Abstract
Moyamoya disease (MMD) is a rare cerebrovascular disease characterized by progressive stenosis of large intracranial arteries and a hazy network of basal collaterals called moyamoya vessels. A polymorphism (R4810K) in the Ring Finger Protein 213 (RNF213) gene, at chromosome 17q25.3, is the strongest genetic susceptibility factor for MMD in East Asian populations. MMD was regarded prevalent in childhood and in East Asian populations. However, the so-called MMD could represent only the tip of the iceberg. MMD is increasingly reported in adult patients and in Western populations. Moreover, the RNF213 variant was recently reported to be associated with non-MMD disorders, such as intracranial atherosclerosis and systemic vasculopathy (e.g., peripheral pulmonary artery stenosis and renal artery stenosis). In this review, we summarize the spectrums of RNF213 vasculopathy in terms of clinical and genetic phenotypes. Continuous efforts are required for pathophysiology-based diagnoses and treatment, which will benefit from collaboration between clinicians and researchers, and between stroke and vascular physicians.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Moyamoya disease (MMD) is a rare cerebrovascular disease characterized by progressive stenosis of large intracranial arteries (including the distal internal carotid artery) and a hazy network of basal collaterals called moyamoya vessels. The etiology of MMD is unknown. As a result, criteria for the diagnosis of MMD are based on characteristic angiographic findings. Most research on angiographic features, diagnostic criteria, and treatment guidelines has been limited to pediatric MMD [1].
The prevalence of adult-onset MMD may be underestimated. Unlike in childhood-onset MMD, typical angiographic features might not be observed in the early phase of adult-onset MMD [2, 3]. One regional, all-inclusive data set of newly registered patients with MMD in Hokkaido, Japan, showed that the age of onset is rising and ischemic presentation is increasing [4]. The annual incidence of MMD has reportedly increased in Japan, China, Taiwan, and Korea [5]. Such changes in the epidemiology of MMD may be derived from the increasing number of adult patients diagnosed with MMD, rather than the actual changes in epidemiology or characteristics of MMD [5].
A polymorphism, R4810K (p.Arg4810Lys), in the Ring Finger Protein 213 (RNF213) gene at chromosome 17q25.3 was identified as the strongest genetic susceptibility factor for MMD in East Asian populations, using genome-wide linkage and exome analysis [6, 7]. RNF213 R4810K-related vasculopathy is not well characterized, except in MMD. However, RNF213 variants may not be the only determinants of MMD. Very recent clinical studies showed that RNF213 variants are associated not only with MMD but also with intracranial atherosclerosis [8] and systemic vascular diseases, such as peripheral pulmonary artery stenosis and renal artery stenosis [9, 10]. Moreover, not all the patients with MMD have this genetic variant.
Therefore, the so-called MMD may represent only the tip of the iceberg. These results call for the redefinition of MMD as a spectrum, considering the heterogeneity of innate angiogenetic capacity, genetic, and environmental factors. The purpose of this review is to summarize the spectrum of RNF213 vasculopathy, in terms of clinical and genetic phenotypes. In addition, the clinical implications of the RNF213 spectrum on the evaluation and management of MMD patients are discussed.
Search Strategy and Selection Criteria
Articles for inclusion in this review were identified using PubMed and ClinicalTrials.gov, with the search terms “moyamoya disease,” “stroke,” “RNF213,” and “cerebrovascular disease,” and were published in English, up until March 2019. We also considered other relevant articles and reviews. The final reference list was generated on the basis of originality and relevance to this topic. Because of space limitations, we were not able to discuss individual pathophysiologies of MMD in depth or with critical analyses.
Spectrums Related to MMD
Phenotypic variation of MMD and related RNF213 vasculopathies may be caused by the complex interaction of the following factors (Fig. 1).
Age Spectrum
In children, ischemic symptoms, especially transient ischemic attack, are predominant, whereas adult patients present with intracranial hemorrhage more often than pediatric patients. In addition, moyamoya collaterals, which are the clinical hallmark of MMD, are more prominent in childhood MMD than in adult-onset MMD [3]. The differences in angiographic findings between childhood and adult MMD could be caused by either a more severe aberrant angiogenesis in childhood MMD or decreased angiogenetic capability in adult MMD. Aberrant angiogenesis and proliferative vasculopathy of MMD are prominent in childhood MMD. A long-term follow-up angiographic study showed that the age at diagnosis was the only independent predictor of contralateral progression [11]. The disease progresses angiographically until adolescence [12], and disease progression is relatively rare in adult MMD, especially in asymptomatic individuals. Conversely, angiogenesis is impaired with increasing age [13]. Aging causes rarefaction and insufficient collateral circulation in multiple tissues, resulting in more severe ischemic tissue injury, and vascular risk factors are associated with poor collaterals in preclinical and clinical studies [14]. Age-related angiogenetic capacity does not only affect the angiographic findings of MMD but also determines the mode of surgical treatment. Indirect revascularization techniques are generally preferable in childhood MMD, while direct bypass techniques are preferable in adult MMD patients [1, 15].
Genetic Spectrum
RNF213 Gene and Inheritance Pattern
The R4810K variant was identified in 95% of patients with familial MMD, 80% with sporadic MMD, and 1.8% of control individuals in a Japanese population [6]. RNF213 encodes a relatively large protein with a dual AAA+ ATPase and E3 ligase activities [16]. In vitro and in vivo experiments revealed that RNF213 is related to angiogenesis and vascular inflammation; however, the exact physiologic functions of RNF213 remain unknown [16]. The R4810K variant is an Asian founder mutation and its prevalence is reported to be up to 2.5% in East Asians [16, 17], although it has not been reported in Western populations. Since the total number of carriers is estimated to be 15 million in Asian countries, the impact on cardiovascular health is extremely significant [18]. Homozygosity for R4810K predicted an earlier onset and a more severe form of MMD in both Japanese [19] and Korean [20] patients with MMD. Prevalence of homozygotes is reported as 7–8% of overall MMD patients. The penetrance rate of MMD in heterozygotes is as low as one per 150–300 [18], whereas the penetrance rate of MMD in homozygotes was calculated to be over 78% [19].
RNF213 Variant Homozygosity and Systemic Vasculopathy
The reason behind the specific site of vascular system involvement is one of the unanswered questions in MMD. Genetic and related changes in circulating factors confer pathophysiological effects on the systemic vessels, as well as major vessels of the circle of Willis. Site specificity and sparing of systemic vessels cannot be explained. There is a possibility that patients with RNF213 variants might present with phenotypes other than MMD. RNF213 vasculopathy could be a systemic disease, with MMD as a central nervous system subtype, especially in homozygous individuals.
Extracranial involvement of MMD has been described in case reports of coronary [21, 22], pulmonary [9], and renal artery stenosis in 7.9% of pediatric MMD patients [23], although genetic information was unavailable. Very recently, Fukushima and colleagues reported two cases of MMD and pulmonary artery stenosis, with homozygosity for R4810K variant [9]. One of them also had renal artery stenosis. It has been suggested that R4810K variant causes classical MMD when present in a heterozygous state, but the same variant results in MMD and systemic vascular diseases when present in the homozygous state, in a gene dosage-dependent manner [9]. We recently reported five index cases and their families harboring homozygous and heterozygous R4810K variants with various manifestations of vascular involvement [10]. Homozygous patients showed a very unique pattern of diffuse narrowing of the aorta and iliofemoral arteries, together with stenosis of renal, celiac, or peripheral pulmonary arteries, regardless of the presence or absence of MMD. Heterozygous patients were mostly asymptomatic or had isolated MMD. Therefore, R4810K is associated with a high penetrance of systemic vasculopathy in homozygous patients, and a low penetrance of MMD in heterozygous patients, suggestive of a gene-dosage effect.
It is possible that a significant proportion of homozygous patients are being treated without consideration of the particular RNF213 variants present. R4810K-related vasculopathy might be important from a therapeutic view point. For example, stent insertion, which is an option for medically intractable intracranial atherosclerotic stenosis, could be harmful for MMD patients. There have been several case series of stent insertion in MMD that showed occlusion by in-stent restenosis due to progressive intimal hyperplasia or serious adverse effects [24,25,26,27]. The same may be true for systemic vasculopathy related to RNF213 variants. While arterial stenosis in fibromuscular dysplasia responds well to balloon angioplasty and atherosclerotic renal artery stenosis to stenting, balloon angioplasty or stenting in R4810K-related vasculopathy might result in immediate elastic recoil or progressive restenosis [10]. In this case, bypass surgery for renal artery stenosis could be considered for R4810K variant–related vascular stenosis, similar to that for MMD.
Genetic Factors Aside from the RNF213 R4810K Variant
RNF213 R4810K is not a susceptibility variant for MMD in Western populations or South Asians. Several non-R4810K variants (rs148731719 and rs397514563) were recently found in Caucasian, and East and South Asian cases with MMD [7, 17, 28, 29]. In addition, clinical manifestations and possibly angiographic findings may differ between Western populations and East Asians [30]. The R4810K variant is reportedly related to ischemic-type MMD, whereas non-R4810K variants (especially A4399T) are associated with hemorrhagic-type MMD [28]. Further genetic studies in these populations are required.
Combinatorial interactions between RNF213 variants and other gene variants must be considered. A recent case series of European familial MMD showed rare candidate variants of RNF213 and PALD1 within the same families, suggesting that variants in these two genes might act synergistically [31]. The penetrance of MMD in carriers was incomplete, at around 25%, suggesting that additional genetic or environmental factors, other than these rare RNF213 variants, are needed to develop MMD [31]. In addition, the interaction of RNF213 variants with other genes or the environment may be the cause of the heterogeneity in the RNF213 phenotype. Moreover, owing to the cell/tissue-specific expression pattern of non-coding RNAs and their remarkable stability in peripheral blood, a number of studies have highlighted the role of circulating non-coding RNAs in angiogenesis and atherogenesis [32]. A prospective study (ClinicalTrials.gov Identifier NCT02074111) is ongoing, to evaluate the levels of circulating microRNAs with respect to RNF213 and caveolin-1 gene polymorphisms in MMD.
Environmental Spectrum
Environmental Factors
Beside genetic influence, additional insult may be required to induce MMD. First, from an epidemiological view point, the incidence rate of MMD is lower than that of carriers of RNF213 variants. Second, recent in vivo experiments using genetically engineered Rnf213 mice, such as Rnf213-deficient mice [33] or Rnf213-knock-in mice [34], addressed the mechanism underlying RNF213 variation in the development of MMD pathology. However, the mice did not develop MMD under normal conditions. These negative results are consistent with the low penetrance rate of RNF213 polymorphisms in patients with MMD, and may indicate the importance of environmental factors in addition to genetic factors [35]. Ito and colleagues subjected Rnf213-deficient mice to ischemic insult and found that post-ischemic angiogenesis was significantly enhanced in mice lacking Rnf213, after chronic hindlimb ischemia [36]. This suggests the potential role of defective RNF213 in the development of abnormal vascular networks in chronic ischemia. Third, clinical data has also shown that environmental factors, such as an autoimmune response and infection/inflammation, may be associated with the angiographic features of MMD [35]. For example, autoimmune thyroid disease has been reported in different MMD populations (i.e., pediatric and adult-onset MMD, East Asians, and Western populations) and may be involved in MMD development [37,38,39]. RNF213 may be a downstream mediator of the IFN-β signaling pathway in endothelial cells. Carriers of the R4810K may be susceptible to cerebral hypoxia because of insufficient angiogenesis, if inflammation and hypoxia occur simultaneously [40]. Pro-inflammatory cytokines activate RNF213 transcription, and RNF213 functions as a common downstream effector of the PI3 kinase-AKT pathway, in endothelial angiogenesis [41]. These in vitro experimental data suggest that although MMD is not an inflammatory disease, inflammation may play an important role in MMD development, and that RNF213 plays a unique role in endothelial cells with respect to gene expression in response to inflammatory signals from the environment. These clinical and preclinical observations may represent the “two-hit theory,” which is apparent in a variety of disorders [35]. RNF213 variation could lead to vascular fragility, which may increase the vulnerability of vessels to hemodynamic stress and secondary insults [35].
Intracranial Atherosclerosis and RNF213 Variants
Both intracranial atherosclerosis and MMD are prevalent in Asians. Although several studies have described the role of RNF213 in vascular development [6, 7], there is limited data on its role in atherosclerotic diseases, and no genetic factors specific to intracranial atherosclerosis have been reported. Patients with RNF213 variation may be prone to atherosclerosis. Miyawaki et al. and Kamimura et al. tested for R4810K in patients with intracranial major artery stenosis without signs of MMD. The variant was present in 21.9–24.3% of patients with non-moyamoya intracranial stenosis [42,43,44]. Similarly, Matsuda et al. performed RNF213 genotyping and vascular studies in 59 relatives of MMD patients. Six of 34 individuals with R4810K showed intracranial steno-occlusive lesions, whereas none of 25 individuals without the variant showed vascular lesions [45]. We recently tested whether RNF213 is also a susceptibility gene for intracranial atherosclerosis in patients whose diagnosis had been confirmed by conventional angiography (absence of basal collaterals) and high-resolution magnetic resonance image (HR-MRI) (i.e., the presence of intracranial plaque and absence of MMD features) [8]. The results confirmed that R4810K was present in a quarter of patients with intracranial atherosclerosis, suggesting that RNF213 is a susceptibility gene, not only for MMD but also for intracranial atherosclerosis in East Asians [8]. Among patients with intracranial atherosclerosis, R4810K carriers were younger, more often women, and more likely to have a family history of MMD and proximal anterior circulation stenosis than non-carriers [8, 44]. A recent large population study in Japan, evaluating R4810K in various stroke subtypes, confirmed that only large artery disease was associated with this variant. Patients with both R4810K and large artery disease showed lower age of stroke onset, female predominance, and anterior circulation distribution, compared with non-carriers [46].
In addition, other studies and ours showed that R4810K is associated with smaller sized intracranial arteries, suggesting impaired vasculogenesis [47, 48]. Hongo et al. measured the outer diameter of the middle cerebral artery (MCA) in a small cohort and showed that the outer diameter of the MCA was smaller in R4810K carriers [47]. Our HR-MRI study also showed that negative remodeling involves all the intracranial arteries measured not only the stenotic MCA segments but also the contralateral MCA, distal internal carotid artery, and basilar artery in patients with this variant [48]. Hemodynamic studies have shown that, in the presence of intracranial atherosclerosis, the R4810K variant predisposes the smaller intracranial arteries to hemodynamic compromise [48].
Evaluation and Treatment in MMD Patients
The spectrums related to MMD may have clinical implications for diagnostic and therapeutic approaches in patients. In addition to the current paradigm of luminographic evaluation (cerebral angiography to identify moyamoya vessels) and bypass surgery to enhance collateral flow, the following diagnostic and therapeutic strategies should be considered, based on variations in RNF213-related vasculopathies.
Evaluation of MMD Patients and Their Families
Unlike in childhood MMD, genetic/molecular or dedicated imaging, rather than angiographic findings, could be particularly helpful in diagnosing MMD in adult patients with presumed MMD, in whom angiographic features of moyamoya vessels are not prominent. Many etiologies can cause intracranial arterial steno-occlusion in adults. For example, HR-MRI can show the characteristic features of MMD (a small vessel diameter, thin vessel wall, and diffuse concentric enhancement, which are consistent with pathogenesis and pathologic features) [49] and exclude other causes (e.g., plaque or dissection) [5, 49]. These features were observed not only with typical angiographic features of basal collaterals but also without them.
Systemic vascular evaluation of the pulmonary, renal, coronary, mesenteric, and aortoiliac arteries should be considered in family members of MMD patients when they present symptoms (i.e., shortness of breath, angina) or show signs of specific systemic vascular involvement (i.e., hypertension at a young age). Systemic evaluation should also be considered in R4810K homozygotes because of the high penetrance rate of systemic vascular involvement. In our institute, polyvascular CT angiography is being used to screen for systemic involvement, especially in R4810K homozygous MMD patients.
Practice guidelines for genetic testing and counseling in MMD patients and family members have not yet been established. Genetic testing in MMD should only occur in the context of genetic counseling and be supported by expertise in this area. A ≥ 3 generation family history should be obtained, that focuses not only on stroke or MMD but also systemic vascular involvement, such as peripheral pulmonary artery stenosis and renal artery stenosis. Patients should be informed that MMD is a familial disorder with low penetrance, and only one in 150–300 R4810K carriers will develop MMD. Genetic testing should be considered in East Asian patients with MMD and a family history of MMD, on both the paternal and maternal sides, who are potentially homozygous for R4810K. Genetic testing might be considered in patients with systemic vasculopathy, who have a family history of MMD. On the contrary, genetic testing in asymptomatic adult MMD patients is not advisable. The benefits of genetic testing in non-East Asian populations are settled. In addition, blood tests for thyroid function and thyroid autoantibodies could be considered in patients with presumed MMD.
Treatment of Underlying Pathophysiology
At present, surgical re-vascularization is the mainstay of MMD treatment. However, surgical treatments pose a risk for perioperative ischemic complications and/or cerebral hyperperfusion syndrome [50]. With a better understanding of MMD pathophysiology, non-surgical approaches targeting MMD pathogenesis may become available to halt or slow disease progression [51]. Possible non-surgical approaches may include the application of certain trophic factors or chemicals that increase angiogenesis [52], anti-cancer drugs to decrease smooth muscle cell proliferation [53], retinoid to attenuate growth factor–stimulated smooth muscle cell migration and proliferation [54, 55], microRNA-based therapies to inhibit microRNAs related to MMD, [56, 57], and stem cell therapy to replace or restore function of endothelial or smooth muscle progenitor cells which are impaired in MMD [58,59,60]. However, none of these approaches has been tested in MMD patients.
In addition, strategies targeted at increasing caveolin-1 levels could be candidate therapies for MMD [61]. Caveolin-1, a scaffolding protein of the caveolae plasma membrane, is involved in the pathogenesis of cancers and vascular diseases [62]. Caveolin-1 overexpression enhances caveolae generation and accelerates capillary tube formation by nearly threefold, while caveolin-1 downregulation reduces capillary formation in vitro and in vivo, and is associated with pathological angiogenesis [62,63,64]. A decreased serum level of caveolin-1 has been reported to be a novel biomarker for MMD [65]. A recent HR-MRI study showed that serum levels of caveolin-1 were correlated with the degree of negative remodeling of major intracranial vessels in MMD patients [66].
Antiplatelet agents are widely used in patients with MMD. Although hemodynamic compromise is the major determinant of stroke in MMD patients, a multimodal MRI study showed that embolic phenomena played an important role in acute ischemic stroke in MMD patients [67]. Given the role of antiplatelet agents in microembolism, in patients with large intracranial stenosis, the short-term use of appropriate antithrombotic agents could be considered for MMD patients with recurrent embolic strokes. Cilostazol, a PDE3 inhibitor, has both antiplatelet and vasodilator action, activates bone marrow–derived endothelial progenitor cells, and inhibits smooth muscle cell proliferation [68, 69]. Statin treatment was reported to decrease matrix metalloprotease-9 levels, to inhibit neointima formation, and to increase circulating endothelial progenitor cells [70, 71].
The role of RNF213 in controlling vascular risk factors is unknown. The R4810K variant might influence vascular risk factors, such as hypertension [72], and could also lead to vascular fragility, increasing vulnerability of vessels to hemodynamic stress and secondary insults [35]. A long-term follow-up of angiographic-confirmed MMD patients showed that diabetes, an important vascular risk factor for intracranial atherosclerosis, was the only independent predictor of ischemic stroke recurrence in patients with MMD [73]. These features suggest that vascular risk factor control may be important in subjects with intracranial stenosis and RNF213 variant carrier status.
Conclusions and Perspectives
Our literature review advocates that MMD requires redefinition, from childhood and cerebral vasculopathy to a broader spectrum vasculopathy affecting both cerebral and systemic vessel systems. Figure 2 shows four spectrums of RNF213 vasculopathy and their examples are provided in Figs. 3 and 4. Both genetic and environmental factors may play important roles in the development and phenotype of RNF213 vasculopathy, through complex mechanisms. Continuous efforts are required for pathophysiology-based diagnoses and treatments, which will benefit from collaboration between both stroke and vascular physicians, and the cooperation of all those involved, from the hospital bed through to the laboratory bench.
a A typical case of moyamoya disease (MMD). A 9-year-old female with a family history of MMD presented recurrent hemiparesis during hyperventilation and crying. Angiography shows occlusion of major intracranial vessels and prominent basal collateral circulations. b A 35-year-old heterozygote female with a healthy vascular risk factor profile presented with transient hemiparesis. Angiography showed no basal collaterals and high-resolution MRI showed eccentric enhancing plaque and negative remodeling, suggestive of RNF213-related premature atherosclerosis
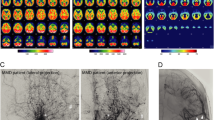
Genetic factors may determine differential features within a family with MMD. (A) A 64-year-old female heterozygote had history of stroke at her age of 50. Angiography showed bilateral carotid occlusion and less prominent moyamoya vessels. (B) The patient’s 27-year-old homozygote son showed systemic involvement, including pulmonary, coronary, renal, and superior mesenteric artery. Computed tomography showed a small aorta. Cerebral involvement was not observed in this patient
References
Roach ES, Golomb MR, Adams R, Biller J, Daniels S, Deveber G, et al. Management of stroke in infants and children: a scientific statement from a Special Writing Group of the American Heart Association Stroke Council and the Council on Cardiovascular Disease in the Young. Stroke. 2008;39(9):2644–91. https://doi.org/10.1161/STROKEAHA.108.189696.
Bang OY, Ryoo S, Kim SJ, Yoon CH, Cha J, Yeon JY, et al. Adult moyamoya disease: a burden of intracranial stenosis in East Asians? PLoS One. 2015;10(6):e0130663. https://doi.org/10.1371/journal.pone.0130663.
Chung JW, Kim SJ, Bang OY, Kim KH, Ki CS, Jeon P, et al. Determinants of basal collaterals in moyamoya disease: clinical and genetic factors. Eur Neurol. 2016;75(3-4):178–85. https://doi.org/10.1159/000445348.
Baba T, Houkin K, Kuroda S. Novel epidemiological features of moyamoya disease. J Neurol Neurosurg Psychiatry. 2008;79(8):900–4. https://doi.org/10.1136/jnnp.2007.130666.
Bang OY, Toyoda K, Arenillas JF, Liu L, Kim JS. Intracranial large artery disease of non-atherosclerotic origin: recent progress and clinical implications. J Stroke. 2018;20(2):208–17. https://doi.org/10.5853/jos.2018.00150.
Kamada F, Aoki Y, Narisawa A, Abe Y, Komatsuzaki S, Kikuchi A, et al. A genome-wide association study identifies RNF213 as the first moyamoya disease gene. J Hum Genet. 2011;56(1):34–40. https://doi.org/10.1038/jhg.2010.132.
Liu W, Morito D, Takashima S, Mineharu Y, Kobayashi H, Hitomi T, et al. Identification of RNF213 as a susceptibility gene for moyamoya disease and its possible role in vascular development. PLoS One. 2011;6(7):e22542. https://doi.org/10.1371/journal.pone.0022542.
Bang OY, Chung JW, Cha J, Lee MJ, Yeon JY, Ki CS, et al. A polymorphism in RNF213 is a susceptibility gene for intracranial atherosclerosis. PLoS One. 2016;11(6):e0156607. https://doi.org/10.1371/journal.pone.0156607.
Fukushima H, Takenouchi T, Kosaki K. Homozygosity for moyamoya disease risk allele leads to moyamoya disease with extracranial systemic and pulmonary vasculopathy. Am J Med Genet A. 2016;170(9):2453–6. https://doi.org/10.1002/ajmg.a.37829.
Chang SA, Song JS, Park TK, Yang JH, Kwon WC, Kim SR, et al. Nonsyndromic peripheral pulmonary artery stenosis is associated with homozygosity of RNF213 p.Arg4810Lys regardless of co-occurrence of moyamoya disease. Chest. 2018;153(2):404–13. https://doi.org/10.1016/j.chest.2017.09.023.
Yeon JY, Shin HJ, Kong DS, Seol HJ, Kim JS, Hong SC, et al. The prediction of contralateral progression in children and adolescents with unilateral moyamoya disease. Stroke. 2011;42(10):2973–6. https://doi.org/10.1161/STROKEAHA.111.622522.
Ezura M, Yoshimoto T, Fujiwara S, Takahashi A, Shirane R, Mizoi K. Clinical and angiographic follow-up of childhood-onset moyamoya disease. Childs Nerv Syst. 1995;11(10):591–4.
Lahteenvuo J, Rosenzweig A. Effects of aging on angiogenesis. Circ Res. 2012;110(9):1252–64. https://doi.org/10.1161/CIRCRESAHA.111.246116.
Faber JE, Zhang H, Lassance-Soares RM, Prabhakar P, Najafi AH, Burnett MS, et al. Aging causes collateral rarefaction and increased severity of ischemic injury in multiple tissues. Arterioscler Thromb Vasc Biol. 2011;31(8):1748–56. https://doi.org/10.1161/ATVBAHA.111.227314.
Jeon JP, Kim JE, Cho WS, Bang JS, Son YJ, Oh CW. Meta-analysis of the surgical outcomes of symptomatic moyamoya disease in adults. J Neurosurg. 2017:1–7. https://doi.org/10.3171/2016.11.JNS161688.
Koizumi A, Kobayashi H, Hitomi T, Harada KH, Habu T, Youssefian S. A new horizon of moyamoya disease and associated health risks explored through RNF213. Environ Health Prev Med. 2016;21(2):55–70. https://doi.org/10.1007/s12199-015-0498-7.
Ma J, Liu Y, Ma L, Huang S, Li H, You C. RNF213 polymorphism and moyamoya disease: a systematic review and meta-analysis. Neurol India. 2013;61(1):35–9. https://doi.org/10.4103/0028-3886.107927.
Liu W, Hitomi T, Kobayashi H, Harada KH, Koizumi A. Distribution of moyamoya disease susceptibility polymorphism p.R4810K in RNF213 in East and Southeast Asian populations. Neurol Med Chir (Tokyo). 2012;52(5):299–303.
Miyatake S, Miyake N, Touho H, Nishimura-Tadaki A, Kondo Y, Okada I, et al. Homozygous c.14576G>A variant of RNF213 predicts early-onset and severe form of moyamoya disease. Neurology. 2012;78(11):803–10. https://doi.org/10.1212/WNL.0b013e318249f71f.
Kim EH, Yum MS, Ra YS, Park JB, Ahn JS, Kim GH, et al. Importance of RNF213 polymorphism on clinical features and long-term outcome in moyamoya disease. J Neurosurg. 2016;124(5):1221–7. https://doi.org/10.3171/2015.4.JNS142900.
St Goar FG, Gominak SC, Potkin BN. Bilateral aortoostial coronary artery disease: moyamoya of the heart? Am J Cardiol. 1999;83(8):1296–9 A10.
Lee JH, Youn TJ, Yoon YE, Park JJ, Hong SJ, Chun EJ, et al. Coronary artery stenosis in moyamoya disease: tissue characterization by 256-slice multi-detector CT and virtual histology. Circulation. 2013;127(20):2063–5. https://doi.org/10.1161/CIRCULATIONAHA.112.136473.
Baek JW, Jo KI, Park JJ, Jeon P, Kim KH. Prevalence and clinical implications of renal artery stenosis in pediatric moyamoya disease. Eur J Paediatr Neurol. 2016;20(1):20–4. https://doi.org/10.1016/j.ejpn.2015.11.002.
Drazin D, Calayag M, Gifford E, Dalfino J, Yamamoto J, Boulos AS. Endovascular treatment for moyamoya disease in a Caucasian twin with angioplasty and Wingspan stent. Clin Neurol Neurosurg. 2009;111(10):913–7. https://doi.org/10.1016/j.clineuro.2009.08.012.
Eicker S, Etminan N, Turowski B, Steiger HJ, Hanggi D. Intracranial carotid artery stent placement causes delayed severe intracranial hemorrhage in a patient with moyamoya disease. J Neurointerv Surg. 2011;3(2):160–2. https://doi.org/10.1136/jnis.2010.003004.
Natarajan SK, Karmon Y, Tawk RG, Hauck EF, Hopkins LN, Siddiqui AH, et al. Endovascular treatment of patients with intracranial stenosis with moyamoya-type collaterals. J Neurointerv Surg. 2011;3(4):369–74. https://doi.org/10.1136/jnis.2011.004754.
Khan N, Dodd R, Marks MP, Bell-Stephens T, Vavao J, Steinberg GK. Failure of primary percutaneous angioplasty and stenting in the prevention of ischemia in moyamoya angiopathy. Cerebrovasc Dis. 2011;31(2):147–53. https://doi.org/10.1159/000320253.
Wu Z, Jiang H, Zhang L, Xu X, Zhang X, Kang Z, et al. Molecular analysis of RNF213 gene for moyamoya disease in the Chinese Han population. PLoS One. 2012;7(10):e48179. https://doi.org/10.1371/journal.pone.0048179.
Cecchi AC, Guo D, Ren Z, Flynn K, Santos-Cortez RL, Leal SM, et al. RNF213 rare variants in an ethnically diverse population with moyamoya disease. Stroke. 2014;45(11):3200–7. https://doi.org/10.1161/STROKEAHA.114.006244.
Kleinloog R, Regli L, Rinkel GJ, Klijn CJ. Regional differences in incidence and patient characteristics of moyamoya disease: a systematic review. J Neurol Neurosurg Psychiatry. 2012;83(5):531–6. https://doi.org/10.1136/jnnp-2011-301387.
Grangeon L, Guey S, Schwitalla JC, Bergametti F, Arnould M, Corpechot M, et al. Clinical and molecular features of 5 European multigenerational families with moyamoya angiopathy. Stroke. 2019;50(4):789–96. https://doi.org/10.1161/STROKEAHA.118.023972.
Tiedt S, Dichgans M. Role of non-coding RNAs in stroke. Stroke. 2018;49(12):3098–106. https://doi.org/10.1161/STROKEAHA.118.021010.
Sonobe S, Fujimura M, Niizuma K, Nishijima Y, Ito A, Shimizu H, et al. Temporal profile of the vascular anatomy evaluated by 9.4-T magnetic resonance angiography and histopathological analysis in mice lacking RNF213: a susceptibility gene for moyamoya disease. Brain Res. 2014;1552:64–71. https://doi.org/10.1016/j.brainres.2014.01.011.
Kanoke A, Fujimura M, Niizuma K, Ito A, Sakata H, Sato-Maeda M, et al. Temporal profile of the vascular anatomy evaluated by 9.4-tesla magnetic resonance angiography and histological analysis in mice with the R4859K mutation of RNF213, the susceptibility gene for moyamoya disease. Brain Res. 2015;1624:497–505. https://doi.org/10.1016/j.brainres.2015.07.039.
Fujimura M, Sonobe S, Nishijima Y, Niizuma K, Sakata H, Kure S, et al. Genetics and biomarkers of moyamoya disease: significance of RNF213 as a susceptibility gene. J Stroke. 2014;16(2):65–72. https://doi.org/10.5853/jos.2014.16.2.65.
Ito A, Fujimura M, Niizuma K, Kanoke A, Sakata H, Morita-Fujimura Y, et al. Enhanced post-ischemic angiogenesis in mice lacking RNF213; a susceptibility gene for moyamoya disease. Brain Res. 2015;1594:310–20. https://doi.org/10.1016/j.brainres.2014.11.014.
Kim SJ, Heo KG, Shin HY, Bang OY, Kim GM, Chung CS, et al. Association of thyroid autoantibodies with moyamoya-type cerebrovascular disease: a prospective study. Stroke. 2010;41(1):173–6. https://doi.org/10.1161/STROKEAHA.109.562264.
Bower RS, Mallory GW, Nwojo M, Kudva YC, Flemming KD, Meyer FB. Moyamoya disease in a primarily White, Midwestern US population: increased prevalence of autoimmune disease. Stroke. 2013;44(7):1997–9. https://doi.org/10.1161/STROKEAHA.111.000307.
Li H, Zhang ZS, Dong ZN, Ma MJ, Yang WZ, Han C, et al. Increased thyroid function and elevated thyroid autoantibodies in pediatric patients with moyamoya disease: a case-control study. Stroke. 2011;42(4):1138–9. https://doi.org/10.1161/STROKEAHA.110.608471.
Kobayashi H, Matsuda Y, Hitomi T, Okuda H, Shioi H, Matsuda T, et al. Biochemical and functional characterization of RNF213 (mysterin) R4810K, a susceptibility mutation of moyamoya disease, in angiogenesis in vitro and in vivo. J Am Heart Assoc. 2015;4(7). https://doi.org/10.1161/JAHA.115.002146.
Ohkubo K, Sakai Y, Inoue H, Akamine S, Ishizaki Y, Matsushita Y, et al. Moyamoya disease susceptibility gene RNF213 links inflammatory and angiogenic signals in endothelial cells. Sci Rep. 2015;5:13191. https://doi.org/10.1038/srep13191.
Miyawaki S, Imai H, Takayanagi S, Mukasa A, Nakatomi H, Saito N. Identification of a genetic variant common to moyamoya disease and intracranial major artery stenosis/occlusion. Stroke. 2012;43(12):3371–4. https://doi.org/10.1161/STROKEAHA.112.663864.
Miyawaki S, Imai H, Shimizu M, Yagi S, Ono H, Mukasa A, et al. Genetic variant RNF213 c.14576G>A in various phenotypes of intracranial major artery stenosis/occlusion. Stroke. 2013;44(10):2894–7. https://doi.org/10.1161/STROKEAHA.113.002477.
Kamimura T, Okazaki S, Morimoto T, Kobayashi H, Harada K, Tomita T, et al. Prevalence of RNF213 p.R4810K variant in early-onset stroke with intracranial arterial stenosis. Stroke. 2019:STROKEAHA118024712. https://doi.org/10.1161/STROKEAHA.118.024712.
Matsuda Y, Mineharu Y, Kimura M, Takagi Y, Kobayashi H, Hitomi T, et al. RNF213 p.R4810K variant and intracranial arterial stenosis or occlusion in relatives of patients with moyamoya disease. J Stroke Cerebrovasc Dis. 2017;26(8):1841–7. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.04.019.
Okazaki S, Morimoto T, Kamatani Y, Kamimura T, Kobayashi H, Harada K, et al. moyamoya disease susceptibility variant RNF213 p.R4810K increases the risk of ischemic stroke attributable to large-artery atherosclerosis. Circulation. 2019;139(2):295–8. https://doi.org/10.1161/CIRCULATIONAHA.118.038439.
Hongo H, Miyawaki S, Imai H, Shinya Y, Ono H, Mori H, et al. Smaller outer diameter of atherosclerotic middle cerebral artery associated with RNF213 c.14576G>A variant (rs112735431). Surg Neurol Int. 2017;8:104. https://doi.org/10.4103/sni.sni_59_17.
Choi EH, Lee H, Chung JW, Seo WK, Kim GM, Ki CS, et al. The Ring Finger Protein 213 variant and plaque characteristics, vascular remodeling, and hemodynamics in patients with intracranial atherosclerotic stroke: a high-resolution MRI and hemodynamic study. J Am Heart Assoc. In Press.
Ryoo S, Cha J, Kim SJ, Choi JW, Ki CS, Kim KH, et al. High-resolution magnetic resonance wall imaging findings of moyamoya disease. Stroke. 2014;45(8):2457–60. https://doi.org/10.1161/STROKEAHA.114.004761.
Fujimura M, Shimizu H, Inoue T, Mugikura S, Saito A, Tominaga T. Significance of focal cerebral hyperperfusion as a cause of transient neurologic deterioration after extracranial-intracranial bypass for moyamoya disease: comparative study with non-moyamoya patients using N-isopropyl-p-[(123)I]iodoamphetamine single-photon emission computed tomography. Neurosurgery. 2011;68(4):957–64; discussion 64-5. https://doi.org/10.1227/NEU.0b013e318208f1da.
Bang OY, Fujimura M, Kim SK. The pathophysiology of moyamoya disease: an update. J Stroke. 2016;18(1):12–20. https://doi.org/10.5853/jos.2015.01760.
Bang OY, Goyal M, Liebeskind DS. Collateral circulation in ischemic stroke: assessment tools and therapeutic strategies. Stroke. 2015;46(11):3302–9. https://doi.org/10.1161/STROKEAHA.115.010508.
Guo DC, Papke CL, Tran-Fadulu V, Regalado ES, Avidan N, Johnson RJ, et al. Mutations in smooth muscle alpha-actin (ACTA2) cause coronary artery disease, stroke, and moyamoya disease, along with thoracic aortic disease. Am J Hum Genet. 2009;84(5):617–27. https://doi.org/10.1016/j.ajhg.2009.04.007.
Kim SK, Yoo JI, Cho BK, Hong SJ, Kim YK, Moon JA, et al. Elevation of CRABP-I in the cerebrospinal fluid of patients with moyamoya disease. Stroke. 2003;34(12):2835–41. https://doi.org/10.1161/01.STR.0000100159.43123.D7.
Lee JY, Moon YJ, Lee HO, Park AK, Choi SA, Wang KC, et al. Deregulation of retinaldehyde dehydrogenase 2 leads to defective angiogenic function of endothelial colony-forming cells in pediatric moyamoya disease. Arterioscler Thromb Vasc Biol. 2015;35(7):1670–7. https://doi.org/10.1161/ATVBAHA.115.305363.
Dai D, Lu Q, Huang Q, Yang P, Hong B, Xu Y, et al. Serum miRNA signature in moyamoya disease. PLoS One. 2014;9(8):e102382. https://doi.org/10.1371/journal.pone.0102382.
Park YS, Jeon YJ, Lee BE, Kim TG, Choi JU, Kim DS, et al. Association of the miR-146aC>G, miR-196a2C>T, and miR-499A>G polymorphisms with moyamoya disease in the Korean population. Neurosci Lett. 2012;521(1):71–5. https://doi.org/10.1016/j.neulet.2012.05.062.
Kim JH, Jung JH, Phi JH, Kang HS, Kim JE, Chae JH, et al. Decreased level and defective function of circulating endothelial progenitor cells in children with moyamoya disease. J Neurosci Res. 2010;88(3):510–8. https://doi.org/10.1002/jnr.22228.
Jung KH, Chu K, Lee ST, Park HK, Kim DH, Kim JH, et al. Circulating endothelial progenitor cells as a pathogenetic marker of moyamoya disease. J Cereb Blood Flow Metab. 2008;28(11):1795–803. https://doi.org/10.1038/jcbfm.2008.67.
Kang HS, Moon YJ, Kim YY, Park WY, Park AK, Wang KC, et al. Smooth-muscle progenitor cells isolated from patients with moyamoya disease: novel experimental cell model. J Neurosurg. 2014;120(2):415–25. https://doi.org/10.3171/2013.9.JNS131000.
Navarro G, Borroto-Escuela DO, Fuxe K, Franco R. Potential of caveolae in the therapy of cardiovascular and neurological diseases. Front Physiol. 2014;5:370. https://doi.org/10.3389/fphys.2014.00370.
Frank PG, Woodman SE, Park DS, Lisanti MP. Caveolin, caveolae, and endothelial cell function. Arterioscler Thromb Vasc Biol. 2003;23(7):1161–8. https://doi.org/10.1161/01.ATV.0000070546.16946.3A.
Liu J, Wang XB, Park DS, Lisanti MP. Caveolin-1 expression enhances endothelial capillary tubule formation. J Biol Chem. 2002;277(12):10661–8. https://doi.org/10.1074/jbc.M110354200.
Chang SH, Feng D, Nagy JA, Sciuto TE, Dvorak AM, Dvorak HF. Vascular permeability and pathological angiogenesis in caveolin-1-null mice. Am J Pathol. 2009;175(4):1768–76. https://doi.org/10.2353/ajpath.2009.090171.
Bang OY, Chung JW, Kim SJ, Oh MJ, Kim SY, Cho YH, et al. Caveolin-1, ring finger protein 213, and endothelial function in moyamoya disease. Int J Stroke. 2016;11(9):999–1008. https://doi.org/10.1177/1747493016662039.
Chung JW, Kim DH, Oh MJ, Cho YH, Kim EH, Moon GJ, et al. Cav-1 (caveolin-1) and arterial remodeling in adult moyamoya disease. Stroke. 2018;49(11):2597–604. https://doi.org/10.1161/STROKEAHA.118.021888.
Kim DY, Son JP, Yeon JY, Kim GM, Kim JS, Hong SC, et al. Infarct pattern and collateral status in adult moyamoya disease: a multimodal magnetic resonance imaging study. Stroke. 2017;48(1):111–6. https://doi.org/10.1161/STROKEAHA.116.014529.
Kawabe-Yako R, Ii M, Masuo O, Asahara T, Itakura T. Cilostazol activates function of bone marrow-derived endothelial progenitor cell for re-endothelialization in a carotid balloon injury model. PLoS One. 2011;6(9):e24646. https://doi.org/10.1371/journal.pone.0024646.
Kim MJ, Park KG, Lee KM, Kim HS, Kim SY, Kim CS, et al. Cilostazol inhibits vascular smooth muscle cell growth by downregulation of the transcription factor E2F. Hypertension. 2005;45(4):552–6. https://doi.org/10.1161/01.HYP.0000158263.64320.eb.
Golab-Janowska M, Paczkowska E, Machalinski B, Meller A, Kotlega D, Safranow K, et al. Statins therapy is associated with increased populations of early endothelial progenitor (CD133+/VEGFR2+) and endothelial (CD34-/CD133- /VEGFR2+) cells in patients with acute ischemic stroke. Curr Neurovasc Res. 2018;15(2):120–8. https://doi.org/10.2174/1567202615666180611120546.
Porter KE, Turner NA. Statins for the prevention of vein graft stenosis: a role for inhibition of matrix metalloproteinase-9. Biochem Soc Trans. 2002;30(2):120–6. https://doi.org/10.1042/.
Koizumi A, Kobayashi H, Liu W, Fujii Y, Senevirathna ST, Nanayakkara S, et al. P.R4810K, a polymorphism of RNF213, the susceptibility gene for moyamoya disease, is associated with blood pressure. Environ Health Prev Med. 2013;18(2):121–9. https://doi.org/10.1007/s12199-012-0299-1.
Noh HJ, Kim SJ, Kim JS, Hong SC, Kim KH, Jun P, et al. Long term outcome and predictors of ischemic stroke recurrence in adult moyamoya disease. J Neurol Sci. 2015;359(1-2):381–8. https://doi.org/10.1016/j.jns.2015.11.018.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bang, O.Y., Chung, JW., Kim, D.H. et al. Moyamoya Disease and Spectrums of RNF213 Vasculopathy. Transl. Stroke Res. 11, 580–589 (2020). https://doi.org/10.1007/s12975-019-00743-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-019-00743-6