Abstract
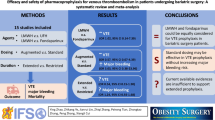
To assess the association between low-molecular weight heparin (LMWH) and unfractionated heparin (UFH) in the prevention of venous thromboembolism (VTE) among participants undergoing general surgery. LMWH and UFH are the standard of practice in the prevention of VTE in surgery. However, in the context of general surgery, studies comparing the effectiveness of these treatments are limited. A systematic search was conducted to find studies which examined the comparative effectiveness between LMWH and UFH in the prophylaxis of VTE in the context of general surgery. The number of events of VTE in groups receiving LMWH or UFH was the primary outcome of interest, and was used to calculate odds-ratios. Amongst 33,068 participants pooled from twelve studies, the rate of VTE was 1.3% in those treated with LMWH, and 3.1% in those treated with UFH. Although there was a wide difference in rates due to clinical heterogeneity, there was no statistically significant difference between treatment effects [OR 0.77; 95% CI 0.58–1.03; p value = 0.0783; I2= 62.3%; 12 studies]. In terms of the sensitivity analysis, sources overly contributing to heterogeneity were removed. The random-effects model continued to show insignificance between LMWH and UFH in the prevention of VTE in participants undergoing general surgery [OR 0.86; 95% CI 0.69–1.08; p value = 0.2005; I2= 0%; 9 studies]. Results show an equal effectiveness in the prevention of VTE between participants undergoing general surgery in those allocated to receive LMWH to those allocated to receive UFH.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Venous thromboembolism (VTE), defined as deep vein thrombosis (DVT), pulmonary embolism (PE), or both, is a frequent postoperative complication and the fifth most common reason for unplanned hospital readmissions after surgery [1]. Additionally, VTE treatment poses a significant economic burden—estimated healthcare cost associated with hospital-acquired VTE in 2011 was $9.0–$18.2 billion [2]. Although differing guidelines exist, the historical standard of care for VTE prophylaxis is administration of a short acting anticoagulant such as unfractionated heparin (UFH) or low-molecular weight heparin (LMWH), in conjunction with further pharmacological and non-pharmacological therapy [3, 4].
While extensive studies have compared the effectiveness of LMWH vs. UFH for VTE prophylaxis in the setting of orthopedic or trauma surgeries [5,6,7], such studies in the context of general abdominal surgery are limited. This gap in knowledge is important, as it is well established that patients undergoing general surgery are at relatively high risk for VTE [8,9,10]. In a cohort of 1,295,291 patients, Cramer et al. [11] found the overall 30-day rate of VTE was 1.2% for general surgery, 0.7% for plastic surgery, and 0.5% for otolaryngology. Similarly, Agnelli et al. [12] found in a cohort of 2373 patients that overall rates of VTE were 2.83% in general surgery, 2.0% in gynecological surgery, and 0.87% in urological surgery. This emphasizes the importance of establishing best practices in VTE prophylaxis for general abdominal surgery.
Presently, two advantages in using LMWH over UFH are more predictable pharmacokinetics and reduced overall cost. Generally, LMWH may be given once a day, whereas UFH require two to three administrations. Even though the cost of acquisition of LMWH is greater than that of UFH, that difference is offset by improved outcomes, fewer instances of hemorrhage and heparin-induced thrombocytopenia (HIT), and less need for anticoagulant monitoring [13]. Furthermore, different formulations of biosimilar LMWH have improved availability.
However, given the relatively high risk of VTE in general surgeries, as well as the growing prevalence of emergency general surgery (EGS) operations, it is increasingly important to understand available data regarding VTE prophylaxis. This study thus aims to provide a contemporary examination of the differences between LMWH vs. UFH for VTE prophylaxis exclusively in general surgery, to guide clinical decision making and improve patient outcomes.
Methods
Inclusion and exclusion criteria
The initial search consisted of all study types which assessed the comparative effectiveness of LMWH and UFH in the prophylaxis of VTE. Studies of all languages were included. All studies consisted of patients over the age of 18. Studies that researched these interventions out of the context of general surgery, were excluded. In addition, studies that contained pregnant participants were excluded.
Search strategy
The PRISMA guideline [14] was followed in conducting and reporting this systematic review and meta-analysis. The review protocol was not registered in a repository. This meta-analysis project includes primary research studies of populations relevant to the study topic, relevant interventions, i.e., unfractionated heparin and low-molecular weight heparin, and relevant outcomes, i.e., prevention of venous thromboembolisms following surgical procedures.
Databases such as PubMed, The Cochrane Library, CINAHL, SCOPUS, and Web of Science were comprehensively searched from the date of database inception to September 2019. EMBASE was not searched due to the lack of access to the database. A separate search was also performed in ClinicalTrials.gov for grey literature. The final search strategy is featured in the Supplemental Online Resource 1.
Search results were limited to comparative study as publication type. No other filters were applied in the searches. Similar search terms and strategies were used to search the other included databases. All search results were exported to an EndNote library. Duplicate references were removed via the EndNote built-in function as well as manually. Custom columns for Reviewer 1 and Reviewer 2 were created in the EndNote library for the two subject experts to perform screening before the EndNote library was shared with them. The numbers of results searched, screened, and included for final review and analysis were all displayed in the study flow diagram (see Supplemental Online Resource 2).
Outcomes
The primary outcome of interest was the event of VTE. Of the twelve studies included in the meta-analysis, eight studies [15,16,17,18,19,20,21,22] used a fibrinogen uptake test (FUT) for outcome assessment. Three studies [23,24,25] used venography and one study [26] did not report their testing method. All studies using an FUT for outcome assessment conducted the test daily for every participant regardless of symptoms. Of the three studies using venography, the Kakkar et al. study conducted an ascending venography when sings of deep vein thrombosis developed. The Mcleod et al. study conducted a bilateral contrast venography routinely between postoperative days 5 and 9. And the Leizorovicz et al. study conducted a phlebogram only on participants who returned a positive FUT. Major bleeding and deaths were secondary and tertiary outcomes of interest, respectively. Ten studies [15,16,17,18, 20, 22,23,24,25,26] reported major bleeding as an outcome and five studies [15, 17, 20, 21, 23] reported deaths as an outcome. Heparin induced thrombocytopenia (HIT) was a quaternary outcome of interest. Four studies [19,20,21, 25] reported HIT as an outcome.
Data abstraction and quality assessment
Data were extracted manually. Paired investigators reviewed the extracted data and disagreements were resolved with mutual consensus. The risk of bias for each study was investigated independently by two reviewers. Studies that were randomized and double-blinded were considered as having a low risk of bias.
Data synthesis and analysis
Statistical code for the analysis is included in Supplemental Online Resource 3. Odds-ratios (OR) with 95% confidence intervals, were used to quantify the association between prophylaxis of VTE in LMWH vs. UFH in each study. A random-effects model was used to estimate pooled effect sizes. An I2 statistic was used to assess heterogeneity, with an I2 value of > 50% signaling high heterogeneity. The significance level was set at 0.05. A forest plot was fit to visualize the results of the meta-analysis. In addition, an inverted funnel plot was fit to study potential publication bias (Supplemental Online Resource 3: Section 1.1).
Influence analysis was then conducted to study potential outliers. This analysis was based on the leave-one-out method, where the results of the meta-analysis are repeatedly calculated, each time leaving out one study. This way studies that over exert their influence on the heterogeneity of the meta-analysis can be easily detected. Outlying studies were detected using the DFFITS value, Cook’s distance, and covariance ratios [27] (Supplemental Online Resource 3: Section 1.2).
To validate the findings, sensitivity analysis was conducted independent of the influence analysis. A Graphic Display of Heterogeneity (GOSH) plot was used to study effect-size heterogeneity patterns in the data [28] (Supplemental Online Resource 3: Section 1.3). Clustering algorithms were used to study sub clusters in the GOSH plot to understand which studies were causing cluster imbalance. The algorithms employed were a k-means, Density-based spatial clustering of applications with noise (DBSCAN), and a Gaussian Mixture Model (Supplemental Online Resource 3: Section 1.4). The three algorithms independently reported the potential outlying studies. A random-effects model, with its respective forest plot, was then fit with the outlying studies excluded (Supplemental Online Resource 3: Section 1.5). In addition, random-effects models were fit to estimate pooled effect sizes for the outcomes of major bleeding, death, and HIT (Supplemental Online Resource 3: Section 1.6). All analysis was conducted using R software, and R packages, ‘meta’, ‘dmetar’, and ‘metafor’.
Results
Study characteristics
The main characteristics of the included studies are summarized in Table 1. Additional study characteristics including surgery types, treatment strategies, and average duration of surgery is reported in supplemental Online Resource 5. Twelve studies examining the comparative effectiveness of LMWH vs. UFH in the prevention of post-surgical thromboembolic events, exclusively in general surgery, were included in the meta-analysis. Of the twelve included studies, ten studies were randomized controlled trials (RCT). Of these, five studies [17,18,19, 24, 25], were randomized and double-blinded and another five studies [15, 16, 20, 21, 23], were randomized but not double-blinded. The two remaining studies [22, 26] were neither randomized, nor double-blinded. In addition, nine [15, 16, 18, 20,21,22,23,24, 26], of the twelve studies include a detailed description of the types of surgeries performed in the RCT. Treatment strategy was consistent across the studies, with all twelve studies starting treatment one to 4 h, typically 2 h, before surgery. All studies continued treatment up until at least the 5th post-operative day, typically continuing up until the 7th day or until the participant is fully mobile. Furthermore, five [15, 17, 20,21,22] out of 12 studies reported duration of surgery. The pooled average duration of surgery in both groups was approximately 128 min (Supplemental Online Resource 5).
As a result of the inclusion of two studies, the Birkmeyer et al. study [26] and the European Fraxiparin Study (EFS) Group study [15], the I2 statistic, used to test heterogeneity of treatment effect, increased from 14.3 to 62.3%. The two studies [15, 26], account for a majority of the heterogeneity in the meta-analysis. To support our results and ensure that they are robust, a sensitivity analysis was performed and the results of the meta-analysis are presented both with and without these studies, i.e., with and without a homogenous study population.
The meta-analysis consists of 33,068 participants, pooled from twelve studies, who underwent general surgery. Of these participants, 22,282 were treated with LMWH and the remaining 10,786 were treated with UFH.
Venous thromboembolic events
The results concerning the comparative effectiveness of LMWH vs. UFH are shown in Table 2 and Fig. 1. A total of 646 events of VTE were recorded between the LMWH and UFH groups using the outcome assessments mentioned in Table 1. Of them, 308 (1.3%) events occurred in patients given LMWH, and 338 (3.1%) events occurred in patients given UFH. The random-effects model reported an Odds-ratio (OR) of 0.77 [95% CI 0.58–1.03; p value = 0.0783; I2= 62.3%]. With an insignificant result, our random-effects model reported no statistically significant difference between LMWH and UFH in the prevention of VTE in participants undergoing general surgery. Since our I2 value is high, inferences from this result must be made with caution. The rates of VTE between the two groups are quite different (LMWH: 1.3%; UFH: 3.1%). In this case, the model is unable to distinguish whether the difference in rates of VTE is due to treatment effect or due to clinical heterogeneity between the two groups. Due to this high level of heterogeneity, a comprehensive sensitivity analysis was performed. The inverted funnel plot for the outcome of VTE did not suggest publication bias (see Supplemental Online Resource 4).
Sensitivity analysis
As our original study population, pooled from twelve studies, had a high level of heterogeneity, a sensitivity analysis was conducted to identify studies that were inflating their influence on the overall results. The three algorithms independently identified three studies [24, 29, 35], that were contributing to the majority of the heterogeneity in the meta-analysis. When the three identified studies [15, 20, 26], were removed, the pooled study population was 9452. There were 158 (3.3%) events of VTE in 4713 participants allocated to the LMWH group, and there were 182 (3.8%) events of VTE in 4739 participants allocated to the UFH group. The I2 statistic was 0%, signaling a homogenous population. The random-effects model reported an OR of 0.86 [95% CI, 0.69–1.08; p value = 0.2005; I2= 0%]. With an insignificant result, we can conclude that there is no statistically significant difference between LMWH and UFH in the prevention of VTE in participants undergoing general surgery. The results of the meta-analysis with and without a homogenous population are reported in Table 3.
Major bleeding
The ten studies [15,16,17,18, 20, 22,23,24,25,26] that reported events of major bleeding had a pooled study population of 31,405 participants. There were 249 events of major bleeding observed in 21,450 participants allocated to receive LMWH (1.2%). There were 271 events of major bleeding observed in 9,955 participants allocated to receive UFH (2.7%). The random-effects model gives a pooled odds-ratio of 0.83 [95% CI 0.64–1.08; p value = 0.1580; I2= 41%]. With an insignificant p value, there is no correlation in events of major bleeding in general surgery between participants given LMWH, and participants given UFH. An I2 statistic of 41% signaled moderate heterogeneity in the study population. Due to the moderate heterogeneity, inferences from this result must be made with caution.
Deaths
The five studies [15, 17, 20, 21, 23], that reported events of death had a pooled study population of 9247 participants. There were 31 (0.67%) deaths observed in 4622 participants allocated to receive LMWH. There were 33 (0.71%) deaths observed in 4625 participants allocated to receive UFH. The random-effects model gives a pooled odds-ratio of 0.88 [95% CI 0.53–1.45; p value = 0.6050; I2= 0%]. With an insignificant result, we can conclude that there is no correlation in deaths between participants given LMWH and participants given UFH, when undergoing general surgery. An I2 statistic of 0% signaled a homogeneous population.
Thrombocytopenia
UFH is known to have a higher rate of heparin-induced thrombocytopenia (HIT) than LMWH. Out of the twelve studies, four studies [19,20,21, 25] measured HIT as an outcome. The four studies had a pooled study population of 4026 participants. There were 18 (0.89%) events of HIT observed in 2018 participants allocated to receive LMWH. There were 27 (1.34%) events of HIT observed in 2008 participants allocated to receive UFH. The random-effects model gives a pooled odds-ratio of 0.66 [95% CI 0.37–1.21; p value = 0.1840; I2= 0%]. With an insignificant result, our analysis of the four pooled studies shows no correlation in the event of HIT between participants given LMWH and participants given UFH, when undergoing general surgery.
Discussion
Our study demonstrates that in participants undergoing general surgery, no association is seen in the rate of VTE between participants allocated to low-molecular weight heparin (LMWH) and those allocated to unfractionated heparin (UFH). Before sensitivity analysis, our original population pooled from twelve studies had a high level of heterogeneity (I2= 62.3%), indicating a population with a wide range of risk for VTE. Although the initial rates of VTE were vastly different (LMWH: 1.3%; UFH: 3.1%), we were not able to tell with certainty, whether that difference is attributable to the treatment effect or to clinical heterogeneity between the two groups. Thus, we identified and removed studies that were statistically and clinically heterogeneous, to create a homogenous study population. This clinical heterogeneity which was causing the statistical heterogeneity in our studies, could have risen from a wide difference in outcome assessment, varying dose amounts, and/or varying surgery types and lengths. After sensitivity analysis, the rate of VTE, now pooled from nine studies, were similar in the two groups (LMWH: 3.3%; UFH: 3.8%). With a homogeneous population, our results continued to show insignificance between the two treatment effects. We could now conclude with certainty that there is no difference in the rate of VTE between the two groups.
In investigating the secondary outcome of major bleeding, no association is seen in the event of major bleeding between LMWH and UFH. However, our random-effects model returned an I2 value of 41%, signaling moderate heterogeneity that requires further investigation. This heterogeneity stems from the clinical heterogeneity in the study population and dissimilar reporting criteria for the endpoint of major bleeding. For example, in some studies, major bleeding was defined as a hemorrhage, while in others it was defined as a severe hemorrhage potentially reconciling the difference in rates of major bleeding between the two groups (LMWH: 1.2%; UFH: 2.7%). Although a sensitivity analysis could be conducted to gather a more robust result, due to the dissimilar reporting criteria for major bleeding, results for this outcome should be interpreted with caution. We remain uncertain whether the difference in rates of major bleeding between the two groups is due to the treatment effect, or due to clinical heterogeneity and dissimilar reporting criteria. In assessing our third outcome of death, with a homogeneous population, we can conclude that no association is seen in deaths between the LMWH and UFH groups. And lastly, in assessing our fourth outcome of HIT, with a homogeneous population, we can conclude that no association is seen in HIT between the LMWH and UFH groups. However, the outcome of HIT requires further analysis in a more contemporary randomized clinical trial (RCT) setting.
The results of our study should be interpreted within the context of results of prior similar studies. Our results are consistent with those of previous clinical trials and grouped analysis in general surgical patients that have shown lack of difference in VTE outcomes between LMWH and UFH [29,30,31,32]. The overall thromboembolic event rate in this study after sensitivity analysis (3.3–3.8%) is consistent with other large trials [7, 33,34,35,36,37,38]. In addition to the VTE event rate, we analyzed the pooled results of major bleeding and mortality among studies that looked at these outcomes. In our pooled analysis, we found no statistical difference in major bleeding events between patients receiving LMWH or UFH. We observed, overall, major bleeding rates of 1.2% and 2.7%, respectively, for LMWH and UFH. Although not statistically different and biased in heterogeneity, this is in contrast to the results of the ENOXACAN study: major bleeding was seen in 4.1% of patients receiving LMWH and 2.9% of those receiving UFH [39]. However, previous meta-analyses have not observed increased bleeding with LMWH in general surgery patients [34,35,36]. A summary of 33 general surgical trials comparing UFH and LMWH found a significantly lower risk of bleeding with LMWH [40], and a 1997 meta-analysis of general surgery trials also found that bleeding was greater with LMWH vs. UFH in VTE prophylaxes; however, this was dose dependent.
In summary, our findings in this meta-analysis regarding the lack of superiority in VTE prophylaxis of LMWH are also demonstrated among other general surgery trials and meta-analyses. Although LMWHs have been advocated in multiple specialties for VTE prophylaxis because of effectiveness, safety, and once-day dosing convenience, our results showed equal effectiveness, and no difference in bleeding or mortality between UFH and LMWH, given the limitations discussed above. Besides effectiveness and safety, considerations of cost and logistics can be important in deciding which VTE prophylaxis regimen to use. Although LMWH has the advantage of once-a-day dosing vs. two or three daily doses for, in the United States, the cost of LMWH is much higher than that of UFH. Etchells et al., found via economic analysis that the strategy of prophylaxis with Low Dose Heparin (LDH) was equally effective, safer, and less expensive for colorectal surgery patients in a baseline and sensitivity analysis [41]. In other words, a strategy of enoxaparin prophylaxis was associated with over $100,000 higher cost than UFH for 7 days of prophylaxis. This is clearly an important consideration when deciding the regimen of VTE prophylaxis in general surgery patients.
Limitations
A limitation of this study is the lack of recent literature in our subject area. With older studies, we risk the use of data obtained using outdated protocols and procedures. The outcome assessment used to diagnose DVT was one such limitation. Eight studies [15,16,17,18,19,20,21,22] used a FUT for outcome assessment. A FUT is an outdated mode of diagnosis and has been replaced by other diagnostic tests due to a high rate of false positives [42]. Ideally, studies using a duplex ultrasound (DUS) would reduce the risk of false positives in our meta-analysis. When comparing specificities, a FUT has a specificity rate of 71%, while a DUS has a specificity rate of 97% [42]. Another limitation is the clinical heterogeneity between studies. The 95% confidence interval for the effect size sensitivity analysis between LMWH vs. UFH was 0.69–1.08. This range represents anywhere from a 31% reduction to an 8% increase in odds of VTE. This wide confidence interval stems from the clinical heterogeneity in our studies. For example, in addition to the difference in dose of LMWHs, the treatments also vary in molecular weight, and determination of an optimal dose requires further investigation. Moreover, although within the context of general surgery, our studies consisted of participants undergoing surgeries of varying duration and risk. Many studies have reported the exact surgeries that were performed in the RCT; however, many studies have only stated umbrella terms like “major abdominal surgery” and a majority have not reported average surgery duration. Likewise, the studies consisted of participants with varying risk factors for VTE such as obesity, hypertension, varicose veins, malignancies, and heart failure. Due to insufficient data reporting, we were unable to investigate the association between these risk factors and the event of VTE. Ideally, a subgroup analysis would be conducted for each risk factor. And lastly, of the twelve studies, one [25] study that we know of was industry supported.
Conclusions
Our results show an equal effectiveness in the prevention of VTE between participants undergoing general surgery in those allocated to receive LMWH to those allocated to receive UFH. Our results also show similar rates in mortality and heparin-induced thrombocytopenia between participants allocated to received LMWH and those allocated to received UFH. The outcome of major bleeding was not quantifiable due to inadequate data.
References
Merkow RP, Ju MH, Chung JW et al (2015) Underlying reasons associated with hospital readmission following surgery in the United States. JAMA 313(5):483–495
Mahan CE, Borrego ME, Woersching AL, Federici R, Downey R, Tiongson J et al (2012) Venous thromboembolism: annualised United States models for total, hospital-acquired and preventable costs utilising long-term attack rates. Thromb Haemost 108:291–302
Anderson DR, Morgano GP, Bennet C et al (2019) American Society of Hematology 2019 guidelines for management of venous thromboembolism: prevention of venous thromboembolism in surgical hospitalized patients. Blood Adv. 3(23):3898–3944
Kearon C, Akl EA, Comerota AJ et al (2012) Antithrombotic therapy for VTE disease: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2 Suppl):e419S–e496S
Jacobs BN, Cain-Nielsen AH, Jakubus JL et al (2017) Unfractionated heparin versus low-molecular-weight heparin for venous thromboembolism prophylaxis in trauma. J Trauma Acute Care Surg 83(1):151–158
Simonneau G, Sors H, Charbonnier B et al (1997) A comparison of low-molecular-weight heparin with unfractionated heparin for acute pulmonary embolism. NEJM 337:663–669
O’Donnell M, Weitz JI (2003) Thromboprophylaxis in surgical patients. Can J Surg 46(2):129–135
Huber O, Bounameaux H, Borst F, Rochner A (1992) Postoperative pulmonary embolism after hospital discharge. An underestimated risk. Arch Surg 127:310–313
Clagett GP, Reisch JS (1988) Prevention of venous thromboembolism in general surgical patients. Results of meta-analysis. Ann Surg 208:227–240
Collins R, Scrimgeour A, Yusuf S et al (1988) Reduction in fatal pulmonary embolism and venous thrombosis by perioperative administration of subcutaneous heparin. Overview of results of randomized trials in general, orthopedic, and urologic surgery. N Engl J Med 318:1162–1173
Cramer JD, Dilger AE, Schneider A, Smith SS, Samant S, Patel UA (2018) Risk of venous thromboembolism among otolaryngology patients vs general surgery and plastic surgery patients. JAMA Otolaryngol Head Neck Surg 144(1):9–17. https://doi.org/10.1001/jamaoto.2017.1768
Agnelli G, Bolis G, Capussotti L et al (2006) A clinical outcome-based prospective study on venous thromboembolism after cancer. Ann Surg 243:89–95
McGarry LJ, Thompson D, Weinstein MC, Goldhaber SZ (2004) Cost effectiveness of thromboprophylaxis with a low-molecular-weight heparin versus unfractionated heparin in acutely ill medical inpatients. Am J Manag Care 10(9):632–642
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341
National Library of Medicine (1988) Comparison of a low molecular weight heparin and unfractionated heparin for the prevention of deep vein thrombosis in patients undergoing abdominal surgery. The European Fraxiparin Study (EFS) Group. Br J Surg 75(11):1058–1063. https://doi.org/10.1002/bjs.1800751105
Garcea D, Martuzzi F, Santelmo N et al (1992) Post-surgical deep vein thrombosis prevention: evaluation of the risk/benefit ratio of fractionated and unfractionated heparin. Curr Med Res Opin 12(9):572–583. https://doi.org/10.1185/03007999209111524
Kakkar VV, Boeckl O, Boneu B et al (1997) Efficacy and safety of a low-molecular-weight heparin and standard unfractionated heparin for prophylaxis of postoperative venous thromboembolism: European multicenter trial. World J Surg 21(1):2–9. https://doi.org/10.1007/s002689900185
Kakkar VV, Stringer MD, Hedges AR et al (1989) Fixed combinations of low-molecular weight or unfractionated heparin plus dihydroergotamine in the prevention of postoperative deep vein thrombosis. Am J Surg 157(4):413–418. https://doi.org/10.1016/0002-9610(89)90589-8
Liezorovicz A, Picolet H, Peyrieux JC, Boissel JP (1991) Prevention of perioperative deep vein thrombosis in general surgery: a multicentre double blind study comparing two doses of Logiparin and standard heparin. Br J Surg 78(4):412–416. https://doi.org/10.1002/bjs.1800780410
Nurmohamed MT, Verhaeghe R, Haas S et al (1995) A comparative trial of a low molecular weight heparin (enoxaparin) versus standard heparin for the prophylaxis of postoperative deep vein thrombosis in general surgery. Am J Surg 169(6):567–571. https://doi.org/10.1016/S0002-9610(99)80222-0
Samama M, Combe S (1990) Prevention of thromboembolic disease in general surgery with enoxaparin (Clexane). Acta Chir Scand Suppl 556:91–95
Verardi S, Casciani CU, Nicora E et al (1988) A multicentre study on LMW-heparin effectiveness in preventing postsurgical thrombosis. Int Angiol 7(3 Suppl):19–24. http://search.proquest.com/docview/78610924/
Kakkar V, Cohen A, Edmonson R et al (1993) Low molecular weight versus standard heparin for prevention of venous thromboembolism after major abdominal surgery. Lancet 341(8840):259–265. https://doi.org/10.1016/0140-6736(93)92614-Y
Leizorovicz A, Bara L, Samama M, Haugh M (1993) Factor Xa inhibition: correlation between the plasma levels of anti-Xa activity and occurrence of thrombosis and haemorrhage. Thromb Haemost 23(Suppl 1):89–98. https://doi.org/10.1159/000216915
Mcleod S, Geerts H, Sniderman W et al (2001) Subcutaneous heparin versus low-molecular-weight heparin as thromboprophylaxis in patients undergoing colorectal surgery: results of the Canadian colorectal DVT prophylaxis trial: a randomized, double-blind trial. Ann Surg 233(3):438–444. https://doi.org/10.1097/00000658-200103000-00020
Birkmeyer NJO, Finks JF, Carlin AM et al (2012) Comparative effectiveness of unfractionated and low-molecular-weight heparin for prevention of venous thromboembolism following bariatric surgery. Arch Surg (Chicago Ill : 1960) 147(11):994–998. https://doi.org/10.1001/archsurg.2012.2298
Viechtbauer W, Cheung MW-L (2010) Outlier and influence diagnostics for meta-analysis. Res Synth Methods 1(2):112–125. https://doi.org/10.1002/jrsm.11
Olkin I, Dahabreh IJ, Trikalinos TA, Olkin I (2012) GOSH—a graphical display of study heterogeneity. Res Synth Methods 3(3):214–223. https://doi.org/10.1002/jrsm.1053
Clagett GP, Anderson FA, Geerts W et al (1998) Prevention of venous thromboembolism. Chest 114(suppl):S531–S560
Koch A, Bouges S, Ziegler S et al (1997) Low-molecular-weight heparin and unfractionated heparin in thrombosis prophylaxis after major surgical intervention: update of previous meta-analyses. Br J Surg 84:750–759
Nurmohamed MT, Rosendall FR, Buller HR et al (1992) Low-molecular weight heparin versus standard heparin in general and orthopaedic surgery: a meta-analysis. Lancet 340:152–156
Leicorovicz A, Haugh MC, Chapuis FR et al (1992) Low-molecular-weight heparin in prevention of perioperative thrombosis. Br Med J 305:913–920
Aziz F, Patel M, Ortenzi G, Reed AB (2015) Incidence of postoperative deep venous thrombosis is higher among cardiac and vascular surgery patients as compared with general surgery patients. Ann Vasc Surg 29(4):661–669
Du W, Zhao X, Nunno A, Li Y, Gu Y (2020) Risk factors for venous thromboembolism in individuals undergoing coronary artery bypass grafting. J Vasc Surg Venous Lymphat Disord 8(4):551–557. https://doi.org/10.1016/j.jvsv.2019.06.022
Panhwar MS, Ginwalla M, Kalra A et al (2019) Association of acute venous thromboembolism with in-hospital outcomes of coronary artery bypass graft surgery. J Am Heart Assoc 8(19):e013246. https://doi.org/10.1161/jaha.119.013246
Agnelli C (2004) Prevention of venous thromboembolism in surgical patients. Circulation 110(4):4–12
Bergqvist D, Burmark US, Frisell J et al (1986) Low-molecular-weight heparin once daily compared with conventional low-dose heparin twice daily. A prospective double-blind multicentre trial on preventing post-operative thrombosis. Br J Surg 3:204
Leizorovicz A, Picolet H, Peyrieux JC et al (1991) Prevention of perioperative deep vein thrombosis in general surgery: a multicentre double blind study comparing two doses of Logiparin and standard heparin. Br J Surg 78:412–416
ENOXACAN Study Group (1997) Efficacy and safety of enoxaparin versus unfractionated heparin for prevention of deep vein thrombosis in elective cancer surgery: a double-blind randomized multicentre trial with venographic assessment. Br J Surg 84:1099–1103
Palmer AJ, Schramm W, Kirchhof B et al (1997) Low-molecular-weight heparin and unfractionated heparin for prevention of thromboembolism in general surgery: a meta-analysis of randomized clinical trials. Haemostasis 27:65–74
Etchells E, McLeod RS, Geerts W et al (1999) Economic analysis of low dose heparin vs. the low-molecular-weight heparin enoxaparin for prevention of venous thromboembolism after colorectal surgery. Arch Intern Med 159:1221–1228
Norton JA (2012) Surgery: basic science and clinical evidence, 2nd edn. Springer, New York
Author information
Authors and Affiliations
Contributions
All authors have contributed equally to all aspects of this project.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Research involving human participants and/or animals
This research does not involve human participants and/or animals.
Informed consent
Informed consent was not needed as this was an analysis of existing literature.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Nair, P., Trivedi, R., Hu, P. et al. Low-molecular weight vs. unfractionated heparin for prevention of venous thromboembolism in general surgery: a meta-analysis. Updates Surg 73, 75–83 (2021). https://doi.org/10.1007/s13304-020-00872-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-020-00872-w