Abstract
Accumulating evidences demonstrate that a population of suppressive cells known as myeloid-derived suppressor cells (MDSCs) is key immune modulators which suppress antitumor immunity. In this study, we found that the level of circulating CD14+HLA-DR−/low cells in patients was significantly higher than that of healthy donors and was correlated with tumor burden, lymph node metastasis, and tumor, node, and metastasis (TNM) clinical stage. More importantly, we for the first time find the level of CD14+HLA-DR−/low is a biological indicator of poor prognosis through the analysis of 3-year overall survival. Furthermore, we evidenced that the proportion of CD14+HLA-DR−/low cells in the tumor metastatic tumor-draining lymph nodes (TDLNs) was notably higher compared to tumor-free TDLNs. Additionally, CD14+HLA-DR−/low cells from esophageal squamous cell carcinoma (ESCC) patients expressed dramatically increased programmed death ligand 1 (PD-L1) comparing to that from healthy control. Subsequently, blocking PD-L1 pathway by antibody could effectively reverse the suppressive effect on autologous T cell proliferation mediated by CD14+HLA-DR−/low cells in vitro. In conclusion, our data revealed CD14+HLA-DR−/low MDSCs which increase in ESCC patients is a novel poor prognostic indicator and may exert immunosuppressive properties through PD-L1/PD-1 pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with malignancy are known to be immunologically depressed. Tumor cells actively induce the anergy and exhaustion of effector T cells and promote the expansion of negative regulatory immunocytes, which downregulate antitumor immunity [1–3]. Myeloid-derived suppressor cells (MDSCs) represent a heterogeneous population of the myeloid cell lineage which comprised myeloid progenitor cells and immature myeloid cells (IMCs). Normally, IMCs generated in the bone marrow quickly differentiate into mature granulocytes and macrophages or dendritic cells (DCs). In pathological conditions such as cancer [4–6], infectious diseases [7, 8], stress [9], chemotherapy [10], or some autoimmunity [11, 12], a partial blockage in the differentiation of IMCs into mature myeloid cells results in an expansion of the MDSC population.
In mice, MDSCs are defined based on the expression of Gr1 and CD11b. Granulocytic MDSCs have a CD11b+Ly6G+Ly6Clow phenotype, and monocytic MDSCs are CD11b+Ly6G−Ly6Chigh [13, 14]. In humans, MDSCs are generally agreed to be CD14−CD11b+ cells, or more precisely, cells that express the common myeloid marker CD33 but lack the expression of the markers of mature myeloid and lymphoid cells as well as the MHC class II molecule HLA-DR [4, 15]. In renal cancer patients, a CD11b−CD15+CD14− population was shown to have characteristics of MDSCs [16]. In several recent studies, a new subset of CD14+HLA-DR−/low cells was identified in the peripheral blood or tumor tissue from patients with melanoma [17, 18], hepatocellular carcinoma [19], ovarian carcinoma [20], prostate cancer [21], and carcinoma of the head and neck [22], supporting the concept of MDSC heterogeneity and plasticity. This heterogeneity suggests that there may be no specific markers that precisely define MDSCs and that suppressive activity is the ultimate defining characteristic [23]. Therefore, different types and different stages of human tumors might induce different subtypes of MDSCs [17, 19]. As a newly identified MDSC population, CD14+HLA-DR−/low cells has been the focus of attention for their suppressive activity in antitumor immunity and clinical relevance.
Esophageal carcinoma constitutes the sixth cause of cancer-related deaths worldwide [24]. Despite the ongoing research and clinical intervention in esophageal squamous cell carcinoma (ESCC), the long-term survival of patients remains poor. Surgical treatment alone for locally advanced disease results in a 5-year survival rate of only 20–25 %. Although the addition of combined modality strategies of preoperative or postoperative chemoradiotherapy was reported to improve the 5-year survival rates by 10–15 % [25, 26], the therapeutic toxicity remains to be a big problem. Therefore, development of new therapy modalities for ESCC is in dire need. Further understanding of the mechanism of suppressive activity mediated by negative regulatory immunocytes such as MDSCs might provide a new approach to the development of new immune therapies for ESCC.
In this study, we intend to detect the levels of CD14+HLA-DR−/low cells in ESCC patients and analyze its clinical significance.
Material and methods
Ethics statement
This study was approved by the ethics committee of the First Affiliated Hospital of Soochow University (Suzhou, China) for clinical investigation, and written informed consent was obtained from patients or their relatives before enrollment.
Patients and specimens
Peripheral blood was obtained from 78 patients with pathologically and clinically confirmed ESCC from June 2010 to December 2010. The patients had never been diagnosed as malignancy before and had not received antitumor drugs, radiotherapy, or surgery before blood was drawn. All the patients had undergone surgical treatment as initial therapy, with 76 cases that received esophagectomy, and two cases with unresectable tumor that received exploratory thoracotomy and gastrostomy. Each patient was classified on the basis of the tumor, node, and metastasis (TNM) classifications of malignant tumors by the International Union Against Cancer (UICC) after operation. Patient characteristics are summarized in Table 1. Blood samples from 12 randomly selected patients who had accepted esophagectomy were resurveyed 30 days after surgery and before postoperative chemotherapy or radiotherapy. Survival status and postoperative data were gained from telephone contacts and hospital records, respectively. The survival time was measured as the interval between date of surgical treatment and date of death for any cause. Thirty-five age- and gender-matched healthy volunteers (62.63 ± 9.38 years; female/male = 8/27) were recruited as a control group. We defined as healthy donors those who had never received any diagnosis of malignancy and showed no abnormalities in complete blood cell counts, C-reactive proteins, erythrocyte sedimentation rate, liver function tests, or chest X-rays in a medical checkup.
Flow cytometry analysis
Peripheral blood samples were stained with fluorochrome-conjugated mAbs and then analyzed by multicolor flow cytometry (FC500, Beckman Coulter, France). Isotype-matched antibodies were used as controls. The mAbs used in this study are listed as follows: fluorescein isothiocyanate HLA-DR-ECD, CD14-PE, CD11b-FITC, CD33-PC5 CD80-PE, CD86-PE, PD-L1-PE, B7-H3-PE (BioLegend, USA), and B7-H4-PE (Santa Cruz Biotechnology, USA). Respective immunoglobulin G (IgG) isotype-matched controls (BioLegend, USA) were used as negative controls. Data were analyzed with CXP software (Beckman Coulter).
Fresh tumor-draining lymph nodes (TDLNs) of ESCC patients were collected during esophagectomy (two nodes for one case, one node is nearby the tumor site and the other one is far from the tumor site). The nodes were cut apart along macroaxis. Specimens were gently minced and passed through a cell strainer to achieve a single-cell suspension. Then, the frequency of CD14+HLA-DR−/low cells was detected. According to the result of pathological examination, tumor metastatic lymph nodes and autologous tumor-free lymph nodes from eight patients were enrolled in this research.
The frequency of CD14+HLA-DR−/low cells (%) on total single cells from peripheral blood mononuclear cell (PBMC) or TDLN tissues = CD14 (%) × CD14+HLA-DR−/low (%).
Cell isolation and sorting
PBMCs were separated from fresh blood samples (50 mL) by Ficoll density gradient centrifugation. The CD3+ T cells were magnetically enriched by using the CD3-negative isolation kit (STEMCELL, Canada) from PBMC, and the purity >95 % is selected for the following study. The purified CD14+HLA-DR−/low and CD14+HLA-DRhigh cells were sorted by using the Beckman Coulter MoFloTM cell sorting system (Beckman Coulter, France), and the purity >90 % was chosen for the following experiment.
Carboxyfluorescein succinimidyl ester-based suppression assay
CD3+ T cells were labeled with carboxyfluorescein succinimidyl ester (CFSE) (Invitrogen, USA) according to the manufacturer’s instructions. The labeled T cells (1 × 105/well) were incubated with sorted CD14+HLA-DRlow/− cells (2.5 × 104/well) from the same patient in 96-well plates in the presence of CD3/CD28 mAbs immunobeads (Miltenyi Biotec, German). T cells alone were used as control. After 72 h, cells were harvested for flow analysis. For blocking experiments, we intervened programmed death ligand 1 (PD-L1) by using a blocking antibody (1 μg/mL, eBioscience, USA, clone MIH1) in the co-culture of CD14+HLA-DR−/low cells and autologous T cells.
Statistical analysis
The data is reported as mean ± SD. Flow cytometry data between different groups were compared by two-sample t test (Mann-Whitney test). Paired t test was used to compare the frequency of circulating CD14+HLA-DR−/low cells pre- and post-operation. Levels of CD14+HLA-DR−/low cells in tumor metastatic and tumor-free TDLNs were also compared by paired t test. One-way analysis of variance was used to test of differences between more than two groups. Fisher’s exact test was performed to analyze the clinical significance of circulating CD14+HLA-DR−/low cells. Kaplan-Meier survival curves were created for descriptive purposes and compared by log-rank test. All analyses were carried out by using the GraphPad Prism 5.0 software (version 5.01). *p values <0.05 and **p values <0.01 were considered to be statistically significant.
Results
The CD14+HLA-DR−/low cells in the peripheral blood were significantly increased in patients with ESCC
We firstly examined the levels of two subpopulations of MDSCs marked as CD14+HLA-DR−/low cells and CD11b+CD33+CD14−HLA-DR−/low cells presented in the peripheral blood of patients with ESCC and healthy donors. The percentage of circulating CD14+HLA-DR−/low cells in ESCC patients was significantly higher than that of healthy donors (1.85 ± 1.59 vs 0.611 ± 0.58 %, p < 0.001; as shown in Fig. 1a, b). However, CD11b+CD33+CD14−HLA-DR−/low cells were not different between patients and healthy donors (data not shown). Our data indicated that CD14+HLA-DR−/low cells but not CD11b+CD33+CD14−HLA-DR−/low cells significantly increase in patients with ESCC. Additionally, we found the frequency of circulating CD14+HLA-DR−/low cells significantly decreased with the removal of tumor mass (1.81 ± 0.89 vs 1.01 ± 0.42 %, p = 0.0135, as shown in Fig. 1c). Maybe, our data indicated that tumor burden induced the accumulation of circulating CD14+HLA-DR−/low cells in patient with ESCC.
The frequency of circulating CD14+HLA-DR−/low cells in PBMC from healthy control and ESCC patients. a Flow cytometry analysis of circulating CD14+HLA-DR−/low cells in ESCC patients and healthy donors. Representative data from one ESCC patient and one healthy donor. For the CD14+HLA-DR−/low cells, PBMCs were stained with HLA-DR-ECD and CD14-PE mAb. Flow cytometry analysis was performed with gates set on PBMC, and the results were presented as a percentage of CD14+HLA-DR−/low cells in PBMC. b Summary of frequency of circulating CD14+HLA-DR−/low cells in PBMC obtained from ESCC patients (n = 78) and healthy donors (n = 35). Lines indicate mean values. c Comparison of levels of CD14+HLA-DR−/low in PBMC from ESCC patients before and after operation. Student t test (paired test) was performed, and each dot represents one case (n = 12)
The frequency of circulating CD14+HLA-DR−/low cells was correlated with tumor burden, lymph node metastasis, and tumor stage
Next, we assessed whether the level of circulating CD14+HLA-DR−/low cells was associated with tumor progression. Through clinical data analysis, we found that the increase in circulating CD14+HLA-DR−/low cells was correlated with lymph node metastasis (p = 0.0093) and later clinical stage (p = 0.0486), but not with other characteristics, such as age, gender, and pathological differentiation (as shown in Table 2). These results suggested that circulating CD14+HLA-DR−/low cells might be involved in tumor metastasis and progression.
CD14+HLA-DR−/low cells accumulated in the tumor metastatic lymph node
Since CD14+HLA-DR−/low cells were correlated with lymph node metastasis, we analyzed the frequency of CD14+HLA-DR−/low cells in the tumor metastatic TDLNs and tumor-free TDLNs of the same patient with ESCC. We found a significant increase in the percentage of CD14+HLA-DR−/low cells in the tumor metastatic lymph nodes compared with tumor-free nodes (0.81 ± 0.78 vs 0.20 ± 0.21 %, p = 0.0453, Fig. 2).
CD14+HLA-DR−/low cells increased in the tumor metastatic TDLNs. a Flow cytometry analysis of CD14+HLA-DR−/low cells in the tumor-free lymph nodes and autologous tumor metastatic lymph nodes. Representative data from one tumor-free lymph node and one tumor metastatic lymph node. For the CD14+HLA-DR−/low cells, PBMCs were stained with HLA-DR-ECD and CD14-PE mAb. b Frequency of CD14+HLA-DR−/low cells in the tumor-free lymph nodes (n = 8) and autologous tumor metastatic lymph nodes (n = 8). Lines indicate mean values
CD14+HLA-DR−/low cells suppressed T cell proliferation depending upon PD-L1/PD-1 signal
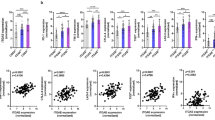
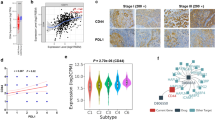
Co-stimulatory and co-inhibitory molecules, particularly B7 superfamily members, play an important role in regulating T cell responses. To evaluate the potential mechanism of CD14+HLA-DR−/low cells in suppressing T proliferation, we examined the surface expression of B7 family molecules on peripheral circulating CD14+HLA-DR−/low cells from patients with ESCC and healthy donors. Very interestingly, only co-inhibitory molecule PD-L1 was significantly highly expressed on CD14+HLA-DR−/low cells (Fig. 3a, b). Therefore, we estimated that CD14+HLA-DR−/low cells suppressed T cell proliferation depending on PD-L1. We blocked PD-L1 pathway using a special antibody against PD-L1 in the co-culture of CD14+HLA-DR−/low cells and autologous T cells. We found that T cell proliferative suppression was effectively reversed by blocking PD-L1 pathway (Fig. 3c).
CD14+HLA-DR−/low cells suppress autologous T cell proliferation depending on PD-L1. a The expression of co-stimulatory molecules CD80, CD86, PD-L1, B7-H3, and B7-H4 on CD14+HLA-DR−/low cells was examined by flow cytometry. Representative data from one ESCC patient and healthy donor. CD14+HLA-DR−/low cells were stained with CD80-PE, CD86-PE, PD-L1-PE, B7-H3-PE, and B7-H4-PE mAb. b The summary of expression of co-stimulatory molecules CD80, CD86, PD-L1, B7-H3, and B7-H4 on CD14+HLA-DR−/low cells from patients with ESCC (n = 15) and healthy donors (n = 10). c Proliferation of anti-CD3/anti-CD28-stimulated autologous T cells co-cultured with CD14+HLA-DR−/low cells in the presence of PD-L1 mAb or IgG was measured by dilution of CFSE staining intensity using flow cytometry. Summary data was list (n = 3). One-way ANOVA was performed and data are presented as means ± SEM. **p < 0.05; *p < 0.01; ns represents p > 0.05
The high level of circulating CD14+HLA-DR−/low cells serves as a poor prognostic marker in patients with ESCC
The patients were followed up for 3 years until December 2013; four cases were lost to follow-up, and the 3-year overall survival rate was 56.41 %. Two cases died within 30 days after surgery (20 and 21 days, respectively) and were excluded in this survival analysis. ROC analysis indicated that an optimal cutoff point for the frequency of circulating CD14+HLA-DR−/low cells in predicting the 3-year overall survival is 2.38 %. Based on this cutoff value, the patients were divided into two groups, with 54 cases (71 %) in CD14+HLA-DR−/low cells high level group and 22 cases (29 %) in CD14+HLA-DR−/low low level group. Kaplan-Meier survival curves showed that patients of the high level group had a significantly poorer outcome comparing to the low level group (log-rank test, p = 0.0017) (Fig. 4).
High level of circulating CD14+HLA-DR−/low cells serves as a poor prognostic marker for the survival of patients with ESCC. Kaplan-Meier survival curves for ESCC patients who have received surgical treatment. Kaplan-Meier survival curves showed that patients of CD14+HLA-DR−/low cells high level group (n = 22) had a significantly poorer outcome comparing to CD14+HLA-DR−/low cells low level group (n = 54)
Discussion
Accumulating evidences demonstrate that MDSCs are key immune modulators which suppress lymphocyte responses in tumor-bearing animals and cancer patients. MDSCs were firstly described in patients with cancer as natural suppressor cells in 1980s [27–29]. Subsequently, this immature, myeloid-derived, and suppressive population was detected in tumor-bearing mice and was named as immature myeloid cells (IMCs) or myeloid suppressor cells (MSCs). In 2007, these cells were suggested to be named as myeloid-derived suppressor cells (MDSCs) for its myeloid origin and biological function [30]. The characteristics and biological functions of MDSCs have always been in the center of concerns.
It has been proved that MDSCs represent a heterogeneous population of immunosuppressive cells. In the past several years, a new subset of CD14+ HLA-DR−/low cells was identified in the peripheral blood or tumor tissue from a variety of malignancy patients. In 2006, one group described a population of CD14+CD16+HLA-DR− cells increased in ascites of patients with epithelial ovarian cancer [20]. In 2007, Filipazzi and colleagues identified a subset of CD14+HLA-DR−/low myeloid suppressor cells in peripheral blood of melanoma patients with modulation by a granulocyte-macrophage colony-stimulation factor-based antitumor vaccine [17]. In 2008, Hoechst and colleagues observed CD14+HLA-DR−/low cells in the blood and tumor of hepatocellular carcinoma patients [19]. Furthermore, they proposed that this new type of MDSCs exerted their immunosuppressive function through the induction of regulatory T cells (Tregs) in co-cultured CD4+ T cells [19]. Soon, several studies identified the CD14+ HLA-DR−/low cells in the peripheral blood or tumor from patients with ovarian carcinoma [20], prostate cancer [21], and carcinoma of the head and neck [22], respectively.
In this paper, we also observed a significant increase of CD14+HLA-DR−/low cells rather than CD11b+CD33+CD14−HLA-DR−/low cells in the peripheral blood of patients with ESCC compared with healthy donors. Additionally, the levels of circulating CD14+HLA-DR−/low cells were notably correlated with lymph node metastasis, TNM clinical stage, and 3-year overall survival. Furthermore, in the case-to-case analysis, the levels of circulating CD14+HLA-DR−/low cells decreased with the removal of tumor mass by surgical treatment, which indicated that tumor burden induced the accumulation of circulating CD14+HLA-DR−/low cells in patient with ESCC. Our data suggested that CD14+HLA-DR−/low cells really represent an important immunosuppressive component involved in the tumor immune escape of ESCC, and the frequency of circulating CD14+HLA-DR−/low cells might provide a novel prognostic indicator of ESCC.
In fact, the survival analysis of prognostic factors indicated that the differentiation, T factor, N factor, and circulating CD14+HLA-DR−/low MDSC levels significantly correlated with prognosis of patients with ESCC (p < 0.05, respectively, data not shown). However, if differentiation, T factor, N factor, and circulating CD14+HLA-DR−/low MDSC levels were selected to analyze in a Cox model; Cox multivariate regression analysis indicated only the T factor is an independent risk factor for death (data not shown). That is to say, circulating CD14+HLA-DR−/low MDSC levels is not an independent prognostic indicator for patients with ESCC.
MDSCs also play an important role in tumor metastatic spread. CD11b+/Ly6Cmed/Ly6G+ cells were identified as key constituents of the premetastatic niche in mammary and melanoma experimental metastasis models [31]. In highly metastatic murine mammary tumors, Gr-1+/CD11b+ MDSCs selectively express proteins involved in the c-glutamyl transferase, glutathione synthase pathways, and other pathways involved in platelet aggregation, as well as lipid and amino acid metabolism [32]. Compromised recruitment of MDSCs inhibits tumor growth and pulmonary metastasis of breast cancer mouse model [33]. We found a higher percentage of CD14+HLA-DR−/low cells in the tumor metastatic TDLNs compared with the corresponding tumor-free ones. It indicated that CD14+HLA-DR−/low cells might contribute to the lymph node metastasis of ESCC.
The mechanisms of immune suppression by MDSCs include nutrient starvation [34] and induction of Tregs [35]. Several key molecules, such as arginase 1 (ARG-1), inducible nitric oxide synthase (iNOS), and transforming growth factor β (TGF-β) [36], as well as some other immunosuppressive cytokines [37, 38] mediate these suppressive modalities. It is reported recently that monocytic MDSCs are the main source of key immunosuppressive factors such as ARG-1, reactive oxygen species (ROS), and TGF-β1 in neuroblastoma tumor-bearing mice [39]. In addition to their suppressive effects on adaptive immune responses, MDSCs have also been reported to regulate innate immune responses by modulating the cytokine production of macrophages [40]. However, the immune suppression mechanisms of CD14+HLA-DR−/low cells remain controversial. For instance, CD14+HLA-DR−/low cells in hepatocellular carcinoma patients had high arginase activity, but they did not secrete TGF-β [19], while in melanoma patients, suppressive activity of CD14+HLA-DR−/low cells was reported to be mediated by TGF-β rather than arginase [17]. MDSCs are driven by tumor burden and by the diversity of factors produced by the tumor and by host cells in the tumor microenvironment. Thus, the biological functions and phenotype of MDSCs driven by the tumor microenvironment of multiple types of tumors and different stages of the diseases might be various.
It is now clear that MDSCs, though heterogeneous, particularly contribute to the establishment of tumor antigen-specific tolerance and immune escape. To achieve effective antitumor immunity, tumor-induced immunosuppression must be reversed. In mouse models, MDSC depletion or the blockage of their suppressive pathways delays tumor development and growth [41]. The inhibition of certain signaling pathway such as paired immunoglobulin-like receptors B (PIR-B) promoted MDSCs and differentiated and retarded tumor growth of tumor-bearing mice [42]. In humans, several approaches, such as the use of chemotherapeutic agents and induction of the differentiation of MDSCs, have been described for the deletion of MDSCs [5, 43].
To investigate the effect of CD14+HLA-DR−/low cells on T responses, we firstly examined the suppressive activity of CD14+HLA-DR−/low cells. As expected, CD14+HLA-DR−/low cells were able to suppress effectively both the proliferation of T cells in the presence of anti-CD3/anti-CD28 mAb. These results suggest that CD14+HLA-DR−/low cells in ESCC patients contribute to the immune suppressive status. To further investigate the mechanism of this immune suppression, we examined the expression of co-stimulatory molecules which play important role in the regulation of T cell responses. Our data indicated that CD14+HLA-DR−/low cells from patients with ESCC express a higher level of PD-L1 compared with those from healthy donors, whereas other co-stimulatory molecules such as CD80, CD86, B7-H3, and B7-H4 were not found to be significantly different. Similarly, PD-L1 highly expressed CD14+HLA-DR−/low cells were also detected in squamous cell carcinoma of the head and neck [22].
As an important co-inhibitor molecule, programmed death ligand 1 (PD-L1), is able to suppress T cell response effectively. Recently, in clinical trials, antibodies against PD-1 and PD-L1 were used to block PD-1/PD-L1 pathway for the treatment of advanced cancers (including non-small cell lung cancer, melanoma, and renal cell cancer) and yielded encouraging results [44, 45]. It suggests that PD1/PD-L1 pathway, as an important immune checkpoint, is of major importance in tumor immune resistance. Blockage of PD1/PD-L1 pathway may be a novel immunotherapy for cancer. To confirm whether PD-L1 contributed to CD14+HLA-DR−/low cell-mediated suppressive activity, we examined the effect of PD-L1 by using a blocking antibody against PD-L1 in the suppressing experiment. As expected, we found blocking PD-L1 could effectively reverse the suppressive activity of CD14+HLA-DR−/low cells. Thus, the preferential expression of PD-L1 could contribute to immunosuppressive properties of CD14+HLA-DR−/low cells in ESCC patients.
To sum up, our data suggest that in patients with ESCC, CD14+HLA-DR−/low cells act as potent immunosuppressive cells, particularly contributing to the tumor immune escape from the host immune system. Furthermore, the frequency of circulating CD14+HLA-DR−/low cells might provide a novel but not independent prognostic indicator of ESCC. Additionally, PD1/PD-L1 pathway may be an immune checkpoint of tumor immune resistance mediated by CD14+HLA-DR−/low cells.
Abbreviations
- MDSCs:
-
Myeloid-derived suppressor cells
- ESCC:
-
Esophageal squamous cell carcinoma
- PD-L1:
-
Programmed death ligand 1
- TDLNs:
-
Tumor-draining lymph nodes
- PBMCs:
-
Peripheral blood mononuclear cells
- ARG-1:
-
Arginase-1
- ROS:
-
Reactive oxygen species
- iNOS:
-
Inducible nitric oxide synthase
- TGF-β:
-
Transforming growth factor β
- Tregs:
-
Regulatory T cells
- PIR-B:
-
Paired immunoglobulin-like receptors B
- CFSE:
-
Carboxyfluorescein succinimidyl ester
References
Poschke I, Mougiakakos D, Kiessling R. Camouflage and sabotage: tumor escape from the immune system. Cancer Immunol Immunother. 2011;60:1161–71.
Talmadge JE. Immune cell infiltration of primary and metastatic lesions: mechanisms and clinical impact. Semin Cancer Biol. 2011;21:131–8.
Whiteside TL. Immune responses to malignancies. J Allergy Clin Immunol. 2010;125:S272–283.
Almand B, Clark JI, Nikitina E, van Beynen J, English NR, Knight SC, et al. Increased production of immature myeloid cells in cancer patients: a mechanism of immunosuppression in cancer. J Immunol. 2001;166:678–89.
Diaz-Montero CM, Salem ML, Nishimura MI, Garrett-Mayer E, Cole DJ, Montero AJ. Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol Immunother. 2009;58:49–59.
Sica A, Bronte V. Altered macrophage differentiation and immune dysfunction in tumor development. J Clin Invest. 2007;117:1155–66.
Haile LA, von Wasielewski R, Gamrekelashvili J, Kruger C, Bachmann O, Westendorf AM, et al. Myeloid-derived suppressor cells in inflammatory bowel disease: a new immunoregulatory pathway. Gastroenterology. 2008;135:871–81.
Brys L, Beschin A, Raes G, Ghassabeh GH, Noel W, Brandt J, et al. Reactive oxygen species and 12/15-lipoxygenase contribute to the antiproliferative capacity of alternatively activated myeloid cells elicited during helminth infection. J Immunol. 2005;174:6095–104.
Makarenkova VP, Bansal V, Matta BM, Perez LA, Ochoa JB. CD11b+/Gr-1+ myeloid suppressor cells cause T cell dysfunction after traumatic stress. J Immunol. 2006;176:2085–94.
Angulo I, de las Heras FG, Garcia-Bustos JF, Gargallo D, Munoz-Fernandez MA, Fresno M. Nitricoxide-producing CD11b+Ly-6G(Gr-1)+CD31(ER-MP12)+ cells in the spleen of cyclophosphamide-treated mice: implications for T-cell responses in immunosuppressed mice. Blood. 2000;95:212–20.
Zhu B, Bando Y, Xiao S, Yang K, Anderson AC, Kuchroo VK, et al. CD11b+Ly-6Chi suppressive monocytes in experimental auto-immune encephalomyelitis. J Immunol. 2007;179:5228–37.
Kerr EC, Raveney BJ, Copland DA, Dick AD, Nicholson LB. Analysis of retinal cellular infiltrate in experimental autoimmune uveoretinitis reveals multiple regulatory cell populations. J Autoimmun. 2008;31:354–61.
Youn JI, Nagaraj S, Collazo M, Gabrilovich DI. Subsets of myeloid-derived suppressor cells in tumor-bearing mice. J Immunol. 2008;181:5791–802.
Hestdal K, Ruscetti FW, Ihle JN, Jacobsen SE, Dubois CM, Kopp WC, et al. Characterization and regulation of RB6-8C5 antigen expression on murine bone marrow cells. J Immunol. 1991;147:22–8.
Ochoa AC, Zea AH, Hernandez C, Rodriguez PC. Arginase, prostaglandins, and myeloid-derived suppressor cells in renal cell carcinoma. Clin Cancer Res. 2007;13:721s–6s.
Zea AH, Rodriguez PC, Atkins MB, Hernandez C, Signoretti S, Zabaleta J, et al. Arginase-producing myeloid suppressor cells in renal cell carcinoma patients: a mechanism of tumor evasion. Cancer Res. 2005;65:3044–8.
Filipazzi P, Valenti R, Huber V, Pilla L, Canese P, Iero M, et al. Identification of a new subset of myeloid suppressor cells in peripheral blood of melanoma patients with modulation by a granulocyte-macrophage colony-stimulation factor-based antitumor vaccine. J Clin Oncol. 2007;25:2546–53.
Poschke I, Mougiakakos D, Hansson J, Masucci GV, Kiessling R. Immature immunosuppressive CD14+HLA-DR-/low cells in melanoma patients are Stat3hi and overexpress CD80, CD83, and DC-sign. Cancer Res. 2010;70:4335–45.
Hoechst B, Ormandy LA, Ballmaier M, Lehner F, Krüger C, Manns MP, et al. A new population of myeloid-derived suppressor cells in hepatocellular carcinoma patients induces CD4+CD25+Foxp3+ T cells. Gastroenterology. 2008;135:234–43.
Gordon IO, Freedman RS. Defective antitumor function of monocyte-derived macrophages from epithelial ovarian cancer patients. Clin Cancer Res. 2006;12:1515–24.
Vuk-Pavlović S, Bulur PA, Lin Y, Qin R, Szumlanski CL, Zhao X, et al. Immunosuppressive CD14+HLA-DRlow/- monocytes in prostate cancer. Prostate. 2010;70:443–55.
Chikamatsu K, Sakakura K, Toyoda M, Takahashi K, Yamamoto T, Masuyama K. Immunosuppressive activity of CD14+HLA-DR- cells in squamous cell carcinoma of the head and neck. Cancer Sci. 2012;103:976–83.
Ostrand-Rosenberg S, Sinha P. Myeloid-derived suppressor cells: linking inflammation and cancer. J Immunol. 2009;182(8):4499–506.
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90.
Cunningham D, Allum WH, Stenning SP, Thompson JN, Van de Velde CJ, Nicolson M, et al. Perioperative chemotherapy versus surgery alone for resectable gastroesophageal cancer. N Engl J Med. 2006;355:11–20.
Tepper J, Krasna MJ, Niedzwiecki D, Hollis D, Reed CE, Goldberg R, et al. Phase III trial of trimodality therapy with cisplatin, fluorouracil, radiotherapy, and surgery compared with surgery alone for esophageal cancer: CALGB 9781. J Clin Oncol. 2008;26:1086–92.
Young MR, Newby M, Wepsic TH. Hematopoiesis and suppressor bone marrow cells in mice bearing large metastatic Lewis lung carcinoma tumors. Cancer Res. 1987;47:100–5.
Buessow SC, Paul RD, Lopez DM. Influence of mammary tumor progression on phenotype and function of spleen and in situ lymphocytes in mice. J Natl Cancer Inst. 1984;73:249–55.
Strober S. Natural suppressor (NS) cells, neonatal tolerance, and total lymphoid irradiation: exploring obscure relationships. Annu Rev Immunol. 1984;2:219–37.
Gabrilovich DI, Bronte V, Chen SH, Colombo MP, Ochoa A, Ostrand-Rosenberg S, et al. The terminology issue for myeloid-derived suppressor cells. Cancer Res. 2007;67:425–6.
Sceneay J, Chow MT, Chen A, Halse HM, Wong CS, Andrews DM, et al. Primary tumor hypoxia recruits CD11b+/Ly6Cmed/Ly6G+ immune suppressor cells and compromises NK cell cytotoxicity in the premetastatic niche. Cancer Res. 2012;72:3906–11.
Boutte AM, McDonald WH, Shyr Y, Yang L, Lin PC. Characterization of the MDSC proteome associated with metastatic murine mammary tumors using label-free mass spectrometry and shotgun proteomics. PLoS ONE. 2011;6:e22446.
Yu F, Shi Y, Wang J, Li J, Fan D, Ai W. Deficiency of Kruppel-like factor KLF4 in mammary tumor cells inhibits tumor growth and pulmonary metastasis and is accompanied by compromised recruitment of myeloid-derived suppressor cells. Int J Cancer. 2013;133:2872–83.
Rodriguez PC, Ochoa AC. Arginine regulation by myeloid derived suppressor cells and tolerance in cancer: mechanisms and therapeutic perspectives. Immunol Rev. 2008;222:180–91.
Serafini P, Mgebroff S, Noonan K, Borrello I. Myeloid-derived suppressor cells promote cross-tolerance in B-cell lymphoma by expanding regulatory T cells. Cancer Res. 2008;68:5439–49.
Gabrilovich DI, Nagaraj S. Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol. 2009;9:162–74.
Kusmartsev S, Gabrilovich DI. Role of immature myeloid cells in mechanisms of immune evasion in cancer. Cancer Immunol Immunother. 2006;55:237–45.
Ostrand-Rosenberg S. Myeloid-derived suppressor cells: more mechanisms for inhibiting antitumor immunity. Cancer Immunol Immunother. 2010;59:1593–600.
Bianchi G, Vuerich M, Pellegatti P, Marimpietri D, Emionite L, Marigo I, et al. ATP/P2X7 axis modulates myeloid-derived suppressor cell functions in neuroblastoma microenvironment. Cell Death Dis. 2014;5:e1135. doi:10.1038/cddis.2014.109.
Sinha P, Clements VK, Bunt SK, Albelda SM, Ostrand-Rosenberg S. Crosstalk between myeloid-derived suppressor cells and macrophages subverts tumor immunity toward a type 2 response. J Immunol. 2007;179:977–83.
Minu KS, Li Z, Harris-White M, Upendra K, Min H, Ming F, et al. Myeloid suppressor cell depletion augments antitumor activity in lung cancer. PLoS ONE. 2012;7:e40677.
Ma G, Pan PY, Eisenstein S, Divino CM, Lowell CA, Takai T, et al. Paired immunoglobin-like receptor-B regulates the suppressive function and fate of myeloid-derived suppressor cells. Immunity. 2011;34:385–95.
Vincent J, Mignot G, Chalmin F, Ladoire S, Bruchard M, Chevriaux A, et al. 5-Fluorouracil selectively kills tumor-associated myeloid-derived suppressor cells resulting in enhanced T cell-dependent antitumor immunity. Cancer Res. 2010;70:3052–61.
Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med. 2012;366:2443–54.
Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012;366:2455–65.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (Grants 31300746 to H.H., 81372276 to G.Z., 31320103918 to X.Z.), the Natural Science Foundation of Jiangsu (Grant BK20131158 to G.Z.), and by the Natural Science Foundation of Suzhou (Grant SYS201323 to H.H.).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding authors
Additional information
Haitao Huang and Guangbo Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Huang, H., Zhang, G., Li, G. et al. Circulating CD14+HLA-DR−/low myeloid-derived suppressor cell is an indicator of poor prognosis in patients with ESCC. Tumor Biol. 36, 7987–7996 (2015). https://doi.org/10.1007/s13277-015-3426-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-3426-y