Abstract
Diabetic macroangiopathy, a prevalent and severe complication of diabetes mellitus, significantly contributes to the increased morbidity and mortality rates among affected individuals. This complex disorder involves multifaceted molecular mechanisms that lead to the dysfunction and damage of large blood vessels, including atherosclerosis (AS) and peripheral arterial disease. Understanding the intricate pathways underlying the development and progression of diabetic macroangiopathy is crucial for the development of effective therapeutic interventions. This review aims to shed light on the molecular mechanism implicated in the pathogenesis of diabetic macroangiopathy. We delve into the intricate interplay of chronic inflammation, oxidative stress, endothelial dysfunction, and dysregulated angiogenesis, all of which contribute to the vascular complications observed in this disorder. By exploring the molecular mechanism involved in the disease we provide insight into potential therapeutic targets and strategies. Moreover, we discuss the current therapeutic approaches used for treating diabetic macroangiopathy, including glycemic control, lipid-lowering agents, and vascular interventions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
This review provides a comprehensive overview of the molecular mechanisms underlying diabetic macroangiopathy, a complication commonly seen in individuals with diabetes. |
Type 2 diabetes mellitus accelerates atherosclerosis and an increased risk of thrombotic vascular events due to dyslipidemia, endothelial dysfunction, poor fibrinolytic balance, and irregular blood flow. |
Tight glycemic management, normal lipid profiles, frequent physical exercise, a healthy lifestyle, and pharmaceutical therapies are useful tools to avoid and treat diabetic macroangiopathy. |
Introduction
Type 2 diabetes mellitus (T2DM) is a metabolic disorder with high blood sugar levels due to the body’s resistance to insulin [1]. T2DM affects 90% of individuals with diabetes and poses a significant threat to human health, making it a public health concern globally [2,3,4]. The complications of diabetes can be characterized on the basis of their involvement in heart and brain diseases [5,6,7]. These complications are exacerbated by diabetes while the envelopment of multiple diseases worsens the prognosis [1, 8]. While recent studies have provided valuable insights into the pathophysiology of diabetes complications, the increasing specialization in medical research has led to a focus on individual lesions rather than a comprehensive understanding of the overall picture. Therefore, it is crucial to conduct a comprehensive study that encompasses various systems and angiopathies to fully comprehend the complexities of diabetes complications.
The process of wound healing involves several key steps including hemostasis, inflammation, proliferation, and remodeling [9]. During the proliferative stage, angiogenesis occurs which involves the growth of immature, permeable, and redundant blood vessels [10, 11]. This process is mediated by proangiogenic factors, with vascular endothelial growth factor (VEGF) playing a significant role [12]. Microvasculature resolution factors like protein sprouty homolog 2 (SPRY2) inhibit the formation of capillaries, while pigment epithelium-derived factor (PEDF) is responsible for apoptosis-driven pruning of blood vessels during wound maturation [13, 14].
Diabetes complications are often categorized into macro- and microvascular angiopathy, and their consequences are defined by the target organs [2]. Macrovascular disease which includes peripheral vascular disorders, myocardial infarction, and stroke is the leading cause of mortality and morbidity in people with diabetes [5]. In addition to the traditional mechanisms of macrovascular disease, i.e., underlying obstructive atherosclerotic diseases affecting large arteries, other factors contribute to the development of diabetic vasculopathy [2]. The production of advanced glycation end products and their interaction with specific receptors leads to the overexpression of various cytokines. Diabetes also activates hemodynamic pathways which can be worsened by concurrent systemic hypertension. Aside from these mechanisms, hyperglycemia, non-enzymatic glycosylation, lipid modification, vasculature remodeling, and growth factor activation all contribute to the development of diabetic vasculopathy [15, 16].
This article reviews the general pathological manifestations of macrovascular lesions, the molecular mechanisms involved in different target organs, and potential therapeutic targets. This review will summarize the most recent research on the significance of proper capillary growth, function, and maturation in diabetic wound healing. This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Pathophysiology of Macrovascular Angiopathy in People with Diabetes
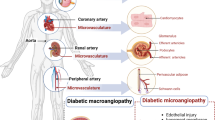
People with diabetes typically exhibit localized and systemic vascular problems known as diabetic vasculopathy, which are exacerbated by a variety of comorbidities such as hypertension [17]. Diabetes increases the chance of developing coronary artery disease (CAD), peripheral artery disease (PAD), and cerebrovascular disease by a factor of 2–4 [18]. People with diabetes have higher morbidity and mortality rates due to vascular disease, which accounts for the largest proportion of cases of death [19]. Figure 1 explains the detailed pathophysiology of T2DM complications and their consequences. Advanced glycation products and systemic inflammation exacerbate diabetes-related comorbidities. Most macrovascular events take longer to manifest clinically, but when they do, they are life-threatening [20]. This emphasizes the necessity of detecting vascular injury as early and accurately as possible [21, 22]. Tissues with elevated contractility, such as the heart, are at a higher risk of developing macrovascular problems because arteries, such as the coronaries, become occluded even from physiologic contractility, which is worse when combined with pathologic vascular occlusion [2]. The metabolic, humoral, and hemodynamic variables that contribute to the distinctive dysfunction of diabetic vasculopathy are all interconnected [23]. Hyperglycemia-induced oxidative stress, for example, enhances both advanced glycation end product (AGE) production and protein kinase C (PKC) activation. Hyperglycemia, non-enzymatic glycation, lipid modification, vascular remodeling, cytokine production, and growth factor activation are theorized to facilitate diabetic vascular injury [24, 25]. The pathophysiology of these pathways is discussed and summarized in Fig. 1.
Pathophysiology of diabetic macrovasculopathy and its consequences. SOD superoxide dismutase, ALDH2 acetaldehyde dehydrogenase, PKC protein kinase C, AGEs advanced glycation end products, VSM vascular smooth muscle, RAGE receptor for advanced glycation end products, FFA free fatty acids, TG triglycerides, NF-kb nuclear factor kappa-B, IL-6 interleukin-6, MCP monocyte chemoattractant protein, TNFα tumor necrosis factor-α), ROS reactive oxygen species
Hyperglycemia
Persistent hyperglycemia is now acknowledged as a major contributor to T2DM vasculopathy development [26]. When combined with other variables, hyperglycemia may hasten the onset of atherosclerosis (AS) in people with diabetes. In addition, hyperglycemia stimulates apoptosis, lowers endothelial cell (EC) replication, and hastens the progression of AS. The glycation of proteins and lipids in the arterial wall is the most important of these processes. Glucose-induced damage is caused by advanced glycation, PKC activation, and sorbitol accumulation. Early glycated proteins on collagen, intestinal tissues, and blood vessels undergo a series of chemical reactions that result in permanent AGEs (Fig. 1). AGEs possess a plethora of potentially hazardous chemical and biological features. They gradually build up with age and steadily accumulate. The phrase “AGE formation” refers to the biochemical attachment of glucose to the amino group of a protein that occurs without the intervention of an enzyme. This process produces a reversible material called a Schiff base, which can subsequently be rearranged to produce an Amadori product, the most well-known of which is hemoglobin A1c (HbA1c). Permanent AGE formation alters molecule structure, modifies enzyme activity, reduces the ability of proteins and lipids to degrade and recognize receptors, and interferes with normal protein and lipid function [27, 28]. Plasma glucose levels and the degree of non-enzymatic glycation are significantly associated, highlighting the importance of monitoring HbA1c as a useful adjunct in diabetes treatment. AGEs generate oxidative stress, impair the function of the vascular barrier, enhance vascular permeability, and improve the adhesion of VCAM-1, a vascular cell adhesion molecule, by binding to AGE receptors (RAGE) on ECs. The expression of VCAM-1 on monocytes, which may enhance monocyte migration, may constitute one of the early steps of vascular remodeling [29]. Previous studies have revealed that mesenchymal stem cells (MSCs), a specific type of stem cell, are involved in the pathogenesis of diabetes [30, 31]. Studies have shown that both type 1 and type 2 diabetes are associated with a decrease in the number and function of circulating and tissue-resident stem/progenitor cells including MSCs [30, 32]. This suggests that the macrovascular complications of diabetes may be partly attributed to a stem cell vasculopathy, where the impaired stem cell compartment fails to regenerate dying endothelial or vascular smooth muscles [31]. In T2DM, the reduction of vascular stem cells is directly related to the glycemic level, and this reduction is also observed in individuals with impaired glucose regulation [2]. However, it is unclear whether the decrease or dysfunction of stem cells is a direct consequence of glucose level disturbances, and to what extent the hyperglycemia contributes to this mechanism.
Lipids and Lipoproteins
Lipid metabolism plays a significant role in both short- and long-term diabetes symptoms and consequences. In diabetes-related dyslipidemia, there is an increase in total cholesterol and low-density lipid (LDL) levels, while high-density lipid (HDL) levels decrease with the increase in triglyceride levels [33]. The lipoproteins are transported through the EC via vascular transit, which is altered by glycation, oxidation, aggregation, and proteoglycan interaction, or inclusion into immune complexes. There is a predominance of tiny, dense LDL molecules that are more prone to oxidation [34, 35]. In the subendothelial area, LDL molecules are oxidatively transformed into reactive oxygen species (ROS) by macrophages, ECs, and smooth muscle cells (SMCs). Oxidized LDL (Ox-LDL) promotes additional conscription of monocytes to the subendothelial region. Monocytes are activated, differentiate, and then grow into much larger macrophages. Foam cells are created when macrophages accumulate the oxidized lipids in the vascular wall [36]. These foam cells, in turn, activate a slew of inflammatory mediators and growth factors that provoke collagen accumulation and muscle proliferation in the vascular wall [37]. Ox-LDL accumulates in the cell, where it is toxic to ECs and affects their shape and function [38]. Ox-LDL promotes circulating monocyte adherence to injured endothelium, causing them to migrate into the vascular intima. It also enhances the creation of chemoattractants, which aid in migration [39]. Glycation alters apolipoprotein B, which aids in LDL receptor uptake, making the LDL particle more atherogenic. Ox-LDL detected in the intima is more likely to be linked to local matrix proteins via glucose-mediated cross-links. During this process, the LDL undergoes an even more complex oxidation and glycation process [40]. Ox-LDL also lowers nitric oxide (NO) production by blocking NO synthase, which contributes to vasodilation problems [41].
Insulin Resistance
Insulin resistance is a prevalent characteristic of T2DM and cardiovascular diseases (CVDs). Recent research has shown that insulin resistance is an independent risk factor for CVD, affecting almost 80% of people with T2DM [42]. Rising incidence of cardiac infarction, endothelial damage, and stroke is linked to insulin resistance [20, 43]. It appears before the start of diabetes and is related to greater plasma endothelin and von Willebrand factor (vWF) levels even in the absence of diabetes. Insulin resistance induces a rise in blood pressure, which induces the pathways that include sympathetic nervous system activation, renal sodium retention, transmembrane action transport, growth-promoting action of vascular SMCs, and vascular hyper-reactivity [44, 45]. Patients with insulin resistance produce less NO and higher levels of angiotensin and endothelin-1 (ET-1). Insulin stimulates NO, which causes vasodilation and an increase in glucose uptake. Vascular insulin resistance disrupts skeletal muscles blood flow [45, 46]. Furthermore, insulin resistance causes AS and impaired vascular function by reducing fibrinolysis [47]. In patients with insulin resistance, C-creative protein (CRP) levels are elevated, which blocks NO production in the endothelium and increases ET-1 and interleukin (IL)-6 [29].
Oxidative Stress
The role of oxidative stress in people with diabetes vasculopathy is widely accepted. People with diabetes experience higher oxidative stress as a result of free radical generation [48]. Free radicals cause tissue damage in diabetes, which occurs through many metabolic pathways: (i) hyperglycemia-induced ROS formation; (ii) an increase in glucose, unsaturated fat, and glycated protein oxidation; and (iii) an increase in glucose auto-oxidation. These pathways result in increased generation of superoxide ions (O2·− ), hydroxyl radicals (OH·), and peroxides [49]. Superoxide prevents ECs from secreting NO and reduces NO in the subendothelial area. ROS causes cross-linking and fragmentation of lipids and proteins. ROS also hasten the production of AGE, which delivers more free radicals that enhance LDL oxidation. All of these inhibit NO-dependent vasodilation [50, 51].
Activation of PKC
PKC is an intracellular secondary messenger that appears to be active in the tissues of patients with T2DM, such as the heart and aorta. Upon PKC system activation, intracellular hyperglycemia showed a link to the pathophysiology of diabetes complications. In diabetes, the beta isoform of PKC is involved in endothelial-dependent vasodilation abnormalities [29]. It promotes the production of superoxide ions, which react with NO to form peroxynitrite (ONOO), thus causing tissue damage and increased production of macrophages [52]. The PKC system participates in both growth factor transcription and signal transduction. PKC activity in the aftermath of hyperglycemia promotes platelet-derived growth factor (PDGF)-B receptor expression in SMCs and ECs [53, 54]. Furthermore, PKC activation induces the production of transforming growth factor (TGF)-β1, a critical growth factor that governs ECM synthesis. This increases proteoglycan and collagen gene expression while lowering the synthesis of proteolytic enzymes that break down matrix proteins [55]. TGFβ1 overexpression is considered to cause capillary basement membrane thickening and was one of the first structural anomalies detected in practically all tissues of the prediabetic rat.
Growth Factors and Cytokines
Diabetes is connected with the overexpression and activities of cytokine and growth factors. The proliferative cytokines epidermal growth factor and PDGF play a role in macrovascular damage [56]. Metabolic and hemodynamic variables appear to combine to increase the expression of cytokines and growth factors in different vascular areas, contributing to the typical dysfunction seen in diabetic vasculopathy [23]. After migration to the intima, T cell lymphocytes produce cytokines that affect the lesion development. Cytokines are produced by inflammatory cells and fat tissue in wounded tissue. Cytokines are inflammatory mediators that can be detected as a CVD marker. During the inflammatory phase, the release of cytokines and other inflammatory mediators causes cell migration. Interactions between inflammatory cells such as neutrophils, lymphocytes, monocytes/macrophages, and vascular cells (ECs and SMC) characterize the inflammatory response. During inflammation, several cytokines are present, and each has the potential to influence the nature of the inflammatory response [29, 57]. Moreover, pro-inflammatory cytokines may play a role in the destabilization and disintegration of atherosclerotic plaque, as well as the overexpression of matrix metalloproteinases, which are known to play a role in vascular remodeling. Pro-inflammatory cytokine levels that are elevated are CVD markers [58].
Diabetes and Vascular Injury: Mechanism and Complications
The relationship between diabetic vasculopathy and pathological change is closely intertwined. Both diabetes and AS lead to vascular injury, initiating the process of injury repair [22, 59]. In patients with diabetic vasculopathy, vascular damage is consistently observed, often accompanied by multiple comorbidities [1, 9]. Diabetic vasculopathy is characterized by several pathological conditions including endothelial damage, thrombosis, systemic inflammation, and impaired vascular tone/function [5, 60]. Moreover, diabetes hinders the natural progression of tissue restoration throughout the phases of healing [25]. Vascular problems, particularly in T2DM, can have systemic repercussions throughout the body. These vascular deficits might manifest as cardiovascular illness, which eventually leads to peripheral vascular disease (PVD), a disorder that compromises the correct function of the peripheral vessels [61, 62]. Several mechanisms have been identified as contributing to poor diabetic foot ulcer (DFU) healing in previous research, including microbial invasion, epithelial disintegration, and reduced immunological function [63]. The compromised circulatory function of vessels, which can contribute to insufficient healing, is one underlying reason that affects all diabetic ulcers [64]. The mainstream research on vascular function in diabetic wound healing has focused on the altered angiogenic phase that occurs during wound healing in people with diabetes [8, 14, 18, 64]. Few studies have looked at the later stages of wound healing to see if changes in maturity and vascular architecture play a role in diabetes-related poor healing. The subsections that follow will discuss the most prevalent macrovascular issues linked with diabetes (Fig. 2), as well as the clinical symptoms that are linked to macrovascular injury and its therapeutic strategies.
Coronary Heart Disease
T2DM is closely linked to coronary heart disease and this substantial link has been demonstrated in numerous investigations, beginning with the Framingham study [65]. T2DM affects not just the incidence of coronary heart disease (CHD) but also people who have had a coronary intervention. Stent thrombosis, ST-elevation myocardial infarction (STEMI), target lesion revascularization (TLR), and death were examined in a cohort study of 3655 consecutive patients with STEMI treated with primary percutaneous coronary intervention (PCI) and stent implantation (316 patients with DM, 8.6%; 3339 patients with DM, 91.4%) [66]. Diabetes also has a deleterious impact on patients undergoing coronary artery bypass graft (CABG) surgery [67, 68]. Another study compared total operational mortality and 12 morbidity outcomes in 6711 patients with and without T2DM over 8 years [69].
Cardiomyopathy
The term diabetes cardiomyopathy (DCM) was used to describe a cardiac condition characterized by aberrant myocardial performance or structure in the absence of epicardial CAD, hypertension, or severe valve disease [70, 71]. Diabetes-related cardiomyopathy is distinguished by heart hypertrophy and diastolic dysfunction [72]. Diabetes-related cardiomyopathy processes have garnered attention, particularly because of aberrant cardiac metabolism, glucotoxicity and lipotoxicity, and defective mitochondrial function, which causes oxidative stress and inflammation [70, 73]. The heart, unlike other organs, has high energy requirements and the primary sources of energy for cardiac function are fatty acid oxidation and aerobic glucose catabolism [74]. Insulin resistance stimulates hepatocyte lipid synthesis and adipocyte lipolysis, culminating in greater circulatory fatty acids and triglyceride levels. Lipid accumulation and fatty acid-induced lipotoxicity impair fatty acid oxidation activity in the heart, thus leading to endoplasmic reticulum (ER) stress, autophagy, apoptosis, and ventricular remodeling [74, 75]. The primary diabetic glycotoxin metabolites are AGEs, which are linked to the formation and progression of DCM [76, 77]. These by-products bind to AGE receptors (RAGEs) promoting the production of ROS, nuclear factor kappa-B (NF-kb), and pro-inflammatory cytokines such as IL-1, IL-6, IL-18, and tumor necrosis factor alpha (TNFα), which induces the intracellular production of ROS and initiates oxidative stress [2, 78, 79]. AGEs/RAGEs are responsible for structural alterations in the myocardium. RAGEs on EC macrophages and smooth muscle cells stimulate inflammatory signals via AGEs. This activation promotes the development of DCM by increasing ROS generation and decreasing nitric oxide synthesis [17, 80]. Hyperglycemia inhibits the production of the JunD-proto-oncogene component as well as the free radical scavengers superoxide dismutase 1 and aldehyde dehydrogenase 2 [81,82,83]. Furthermore, this process also regulates the release of inflammatory substances such as NFB and membrane cofactor protein-1 (MCP-1), as well as IL-6 and TNF, all of which contribute to myocardial deterioration and the advancement of heart failure [84, 85]. Elevated blood sugar levels enhance the expression of LncDACH1, which further exacerbates DCM by promoting mitochondrial oxidative stress and increasing the degradation of nicotinamide adenine dinucleotide (NAD)-dependent deacetylase sirtuin-3 (SIRT) through ubiquitination-mediated pathways, ultimately leading to increased mortality. PKC is a G protein-coupled receptor system effector, and vascular Ox-LDL controls vascular tone. Excess ROS, AGEs, and diacylglycerol (DAG) may activate PKC, affecting vascular smooth muscle (VSM) function and causing vascular hyperresponsiveness and remodeling as well as the acceleration of diabetic heart disease (DHD) development [86,87,88,89]. Hyperglycemia activates conventional inflammatory pathways as well as oxidative damage [90, 91]. Hyperglycemia increases the expression of MCP-1 and NLR family pyrin domain-containing 3 inflammasomes (NLPR3), causing myocardial fibrosis and cardiac failure, as well as exacerbating the development of DCM [91]. Thus, the structural function of the heart is compromised, which aids in the progression of DHD, through several molecular pathways working together.
Arrhythmias and Sudden Death
Chronic hyperglycemia in T2DM produces a variety of heart function abnormalities, including arrhythmias and sudden cardiac death (SCD). In T2DM, various forms of arrhythmias are mostly related to cardiac autonomic neuropathy [81, 92, 93]. Among the various arrhythmias, atrial fibrillation (AF) is the most common and important cardiac arrhythmia in clinical practice because of its association with increased cardiovascular and cerebrovascular morbidity and mortality [61, 94]. Recent research has found that people with diabetes are more likely to have AF. Movahed et al. studied 293,124 patients with diabetes and 552,624 patients with hypertension and found that diabetes was a significant risk factor for the occurrence of AF, which can lead to heart failure, left ventricular (LV) hypertrophy, and CAD [95].
Cerebrovascular Disease
One of the most devastating macrovascular complications of diabetes is stroke. Hyperglycemia raises the chance of having a stroke. This increased risk is widespread among people with diabetes and has been associated with worse clinical outcomes (including increased mortality), especially after the occurrence of the stroke [96, 97]. Elevated blood glucose levels are associated with pathological alterations in the brain and impaired brain function. Diabetes, as well as pre-DM, can enhance the development of dementia [76, 97, 98]. However, the imaging changes do not match the degree of cognitive impairment, and the process should be investigated further. Diabetic cerebral microangiopathy is characterized by several complex imaging changes (cerebral atrophy, subcortical microinfarcts, cerebral white matter hyperintensity, lacunar infarction, perivascular space, and cerebral microhemorrhage), as well as widespread deleterious consequences [2, 99].
The central nervous system is extremely reliant on glucose for energy. A disruption in carbohydrate metabolism can lead to an imbalance in cerebral energy metabolism and encourage lesion formation [20]. In diabetes, hyperactivation of the sorbitol route increases aldose reductase activity considerably and systemically. This causes insulin resistance, which causes extensive oxidative damage and an increase in inflammatory cytokines [100,101,102]. By modulating glucagon-like peptide (GLP)-1 receptors and insulin receptor substrate (IRS) receptors, the insulin receptor signaling system helps to maintain normal brain and cognitive processes [103, 104]. In tissue other than the brain, insulin stimulates the glucose transporter (GLUT) family of glucose transporters; however, in the brain, GLUT is directly regulated by glucose or cAMP [105, 106]. Dysfunction of vascular endothelial cells leads to the release of inflammatory mediators that compromise the blood–brain barrier (BBB), potentially exposing the brain parenchyma to neurotoxic proteins. IL-1, IL-6, IL-10, TNF, VCAM-1, matrix metalloproteinase-2 (MMP-2), and MMP-9 are classical inflammatory mediators that signal vascular neuroinflammation [107, 108]. P38 stimulates microglia and enhances nerve cell death by facilitating the mitogen-activated protein kinase (MAPK) pathway [109]. Hyperglycemia triggers inflammatory and adoptive reactions that expedite ER stress and mitochondrial dysfunction [24, 48, 110]. Moreover, glutamate serves as a vital excitatory neurotransmitter, with N-methyl-d-aspartic acid receptors (NMDA) playing a key role in regulating neurogenesis and synaptic plasticity [111, 112].
Peripheral Vascular (Arterial) Disease
People with diabetes are more likely to develop PVD, which, although frequently neglected, is one of the most serious and prevalent vascular consequences of diabetes. However, representative data are scarce on PVD in community-based office practice [67, 113]. In a clinically supervised cross-sectional study in Germany, general practitioners used bilateral Doppler ultrasound to calculate the ankle brachial index (ABI) of 6880 consecutive, unselected patients aged 65 years or older [114]. Poorer revascularization results are one of the negative effects of diabetes on vascular function. It appears that patients with PAD have a significantly higher rate of cardiovascular events [115]. A 3000-person Japanese clinical investigation found that low ABI is an independent risk factor promoting higher cardiovascular events and mortality in both individuals with and without diabetes [116]. PVD raises the incidence of not only coronary atherosclerotic events but also significant adverse limb events such as amputation in such patients [2]. PVD can cause diabetic foot syndrome and PAD, both of which have a negative impact on the quality of life in people with diabetes [117, 118]. Large artery AS has historically been thought to predominate in PAD. Energy and inflammation, oxidative stress, insulin resistance, AGEs, nerve growth factors, polyol pathway activation, and hexosamine and PKC pathway activation are essential pathogenic variables and processes shared by various DM vascular problems [76, 119]. Recent research has focused on glucose and fatty acid metabolism, brain metabolism, and exosome control. Peripheral neuropathy is much more understood than PVD. Glucose overload and high fatty acid metabolism result in decreased ATP synthesis, excessive ROS creation, and poor mitochondrial activity, all of which contribute to increased oxidative stress and the formation of AGEs from glycosylation of diverse proteins [120, 121]. The vicious circle of these events enhances ROS generation and ER stress, resulting in DNA damage and cell demise. These mechanisms finally manifest as elevated pro-inflammatory factors, which in turn drive the synthesis of AGEs, resulting in oxidative stress and endothelial dysfunction [122, 123].
Neovascularization: Mechanism, Structural, and Functional Characteristics
Diabetes, unlike diabetic nephropathy and retinopathy, reduces angiogenesis in wound healing [89, 113, 124]. Diabetes-related wounds have reduced vascularity and capillary density as a result of insufficient angiogenesis [125]. Furthermore, diabetes causes considerable wound closure delays, and chronic non-wounds are common. Numerous investigations have shown that inadequate angiogenesis contributes to the pathologic wound healing seen in diabetes [126,127,128,129]. Many of the described variations in wound angiogenic response that are noticed in the context of diabetes are reviewed below.
Role of the Immune System in Vascular Wound Healing
In the case of diabetic wounds, the activity of innate immune cells necessary for wound healing is disrupted [25, 130]. In typical wound healing, macrophages undergo a transition from a pro-inflammatory state to a pro-reparative state, promoting tissue regeneration. However, in diabetic wounds where macrophages are deficient, the altered morphology of the wounds fails to stimulate tissue repair effectively [12, 130, 131]. A recent study showed that recovery was markedly delayed in db/db mice [132,133,134,135]. Khanna et al. reported reduced efferocytosis as a result of macrophages at the wound site of db/db mice, resulting in an enhanced apoptotic burden and inflammatory profile [136]. Since macrophages are a major source of VEGF and other pro-angiogenic mediators in wounds, the observed reduction in diabetic wound angiogenesis may be connected to the lack of macrophage presence. A recent study found that VEGF-A protein and mRNA levels were considerably lower in wounds of db/db mice than in healthy controls [137]. A follow-up study by Galiano et al. confirmed that wounds in db/db mice treated with VEGF-A healed at a faster rate compared to the control group. Additionally, the study revealed that the VEGF-A-treated mice experienced increased vascular permeability, distorted blood vessels, and edema until the VEGF therapy was discontinued [138].
Role of MicroRNA in Wound Healing
MicroRNAs (miRNAs) can influence angiogenesis and other aspects of wound healing, and they are expressed differently in diabetic wounds [139, 140]. The miRNAs are non-coding and have a known role in post-translational modifications or gene silencing. During diabetic wound healing several miRNAs have been identified with altered expression [141, 142]. MiR26-b is a miRNA that is abundant in diabetic ECs, and inhibiting it in diabetic wound models improved wound closure and granulation tissue formation [143]. Furthermore, decreased expression of miR-200b, which has been shown to promote TNF expression, results in enhanced angiogenesis in diabetic wound skin [144]. In diabetic mice models, in vivo and in vitro studies using local miR27-b, which is considered to influence levels of angiogenic protein thrombospondin 1 (TSP1) in the wound bed, demonstrated that miR27-b restoration controls angiogenesis [145, 146].
Current Developments in Diabetic Vascular Angiopathy Treatments
Correcting insulin resistance, and beta cell dysfunction, normalizing hepatic glucose output, and preventing, delaying, or reversing diabetic consequences are all important components of the optimal type 2 diabetes treatment plan. The following section discusses the primary treatment modalities now available to manage type 2 diabetes: insulin, oral antidiabetic medications, and lifestyle adjustment including suitable diet and exercise programs. Treatments often advance in a stepwise manner, starting with lifestyle changes and progressively adding insulin and one or more oral medications. The search for viable medicines to address the large patient population impacted by chronic, non-healing lesions in diabetes has been fruitless. In this section, we explore the available medications that aim to enhance diabetic angiogenesis and vascular perfusion. Despite the progress made in research, moving from laboratory experiments to clinical trials and eventually to practical applications, these treatments have not proven to be the ultimate solution for healing chronic diabetic wounds [1]. In addition to hyperglycemia and hyperinsulinemia, type 2 diabetes is a diverse illness with several underlying pathophysiological processes. It is characterized by dyslipidemia, hypertension, and hypercoagulability. Table 1 lists the currently available treatment modalities.
Hyperbaric Oxygen Treatment
Hyperbaric oxygen treatment (HBOT) is one technique that has been widely used in clinics. HBOT involves a patient breathing 100% oxygen in a confined chamber with pressures higher than those seen at sea level. This treatment improves tissue hypoxia and vascular perfusion, reduces inflammation and edema, and increases angiogenesis [147]. Numerous studies in patients with DFU have indicated that those who receive HBOT have higher recovery rates and a lower chance of major limb amputation [148,149,150,151]. Unfortunately, HBOT is too expensive for many patients, and although it has a 20-year track record in the clinic, it is still not a full solution for treating non-healing diabetic foot lesions.
Therapies with VEGF and PDGF
Another therapy strategy has been to employ growth factors such as VEGF and PDGF. These molecules, as previously established, are crucial in the proliferative and maturation phases of wound healing. Several in vivo diabetic models have shown that administering VEGF and its isoforms topically promotes wound healing. However, in human DFUs, topical VEGF treatment with recombinant VEGF (rh-VEGF) (Telberim) had little effectiveness. In various phase I studies, patients who received topical VEGF had better recovery outcomes compared to those who did not. However, phase II clinical trials showed no substantial impact, which led to the discontinuation of the drug therapy [12, 138, 152, 153]. In 1997, becaplermin (Regranex) containing recombinant PDGF became available for the first time. In clinical research, topical becaplermin treatment resulted in a 43% increase in wound closure over placebo in patients, as well as a 32% reduction in time to wound closure and complete healing of ulcers in 57.5% of patients [154]. Unfortunately, becaplermin has been plagued by numerous problems. It is an expensive treatment. Furthermore, rash and burning sensations at the site of application, as well as higher risks of osteomyelitis and cellulitis, have been recorded [155]. The most concerning adverse side effect of the medicine is the possible elevated risk of cancer in users who receive more than three tubes of topical therapy, prompting the US Food and Drug Administration (FDA) to issue a warning. As a result, despite encouraging findings in animal models, topical growth factors have yet to translate successfully to the clinic [153]. While single growth factors have had limited effectiveness in the treatment of wounds, platelet-derived therapies have been proposed as a prospective enhancement since they supply a variety of factors. Platelets contain a high concentration of growth factors such as PDGF, TGF, FGF-2, EGF, and VEGF. Platelet derivatives, such as platelet-rich plasma, platelet gel, and platelet-rich fibrin, have thus been investigated for repair and regeneration procedures in both hard and soft tissues. Platelet derivatives have several advantages, including the multifactorial approach and the ability to create the derivatives from the patient’s platelets, reducing patient exposure to exogenous drugs [156].
Aside from growth factors, several intriguing novel therapeutics for diabetic wounds are now being investigated. These include the utilization of cells like stem cells and macrophages, as well as sophisticated bioengineering technologies to stimulate tissue healing responses. Table 2 lists the drugs with their targets and mode of action as a result of clinical trials performed in mice studies.
Thiazolidinediones
The oral antidiabetic drugs known as thiazolidinediones offer a cutting-edge strategy for enhancing glycemic management through insulin resistance. Furthermore, thiazolidinediones have cardiovascular preventive qualities beyond glycemic management and reduce dyslipidemia, thereby decreasing the prevalence of CV problems [176]. Angiotensin-converting enzyme (ACE) inhibitors, in addition to antidiabetic medications, may postpone or prevent CV consequences in people with diabetes [177]. In addition to reducing diabetes-related microvascular and macrovascular problems, ACE inhibitor medication also seems to enhance insulin sensitivity and glucose metabolism. ACE inhibitors lower cardiovascular events in high-risk individuals by 22%, according to the Heart Outcomes Prevention Evaluation (HOPE) study. This medication is also linked to a large (34%) decrease in new diabetes diagnoses [178].
HMG-CoA Reductase Inhibitors
The benefits of primary and secondary prevention of vascular illnesses have been demonstrated by treating dyslipidemia in type 2 diabetes with statins (HMG-CoA reductase inhibitors) [179,180,181]. Furthermore, several studies have demonstrated advantages linked to the use of fibrates. Statins reduce LDL-C, enhance TC/HDL-cholesterol (HDL-C) and decrease apolipoprotein B; fibrates decrease TGs. They also increase HDL-C, decrease TC/HDL-C, and change the size of LDL particles from smaller to larger. These medications have beneficial effects on various components of the insulin resistance syndrome [182, 183]. They may affect CV risk variables and reduce CV mortality in T2DM and patients with insulin resistance as insulin sensitizers.
SGLTs, DPP4 Inhibitors, and GLP-1RAs in Diabetes and Vasculopathy
Recent evidence has suggested that sodium-glucose cotransporter 2 (SGLTs) inhibitors not only regulate glucose levels but also have a protective effect on macro- and microvascular levels [184]. Specifically, the EMPA-REG outcome trial, which was focused on empagliflozin, demonstrated that this medication reduced the risk of developing or worsening nephropathy in individuals with T2DM who were at high risk for cardiovascular complications when compared to placebo [185].
Dipeptidyl peptidase 4 (DPP4) inhibitors are orally administered antidiabetic drugs with low molecular weight that specifically and rapidly inhibit DPP enzymatic activity [186]. DPP is an enzyme found on the surface of most cell types that can break down various substances, including GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) [187]. Inhibiting DPP can enhance insulin secretion from pancreatic cells and suppress glucagon secretion by prolonging the effects of GLP-1 and GIP in the body, thus lowering blood glucose levels. All DPP inhibitors that have been approved demonstrate similar effectiveness in reducing glycemic levels, resulting in a moderate reduction (0.5–0.8%) in HbA1c [188]. There have been very few direct comparisons of DPP inhibitors in head-to-head trials. In an 18-week trial involving 800 patients with inadequately controlled type 2 diabetes on metformin, saxagliptin 5 mg daily and sitagliptin 100 mg showed similar reductions in HbA1c (− 0.52% vs − 0.26%) [189]. While the risk of hypoglycemia is low, DPP inhibitors do not provide cardiovascular benefits, and there have been concerns regarding their association with heart failure risk since their clinical use began [186].
The effect of GLP-1 receptor agonists (GLP-1RAs) on glycemic control varies depending on whether they are short-acting or long-acting preparations [190, 191]. Short-acting GLP-1RAs primarily work by slowing down the emptying of the stomach, as well as increasing insulin secretion, leading to a reduction in post-meal glucose levels. On the other hand, long-term GLP-1RAs focus on lowering fasting blood glucose levels by stimulating insulin secretion and reducing glucagon [192]. These differences in pharmacodynamics, along with the varying half-lives, may contribute to the differences in effectiveness observed in clinical trials [191, 193].
Insulin Therapy
While monotherapy is typically the initial recommendation, it may be necessary to use combination therapy with medications that have additive or synergistic effects to achieve proper blood glucose control [29]. In the long term, exogenous insulin maybe required, often in combination with oral medications, as the natural progression of the disease is characterized by a gradual depletion of beta cells. Furthermore, as a result of insulin resistance and the prevalence of metabolic syndrome in patients with T2DM, a comprehensive approach involving aggressive treatment of arterial hypertension and dyslipidemia is recommended to minimize the occurrence of diabetes-related complications [29, 178].
Conclusion
The processes underlying the development of macrovasculopathy in T2DM are complex and remain unknown. Diabetes-related metabolic dysregulation has a negative impact on every cellular constituent within the arterial wall, promoting various macrovascular illnesses through endothelial dysfunction, vasoconstriction, and inflammation. Diabetes can cause accelerated AS and an increased risk of thrombotic vascular events due to dyslipidemia, endothelial dysfunction, platelet hyper-reactivity, poor fibrinolytic balance, and irregular blood flow. The initiators of vasculopathy, which eventually lead to long-term consequences, can be treated and avoided through tight glycemic management, normal lipid profiles, frequent physical exercise, a healthy lifestyle, and pharmaceutical therapies.
References
Okonkwo UA, Dipietro LA. Diabetes and wound angiogenesis. Int J Mol Sci. 2017. https://doi.org/10.3390/IJMS18071419.
Li Y, Liu Y, Liu S, et al. Diabetic vascular diseases: molecular mechanisms and therapeutic strategies. Signal Transduct Target Ther. 2023. https://doi.org/10.1038/s41392-023-01400-z.
Shaw JE, Sicree RA, Zimmet PZ. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res Clin Pract. 2010;87:4–14. https://doi.org/10.1016/J.DIABRES.2009.10.007.
Harding JL, Pavkov ME, Magliano DJ, Shaw JE, Gregg EW. Global trends in diabetes complications: a review of current evidence. Diabetologia. 2019;62:3–16. https://doi.org/10.1007/S00125-018-4711-2.
Tomic D, Shaw JE, Magliano DJ. The burden and risks of emerging complications of diabetes mellitus. Nat Rev Endocrinol. 2022;18:525–39. https://doi.org/10.1038/s41574-022-00690-7.
Zimmet P, Alberti KGMM, Shaw J. Global and societal implications of the diabetes epidemic. Nature. 2001;414:782–7. https://doi.org/10.1038/414782a.
Fowler MJ. Microvascular and macrovascular complications of diabetes. Clin Diabetes. 2008;26:77–82. https://doi.org/10.2337/diaclin.26.2.77.
Kong P, Xie X, Li F, Liu Y, Lu Y. Placenta mesenchymal stem cell accelerates wound healing by enhancing angiogenesis in diabetic Goto-Kakizaki (GK) rats. Biochem Biophys Res Commun. 2013;438:410–9. https://doi.org/10.1016/j.bbrc.2013.07.088.
Okonkwo UA, Chen L, Ma D, et al. Compromised angiogenesis and vascular integrity in impaired diabetic wound healing. PLoS ONE. 2020. https://doi.org/10.1371/JOURNAL.PONE.0231962.
Demidova-Rice TN, Hamblin MR, Herman IM. Acute and impaired wound healing: pathophysiology and current methods for drug delivery, part 1: normal and chronic wounds: biology, causes, and approaches to care. Adv Skin Wound Care. 2012;25:304–14. https://doi.org/10.1097/01.ASW.0000416006.55218.D0.
Singh MR, Saraf S, Vyas A, Jain V, Singh D. Innovative approaches in wound healing: trajectory and advances. Artif Cells Nanomed Biotechnol. 2013;41:202–12. https://doi.org/10.3109/21691401.2012.716065.
Johnson KE, Wilgus TA. Vascular endothelial growth factor and angiogenesis in the regulation of cutaneous wound repair. Adv Wound Care. 2014;3:647. https://doi.org/10.1089/WOUND.2013.0517.
Wietecha MS, Król MJ, Michalczyk ER, Chen L, Gettins PG, Dipietro LA. Pigment epithelium-derived factor as a multifunctional regulator of wound healing. Am J Physiol Heart Circ Physiol. 2015;309:H812–26. https://doi.org/10.1152/AJPHEART.00153.2015.
Chen L, Dipietro LA. Production and function of pigment epithelium-derived factor in isolated skin keratinocytes. Exp Dermatol. 2014;23:436–8. https://doi.org/10.1111/EXD.12411.
Schalkwijk CG, Micali LR, Wouters K. Advanced glycation endproducts in diabetes-related macrovascular complications: focus on methylglyoxal. Trends Endocrinol Metab. 2023;34:49–60. https://doi.org/10.1016/J.TEM.2022.11.004.
Rungratanawanich W, Qu Y, Wang X, Essa MM, Song BJ. Advanced glycation end products (AGEs) and other adducts in aging-related diseases and alcohol-mediated tissue injury. Exp Mol Med. 2021;53:168–88. https://doi.org/10.1038/s12276-021-00561-7.
Orasanu G, Plutzky J. The pathologic continuum of diabetic vascular disease. J Am Coll Cardiol. 2009. https://doi.org/10.1016/j.jacc.2008.09.055.
Schelbert HR. Coronary circulatory function abnormalities in insulin resistance. Insights from positron emission tomography. J Am Coll Cardiol. 2009;53:3–8.
Isomaa B, Almgren P, Tuom T. Cardiovascular morbidity and mortality. Diabetes Care. 2001;24:683–9.
Mota RI, Morgan SE, Bahnson EM. Diabetic vasculopathy: macro and microvascular injury. Curr Pathobiol Rep. 2020. https://doi.org/10.1007/S40139-020-00205-X.
Paneni F, Beckman JA, Creager MA, Cosentino F. Diabetes and vascular disease: pathophysiology, clinical consequences, and medical therapy: part I. Eur Heart J. 2013;34:2436–43. https://doi.org/10.1093/EURHEARTJ/EHT149.
Beckman JA, Paneni F, Cosentino F, Creager MA. Diabetes and vascular disease: pathophysiology, clinical consequences, and medical therapy: part II. Eur Heart J. 2013;34:2444–56. https://doi.org/10.1093/EURHEARTJ/EHT142.
Cooper ME, Bonnet F, Oldfield M, Jandeleit-Dahm K. Mechanisms of diabetic vasculopathy: an overview. Am J Hypertens. 2001;14:475–86. https://doi.org/10.1016/S0895-7061(00)01323-6.
Papachristoforou E, Lambadiari V, Maratou E, Makrilakis K. Association of glycemic indices (hyperglycemia, glucose variability, and hypoglycemia) with oxidative stress and diabetic complications. J Diabetes Res. 2020. https://doi.org/10.1155/2020/7489795.
Patel S, Srivastava S, Singh MR, Singh D. Mechanistic insight into diabetic wounds: pathogenesis, molecular targets and treatment strategies to pace wound healing. Biomed Pharmacother. 2019;112: 108615. https://doi.org/10.1016/J.BIOPHA.2019.108615.
Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329:977–86. https://doi.org/10.1056/NEJM199309303291401.
Aronson D, Rayfield EJ. How hyperglycemia promotes atherosclerosis: molecular mechanisms. Cardiovasc Diabetol. 2002. https://doi.org/10.1186/1475-2840-1-1.
Flier JS, Underhill LH, Brownlee M, Cerami A, Vlassara H. Advanced glycosylation end products in tissue and the biochemical basis of diabetic complications. N Engl J Med. 1988;318:1315–21. https://doi.org/10.1056/NEJM198805193182007.
Rahman S, Rahman T, Ismail AAS, Rashid ARA. Diabetes-associated macrovasculopathy: pathophysiology and pathogenesis. Diabetes Obes Metab. 2007;9:767–80. https://doi.org/10.1111/J.1463-1326.2006.00655.X.
Gao S, Zhang Y, Liang K, Bi R, Du Y. Mesenchymal stem cells (MSCs): a novel therapy for type 2 diabetes. Stem Cells Int. 2022. https://doi.org/10.1155/2022/8637493.
Elshemy MM, Asem M, Allemailem KS, Uto K, Ebara M, Nabil A. Antioxidative capacity of liver- and adipose-derived mesenchymal stem cell-conditioned media and their applicability in treatment of type 2 diabetic rats. Oxid Med Cell Longev. 2021. https://doi.org/10.1155/2021/8833467.
Cooper-DeHoff RM, Pacanowski MA, Pepine CJ. Cardiovascular therapies and associated glucose homeostasis. Implications across the dysglycemia continuum. J Am Coll Cardiol. 2009. https://doi.org/10.1016/j.jacc.2008.10.037.
Watkins PJ. ABC of diabetes: cardiovascular disease, hypertension, and lipids. BMJ. 2003;326:874. https://doi.org/10.1136/BMJ.326.7394.874.
Steinberg D. Low density lipoprotein oxidation and its pathobiological significance. J Biol Chem. 1997;272:20963–6. https://doi.org/10.1074/jbc.272.34.20963.
Moldogazieva NT, Mokhosoev IM, Mel’Nikova TI, Porozov YB, Terentiev AA. Oxidative stress and advanced lipoxidation and glycation end products (ALEs and AGEs) in aging and age-related diseases. Oxid Med Cell Longev. 2019. https://doi.org/10.1155/2019/3085756.
Schwartz CJ, Valente AJ, Sprague EA, Kelley JL, Cayatte AJ, Rozek MM. Pathogenesis of the atherosclerotic lesion. Implications for diabetes mellitus. Diabetes Care. 1992;15:1156–67. https://doi.org/10.2337/DIACARE.15.9.1156.
Meeuwisse-Pasterkamp SH, van der Klauw MM, Wolffenbuttel BHR. Type 2 diabetes mellitus: prevention of macrovascular complications. Expert Rev Cardiovasc Ther. 2008;6:323–41. https://doi.org/10.1586/14779072.6.3.323.
Dzau VJ. Tissue angiotensin and pathobiology of vascular disease a unifying hypothesis. Hypertension. 2001;37:1047–52. https://doi.org/10.1161/01.HYP.37.4.1047.
Schmidt AM. Diabetes mellitus and cardiovascular disease. Arterioscler Thromb Vasc Biol. 2019;39:558–68. https://doi.org/10.1161/ATVBAHA.119.310961.
Bucala R, Makita Z, Koschinsky T, Cerami A, Vlassara H. Lipid advanced glycosylation: pathway for lipid oxidation in vivo. Proc Natl Acad Sci USA. 1993;90:6434–8. https://doi.org/10.1073/PNAS.90.14.6434.
Yamagishi S, Matsui T, Nakamura K. Kinetics, role and therapeutic implications of endogenous soluble form of receptor for advanced glycation end products (SRAGE) in diabetes. Curr Drug Targets. 2007;8:1138–43. https://doi.org/10.2174/138945007782151298.
Bonora E, Formentini G, Calcaterra F, et al. HOMA-estimated insulin resistance is an independent predictor of cardiovascular disease in type 2 diabetic subjects: prospective data from the verona diabetes complications study. Diabetes Care. 2002;25:1135–41. https://doi.org/10.2337/DIACARE.25.7.1135.
Båvenholm P, Proudler A, Tornvall P, et al. Insulin, intact and split proinsulin, and coronary artery disease in young men. Circulation. 1995;92:1422–9. https://doi.org/10.1161/01.CIR.92.6.1422.
D’souza, Anna Marie. The effects of leptin knockout and insulin suppression on glucose metabolism in rodents. T. University of British Columbia, 2017. Web. 24 Jan. 2024. Electronic Theses and Dissertations (ETDs) 2008+. https://doi.org/10.14288/1.0354409
Patel TP, Rawal K, Bagchi AK, et al. Insulin resistance: an additional risk factor in the pathogenesis of cardiovascular disease in type 2 diabetes. Heart Fail Rev. 2016;21:11–23. https://doi.org/10.1007/s10741-015-9515-6.
Egan BM, Greene EL, Goodfriend TL. Insulin resistance and cardiovascular disease. Am J Hypertens. 2001;14:116S-125S. https://doi.org/10.1016/S0895-7061(01)02078-7/2/AJH.116S.F4.JPEG.
Meigs JB, D’Agostino RB, Wilson PWF, Cupples LA, Nathan DM, Singer DE. Risk variable clustering in the insulin resistance syndrome: the Framingham offspring study. Diabetes. 1997;46:1594–600. https://doi.org/10.2337/DIACARE.46.10.1594.
Fiorentino T, Prioletta A, Zuo P, Folli F. Hyperglycemia-induced oxidative stress and its role in diabetes mellitus related cardiovascular diseases. Curr Pharm Des. 2013;19:5695–703. https://doi.org/10.2174/1381612811319320005.
Baynes JW. Role of oxidative stress in development of complications in diabetes. Diabetes. 1991;40:405–12. https://doi.org/10.2337/DIAB.40.4.405.
Tesfamariam B, Cohen RA. Free radicals mediate endothelial cell dysfunction caused by elevated glucose. Am J Physiol. 1992. https://doi.org/10.1152/AJPHEART.1992.263.2.H321.
Giugliano D, Ceriello A, Paolisso G. Oxidative stress and diabetic vascular complications. Diabetes Care. 1996;19:257–67. https://doi.org/10.2337/DIACARE.19.3.257.
Hamilton SJ, Watts GF. Endothelial dysfunction in diabetes: pathogenesis, significance, and treatment. Rev Diabet Stud. 2013;10:133. https://doi.org/10.1900/RDS.2013.10.133.
Kawano M, Koshikawa T, Kanzaki T, Morisaki N, Saito Y, Yoshida S. Diabetes mellitus induces accelerated growth of aortic smooth muscle cells: association with overexpression of PDGF beta-receptors. Eur J Clin Invest. 1993;23:84–90. https://doi.org/10.1111/J.1365-2362.1993.TB00745.X.
Inaba T, Ishibashi S, Gotoda T, et al. Enhanced expression of platelet-derived growth factor-beta receptor by high glucose. Involvement of platelet-derived growth factor in diabetic angiopathy. Diabetes. 1996;45:507–12. https://doi.org/10.2337/DIAB.45.4.507.
Blankenberg FG, Wen P, Dai M, et al. Detection of early atherosclerosis with radiolabeled monocyte chemoattractant protein-1 in prediabeteic Zucker rats. Pediatr Radiol. 2001;31:827–35. https://doi.org/10.1007/S002470100000/METRICS.
Gilbert RE, Rumble JR, Cao Z, et al. Endothelin receptor antagonism ameliorates mast cell infiltration, vascular hypertrophy, and epidermal growth factor expression in experimental diabetes. Circ Res. 2000;86:158–65. https://doi.org/10.1161/01.RES.86.2.158.
Haybar H, Bandar B, Torfi E, Mohebbi A, Saki N. Cytokines and their role in cardiovascular diseases. Cytokine. 2023. https://doi.org/10.1016/J.CYTO.2023.156261.
Blake GJ, Ridker PM. Novel clinical markers of vascular wall inflammation. Circ Inflamm. 2001. https://doi.org/10.1161/hh2101.099270.
Lüscher TF, Creager MA, Beckman JA, Cosentino F. Diabetes and vascular disease. Pathophysiology, clinical consequences, and medical therapy: part II. Circulation. 2003;108:1655–61. https://doi.org/10.1161/01.CIR.0000089189.70578.E2.
Shah AD, Langenberg C, Rapsomaniki E, et al. Type 2 diabetes and incidence of cardiovascular diseases: a cohort study in 1·9 million people. Lancet Diabetes Endocrinol. 2015;3:105–13. https://doi.org/10.1016/S2213-8587(14)70219-0.
Kosiborod M, Gomes MB, Nicolucci A, et al. Vascular Complications in patients with type 2 diabetes: prevalence and associated factors in 38 countries (the DISCOVER Study Program). Cardiovasc Diabetol. 2018. https://doi.org/10.1186/S12933-018-0787-8.
Sun B, Luo Z, Zhou J. Comprehensive elaboration of glycemic variability in diabetic macrovascular and microvascular complications. Cardiovasc Diabetol. 2021. https://doi.org/10.1186/s12933-020-01200-7.
Zhou X, Yu L, Zhao Y, Ge J. Panvascular medicine: an emerging discipline focusing on atherosclerotic diseases. Eur Heart J. 2022;43:4528–31. https://doi.org/10.1093/EURHEARTJ/EHAC448.
Pepine CJ. Insulin as a cardiovascular therapeutic: improving glycemic control in patients with coronary artery disease. J Am Coll Cardiol. 2009. https://doi.org/10.1016/j.jacc.2008.04.074.
Qazi MU, Malik S. Diabetes and cardiovascular disease: insights from the framingham heart study. Glob Heart. 2013;8:43–8. https://doi.org/10.1016/j.gheart.2012.12.008.
Jensen LO, Maeng M, Thayssen P, et al. Influence of diabetes mellitus on clinical outcomes following primary percutaneous coronary intervention in patients with ST-segment elevation myocardial infarction. Am J Cardiol. 2012;109:629–35. https://doi.org/10.1016/J.AMJCARD.2011.10.018.
Ram E, Sternik L, Klempfner R, et al. Type 2 diabetes mellitus increases the mortality risk after acute coronary syndrome treated with coronary artery bypass surgery. Cardiovasc Diabetol. 2020;19:1–9. https://doi.org/10.1186/S12933-020-01069-6/FIGURES/4.
Einarson TR, Acs A, Ludwig C, Panton UH. Prevalence of cardiovascular disease in type 2 diabetes: a systematic literature review of scientific evidence from across the world in 2007–2017. Cardiovasc Diabetol. 2018;17:83. https://doi.org/10.1186/s12933-018-0728-6.
Scott EW, Chris EAE. The influence of diabetes mellitus in patients undergoing coronary artery bypass graft surgery: a prospective cohort study. 2023. https://pubmed.ncbi.nlm.nih.gov/18807674/. Accessed 7 Sep 2023.
Jia G, Hill MA, Sowers JR. Diabetic cardiomyopathy. Circ Res. 2018;122:624–38. https://doi.org/10.1161/CIRCRESAHA.117.311586.
Rydén L, Armstrong PW, Cleland JGF, et al. Efficacy and safety of high-dose lisinopril in chronic heart failure patients at high cardiovascular risk, including those with diabetes mellitus: results from the ATLAS trial. Eur Heart J. 2000;21:1967–78. https://doi.org/10.1053/EUHJ.2000.2311.
Paolillo S, Marsico F, Prastaro M, et al. Diabetic cardiomyopathy: definition, diagnosis, and therapeutic implications. Heart Fail Clin. 2019;15:341–7. https://doi.org/10.1016/J.HFC.2019.02.003.
Tarquini R, Pala L, Brancati S, et al. Clinical approach to diabetic cardiomyopathy: a review of human studies. Curr Med Chem. 2017;25:1510–24. https://doi.org/10.2174/0929867324666170705111356.
Marwick TH, Ritchie R, Shaw JE, Kaye D. Implications of underlying mechanisms for the recognition and management of diabetic cardiomyopathy. J Am Coll Cardiol. 2018;71:339–51. https://doi.org/10.1016/J.JACC.2017.11.019.
Tawakol A, Jaffer F. Imaging the intersection of oxidative stress, lipids, and inflammation: progress toward personalized care of atherosclerosis. J Am Coll Cardiol. 2018;71:336–8. https://doi.org/10.1016/J.JACC.2017.11.031.
Khalid M, Petroianu G, Adem A. Advanced glycation end products and diabetes mellitus: mechanisms and perspectives. Biomolecules. 2022. https://doi.org/10.3390/BIOM12040542.
Adeshara KA, Bangar NS, Doshi PR, Diwan A, Tupe RS. Action of metformin therapy against advanced glycation, oxidative stress and inflammation in type 2 diabetes patients: 3 months follow-up study. Diabetes Metab Syndr Clin Res Rev. 2020;14:1449–58. https://doi.org/10.1016/j.dsx.2020.07.036.
Lin KH, Ali A, Kuo CH, et al. Carboxyl terminus of HSP70-interacting protein attenuates advanced glycation end products-induced cardiac injuries by promoting NFκB proteasomal degradation. J Cell Physiol. 2022;237:1888–901. https://doi.org/10.1002/JCP.30660.
Su SC, Hung YJ, Huang CL, et al. Cilostazol inhibits hyperglucose-induced vascular smooth muscle cell dysfunction by modulating the RAGE/ERK/NF-ΚB signaling pathways. J Biomed Sci. 2019. https://doi.org/10.1186/S12929-019-0550-9.
Twarda-clapa A, Olczak A, Białkowska AM, Koziołkiewicz M. Advanced glycation end-products (AGEs): formation, chemistry, classification, receptors, and diseases related to AGEs. Cells. 2022. https://doi.org/10.3390/CELLS11081312.
Hussain S, Khan AW, Akhmedov A, et al. Hyperglycemia induces myocardial dysfunction via epigenetic regulation of JunD. Circ Res. 2020;127:1261–73. https://doi.org/10.1161/CIRCRESAHA.120.317132.
Paneni F, Osto E, Costantino S, et al. Deletion of the activated protein-1 transcription factor JunD induces oxidative stress and accelerates age-related endothelial dysfunction. Circulation. 2013;127:1229–40. https://doi.org/10.1161/CIRCULATIONAHA.112.000826.
Costantino S, Akhmedov A, Melina G, et al. Obesity-induced activation of JunD promotes myocardial lipid accumulation and metabolic cardiomyopathy. Eur Heart J. 2019;40:997–1008. https://doi.org/10.1093/eurheartj/ehy903.
Wang Y, Luo W, Han J, et al. MD2 activation by direct AGE interaction drives inflammatory diabetic cardiomyopathy. Nat Commun. 2020;11:1–16. https://doi.org/10.1038/s41467-020-15978-3.
De Ferranti SD, De Boer IH, Fonseca V, et al. Type 1 diabetes mellitus and cardiovascular disease: a scientific statement from the American Heart Association and American Diabetes Association. Diabetes Care. 2014;37:2843–63. https://doi.org/10.2337/dc14-1720.
Zhang T, Sell P, Braun U, Leitges M. PKD1 protein is involved in reactive oxygen species-mediated mitochondrial depolarization in cooperation with protein kinase Cδ (PKCδ). J Biol Chem. 2015;290:10472. https://doi.org/10.1074/JBC.M114.619148.
Ishii H, Koya D, King GL. Protein kinase C activation and its role in the development of vascular complications in diabetes mellitus. J Mol Med. 1997;76:21–31. https://doi.org/10.1007/S001090050187.
Koya D, King GL. Protein kinase C activation and the development of diabetic complications. Diabetes. 1998;47:859–66. https://doi.org/10.2337/DIABETES.47.6.859.
Das Evcimen N, King GL. The role of protein kinase C activation and the vascular complications of diabetes. Pharmacol Res. 2007;55:498–510. https://doi.org/10.1016/j.phrs.2007.04.016.
Li G, Yang L, Feng L, et al. Front cover: syringaresinol protects against type 1 diabetic cardiomyopathy by alleviating inflammation responses, cardiac fibrosis, and oxidative stress. Mol Nutr Food Res. 2020;64:2070040. https://doi.org/10.1002/MNFR.202070040.
García-Díez E, López-Oliva ME, Caro-Vadillo A, et al. Supplementation with a cocoa-carob blend, alone or in combination with metformin, attenuates diabetic cardiomyopathy, cardiac oxidative stress and inflammation in Zucker diabetic rats. Antioxidants. 2022. https://doi.org/10.3390/ANTIOX11020432.
Al-Lahham S, Roelofsen H, Rezaee F, et al. Propionic acid affects immune status and metabolism in adipose tissue from overweight subjects. Eur J Clin Invest. 2012;42:357–64. https://doi.org/10.1111/J.1365-2362.2011.02590.X.
DeFronzo RA, Ferrannini E, Groop L, et al. Type 2 diabetes mellitus. Nat Rev Dis Prim. 2015;1:1–22. https://doi.org/10.1038/nrdp.2015.19.
Agarwal G, Singh S. Arrhythmias in type 2 diabetes mellitus. Indian J Endocrinol Metab. 2017;21:715. https://doi.org/10.4103/IJEM.IJEM_448_16.
Movahed M-R, Hashemzadeh M, Mazen Jamal M. Diabetes mellitus is a strong, independent risk for atrial fibrillation and flutter in addition to other cardiovascular disease. Int J Cardiol. 2005;105(3):315-8. https://doi.org/10.1016/j.ijcard.2005.02.050.
Chen R, Ovbiagele B, Feng W. Diabetes and stroke: epidemiology, pathophysiology, pharmaceuticals and outcomes. Am J Med Sci. 2016;351:380. https://doi.org/10.1016/J.AMJMS.2016.01.011.
Mosenzon O, Cheng AYY, Rabinstein AA, Sacco S. Diabetes and stroke: what are the connections? J Stroke. 2023;25:26. https://doi.org/10.5853/JOS.2022.02306.
Banday MZ, Sameer AS, Nissar S. Pathophysiology of diabetes: an overview. Avicenna J Med. 2020;10:174. https://doi.org/10.4103/AJM.AJM_53_20.
Li Y, Zeng KW, Wang XM. Cerebral microangiopathy of diabetes. Zhongguo Zhong Yao Za Zhi. 2017;42:2247–53. https://doi.org/10.19540/J.CNKI.CJCMM.2017.0104.
Singh M, Kapoor A, Bhatnagar A. Physiological and pathological roles of aldose reductase. Metabolites. 2021. https://doi.org/10.3390/METABO11100655.
Wilson DK, Bohren KM, Gabbay KH, Quiocho FA. An unlikely sugar substrate site in the 1.65 Å structure of the human aldose reductase holoenzyme implicated in diabetic complications. Science. 1992;257:81–4. https://doi.org/10.1126/SCIENCE.1621098.
Umegaki H, Hayashi T, Nomura H, et al. Cognitive dysfunction: an emerging concept of a new diabetic complication in the elderly. Geriatr Gerontol Int. 2013;13:28–34. https://doi.org/10.1111/J.1447-0594.2012.00922.X.
White MF. The IRS-signalling system in insulin and cytokine action. Philos Trans R Soc B Biol Sci. 1996;351:181–9. https://doi.org/10.1098/rstb.1996.0015.
White MF. The insulin signalling system and the IRS proteins. Diabetologia. 1997. https://doi.org/10.1007/S001250051387.
Furtado LM, Poon V, Klip A. GLUT4 activation: thoughts on possible mechanisms. Acta Physiol Scand. 2003;178:287–96. https://doi.org/10.1046/j.1365-201X.2003.01160.x.
Furtado LM, Somwar R, Sweeney G, Niu W, Klip A. Activation of the glucose transporter GLUT4 by insulin. Biochem Cell Biol. 2002;80:569–78. https://doi.org/10.1139/O02-156.
Theofilis P, Sagris M, Oikonomou E, et al. Inflammatory mechanisms contributing to endothelial dysfunction. Biomedicines. 2021. https://doi.org/10.3390/BIOMEDICINES9070781.
Mussbacher M, Salzmann M, Brostjan C, et al. Cell type specific roles of NF-κB linking inflamation and thrombosis. Front Immunol. 2019. https://doi.org/10.3389/fimmu.2019.00085.
Botham KM, Wheeler-Jones CPD. Postprandial lipoproteins and the molecular regulation of vascular homeostasis. Prog Lipid Res. 2013;52:446–64. https://doi.org/10.1016/j.plipres.2013.06.001.
Madonna R, De Caterina R. Cellular and molecular mechanisms of vascular injury in diabetes - part I: pathways of vascular disease in diabetes. Vascul Pharmacol. 2011;54:68–74. https://doi.org/10.1016/j.vph.2011.03.005.
Mattson MP. Glutamate and neurotrophic factors in neuronal plasticity and disease. Ann N Y Acad Sci. 2008;1144:97–112. https://doi.org/10.1196/ANNALS.1418.005.
Taylor S, Srinivasan B, Wordinger RJ, Roque RS. Glutamate stimulates neurotrophin expression in cultured müller cells. Mol Brain Res. 2003;111:189–97. https://doi.org/10.1016/S0169-328X(03)00030-5.
Huysman F, Mathieu C. Diabetes and peripheral vascular disease. Acta Chir Belg. 2009;109:587–94. https://doi.org/10.1080/00015458.2009.11680493.
Aquino R, Johnnides C, Makaroun M, et al. Natural history of claudication: long-term serial follow-up study of 1244 claudicants. J Vasc Surg. 2001;34:962–70. https://doi.org/10.1067/MVA.2001.119749.
Golledge J, Leicht A, Crowther RG, Clancy P, Spinks WL, Quigley F. Association of obesity and metabolic syndrome with the severity and outcome of intermittent claudication. J Vasc Surg. 2007;45:40–6. https://doi.org/10.1016/j.jvs.2006.09.006.
Yokoyama H, Sone H, Honjo J, et al. Relationship between a low ankle brachial index and all-cause death and cardiovascular events in subjects with and without diabetes. J Atheroscler Thromb. 2014;21:574–81. https://doi.org/10.5551/JAT.22491.
Altoijry A, AlGhofili H, Alanazi SN, et al. Diabetic foot and peripheral arterial disease: single centre experience. Saudi Med J. 2021;42:49–55. https://doi.org/10.15537/SMJ.2021.1.25640.
Al-Thani H, El-Menyar A, Koshy V, et al. Implications of foot ulceration in hemodialysis patients: a 5-year observational study. J Diabetes Res. 2014. https://doi.org/10.1155/2014/945075.
Rains JL, Jain SK. Oxidative stress, insulin signaling, and diabetes. Free Radic Biol Med. 2011;50:567–75. https://doi.org/10.1016/J.FREERADBIOMED.2010.12.006.
Newsholme P, Keane KN, Carlessi R, Cruzat V. Oxidative stress pathways in pancreatic β-cells and insulin-sensitive cells and tissues: importance to cell metabolism, function, and dysfunction. Am J Physiol Cell Physiol. 2019;317:C420–33. https://doi.org/10.1152/ajpcell.00141.2019.
Gurzov EN, Tran M, Fernandez-Rojo MA, et al. Hepatic oxidative stress promotes insulin-STAT-5 signaling and obesity by inactivating protein tyrosine phosphatase N2. Cell Metab. 2014;20:85. https://doi.org/10.1016/J.CMET.2014.05.011.
Malhotra JD, Kaufman RJ. Endoplasmic reticulum stress and oxidative stress: a vicious cycle or a double-edged sword? Antioxid Redox Signal. 2007;9:2277–93. https://doi.org/10.1089/ARS.2007.1782.
Malhotra JD, Kaufman RJ. The endoplasmic reticulum and the unfolded protein response. Semin Cell Dev Biol. 2007;18:716–31. https://doi.org/10.1016/j.semcdb.2007.09.003.
Kotlarsky P, Bolotin A, Dorfman K, Knyazer B, Lifshitz T, Levy J. Link between retinopathy and nephropathy caused by complications of diabetes mellitus type 2. Int Ophthalmol. 2015;35:59–66. https://doi.org/10.1007/S10792-014-0018-6.
Jawa A, Kcomt J, Fonseca VA. Diabetic nephropathy and retinopathy. Med Clin N Am. 2004;88:1001–36. https://doi.org/10.1016/j.mcna.2004.04.012.
Fadini GP, Albiero M, Bonora BM, Avogaro A. Angiogenic abnormalities in diabetes mellitus: mechanistic and clinical aspects. J Clin Endocrinol Metab. 2019;104:5431–44. https://doi.org/10.1210/JC.2019-00980.
Simo R, Carrasco E, Garcia-Ramirez M, Hernandez C. Angiogenic and antiangiogenic factors in proliferative diabetic retinopathy. Curr Diabetes Rev. 2006;2:71–98. https://doi.org/10.2174/157339906775473671.
Liu ZL, Chen HH, Zheng LL, Sun LP, Shi L. Angiogenic signaling pathways and anti-angiogenic therapy for cancer. Signal Transduct Target Ther. 2023;8:1–39. https://doi.org/10.1038/s41392-023-01460-1.
Caldwell RB, Bartoli M, Behzadian MA, et al. Vascular endothelial growth factor and diabetic retinopathy: pathophysiological mechanisms and treatment perspectives. Diabetes Metab Res Rev. 2003;19:442–55. https://doi.org/10.1002/dmrr.415.
Caputa G, Flachsmann LJ, Cameron AM. Macrophage metabolism: a wound-healing perspective. Immunol Cell Biol. 2019;97:268–78. https://doi.org/10.1111/IMCB.12237.
Wilson K. Wound healing: the role of macrophages. Nurs Crit Care. 1997;2:291–6.
Wang B, Chandrasekera P, Pippin J. Leptin- and leptin receptor-deficient rodent models: relevance for human type 2 diabetes. Curr Diabetes Rev. 2014;10:131–45. https://doi.org/10.2174/1573399810666140508121012.
Belke DD, Severson DL. Diabetes in mice with monogenic obesity: the db/db mouse and its use in the study of cardiac consequences. Methods Mol Biol. 2012;933:47–57. https://doi.org/10.1007/978-1-62703-068-7_4.
Hofmann A, Peitzsch M, Brunssen C, et al. Elevated steroid hormone production in the db/db mouse model of obesity and type 2 diabetes. Horm Metab Res. 2017;49:43–9. https://doi.org/10.1055/S-0042-116157.
Suriano F, Vieira-Silva S, Falony G, et al. Novel insights into the genetically obese (ob/ob) and diabetic (db/db) mice: two sides of the same coin. Microbiome. 2021. https://doi.org/10.1186/S40168-021-01097-8.
Khanna S, Biswas S, Shang Y, et al. Macrophage dysfunction impairs resolution of inflammation in the wounds of diabetic mice. PLoS ONE. 2023. https://doi.org/10.1371/journal.pone.0009539.
Chen S, Saeed AFUH, Liu Q, et al. Macrophages in immunoregulation and therapeutics. Signal Transduct Target Ther. 2023. https://doi.org/10.1038/s41392-023-01452-1.
Galiano RD, Tepper OM, Pelo CR, et al. Topical vascular endothelial growth factor accelerates diabetic wound healing through increased angiogenesis and by mobilizing and recruiting bone marrow-derived cells. Am J Pathol. 2004;164:1935–47. https://doi.org/10.1016/S0002-9440(10)63754-6.
Sun LL, Li WD, Lei FR, Li XQ. The regulatory role of microRNAs in angiogenesis-related diseases. J Cell Mol Med. 2018;22:4568–87. https://doi.org/10.1111/JCMM.13700.
Tiwari A, Mukherjee B, Dixit M. MicroRNA key to angiogenesis regulation: MiRNA biology and therapy. Curr Cancer Drug Targets. 2017;18:266–77. https://doi.org/10.2174/1568009617666170630142725.
Winkle M, El-Daly SM, Fabbri M, Calin GA. Noncoding RNA therapeutics — challenges and potential solutions. Nat Rev Drug Discov. 2021;20:629–51. https://doi.org/10.1038/s41573-021-00219-z.
Lenkala D, LaCroix B, Gamazon ER, Geeleher P, Im HK, Huang RS. The impact of MicroRNA expression on cellular proliferation. Hum Genet. 2014;133:931–8. https://doi.org/10.1007/s00439-014-1434-4.
Kim M, Zhang X. The profiling and role of MiRNAs in diabetes mellitus. J diabetes Clin Res. 2019;1:5. https://doi.org/10.33696/DIABETES.1.003.
Gollavilli PN, Parma B, Siddiqui A, et al. The role of MiR-200b/c in balancing EMT and proliferation revealed by an activity reporter. Oncogene. 2021;40:2309–22. https://doi.org/10.1038/s41388-021-01708-6.
Kottaisamy CPD, Raj DS, Prasanth Kumar V, Sankaran U. Experimental animal models for diabetes and its related complications—a review lab. Anim Res. 2021;37(1):14. https://doi.org/10.1186/S42826-021-00101-4.
Fang JY, Lin CH, Huang TH, Chuang SY. In vivo rodent models of type 2 diabetes and their usefulness for evaluating flavonoid bioactivity. Nutrients. 2019. https://doi.org/10.3390/NU11030530.
Tiaka EK, Papanas N, Manolakis AC, Maltezos E. The role of hyperbaric oxygen in the treatment of diabetic foot ulcers. Angioology. 2011;63:302–14. https://doi.org/10.1177/0003319711416804.
Kaya A, Aydin F, Altay T, Karapinar L, Ozturk H, Karakuzu C. Can major amputation rates be decreased in diabetic foot ulcers with hyperbaric oxygen therapy? Int Orthop. 2009;33:441. https://doi.org/10.1007/S00264-008-0623-Y.
Abidia A, Laden G, Kuhan G, et al. The role of hyperbaric oxygen therapy in ischaemic diabetic lower extremity ulcers: a double-blind randomized-controlled trial. Eur J Vasc Endovasc Surg. 2003;25:513–8. https://doi.org/10.1053/EJVS.2002.1911.
Al-Waili NS, Butler GJ, Beale J, et al. Influences of hyperbaric oxygen on blood pressure, heart rate and blood glucose levels in patients with diabetes mellitus and hypertension. Arch Med Res. 2006;37:991–7. https://doi.org/10.1016/J.ARCMED.2006.05.009.
Stoekenbroek RM, Santema TB, Legemate DA, Ubbink DT, Van Den Brink A, Koelemay MJW. Hyperbaric oxygen for the treatment of diabetic foot ulcers: a systematic review. Eur J Vasc Endovasc Surg. 2014;47:647–55. https://doi.org/10.1016/J.EJVS.2014.03.005.
Kwon MJ, An S, Choi S, et al. Effective healing of diabetic skin wounds by using nonviral gene therapy based on minicircle vascular endothelial growth factor DNA and a cationic dendrimer. J Gene Med. 2012;14:272–8. https://doi.org/10.1002/JGM.2618.
Barrientos S, Brem H, Stojadinovic O, Tomic-Canic M. Clinical application of growth factors and cytokines in wound healing. Wound Repair Regen. 2014;22:569. https://doi.org/10.1111/WRR.12205.
Steed DL. Clinical evaluation of recombinant human platelet-derived growth factor for the treatment of lower extremity ulcers. Plast Reconstr Surg. 2006. https://doi.org/10.1097/01.PRS.0000222526.21512.4C.
Smiell JM, Wieman TJ, Steed DL, Perry BH, Sampson AR, Schwab BH. Efficacy and safety of becaplermin (recombinant human platelet-derived growth factor-BB) in patients with nonhealing, lower extremity diabetic ulcers: a combined analysis of four randomized studies. Wound Repair Regen. 1999;7:335–46. https://doi.org/10.1046/J.1524-475X.1999.00335.X.
De Pascale MR, Sommese L, Casamassimi A, Napoli C. Platelet derivatives in regenerative medicine: an update. Transfus Med Rev. 2015;29:52–61. https://doi.org/10.1016/J.TMRV.2014.11.001.
Bagheri M, Jahromi BM, Mirkhani H, et al. Azelnidipine, a new calcium channel blocker, promotes skin wound healing in diabetic rats. J Surg Res. 2011. https://doi.org/10.1016/J.JSS.2011.02.039.
Babaei S, Bayat M, Nouruzian M, Bayat M. Pentoxifylline improves cutaneous wound healing in streptozotocin-induced diabetic rats. Eur J Pharmacol. 2013;700:165–72. https://doi.org/10.1016/J.EJPHAR.2012.11.024.
Hamed S, Ullmann Y, Masoud M, Hellou E, Khamaysi Z, Teot L. Topical erythropoietin promotes wound repair in diabetic rats. J Invest Dermatol. 2010;130:287–94. https://doi.org/10.1038/JID.2009.219.
Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group (1998). Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. New Engl J Med. 1998;339(19):1349–57. https://doi.org/10.1056/NEJM199811053391902.
Scott JR, Tamura RN, Muangman P, Isik FF, Xie C, Gibran NS. Topical substance P increases inflammatory cell density in genetically diabetic murine wounds. Wound Repair Regen. 2008;16:529–33. https://doi.org/10.1111/J.1524-475X.2008.00400.X.
Hou Z, Nie C, Si Z, Ma Y. Deferoxamine enhances neovascularization and accelerates wound healing in diabetic rats via the accumulation of hypoxia-inducible factor-1α. Diabetes Res Clin Pract. 2013;101:62–71. https://doi.org/10.1016/J.DIABRES.2013.04.012.
Romana-Souza B, Nascimento AP, Monte-Alto-Costa A. Propranolol improves cutaneous wound healing in streptozotocin-induced diabetic rats. Eur J Pharmacol. 2009;611:77–84. https://doi.org/10.1016/J.EJPHAR.2009.03.053.
Kaur P, Sharma AK, Nag D, et al. Novel nano-insulin formulation modulates cytokine secretion and remodeling to accelerate diabetic wound healing. Nanomed Nanotechnol Biol Med. 2019;15:47–57. https://doi.org/10.1016/J.NANO.2018.08.013.
Lee CH, Chang SH, Chen WJ, et al. Augmentation of diabetic wound healing and enhancement of collagen content using nanofibrous glucophage-loaded collagen/PLGA scaffold membranes. J Colloid Interface Sci. 2015;439:88–97. https://doi.org/10.1016/J.JCIS.2014.10.028.
Wang X, Sng MK, Foo S, et al. Early controlled release of peroxisome proliferator-activated receptor β/δ agonist gw501516 improves diabetic wound healing through redox modulation of wound microenvironment. J Control Release. 2015;197:138–47. https://doi.org/10.1016/J.JCONREL.2014.11.001.
Young GH, Lin JT, Cheng YF, et al. Modulation of adenine phosphoribosyltransferase-mediated salvage pathway to accelerate diabetic wound healing. FASEB J. 2021;35:e21296–e21296. https://doi.org/10.1096/FJ.202001736RR.
Whittam AJ, Maan ZN, Duscher D, et al. Small molecule inhibition of dipeptidyl peptidase-4 enhances bone marrow progenitor cell function and angiogenesis in diabetic wounds. Transl Res. 2019;205:51–63. https://doi.org/10.1016/J.TRSL.2018.10.006.
Hozzein WN, Badr G, Badr BM, et al. Bee venom improves diabetic wound healing by protecting functional macrophages from apoptosis and enhancing Nrf2, Ang-1 and Tie-2 signaling. Mol Immunol. 2018;103:322–35. https://doi.org/10.1016/J.MOLIMM.2018.10.016.
Kawai K, Kageyama A, Tsumano T, et al. Effects of adiponectin on growth and differentiation of human keratinocytes—implication of impaired wound healing in diabetes. Biochem Biophys Res Commun. 2008;374:269–73. https://doi.org/10.1016/J.BBRC.2008.07.045.
Moura LIF, Dias AMA, Leal EC, Carvalho L, De Sousa HC, Carvalho E. Chitosan-based dressings loaded with neurotensin–an efficient strategy to improve early diabetic wound healing. Acta Biomater. 2014;10:843–57. https://doi.org/10.1016/J.ACTBIO.2013.09.040.
Gooyit M, Peng Z, Wolter WR, et al. A chemical biological strategy to facilitate diabetic wound healing. ACS Chem Biol. 2014;9:105–10. https://doi.org/10.1021/CB4005468.
Galeano M, Polito F, Bitto A, et al. Systemic administration of high-molecular weight hyaluronan stimulates wound healing in genetically diabetic mice. Biochim Biophys Acta. 2011;1812:752–9. https://doi.org/10.1016/J.BBADIS.2011.03.012.
Chong HC, Chan JSK, Goh CQ, et al. Angiopoietin-like 4 stimulates STAT3-mediated INOS expression and enhances angiogenesis to accelerate wound healing in diabetic mice. Mol Ther. 2014;22:1593–604. https://doi.org/10.1038/MT.2014.102.
Brown RL, Breeden MP, Greenhalgh DG. PDGF and TGF-alpha act synergistically to improve wound healing in the genetically diabetic mouse. J Surg Res. 1994;56:562–70. https://doi.org/10.1006/JSRE.1994.1090.
Reynolds K, Goldberg RB. Thiazolidinediones: beyond glycemic control. Treat Endocrinol. 2006;5:25–36. https://doi.org/10.2165/00024677-200605010-00004.
Hughes K, Aw TC, Kuperan P, Choo M. Central obesity, insulin resistance, syndrome X, lipoprotein(a), and cardiovascular risk in Indians, Malays, and Chinese in Singapore. J Epidemiol Community Health. 1997;51:394–9. https://doi.org/10.1136/JECH.51.4.394.
McFarlane SI, Kumar A, Sowers JR. Mechanisms by which angiotensin-converting enzyme inhibitors prevent diabetes and cardiovascular disease. Am J Cardiol. 2003;91:30–7. https://doi.org/10.1016/S0002-9149(03)00432-6.
Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med. 1998;339:1349–57. https://doi.org/10.1056/NEJM199811053391902.
Sacks FM, Pfeffer MA, Moye LA, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels cholesterol and recurrent events trial investigators. N Engl J Med. 1996;335:1001–9. https://doi.org/10.1056/NEJM199610033351401.
Pyörälä K, Pedersen TR, Kjekshus J, Faergeman O, Olsson AG, Thorgeirsson G. Cholesterol lowering with simvastatin improves prognosis of diabetic patients with coronary heart disease. A subgroup analysis of the Scandinavian simvastatin survival study (4S). Diabetes Care. 1997;20:614–20. https://doi.org/10.2337/DIACARE.20.4.614.
Steiner G, Hamsten A, Hosking J, et al. Effect of fenofibrate on progression of coronary-artery disease in type 2 diabetes: the diabetes atherosclerosis intervention study, a randomised study. Lancet. 2001;357:905–10. https://doi.org/10.1016/S0140-6736(00)04209-4.
Elkeles RS, Diamond JR, Poulter C, et al. Cardiovascular outcomes in type 2 diabetes: a double-blind placebo-controlled study of bezafibrate: the St Mary’s, Ealing, Northwick Park Diabetes Cardiovascular Disease Prevention (SENDCAP) study. Diabetes Care. 1998;21:641–8. https://doi.org/10.2337/DIACARE.21.4.641.
Forzano I, Wilson S, Lombardi A, et al. SGLT2 inhibitors: an evidence-based update on cardiovascular implications. Expert Opin Investig Drugs. 2023;32:839–47. https://doi.org/10.1080/13543784.2023.2263354.
Fitchett D, Inzucchi SE, Cannon CP, et al. Empagliflozin reduced mortality and hospitalization for heart failure across the spectrum of cardiovascular risk in the EMPA-REG OUTCOME trial. Circulation. 2019;139:1384–95. https://doi.org/10.1161/CIRCULATIONAHA.118.037778.
Giugliano D, Longo M, Signoriello S, et al. The effect of DPP-4 inhibitors, GLP-1 receptor agonists and SGLT-2 inhibitors on cardiorenal outcomes: a network meta-analysis of 23 CVOTs. Cardiovasc Diabetol. 2022. https://doi.org/10.1186/S12933-022-01474-Z.
Demuth HU, McIntosh CHS, Pederson RA. Type 2 diabetes—therapy with dipeptidyl peptidase IV inhibitors. Biochim Biophys Acta. 2005;1751:33–44. https://doi.org/10.1016/J.BBAPAP.2005.05.010.
Craddy P, Palin HJ, Johnson KI. Comparative effectiveness of dipeptidylpeptidase-4 inhibitors in type 2 diabetes: a systematic review and mixed treatment comparison. Diabetes Ther. 2014;5:1–41. https://doi.org/10.1007/S13300-014-0061-3.
Dou J, Ma J, Liu J, Wang C, et al. Efficacy and safety of saxagliptin in combination with metformin as initial therapy in chinese patients with type 2 diabetes: results from the START study, a multicentre, randomized, double-blind, active-controlled, phase 3 trial. Diabetes Obes Metab. 2018;20:590–8. https://doi.org/10.1111/DOM.13117.
Behary P, Tharakan G, Alexiadou K, et al. Combined GLP-1, oxyntomodulin, and peptide YY improves body weight and glycemia in obesity and prediabetes/type 2 diabetes: a randomized, single-blinded. Placebo-Controlled Study Diabetes Care. 2019;42:1446–53. https://doi.org/10.2337/DC19-0449.
Yeh TL, Tsai MC, Tsai WH, Tu YK, Chien KL. Effect of glucagon-like peptide-1 receptor agonists on glycemic control, and weight reduction in adults: a multivariate meta-analysis. PLoS ONE. 2023. https://doi.org/10.1371/JOURNAL.PONE.0278685.
Müller TD, Finan B, Bloom SR, et al. Glucagon-like peptide 1 (GLP-1). Mol Metab. 2019;30:72–130. https://doi.org/10.1016/J.MOLMET.2019.09.010.
Nauck MA, Meier JJ. Are all GLP-1 agonists equal in the treatment of type 2 diabetes? Eur J Endocrinol. 2019;181:R211–34. https://doi.org/10.1530/EJE-19-0566.
Funding
This work and the journal’s Rapid Service Fee were supported by the National Natural Science Foundation of China (82374404), the Major Science and Technology Project of Sichuan Province (No. 2022ZDZX0022), the Innovation Team and Talents Cultivation Program of National Administration of Traditional Chinese Medicine (No. ZYYCXTD-C-202209) and the Talent Support Project of the National Administration of Traditional Chinese Medicine: Qihuang Scholar (National Chinese Medicine Letter 2022 No.6).
Author information
Authors and Affiliations
Contributions
Chunguang Xie conceived the idea and outlined the sketch. Jiacheng Yin wrote the initial manuscript. Xiaoxu Fu and Yuling Leng assisted in the literature collection and figures. Lianjun Ao, Yue Luo, and Chunguang Xie revised the final draft and made the corrections. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
Jiacheng Yin, Xiaoxu Fu, Yue Luo, Yuling Leng, Lianjun Ao and Chunguang Xie declare no conflict of interest.
Ethical Approval
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Yin, J., Fu, X., Luo, Y. et al. A Narrative Review of Diabetic Macroangiopathy: From Molecular Mechanism to Therapeutic Approaches. Diabetes Ther 15, 585–609 (2024). https://doi.org/10.1007/s13300-024-01532-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-024-01532-7