Abstract
Objective
To identify the relationship between binge eating and alcohol consumption.
Methods
This is an integrative literature review of publications from 2015 to 2019, using the Pubmed, Cinhahl, Psynet, Lilacs, Embase and Web of Science virtual databases and the descriptors (“Binge-Eating” OR “Bulimia”) AND Alcohol* in English, Spanish and Portuguese.
Results
A total of 964 articles were found. After reading the titles and abstracts and excluding duplicates, 36 articles were included in the final sample (35 in English and one in Portuguese). They were grouped into three thematic categories: “sample profile and characterization”, “genetic and environmental factors”, and “emotions and behavior”.
Conclusions
The data indicate the existence of a relationship between binge eating and alcohol use, and some factors were associated with this comorbidity. Still, there were few publications on the theme at the national level, indicating the need for developing more research. These findings may support therapeutic actions and strategies for identification of cases, embracing approaches and more effective treatments to meet the individual’s biopsychosocial demands.
Level of evidence
Level V, narrative review.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Eating disorders (ED) are defined as psychiatric conditions that cause changes in the diet and/or eating behavior and may affect the consumption or absorption of food. Their etiology is multifactorial and they are more prevalent in women and characterized by excessive concern with body and weight, compromising the physical health and biopsychosocial development of the individual [1].
Among ED, bulimia nervosa (BN) and binge eating disorder (BED) have similar characteristics in terms of recurrent episodes of high food intake within a short period of time associated with the feeling of loss of control and guilt. The main difference is that in BN, there are compensatory behaviors for the control of body weight such as self-induced vomiting, use of laxatives, diuretics, restrictive diets and excessive physical exercise [2].
Binge eating present in BN can start with a decrease in consumption of foods considered hypercaloric and prohibited to promote weight loss and body satisfaction. The occurrence of the binge eating/guilt/compensatory behavior cycle can become chronic and intermittent with periods of remission. Although the absence of compensatory behavior is evident in BED, the constant practice of restrictive diets in the development of binge eating in these people takes place frequently [1, 3].
Bulimia nervosa affects more young women and young adults, while BED prevails in adults, regardless of ethnicity and sex. People with BN usually have normal weight or are overweight while those with BED are overweight and obese and seek treatment to lose weight. Although obesity is not a diagnostic criterion for BED, this eating disorder is associated with the severity of obesity [4, 5].
Low self-esteem, childhood trauma by violence, childhood obesity, early pubertal maturation, genetic factors and social vulnerabilities predispose to greater risk for development of these conditions. In BN, there is a greater concern with body image than in BED, which generates the constant evaluation and distorted perception of body size and shape. However, people with BED use health services with more frequency [1, 5, 6].
These disorders are associated with several health problems such as depression, anxiety, post-traumatic stress, personality disorders, and abuse of psychoactive substances, especially alcohol [4, 7, 8]. Specifically, the search to regulate negative emotions and the tendency to act impulsively are behaviors that influence the occurrence of binge eating and excessive consumption of alcoholic beverages [9,10,11].
Studies demonstrate gaps in the relationship between alcohol consumption patterns and ED, as well as little understanding of the possible causes and consequences of ED and the use of alcohol [4, 11]. This evidence motivated further studies to explain the cause–effect relationship between ED and alcohol consumption, and added environmental, biological, personality and other behavioral factors as variables [12]. A Colombian survey of adolescents of both sexes with ED found that up to 50% of them were abusing alcohol or some illicit drug. Those who abused alcohol or other drugs were up to 11 times more likely to have ED [13].
The simultaneous occurrence of ED and alcohol consumption is still poorly elucidated in the literature, especially in Brazil. People with ED do not usually report this habit during clinical evaluations, or its relationship with life habits, even when questioned [14]. To contribute to the improvement of patient care, this study aimed to identify the relationship between binge eating and alcohol consumption.
Methodology
This is an integrative literature review, where we sought to identify, analyze and synthesize the results of primary studies that provided evidence on factors associated with binge eating in BN and BED and alcohol consumption.
The integrative review presents a broad methodological approach of reviews, allowing the inclusion of studies with different designs so as to provide a thorough understanding of the studied theme [15]. This methodological strategy involves the following steps: identification of the theme and guiding question, establishment of inclusion and exclusion criteria, literature search, data organization, definition of the information to be extracted from the selected studies, analysis of the studies included in the review, interpretation of results, and synthesis of knowledge [16].
To formulate the guiding question of the study, the PICO strategy was applied, where P (population): women with binge eating disorder who consume alcoholic beverages; I (intervention): factors associated with alcohol consumption in women with binge eating disorder; C (control): it does not apply to integrative reviews; O (outcome): the main evidence found in the literature [17]. Based on this procedure, the following question was established: what are the factors associated with binge eating and alcohol consumption that are evident in the literature?
The studies came from journals indexed in the following electronic databases, from 2015 to 2019: Pubmed, Cinhahl, Psynet, Lilacs, Embase, and Web of Science. The Health Descriptors (DeCS) and Medical Subject Headings (MeSH) were consulted, and the descriptors that were identified and used in the search were: (“Binge-Eating” OR “Bulimia”) AND Alcohol*, in Portuguese, English and Spanish.
We included original articles, conducted with human beings regardless of sex and age, with a quantitative and qualitative approach, experimental or non-experimental, with information on binge eating and alcohol consumption. On the other hand, editorials, books, or book chapters, dissertations or theses, case reports, letters, opinion articles, comments, abstracts in annals, essays, studies that reused data from previous works, and duplicate publications were excluded.
An instrument was prepared for the synthesis and analysis of the data including the following items: identification of the article, objective, study design, participants, main results, keywords and thematic categories.
Results
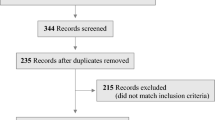
A total of 964 articles were found presenting information about alcohol consumption and binge eating: 160 articles in Pubmed, 80 in Cinahl, 147 in PsycINFO, 41 in Lilacs, 322 in Embase, and 214 in Web of Science.
At first, the titles and abstracts of the total sample were read, resulting in the exclusion of 776 articles. In a second moment, 134 of the 188 articles that remained were excluded because they were duplicated. In a third moment, 54 articles were read in full, and 18 were excluded, because they only addressed alcohol use or binge eating, or drug use without specifying alcohol and ED other than BN and/or BED. Thus, the final sample was composed of 36 articles that were read in an exploratory way.
Among the selected articles, 35 were published in English and 1 in Portuguese. As for the origin of the studies, there was a concentration of scientific productions in the United States of America, with 21 articles, followed by Brazil, with 4, Italy with 2, and Finland, Spain, France, Australia, Russia, Korea and the United Kingdom, each 1 with 1 article. One article was carried out by researchers from Iraq and Afghanistan and another by the United Kingdom, United States of America and Finland.
Regarding the publication period, it was observed that the year of greatest dissemination was in 2015 with 12 articles. In 2016, six articles were published, seven articles in 2017 as well as in 2018, and four in 2019. Among the studies analyzed, 29 of them were found in more than 1 database, 1 exclusively at Pubmed, 1 at PsycINFO, 1 at Cinahl, 2 at Embase, 2 at Web of Science.
The critical reading and analysis of the articles made it possible to highlight the main results on binge eating (BN and BED) and alcohol use, with the identification of keywords. These keywords were then grouped into the following thematic categories: Sample profile and characterization, Genetic and environmental factors, and Emotions and behavior.
Category 1—sample profile and characterization
The articles that aimed to describe BN and BED characteristics related to alcohol use corresponded to a total of 15. Studies on the prevalence and incidence of ED and alcohol use stood out, and were associations with sociodemographic conditions (sex, age, ethnicity, marital status) and clinical aspects (binge eating practices, dieting, compensatory methods, concern with weight and image body) (Table 1).
Category 2—genetic and environmental factors
Genetic and environmental factors influence the appearance of BN and BED and the use of alcohol were addressed in seven studies. Genetic factors comprise types of twinning and races while environmental factors are determined by childhood experiences, traumatic and stressful experiences, sexual and physical abuse, violence, ideal body phenotype, weight stigma, social minorities and culture (Table 2).
Category 3—emotions and impulsivity
The understanding of binge eating and alcohol use from an emotional and behavioral point of view was addressed in 14 of the studies showing emotional dysregulation, perfectionism, impulsivity, anxiety, depression, negative effects and risk of suicide (Table 3).
The 19 articles in the final sample were read in an exploratory manner. Of these, 16 were published in English and three in Portuguese. Regarding the origin of the studies, there was a concentration of scientific productions from the United States, with 12 articles, followed by three publications in Brazil, two in Sweden, one in Finland and one in England.
Regarding the time of publication, it was observed that three articles were published in 2013, and only one in 2014. In turn, 2015 was the year with more publications, with a total of seven articles. Five articles were published in 2016, and three in 2017. Among the studies analyzed, 13 were present in more than one database, three were exclusively in Pubmed, 2 in the Web of Science, and one in PsycINFO.
The reading and critical analysis of the articles made it possible to group the data into three thematic categories: sample profile and characterization, genetic and environmental factors, and emotions and impulsivity.
Discussion
Regarding the category 1—sample profile and characterization, due to the fact that females have a higher incidence of ED when compared to males [4], some researchers investigated the occurrence of these conditions only in women [11, 27, 29]. Those who investigated in both sexes confirmed the predominance in women [28, 30, 31]. A study in Russia found that the prevalence of BED and BN was similar between the sexes [23]. Another found a relatively higher proportion of BED among men [18, 20]. Notwithstanding the shortage of studies involving men demonstrated by these data and the low prevalence of ED in this sex, greater knowledge about the epidemiological aspects can be useful to outline prevention and treatment strategies.
Regarding age, there was a higher frequency of ED and alcohol consumption in young adults aged up to 38 years [29,30,31]. Only one study revealed that the probability of binge episodes was present in older individuals, aged 34–54 years [28]. An average age of 27 years was observed for BN and 30.9 years for BED [30]. A study with women with ED identified that more than 80% of them tried alcohol at age 16 and experienced excessive intake until loss of consciousness, and 13.8% did so throughout life [11].
Regarding ethnicity, there was a predominance of ED in white women who consumed alcoholic beverages [14, 29, 30]. Differing from these findings, a study in Brazil found a higher prevalence in brown/black people [18]. These data may be explained by miscegenation in the country.
As for marital status, a study involving 2458 individuals of both sexes showed that those with BED were more likely to be single or to get married and divorce afterwards. In addition, they were twice as likely to report symptoms of alcohol use disorder [20]. Corroborating these findings, a study of women who abused psychoactive substances found that most of them were divorced or single [14].
The survey of the current study indicated that there is a simultaneous occurrence of alcohol consumption and ED, in greater proportion in the presence of episodes of binge eating such as BN [19, 22, 29, 30], BED [19, 22, 30], and compulsive-purgative type of anorexia nervosa [30]. However, users of alcohol and other drugs from a Psychosocial Care Center had more symptoms of anorexia nervosa than those typical of BN [31]. This finding was corroborated by another study with 153 university students where it was identified that participants with symptoms of anorexia nervosa and BN consumed more alcoholic beverages, while this consumption was not found in the probable cases of BED [29].
In the United States, a study with 122 women undergoing treatment for psychoactive substance use revealed that 21% of them had ED, and of these, 20% reported one or more episodes of binge eating in the last 28 days [53]. Another study identified an association between the use of alcohol and BED, showing a 65% greater chance of developing BED in people who use alcohol [20].
The Longitudinal Study on Adult Health (ELSA-Brazil) interviewed 15,074 people and found that 6.5% reported 2 or more episodes of binge eating per week and were more likely to have a pattern of high alcohol intake over short periods of time, once or twice a week (8.9%) [28].
A study evaluated the prevalence of alcohol use and BED after Roux-en-Y gastric bypass surgery in 46 patients (33 women and 13 men) and found that alcohol use was frequent throughout the lives of these people and that BED and alcohol use were frequently associated, although no statistical significance was found [26].
The type of psychoactive substance most consumed by patients with ED was alcohol [24, 30, 31]. However, in the results of Killeen et al. [53], cocaine was identified as the most consumed drug, followed by alcohol. Purging was also linked to smoking and excessive consumption of alcohol, marijuana and other drugs in the United Kingdom, United States and Finland [21].
Other relevant factors were physical inactivity and obesity. People with recurrent binge eating episodes are more likely to be sedentary (64.6%) and obese (45.9%) [28]. In contrast, a study of women who abused psychoactive substances showed that 18.7% of them performed excessive physical exercise as a way to control weight [53]. Excessive physical exercise [25, 29], restrictive diets [25, 29], fasting and purging were more subject to problematic alcohol use [29].
Another aspect found in this category concerns body image. Women who used alcohol were dissatisfied with their weight (36%) and their body (34%) due to their feelings of guilt while eating (45.5%), fear of losing control over their diet (30%), and a strong desire to lose weight (50%) [54]. Among women, excessive alcohol use was associated with dissatisfaction with weight and compulsive eating, and among men, with excess weight, vomiting and use of laxatives [23].
With regard to category 2—genetic and environmental factors, the genetic influence on the development of bulimic symptoms and alcohol consumption is clear and recognized in the literature [1, 5, 38]. Genes can predetermine a person’s characteristics that directly or indirectly lead to risk behaviors such as disordered eating and alcohol consumption, and it is believed that both conditions have common neural pathways [38].
A study carried out in the USA with adolescents between 16 and 17 years old of both sexes identified phenotypic and genetic correlations between involvement of alcohol use, desire for a lean body and body dissatisfaction, which were significantly higher in females. It was also observed that these environmental and phenotypic correlations were not exclusive between alcohol use, binge eating and/or compensatory behaviors [33].
Another study found different results, where the association between alcohol use and bulimic symptoms was almost twice as high in monozygotic twins as in dizygotic twins. It also demonstrated a significant association between alcohol use and bulimic symptoms in males [38]. These findings suggest that genetic factors have a strong influence on binge eating and alcohol consumption [33, 38].
A study of 3540 twins evaluated the use of nicotine, alcohol and cannabis and found that those who started drinking alcohol early (before 15 years of age) were more likely to develop binge eating and compensatory methods when compared to those who had this experience later on [37].
To identify ethnicity as a genetic factor, a study compared Afro-descendant twins with American twins and observed that the latter group was more predisposed to binge eating and alcohol consumption, although without statistically significant difference [36].
Regarding environmental factors, it is known that experiences of parents are significantly associated with the development of ED and propensity to use psychoactive substances in children [33]. The literature confirms this finding by demonstrating that depression and the use of psychoactive substances in parents increase the risk of involvement of children with alcohol consumption, eating difficulties or both [54, 55].
Another environmental factor is the history of trauma, specifically as a result of cases of violence and post-traumatic stress [34]. A study carried out with 429 self-reported sexual minorities (lesbian and bisexual people) evaluated binge eating and alcohol use as potential aggravating symptoms of post-traumatic stress, with only binge eating showing a significant association [32]. Still unexpectedly, there was no relationship between a stressful event and alcohol use, since another study with sexual minorities identified this relationship [35]. In general, people in these groups who use alcohol and binge eating report more discrimination, stressful situations, less positive affect and less social support [35].
Regarding category 3—emotions and impulsivity, it is known that binge eating and alcohol consumption are behaviors that are linked to emotional dysregulation [49], impulsivity [43], or both [10, 56]. This comorbidity may be associated with suicide ideation and suicide attempts, anxiety and mood disorders.
Pisetsky et al. [49] evaluated positive and negative emotions in 133 women with BN before and after drunkness and 33.8% of them self-reported at least one episode of alcohol intoxication during the studied period. The results indicated that sadness was stable before drinking alcohol, and a few hours later, this feeling was augmented, suggesting that alcohol did not serve as a mechanism of emotional regulation. Researchers also noted that alcohol and/or food consumption could be a strategy of emotional regulation for coping with suffering, and acting impulsively was a strategy to avoid or divert such negative emotions [56].
A study carried out in Spain with 70 women undergoing treatment for BN showed the association of this condition with alcohol abuse when compared to a non-clinical sample of 70 controls, and also confirmed associations with symptoms of depression, impulsivity, severe traits of borderline personality and self-destructive behaviors for abuse of alcohol in patients with BN. These findings suggest that depressive symptoms and increased cortisol levels could be behind these relationships [39].
Negative emotions and a tendency to act impulsively are common behaviors related to binge eating and heavy drinking [40, 47]. In fact, individuals who drink alcohol are more likely to adopt hasty actions, such as binge eating, when they feel negative emotions [40, 47]. A study examined the use of alcohol and binge eating among adolescents of both sexes and revealed that dysregulation of emotion was a predictor for excessive use of alcohol only in males, mainly due to the difficulty in controlling impulses or reacting before negative emotions [56]. Men are more likely to use emotional regulation strategies in attempts to control impulsivity or change a situation that is believed to drive their emotions than women [52]. However, other results investigating impulsivity in BN patients with and without alcohol consumption did not identify differences between the groups when assessing meal intake and other forms of impulsivity [43].
Symptoms of BN were significantly associated with treatment rejection among young adult men under treatment for psychoactive substance use after controlling problems related to alcohol. A possible reason for the association between symptoms of BN and rejection of treatment is that people with BN who use alcohol and other drugs have high levels of impulsivity and more difficulties with tolerance, distress and emotional regulation [48].
The main limitation of this study is the heterogeneity of the methodologies of the included studies, as they used different diagnostic criteria for BN, BED and alcohol use, and also diverse research instruments and number of participants. The results were discussed considering the multifactorial approach to ED and alcohol use. However, gaps remained as to whether BN, BED and alcohol use share more characteristics and associated factors, because only 18 of the 36 studies in this review compared BN and alcohol use, or BED and alcohol use, or BN, BED and alcohol use.
This review identified that most studies were published in English and only one in Portuguese, in peer-reviewed journals indexed in the selected databases. Studies published between 2015 and 2019 were explored to obtain more up-to-date data, and an increase in research in this area was observed. Longitudinal investigations and randomized clinical trials are needed to better understand the causes and long-term consequences of the relationship between BN, BED and alcohol use that may provide subsidies for the treatment of these serious mental problems.
What is already known on this subject?
Little was known about the association between binge eating and alcohol use before conducting this study, characterizing a gap in knowledge about the factors involved and demonstrating the need for further research to elucidate this question.
What your study adds?
After this investigation, a relationship was identified between binge eating and alcohol use determined by multifactorial characteristics involving sociodemographic (age, sex, marital status), nutritional (dieting, purging and body dissatisfaction), genetic and environmental (traumas, sexual minorities), and emotional (emotional deregulation and impulsive behaviors) factors.
Final considerations
The results of the present study indicated that there is a relationship between binge eating and alcohol use, which is not influenced by a single variable. The investigation showed that sociodemographic, nutritional, genetic, environmental and emotional characteristics of the analyzed samples proved to be relevant in this phenomenon. However, there are few publications on the theme addressed, and therefore further research is needed. These findings may support therapeutic actions and strategies for the identification of cases, embracing approaches, and more effective treatments to meet the individuals’ biopsychosocial demands.
References
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Association, Arlington
Berkman ND, et al (2015) Management and outcomes of binge eating disorder. Comparative Effectiveness Review No. 160. (Prepared by RTI International—University of North Carolina Evidence-based Practice Centre under Contract No. 290-2012-00008-1.) AHRQ Publication No. 15(16)-EHC030-EF. Agency for Healthcare Research and Quality, Rockville, December 2015. http://www.effectivehealthcare.ahqr.gov/reports/final.cfm
Soihet ADS, Silva AD (2019) Efeitos psicológicos e metabólicos da restrição alimentar no transtorno de compulsão alimentar. Nutr Bras 18:55–62. https://doi.org/10.33233/nb.v18i1.2563
Udo T, Grilo CM (2018) Prevalence and correlates of DSM-5-defined eating disorders in a nationally representative sample of U.S. adults. Biol Psychiatry 84:345–354. https://doi.org/10.1016/j.biopsych.2018.03.014
Hilbert A et al (2019) Meta-analysis of the efficacy of psychological and medical treatments for binge-eating disorder. J Consult Clin Psychol 87:91–105. https://doi.org/10.1037/ccp0000358
Lewer M, Bauer A, Hartmann AS, Vocks S (2017) Different facets of body image disturbance in binge eating disorder: a review. Nutrients 9:1294. https://doi.org/10.3390/nu9121294
Olguin P et al (2016) Medical comorbidity of binge eating disorder. Eat Weight Disord 22:13–26. https://doi.org/10.1007/s40519-016-0313-5
Cooper Z, Calugi S, Dalle Grave RI (2019) Controlling binge eating and weight: a treatment for binge eating disorder worth researching? Eat Weight Disord. https://doi.org/10.1007/s40519-019-00734-4
Grucza RA, Przybeck TR, Cloninger CR (2007) Prevalence and correlates of binge eating disorder in a community sample. Compr Psychiatry 48:124–131. https://doi.org/10.1016/j.comppsych.2006.08.002
Stojek MM, Fischer S, Murphy CM, MacKillop J (2014) The role of impulsivity traits and delayed reward discounting in dysregulated eating and drinking among heavy drinkers. Appetite 80:81–88. https://doi.org/10.1016/j.appet.2014.05.004
Mustelin L, Latvala A, Raevuori A, Rose RJ, Kaprio J, Keski Rahkonen A (2016) Risky drinking behaviors among women with eating disorders—a longitudinal community-based study. Int J Eat Disord 49:563–571. https://doi.org/10.1002/eat.22526
Gregorowski C, Seedat S, Jordaan GP (2013) A clinical approach to the assessment and management of co-morbid eating disorders and substance use disorders. BMC Psychiatry 13:289. https://doi.org/10.1186/1471-244X-13-289
Center on Addiction and Substance Abuse (CASA) (2003) Food for thought: substance abuse and eating disorders. The National Center on Addiction and Substance Abuse, Columbia University, New York. https://www.centeronaddiction.org/addiction-research/reports/food-thought-substance-abuse-and-eating-disorders
Killeen TK et al (2011) Assessment and treatment of co-occurring eating disorders in privately funded addiction treatment programs. Am J Addict 20:205–211. https://doi.org/10.1111/j.1521-0391.2011.00122.x
Souza MT, Silva MD, Carvalho R (2010) Revisão integrativa: o que é e como fazer. Einstein (São Paulo) 8:102–106. https://doi.org/10.1590/s1679-45082010rw1134
Mendes KDS, de Silveira RC CP, Galvão CM (2009) Revisão integrativa: método de pesquisa para a incorporação de evidências na saúde e na enfermagem. Texto contexto—enferm 17:758–764
Brasil (2012) Ministério da Saúde. Diretrizes metodológicas: elaboração de revisão sistemática e metanálise de ensaios clínicos randomizado. Editora do Ministério da Saúde, Brasília
Freitas FM, Moraes CL, Braga JU, Reichenheim ME, da Veiga GV (2018) Abusive alcohol consumption among adolescents: a predictive model for maximizing early detection and responses. Public Health 159:99–106. https://doi.org/10.1016/j.puhe.2018.02.008
Rolland B, Naassila M, Duffau C, Houchi H, Gierski F, André J (2017) Binge eating, but not other disordered eating symptoms, is a significant contributor of binge drinking severity: findings from a cross-sectional study among french students. Front Psychol 8:1878. https://doi.org/10.3389/fpsyg.2017.01878
Mitchell JE et al (2015) Eating behavior and eating disorders in adults before bariatric surgery. Int J Eat Disord 48:215–222. https://doi.org/10.1002/eat.22275
Solmi F et al (2015) Prevalence of purging at age 16 and associations with negative outcomes among girls in three community-based cohorts. J Child Psychol Psychiatry 56:87–96. https://doi.org/10.1111/jcpp.12283
Chapa DAN, Bohrer BK, Forbush KT (2018) Eating behaviors is the diagnostic threshold for bulimia nervosa clinically meaningful? Eat Behav 28:16–19. https://doi.org/10.1016/j.eatbeh.2017.12.002
Stickley A et al (2015) Binge drinking and eating problems in russian adolescents. Alcohol Clin Exp Res 39:540–547. https://doi.org/10.1111/acer.12644
Slane JD et al (2016) Eating behaviors: prevalence, psychiatric comorbidity, and associations with body mass index among male and female Iraq and Afghanistan veterans. Mil Med 181:e1650–e1656. https://doi.org/10.7205/MILMED-D-15-00482
Castañeda G et al (2019) Examining the effect of weight conscious drinking on binge drinking frequency among college freshmen. J Am Coll Health 26:1–8. https://doi.org/10.1080/07448481.2019.1642204
Freire CC, Zanella MT, Arasaki CH, Segal A (2019) Binge eating disorder is not predictive of alcohol abuse disorders in long-term follow-up period after Roux-en-Y gastric bypass surgery. Eat Weight Disord. https://doi.org/10.1007/s40519-019-00663-2
Łowińska A, Ziółkowska B (2017) Comorbidity of alcohol dependence and abnormal eating behaviours in women in early and middle adulthood. Alcohol Drug Addict 30:279–294. https://doi.org/10.5114/ain.2017.73666
Souza da Silva T, Bisi Molina MDC, Antunes Nunes MA, Perim de Faria C, Valadão Cade N (2016) Binge eating, sociodemographic and lifestyle factors in participants of the ELSA-Brazil. J Eat Disord 4:25. https://doi.org/10.1186/s40337-016-0095-1
Martin JL, Groth G, Longo L, Rocha TL, Martens MP (2015) Disordered eating and alcohol use among college women: associations with race and big five traits. Eat Behav 17:149–152. https://doi.org/10.1016/j.eatbeh.2015.02.002
Fouladi F et al (2015) Prevalence of alcohol and other substance use in patients with eating disorders. Eur Eat Disord Rev 23:531–536. https://doi.org/10.1002/erv.2410
Freitas PHB et al (2015) Transtornos Alimentares e o uso de drogas: Perfil Epidemiológico. Rev Baiana Enfermagem 29:146–155
Cronce LM, Berdard-Gilligan MA, Zimmerman L, Hodge KA, Kaysen D (2017) Alcohol and binge eating as mediators between posttraumatic stress disorder symptom severity and body mass index. Obesity 25:801–806. https://doi.org/10.1002/oby.21809
Baker JH et al (2018) Associations between alcohol involvement and drive for thinness and body dissatisfaction in adolescent twins: a bivariate twin study. Alcohol Clin Exp Res 42:2214–2223. https://doi.org/10.1111/acer.13868
Brewerton TD, Dansky BS, O’neil PM, Kilpatrick DG (2015) The number of divergent purging behaviors is associated with histories of trauma, PTSD, and comorbidity in a national sample of women. Eat Disord 23:422–429. https://doi.org/10.1080/10640266.2015.1013394
Mason TB, Lewis RJ (2018) Clustered patterns of behavioral and health-related variables among young lesbian women. Behav Ther 50:683–695. https://doi.org/10.1016/j.beth.2018.10.006
Munn-Chernoff MA et al (2015) Bulimic behaviors and early substance use: findings from a Cotwin-control study. Alcohol Clin Exp Res 39:1740–1748. https://doi.org/10.1111/acer.12829
Munn-Chernoff MA et al (2015) Genetic overlap between alcohol use disorder and bulimic behaviors in European American and African American women. Drug Alcohol Depend 153:335–340. https://doi.org/10.1016/j.drugalcdep.2015.05.043
Baker JH, Munn-Chernoff MA, Lichtenstein P, Larsson H, Maes H, Kendler KS (2017) Shared familial risk between bulimic symptoms and alcohol involvement during adolescence. J Abnorm Psychol 126:506–518. https://doi.org/10.1037/abn0000268
Vaz-Leal FJ et al (2015) Neurobiological and clinical variables associated with alcohol abuse in bulimia nervosa. Eur Eat Disord Rev 23:185–192. https://doi.org/10.1002/erv.2352
Fazzino TL, Raheel A, Peppercorn N, Forbush K, Kirby T, Sher KJ et al (2018) Motives for drinking alcohol and eating palatable foods: an evaluation of shared mechanisms and associations with drinking and binge eating. Addict Behav 85:113–119. https://doi.org/10.1016/j.addbeh.2018.04.025
Elmquist JA, Shorey RC, Anderson S, Stuart GL (2018) Experiential avoidance and bulimic symptoms among men in residential treatment for substance use disorders: a preliminary examination. J Psychoactive Drugs 50:81–87. https://doi.org/10.1080/02791072.2017.1368746
Trojanowski PJ, Adams LM, Fischer S (2019) Understanding profiles of student binge drinking and eating: the importance of motives. Addict Behav 96:148–155. https://doi.org/10.1016/j.addbeh.2019.04.025
Sysko R, Ojserkis R, Schebendach J, Evans SM, Hildebrandt T, Walsh BT (2017) Impulsivity and test meal intake among women with bulimia nervosa. Appetite 112:1–8. https://doi.org/10.1016/j.appet.2017.01.005
Wakefor G, Kannis-Dymand L, Statham D (2017) Anger rumination, binge eating, and at-risk alcohol use in a university sample. Aust J Psychol. https://doi.org/10.1111/ajpy.12187
Becker DF, Grilo CM (2015) Comorbidity of mood and substance use disorders in patients with binge-eating disorder: associations with personality disorder and eating disorder pathology. J Psychosom Res 79:159–164. https://doi.org/10.1016/j.jpsychores.2015.01.016
Pompili S, Laghi F (2017) Binge eating and binge drinking among adolescents : the role of drinking and eating motives. J Health Psychol 24:1505–1516. https://doi.org/10.1177/1359105317713359
Kim YR et al (2018) Determinants of binge eating disorder among normal weight and overweight female college students in Korea. Eat Weight Disord 23:849–860. https://doi.org/10.1007/s40519-018-0574-2
Elmquist J, Shorey RC, Anderson SE, Temple JR, Stuart GL (2016) The relationship between eating disorder symptoms and treatment rejection among young adult men in residential substance use treatment. Subst Abuse 10:39–44. https://doi.org/10.4137/SART.S33396
Pisetsky EM et al (2016) An examination of affect prior to and following episodes of getting drunk in women with bulimia nervosa. Psychiatry Res 240:202–208. https://doi.org/10.1016/j.psychres.2016.04.044
Mole TB, Irvine MA, Worbe Y, Collins P, Mitchell SP, Bolton S et al (2015) Impulsivity in disorders of food and drug misuse. Psychol Med 45:771–782. https://doi.org/10.1017/S0033291714001834
Racine SE, Martin SJ (2016) Exploring divergent trajectories: disorder-specific moderators of the association between negative urgency and dysregulated eating. Appetite. 103:45–53. https://doi.org/10.1016/j.appet.2016.03.021
Pompili S, Laghi F (2018) Drunkorexia among adolescents: the role of motivations and emotion regulation. Eat Behav 29:1–7. https://doi.org/10.1016/j.eatbeh.2018.01.001
Killeen T, Brewerton TD, Campbell A, Cohen LR, Hien DA (2015) Exploring the relationship between eating disorder symptoms and substance use severity in women with comorbid PTSD and substance use disorders. Am J Drug Alcohol Abuse 41:547–552. https://doi.org/10.3109/00952990.2015.1080263
Cranford JA, Zucker RA, Jester JM, Puttler LI, Fitzgerald HE (2010) Parental alcohol involvement and adolescent alcohol expectancies predict alcohol involvement in male adolescents. Psychol Addict Behav 24:386–396. https://doi.org/10.1037/a0019801
Bould H, Koupil I, Dalman C, DeStavola B, Lewis G, Magnusson C (2015) Parental mental illness and eating disorders in offspring. Int J Eat Disord 48:383–391. https://doi.org/10.1002/eat.22325
Mikheeva OV, Tragesser SL (2016) Personality features, disordered eating, and alcohol use among college students: a latent profile analysis. Pers Individ Dif 94:360–365. https://doi.org/10.1016/j.paid.2016.02.004
Funding
No funding or grants were used for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares no conflicts of interest.
Ethical approval
This article does not include studies conducted with human beings of animals.
Informed consent
Formal consent is not required for this type of study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The article is part of the Topical Collection on Food and Addiction.
Rights and permissions
About this article
Cite this article
Azevedo, L.D.S., de Souza, A.P.L., Ferreira, I.M.S. et al. Binge eating and alcohol consumption: an integrative review. Eat Weight Disord 26, 759–769 (2021). https://doi.org/10.1007/s40519-020-00923-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-020-00923-6