Abstract
Tension-type headache (TTH) is the most prevalent headache type in all age groups worldwide, including patients with advanced age. Because of its high prevalence and possible association with medical and psychiatric co-morbidities, TTH has a major socioeconomic impact. The lifetime prevalence of TTH ranges between 30 and 78 %, and the 1-year prevalence in individuals over the age of 55 years is 35.8 % (27.8 % in men, 42.4 % in women). Since the prevalence of secondary headache disorders increases in the elderly, the initial evaluation of this group of patients with a new-onset headache or a change in a pre-existing headache pattern should be directed towards their exclusion. This article reviews the diagnostic and treatment dilemmas encountered in elderly patients with tension-type headaches, highlighting both pharmacological and non-pharmacological interventions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Tension-type headache is the most common primary headache subtype in adults, including the elderly population. |
The prevalence of secondary headaches increases with age, so careful investigation is required to exclude them. |
The pharmacological management of primary headaches is divided into acute and prophylactic treatments. Multiple medical co-morbidities, polypharmacy and medication intolerance may limit those options, making alternative approaches, such as biofeedback and relaxation techniques, of extreme importance. |
1 Introduction
Headache is a common complaint in the elderly, with tension-type headache (TTH) being the most common subtype [1]. Despite the decline in the prevalence of TTH to less than 5 per 1,000 person-years at 55–64 years of age, many elderly patients with new-onset headache have TTH. As the elderly population continues to grow, it is imperative for clinicians to be able to manage their headaches. Special considerations in this population include the higher prevalence of secondary headache disorders, multiple medical co-morbidities and polypharmacy. Since the incidence of secondary headache disorders increases with advanced age, it behoves the treating clinician to search for ‘red flags’ or worrisome features in the history and on examination, to help identify or exclude secondary disorders. Giant cell arteritis, intracranial neoplasm and intracranial haemorrhage are among the most concerning ones. Once a primary diagnosis is established, a combination of pharmacological and non-pharmacological approaches may be employed in the management of TTH in the elderly.
2 Diagnostic Criteria and Clinical Features
TTH is divided into three subtypes based on attack frequency (Table 1): an infrequent episodic form, in which headaches occur on 1 day or less per month; a frequent episodic form, in which headaches occur on between 1 and 14 days per month for at least 3 consecutive months; and a chronic form, with 15 or more headache days per month. A headache diary is often helpful to determine the predominant subtype, facilitating diagnosis and maximizing treatment. All three subtypes are further subdivided on the basis of the presence or absence of pericranial tenderness [1].
The most recent International Classification of Headache Disorders (ICHD-3 beta) definition of TTH requires at least 10 episodes of headache lasting from 30 min to 7 days. At least two of the following should be present: bilateral location, pressing or tightening (non-pulsating) quality, mild or moderate intensity, and not aggravated by routine physical activity [2]. An appropriate history and physical examination, including neurological examination, should not suggest any other disorder.
Photophobia and phonophobia cannot both be present. Nausea and vomiting should be absent in both infrequent and frequent episodic tension-type headache (ETTH) forms, but mild nausea may be present in chronic tension-type headache (CTTH). Moderate to severe nausea and vomiting precludes the diagnosis of CTTH.
The pain is usually perceived by patients as dull and is often described as a band-like sensation around the head. The majority of patients with ETTH experience mild to moderate pain, which is rarely disabling. Most patients with TTH lack associated features. In a large Danish study, Rasmussen et al. [3] described that among 578 subjects with TTH, only 4.2 % (n = 24) had nausea accompanying the headache, 0 % had vomiting, 18 % (n = 105) had anorexia, 10.6 % (n = 61) had photophobia and 12.8 % (n = 74) had phonophobia. Among the primary headaches, TTH was the one with less defined characteristics—that is, it was usually diagnosed by the lack of certain features, rather than by their inclusion. In this setting, it is difficult to target treatment, especially when little is known about the underlying pathophysiology of this condition. In many studies, patients with migraine have not been excluded; thus, patients deemed to have TTH could have possibly had mild or probable migraine instead.
Given the generally lower intensity level of pain and typical absence of migraine-associated symptoms, patients with TTH may not seek medical attention for years, leading to an underestimation of the rate of diagnosis. Without medical support and advice, these patients are vulnerable to inadequate and insufficient treatment, medication overuse and treatment refractoriness. An additional area of caution for TTH, especially in the elderly population, is the possibility of medication interactions and adverse effects. Frequent ETTH and CTTH can be accompanied by significant disability and co-morbidity. Risk factors for the development of chronic TTH in the elderly are similar to those in the younger adult population and include analgesic overuse, depression, higher frequency of headaches and co-morbid pain syndromes [4].
Hypnic headache, a rare primary headache disorder with predominant onset later in life, can be differentiated by its relative short duration and occurrence exclusively during sleep, causing wakening [5]. It is important for it to be excluded, since its treatment differs from that given for TTH.
Sleep disruption appears to be a risk factor for headache attacks and chronification [6]. Nocturnal hypertension, nocturnal hypoglycaemia and sleep apnoea—all commonly seen with advanced age—are now recognizable and potentially treatable pathological states during sleep [7]. Sleep apnoea is highly prevalent in subjects after the age of 60 years and affects older men and women similarly [8], with a variable prevalence that may reach 87 %, depending on the study population and inclusion criteria [9].
3 Epidemiology
The lifetime prevalence of TTH ranges between 30 and 78 % [2]. In the Bruneck study in Northern Italy [10], the 1-year prevalence of TTH in the elderly was 35.8 % (27.8 % in men and 42.4 % in women). In a large American study, Schwartz et al. estimated the 1-year prevalence of ETTH to be 38.3 %. This percentage was higher among women than among men in all age, race and education groups, with an overall prevalence ratio of 1.16. Prevalence peaked in the 30-year-old age group in both men (42.3 %) and women (46.9 %). The 1-year prevalence of CTTH was 2.2 % [11].
Despite the fact that the incidence of TTH declines with age, it has a greater tendency to persist later in life when compared with migraine, thus having a major socioeconomic impact. Most elderly persons with new-onset primary headache have TTH, which may be managed by the primary care provider, a neurologist or a combination of both.
3.1 Pathophysiology
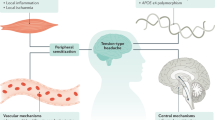
TTH pathophysiology is still not completely understood. Despite what the name suggests, TTH is not caused by tense muscles or stress; rather, these conditions may exacerbate TTH [1]. Studies utilizing surface electromyography (EMG) and pressure algometry have failed to yield significant results [12]. Pericranial myofascial tenderness is frequent in patients with TTH and migraine, and may represent a disturbance in pain-modulating pathways, characterized by peripheral and central neuronal hyperexcitability in both [13]. Bendtsen proposed that the main problem in CTTH consists of increased nociceptive input to supraspinal structures, resulting in central sensitization, similar to what Olesen [14] had suggested one decade before. The central neuroplastic changes, on the other hand, would affect the regulation of peripheral mechanisms and would therefore increase pericranial muscle activity and the release of neurotransmitters in the myofascial tissues [15]. Using voxel-based morphometry neuroimaging, Schmidt-Wilcke et al. [16] demonstrated reduced grey matter in central nervous system pain-transmitting networks in patients with CTTH but not in patients with migraine headache and concomitant medication overuse headache or in control subjects without any history of headache. The authors were not able to stipulate if the changes involved in pain-processing structures in CTTH sufferers represented the cause or the consequence of chronic head pain. Migraine pathophysiology and its related trigeminocervical complex have been well studied in animal models, with the majority of work conducted by Goadsby and colleagues. Future studies may help to identify the overlapping components between those two disorders and may explain why so frequently we see both headache phenotypes in one individual.
4 Treatment
Few controlled trials of medications have been done in patients with TTH. This speaks to the observation that over-the-counter (OTC) medications seem effective, with little incentive from pharmaceutical companies to test them systematically or to develop new ones. Even more, most studies do not exclude a past history of concomitant migraine disorder, which makes it difficult to draw a conclusion in terms of the efficacy of the drug being studied in ‘pure’ TTH.
The treatment of elderly patients with primary headache disorders is multifaceted, including acute, prophylactic, transitional [17] and alternative approaches. Co-morbid disease may mask or complicate headache conditions [18]. Pain disorders in general are often undiagnosed or undertreated in the elderly [12].
Before starting treatment, it is important to record the frequency and severity of each attack and the amount of medication consumed to treat it. This will not only allow the treating physician to obtain a baseline against which progress can be evaluated; it can also reveal potential headache triggers and unmask medication overuse. Analgesic overuse may increase the frequency of TTH and render it refractory to treatment, although most studies do not exclude the possibility of those patients having migraine. It is unclear if pure TTH is susceptible to chronification in the setting of medication overuse [19, 20].
Identifying and managing conditions such as sleep apnoea, excessive caffeine intake and psychiatric co-morbidities, such as depression and anxiety, are also helpful in controlling headache progression.
Awareness of drug pharmacokinetics and drug–drug interactions are mandatory, with additive sedative, anticholinergic and antiarrhythmic effects being examples of potential problems that physicians may face upon treating TTH in the elderly [21]. Impaired metabolism, delayed excretion of drugs and co-morbid cardiovascular risk factors can limit treatment, making non-pharmacological options, such as biofeedback and peripheral nerve blocks, a better option, even when supportive evidence for such treatments is less obvious.
The pharmacological treatment of TTH is similar to that of other headache types and is divided into acute and preventive treatments. The selected medications for treatment should target not only efficacy but also tolerability.
5 Acute Treatment
Acute treatment is most often done with simple analgesics (aspirin and paracetamol [acetaminophen), as well as with non-steroidal anti-inflammatory drugs (NSAIDs) [22].
A double-blind randomized trial found aspirin 500–1,000 mg and paracetamol 1,000 mg statistically superior to placebo in TTH treatment [23]. Only patients meeting the International Headache Society diagnostic criteria for episodic TTH but not those for migraine were included in the study. NSAIDs are among the most prescribed medication in the United States with over 98 million prescriptions filled and an estimated 23 million Americans using over-the-counter (OTC) NSAIDs in 2012 (Alliance for Rational Use of NSAIDs 2012) [24]. Current guidelines for chronic pain in elderly persons recognize that NSAIDs provide better efficacy than paracetamol (acetaminophen) for relief of osteoarthritis and rheumatoid arthritis conditions [25, 26].
There is no clear evidence for using one NSAID over another although some suggest ibuprofen as a first choice given its favourable side-effect profile [27]. In a randomized, double-blind study in 345 subjects with tension-type headache, Lange et al. [28] compared a single dose of 12.5 or 25 mg ketoprofen versus 200 mg ibuprofen versus 275 mg naproxen sodium and found no statistically significant difference among all treatments in this respect. The study does not clarify if patients with history of concomitant migraine were excluded.
Despite their clear benefit NSAIDs are associated with potential adverse effects, influenced by patient’s age, co-morbidities, class of NSAID and dosing. They should be avoided or used with caution in patients with renal dysfunction, cardiovascular disease [29], haematological disorders [30] or pre-existing peptic ulcer disease [31].
NSAIDs should preferably not be used in conjunction with aspirin, given the increased risk of gastrointestinal bleeding [32]. NSAIDs can cause an almost 13-fold increase in the risk of haemorrhagic peptic ulcer disease in patients receiving oral anticoagulants [33].
Masso Gonzalez et al. [34] raised the concern of increased upper gastrointestinal bleeding with cyclo-oxygenase (COX)-1 inhibition and even higher rates with NSAIDs that combine COX-1 and COX-2 inhibition, such as indomethacin, ketoprofen, ketorolac, naproxen and piroxicam. It is also known that mortality from peptic ulcers and associated complications, such as gastrointestinal bleeding, increase with age [35].
Caffeine is a trimethylxanthine derivative which, when used in moderation, can act as a mild analgesic and analgesic adjunctive for headache, including TTH [36]. Its mechanism may be related to the antagonism of glial and neuronal adenosine receptors. Caffeine should be used with caution because of the risk of caffeine withdrawal headaches or, when it is taken in excess, causing overuse headache.
Regular use of opioids and barbiturates should be avoided in all primary headaches because of their potential for abuse and dependency [37]. In addition, opioids have been linked to central sensitization, making both acute and prophylactic treatment less responsive [38]. A case–control study evaluated the association between common medications prescribed to individuals aged 65 years or more and injurious falls. Ten of the top 20 most commonly prescribed medications, and in particular those affecting the central nervous system, such as opioids, significantly increased the risk of fall injuries [39].
Triptans are commonly used in the treatment of migraine headache, but their role in the treatment of TTH is still unclear. Brennum et al. [40] reported that subcutaneous administration of 2–4 mg of sumatriptan induced modest but greater relief than placebo in patients with so-called TTH. The most common adverse events were a sensation of heaviness (in 7 patients), nausea (in 4 patients), sedation (in 3 patients), paraesthesias (in 2 patients) and dizziness (in 2 patients), mostly perceived by those who got the 4 mg dose. The headache diagnosis was based on the medical history, clinical examination and evaluation of a diary detailing headache symptoms. The diagnosis of CTTH was determined according to the IHS criteria. Three of the patients also had a history of migraine, but the authors were not clear if a prior or concomitant diagnosis of migraine was excluded for all of the evaluated patients. Triptans may be beneficial in patients who have TTH with certain migrainous features or who suffer from both conditions, but more studies are needed to prove their efficacy in pure TTH [41]. Despite their vasoactive properties, there is growing evidence suggesting that the chest symptoms reported with triptans are rarely related to ischaemic mechanisms [42]. Nevertheless, triptans should be prescribed with caution in patients with cardiovascular risk factors. Current guidelines state that patients at low risk of coronary heart disease (with one or no risk factors) can be prescribed triptans without the need for a more intensive cardiovascular evaluation, while those at intermediate risk (with two or more risk factors) require more intensive cardiovascular evaluation before triptans can be prescribed. Finally, patients with coronary heart disease, considered high risk, should not be prescribed triptans at all. Primary independent risk factors include cigarette smoking (any amount), elevated systolic blood pressure, elevated serum total cholesterol and low-density lipoprotein (LDL) cholesterol levels, low serum high-density lipoprotein (HDL) cholesterol levels, diabetes mellitus and advanced age [43].
Caution should be taken regarding possible additive vasoconstrictor properties of triptans when they are administered in combination with other vasoactive drugs, such as ergotamines, especially in elderly patients with possible occult coronary artery disease. Even more controversial is the concern about co-administering triptans and selective serotonin reuptake inhibitor (SSRIs), and the theoretical hypothesis of inducing serotonin syndrome, based on their pharmacological properties. There is no current consensus, and weighting risks and benefits for each patient seems to be the most reasonable approach [44].
6 Prophylactic Treatment
The tricyclic antidepressant (TCA) amitriptyline has been shown to be effective in prophylactic treatment of CTTH [45–47]. Amitriptyline blocks the neuronal reuptake of serotonin and noradrenaline, although this is not the only mode of action of its antinociceptive properties. N-methyl-D-aspartate (NMDA) receptor antagonism and blockade of muscarinic receptors and ion channels may play a role as well [48]. In an open-label study, 25 mg/day of amitriptyline was found to significantly reduce the frequency and duration of chronic but not episodic TTH [49]. TCAs should be used with caution in the elderly population because of the potential for anticholinergic side effects, such as confusion, sedation with an increased risk of falls, orthostatic hypotension, urinary retention, tachycardia and electrocardiographic changes, such as QT-interval prolongation [50].
The rates of depression and anxiety disorders are significantly higher in the headache population than in the general population [12]. Depression reduces the quality of life of these patients [51]. TCAs are probably more effective for headaches than SSRIs; they are efficacious for TTH in patients without overt depression [52].
Nortriptyline, a metabolite of amitriptyline, has more selective noradrenergic reuptake inhibition [53]. Nortriptyline is believed to be better tolerated than amitriptyline although, in an open-label trial, both drugs were found to be equivalent for overall adverse effects and discontinuation rates. Weight gain was more common with amitriptyline, while dry mouth was found to be more associated with nortriptyline [54]. Further studies are needed to establish their exact efficacy in TTH [17].
Mirtazapine, a generally better-tolerated noradrenergic and specific serotonergic antidepressant, was recently demonstrated to be effective in prophylactic treatment of CTTH. Patients with a history of migraine of <1 day/month were not excluded from this study [55].
The current studies with SSRIs show effective results in prophylaxis of migraine [56–59] but, although they are associated with fewer adverse events than TCAs, there are not enough data to support use of SSRIs for CTTH prevention.
Venlafaxine is a selective serotonin and noradrenaline reuptake inhibitor with a better side-effect profile than TCAs. Positive results were reported when it was used as a prophylactic medication in chronic migraine [60, 61]. In a retrospective study including 56 subjects with CTTH and 114 subjects with migraine, venlafaxine extended release (XR) 150 mg was safe and effective in reducing the frequency of both TTH and migraine. For the CTTH group, statistically significant improvement was only noticed after the second month of treatment. Further randomized controlled trials will be helpful to determine the potential value of this drug [62].
Tizanidine, a central muscle relaxant, has been effective in treatment of CTTH [63–65]. In an open-label randomized clinical trial in 18 CTTH patients, Bettucci et al. [66] showed that the combination of tizanidine with amitriptyline was faster than amitriptyline alone in providing an improvement in the headache pattern and correlated with quality of life. In this study, subjects with co-existence of migraine (according to the IHS criteria) and CTTH were excluded.
Lampl et al. [13] reported an open study evaluating the effectiveness and safety of topiramate for the prophylaxis of CTTH. A total of 46 patients completed 24 weeks of treatment with topiramate. Headache frequency declined from 23.50 ± 5.32 to 12.58 ± 6.28 days, with 73 % of patients achieving a 50 % reduction in headache frequency at weeks 13–24. Improvements in mood, sleep, quality of life and severity of pain were also noted. Patients with concomitant migraine with and/or without aura, or with headache with migrainous features (including pulsating pain or aggravation by exercise) and those with analgesic overuse (>15 days) were not enrolled. Weight loss is a common adverse effect and should be followed closely.
A randomized double-blind placebo-controlled trial comparing memantine 20–40 mg/day and placebo did not demonstrate a substantial effect in prophylactic treatment of CTTH [67]. The exclusion criteria were a history of more than one migraine attack per month during the previous year, serious somatic or psychiatric diseases, overuse of analgesics and intake of prophylactic headache medication.
The role of onabotulinum toxin A for the treatment of CTTH has still to be established, with mixed data suggesting its effectiveness [68]. Karadaş et al. [69] showed that the frequency and severity of CTTH were decreased at the second month after treatment with 50 units of botulinum toxin A, and this significance continued at the fourth month after treatment. In a systematic review published in JAMA, Jackson and colleagues found no benefit of botulinum toxin A in episodic migraine and CTTH [70]. Similar ineffective findings were supported by a 2008 American Academy of Neurology practice parameter [71].
Peripheral nerve blocks may be effective for TTH, but the current data are mixed and limited [72]. Given its relative safety and tolerance, this therapy can be considered in elderly patients who have failed other treatments.
6.1 Non-pharmacological Approaches
Psychological and non-conventional approaches are adjunctive measures to treat TTH. Mental stress is not the underlying cause of TTH, yet for some patients it serves as a trigger or exacerbating factor [12]. Psychological stressors, when not identified and appropriately addressed, can potentially increase the risk of chronification. Huber and Henrich [73] suggest that stress may have a hyperalgesic effect on pathways that have been previously sensitized in CTTH sufferers. Literature reviews support the use of psychological assessment tools, such as the Minnesota Multiphasic Personality Index, Beck’s Depression Scale, Hamilton Anxiety Scale, Zuckerman–Kuhlman Personality Questionnaire and Sensation Seeking Scale [74]. A range of psychological therapies, including relaxation training, cognitive behavioural therapy, biofeedback and mindfulness, have demonstrated utility and similar effectiveness in treating TTH and its associated disability [75–79], although little research has focused on the elderly population [12]. An uncontrolled series of 16 older headache patients (aged 60–77 years) diagnosed as having tension, mixed or migraine headache showed beneficial outcomes with various combinations of relaxation, cognitive coping and feedback [80]. Among other reasons, impaired cognition, such as in dementia, cultural false beliefs and out-of-pocket costs may be barriers to non-pharmacological treatment [12].
7 Conclusions
TTH is a common complaint in the elderly and can cause significant impairment. Since the incidence of secondary headache disorders increases with advanced age, investigation is required to exclude underlying pathology. Successful management of TTH combines pharmacological and non-pharmacological approaches. Pharmacological management is divided into acute and preventive treatments. Some of the available clinical trials do not mention if a previous or current concomitant history of migraine was excluded, making it difficult to draw any conclusion, since most of those medications are known to work for migraine-type headache. Polypharmacy, co-morbid disorders, impaired metabolism and drug excretion are common limiting factors when considering the most effective treatment for elderly patients with TTH. Non-pharmacological options, such as biofeedback and relaxation techniques, become fundamentally important in this population of headache sufferers, especially when acute and preventive medications are poorly tolerated or contraindicated. However, barriers such as high costs, impaired cognition and cultural resistance may limit the use of non-pharmacological treatments. More randomized controlled trials are necessary to determine the safest and most effective treatments in elderly patients with TTH.
References
Crystal SC, Grosberg BM. Tension-type headache in the elderly. Curr Pain Headache Rep. 2009;13(6):474–8.
Headache Classification Subcommittee of the International Headache Society (IHS). The international classification of headache disorders, 3rd edition (beta version). Cephalalgia. 2013 Jul;33(9):629–808.
Rasmussen BK, Jensen R, Olesen J. A population-based analysis of the diagnostic criteria of the International Headache Society. Cephalalgia. 1991;11(3):129–34.
Crystal SC, Robbins MS. Epidemiology of tension-type headache. Curr Pain Headache Rep. 2010;14(6):449–54.
Manni R, Ghiotto N. Hypnic headache. Handb Clin Neurol. 2010;97:469–72.
Holland PR. Headache and sleep: shared pathophysiological mechanisms. Cephalalgia. 2014 Sep;34(10):725–44.
Javaheri S, Redline S. Sleep, slow-wave sleep, and blood pressure. Curr Hypertens Rep. 2012;14(5):442–8.
Launois SH, Pépin JL, Lévy P. Sleep apnea in the elderly: a specific entity? Sleep Med Rev. 2007;11(2):87–97.
Polese JF, Santos-Silva R, de Oliveira Ferrari PM, Sartori DE, Tufik S, Bittencourt L. Is portable monitoring for diagnosing obstructive sleep apnea syndrome suitable in elderly population? Sleep Breath. 2013;17(2):679–86.
Schwaiger J, Kiechl S, Seppi K, Sawires M, Stockner H, Erlacher T, Mairhofer ML, Niederkofler H, Rungger G, Gasperi A, Poewe W, Willeit J. Prevalence of primary headaches and cranial neuralgias in men and women aged 55–94 years (Bruneck study). Cephalalgia. 2009;29(2):179–87.
Schwartz BS, Stewart WF, Simon D, Lipton RB. Epidemiology of tension-type headache. JAMA. 1998;279(5):381–3.
Rosen NL. Psychological issues in the evaluation and treatment of tension-type headache. Curr Pain Headache Rep. 2012;16(6):545–53.
Lampl C, Marecek S, May A, Bendtsen L. A prospective, open-label, long-term study of the efficacy and tolerability of topiramate in the prophylaxis of chronic tension-type headache. Cephalalgia. 2006;26(10):1203–8.
Olesen J. Clinical and pathophysiological observations in migraine and tension-type headache explained by integration of vascular, supraspinal and myofascial inputs. Pain. 1991;46(2):125–32.
Bendtsen L. Central sensitization in tension-type headache possible pathophysiological mechanisms. Cephalalgia. 2000;20(5):486–508.
Schmidt-Wilcke T, Leinisch E, Straube A, Kämpfe N, Draganski B, Diener HC, Bogdahn U, May A. Gray matter decrease in patients with chronic tension type headache. Neurology. 2005;65(9):1483–6.
Robbins MS, Lipton RB. Management of headache in the elderly. Drugs Aging. 2010;27(5):377–98.
Pitkala KH, Strandberg TE, Tilvis RS. Management of nonmalignant pain in home-dwelling older people: a population-based survey. J Am Geriatr Soc. 2002;50(11):1861–5.
Kristoffersen ES, Lundqvist C. Medication-overuse headache: epidemiology, diagnosis and treatment. Ther Adv Drug Saf. 2014;5(2):87–99.
Colás R, Muñoz P, Temprano R, Gómez C, Pascual J. Chronic daily headache with analgesic overuse: epidemiology and impact on quality of life. Neurology. 2004;62(8):1338–42.
Seymour RM, Routledge PA. Important drug–drug interactions in the elderly. Drugs Aging. 1998;12(6):485–94.
Bigal Marcelo E, Rapoport Alan M, Hargreaves Richard. Advances in the pharmacologic treatment of tension-type headache. Curr Pain Headache Rep. 2008;12(6):442–6.
Steiner TJ, Lange R, Voelker M. Aspirin in episodic tension-type headache: placebo-controlled dose-ranging comparison with paracetamol. Cephalalgia. 2003;23:59–66.
Fowler Terri O, Durham Catherine O, Planton Jonathan, Edlund Barbara J. Use of nonsteroidal anti-inflammatory drugs in the older adult. J Am Assoc Nurse Pract. 2014;26(8):414–23.
Zhang W, Doherty M, Leeb BF, et al. EULAR evidence based recommendations for the management of hand osteoarthritis: report of a Task Force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis. 2007;66(3):377–88.
Zhang W, Moskowitz RW, Nuki G, et al. OARSI recommendations for the management of hip and knee osteoar thritis, part II: OARSI evidence-based, expert consensus guidelines. Osteoarthr Cartil. 2008;16(2):137–62.
Verhagen AP, Damen L, Berger MY, Passchier J, Merlijn V, Koes BW. Is any one analgesic superior for episodic tension-type headache? J Fam Pract. 2006;55(12):1064–72.
Lange R, Lentz R. Comparison ketoprofen, ibuprofen and naproxen sodium in the treatment of tension-type headache. Drugs Exp Clin Res. 1995;21(3):89–96.
Kearney PM, Baigent C, Godwin J, Halls H, Emberson JR, Patrono C. Do selective cyclo-oxygenase-2 inhibitors and traditional non-steroidal anti-inflammatory drugs increase the risk of atherothrombosis? Meta-analysis of randomised trials. BMJ. 2006;332(7553):1302–8.
Antman EM, Bennett JS, Daugherty A, Furberg C, Roberts H, Taubert KA. American Heart Association. Use of nonsteroidal antiinflammatory drugs: an update for clinicians: a scientific statement from the American Heart Association. Circulation. 2007;115(12):1634–42.
Hippisley-Cox J, Coupland C, Logan R. Risk of adverse gastrointestinal outcomes in patients taking cyclo-oxygenase-2 inhibitors or conventional non-steroidal anti-inflammatory drugs: population based nested case–control analysis. BMJ. 2005;331(7528):1310–6.
Masclee GM, Valkhoff VE, Coloma PM, de Ridder M, Romio S, Schuemie MJ, Herings R, Gini R, Mazzaglia G, Picelli G, Scotti L, Pedersen L, Kuipers EJ, van der Lei J, Sturkenboom M. Risk of upper gastrointestinal bleeding from different drug combinations. Gastroenterology. 2014 Oct;147(4):784–92.e9.
Shorr RI, Ray WA, Daughert JR, et al. Concurrent use of nonsteroidal anti-inflammatory drugs and oral anticoagulants places elderly persons at high risk for hemorrhagic peptic ulcer disease. Arch Intern Med. 1993;153:1665–70.
Masso Gonzalez EL, Patrignani P, Tacconelli S, et al. Variability among nonsteroidal antiinflammatory drugsin risk of upper gastrointestinal bleeding. Arthr Rheum. 2010;62(6):1592–601.
Franceschi M, Di Mario F, Leandro G, et al. Acid-related disorders in the elderly. Best Pract Res Clin Gastroenterol. 2009;23(6):839–48.
Shapiro RE. Caffeine and headaches. Curr Pain Headache Rep. 2008;12(4):311–5.
Silberstein SD. Practice parameter: evidence-based guidelines for migraine headache (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2000;55(6):754–62.
Bigal ME, Serrano D, Buse D, et al. Acute migraine medications and evolution from episodic to chronic migraine: a longitudinal population-based study. Headache. 2008;48:1157–68.
Kuschel BM, Laflamme L, Möller J. The risk of fall injury in relation to commonly prescribed medications among older people—a Swedish case–control study. Eur J Public Health. doi:10.1093/eurpub/cku120.
Brennum J, Kjeldsen M, Olesen J. The 5-HT1-like agonist sumatriptan has a significant effect in chronic tension-type headache. Cephalalgia. 1992;12(6):375–9.
Lipton RB, Stewart WF, Cady R, et al. 2000 Wolfe Award. Sumatriptan for the range of headaches in migraine sufferers: results of the Spectrum study. Headache. 2000;40:783–91.
Dodick DW, Martin VT, Smith T, Silberstein S. Cardiovascular tolerability and safety of triptans: a review of clinical data. Headache. 2004;44(Suppl 1):S20–30.
Papademetriou V. Cardiovascular risk assessment and triptans. Headache. 2004;44(Suppl 1):S31–9.
Rolan PE. Drug interactions with triptans: which are clinically significant? CNS Drugs. 2012;26(11):949–57.
Bendtsen L, Jensen R, Olesen J. A non-selective (amitriptyline), but not a selective (citalopram), serotonin reuptake inhibitor is effective in the prophylactic treatment of chronic tension-type headache. J Neurol Neurosurg Psychiatry. 1996;61:285–90.
Bendtsen L, Jensen R, Olesen J. Amitriptyline, a combined serotonin and noradrenaline re-uptake inhibitor, reduces exteroceptive suppression of temporal muscle activity in patients with chronic tension-type headache. Electroencephaogr Clin Neurophysiol. 1996;101:418–22.
Göbel H, Hamouz V, Hansen C, et al. Chronic tension type headache: amitriptyline reduces clinical headache duration and experimental pain sensitivity but does not alter pericranial muscle activity readings. Pain. 1994;59:241–9.
Ashina S, Bendtsen L, Jensen R. Analgesic effect of amitriptyline in chronic tension-type headache is not directly related to serotonin reuptake inhibition. Pain. 2004;108:108–14.
Cerbo R, Barbanti P, Fabbrini G, et al. Amitriptyline is effecttive in chronic but not in episodic tension-type headache: pathogenetic implications. Headache. 1998;38:453–7.
Darowski A, Chambers SA, Chambers DJ. Antidepressants and falls in the elderly. Drugs Aging. 2009;26(5):381–94.
Peñacoba-Puente C, Fernández-de-Las-Peñas C, González-Gutierrez JL, Miangolarra-Page JC, Pareja JA. Interaction between anxiety, depression, quality of life and clinical parameters in chronic tension-type headache. Eur J Pain. 2008;12(7):886–94.
Bendtsen L, Jensen R, Olesen J. A non-selective (amitriptyline), but not a selective (citalopram), serotonin reuptake inhibitor is effective in the prophylactic treatment of chronic tension-type headache. J Neurol Neurosurg Psychiatry. 1996;61(3):285–90.
Buchanan Thomas M, Ramadan Nabih M. Prophylactic pharmacotherapy for migraine headaches. Semin Neurol. 2006;26(2):188–98.
Liu WQ, Kanungo A, Toth C. Equivalency of tricyclic antidepressants in open-label neuropathic pain study. Acta Neurol Scand. 2014;129(2):132–41.
Bendtsen L, Jensen R. Mirtazapine is effective in the prophylactic treatment of chronic tension-type headache. Neurology. 2004;62:1706–11.
Adly C, Straumanis J, Chesson A. Fluoxetine prophylaxis of migraine. Headache. 1992;32:101–4.
Bank J. A comparative study of amitriptyline and fluvoxamine in migraine prophylaxis. Headache. 1994;34(8):476–8.
D’Amato CC, Pizza V, Marmolo T, Giordano E, Alfano V, Nasta A. Fluoxetine for migraine prophylaxis: a double-blind trial. Headache. 1999;39:716–9.
Nascimento ED. Profilaxia da migranea. Estudo aberto a venlafaxina em 42 pacientes. Arq Neuropsiquiatr. 1998;56:744–6.
Ozyalcin SN, Talu GK, Kiziltan E, Yucel B, Ertas M, Disci R. The efficacy and safety of venlafaxine in the prophylaxis of migraine. Headache. 2005;45:144–52.
Diamond S. Efficacy and safety profile of venlafaxine in chronic headache. Headache Q Curr Treat Res. 1995;6:212–4.
Adelman LC, Adelman JU, Von Seggern R, Mannix LK. Venlafaxine extended release (XR) for the prophylaxis of migraine and tension-type headache: a retrospective study in a clinical setting. Headache. 2000;40:572–80.
Saper JR, Winner PK, Lake AE 3rd. An open-label dose-titration study of the efficacy and tolerability of tizanidine hydrochloride tablets in the prophylaxis of chronic daily headache. Headache. 2001;41(4):357–68.
Fogelholm R, Murros K. Tizanidine in chronic tension-type headache: a placebo controlled double blind cross-over study. Headache. 1992;32:509–13.
Shimomura T, Awaki E, Kowa H, Takahashi K. Treatment of tension-type headache with tizanidine hydrochloride: its efficacy and relationship to the plasma MHPG concentration. Headache. 1991;31:601–4.
Bettucci D, Testa L, Calzoni S, Mantegazza P, Viana M, Monaco F. Combination of tizanidine and amitriptyline in the prophylaxis of chronic tension-type headache: evaluation of efficacy and impact on quality of life. J Headache Pain. 2006;7(1):34–6.
Lindelof K, Bendtsen L. Memantine for prophylaxis of chronic tension-type headache—a double-blind, randomized, crossover clinical trial. Cephalalgia. 2009;29(3):314–21.
Harden RN, Cottrill J, Gagnon CM, Smitherman TA, Weinland SR, Tann B, Joseph P, Lee TS, Houle TT. Botulinum toxin a in the treatment of chronic tension-type headache with cervical myofascial trigger points: a randomized, double-blind, placebo-controlled pilot study. Headache. 2009;49(5):732–43.
Karadaş O, Ipekdal IH, Ulaş UH, Kütükçü Y, Odabaşi Z. Botulinum neuro-toxin type-A in the treatment of chronic tension type headache associated with pericranial tenderness. Agri. 2012;24(1):9–14.
Jackson JL, Kuriyama A, Hayashino Y. Botulinum toxin A for prophylactic treatment of migraine and tension headaches in adults: a meta-analysis. JAMA. 2012;307(16):1736–45.
Naumann M, So Y, Argoff CE, Childers MK, Dykstra DD, Gronseth GS, Jabbari B, Kaufmann HC, Schurch B, Silberstein SD, Simpson DM, Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Assessment: botulinum neurotoxin in the treatment of autonomic disorders and pain (an evidence-based review): report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology. 2008;70(19):1707–14.
Tobin J, Flitman S. Occipital nerve blocks: when and what to inject? Headache. 2009;49(10):1521–33.
Huber D, Henrich G. Personality traits and stress sensitivity in migraine patients. Behav Med. 2003;29(1):4–13.
Roditi D, Robinson ME. The role of psychological interventions in the management of patients with chronic pain. Psychol Res Behav Manag. 2011;4:41–9.
Hammill JM, Cook TM, Rosecrance JC. Effectiveness of a physical therapy regimen in the treatment of tension-type headache. Headache. 1996;36(3):149–53.
Bruhn P, Olesen J, Melgaard B. Controlled trial of EMG feedback in muscle contraction headache. Ann Neurol. 1979;6(1):34–6.
Holroyd KA, O’Donnell FJ, Stensland M, Lipchik GL, Cordingley GE, Carlson BW. Management of chronic tension-type headache with tricyclic antidepressant medication, stress management therapy, and their combination: a randomized controlled trial. JAMA. 2001;285(17):2208–15.
Nestoriuc Y, Rief W, Martin A. Meta-analysis of biofeedback for tension-type headache: efficacy, specificity, and treatment moderators. J Consult Clin Psychol. 2008;76(3):379–96.
Nestoriuc Y, Martin A, Rief W, Andrasik F. Biofeedback treatment for headache disorders: a comprehensive efficacy review. Appl Psychophysiol Biofeedback. 2008;33(3):125–40.
Kabela E, Blanchard EB, Appelbaum KA, Nicholson N. Self-regulatory treatment of headache in the elderly. Biofeedback Self Regul. 1989;14(3):219–28.
Acknowledgments
Dr. Silberstein has acted as a consultant and/or advisory panel member for Alder Biopharmaceuticals; Allergan, Inc.; Amgen; Avanir Pharmaceuticals, Inc.; eNeura Inc.; ElectroCore Medical, LLC; Medscape, LLC; Medtronic, Inc.; Mitsubishi Tanabe Pharma America, Inc.; Neuralieve; NINDS; Pfizer, Inc.; Supernus Pharmaceuticals, Inc.; and Teva Pharmaceuticals. His employer receives research support from Allergan, Inc.; Amgen; Cumberland Pharmaceuticals, Inc.; ElectroCore Medical, LLC; Labrys Biologics; Eli Lilly and Company; Merz Pharmaceuticals; and Troy Healthcare.
Dr. Wrobel Goldberg has no conflict of interest.
Dr. Grosberg served on the advisory board for Tribute Pharmaceutical and on the speaker's board of Zogenix. Dr. Grosberg is a director of the Montefiore Headache Center, which receives research support from Allergan, Electrocore, and Novartis.
No funding was received for this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wrobel Goldberg, S., Silberstein, S. & Grosberg, B.M. Considerations in the Treatment of Tension-Type Headache in the Elderly. Drugs Aging 31, 797–804 (2014). https://doi.org/10.1007/s40266-014-0220-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-014-0220-2