Abstract
Purpose of Review
This paper aims to review low energy availability (low EA), compare the Female Athlete Triad (Triad) and Relative Energy Deficiency in Sport (RED-S) screening tools and eating disorder/disordered eating questionnaires, and discuss multidisciplinary awareness, education, and treatment strategies. It provides an overview on the current state of the Triad and RED-S and assists clinicians with an overview of options for screening tools for their practice.
Recent Findings
Triad Consensus Panel Screening Questions, Preparticipation Physical Exam (PPE), and Periodic Health Exam (PHE) share overlapping questions from the Triad Consensus Panel Screening Questions. The Low Energy Availability in Females Questionnaire (LEAF-Q) is used in complement with eating disorder/disordered eating questionnaires (Table 2).
Summary
It is important to screen athletes for low EA during the PPE. If concerned for low EA, referral to healthcare professional and registered dietician is warranted. Education for athletes, coaches, and multidisciplinary providers is needed to increase awareness of low EA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 1992, the Female Athlete Triad (Triad) was originally defined as an association of disordered eating, amenorrhea, and osteoporosis [1••, 2, 3]. In 2007, it was re-defined as three interrelated components of the Triad existing on a spectrum of low energy availability (EA) (with or without disordered eating), menstrual dysfunction, and low bone mineral density among female athletes [4•, 5••, 6,7,8,9,10]. In 2014, the Female Athlete Triad Coalition Consensus Statement proposed a risk stratification system regarding sports participation and return to play [1••]. That same year, the International Olympic Committee (IOC) introduced the term Relative Energy Deficiency in Sport (RED-S) as a more comprehensive syndrome than the Female Athlete Triad [11••].
Underpinning both the Triad and RED-S is low EA, which is caused by insufficient energy intake to account for the cost of exercise [1•, 11••]. Low EA can be challenging to diagnose because of subtle symptomatology and health consequences that are not readily apparent. Weight is not an accurate sole indicator of energy availability [7, 12]; therefore, further investigation is indicated. Many athletes along with medical providers are not familiar with the Triad or RED-S and their risk factors. Critical and preventable health and performance consequences are associated with low EA; thus, awareness and education is needed for athletes and multidisciplinary providers who will have the opportunity to screen athletes. With varied screening tools, it can be overwhelming for clinicians to know which screening tools to use. This paper aims to provide an overview on the current state of the Triad and RED-S and assist clinicians with an overview of options for screening tools while also reviewing low EA, multidisciplinary awareness, education, and treatment strategies.
Comparing the Triad and RED-S
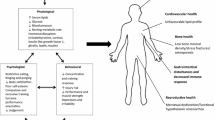
Both the Triad and RED-S call attention to the importance of appropriate EA to prevent poor health outcomes [13]. Relative Energy Deficiency in Sport (RED-S) is a complex clinical syndrome referring to impaired physiological functioning due to a relative energy deficit caused by greater energy expenditure than energy intake. The RED-S conceptual model expands upon the health consequences from the Triad and is inclusive of endocrine, metabolic, hematological, growth and development, psychological, cardiovascular, gastrointestinal, and immunological health consequences [11••, 14••, 15••].
RED-S includes male athletes, adds broader context to athletes with disabilities, and expands upon potential health and performance consequences of low EA [11••]. Male athletes have historically been excluded from the Triad; however, male athletes also experience low energy availability and a review of the literature suggests that male athletes may experience health issues parallel to those of the Triad [5••]. Knowledge about mechanisms unique to each sex will be helpful to create evidence-based guidelines [5••].
Controversy exists regarding acceptance of RED-S [13]. The authors of the 2014 Female Athlete Triad Coalition Consensus Statement refuted the IOC Consensus Statement on Relative Energy Deficiency in Sport (RED-S) stating that RED-S is a theoretical construct without scientific research that de-emphasizes the most concerning health sequelae from the Female Athlete Triad, notably negative bone outcomes, reproductive disorders, and eating disorders/disordered eating [16].
Despite the Triad being more rigorously researched, the medical community continues to call upon both the Triad and RED-S for additional research. Further inclusion of populations and possible physiologic sequelae within the Female Athlete Triad, and for additional scientific rigor to support the RED-S and establish causal effects within the pinwheel (Fig. 1), which will take years of experiments and peer review [8, 13]. Rather than the Triad and RED-S being seen as adversarial, much of the future research can improve understanding of both syndromes given their unified link to low EA.
Triad and RED-S. Reproduced from Mountjoy et al. [14••] with permission from BMJ Publishing Group Ltd.
Emphasis needs to be on educating the athlete, coach, and multidisciplinary providers on low EA and the downstream consequences. Athletes may be less familiar with the Triad and RED-S syndromes, but the concept of fueling the body appropriately for their activity level, will lead to a healthier long-term lifestyle which is an understandable concept that should be presented to athletes.
Low Energy Availability
The Triad and RED-S are caused by an energy mismatch between an athlete’s energy intake and estimated energy expenditure as defined by the equation below [15••]:
[15••]
Optimal EA for physiological function is usually 45 kcal/kg FFM/day, and generally considered low when < 30 kcal/kg FFM/day; however, different studies have varying lower limits of normal [7, 15••, 17].
Assessment of EA
Measuring EA is challenging. Many studies use screening tools as a surrogate for low EA. There is no universal standard for defining low EA (though many studies do use < 30 kcal/kg FFM/day), and there is no single sensitive tool to detect low EA among female and male athletes [18, 19]. There are limitations to directly measuring EA both practically and reliably, including wearable devices that may underestimate energy expenditure [15, 20]. While dietary and exercise logs can provide energy estimates, dietary survey validity and reliability are questioned for under-reporting [15••, 19, 21]. Questionnaires and blood hormone concentrations provide more accurate markers of EA than dietary and training estimations [18].
Athletes can have a stable body weight and still have low EA, therefore, body weight is not a sole reliable indicator of energy balance [7, 12]. Imperfect surrogate markers for low EA include BMI ≤ 17.5 kg/m2, ≥ 10% weight loss in 1 month, or < 85% expected body weight for adolescents [1••, 15••]. It has been suggested that low fat mass, low free T3, reduced resting metabolic rate, and leptin levels may be useful as indicators of low EA [1••, 7]. Supplemental EA tools include Dual energy X-ray absorptiometry (DXA) measurement of body composition [15••], heart rate monitor, and electrical impedance body composition scale [17]. DXA, air displacement plethysmography, skinfold measurements, and bioelectrical impedance estimate body fat; practical application of these methods is limited by cost and availability [1••]. EA can also fluctuate in time; therefore, diligence is needed with routine screening tools.
Sport Pressures
Athletes experience internal and external pressure to achieve “ideal” body types, which can increase the risk for nutritional deficits, especially sports emphasizing aesthetics, leanness, and weight-specific sports [5••, 22]. There are also sociocultural demands, body weight pressures, and performance pressures which may intentionally or inadvertently lead to low EA [4•, 22, 23]. Athletes competing in weight-sensitive (i.e., wrestling) and leanness sports have known challenges with attempting rapid weight loss, dieting, and frequent weight fluctuations, which increases the risk of an energy deficit [22].
The pressure to achieve leanness is exemplified by Mary Cain, the youngest American track and field athlete to make a World Championships team in 2013 at the age of 17, later a World Champion in 2014 [24]. Cain joined Nike’s Oregon Project with a coach but without a sports psychologist or nutritionist. She describes the pressure to get “thinner and thinner” [24]. Cain cites a culture of body shaming by being weighed publicly in front of her fellow runners, prescribed birth control pills and diuretics, loss of her menstrual cycle for a combined total of 3 years, and five fractured bones [24]. While her story of negative health outcomes is devastating, it is a critical example of the multidisciplinary education and support needed for athletes.
Prevalence
The prevalence of low EA among female athletes has been described more so than the prevalence among male athletes and para-athletes (para-athlete refers to athletes with a disability who practice parasports and encompasses a wide range of disabilities including but not limited to impaired mobility in limb(s), visual impairment, and/or coordination impairments) [10, 15••, 25]. Prevalence of low EA ranges from 22 to 58% [26]. Among female athletes 15–30 years old presenting to a sports medicine clinic, Ackerman et al. report a staggeringly high 47.3% presenting with low EA [8]. Among recreationally competitive male endurance athletes, the prevalence of low EA is 47.2% [27]. Among national/world-class female and male distance athletes, low EA was present in 25% of male and 31% of female athletes [18].
Rates of US athletes qualifying for components of the Triad are striking. Among female collegiate athletes participating in various sports, 25.0% met criteria for disordered eating, 25.9% for menstrual irregularity, and 1.8% for low bone mass [28]. Comparing lean versus non-lean sports athletes revealed a higher prevalence of all three Triad criteria in lean sports athletes 1.5–6.7% versus non-lean sports athletes 0–2.0% [10]. The prevalence of disordered eating ranged greatly and was similar between lean sports athletes and non-lean sports athletes at 1.5–89.2% and 0.0–89.2%, respectively [10].
Male Athletes
The term Female Athlete Triad has been modified to the Triad to be more inclusive given that males experience low EA [29], hypogonadotropic hypogonadism with reduced sex steroids, and low bone mineral density [5••]. Male athletes suffer from suppression of serum testosterone [15••], influences on the hypothalamic-pituitary-testicular axis, and metabolic hormone levels [5••]. Compared with females, males may need to have more restrictive thresholds of low EA to have effects on bone metabolism and endocrine function [29]. While low EA has been shown to have pathological effects on women at < 30 kcal/kg FFM, Fagerberg et al. report that effects from low EA are apparent at a lower threshold in men at ∼ 20–25 kcal/kg FFM [30]. Specific populations of male athletes at risk of low EA demonstrating symptoms of the RED-S have been shown in cyclists, combat sports, jockeys, rowers, and distance runners [31]. Sex-specific screening inclusive of male athletes is important to address modifiable risk factors [29]. The International Olympic Committee reports that the Low Energy Availability in Males Questionnaire (LEAM-Q) is in development, which is similar to the Low Energy Availability in Females Questionnaire (LEAF-Q) [15••].
Para-athletes
There is no current data for what defines low EA among athletes with various disabilities [32]; therefore, scant literature exists regarding the prevalence of the Triad/RED-S among para-athletes. EA is calculated based on kilograms of fat-free mass (FFM) which may be different in athletes with disability [32]. Baseline energy expenditure is reduced among athletes who use a wheelchair for mobility [15••, 32]. Amputees using a prosthesis may have increased energy needs. Para-athletes are at risk for impaired bone health due to altered skeletal loading. Leg bone mineral density is significantly lower in wheelchair athletes with spinal disorders than athletes with amputations [33]. Among para-athletes training for the 2016 or 2018 Paralympic Games, who are survey responders, 9.2% of athletes reported bone stress injuries [34]. Among 260 elite para-athletes (150 male, 110 female), < 10% of athletes reported awareness of the Triad/RED-S [35]. 44.2% of these elite para-athletes felt pressure to maintain body weight, and > 50% attempted to change their weight or body composition for sports performance [35].
Health Consequences of Low EA on Organ Systems
Health consequences of low EA are multifactorial and span several organ systems. Compared with athletes with adequate EA, athletes with low EA were more likely to have metabolic, bone, cardiovascular, gastrointestinal [8], immunologic, and hematologic issues [14••].
Endocrine
During low EA, metabolic processes may be suppressed including menstrual function in female athletes [1••, 36]. Low EA leads to disruption of the hypothalamic gonadotropin-releasing hormone pathway and luteinizing hormone pulsatility causing functional hypothalamic amenorrhea [11••, 36, 37]. Only recently have the effects of low EA on the endocrine system been described in male athletes [15••, 31, 36]. Koehler et al. reports an association with reduced leptin in exercising men after 4 days of low EA defined as 15 kcal kg/LBM·day [38].
Bone Health
Bone remodeling depends on mechanical loading as well as EA [15••, 17, 39]. Altered bone microarchitecture, altered bone turnover markers, and decreased bone mineral density are present in female athletes with oligomenorrhea/amenorrhea or low EA secondary to hypoestrogenic state, leading to an increased lifetime fracture risk [1••, 15••, 40, 41]. Bone stress injuries in collegiate athletes were found to be twice as likely in moderate-risk athletes versus low-risk athletes using the Female Athlete Triad Cumulative Risk Assessment score when adjusting for age and cross-country running participation [29].
Cardiovascular
Hypoestrogenism in athletes with exercise-associated amenorrhea is a risk for endothelial dysfunction and unhealthy lipid profile leading to early atherosclerosis among differing cardiac pathologies [1••, 15••, 42].
Gastrointestinal
There is a higher self-reported incidence of gastrointestinal dysfunction by female athletes between the ages of 15 and 30 with low EA, with reported GI issues such as constipation and delayed gastric emptying [8, 15••].
Immunologic
A reduction in energy intake combined with an increase in physical training demonstrated fat loss and an alteration of immune function parameters including white blood cells, immunoglobulin G glycome, leukocyte transcriptome, and cytokine profile, which recovers with regaining weight [43].
Hematologic
Iron is a part of oxygen transportation and mitochondrial ATP production. Iron deficiency contributes to energy deficiency by decreasing metabolic efficiency. Among the consequences of iron deficiency and anemia, it may negatively affect bone health and thyroid function [44].
Physical and Mental Consequences of Low EA
Athletic Performance
Questionnaires measuring low EA demonstrate strong associations between low EA and performance consequences [8]. Compared with athletes with adequate EA, athletes with low EA were significantly more likely to report judgment impairments, decreased training response, and decrease in endurance [8]. While athletic performance may initially be improved by overtraining, habitual overtraining may lead to low EA and have a detrimental impact on athletic performance. Injuries associated with low EA increase loss of practice and competition time [1••].
Mental Health
Low EA has demonstrated negative psychological health consequences [8, 11••, 13, 15••]. Anxiety, depression, and disordered eating, including anorexia nervosa and bulimia, may be present in athletes and precede a diagnosis of the Triad/RED-S [45]. Conversely, low EA contributes to psychological distress including depression and irritability [14••, 15••, 30].
Eating Disorders
Eating disorders are clinical mental disorders and may be accompanied by other psychiatric problems including low self-esteem, depression, and anxiety disorders [4•]. The DSM-5 includes eight different feeding and eating disorders [8]. In contrast, disordered eating may include “restrictive eating, fasting, frequently skipped meals, diet pills, laxatives, diuretics, enemas, overeating, binge-eating, and then purging” [4•].
Eating disorders start to develop in adolescence, and the timing may coincide with sports specialization [46]. While nutrition counseling is important for many athletes, treatment of clinically diagnosed eating disorders should include medical treatment from health professionals [4•, 9].
There are many screening tools for eating disorders/disordered eating in the general population, some of which target athletes [15••]. Please see Table 2. The Preparticipation Physical Exam (PPE) also includes specific questions to assess disordered eating behaviors and attitudes [48].
Screening Tools
There is a lack of consensus regarding which screening/risk assessment tools are best for assessing an athlete’s health risk and consideration for sports participation [49••]. The optimal time to screen for the Triad/RED-S is during the PPE, annual check-ups, and/or when athletes/patients are evaluated by their clinicians for health-related concerns [1••, 46, 50••]. The PPE at the high school and collegiate levels is a critical screening tool for early warning signs and symptoms of the Triad and RED-S [51]. The PPE includes evaluation for signs of an eating disorder, menstrual history including contraceptive use, history of bone stress injuries, and body mass index; positive responses require further investigation. [1••, 48, 51].
Table 1 compares the following screening tools: the Low Energy Availability in Females Questionnaire (LEAF-Q) [52•], the Triad Consensus Panel Screening Questions [1••], the Preparticipation Physical Exam (PPE) 5th Edition [48], and Periodic Health Exam from IOC Consensus Statement [53].
The Triad Consensus Panel Screening Questions are depicted in Box 1. There is significant overlap between the Triad Consensus Panel Screening Questions, the Preparticipation Physical Exam (PPE) 5th Edition Medical History, and the Periodic Health Exam IOC Consensus Statement on Evaluation of Elite Athletes as shown in Table 1. All of the screening tools are beneficial because they will screen for parts of the Triad/RED-S/Low EA; however, some cast a wider net than others and are more time-intensive. The PPE and Periodic Health Exam are the longest screening tools and most useful for overall annual athlete screening. The LEAF-Q and the Triad Consensus Panel Screening Questions are shorter and more useful for a short office setting when time is limited.
The PPE and the Periodic Health Exam IOC Consensus Statement on Evaluation of Elite Athletes survey both male and female athletes. The LEAF-Q and the Triad Consensus Panel Screening Questions (Box 1) focus on female athletes and the Triad. The LEAF-Q classifies current EA, reproductive function, and bone health, qualifying its usefulness as a screening tool to identify female athletes at risk for the Triad and complements validated eating disorder/disordered eating screening tools [52•]. As referenced above, the Low Energy Availability in Males Questionnaire (LEAM-Q) is in development [15••].
Box 1 Triad consensus panel screening questions
Have you ever had a menstrual period/ How old were you when you had your first menstrual period? When was your most recent menstrual period? How many periods have you had in the past 12 months? Are you presently taking any female hormones (estrogen, progesterone, birth control pills)? Do you worry about your weight? Are you trying to or has anyone recommended that you gain or lose weight? Are you on a special diet or do you avoid certain types of foods or food groups? Have you ever had an eating disorder? Have you ever had a stress fracture? Have you ever been told you have low bone density (osteopenia or osteoporosis) |
Reproduced from 2014 Female Athlete Triad Coalition Consensus Statement on Treatment and Return to Play of the Female Athlete Triad: 1st International Conference held in San Francisco, CA, May 2012, and 2nd International Conference held in Indianapolis, IN, May 2013, De Souza et al. [1••] with permission from BMJ Publishing Group Ltd.
Screening Tools for Disordered Eating/Eating Disorders
Both the Triad and RED-S fall on a spectrum of low EA with or without disordered eating. There are specific screening tools for disordered eating/eating disorders as summarized in Table 2. Flagged responses from the general screening tools should prompt further evaluation with specific disordered eating/eating disorder screening tools. It is important to note that under-fueling and overtraining can lead to low EA, and disordered eating/eating disorder is not a prerequisite to the Triad/RED-S. (Please see Table 2 for the details of the disordered eating/eating disorder screening tools.)
Clinical Risk Assessment Tools for Sports Participation
Overview of Triad CRA and RED-S CAT
The Female Athlete Triad Cumulative Risk Assessment (Triad CRA) and the Relative Energy Deficiency in Sport Clinical Assessment Tool (RED-S CAT) are clinical risk assessment tools that are useful for multidisciplinary providers to assess health risk and assess readiness for Sports Participation [1••, 14••, 49••]. The Triad CRA uses a point system based on evidence-based risk factors for the Female Athlete Triad including EA, body mass index, delayed menarche, oligomenorrhea and/or amenorrhea, and history of stress reaction/fracture to categorize athletes into low, moderate, and high risk for sports participation [1••]. The RED-S CAT similarly categorizes athletes into low, moderate, and high risk for sports participation [14•]. Holtzman et al. compared the Triad CRA and RED-S CAT risk assessment tools and found that the RED-S CAT tends to assign athletes to higher risk levels than the Triad CRA and that the assessment tools agreed on the same risk assessment level in 55.5% of participants [49••]. The risk level differences suggest different sensitivities and future research should be focused on understanding health outcomes in athletes to refine each scoring system [49••].
Multidisciplinary Awareness, Education, and Treatment Strategies
Physician Awareness
Awareness of the Triad/RED-S is necessary among physicians in multiple disciplines to provide screening, diagnosis, treatment plans, and sports participation decisions. Few studies demonstrate multidisciplinary awareness among the Triad /RED-S. Among 931 multispecialty physicians, only 37% were aware of the Triad, and 51% felt comfortable referring or treating a patient with the Triad [50••]. There were a broad spectrum of specialties surveyed from primary care to surgical specialties [50••]. Categorized by specialty, the Triad awareness rate was highest among orthopedic surgeons 80%, then obstetrics and gynecology 55%, physical medicine and rehabilitation/rheumatology 52%, psychiatry 11%, radiology 10%, and anesthesia 9% [50••]. Among all specialties, only 51% of physicians felt comfortable treating or referring a patient with the Triad [50••].
Athlete and Coach Awareness
Many athletes are not aware of the long-term health consequences of low EA. Among Australian female exercisers ages 18–40 years, 45% of participants did not think that amenorrhea was related to bone health, and 22% of lean sports athletes would not seek treatment if experiencing amenorrhea (compared with 3.2% in non-lean sports athletes) [54]. Among American female high school track athletes, 90% of athletes provided incorrect answers when asked about menstrual irregularity and bone health [55]. Few adolescent girls (7.5%) are aware that not having a menstrual cycle for 6 months increases the risk of getting osteoporosis [56]. Among young adult male and female dancers, only 29% of dancers were aware of the RED-S [57].
Coach awareness was also surveyed to be low (average 2.97 out of 8 possible points) about the Triad [58]. Among National Collegiate Athletic Association Division I, II, and III institutions across the USA, athletic trainers and strength and conditioning specialists were found to have adequate sports nutrition knowledge; however, athletes and coaches were found to have inadequate sports nutrition knowledge [59].
Education—Low Energy Availability
Education helps to prevent and treat low EA by assisting athletes to first understand the etiology of their symptoms. Registered dieticians (with a focus on sports nutrition) and sports medicine specialists can provide education with the use of online resources. Free nutrition handouts from the Collegiate and Professional Sports Dietitians Association for Collegiate are available in https://www.sportsrd.org/downloadable-resources/ [60].
These nutrition handouts can be given to athletes, coaches, athletic trainers, strength coaches, and other allied healthcare members. The handouts include sport-specific athlete nutrition for several sports. Educational interventions for athletes have been successful when counseling and resources have been provided to the athlete, their support network, [61] and include an intervention with a registered dietitian [62]. Education needs to be adapted to all athletes (male and female) of all sports and age levels [8, 63]. It will be important to continue to develop sport-specific education that highlights health and performance consequences [22].
Treatment
It is imperative to address the underlying causes leading to the Triad/RED-S and center treatment on restoring EA by modifying nutrition and exercise [1•, 9]. The goal is to increase energy availability through modifications of nutrition and exercise [1••]. Athletic amenorrhea may be related to caloric restriction [64]. It is recommended to focus on restoration of body weight to resume menses and improve bone health [1••].
Non-pharmacologic Treatment
Non-pharmacologic treatment methods are recommended to encourage healthy nutrition and weight gain in underweight athletes or athletes with low EA [65]. Education about EA (increasing dietary intake and/or decreasing energy expenditure) by a physician and dietitian helps to restore regular menstrual cycles in female collegiate athletes with menstrual disturbances without using pharmacologic intervention [66]. Athletes with a ≥ 5-lb. (2.2 kg) weight gain were twice as likely to resume menses compared with athletes with less weight gain [65]. Arends et al. states that weight gain or an increase in body mass index may be helpful to predict the return of menses, yet may take longer than 1 year to restore regular menstrual cycles [65]. On average in oligo/amenorrheic female athletes, the athletes with spontaneous return of menses tended to have a higher calorie intake than women who stayed oligo/amenorrheic, and menses has proven beneficial for bone health [64].
Nutrition Counseling
A careful nutrition assessment is warranted to ensure adequate energy availability as well as macronutrient intake [67]. Referral to a registered dietician that focuses on sports nutrition is important, as is referral to a sports medicine specialist.
Pharmacologic Treatment
Treatment of amenorrheic female athletes with oral contraception will mask amenorrhea, and Keay et al. report that it does not support bone health and may even exacerbate bone loss by suppressing IGF-1 [66, 68]. Exogenous estrogen replacement in young women can potentially result in premature growth plate closure [65]. Cobb et al. came up with inconclusive results from the first randomized trial to examine if oral contraceptives can protect female athletes ages 18–26 from stress fractures [64]. There are no studies evaluating bisphosphonate use in female athletes with the Triad. Bisphosphonates are not FDA-approved to decrease fracture risk in young athletes, and the 2014 Female Athlete Triad Coalition Consensus Panel recommends that an endocrinologist oversee any consideration of bisphosphonate therapy in a young woman [1••]. Adequate amounts of micronutrients, calcium and vitamin D are recommended for overall bone health [1, 69].
Psychological Treatment
Certain mental health disorders may present with a component of disordered eating or clinically diagnosed eating disorder. Appropriate care with a team consisting of physicians trained to treat mental health disorders (with and without medication), psychiatrist, and psychologist is warranted for patients presenting with the Triad/RED-S. Multidisciplinary care is imperative for the psychological health of athletes. Education of the coaches, parents, and athletic trainers who regularly meet with the athlete is important to reinforce the psychological support needed for health maintenance.
Conclusions
The Female Athlete Triad is a spectrum of low EA (with or without disordered eating), menstrual dysfunction, and low bone mineral density among female athletes. Relative Energy Deficiency in Sport is a complex clinical syndrome referring to impaired physiological functioning (including Triad markers and other systems) due to a relative energy deficit. The Triad has a greater body of evidence and validation, while the RED-S includes male athletes and adds broader context to athletes with disabilities; both seek to expand upon potential health and performance consequences of low EA.
Low EA affects multiple body systems and has serious consequences for health and performance. Early detection with screening tools in a multidisciplinary setting is crucial, yet several challenges exist. Diagnosis can be challenging due to health consequences that are not readily apparent, lack of universal standard for diagnosis of EA, and no single sensitive tool to detect low EA.
Educating medical professionals from a wide range of specialties is necessary in order to appropriately screen and initiate the treatment process. Several screening tools exist, yet consensus is lacking regarding which screening tools are best for assessing athlete’s health risks. The preparticipation physical examination, annual check-ups, and clinic visits for health-related concerns are optimal times to screen for the Triad/RED-S. Screening tools have historically been limited to specific genders and populations. To optimize health in this population, there is a need to advance screening tools with future research.
Further workup is warranted by medical professionals with referral to physicians with specific low EA training (i.e., sports medicine physicians), counseling by registered dieticians, and mental health specialists. It is imperative to address the underlying cause leading to the Triad/RED-S and center treatment on restoring EA through modifications of nutrition and exercise. Awareness and education regarding the Triad/RED-S is needed for athletes, coaches, athletic trainers, and multidisciplinary healthcare professionals.
Change history
12 November 2020
A Correction to this paper has been published: <ExternalRef><RefSource>https://doi.org/10.1007/s40141-020-00303-2</RefSource><RefTarget Address="10.1007/s40141-020-00303-2" TargetType="DOI"/></ExternalRef>
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
•• De Souza M, Nattiv A, Joy E, et al. 2014 Female Athlete Triad Coalition Consensus Statement on treatment and return to play of the female athlete triad. Curr Sports Med Rep. 2014;13(4):219–32. https://doi.org/10.1249/jsr.0000000000000077This article describes the 2014 Female Athlete Triad Coalition Consensus Statement.
Otis C, Drinkwater B, Johnson M, Loucks A, Wilmore J. ACSM Position Stand: the Female Athlete Triad. Medicine and Science in Sports & Exercise. 1997;29(5):i–ix. https://doi.org/10.1097/00005768-199705000-00037.
Yeager K, Agostini R, Nattiv A, Drinkwater B. The female athlete triad: disordered eating, amenorrhea, osteoporosis. Med Sci Sports Exerc. 1993;25(7):775–7. https://doi.org/10.1249/00005768-199307000-00003.
• Nattiv A, Loucks AB, Manore MM, et al. American College of Sports Medicine. American College of Sports Medicine position stand. The female athlete triad. Med. Sci. Sports Exerc. 2007;39:1867–82. https://doi.org/10.1249/mss.0b013e318149f111This article describes the 2007 American College of Sports Medicine position stand on the Female Athlete Triad.
•• Tenforde A, Barrack M, Nattiv A, Fredericson M. Parallels with the Female Athlete Triad in male athletes. Sports Medicine. 2015;46(2):171–82. https://doi.org/10.1007/s40279-015-0411-yThis article compares features of the Female Athlete Triad in Male Athletes.
Kraus E, Tenforde A, Nattiv A, et al. Bone stress injuries in male distance runners: higher modified Female Athlete Triad Cumulative Risk Assessment scores predict increased rates of injury. Br J Sports Med. 2018;53(4):237–42. https://doi.org/10.1136/bjsports-2018-099861.
Statuta S. The female athlete triad, relative energy deficiency in sport, and the male athlete triad. Curr Sports Med Rep. 2020;19(2):43–4. https://doi.org/10.1249/jsr.0000000000000679.
Ackerman K, Holtzman B, Cooper K, et al. Low energy availability surrogates correlate with health and performance consequences of relative energy deficiency in sport. Br J Sports Med. 2018;53(10):628–33. https://doi.org/10.1136/bjsports-2017-098958.
Javed A, Tebben P, Fischer P, Lteif A. Female athlete triad and its components: toward improved screening and management. Mayo Clin Proc. 2013;88(9):996–1009. https://doi.org/10.1016/j.mayocp.2013.07.001.
Gibbs JC, Williams NI, De Souza MJ. Prevalence of individual and combined components of the female athlete triad. Med Sci Sports Exerc. 2013;45:985–96. https://doi.org/10.1249/mss.0b013e31827e1bdc.
•• Mountjoy M, Sundgot-Borgen J, Burke L, et al. The IOC Consensus Statement: beyond the Female Athlete Triad—Relative Energy Deficiency in Sport (RED-S). Br J Sports Med. 2014;48(7):491–7. https://doi.org/10.1136/bjsports-2014-093502This article introduces Relative Energy Deficiency in Sport (RED-S) by the International Olympic Committee in 2014.
Loucks A. Energy balance and body composition in sports and exercise. J Sports Sci. 2004;22(1):1–14. https://doi.org/10.1080/0264041031000140518.
Williams N, Koltun K, Strock N, De Souza M. Female athlete triad and relative energy deficiency in sport. Exerc Sport Sci Rev. 2019;47(4):197–205. https://doi.org/10.1249/jes.0000000000000200.
•• Mountjoy M, Sundgot-Borgen J, Burke L, et al. The IOC relative energy deficiency in sport clinical assessment tool (RED-S CAT). Br J Sports Med. 2015;49(21):1354. https://doi.org/10.1136/bjsports-2015-094873This article introduces the Relative Energy Deficiency in Sport Clinical Assessment Tool (RED-S CAT).
•• Mountjoy M, Sundgot-Borgen J, Burke L, et al. International Olympic Committee (IOC) Consensus Statement on Relative Energy Deficiency in Sport (RED-S): 2018 update. Int J Sport Nutr Exerc Metab. 2018;28(4):316–31. https://doi.org/10.1123/ijsnem.2018-0136This article reviews RED-S and provides current updates from 2018 from the International Olympic Committee.
De Souza M, Williams N, Nattiv A, et al. Misunderstanding the female athlete triad: refuting the IOC Consensus Statement on Relative Energy Deficiency in Sport (RED-S). Br J Sports Med. 2014;48(20):1461–5. https://doi.org/10.1136/bjsports-2014-093958.
Loucks A. Low energy availability in the marathon and other endurance sports. Sports Med. 2007;37(4):348–52. https://doi.org/10.2165/00007256-200737040-00019.
Heikura IA, Uusitalo ALT, Stellingwerff T, Bergland D, Mero AA, Burke LM. Low energy availability is difficult to assess but outcomes have large impact on bone injury rates in elite distance athletes. Int J Sport Nutr Exerc Metab. 2018;28:403–11. https://doi.org/10.1123/ijsnem.2017-0313.
Burke L, Lundy B, Fahrenholtz I, Melin A. Pitfalls of conducting and interpreting estimates of energy availability in free-living athletes. Int J Sport Nutr Exerc Metab. 2018;28(4):350–63. https://doi.org/10.1123/ijsnem.2018-0142.
Murakami H, Kawakami R, Nakae S, Nakata Y, Ishikawa-Takata K, Tanaka S, et al. Accuracy of wearable devices for estimating total energy expenditure. JAMA Intern Med. 2016;176(5):702–3. https://doi.org/10.1001/jamainternmed.2016.0152.
Stubbs R, O’Reilly L, Whybrow S, et al. Measuring the difference between actual and reported food intakes in the context of energy balance under laboratory conditions. Br J Nutr. 2014;111(11):2032–43. https://doi.org/10.1017/s0007114514000154.
Sundgot-Borgen J, Garthe I. Elite athletes in aesthetic and Olympic weight-class sports and the challenge of body weight and body compositions. J Sports Sci. 2011;29(sup1):S101–14. https://doi.org/10.1080/02640414.2011.565783.
Kong P, Harris LM. The sporting body: body image and eating disorder symptomatology among female athletes from leanness focused and nonleanness focused sports. J Psychol. 2015;149:141–60. https://doi.org/10.1080/00223980.2013.846291.
Cain M. Opinion | I was the fastest girl in America, until i joined Nike. Nytimes.com. https://www.nytimes.com/2019/11/07/opinion/nike-running-mary-cain.html. Published 2020.
Para athletics classification explained. International Paralympic Committee. https://www.paralympic.org/news/para-athletics-classification-explained. Published 2020.
Logue D, Madigan S, Melin A, et al. Low energy availability in athletes 2020: an updated narrative review of prevalence, risk, within-day energy balance, knowledge, and impact on sports performance. Nutrients. 2020;12(3):835. https://doi.org/10.3390/nu12030835.
Lane H, Smith-Ryan K, Registar-Mihalik O. Prevalence of low energy availability in competitively trained male endurance athletes. Medicina (B Aires). 2019;55(10):665. https://doi.org/10.3390/medicina55100665.
Beals K, Hill A. The prevalence of disordered eating, menstrual dysfunction, and low bone mineral density among US collegiate athletes. Int J Sport Nutr Exerc Metab. 2006;16(1):1–23. https://doi.org/10.1123/ijsnem.16.1.1.
Tenforde A, Carlson J, Chang A, et al. Association of the Female Athlete Triad Risk Assessment Stratification to the development of bone stress injuries in collegiate athletes. Am J Sports Med. 2016;45(2):302–10. https://doi.org/10.1177/0363546516676262.
Fagerberg P. Negative consequences of low energy availability in natural male bodybuilding: a review. Int J Sport Nutr Exerc Metab. 2018;28(4):385–402. https://doi.org/10.1123/ijsnem.2016-0332.
Burke L, Close G, Lundy B, Mooses M, Morton J, Tenforde A. Relative energy deficiency in sport in male athletes: a commentary on its presentation among selected groups of male athletes. Int J Sport Nutr Exerc Metab. 2018;28(4):364–74. https://doi.org/10.1123/ijsnem.2018-0182.
Blauwet C, Brook E, Tenforde A, et al. Low energy availability, menstrual dysfunction, and low bone mineral density in individuals with a disability: implications for the para athlete population. Sports Med. 2017;47(9):1697–708. https://doi.org/10.1007/s40279-017-0696-0.
Shimizu Y, Mutsuzaki H, Tachibana K, Hotta K, Wadano Y. Investigation of the Female Athlete Triad in Japanese elite wheelchair basketball players. Medicina (B Aires). 2019;56(1):10. https://doi.org/10.3390/medicina56010010.
Tenforde A, Brook E, Broad E, et al. Prevalence and anatomical distribution of bone stress injuries in the elite para athlete. Am J Phys Med Rehabil. 2019;98(11):1036–40. https://doi.org/10.1097/phm.0000000000001287.
Brook E, Tenforde A, Broad E, et al. Low energy availability, menstrual dysfunction, and impaired bone health: a survey of elite para athletes. Scand J Med Sci Sports. 2019;29(5):678–85. https://doi.org/10.1111/sms.13385.
Elliott-Sale K, Tenforde A, Parziale A, Holtzman B, Ackerman K. Endocrine effects of relative energy deficiency in sport. Int J Sport Nutr Exerc Metab. 2018;28(4):335–49. https://doi.org/10.1123/ijsnem.2018-0127.
Loucks A. Energy availability, not body fatness, regulates reproductive function in women. Exerc Sport Sci Rev. 2003;31(3):144–8. https://doi.org/10.1097/00003677-200307000-00008.
Koehler K, Hoerner N, Gibbs J, et al. Low energy availability in exercising men is associated with reduced leptin and insulin but not with changes in other metabolic hormones. J Sports Sci. 2016;34(20):1921–9. https://doi.org/10.1080/02640414.2016.1142109.
Andreoli A, Monteleone M, Van Loan M, et al. Effects of different sports on bone density and muscle mass in highly trained athletes. Med Sci Sports Exerc. 2001;33:507–11. https://doi.org/10.1097/00005768-200104000-00001.
Ackerman KE, Nazem T, Chapko D, Russell M, Mendes N, Taylor AP, et al. Bone microarchitecture is impaired in adolescent amenorrheic athletes compared with eumenorrheic athletes and nonathletic controls. J Clin Endocrinol Metab. 2011;96:3123–33. https://doi.org/10.1210/jc.2011-1614.
Ackerman KE, Cano Sokoloff N, DE Nardo MG, et al. Fractures in relation to menstrual status and bone parameters in young athletes. Med Sci Sports Exerc. 2015;47:1577–86. https://doi.org/10.1249/mss.0000000000000574.
O’Donnell E, Goodman JM, Harvey PJ. Clinical review: cardiovascular consequences of ovarian disruption: a focus on functional hypothalamic amenorrhea in physically active women. J Clin Endocrinol Metab. 2011;96:3638–48. https://doi.org/10.1210/jc.2011-1223.
Sarin HV, Gudelj I, Honkanen J, Ihalainen JK, Vuorela A, Lee JH, et al. Molecular pathways mediating immunosuppression in response to prolonged intensive physical training, low-energy availability, and intensive weight loss. Front Immunol. 2019;10. https://doi.org/10.3389/fimmu.2019.00907.
Petkus D, Murray-Kolb L, De Souza M. The unexplored crossroads of the female athlete triad and Iron deficiency: a narrative review. Sports Med. 2017;47(9):1721–37. https://doi.org/10.1007/s40279-017-0706-2.
Chang C, Putukian M, Aerni G, Diamond A, Hong G, Ingram Y, et al. Mental health issues and psychological factors in athletes: detection, management, effect on performance and prevention: American Medical Society for Sports Medicine Position Statement—Executive Summary. Br J Sports Med. 2019;54(4):216–20. https://doi.org/10.1136/bjsports-2019-101583.
Sundgot-Borgen J, Meyer NL, Lohman TG, Ackland TR, Maughan RJ, Stewart AD, et al. How to minimise the health risks to athletes who compete in weight-sensitive sports review and position statement on behalf of the Ad Hoc Research Working Group on Body Composition, Health and Performance, under the auspices of the IOC Medical Commission. Br J Sports Med. 2013;47(16):1012–22. https://doi.org/10.1136/bjsports-2013-092966.
Mitchell JJ, Robert-Mccomb JJ. (2014) Screening for disordered eating and eating disorders in female athletes. In: Robert-McComb JJ, Norman RL, Zumwalt M (eds) The Active Female. Springer, New York. https://doi.org/10.1007/978-1-4614-8884-2_13.
Preparticipation Physical Evaluation (PPE). AAP.org. https://www.aap.org/en-us/advocacy-and-policy/aap-health-initiatives/Pages/PPE.aspx. Published 2020.
•• Holtzman B, Tenforde A, Parziale A, Ackerman K. Characterization of risk quantification differences using Female Athlete Triad Cumulative Risk Assessment and Relative Energy Deficiency in Sport Clinical Assessment Tool. Int J Sport Nutr Exerc Metab. 2019;29(6):569–75. https://doi.org/10.1123/ijsnem.2019-0002This article compares the risk assessment tools the Female Athlete Triad Cumulative Risk Assessment Tool and the Relative Energy Deficiency in Sport Clinical Assessment Tool with low, medium, and high risk for return to play.
•• Curry E, Logan C, Ackerman K, McInnis K, Matzkin E. Female Athlete Triad awareness among multispecialty physicians. Sports Med Open. 2015;1(1). https://doi.org/10.1186/s40798-015-0037-5This article assesses multispecialty physician awareness of the Female Athlete Triad and compares awareness among specialties.
Rumball JS, Lebrun CM. Preparticipation physical examination: selected issues for the female athlete. Clin J Sport Med. 2004;14(3):153–60. https://doi.org/10.1097/00042752-200405000-00008.
• Melin A, Tornberg ÅB, Skouby S, et al. The LEAF questionnaire: a screening tool for the identification of female athletes at risk for the female athlete triad. Br J Sports Med. 2014;48(7):540–5. https://doi.org/10.1136/bjsports-2013-093240This article details the LEAF questionnaire (LEAF-Q), a screening tool to assess Female Athlete Triad risk factors.
Ljungqvist A, Jenoure P, Engebretsen L, Alonso JM, Bahr R, Clough A, et al. The International Olympic Committee (IOC) Consensus Statement on periodic health evaluation of elite athletes March 2009. Br J Sports Med. 2009;43(9):631–43. https://doi.org/10.1136/bjsm.2009.064394.
Miller S, Kukuljan S, Turner A, van der Pligt P, Ducher G. Energy deficiency, menstrual disturbances, and low bone mass: what do exercising Australian women know about the female athlete triad? Int J Sport Nutr Exerc Metab. 2012;22(2):131–8. https://doi.org/10.1123/ijsnem.22.2.131.
Feldmann J, Belsha J, Eissa M, Middleman A. Female adolescent athletes’ awareness of the connection between menstrual status and bone health. J Pediatr Adolesc Gynecol. 2011;24(5):311–4. https://doi.org/10.1016/j.jpag.2011.05.011.
Martin J, Coviak C, Gendler P, Kim K, Cooper K, Rodrigues-Fisher L. Female adolescentsʼ knowledge of bone health promotion behaviors and osteoporosis risk factors. Orthop Nurs. 2004;23(4):235–44. https://doi.org/10.1097/00006416-200407000-00008.
Keay N, Overseas A, Francis G. Awareness and indicators of low energy availability in male and female dancers. https://www.medrxiv.org/content/10.1101/2020.06.28.20141580v2. Published 2020.
Brown K, Wengreen H, Beals K. Knowledge of the female athlete triad, and prevalence of triad risk factors among female high school athletes and their coaches. J Pediatr Adolesc Gynecol. 2014;27(5):278–82. https://doi.org/10.1016/j.jpag.2013.11.014.
Torres-McGehee TM, Pritchett KL, Zippel D, et al. Sports nutrition knowledge among collegiate athletes, coaches, athletic trainers, and strength and conditioning specialists. J Athl Train. 2012;47:205–11. https://doi.org/10.4085/1062-6050-47.2.205.
Downloadable Resources - CPSDA | SportsRd.org | Collegiate & Professional Sports Dietitians Association. CPSDA | SportsRd.org | Collegiate & Professional Sports Dietitians Association. https://www.sportsrd.org/downloadable-resources/. Published 2020.
Martinsen M, Bahr R, Borresen R, Holme I, Pensgaard A, Sundgot-Borgen J. Preventing eating disorders among young elite athletes. Med Sci Sports Exerc. 2014;46(3):435–47. https://doi.org/10.1249/mss.0b013e3182a702fc.
Valliant MW, Emplaincourt HP, Wenzel RK, et al. Nutrition education by a registered dietitian improves dietary intake and nutrition knowledge of a NCAA female volleyball team. Nutrients. 2012;4:506–16. https://doi.org/10.3390/nu4060506.
•• Ackerman K, Stellingwerff T, Elliott-Sale K, et al. #REDS (Relative Energy Deficiency in Sport): time for a revolution in sports culture and systems to improve athlete health and performance. Br J Sports Med. 2020;54(7):369–70. https://doi.org/10.1136/bjsports-2019-101926This recent 2020 editorial article calls for a revolution in sports culture through a paradigm shift, and identifies several needs for the prevention, diagnosis, and treatment of RED-S to improve athlete health.
Cobb KL, Bachrach LK, Sowers M, et al. The effect of oral contraceptives on bone mass and stress fractures in female runners. Med Sci Sports Exerc. 2007;39:1464–73. https://doi.org/10.1249/mss.0b013e318074e532.
Arends J, Cheung M, Barrack M, Nattiv A. Restoration of menses with nonpharmacologic therapy in college athletes with menstrual disturbances: a 5-year retrospective study. Int J Sport Nutr Exerc Metab. 2012;22(2):98–108. https://doi.org/10.1123/ijsnem.22.2.98.
Keay N. 2018 UPDATE: relative energy deficiency in sport (RED-S) | BJSM blog-social media’s leading SEM voice. British Journal of sports medicine blog. https://blogs.bmj.com/bjsm/2018/05/30/2018-update-relative-energy-deficiency-in-sport-red-s/. published 2018.
Tenforde AS, Carlson JL, Sainani KL, et al. Sport and triad risk factors influence bone mineral density in collegiate athletes. MSSE. 2018;50(12):2536–43. https://doi.org/10.1249/mss.0000000000001711.
Liu S. Effect of oral contraceptives and hormone replacement therapy on bone mineral density in premenopausal and perimenopausal women: a systematic review. Br J Sports Med. 2006;40(1):11–24. https://doi.org/10.1136/bjsm.2005.020065.
Thein-Nissenbaum J, Hammer E. Treatment strategies for the female athlete triad in the adolescent athlete: current perspectives. Open Access J Sports Med. 2017;8:85–95. https://doi.org/10.2147/oajsm.s100026.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Brandee Waite has served on the medical board for level 42 AI. Alexandra Warrick and Marcia Faustin do not have any potential conflicts of interest to disclose.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The original version of this article unfortunately contained a mistake in the Title. “Relative Energy Deficiency in Syndrome (RED-S)” should be presented as “Relative Energy Deficiency in Sport (RED-S)”.
This article belongs to the Topical Collection on Sports Medicine Rehabilitation
Rights and permissions
About this article
Cite this article
Warrick, A., Faustin, M. & Waite, B. Comparison of Female Athlete Triad (Triad) and Relative Energy Deficiency in Sport (RED-S): a Review of Low Energy Availability, Multidisciplinary Awareness, Screening Tools and Education. Curr Phys Med Rehabil Rep 8, 373–384 (2020). https://doi.org/10.1007/s40141-020-00296-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40141-020-00296-y