Abstract
Hepatobiliary scintigraphy has been widely used for the differential diagnosis of neonatal cholestasis. Relatively good hepatic uptake with no evidence of excretion into the bowel for up to 24 h is a representative finding of biliary atresia. Hepatobiliary scintigraphy has very high sensitivity and moderate specificity. Here, we report a false-positive case of hepatobiliary scintigraphy in a child with a choledochal cyst, which mimicked biliary atresia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neonatal cholestasis is a condition in which bile components accumulate in the liver by a defect of the intrahepatic production or the transmembrane transport of bile, or a mechanical obstruction [1]. Biliary atresia is the primary cause of neonatal cholestasis, and prompt diagnosis is essential. Hepatobiliary scintigraphy (HBS) has been widely accepted for the investigation of neonatal cholestasis. HBS has a very high sensitivity for biliary atresia, while the specificity is moderate [2]. False positives are bile plug syndrome and severe neonatal hepatitis [2, 3]. Therefore, the non-visualization of the gallbladder is not a specific finding. Readers should be aware of the false-positive findings of HBS to prevent misinterpretation.
Here, we report a case of HBS in a child with a choledochal cyst, which mimicked biliary atresia.
Case report
A 2-month-old child was referred for evaluation of jaundice. Laboratory test results were total bilirubin 13.0 mg/dL, direct bilirubin 10.7 mg/dL, alkaline phosphatase (ALP) 841 IU/L, alanine aminotransferase (ALT) 456 IU/L, and aspartate aminotransferase (AST) 653 IU/L. The child underwent magnetic resonance imaging (MRI) and ultrasonography (USG). MRI showed a 1.8-cm-sized choledochal cyst in the hepatic hilum and a 1.7-cm-sized atretic gallbladder (Fig. 1a). Additionally, USG suggested the presence of biliary atresia based on the triangular cord sign (Fig. 1b). No stone or sludge was observed. Kidneys were normal. Laboratory results and the presence of a choledochal cyst with biliary atresia on radiography excluded the possibility of other structural obstructions and non-structural diseases [1].
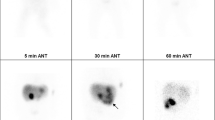
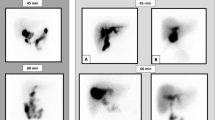
Two days later, hepatobiliary scintigraphy with Tc-99 m diisopropyl iminodiacetic acid (DISIDA) was performed to evaluate neonatal jaundice. Hepatic extraction decreased slightly, and parenchymal transit was delayed. Photon defect was observed at the hepatic hilum due to the choledochal cyst. Gallbladder and intestine were not visualized for up to 24 h after the injection (Fig. 2). These findings were suggestive of biliary atresia.
Eleven days after hepatobiliary scintigraphy, surgery was performed to confirm the diagnosis and fix the cause of cholestasis. A cystic lesion in the hepatic hilum was identified, and an intraoperative cholangiogram revealed patent intrahepatic bile ducts (Fig. 3), thus excluding biliary atresia. The choledochal cyst was surgically removed (Fig. 4a and b), and a liver biopsy was concomitantly done (Fig. 4c). Histology revealed the presence of hepatocanalicular cholestasis and giant cell transformation of hepatocytes, which was consistent with neonatal hepatitis. Laboratory results about 1 month after cystectomy were total bilirubin 1.3 mg/dL, direct bilirubin 1.2 mg/dL, ALP 298 IU/L, ALT 15 IU/L, and AST 117 IU/L.
Discussion
Choledochal cysts are congenital cystic dilatations of bile ducts. The incidence of choledochal cysts is 1 in 100,000–150,000 in the Western population and 1 in 1000 in the Asian population. It has a female predominance, reported as 4:1 to 3:1 [4]. Choledochal cysts are classified into five subtypes according to the location of cystic dilatation, as suggested by Todani [5]. Type I is a cystic dilatation of the extrahepatic bile duct, and they are the most common type of choledochal cysts.
Abdominal pain, jaundice, and abdominal mass are common symptoms in most child cases. Surgical intervention is the treatment of choice, and it should be based on cyst type and associated hepatobiliary pathology [6]. The typical surgical procedure involves cyst excision with Roux-en-Y biloenteric drainage [4].
USG and MRI are the main diagnostic tools for evaluating the hepatobiliary system in neonates. In this case, USG revealed the presence of biliary atresia based on the triangular cord sign as well as a choledochal cyst in the hepatic hilum. Triangular cord sign is a triangular or tubular echogenic density seen immediately cranial to the portal vein bifurcation, and it is a useful marker for biliary atresia [7].
HBS is also a useful imaging tool for evaluating neonatal cholestasis. On HBS, choledochal cysts are presented as dilated cysts communicating functionally with the bile duct system [8]. A cystic mass with dilated bile ducts on USG combined with the radiotracer accumulation on scintigraphy is diagnostic of choledochal cyst.
Cystic biliary atresia, an uncommon variant of biliary atresia, has similar clinical and sonographic features to a choledochal cyst; thus, it should be considered as part of the differential diagnosis [9]. Sonographic findings of the present case were suggestive of cystic biliary atresia rather than choledochal cyst [10, 11]. On the contrary, postoperative histopathology and laboratory tests confirmed the diagnosis of choledochal cyst with neonatal hepatitis.
Non-visualization of gallbladder and intestines on HBS is not always conclusive. This can also be seen in bile plug syndrome, Alagille syndrome, and cystic fibrosis [3]. Physical examination, USG, and liver biopsy are used to discriminate biliary atresia from other causes of neonatal cholestasis. Meanwhile, hepatic extraction rate on HBS is helpful in differentiating between biliary atresia and severe hepatitis.
In this case, there was no radiotracer accumulation in the cystic mass until 24 h after the injection, which is atypical of choledochal cyst. Also, choledochal cyst and biliary atresia may have similar clinical symptoms and signs, or they even coexist [12, 13]. Therefore, choledochal cysts should be included in the differential diagnosis when there was no radiotracer accumulation in the gallbladder and intestines on scintigraphy.
References
Gotze T, Blessing H, Grillhosl C, Gerner P, Hoerning A. Neonatal cholestasis - differential diagnoses, current diagnostic procedures, and treatment. Front Pediatr. 2015;3:43.
Anand SS, Handa RK, Singh J, Sinha I. Hepato-biliary scintigraphy in diagnosis of biliary atresia. Med J Armed Forces India. 2006;62:20–1.
Howman-Giles R, Uren R, Bernard E, Dorney S. Hepatobiliary scintigraphy in infancy. J Nucl Med. 1998;39:311–9.
Bhavsar MS, Vora HB, Giriyappa VH. Choledochal cysts : a review of literature. Saudi J Gastroenterol. 2012;18:230–6.
Todani T, Watanabe Y, Narusue M, Tabuchi K, Okajima K. Congenital bile duct cysts: classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg. 1977;134:263–9.
Khandelwal C, Anand U, Kumar B, Priyadarshi RN. Diagnosis and management of choledochal cysts. Indian J Surg. 2012;74:401–6.
Tan Kendrick AP, Phua KB, Ooi BC, Subramaniam R, Tan CE, Goh AS. Making the diagnosis of biliary atresia using the triangular cord sign and gallbladder length. Pediatr Radiol. 2000;30:69–73.
Kirks DR, Coleman RE, Filston HC, Rosenberg ER, Merten DF. An imaging approach to persistent neonatal jaundice. AJR Am J Roentgenol. 1984;142:461–5.
Schooler GR, Mavis A. Cystic biliary atresia: a distinct clinical entity that may mimic choledochal cyst. Radiol Case Rep. 2018;13:415–8.
Zhou LY, Guan BY, Li L, Xu ZF, Dai CP, Wang W, et al. Objective differential characteristics of cystic biliary atresia and choledochal cysts in neonates and young infants: sonographic findings. J Ultrasound Med. 2012;31:833–41.
Kim WS, Kim IO, Yeon KM, Park KW, Seo JK, Kim CJ. Choledochal cyst with or without biliary atresia in neonates and young infants: US differentiation. Radiology. 1998;209:465–9.
Fatahi N, Mohammadipoor A, Malekmarzban A. Extra hepatic biliary atresia associated with choledochal cyst: a challenging neonatal obstructive jaundice. J Neonatal Surg. 2014;3:20.
Torrisi JM, Haller JO, Velcek FT. Choledochal cyst and biliary atresia in the neonate: imaging findings in five cases. AJR Am J Roentgenol. 1990;155:1273–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Il-Hyun Kim, Young-Sil An, Su Jin Lee, Jeong Hong, and Joon-Kee Yoon declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Informed Consent
The institutional review board of our institute approved this study, and the requirement to obtain informed consent was waived.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, IH., An, YS., Lee, S.J. et al. Hilar Choledochal Cyst Mimicking Biliary Atresia on Hepatobiliary Scintigraphy: a Case Report. Nucl Med Mol Imaging 55, 96–99 (2021). https://doi.org/10.1007/s13139-021-00688-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-021-00688-5