Abstract
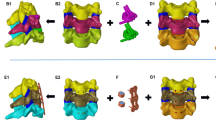
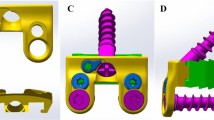
Cage plus plate (CP) and zero-profile (Zero-P) devices are widely used in anterior cervical discectomy and fusion (ACDF). This study aimed to compare adjacent segment biomechanical changes after ACDF when using Zero-P device and CP in different segments. First, complete C1—C7 cervical segments were constructed and validated. Meanwhile, four surgery models were developed by implanting the Zero-P device or CP into C4—C5 or C5—C6 segments based on the intact model. The segmental range of motion (ROM) and maximum value of the intradiscal pressure of the surgery models were compared with those of the intact model. The implantation of CP and Zero-P devices in C4—C5 segments decreased ROM by about 91.6% and 84.3%, respectively, and increased adjacent segment ROM by about 8.3% and 6.82%, respectively. The implantation of CP and Zero-P devices in C5—C6 segments decreased ROM by about 93.3% and 89.9%, respectively, while increasing adjacent segment ROM by about 4.9% and 4%, respectively. Furthermore, the implantation of CP and Zero-P devices increased the intradiscal pressure in the adjacent segments of C4—C5 segments by about 4.5% and 6.7%, respectively. The implantation of CP and Zero-P devices significantly increased the intradiscal pressure in the adjacent segments of C5—C6 by about 54.1% and 15.4%, respectively. In conclusion, CP and Zero-P fusion systems can significantly reduce the ROM of the fusion implant segment in ACDF while increasing the ROM and intradiscal pressure of adjacent segments. Results showed that Zero-P fusion system is the best choice for C5—C6 segmental ACDF. However, further studies are needed to select the most suitable cervical fusion system for C4—C5 segmental ACDF. Therefore, this study provides biomechanical recommendations for clinical surgery.
摘要
Cage-Plate融合器(CP)系统和零切迹融合器(Zero-P)系统广泛用于颈椎前路椎间盘切除和融合术中(ACDF)。本研究对比分析了不同节段ACDF植入CP或Zero-P融合器系统后相邻节段生物力学特性。首先, 建立了完整C1—C7颈椎节段的模型, 并对其有效性进行了验证。同时, 通过在完整模型的基础上将Zero-P或CP植入C4—C5或C5—C6节段, 建立了四种手术模型。将手术模型的节段活动度(ROM)和椎间盘内压最大值与完整模型进行比较。C4—C5植入CP、Zero-P使其ROM平均减少了91.6%, 84.3%; 临近节段ROM平均增大了8.3%, 6.82%。C5—C6植入CP、Zero-P使其ROM平均减少了93.3%, 89.9%; 临近节段ROM平均增大了4.9%, 4%。此外, C4—C5植入CP、Zero-P使临近节段椎间盘内压平均增大了4.5%, 6.7%。C5—C6植入CP、Zero-P使临近节段椎间盘内压平均增大了54.1%, 15.4%。总之, 植入CP和Zero-P融合器系统均会显著降低ACDF中植入节段的ROM, 同时增加相邻节段的ROM和椎间盘内压力。结果表明, Zero-P融合器系统是C5—C6节段ACDF的最佳选择。然而, 需要进一步的研究来选择最适合C4—C5节段ACDF的颈椎融合器系统。同时, 本研究为临床手术提供生物力学建议。
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
BURKHARDT B W, BRIELMAIER M, SCHWERDTFEGER K, et al. Smith-Robinson procedure with and without Caspar plating as a treatment for cervical spondylotic myelopathy: A 26-year follow-up of 23 patients [J]. European Spine Journal, 2017, 26: 1246–1253.
YANG J J, YU C H, CHANG B S, et al. Subsidence and nonunion after anterior cervical interbody fusion using a stand-alone polyetheretherketone (PEEK) cage [J]. Clinics in Orthopedic Surgery, 2011, 3(1): 16–23.
HILIBRAND A S, ROBBINS M. Adjacent segment degeneration and adjacent segment disease: The consequences of spinal fusion? [J]. The Spine Journal: Official Journal of the North American Spine Society, 2004, 4 (6 Suppl): 190S–194S.
ARUN R, FREEMAN B J C, SCAMMELL B E, et al. 2009 ISSLS Prize Winner: What influence does sustained mechanical load have on diffusion in the human intervertebral disc? An in vivo study using serial post-contrast magnetic resonance imaging [J]. Spine, 2009, 34(21): 2324–2337.
CHUNG J Y, PARK J B, SEO H Y, et al. Adjacent segment pathology after anterior cervical fusion [J]. Asian Spine Journal, 2016, 10(3): 582–592.
CHENY Y, LIU Y, CHEN H J, etal. Comparison of curvature between the zero-P spacer and traditional cage and plate after 3-level anterior cervical discectomy and fusion: Mid-term results [J]. Clinical Spine Surgery, 2017, 30(8): E1111–E1116.
VANEK P, BRADAC O, DELACY P, et al. Anterior interbody fusion of the cervical spine with Zero-P spacer: Prospective comparative study-clinical and radiological results at a minimum 2 years after surgery [J]. Spine, 2013, 38(13): E792–E797.
ZHANG T X, GUO N N, GAO G, et al. Comparison of outcomes between Zero-p implant and anterior cervical plate interbody fusion systems for anterior cervical decompression and fusion: A systematic review and meta-analysis of randomized controlled trials [J]. Journal of Orthopaedic Surgery and Research, 2022, 17(1): 1–9.
HUA W B, ZHI J G, KE W C, et al. Adjacent segment biomechanical changes after one- or two-level anterior cervical discectomy and fusion using either a zero-profile device or cage plus plate: A finite element analysis [J]. Computers in Biology and Medicine, 2020, 120: 103760.
FAIZAN A, GOEL V K, GARFIN S R, et al. Do design variations in the artificial disc influence cervical spine biomechanics? A finite element investigation [J]. European Spine Journal, 2012, 21(5): 653–662.
CAO F, FU R C, WANG W Y. Comparison of biomechanical performance of single-level triangular and quadrilateral profile anterior cervical plates [J]. PLoS One, 2021, 16(4): e0250270.
HONG-WAN N, EE-CHON T, ZHANG Q H. Biomechanical effects of C2–C7 intersegmental stability due to laminectomy with unilateral and bilateral facetectomy [J]. Spine, 2004, 29(16): 1737–1745.
HSU C C, CHANG T K, HUY D C. Biomechanical comparison of different vertebral plate designs for anterior cervical discectomy and fusion using nonlinear C3-T2 multi-level spinal models [J]. Computer-Aided Design and Applications, 2015, 12(2): 226–231.
KWON J W, BANG S H, KWON Y W, et al. Biomechanical comparison of the angle of inserted screws and the length of anterior cervical plate systems with allograft spacers [J]. Clinical Biomechanics, 2020, 76: 105021.
NISHIZAWA S, YOKOYAMA T, YOKOTA N, et al. High cervical disc lesions in elderly patients - presentation and surgical approach [J]. Acta Neurochirurgica, 1999, 141(2): 119–126.
ZOU X N, XUE Q Y, LI H S, et al. Effect of alendronate on bone ingrowth into porous tantalum and carbon fiber interbody devicesAn experimental study on spinal fusion in pigs [J]. Acta Orthopaedica Scandinavica, 2003, 74(5): 596–603.
LIU N, LU T, WANG Y B, et al. Effects of new cage profiles on the improvement in biomechanical performance of multilevel anterior cervical corpectomy and fusion: A finite element analysis [J]. World Neurosurgery, 2019, 129: e87–e96.
MERCER S, BOGDUK N. The ligaments and anulus fibrosus of human adult cervical intervertebral discs [J]. Spine, 1999, 24(7): 619–626.
WEI W, LIAO S H, SHI S Y, et al. Straightened cervical lordosis causes stress concentration: A finite element model study [J]. Australasian Physical & Engineering Sciences in Medicine, 2013, 36(1): 27–33.
HUSSAIN M, NASSR A, NATARAJAN R N, et al. Biomechanics of adjacent segments after a multilevel cervical corpectomy using anterior, posterior, and combined anterior-posterior instrumentation techniques: A finite element model study [J]. The Spine Journal, 2013, 13(6): 689–696.
GOEL V K, CLAUSEN J D. Prediction of load sharing among spinal components of a C5-C6 motion segment using the finite element approach [J]. Spine, 1998, 23(6): 684–691.
LEE S H, IM Y J, KIM K T, et al. Comparison of cervical spine biomechanics after fixed- and mobile-core artificial disc replacement: A finite element analysis [J]. Spine, 2011, 36(9): 700–708.
PANJABI M M, CRISCO J J, VASAVADA A, et al. Mechanical properties of the human cervical spine as shown by three-dimensional load-displacement curves [J]. Spine, 2001, 26(24): 2692–2700.
ZHANG Q H, TEO E C, NG H W, et al. Finite element analysis of moment-rotation relationships for human cervical spine [J]. Journal of Biomechanics, 2006, 39(1): 189–193.
XIE N, YUAN W, YE X J, et al. Anterior cervical locking plate-related complications; prevention and treatment recommendations [J]. International Orthopaedics, 2008, 32(5): 649–655.
BALARAM A K, GHANAYEM A J, O’LEARY P T, et al. Biomechanical evaluation of a low-profile, anchored cervical interbody spacer device at the index level or adjacent to plated fusion [J]. Spine, 2014, 39(13): E763–E769.
CHANG U, KIM D H, LEE M C, et al. Changes in adjacent-level disc pressure and facet joint force after cervical arthroplasty compared with cervical discectomy and fusion[J]. Journal of Neurosurgery Spine, 2007, 7(1): 33–39.
GALBUSERA F, BRAYDA-BRUNO M, WILKE H J. Is post-contrast MRI a valuable method for the study of the nutrition of the intervertebral disc? [J]. Journal of Biomechanics, 2014, 47(12): 3028–3034.
ECK J C, HUMPHREYS S C, LIM T H, et al. Biomechanical study on the effect of cervical spine fusion on adjacent-level intradiscal pressure and segmental motion [J]. Spine, 2002, 27(22): 2431–2434.
Author information
Authors and Affiliations
Corresponding author
Additional information
Foundation item: the National Natural Science Foundation of China (Nos. 32260235 and 82260446)
Rights and permissions
About this article
Cite this article
Ye, P., Fu, R. & Wang, Z. Adjacent Segment Biomechanical Changes After Implantation of Cage Plus Plate or Zero-Profile Device in Different Segmental Anterior Cervical Discectomy and Fusion. J. Shanghai Jiaotong Univ. (Sci.) (2023). https://doi.org/10.1007/s12204-023-2633-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12204-023-2633-8
Key words
- biomechanics
- finite element analysis
- adjacent segment degeneration
- range of motion (ROM)
- intradiscal pressure