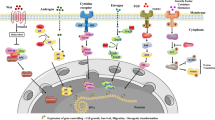
Abstract
Purpose of Review
Cancer of the bladder is a serious health problem with significant mortality once it progresses to advanced stages. Moreover, chronic surveillance and treatments are required to prevent the inherent high recurrence and aggressive nature of these tumors. As a result, not only the quality of life for the patients is affected but it also adds to the treatment cost, making it one of the costliest cancers to treat. Therefore, it is highly imperative to consider preventive options that have been largely neglected.
Recent Findings
Although smoking prevalence is decreasing, a decline in BC incidence has not been seen, yet suggesting that smoking history and other factors still pose a threat to develop BC. With the increase of diabetic and obese populations, the risk for BC is also increasing. In spite of their modifiable nature, advancement in diagnosis, understanding of the disease, and enormous preclinical chemoprevention data, efforts in that direction for screening and primary or secondary prevention of this disease have been unsatisfactory. Moreover, no new therapeutic were approved for the last three decades; thus, the 5-year survival of BC patients has also not improved for decades.
Summary
In the current review, we have discussed the central role of inflammation in the major risk factors such as smoking, diabetes, obesity, and infection leading to BC. We summarized the preclinical data of promising anti-inflammatory agents for primary, secondary, as well as tertiary prevention. Thus, we believe that developing chemopreventive strategies for bladder cancer by targeting inflammation is highly desirable.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bladder cancer (BC) is a global health problem affecting nearly 430,000 people annually, making it the 9th most common cancer worldwide. More than one third of these patients (165,000) die each year [1]. Worldwide bladder cancer incidence trends indicate its direct correlation with the level of human development [2]. Data suggest that developed countries have a threefold higher incidence of BC compared to less-developed nations (ASR of 9.5 and 3.3 per 100,000, respectively). In countries like Germany, there has been a sharp increase in BC cases among both men (35% increase) and women (75% increase) in the last three decades.
There are several identified factors like age, gender, race, and genetics that increase the risk for BC. The incidence of bladder cancer increases with age with a majority of the BC diagnoses being among 50–70-year age groups of both sexes. Since the 1950s, the incidence of bladder cancer has risen by approximately 50%. It is to be anticipated that, with the aging of the population, this trend will continue. Furthermore, BC is cancer with a very high disparity based on gender. Males are at three to four times higher risk of developing BC compared to females. This is partly due to a higher prevalence of smoking among men compared to women. [3]. Therefore, older men with smoking habit are at very high risk for BC compared to other groups. At least 77% of BC cases are among men ranking it the 7th most common while in females, it is 19th in terms of incidence worldwide [2]. Although BC is prevalent among all ethnic groups, it is two times more frequent among whites than in the black population. Only 7% of BC cases are linked to genetic factors [4]. In general, there is a significant fraction of the population that represents a combination of all these risk factors, e.g., white, older men with a smoking habit may have very high risk for BC compared to other groups. Unfortunately, all these factors are non-modifiable; hence, they cannot have any role in prevention and thus motivates us to explore other options to achieve this unmet goal.
Other risk factors are lifestyle, occupation, or environment-related which are modifiable and can have a significant effect on the development of this disease. Some of these factors contribute positively while others are negatively associated. For example, occupations dealing with tobacco (Relative risk (RR) 1.72) or dye (RR 1.58) have a high risk for BC. The combined probability of causation was calculated to be 81.8%. Tobacco smoking remains the most imperative modifiable risk factor due to strong association between smoking history and BC. Statistically significant associations were observed for current (RR 3.14) or former (RR 1.83) cigarette, pipe (RR 1.9), or cigar (RR 2.3) smokers [5, 6] (Fig. 1). Thus, avoiding smoking or quitting alone can have a significant impact on BC in the long run. Although the prevalence rates of smoking have been declining, the absolute number of smokers has been increasing due to growing world populations [20]. Preventing or reducing the effect of positively contributing factors or vice versa can bring down BC cancer incidence. For example, (i) reduction in occupational exposure to aromatic amines led to a decrease in BC incidence [21]; (ii) in Egypt, a marked decrease in the incidence of squamous cell carcinomas of the bladder was observed due to a reduction in Schistosoma infection [22,23,24]. Similarly intervening with the carcinogenesis process in the timely manner in order to prevent the initiation or progression of the disease is beneficial as well. There have been considerable advancements in our knowledge regarding the timing, sequence, and molecular changes in the carcinogenesis process of the urothelium. This provides a unique and immense opportunity for early diagnosis as well as intervention for prevention. In this review, we discuss bladder cancer prevention, including the target, cohorts, agents, and strategies.
Preventing Bladder Cancer
While BC remains a major health issue, it also continues to be a burden on the health care system due to high recurrence rates [25] and long-term monitoring of patients, resulting in the highest per patient lifetime costs among all cancers. In the USA, the annual cost of care for bladder cancer was estimated to be $US4 billion [26]. Approximately 75% of all bladder tumors are non-muscle invasive (NMIBCs) at diagnosis [27, 28]. A quarter of these tumors are T1 stage disease with an invasion of the lamina propria [29] and represent a clinical challenge because of their aggressive nature and heterogeneous outcomes [30]. In spite of sophisticated treatment methods such as combination of urine-based markers, fluorescence-guided cystoscopy, and intravesical instillations, close to 50% of these tumors recur within 2–5 years and many of which progress to muscle invasion disease that pose a high risk for metastasis in those patients [27] and death from systemic disease [31]. Therefore, regular follow-up is necessary to detect recurrences at the earliest possible stage which makes bladder cancer the most expensive of all cancer entities in healthcare systems [26, 32]. BC is preventable because, like many other cancers, it also takes significant time (~ 20 years) from the time of initiation to transform into malignant cells [33]. In relative terms, it means that most of the tumors that are diagnosed between 55 and 75 years of age were actually initiated at a young age between 35 and 55 years. Thus, screening high-risk individuals at an early stage gives an immense opportunity to intervene and prevent this disease.
Unfortunately, in spite of the highly preventable nature, in many ways, bladder cancer remains a neglected disease. Bladder cancer is diagnosed by microscopic examination of cells from urine or bladder tissue and examination of the bladder wall with a cystoscope; novel methods based on urine biomarkers or DNA are being developed and reported. While these procedures are simple, there is currently no screening method recommended for people at average risk. Currently, there are neither approved preventives, nor the treatment options for BC have altered for decades. While some initial response has been noted for existing therapies, many patients experience toxic side effects and tumor recurrence despite the therapy [34,35,36]. Therefore, developing preventive agents against BC can prove to be pivotal.
Target Population
For any screening program, it is important to identify the high-risk target population. Since there is clear evidence on the risk association of BC with certain factors, it is easy to identify the high-risk cohorts. The risk of BC is twofold to sixfold higher for smokers than for non-smokers. As smoking is a strongly associated modifiable habit, for primary prevention, there have been many efforts to encourage people to quit smoking and as a result, the number of smokers has been going down annually. Policies to raise cigarette prices by increasing excise taxes have helped in reducing tobacco consumption. Since 2002, the number of former smokers has increased gradually compared to current smokers in the USA [37]. While this has led to a drop in the incidence of some smoking associated cancers, particularly lung cancer, bladder cancer incidence has remained unchanged for the past four decades [1]. This suggests that smoking has a long-term effect and even former smokers are still at a considerable risk for BC. So, these former smokers should be considered for screening and prevention. Recent data also indicate an increasing trend in people switching to smokeless tobacco products. While we do not have any evidence suggesting the role of these new smoking products in cancer risk, it is definitely important to be cautious and discourage their use in the primary prevention settings. Thus, smoking status should be one of the important criteria to be considered for selecting the high-risk groups.
The second criteria are health conditions such as diabetes [7,8,9,10,11] and obesity [12,13,14] since several studies have indicated their association with BC (Fig. 1). The proportion of the obese, diabetic and aging population is increasing globally and more rapidly in the developing world. Therefore, the population at risk for BC is also increasing. Since type 2 diabetes is the most common form of diabetes, affecting 85–90% of all people with the disease, this can be another criterion. Obesity itself cannot be considered a criterion for screening; there are approximately 70% adults are overweight or obese in the USA [1]. However, this, in combination with other discussed factors, can be used to shortlist the cohort group. Urinary tract infection with Schistosoma haematobium alone is estimated to be responsible for 50% of the BC cases in parts of Africa and Middle East countries [38, 39]. Additionally, patients with spinal cord injury (SCI) and spina bifida also experience bladder inflammation, due to bladder dysfunction, frequent bladder infections, and required catheterization, which significantly increase their risk for BC [40]. In these patients, BC tends to present itself at an earlier age and at a more advanced pathological stage than bladder cancer in the general population. More than half of SCI patients develop transitional cell carcinoma with locally advanced stage (T3 or greater) or lymph node metastases in 88% of these cases [41]. Thus, screening of these patients for early detection of bladder cancer is very important because the symptoms are atypical.
Since strong evidence is available regarding the association of bladder cancer with these cohorts, particularly population groups such as smokers (particularly men), diabetics, obese individuals (Fig. 1), or spinal cord injury patients, there is an urgent need to develop or implement screening and chemoprevention in the target population the prevention of this disease.
Risk Factors and Bladder Inflammation
Cells in the urothelium experience chronic exposure to a variety of chemicals excreted through the renal pathway. Some of these chemicals, like tobacco smoke chemicals, may have direct carcinogenic effects while others may induce inflammation of the bladder. Additionally, chronic diseases/conditions such as diabetes, interstitial cystitis (IC), bladder/kidney stones (bladder calculi) or UT infections, indwelling catheters are all known to cause inflammation of the bladder. All these factors individually or in synergy can result in the malignant transformation of bladder urothelium. Below, we have discussed the evidence for the role of these factors in inducing inflammation in bladder.
Smoking
Smoking remains a leading preventable risk factor for many diseases. Despite a large amount of evidence supporting the risks of cancer due to smoking, roughly 45 million people in the USA remain smokers [42, 43] and many more are regularly exposed to passive smoke. Ever-smokers are considered to have 2.5 times higher risk for bladder cancer than non-smokers [44]. Tobacco has been found to be responsible for about half of all bladder cancer cases [45, 46] and 40% of all bladder cancer deaths [47]. Mechanistically, smoking contributes to bladder cancer both directly and indirectly. Molecules in the tobacco smoke enter the circulation and are eliminated through the urinary pathway. The urothelium is thus exposed to a very high concentration of these toxic chemicals in the urine which may have direct genotoxic effects on it. Indirectly, the carcinogenic effects of smoking are linked to its role in inflammation or diabetes which are risk factors for bladder cancer.
Additionally, smoking may induce systemic inflammation due to its direct effect on the inflammatory mediators. Data suggest a positive association of a higher level of inflammatory biomarkers to smoking parameters (status, burden (pack-years), and intensity (number of cigarettes per day)) [48]. Circulating levels of inflammatory molecules like platelet-activating factor (PAF) and prostaglandin E2 (PGE2) are known to be higher in smokers than in non-smokers [49,50,51]. Bladder endothelial cells display increased PAF accumulation and increased inflammatory cell adherence in response to cigarette smoke extract (CSE). Marentette et al. [52] concluded that exposure to cigarette smoke increases the susceptibility for developing bladder inflammation by inhibiting the activity of PAF-AH and increasing accumulation of endothelial cell PAF. Experimental evidence suggests that carbon black can promote cancer in animal models. Nanosized carbon black generated due to incomplete combustion of tobacco was found to accumulate in exposed tissue myeloid dendritic cells and macrophages. This accumulation in innate immune cells can initiate and sustain inflammation [53]. In this context of the link between smoking and inflammation, it is interesting to see that regular use of anti-inflammatory drugs was associated with a reduced risk (HR 0.87) for BC among smokers, which included both men and women. However, the risk reduction was very strong among non-smokers (HR 0.52) compared to current smokers (HR 0.80) [54].
Diabetes
Several epidemiological studies and systematic reviews have shown positive associations between diabetes mellitus and the risk for bladder cancer (up to 24% higher risk) [7,8,9,10,11]. Prevalence of diabetes has increased substantially over the past few decades, thus making it important to consider the role of diabetes from the prevention aspect. Diabetes is well known to cause bladder dysfunction, and recent studies have also shown a link between diabetes and bladder inflammation [55,56,57,58].
It is considered that toll-like receptor-4 (TLR4) inflammatory pathway is important for some of the biological effects of diabetes on the bladder. An increase in TLR4 expression and signaling along with increased circulating levels of specific endogenous ligands, including high-mobility group box protein 1 (HMGB1), have been observed in diabetes [55]. In STZ-induced diabetes mouse model, increased protein levels of TLR4, MyD88, and HMGB1 were observed in bladders, suggesting TLR4 pathway activation under diabetic conditions. Genetic knockdown of TLR4 or its inhibition using antagonist CLI-095 was found to be protective against diabetic complications in these animals, further supporting this idea. Further analysis showed that HMGB1, which is passively released from necrotic cells or secreted from immune cells, mediates TLR4 activation in diabetes [56]. TLR4 activation during diabetes, sustained by continuously increased levels of its ligands, leads to increased production of ROS and cytokines, which stimulate the proliferation of bladder smooth muscle cells and alter their contractile responses. Bladder cancer cells have aberrant expression of TLR4 [57, 58]; in vitro studies demonstrated that the TLR4 activation protected the cancer cells from cytotoxic T lymphocyte killing [58]. Thus, studies provide the evidence for the link between diabetes and inflammation in bladder cancer.
Obesity
Obesity is also a risk factor for many solid cancers, including bladder, and statistics indicate that there is a gradual increase in obesity rates. Meta-analysis of 15 cohort studies found that pre-obese and obese conditions had a statistically significant, 7 and 10%, increased risk of bladder cancer, respectively. The dose-response meta-analysis showed a 4.2% increase in the risk of BC for each 5 kg/m2 increment of BMI, indicating a linear association between BMI and bladder cancer [13]. While the exact biological mechanisms driving the positive association between obesity and bladder cancer are still not well understood, it could be due to the elevated production of insulin and insulin-like growth factor-I that modify cell proliferation, apoptosis, and angiogenesis [59], thus enhancing tumor growth [60], and leading to bladder cancer [61, 62]. Obesity may also cause chronic low-grade inflammation leading to an alteration of local and systemic levels of cytokines (interleukin-6, C-reactive protein) and adipokines (leptin, adiponectin) [63], which may play a role in bladder carcinogenesis [64, 65].
Targeting Inflammation
Chronic inflammation may not only be the host’s response to bladder cancer development but also actually elicit bladder carcinogenesis. While it is also important that effective cancer control requires an intact immune system, a large amount of evidence suggests that inflammation has a direct effect on cell differentiation, proliferation, and invasion [66]. Local inflammation is elicited by intravesical instillations of Bacillus-Calmette-Guerin (BCG), which prevent the invasion of tumor cells and provide long-term recurrence-free survival in patients. The clinical benefits seen in BCG patients suggest that the immune system itself plays an important role in arresting bladder cancer progression [67]. In recent years, inflammation has taken the center stage in cancer with an increasing interest and initiation of clinical trials towards immune-therapies and vaccine-based preventives.
Differential expression of key enzymes of inflammation is seen during carcinogenesis. Normal urothelial cells predominantly express high levels of cycloxygenase (COX)-1, while bladder cancer cells show COX-2 overexpression [68]. Therefore, the mechanisms that modify the expression of COX isoforms may possibly contribute to the transformation of normal urothelial cells to cancer cells. In bladder cancer cell lines, inhibition of COX activity using ibuprofen showed a reduction in cell viability via induction of proximate cell membrane glycoprotein, p75 neurotrophin receptor (p75NTR) [69]. Similarly, pharmacological inhibition of COX-2 in vivo has shown a reduction in the incidence of preneoplastic and neoplastic lesions in the BBN-pretreated bladder mucosa and reduced serum transforming growth factor-β1 and C-reactive protein (CRP) levels [70], indicating that targeting inflammation at an early stage can prevent cancer initiation. The exact mechanism through which the invasive potential of bladder cancer cells is regulated by the immune system remains unclear; however, recent evidence also points towards macrophages for their role in this process [71]. Further linking the connection of inflammation and chemoresistance and tumor recurrence found that nuclear localization of COX-2 was significantly associated with upregulation of stem cell markers Oct3/4 and CD44v6 in bladder cancer tissues [72] while inflammation mediators such as PGE2 can induce proliferation of cancer stem cells (CSCs) [73]. In another mouse study, pretreatment with celecoxib leads to a decrease in PGE2 and PGE2 induced CK14-CSC proliferation with an increase in tumor regression by cisplatin/gemcitabine [74]. These studies clearly suggest that inflammation has its role at multiple stages of bladder cancer as well as provide evidence that inhibition of inflammatory pathways using safer anti-inflammatory agents can have significant benefits by suppressing tumor-promoting mediators at various levels of carcinogenesis. The existence of indisputable evidence from a large number of preclinical and clinical studies indicates the protective role of anti-inflammatory agents [15,16,17,18,19]. With the recent approval of aspirin for low-risk colon adenoma patients, it is highly recommended that trials should be initiated for prevention of BC recurrence and progression.
BC Chemoprevention Using Anti-Inflammatory Agents
As discussed above, the role of inflammation in urothelial carcinogenesis is very clear and is a promising target for bladder cancer. Both human and animal model urothelial tumors are reported to show COX-2 overexpression, a key enzyme in inflammation, that was directly associated with high tumor grade and stage and is also considered as an independent predictor of disease progression and survival in humans [75].
Numerous preclinical studies using well-recognized animal models of BC support the hypothesis that suppressing inflammatory pathway may have similar preventive effects in BC [76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93] (Table 1). BBN-induced rat model of bladder cancer has been a widely used animal model for testing agents against BC in chemopreventive studies. Alternatively, we have developed a transgenic mouse model (UPII-SV40T) for chemoprevention studies in which urothelial tumorigenesis is driven by uroplakin II-driven SV40T expression [85, 90, 94, 95, 98] (Fig. 2). Studies with both COX-2 specific and non-specific agents have all demonstrated the chemopreventive efficacy of anti-inflammatory agents. These agents not only suppressed tumor growth but were also found to inhibit tumor progression, invasion, and chemoresistance. These findings provide strong support for the use of anti-inflammatory agents at all stages of cancer, starting from primary prevention to tertiary prevention. Evaluation of chemopreventive efficacy of several anti-inflammatory agents in multiple animal models providing a strong case in favor of these agents. Klein et al. [100] found that COX-2 inhibitors were able to prevent bladder tumorigenesis throughout premalignant hyperproliferation and further transformation. Likewise, celecoxib, a highly COX-2 specific agent, was observed to effectively inhibit not just development and tumor growth, but also enhanced survival in a murine model of nitrosamine-induced bladder cancer [80]. Another widely used non-steroidal anti-inflammatory drug (NSAID), naproxen, was shown to prevent bladder cancer in rat models [86, 88]. In view of the gastrointestinal (GI) toxicity and cardiovascular (CV) risk associated with certain anti-inflammatory agents, we have investigated other safer NSAIDs as chemopreventive agents against BC with similar results [85, 90]. Using a SV40T-driven muscle invasive bladder cancer mouse model, we were able to demonstrate that administration of nitric oxide-releasing naproxen (NO-naproxen), a GI safe prodrug of naproxen, at an early stage of BC was effective in suppressing bladder cancer in this transgenic mouse model [90]. Lubet et al. [88] have also reported similar results with this agent in BBN-induced rat model. Considering the CV risk associated with COX-2 specific agents, we have also explored other methods and agents for developing safer chemopreventive agents. Data suggests that targeting dual COX-LOX pathways using agents such as licofelone will protect against these side effects. Therefore, we have also tested this agent and found that oral administration of licofelone was able to suppress tumor growth as well as prevent invasion of the tumors into the muscle [85] (Fig. 2). These studies using multiple models of bladder cancer clearly indicate the potential of anti-inflammatory agents for primary and secondary prevention of bladder cancer in high risk and early stage bladder cancer patients, respectively.
Stepwise progression of TCC in mouse model (UPII-SV40T). Data from multiple studies using well-established preclinical animal models indicate strong chemopreventive effect of several agents known to inhibit (red arrow) or modulate (green arrow) specific target proteins such as COX-2, ODC, mTOR, or TP53
Studies have also shown that these agents can have significant benefits even in the late-stage cancers in terms of tumor sensitization to standard therapies, increasing survival, etc. In canine model of invasive BC, combining Cox inhibitor piroxicam (0.3 mg/kg) to standard therapeutic cisplatin leads to tumor size shrinkage, a favorable survival benefit compared to the group with cisplatin alone [93]. Similarly, in an orthotopic murine model of urothelial carcinoma, celecoxib was shown to improve the effectiveness of intravesical BCG, the most commonly used therapy to prevent tumor recurrence. Combining celecoxib with BCG was found to increase tumor infiltration of CD4+ T cells with a significant reduction of tumor burden in a dose-dependent manner compared with intravesical BCG alone and with untreated controls [101]. Clinical trials in humans have also confirmed similar benefits of these anti-inflammatory agents. During the 6-year follow-up in NMIBC treated with celecoxib or MMC, celecoxib treatment led to longer disease-free survival, fewer recurrences, and adverse events [102]. While in yet another trial, celecoxib (200 mg twice daily) was able to prevent bladder cancer recurrence following TURBT, supporting a beneficial effect of celecoxib in the treatment of NMIBC [103]. CSCs or tumor initiation cells that have accumulated a set of genetic changes that can drive tumorigenesis are widely considered to be the source of tumor heterogeneity which drives drug resistance and tumor recurrence [104]. Since it is not known how many genetic events must be counteracted in order to achieve tumor eradication, preventing the evolution of heterogeneity by targeting these subpopulations may be a feasible alternative. In the orthotopic mouse model, it was found that tumor response to cisplatin plus gemcitabine was much greater when combined with celecoxib compared to the standard therapy alone. Further investigation showed that the standard therapy led to a release of pro-inflammatory molecule PGE2 that induced CSC proliferation resulting in tumor relapse and resistance to standard therapy [73]. Therefore, suppressing the PGE2 formation by including celecoxib to the standard therapy inhibited this process leading to the elimination of CSCs that drive tumor recurrence and resistance [73]. Thus, data support the use of anti-inflammatory agents as an adjuvant to standard therapies for preventing tumor heterogeneity and drug resistance and tumor relapse that can have a significant effect on patient survival. These studies warrant further investigation of safer NSAID combination with standard therapies in preclinical and clinical settings for secondary and tertiary prevention of BC and to improve the response and benefits of currently available therapies.
Inflammation-targeting agents are being investigated in clinical trials. A randomized phase IIb/III trial for studying celecoxib in preventing disease recurrence in patients who have bladder cancer has been completed recently [NCT00006124, NCT02343614] and is under investigation for MIBC [NCT02885974]. A phase 4 clinical trial is underway to evaluate the perioperative aspirin continuation vs discontinuation in BC patients [NCT02350543]. Currently, there is an ongoing randomized, phase III, multicenter, double-blind, placebo-controlled clinical trial called BOXIT (Bladder COX-2 Inhibition Trial) to determine if the addition of the oral COX-2 inhibitor, celecoxib, to standard therapy is more effective in terms of disease recurrence at 3 years compared to standard therapy alone for the treatment of NMIBC in intermediate and high-risk patients [105]. Although mounting data are in favor of the chemopreventive effect of anti-inflammatory agents against bladder cancer, it is also important to consider the side effects on renal function, particularly for the primary and secondary settings. Since it is known that glomerular function is dependent on PGE2, high doses or strong COX-2 specific agents may have negative effects on the kidneys. Interesting research is also underway to develop the renal safe anti-inflammatory agents (e.g., celecoxib-polylactic acid or celecoxib + misoprostol) [106, 107].
While anti-inflammatory agents have a strong case many other promising compounds like DFMO, metformin, etc. [77, 78, 87, 94,95,96,97, 99], and several natural agents [77, 78, 82, 108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123] (Table 2) have also been tested in preclinical animal models that need further validation in clinical settings. Many of these natural agents are not only shown to have anti-inflammatory properties but also known for other antioxidant, antiproliferative, immunmodulating properties. Several of these agents, such as diclofenac [NCT01542567], celecoxib [NCT00006124], rapamycin [NCT03298958], erlotinib, and green tea extract [NCT00088946, NCT00666562], are being investigated at various phases of clinical trials for prevention of BC. We hope that more trials will be initiated and results from ongoing trial will lead to approval of promising agents for primary and secondary prevention of BC.
Conclusion
There are several favorable reasons why BC is a preventable disease. Primary prevention can be achieved as the high-risk factors such as smoking are modifiable and other risk cohorts can be identified for screening. Secondly, the majority of bladder tumors are non-muscle invasive that are manageable when diagnosed; thus, secondary prevention can prevent the disease progression. Thirdly, like many cancers, even BC takes several years after initiation to be transformed into malignant form; thus, there is ample of time for identification, screening, and prevention. Finally, data indicates that combining preventives with standard therapies can have tumor response and survival benefits. Hence, appropriate measures can be taken to prevent recurrence and progression to an advanced stage.
References
American Cancer Society. Global cancer facts & figures. 3rd ed. Atlanta: American Cancer Society; 2015.
Antoni S, Ferlay J, Soerjomataram I, et al. Bladder cancer incidence and mortality: a global overview and recent trends. Eur Urol. 2017;71(1):96–108.
Hemelt M, Yamamoto H, Cheng KK, et al. The effect of smoking on the male excess of bladder cancer: a meta-analysis and geographical analyses. Int J Cancer. 2009;124:412–9.
Czene K, Lichtenstein P, Hemminki K. Environmental and heritable causes of cancer among 9.6 million individuals in the Swedish family-cancer database. Int J Cancer. 2002;99:260–6.
van Osch FHM, Sylvia HJ, et al. Quantified relations between exposure to tobacco smoking and bladder cancer risk: a meta-analysis of 89 observational studies. Int J Epidemiol. 2016;45(3):857–70.
Pitard A, Brennan P, Clavel J, et al. Cigar, pipe, and cigarette smoking and bladder cancer risk in European men. Cancer Causes Control. 2001;12:551–6.
Fang H, Yao B, Yan Y, et al. Diabetes mellitus increases the risk of bladder cancer: an updated meta-analysis of observational studies. Diabetes Technol Ther. 2013;15(11):914–22.
Zhu Z, Wang X, Shen Z, et al. Risk of bladder cancer in patients with diabetes mellitus: an updated meta-analysis of 36 observational studies. BMC Cancer. 2013;13:310.
Larsson SC, Orsini N, Brismar K, et al. Diabetes mellitus and risk of bladder cancer: a meta-analysis. Diabetologia. 2006;49:2819–23.
Zhu Z, Zhang X, Shen Z, et al. Diabetes mellitus and risk of bladder cancer: a meta-analysis of cohort studies. Baradaran HR, ed. PLoS One. 2013;8(2):e56662.
Xu X, Wu J, Mao Y, et al. Diabetes mellitus and risk of bladder cancer: a meta-analysis of cohort studies. PLoS One. 2013;8(3):e58079.
Zhao L, Tian X, Duan X, et al. Association of body mass index with bladder cancer risk: a dose-response meta-analysis of prospective cohort studies. Oncotarget. 2017;8(20):33990–4000.
Sun JW, Zhao LG, Yang Y, et al. Obesity and risk of bladder cancer: a dose-response meta-analysis of 15 cohort studies. PLoS One. 2015;10(3):e0119313.
Qin Q, Xu X, Wang X, et al. Obesity and risk of bladder cancer: a meta-analysis of cohort studies. Asian Pac J Cancer Prev. 2013;14(5):3117–21.
Zhang H, Jiang D, Li X. Use of nonsteroidal anti-inflammatory drugs and bladder cancer risk: a meta-analysis of epidemiologic studies. PLoS One. 2013;8(7):e70008.
Blumentals WA, et al. Analgesic therapy and the prevention of bladder cancer. Urol Oncol. 2004;22(1):11–5.
Shih C, Hotaling JM, Wright JL, et al. Long-term NSAID use and incident urothelial cell carcinoma in the VITamins and Lifestyle study. Urol Oncol. 2013;31(8):10.
Baris D, Karagas MR, Koutros S, et al. Nonsteroidal anti-inflammatory drugs and other analgesic use and bladder cancer in northern New England. Int J Cancer. 2013;132:162–73.
Fortuny J, et al. Use of analgesics and nonsteroidal anti-inflammatory drugs, genetic predisposition, and bladder cancer risk in Spain. Cancer Epidemiol Biomark Prev. 2006;15(9):1696–702.
Ng M, Freeman MK, Fleming TD, et al. Smoking prevalence and cigarette consumption in 187 countries, 1980–2012. JAMA. 2014;311:183–92.
Vineis P, Wild CP. Global cancer patterns: causes and prevention. Lancet. 2014;383:549–57.
Salem HK, Mahfouz S. Changing patterns (age, incidence, and pathologic types) of schistosoma-associated bladder cancer in Egypt in the past decade. Urology. 2012;79:379–83.
Felix AS, Soliman AS, Khaled H, et al. The changing patterns of bladder cancer in Egypt over the past 26 years. Cancer Causes Control. 2008;19:421–9.
Gouda I, Mokhtar N, Bilal D, et al. Bilharziasis and bladder cancer: a time trend analysis of 9843 patients. J Egypt Natl Canc Inst. 2007;19:158–62.
Clark PE, Agarwal N, Biagioli MC, et al. Bladder cancer. J Natl Compr Cancer Netw. 2013;11:446–75.
Yeung C, Dinh T, Lee J. The health economics of bladder cancer: an updated review of the published literature. PharmacoEconomics. 2014;32(11):1093–104.
Stenzl A, Cowan NC, DeSantis M, et al. Treatment of muscle-invasive and metastatic bladder cancer: update of the EAU guidelines. Eur Urol. 2011;59(6):1009–18.
Nepple KG, O’Donnell MA. The optimal management of T1 high-grade bladder cancer. Can Urol Assoc J. 2009;3(6 Suppl 4):S188–92.
Nieder AM, Brausi M, Lamm D, et al. Management of stage T1 tumors of the bladder: International Consensus Panel. Urology. 2005;66(6 Suppl 1):108–25.
Babjuk M, Burger M, Zigeuner R, et al. EAU guidelines on nonmuscle-invasive urothelial carcinoma of the bladder: update 2013. Eur Urol. 2013;64(4):639–53.
Van Rhijn BW, Burger M, Lotan Y, et al. Recurrence and progression of disease in nonmuscle- invasive bladder cancer: from epidemiology to treatment strategy. Eur Urol. 2009;56(3):430–42.
Stenzl A, Hennenlotter J, Schilling D. Can we still afford bladder cancer? Curr Opin Urol. 2008;18(5):488–92.
Kelloff GJ, Sigman CC, Johnson KM, et al. Perspectives on surrogate end points in the development of drugs that reduce the risk of cancer. Cancer Epidemiol Biomark Prev. 2000;9:127–37.
Oddens JR, Sylvester RJ, Brausi MA, et al. The effect of age on the efficacy of maintenance bacillus Calmette-Guérin relative to maintenance epirubicin in patients with stage ta T1 urothelial bladder cancer: results from EORTC genito-urinary group study 30911. Eur Urol. 2014;66(4):694–701.
Koya MP, Simon MA, Soloway MS. Complications of intravesical therapy for urothelial cancer of the bladder. J Urol. 2006;175(6):2004–10.
Colombel M, Saint F, Chopin D, Malavaud B, Nicolas L, Rischmann P. The effect of ofloxacin on bacillus calmette-guerin induced toxicity in patients with superficial bladder cancer: results of a randomized, prospective, double-blind, placebo controlled, multicenter study. J Urol. 2006;176(3):935–9.
National Center for Chronic Disease Prevention and Health Promotion (US) Office on Smoking and Health. The health consequences of smoking—50 years of progress: a report of the surgeon general. Atlanta: Centers for Disease Control and Prevention (US); 2014. 13, Patterns of Tobacco Use Among U.S. Youth, Young Adults, and Adults
Parkin DM. The global burden of urinary bladder cancer. Scand J Urol Nephrol Suppl. 2008;218:12–20.
Steinmann P, Keiser J, Bos R, Tanner M, Utzinger J. Schistosomiasis and water resources development: systematic review, metaanalysis, and estimates of people at risk. Lancet Infect Dis. 2006;6:411–25.
Gui-Zhong L, Li-Bo M. Bladder cancer in individuals with spinal cord injuries: a meta-analysis. Spinal Cord. 2017;55(4):341–5.
Austin JC, Elliott S, Cooper CS. Patients with spina bifida and bladder cancer: atypical presentation, advanced stage and poor survival. J Urol. 2007;178(3 Pt 1):798–801.
Kandel D, Schaffran C, MC H, et al. Age-related differences in cigarette smoking among whites and African-Americans: evidence for the crossover hypothesis. Drug Alcohol Depend. 2011;118(2–3):280–7.
King BA, Dube SR, Tynan MA. Current tobacco use among adults in the United States: findings from the National Adult Tobacco Survey. Am J Public Health. 2012;102(11):e93–e100.
Cumberbatch MG, Rota M, Catto JW, et al. The role of tobacco smoke in bladder and kidney carcinogenesis: a comparison of exposures and meta-analysis of incidence and mortality risks. Eur Urol. 2016;70:458–66.
Freedman ND, Silverman DT, Hollenbeck AR, et al. Association between smoking and risk of bladder cancer among men and women. JAMA. 2011;306:737–45.
Agudo A, Bonet C, Travier N, et al. Impact of cigarette smoking on cancer risk in the European prospective investigation into cancer and nutrition study. J Clin Oncol. 2012;30:4550–7.
Park S, Jee SH, Shin HR, et al. Attributable fraction of tobacco smoking on cancer using population-based nationwide cancer incidence and mortality data in Korea. BMC Cancer. 2014;14:406.
Kianoush S, Yakoob MY, Al-Rifai M, et al. Associations of cigarette smoking with subclinical inflammation and atherosclerosis: ELSA-Brasil (The Brazilian Longitudinal Study of Adult Health). J Am Heart Assoc. 2017; 6(6).
Kispert SE, Marentette J, Campian EC, et al. Cigarette smoke-induced urothelial cell damage: potential role of platelet-activating factor. Physiol Rep. 2017;5(5):e13177.
Imaizumi T, Satoh K, Yoshida H, Kawamura Y, et al. Effect of cigarette smoking on the levels of platelet-activating factor-like lipid(s) in plasma lipoproteins. Atherosclerosis. 1991;87(1):47–55.
Narahara H, Johnston JM. Smoking and preterm labor: effect of a cigarette smoke extract on the secretion of platelet-activating factor—acetylhydrolase by human decidual macrophages. Am J Obstet Gynecol. 1993;169(5):1321–6.
Marentette J, Kolar G, McHowat J. Increased susceptibility to bladder inflammation in smokers: targeting the PAF–PAF receptor interaction to manage inflammatory cell recruitment. Physiol Rep. 2015;3(12):e12641.
Kheradmand F, You R, HeeGu B, et al. Cigarette smoke and DNA cleavage promote lung inflammation and emphysema. Trans Am Clin Climatol Assoc. 2017;128:222–33.
Daugherty SE, Pfeiffer RM, Sigurdson AJ, et al. Nonsteroidal antiinflammatory drugs and bladder cancer: a pooled analysis. Am J Epidemiol. 2011;173(7):721–30.
Dasu MR, Devaraj S, Park S, et al. Increased toll-like receptor (TLR) activation and TLR ligands in recently diagnosed type 2 diabetic subjects. Diabetes Care. 2010;33:861–8.
Szasz T, Wenceslau CF, Burgess B, et al. Toll-like receptor 4 activation contributes to diabetic bladder dysfunction in a murine model of type 1 diabetes. Diabetes. 2016;65(12):3754–64.
Le PT, Pearce MM, Zhang SB, et al. IL22 regulates human urothelial cell sensory and innate functions through modulation of the acetylcholine response, immunoregulatory cytokines and antimicrobial peptides: assessment of an in vitro model. PLoS One. 2014;9:e111375.
Wang YH, Cao YW, Yang XC, et al. Effect of TLR4 and B7-H1 on immune escape of urothelial bladder cancer and its clinical significance Asian Pac. J Cancer Prev. 2013;15:1321–6.
Iwamura M, Ishibe M, Sluss PM, et al. Characterization of insulin-like growth factor I binding sites in human bladder cancer cell lines. Urol Res. 1993;21:27–32.
Bianchini F, Kaaks R, Vainio H. Overweight, obesity, and cancer risk. Lancet Oncol. 2002;3:565–74.
Zhao H, Grossman HB, Spitz MR, et al. Plasma levels of insulin-like growth factor-1 and binding protein-3, and their association with bladder cancer risk. J Urol. 2003;169:714–7.
Probst-Hensch NM, Wang H, Goh VHH, et al. Determinants of circulating insulin-like growth factor I and insulin-like growth factor binding protein 3 concentrations in a cohort of Singapore men and women. Cancer Epidemiol Biomarkers Prev. 2003;12:739.
Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer. 2004;4:579–91.
Hilmy M, Bartlett JMS, Underwood MA, et al. The relationship between the systemic inflammatory response and survival in patients with transitional cell carcinoma of the urinary bladder. Br J Cancer. 2005;92:625–7.
Andrews B, Shariat SF, Kim JH, et al. Preoperative plasma levels of interleukin-6 and its soluble receptor predict disease recurrence and survival of patients with bladder cancer. J Urol. 2002;167:1475–81.
Balkwill F, Mantovani A. Cancer and inflammation: implications for pharmacology and therapeutics. Clin Pharmacol Ther. 2010;87(4):401–6.
Kawai K, Miyazaki J, Joraku A, et al. Bacillus Calmette-Guerin (BCG) immunotherapy for bladder cancer: current understanding and perspectives on engineered BCG vaccine. Cancer Sci. 2013;104(1):22–7.
Boström PJ, Aaltonen V, Söderström KO, et al. Expression of cyclooxygenase-1 and -2 in urinary bladder carcinomas in vivo and in vitro and prostaglandin E2 synthesis in cultured bladder cancer cells. Pathology. 2001;33(4):469–74.
Khwaja F, Allen J, Lynch J, et al. Ibuprofen inhibits survival of bladder cancer cells by induced expression of the p75NTR tumor suppressor protein. Cancer Res. 2004;64(17):6207–13.
Parada B, Sereno J, Reis F, et al. Anti-inflammatory, anti-proliferative and antioxidant profiles of selective cyclooxygenase-2 inhibition as chemoprevention for rat bladder carcinogenesis. Cancer Biol Ther. 2009;8(17):1615–22.
Ajili F, Kourda N, Darouiche A, et al. Prognostic value of tumor-associated macrophages count in human non-muscle-invasive bladder cancer treated by BCG immunotherapy. Ultrastruct Pathol. 2013;37(1):56–61.
Thanan R, Murata M, Ma N, et al. Nuclear localization of COX-2 in relation to the expression of stemness markers in urinary bladder cancer. Mediat Inflamm. 2012;2012:165879.
Kurtova AV, Xiao J, Mo Q, et al. Blocking PGE2-induced tumour repopulation abrogates bladder cancer chemoresistance. Nature. 2015;517(7533):209–13.
Van der Horst G, Bos L, van der Pluijm G. Epithelial plasticity, cancer stem cells, and the tumor-supportive stroma in bladder carcinoma. Mol Cancer Res. 2012;10:995–1009.
Shariat S, Kim J, Ayala G, et al. Cyclooxygenase-2 is highly expressed in carcinoma in situ and T1 transitional cell carcinoma of the bladder. J Urol. 2003;169:938–42.
Rao KV, Detrisac CJ, Steele VE, et al. Differential activity of aspirin, ketoprofen and sulindac as cancer chemopreventive agents in the mouse urinary bladder. Carcinogenesis. 1996;17(7):1435–8.
El-Ashmawy NE, Khedr EG, El-Bahrawy HA, Al-Tantawy SM. Chemopreventive effect of omega-3 polyunsaturated fatty acids and atorvastatin in rats with bladder cancer. Tumour Biol. 2017;39(2):1010428317692254.
Moon RC, Kelloff GJ, Detrisac CJ, et al. Chemoprevention of OH-BBN-induced bladder cancer in mice by oltipraz, alone and in combination with 4-HPR and DFMO. Anticancer Res. 1994;14(1A):5–11.
Parada B, Reis F, Pinto A, et al. Chemopreventive efficacy of atorvastatin against nitrosamine-induced rat bladder cancer: antioxidant, anti-proliferative and anti-inflammatory properties. Int J Mol Sci. 2012;13(7):8482–99.
Grubbs CJ, Lubet RA, Koki AT, et al. Celecoxib inhibits N-butyl-N-(4-hydroxybutyl)-nitrosamine-induced urinary bladder cancers in male B6D2F1 mice and female Fischer-344 rats. Cancer Res. 2000;60(20):5599–602.
Sereno J, Parada B, Reis F, et al. Preventive but not curative efficacy of celecoxib on bladder carcinogenesis in a rat model. Mediat Inflamm. 2010;2010:380937.
Bhattacharya A, Li Y, Shi Y, Zhang Y. Enhanced inhibition of urinary bladder cancer growth and muscle invasion by allyl isothiocyanate and celecoxib in combination. Carcinogenesis. 2013;34(11):2593–9.
Grubbs CJ, Juliana MM, Eto I, et al. Chemoprevention by indomethacin of N-butyl-N-(4-hydroxybutyl)-nitrosamine-induced urinary bladder tumors. Anticancer Res. 1993;13(1):33–6.
Lubet RA, Huebner K, Fong LY, et al. 4-Hydroxybutyl(butyl)nitrosamine-induced urinary bladder cancers in mice: characterization of FHIT and survivin expression and chemopreventive effects of indomethacin. Carcinogenesis. 2005;26(3):571–8.
Madka V, Mohammed A, Li Q, et al. Chemoprevention of urothelial cell carcinoma growth and invasion by the dual COX-LOX inhibitor licofelone in UPII-SV40T transgenic mice. Cancer Prev Res (Phila). 2014;7(7):708–16.
Steele VE, Rao CV, Zhang Y, et al. Chemopreventive efficacy of naproxen and no-naproxen in rodent models of colon, urinary bladder, and mammary cancers. Cancer Prev Res (Phila). 2009;2(11):951–6.
Nicastro HL, Grubbs CJ, Margaret Juliana M, et al. Preventive effects of NSAIDs, NO-NSAIDs, and NSAIDs plus difluoromethylornithine in a chemically induced urinary bladder cancer model. Cancer Prev Res (Phila). 2014;7(2):246–54.
Lubet RA, Scheiman JM, Bode A, et al. Prevention of chemically-induced urinary bladder cancers by naproxen: protocols to reduce gastric toxicity in humans do not alter preventive efficacy. Cancer Prev Res (Phila). 2015;8(4):296–302.
Kim M-S, Kim J-E, Lim DY, et al. Naproxen induces cell cycle arrest and apoptosis in human urinary bladder cancer cell lines and chemically induced cancers by targeting PI3-K. Cancer Prev Res (Phila). 2014;7(2):236–45.
Madka V, Mohammed A, Li Q, et al. Nitric oxide-releasing naproxen prevents muscle invasive bladder cancer. [abstract]. In: Proceedings of the 107th Annual Meeting of the American Association for Cancer Research; 2016 Apr 16–20; New Orleans, LA. Philadelphia (PA): AACR; Cancer Res 2016;76(14 Suppl):Abstract nr 5241.
Moon RC, Kelloff GJ, Detrisac CJ, et al. Chemoprevention of OH-BBN-induced bladder cancer in mice by piroxicam. Carcinogenesis. 1993;14(7):1487–9.
Henry CJ, McCaw DL, Turnquist SE, et al. Clinical evaluation of mitoxantrone and piroxicam in a canine model of human invasive urinary bladder carcinoma. Clin Cancer Res. 2003;9(2):906–11.
Mohammed SI, Craig BA, Mutsaers AJ, et al. Effects of the cyclooxygenase inhibitor, piroxicam, in combination with chemotherapy on tumor response, apoptosis, and angiogenesis in a canine model of human invasive urinary bladder cancer. Mol Cancer Ther. 2003;2(2):183–8.
Madka V, Zhang Y, Li Q, et al. p53-stabilizing agent CP-31398 prevents growth and invasion of urothelial cancer of the bladder in transgenic UPII-SV40T mice. Neoplasia. 2013;15(8):966–74.
Madka V, Mohammed A, Li Q, et al. TP53 modulating agent, CP-31398 enhances antitumor effects of ODC inhibitor in mouse model of urinary bladder transitional cell carcinoma. Am J Cancer Res. 2015;5(10):3030–41.
Salim EI, Wanibuchi H, Morimura K, et al. Inhibitory effects of 1,3-diaminopropane, an ornithine decarboxylase inhibitor, on rat two-stage urinary bladder carcinogenesis initiated by N-butyl-N-(4-hydroxybutyl)nitrosamine. Carcinogenesis. 2000;21(2):195–203.
Liu Z, Yokoyama NN, Blair CA, et al. High sensitivity of an ha-RAS transgenic model of superficial bladder cancer to metformin is associated with 240-fold higher drug concentration in urine than serum. Mol Cancer Ther. 2016;15(3):430–8.
Madka V, Mohammed A, Li Q, et al. Targeting mTOR and p53 signaling inhibits muscle invasive bladder cancer in vivo. Cancer Prev Res (Phila). 2016;9(1):53–62.
George SK, Tovar-Sepulveda V, Shen SS, et al. Chemoprevention of BBN-induced bladder carcinogenesis by the selective estrogen receptor modulator tamoxifen. Transl Oncol. 2013;6(3):244–55.
Klein R, van Pelt C, Sabichi A, et al. Transitional cell hyperplasia and carcinomas in urinary bladders of transgenic mice with keratin 5 promoter-driven cyclooxygenase-2 overexpression. Cancer Res. 2005;65:1808–13.
Dovedi S, Kirby J, Davies B, et al. Celecoxib has potent antitumour effects as a single agent and in combination with BCG immunotherapy in a model of urothelial cell carcinoma. Eur Urol. 2008;54:621–30.
Pagliarulo V, Ancona P, Martines I, et al. Celecoxib for the prevention of nonmuscle invasive bladder cancer: results from a matched control study. Ther Adv Urol. 2015;7(6):303–11.
Sabichi A, Lee J, Grossman H, et al. A randomized controlled trial of celecoxib to prevent recurrence of non-muscle invasive bladder cancer. Cancer Prev Res. 2011;4:1580–9.
Burrell RA, McGranahan N, Bartek J, et al. The causes and consequences of genetic heterogeneity in cancer evolution. Nature. 2013;501:338–45.
Kelly JD, Maynard L, Mostafid A, et al. Celecoxib for the treatment of non-muscle invasive bladder cancer (NMIBC): results of the randomised BOXIT trial (CRUK/07/004). BJU Int. 2015;115(Suppl 7):11. #8
Harirforoosh S, West KO, Murrell DE, et al. Assessment of celecoxib poly(lactic-co-glycolic) acid nanoformulation on drug pharmacodynamics and pharmacokinetics in rats. Eur Rev Med Pharmacol Sci. 2016;20(22):4818–29.
Cooper DL, Murrell DE, Conder CM, et al. Exacerbation of celecoxib-induced renal injury by concomitant administration of misoprostol in rats. PLoS One. 2014;9(2):e89087.
Sugie S, Vinh PQ, Rahman KM, et al. Suppressive effect of 1,4-phenylene diisothiocyanate on N-butyl-N-(4-hydroxybutyl)nitrosamine-induced urinary bladder carcinogenesis in male ICR mice. Int J Cancer. 2005;117(4):524–30.
Becci PJ, Thompson HJ, Grubbs CJ, et al. Inhibitory effect of 13-cis-retinoic acid on urinary bladder carcinogenesis induced in C57BL/6 mice by N-butyl-N-(4-hydroxybutyl)-nitrosamine. Cancer Res. 1978;38(12):4463–6.
Miyazawa K, Miyamoto S, Suzuki R, et al. Dietary beta-cryptoxanthin inhibits N-butyl-N-(4-hydroxybutyl) nitrosamine-induced urinary bladder carcinogenesis in male ICR mice. Oncol Rep. 2007;17(2):297–304.
Masuda C, Wanibuchi H, Sekine K, et al. Chemopreventive effects of bovine lactoferrin on N-butyl-N-(4-hydroxybutyl)nitrosamine-induced rat bladder carcinogenesis. Jpn J Cancer Res. 2000;91(6):582–8.
Parada B, Reis F, Cerejo R, et al. Omega-3 fatty acids inhibit tumor growth in a rat model of bladder cancer. BioMed Res Int. 2013;2013:368178, 11 pages.
Prabhu B, Balakrishnan D, Sundaresan S. Antiproliferative and anti-inflammatory properties of diindolylmethane and lupeol against N-butyl-N-(4-hydroxybutyl) nitrosamine induced bladder carcinogenesis in experimental rats. Hum ExpToxicol. 2016;35(6):685–92.
Zi X, Simoneau AR, Flavokawain A. A novel chalcone from kava extract, induces apoptosis in bladder cancer cells by involvement of Bax protein-dependent and mitochondria-dependent apoptotic pathway and suppresses tumor growth in mice. Cancer Res. 2005;65(8):3479–86.
Liu Z, Xu X, Li X, et al. Kava chalcone, flavokawain A, inhibits urothelial tumorigenesis in the UPII-SV40T transgenic mouse model. Cancer Prev Res (Phila). 2013;6(12):1365–75.
Yang M, Tanaka T, Hirose Y, et al. Chemopreventive effects of diosmin and hesperidin on N-butyl-N-(4-hydroxybutyl)nitrosamine-induced urinary-bladder carcinogenesis in male ICR mice. Int J Cancer. 1997;73(5):719–24.
Dornelas CA, Fechine-Jamacaru FV, Albuquerque IL, et al. Chemoprevention with green propolis green propolis extracted in L-lysine versus carcinogenesis promotion with L-lysine in N-butyl-N-[4-hydroxybutyl] nitrosamine (BBN) induced rat bladder cancer. Acta Cir Bras. 2012;27(2):185–92.
Wang YW, Chuang JJ, Chang TY, et al. Antiangiogenesis as the novel mechanism for justicidin A in the anticancer effect on human bladder cancer. Anti-Cancer Drugs. 2015;26(4):428–36.
Yuan X, Li T, Xiao E, et al. Licochalcone B inhibits growth of bladder cancer cells by arresting cell cycle progression and inducing apoptosis. Food Chem Toxicol. 2014;65:242–51.
Abbaoui B, Telu KH, Lucas CR, et al. The impact of cruciferous vegetable isothiocyanates on histone acetylation and histone phosphorylation in bladder cancer. J Proteome. 2017;156:94–103.
Tyagi A, Raina K, Singh RP, et al. Chemopreventive effects of silymarin and silibinin on N-butyl-N-(4-hydroxybutyl) nitrosamine induced urinary bladder carcinogenesis in male ICR mice. Mol Cancer Ther. 2007;6(12 Pt 1):3248–55.
Singh RP, Tyagi A, Sharma G, Mohan S, Agarwal R. Oral silibinin inhibits in vivo human bladder tumor xenograft growth involving down-regulation of survivin. Clin Cancer Res. 2008;14(1):300–8.
Vinh PQ, Sugie S, Tanaka T, et al. Chemopreventive effects of a flavonoid antioxidant silymarin on N-butyl-N-(4-hydroxybutyl)nitrosamine-induced urinary bladder carcinogenesis in male ICR mice. Jpn J Cancer Res. 2002;93(1):42–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Cancer Chemoprevention
Rights and permissions
About this article
Cite this article
Madka, V., Asch, A.S. & Rao, C.V. Targeting Inflammation for Bladder Cancer Chemoprevention. Curr Pharmacol Rep 3, 447–457 (2017). https://doi.org/10.1007/s40495-017-0116-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40495-017-0116-z