Abstract
Background
Bone cancer pain (BCP) seriously affects patient’s quality of life, which remains a difficult clinical problem, lacking effective drugs for treating it. The inflammation in the spinal cord involves the pathogenesis of BCP. The inhibition of spinal phosphatidylinositol 3-kinase (PI3K)/protein kinase B (AKT) signaling pathway or spinal P2X7 receptor (P2X7R) has previously been shown to alleviate BCP. Naringenin (NAR) has analgesic role and anti-inflammatory property.
Objective
The present study investigated the protection of NAR against BCP and explored whether the inhibition of spinal inflammation and the blockade of spinal P2X7R/PI3K/AKT signaling involved in this protection.
Result
NAR significantly alleviated mechanical allodynia (the increase of paw withdrawal threshold in Von Frey test) and thermal hyperalgesia (the increase of paw withdrawal latency in Hargreaves test) in BCP rats. Additionally, NAR inhibited inflammatory cytokines (the reduced levels of tumor necrosis factor-α (TNF-α), interleukin-1β (IL-1β) and interleukin-6 (IL-6) were measured using Elisa assay) and down-regulated P2X7R/PI3K/AKT signaling (the decreased P2X7R expression, the reduced ratios of phosphorylated (p)-PI3K/PI3K and p-AKT/AKT, which were detected Western blot) in the spinal cord of BCP rats.
Conclusion
NAR alleviated BCP through inhibiting inflammatory cytokines and down-regulating P2X7R/PI3K/AKT signaling in the spinal cord of rats. These findings revealed that NAR, as an effective agent against BCP, may provide an effective approach in the management of bone cancer patients.
Graphic abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bone cancer pain (BCP) is a typical symptom of the patients with bone tumor or tumor skeletal metastases (Rodriguez et al. 2019), which seriously decreases patient’s physical function and quality of life, is estimated to impact about 36–50% of cancer patients (Frost et al. 2016). Currently, given the mechanism underlying BCP is not yet clear and the existing drug interventions are still not satisfactory, BCP remains an intractable clinical problem (Mantyh 2013). Therefore, exploitation of more effective and rational new treatment strategies for BCP is urgently needed.
Naringenin (NAR) is a naturally occurring flavanone, like other flavonoids, which is known for its antioxidant and anti-inflammatory properties and thus has potential to be used as a therapeutic tool (Yang et al. 2020; Zeng et al. 2018). Given neuroinflammation plays a key role in pain (Matsuda et al. 2019), increasing studies suggest that the potential of NAR in analgesia has been gradually explored. The analgesic effects of NAR on neuropathic pain caused by spinal nerve ligation (Hu and Zhao 2014) and chronic compression nerve injury (Kaulaskar et al. 2012) in rats has been reported. In addition, NAR ameliorates diabetic neuropathic pain (Singh et al. 2020). Furthermore, a series of studies have shown that NAR inhibits inflammatory pain (Pinho-Ribeiro et al. 2016). Despite the above literatures demonstrated the analgesic effects of NAR in some diseases, whether NAR counteracts BCP is still unknown. Therefore, rats were injected with Walker 256 tumor cells to construct a model of BCP for exploring the potential therapeutic function of NAR on BCP and its underlying mechanisms.
P2X7 receptor (P2X7R) is a subtype of ATP-gated ion channel purinergic receptor, which is mainly expressed in glial cells in the dorsal horn of spinal cord. P2X7R activation can promote the release of various inflammatory mediators by glial cells and mediate the central sensitization of spinal cord (Calzaferri et al. 2020). Cumulative investigations suggested that anti-nociceptive effects of P2X7R inhibition or knockout in various neuropathic and inflammatory pain (Burnstock 2016). Recent, it has been confirmed that P2X7R-specific inhibitor BBG was to be capable of relieving BCP-associated symptoms (Yang et al. 2015). Based on these, previous studies suggested that spinal P2X7R as a possible target in BCP treatment, and we further investigated whether the down-regulation of spinal P2X7R is involved in the protection of NAR against BCP.
Phosphatidylinositol 3-kinase (PI3K)/protein kinase B (AKT) pathway is essential in the development and maintenance of chronic pain, especially in BCP (Chen et al. 2017). The activation of PI3K/AKT signal pathway in the spinal cord was reported to participate in the progression of BCP (Guan et al. 2015a, b). In contrast, the inhibition of PI3K/AKT attenuates the mechanical nociception in BCP rats and suppresses BCP-associated behaviors (Guan et al. 2015a, b; Huang and Zhang 2014; Peng et al. 2019). For example, the short interference RNA (siRNA) targeting NMUR2 relieves nociception in rat through inhibiting spinal PI3K/AKT pathways (Peng et al. 2019). These observations indicated that the down-regulation of spinal PI3K/AKT may be a novel candidate for BCP therapy. Notably, the P2X7R is a key modulator of the PI3K/AKT signaling. In experimental neuroblastoma cells, P2X7R stimulation enhances PI3K/AKT and P2X7R silencing or antagonist administration reduces the activity of PI3K/AKT (Amoroso et al. 2015). In addition, highly expressed P2X7R promotes growth and metastasis of human HOS/MNNG osteosarcoma cells via activation of PI3K/AKT signaling (Zhang et al. 2019). Therefore, the aforementioned studies led us to a hypothesis that inhibition of the spinal P2X7R/PI3K/AKT pathway contributes to the protective role of NAR against BCP.
The present study aimed to confirm the antagonized function of NAR on BCP and explore underlying mechanisms. The results demonstrated that NAR significantly relieves nociception, suppresses spinal inflammation and decreases the spinal P2X7R/PI3K/AKT pathway in rats with BCP. These findings suggested NAR as a novel therapeutic approach for treatment of BCP, which may be related to the inhibition of spinal inflammatory cytokines by the blocked spinal cord P2X7R/PI3K/ AKT signaling pathway.
Materials and methods
Material
NAR were supplied by Sigma‑Aldrich; Merck KGaA (St. Louis, MO, USA). The BCA protein assay kit was obtained from Beyotime Biotechnology, Inc (Shanghai, China). The enzyme-linked immunosorbent assay (Elisa) kits for tumor necrosis factor-α (TNF-α), Iterleukin-1 beta (IL-1β) and Iterleukin-6 (IL-6) were purchased from R&D Systems (R&D Systems, Minneapolis, MN). Specific monoclonal antibodies against phosphorylated (p)-PI3K, PI3K, p-AKT, AKT and P2X7R were supplied by obtained from Cell Signaling Technology, Inc (Boston, USA). GAPDH antibody and anti-rabbit IgG-HRP-linked antibody were purchased by Proteintech (Danvers, MA, USA).
Preparation of tumor cells
As described previously (Mao-Ying et al. 2006), after intraperitoneal injection (i.p.) of Walker 256 tumor cells into the rats for 1 week, the carcinoma cells were extracted, washed with PBS, and re-suspended to a final concentration of 5 × 105 cells/10 μL. The same concentration of cancer cells was used as a sham operation group after being inactivated for 30 min.
Animals
100 adult female Sprague–Dawley rats (age 8–10 weeks; weight 220–250 g) were supplied by Hunan SJA Laboratory Animal Co., Ltd (Hunan, China). All rats were kept in single cages in a specific-pathogen-free environment with constant temperature (22 ± 2 °C) and humidity (50%), under a 12-h light/dark cycle. Adequate food and water were provided to the rats and change bedding frequently to ensure a comfortable environment. This study was approved by the Experimental Animals Welfare and Ethics Committee of Hengyang Center Hospital.
Establishment of BCP model
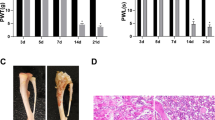
The model of BCP was established by injecting Walker 256 tumor cells into the marrow cavity of leg of the rats as previously described (Gu et al. 2020; Mao-Ying et al. 2006). The steps are as follows: rats were anesthetized with pentobarbital sodium (60 mg/kg. i.p.) and fixed on the operating table in supine position. Subsequently, 1 cm superficial incision was made in the right leg to expose the rat’s right tibia, and a small hole was drilled in the lower third. Then, the cancer cells (10 μL, 5 × 105) or heat-inactivated cancer cells (Sham group) were slowly injected into the marrow cavity using a micro-syringe. The syringe was left in place for an additional 2 min to prevent any leakage of tumor cells followed by sealing the hole with bone wax immediately. Finally, penicillin was used locally at the wound to prevent subsequent infection and then layered sutures.
Experimental protocol
After a week of adaptation to the experimental environment, the rats were randomly distributed into 5 groups (20 rats in each group): (1) Sham group: rats that injected with inactivated Walker 256 cells; (2) BCP group: rats that were injected with activated Walker 256 cells and then orally treated with vehicle (saline, 1.5 mL) for 10 days; (3) BCP + low-dose NAR group: rats were injected with activated Walker 256 cells and then orally treated with NAR (16.7 mg/kg/day; diluted in saline) for 10 days; (4) BCP + middle-dose NAR group: rats were injected with activated Walker 256 cells and then orally treated with NAR (50 mg/kg/day; diluted in saline) for 10 days; (5) BCP + high-dose NAR group: rats were injected with activated Walker 256 cell and then orally treated with NAR 150 mg/kg/day; diluted in saline) for 10 days. NAR (16.7–150 mg/kg) or vehicle was treated once per day from postoperative days (POD) 6–15. For better understanding, schematic diagram of the experimental schedule are illustrated in Fig. 1.
Mechanical allodynia test
The mechanical allodynia of rats was tested using Von Frey filaments (IITC, USA) as previously described (Campana and Rimondini 2021; Xu et al. 2019). After rats had habituated to the experimental environment for at least 2 days, baseline levels were measured the day before surgery to narrow the error. Before the test, each rat was isolated in a plexiglass chamber (25 × 20 × 20 cm) with iron grids (0.5 × 0.5 cm) on the bottom and allowed it for at least 30 min for adaption. During the formal test, a pressure was vertically exerted on the plantar surface of the operated hind leg for 2–3 s until the positive signs were shown up (rapidly pull back or bit or lick or shake the tested hind leg). The measurement was repeated three times with a gap of 5 min each time. The maximal level tolerance in grams is defined as the paw withdrawal threshold (PWT), the value of PWT was calculated as the average value of the three tests. All the data collected were according to the laws of Dixon’s up–down method.
Thermal hyperalgesia test
The thermal hyperalgesia was assessed by measuring the paw withdrawal latency (PWL) in response to heat stimulation using Hargreaves test as described by previous report (Campana and Rimondini 2021; Xu et al. 2019). Specifically, an acclimation period of 30 min was applied for each test before starting. Each experimental rats were put in Plexiglas chambers with elevated glass floor, which was heated evenly by a radiant heat source (IITC Life Science, Woodland Hills, CA). During the test, the thermal stimulus was concentrated and transmitted to the position of hind paw. The PWL to heat stimulation were recorded as the time from the onset of radiant heating to the obvious withdrawal of the hind paw, and a 20 s cutoff automatically was set to prevent tissue damage. Thermal stimuli were delivered three times to hind paw at intervals of 5–8 min, the average of three measurements of PWL was used as the result of each test session.
Enzyme-linked immunosorbent assay (Elisa) for inflammatory cytokines
On the next day after NAR last treatment, the whole spinal cord at the L4–L5 segments was rapidly dissected from anesthetized rats (n = 5 each group). The tissue samples were homogenized in ice-cold PBS and centrifuged (12,000×g, 10 min, 4 °C). Finally, the supernatant was aspirated to measure the levels of TNF-α, IL-1β and IL-6 using Elisa kits (TNF-α kit: RTA00; IL-1β kit: RLB00; IL-6 kit: R6000B; R&D Systems) according to the previously described protocol (Griffin et al. 2006). The results were expressed as pg/mg (per protein).
Western blot analysis
The protein levels of p-PI3K, PI3K, p-AKT, AKT and P2X7R were measured by western blotting. The next day after NAR treatment ended, the rats (n = 5 each group) were deeply anesthetized with pentobarbital sodium (60 mg/kg, i.p.) and then the L4–L5 segments of ipsilateral spinal cord were harvested. Next, the tissue samples was homogenized in ice-cold homogenizing buffer and the centrifuged at 12,000×g for 30 min at 4 °C. The supernatant was extracted and the protein concentration was analyzed using a BCA protein assay kit. Subsequently, equal amounts of protein (10 μg) was loaded on 10% SDS polyacrylamide gels (8–12%) and transferred onto PVDF membranes by electroblotting. The membrane was blocked with TBS-Tween-20 containing 5% non-fat milk for 2 h at room temperature (RT) and incubated with primary antibodies (1:1000) for overnight at 4 °C. After the membranes were washed with TBS-T and further incubated horseradish peroxidase-conjugated goat anti-rabbit IgG (1:5000) for 2 h at 4 °C. Then, the membranes were washed with TBS-T buffer and added with electrogenerated chemiluminescence (ECL) reagent (Thermo Fisher Scientific, Inc.). Finally, the immunoreactive bands were visualized by Tanon-5600 Imaging System (Tanon Science and Technology Co., Ltd.). The gray values of bands were analyzed by Image Lab software (Bio-Rad), and normalized with GAPDH.
Statistical analysis
All experiments were repeated ≥ 3 times, and statistical analyses were performed using SPSS 20.0 software (IBM Corp.). Data are presented as the mean ± SEM, and the significance of intergroup discrepancy was assessed using one-way analysis of variance (ANOVA) and Tukey's post hoc test. Two-tailed P < 0.05 was considered to indicate a statistically significant difference.
Results
NAR does not affect body weight in BCP rats
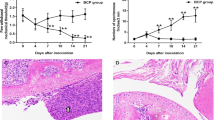
The results of the body weight growth curve revealed that the body weight of BCP group rats was significantly lower than that of the sham group from the postoperative days (POD) 15 (F4,45 = 3.743, P < 0.05), and gradually decreased from POD 18 (Fig. 2). These results indicated that BCP rats gradually lost weight, as a sign of successful bone cancer modeling. In addition, different concentrations of NAR (16.7, 50 and 150 mg/kg) did not change the body weight of BCP rats, eliminating the interference of animal weight on the experimental results (Fig. 2).
Effect of NAR on body weight in BCP rats. Rats were injected with Walker 256 cells and then treated with different doses of NAR (16.7, 50 and 150 mg/kg, p.o.) once per day for 10 days from postoperative days (POD) 6–15. The body weight of rats was measured on baseline and POD 3, 6, 9, 12, 15, 18, 21, 24. Data are expressed as the mean ± SEM (number of repeated measurements: n = 10/group). *P < 0.05, ***P < 0.001 compared with the sham group
NAR ameliorates mechanical allodynia in a dose-dependent manner of BCP rats
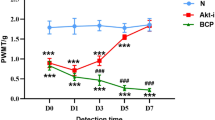
To assess the antinociceptive role of NAR in BCP, we first explored whether NAR alleviates mechanical allodynia by observing the effect of NAR on the PWT in BCP rats. We found that the PWT of BCP rats showed a significant decrease on POD 6 and continued to decline at a certain speed compared with sham group as a sign of successful BCP modeling (Fig. 3A). However, NAR (16.7, 50 and 150 mg/kg) significantly elevated the PWT of BCP rats in a dose-dependent compared with that in the vehicle-treated BCP group (POD 9: F4,45 = 16.732, P < 0.05; POD 12: F4,45 = 32.417, P < 0.01; POD 15: F4,45 = 46.902, P < 0.001; POD 18: F4,45 = 59.828, P < 0.05; POD 21: F4,45 = 123.418, P < 0.001). The analgesic effect of NAR was started on POD 9, 3 days after beginning NAR treatment, and this effect of NAR were still observed on POD 21, 6 days after the treatment was stopped. However, the effect of NAR at low dosage, 16.7 mg/kg, started on POD 12 and lasted only for 3 days after drug withdrawal (Fig. 3A). Additionally, there was no significant difference in baseline PWT level between groups (F4,45 = 0.144, P > 0.05). These results indicated that NAR improved mechanical allodynia in BCP rats.
Effect of NAR on mechanical allodynia and thermal hyperalgesia in the BCP rats. Rats were injected with Walker 256 cells and then treated with different doses of NAR (16.7, 50 and 150 mg/kg, p.o.) once per day for 10 days from postoperative days (POD) 6–15. The BCP performance of rats was test using the mechanical allodynia test (Von Frey test) and thermal hyperalgesia test (Hargreaves test), the PWT (A) and PWL (B) were recorded. Data are expressed as the mean ± SEM (number of repeated measurements: n = 10/group). ***P < 0.001 compared with the sham group; #P < 0.05, ##P < 0.01 and ###P < 0.001 compared with the BCP group
NAR ameliorates thermal hyperalgesia in a dose-dependent manner of BCP rats
To assess the antinociceptive role of NAR in BCP, we further explored whether NAR alleviates thermal hyperalgesia by observing the effect of NAR on the PWL in BCP rats. We found that the PWL of BCP rats showed a significant decrease on POD 6 and continued to decline at a certain speed compared with sham group, which further confirms the successful BCP modeling (Fig. 3B). In contrast, NAR (16.7, 50 and 150 mg/kg) significantly elevated the PWL of BCP rats in a dose-dependent of BCP rats (POD 9: F4,45 = 20.091, P < 0.01; POD 12: F4,45 = 34.582, P < 0.001; POD 15: F4,45 = 56.523, P < 0.001; POD 18: F4,45 = 84.422, P < 0.01; POD 21: F4,45 = 123.418, P < 0.001). The analgesic effect of NAR started on POD 9, 3 days after beginning NAR treatment, and this effect of NAR were still observed on POD 21, 6 days after the treatment was stopped. However, the effect of NAR at low (16.7 mg/kg) and middle (50 mg/kg) dosage, started on POD 12 and lasted only for 3 days after drug withdrawal (Fig. 3B). Additionally, there was no significant difference in baseline PWL level between groups (F4,45 = 0.567, P > 0.05). These results indicated that NAR improved thermal hyperalgesia in BCP rats.
NAR suppresses inflammatory cytokines in spinal cord of BCP rats
To verify whether the analgesic action of NAR in BCP is accompanied with the inhibition of inflammatory in spinal cord, we next determined that NAR down-regulated inflammatory cytokines of spinal cord by examining the effects of NAR on the levels of TNF-α, IL-1β and IL-6 in BCP rats. Elisa results revealed that the levels of TNF-α, IL-1β and IL-6 in spinal cord of BCP rats significantly increased compared with sham group. However, NAR (16.7, 50 and 150 mg/kg) dramatically suppressed the increases of TNF-α (F4,20 = 315.663, P < 0.01), IL-1β (F4,20 = 125.237, P < 0.05) and IL-6 (F4,20 = 109.587, P < 0.05) in spinal cord of BCP model rat in a dose-dependent manner (Fig. 4A–C). These results indicated inhibition of spinal inflammatory may contribute to the NAR-provided protection against allodynia in BCP rats.
Effect of NAR on inflammatory cytokines in the spinal cord of BCP rats. Rats were injected with Walker 256 cells and then treated with different doses of NAR (16.7, 50 and 150 mg/kg, p.o.) once per day for 10 days from postoperative days (POD) 6–15. The levels of TNF-α (A), IL-1β (B) and IL-6 (C) in spinal cord were determined by Elisa. Data are expressed as the mean ± SEM (number of repeated measurements: n = 3/group). ***P < 0.001, compared with the sham group; #P < 0.05, ##P < 0.01 and ###P < 0.001 compared with the BCP group
NAR down-regulates spinal P2X7R/ PI3K/AKT signaling in BCP rats
To investigate whether the potential mechanisms of the analgesic function of NAR in BCP involves the down-regulation of P2X7R/PI3K/AKT signaling pathway, we explored the effect of NAR on P2X7R/PI3K/AKT signaling in spinal cord of BCP rats. Western blotting results demonstrated that NAR (16.7, 50 and 150 mg/kg) obviously reversed the up-regulations of P2X7R expression level (F4,10 = 41.611, P < 0.01) as well as the ratios of p-PI3K/PI3K (F4,10 = 38.223, P < 0.05) and p-AKT/AKT (F4,10 = 23.105, P < 0.05) in spinal cord of BCP rats in a dose-dependent manner (Fig. 5A–D). These results revealed that NAR may relieve BCP by preventing P2X7R/PI3K/AKT signaling up-regulation in rat spinal cord.
Effect of NAR on P2X7R/PI3K/AKT signaling in the spinal cord of BCP rats. Rats were injected with Walker 256 cell and then treated with different doses of NAR (16.7, 50 and 150 mg/kg, p.o.) once per day for 10 days from postoperative days (POD) 6–15. The protein expression levels of P2X7R, p-PI3K, PI3K, p-AKT and AKT in spinal cord were detected by western blotting. Data are expressed as the mean ± SEM (number of repeated measurements: n = 3/group). ***P < 0.001 compared with the sham group; #P < 0.05, ##P < 0.01 and ###P < 0.001 compared with the BCP group
Discussion
The analgesic role of NAR has been previously reported (Hu and Zhao 2014; Kaulaskar et al. 2012; Pinho-Ribeiro et al. 2016; Singh et al. 2020). Spinal inflammation involves the development of BCP (Chen et al. 2019). Additionally, the inhibition of P2X7R (Yang et al. 2015) or PI3K/AKT signaling (Guan et al. 2015a, b; Huang and Zhang 2014; Peng et al. 2019) in the spinal cord alleviates BCP. The present study used cancer cell injection-induced-BCP rats to investigate whether NAR could ameliorate BCP, and further explore whether the inhibition of inflammation and P2X7R/PI3K/AKT in spinal cord involves this protection. Our findings revealed that NAR prevented BCP by inhibiting inflammatory cytokines and P2X7R/PI3K/AKT signaling in the spinal cord.
Currently, BCP remains a challenging problem in the clinic due to its complex and poorly elucidated etiology and mechanisms (Mantyh 2013). Therefore, effective approaches against BCP may provide a better outcome in the management of bone cancer patients. In the present work, the female SD rats were intramedullary injected with Walker 256 cells to establish the ex vivo model of BCP, which is widely used to explore the mechanism of analgesic drugs due to its stable and sustaining pain-related behaviors (Akoury et al. 2019). BCP manifests as spontaneous pain, hyperalgesia, and allodynia (Urch 2004). In our work, we detected the mechanical allodynia and thermal hyperalgesia of BCP rats. The present results showed that the PWT and PWL in BCP rats presented a significant decrease on POD 6 and continued to decline at a certain speed compared to sham rats until POD 24, which was generally in line with the previous research results (Ni et al. 2019, 2020). In conclusion, the BCP model was established successfully.
Inflammation is a key contributor for cancer pain, in another word, cancer-related inflammation is a cause of cancer pain (Chen et al. 2019). It has been shown that the activated glial cells of spinal cord contributed to the development and maintenance of BCP by releasing pro-inflammatory cytokines such IL-6, IL-1β, and TNF-α. (Liu et al. 2018; Shen et al. 2014). Consistent with this, we found BCP rats had higher the levels of TNF-α, IL-1β and IL-6 in spinal cord compared with sham rats in the present work. Interestingly, NAR has powerful anti-inflammatory action in central nervous system (Zeng et al. 2018) and analgesic role in a variety of disease models (Hu and Zhao 2014; Pinho-Ribeiro et al. 2016; Singh et al. 2020). Therefore, we aimed to explore the analgesic function of NAR in BCP and whether it is related to the inhibition of spinal inflammation. We found that NAR reversed the reduced PWT and PWL in BCP rats in a dose-dependent manner, suggesting that NAR exerted anti-nociception in BCP model. Therefore, it can be suggested that NAR is an effective therapeutic drug for BCP in bone cancer patients. In addition, NAR obviously decreased the levels of TNF-α, IL-1β and IL-6 in spinal cord of BCP rats, revealing NAR improve BCP by inhibiting spinal cord inflammation cytokines in rats. It has previously been confirmed that the analgesic effect of NAR in rats with spinal nerve ligation‑induced neuropathic pain were exerted by suppressing inflammatory in spinal dorsal horn (Hu and Zhao 2014). These previous findings offer a reasonable explanation for the results obtained in the present study.
The present study further investigated the possible underlying mechanism for the protective role of NAR against BCP. It has been confirmed that of the deactivation of PI3K/AKT signaling ameliorates BCP (Guan et al. 2015a, b; Huang and Zhang 2014; Peng et al. 2019). Notably, the targeted inhibition of P2X7R may be an effective treatment for BCP (Burnstock 2016; Yang et al. 2015). Therefore, it was hypothesized that the P2X7R/PI3K/AKT signaling in spinal cord may be involved in NAR-mediated the protection against BCP. Our study evaluated the role of NAR on spinal P2X7R/PI3K/AKT signaling pathway in BCP rats. It was revealed that NAR reversed the up-regulations of P2X7R expression level, as well as the ratios of p-PI3K/PI3K and p-AKT/AKT in spinal cord of BCP rats, which indicated that the down-regulation of the P2X7R/PI3K/AKT signaling contributed to the beneficial effect of NAR on BCP. It has previously been confirmed that NAR improve pathological status by inhibiting PI3K/AKT signal in a variety of diseases (Zhao et al. 2017; Zhou et al. 2019). And, teniposide ameliorates BCP in rats via the inhibited P2X7R had been demonstrated (Yan et al. 2018). These previous findings offer a reasonable explanation for the results obtained in the present study.
In the above results, we found that NAR inhibited P2X7R/PI3K/AKT signaling and inflammatory cytokines in the spinal cord while exerting the anti-BCP effect. Both PI3K/AKT signaling (Yeung et al. 2018) and P2X7R (Adinolfi et al. 2018) have been widely demonstrated to play a major role in the inflammatory response (Adinolfi et al. 2018; Yeung et al. 2018), so it would be interesting to further explore the relationship between PI3K/AKT/P2X7R pathway and cytokines (TNF-α, IL-1β, IL-6) under BCP with NAR, thus deepen the mechanism depth of our research. Evidence shows that PI3K/AKT signaling pathways enable the transcription factor nuclear factor κB (NF-κB) to enhance the activity of inflammatory mediator genes, so the PI3K/AKT/NF-κB axis is essential for the expression of pro-inflammatory genes such as TNF-α, IL-1β and IL-6 (Cianciulli et al. 2016; Yeung et al. 2018). In addition, a decrease of inflammatory mediators such as TNF-α and IL-6 production in PI3K-γ knockout mice showed the importance of PI3K in the regulation of inflammatory responses (Crackower et al. 2002). And, PI3K signal regulate IL-6 secretion by interacting with CD80/CD86 on the surface of dendritic cells. Studies have shown that inhibition of PI3K signaling during TLR-mediated inflammation can inhibit the secretion of pro-inflammatory cytokines such as IL-6 in macrophages and dendritic cells (Shi et al. 2016). On the other hand, the P2X7R is expressed by virtually all immune and inflammatory cells, and is up-regulated during inflammation (Di Virgilio 2015). P2X7R play key role during innate immune responses by triggering the NLRP3 inflammasome rapidly, which could consecutively facilitate caspase-1 meditated maturation and release of the pro-inflammatory cytokines IL-1β (Di Virgilio 2007; Shen et al. 2018). The pro-inflammatory cytokines secreted following P2X7R activation include not only IL-1β and IL-18 but also IL-6 and IL-1α (Englezou et al. 2015; Gicquel et al. 2015). Consistent with PI3K/AKT signaling, P2X7R also activates NF-κB to promote expression of several inflammatory genes, including TNF-α and IL-1β (Genetos et al. 2011). Taken together, in the study, we speculated that the improvement of BCP by NAR was achieved through inhibiting spinal inflammatory cytokines by down-regulating spinal P2X7R/PI3K/AKT signaling.
In conclusion, the present study demonstrated that NAR had ability to prevent mechanical allodynia and thermal hyperalgesia, suppress spinal inflammation and down-regulate the spinal P2X7R/PI3K/AKT signaling in BCP rats. These results indicated that NAR ameliorated BCP by inhibiting the spinal inflammation and down-regulating the spinal P2X7R/PI3K/AKT, and suggest that NAR may act as a potential preventive agent for BCP, which is important for improving the therapeutic effect of bone cancer patients.
References
Adinolfi E, Giuliani AL, De Marchi E et al (2018) The P2X7 receptor: a main player in inflammation. Biochem Pharmacol 151:234–244
Akoury E, Ahangar P, Nour A et al (2019) Low-dose zoledronate for the treatment of bone metastasis secondary to prostate cancer. Cancer Cell Int 19:28
Amoroso F, Capece M, Rotondo A et al (2015) The P2X7 receptor is a key modulator of the PI3K/GSK3beta/VEGF signaling network: evidence in experimental neuroblastoma. Oncogene 34:5240–5251
Burnstock G (2016) Purinergic mechanisms and pain. Adv Pharmacol 75:91–137
Calzaferri F, Ruiz-Ruiz C, de Diego AMG et al (2020) The purinergic P2X7 receptor as a potential drug target to combat neuroinflammation in neurodegenerative diseases. Med Res Rev 40:2427–2465
Campana G, Rimondini R (2021) Mechanical nociception in mice and rats: measurement with automated von Frey equipment. Methods Mol Biol 2201:195–198
Chen SP, Zhou YQ, Liu DQ et al (2017) PI3K/Akt pathway: a potential therapeutic target for chronic pain. Curr Pharm Des 23:1860–1868
Chen J, Cong X, Zhan X et al (2019) Effects of parecoxib on pain threshold and inflammatory factors IL-1beta, IL-6 and TNF-in spinal cord of rats with bone cancer pain. J Coll Physicians Surg Pak 29:528–531
Cianciulli A, Calvello R, Porro C et al (2016) PI3k/Akt signalling pathway plays a crucial role in the anti-inflammatory effects of curcumin in LPS-activated microglia. Int Immunopharmacol 36:282–290
Crackower MA, Oudit GY, Kozieradzki I et al (2002) Regulation of myocardial contractility and cell size by distinct PI3K-PTEN signaling pathways. Cell 110:737–749
Di Virgilio F (2007) Liaisons dangereuses: P2X(7) and the inflammasome. Trends Pharmacol Sci 28:465–472
Di Virgilio F (2015) P2X receptors and inflammation. Curr Med Chem 22:866–877
Englezou PC, Rothwell SW, Ainscough JS et al (2015) P2X7R activation drives distinct IL-1 responses in dendritic cells compared to macrophages. Cytokine 74:293–304
Frost CO, Hansen RR, Heegaard AM (2016) Bone pain: current and future treatments. Curr Opin Pharmacol 28:31–37
Genetos DC, Karin NJ, Geist DJ et al (2011) Purinergic signaling is required for fluid shear stress-induced NF-kappaB translocation in osteoblasts. Exp Cell Res 317:737–744
Gicquel T, Robert S, Loyer P et al (2015) IL-1beta production is dependent on the activation of purinergic receptors and NLRP3 pathway in human macrophages. FASEB J 29:4162–4173
Griffin R, Nally R, Nolan Y et al (2006) The age-related attenuation in long-term potentiation is associated with microglial activation. J Neurochem 99:1263–1272
Gu W, Sun Y, Gu W et al (2020) The analgesic effects of pioglitazone in the bone cancer pain rats via regulating the PPARgamma/PTEN/mTOR signaling pathway in the spinal dorsal horn. Biomed Pharmacother 131:110692
Guan X, Fu Q, Xiong B et al (2015a) Activation of PI3Kgamma/Akt pathway mediates bone cancer pain in rats. J Neurochem 134:590–600
Guan XH, Fu QC, Shi D et al (2015b) Activation of spinal chemokine receptor CXCR3 mediates bone cancer pain through an Akt-ERK crosstalk pathway in rats. Exp Neurol 263:39–49
Hu CY, Zhao YT (2014) Analgesic effects of naringenin in rats with spinal nerve ligation-induced neuropathic pain. Biomed Rep 2:569–573
Huang HJ, Zhang M (2014) Downregulation of PI3Kcb utilizing adenovirus-mediated transfer of siRNA attenuates bone cancer pain. Int J Clin Exp Pathol 7:8127–8135
Kaulaskar S, Bhutada P, Rahigude A et al (2012) Effects of naringenin on allodynia and hyperalgesia in rats with chronic constriction injury-induced neuropathic pain. Zhong Xi Yi Jie He Xue Bao 10:1482–1489
Liu S, Liu YP, Lv Y et al (2018) IL-18 contributes to bone cancer pain by regulating glia cells and neuron interaction. J Pain 19:186–195
Mantyh P (2013) Bone cancer pain: causes, consequences, and therapeutic opportunities. Pain 154(Suppl 1):S54–S62
Mao-Ying QL, Zhao J, Dong ZQ et al (2006) A rat model of bone cancer pain induced by intra-tibia inoculation of Walker 256 mammary gland carcinoma cells. Biochem Biophys Res Commun 345:1292–1298
Matsuda M, Huh Y, Ji RR (2019) Roles of inflammation, neurogenic inflammation, and neuroinflammation in pain. J Anesth 33:131–139
Ni H, Wang Y, An K et al (2019) Crosstalk between NFkappaB-dependent astrocytic CXCL1 and neuron CXCR2 plays a role in descending pain facilitation. J Neuroinflamm 16:1
Ni H, Xu M, Xie K et al (2020) Liquiritin alleviates pain through inhibiting CXCL1/CXCR2 signaling pathway in bone cancer pain rat. Front Pharmacol 11:436
Peng S, Lu Y, Li P et al (2019) The short interference RNA (siRNA) targeting NMUR2 relieves nociception in a bone cancer pain model of rat through PKC-ERK and PI3K-AKT pathways. Biochem Biophys Res Commun 512:616–622
Pinho-Ribeiro FA, Zarpelon AC, Fattori V et al (2016) Naringenin reduces inflammatory pain in mice. Neuropharmacology 105:508–519
Rodriguez C, Ji M, Wang HL et al (2019) Cancer pain and quality of life. J Hosp Palliat Nurs 21:116–123
Shen W, Hu XM, Liu YN et al (2014) CXCL12 in astrocytes contributes to bone cancer pain through CXCR4-mediated neuronal sensitization and glial activation in rat spinal cord. J Neuroinflamm 11:75
Shen HH, Yang YX, Meng X et al (2018) NLRP3: a promising therapeutic target for autoimmune diseases. Autoimmun Rev 17:694–702
Shi ZM, Han YW, Han XH et al (2016) Upstream regulators and downstream effectors of NF-kappaB in Alzheimer’s disease. J Neurol Sci 366:127–134
Singh P, Bansal S, Kuhad A et al (2020) Naringenin ameliorates diabetic neuropathic pain by modulation of oxidative-nitrosative stress, cytokines and MMP-9 levels. Food Funct 11:4548–4560
Urch C (2004) The pathophysiology of cancer-induced bone pain: current understanding. Palliat Med 18:267–274
Xu M, Ni H, Xu L et al (2019) B14 ameliorates bone cancer pain through downregulating spinal interleukin-1beta via suppressing neuron JAK2/STAT3 pathway. Mol Pain 15:1744806919886498
Yan J, Sun J, Zeng Z (2018) Teniposide ameliorates bone cancer nociception in rats via the P2X7 receptor. Inflammopharmacology 26:395–402
Yang Y, Li H, Li TT et al (2015) Delayed activation of spinal microglia contributes to the maintenance of bone cancer pain in female Wistar rats via P2X7 receptor and IL-18. J Neurosci 35:7950–7963
Yang L, Liu X, Zhang N et al (2020) Flavonoids in resina draconis protect against pulmonary fibrosis via the TGF-β1/NOTCH1 pathway. Mol Cell Toxicol 16:193–201
Yeung YT, Aziz F, Guerrero-Castilla A, Arguelles S (2018) Signaling pathways in inflammation and anti-inflammatory therapies. Curr Pharm Des 24:1449–1484
Zeng W, Jin L, Zhang F et al (2018) Naringenin as a potential immunomodulator in therapeutics. Pharmacol Res 135:122–126
Zhang Y, Cheng H, Li W et al (2019) Highly-expressed P2X7 receptor promotes growth and metastasis of human HOS/MNNG osteosarcoma cells via PI3K/Akt/GSK3beta/beta-catenin and mTOR/HIF1alpha/VEGF signaling. Int J Cancer 145:1068–1082
Zhao M, Li C, Shen F et al (2017) Naringenin ameliorates LPS-induced acute lung injury through its anti-oxidative and anti-inflammatory activity and by inhibition of the PI3K/AKT pathway. Exp Ther Med 14:2228–2234
Zhou J, Xia L, Zhang Y (2019) Naringin inhibits thyroid cancer cell proliferation and induces cell apoptosis through repressing PI3K/AKT pathway. Pathol Res Pract 215:152707
Acknowledgements
This study was supported by the Hunan Provincial Innovation Foundation for Postgraduate (CX2020B633).
Author information
Authors and Affiliations
Contributions
JGS performed the experiments, analyzed the data and writing the manuscript. LL responsible for the experimental design and manuscript revision. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The author Jian-Gang Song declares that he has no conflict of interest and author Lv Liu also declares that she has no conflict of interest.
Ethics approval
The present study was approved by the University Animal Care and Use Committee of Hengyang Center Hospital (Hengyang, China).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Song, JG., Liu, L. Naringenin alleviates bone cancer pain in rats via down-regulating spinal P2X7R /PI3K/AKT signaling: involving suppression in spinal inflammation. Mol. Cell. Toxicol. 17, 475–484 (2021). https://doi.org/10.1007/s13273-021-00156-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13273-021-00156-3