Sendler E, Moskovtsev SI, et al. Absence of sperm RNA elements correlates with idiopathic male infertility. Sci Transl Med. 2015;7(295):295re6-re6. doi:10.1126/scitranslmed.aab1287 .This study identifies germline RNAs with potential roles as biomarkers of male infertility
García-López J, Alonso L, Cárdenas DB, et al. Diversity and functional convergence of small noncoding RNAs in male germ cell differentiation and fertilization. RNA. 2015;21(5):946–62. doi:10.1261/rna.048215.114.
Starega-Roslan J, Galka-Marciniak P, Krzyzosiak WJ. Nucleotide sequence of miRNA precursor contributes to cleavage site selection by dicer. Nucleic Acids Res. 2015;43(22):10939–51. doi:10.1093/nar/gkv968.
Rajan KS, Ramasamy S. Retrotransposons and piRNA: the missing link in central nervous system. Neurochem Int. 2014;77:94–102. doi:10.1016/j.neuint.2014.05.017.
Watanabe T. Cheng E-c, Zhong M et al. retrotransposons and pseudogenes regulate mRNAs and lncRNAs via the piRNA pathway in the germline. Genome Res. 2015;25(3):368–80. doi:10.1101/gr.180802.114.
Klengel T, Dias BG, Ressler KJ. Models of intergenerational and transgenerational transmission of risk for psychopathology in mice. Neuropsychopharmacology. 2016;41(1):219–31. doi:10.1038/npp.2015.249 .An overview of the transmission of neurological disease risk across generations , a concept that can be extended to environmental exposures
Gapp K, Jawaid A, Sarkies P, et al. Implication of sperm RNAs in transgenerational inheritance of the effects of early trauma in mice. Nat Neurosci. 2014;17(5):667–9. doi:10.1038/nn.3695.
Fullston T, Ohlsson Teague EMC, Palmer NO, et al. Paternal obesity initiates metabolic disturbances in two generations of mice with incomplete penetrance to the F2 generation and alters the transcriptional profile of testis and sperm microRNA content. FASEB J. 2013;27(10):4226–43. doi:10.1096/fj.12-224048.
Dias BG, Ressler KJ. Parental olfactory experience influences behavior and neural structure in subsequent generations. Nat Neurosci. 2014;17(1):89–96. doi:10.1038/nn.3594.
Cossetti C, Lugini L, Astrologo L, et al. Soma-to-germline transmission of RNA in mice xenografted with human tumour cells: possible transport by exosomes. PLoS One. 2014;9(7):e101629. doi:10.1371/journal.pone.0101629 .A proof-of-principle study demonstrating that mouse sperm can acquire RNAs from somatic cells in distant tissues
Johnson GD, Mackie P, Jodar M, et al. Chromatin and extracellular vesicle associated sperm RNAs. Nucleic Acids Res. 2015;43(14):6847–59. doi:10.1093/nar/gkv591.
Chen Q, Yan M, Cao Z, et al. Sperm tsRNAs contribute to intergenerational inheritance of an acquired metabolic disorder. Science. 2016;351(6271):397–400. doi:10.1126/science.aad7977.
Shea Jeremy M, Serra Ryan W, Carone Benjamin R, et al. Genetic and epigenetic variation, but not diet, shape the sperm methylome. Dev Cell. 2015;35(6):750–8. doi:10.1016/j.devcel.2015.11.024.
Lambrot R, Xu C, Saint-Phar S, et al. Low paternal dietary folate alters the mouse sperm epigenome and is associated with negative pregnancy outcomes. Nat Commun. 2013;4:2889. doi:10.1038/ncomms3889.
Terashima M, Barbour S, Ren J, et al. Effect of high fat diet on paternal sperm histone distribution and male offspring liver gene expression. Epigenetics. 2015;10(9):861–71. doi:10.1080/15592294.2015.1075691.
van de Werken C, van der Heijden GW, Eleveld C, et al. Paternal heterochromatin formation in human embryos is H3K9/HP1 directed and primed by sperm-derived histone modifications. Nat Commun. 2014;5:5868. doi:10.1038/ncomms6868.
Guerrero-Bosagna C, Covert TR, Haque MM, et al. Epigenetic transgenerational inheritance of vinclozolin induced mouse adult onset disease and associated sperm epigenome biomarkers. Reproductive toxicology (Elmsford, NY). 2012;34(4):694–707. doi:10.1016/j.reprotox.2012.09.005.
Guerrero-Bosagna C, Savenkova M, Haque MM, et al. Environmentally induced epigenetic transgenerational inheritance of altered Sertoli cell transcriptome and epigenome: molecular etiology of male infertility. PLoS One. 2013;8(3):e59922. doi:10.1371/journal.pone.0059922.
Doyle TJ, Bowman JL, Windell VL, et al. Transgenerational effects of di-(2-ethylhexyl) phthalate on testicular germ cell associations and spermatogonial stem cells in mice. Biol Reprod. 2013;88(5):112. doi:10.1095/biolreprod.112.106104.
Dobrzyńska M, Tyrkiel E, Derezińska E, et al. Two generation reproductive and developmental toxicity following subchronic exposure of pubescent male mice to di(2-ethylhexyl)phthalate. Annals of Agricultural and Environmental Medicine. 2012;19(1):31–7.
Manikkam M, Tracey R, Guerrero-Bosagna C, et al. Plastics derived endocrine disruptors (BPA, DEHP and DBP) induce epigenetic transgenerational inheritance of obesity, reproductive disease and sperm epimutations. PLoS One. 2013;8(1):e55387. doi:10.1371/journal.pone.0055387.
Iqbal K, Tran DA, Li AX, et al. Deleterious effects of endocrine disruptors are corrected in the mammalian germline by epigenome reprogramming. Genome Biol. 2015;16(1):59. doi:10.1186/s13059-015-0619-z.
Lombó M, Fernández-Díez C, González-Rojo S, et al. Transgenerational inheritance of heart disorders caused by paternal bisphenol a exposure. Environ Pollut. 2015;206:667–78. doi:10.1016/j.envpol.2015.08.016.
Li G, Chang H, Xia W, et al. F0 maternal BPA exposure induced glucose intolerance of F2 generation through DNA methylation change in Gck. Toxicol Lett. 2014;228(3):192–9. doi:10.1016/j.toxlet.2014.04.012.
Doshi T, D’souza C, Vanage G. Aberrant DNA methylation at Igf2–H19 imprinting control region in spermatozoa upon neonatal exposure to bisphenol a and its association with post implantation loss. Mol Biol Rep. 2013;40(8):4747–57. doi:10.1007/s11033-013-2571-x.
Eustache F, Mondon F, Canivenc-Lavier MC, et al. Chronic dietary exposure to a low-dose mixture of Genistein and vinclozolin modifies the reproductive Axis, testis transcriptome, and fertility. Environ Health Perspect. 2009;117(8):1272–9. doi:10.1289/ehp.0800158.
Gazo I, Linhartova P, Shaliutina A, et al. Influence of environmentally relevant concentrations of vinclozolin on quality, DNA integrity, and antioxidant responses of sterlet Acipenser ruthenus spermatozoa. Chem Biol Interact. 2013;203(2):377–85. doi:10.1016/j.cbi.2013.01.004.
Stouder C, Paoloni-Giacobino A. Transgenerational effects of the endocrine disruptor vinclozolin on the methylation pattern of imprinted genes in the mouse sperm. Reproduction. 2010;139(2):373–9. doi:10.1530/rep-09-0340.
O'Flaherty CM, Chan PT, Hales BF, et al. Sperm chromatin structure components are differentially repaired in cancer survivors. J Androl. 2012;33(4):629–36. doi:10.2164/jandrol.111.015388.
Maselli J, Hales BF, Chan P, et al. Exposure to bleomycin, etoposide, and cis-platinum alters rat sperm chromatin integrity and sperm head protein profile. Biol Reprod. 2012;86(5):166 . doi:10.1095/biolreprod.111.098616.1-10
Berthaut I, Montjean D, Dessolle L, et al. Effect of temozolomide on male gametes: an epigenetic risk to the offspring? J Assist Reprod Genet. 2013;30(6):827–33. doi:10.1007/s10815-013-9999-8.
Zhu H, Li K, Liang J, et al. Changes in the levels of DNA methylation in testis and liver of SD rats neonatally exposed to 5-aza-2′-deoxycytidine and cadmium. J Appl Toxicol. 2011;31(5):484–95. doi:10.1002/jat.1673.
Acknowledgments
The graduate student assistantship to M.S.E. from Wayne State University’s Center for Molecular Medicine and Genetics is gratefully acknowledged. This work was supported in part by the Charlotte B. Failing Professorship to S.A.K.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
M.S. Estill and S.A. Krawetz declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article contains references to studies with human or animal subjects performed by one of the authors. All studies involving human biological specimens were carried out in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted.
Additional information
This article is part of the Topical Collection on Environmental Epigenetics
Rights and permissions
About this article
Cite this article
Estill, M.S., Krawetz, S.A. The Epigenetic Consequences of Paternal Exposure to Environmental Contaminants and Reproductive Toxicants. Curr Envir Health Rpt 3, 202–213 (2016). https://doi.org/10.1007/s40572-016-0101-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-016-0101-4