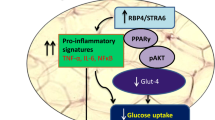
Abstract
S-resistin is a non-secretable resistin spliced variant, which is expressed mainly in the white adipose tissue from Wistar rats. Previous results confirmed that 3T3-L1 cells expressing s-resistin (3T3-L1-s-res) showed an inflammatory response and exhibited a decrease in glucose transport, both basal and insulin-stimulated. Here we present evidences demonstrating for the first time that s-resistin, like resistin, blocks insulin signalling pathway by inhibiting insulin receptor, insulin receptor substrate 1, protein kinase B/Akt and the mammalian target of rapamycin phosphorylation, and increasing the suppressor of cytokine signalling 3 levels being the later probably due to augmented of leptin expression. Thus, our data suggest that s-resistin could act by a still unknown intracrine pathway as an intracellular sensor, regulating the adipocyte insulin sensitivity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The control of body weight, glucose, and lipid homeostasis is exerted by a complex network composed by peripheral tissues, neuronal circuits of the central nervous system (CNS), as well as by several hormones such as leptin, insulin, or resistin [32]. The adipose tissue secretes cytokines and growth factors, named adipokines, which act in a paracrine-endocrine way on peripheral tissues modulating their response to different nutritional factors. Furthermore, adipocytes express receptors for most of these factors, constituting by itself autocrine targets for these signals [27].
Since its characterization in rodents, the adipokine resistin has been implicated in insulin resistance, obesity, and type 2 diabetes development [13, 33]. Initial results showed that in vivo administration of recombinant resistin impairs glucose tolerance and insulin action in normal mice, whereas anti-resistin antibody administration enhances insulin sensitivity of insulin-resistant and obese mice [33]. Moreover, according to Banerjee et al. [2], mice lacking resistin display low blood glucose levels after fasting, indicating that resistin acts on peripheral tissues, disrupting insulin response at different levels. Thus, in liver, resistin promotes phosphoenolpyruvate carboxykinase (PEPCK) activity, increasing endogenous glucose production [2], whereas in adipose tissue it decreases fatty acid oxidation, increasing the levels of free fatty acid in plasma [30]. Both effects contribute to the development of insulin resistance.
In rodents, resistin has also been involved in the regulation of adipocyte differentiation through a feedback mechanism [13]. Several studies showed that overexpression of resistin in 3T3-L1 fibroblast increased the expression and secretion of proinflammatory cytokines such as tumor necrosis factor alpha (TNFα) and interleukin 6 (IL-6) and decreased the insulin stimulated glucose uptake. These results suggest that an inflammatory pathway might mediate resistin effects impairing insulin action and adipogenesis [8, 10]. Although the resistin receptor has not been identified yet, it was described that some mouse receptors, as an isoform of decorin or the tyrosine kinase-like orphan receptor (ROR) 1, could act as functional resistin receptors and therefore, mediate some resistin functions such glucose uptake and adipogenesis [5, 29].
In Wistar rats, we have identified a novel isoform of resistin, named s-resistin (Short-resistin), which is expressed mainly in the white adipose tissue. This isoform is generated by alternative splicing from rat resistin gene [6]. S-resistin lacks the secretion signal peptide and, in transfected cells, shows a predominantly nuclear location. Thus, the splicing machinery generates a non-secretable protein that could act as an intracrine regulator of gene expression. Interestingly, resistin and s-resistin expression is differentially regulated by fat depot, aging, or nutritional status [7]. These data point out that alternative splicing plays a role in this regulation.
Previous studies with 3T3-L1 adipocytes stably expressing resistin and s-resistin demostrated that both isoforms modified in a different way the expression pattern of key pro-adipogenic transcription factors. Likewise, both isoforms impair at different degrees the insulin-stimulated glucose transport, and promote IL-6 and plasminogen activity inhibitor type 1 (PAI-1) secretion, but only s-resistin increased the TNFα expression and secretion in early and intermediate stages of adipocyte differentiation. These data suggest that the s-resistin variant carries out additional functions in insulin response and adipocyte differentiation [8].
Besides, several studies indicated that resistin interferes in different stages on the intracellular insulin signalling pathway. On the one hand, resistin directly influences insulin signalling increasing the suppressor of cytokine signalling 3 (SOCS-3) levels in 3T3-L1 adipocytes, and thus, inhibiting the ability of the insulin receptor (IR) to recruit and activate the insulin receptor subtrate-1 (IRS-1) [34]. In addition, resistin decreased the activated state of AMP-activated kinase (AMPK), which is involved in glucose homeostasis in liver, skeletal muscle, and white adipose tissue [21, 30, 34]. However, at the moment, the effect of s-resistin on intracellular insulin signalling pathway has not been studied. Since s-resistin is an intracellular protein, it is possible that some of its effects on insulin action could be different from those described for the long resistin isoform.
In an attempt to investigate the effect of s-resistin on the intracellular insulin pathway, we compared the insulin response of adipocytes stably expressing resistin or s-resistin. Our results indicate that s-resistin impairs insulin response by decreasing IRβ, IRS-1, and S-473-Akt/protein kinase B phosphorylation and glucose transporter 4 (GLUT4) expression levels. Also, the changes in the expression pattern of transcription factors involved in lipid metabolism as sterol regulatory element-binding protein 1c (SREBP-1c) and forkhead box subfamily O1a (FoxO1a), adipogenesis as mammalian target of rapamycim (mTOR) and inflammation (TNFα and IL-6) in adipocytes expressing s-resistin, indicate that this isoform increases the inflammatory state and promotes adipocyte insulin and leptin resistance.
Materials and methods
Cell lines and cell culture of 3T3-L1 cells
Murine 3T3-L1 pre-adipocytes purchased from American Type Culture Collection, ATCC (ATTCC CL-173) was used as control and transduced cell lines 3T3-L1-res (resistin) and 3T3-L1-s-res (s-resistin) were previously obtained in our laboratory [8].
Murine 3T3-L1 pre-adipocytes (purchased from American Type Culture Collection, ATCC) and transduced cell lines were grown in Dulbecco’s modified Eagle’s medium (DMEM) containing 10 % fetal bovine serum (FBS) (Gibco BRL) and 100 U/ml penicillin (Gibco) and 100 mg/ml streptomycin (Gibco) at 37 °C in a 5 % CO2 atmosphere.
Differentiation stimulation protocol
3T3-L1 fibroblast or transduced cell lines were grown and differentiated into adipocytes in p100 culture dishes, as described previously [9]. Briefly, cells were grown as described above and 2 days after full confluence (day 0), were differentiated by incubation during 2 days in DMEM containing 25 mM glucose, 0.8 mM isobutylmethylxanthine (IBMX, Sigma), 1 μM dexamethasone (DEX, Sigma), 174 nM insulin (Sigma), and 10 % FBS and then for 2 days in DMEM containing 25 mM glucose, 174 nM insulin, and 10 % FBS. Next, cells were maintained (14 days) in the same medium without insulin until use.
Insulin incubations
Fourteen days after initiation of differentiation, cells were incubated in DMEM without FBS during 8 h and then, they were incubated at different times with 100 nM insulin [8]. 3T3-L1 fibroblast or transduced cell lines were grown in p60 culture dishes. The changes in the proteins of the insulin signalling pathway were analyzed at 5, 10, 15, and 30 min in the presence and absence of insulin, whereas 4 h was chosen to note the alterations in mRNA levels.
RNA isolation and semi-quantitative RT-PCR analysis
Total RNA from 3T3-L1 cells and 3T3-L1 stably transfected cell lines was isolated using RNA-Easy Mini Kit (Qiagen, Hilden, Germany) following the manufacturer’s instructions. Complementary DNA (cDNA) was synthesized from 1 μg of DNase-treated RNA [25].
Primers
All the primers used in real time q-PCR were supplied by Bonsai Technologies: mTOR (sense primer, 5′-CTCTCTGACCCAGTTCGTCC-3′; antisense primer 5′-AGTCTGGCTAACCACGTGGG-3′); SREBP 1c (sense primer, 5′-CTCATCAACAACCAAGACAGT-3′; antisense primer 5′-GTGCAGGTGTCACCTTGGGT-3′); SOCS-3 (sense primer, 5′-GCGGGCACCTTTCTTATCC- 3′; antisense primer 5′-TCCCCGACTGGGTCTTGAC- 3′); leptin (sense primer 5′-CACCCCATTCTGAGTTTGTCC- 3′; antisense primer 5′-ACGCCATCCAGGCTCTC-3′); FoxO1a (sense primer 5′-CAATCTGTCCCTTCACAGCA-3′; antisense primer 5′-ACTGTTGTTGTCCATGGACG-3′), and 18S rRNA (sense primer 5′-CGGCTACCACATCCAAGGAA-3′; antisense primer 5′-GCTGGAATTACCGCGGCT-3′).
Real time q-PCR analysis
Real-time quantitative PCR (q-PCR) was performed by using ABI PRISM 7500 Fast Sequence Detection System instrument and software (Applied Biosystem, Foster City, CA). Relative quantification of target cDNA in each sample was performed from 10 ng of cDNA in TaqMan One-Step real-time PCR Master Mix and using Pre-Developed TaqMan Assay Reagents (PE Applied Biosystem) for: GLUT4 (Mm00436615_m1), TNFα (Mm00443258_m1), resistin (Mm00445641_m1), IL-6 (Mm00446190_m1), and 18S rRNA (Hs99999901_s1) with VIC as real time reporter was used as control to normalize gene expression. Furthermore, relative quantification of target cDNA in each sample was performed from 10 ng of cDNA in SYBR-Green One-Step real-time PCR Master Mix with the primers described previously. The ΔΔCT method was used to calculate the relative differences between experimental conditions and control groups as fold change in gene expression [18].
Protein isolation and western blot analysis
Cell extracts were obtained following cell lysis in a buffer containing 10 mM Tris pH = 8; 120 mM NaCl, Triton X-100, and 1 mM EDTA. A protease inhibitor mixture (Roche) was added before extraction. Protein concentrations were determined by the method of Bradford in accordance with the manufacturer’s instructions (BioRad). The lysates were fractionated on a SDS-PAGE gel and blotted for 2 h at 90 V. Forty milligrams of protein were loaded per gel. Western Blot analysis was performed according to standard protocols.
The following primary antibodies were used in this study: β-actin (Sigma, 1:1000 dilution), SOCS-3 (Santa Cruz, 1:500), pAkt S-473 (Cell Signalling, 1:500), pAkt T-308 (Cell Signalling 1:500), Akt (Cell Signaling, 1:500), pFoxO1a S-319 (Abcam 1:500), FoxO1a (Abcam 1:400), pIRβ Y-1146 (Sigma, 1:500), IRβ (Santa Cruz, 1:500), pIRS-1 Y-632(SAB Signalling, 1:500), IRS-1 (Cell Signalling, 1:500), p mTOR S-2448(Abcam, 1:500), and mTOR (Abcam, 1:1000). Goat anti-rabbit IgG-HRP and rabbit anti-Mouse IgG-HRP (Sigma) were used as secondary antibodies, and ECL (Amersham) reagent was used for developing. Different times were used for each protein according to the maximum activity observed. Bands were quantified by scanning densitometry with exposure in the linear range using a Gel DocTM EZ Imager system (Bio-Rad) with the Image Lab software system (version 3.0.1, Bio-Rad Laboratories), and normalized to that of β-actin. The densitometric relative levels of phosphorylated proteins were normalized to the corresponding amount of total protein mass in the same sample.
Statistical analysis
Statistical analysis was performed using one-way ANOVA (GraphPad Prism 5.03 software, GraphPad Software, Inc., San Diego, CA). When the main effect was significant, the Bonferroni post hoc test was applied to determine individual differences between means. P values less than 0.05 were considered statistically significant.
Results
S-resistin decreases insulin action in 3T3-L1 cells
To establish the time for insulin maximal activation of the different proteins involved in the early steps on the insulin signaling pathway, we analyzed the phosphorylation of the IR, IRS-1, Akt, FoxO1a, and mTOR as well as the SOCS-3 protein levels, in response to insulin stimulation at different period of time in 3T3-L1 control cells (Fig. 1). Once established, the time for insulin maximal activation of each protein in control cells, we studied the protein levels and the insulin-stimulated phosphorylation of different intermediates of the insulin signalling pathway in cells stably expressing s-resistin (3T3-L1-s-res) and resistin (3T3-L1-res), to understand the possible molecular alterations exerted by s-resistin on insulin action in these cells.
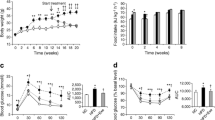
Time-course phosphorylation of different intermediates of the insulin signalling pathway in response to insulin in 3T3-L1 control cells. Control 3T3-L1 cells were treated for 5, 10, 15, and 30 min with 100 nM insulin as described in materials and methods section. The arrows indicate the determinate time for the maximal activation of each protein. a–e Phosphorylation levels, f Total levels. Values are the means ± SEM; n = 3 independent experiments per time tested. *p ≤ 0.01, **p ≤ 0.05
First, we analyzed basal and insulin-stimulated tyrosine phosphorylation of the early proteins involved on the insulin signalling pathway like IR and IRS-1. Thus, 3T3-L1-s-res cells show reduced levels (30 %) of IR phosphorylation upon insulin treatment (Fig. 2a). This decrease was more pronounced in cells stably expressing resistin (3T3-L1-res), where IR phosphorylation dropped to the half of the values observed in insulin stimulated control cells. Also, we found that both cell types had diminished IRS-1 phosphorylation compared to 3T3-L1 control cells (Fig. 2b). In this case, s-resistin has a more significant effect, inducing a 70 % decrease in IRS-1 phosphorylation compared to the 40 % caused by resistin. These results confirm that s-resistin, like resistin, blocks initial steps in the pathway of insulin signalling in 3T3-L1 adipocytes.
Effect of resistin and s-resistin on the activity of IR and IRS-1 in 3T3-L1 cells stimulated with insulin. Control 3T3-L1 cells, as well as cells stably expressing resistin (3T3-L1-res) and the short resistin isoform (3T3-L1-s-res) were treated for 5 min (for IR) or 15 min (for IRS-1) with 100 nM insulin. Representative western blots show total (T IRβ, T IRS-1) and phosphorylated (P Y1146-IRβ, P Y632-IRS-1) levels of IR (a) and IRS-1 (b). Densitometry analysis of the degree of phosphorylation of IRβ (c) and IRS-1 (d) upon stimulation with insulin is presented. Values are the means ± SEM; n = 3 independent experiments per group of cells. Values that do not share the same superscript letter are significantly different (p ≤ 0.05)
S-resistin decreases S473-Akt phosphorylation and mTOR activity but increases FoxO1a phosphorylation
We next studied further alterations exerted by s-resistin on the insulin signalling pathway down-stream from IR and IRS-1. Specifically, we focused our attention on the phosphorylation and subsequent activation of Akt and their target mTOR. Western blot analysis demonstrated that both resistin isoforms impaired insulin-stimulated S473-Akt phosphorylation in 3T3-L1 cells, although the inhibition of resistin was more pronounced (75 % for resistin and 50 % for s-resistin, vs control, Fig. 3b). However, resistin isoforms diverged in their effects on T308-Akt phosphorylation in insulin-stimulated cells. While resistin inhibited by a 40 % T308-Akt phosphorylation, s-resistin had no effect (Fig. 3c).
Effect of resistin and s-resistin on the activity of Akt in 3T3-L1 cells stimulated with insulin. Control 3T3-L1 cells, as well as cells stably expressing resistin (3T3-L1-res) and the short resistin isoform (3T3-L1-s-res) were treated for 15 min with 100 nM insulin. Representative western blots (a) show total (T Akt) and phosphorylated S473-Akt (P S473-Akt), T308-Akt (P T308-Akt) levels of Akt. Densitometry analysis of the degree of phosphorylation on S473-Akt (b) or T308-Akt (c) upon stimulation with insulin is presented. Values are the means ± SEM; n = 3 independent experiments per group of cells. Values that do not share the same superscript letter are significantly different (p ≤ 0.05)
mTOR is an Akt-activated protein involved in the regulation of nutrient uptake and cell growth, among other processes [15]. Our results indicate that cells stably expressing both resistin isoforms impair insulin-stimulated mTOR phosphorylation compared to control insulin stimulated cells (22.5 % in 3T3-L1-s-res and 25 % in 3T3-L1-res, Fig. 4a). These results could be directly related to the decline in S473-Akt phosphorylation previously observed in 3T3L1-s-res and 3T3L1-res cells (Fig. 3a).
Effect of resistin and s-resistin on the activity of mTOR and FoxO1a in 3T3-L1 cells stimulated with insulin. Control 3T3-L1 cells, as well as cells stably expressing resistin (3T3-L1-res) and the short resistin isoform (3T3-L1-s-res) were treated for 30 min with 100 nM insulin. Representative western blots show total (T mTOR and T FoxO1a) and phosphorylated (P S2448-mTOR and P S319-FoxO1a) levels of mTOR (a) and FoxO1a (b). Densitometry analysis of the degree of phosphorylation of mTOR (c) or FoxO1a (d) upon stimulation with insulin is presented. Values are the means ± SEM; n = 3 independent experiments per group of cells. Values that do not share the same superscript letter are significantly different (p ≤ 0.05)
One of the target proteins inactivated by Akt phosphorylation during insulin response is the transcription factor FoxO1a. The active dephosphorylated form of FoxO1a is involved in various cellular processes such as cell cycle regulation, gluconeogenesis activation, and stress response [28]. After being inactivated by Akt phosphorylation, FoxO1a is excluded from the nucleus, which leads to its degradation by the proteosome [23]. Despite the low phosphorylation levels of Akt upon insulin stimulation of cells stably expressing both resistin isoforms (Fig. 3a), surprisingly we observed a marked increase in the insulin-stimulated phosphorylation levels of FoxO1a compared with control cells, especially in 3T3-L1-s-res cells (410 %, Fig. 4b).
Insulin increases SOCS-3 levels in 3T3-L1-s-res adipocytes
The SOCS-3 protein blocks certain cytokine signals, as well as insulin and leptin pathways [14, 20]. Since previous reports demonstrated that resistin induced SOCS-3 expression in 3T3-L1 cells, inhibiting insulin action [34], we set out to analyze if s-resistin could exert a similar effect on SOCS-3. The results shown in Fig. 5 indicate that s-resistin increases SOCS-3 protein levels in 3T3-L1 cells after 15 min of incubation with insulin. However, it is noteworthy that while the 3T3-L1-res cells have elevated SOCS-3 levels even in the absence of insulin (Fig. 5a, b), in the cells stably expressing s-resistin, incubation with insulin upregulated SOCS-3 expression in a time-dependent manner.
Effect of resistin and s-resistin on SOCS-3 protein levels in 3T3-L1 cells stimulated with insulin. Control 3T3-L1 cells, as well as cells stably expressing resistin (3T3-L1-res) and the short resistin isoform (3T3-L1-s-res) were treated for 15 min with 100 nM insulin. Representative western blots (a) show SOCS-3 total levels. Densitometry analysis (b) of the protein level of SOCS-3 upon stimulation with insulin is presented. Values are the means ± SEM; n = 3 independent experiments per group of cells. Values that do not share the same superscript letter are significantly different (p ≤ 0.05)
S-resistin regulates the mRNA levels of transcription factors, inflammatory cytokines, and proteins involved in adipogenesis and insulin response
Table 1 summarizes the effects of resistin and s-resistin overexpression in 3T3-L1 cells on the mRNA levels of key proteins and transcription factors involved in lipid metabolism (SREBP-1c and FoxO1a), adipogenesis (mTOR), inflammation (TNF-α and IL-6), and insulin response (GLUT-4, SOCS-3, resistin, and leptin). As shown in Table 1, after 4 h of incubation with insulin, 3T3-L1-s-res cells have much higher mRNA levels of SREBP-1c, mTOR, and FoxO1a. This expression pattern was also observed in the absence of insulin, suggesting that s-resistin induces lipogenesis and alters adipogenesis. In addition, the expression of GLUT-4 is significantly decreased in 3T3-L1-s-res compared to controls. These expression levels remain unchanged regardless of treatment with insulin. Besides, insulin significantly increases SOCS-3 expression in cells that express s-resistin. These results indicate that s-resistin might decrease insulin sensitivity and induce leptin and insulin resistance in 3T3-L1 adipocytes.
We next examined the expression levels of the proinflamatory cytokines TNF-α and IL-6. Independently of insulin, s-resistin enhanced the expression of these proinflammatory cytokines (Table 1). On the other hand, resistin expression in 3T3-L1-s-res is significantly lower than in control adipocytes. Furthermore, while in control cells, resistin expression levels decrease in response to insulin, in cells expressing s-resistin this is not observed. In addition, 3T3-L1-s-res have higher leptin mRNA levels than control cells, and this difference is augmented upon insulin treatment. These results are consistent with an alteration of the adipogenic process and the induction of leptin resistance.
Discussion
Resistin is an adipokine that affects insulin response in target tissues such as liver, muscle, or hypothalamus, as well as on adipose tissue through a paracrine/autocrine effects. In Wistar rats, it has been described that two resistin variants, resistin and s-resistin, originated by alternative splicing [6]. S-resistin appears as an intracellular short isoform, whose cellular functions are not clear. Several studies of different research groups indicated that the secreted form, resistin, interferes in the intracellular insulin signalling at the early stages of the pathway [24, 30, 34]. However, s-resistin effects over cell insulin signalling are still obscure. Previous results from our research group confirmed that 3T3-L1 adipocytes stably expressing s-resistin isoform, the 3T3-L1-s-res cells, exhibit a decrease in glucose transport, both basal and insulin-stimulated [8]. Here, we demonstrated that s-resistin blocks the signalling pathway of insulin since early stages through a lower activation of IR, IRS-1, Akt, and mTOR, and increased mRNA and protein levels of SOCS-3.
SOCS-3 is a well-known inhibitor of insulin signalling that belongs to the suppressor of cytokine signalling (SOCS) family. It has been described that pre-treatment of 3T3-L1 adipocytes with resistin up-regulates SOCS-3 expression and blocks insulin signalling pathway. In addition, 3T3-L1 adipocytes exposed to a dominant negative SOCS-3 protein prior to resistin treatment blocked the resistin-induced reduction in insulin receptor phosphorylation. Thus, resistin appears to decrease insulin signalling by increasing SOCS-3 levels [34]. SOCS-3 interacts with the insulin receptor, probably to prevent its phosphorylation and inhibits therefore the phosphorylation and activation of IRS1 and Akt [3].
We do not observe an increase in basal SOCS-3 mRNA levels prior to insulin treatment in 3T3-L1-res cells (Table 1), probably because the increase of SOCS-3 expression, described previously [34], is dose-dependent and is observed when adipocytes are incubated with resistin concentrations above 10 ng/ml. However, cell clones used in this study expressed a single copy of resistin (3T3-L1-res) and s-resistin (3T3-L1-s-res) transgenes, respectively [8]. Therefore, 3T3-L1-res cells have very low resistin levels in the culture medium, insufficient to induce SOCS-3 expression, although SOCS-3 protein levels remain elevated.
Nevertheless and in agreement with the work of Steppan et al. [34], our results show that insulin treatment increased SOCS-3 mRNA and protein levels in 3T3-L1-res and 3T3-L1-s-res cells, compared to control cells. These data suggest that s-resistin isoform decreases insulin signalling by up-regulating SOCS-3 through an unknown intracrine mechanism. In consequence, in 3T3-L1-s-res cells, we observed a decrease in IR, IRS-1, Akt, and mTOR phosphorylation as well as undetectable GLUT-4 expression levels, confirming that in adipocytes stably expressing s-resistin the insulin signal transmission was attenuated.
In addition, we observed that both isoforms of resistin bring about an increase in the phosphorylation and consequent inactivation of FoxO1a. FoxO1a is a transcription factor involved mainly in the inhibition of hepatic glucose production and the stimulation of pancreatic β-cells proliferation by insulin. Previous studies demonstrated that Akt/PKB phosphorylates Foxo factors, leading to alteration of their transcription activity and cellular localization [19, 35]. Despite the low levels of insulin-stimulated Akt phosphorylation exhibited by our cells, surprisingly we observed a marked increase in the phosphorylation levels of this FoxO1a, especially by s-resistin. As previously suggested, it is possible that members of mitogen-activated protein kinases (MAPK) family could phosphorylate FoxO1a [1]. More studies should be done to elucidate this point.
Furthermore, compared to control 3T3-L1 cells, 3T3-L1 cells stably expressing s-resistin increased significantly the expression levels of transcription factors involved in lipid metabolism such as SREBP-1c, mTOR, and FoxO1a. This would confirm that the short isoform of resistin induces alterations in adipogenesis, as FoxO1a increased the expression of various cell cycle inhibitors and Chop 10, the modulator of C/EBP, necessary for the proper development of the adipogenic process [23]. Also, it is described that the absence of FoxO1a in adipose tissue prevents insulin resistance [23]. Therefore, these high levels of FoxO1a expression confirm the evidences, described above, that both, resistin and s-resistin, blocked, at least partially the insulin signalling pathway and could generate insulin resistance in adipocyte cells. On the other hand, the high levels of expression of SREBP-1c observed in the 3T3-L1-s-res cell line indicate that fatty acid synthesis could be increased in these adipocytes compared to control cells. It has been described that this factor is responsible for the activation of genes that are directly involved in the lipogenic processes [22]. This result agrees with the observed increase in FAS and DGAT2 expression in these adipocytes (data not shown).
There are several studies analyzing the effect of insulin on resistin expression in adipose tissue [3, 4], in isolated adipocytes and in 3T3-L1 cells [12, 17]. Specifically, it has been reported that insulin inhibits resistin expression in 3T3-L1 adipocytes, even at sub-physiological concentrations [12]. This is consistent with our results, since we also observe a decrease in resistin expression upon incubation of 3T3-L1 cells with insulin. By contrast, in the 3T3-L1-res and 3T3-L1-s-res adipocytes, basal resistin levels are lower compared to control cells and the addition of insulin does not change resistin expression. Since resistin expression is a feature of the mature adipocyte, this decline would confirm the alterations present in both cell clones in the adipogenic process [8]. Most likely, both isoforms could regulate their own synthesis by increasing the expression and the release of pro-inflammatory cytokines such TNFα and IL-6 [8]. Given that TNFα impairs adipocyte differentiation, promotes insulin resistance, and also acts as a potent negative regulator of resistin expression [16, 31], its increased expression by s-resistin and resistin could explain the decreased insulin response and the low resistin expression observed herein.
On the other hand, previous results of our research group have shown that in isolated adipocytes [26] and in white adipose tissue [11], leptin decreases insulin response, reduces the lipogenic capacity of adipocytes, and activates lipolysis, limiting thereby the size of adipose tissue. Furthermore, intracerebroventricular leptin injections in Wistar rats induced SOCS-3 expression and protein levels in adipose tissue, contributing to reduce the insulin response from this tissue [4]. Our results show that the mRNA levels of leptin are significantly increased by s-resistin and especially by the resistin isoform, concomitantly with the increase in SOCS-3 levels, indicating the important role of resistin isoforms in the development of adipocyte leptin resistance.
In summary, this work constitutes the first report on s-resistin effects on the insulin signalling pathway. Our results indicate that the s-resistin isoform, like resistin, impairs cell insulin response, possibly through a mediated increase of SOCS-3 mRNA and protein levels, as well as by inducing an inflammatory state in adipocytes. Thus, s-resistin could be also implicated in the development of adipocyte leptin resistance. Resistin is a secreted protein that may interact in a paracrine/autocrine manner with its still unidentified receptor on the adipocyte cell surface. Through unknown signal cascades, resistin increases SOCS-3 expression and impairs insulin actions. Nevertheless, s-resistin is a non-secretable intracellular protein that could act as an intracellular sensor, by a still unknown intracrine pathway, regulating the differentiation process and cell insulin sensitivity. Further studies will be required to understand the physiological relevance of this short, non-secretable, resistin isoform.
References
Asada S, Daitoku H, Matsuzaki H, Saito T, Sudo T et al (2007) Mitogen-activated protein kinases, Erk and p38, phosphorylate and regulate Foxo 1. Cell Signal 19:519–527
Banerjee RR, Rangwala SM, Shapiro JS, Rich AS, Rhoades B, Qi Y, Wang J, Rajala MW, Pocai A, Scherer PE, Steppan CM, Ahima RS, Obici S, Rossetti L, Lazar MA (2004) Regulation of fasted blood glucose by resistin. Science 303:1195–1198
Barnes KM, Miner JL (2009) Role of resistin in insulin sensitivity in rodents and humans. Curr Protein Pept Sci 10:96–107
Bonzón-Kulinchenko E, Fernández-Agulló T, Moltó E, Serrano R, Fernández A, Ros M, Carrascosa JM, Arribas C, Martínez C, Andrés A, Gallardo N (2011) Regulation of insulin- stimulated glucose uptake in rat white adipose tissue upon chronic central leptin infusion: effects on adiposity. Endocrinology 152:1366–1377
Daquinag AC, Zhang Y, Amaya-Manzanares F, Simmons PJ, Kolonin MG (2011) An isoform of decorin is a resistin receptor on the surface of adipose progenitor cells. Cell Stem Cell 9:74–86
Del Arco A, Peralta S, Carrascosa JM, Ros M, Andrés A, Arribas C (2003) Alternative splicing generates a novel non-secretable resistin isoform in Wistar rats. FEBS Lett 555:243–249
Fernández CM, Moltó E, Gallardo N, del Arco A, Martínez C, Andrés A, Ros M, Carrascosa JM, Arribas C (2009) The expression of rat resistin isoforms is differentially regulated in visceral adipose tissues: effects of aging and food restriction. Metab Clin Exp 58:204–211
Fernández CM, del Arco A, Gallardo N, Aguado L, Rodríguez M, Ros M, Carrascosa JM, Andrés A, Arribas C (2010) S-resistin inhibits adipocyte differentiation and increased TNFα expression and secretion in 3T3-L1 cells. Biochim Biophys Acta 1803:1131–1141
Frost SC, Lane MD (1985) Evidence for the involvement of vicinal sulfhydryl groups in insulin-activated hexose transport by 3T3-L1 adipocytes. J Biol Chem 260:1646–2652
Fu Y, Luo L, Luo N, Garvey WT (2006) Proinflammatory cytokine production and insulin sensitivity regulated by overexpression of resistin in 3T3-L1 adipocytes. Nutr Metab 19:3–28
Gallardo N, Bonzón-Kulichenko E, Fernández-Agulló T, Moltó E, Gómez-Alonso S, Blanco P, Carrascosa JM, Ros M, Andrés A (2007) Tissue-specific effects of central leptin on the expression of genes involved in lipid metabolism in liver and white adipose tissue. Endocrinology 148:5604–5610
Haugen F, JØrgensen A, Drevon CA, Trayhurn P (2001) Inhibition by insulin of resistin gene expression in 3T3-L1 adipocytes. FEBS Lett 507:105–108
Kim K-H, Lee K, Moon YS, Sul H-S (2001) A cystein adipose tissue-specific secretory factor inhibits adipocyte differentiation. J Biol Chem 276:11252–11256
Krebs DL, Hilton DJ (2001) SOCS proteins: negative regulators of cytokine signalling. Stem Cells 19:378–387
Laplante M, Sabatini DM (2012) mTOR signalling in growth control and disease. Cell 149:274–293
Li Y, Totsune K, Takeda K, Furuyama K, Shibahara S, Takahashi K (2003) Differential expression of adrenomedullin and resistin in 3T3-L1 adipocytes treated with tumor necrosis factor- alpha. Eur J Endocrinol 149:231–238
Liu F, Fan HQ, Qiu J, Wang B, Zhang M, Gu N, Zhang CM, Fei L, Pan XQ, Guo M, Chen RH, Guo XR (2008) A paradox: insulin inhibits expression and secretion of resistin which induces insulin resistance. World J Gastroenterol 14:95–100
Livak K, Schmittgen T (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−delta delta C (T) method. Methods 25:402–408
Matsuzaki H, Daitoku H, Hatta M, Tanaka K, Fukamizu A (2003) Insulin-induced phosphorylation of FKHR (Foxo1) targets to proteasomal degradation. Proc Natl Acad Sci U S A 100:11285–11290
Morton GJ, Schwatz MW (2011) Leptin and the central nervous system control of glucose metabolism. Physiol Rev 91:389–411
Muse ED, Obici S, Bhanot S, Monia BP, McKay RA, Rajala MW, Scherer PE, Rossetti L (2004) Role of resistin in diet-induced hepatic insulin resistance. J Clin Invest 114:232–239
Nadeau KJ, Letiner JW, Gurerich I, Draznin B (2004) Insulin regulation of sterol regulatory element-binding protein-1 expression in L-6 muscle cells and 3T3-L1 adipocytes. J Biol Chem 279:34380–34387
Nakae J, Kitamura T, Kitamura Y, Biggs WH, Arden KC, Accili D (2003) The Forkhead transcription factor Foxo1 regulates adipocyte differentiation. Dev Cell 4:119–129
Palanivel R, Maida A, Liu Y, Sweeney G (2006) Regulation of insulin signalling, glucose uptake and metabolism in rat skeletal muscle cells upon prolonged exposure to resistin. Diabetologia 49:183–190
Peralta S, Carrascosa JM, Gallardo N, Ros M, Arribas C (2002) Ageing increases SOCS-3 expression in rat hypothalamus: effects of food restriction. Biochem Biophys Res Comm 296:425–428
Pérez D, Fernández-Galaz C, Fernández-Agulló T, Arribas C, Andrés A, Ros M, Carrascosa JM (2004) Leptin impairs insulin signaling in rat adipocytes. Diabetes 53:347–353
Proenca ARG, Sertié RAL, Oliveira AC, Campaña AB, Caminhotto RO, Chimin P, Lima FB (2014) New concepts in white adipose tissue physiology. Braz J Med Biol Res 47:192–205
Ronnebaum SM, Patterson C (2010) The FoxO family in cardiac function and dysfunction. Annu Rev Physiol 72:81–94
Sánchez-Solana B, Laborda J, Baladron V (2012) Mouse resistin modulates adipogenesis and glucose uptake in 3T3-L1 preadipocytes through the ROR1 receptor. Mol Endocrinol 26:110–127
Satoh H, Nguyen A, Miles PDG, Imamura T, Usui I, Olefski JM (2004) Adenovirus-mediated chronic “hyper-resistinemia” leads to in vivo insulin resistance in normal rats. J Clin Invest 114:224–231
Shojima N, Sakoda H, Ogihara T, Fujishiro M, Katagiri H, Anai M, Onishi Y, Ono H, Inukai K, Abe M, Fukushima Y, Kikuchi M, Oka Y, Asano T (2002) Humoral regulation of resistin expression in 3T3-L1 and mouse adipose cells. Diabetes 51:1737–1744
Sisley S, Sandoval D (2011) Hypothalamic control of energy and glucose metabolism. Rev Endocr Metab Disord 12:219–233
Steppan CM, Bailey ST, Bhat S, Brown EJ, Banerjee RR, Wrght CM, Patel HR, Ahima R, Lazar M (2001) The hormone resistin links obesity to diabetes. Nature 409:307–312
Steppan CM, Wang J, Whiteman EL, Birnbaum MJ, Lazar MA (2005) Activation of SOCS-3 by resistin. Mol Cell Biol 25:1569–1575
Tran H, Brunet A, Griffith EC, Greenberg ME (2003) The many forks in FOXO’s road. Sci STKE 172:RE5
Acknowledgments
MR was a recipient of a predoctoral fellowship from Universidad de Castilla-La Mancha and from BFU2012-39705-C03-01 from Ministerio de Ciencia e Innovación (Spain). This work was supported by research grants PI-2007/60 from Junta de Comunidades de Castilla-La Mancha (JCCM) FISCAM; DGI-BFU2008-C03-02/BFI and BFU2012-39705-C03-01 from Ministerio de Ciencia e Innovación (Spain). The helpful comments and suggestions of PhD. A. del Arco are acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rodríguez, M., Moltó, E., Aguado, L. et al. S-resistin, a non secretable resistin isoform, impairs the insulin signalling pathway in 3T3-L1 adipocytes. J Physiol Biochem 71, 381–390 (2015). https://doi.org/10.1007/s13105-015-0418-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-015-0418-8