Abstract
Objective
The Scatchard plot of anti-insulin antibodies is curvilinear, indicating heterogeneity in binding sites. However, the relationship between bound insulin (B) and free insulin (F) in patients with anti-insulin antibodies has not yet been elucidated. This study aimed to determine this relationship.
Methods
We studied two insulin-treated patients with diabetes who had high titers of anti-insulin antibodies. The B and F levels were measured using daily blood samples. Assuming that the law of mass action is applicable to the reactions between insulin and anti-insulin antibody forms, we plotted the bound-to-free ratio (B/F) vs. B using patient data. We also performed an equilibrium binding assay in vitro.
Results
Some of the B/F vs. B plots of the daily variation showed an approximately linear relationship, while the Scatchard plots of in vitro data became curvilinear.
Conclusion
Our study suggests that the one-site (high-affinity site) of anti-insulin antibodies accounts, for the most part, for insulin pharmacokinetics within physiological insulin concentrations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The equilibrium binding assay [1] is widely used to quantify and characterize anti-insulin antibodies. In this assay, insulin is added to deinsulinized sera at various concentrations in vitro, and the affinity and capacity of anti-insulin antibodies are calculated based on bound insulin (B) and free insulin (F). The Scatchard plot, which shows the bound-to-free ratio (B/F) vs. B, is curvilinear for anti-insulin antibodies, indicating heterogeneity in binding sites [1, 2]. However, the relationship between B and F in patients with anti-insulin antibodies has not yet been clarified in detail.
The law of mass action should apply to the reactions between insulin and anti-insulin antibodies [3]. If anti-insulin antibodies have a single binding site, the Scatchard plot shows a straight line, following the equation [3, 4]:
where Bmax is the binding capacity and Ka is the affinity constant.
When there are ≥ 2 binding sites, a nonlinear relationship is obtained, following the equation [4]:
This equation can be transformed into:
Assuming that the quantity and characterization of anti-insulin antibodies remains constant and the reaction of insulin and anti-insulin antibodies is at equilibrium in vivo, the relationship between B and F is represented by the equation derived from the law of mass action. Since insulin is continuously produced and used, the reaction cannot be at complete equilibrium in practice. However, the reaction proceeds toward equilibrium. Therefore, samples of B and F should be distributed according to the relationship in Eq. 1. Based on this hypothesis, we evaluated the relationship between B and F in vivo.
Materials and methods
Patients
Two insulin-treated patients with diabetes, who had high titers of anti-insulin antibodies, were included in this study. The criteria of high titer of anti-insulin antibodies is unclear in general. A past study reported that it was difficult to perform Scatchard analysis when 125I-Insulin binding rate ≤ 50% [5]. Therefore, to perform the analysis we selected patients who had 125I-Insulin binding rate ≥ 70%. Written informed consent was obtained from the patients. These patients had postprandial hyperglycemia but no apparent hypoglycemic episodes, and were admitted to Kanazawa University Hospital (Kanazawa, Japan). Table 1 provides the clinical information of the two patients. Patient 1 had a low titer of glutamic acid decarboxylase (GAD) antibody (2.0 U/mL). He had a history of insulin allergy and tested positive for insulin-specific IgE antibody. His anti-insulin antibodies had not been tested before admission. He was treated for hypothyroidism with levothyroxine 75 μg, but had no thyroid autoantibodies. Patient 2 had received insulin therapy for 9 years, and his anti-insulin antibodies were detected 7 years ago (125I-Insulin binding rate 26.7%). He had subclinical hypothyroidism but no thyroid autoantibodies. Neither patient had taken sulfhydryl-containing drugs or other drugs, reportedly associated with insulin autoimmune syndrome, and had other autoimmune antibodies. Their medical history and the absence of hypoglycemic episodes suggested their anti-insulin antibodies were caused by exogenous insulin therapy.
Anti-insulin antibodies (125I-Insulin binding rate) and C-peptide immunoreactivity
125I-Insulin binding rate was measured using a radioimmunoassay kit (Yamasa Corporation, Chiba, Japan). C-peptide immunoreactivity was determined using a chemiluminescent enzyme immunoassay with Lumipulse Presto C-peptide (Fujirebio Inc., Tokyo, Japan).
Daily variation of plasma glucose and plasma insulin
We evaluated the daily variation of plasma glucose, F, and total insulin (T) five times daily (premeal and 2 h after meals, except after dinner) or six times daily (before and 2 h after meals). We measured F using polyethylene glycol [PEG] 6000 precipitation and T using the acid-PEG method according to a previous report [6], with modifications. B was calculated as T minus F [7]. Patient 1 took tests twice over 3 months. For the first test, patient 1 was administered liraglutide and insulin lispro as follows: before breakfast (14 units), lunch (6 units), and dinner (4 units). Data from this test were referred to as patient 1–1. For the second test, insulin therapy was withdrawn for 21.5 days, and metformin, pioglitazone, and liraglutide were administered. Data from this test were referred to as patient 1–2. Patient 2 was withdrawn from insulin detemir for 9.5 days and treated with metformin, repaglinide, and liraglutide. Immunoreactive insulin (IRI) was measured using a sandwich enzyme immunoassay system (E test Tosoh II IRI; Tosoh Corporation, Tokyo, Japan). For patient 1–1, the IRI was measured using a chemiluminescence immunological assay (Chemilumi Insulin; Kyowa Medics, Tokyo, Japan). The conversion factor (μIU/mL to pmol/L) for IRI was 6.0.
Scatchard plot (B/F vs. B plot) and Ka and Bmax by the one-site model in vivo
Using the daily variation measurement data of B and F, we plotted B/F vs. B. We subsequently analyzed the linearity of the plot using a linear regression model. For the Scatchard analysis, the negative slope equals Ka and the x-axis intercept equals Bmax [8]. However, this is not the optimal method because linearizing the transformation distorts experimental errors [9]. To evaluate the Ka and Bmax of the anti-insulin antibodies more accurately, we analyzed the saturation binding curve in vivo by nonlinear least-squares fitting of the one-site model.
Equilibrium binding assay and Scatchard plot in vitro estimated with a two-site model
We also measured the equilibrium of binding in vitro using 125I-labeled human insulin [1]. Antibody-bound insulin was removed from serum samples using dextran-coated charcoal. Then, the serum was incubated with 125I -labeled human insulin, along with formulations containing varying concentrations of excess unlabeled insulin. Finally, the reaction mixture was precipitated with γ-globulin and PEG, and the radioactivity of the precipitate was counted. Serum samples were collected before breakfast to measure daily variation. We calculated the Ka and Bmax using a weighted nonlinear regression technique with a weighting factor of 1/Y2 fitting of the two-site model.
Statistical analyses and curve fitting
Linear regression and curve fitting were performed using GraphPad Prism ver.6.07 (GraphPad Software, Inc., La Jolla, CA, USA).
Results
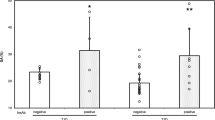
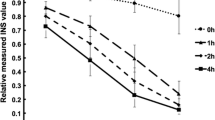
Figure 1A shows the daily fasting data before breakfast. Figure 1B shows the daily variations in T, F, and plasma glucose. In both cases, T reached its lowest point before breakfast, and changes in the F level tended to follow those of the T level.
The result of daily variation and an equilibrium binding assay in vitro. A Fasting data. B Daily variation in total insulin, free insulin, and plasma glucose. C Scatchard plot (B/F vs. B plot) and Ka and Bmax by the one-site model in vivo. D Scatchard plot and Ka and Bmax by the two-site model in vitro. Patient 1–1 and patient 1–2 indicate patient 1’s data from the first and second test, respectively. T-IRI total immunoreactive insulin (pmol/L), F-IRI free immunoreactive insulin (pmol/L), PG plasma glucose (mg/dL), BB before breakfast, AB after breakfast, BL before lunch, AL after lunch, BD before dinner, AD after dinner, B bound insulin (10–8 M) F free insulin, B/F bound/free ratio, Ka affinity constant (1/10–8 M), Bmax binding capacity (10–8 M)
The B/F vs. B plots in vivo for patient 1–1 and patient 2 were approximately linear (Fig. 1C). The linear regression analysis results were as follows: patient 1–1 R squared = 0.770; patient 2 R squared = 0.8925. The B/F vs. B plot of patient 1–2 was distributed in a negative slope. In both cases, the Scatchard plots in vitro became curvilinear (Fig. 1D).
Discussion
Some of B/F vs. B plots in vivo showed an approximately linear relationship. This indicates that the binding reached near equilibrium in patients and the one-site of anti-insulin antibodies mainly determined insulin pharmacokinetics.
Only two data points were deemed inconclusive. Therefore, we theoretically supported this finding. Curvilinear Scatchard plots in vitro showed apparent linear regions [1, 2]. We consider that the approximately linear B/F vs B plots in vivo correspond to the linear regions of the Scatchard plots in vitro because the in vivo insulin levels were limited.
In the two-site model, the relationship between B and F is defined by the equation [4, 10]:
Equation 2 can be transformed to Eq. 3:
Equations 2 and 3 are both curvilinear. However, when the value of F approaches 0, Eq. 3 approximates the following linear expression:
This may be understood using patient 1–1 in vitro data (Ka1:0.381, Ka2:0.00258, Bmax1:16.35, Bmax2:37.12).
Two-site model: \({\text{B}}/{\text{F}}\, = \,\, - \,\left( {0.{3836}\, + \,0.000{9833}\, \times \,{\text{F}}} \right)\, \times \,{\text{B}}\, + \,{6}.{325}\, + \,0.0{5256}\, \times \,{\text{F}}\)
When F approaches 0, this equation approximates the next equation:
We show this visually using a graph. Figure 2 shows a comparison of Eqs. 2 and 4 using in vitro data from patient 1–1. When the value of F is lower than 1.0 (10–8 M), B becomes lower than 4.6 (10–8 M), and the two graphs become similar. We suggest that the plot line in vivo (Fig. 1C) is not a completely straight line but instead approximates the straight part of a hyperbola.
Comparison of \({\text{B}}/{\text{F}}\, = \,{\text{B}}_{{{\text{max1}}}} \, \times \,{\text{K}}_{{{\text{a1}}}} /\left( {{1}\, + \,{\text{K}}_{{{\text{a1}}}} \, \times \,{\text{F}}} \right)\, + \,{\text{B}}_{{{\text{max2}}}} \, \times \,{\text{K}}_{{{\text{a2}}}} /\left( {{1}\, + \,{\text{K}}_{{{\text{a2}}}} \, \times \,{\text{F}}} \right)\) and \({\text{B}}/{\text{F}}\, = \,\, - \,\left( {{\text{K}}_{{{\text{a1}}}} \, + \,{\text{K}}_{{{\text{a2}}}} } \right)\, \times \,{\text{B}}\, + \,{\text{K}}_{{{\text{a1}}}} \, \times \,{\text{B}}_{{{\text{max1}}}} \, + \,{\text{K}}_{{{\text{a2}}}} \, \times \,{\text{B}}_{{{\text{max2}}}}\) using Ka1, Ka2, Bmax1 and Bmax2 of patient 1–1 in vitro. Ka1: 0.381 (1/10–8 M), Ka2: 0.00258 (1/10–8 M), Bmax1: 16.35 (10–8 M), Bmax2: 37.12 (10–8 M). Green circles: \({\text{B}}/{\text{F}}\, = \,{\text{B}}_{{{\text{max1}}}} \, \times \,{\text{K}}_{{{\text{a1}}}} /\left( {{1}\, + \,{\text{K}}_{{{\text{a1}}}} \, \times \,{\text{F}}} \right)\, + \,{\text{B}}_{{{\text{max2}}}} \, \times \,{\text{K}}_{{{\text{a2}}}} /\left( {{1}\, + \,{\text{K}}_{{{\text{a2}}}} \, \times \,{\text{F}}} \right)\). Red squares: \({\text{B}}/{\text{F}}\, = \,\, - \,\left( {{\text{K}}_{{{\text{a1}}}} \, + \,{\text{K}}_{{{\text{a2}}}} } \right)\, \times \,{\text{B}}\, + \,{\text{K}}_{{{\text{a1}}}} \, \times \,{\text{B}}_{{{\text{max1}}}} \, + \,{\text{K}}_{{{\text{a2}}}} \, \times \,{\text{B}}_{{{\text{max2}}}}\)
The equilibrium binding assay in vitro showed that Ka1 > > Ka2 and Ka1 × Bmax1 > > Ka2 × Bmax2. Therefore, Eq. 4 is strongly affected by Ka1 and Bmax1, indicating that the high-affinity sites of anti-insulin antibodies have a predominant influence on insulin pharmacokinetics. Some previous reports have supported this finding [7, 11,12,13].
Because of the polyclonal nature of anti-insulin antibodies, the two-site model might not be a perfect model since three or more binding sites might exist [2, 14]. Using the three-site model, the relationship between B and F is defined by:
When the value of F approaches 0, this equation approximates the following linear expression:
The equation of the more binding-site model defined as Eq. 1 also approaches a linear expression when F approaches 0. Therefore, our theory holds good for more binding-site models.
It is uncertain whether our results would apply to patients other than patients 1 and 2 described in this study. We suggest that the condition that the B/F vs. B plots of the daily variation become linear is as follows.
-
1.
The quantity and characterization of anti-insulin antibodies remain constant and the reaction of insulin and anti-insulin antibodies is at equilibrium in vivo. This condition is necessary for the B/F vs. B plot to become a line (straight or curve line).
-
2.
The binding capacity of the high-affinity site in vivo exceeds the range of insulin concentrations. When insulin concentrations exceed the binding capacity in vivo, the B/F vs. B plots should be curvilinear.
Another patient with type 1 diabetes mellitus who had a moderate titer of anti-insulin antibodies underwent the same evaluation (Supplemental Figure S1). This patient tested for evaluation of the influence of anti-insulin antibodies because she had brittle diabetes. The B/F vs. B plot for this patient did not show a line. This may be because the binding of insulin and the antibodies did not reach equilibrium. Whether the binding reaches near-equilibrium may depend on various factors such as association and dissociation rate constants of anti-insulin antibodies [15], or the provided rate of endogenous and exogeneous insulin. The two patients might have unique anti-insulin antibodies that were easy to reach near-equilibrium and had a high binding capacity.
Our study had some limitations. The accuracy of the measurement of T and F levels was not guaranteed. PEG precipitation of plasma influences the results of insulin immunoassay [16]. This influence depends on the immunoassay. And according to a previous report, the cross-reaction rate for Chemilumi Insulin (IRI for patient 1–1) is 86.7% for lispro [17]. Therefore, the data of patient 1–1 could not be compared with other data. However, it should not influence our main point, which is the linear relationship in the B/F vs. B plots in vivo. Additionally, F levels may have changed in the samples before measurement [18, 19]. It is possible that, after sampling, insulin and anti-insulin antibodies came closer to equilibrium, and B/F vs. B showed a more linear relationship. However, it is difficult to completely solve this problem because centrifugation and PEG are time-consuming [19]. Another limitation is the small sample size. Since patients with high titers of anti-insulin antibodies are rare, we could not expand the sample size. The essential point of this article is the theoretical explanation of the latter part.
In conclusion, the two patients described in our study showed an approximately linear relationship in the B/F vs. B plots in vivo. This relationship is a novel finding of insulin pharmacokinetics in patients with diabetes who have anti-insulin antibodies. These results indicate that the one-site (high-affinity site) of anti-insulin antibodies mainly determines insulin pharmacokinetics within physiological insulin concentrations.
Data availability
The deidentified participant data will be shared on a request basis. Please contact Hiroyuki Asaka (daitoku@muse.ocn.ne.jp). But the data used in this study has been restricted by the Kanazawa University IRB.
References
Goldman J, Baldwin D, Pugh W, Rubenstein AH. Equilibrium binding assay and kinetic characterization of insulin antibodies. Diabetes. 1978;27:653–60.
Fineberg SE, Kawabata TT, Finco-Kent D, Fountaine RJ, Finch GL, Krasner AS. Immunological responses to exogenous insulin. Endocr Rev. 2007;28:625–52.
Berson SA, Yalow RS. Quantitative aspects of the reaction between insulin and insulin-binding antibody. J Clin Invest. 1959;38:1996–2016.
Weder HG, Schildknecht J, Lutz RA, Kesselring P. Determination of binding parameters from Scatchard plots. Theoretical and practical considerations. Eur J Biochem. 1974;42:475–81.
Sasakuma F, Matsumiya K, Onishi M, Kitamura H, Hasegawa K. Studies on insulin and anti-insulin antibody levels in sera of insulin-treated patients. Japanese J Clin Chem. 1987;16:148–55 (In Japanese).
Nakagawa S, Nakayama H, Sasaki T, Yoshino K, Yu YY, Shinozaki K, Aoki S, Mashimo K. A simple method for the determination of serum free insulin levels in insulin-treated patients. Diabetes. 1973;22:590–600.
Van Haeften TW, Krom BA, Gerich JE. Prolonged fasting hypoglycemia due to insulin antibodies in patient with non-insulin-dependent diabetes mellitus: effect of insulin withdrawal on insulin-antibody-binding kinetics. Diabetes Care. 1987;10:160–3.
Scatchard G. The attractions of proteins for small molecules and ions. Ann NY Acad Sci. 1949;51:660–72.
Motulsky HJ, Ransnas LA. Fitting curves to data using nonlinear regression: a practical and nonmathematical review. FASEB J. 1987;1:365–74.
Rosenthal HE. A graphic method for the determination and presentation of binding parameters in a complex system. Anal Biochem. 1967;20:525–32.
Van Haeften TW, Heiling VJ, Gerich JE. Adverse effects of insulin antibodies on postprandial plasma glucose and insulin profiles in diabetic patients without immune insulin resistance. Implications for intensive insulin regimens. Diabetes. 1987;36:305–9.
Van Haeften TW, Bolli GB, Dimitriadis GD, Gottesman IS, Horwitz DL, Gerich JE. Effect of insulin antibodies and their kinetic characteristics on plasma free insulin dynamics in patients with diabetes mellitus. Metabolism. 1986;35:649–56.
Eguchi Y. Scatchard analysis of insulin autoantibodies in the insulin autoimmune syndrome. J Tokyo Wom Med Univ. 1989;59:1296–305 (In Japanese).
Greenfield JR, Tuthill A, Soos MA, Semple RK, Halsall DJ, Chaudhry A, O’Rahilly S. Severe insulin resistance due to anti-insulin antibodies: response to plasma exchange and immunosuppressive therapy. Diabet Med. 2009;26:79–82.
Ismail AA. The insulin autoimmune syndrome (IAS) as a cause of hypoglycaemia: an update on the pathophysiology, biochemical investigations and diagnosis. Clin Chem Lab Med. 2016;54:1715–24.
Church D, Cardoso L, Bradbury S, Clarke C, Stears A, Dover A, Halsall D, Semple R. Diagnosis of insulin autoimmune syndrome using polyethylene glycol precipitation and gel filtration chromatography with ex vivo insulin exchange. Clin Endocrinol (Oxf). 2017;86:347–53.
Ono Y, Kume Y, Kaneko M, Nagatomo R, Yuasa K, et al. Evaluation of the reagent “Chemilumi Insulin” “Chemilumi C-peptide” by automated chemiluminescent immune analyzer ADVIA Centaur XP. JJCLA. 2013;38:51–6 (In Japanese).
Hanning I, Home PD, Alberti KGMM. Measurement of free insulin concentration: the influence of the timing of extraction of insulin antibodies. Diabetologia. 1985;28:831–5.
Oyama H, Yoneda M, Tsushima K, Matsuki M, Nishida S, Horino M. Plasma profiles of total and free insulins in diabetic patients with insulin antibodies (I): study on subcutaneous insulin administration. J Japan Diab Soc. 1990;33:379–85 (In Japanese).
Acknowledgements
We thank the patients who participated in this study.
Funding
None.
Author information
Authors and Affiliations
Contributions
HA conceived and designed the study, analyzed the data, and drafted the manuscript for publication. SK designed the study and reviewed the manuscript. DC supervised the study, contributed to discussion, and reviewed and edited the manuscript. MK, MU, KY, KA, and TY reviewed the manuscript. All authors edited, reviewed, and approved the final version of the manuscript. HA is the guarantor of this work, and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any potential conflicts of interest associated with this research.
Human and animal rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and/or with the Helsinki Declaration of 1964 and later versions. This study was approved by the ethics committee of Kanazawa University (approval No. 1917-1/ September 16, 2015, approval No. 1917-2/February 21, 2017).
Informed consent
Written informed consent was obtained from the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
13340_2023_641_MOESM1_ESM.pdf
Supplementary file1 The results of the patient with type 1 diabetes mellitus who had moderate anti-insulin antibodies (Patient 3). A: Fasting data. B: Daily variation in total insulin, free insulin, and plasma glucose. C: Scatchard plot (B/F vs. B plot) and Ka and Bmax by one-site model in vivo. D: Scatchard plot using 125I-labeled porcine insulin and Ka and Bmax by the two-site model in vitro. The patient was treated with continuous subcutaneous insulin infusion with insulin lispro (4.0, 6.9, and 6.7 units before breakfast, lunch, and dinner, respectively) and total daily basal insulin (15.6 units/day). T-IRI, total immunoreactive insulin (pmol/L); F-IRI, free immunoreactive insulin (pmol/L); PG, plasma glucose (mg/dL); B, bound insulin (10−8 M); F, free insulin; B/F, bound/free ratio; Ka, affinity constant (1/10−8 M); Bmax, binding capacity (10−8 M) (PDF 68 KB)
About this article
Cite this article
Asaka, H., Karashima, S., Chujo, D. et al. In vivo relationship between bound and free insulin in patients with diabetes having anti-insulin antibodies. Diabetol Int 14, 427–433 (2023). https://doi.org/10.1007/s13340-023-00641-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-023-00641-1