Abstract
A large proportion of human malaria infections is asymptomatic, yet serves as a reservoir that sustains malaria transmission. To achieve malaria elimination, it is important to understand how asymptomatic infections affect malaria transmission among humans. Here we propose a simple mathematical model of malaria transmission with both symptomatic and asymptomatic infections, and investigate the effect of interventions targeting the reservoir population during an early phase of malaria spread under different transmission settings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Malaria is a vector-borne disease that imposes a huge health burden on the world’s most vulnerable populations. To understand malaria transmission dynamics, many mathematical models have been proposed and used in data analysis [1]. A basic model of malaria spread is “Ross model” [2]:
Here \(I_h \left( t \right) \) and \(I_m \left( t \right) \) are the proportions of infected humans and mosquitoes, respectively. Parameters a, b, c, m, r, and \(\mu \) represent the human-biting rate of a single mosquito, the proportion of bites by infectious mosquitoes on susceptible humans producing a patient infection, the proportion of bites by susceptible mosquitoes on infected humans producing a disease vector, the number of female mosquitoes per human host, the rate of human recovery from infection (i.e., \(1/\gamma \) is the average duration of an infection), and the rate of mosquito mortality (i.e., \(1/\mu \) is mosquito life expectancy), respectively [2, 3]. The basic reproduction number is defined as the average number of secondary cases of malaria arising from a single case in a completely susceptible population, and in the Ross model turns out to be \(R_0 =ma^{2}bc/r\mu \). Malaria can spread in a population only if \(R_0 >1\). The Ross model describes the basic features of malaria transmission and has served as a basic theoretical framework for malaria control [1, 4, 5].
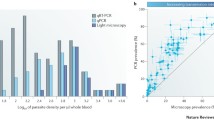
Fighting malaria over the last decade with controlled interventions resulted in a remarkable decline in global malaria morbidity and mortality [6]. However, it remains unclear whether complete eradication of malaria will be achieved by currently available interventions. In low transmission setting, most of the asymptomatic infections are with submicroscopic parasitemia and difficult to detect through routine surveillance (requiring molecular methods) [7]. These infections account for more than 60% of the total [8] and, as such, represent a “human reservoir” for malaria transmission that interferes with eradication efforts [7–9]. It is therefore believed that finding and treating the asymptomatic population is an important way forward. Interestingly, simulation studies so far suggested that targeting asymptomatic infections could reduce malaria transmission [4, 10]. Here, we develop a simple mathematical model of malaria transmission with both symptomatic and asymptomatic infections, and investigate how interventions targeting the reservoir population impact the early phase of malaria spread. Furthermore, we discuss how our simple model will be applied to reported annual malaria cases for extracting quantitative information on malaria spread.
2 Results
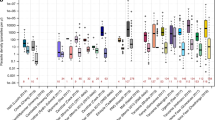
Immunity is an important factor determining whether a malaria patient shows clinical symptoms [7, 8]. For example, in areas of high malaria transmission, people are always exposed to malaria infections, and therefore acquire immunity against the disease. Increased immunity decreases the parasite density in an individual and moderates the severity of symptoms [11]. Interestingly, in high transmission settings, the proportion of asymptomatic malaria infections tends to be above 90% [8, 12]. Even in low transmission areas, it is shown that more than 60% of malaria infections fail to show clinical symptoms [8]. However, some fraction of these asymptomatic patients are malaria gametocyte carriers who are essential for malaria transmission (i.e., infectious) [13], and therefore they act as a human reservoir for the disease [7–9]. Thus, all malaria cases, including asymptomatic infections, should be detected and treated to achieve better control. Using a simple mathematical model, we investigate the effect of human reservoir reduction on an early phase of malaria spread, and identify important factors for an improved effectiveness.
2.1 A mathematical model for malaria spread
Modifying the Ross model [2], we develop a simple mathematical model describing malaria spread as follows:
The human population is divided into five compartments: susceptible (S); exposed (i.e., latent but non-infectious) (E); symptomatic infectious (I); asymptomatic infectious (A); and “reported” as malaria infection and treated (R). Because the birth and death rate are assumed to be same (i.e., d), the total human population remains constant (i.e., \(N\left( t \right) =S\left( t \right) +E\left( t \right) +I\left( t \right) +A\left( t \right) +R\left( t \right) =N)\). We assume that the mean latency period in a human is \(1/\varepsilon \), and thereafter the proportion f develops symptomatic disease, whereas the remainder \(1-f\) is asymptomatic. The mean rate of natural clearance of gametocyte is \(\theta \) for both symptomatic and asymptomatic infections. Even if malaria patients show acute clinical symptoms, symptomatic individuals become asymptomatic at the rate, r (i.e., 1 / r is the mean symptomatic period) because the symptoms sometimes disappear without clearance of the gametocytes. Parameter q is the rate of detection and recovery from clinical malaria by treatment, and \(\eta \) is the relative rate of detection and treatment \((0<\eta <1)\). Because of the treatment, the mean rate of the natural clearance of gametocyte is increased \((1+\varphi )\)-fold for individuals reported as the cases of malaria infection. Furthermore, the female mosquito population is divided into three compartments: susceptible \((V_s )\); exposed \((V_E )\); and infectious \((V_I )\). The mosquitoes die with rate \(\mu \), but the total mosquito population, \(N_V \left( t \right) \), is maintained by the constant birth, g. The mean latent period in a mosquito is \(1/\varepsilon _V \). The force of infection experienced by humans and mosquitoes, respectively, is defined as follows:
Here a, b, and c are the human-biting rate of a mosquito, the proportion of bites by infectious mosquitoes on susceptible humans producing a patient infection, and the proportion of bites by susceptible mosquitoes on infected humans producing a disease vector, respectively. Note that \(a\times N_V \left( t \right) /N\left( t \right) \) represents the biting rate per human host. For convenience, we define \(\beta =ab\) and \(\beta _V =ac\). Our mathematical model (1-2) is a simplified version of a previous model discussed in [5, 14]. All variables and parameters are summarized in Table 1.
2.2 Derivation of the basic reproduction number
The basic reproduction number, i.e., the average number of secondary (human) cases produced by a human primary case in a completely susceptible population, is an important quantity characterizing disease transmission and intervention impact [3]. We derived the basic reproduction number from model (1-2) as follows [15–17]. At the beginning of malaria spread, the equation for exposed human individuals is
because we could assume that the number of susceptible human individuals is approximately equal to the total human population (i.e., \(S\left( t \right) =N\)). Applying the variation of constants formula to the above equation, we have
where, for simplicity, we assume that the infection process starts at \(t=0\). In the above expression, \(\phi _1 \left( s \right) \) denotes the distribution function of waiting time in compartment \(E\left( t \right) \) given by
and, \(*\) denotes the convolution of functions. In a similar manner, if we define the distribution functions of waiting time for other compartments,
then the linearized equations of model (1-2) at the disease-free steady state, \(\left( {N,0,0,0,0,b/\mu ,0,0} \right) \), are rewritten by the following integral equations:
Here, \(N_V^*=b/\mu \) and \(m=N_V^*/N\). Therefore, we arrived at the following renewal equation for compartment, \(E\left( t \right) \):
The kernel of the above renewal equation is given by
From the general theory of the basic reproduction number [16, 17], \(R_0\) for the exposed human individuals is
The disease-free steady state is globally asymptotically stable if \(R_0 <1\), because, in the model (1-2), \(E\left( t \right) \) and \(V_E \left( t \right) \) satisfy inequalities \(E\left( t \right) \le \beta \left( {V_I *\phi _1} \right) \left( t \right) \) and \(V_E \left( t \right) \le m\beta _V \left\{ {\phi _2 *\left( {I+A} \right) } \right\} \left( t \right) \) [17]. Therefore, \(R_0 <1\) is a sufficient condition to eradicate the disease.
2.3 Impact of control intervention targeting asymptomatic infection
It is difficult to detect malaria infection without any clinical symptoms or molecular methods [7–9]. Accordingly, the relative rate of detection and treatment is usually close to zero in current malaria case management (i.e., \(\eta =0\)). To investigate how malaria control interventions targeting the reservoir population impact the early phase of malaria spread, we analyzed the sensitivity of the basic reproduction number, \(R_0 \), to \(0<\eta <1\). Because \(R_0\) is a function of parameter \(\eta \), we redefine the basic reproduction number as \(R_0 \left( \eta \right) \), and consider the effect of intervention on \(R_0\) as follows:
where we ignore the natural death rate (i.e., \(d=0)\) because it is too small compared with other parameters. Interestingly, the sensitivity of \(R_0\) to \(\eta \) depends only on four parameters: \(\theta , r, q\), and f. Here we fixed \(\theta =1/180, r=1/180\), and \(q=1/21\) [4, 10, 14]. In Fig.1, solid and dashed curves represent the sensitivity in a high \((1-f=55\)%) and a low \((1-f=5\)%) transmission setting, respectively. Although the transmission setting is usually defined using the entomological inoculation rate (EIR) or the transmission intensity [4, 18], as reviewed in [7, 8], there is a strong and positive correlation between the transmission intensity and f (i.e., the proportion of asymptomatic population with malaria parasitemia). Thus, we simply assumed that the difference in f corresponds to that in the transmission settings. When the efficacy of the intervention is relatively low (up to \(\eta =0.4)\), the effect, \(1-R_0 \left( \eta \right) /R_0 \left( 0 \right) \), dramatically increases in both settings. As the efficacy of the intervention approaches 100% (i.e., the parameter \(\eta \) approaches 1), the effect of intervention saturates. Interestingly, the saturated value in the high transmission setting is 83.5% which is much higher than 54.5% in the low transmission setting, meaning that the intervention in the former setting is more efficient (the solid curve is always above the dashed curve in Fig.1). In other words, if we could maintain the control intervention efficacy close to 100%, the control intervention would be effective in reducing the basic reproduction number—the control might block a malaria spread with the basic reproduction number less than 8.77 and 6.49 in the high and the low setting, respectively. In contrast, if the basic reproduction number is above 8.77 and 6.49 in the high and the low setting, respectively, the control intervention alone could not prevent malaria spread. In fact, it is reported that the basic reproduction number in the high malaria transmission areas sometimes exceeds 100 [19]. This high number implies that the impact of the control intervention applied to the human reservoir is limited in the high transmission setting, which is consistent with previous prediction by simulation studies in Ref. [4]. For malaria control, it is important to estimate the basic reproduction number and to execute multi-control strategies depending on a transmission setting [4, 8, 20].
Impact of control intervention targeting asymptomatic infection on the basic reproduction number: the sensitivity of the basic reproduction number to \(0<\eta <1\) in the high \((1-f=45\)%) and the low \((1-f=95\)%) transmission setting (i.e., \(1-R_0 \left( \eta \right) /R_0 \left( 0 \right) )\) is shown using solid and dashed curves, respectively. Here, the parameters are fixed at \(\theta =1/180, r=1/180\), and \(q=1/21\)
2.4 Relation between the basic reproduction number and the Malthusian parameter
In areas of high seasonal transmission, it is believed that asymptomatic patients persist over the course of dry season and reseed transmission when mosquito populations increase along with wetter conditions [8, 20, 21]. Therefore, malaria outbreak occurs every year during the rainy season. Quantifying the annual basic reproduction number, \(R_0 \), during an early phase of malaria spread is important to evaluate whether control interventions mitigate malaria spread [1, 3, 16]. Here we explained that our simple model will be applied to annual malaria case reports to extract quantitative information on malaria spread. Note that many parameter values in the mathematical model are unknown, especially those appearing in the force of infection.
The Malthusian parameter for malaria, i.e., the speed of malaria spread, is the dominant real root of the Euler–Lotka equation [22]:
where \(\hat{\varPhi }\left( *\right) \) denotes the Laplace transformation of function \(\varPhi \left( *\right) \). Because the Laplace transformation turns convolution into multiplication, the Euler–Lotka equation is rewritten as
In addition, if we define the mean waiting time in each compartment as
then each Laplace transformation is explicitly calculated as follows:
The dominant real root of the above sixth degree equation in \(\lambda \) corresponds to the Malthusian parameter. Thus, from the Euler–Lotka equation, we arrive to the following relation:
Interestingly, the basic reproduction number is expressed as a function of the Malthusian parameter. Although in most of the countries where malaria is endemic, a relatively large fraction of the population (both human and mosquito) is already infectious at the start of a malaria season, thus driving yearly outbreaks, all information on population having an immunity against malaria is included in the initial slope of malaria cases. Because the Malthusian parameter is usually estimated from the growth rate of the reported malaria cases (i.e., the time evolution of \(qI\left( t \right) +\eta qA\left( t \right) \) at the beginning of malaria spread), it is possible for us to estimate the basic reproduction number just by knowing the mean waiting times \(({\Delta }_1 , {\Delta }_2 , {\Delta }_3 , {\Delta }_4 \), and \({\Delta }_6 )\), and parameters f and \(\gamma \), all of which are directly observed in clinical patients.
3 Discussion
To derive analytical expressions for the basic reproduction number \((R_0 )\) and the effect of intervention \((1-R_0 \left( \eta \right) /R_0 \left( 0 \right) )\), we used a simple model (1-2), inspired by a previously proposed model in Refs. [5, 14]. By analyzing the sensitivity of \(R_0\) to \(0<\eta <1\), we showed that, depending on the transmission setting as defined by EIR [1, 7, 8], the effect of malaria control interventions targeting the reservoir population is different (see the solid and dashed curves in Fig. 1). As mentioned above, it is considered that a host’s immune response to malaria infection plays an important role [11] (here, the parameter f is assumed to be determined by the host’s immunity). In some areas, in fact, it is reported that high gametocyte carriage amongst asymptomatic patients may be the cause of a sustained low level transmission despite strict enforcement of malaria control measures. Thus, asymptomatic infection may contribute to malaria spread. Furthermore, the dynamics of the gametocyte density in patients is a critical factor in determining malaria transmission [7–9, 13]. Previous transmission experiments showed a positive relationship between gametocyte density and the prevalence of infection in mosquitoes [8, 23]. The probability of mosquito infection depends on gametocyte density [7, 8]. Although no clear relationship between asymptomatic infection and gametocyte density has been established, the effect that biting symptomatic infected individuals has on the probability of a susceptible mosquito becoming infected might be different from that of biting asymptomatic infected individuals, because the density of gametocyte is likely different depending on the host’s immunity level. Taking into account the gametocyte density in the force of infection using term \(\beta _V \left( {I\left( t \right) +\sigma A\left( t \right) } \right) /N\left( t \right) \), where \(\sigma \) is a scaling parameter, and evaluating the malaria control interventions that target the reservoir population will be the focus of a future work.
References
Mandal, S., Sarkar, R.R., Sinha, S.: Mathematical models of malaria—a review. Malar. J. 10, 202 (2011). doi:10.1186/1475-2875-10-202
Ross, R.: Some a priori pathometric equations. Br. Med. J. 1(2830), 546 (1915)
Anderson, R.M., May, R.M., Anderson, B.: Infectious Diseases of Humans: Dynamics and Control. Wiley Online Library (1992)
Griffin, J.T., Hollingsworth, T.D., Okell, L.C., Churcher, T.S., White, M., Hinsley, W., et al.: Reducing Plasmodium falciparum malaria transmission in Africa: a model-based evaluation of intervention strategies. PLoS Med. 7(8), e1000324 (2010). doi:10.1371/journal.pmed.1000324
Mandal, S., Sinha, S., Sarkar, R.R.: A realistic host-vector transmission model for describing malaria prevalence pattern. Bull. Math. Biol. 75(12), 2499–2528 (2013). doi:10.1007/s11538-013-9905-7
World Health Organization: World Malaria Report 2015 (2015). http://www.apps.who.int/iris/bitstream/10665/200018/1/9789241565158_eng.pdf
Lin, J.T., Saunders, D.L., Meshnick, S.R.: The role of submicroscopic parasitemia in malaria transmission: what is the evidence? Trends Parasitol. 30(4), 183–190 (2014). doi:10.1016/j.pt.2014.02.004
Lindblade, K.A., Steinhardt, L., Samuels, A., Kachur, S.P., Slutsker, L.: The silent threat: asymptomatic parasitemia and malaria transmission. Expert Rev. Anti-Infect. Ther. 11(6), 623–639 (2013). doi:10.1586/eri.13.45
Laishram, D.D., Sutton, P.L., Nanda, N., Sharma, V.L., Sobti, R.C., Carlton, J.M., et al.: The complexities of malaria disease manifestations with a focus on asymptomatic malaria. Malar. J. 11, 29 (2012). doi:10.1186/1475-2875-11-29
Okell, L.C., Griffin, J.T., Kleinschmidt, I., Hollingsworth, T.D., Churcher, T.S., White, M.J., et al.: The potential contribution of mass treatment to the control of Plasmodium falciparum malaria. PLoS One 6(5), e20179 (2011). doi:10.1371/journal.pone.0020179
Crompton, P.D., Moebius, J., Portugal, S., Waisberg, M., Hart, G., Garver, L.S., et al.: Malaria immunity in man and mosquito: insights into unsolved mysteries of a deadly infectious disease. Annu. Rev. Immunol. 32, 157–187 (2014). doi:10.1146/annurev-immunol-032713-120220
Minakawa, N., Kongere, J.O., Dida, G.O., Ikeda, E., Hu, J., Minagawa, K., et al.: Sleeping on the floor decreases insecticide treated bed net use and increases risk of malaria in children under 5 years of age in Mbita District, Kenya. Parasitology 142(12), 1516–1522 (2015). doi:10.1017/s0031182015000955
Bousema, T., Drakeley, C.: Epidemiology and infectivity of Plasmodium falciparum and Plasmodium vivax gametocytes in relation to malaria control and elimination. Clin. Microbiol. Rev. 24(2), 377–410 (2011). doi:10.1128/cmr.00051-10
Filipe, J.A., Riley, E.M., Drakeley, C.J., Sutherland, C.J., Ghani, A.C.: Determination of the processes driving the acquisition of immunity to malaria using a mathematical transmission model. PLoS Comput. Biol. 3(12), e255 (2007). doi:10.1371/journal.pcbi.0030255
Iwami, S., Takeuchi, J.S., Nakaoka, S., Mammano, F., Clavel, F., Inaba, H., et al.: Cell-to-cell infection by HIV contributes over half of virus infection. Elife 4, e08150 (2015). doi:10.7554/eLife.08150
Inaba, H.: On a new perspective of the basic reproduction number in heterogeneous environments. J. Math. Biol. 65(2), 309–348 (2012). doi:10.1007/s00285-011-0463-z
Diekmann, O., Heesterbeek, H., Britton, T.: Mathematical Tools for Understanding Infectious Disease Dynamics. Princeton University Press, Princeton (2012)
Pothin, E., Ferguson, N.M., Drakeley, C.J., Ghani, A.C.: Estimating malaria transmission intensity from Plasmodium falciparum serological data using antibody density models. Malar. J. 15, 79 (2016). doi:10.1186/s12936-016-1121-0
Smith, D.L., McKenzie, F.E., Snow, R.W., Hay, S.I.: Revisiting the basic reproductive number for malaria and its implications for malaria control. PLoS Biol. 5(3), e42 (2007). doi:10.1371/journal.pbio.0050042
Griffin, J.T.: The interaction between seasonality and pulsed interventions against malaria in their effects on the reproduction number. PLoS Comput. Biol. 11(1), e1004057 (2015). doi:10.1371/journal.pcbi.1004057
Babiker, H.A., Abdel-Muhsin, A.M., Ranford-Cartwright, L.C., Satti, G., Walliker, D.: Characteristics of Plasmodium falciparum parasites that survive the lengthy dry season in eastern Sudan where malaria transmission is markedly seasonal. Am J Trop. Med. Hyg. 59(4), 582–590 (1998)
Wallinga, J., Lipsitch, M.: How generation intervals shape the relationship between growth rates and reproductive numbers. Proc. Biol. Sci. 274(1609), 599–604 (2007)
Lacroix, R., Mukabana, W.R., Gouagna, L.C., Koella, J.C.: Malaria infection increases attractiveness of humans to mosquitoes. PLoS Biol. 3(9), e298 (2005). doi:10.1371/journal.pbio.0030298
Acknowledgments
This research was carried out for the iDEWS project supported in part by SATREPS Program of JICA/AMED in Japan and ACCESS (NRF/DST) in South Africa (to T.F., M.J., A.T., N.M. and S.I.); the Japan Science and Technology Agency (JST) Program to Disseminate Tenure Tracking System (to M.J.); JST PRESTO program (to S.I.); JST RISTEX program (to S.I.); JST CREST program (to H.I. and S.I.); The Japan Society for the Promotion of Science (JSPS) KAKENHI Grant Numbers 15KT0107, 26287025, 16H04845 and 16K13777 (to S.I.); and The Japan Agency for Medical Research and Development, AMED (to S.I.).
Author information
Authors and Affiliations
Corresponding author
Additional information
Dedicated to the 75th birthday of Professor Masayasu Mimura.
About this article
Cite this article
Funo, T., Inaba, H., Jusup, M. et al. Impact of asymptomatic infections on the early spread of malaria. Japan J. Indust. Appl. Math. 33, 671–681 (2016). https://doi.org/10.1007/s13160-016-0228-6
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13160-016-0228-6