Abstract
The computed tomography angiography (CTA) Spot Sign is an effective means of predicting hematoma expansion (HE) in the context of spontaneous intracerebral hemorrhage (ICH). We investigated whether continuous CTA source images could differentiate the Spot Sign and blood vessels in the hematoma, and whether it would improve Spot Sign accuracy as an HE predictor. We screened for the presence of CTA Spot Sign in individuals affected by spontaneous ICH within 24 h of symptom development. Based on our findings, we determined the sensitivity, specificity, and positive/negative predictive values of this sign as a predictor of HE both on its own and following the exclusion of blood vessels. In addition, a receiver-operating characteristic approach was used to assess the accuracy of Spot Sign with and without elimination of vascular interference. A total of 265 patients were included in this study. The Spot Sign was observed in 100 patients, including in 29 patients wherein it was confirmed to be blood vessels as determined based upon continuous CTA source images. With respect to predicting HE, Spot Sign sensitivity, specificity, positive predictive values, and negative predictive values were 57%, 71%, 48% and 78%, respectively. Following the exclusion of blood vessels, these values were 57%, 87%, 68% and 81%, respectively. Spot Sign area under the curve after excluding blood vessels was 0.718, which was higher than that of the Spot Sign (0.638). After continuous CTA, source images are used to exclude blood vessels in the hematoma, the Spot Sign is thus more accurate in predicting HE.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Spontaneous ICH is the least treatable form of stroke, making up 10–15% of stroke cases in the world [1]. In recent years, several studies have been conducted in an effort to improve outcomes, but the mortality rate is still high, with just 12–39% of survivors remaining able to live on their own after 6 months [2]. HE is linked to negative ICH patient outcomes, and this can potentially be modified if predicted or identified early [3, 4]. Therefore, clarifying why radiological findings are predictive of HE may be of clinical value for ICH patients [4]. In several previous studies, the Spot Sign on CTA had been shown to be an effective indicator of HE [5,6,7]. The 2015 AHA/ASA Guideline also posit that the CTA can help to identify patients at risk for HE [8]. This sign was found to be associated with higher risk of intraoperative bleeding, postoperative bleeding, as well as to large remainder hematoma volumes in ICH patients via hematoma evacuation [9]. This sign has also been shown to predict worse mortality and outcomes in IHC patients [10, 11]. Generally, the Spot Sign is defined as at least 1 focus of contrast pooling within the ICH: high Hounsfield unit (HU) value (> 120); and any size and shape [10, 12]. The Spot Sign is often considered to be the enhancement point that is formed via leakage of contrast medium in hematomas [5]. However, we often find that these enhancement points might also be the cross section of blood vessels or an aneurysm in the hematoma, potentially affecting Spot Sign accuracy. Continuous CTA source images can better identify blood vessels in hematomas, enhancing Spot Sign sensitivity and specificity as a means of predicting HE. We, therefore, performed a retrospective cohort study to explore factors affecting Spot Sign accuracy as an HE predictor.
Materials and methods
Study design and patients
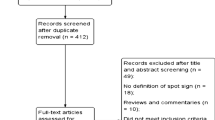
We retrospectively analyzed cases which were recorded in the ICH database between March 2017 and September 2018, Northern Jiangsu People’s Hospital. The Biomedical Ethics Committee of Northern Jiangsu People’s Hospital approved this study. Inclusion criteria: (1) spontaneous ICH as confirmed via CT scanning; (2) CT and CTA performed upon admission and no more than 24 h following symptom development; (3) age ≥ 18 years; (4) follow-up CT scan was conducted within 24 h after CTA. Exclusion criteria: (1) ICH caused by moyamoya disease, infarction, tumor or trauma; (2) surgical evacuation prior to follow-up scan; (3) unavailable initial CT or follow-up CT; (4) simple intraventricular or subarachnoid hemorrhage. Spontaneous ICH patients underwent treatment in a devoted stroke unit in a manner consistent with the latest guidelines [13, 14].
Clinical data
We gathered basic patient data including age, gender, blood pressure upon admission, time between symptom development and CT, anticoagulant use, medical history (factors including previous strokes, smoking history, diabetes, or hypertension), as well as available laboratory data including platelet levels, activated partial thromboplastin time, international normalized ratios, prothrombin times, fibrinogen levels, and calcium levels.
Imaging acquisition
The CT scans which use a 64-slice Discovery CT750HD scanner were conducted based upon standard clinical parameters using contiguous 5-mm axial slices from the skull base to vertex. For the CTA, 50–100 mL of iodixanol injection (270 mg I/mL) was intravenously injected (5 mL/s) using a power injector as follows: 80 kVp; 375 mA; slice thickness, 0.625 mm. Within 24 h of CTA, a follow-up CT scan was conducted to assess hematoma size.
Imaging marker detection
The images were obtained for neuroradiologists’ further evaluation. Two independent individuals experienced in reading such imaged independently assessed images for CTA Spot Sign. Hemorrhages were identified based on their locations in the basal ganglia, brain lobe, brain stem, or cerebellum. The continuous CTA source images were used to assess whether the Spot Sign was due to a cross section of a blood vessel or aneurysm in the hematoma. The specific criteria used for this determination were as follows: if the Spot Sign is of a continuous linear density extending from the surface of the brain or ventricle into the hematoma, it is considered a blood vessel [15]. During the rating process, the two independent neuroradiologists had been blinded to both clinical details and other scans from the same patients. Disagreements between readers were resolved via discussion. We further evaluated other HE predictors, such as satellite sign, blend sign, black hole sign, margin irregularity, and hematoma density heterogeneity as previously described [16,17,18,19,20].
Hematoma volume measurement
The ABC/2 approach was used to determine hematoma volume, with A being the largest diameter of the largest hematoma image, B being the largest diameter perpendicular to A, and C being the hematoma vertical depth [21]. HE was detected based upon hematoma relative growth > 33% or hematoma absolute growth > 6 mL upon follow-up imaging [5, 22].
Statistical analysis
Excel 2016 and SPSS v25.0 were used for all analyses. We compared all collected baseline information between patients. Normal distribution data were present in mean ± standard deviation (SD); non-normal distribution data were present in median and maximum and minimum. Continuous variables were compared via F tests and t tests. Discrete variables are instead given as percentages (%) and were compared via χ2 tests. Spot Sign odds ratios (ORs) and 95% confidence intervals (CIs) were established via multivariable logistic regression analyses. The variables incorporated into this analysis were those with a P < 0.05 in a univariate analysis, and those reported to be linked to HE in past research. The k values were used to analyze the inter-reader reliability. Statistical significance was assumed if P < 0.05 (Fig. 1).
Illustration of CTA Spot Sign and blood vessels in the hematoma. a1 The baseline CT image in a patient with basal ganglia hemorrhage. a2–a17 Continuous CTA source images showed the Spot Sign did not extend beyond the hematoma. A small focus of enhancement (white arrow) should be interpreted as a “Spot Sign”. a18 The 24-h follow-up CT image showed the HE. b1 The baseline CT image in a patient with lobe hemorrhage. b2–b17 Continuous CTA source images showed the Spot Sign extended beyond the hematoma. A small focus of enhancement (white arrow) should not be interpreted as a “Spot Sign”. b18 The 24-h follow-up CT image showed no HE
Results
A total of 265 spontaneous ICH patients (185 men and 80 women) were included in our study. In this study, the time interval from spontaneous ICH onset to initial CT was 2.94 ± 2.73 h. The mean age of these patients was 62.89 ± 12.93 years. The mean baseline hematoma volume was 22.37 ± 23.11 mL. Hematoma locations included the basal ganglia (191, 72.08%), lobar (47, 17.74%), cerebellum (15, 5.66%), and brain stem (12, 4.52%). A total of 85 out of 265 patients experienced HE, with a mean volume of 29.55 ± 29.51 mL. Baseline clinical characteristics of the HE and non-HE groups are compiled in Table 1. We detected the Spot Sign in 100 patients, including 29 patients in whom it was confirmed to be the result of a blood vessel using continuous CTA source images. Compared to patients without HE, a higher proportion of patients with HE exhibited the Spot Sign. Inter-observer reliability for Spot Sign and hematoma-crossing blood vessels was good between the two neuroradiologists (k = 0.943 and 0.925). The univariate and multivariate logistic regression analyses are shown in Tables 2 and 3, respectively. In the univariate analysis, systolic blood pressure at admission, history of diabetes mellitus, time to first CT scan, initial hematoma volume, irregular shape, heterogeneous density, satellite sign, black hole sign, Spot Sign, and the Spot Sign after excluding blood vessels were all associated with HE. Before excluding blood vessels in the hematoma, a multivariate logistic regression analysis determined that having a history of diabetes mellitus (OR 3.631; 95% CI of OR 1.638–8.050; P = 0.002), the time to first CT scan(OR 0.751; 95% CI of OR 0.638–0.884; P = 0.001), the irregular shape(OR 2.412; 95% CI of OR 1.209–4.810; P = 0.012), heterogeneous density (OR 2.125; 95% CI of OR 1.098–4.112; P = 0.025), and the satellite sign (OR 1.983; 95% CI of OR 1.021–3.853; P = 0.043) independently predicted HE. After excluding blood vessels in the hematoma, the multivariate logistic regression analysis showed that a history of diabetes (OR 3.474; 95% CI of OR 1.547–7.798; P = 0.003), the time to first CT scan (OR 0.785; 95% CI of OR 0.675–0.914; P = 0.002), the satellite sign (OR 2.442; 95% CI of OR 1.270–4.694; P = 0.007), and the Spot Sign after excluding blood vessels (OR 7.112; 95% CI of OR 3.621–13.970; P < 0.001) were all independent predictors of HE.
Spot Sign was associated with sensitivity, specificity, positive predictive values, and negative predictive values of 57%, 71%, 48%, and 78%, respectively, as a means of HE detection. When blood vessels were excluded, these same predictive values were 57%, 87%, 68%, and 81%, respectively. The accuracy of other predictors is detailed in Table 4. Results of ROC curve analyses for these two assessments of Spot Sign as a predictor of HE are shown in Fig. 2.
Discussion
Contrast extravasation that is ongoing in CTA source images can be identified as a Spot Sign. In the present study, we detected a Spot Sign incidence rate of roughly 27%, consistent with previous studies identifying a rate between 18 and 72% [23, 24]. The Spot Sign which has been hypothesized to reflect active extravasation of the contrast was termed as a visual manifestation of persistent bleeding [12, 25]. Wada et al. were the first to suggest that there was an association between Spot Sign and the extent of hematoma progression [26]. This was consistent with our finding that there was an association between Spot Sign presence and an elevated HE risk. Similarly, Demchuk et al. [5] also found this Spot Sign to predict HE, and to be a valuable criteria for future trials of hemostatic therapy in spontaneous ICH patients.
Although the CTA Spot Sign is a good predictor of HE, the rates of detection were different in previous studies. Demchuk et al. found the Spot Sign sensitivity, specificity, positive predictive values, and negative predictive values to be 51%, 85%, 61%, and 78%, respectively [5]. In contrast, Wada et al. found these same values to be 91%, 89%, 77%, and 96%, respectively, [25] while Han et al. found them to be 57.38%, 90.48%, 74.47%, and 81.43%, respectively [6]. In a previous meta-analysis of Spot Sign, Du et al. calculated a pooled sensitivity of 53% and a specificity of 88% [27]. There may be a range of causes underlying the differences in sensitivity and specificity in these previous studies. For one, the Spot Sign may be affected by different hematoma volumes. Wang et al. found that when the hematoma volumes are > 30 mL; the Spot Sign accuracy for predicting HE is higher [28]. Dowlatshahi et al. found that when the hematoma volumes are small, the probability of Spot Sign is low as is the HE risk [29]. Second, the different timing of scans in previous studies may have yielded different predictive accuracies for the CTA Spot Sign [30]. Ciura et al. found that incorporating a 90-s delay during CTA was sufficient to enhance Spot Sign sensitivity as an HE predictor [31]. Third, Spot Sign positive predictive value for HE decreases as the ICH onset-to-CTA time increases [32]. Finally, the Spot Sign could actually be a cross section of blood vessel or aneurysm in hematoma, which also is one of the possible causes. We differentiated between blood vessels and contrast extravasation in the hematoma using continuous CTA source images, yielding increased Spot Sign specificity, positive predictive values, and negative predictive values of 48%, 78–87%, 68%, and 81%, respectively. At the same time, our study also found that density heterogeneity, irregular shape, satellite sign, and black hole sign can also all predict the expansion of hematoma, consistent with previous work. For example, Blacquiere et al. found that density heterogeneity and irregular shape are associated with HE at 24 h [17]. Li et al. found black hole sign to be predictive of the expansion of hematoma [19]. Zhiyuan et al. found the satellite sign to be predictive of the expansion of hematoma [33]. A multiple indicator-based combined diagnostic strategy can thus be implemented to improve the accuracy of the prediction of HE in the future.
Our study is limited owing to its retrospective nature and single center design. Moreover, the sample size was relatively limited. In addition, the symptom onset-to-CTA time was relatively long, potentially influencing the predictive accuracy of this indicator. Finally, due to CT equipment and subsequent processing, some blood vessels or aneurysm in the hematoma still cannot be identified. To address these issues, future multicenter studies with larger sample populations, better CT machinery/subsequent processing, and a briefer period of time between symptom onset and CTA will be needed.
Conclusions
In summary, the CTA Spot Sign is an effective indicator for predicting the expansion of hematomas in patients with ICH, providing an avenue for defining the basis of patient treatment. Previous studies have detected variations in the utility, sensitivity, and specificity of Spot Sign for HE prediction, potentially for a range of reasons. One such reason is that the cross section of blood vessels or aneurysms in the hematoma can be mistaken for Spot Signs. In our study, a continuous CTA source images silhouette technique was used to distinguish the blood vessels from the hematoma, which improved the accuracy of the Spot Sign prediction for HE and thus increased the value of the Spot Sign in clinical contexts.
References
Caplan LR (2009) Intracerebral haemorrhage. Lancet 373(9675):1632–1644
van Asch CJ, Luitse MJ, Rinkel GJ et al (2010) Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: a systematic review and meta-analysis. Lancet Neurol 9(2):167–176
Brouwers HB, Chang Y, Falcone GJ et al (2014) Predicting hematoma expansion after primary intracerebral hemorrhage. Jama Neurol 71(2):158–164
Brouwers HB, Greenberg SM (2013) Hematoma expansion following acute intracerebral hemorrhage. Cerebrovasc Dis 35(3):195–201
Demchuk AM, Dowlatshahi D, Rodriguez-Luna D et al (2012) Prediction of haematoma growth and outcome in patients with intracerebral haemorrhage using the CT-angiography Spot Sign (PREDICT): a prospective observational study. Lancet Neurol 11(4):307–314
Han JH, Lee JM, Koh EJ et al (2014) The Spot Sign predicts hematoma expansion, outcome, and mortality in patients with primary intracerebral hemorrhage. J Korean Neurosurg Soc 56(4):303–309
Brouwers HB, Mcnamara KA, Ayres AM et al (2012) CTA Spot Sign predicts hematoma expansion in patients with delayed presentation after intracerebral hemorrhage. Neurocrit Care 17(3):421–428
Hemphill J C, Greenberg S M, Anderson C S et al (2015) Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the America Heart Association/American Stroke Association. Stroke: STR. 0000000000000069
Brouwers HB, Raffeld MR, Nieuwenhuizen KMV et al (2011) CT angiography Spot Sign in intracerebral hemorrhage predicts active bleeding during surgery. Neurology 83(10):883
Almandoz JED, Yoo AJ, Stone MJ et al (2009) Systematic characterization of the computed tomography angiography Spot Sign in primary intracerebral hemorrhage identifies patients at highest risk for hematoma expansion the Spot Sign score. Stroke 40(9):2994
Romero JM, Brouwers HB, Lu J et al (2013) Prospective validation of the computed tomographic angiography Spot Sign score for intracerebral hemorrhage. Stroke 44(11):3097–3102
Brouwers HB, Goldstein JN, Romero JM et al (2012) Clinical applications of the computed tomography angiography Spot Sign in acute intracerebral hemorrhage: a review. Stroke 43(12):3427–3432
Dixit D, Thomas Z (2015) Letter by Dixit and Thomas regarding article, “Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: a Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association”. Stroke J Cereb Circ 46(11):5844–5857
Steiner T, Al-Shahi SR, Beer R et al (2015) European Stroke Organisation (ESO) guidelines for the management of spontaneous intracerebral hemorrhage. Int J Stroke 9(7):840–855
Gazzola S, Aviv RI, Gladstone DJ et al (2008) Vascular and nonvascular mimics of the CT angiography “Spot Sign” in patients with secondary intracerebral hemorrhage. Stroke 39(4):1177–1183
Barras CD, Tress BM, Christensen S et al (2009) Density and shape as CT predictors of intracerebral hemorrhage growth. Stroke J Cereb Circ 40(4):1325
Blacquiere D, Demchuk AM, Al-Hazzaa M et al (2015) Intracerebral hematoma morphologic appearance on noncontrast computed tomography predicts significant hematoma expansion. Stroke 46(11):3111–3116
Li Q, Zhang G, Huang YJ et al (2015) Blend sign on computed tomography: novel and reliable predictor for early hematoma growth in patients with intracerebral hemorrhage. Stroke 46(8):2119
Li Q, Zhang G, Xiong X et al (2016) Black hole sign: novel imaging marker that predicts hematoma growth in patients with intracerebral hemorrhage. Stroke 47(7):1777–1781
Shimoda Y, Ohtomo S, Arai H et al (2017) Satellite sign: a poor outcome predictor in intracerebral hemorrhage. Cerebrovasc Dis 44(3–4):105–112
Kothari RU, Brott T, Broderick JP et al (1996) The ABCs of measuring intracerebral hemorrhage volumes. Stroke 27(8):1304–1305
Dowlatshahi D, Demchuk AM, Flaherty ML et al (2011) Defining hematoma expansion in intracerebral hemorrhage: relationship with patient outcomes. Neurology 76(14):1238–1244
Li N, Wang Y, Wang W et al (2011) Contrast extravasation on computed tomography angiography predicts clinical outcome in primary intracerebral hemorrhage: a prospective study of 139 cases. Stroke J Cereb Circ 42(12):3441–3446
Rodriguez-Luna D, Rubiera M, Ribo M et al (2011) Ultraearly hematoma growth predicts poor outcome after acute intracerebral hemorrhage. Neurology 77(17):1599–1604
Dowlatshahi D, Hogan MJ, Sharma M et al (2013) Ongoing bleeding in acute intracerebral haemorrhage. Lancet 381(9861):152
Wada R, Aviv RI, Fox AJ et al (2007) CT angiography “Spot Sign” predicts hematoma expansion in acute intracerebral hemorrhage. Stroke 38(4):1257
Du FZ, Jiang R, Gu M et al (2014) The accuracy of Spot Sign in predicting hematoma expansion after intracerebral hemorrhage: a systematic review and meta-analysis. PLoS One 9(12):e115777
Wang YH, Fan JY, Luo GD et al (2011) Hematoma volume affects the accuracy of computed tomographic angiography ‘Spot Sign’ in predicting hematoma expansion after acute intracerebral hemorrhage. Eur Neurol 65:150–155
Dowlatshahi D, Yogendrakumar V, Aviv RI et al (2016) Small intracerebral hemorrhages have a low Spot Sign prevalence and are less likely to expand. Int J Stroke 11(2):191
Tsukabe A, Watanabe Y, Tanaka H et al (2014) Prevalence and diagnostic performance of computed tomography angiography Spot Sign for intracerebral hematoma expansion depend on scan timing. Neuroradiology 56(12):1039–1045
Ciura VA, Brouwers HB, Pizzolato R et al (2014) Spot Sign on 90 second delayed CTA improves sensitivity for hematoma expansion and mortality: a prospective study. Stroke J Cereb Circ 45(11):3293
Dowlatshahi D, Brouwers HB, Demchuk AM et al (2016) Predicting intracerebral hemorrhage growth with the Spot Sign: the effect of onset-to-scan time Stroke J Cereb Circ 47(3):695
Yu Z, Zheng J, Ali H et al (2017) Significance of satellite sign and Spot Sign in predicting hematoma expansion in spontaneous intracerebral hemorrhage. Clin Neurol Neurosurg 162:67–71
Acknowledgements
The largest acknowledgment goes to the patients who participated in this study and as well as to everyone who contributed to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of our institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pan Yi and Min Xu contributed equally to this work; they are considered as co-first authors.
Rights and permissions
About this article
Cite this article
Yi, P., Xu, M., Chen, P. et al. Eliminating vascular interference from the Spot Sign contributes to predicting hematoma expansion in individuals with spontaneous cerebral hemorrhages. Acta Neurol Belg 121, 521–528 (2021). https://doi.org/10.1007/s13760-019-01244-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-019-01244-x