Abstract
Background
Periodontitis, a common inflammatory disease in adults, causes the loss of alveolar bone, eventually leading to tooth loss. The inhibition of osteogenic differentiation of periodontal ligament stem cells (PDLSCs) might be involved in the development of alveolar bone loss.
Objective
The aim of the present study was to investigate the regulatory roles of nuclear factor erythroid-2-related factor 2 (Nrf2) during the osteogenic differentiation of PDLSCs in the presence of LPS.
Results
In the present study, LPS reduced cell viability, inhibited osteogenic differentiation, and caused oxidative stress in PDLSCs. Antioxidants, glutathione (GSH), N-acetyl-L-cysteine (NAC), and ascorbic acid (AA), had rescue effects. Furthermore, LPS reduced antioxidant capability and expression of Nrf2 and its down-stream antioxidant genes. Nrf2 over-expression abolished the cytotoxic effects of LPS by alleviating ROS level.
Conclusion
LPS induced oxidative stress through downregulating Nrf2-mediated antioxidant pathways, and inhibited osteogenic differentiation in PDLSCs. Strategies enhancing antioxidant capability could reverse the impaired osteogenic potential caused by LPS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Periodontitis is a type of gum disease caused by bacterial infection, and results in the destruction of the periodontal ligament, cementum, and alveolar bone (Kumar 2019). Lipopolysaccharide (LPS) from several Gram-negative bacteria is identified as the dominant stimulus. LPS disrupts the balance between formation and resorption of alveolar bone, induces inflammatory bone resorption in periodontitis, and eventually causes teeth to loosen or leads to tooth loss (Henderson and Kaiser, 2018). Prevention of alveolar bone loss is a challenge for periodontitis treatment.
Periodontal ligament stem cells (PDLSCs), located within the periodontal ligamental tissues, are multipotent stem cells, and can different into periodontal ligaments, cementum, alveolar bone, cartilage, neurons, adipocytes and blood vessels (Zhu and Liang 2015). Therefore, PDLSCs possess the potential of cementum regeneration, and periodontal tissue repair. It has been revealed that inflammatory microenvironment in the periodontium suppresses the differentiation potential of PDLSCs (Zheng et al. 2015). LPS directly inhibits osteogenic differentiation of PDLSCs (Kukolj et al. 2018, Wang et al. 2020). Although extensive research has been carried out, the underlying mechanisms involved in the osteogenic differentiation of PDLSCs under an inflammatory microenvironment have not been fully elucidated.
An imbalance between reactive oxygen species (ROS) production and antioxidant defense system leads to oxidative stress. Nuclear factor erythroid-2-related factor 2 (Nrf2) is a master transcription factor that maintains redox balance (Zhang et al. 2021). Under oxidative stress, Nrf2 translocates to the nucleus, and regulates antioxidant response element (ARE) dependent expression of antioxidant defense enzymes, including catalase (CAT), glutathione peroxidase 4 (GPX4), glutathione reductase (GSR), glutamate-cysteine ligase catalytic subunit (GCLC) etc. (Tonelli et al. 2018). Oxidative stress can be induced by LPS exposure in various cell types, including kidney tubular cells (Feng et al. 2020), macrophages (Li et al. 2010, Tanaka et al. 2018), neuronal cells (Shah et al. 2017), epithelial cells (Shi et al. 2019), and lung cells (Dong and Yuan 2018). It has been revealed that Nrf2 activation protects against oxidative stress-induced cytotoxic effects in PDLSCs (Liu et al. 2017; Jia et al. 2020). LPS inhibits osteogenic differentiation and induces oxidative stress in PDLSCs (Zhao et al. 2020). Whether increased ROS level induced by LPS was associated with Nrf2 inhibition and inhibited osteogenic differentiation had not been investigated yet.
In order to reveal the underlying mechanisms of cytotoxic effects of LPS on PDLSCs, we investigated the influence of LPS on oxidative stress and the rescue effects of antioxidants, including glutathione (GSH), N-acetyl-L-cysteine (NAC), and ascorbic acid (AA). We also explored the regulatory roles of Nrf2 during the osteogenic differentiation of PDLSCs in the presence of LPS.
Results
LPS decreases cell viability and induces oxidative stress in PDLSCs
To assess the influence of LPS on cell viability of PDLSCs, the cells were treated with LPS at different concentrations (0–0.4 μg/mL). Our results demonstrated that LPS significantly inhibited cell viability in a dose-dependent manner on day 2 (Fig. 1A). The inhibitory effects of LPS at 0.1 μg/mL began on day 1 and reached the maximum on day 2 (Fig. 1B). Based on the above findings, LPS at a concentration of 0.1 μg/mL was used in subsequent experiments. We then investigated whether LPS could induce cell oxidative stress or not. Upon LPS treatment, the level of cellular ROS, MDA, superoxide, and H2O2 was markedly increased (Fig. 1C-F). These results suggest that LPS has strongly inhibitory effects on PDLSCs viability, and induces oxidative stress. The cytotoxic effects of LPS on PDLSCs may be associated with the elevated oxidative damage.
LPS decreases cell viability and induces oxidative stress in PDLSCs. A PDLSCs were treated with different concentrations of LPS from 0.05 to 0.4 μg/mL. Cell viability was detected on day 2. B PDLSCs were treated with 0.1 μg/mL LPS for 3 days. Cell viability was detected on day 1, 2, and 3. C-F Cellular ROS, MDA, superoxide, and H2O2 were detected on day 2. All the data were presented as the mean ± SD. *P<0.05, **P<0.01, ***P<0.001 vs. 0 μM or Ctrl. Ctrl control, LPS lipopolysaccharides
Antioxidants restore the cytotoxic effects induced by LPS
ROS-scavenging enzymes play a defensive role against oxidative stress. A significant reduction of their activities could induce cellular oxidative stress. In the presence of LPS, the activities of three main anti-oxidative enzymes including SOD, CAT, and GSH-Px were significantly decreased (Fig. 2A-C). When antioxidants NAC, AA and GSH were added, the inhibitory effects of cell viability induced by LPS were restored to the control level (Fig. 2D-F). The antioxidants alone did not negatively affect cell viability. These results indicate that the oxidative stress induced by LPS is associated with inhibitory activities of antioxidant enzymes.
LPS reduces the antioxidant capability of LPS-treated PDLSCs. PDLSCs were treated with 0.1 μg/mL LPS for 2 days. After that, the activities of cellular SOD (A), CAT (B), and GSH-Px (C) were detected. (D-F) Antioxidants, NAC, AA, or GSH, were added along with LPS. Cell viability was detected on day 2. All the data were presented as the mean ± SD. *P<0.05, **P<0.01, ***P<0.001. AA ascorbic acid, Ctrl control, LPS lipopolysaccharides, NAC acetylcysteine, GSH glutathione
Antioxidants restore the osteogenic differentiation of PDLSCs in the presence of LPS
Since antioxidants rescued the decreased viability of PDLSCs in the presence of LPS, we then investigated the rescue effects of antioxidants on osteogenic differentiation. Our results showed that LPS alone significantly decreased mineralization (Fig. 3A), ALP expression (Fig. 3B-D), and ALP activity (Fig. 3B-D) in PDLSCs. In contrast, antioxidants NAC or AA significantly stimulated mineralization (Fig. 3A), ALP expression (Fig. 3B-C), and ALP activity (Fig. 3B-C). Although GSH did not have such positive effects on mineralization, GSH promoted both expression and activity of ALP (Fig. 3D). When PDLSCs were treated with LPS along with the antioxidants, the osteogenic differentiation was rescued to the control level.
The rescue effects of antioxidants on osteogenic differentiation in the presence of LPS. PDLSCs were treated with LPS (0.1 μg/mL), antioxidants (5 mM NAC, 5 mM AA, or 3 mM GSH), or their combinations under osteogenic condition for 21 days. The formed mineralized nodules were stained by Alizarin Red S. The mineralization was evaluated by the area of mineralized nodules. ALP mRNA expression was detected on day 14. ALP activity was detected on day 14. A Representative images of mineralized nodules. B Effects of NAC and LPS on mineralization, ALP mRNA expression, and ALP activity. C Effects of AA and LPS on mineralization, ALP mRNA expression, and ALP activity. D Effects of GSH and LPS on mineralization, ALP mRNA expression, and ALP activity. All the data were presented as the mean ± SD. *P<0.05, **P<0.01, ***P<0.001. AA ascorbic acid, ALP alkaline phosphatase, Ctrl control, LPS lipopolysaccharides, NAC acetylcysteine, GSH glutathione
LPS suppresses Nrf2-mediated antioxidant pathways in PDLSCs
To further identify whether the cytotoxic effects of LPS on PDLSCs were dependent on Nrf2-ARE pathway, the mRNA and protein levels of Nrf2 and its down-stream antioxidant genes were detected. As was illustrated in Fig. 4A and B, the protein and mRNA levels of Nrf2 were markedly reduced in LPS-treated PDLSCs. Consistent with the alterations of Nrf2, LPS also significantly inhibited mRNA expression of Nrf2 down-stream antioxidant genes, including HO-1, NQO1, GCLC, and CAT (Fig. 4C-F). These results suggest that LPS suppresses Nrf2-mediated antioxidant pathways in PDLSCs.
LPS downregulates expression of Nrf2-mediated antioxidant genes. PDLSCs were treated with LPS 0.1 μg/mL for 2 days. A Nrf2 protein level was detected by immunoblot assay. B-F The mRNA levels of Nrf2 and several genes of the down-stream of Nrf2 were detected by Quantitative PCR method, including GPX4, GSR1, GCLC, and CAT. All the data were presented as the mean ± SD. *P<0.05, **P<0.01, ***P<0.001 vs. Ctrl. Ctrl control, LPS lipopolysaccharides
Nrf2 over-expression abolishes the cytotoxic effects of LPS
To further demonstrate the involvement of Nrf2 inhibition on the cytotoxic effects of LPS on PDLSCs, lentiviral method was used to upregulate Nrf2 expression. The efficient functional over-expression of Nrf2 was determined by immunoblot assay. Our results demonstrated that the protein level of Nrf2 was increased by about 60% after Nrf2-overexpressing lentiviral transduction (Fig. 5A). Nrf2 over-expression did not affect PDLSCs viability, but restored the inhibitory effects induced by LPS (Fig. 5B). Compared with the NC (negative control) cells, Nrf2-OE cells exhibited an increased capability of mineralization, and even rescued the inhibitory effects by LPS to the Nrf2-OE level (Fig. 5C). Nrf2 over-expression also restored the stimulatory production of ROS by LPS to the NC level (Fig. 5D). Our results showed that transfection of PDLSCs with the Nrf2-overexpressing lentiviral vector upregulated Nrf2 expression, and rescued the inhibitory effects of LPS on viability, mineralization, and ROS production in PDLSCs, suggesting that Nrf2 inhibition is essential for the cytotoxic effects of LPS on PDLSCs.
Nrf2 over-expression abolishes the inhibitory effects of LPS. A PDLSCs were infected with Nrf2-overexpressing lentivirus and the corresponding negative control lentivirus. The interference efficiency was detected by immunoblot assay. Cell viability (B) and ROS production (D) were detected on day 2. C The formation of mineralized nodules during osteogenic differentiation was detected on day 21. All the data were presented as the mean ± SD. *P<0.05, **P<0.01, ***P<0.001. LPS lipopolysaccharides, NC negative control, OE over-expression
Discussion
LPS is a key factor inducing oxidative stress and alveolar bone loss during periodontitis. PDLSCs, which reside in the perivascular space of the periodontium, possess the potential of alveolar bone regeneration (Sczepanik et al. 2020). In the present study, we demonstrated that LPS significantly reduced viability and osteogenic differentiation in PDLSCs. LPS also caused oxidative stress and decreased antioxidant capability. Antioxidants or Nrf2 over-expression rescued the cytotoxic effects of LPS. These results suggest that downregulation of Nrf2-mediated antioxidant pathway is involved in the cytotoxic effects of LPS on PDLSCs.
LPS from Gram-negative bacteria plays a pivotal role in the development of periodontitis. An experimental periodontitis model can be obtained by topical application of LPS into gingival sulcus (Yoshinaga et al. 2012). LPS has been demonstrated to disrupt the balance between bone formation and resorption, eventually leading to bone loss (Chen et al. 2020). The osteogenic differentiation potential is closed associated with PDLSCs-based cementum regeneration. It has been revealed that LPS has cytotoxic effects on PDLSCs. LPS reduces PDLSCs proliferation, inhibits osteogenic differentiation, and causes apoptosis (Duan et al. 2020; Keong et al. 2020; Wang et al. 2020). The cytotoxic effects are related with decreased antioxidant capability. Our results showed that LPS significantly reduced activities of antioxidant enzymes, including SOD, CAT, and GSH-Px. Antioxidants, NAC, AA, or GSH, had rescue effects. The decreased cell viability and osteogenic differentiation were restored to the control level.
PDLSCs with osteogenic differentiation potential can form new bone, and are regarded as the seed cells for alveolar bone formation. Inflammatory response impairs the osteogenic differentiation of PDLSCs, which may be involved in the destruction of alveolar bone. Some pathways have been identified to reveal the underlying mechanisms for the cytotoxic effects of LPS. LPS inhibits osteogenic differentiation of PDLSCs by upregulation of miR-148a and downregulation of neuropilin 1 (NRP1) (Bao et al. 2019). Extracellular signal-regulated protein kinases 1 and 2 (ERK1/2) activation and toll-like receptor 4-mediated ephrinB2 downregulation are involved in the inhibition of osteogenic differentiation by LPS (Kukolj et al. 2018; Wang et al. 2020). LncRNA-TUG1 is highly expressed in PDLSCs during osteogenic differentiation. LncRNA-TUG1 promotes osteogenic differentiation of PDLSCs through sponging miR-222-3p to negatively regulate Smad2/7 (Wu et al. 2020). The adipogenic differentiation of PDLSCs can be induced under inflammatory conditions (Yu et al. 2019). Exendin-4 rescues osteogenic differentiation of PDLSCs through regulating Wnt and NF-κB signaling in the presence of LPS (Liu et al. 2019). The present study demonstrated that LPS induced oxidative stress in PDLSCs by reducing antioxidant capability. Antioxidants rescued the inhibitory effects of osteogenic differentiation in the presence of LPS.
Nrf2 is a pivotal modulator for redox balance. Under oxidative stress, Nrf2 translocates into the nucleus, and binds to ARE elements in the promoter regions to activate a battery of antioxidant genes (Zhang et al. 2021). Nrf2 improves the potential of osteogenic differentiation of PDLSCs. Cyclic mechanical stretch promotes Nrf2 nuclear translocation and enhances osteogenic differentiation in PDLSCs (Xi et al. 2021). Nrf2 alleviates the oxidative stress induced by hydrogen peroxide, and inhibits PDLSCs apoptosis by activating its down-stream antioxidant pathways (Liu et al. 2017). On the contrary, Nrf2 inhibition can reduce antioxidant capability and causes oxidative stress. Our results showed that LPS significantly inhibit the expression of Nrf2 and its down-stream antioxidant genes, suggesting that Nrf2 inhibition may be associated with the cytotoxic effects of LPS on PDLSCs. Nrf2 over-expression restored the oxidative stress and cytotoxic effects induced by LPS. Our results suggest that LPS induces oxidative stress and inhibits osteogenic differentiation in PDLSCs through downregulating Nrf2-mediated antioxidant pathway. How LPS caused Nrf2 degradation is needed to be further explored.
Conclusion
LPS decreased viability and osteogenic differentiation of PDLSCs. Antioxidants or Nrf2 over-expression had a direct rescue effect. LPS exerted a cytotoxic effect on PDLSCs through suppressing Nrf2 and inducing oxidative stress. This study provided a new insight into the role of Nrf2 in alveolar bone resorption during periodontitis. Therapeutic strategies enhancing antioxidant capability could be helpful in preventing alveolar bone loss during periodontitis.
Materials and methods
PDLSCs isolation, culture and transduction
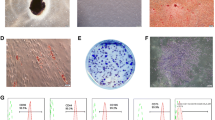
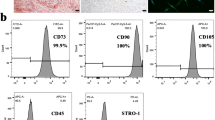
PDLSCs were isolated from rat periodontal ligament tissues according to the standard method (Duan et al. 2018). Briefly, dental molars were extracted from male 6-week-old SD rats. Periodontal tissues were scraped from the middle third of root surface, cut into small pieces and digested with 1 mg/mL collagenase type I (Invitrogen, Carlsbad, CA, USA) for 1 h at 37 °C. The digested tissues were filtered through a 70 μm cell strainer (BD Biosciences, Bedford, MA, USA) to obtain single-cell suspensions. The cells were maintained in DMEM supplemented with 10% fetal bovine serum (FBS; Invitrogen, Carlsbad, CA, USA), 100 U/ml penicillin (Beyotime, Shanghai, China), and 100 mg/ml streptomycin (Beyotime, Shanghai, China) and incubated at 37°C in 5% CO2. The cells at 3 to 5 passages were used. The protocol was approved by the ethics committees for laboratory animals of Xinjiang Medical University.
For LPS treatment, LPS (Sigma-Aldrich, Boston, MA, USA) at concentrations of 0.05, 0.1, 0.2, and 0.4 μg/mL was added into the medium. For antioxidants treatment, acetylcysteine (NAC, 5 mM; Solarbio, Beijing, China) (Mao et al. 2016), L-ascorbic acid (AA, 5mM; Sigma-Aldrich, St. Louis, MO, USA) (Hou et al. 2020), or reduced glutathione (GSH, 3mM; Solarbio, Beijing, China) was added into the medium.
Nrf2-overexpressing lentivirus and the corresponding negative control lentivirus were designed and constructed by TaKaRa (Dalian, China). For lentiviral transduction, 1×105 cells/well were seeded into 24-well plates and infected with lentiviruses at a multiplicity of transfection (MOI) of 40 plus 5 μg/mL Polybrene (Sigma-Aldrich, Boston, MA, USA) for 6 h. Afterward, the cells were replaced with osteogenic medium.
Osteogenic differentiation
For osteogenic differentiation, the cells were seeded in a 12-well plate at a density of 5×104 cells/cm2 and incubated with 10 nM dexamethasone (Sigma-Aldrich, St. Louis, MO, USA), 5 mM β-glycerophosphate (Sigma-Aldrich, St. Louis, MO, USA) and 50 mg/L ascorbic acid (Sigma-Aldrich, St. Louis, MO, USA) for 21 days. Mineralized nodules were stained by Alizarin Red S (Sigma-Aldrich, St. Louis, MO, USA) and photographed by a scanner. The areas of mineralized nodules were analyzed in each well (about 4.5 cm2) by Image J software (National Institutes of Health, Bethesda, MD, USA). Alkaline phosphatase (ALP) activity was measured by an ALP assay kit (Solarbio, Beijing, China) on day 14.
Cell viability assay
CCK8 method was used to detect cell viability. PDLSCs cells were seed in a 96-well plate at a density of 5000 cells/well. At the indicated time points, 20 μl of CCK8 reagent was added to each well and incubated for 2 h at 37 °C. The absorbance at 450 nm was measured using a microplate reader (Bio-Rad, Hercules, CA, USA).
Measurement of cellular ROS
PDLSCs cells were seed in a 96-well plate at a density of 5000 cells/well. After treated with LPS on day 2, the cells were washed with serum-free medium and incubated with 2 μM DCFH-DA (Solarbio, Beijing, China) at 37 °C for 30 min. The fluorescence was measured at 525 nm with excitation at 488 nm using a microplate reader (Bio-Rad, Hercules, CA, USA).
Measurement of oxidative stress indices
PDLSCs cells were seed in a 96-well plate at a density of 5000 cells/well. After the cells were treated with LPS on day 2, the oxidative stress indices, including malondialdehyde (MDA), superoxide, hydrogen peroxide (H2O2), and the activities of antioxidant enzymes (superoxide dismutase, SOD; CAT; and glutathione peroxidase, GSH-Px) were respectively measured with the corresponding commercial kits (Beyotime, Shanghai, China) according to the manufacturer’s protocols. These oxidative stress indices were normalized by the total protein amount.
Immunoblot assay
PDLSCs cells were seeded into 6-well plates. After the cells were treated with LPS or infected with Nrf2-overexpressing lentivirus, total protein was extracted using RIPA buffer (Beyotime, Shanghai, China). Fifty micrograms of protein per sample was separated by 10% SDS-PAGE gel and transferred onto PVDF membranes (Millipore, Bedford, MA, USA). The membranes were blocked with 5% non-fat milk, incubated with primary antibodies against Nrf2 and GAPDH at 4 °C overnight, and incubated with horseradish peroxidase-conjugated secondary antibodies (Beyotime, Shanghai, China) for 1 h at room temperature. The protein bands were visualized using ECL reagent (Beyotime, Shanghai, China), and photographed by ChemiDoc Imaging System (Bio-Rad, Hercules, CA, USA).
Quantitative polymerase chain reaction (qPCR)
Total RNA was extracted using Trizol regent (Beyotime, Shanghai, China) and reversely transcribed into cDNA with a PrimeScript™ RT reagent Kit (TaKaRa, Dalian, China) according to the manufacturer’s instruction. Quantitative PCR was performed to evaluate the mRNA expression of genes using SYBR Premix Ex Taq II (Takara, Dalian, China). The primer sequences of these genes were as follows: ALP, 5'-AGCTTCAGATCGTGCTGACC-3', 5-GTGTACCCCGAGATCCGTTC-3; CAT, 5'-TTTTCACCGACGAGATGGCA-3', 5'-AAGGTGTGTGAGCCATAGCC-3'; GAPDH: 5'-GCATCTTCTTGTGCAGTGCC-3', 5'-GATGGTGATGGGTTTCCCGT-3'; Nrf2, 5'-CACATCCAGTCAGAAACCAGTGG-3', 5'-GGAATGTCTGCGCCAAAAGCTG-3'; GCLC, 5'-ACCAGTTGGCCACTATCTGC-3', 5'-GGCACTGGTGTGGACCTAGA-3'; GPX4, 5'-ATTCCCGAGCCTTTCAACCC-3', 5'-TATCGGGCATGCAGATCGAC-3'; GSR1, 5'-TGCACTTCCCGGTAGGAAAC-3', 5'-GATCGCAACTGGGGTGAGAA-3'. For GAPDH has been revealed to be stable during stem cell differentiation to the osteogenic lineage, GAPDH was used as the internal reference gene (Quiroz et al. 2010). The mRNA expression was calculated by 2−ΔΔCt method.
Statistical analysis
All experiments were performed in triplicate. The data were expressed as mean±standard deviation (SD). Statistical significances were performed with GraphPad Prism software (GraphPad, La Jolla, CA, USA). The difference between control and LPS group was analyzed by Student’s t test. The difference among multiple groups was analyzed by one-way ANOVA with Newman–Keuls. P<0.05 was considered statistically significant.
Reference
Bao L et al (2019) Dysfunction of MiR-148a-NRP1 functional axis suppresses osteogenic differentiation of periodontal ligament stem cells under inflammatory microenvironment. Cell Reprogram 21(6):314–322
Chen Y et al (2020) Carnosol attenuates RANKL-induced osteoclastogenesis in vitro and LPS-induced bone loss. Int Immunopharmacol 89:106978
Dong Z, Yuan Y (2018) Accelerated inflammation and oxidative stress induced by LPS in acute lung injury: ιnhibition by ST1926. Int J Mol Med 41(6):3405–3421
Duan et al (2018) Study of platelet-rich fibrin combined with rat periodontal ligament stem cells in periodontal tissue regeneration. J Cell Mol Med 22(2):1047–1055
Duan Y, An W, Wu Y, Wang J (2020) Tetramethylpyrazine reduces inflammation levels and the apoptosis of LPS-stimulated human periodontal ligament cells via the downregulation of miR-302b. Int J Mol Med 45(6):1918–1926
Feng L et al (2020) Role of Nrf2 in lipopolysaccharide-induced acute kidney injury: Protection by human umbilical cord blood mononuclear cells. Oxid Med Cell Longev 2020:6123459
Henderson B, Kaiser F (2018) Bacterial modulators of bone remodeling in the periodontal pocket. Periodontol 2000 76(1):97–108
Hou S et al (2020) Vitamin C improves the therapeutic potential of human amniotic epithelial cells in premature ovarian insufficiency disease. Stem Cell Res Ther 11(1):159
Jia L, Xiong Y, Zhang W, Ma X, Xu X (2020) Metformin promotes osteogenic differentiation and protects against oxidative stress-induced damage in periodontal ligament stem cells via activation of the Akt/Nrf2 signaling pathway. Exp Cell Res 386(2):111717
Keong JY et al (2020) Effect of lipopolysaccharide on cell proliferation and vascular endothelial growth factor secretion of periodontal ligament stem cells. Saudi Dent J 32(3):148–154
Kukolj T et al (2018) Lipopolysaccharide can modify differentiation and immunomodulatory potential of periodontal ligament stem cells via ERK1,2 signaling. J Cell Physiol 233(1):447–462
Kumar S (2019) Evidence-based update on diagnosis and management of gingivitis and periodontitis. Dent Clin North Am 63(1):69–81
Li L, Maitra U, Singh N, Gan L (2010) Molecular mechanism underlying LPS-induced generation of reactive oxygen species in macrophages. FASEB J 24:422.3-422.3
Liu Y et al (2017) Nrf2 inhibits periodontal ligament stem cell apoptosis under excessive oxidative stress. Int J Mol Sci 18(5):1076
Liu H, Zheng J, Zheng T, Wang P (2019) Exendin-4 regulates Wnt and NF-κB signaling in lipopolysaccharide-induced human periodontal ligament stem cells to promote osteogenic differentiation. Int Immunopharmacol 75:105801
Mao G, Goswami M, Kalen AL, Goswami PC, Sarsour EH (2016) N-acetyl-L-cysteine increases MnSOD activity and enhances the recruitment of quiescent human fibroblasts to the proliferation cycle during wound healing. Mol Biol Rep 43(1):31–39
Quiroz FG et al (2010) Housekeeping gene stability influences the quantification of osteogenic markers during stem cell differentiation to the osteogenic lineage. Cytotechnology 62(2):109–120
Sczepanik FSC et al (2020) Periodontitis is an inflammatory disease of oxidative stress: we should treat it that way. Periodontol 84(1):45–68
Shah SA et al (2017) Melatonin stimulates the SIRT1/Nrf2 signaling pathway counteracting lipopolysaccharide (LPS)-induced oxidative stress to rescue postnatal rat brain. CNS Neurosci Ther 23(1):33–44
Shi H et al (2019) VA inhibits LPS-induced oxidative stress via modulating Nrf2/NF-κB-signalling pathways in bovine mammary epithelial cells. Ital J Anim Sci 18(1):1099–1110
Tanaka M et al (2018) Terminalia bellirica (Gaertn.) Roxb. extract and gallic acid attenuate LPS-induced inflammation and oxidative stress via MAPK/NF-κB and Akt/AMPK/Nrf2 pathways. Oxid Med Cell Longev 2018:9364364
Tonelli C, Chio IIC, Tuveson DA (2018) Transcriptional regulation by Nrf2. Antioxid Redox Signal 29(17):1727–1745
Wang W et al (2020) Lipopolysaccharide inhibits osteogenic differentiation of periodontal ligament stem cells partially through toll-like receptor 4-mediated ephrinB2 downregulation. Clin Oral Investig 24(10):3407–3416
Wu D et al (2020) Long noncoding RNA TUG1 promotes osteogenic differentiation of human periodontal ligament stem cell through sponging microRNA-222-3p to negatively regulate Smad2/7. Arch Oral Biol 117:104814
Xi X et al (2021) Nrf2 activation is involved in osteogenic differentiation of periodontal ligament stem cells under cyclic mechanical stretch. Exp Cell Res 403(2):112598
Yoshinaga Y et al (2012) Topical application of lipopolysaccharide into gingival sulcus promotes periodontal destruction in rats immunized with lipopolysaccharide. J Periodontal Res 47(5):674–680
Yu B, Li Q, Zhou M (2019) LPS-induced upregulation of the TLR4 signaling pathway inhibits osteogenic differentiation of human periodontal ligament stem cells under inflammatory conditions. Int J Mol Med 43(6):2341–2351
Zhang L et al (2021) Nrf2 is a potential modulator for orchestrating iron homeostasis and redox balance in cancer cells. Front Cell Dev Biol 9:728172
Zhao B et al (2020) Effects of rutin on the oxidative stress, proliferation and osteogenic differentiation of periodontal ligament stem cells in LPS-induced inflammatory environment and the underlying mechanism. J Mol Histol. 51(2):161–171
Zheng W, Wang S, Wang J, Jin F (2015) Periodontitis promotes the proliferation and suppresses the differentiation potential of human periodontal ligament stem cells. Int J Mol Med 36(4):915–922
Zhu W, Liang M (2015) Periodontal ligament stem cells: current status, concerns, and future prospects. Stem Cells Int 2015:972313
Acknowledgements
This work was supported by the funds of First Affiliated Hospital of Xinjiang Medical University (Affiliated Stomatological Hospital).
Funding
First Affiliated Hospital of Xinjiang Medical University (Affiliated Stomatological Hospital).
Author information
Authors and Affiliations
Contributions
YC conceived and designed the experiments; AG and JZ conducted the experiments; YC analyzed and interpreted the experimental results; YC wrote the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflicts of interest. Yue Chen declares that she has no conflict of interest. Awuti Gulinuer declares that he has no conflict of interest. Jin Zhao declares that he has no conflict of interest.
Ethical approval
The protocol of isolation of rat periodontal ligament stem cells was approved by the ethics committees for laboratory animals of Xinjiang Medical University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Y., Gulinuer, A. & Zhao, J. Lipopolysaccharide induces oxidative stress and inhibits osteogenic differentiation in periodontal ligament stem cells through downregulating Nrf2. Mol. Cell. Toxicol. 19, 247–254 (2023). https://doi.org/10.1007/s13273-022-00253-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13273-022-00253-x