Abstract
Coronary microvascular dysfunction (CMD) is a prevalent cause of ischemic heart disease and is associated with poorer quality of life and worse patient outcomes. Both functional and structural abnormalities of the microcirculation can generate ischemia in the absence of epicardial stenosis or worsen concomitant obstructive coronary artery disease (CAD). The invasive assessment of CMD allows for the evaluation of the entirety of the coronary vascular tree, from the large epicardial vessels to the microcirculation, and enables the study of vasomotor function through vasoreactivity testing. The standard evaluation of CMD includes vasomotor assessment with acetylcholine, as well as flow- and resistance-derived indices calculated with either thermodilution or Doppler guidewires. Tailored treatment based upon the information gathered from the invasive evaluation of CMD has been demonstrated to reduce the burden of angina; therefore, a thorough understanding of these procedures is warranted with the aim of improving the quality of life of the patient. This review summarizes the most widespread approaches for the invasive evaluation of CMD, with a focus on patients with ischemia and non-obstructive CAD.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Myocardial ischemia is a leading cause of morbidity and mortality. Historically, epicardial coronary artery stenoses have been considered the central cause of this pathological condition. However, coronary microvascular dysfunction (CMD) is acknowledged as an important contributor to myocardial ischaemia. CMD refers to a broad spectrum of structural and functional disorders affecting the coronary microcirculation, subsequently leading to coronary blood flow impairment in response to increased myocardial oxygen demand. The condition can affect small pre-arterioles and arterioles, which are the main drivers of coronary flow resistance, and responsible for the regulation and distribution of flow to the underlying myocardium, but also to the capillary network. CMD can coexist with epicardial coronary artery disease (CAD), in conjunction with other cardiovascular conditions, such as cardiomyopathies and valvular diseases. Nevertheless, it can also occur in the absence of significant epicardial CAD or structural heart disease.
Recently, studies have highlighted the importance of CMD as a cause of ischemia without obstructive epicardial stenoses (ischemia with non-obstructive coronary arteries, INOCA) in patients routinely investigated in clinical practice. Patients with INOCA frequently experience a high burden of symptoms with a reduced quality of life, repeated hospitalizations, and unnecessary diagnostic procedures in both the short and long terms. In an effort to improve the management of patients with INOCA, consensus documents have been published with the aim of standardizing definitions and providing evidence-based guidance.1
An appropriate evaluation of the coronary microcirculation and vasomotor function is key for the optimal management of INOCA. The coronary microcirculation is beyond the resolution of conventional invasive coronary angiography (0.5 mm). Therefore, alternative diagnostic procedures are warranted. Although several non-invasive modalities allow for the assessment of CMD, invasive evaluation remains the gold standard. Despite its obvious limitations and albeit low risks, the invasive approach has several advantages over non-invasive techniques, including the ability to exclude functionally significant epicardial CAD in the same procedure and the possibility to infuse intracoronary vasoactive agents, such as acetylcholine. For these reasons, the comprehensive assessment of patients with INOCA and its classification into endotypes cannot be properly performed without the invasive evaluation of the coronary artery vasculature; hence, this approach is endorsed by the current European and American guidelines of chronic coronary syndromes (CCS) and chest pain.2,3
In this review, we will revisit invasive tools for evaluation of CMD in the catheterization laboratory, in conjunction with a discussion on the technical aspects and value in daily clinical practice.
Evaluation of coronary vasomotor disorders
Vasoreactivity testing is used to assess endothelium-mediated vasodilation of the coronary arteries. At rest, myocardial oxygen extraction is almost maximal (≈80%), so tissue oxygen supply is largely dependent on coronary blood flow. Therefore, in instances of increased demand, the only way to match myocardial oxygen delivery is through increasing blood flow.
Coronary perfusion is dictated by the arterioles and small arterioles (< 400 μm) that make up most of the resistance circuit of the heart. The variations in vascular tone of these vessels is responsible for the regulation and distribution of blood flow in the underlying capillary bed. Continuous changes in smooth muscle tone allows for the maintenance of a constant blood flow across a wide range of perfusion pressures. Moreover, when myocardial oxygen demand increases, arteriolar vasodilation enables the matching of these requirements.4 In this setting, the vascular endothelium plays a central role. Endothelial cells integrate several stimuli, such as mechanical (shear stress), chemical (local oxygen concentration), and neurohormonal (acetylcholine) signals. These inputs lead to the production of nitric oxide (NO) and endothelium-derived hyperpolarizing factors which induce vasodilation of the vascular smooth muscle of large epicardial arteries and small arterioles.
The most widely utilized approach to explore endothelium-mediated vasodilation in the catheterization laboratory is with the intracoronary infusion of Acetylcholine (Ach).5 Normal healthy endothelial cells respond to Ach through liberation of vasoactive mediators that induce arteriolar vasodilation. However, in the presence of a dysfunctional endothelium failing to produce such mediators, Ach directly stimulates muscarinic receptors in smooth muscle cells, thereby inducing vasoconstriction.
Constriction of large epicardial vessels can be directly assessed with standard invasive coronary angiography or with the support of quantitative angiographic analysis. However, constriction of the small arterioles and quantification of coronary blood flow can only be indirectly measured with dedicated intracoronary wires.
Different approaches for vasoreactivity testing using Ach are available. In the ENCORE trials (Evaluation of Nifedipine and Cerivastatin On Recovery of coronary Endothelial function), continuous infusion with a mechanical pump and a microcatheter into the coronary artery was used.6,7 However, this technique is cumbersome and has been largely substituted with manual boluses of increasing concentrations of Ach. Although traditionally a maximal dose of 100 mcg for the left coronary artery (LCA) and 50 mcg for the right coronary artery (RCA) have been used, contemporary protocols using 200 mcg for the LCA and 100 mcg for the RCA have demonstrated increased sensitivity, without negatively impacting specificity.8 During Ach testing, bradycardia or transient atrio-ventricular (AV) block are frequent, yet normally not clinically relevant or harmful. Self-limiting atrial fibrillation has also been reported in up to 8% of procedures, especially if the RCA is evaluated.
In patients with angina referred for coronary angiography, the prevalence of vasomotor disorders is high. In the study by Pargaonkar et al., 68.1% of patients with angina and non-obstructive CAD exhibited endothelial dysfunction, defined as a > 20% narrowing in luminal diameter in response to intracoronary Ach administration. Additionally, in this study men appeared to demonstrate an increased response to Ach, in comparison to women.9 In another study, Ong et al. evaluated patients with angina and non-obstructive CAD, and the prevalence of vasoconstriction secondary to Ach was found to be similar (62%), with nearly half of the cases presenting as microvascular spasm.10
Epicardial coronary spasm is the cause of vasospastic angina (VSA), also known as Prinzmetal’s or variant angina. The standardized criteria for VSA definition include the presence of angina, ischemic electrocardiographic changes, and evidence of coronary spasm (> 90% of constriction in the epicardial vessels), either spontaneously or in response to a provocative stimulus.11 From a pathological standpoint, spasm is caused by a triggering stimulus that excites hyperreactive vascular smooth muscle cells. Several stimuli have been identified, but the precise mechanism of smooth muscle cells hyperreactivity is poorly understood.
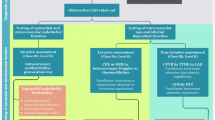
Despite being often regarded as a disease limited to the epicardial vessels, VSA is frequently associated with underlying disturbances in the coronary microcirculation. In the CORonary MICrovascular Angina (CorMiCa) trial, patients with INOCA were evaluated with vasoreactivity tests and an adenosine infusion to measure coronary flow reserve (CFR) and the index of microvascular resistance (IMR). In this study, 16.6% of patients had isolated VSA, while 20.5% presented with VSA in addition to CMD (defined as low CFR and/or high IMR).12 Additionally, Suda et al. identified that patients with VSA, who also exhibited high IMR (> 18), showed an increased incidence of major adverse cardiovascular event (MACE) than those with VSA and normal microvascular function.13 These findings emphasize that for a correct evaluation of patients with INOCA both epicardial vasomotor and microvascular function should be assessed (Figure 1).
Acetylcholine testing. Figure demonstrating the invasive physiological assessment of CMD and vasomotor disorders in a 65-year-old female, with repeated episodes of angina at rest. Coronary angiography identified no obstructive CAD. In Panel A and Panel B, baseline coronary angiography shows the wire advanced into the distal LAD and a resting ECG without repolarization abnormalities. Following the infusion of intracoronary acetylcholine (up to 200 mcg, Panel C and Panel D), the patient described chest pain with similar characteristics to her previous episodes, supported by an ECG with pronounced ST-segment depression in the anterior leads. Coronary angiography showed an absence of epicardial coronary spasm. After the infusion of intravenous adenosine, CFR and IMR were calculated, with normal values (Panel E). A final diagnosis of microvascular spasm was established
Alternatively, coronary vasomotor disorders can solely affect the microcirculation, with a relative sparing of large epicardial vessels. The standardized criteria for defining microvascular spasm include the presence of ischemic changes in the electrocardiogram and reproducibility of symptoms during acetylcholine testing, in the absence of epicardial spasm on coronary angiography.14 Although it has been less studied than VSA, its prevalence is almost equal as identified by Ong et al.10 Several pathogenic hypotheses exist, all of them placing endothelial dysfunction at the core. It is known that endothelial dysfunction is associated with cardiovascular risk factors,15 as well as with serum concentrations of asymmetrical dimethylarginine (an inhibitor of nitric oxide synthase)16 and decreased shear stress.17
State-of-the-art treatments for coronary vasomotor disorders focus on the use of calcium channel blockers to induce smooth muscle relaxation, but the association of endothelial dysfunction with modifiable risk factors may be a potential target for lifestyle changes and pharmacotherapy, specifically directed to improve the function of the vascular endothelium. Accordingly, statins and angiotensin-converting enzyme inhibitors might have a promising role in the management of this disease. Other drugs (e.g., endothelin receptor antagonists) are under investigation, and future trials are warranted to precisely address the benefits of these treatments on symptoms and prognosis.
Coronary flow-derived parameters
Measuring flow is critical for the accurate evaluation of coronary microvascular function. It is essential that a normal coronary circulation supplies sufficient blood flow to meet the myocardial demands of oxygen under resting conditions. In addition, during exertion or stress, the increase in the demand must be matched by a proportional increase in flow. This dynamicity of blood perfusion is one of the main singularities of the coronary vascular bed. A number of flow-derived parameters measured both at rest and during maximal hyperemia allow for the estimation of various indices that characterize microvascular function (Table 1).
Coronary flow reserve
Coronary flow reserve (CFR) is a physiological index which assesses the ability of the entire coronary bed (both the epicardial vessels and the microvasculature) to actively adapt its size to satisfy an increased oxygen demand from the myocardium. Thus, once severe obstructive disease of the epicardial arteries is ruled out, reduced CFR is one of the hallmarks of CMD.1 Measurements of CFR can be performed noninvasively, using transthoracic Doppler echocardiography,18 positron emission tomography (PET), or stress cardiac magnetic resonance (CMR). However, an invasive evaluation with either thermodilution or Doppler flow velocity is endorsed by the European Society of Cardiology (ESC) guidelines on CCS and the 2021 American Heart Association/American College of Cardiology Guideline for the Evaluation and Diagnosis of Chest Pain, with a IIa recommendation in patients with persistent symptoms and angiographically normal coronary arteries or with moderate non-flow-limiting stenosis.2,3
Invasive coronary function testing is usually performed in the LAD artery, as it provides perfusion to a larger myocardial mass. Still, additional studies in other coronary territories may be appropriate if the initial results are negative and clinical suspicion is high. Steady-state hyperemia is achieved with an endothelium-independent vasodilator, such as adenosine. An intravenous infusion of 140 µg⋅Kg⋅min is commonly used, although intracoronary boluses of up to 200 µg may be an alternative.19
CFR determination with thermodilution requires a pressure–temperature sensor guidewire (PressureWire X, Abbott Vascular, Santa Clara, CA). At least three consecutive intracoronary injections of saline at room temperature must be performed in order to calculate the time needed for the solution to travel from the tip of the guiding catheter to the distal temperature sensor of the wire, which is known as the mean transit time (Tmn). CFR is calculated from dividing resting Tmn by hyperemic Tmn (CFR = Tmn (rest)/Tmn (hyperemia)). The recommended cut-off value for thermodilution-based CFR, suggestive of CMD, is 2.0.20
CFR can also be calculated using a Doppler wire (ComboWire XT or Flowire, Philips Volcano Corporation, San Diego, CA, USA) as the ratio of the coronary flow velocity (CFV) in hyperemia to rest (CFR = CFVhyperemia/CFVrest). Studies assessing the prognostic role of CFR determined by Doppler have used cut-off values of 2.5 or lower.21 The process for CFR calculation using thermodilution and Doppler is depicted in Figures 2 and 3.
Regarding the prognostic yield of CFR, in a meta-analysis of 79 studies gathering 59,740 patients, Kelshiker et al. reported that an impaired CFR was related to a higher incidence of MACE in patients with acute coronary syndromes (ACS), heart failure, heart transplant, and diabetes. Moreover, it was associated with a higher all-cause mortality and MACE in patients without obstructive CAD.22 Concordant studies across non-invasive and invasive modalities support the notion that abnormal CFR confers a worse prognosis in terms of mortality and cardiac events, regardless of the presence or absence of flow-limiting CAD, and that the more severely impaired the global CFR is, the higher the risk.23,24
Absolute coronary flow
Although CFR is one of the standard physiological indexes to characterize CMD, it is not free from certain limitations: (1) It is indirectly estimated as a surrogate of true coronary flow; (2) its calculation requires the achievement of steady-state hyperemia with adenosine, which may be associated with several adverse effects25; (3) thermodilution may overestimate CFR at higher values and partly depends on operator’s injections, resulting in a large intra-observer variability; and (4) regarding Doppler-based measurements, obtaining a stable signal may be challenging.26
To overcome these drawbacks a novel method has been validated to directly quantify absolute coronary blood flow (Q), being safe, highly reproducible, and operator independent, without requiring adenosine administration.27 The technique is based on continuous thermodilution, achieving stable hyperemia by intracoronary infusion of saline at room temperature, at a rate of 20 mL⋅min with a dedicated monorail catheter (RayFlow, Hexacath, Paris, France). This double-lumen infusion catheter carries 4 lateral outer side holes through which saline can flow, providing homogenous mixing with blood, and 2 central holes between the outer and inner lumens to enable a measurement of the infusion temperature when the wire sensor is pulled back into the infusion catheter.28
Absolute Q in mL⋅min can be calculated according to the following formula:
where Qi represents saline infusion flow (20 mL⋅min), Ti stands for infusion temperature, and T is the mixing temperature.29 An example of this calculation is shown in Figure 4.
Continuous thermodilution for the calculation of absolute flow and resistance. Clinical case depicting the measurement of absolute coronary flow and resistance using continuous thermodilution. A dedicated monorail microcatheter (RayFlow, Hexacath, Paris, France) with lateral holes allows for the continuous infusion of saline (Panel A). This microcatheter is advanced over a pressure–temperature sensor guidewire (PressureWire X, Abbott Vascular, Santa Clara, CA, USA), positioned toward the distal LAD in a patient with diffuse epicardial atherosclerosis (Panel B). Then, a continuous infusion of saline is started at a rate of 20 ml⋅min. The distal tip of the wire will measure the mixing temperature (resulting from the combination of infused saline with blood). Subsequently, the sensor is withdrawn into the catheter to measure the infusion temperature. This data will allow for the calculation of absolute coronary flow (Q, L⋅min) and absolute coronary resistance (R, mmHg⋅L⋅min) (Panel C)
Nevertheless, the use of absolute Q in daily clinical practice has been hampered since its normal values are still a matter of debate. When exploring the relationship between absolute Q and the standard physiological indexes in the different endotypes of INOCA, Konst et al. defined low and high absolute Q based on the 50th percentile of the study population.30 In this work, absolute Q was not associated with positive or negative response to Ach, although a significant correlation between Q and CFR was found and low Q was reported as a predictor of angina severity. Also, a good correlation between continuous thermodilution-based absolute Q and [15O] H2O PET-derived flow measurement has been described.26 The main limitation of continuous thermodilution relates to the fact that it does not take into account the amount of myocardial mass of the perfusion territory, as well as a considerable inter-individual variability, limiting the use of these measurements for individual clinical decision-making.31 However, the association of this technique with non-invasive methods to quantify myocardial mass, such as computed tomography (CT) or CMR, has been proposed to compare CFR measurements among different myocardial territories and patients.32
Coronary resistance-derived parameters
As an elegant analogy to the founding role of Ohm’s law used in electrical circuits, the Hansen–Poiseuille’s law (and more deeply the Navier–Stokes equations) governs fluid dynamics. In all of these mathematical interpretations of physical phenomena, the concept of Resistance is established as the fundamental measurement of opposition to Flow.
Since the coronary microcirculation uses resistance as the key determinant of myocardial blood flow distribution, it is only natural that its estimation would become of interest, largely increasing the field of influence of coronary physiology and our understanding of patterns of microvascular disease.
As resistance cannot be measured directly, it must be estimated using the known relationships between flow and pressure and presented in the form of a mathematical index. As previously described, coronary flow can be estimated invasively using two different methods: Doppler and Thermodilution. From the combination of these measurements with intracoronary pressure estimations, numerous indices with the aim of evaluating the resistance to coronary flow can be derived.
Index of microcirculatory resistance
The Index of Microcirculatory Resistance (IMR) was firstly developed by Fearon et al. and is calculated from estimates of maximal distal coronary flow during hyperemia and pressure.33 In practice, using a pressure–temperature sensor guidewire and after obtaining coronary hyperemia, Tmn is calculated from the recorded thermodilution curves. To calculate IMR, the measured distal pressure (Pd) is multiplied by the Tmn, as shown in the following equation:
When compared with CFR, IMR is less dependent on hemodynamic conditions and can provide a more reproducible assessment of the microcirculation34 and, although a numeric division of a continuous variable has its understandable drawbacks, the cut-off of ≤ 25 is currently used for ‘normal’ and > 25 for increased microvascular resistance.35,36 In the presence of an epicardial stenosis, the subtended collateral flow might hinder the estimation of the ‘real’ resistance without invasively measuring the coronary wedge pressure (Pw).37 To address this matter, Yong et al. developed an equation to correct for the presence of a significant epicardial stenosis, as shown38:
There is ample evidence regarding the usefulness of IMR in the context of obstructive CAD. In the study by Echavarria-Pinto et al., an abnormal IMR was found in up to one-third of symptomatic patients with stable CAD and intermediate epicardial stenosis.39 In other studies, IMR showed no significant correlation with FFR,40 nor is it influenced by the angiographic severity of epicardial lesions.[41] This independence from upstream epicardial disease gives IMR some conceptual advantages. However, its prognostic role as an independent metric is still a matter of debate. In the recent meta-analysis by Kelshiker et al., the impact of an abnormal IMR on patient prognosis was much lower than an abnormal CFR (Hazard ratio for MACE of 1.02, compared with 3.4 for low CFR) and did not reach significance in a subgroup analysis (in CCS or ACS).22 Furthermore, in a study by Lee et al. of 867 patients, IMR was associated with MACE in a subgroup of patients with only an abnormal CFR.42 Promising results, however, have been reported in the context of ST-segment elevation myocardial infarction (STEMI), where IMR values after primary PCI correlate with a larger infarct size, lower left ventricular ejection fraction and less myocardial viability.43,44 Moreover, a high IMR after revascularization has been shown to be an independent predictor of death and hospitalization from heart failure.45
In the setting of patients with INOCA, Lee et al. conducted an invasive functional assessment of coronary microcirculation in 139 patients with exertional chest pain and normal epicardial arteries and identified the prevalence of high IMR to be approximately 21%.46 The recently published CorMiCa trial incorporated IMR as a marker of CMD, along with reduced CFR. This study identified that medical therapy resulted in a sustained improvement in anginal symptoms and a better quality of life, based on invasive functional assessments, including IMR.47
Hyperemic microvascular resistance
Hyperemic Microvascular Resistance (HMR) is a resistance index calculated from intracoronary Doppler flow velocity and distal pressure during hyperemia, following this equation48:
where Pd is the distal coronary pressure and CFV is Doppler-measured flow velocity during maximal hyperemia. HMR is measured in mmHg⋅cm⋅s, and values above 2.5 are considered abnormal.49
HMR only correlates modestly with IMR and CFR.50 HMR has been found to be abnormal in approximately 40% of patients with a normal CFR, due to significantly lower average peak velocity values at baseline.51 Combining CFR and HMR can enhance the comprehension of microcirculatory function as, owing to coronary autoregulation, CFR can still be within normal limits despite increased microvascular resistance. Patients with epicardial stenosis and high HMR values exhibit a greater degree of reversible ischemia than those with low HMR, as assessed by myocardial perfusion scintigraphy.52
In STEMI patients, similarly to IMR, increased HMR after successful primary PCI has been associated with higher burden of microvascular injury (measured on CMR) and worse outcomes.53 Conversely, the role of HMR in INOCA is less well established, with most studies focusing on the thermodilution-derived parameters (CFR, IMR). However, although recently the use of intracoronary Doppler has dropped significantly, these measurements are far from disappearing. Further research in the field of INOCA using Doppler-derived indices is expected in the near future.
Resistive reserve ratio
The Resistive Reserve Ratio (RRR) is an integrated index that uses thermodilution-derived CFR and coronary distal pressure (Pd), measured at rest and during hyperemia, and is calculated using the following equation54:
RRR reflects both the vasodilatory capacity of the coronary circulation and the disease burden of the interrogated vessel, in a novel concept to overcome the potential limitations of flow-derived and pressure-derived indices. Coronary Flow Capacity (CFC) was the first index to tackle this issue by combining CFR and an absolute measure of hyperemic coronary flow.55 However, CFC requires a two-step dimensional mapping process for interpretation, and clear cut-off values are yet to be defined.
In a prospective multicenter international registry enrolling 1245 patients with ACS and CCS, low RRR values (< 3.5) were found to be independently associated with long-term MACE, even in the presence of a normal CFR and FFR.56 Specifically relating to patients without obstructive CAD, a study by Toya et al. showed superior prognostic performance of RRR than CFR in predicting long-term survival.57 Whether RRR confers real prognostic advantage over CFR is yet to be determined by additional research.
Microvascular resistance reserve (MRR)
Overcoming some of the limitations of absolute Q, MRR has recently been proposed as a specific index of the microvasculature, independent of autoregulation and myocardial mass, and is based upon operator-independent measurements of absolute values of coronary flow and pressure.58 It is defined as the ratio of true resting to hyperemic microvascular resistance, expressed according to the following formula:
where Pa,rest and Pa,hyperemia represent aortic pressure at rest and at maximum hyperemia, respectively, Pd,hyperemia represents distal coronary pressure measured at hyperemia, and Qrest and Qmax are measured resting and hyperemic blood flow. Therefore, it can be also expressed in more general terms as the ratio of CFR to FFR, corrected for the driving pressures:
De Bruyne et al. reported a strong correlation between thermodilution-derived MRR and index values measured with Doppler. Furthermore, they confirmed that MRR is independent from epicardial resistance and the lower the resulting FFR value the greater the difference between MRR and CFR. However, MRR cut-off values, as well as the clinical and prognostic relevance of MRR compared with other established indices of microvascular function, are not established.58
Other indices
Instantaneous hyperemic diastolic velocity–pressure slope
The Instantaneous Hyperemic Diastolic Velocity–Pressure Slope (IHSVPS) was first proposed by Mancini et al. as an index to evaluate epicardial stenosis severity that was not as dependent on hemodynamics as CFR.59 This concept was later applied to the microcirculation by Escaned et al., using either aortic or distal pressure in the presence or absence of obstructive epicardial stenosis, respectively. IHDVPS is currently calculated as part of an intracoronary pressure–flow analysis using Pd and flow velocity during mid and end-diastole and provides an estimate of diastolic microvascular conductance (Figure 5). It was first validated in post-heart transplant patients, where it demonstrated a positive correlation with arteriolar obliteration and capillary rarefaction associated with allograft vasculopathy.60
Flow–pressure loops for the calculation of IHDPVS and microvascular conductance. An example of the calculation of epicardial and microcirculatory vascular conductance based on instantaneous hyperemic diastolic pressure velocity slopes (IHDPVS), derived from the pressure–flow velocity relationship. Panel A shows intracoronary Doppler measurements of hyperemic coronary flow velocity, in addition to a distal and aortic coronary pressure. Panel B shows a plot with hyperemic coronary flow velocity (Y-axis) and pressure (X-axis). IHDVPS is the slope of the pressure–flow relationship measured in mid to end-diastole and is expressed as a beta coefficient of a regression line, measured in cm⋅s⋅mmHg. Using distal coronary pressure (Pd) for its calculation, IHDVPSPd provides an estimation of microvascular conductance, whereas when using aortic pressure (Pa), IHDVPSPa estimates the overall vascular conductance. Separate assessment of epicardial conductance can be performed based on IHDVPSPa and IHDVPSPd (see text for details). Finally, the intercept of the slope with the X-axis provides a theoretical measurement of zero-flow pressure (Pzf), which has been used as a surrogate of extravascular microcirculatory compression. Cepi epicardial conductance, Cmicro microvascular conductance, Coverall overall vascular conductance (combination of epicardial and microvascular). Image taken with permission from N. Van Der Hoeven
Zero-flow Pressure
Zero-flow pressure (Pzf) is the measured pressure in the absence of coronary flow and is caused by the collapse of the coronary microcirculation due to extravascular compression.61 As such, it can also be used to diagnose microvascular injury and obstruction and it has been found to correlate with perfusion defects after primary PCI49 and infarct area extension in patients with STEMI.62 Currently, its direct measurement is not feasible. Therefore, it is extrapolated from the same pressure–flow loops used to estimate IHDVPS.63
Minimal microvascular resistance
As an alternative to traditional means-per-beat assessments of microcirculatory resistance, phasic analysis of the pressure–flow relationship during diastole can provide a better insight into myocardial perfusion. Minimal microvascular resistance (mMR) was proposed by de Waard et al. as a method to identify microvascular dysfunction during the wave-free period (similarly to the instantaneous wave-free ratio) in the IDEAL study.64 Because it is unaffected by obstructions in the conductance epicardial arteries, it has some theoretical advantages over other validated indices, such as CFR, HMR, or IMR.
Clinical implications
As discussed in the previous paragraphs, invasive tests allow for the interrogation of microvascular functionality from different perspectives. This is important, as derangements of microvascular function may occur in quite different clinical settings and through specific dysfunction pathways. As demonstrated in clinical trials in patients with CCS, outlining the presence of specific endotypes (vasomotor or structural) contributes to better control of angina by linking medical therapy to the results of functional invasive testing. In addition to this, the information obtained contributes to better risk stratification of patients, although randomized trials demonstrating a prognostic benefit of linked medical therapies are still lacking. The latter consideration applies in situations, such as STEMI, hypertensive heart disease, heart failure with preserved ejection fraction, allograft vasculopathy, and others. Yet, it is anticipated that positive evidence of microvascular derangements obtained in patients belonging to these subgroups will be used in the future to test the value of novel therapeutic approaches.
Conclusion
CMD has a high prevalence and extensive clinical implications in daily practice. Both functional and structural abnormalities of the microcirculation can generate ischemia in the absence of epicardial stenosis or worsen concomitant CAD in all of its presentations (from CCS to ACS, including STEMI). The invasive evaluation of CMD confers unique opportunities to evaluate the coronary vascular tree as a whole, from large epicardial vessels to the microcirculation, and allows for vasoreactivity testing. Comprehensive evaluation of CMD includes vasomotor assessment using acetylcholine, as well as flow-derived (CFR) and resistance-derived (IMR, HMR) indices. In addition, several additional parameters provide further information about the dynamic properties of the coronary vasculature, and relevant research in this field has been recently conducted. Current evidence highlights that the information gathered from this evaluation is essential for correct clinical decision-making, with the aim of improving patient’s symptoms and prognosis.
References
Kunadian V, Chieffo A, Camici PG, Berry C, Escaned J, Maas AHEM. An EAPCI Expert Consensus Document on Ischaemia with Non-Obstructive Coronary Arteries in Collaboration with European Society of Cardiology Working Group on Coronary Pathophysiology & Microcirculation Endorsed by Coronary Vasomotor Disorders International. Eur Heart J 2020;41:3504‐20.
Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, et al. 2019 ESC Guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J 2020;41:407‐77.
Gulati M, Levy PD, Mukherjee D, Amsterdam E, Bhatt DL, Birtcher KK, et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Guideline for the Evaluation and Diagnosis of Chest Pain: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation 2021;144:e368-454.
Johnson NP, Gould KL, De Bruyne B. Autoregulation of coronary blood supply in response to demand: JACC review topic of the week. J Am Coll Cardiol 2021;77:2335‐45.
Feenstra RGT, Seitz A, Boerhout CKM, Bukkems LH, Stegehuis VE, Teeuwisse PJI, et al. Principles and pitfalls in coronary vasomotor function testing. EuroIntervention 2022;17:1271‐80.
Lüscher TF, Pieper M, Tendera M, Vrolix M, Rutsch W, Van Den Branden F, et al. A randomized placebo-controlled study on the effect of nifedipine on coronary endothelial function and plaque formation in patients with coronary artery disease: The ENCORE II study. Eur Heart J 2009;30:1590‐7.
Luscher TF, Azancot I, Balbi M, Bonnier JJRM, Desmet W, Diederich KW, et al. Effect of nifedipine and cerivastatin on coronary endothelial function in patients with coronary artery disease: The ENCORE I study (evaluation of nifedipine and cerivastatin on recovery of coronary endothelial function). Circulation 2003;107:422‐8.
Sueda S, Kohno H, Ochi T, Uraoka T. Overview of the Acetylcholine Spasm Provocation Test. Clin Cardiol 2015;38:430‐8.
Pargaonkar VS, Lee JH, Chow EKH, Nishi T, Ball RL, Kobayashi Y, et al. Dose-response relationship between intracoronary acetylcholine and minimal lumen diameter in coronary endothelial function testing of women and men with angina and no obstructive coronary artery disease. Circ Cardiovasc Interv 2020;13:e008587.
Ong P, Athanasiadis A, Borgulya G, Mahrholdt H, Kaski JC, Sechtem U. High prevalence of a pathological response to acetylcholine testing in patients with stable angina pectoris and unobstructed coronary arteries. The ACOVA Study (Abnormal COronary VAsomotion in patients with stable angina and unobstructed coronary arteries). J Am Coll Cardiol 2012;59:655‐62.
Beltrame JF, Crea F, Kaski JC, Ogawa H, Ong P, Sechtem U, et al. International standardization of diagnostic criteria for vasospastic angina. Eur Heart J 2017;38:2565‐8.
Ford TJ, Stanley B, Good R, Rocchiccioli P, McEntegart M, Watkins S, et al. Stratified medical therapy using invasive coronary function testing in Angina: The CorMicA trial. J Am Coll Cardiol 2018;72:2841‐55.
Suda A, Takahashi J, Hao K, Kikuchi Y, Shindo T, Ikeda S, et al. Coronary functional abnormalities in patients with angina and nonobstructive coronary artery disease. J Am Coll Cardiol 2019;74:2350‐60.
Ong P, Camici PG, Beltrame JF, Crea F, Shimokawa H, Sechtem U, et al. International standardization of diagnostic criteria for microvascular angina. Int J Cardiol 2018;250:16‐20.
Gutiérrez E, Flammer AJ, Lerman LO, Elízaga J, Lerman A, Fernández-Avilés F. Endothelial dysfunction over the course of coronary artery disease. Eur Heart J 2013;34:3175.
Cziráki A, Lenkey Z, Sulyok E, Szokodi I, Koller A. L-Arginine-nitric oxide-asymmetric dimethylarginine pathway and the coronary circulation: translation of basic science results to clinical practice. Front Pharmacol 2020;11:1.
Kumar A, Hung OY, Piccinelli M, Eshtehardi P, Corban MT, Sternheim D, et al. Low coronary wall shear stress is associated with severe endothelial dysfunction in patients with nonobstructive coronary artery disease. JACC Cardiovasc Interv 2018;11:2072‐80.
Okura H, Fuyuki H, Kubo T, Iwata K, Taguchi H, Toda I, et al. Noninvasive diagnosis of ischemic and nonischemic cardiomyopathy using coronary flow velocity measurements of the left anterior descending coronary artery by transthoracic Doppler echocardiography. J Am Soc Echocardiogr 2006;19:552‐8.
Layland J, Carrick D, Lee M, Oldroyd K, Berry C. Adenosine: physiology, pharmacology, and clinical applications. JACC Cardiovasc Interv 2014;7:581‐91.
Lee JM, Jung JH, Hwang D, Park J, Fan Y, Na SH, et al. Coronary flow reserve and microcirculatory resistance in patients with intermediate coronary stenosis. J Am Coll Cardiol 2016;67:1158‐69.
AlBadri A, Bairey Merz CN, Johnson BD, Wei J, Mehta PK, Cook-Wiens G, et al. Impact of abnormal coronary reactivity on long-term clinical outcomes in women. J Am Coll Cardiol 2019;73:684‐93.
Kelshiker MA, Seligman H, Howard JP, Rahman H, Foley M, Nowbar AN, et al. Coronary flow reserve and cardiovascular outcomes: a systematic review and meta-analysis. Eur Heart J 2022;43:1582‐893.
Taqueti VR. Coronary flow reserve: A versatile tool for interrogating pathophysiology, and a reliable marker of cardiovascular outcomes and mortality. Eur Heart J 2022.
Patel KK, Spertus JA, Chan PS, Sperry BW, Al Badarin F, Kennedy KF, et al. Myocardial blood flow reserve assessed by positron emission tomography myocardial perfusion imaging identifies patients with a survival benefit from early revascularization. Eur Heart J 2020;41:759‐68.
Rahman H, Demir OM, Ryan M, McConkey H, Scannell C, Ellis H, et al. Optimal use of vasodilators for diagnosis of microvascular angina in the cardiac catheterization laboratory. Circ Cardiovasc Interv 2020;13:e009019.
Everaars H, de Waard GA, Driessen RS, Danad I, van de Ven PM, Raijmakers PG, et al. Doppler flow velocity and thermodilution to assess coronary flow reserve: A head-to-head comparison With [15O]H2O PET. JACC Cardiovasc Interv 2018;11:2044‐54.
Keulards DCJ, Veer MVT, Zelis JM, El FM, Zimmermann FM, De VA, et al. Safety of absolute coronary flow and microvascular resistance measurements by thermodilution. EuroIntervention 2021;17:229‐32.
Van’t Veer M, Adjedj J, Wijnbergen I, Tóth GG, Rutten MCM, Barbato E, et al. Novel monorail infusion catheter for volumetric coronary blood flow measurement in humans: In vitro validation. EuroIntervention 2016;12:701‐7.
Xaplanteris P, Fournier S, Keulards DCJ, Adjedj J, Ciccarelli G, Milkas A, et al. Catheter-based measurements of absolute coronary blood flow and microvascular resistance feasibility, safety, and reproducibility in humans. Circ Cardiovasc Interv 2018;11:e006194.
Konst RE, Elias-Smale SE, Pellegrini D, Hartzema-Meijer M, van Uden BJC, Jansen TPJ, et al. Absolute coronary blood flow measured by continuous thermodilution in patients with ischemia and nonobstructive disease. J Am Coll Cardiol 2021;77:728‐41.
Fournier S, Keulards DCJ, Van’t Veer M, Colaiori I, Di Gioia G, Zimmermann FM, et al. Normal values of thermodilution-derived absolute coronary blood flow and microvascular resistance in humans. EuroIntervention 2021;17:E309‐16.
Keulards DCJ, Fournier S, Van’t Veer M, Colaiori I, Zelis JM, Farissi El M, et al. Computed tomographic myocardial mass compared with invasive myocardial perfusion measurement. Heart 2020;106:1489‐94.
Fearon WF, Balsam LB, Farouque HMO, Robbins RC, Fitzgerald PJ, Yock PG, et al. Novel index for invasively assessing the coronary microcirculation. Circulation 2003;107:3129‐32.
Ng MKC, Yeung AC, Fearon WF. Invasive assessment of the coronary microcirculation: Superior reproducibility and less hemodynamic dependence of index of microcirculatory resistance compared with coronary flow reserve. Circulation 2006;113:2054‐61.
Melikian N, Vercauteren S, Fearon WF, Cuisset T, MacCarthy PA, Davidavicius G, et al. Quantitative assessment of coronary microvascular function in patients with and without epicardial atherosclerosis. EuroIntervention 2010;5:939‐45.
Luo C, Long M, Hu X, Huang Z, Hu C, Gao X, et al. Thermodilution-derived coronary microvascular resistance and flow reserve in patients with cardiac syndrome x. Circ Cardiovasc Interv 2014;7:43‐8.
Fearon WF, Aarnoudse W, Pijls NHJ, De Bruyne B, Balsam LB, Cooke DT, et al. Microvascular resistance is not influenced by epicardial coronary artery stenosis severity: Experimental validation. Circulation 2004;109:2269‐72.
Yong AS, Layland J, Fearon WF, Ho M, Shah MG, Daniels D, et al. Calculation of the index of microcirculatory resistance without coronary wedge pressure measurement in the presence of epicardial stenosis. JACC Cardiovasc Interv 2013;6:53‐8.
Echavarria-Pinto M, Escaned J, Macías E, Medina M, Gonzalo N, Petraco R, et al. Disturbed coronary hemodynamics in vessels with intermediate stenoses evaluated with fractional flow reserve: a combined analysis of epicardial and microcirculatory involvement in ischemic heart disease. Circulation 2013;128:2557‐66.
Lee JM, Layland J, Jung JH, Lee HJ, Echavarria-Pinto M, Watkins S, et al. Integrated physiologic assessment of ischemic heart disease in real-world practice using index of microcirculatory resistance and fractional flow reserve: Insights from the International Index of Microcirculatory Resistance Registry. Circ Cardiovasc Interv 2015;8:e002857.
Kobayashi Y, Lee JM, Fearon WF, Lee JH, Nishi T, Choi DH, et al. Three-vessel assessment of coronary microvascular dysfunction in patients with clinical suspicion of ischemia: Prospective observational study with the Index of Microcirculatory Resistance. Circ Cardiovasc Interv 2017;10:e005445.
Lee JM, Choi KH, Doh JH, Nam CW, Shin ES, Hoshino M, et al. Long-term patient prognostication by coronary flow reserve and index of microcirculatory resistance: International registry of comprehensive physiologic assessment. Korean Circ J 2020;50:890‐903.
Fearon WF, Shah M, Ng M, Brinton T, Wilson A, Tremmel JA, et al. Predictive value of the index of microcirculatory resistance in patients with ST-segment elevation myocardial infarction. J Am Coll Cardiol 2008;51:560‐5.
McGeoch R, Watkins S, Berry C, Steedman T, Davie A, Byrne J, et al. The index of microcirculatory resistance measured acutely predicts the extent and severity of myocardial infarction in patients with ST-segment elevation myocardial infarction. JACC Cardiovasc Interv 2010;3:715‐22.
Fearon WF, Low AF, Yong AS, McGeoch R, Berry C, Shah MG, et al. Prognostic value of the Index of Microcirculatory Resistance measured after primary percutaneous coronary intervention. Circulation 2013;127:2436‐41.
Lee BK, Lim HS, Fearon WF, Yong AS, Yamada R, Tanaka S, et al. Invasive evaluation of patients with angina in the absence of obstructive coronary artery disease. Circulation 2015;131:1054‐60.
Ford TJ, Stanley B, Sidik N, Good R, Rocchiccioli P, McEntegart M, et al. 1-year outcomes of angina management guided by invasive Coronary Function Testing (CorMicA). JACC Cardiovasc Interv 2020;13:33‐45.
Verhoeff BJ, Siebes M, Meuwissen M, Atasever B, Voskuil M, De Winter RJ, et al. Influence of percutaneous coronary intervention on coronary microvascular resistance index. Circulation 2005;111:76‐82.
Teunissen PFA, De Waard GA, Hollander MR, Robbers LFHJ, Danad I, Biesbroek PS, et al. Doppler-derived intracoronary physiology indices predict the occurrence of microvascular injury and microvascular perfusion deficits after angiographically successful primary percutaneous coronary intervention. Circ Cardiovasc Interv 2015;8:e001786.
Williams RP, de Waard GA, De Silva K, Lumley M, Asrress K, Arri S, et al. Doppler versus thermodilution-derived coronary microvascular resistance to predict coronary microvascular dysfunction in patients with acute myocardial infarction or stable angina pectoris. Am J Cardiol 2018;121:1‐8.
Yamanaga K, Tsujita K, Komura N, Kaikita K, Sakamoto K, Miyazaki T, et al. Physiological basis of discordance between coronary flow velocity reserve and hyperemic microvascular resistance for evaluating coronary microvascular dysfunction in patients without atherosclerotic obstruction. Int J Cardiol 2015;201:535‐7.
Nolte F, Van De Hoef TP, Meuwissen M, Voskuil M, Chamuleau SAJ, Henriques JPS, et al. Increased hyperaemic coronary microvascular resistance adds to the presence of myocardial ischaemia. EuroIntervention 2014;9:1423‐31.
Waard GA, Fahrni G, De Wit D, Kitabata H, Williams R, Patel N, et al. Hyperaemic microvascular resistance predicts clinical outcome and microvascular injury after myocardial infarction. Heart 2018;104:127‐34.
Layland J, Carrick D, McEntegart M, Ahmed N, Payne A, McClure J, et al. Vasodilatory capacity of the coronary microcirculation is preserved in selected patients with non-ST-segment-elevation myocardial infarction. Circ Cardiovasc Interv 2013;6:231‐6.
Hamaya R, Yonetsu T, Kanaji Y, Usui E, Hoshino M, Yamaguchi M, et al. Diagnostic and prognostic efficacy of coronary flow capacity obtained using pressure-temperature sensor-tipped wire–derived physiological indices. JACC Cardiovasc Interv 2018;11:728‐37.
Lee SH, Lee JM, Park J, Choi KH, Hwang D, Doh JH, et al. Prognostic implications of resistive reserve ratio in patients with coronary artery disease. J Am Heart Assoc 2020;9:e015846.
Toya T, Ahmad A, Corban MT, Özcan I, Sara JD, Sebaali F, et al. Risk stratification of patients with nonobstructive coronary artery disease using resistive reserve ratio. J Am Heart Assoc 2021;10:20464.
De Bruyne B, Pijls NHJ, Gallinoro E, Candreva A, Fournier S, Keulards DCJ, et al. Microvascular resistance reserve for assessment of coronary microvascular function: JACC Technology Corner. J Am Coll Cardiol 2021;78:1541‐9.
Mancini GBJ, McGillem MJ, DeBoe SF, Gallagher KP. The diastolic hyperemic flow versus pressure relation: A new index of coronary stenosis severity and flow reserve. Circulation 1989;80:941‐50.
Escaned J, Flores A, García-Pavía P, Segovia J, Jimenez J, Aragoncillo P, et al. Assessment of microcirculatory remodeling with intracoronary flow velocity and pressure measurements: Validation with endomyocardial sampling in cardiac allografts. Circulation 2009;120:1561‐8.
Bellamy RF. Diastolic coronary artery pressure-flow relations in the dog. Circ Res 1978;43:92‐101.
Patel N, Petraco R, Dall’Armellina E, Kassimis G, De Maria GL, Dawkins S, et al. Zero-flow pressure measured immediately after primary percutaneous coronary intervention for ST-segment elevation myocardial infarction provides the best invasive index for predicting the extent of myocardial infarction at 6 months: An OxAMI study. JACC Cardiovasc Interv 2015;8:1410‐21.
van der Hoeven NW, de Waard GA, Quirós A, de Hoyos A, Broyd CJ, Nijjer SS, et al. Comprehensive physiological evaluation of epicardial and microvascular coronary domains using vascular conductance and zero flow pressure. EuroIntervention 2019;14:E1593‐600.
de Waard GA, Nijjer SS, van Lavieren MA, van der Hoeven NW, Petraco R, van de Hoef TP, et al. Invasive minimal Microvascular Resistance is a new index to assess microcirculatory function independent of obstructive coronary artery disease. J Am Heart Assoc 2016;5:e004482.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Travieso was the recipient of a unrestricted research grant by Philips. Dr. Mejia-Renteria has received consultancy fees from Medis Medical Imaging and speaker fees from Philips and Abbott. Dr. Javier Escaned has received consultancy and speaker fees from Abbott and Philips. The other authors Adrian Jeronimo-Baza, Daniel Faria, and Asad Shabbir state that they do not have any conflict of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Travieso, A., Jeronimo-Baza, A., Faria, D. et al. Invasive evaluation of coronary microvascular dysfunction. J. Nucl. Cardiol. 29, 2474–2486 (2022). https://doi.org/10.1007/s12350-022-02997-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-022-02997-4