Abstract
We investigated how subjects with cerebellar ataxia (CA) adapt their postural stability and alignment to a slow and small tilt of the support surface allowing for online postural corrections. Eight subjects with CA and eight age- and gender-matched healthy control subjects participated in the study. Subjects stood eyes closed for 1 min after which the support surface was tilted 5° toes-up at a ramp velocity of 1°/s. The toes-up position was held for 2.5 min after which the surface rotated back down to level with identical tilt characteristics. As reflected by the large number of falls, subjects with CA had marked difficulty adapting their posture to the up-moving incline in contrast to control subjects. Subjects with CA who lost their balance had faster trunk velocity and excessive backward trunk reorientation beginning within the first second after onset of the tilting surface. In contrast, the down-moving tilt to level did not result in instability in CA subjects. These results suggest that instability and falls associated with CA derive from an inability to maintain trunk orientation to vertical while standing on a slow-moving or unstable surface. This study underscores the importance of the cerebellum in the online sensory control of the upper body orientation during small amplitude and slow velocity movements of the support surface.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Falls and postural instability are common in individuals with cerebellar ataxia [1, 2]. Cerebellar damage has shown to cause postural instability when standing on fast-moving surfaces with large perturbations [3–7]. Postural responses in patients with cerebellar disorders are hypermetric but with normal latencies and inability to scale response amplitudes to predicted perturbation amplitudes [4, 7, 8]. Such fast perturbations limit the possibility of corrections during movement execution so postural response scaling is based on sensory predictions, a key role of the cerebellum in motor control (internal model) [9, 10]. For example, in upper limb reaching, it has been shown that corrections occurring during movement cause error accumulation in subjects with cerebellar ataxia, which results in increased end-point errors [11].
The role of the cerebellum in postural stability when adapting to slow and small perturbations of the supporting surface remains poorly understood. When standing on a slow upward tilting surface of small amplitude, multiple postural adjustments must be made. These adjustments are especially important in ankle dorsiflexion and needs to be proportional to the surface motion to maintain upright balance. We have previously shown that healthy adults respond to this minor perturbation by maintaining trunk orientation to vertical while allowing ankle rotation during the surface motion, even with eyes closed [12]. Thus, it is not clear whether subjects with cerebellar ataxia, who are known to have difficulty walking or standing on an inclined surface and who accumulate errors with motor tasks, are able to correct their movement during slow movements to maintain postural stability.
In the present study, we investigated the role of the cerebellum in adapting to a slowly inclining surface during standing in subjects with cerebellar ataxia (CA) and healthy adults. We hypothesized that the cerebellum significantly contributes to this slow adaptation process involving a gradual recalibration of sensory information to optimize motor performance. Thus, it is expected that cumulative errors, due to multiple postural adjustments, would lead to decreased stability in subjects with CA standing on a slow inclining surface. Therefore, we expect that measures of segmental orientation, to maintain verticality, rather than postural stability as measured by sway would be more affected by a slow and small incline of the supporting surface.
Patients and Methods
Subjects
Eight subjects with CA (age 58 years [SD 7], height 169 cm [SD 11], and weight 77 kg [SD 14]) and eight age- and gender-matched healthy control subjects (age 57 years [SD 6], height 171 cm [SD 11], and weight 75 kg [SD 13]) participated in the study. Table 1 summarizes the diagnosis, onset, disease severity with the scale for the assessment and rating of ataxia (SARA) [13], and balance function in the subjects with CA. All subjects were screened with a health history evaluation to ensure that they were free of musculoskeletal and other neurological impairments that could affect postural control. All participants were ambulatory and did not require any assisting device. Prior to their participation in the experiment, all subjects gave their informed consent in accordance to the Institutional Review Board of the Oregon Health & Science University regulations and the Declaration of Helsinki.
Experimental Setup and Protocol
As illustrated in Fig. 1a, each trial consisted of a 1-min baseline period of quiet stance with eyes closed to avoid anticipation of the upcoming surface motion and to obtain a stable upright standing baseline. The force platform was then tilted 5° toes-up (Tilt-Up) at a ramp velocity of 1°/s. Surface tilts were driven by a computer-controlled hydraulic system, with the axis of surface rotation located at approximately ankle height. The surface tilted at a constant velocity with a cosine function at the start and end of the ramp to limit acceleration and create gradual, rather than abrupt, onset and offset of surface tilts, without activating short-latency, somatosensory-triggered destabilizing bursts of the gastrocnemius muscle [14–16]. The support surface was held in the up position (5°) for 2.5 min to allow subject to adapt to their posture to the incline surface. A Tilt-Down motion to bring back the foot position to a flat surface (0°) followed with the same displacement characteristics as the toes-up tilt (1°/s). All subjects maintained quiet stance on the stationary flat surface for a minimum of 3 min for them to stabilize their posture following the toes-up adaptation and slow Tilt-Down motion. Two trials were performed in all participants except for two of the CA subjects who only performed one trial due to excessive fatigue.
a Illustration of the surface position during one trial. The trials started with a 1-min baseline period of quiet stance followed by a 5° toes-up tilt. The support surface was held in the up position for 2.5 min and followed by a 5° toes-down tilt. Thereafter, the surface was held horizontal for a minimum of 3 min. Shaded areas represent the five, 45-s intervals before, during, and after the inclines used for analysis. b Representative example of the center of mass (COM) and center of pressure (COP) displacement during tilting in a representative subject with cerebellar ataxia (gray) and in a control subject (black). c Top row shows example stabilograms from a control and a cerebellar subject for the duration of each interval presented. Below are mean position and sway (i.e., 95 % confidence interval [CI]) of the COP during the five intervals. Data shown is from all subjects and all trials with intervals with loss of balance removed. Asterisk denotes significant differences of main effects
During each trial, the subjects stood upright on the force platform with their head facing forward, arms crossed, and wearing a blindfold ensuring that vision was occluded for the duration of the trial. Subjects stood with their bare feet spaced at comfortable width, at approximately hip width. The position of the feet was marked on the floor to ensure subjects were tested in the same position on all trials. Subjects wore a safety harness attached to an overhead beam to ensure safety during trials without providing directional/spatial cues for postural alignment. The subjects were instructed to “stand in a relaxed way and try to maintain your balance.” To further assure subject safety, a research assistant stood beside all subjects during each trial.
Measurements
Body kinematics were recorded at 60 Hz using an eight-camera motion analysis system (Motion Analysis, Santa Rosa, CA) and 22 retro-reflective markers placed bilaterally on the trunk, hips, legs, feet, and tilting surface. Marker positions were then used to calculate the orientation of body segment angles (shank, thigh, and trunk) on the right side of the body. The shank segment was defined from the lateral malleolus to the axis of rotation of the knee, the thigh segment from the axis of rotation of the knee to the greater trochanter, and the trunk segment from the greater trochanter to the seventh cervical vertebra. Segment angular velocity was obtained from the first derivative of the angular position.
Subjects stood on a custom-made dual-plate force platform with four vertical force sensors beneath each foot. Forces were sampled at 120 Hz, and the center or pressure (COP) was calculated from the combined vertical forces of each force plate [17]. COP data were low-pass filtered at 0.1 Hz using a dual-pass second-order Butterworth filter. For two CA subjects, collection of the force platform data failed. As illustrated in Fig. 1b, the center of mass (COM) closely followed the COP position; hence, COM data was used for these subjects.
Analyses
Each trial was coded as a loss of balance (LOB) or a non-loss of balance trial (No LOB). Trials were identified as LOB if the subject needed to be caught or touched by the research assistant and/or the safety harness to prevent falling, if the subject took one or more steps, or if the subject touched or held onto the research assistant. The time of onset of the LOB was detected by a sudden reduction in vertical forces as registered by the force plates and also visually, by analyzing video recordings of the sessions as well as with motion analysis data used for kinematic analysis. LOB occurred only in the CA group in 11/14 of the trials. Ten of these trials with LOB could be analyzed for kinematic strategy, COP displacement, and variability for up to the moment of LOB. The LOB in these 10 trials occurred after a minimum of 1.3 s (mean onset of LOB was 1.9 s); hence, sufficient data was available to analyze prior to LOB. After LOB, subjects were supported to recover balance and instructed to reposition the displaced foot so the trial could be continued. In order to analyze data for these trials post-LOB, the COP displacement was calculated in relation to the heels of the subjects for all trials. Thus, during trials with LOB involving a displacement of the feet, we could continue to quantify changes in COP displacement while excluding the LOB intervals.
Kinematic strategies were quantified from body segment displacements in response to the upward surface tilts by measuring the angular displacement and velocity of the shank, thigh, and trunk segment in the sagittal plane with respect to the gravity vertical reference. In addition, we measured peak backward angular displacement and velocity. This additional metric allowed for the comparison of trunk kinematics of all subject prior to any intervention from the assistant or reaction from the subjects (stepping or grasping).
Postural stability before, during, and after tilting was also quantified to determine if subjects adapted to each surface positions. The mean position and variability (i.e., standard deviation) of the COP are in the direction of the perturbation (i.e., the anterior-posterior direction). As illustrated in Fig. 1a, COP measures were obtained during five 45-s intervals: (1) before incline (baseline), (2) early and (3) later during the incline, and (4) early and (5) later after the returning to neutral position. These different intervals were selected to assess postural stability immediately after surface motions and after adaptation (or readaptation) to the new surface position.
Levene’s test for homogeneity of variances and Mauchleys Sphericity test were non-significant (p < 0.120) for the mean of COP during the intervals standing on a flat or inclined surface; therefore, a repeated measures analysis of variance [intervals × groups] and main effects were explored with Tukey HSD test. Due to the small sample size, non-parametric statistics (Mann-Whitney U test) were used to investigate differences between control and CA subjects that maintained or lost their balance. Spearman rank order correlation (r s) was used to investigate the relationship between the disease severity and loss of balance in the CA group. The significance level was set at p < 0.05.
Results
Postural Alignment Deficits with Cerebellar Ataxia
Subjects with CA showed marked difficulty in adapting their posture to a low-amplitude (5°) very slow (1°/s) up-moving incline, in contrast to control subjects who showed no difficulty performing the task, as seen in Table 2 and in Fig. 2. During Tilt-Up, in 11 (seven different individuals) out of 14 trials, subjects with CA needed to be caught or took a step in at least one of the trials attempted. Loss of balance occurred in every attempt in four subjects, on the first attempt only in one participant, and on the second trial only in one other subject (two subjects only performed one trial: one with and one without LOB). In contrast, standing on a Tilt-Down moving surface was not as challenging for subjects with CA in that subjects were caught or took a step in only two trials (two different individuals, one on the first and one on the second attempt). Control subjects easily adapted to the slowly moving surface as they remained stable in all trials. There was no relationship between loss of balance during the surface tilts and disease severity (total SARA score r s = −0.15, p > 0.05).
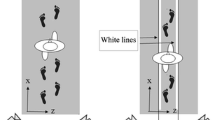
Examples of segment orientation (right-side markers illustrated only) in one control subject and one subject with cerebellar ataxia. Each data point represents the raw data at each second during the surface tilt corresponding to each degree of surface tilt-up rotation. The cerebellar subject lost balance and took a step (with the left foot). b Mean group segment orientation of the shank, thigh, and trunk segments are shown on the left at initial position (0°, light gray) and at 5° upward tilt of the surface in controls and subjects with cerebellar ataxia that maintained balance (No LOB, 3 trials in 3 different subjects). Subjects with cerebellar ataxia who lost their balance (LOB, 11 trials in 7 different subjects) are at 2° of upward tilt of the surface corresponding to pre-balance loss. On the right, mean shank (bottom), thigh (middle), and trunk (top) segment orientation at each degree (0° to 5°) during up-moving tilt of the surface in subjects with cerebellar ataxia who lost their balance (LOB, gray), who did not lose their balance (No LOB, dashed gray) and controls (black with gray shaded area corresponding to +/− SD of the control subject data)
Control subjects maintained balance on the up- and down-rotating surface with minimal change in their postural alignment except for ankle rotation that followed the surface motion (5°), e.g., an ankle strategy, in which ankle rotation was larger than the trunk motion described below. Subjects with CA who were able to maintain balance on the up-moving surface generated a hip strategy, as seen in Fig. 2b (No LOB). This hip strategy was expressed by a forward trunk tilt from initial position, combined with a backward tilt of the thigh segment. When subjects with CA lost their balance (No LOB) during the Tilt-Up incline, they reoriented their trunk backward instead of forward to maintain balance.
There was no difference in initial trunk, thigh, or shank segment orientation between groups (p > 0.05), and differences were only observed in trunk segment orientation (as reflected in Fig. 2b). In fact, during toes-up surface tilting, the peak trunk extension was larger in CA subjects who lost their balance (9°) in contrast to control subjects who only moved slightly (3°, U = 5, Z = 3.9353, p < 0.001). In addition, trunk peak extension velocity during the toes-up tilt was larger in CA subjects with loss of balance in contrast to control subjects (17.6 vs. 7.2 mm/s, U = 16, Z = 3.3942, p < 0.001).
Postural Stability on a Tilted Surface in Subjects with Cerebellar Ataxia
In all conditions, subjects with CA had larger COP sway, as measured by the standard deviation of their COP displacement, compared to control subjects (Fig. 1c). Sway was more than twofold that of control subjects (118 % larger with a main effect of group: F(1,12)=73.980 p < 0.001). Both subjects with CA and control subjects adjusted their COP position backward when standing on the incline (Fig. 1c [F(4,48) = 7.957, p < 0.05, incline (I and II) vs. baseline and the post-incline periods]).
Discussion
This study showed that adapting to a very slow, low-amplitude, toes up-tilting incline is compromised in subjects with cerebellar ataxia, as reflected by their hypermetric trunk extension responses, frequent loss of equilibrium. Postural control during these very slow surface rotations is not reflexive but involves online sensory feedback and integration from the somatosensory and vestibular systems.
Subjects with CA had more difficulty maintaining balance on an up- than down-moving surface rotation. These findings are consistent with previous studies showing that the backward moving direction (i.e., Tilt-Up) is most challenging for upright standing subjects with CA [4, 5]. The reason for more difficulty balancing during toes-up than during toes-down surface tilts is not known but may be related to the relative biomechanical difficulty in using tibialis anterior muscles and hip extensors to prevent backward displacement of the COM behind the heels compared to using gastrocnemius and soleus muscles and hip flexors to prevent forward displacement of the COM over the toes [18, 19]. Ankle range of motion in dorsiflexion is also smaller compared to plantarflexion [20], and the COP in normal upright stance is located more posteriorly than anteriorly in relation to the foot limits of stability [21]. In addition, the downward tilt in this experiment was a movement going from dorsiflexion to a neutral position and not an actual plantarflexion (i.e., not challenging the COP anteriorly) which could also explain the additional difficulty in maintaining balance in the up-moving surface rotation.
Interestingly, CA subjects more easily adapted to a fast-moving surface (60°/s) [4] in contrast to our slower tilt velocity protocol (1°/s), suggesting that subjects with CA have more difficulty regulating continuous sensory feedback control of postural orientation than in triggering a fast, automatic postural response [7]. Recent sensory feedback models explain the scaling of muscle activity due to perturbations at different accelerations and velocities [22]. The loss of equilibrium we observed in subjects with CA could be due to deficiencies in somatosensory and vestibular feedback processing and to inappropriate scaling of online postural corrections, especially in the trunk (i.e., accumulation of errors as observed in studies of upper-limb reaching [11]). Alternatively, use of vestibular input as a sensory reference for vertical orientation may have been compromised by impaired vestibulo-cerebellar function, which was not tested.
Falls in subjects with CA standing on a slow up-moving incline seemed to be caused by a change in postural alignment characterized by an early backward reorientation of the trunk segment. As illustrated in Fig. 2b, right panel, after 1° of upward surface tilt, cerebellar subjects who lost their balance showed large backward movements of the trunk and thigh, in contrast to control subjects and CA subjects who tilted their trunks forward to maintain balance. Early hypermetric shifts in the trunk segmental orientation in individuals with CA has previously been observed in trunk flexion during fast surface tilts [4, 7]. In the present study, an extension of the trunk was observed in subjects with CA that lost their balance while subjects who were able to maintain balance reoriented their trunk forward (Fig. 2b, right panel). This early extension of the trunk in subjects with CA might indicate an inability to coordinate multiple joints simultaneously resulting in lack of global control of the trunk in space [23, 24] and/or the result of error accumulation in postural alignment adjustments [11]. It is not clear whether the extension observed in the trunk is an active reorientation of the segment to follow the support surface or whether the lack of flexion adjustment in the trunk was responsible for the backward reorientation of the trunk segment leading to a loss of balance.
There was no difference in mean COP position between groups as both controls and subjects with CA adjusted their position to the incline similarly. Subjects with CA have been found to have increased sway in comparison to controls, and our findings are consistent with previous studies [3, 25, 26]. Postural sway in subjects with CA did not further increase when standing on the inclined surface. Together with the hypermetric trunk responses observed, increased sway variability may still further amplify a less favorable position to maintain postural equilibrium when orientation of the standing surface changes, especially if subjects with CA sway closer to their limits of stability.
The relatively small number of subjects and various etiologies of the subjects with CA limit the generalization of these results. Although we could not find a learning or familiarization pattern in our dataset, we cannot exclude that participants did not learn the task because of the limited number of trials and the same test order (flat, upward tilt, and tilt back down to flat). Future studies should investigate whether subjects with CA can learn to maintain balance with repeated trials and whether falls and postural instability in subjects with CA depend on the speed or amplitude of the surface perturbation. In addition, a better understanding of the role of the visual system in adapting to a slow moving support surface with CA would help provide important information that could help guide compensatory strategies in rehabilitation. Finally, it would also be relevant to determine whether the location of the cerebellar lesion affects the ability to maintain balance on a slow-moving support surface.
This study demonstrates that individuals with CA experience more falls arising more from an inability to maintain trunk orientation vertical when standing on a rotating surface rather than changes in postural sway. These hypermetric extension responses seem to be caused by a deficit in sensory feedback control during the online adaptation to slow and long perturbations likely resulting in error accumulation.
Abbreviations
- ABC:
-
Activities-specific Balance Confidence scale
- BESTest:
-
Balance Evaluation Systems Test
- CA:
-
Cerebellar ataxia
- COM:
-
Center of mass
- COP:
-
Center of pressure
- DTR:
-
Deep tendon reflex
- LOB:
-
Loss of balance
- MSA-C:
-
Multiple system atrophy cerebellar dysfunction subtype
- SAOA:
-
Sporadic adult-onset ataxia
- SARA:
-
Scale for the assessment and rating of ataxia
- SCA:
-
Spinocerebellar ataxia
References
van de Warrenburg BP, Steijns JA, Munneke M, Kremer BP, Bloem BR. Falls in degenerative cerebellar ataxias. Mov Disord. 2005;20:497–500.
Fonteyn EM, Schmitz-Hubsch T, Verstappen CC, Baliko L, Bloem BR, Boesch S, et al. Falls in spinocerebellar ataxias: Results of the EuroSCA Fall Study. Cerebellum. 2010;9:232–9.
Baloh RW, Jacobson KM, Beykirch K, Honrubia V. Static and dynamic posturography in patients with vestibular and cerebellar lesions. Arch Neurol. 1998;55:649–54.
Bakker M, Allum JH, Visser JE, Gruneberg C, van de Warrenburg BP, Kremer BH, et al. Postural responses to multidirectional stance perturbations in cerebellar ataxia. Exp Neurol. 2006;202:21–35.
Kung UM, Horlings CG, Honegger F, Kremer HP, Bloem BR, van De Warrenburg BP, et al. Postural instability in cerebellar ataxia: correlations of knee, arm and trunk movements to center of mass velocity. Neuroscience. 2009;159:390–404.
Oude Nijhuis LB, Hegeman J, Bakker M, Van Meel M, Bloem BR, Allum JH. The influence of knee rigidity on balance corrections: a comparison with responses of cerebellar ataxia patients. Exp Brain Res. 2008;187:181–91.
Horak FB, Diener HC. Cerebellar control of postural scaling and central set in stance. J Neurophysiol. 1994;72:479–93.
Diener HC, Dichgans J, Bacher M, Guschlbauer B. Characteristic alterations of long-loop "reflexes" in patients with Friedreich's disease and late atrophy of the cerebellar anterior lobe. J Neurol Neurosurg Psychiatry. 1984;47:679–85.
Kawato M. Internal models for motor control and trajectory planning. Curr Opin Neurobiol. 1999;9:718–27.
Wolpert DM, Ghahramani Z, Jordan MI. An internal model for sensorimotor integration. Science. 1995;269:1880–2.
Day BL, Thompson PD, Harding AE, Marsden CD. Influence of vision on upper limb reaching movements in patients with cerebellar ataxia. Brain. 1998;121(Pt 2):357–72.
Kluzik J, Horak FB, Peterka RJ. Differences in preferred reference frames for postural orientation shown by after-effects of stance on an inclined surface. Exp Brain Res. 2005;162:474–89.
Schmitz-Hubsch T, du Montcel ST, Baliko L, Berciano J, Boesch S, Depondt C, et al. Scale for the assessment and rating of ataxia: development of a new clinical scale. Neurology. 2006;66:1717–20.
Allum JH, Honegger F, Pfaltz CR. The role of stretch and vestibulo-spinal reflexes in the generation of human equilibrating reactions. Prog Brain Res. 1989;80:399–409.
Beckley DJ, Bloem BR, Remler MP, Roos RA, Van Dijk JG. Long latency postural responses are functionally modified by cognitive set. Electroencephalogr Clin Neurophysiol. 1991;81:353–8.
Diener HC, Horak FB, Nashner LM. Influence of stimulus parameters on human postural responses. J Neurophysiol. 1988;59:1888–905.
Henry SM, Fung J, Horak FB. Control of stance during lateral and anterior/posterior surface translations. IEEE Trans Rehabil Eng. 1998;6:32–42.
Nashner LM. Fixed patterns of rapid postural responses among leg muscles during stance. Exp Brain Res. 1977;30:13–24.
Horak FB, Nashner LM. Central programming of postural movements: adaptation to altered support-surface configurations. J Neurophysiol. 1986;55:1369–81.
Soucie JM, Wang C, Forsyth A, Funk S, Denny M, Roach KE, et al. Range of motion measurements: reference values and a database for comparison studies. Haemophilia. 2011;17:500–7.
Jonsson E, Henriksson M, Hirschfeld H. Does the functional reach test reflect stability limits in elderly people? J Rehabil Med. 2003;35:26–30.
Welch TD, Ting LH. A feedback model explains the differential scaling of human postural responses to perturbation acceleration and velocity. J Neurophysiol. 2009;101:3294–309.
Earhart GM, Bastian AJ. Selection and coordination of human locomotor forms following cerebellar damage. J Neurophysiol. 2001;85:759–69.
Van de Warrenburg BP, Bakker M, Kremer BP, Bloem BR, Allum JH. Trunk sway in patients with spinocerebellar ataxia. Mov Disord. 2005;20:1006–13.
Diener HC, Dichgans J, Bacher M, Gompf B. Quantification of postural sway in normals and patients with cerebellar diseases. Electroencephalogr Clin Neurophysiol. 1984;57:134–42.
Mauritz KH, Schmitt C, Dichgans J. Delayed and enhanced long latency reflexes as the possible cause of postural tremor in late cerebellar atrophy. Brain. 1981;104:97–116.
Acknowledgments
The authors thank Cristiane Zampieri and Kelly Bartow for their help with data collection as well as Triana Nagel for her help in the subject recruitment and data collection. This research was supported by the NIH R01-DC004082 and NIH R37-AG006457.
Conflict of interest
None of the authors have any financial and personal relationships that might bias the work presented in the current manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Paquette, C., Franzén, E. & Horak, F.B. More Falls in Cerebellar Ataxia When Standing on a Slow Up-Moving Tilt of the Support Surface. Cerebellum 15, 336–342 (2016). https://doi.org/10.1007/s12311-015-0704-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-015-0704-6