Abstract
Lead exposure is one of the major environmental issues to alter the health and well being of man and animals. Blood being the easy target for lead intoxication shows prominent effects and alteration of several hematological parameters may be regarded as a bio indicator of lead intoxication. Blood lead levels above 10 μg/dL have been associated with numerous manifestations. Anaemia is reported after acute and chronic exposure of lead in both workers of lead factory and in laboratory animals, accomplished either through impairment of heme biosynthesis or by enhanced rate of blood cell destruction. This is confirmed by marked reductions in blood haemoglobin level and haematocrit value and echinocytic transformation of normal erythrocytes after lead exposure. The number of total leucocytes tends to increase with the increase in basophils, eosinophils and lymphocytes possibly due to direct toxic action of lead on leucopoiesis in lymphoid organs. High levels of lead inhibit aggregation of platelets both in human and rat blood. Lead induced changes in the red blood membrane include the changes in lipids and proteins profile of some membrane-associated enzymes or in ions transport mechanisms. The mechanism of lead toxicity may be due, in part, to disruption of calcium-mediated processes. The chronic exposure to lead can result in a drastic changes in the cholesterol and phospholipid content, hexose, hexosamine and sialic acid levels and membrane acetyl cholinesterase, NADH dehydrogenase and Na+–K+ ATPase levels. Moderate exercise, intake of methionine, glycine, curcumin, methionine, carotene and pectin enriched food and vitamin C could reduce the severity of lead toxicity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lead (Pb) has been recognized as one of the most emerging hazardous heavy metals among environmental pollutants (ATSDR 2007). Tons of lead is discharged from electric battery manufacturing, lead smelting, and mining activities, as well as internal combustion engines fuelled with leaded petroleum and lead bearing products, forming the primary sources of lead contamination. A recent report holds that 33 % of over 370 water samples from the top 26 cities of India tested positive from harmful content of lead (over 10 parts per billion); resulting mainly from PVC pipes used in plumbing, sanitation and agriculture (The Lead Group Inc. 2010). Lead exposure from conventional use of vermillion, lead enriched toys and paints are increasingly aggravating the situation.
Lead has been mined and used by mankind for 6000 years, and the history of lead poisoning is nearly 2500 years old (Hernberg 2000). In early days Romans used lead compounds for glazing pottery, and metallic lead for cooking utensils and piping. In middle ages, lead was widely used both for industrial, domestic, and medicinal purposes. Certain folk remedies for digestive ailments have been found to contain very high levels of lead. In new age i.e. during fifteenth to eighteenth centuries, especially in Europe and later in America, the use of lead and its compounds gained increased use in pottery, piping, shipbuilding, window making, the arms industry, pigments, and later book printing industries. This led to more exposure to lead compounds and subsequent entry of lead in food chain. Today, most bullets for shotguns, handguns, and rifles are made of a lead core surrounded by a copper or steel jacket to protect the lead from changing shape at high speeds. Lead is a key component in various cosmetics, the pigment in many paints, a sweet and sour condiment popular for seasoning and adulterating food; a wine preservative and reliable piping for the vast network plumbing and for making colourful toys for children. Lead is commonly used in painting and soldering and in making stained glass, jewellery, pottery, ammunition, or fishing sinkers. The addition of lead to gasoline is one of the greatest public health failures of the twentieth century. The current threshold for lead toxicity, defined as a blood lead level of 10 μg/dL, was adopted by the United States (US) Centers for Disease Control and Prevention (CDC) in 1991 and the World Health Organization in 1995.
In children the list of lead toxic effects includes intellectual deficits, reading problems, school failure and delinquent behaviour; all these effects have substantial public health impact and are apparently long lasting and irreversible. In adults it is associated with subsequent vascular mortality (Rossi 2008). Actually a large amount of lead and related elements like cadmium have been released into the environment due to mineral processing activities and have impacted water resources, soils, vegetables, and crops.
In some areas, this pollution is extremely hazardous to human health (Zhang et al. 2012). The most prominent effects are cognitive deficiencies in children, renal impairment, hypertension, cataracts, and reproductive problems such as miscarriage, stillbirth, and decreased fertility in men and women (Patrick 2006). Sciarillo et al. (1992), observed delinquent, antisocial and aggressive behaviours in human. According to Tanquerel des Planches (1850) abdominal pain and peripheral neuropathy are two significant symptoms of lead toxicity in man. This metal affects almost all major body organs, particularly the CNS. Various molecular, cellular and intracellular mechanisms including the generation of oxidative stress, ionic mechanism and apoptosis have been proposed to explain the toxicological profile of lead (Farhat and Khademi 2015).
Chronic exposure of lead compounds through inhalation or ingestion results in adverse effect on the blood, central nervous system, and cardio vascular system, kidneys and vitamin D metabolism. Children are particularly sensitive and exposure of lead can also result in reduced cognitive development and reduced growth. Adverse effect on human reproduction has also been reported. Lead compounds can be persistent in the environment and have the potential to accumulate in food chains. Lead is classified as possible human carcinogen based upon the fact that exposure of animals to high level of lead have produced cancer usually in kidneys.
One of the easy targets for lead toxicity is the hematological system (Mojzis and Nistiar 2001) and anemia is probably one of the most well-known toxic effects of lead. The haemolytic effect of lead is reported from the blood of smelter worker and from the individuals living around a lead releasing factory. The in vitro and in vivo studies with murine models also indicate the similar hemotoxic effect of lead.
This review attempts to elucidate the mechanism of action of lead and consequent haematological manifestations of lead toxicity in both human and in experimental animals.
Effect of Lead Toxicity on Non-human Animals
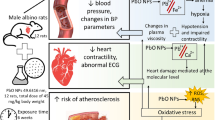
Since lead is a ubiquitous and naturally occurring metal, it can be mobilized and released into the environment at higher than background concentrations as a result of anthropogenic activity and exposure to elevated concentrations of lead from natural and human sources can be hazardous to wildlife (Scheuhammer and Norris 1995). Lead is one of the most studied toxicants, and found to be toxic to several physiological systems in vertebrates, including the nervous, renal, cardiovascular, reproductive, immune, and hematologic systems. In male Wistar rats, after 4 weeks, blood pressure responses to lead were biphasic. Low lead levels reduced blood pressure, dilated the carotid artery and increased cardiac output. At higher lead doses, rats had increased blood pressure (Wildemann et al. 2015).
The adverse effects are also well pronounced in lead exposed non-human vertebrates (Table 1), which are now being explored by the veterinarians and wildlife professionals to fully identify the lead exposure risks to mankind. Conservationists recognize that hunting, angling and shooting sports deposit thousands of tons of lead into the environment each year (Pokras and Kneeland 2009) and the flesh of the birds and animals hunted with lead enriched gun shots, become a source of lead poisoning of the human being. Lead can accumulate in invertebrates and plants, but its influence on food chain is yet to be discovered (Pattee and Pain 2003).
Absorption and Pharmacokinetics of Lead in Human
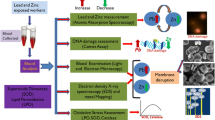
The pharmacokinetics of lead in humans is complex and its absorption is inversely proportional to chronologic age of the victim and the smaller the particle, the more completely the lead is absorbed. Thus, exposure to lead dust results in higher absorption than exposure to the equivalent amount of lead from chips of lead paint. The organic lead compounds (i.e. tetraethyl lead) are readily absorbed through intact skin. The majority (nearly 100 %) of lead inhaled as vapour or fumes is absorbed directly through the lungs. Although the blood generally carries only a small fraction of the total lead body burden, it serves as the initial receptacle of absorbed lead and distributes (Fig. 1) lead throughout the body, resulting in a number of physiological manifestations and also making it available to other tissues or for excretion. The elimination half-life of lead in adult human blood has been estimated to be 1 month, whereas in children it may be as high as 10 months. Blood lead is also important because the blood lead level (BLL) is the most widely used measure of lead exposure. The less sensitive erythrocyte protoporphyrin (EP) assay is also used as a measure of blood lead.
Lead in Blood
After lead is absorbed from the gastrointestinal tract or the lungs, it enters the blood stream and since lead is not converted to any acceptable or assimilable form, it remains stored as body “burden” of lead and about 95 % of the total body stores of lead are found in bone. In blood, about 99 % of lead remains in the red blood cells (RBC) and only 1 % in plasma with a half life of 28 days (US Department of Health and Human Services 2000). Systolic blood pressure (5.32 %, p = 0.05) and diastolic blood pressure (5.87 %, p = 0.05) were significantly increased in the automobile workers as compared to controls (Dongre et al. 2011). Valentine et al. (1976) documented the report of lead-induced deficiency when sufficiently severe gives rise to findings similar to the hereditary disorder.
Animals with lead-induced hypertension exhibited oxidative stress which was associated with mild up-regulation of superoxide-generating enzyme and NAD(P)H oxidase (Vaziri et al. 2003).
Mode of Action of Lead on Blood
Lead induced anaemia is produced principally by two mechanisms: impairment of heme biosynthesis and increased rate of blood cell destruction (Schwartz et al. 1990). Hemolytic anaemia may be induced by the inhibition of haemoglobin synthesis (Piomelli et al. 1982; Gurer et al. 1998). Previously, lead-induced anemia was considered to be resulted from the inhibition of δ-aminolevulinic acid dehydratase participating in the heme biosynthesis. However, little is known whether lead could affect the destruction of erythrocyte. In their study, Jang et al. (2011) demonstrated that lead could accelerate the splenic sequestration of erythrocytes through phosphatidylserine (PS) exposure and subsequently increased erythrophagocytosis (Table 2).
Although the precise mechanisms of action of lead toxicity are not clear, in vitro studies demonstrated that lead can interfere with fundamental biochemical processes which are accomplished by binding to proteins and/or interference with calcium dependent processes (Goldstein 1993). Hence, the mechanism of lead toxicity may be due, in part, to disruption of calcium-mediated processes which leads to neurotoxicity (Pounds 1984; Simons 1993). Lead activates protein kinase C in human erythrocytes after exposure to lead in vitro (Hwang et al. 2001). Such activation is evident from the erythrocytes isolated from workers in the lead industry and this may be directly relevant to the neurotoxicity of lead. Although the effects of Pb2+ on Ca2+ fluxes and calcium-regulated events have been suggested as major mechanisms involved in Pb2+ toxicity (Bressler et al. 1999; Marchetti 2003; Toscano and Guilarte 2005), other potential mechanisms include the capacity of Pb2+ to affect cell membrane composition. According to Kempe et al. (2005) exposure to Pb2+ ions at concentrations relevant for toxicity activates K+ channels, leading to K+ loss and erythrocyte shrinkage and favoring phosphatidylserine exposure at the surface of the cell membrane. The affected erythrocytes are removed from circulating blood that in turn leads to the development of anemia after Pb2+ intoxication. The study of Golalipour et al. (2007) on effect of lead intoxication showed that hematologic effects of lead are reversible and after recovery period, most of parameters were close to normal in 36 male adult albino Wistar rats. In brief, lead interferes with calcium and iron metabolism by forming complexes with sulfhydryl groups and other ligands, remaining at the active sites of the associated enzymes (Selevan et al. 2003). Slobozhanina et al. (2005) opined that low concentrations of lead did not produce reactive oxygen species in erythrocytes in vitro, but can change the physicochemical state of proteins and lipids in erythrocyte and lymphocyte membranes and thereby changes the functions of the receptors and channels present at the plasma membrane level resulting in the alteration in the molecular composition of the intracellular space and cell functions.
Biomarker of Lead Toxicity in Blood
In early days, basophilic stippling of red blood cells was considered as a classic sign of lead poisoning which is replaced by measurement of blood lead and zinc protoporphyrin levels for biological monitoring of lead-exposed workers (Cheson et al. 1984). Wibowo et al. (1979) found a relationship between blood lead (Pb–B) and lead manganese (Pb–Mn) concentration and the interaction between lead and manganese is mediated through a relationship between Pb and Mn porphyrin interactions in erythrocytes.
In laboratories, the titre of the lead affected enzymes involved in haem biosynthesis (Fig. 2) is measured to quantify the effect of lead on blood. These key enzymes are delta aminolevulinic acid dehydratase (ALAD) and haem synthetase, impaired synthesis of which reduces the concentration of delta aminolevulinic acid dehydratase (BLL of 5–10 μg/dL) and elevation of protoporphyrin in the RBC (BLL > 20 μg/dL) respectively. Since δ-aminolevulinic acid dehydratase (ALAD) activity in lead workers was inhibited by lead sensitively and stoichiometrically, ALAD activity may be adopted as a reliable biomarker of lead toxicity in human (Chiu et al. 2013).
Roels and Lauwerys (1987) studied the relations of PbB to heme synthesis biomarkers and reported no evident threshold for inhibition of aminolevulinic acid dehydratase synthesis at Pb as low as 8–10 µg/dL, while the threshold for increasing erythrocyte protoporphyrin levels was evident in the range of 15–20 µg/dL, consistent with other studies, including two meeting criteria for inclusion in this report (Rabinowitz et al. 1986; Hammond et al. 1985). Moreover, The NAD+, ATP, and NADP+ concentrations in erythrocytes seem to be the most sensitive indicators of the effects of Pb2+ on cell energy metabolism even at low levels of exposure (Baranowska-Bosiacka and Hlynczak 2004).
Since Karita et al. (2005) found lead exposure in all the workers was negatively associated with Hb, Hct, and RBC, after controlling for age and working status, these parameters may be recognized as nonspecific but useful markers of lead toxicity.
However, a marked change in the morphological, biochemical and numerical changes in blood cells resulted from chronic and acute exposure at lead.
Changes in Erythrocytes
Erythrocyte deformability (ED) is an important physiological factor which plays an essential role in delivery of oxygen to the tissues through bringing about significant changes in viscoelastic and geometric properties of the membrane accompanied by a change in internal viscosity (Mokken et al. 1992). Marked reductions in blood haemoglobin level, haematocrit value and erythrocyte count were observed after 1 and 2 weeks of intraperitoneal treatment of Swiss mice with lead nitrate (8 mg/kg for 5 consecutive days per week), as compared to the respective controls. Echinocytic transformation of many erythrocytes and the formation of a few microcytes, as revealed by both light and scanning electron microscopy, indicated the anaemia to be anisocytic and haemolytic in nature (Ray and Sarkar 2013). Such changes were confirmed by Ahyayauch et al. (2013), from a comparative study of chronically lead exposed erythrocytes, acutely lead exposed erythrocytes, and model membranes (LUV) concluded that in all cases lead increased membrane permeability and the overall membrane lipid order and brought about change in erythrocyte morphology, giving rise to macrocytic and echinocytic forms. Jang et al. (2011) also observed abnormal shape changes of erythrocytes and micro vesicle generation after exposure to Pb2+. The erythrocytes of the lead exposed individuals exhibited anisocytosis, moderate to marked hypochromasia and polychromasia, where many erythrocytes were coarsely or finely stippled. Basophilic stippling of red blood cells (BSC), formed by the inclusions of aggregated ribosomes, often mimicking the siderotic (iron) granules, Heinz bodies or even reticulocytes, has been noted in lead intoxication since 1899 (Cheson et al. 1984) and was considered a classic sign of lead poisoning.
Wistar rats fed with lead and chlorpyrifos showed Anisocytosis, a characteristic feature of moderate to severe anemia. (Ambali et al. 2011). Al-Ali and Abdula (2007) in 24 Balb/c mice found a significant decrease in hemoglobin concentration after acute and chronic lead exposure, that may be resulted from the effect of lead on the haemopoietic system may cause anemia which may result from shortened life span of erythrocytes that due to increase of their membrane fragility, and in another hand, it may cause a decreased hemoglobin synthesis which may result from decreased levels of enzymes involved in heme synthesis.
Previously, lead-induced anemia was considered to be from the inhibition of δ-aminolevulinic acid dehydratase participating in the heme biosynthesis (Jang et al. 2011). They demonstrated that lead could accelerate the splenic sequestration of erythrocytes through phosphatidylserine (PS) exposure and subsequently increased erythrophagocytosis. They found that the oral administration of Pb2+ increased phosphatidylserine exposure on erythrocytes in rat in vivo, leading to reduction of hematocrit and hemoglobin.
Reduction in RBCs, PCV, Hb, MCV, MCH and MCHC following exposure to lead acetate in rats revealed microcytic hypochromic anemia due to effect of lead on activity of α aminolevulinic acid dehydratase (ALAD), key enzyme of heme synthesis. Pb2+ inhibited the conversion of coproporphyrinogen III to protoporphyrin IX leading to reduction in haemoglobin production and shortened life span of erythrocytes (Klassen 2001). Progressive destruction of RBCs due to binding of Pb2+ with RBCs, resulted in the increase of cell fragility and destruction (Rous 2000).
However, cytochemical tests indicated that lead treatment did not interfere with utilization of iron for haemoglobin synthesis and hence did not cause denaturation of haemoglobin in already formed erythrocytes (Ray and Sarkar 2013).
Dongre et al. (2011) made an experiment with 30 automobile workers with occupational lead exposure and same number of healthy people with non-occupational lead exposure of same age as control from same place for hematological analysis. They found decreased non-activated erythrocyte δ-aminolevulinic acid dehydratase (δ-ALAD) and activated δ-ALAD levels in automobile workers as compared to control subjects. But the ratio of activated/nonactivated δ-ALAD was significantly increased (43.83 %) in automobile workers as compared to controls. In automobile workers heamoglobin, hematocrit, mean corpuscle volume, mean corpuscle hemoglobin, mean corpuscle hemoglobin concentration, red blood cell count were significantly decreased.
Although according to some reports (Tola 1975; Valentine et al. 1982; Grandjean et al. 1989; Romeo et al. 1996) stating that lead exposure did not negatively correlate with Hb levels, and Hb tended to increase with the elevated blood lead in Israeli industrial workers (Froom et al. 1999). Makino et al. (1997) found a significant positive relationship between blood lead and Hb count among 1573 workers with BPbs of 0.05–1.88 μmol/L.
Erythrocyte microrheology changes were measured using cation-osmotic hemolysis (COH) in healthy rats and rats after 6 and 12 months of lead ingestion (Mojzis and Nistiar 2001), where by using COH, properties of two membrane constituents, spectrine membrane skeleton and membrane bilayer were studied. COH in rats after 12 months of lead ingestion was found significantly lower only in the area with lower ionic strength.
Erythrocyte nucleotidase has been shown to be inhibited by low concentrations of lead in vitro (Paglia et al. 1975). Since blood and erythrocyte lead are virtually synonymous (Albahary 1972), the most lead-sensitive proteins of the erythrocyte remain affected so far the blood lead levels remain elevated. Severe lead-induced deficiency when gives rise to findings similar to the hereditary disorder, whereas pyrimidine-containing nucleotides are virtually absent in the erythrocytes of normal and reticulocyte-rich blood, 12 % of erythrocyte nucleotides in the blood of a patient with lead intoxication contained cytidine. Nucleotidase activity was about 25 % that in normal erythrocytes and 15 % or less of that expected in comparable reticulocyte-rich blood. The distribution of nucleotidase activity in patient erythrocytes is unknown and much more severe deficiency could have been present in subsets of the cell populations analyzed (Valentine et al. 1976). Genetically determined deficiency of this enzyme is associated with chronic hemolysis, marked basophilic stippling of erythrocytes on stained blood films, and unique intra erythrocytic accumulations of pyrimidine-containing nucleotides.
Changes in Leucocytes
Acute and chronic feeding of lead nitrate resulted in the elevation of total WBC count (Shah and Altindog 2005; Al-Ali and Abdula 2007) with the increase in basophils, eosinophils and lymphocytes and females were more hematologically affected with lead compared to males (Al-Ali and Abdula 2007). Patients with a high level of blood lead were reported to have relatively high number of these types of white blood cells (Al-Temimi et al. 2002).
In automobile workers of Karnataka having regular exposure to lead, increased total white blood cell count as compared to the controls was found (Dongre et al. 2011). Analysis total leucocytes count and differential leukocyte count revealed leucopenia and lymphopenia in lead exposed male and female adult rats (Suradkar et al. 2009). Although no significant change was observed in neutrophil, eosinophil, basophil and monocyte count in any treatment groups, the total lymphocyte count decreased significantly. This was probably due to direct toxic action of lead on leucopoiesis in lymphoid organs or increased lysis due to presence of lead in the body (Avadheshkumar et al. 1998).
In Swiss albino mice, Ray and Sarkar (2013) observed a marked change in TC and DC of leucocytes, where TC of leucocytes was considerably decreased along with a fall in the DC of lymphocytes but with an increase in the number of neutrophils. This led the authors to conclude that chronic lead treatment might gradually exert a cytotoxic action on both lymphopoietic and myelopoietic tissues, resulting in a marked leucopenia in the treated mice.
Sharma et al. (2012) studied the alterations in different types of white blood cells (WBC) due to chronic lead acetate toxicity in neonates after feeding lead acetate to Swiss mice from 10th day of gestation to 21th day of lactation fed on a standard diet and water ad libitum and concluded that lead induced hematological disorders in white blood cells were neutrophilic degeneration, formation of immature cells, abnormal neutrophils, reactive and plasmacytoid lymphocyte, reactive monocyte etc. Lead also caused fluctuations in the number of various cell types at different stages of postnatal development.
Changes in platelets
López et al. (1992) found high levels of lead inhibit aggregation of platelets both in human and rat blood although rat platelets were about ten times more sensitive to the effect of lead than that of in human. According to Ohyashiki et al. (1991), the platelet membrane is highly vulnerable to oxidative stress than the erythrocyte membrane. The levels of platelet count (PLT), plateletcrit (PCT) and mean platelet mass (MPM) were significantly decreased and platelet distribution width (PDW), platelet large cell ratio (P-LCR) and mean platelet volume were increased with an increase in blood lead levels as a result of lead–lead exposure in 429 male workers, serving in acid battery plant process (Barman et al. 2014) this might be the cause of impairment of coagulation function after endothelial tissue injury in these workers.
The thrombocytopenia in male Wistar rats, orally administered with lead and chlorpyrifos might be due to oxidative damage to the platelet membranes. This resulted in the formation of lipid peroxides within the platelet membranes thereby provoking cellular lysis (Ambali et al. 2011) and drop in platelet count.
Biochemical Changes
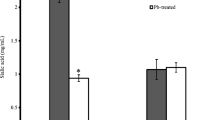
It was found that lead induced changes in the red blood membrane lipids and proteins (Jehan and Motlag 1995; Bellom-Ohvi et al. 1996), in the activity of some membrane-associated enzymes (Jehan and Motlag 1995) or in ions transport mechanisms (Calderon-Sahnas et al. 1999). Furthermore, it was documented that chronic exposure to lead can result in an erythrocyte deformability decrease (Honguchi et al. 1991; Terayama 1993) resulting in anaemia. Jehan and Motlag (1995) found that lead induced drastic changes in the cholesterol and phospholipid content, hexose, hexosamine and sialic acid levels and activities of the erythrocyte membrane enzymes—acetyl cholinesterase (AChE), NADH dehydrogenase and Na+–K+ ATPase. Valentine et al. (1976) in the blood of a 26-year-old Mexican–American spray painter, found although the total and differential leukocyte count and blood platelets were normal, but a moderately severe persistent anaemia with reticulocytosis ranging from 9.5 to 24 %. In lead intoxication, porphyrin was also found to accumulate in the erythrocytes, but in the form of zinc protoporphyrin (ZPP) (Lamola et al. 1975).
Lead intoxication is accompanied by a genetically determined acquired deficiency of erythrocyte pyrimidine-specific, 5′-nucleotidase as depicted by the influence of Pb ions on energy metabolism of erythrocytes in rats and consequent alterations in the concentration of high energy purine nucleotides and their derivative (Baranowska-Bosiacka et al. 2004). These rats were found to suffer from chronic hemolysis, marked basophilic stippling of erythrocytes on stained blood films, and unique intra erythrocytic accumulations of pyrimidine-containing nucleotides. The findings indicate that the hemolytic anemia and increased basophilic stippling characteristic of certain cases of lead intoxication might share a common etiology with essentially identical features of the genetically determined disorder (Valentine et al. 1976). Lead was found to cause a decrease of the high-energy purine nucleotide concentrations in erythrocytes and an increase in the products of their catabolism.
Effect of Acute and Chronic Exposure
Pb2+ effects on red blood cells after acute treatments reproduce faithfully the effects of chronic intoxication except that acute effects require lead concentrations 2–3 orders of magnitude higher. Liposomes exhibited a similar sensitivity to Pb2+ than erythrocytes in acute treatments. The parallelism between membrane effects of Pb2+ in the three systems under study reflects that the data are relevant to human intoxication by lead. In particular the observation that exposure to low (1–2 μM) Pb2+ concentrations for extended periods of time has the same effects on membranes to that of acute treatments with 50–500 μM Pb2+ supports the contention that the data in this paper can be at the origin of certain signs, e.g. anaemia, of lead intoxication in humans (Ahyayauch et al. 2013).
From an epidemiologic study in 1974 to assess the association between blood lead level and hematocrit in 579 1 to 5-year-old children living near a primary lead smelter Schwartz et al. (1990) found that blood lead levels ranged from 11 to 164 μg/dL. They found a strong non-linear, dose–response relationship between blood lead level and hematocrit and this relationship was influenced by age but was independent of iron deficiency. These findings suggested that blood lead levels close to the currently recommended limit value of 1.21 μmol/L (25 μg/dL) are associated with dose-related depression of hematocrit in young children.
Effect of occupational lead-exposure on the gene expression (Sod1) and activity (SOD) of superoxide dismutase, catalase and glutathione peroxidase (GPx, Gpx1) of leukocytes and erythrocytes of healthy male employees of a lead–zinc works resulted in increased expression of Sod1 and Gpx1 in erythrocytes whereas SOD activity in leukocytes was raised only in the subgroups having low exposure to lead (Kasperczyk et al. 2012). The environmental lead exposure in blood inhibits delta-aminolevulinic acid dehydratase activity (ALA-D) from whole blood, tested in 241 urban mothers and their newborns (Campagna et al. 1999).
Remedial Measures
Results of the experiments with Male Sprague–Dawley rats showed that lead administration reduced blood superoxide dismutase (SOD), glutathione peroxidase (GPx) and catalase (CAT) and increased Tumour Necrosis factor (TNF-α); in the controls, but in the exercise group, changes were not statistically significant. Although malondialdehyde (MDA) in both groups increased after lead injections but it was significantly lower in exercise group compared to the sedentary animals, from which Mohammadi et al. (2013) concluded that voluntary exercise might be considered as a preventive tool against lead-induced oxidative stress and inflammation. Modulation of cellular thiols for protection against reactive oxygen species (ROS) has been used as a therapeutic strategy against lead poisoning (Flora et al. 2012).
The role of amino acids and other nutrients in fighting lead poisoning were studied thoroughly by LEAD Group Incorporated ABN (2010). According to their report, other nutrients that have influence on lead level are methionine, glycine, curcumin, methionine, carotene and pectin, and nutrients found in garlic. From animal studies it was found that garlic could reduce blood and tissue lead levels, probably by the sulfur-based compounds essential for amino acid construction and antioxidant function, including methionine. Cysteine, at high concentration, reversed the effect of the metals. d-Penicillamine (d-P) was a chelator drug which is used for treatment of lead toxicity for several years but is no longer in use for its side effects. Chelation can be effective at reducing the total lead body burden and is critical in managing acute toxicity. The preferred chelating agent is Succimer. Ambali et al. (2011) opined that Vitamin C was able to mitigate the anemia induced by co-exposure to CPF and lead through the improvement of iron absorption (Naidu 2003) and reduction of lipoperoxidative damage of the erythrocyte membranes. Salawu (2010) opined that tomato could prevent some major adverse effects of lead intoxication on blood constituents.
Owolabi et al. (2012) studied the regenerative effect of Moringa oleifera extract on hematological parameters in lead intoxicated and control adult Wistar rat and found that the extract could reduce the severity of lead toxicity. Flora et al. (2012) pointed that the chelation therapy and newer therapeutic strategies, like nanoencapsulation, to treat lead induced toxic manifestations.
Genetic Susceptibility to Lead Intoxication
Onalja and Claudio (2000) reported the involvement of three very important polymorphic genes influencing susceptibility to lead exposure. Inhibition of erythrocyte δ-ALAD was considered as sensitive indicator of lead exposure. Kelada et al. (2001) described eight variants of this gene but with one polymorphism that yields two polymorphic alleles—ALAD-1 and ALAD-2, imparting susceptibility to lead toxicity. It was found that individuals homozygous for the ALAD-1 allele have a higher body burden of lead and may be at a higher risk of the long term effects of lead. In a case study of a 30-year old male working in a lead acid battery factory for over 6 years, Bijoor and Venkatesh (2007) found that despite very high levels of blood lead (82.8 and 47.5 μg/dL), the patient was asymptomatic with unaffected blood parameters. From detail analysis with PCR-based genotyping followed by an electrophoretic technique, Bijoor and Venkatesh (2007) concluded that some polymorphic genes of ALAD must be operative and confirmed the fact that the effect of lead and the appearance of signs and symptoms of lead poisoning are genetically determined.
Conclusion
Lead has a more severe effect on the blood-forming system in iron deficient people. Globally, governments have undertaken a broad spectrum of regulatory initiatives, both domestically and through international collaboration, to reduce human and ecological exposure to lead and other hazardous chemicals. While progress varies from country to country, it is generally acknowledged that collectively, these measures are contributing to improvements in human health.
Generally young children and expectant mothers, suffering from iron deficiency are more susceptible to lead intoxication than the adult men. Because the combination of iron deficiency and lead exposure cause more severe effects on the blood forming system than either condition alone, women and children tend to show more severe effects. Blood lead level was significantly higher in the exposed workers with anemia than in those without anemia, intake of iron enriched nutrients and food supplemented with sulphur containing amino acids may improve the situation. However, consciousness about the sources of lead poisoning is a pre requisite to avoid the health hazards associated with acute and chronic lead exposure.
References
Ahyayauch, H., W. Sansar, A. Rendon-Ramǐreza, F.M. Goni, Md. Bennouna, and H. Gamrani. 2013. Effects of chronic and acute lead treatments on the biophysical properties of erythrocyte membranes, and a comparison with model membranes. FEBS Open Bio 3: 212–217.
Al-Ali, S.J.K., and A.F. Abdula. 2007. Effect of acute and chronic lead nitrate exposure on some physiological parameters in experimental mice. Basic Journal of Veterinary Research 6(2): 78–88.
Albahary, C. 1972. Lead and hemopoiesis. The mechanism and consequences of the erythropathy of occupational lead poisoning. American Journal of Medicine 52: 367–378.
Al-Temimi, F.A., P. George, and V. Ankarath. 2002. A case of recurrent abdominal pain. SQU Journal for Scientific Research: Medical Science 4(1): 49–53.
Ambali, S.F., M. Angani, M. Shittu, and Md.U. Kawu. 2011. Hematological changes induced by subchronic co-administration of chlorpyrifos and lead in Wistar rats: Alleviating effect of vitamin C. Der Pharmacia Sinica 2(2): 276–284.
ATSDR (Agency for Toxic Substances and Disease Registry). 2007. Case studies in environmental medicine (CSEM) lead toxicity course: WB 1105.
Avadheshkumar, R.S. Chauhan, and N.P. Singh. 1998. Immunopathological effect of lead on cell mediated immunity in chicken. Indian Journal of Veterinary Pathology 22(1): 22–25.
Baranowska-Bosiacka, I., and A.J. Hlynczak. 2004. Effect of lead ions on rat erythrocyte purine content. Biological Trace Element Research 100: 1–15.
Baranowska-Bosiacka, I., A.J. Hlynczak, B. Wiszniewska, and M. Marchlewicz. 2004. Disorders of purine metabolism in human erythrocytes in the state of lead contamination. Polish Journal of Environmental Studies 13(5): 467–476.
Barman, T., R. Kalahasthi, and H.R. Rajmohan. 2014. Effects of lead exposure on the status of platelet indices in workers involved in a lead-acid battery manufacturing plant. Journal of Exposure Science and Environmental Epidemiology 24(6): 629–633.
Behrens, J., and J. Brooks. 2000. Wind in their wings: The condor recovery program. Endangered Species Bulletin 25: 8–9.
Bellom-Ohvi, L., M. Annadata, G.W. Goldstein, and J.P. Bressler. 1996. Phosphorylation of membrane proteins in erythrocytes treated with lead. Biochemical Journal 315: 401–406.
Bijoor, A.R., and T. Venkatesh. 2007. Genetic susceptibility to lead poisoning—A case report. Indian Journal of Clinical Biochemistry 22(2): 162–163.
Bressler, J., K.A. Kim, T. Chakraborti, and G. Goldstein. 1999. Molecular mechanisms of lead neurotoxicity. Neurochemistry Research 24: 595–600.
Burco, J., A.M. Myers, K. Schuler, and C. Gillin. 2012. Acute lead toxicosis via ingestion of spent ammunition in a free-ranging cougar (Puma concolor). Journal of Wildlife Diseases 48(1): 216–219.
Burger, J., and M. Gochfeld. 2005. Effects of lead on learning in herring gulls: An avian wildlife model for neurobehavioral deficits. Neurotoxicology 26(4): 615–624.
Calderon-Sahnas, J.V., M.A. Quintanar-Escorza, C.E. Hernandez-Luna, and M.T. Gonzales-Martmez. 1999. Effect of lead on the calcium transport in human erythrocyte. Human Experimental Toxicology 18: 146–153.
Campagna, D., G. Huel, F. Girard, J. Sahuquillo, and P. Blot. 1999. Environmental lead exposure and activity of δ-aminolevulinic acid dehydratase (ALA-D) in maternal and cord blood. Toxicology 134(2–3): 143–152.
Camus, A.C., M. Mark, D. Mitchelaln, and J.E. Williams. 1998. Elevated lead levels in farmed american alligators Alligator mississippiensis consuming nutria Myocastor coypus meat contaminated by lead bullets. Journal of the World Aquaculture Society 29: 370–376.
Cheson, B.D., W.N. Rom, and R.C. Webber. 1984. Basophilic stippling of red blood cells: A non-specific finding of multiple etiology. American Journal of Industrial Medicine 5: 327.
Chiu, Y.W., T.Y. Liu, and H.Y. Chuang. 2013. The effects of lead exposure on the activities of δ-amino levulinic acid dehydratase with the modification of the relative genotypes. In E3S Web of conferences, vol. 1, 26005.
Church, M.E., R. Gwiazda, R.W. Risebrough, K. Sorenson, C.P. Chamberlain, S. Farry, W. Heinrich, B.A. Rideout, and D.R. Smith. 2006. Ammunition is the principal source of lead accumulated by California condors re-introduced to the wild. Environmental Science and Technology 40: 6143–6615.
Clark, A.J., and A.M. Scheuhammer. 2003. Lead poisoning in upland-foraging birds of prey in Canada. Ecotoxicology 12: 23–30.
Craighead, D., and B. Bedrosian. 2008. Blood lead levels of common ravens with access to big-game offal. Journal of Wildlife Management 72(1): 240–245.
Cruz-Martinez, L., P.T. Redig, and J. Deen. 2012. Lead from spent ammunition: a source of exposure and poisoning in bald eagles. Human-Wildlife Interactions 6: 94–104.
De Francisco, N., J.D. Ruiz Troya, and E.I. Agüera. 2003. Lead and lead toxicity in domestic and free living birds. Avian Pathology 32(1): 3–13.
Dongre, N.N., N. Adinath, A. Suryakar, J. Patil, J.G. Ambekar, and D.B. Rathi. 2011. Biochemical effects of lead exposure on systolic and diastolic blood pressure, heme biosynthesis and hematological parameters in automobile workers of north Karnataka (India). Indian Journal of Clinical Biochemistry 26(4): 400–406.
Farhat, A.S., and G. Khademi. 2015. Blood lead level and seizure: a narrative review. Reviews in Clinical Medicine 2(2): 84–87.
Fisher, I.J., D.J. Pain, and V.G. Thomas. 2006. A review of lead poisoning from ammunition sources in terrestrial birds. Biology of Conservation 131(3): 421–432.
Flora, G., D. Gupta, and A. Tiwari. 2012. Toxicity of lead: A review with recent updates. Interdisciplinary Toxicology 5(2): 47–58.
Franson, J.C. 1996. Interpretation of tissue lead residues in birds other than waterfowl. In Environmental contaminants in wildlife–Interpreting tissue concentrations, ed. W.N. Beyer, G.H. Heinz, and A.W. Redmon-Norwood, 265–279. Boca Raton, FL: CRC.
Froom, P., E. Kristal-Boneh, J. Benbassat, R. Ashkanazi, and J. Ribak. 1999. Lead exposure in battery-factory workers is not associated with anemia. Journal of Occupational and Environmental Medicine 41: 120–123.
Gangoso, L., P. Álvarez-Lloret, A.B. Alejandro, R. Navarro, R. Mateo, F. Hiraldo, and J.A. Donázar. 2009. Long-term effects of lead poisoning on bone mineralization in vultures exposed to ammunition sources. Environmental Pollution 157: 569–574.
Golalipour, M.J., D. Roshandel, G. Roshandel, S. Ghafari, M. Kalavi, and K. Kalavi. 2007. Effect of lead intoxication and d-penicillamine treatment on hematological indices in rats. International Journal of Morphology 2S(4): 717–722.
Goldstein, G.W. 1993. Evidence that lead acts as a calcium substitute in second messenger metabolism. Neurotoxicology 14: 97–102.
Grandjean, P., B.M. Jensen, S.H. Sando, P.J. Jørgensen, and S. Antonsen. 1989. Delayed blood regeneration in lead exposure: An effect on reserve capacity. American Journal of Public Health 79: 1385–1388.
Gurer, H., H. Ozgunes, R. Neal, D.R. Spitz, and N. Ercal. 1998. Antioxidant effects of N acetylcysteine and succimer in red blood cells from lead exposed rats. Toxicology 128: 181–182.
Hammond, P.B., R.L. Bornschein, and P.A. Succop. 1985. Dose–effect and dose–response relationships of blood lead to erythrocytic protoporphyrin in young children. Environmental Research 38: 187–196.
Hernberg, S. 2000. Lead poisoning in a historical perspective. American Journal of Industrial Medicine 38: 244–254.
Holem, R.R., W.A. Hopkins, and L.G. Talent. 2006. Effect of acute exposure to malathion and lead on sprint performance of the western fence lizard (Sceloporus occidentalis). Archives of Environment Contamination Toxicology 51(1): 111–116.
Honguchi, S., S. Matsumura, K. Fukumoto, I. Karai, G. Endo, K. Teramoto, K. Shmagawa, I. Kiyota, F. Wakitam, and S. Takise. 1991. Erythrocyte deformability in workers exposed to lead. Osaka City Medical Journal 37: 149–155.
Hwang, K.Y., B.S. Schwartz, B.K. Lee, P.T. Strickland, A.C. Todd, and J.P. Bressler. 2001. Associations of lead exposure and dose measures with erythrocyte protein kinase C activity in 212 current Korean lead workers. Toxicological Sciences 62: 280–288.
Jang, W.H., K.M. Lin, K. Kim, J.Y. Noh, S. Kang, Y.K. Chang, and J.H. Chung. 2011. Low level of lead can induce phosphatidylserine exposure and erythrophagocytosis. Toxicological Science 122: 177–184.
Janssen, D.L., J.E. Oosterhuis, J.L. Allen, M.P. Anderson, D.G. Kelts, and S.N. Wiemeyer. 1986. Lead poisoning in free ranging California Condors. Journal of the American Veterinary Medical Association 189: 1115–1117.
Janssens, E., T. Dauwe, E. Van Duyse, J. Beernaert, R. Pinxten, and M. Eens. 2003. Effects of heavy metal exposure on aggressive behavior in a small territorial songbird. Archives of Environmental Contamination and Toxicology 45: 121–127.
Jehan, Z.S., and D.B. Motlag. 1995. Metal induced changes m the erythrocyte membrane of rats. Toxicological Letters 78: 127–133.
Karita, K., E. Yano, M. Dakeishi, T. Iwata, and K. Murata. 2005. Benchmark dose of lead inducing anemia at the workplace. Risk Analysis 25(4): 957–962.
Kasperczyk, A., G. Machnik, M. Dobrakowski, D. Sypniewski, E. Birkner, and S. Kasperczyk. 2012. Gene expression and activity of antioxidant enzymes in the blood cells of workers who were occupationally exposed to lead. Toxicology 301(1–3): 79–84.
Kelada, S.N., E. Shelton, R.B. Kaufmann, and M.J. Khoury. 2001. d-Aminolevulinic acid dehydratase genotype and lead toxicity. American Journal of Epidemiology 154(1): 1–13.
Kelly, T.R., and C.K. Johnson. 2011. Lead exposure in free-flying turkey vultures is associated with big game hunting in California. PLoS ONE 6(4): e15350. doi:10.1371/journal.pone.0015350.
Kempe, D.S., P.A. Lang, K. Eisele, B.A. Klarl, T. Wieder, S.M. Huber, C. Duranton, and F. Lang. 2005. Stimulation of erythrocyte phosphatidylserine exposure by lead ions. American Journal of Physiology and Cell Physiology 288: C396–C402.
Kenntner, N., F. Tataruch, and O. Krone. 2001. Heavy metals in soft tissue of White tailed Eagles found dead or moribund in Germany and Austria from 1993 to 2000. Environmental Toxicology and Chemistry 20: 1831–1837.
Klassen, C.D. 2001. Casarett and Doull’s toxicology: The basic science of poisons, 6th ed, 812–841. New York: McGraw-Hill.
Lamola, A.A., S. Piomelli, M.B. Poh-Fitzpatric, T. Yamane, and L.C. Harbor. 1975. Erythropoietic protoporphyria and lead intoxication: The molecular basis for difference in cutaneous photosensitivity. II. Different binding of erythrocyte protoporphyrin to hemoglobin. Journal of Clinical Investigation 56: 1528–1535.
LEAD Group Incorporated ABN. 2010. Fact sheet: Nutrients that reduce lead poisoning. 1–10. http://www.lead.org.au/fs/Fact_sheetNutrients_that_reduce_lead_poisoning_June_2010.pdf.
Li, W., S. Han, T.R. Gregg, F.W. Kemp, A.L. Davidow, D.B. Louria, A. Siegel, and J.D. Bogden. 2003. Lead exposure potentiates predatory attack behavior in the cat. Environmental Research 92: 197–206.
López, J.P., A. de la Peña, and G. Baños de MacCarthy. 1992. Effect of lead and cadmium on platelet aggregation. Archivo del Instituto de cardiologica de Mexico 62(4): 317–324.
Makino, S., Y. Shimizu, and T. Takata. 1997. A study on the relationship between blood lead levels and anemia indicators in workers exposed to low levels of lead. Industrial Health 35: 537–541.
Marchetti, C. 2003. Molecular targets of lead in brain neurotoxicity. Neurotoxicity Research 5: 221–236.
Mateo, R., R. Cadenas, M. Manez, and R. Guitart. 2001. Lead shot ingestion in two raptor species from Doñana, Spain. Ecotoxicology and Environmental Safety 48: 6–10.
Meretsky, V.J., N.F.R. Snyder, S.R. Beissinger, D.A. Clendenen, and J.W. Wiley. 2000. Demography of the California Condor: Implications for re-establishment. Conservation Biology 14: 957–967.
Mohammadi M., R. Ghaznavi, R. Keyhanmanesh, H. R. Sadeghipour, R. Naderi and H. Mohammadi. 2013. Exercise prevents lead-induced elevation of oxidative stress and inflammation markers in male rat blood. The Scientific World Journal 2013, Article ID 320704.
Mojzis, J., and F. Nistiar. 2001. Lead-induced changes of cation-osmotic hemolysis in rats. General Physiology and Biophysics 20: 315–319.
Mokken, F.C., M. Kedaria, C.P. Henny, M.R. Hardeman, and A.W. Gelb. 1992. The clinical importance of erythrocyte deformability, a hemorrheological parameter. Annals of Hematology 64: 113–122.
Naidu, K.A. 2003. Vitamin C in human health and disease is still a mystery? An overview. Nutrition Journal 2: 7–16.
Ohyashiki, T., M. Kobayashi, and K. Mashi. 1991. Oxygen-radical-mediated lipid peroxidation and inhibition of ADP-induced platelet aggregation. Archives of Biochemistry and Biophysics 228: 282–286.
Onalja, A.O., and L. Claudio. 2000. Genetic susceptibility to lead poisoning. Environmental Health Perspective 108(1): 23–28.
Owolabi, J.O., E. Opoola, and E.A. Caxton-Martins. 2012. Healing and prophylactic effects of Moringa oleifera leaf extract on lead induced damage to haematological and bone marrow elements in adult Wistar rat models. Open Access Scientific Reports 1: 386. doi:10.4172/scientificreports.386.
Paglia, D.E., W.N. Valentine, and J.G. Dahlgren. 1975. Effects of low-level lead exposure on pyrimidine 5′-nucleotidase and other erythrocyte enzymes. Possible role of pyrimidine 5′-nucleotidase in the pathogenesis of lead-induced anemia. The Journal of Clinical Investigation 56: 1164–1169.
Patrick, L. 2006. Lead toxicity, a review of the literature: Part I: Exposure, evaluation, and treatment. Alternative Medicine Review 11: 2–22.
Pattee, O.H., and D.J. Pain. 2003. Lead in the environment. In Handbook of ecotoxicology, 2nd ed, ed. D.J. Hoffman, B.A. Rattner, G.A. Burton Jr, and J. Cairns Jr, 373–408. New York, NY: Lewis Publishers.
Piomelli, S., C. Seaman, D. Zullow, A. Curran, and B. Davidow. 1982. Threshold for lead damage to heme synthesis in urban children. Proceedings of National Academy of Sciences USA 79: 3335–3339.
Platt, S.R., K.E. Helmick, J. Graham, R.A. Bennett, L. Phillips, C.L. Chrisman, and P.E. Ginn. 1999. Peripheral neuropathy in a Turkey Vulture with lead toxicosis. Journal of the American Veterinary Medical Association 214: 1218–1220.
Pokras, M.A., and R. Chafel. 1992. Lead toxicosis from ingested fishing sinkers in adult Common Loons (Gavia immer) in New England. Journal of Zoo and Wildlife Medicine 23: 92–97.
Pokras, M.A., and M.R. Kneeland. 2009. Understanding lead uptake and effects across species lines: A conservation medicine based approach. In Ingestion of lead from spent ammunition: implications for wildlife and humans, ed. R.T. Watson, M. Fuller, M. Pokras, and W.G. Hunt, 7–22. Boise, ID: The Peregrine Fund.
Pounds, J.G. 1984. Effect of lead intoxication on calcium homeostasis and calcium-mediated cell function: A review. Neurotoxicology 5: 295–332.
Rabinowitz, M.B., A. Leviton, and H.L. Needleman. 1986. Occurrence of elevated protoporphyrin levels in relation to lead burden in infants. Environmental Research 39: 253–257.
Ray, R.R., and N.K. Sarkar. 2013. Lead (Pb) induced anaemia in swiss mice-light and scanning electron microscopic studies. International Journal of Pharma and Bio Sciences 4(1B): 22–30.
Roels, H.A., and R. Lauwerys. 1987. Evaluation of dose–effect and dose–response relationships for lead exposure in different Belgian population groups (fetus, child, adult men and women). Journal of Trace Elements in Medicine and Biology 4(2): 80–87.
Romeo, R., C. Aprea, P. Boccalon, D. Orsi, B. Porcelli, and P. Sartorelli. 1996. Serum erythropoietin and blood lead concentrations. International Archives of Occupational and Environmental Health 69: 73–75.
Rossi, E. 2008. Low level environmental lead exposure—A continuing challenge. Clinical and Biochemical Review 29: 63–70.
Rous, P. 2000. The effect of heavy metals boundary contaminated soil on haematological and selected biochemical parameters in blood plasma of rabbits. Acta-Universitatis-Agriculturae-et-Silviculturae-Mendelianae-Brunensis 48(3): 93–99.
Salawu, E.O. 2010. Lycopersicon esculentum (tomato) prevents adverse effects of lead on blood constituents. Malaysian Journal of Medical Science 17(3): 13–18.
Scheuhammer, A.M., and S.L. Norris. 1995. A review of the environmental impacts of lead shotshell ammunition and lead fishing weights in Canada. Canadian Wildlife Service Occasional. Paper No. 88, Ottawa, Canada.
Schwartz, J., P.J. Landrigan, E.L. Baker, W.A. Orenstein, and I.H. von Lindern. 1990. Lead-induced anemia: Dose–response relationships and evidence for a threshold. American Journal of Public Health 80(2): 165–168.
Sciarillo, W.G., G. Alexander, and K.P. Farrell. 1992. Lead exposure and child behavior. American Journal of Public Health 82: 1356–1360.
Selevan, S.G., D.C. Rice, K.A. Hogan, S.Y. Euling, A. Pfahles-Hutchens, and J. Bethel. 2003. Blood lead concentration and delayed puberty in girls. The New England Journal of Medicine 348(16): 1527–1536.
Shah, S.L., and A. Altindog. 2005. Alteration in the immunological parameters Tench (Tinca tinca L. 1758) after acute and chronic exposure to lethal and sublethal treatments with mercury, cadmium and lead. Turkish Journal of Veterinary and Animal Sciences 29: 1163–1168.
Sharma, R., K. Panwar, and S. Mogra. 2012. Effects of prenatal and neonatal exposure to lead on white blood cells in Swiss mice. Journal of Cell and Molecular Biology 10(1): 33–40.
Sidor, I.F., M.A. Pokras, A.R. Major, R.H. Poppenga, K.M. Taylor, and R.M. Miconi. 2003. Mortality of common loons in New England, 1987–2000. Journal of Wildlife Diseases 39: 306–315.
Sileo, L., and S.I. Fefer. 1987. Paint chip poisoning of Laysan Albatross at Midway Atoll. Journal of Wildlife Diseases 23: 432–437.
Simons, T.J. 1993. Lead–calcium interactions in cellular lead toxicity. Neurotoxicology 14: 77–85.
Slobozhanina, E.I., N.M. Kozlova, L.M. Lukyanenko, O.B. Oleksiuk, R. Gabbianelli, D. Fedeli, G.C. Caulini, and G. Falcioni. 2005. Lead-induced changes in human erythrocytes and lymphocytes. Applied Toxicology 25(2): 109–114.
Stauber, E., N. Finch, P.A. Talcott, and J.M. Gay. 2010. Lead poisoning of bald (Haliaeetus leucocephalus) and golden (Aquila chrysaetos) eagles in the U.S. inland Pacific northwest region—An 18-year retrospective study: 1991–2008. Journal of Avian Medicine and Surgery 24(4): 279–287.
Suradkar, S.G., D.J. Ghodasara, P. Vihol, J. Patel, V. Jaiswal, and K.S. Prajapati. 2009. Haemato-biochemical alterations induced by lead acetate toxicity in Wistar rats. Veterinary World 2(11): 429–431.
Tanquerel des Planches, L. 1850. Lead diseases: A treatise. Boston, MA: Tappan, Whittemore and Mason.
Terayama, K. 1993. Effects of lead on electrophoretic mobility, membrane sialic acid, deformability and survival of rat erythrocytes. Industrial Health 31: 113–126.
Tola, S. 1975. Occupational lead exposure in Finland: IV. The polyvinyl chloride plastic industry. Scandinavian Journal of Work, Environment and Health 1: 173–177.
Toscano, C.D., and T.R. Guilarte. 2005. Lead neurotoxicity: From exposure to molecular effects. Brain Research Reviews 49: 529–554.
US Department of Health and Human Services. (2000). WHO Training Package for the Health Sector. http://ec.europa.eu/health/ph_projects/2003/action3/docs/2003_3_09_a11_en.pdf.
Valentine, W.N., D.E. Paglia, K. Fink, and G. Madokoro. 1976. Association with hemolytic anemia, basophilic stippling, erythrocyte pyrimidine 5′-nucleotidase deficiency, and intraerythrocytic accumulation of pyrimidinase. Journal of Clinical Investigation 58: 926–932.
Valentine, J.L., R.W. Baloh, B.L. Browdy, H.C. Gonick, C.P. Brown, G.H. Spivey, and B.D. Culver. 1982. Subclinical effects of chronic increased lead absorption—A prospective study. Part IV. Evaluation of heme synthesis effects. Journal of Occupational Medicine 24: 120–125.
Vaziri, N.D., C.Y. Lin, F. Farmand, and R.K. Sindhu. 2003. Superoxide dismutase, catalase, glutathione peroxidase and NADPH oxidase in lead-induced hypertension. Kidney International 63(1): 186–194.
Wayland, M., and T. Bollinger. 1999. Lead exposure and poisoning in bald eagles and golden eagles in the Canadian Prairie Provinces. Environmental Pollution 104(3): 341–350.
Wibowo, M.D., H.J.A. Sallé, P. del Castilho, and R.L. Zielhuis. 1979. An effect of erythrocyte protoporphyrin on blood manganese in lead-exposed children and adults. International Archives of Occupational and Environmental Health 43(3): 177–182.
Wildemann, T.M., N. Mirhosseini, S.D. Siciliano, and L.P. Weber. 2015. Cardiovascular responses to lead are biphasic, while methyl mercury, but not inorganic mercury, monotonically increases blood pressure in rats. Toxicology 328: 1–11.
Zhang, X., L. Yang, Y. Li, H. Li, W. Wang, and B. Ye. 2012. Impacts of lead/zinc mining and smelting on the environment and human health in China. Environmental Monitoring and Assessment 184: 2261–2273.
Zook, B.C., J.L. Carpenter, and E.B. Leeds. 1969. Lead poisoning in dogs. Journal of American Veterinary Medical Association 155(8): 1329–1342.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ray, R.R. Haemotoxic Effect of Lead: A Review. Proc Zool Soc 69, 161–172 (2016). https://doi.org/10.1007/s12595-015-0160-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12595-015-0160-9