Abstract
Purpose of Review
Recurrent shoulder instability after stabilization is common in pediatric and adolescent athletes. The purpose of this review is to understand the risk factors that lead to failure of primary surgery and management principles in the setting of recurrent instability following surgical stabilization.
Recent Findings
Rates of recurrence after primary and revision surgical stabilization remain higher than desirable. Risk factors for failure in include glenoid and humeral bone loss, capsular or ligamentous laxity, and young age though few studies have focused specifically on the adolescent population. Arthroscopic, open, and bone block techniques have been described in this population similar to adults.
Summary
Failure after a primary shoulder stabilization remains a common problem in adolescents in no small part because a high proportion of these athletes return to high levels of activity. A thorough understanding of the index procedure and patient-specific risk factors for failure are key to successful planning of revision surgery. The current literature does not allow for firm treatment recommendations in individual pediatric or adolescent athletes, but the guiding principles are similar to those in adults. Specifically, all bony and soft tissue pathology should be identified and assessed, with an understanding that simply repeating the steps of the index procedure typically results in poor outcomes, and often an “escalation” of surgical complexity is required at the time of revision. When appropriately indicated, arthroscopic or open soft tissue procedures and Latarjet coracoid transfer can be safely and successfully implemented for revision shoulder stabilization in young athletes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Shoulder instability in the pediatric population covers a spectrum of pathology including anterior, posterior, and multidirectional instability [1, 2]. Anterior instability represents the vast majority of shoulder instability in this population, and 19% of all anterior shoulder dislocations occur in patients between the ages of 15 and 19 years [3]. In patients age 18 and younger, males and patients greater than 14 years of age have the greatest risk of recurrent shoulder instability, while patients with open physes are less likely to see a recurrence [4]. Estimates of recurrence in the older adolescents (14–18 years) with conservative management are as high as 92% [5].
As a result, surgical intervention is often recommended in this population. Surgical shoulder stabilization has been shown to reduce the risk of recurrence with some authors recommending intervention even after a single dislocation, though this remains controversial [6,7,8,9,10]. Despite lower reported recurrent anterior instability with operative treatment, recurrence after primary stabilization surgery remains high in adolescents. Studies looking specifically at adolescent patients have shown recurrence after primary stabilization surgery to range from 17 to 51%, and rates for specific subpopulations, such as contact athletes or those with glenoid or bipolar bone loss, may be even higher [11,12,13,14,15,16]. Thus, identifying risk factors for failure of primary stabilization surgery is of vital importance to choose the appropriate primary procedure or, when needed, address sources of possible failure in revision surgery.
Though some studies have looked specifically at adolescent populations, the vast majority of studies evaluating outcomes after primary anterior shoulder stabilization surgery have looked at mixed populations from which we can also infer important considerations for management. This review will look at existing evidence as well as provide pearls for evaluation and management of the pediatric and adolescent patient who has failed a primary anterior stabilization.
Risk Factors for Failure of Primary Surgery
Patient Factors
Several patient factors are known risks factors for failure of primary shoulder stabilization surgery, many of them similar to the risk factors for failure of nonoperative management (Table 1). Adolescents have roughly doubled the risk of failure after primary shoulder stabilization as individuals over the age of 20 [17, 18]. Male gender as well as involvement in contact or collision sports may also predispose to failure of primary stabilization [11, 15•, 17]. Finally, ligamentous laxity on preoperative exam results in higher risk of recurrence postoperatively [19, 20•]. Other factors such as the number of preoperative dislocations and the time from initial dislocation to surgery have shown mixed evidence in different populations and have not been shown to independently increase risk in adolescent populations [11, 15•, 17, 18, 21].
Bone loss, on the glenoid or the humeral head, as well as glenoid articular disruption are well-known risk factors for failure of primary stabilization surgery [12, 15•, 19, 22,23,24]. What constitutes “critical” glenoid bone loss remains an active area of research and may be less than the typically quoted 20–25% [25, 26]. In particular, there have been no studies assessing cutoffs for glenoid or humeral bone loss specifically in the adolescent population. Glenoid bone loss was found in one study to be the most common reason for failure of primary stabilization in adolescents [12]. Adolescents and individuals with multiple dislocations are also at a higher risk of having an “off-track” humeral head lesion which can further exacerbate the effect of glenoid bone loss on the stability of the shoulder [27]. In combined lesions, glenoid loss of as little as 8% can affect the biomechanical stability of a soft tissue Bankart repair [28]. Thus, careful attention to the presence of any bone loss must be evaluated as a possible reason for failure of a primary procedure.
Surgical Factors
Surgical factors that predict an increased risk of failure after primary stabilization surgery remain an area of active research and can be divided into patient/surgical selection and technical factors. Few studies have specifically looked at these risk factors in children or adolescents, and most findings are inferences from mixed or adult populations [6, 11, 14, 15•, 29•, 30•]. If not the primary surgeon, details of the primary procedure and preoperative pathology should be obtained either through medical and surgical records and/or in direct discussion with the primary surgeon if necessary to allow and adequate review.
Similar to the adult patient, choosing the right surgery for the right patient is essential in ensuring a successful outcome in pediatric athletes. Arthroscopic soft tissue, open soft tissue, and bone block procedures have all been described in the adolescent population and have shown success in the treatment of instability [6, 11, 14, 29•, 31]. Thus, principles regarding selection of the appropriate procedure for an individual patient are no different than those which apply to the adult instability patient. Failure to adequately address all pathology is a common cause of surgical failure. For example, bony defects and capsular laxity are common findings after failed shoulder instability and can be the result of further injury postoperatively or a failure to address the pathology during the initial surgery (Table 1) [32, 33]. Open surgery should be carefully considered inadequate primary surgery may be the result of inappropriate use of arthroscopy.
Technical factors regarding the position and method of fixation should also be evaluated when critically reviewing a primary surgery as well as planning for a revision. Suture failure and suture cut-through were two of the most common reasons for failure in adolescents undergoing primary stabilization and may be a result of technique [12]. The specific effect of fixation on risk in the pediatric and adolescent patient has not been well elucidated. The type and number of fixation points as independent risk factors have shown mixed results in adult and adolescent populations and may not be as much of a factor as once thought [15•, 19, 21]. Nonetheless, careful attention should be paid to preoperative pathology and surgical description to ensure that fixation was utilized in a manner that would be expected to address the underlying pathology including restoration of labral position and anatomy and appropriate tensioning of capsular or capsulolabral tissue. As noted above, addressing bony deficiency is also of utmost importance, though how best to do this remains an area of research. Numerous methods to address glenoid bone loss in the primary setting have been described, and, in the case of humeral bone loss, remplissage used in addition to Bankart repair may provide a lower risk of recurrence in appropriate adolescent patients [14].
Careful attention should also be paid to the patient’s ability to follow appropriate postoperative protocols. Postoperative restrictions and graduated rehabilitation are a crucial part of successful instability surgery. Premature engagement in restricted activities or return to sport can compromise surgical treatment, and every effort should be made to limit confusion and optimize compliance with postoperative instructions.
Outcomes of Revision Surgery
Few studies have looked specifically at the results of revision stabilization surgery in the adolescent patient. Blackman et al. [12] found a 33% rate of recurrent dislocation and repeat revision surgery in 15 adolescent patients undergoing revision stabilization surgery. Though limited numbers may have affected the findings, the study did not find any consistent risk factors for failure despite looking at commonly believed factors such as age, interval between instability and initial surgery, open or arthroscopic surgery, number of anchors, or bone loss (glenoid or humeral head) [12].
A recent systematic review of studies analyzing revision arthroscopic Bankart repair found a mean failure rate of 12.7% with 62% of patients failing their primary surgery secondary to a traumatic injury [34]. Though other studies have found much higher rates of failure in certain populations, even revision after failure of bony augmentation procedures has shown the ability to successfully restore shoulder stability in adults [20•, 35].
Failure of revision surgery has many of the same risk factors as those of primary surgery. Young age (< 22), ligamentous laxity, and bone loss have all been found to increase the risk of failures after revision stabilization [20•, 36]. Increased number of prior surgeries has also been found to be a risk factor and has been associated with worse overall outcomes including lower return to sport [33, 36,37,38].
As with primary surgery, the type of procedure done in a revision setting remains a significant area of research. Though some evidence has supported the often held belief that open procedures result in better outcomes in revision shoulder stabilization, inconsistent reporting of patient’s factors, specifically bone loss, can make conclusions difficult to interpret in the context of any specific patient [39]. Similar to primary procedures, success has been shown with arthroscopic and open approaches in the revision setting as well. Similarly, the Latarjet for glenoid bone loss and remplissage procedure for humeral head bone loss have been reported with success in the adolescent population [14, 30•]. Additionally, the use of Iliac crest and distal tibia allograft have been described in adult populations for the treatment of glenoid bone loss, but never in children [35, 40]. Distal clavicle autograft has also been utilized in adults for glenoid bone loss; however, the open distal clavicular physes would likely make this undesirable in adolescent patients [41].
Patient Evaluation
History
A detailed history is the critical starting point in the evaluation of a patient with a failed shoulder stabilization. The mechanism of recurrence may provide important clues as to the cause of failure. Trauma is a common cause of recurrent shoulder instability and may result in acute failure of a repair, even in the absence of any technical error [32, 34]. A more insidious onset of instability may indicate that the underlying pathology was not adequately addressed in the initial surgery and should result in further investigation. As mentioned above, preoperative clinical notes as well as operative notes should be obtained to allow a complete review of the patient’s history as well as surgical findings and technique to evaluate risk factors that may have contributed to failure.
Physical Exam
Physical examination of a patient with failed primary shoulder stabilization should incorporate the basic tenets of any physical exam with some specific additions. First, the shoulder should be inspected for scars from previous incisions to provide further information on previous injuries and surgeries. Standard range of motion and strength examinations should be performed, including evaluation of the rotator cuff though injuries are uncommon in this population. A standard neurovascular exam should also be completed with specific focus on the function of the axillary nerve.
Laxity and apprehension on the physical exam can provide important information on present pathology. The standard apprehension and relocation test shoulder be performed as well as repeated at low and midpoints of abduction. Apprehension in lower abduction may indicate bone loss that will need to be addressed at the time of revision. Generalized laxity should be evaluated via the Beighton score which has shown validity for hypermobility in the pediatric population. However, this does not always correlate with laxity in overall range of motion or findings of a sulcus sign which should also be documented [42, 43].
Imaging
X-rays are usually the initial image obtained in the patient with recurrent shoulder instability after surgery and can provide important clues. AP and Scapular Y x-rays should be performed, and special views such as the Bernageau view (for glenoid bone loss) and a Stryker notch view (Hill-Sachs lesion) can help in the initial evaluation of bone loss. CT scans with 3-dimensional reconstruction are the most effective method of measuring bone loss particularly on the glenoid but may be less effective in evaluating the humeral head [44, 45]. Finally, an MRI can provide details on cartilage, labral, capsular, and ligament pathology and should include an arthrogram if there is no acute injury that would result in an effusion. A humeral avulsion of the glenohumeral ligament, or HAGL lesion, must be carefully evaluated for as inability to address a HAGL could lead to treatment failure. Intraoperative evaluation is the only way to truly evaluate the capsular and labral quality for operative decision-making.
Critical evaluation should not only include anatomic factors such as bone loss, chondral changes, and capsular laxity, but careful attention should be paid to the size and location of previous fixation, including cysts that may be present from previous biocomposite anchors. Planning for revision surgery must consider where further fixation might be placed and whether or not adequate fixation can be placed to address the present pathology. Minimal room for further fixation may necessitate use of a bone block procedure even if other indications are not present.
Our Approach
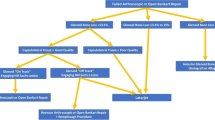
Though attitudes, behaviors, and risk profiles may be different in the pediatric and adolescent population, physes are not typically thought to be important for surgical risk. Thus, as mentioned above, our surgical approach to the failed stabilization surgery remains largely the same in this population as in adults. That being said, we will often be a little less tolerant of surgical risk in younger individuals and will try to exhaust minimally invasive surgical options when at all possible. Based on the aforementioned evidence, our approach divides patients into one of three categories: patients with inadequate primary surgery without critical bone loss, patients with adequate primary surgery without critical bone loss, and patients with critical bone loss (Fig. 1).
Inadequate Primary Surgery with Subcritical Bone Loss and/or an On-Track Hill Sachs
In some patients, there is evidence that either the procedure itself or the execution of the procedure, such as the fixation, may not have adequately addressed the patient’s preoperative pathology. Common errors include anchors that are placed above the equator of the glenoid, not addressing the antero-inferior pathology, as well as failure to address inferior instability with fixation on the inferior glenoid (Fig. 2).
In these cases, and in a patient with no significant risk factors for failure of an arthroscopic repair such as critical bone loss or significant capsular laxity, we will perform revision arthroscopic surgery for failed primary surgery. We use small anchors (< 2 mm) to optimize the number of points of fixation we can use and begin our fixation at the 7 o’clock position on the postero-inferior glenoid (Fig. 3). Fixation here ensures appropriate tightening of the posterior band of the inferior glenohumeral ligament. We include fixation at the 6 o’clock position as well, which also helps to address the inferior component of the instability, before moving to the antero-inferior glenoid (Fig. 4).
Intraoperative findings of patient from Fig. 2 (Left). Revision fixation shown including additional fixation postero-inferiorly at 7 o’clock position to tension posterior inferior glenohumeral ligament (Right)
As noted above, capsular and labral quality may only be fully evaluated arthroscopically, and their poor quality may compromise the ability for an arthroscopic procedure to adequately address instability arthroscopically. Evaluation intraoperatively should involve tactile evaluation of the quality of the tissue with a grasper and attempted reduction of the tissue to its anatomic position. Thin, flimsy tissue that cannot hold a stitch or tissue that cannot be reduced anatomically may limit the options for arthroscopic treatment. Therefore, in planning revision arthroscopic Bankart repair, we are prepared to convert to an open procedure if intraoperative findings dictate.
Adequate Primary Surgery with Subcritical Bone Loss and/or an On-Track Hill Sachs
In the event that an initial primary arthroscopic or open Bankart repair fails, the most important factor in deciding the most appropriate revision procedure is bone loss. As described above, bone loss on the glenoid or humerus can be a risk factor for failure of primary or revision stabilization surgery. Thus, we obtain a 3D CT on all revision patients to evaluate for bone loss before proceeding with surgical intervention. Glenoid bone loss is measured using a best fit circle, or the PICO method, which has been shown to most accurately estimate antero-inferior bone loss [44]. As noted above, what constitutes critical glenoid bone loss remains a source of debate and research particularly in the revision setting. In isolation of other risk factors, we define critical glenoid bone loss necessitating a bone block procedure as 15%.
We also assess humeral head bone loss to determine if a present lesion or on-track or off-track as initially described by Yamamoto et al. [46]. As with defining critical glenoid bone loss, management of humeral bone loss remains an area of active research. Though one study has shown decreased instability recurrence with the addition of remplissage to arthroscopic Bankart repair in adolescent patients, other studies have suggested that remplissage provides no added benefit or may actually be less effective than other procedures particularly in a revision setting [14, 47]. In the setting of either critical glenoid bone loss or an off-track humeral head lesion, it is the author’s preference to perform a Latarjet procedure without additional remplissage.
In the setting of subcritical glenoid bone loss or an on-track humeral head lesion, we evaluate the other risk factors that a patient may have that may put them at high risk to fail a second soft tissue procedure, specifically any contact athlete or individuals with a soft tissue disorder that would make further soft tissues procedures unlikely to provide adequate stability. In the presence of other risk factors, the author’s preference is to still proceed with a Latarjet procedure though each case is considered individually. In the setting of an adequate primary surgery with none of the above risk factors or bone loss, we proceed with an open Bankart repair with capsular shift as previously described by Neer (Fig. 5) [48].
3D CT reconstruction of the right shoulder of a 19-year-old patient who had undergone initial arthroscopic stabilization at age 17. The image shows multiple anchors in the antero-inferior portion of the glenoid. We felt this was adequate fixation to address the present pathology despite the subsequent failure clinically. Therefore, we proceeded with an open Bankart repair with capsular shift for the revision procedure
Any Failed Primary Procedure with Critical Bone Loss or an Off-Track Hill Sachs
Given the effect of bone loss on the biomechanical stability of the shoulder, treating bone loss is of utmost importance in providing a successful outcome for the patient with recurrent shoulder instability after failed primary stabilization. As noted above, our preference for the treatment of a patient with critical glenoid bone loss or an off-track Hill-Sachs lesion is to perform an open Latarjet procedure through a subscapularis split with two screws (Fig. 6).
Imaging of a 17-year-old football player who presented with recurrent instability after primary arthroscopic stabilization. 3D CT reconstruction (left image) showed critical bone loss on the antero-inferior portion of the glenoid. Given the bone loss, we revised the patient with a Latarjet procedure (right image)
Rehabilitation and Return to Sport
If there is any consensus on return-to-play criteria after surgical shoulder stabilization, it is that there is no agreement about what these criteria should be [49, 50]. Indeed, 75% of studies included in a recent systematic review used time alone as their criteria for return to play, with 6 months being the most commonly recommended time-frame [49]. After primary surgical stabilization, rates of return-to-play at pre-injury level are between 65 and 75% [51]. In a recent systematic review by the senior author on revision instability surgery, these rates were similarly between 60 and 70% (unpublished data). As such, the literature would support that with adequate patient selection, the ability to return to sport is not affected by revision status. With this in mind, we follow nearly identical rehabilitation protocols with adolescents undergoing revision should stabilization as for those undergoing primary stabilization.
We favor an evidence-based, three-phase postoperative protocol with criterion rather than time-based metrics for progression, as previously described [52]. A few notable exceptions are as follows: (1) the patient who undergoes arthroscopic revision with a significant capsular imbrication component; this patient should progress slowly with passive range of motion in the first 6–8 weeks after surgery, with the therapist only “taking what the shoulder will give them” in terms of motion, to avoid stretching out the capsular imbrication, and (2) the patient who undergoes an open revision that requires subscapularis tenotomy; this patient should follow subscapularis precautions including no external rotation past neutral for 6 weeks, and no resisted internal rotation for 12 weeks.
Conclusion
Failure after a primary shoulder stabilization remains a common problem in adolescents in no small part because a high proportion of these athletes return to high levels of activity. A thorough understanding of the index procedure and patient-specific risk factors for failure are key to successful planning of revision surgery. The current literature does not allow for firm treatment recommendations in individual pediatric or adolescent athletes, but the guiding principles are similar to those in adults. Specifically, all bony and soft tissue pathology should be identified and assessed, with an understanding that simply repeating the steps of the index procedure typically results in poor outcomes, and often an “escalation” of surgical complexity is required at the time of revision. When appropriately indicated, arthroscopic or open soft tissue procedures and Latarjet coracoid transfer can be safely and successfully implemented for revision shoulder stabilization in young athletes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
McClincy MP, Arner JW, Thurber L, Bradley JP. Arthroscopic Capsulolabral Reconstruction for Posterior Shoulder Instability is Successful in Adolescent Athletes. J Pediatr Orthop. 2018. https://doi.org/10.1097/bpo.0000000000001210.
Watson L, Balster S, Lenssen R, Hoy G, Pizzari T. The effects of a conservative rehabilitation program for multidirectional instability of the shoulder. J Shoulder Elb Surg. 2018;27(1):104–11. https://doi.org/10.1016/j.jse.2017.07.002.
Zacchilli MA, Owens BD. Epidemiology of shoulder dislocations presenting to emergency departments in the United States. J Bone Joint Surg Am. 2010;92(3):542–9. https://doi.org/10.2106/jbjs.I.00450.
Olds M, Donaldson K, Ellis R, Kersten P. In children 18 years and under, what promotes recurrent shoulder instability after traumatic anterior shoulder dislocation? A systematic review and meta-analysis of risk factors. Br J Sports Med. 2016;50(18):1135–41. https://doi.org/10.1136/bjsports-2015-095149.
Postacchini F, Gumina S, Cinotti G. Anterior shoulder dislocation in adolescents. J Shoulder Elb Surg. 2000;9(6):470–4. https://doi.org/10.1067/mse.2000.108385.
Gigis I, Heikenfeld R, Kapinas A, Listringhaus R, Godolias G. Arthroscopic versus conservative treatment of first anterior dislocation of the shoulder in adolescents. J Pediatr Orthop. 2014;34(4):421–5. https://doi.org/10.1097/bpo.0000000000000108.
Franklin CC, Weiss JM. The natural history of pediatric and adolescent shoulder dislocation. J Pediatr Orthop. 2019;39(Issue 6, Supplement 1 Suppl 1):S50–s2. https://doi.org/10.1097/bpo.0000000000001374.
Zaremski JL, Galloza J, Sepulveda F, Vasilopoulos T, Micheo W, Herman DC. Recurrence and return to play after shoulder instability events in young and adolescent athletes: a systematic review and meta-analysis. Br J Sports Med. 2017;51(3):177–84. https://doi.org/10.1136/bjsports-2016-096895.
Longo UG, van der Linde JA, Loppini M, Coco V, Poolman RW, Denaro V. Surgical versus nonoperative treatment in patients up to 18 years old with traumatic shoulder instability: a systematic review and quantitative synthesis of the literature. Arthroscopy. 2016;32(5):944–52. https://doi.org/10.1016/j.arthro.2015.10.020.
Roberts SB, Beattie N, McNiven ND, Robinson CM. The natural history of primary anterior dislocation of the glenohumeral joint in adolescence. Bone Joint J. 2015;97-b(4):520–6. https://doi.org/10.1302/0301-620x.97b4.34989.
Castagna A, Delle Rose G, Borroni M, Cillis BD, Conti M, Garofalo R, et al. Arthroscopic stabilization of the shoulder in adolescent athletes participating in overhead or contact sports. Arthroscopy. 2012;28(3):309–15. https://doi.org/10.1016/j.arthro.2011.08.302.
Blackman AJ, Krych AJ, Kuzma SA, Chow RM, Camp C, Dahm DL. Results of revision anterior shoulder stabilization surgery in adolescent athletes. Arthroscopy. 2014;30(11):1400–5. https://doi.org/10.1016/j.arthro.2014.05.037.
Chapus V, Rochcongar G, Pineau V, Salle de Chou E, Hulet C. Ten-year follow-up of acute arthroscopic Bankart repair for initial anterior shoulder dislocation in young patients. Orthop Traumatol Surg Res. 2015;101(8):889–93. https://doi.org/10.1016/j.otsr.2015.09.029.
Hughes JL, Bastrom T, Pennock AT, Edmonds EW. Arthroscopic Bankart repairs with and without remplissage in recurrent adolescent anterior shoulder instability with Hill-Sachs deformity. Orthop J Sports Med. 2018;6(12):2325967118813981. https://doi.org/10.1177/2325967118813981.
• Kramer J, Gajudo G, Pandya NK. Risk of recurrent instability after arthroscopic stabilization for shoulder instability in adolescent patients. Orthop J Sports Med. 2019;7(9):2325967119868995. https://doi.org/10.1177/2325967119868995This study retrospectively evaluated 36 patients with a mean age of 16 years undergoing arthroscopic stabilization. The authors found a recurrence rate of 33% but found no statistically significant risk factors.
Shymon SJ, Roocroft J, Edmonds EW. Traumatic anterior instability of the pediatric shoulder: a comparison of arthroscopic and open bankart repairs. J Pediatr Orthop. 2015;35(1):1–6. https://doi.org/10.1097/bpo.0000000000000215.
Porcellini G, Campi F, Pegreffi F, Castagna A, Paladini P. Predisposing factors for recurrent shoulder dislocation after arthroscopic treatment. J Bone Joint Surg Am. 2009;91(11):2537–42. https://doi.org/10.2106/jbjs.H.01126.
Wasserstein D, Dwyer T, Veillette C, Gandhi R, Chahal J, Mahomed N, et al. Predictors of dislocation and revision after shoulder stabilization in Ontario, Canada, from 2003 to 2008. Am J Sports Med. 2013;41(9):2034–40. https://doi.org/10.1177/0363546513492952.
Boileau P, Villalba M, Hery JY, Balg F, Ahrens P, Neyton L. Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am. 2006;88(8):1755–63. https://doi.org/10.2106/jbjs.E.00817.
• Su F, Kowalczuk M, Ikpe S, Lee H, Sabzevari S, Lin A. Risk factors for failure of arthroscopic revision anterior shoulder stabilization. J Bone Joint Surg Am. 2018;100(15):1319–25. https://doi.org/10.2106/jbjs.17.01028This study retrospectively reviewed 65 patients with a mean age of 26 (Range 15–57) who underwent revision arthroscopic anterior shoulder stabilization and found age < 22, ligamentous laxity and an off-track humeral head lesion as risk factors for recurrence.
Brown L, Rothermel S, Joshi R, Dhawan A. Recurrent instability after arthroscopic Bankart reconstruction: a systematic review of surgical technical factors. Arthroscopy. 2017;33(11):2081–92. https://doi.org/10.1016/j.arthro.2017.06.038.
Burkhart SS, De Beer JF. Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging hill-Sachs lesion. Arthroscopy. 2000;16(7):677–94. https://doi.org/10.1053/jars.2000.17715.
Locher J, Wilken F, Beitzel K, Buchmann S, Longo UG, Denaro V, et al. Hill-Sachs off-track lesions as risk factor for recurrence of instability after arthroscopic Bankart repair. Arthroscopy. 2016;32(10):1993–9. https://doi.org/10.1016/j.arthro.2016.03.005.
Pogorzelski J, Fritz EM, Horan MP, Katthagen JC, Provencher MT, Millett PJ. Failure following arthroscopic Bankart repair for traumatic anteroinferior instability of the shoulder: is a glenoid labral articular disruption (GLAD) lesion a risk factor for recurrent instability? J Shoulder Elb Surg. 2018;27(8):e235–e42. https://doi.org/10.1016/j.jse.2018.02.055.
Shaha JS, Cook JB, Song DJ, Rowles DJ, Bottoni CR, Shaha SH, et al. Redefining "critical" bone loss in shoulder instability: functional outcomes worsen with "subcritical" bone loss. Am J Sports Med. 2015;43(7):1719–25. https://doi.org/10.1177/0363546515578250.
Shin SJ, Kim RG, Jeon YS, Kwon TH. Critical value of anterior Glenoid bone loss that leads to recurrent Glenohumeral instability after arthroscopic Bankart repair. Am J Sports Med. 2017;45(9):1975–81. https://doi.org/10.1177/0363546517697963.
Lau BC, Conway D, Curran PF, Feeley BT, Pandya NK. Bipolar bone loss in patients with anterior shoulder dislocation: a comparison of adolescents versus adult patients. Arthroscopy. 2017;33(10):1755–61. https://doi.org/10.1016/j.arthro.2017.04.004.
Arciero RA, Parrino A, Bernhardson AS, Diaz-Doran V, Obopilwe E, Cote MP, et al. The effect of a combined glenoid and hill-Sachs defect on glenohumeral stability: a biomechanical cadaveric study using 3-dimensional modeling of 142 patients. Am J Sports Med. 2015;43(6):1422–9. https://doi.org/10.1177/0363546515574677.
• Hatch MD, Hennrikus WL. The open Bankart repair for traumatic anterior shoulder instability in teenage athletes. J Pediatr Orthop. 2018;38(1):27–31. https://doi.org/10.1097/bpo.0000000000000744This case series of 21 teenage patients undergoing open bankart repair for traumatic anterior shoulder instability showed excellent functional outcomes at 2 year follow-up but did note an average 11 degree external rotation loss in 7 patients and no recurrent instability.
• Heyworth BE, Wu M, Kramer DE, Bae DS. The Latarjet Procedure for Anterior Shoulder Instability in Pediatric and Adolescent Athletes. Orthop J Sports Med. 2018;6(7_suppl4):2325967118S00127. https://doi.org/10.1177/2325967118S00127This study retrospectively compared a cohort of 18 adolescent patients undergoing a Latarjet procedure to a cohort of 22 adolescent patients undergoing other procedures for anterior shoulder instability. Recurrence in the Latarjet group was 17% with no cases of nerve palsy or coracoid non-union. Other outcomes and return to sport showed no significant difference despite higher risks amongst the cohort undergoing Latarjet.
Miura K, Tsuda E, Tohyama H, Iwahori Y, Mae T, Mochizuki Y, et al. Can arthroscopic Bankart repairs using suture anchors restore equivalent stability to open repairs in the management of traumatic anterior shoulder dislocation? A meta-analysis. J Orthop Sci. 2018;23(6):935–41. https://doi.org/10.1016/j.jos.2018.06.016.
Tauber M, Resch H, Forstner R, Raffl M, Schauer J. Reasons for failure after surgical repair of anterior shoulder instability. J Shoulder Elb Surg. 2004;13(3):279–85. https://doi.org/10.1016/s1058274604000254.
Marquardt B, Garmann S, Schulte T, Witt KA, Steinbeck J, Potzl W. Outcome after failed traumatic anterior shoulder instability repair with and without surgical revision. J Shoulder Elb Surg. 2007;16(6):742–7. https://doi.org/10.1016/j.jse.2007.02.132.
Abouali JAK, Hatzantoni K, Holtby R, Veillette C, Theodoropoulos J. Revision arthroscopic Bankart repair. Arthroscopy. 2013;29(9):1572–8. https://doi.org/10.1016/j.arthro.2013.04.017.
Provencher MT, Peebles LA, Aman ZS, Bernhardson AS, Murphy CP, Sanchez A, et al. Management of the Failed Latarjet Procedure: outcomes of revision surgery with fresh distal Tibial allograft. Am J Sports Med. 2019;363546519871896. https://doi.org/10.1177/0363546519871896.
Shin JJ, Mascarenhas R, Patel AV, Yanke AB, Nicholson GP, Cole BJ, et al. Clinical outcomes following revision anterior shoulder arthroscopic capsulolabral stabilization. Arch Orthop Trauma Surg. 2015;135(11):1553–9. https://doi.org/10.1007/s00402-015-2294-7.
Cho NS, Yi JW, Lee BG, Rhee YG. Revision open Bankart surgery after arthroscopic repair for traumatic anterior shoulder instability. Am J Sports Med. 2009;37(11):2158–64. https://doi.org/10.1177/0363546509339015.
Privitera DM, Sinz NJ, Miller LR, Siegel EJ, Solberg MJ, Daniels SD, et al. Clinical outcomes following the Latarjet procedure in contact and collision athletes. J Bone Joint Surg Am. 2018;100(6):459–65. https://doi.org/10.2106/jbjs.17.00566.
Friedman LG, Griesser MJ, Miniaci AA, Jones MH. Recurrent instability after revision anterior shoulder stabilization surgery. Arthroscopy. 2014;30(3):372–81. https://doi.org/10.1016/j.arthro.2013.11.019.
Moroder P, Schulz E, Wierer G, Auffarth A, Habermeyer P, Resch H, et al. Neer award 2019: Latarjet procedure vs. iliac crest bone graft transfer for treatment of anterior shoulder instability with glenoid bone loss: a prospective randomized trial. J Shoulder Elb Surg. 2019;28(7):1298–307. https://doi.org/10.1016/j.jse.2019.03.035.
Tokish JM, Fitzpatrick K, Cook JB, Mallon WJ. Arthroscopic distal clavicular autograft for treating shoulder instability with glenoid bone loss. Arthrosc Tech. 2014;3(4):e475–81. https://doi.org/10.1016/j.eats.2014.05.006.
Whitehead NA, Mohammed KD, Fulcher ML. Does the Beighton score correlate with specific measures of shoulder joint laxity? Orthop J Sports Med. 2018;6(5):2325967118770633. https://doi.org/10.1177/2325967118770633.
Smits-Engelsman B, Klerks M, Kirby A. Beighton score: a valid measure for generalized hypermobility in children. J Pediatr. 2011;158(1):119–23, 23.e1–4. https://doi.org/10.1016/j.jpeds.2010.07.021.
Bois AJ, Fening SD, Polster J, Jones MH, Miniaci A. Quantifying glenoid bone loss in anterior shoulder instability: reliability and accuracy of 2-dimensional and 3-dimensional computed tomography measurement techniques. Am J Sports Med. 2012;40(11):2569–77. https://doi.org/10.1177/0363546512458247.
Ozaki R, Nakagawa S, Mizuno N, Mae T, Yoneda M. Hill-sachs lesions in shoulders with traumatic anterior instability: evaluation using computed tomography with 3-dimensional reconstruction. Am J Sports Med. 2014;42(11):2597–605. https://doi.org/10.1177/0363546514549543.
Yamamoto N, Itoi E, Abe H, Minagawa H, Seki N, Shimada Y, et al. Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: a new concept of glenoid track. J Shoulder Elb Surg. 2007;16(5):649–56. https://doi.org/10.1016/j.jse.2006.12.012.
Yang JS, Mehran N, Mazzocca AD, Pearl ML, Chen VW, Arciero RA. Remplissage versus modified Latarjet for off-Track Hill-Sachs lesions with subcritical Glenoid bone loss. Am J Sports Med. 2018;46(8):1885–91. https://doi.org/10.1177/0363546518767850.
Neer CS 2nd, Foster CR. Inferior capsular shift for involuntary inferior and multidirectional instability of the shoulder. A preliminary report. J Bone Joint Surg Am. 1980;62(6):897–908.
Ciccotti MC, Syed U, Hoffman R, Abboud JA, Ciccotti MG, Freedman KB. Return to play criteria following surgical stabilization for traumatic anterior shoulder instability: a systematic review. Arthroscopy. 2018;34(3):903–13. https://doi.org/10.1016/j.arthro.2017.08.293.
Williams RJ 3rd. Editorial commentary: reviewing the science of our unscientific criteria for return to sports after shoulder stabilization. Arthroscopy. 2018;34(3):914–6. https://doi.org/10.1016/j.arthro.2017.12.015.
Ialenti MN, Mulvihill JD, Feinstein M, Zhang AL, Feeley BT. Return to play following shoulder stabilization: a systematic review and meta-analysis. Orthop J Sports Med. 2017;5(9):2325967117726055. https://doi.org/10.1177/2325967117726055.
Ma R, Brimmo OA, Li X, Colbert L. Current concepts in rehabilitation for traumatic anterior shoulder instability. Curr Rev Musculoskelet Med. 2017;10(4):499–506. https://doi.org/10.1007/s12178-017-9449-9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Nicholas A. Bonazza declares that he has no conflict of interest. Jonathan C. Riboh reports Stock options in Restor3d; Research support from Sparta Biopharma.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pediatric Orthopedics
Rights and permissions
About this article
Cite this article
Bonazza, N.A., Riboh, J.C. Management of Recurrent Anterior Shoulder Instability After Surgical Stabilization in Children and Adolescents. Curr Rev Musculoskelet Med 13, 164–172 (2020). https://doi.org/10.1007/s12178-020-09612-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12178-020-09612-4