Abstract
Purpose of Review
Congenital pseudoarthrosis of the tibia and fibula are rare conditions that share common treatment strategies. The purpose of this review is to provide an overview of the recent developments in treatments for both conditions.
Recent Findings
Recent literature has focused on the use of BMP and on gait analysis as a tool for measuring long-term functional outcomes. Recent study has indicated rhBMP-2 may shorten the time to initial healing of pseudoarthroses, but not guarantee bony union. Children with initial fractures before the age of four have been shown to have long-term gait outcomes that may be ultimately comparable to children with prostheses.
Summary
Both congenital pseudoarthrosis of the tibia and fibula are challenging conditions to treat, which require comprehensive approaches to account for both the biological and mechanical components of the conditions.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Congenital pseudoarthrosis of the tibia and fibula are rare, and their presentation usually does not pose a significant diagnostic dilemma. However, their management is challenging and spans many years. A comprehensive approach to assessment and management is imperative. Long-term function should remain the focus of decision-making. The greatest changes in management in recent years has come through the use of bone morphogenic proteins, rod constructs, and guided growth in deformity correction.
Congenital Pseudoarthrosis of the Tibia
Congenital pseudoarthrosis of the tibia (CPT) is typically detected in early childhood with a reported prevalence between 1: 140,000 and 1: 250,000. [1, 2•, 3] Although uncommon, CPT is the most frequently observed type of congenital pseudoarthrosis. [1] Although the condition is termed “congenital,” a true non-union is not present from birth in the majority of cases [1, 4,5,6,7,8,9,10,11]. Rather, the affected tibia presents with a dysplastic, anterolateral bow, cystic pre-fracture, and failure of tubulation early in life (Fig. 1) [1, 5, 8, 10]. Segmental dysplasia and bowing may then progress to fracture in between 15% and 57% of reported cases [2•, 5, 8, 12]. The exact etiology of CPT is unknown and controversy remains over the osteogenic capacity of CPT lesion tissue [3, 7, 10, 13, 14]. Most of the established literature contends that cells from pseudoarthrotic lesions demonstrate decreased osteogenic capability [15,16,17,18,19]. However, a recent case study has been published, which indicates CPT lesion cells may demonstrate osteogenic capacity in vitro [20].
Neurofibromatosis is associated with CPT in between 38% and 90% of patients [1, 2•, 4, 5, 7, 10, 13, 21, 22]. A multidisciplinary approach with genetic counseling to screen for neurofibromatosis is recommended in all patients diagnosed with CPT [23]. Fibular abnormalities are found to be associated with CPT in between 60% and 90% of patients [21, 24, 25]. The pseudoarthrosis typically occurs within the first 4–5 years of life [1]. Multiple classification systems have been proposed to categorize the extreme variability of this condition [1, 4, 7, 9, 13, 26,27,28]. However, there has been little correlation between these classification systems and treatment outcomes, especially in prospective research. [1, 13, 22]
Treatment is wide-ranging and often challenging, incorporating both non-operative and operative elements [1, 2, 29]. If a patient presents anterolateral bowing, with radiographic tibial abnormalities demonstrating risk of CPT, but prior to any true “fracture,” both non-operative treatment with bracing and prophylactic bone-grafting have been used to delay or avoid the development of pseudoarthrosis. The three most commonly used surgical techniques once a fracture has occurred or pseudoarthrosis has clearly developed are intramedullary rod fixation, circular ring fixation, and vascularized fibular grafting. The primary goal for all of these surgical interventions is bony union of the pseudoarthrosis site [14, 30•, 31, 32]. However, all operations are prone to high rates of complications, including non-union and refracture. In between 8% and 33% of cases, amputation may be indicated for patients with poor functional results after the course of treatment, if it is determined that the patient may be better served by a prosthesis [1, 7, 29, 33, 34].
Non-Operative Treatment
Once a tibial bow has been identified in a patient who may develop CPT, non-operative treatment should begin immediately in order to prevent or delay fracture [1, 6, 21]. One goal of extending the pre-intervention period is to allow growth of the eventual distal tibial fragment [6], given that a challenging aspect of surgical intervention post-fracture can be the small size of the distal fragment [9, 13]. It has been found that delaying surgical treatment in order to allow for this extended period of supported growth may be beneficial for achieving union with less functional morbidity in fewer operations [6]. The use of orthoses, pre-fracture, to prevent or delay the development of pseudoarthroses can have a positive impact on post-operative surgical results later in the course of treatment [3]. An ankle-foot orthosis (AFO) for infants prior to their beginning to walk and a knee-ankle-foot orthosis (KAFO) after they pass that milestone are recommended [1].
Prophylactic Bone-Grafting
While patients remain pre-pseudoarthrotic, prophylactic bone-grafting may be beneficial to prevent fracture [1, 5, 12, 21]. Through this procedure, a fibular graft strut is used to protect and support the dysplastic, bowed tibia (Fig. 2). Although McFarland first described the technique of bypass grafting in 1939, Lloyd-Roberts and Shaw were the first to use the procedure in pre-pseudoarthrotic patients [5, 35]. Proponents of the technique contend that while patients may experience fractures while in compliance with bracing protocols, prophylactic bone-grafting may delay fracture if performed early, before pseudoarthroses start to develop [12, 21]. Bypass grafting is not recommended for patients with established pseudoarthroses as a primary treatment, due to higher rates of persistent pseudoarthrosis [5, 21]. One benefit of bypass grafting is that it does not preclude patients from other surgical options if pseudoarthroses do develop [12]. However, in Ofluoglu et al.’s 2008 study of 10 patients treated with prophylactic bone-grafting, all exhibited sustained tibial union at last follow up, although most patients displayed some residual deformity [21].
Anteroposterior and lateral radiographs showing an anterolaterally bowed tibia with associated fibular nonunion. The tibia received a fibular strut bypass graft. The fibula was spanned by a Rush rod and underwent additional bone-grafting. (Images courtesy of Children’s Orthopedic Surgery Foundation)
Intramedullary rod Fixation w/ Autologous Graft
Charnley first introduced the concept of using an intramedullary stainless steel nail as a means of fixation and support for the tibia in cases of CPT in 1956 [36]. The addition of autologous bone-grafting to the Charnley-Williams technique has now become standard of care (Fig. 3) [1, 37]. A review in 2002 examined the effect that variations in technique have on outcomes and found that IM fixations that did not address the fibula in addition to the tibia were ineffective in achieving union over the course of long-term follow up [30•]. This finding remains controversial [1, 29]. The age at fracture has been correlated to functional outcomes as compared to a control group of patients who underwent amputation [6]. All but one patient in the non-amputation cohort underwent IM rod fixation. The results indicate that the age of initial fracture does make a consequential difference to long-term functional outcomes. Children with early fracture (< 4 years) exhibited comparable gait inefficiencies to children with prostheses [6].
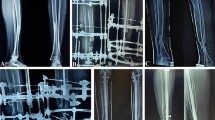
a Pre-operative anteroposterior radiograph illustrating tibial dysplasia with pseudoarthrosis of the mid-distal shaft. b Post-operative anteroposterior radiograph. c Post-operative lateral radiograph. The tibia underwent an osteotomy to excise the pseudoarthrosis and received an IM rod with BMP-2 and iliac crest autograft. The fibula underwent osteotomy and healing. (Images courtesy of Children’s Orthopedic Surgery Foundation)
According to a 2018 meta-analysis by Kesireddy et al., the rate of initial union for IM rod fixation with cortical bone grafts is 74% [2•]. However, the most common complications of this surgery continue to be refracture, ankle valgus deformity, limb-length discrepancy secondary to tibial shortening, and ankle stiffness [1, 29, 30•, 37]. According to their meta-analysis, the published refracture rate for IM fixation is 45% [2•]. There is broad agreement that IM rods should stay in situ as long as possible to minimize the risk of refracture [30•, 36, 37]. However, some authors assert that leaving the rods in for extended periods across the ankle increases the risk of ankle stiffness and muscle atrophy [6, 9, 34, 38•]. In order to minimize the prevalence and severity of this complication, some authors recommend surgically advancing the rod past the ankle joint once the pseudoarthrosis is healed [29].
There is broad agreement that, although valgus deformity is common with CPT and can compromise functional results, such ankle deformity is part of the natural history of CPT rather than an iatrogenic complication of the IM rod crossing the physis [1, 29, 34]. Staples, screws, or an eight-plate across distal tibial physis can be used to correct ankle valgus over what is often a course of 1 to 2 years [1].
Tibial shortening should be expected in almost all CPT patients treated with IM rod fixation [34]. Leg length discrepancy has been found to occur at a rate of 79%, with a mean discrepancy of 2.64 cm for patients with IM rod fixation with autograft [2•]. Shortening is thought to be the result of bone resorption at the pseudoarthrosis site, as well as resection during surgery, rather than physeal injury [29].
Recent study has been undertaken to examine the effects of coupling rhBMP-2, a bone morphogenetic protein, to the IM rod fixation technique [31, 32]. Results indicate that rhBMP-2 may be useful in shortening the time to initial healing of pseudoarthroses but not in guaranteeing bony healing [31, 32]. The addition of rhBMP-2 does not appear to affect refracture rates [31]. There has not been reported any increased rates of complications, such as physeal disturbance, development of primary or secondary tumors, localized tissue reactions, allergic reactions, or infections [31, 32]. However, the published work on rhBMP-2 implications for CPT treatment to date has been largely small retrospective case series. The Children’s Tumor Foundation NF1 Bone Abnormalities Consortium has called for clinical trials to be undertaken to investigate the efficacy of rhBMP-2 and provide evidence-based treatments for CPT [39].
Circular External Fixator and Bone Transport
First described by Ilizarov in 1971, one of the main benefits of an external fixation technique is that it may be used to approach pseudoarthrotic lesions and all of their potential complications, including leg length discrepancy, refracture and ankle valgus, comprehensively [1, 3, 14, 40]. One of the key advantages of the Ilizarov technique is that it may provide a multitargeted approach [38•]; external fixation may be used for compression, distraction, or bone transfer at different tibial levels (Fig. 4) [1, 14, 38•]. Additionally, external fixation may benefit patients by avoiding the donor site morbidity of contralateral free fibular harvest [22]. However, patients in this age group tolerate external fixation devices less well than internal fixation methods and external methods carry an increased risk of infection [14]. The length and complexity of treatment, as well as risk of infection, are potential disadvantages of the technique [22]. Femoral overgrowth potentially triggered by the hyperemic stimulation of distraction osteogenesis has been documented [41]. However, it has also been noted that femoral overgrowth also may occur in atrophic-type CPT patients who have not undergone Ilizarov treatment [41].
The rate of initial union for Ilizarov procedure is 66% and the rate of refracture was 51% in one study [2•]. Although the maximization of cross-sectional healing at the level of the pseudoarthrosis is thought to be important for minimizing the risk of refracture, the united bone may be biologically and mechanically inferior leading to an increased risk of refracture [14, 33, 42]. It has been reported that fibrous hamartomatous tissue was found in all 15 refractures that were explored in one series, leading the authors to conclude that refracture may be the result of a biological as well as mechanical process [42]. Two studies have shown better healing in older children; one had higher healing over 4 years of age and the other showed an increased rate of healing in children older than 3 years [3, 42].
Combination of Intramedullary Rod Fixation and Ilizarov Fixator
The advantage of using a united surgical approach with both IM rod fixation and an Ilizarov fixator is that the technique may combine the benefits of both procedures [40]. In particular, the goal of this combined method is to benefit from the IM rod’s lower refracturing potential and the Ilizarov device’s high rate of union and alignment control [40, 43]. The rate of initial union for this combined approach in one study was 83% and the rate of refracture was 16% [2•]. These rates represent both the highest rate of initial union and lowest rate of refracture reported in a meta-analysis. It is proposed that the low rate of refracture is based upon the correction of diaphyseal alignment, fibular union, and post-operative care, including permanently protecting the tibia with orthoses and an intramedullary nail [40]. This hypothesis is supported by Kesireddy et al.’s report that a combined surgical approach utilizing IM rod fixation and an Ilizarov fixator with cortical bone graft provides the best post-operative results in terms of time to union, refractures, and number of unions [2•].
Vascularized Fibula Graft
Taylor et al. were the first to describe the utilization of vascularized bone graft using microsurgical techniques for the treatment of CPT in 1975 [44]. One of the difficulties of treating CPT is the decreased blood supply to the distal tibial fragment post-fracture [45]. Low blood supply to the affected distal tibia, even after surgical intervention, may contribute to poor healing and non-union [45]. Weiland et al. suggest that the avascular nature of this condition may decrease the practicality of non-vascularized graft use once fracture has occurred [46]. Proponents of vascularized fibula grafts (VFGs) contend that the new blood supply introduced by the procedure strike at one of the main treatment hurdles facing patients with CPT treated with grafts: graft resorption and replacement [45, 47, 48]. Although the procedure is technically challenging and the approach risks injury to the unaffected leg, its proponents assert that this approach offers a good option for patients with a large gap at their pseudoarthrosis site, or once other approaches have failed [1, 47, 48].
Reported rates of initial union and refracture for VFG with IM rod or screw fixation are 66% and 29%, respectively, while reported the rates of initial union and refracture for VFG with external fixation are 100% and 45% respectively, in small series [2•]. Complications for VFG include progressive valgus of both the recipient and donor ankles, in addition to the same set of post-operative complications described above [46, 47, 49]. Some authors advocate for the use of tibiofibular synostoses as a preventative measure in the well leg for patients receiving VFGs as a means to combat the potential development of ankle valgus [46]. However, others have suggested that donor leg tibiofibular synostoses do not have an effect on the development of ankle valgus and state that regardless of prophylactic surgical intervention, there is a reported rate of contralateral/VFG-donor ankle valgus of 25% [48]. Tan et al. therefore suggest a method of ipsilateral fibula transfer to reduce surgical times and decrease both the risk of vascular compromise, as well as the risk of injury or growth disturbance to the contralateral extremity [48]. However, this technique is heavily dependent on having a suitable fibula for transfer and adversely affects the bony lateral support to the involved limb.
Amputation
Amputation, its timing, indications and efficacy in treating CPT, is controversial. While some feel that amputation should be considered as a last resort or that there is no therapeutic indication for amputation in patients with CPT, others suggest it may be beneficial to perform an amputation early in CPT treatment [1, 13, 50]. Among those who advocate for amputation, many agree that the indications for surgery include the following: failure of pseudoarthrotic union after three attempts, leg length discrepancy greater than 5 cm, the development of a deformed foot, and excessive functional loss of the lower extremity [1, 48, 50,51,52]. These indications were established by McCarthy in 1981 [51]. With research into modern surgical techniques, such as the use of rhBMP, some authors are looking for ways to redefine these indications and prevent amputations in patients with CPT [53, 54].
There are three major types of amputation that are utilized in the care of CPT patients: Boyd, Syme, and transtibial (through the pseudoarthrotic lesion) [1, 50, 52, 55•, 56]. Boyd and Syme are both ankle-level amputations thought to treat CPT by removing the torque force of the foot from the lower extremity [55•, 56].
First described by Syme in 1843, Syme amputations differ from Boyd in that Syme are transmalleolar amputations (Fig. 5) and in Boyd amputations the calcaneus is preserved [52, 57]. In both operations, the heel pad is salvaged as a weight-bearing surface [52, 57]. Additionally, both Syme and Boyd amputations offer the benefit of conserving the distal epiphyses, which more proximal amputations remove [52]. Preserving the distal epiphyses reduces the risk of diaphyseal overgrowth-related complications [51].
The Boyd amputation, first described in 1939 by Boyd, was created to avoid some of the common complications of the Syme amputation. In this procedure the calcaneus is preserved distally to allow extra length and stability for the stump [57, 58]. The advantages of the Boyd amputation are increased heel pad stabilization, improved prosthetic suspension, and increased lower limb functionality [56, 58]. Recently, Westbury reported a 69% radiographic union rate of pseudoarthrotic lesions in CPT patients treated with a combined method of a Boyd amputation with tibial rodding [55•]. They attributed the success of their method to continual fracture site compression due to the high end-bearing capacity of the residual limb in a prosthesis, optimal alignment of the limb, complete resection of the pseudoarthrosis site, and the availability and use of copious allograft [55•].
The potential problem of diaphyseal overgrowth is one reason that some authors assert that amputation through the site of pseudoarthrosis is generally not favored for skeletally immature children [55•]. Other cited disadvantages of transtibial amputation through the pseudoarthrotic site are a poor weight-bearing surface, and the more proximal amputation may make for a short residual limb, which may compromise prosthesis fit and functionality [50, 55•].
There is broad agreement that patient conversations regarding amputation should take place early in treatment, both to explain treatment options as well as to prepare patients and families mentally for the risk that amputation may become their best treatment option [11, 50]. In addition to intractable non-union, amputation may be considered or proposed to address pain or poor limb functionality and avoid repeated lengthy hospitalizations [52, 55•].
Conclusions
CPT is a rare condition often associated with neurofibromatosis that may present originally as tibial bowing and later develop into a pseudoarthrotic lesion or may initially present as a fracture. CPT treatment is often challenging, and a wide array of surgical interventions may be utilized for its treatment once lesion development occurs. The most commonly pursued surgical options today include intramedullary rod fixation and/or circular ring fixation, combined with allograft and BMP, with some centers additionally pursuing vascularized fibular grafting. However, all surgical interventions have relatively high rates of non-union, refracture, and other complications. In some cases, amputation may be indicated for patients, particularly in the setting of multiple treatment failures.
Congenital Pseudoarthrosis of the Fibula
Introduction and classification
Congenital pseudoarthrosis of the fibula (CPF) is significantly less common than CPT. However, similar to CPT, it is associated with neurofibromatosis in approximately 40% of patients [59]. Although fibular bowing or pre-pseudoarthrotic changes are present from birth, the diagnosis of CPF like CPT is often delayed until the activities of childhood cause the condition to become symptomatic [59,60,61,62,63]. The fibula bears between 7% and 17% of the weight in the leg, which may contribute to this finding [64, 65]. Dooley and Menelaus have classified CPF into four categories: (1) fibular bowing without fibular pseudoarthrosis, (2) fibular pseudoarthrosis with and (3) without ankle deformity, and (4) fibular pseudoarthrosis with late development of pseudoarthrosis of the tibia (Fig. 6) [66]. Cho has recommended that the last Dooley category, which includes pseudoarthrosis of the tibia, be categorized as a class of tibial pseudoarthrosis, given that the treatment and outcomes of those patients are more dependent upon the tibial condition [62]. Given the high comorbidity rate between fibular pseudoarthrosis and tibial pseudoarthrosis and dysplasia (between 14% and 80% in the reported literature), it is recommended to obtain full-length radiographs of the tibia to assess for tibial dysplasia [29, 30, 33, 34, 42, 60, 61].
Clinical presentation
When pseudoarthroses of the fibula become symptomatic, patients may present with an abnormal gait, valgus deformity of the ankle, or a prominent fibula [1, 62, 66,67,68,69]. Because non-union occurs almost exclusively in the distal quarter of the fibula in CPF, the fibula is no longer able to effectively provide lateral support to the talus through the lateral malleolus in these patients [60, 62, 70,71,72]. Lack of lateral support produces lateral instability of the ankle joint which may load stress across the lateral aspect of the lower tibial epiphysis resulting in ankle valgus [62, 67]. Wiltse also postulates that the push of the distal fibula is necessary for completing normal growth; its absence causes a biomechanical disturbance that should be addressed surgically [73].
It is important to note that pre-pseudoarthrotic changes to the fibula do not lead to pseudoarthrotic lesions in all cases. In a study of 12 patients with congenital pseudoarthrosis of the fibula, it was found that some fibulae may stay intact until skeletal maturity [62]. There is however a progression in patients’ ankles from varus to valgus alignment [62]. Patients with CPF may initially present with a varus deformity of their ankle due to fibular bowing, however over time convert their alignments into valgus due through fibular shortening [1, 62].
Management
The management of patients with CPF begins with serial clinical assessment and radiographs [74]. Prophylactic splinting or bracing has been recommended for patients who have not yet developed a pseudoarthrosis [63, 66, 74, 75], though some authors suggest that bracing’s efficacy is unsupported [59, 62].
If splinting fails or a pseudoarthrosis develops, osteosynthesis (Fig. 7) is indicated for patients with large distal fibular fragments when the space left by the excised lesion can be bridged by a bone graft [1, 60,61,62]. Cho advocated performing well-timed osteosyntheses in CPF patients, preferably when the patient’s ankle had regained a neutral alignment on its projected swing from ankle varus to valgus [62]. Martus and Johnston reviewed five CPF patients who underwent osteosyntheses and found that four of their patients achieved union with their primary operation [67]. Three of those patients went on to maintain clinically neutral ankle alignment over 6.5 years of post-operative follow-up time [67]. They therefore recommend osteosynthesis in skeletally immature patients with CPF to prevent progressive ankle valgus during growth [67]. This recommendation is shared by others [1, 60, 72]. In the case that a fibular osteosynthesis is not possible due to ankle valgus or severe involvement of the fibula, a distal tibial-fibular synostosis should be performed to prevent progressive valgus [1, 62, 67, 73].
Distal tibial-fibular synostosis (Fig. 8) was first described by Langenskiӧld in 1967 [68]. Supporters of this procedure assert that fusing the metaphyses of the distal tibia and fibula will stabilize the ankle joint and prevent progressive valgus [1, 60,61,62,63, 66, 73]. However, controversy exists over whether the procedure should be a primary or secondary operation, or if it should be used only if osteosynthesis is not an option. The distal tibial and fibular physes have been shown to grow at slightly different average rates: 5 mm and 4.5 mm per year respectively [76]. Therefore, some authors argue that, by fusing the two bones together, surgeons create a situation in which unequal distal physeal growth forces the ankle into valgus alignment [67, 77] and recommend tibiofibular synostosis only in the event that osteosynthesis had failed or is not feasible [67]. They warn that, although synostoses may prevent severe ankle valgus, some valgus may still occur or be caused by the surgery [67]. Surgeons who use this surgery contend that while the resulting ankle valgus after synostosis may become clinically significant, synostosis forestalls a greater shortening into ankle valgus due to fibular migration [68].
Medial hemiepiphysiodesis of the tibia by either staple or screw to correct the valgus deformity may be recommended for patients who undergo a tibiofibular synostosis or osteosynthesis (Fig. 9) [60,61,62, 73]. Screw fixation is the main technique used, while other options include partial physeal ablation and staple fixation, although these techniques are becoming less common. Partial physeal ablation has previously been used, however is irreversible and therefore not a good option for young patients. Staple or 8-plate fixation may be indicated with valgus deformity however due to the subcutaneous location of the medial malleolus implant prominence is problematic [61].
Once patients reach skeletal maturity and exhibit valgus alignment, there is broad agreement that supramalleolar osteotomy is the appropriate management when symptomatic. The Ilizarov technique can be used to restore fibular length in combination with a distal tibial osteotomy and restore neutral ankle alignment [1, 62].
Conclusions
Congenital pseudoarthrosis of the fibula is a condition even more rare than CPT, with few cases reported in the English literature. Therefore, most information to support hypotheses about the different surgical techniques comes from case reports or small cohort studies. The most common surgical procedures to treat CPF in the current literature include osteosynthesis, tibiofibular synostosis, and medial hemiepiphysiodesis of the tibia.
Summation
The management of congenital pseudoarthrosis of the tibia and fibula requires a comprehensive approach which considers the biology of the condition and mechanical alignment of the extremity. A variety of techniques may need to be employed, and there is no one approach that fits all. It is essential to consider the impact that a treatment course will have on a child and their family.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Lovell WW, Weintstein SL, Flynn JM. Lovell and Winter’s pediatric orthopaedics. 7th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2014.
• Kesireddy N, Kheireldin RK, Lu A, Cooper J, Liu J, Ebraheim NA. Current treatment of congenital pseudarthrosis of the tibia: a systematic review and meta-analysis. J Pediatr Orthop B. 2018. https://doi.org/10.1097/bpb.0000000000000524 Meta-analysis estabishing statistical significance across studies on congenital pseudoarthrosis of the tibia.
Grill F, Bollini G, Dungl P, Fixsen J, Hefti F, Ippolito E, et al. Treatment approaches for congenital pseudarthrosis of tibia: results of the EPOS multicenter study. European Paediatric Orthopaedic Society (EPOS). J Pediatr Orthop B. 2000;9(2):75–89.
Sofield HA. Congenital pseudarthrosis of the tibia. Clin Orthop Relat Res. 1971;76:33–42.
Lloyd-Roberts GC, Shaw NE. The prevention of pseudarthrosis in congenital kyphosis of the tibia. J Bone Joint Surg Br Vol. 1969;51(1):100–5.
Karol LA, Haideri NF, Halliday SE, Smitherman TB, Johnston CE 2nd. Gait analysis and muscle strength in children with congenital pseudarthrosis of the tibia: the effect of treatment. J Pediatr Orthop. 1998;18(3):381–6.
Masserman RL, Peterson HA, Bianco AJ Jr. Congenital Pseudoarthosis of the tibia a review of the literature and 52 cases from the Mayo Clinic. Clin Orthop Relat Res. 1974;99(140):140–5.
Badgley CE, O'Connor SJ, Kudner DF. Congenital kyphoscoliotic tibia. J Bone Joint Surg Am. 1952;34-a(2):349.
Boyd HB, Sage FP. Congenital pseudarthrosis of the tibia. J Bone Joint Surg Am. 1958;40-a(6):1245–70.
Boyd HB. Pathology and natural history of congenital pseudarthrosis of the tibia. Clin Orthop Relat Res. 1982;(166):5–13.
Morrissy RT, Riseborough EJ, Hall JE. Congenital pseudarthrosis of the tibia. J Bone Joint Surg Br Vol. 1981;63-b(3):367–75.
Strong ML, Wong-Chung J. Prophylactic bypass grafting of the prepseudarthrotic tibia in neurofibromatosis. J Pediatr Orthop. 1991;11(6):757–64.
Morrissy RT. Congenital pseudoarthosis of the tibia, factors that affect results. Clin Orthop Relat Res. 1982;(21):21–7.
Paley D, Catagni M, Argnani F, Prevot J, Bell D, Armstrong P. Treatment of congenital pseudoarthrosis of the tibia using the Ilizarov technique. Clin Orthop Relat Res. 1992;(280):81–93.
Cho TJ, Seo JB, Kim JA, Lee DY, Yoo WJ, Chung CY, et al. Fibrous hamartoma at atrophic congenital pseudoarthrosis of the tibia is not osteogenic but osteoclastic. San Diego: Orthopedic Reserach Society; 2007.
Seebach C, Henrich D, Tewksbury R, Wilhelm K, Marzi I. Number and proliferative capacity of human mesenchymal stem cells are modulated positively in multiple trauma patients and negatively in atrophic nonunions. Calcif Tissue Int. 2007;80(4):294–300. https://doi.org/10.1007/s00223-007-9020-6.
Hofmann A, Ritz U, Hessmann MH, Schmid C, Tresch A, Rompe JD, et al. Cell viability, osteoblast differentiation, and gene expression are altered in human osteoblasts from hypertrophic fracture non-unions. Bone. 2008;42(5):894–906. https://doi.org/10.1016/j.bone.2008.01.013.
Leskela HV, Kuorilehto T, Risteli J, Koivunen J, Nissinen M, Peltonen S, et al. Congenital pseudarthrosis of neurofibromatosis type 1: impaired osteoblast differentiation and function and altered NF1 gene expression. Bone. 2009;44(2):243–50. https://doi.org/10.1016/j.bone.2008.10.050.
Granchi D, Devescovi V, Baglio SR, Leonardi E, Donzelli O, Magnani M, et al. Biological basis for the use of autologous bone marrow stromal cells in the treatment of congenital pseudarthrosis of the tibia. Bone. 2010;46(3):780–8. https://doi.org/10.1016/j.bone.2009.10.044.
Diaz-Solano D, Wittig O, Mota JD, Cardier JE. Isolation and Characterization of multipotential mesenchymal stromal cells from congenital pseudoarthrosis of the tibia: case report. Anat Rec (Hoboken, NJ : 2007). 2015;298(10):1804–14. https://doi.org/10.1002/ar.23198.
Ofluoglu O, Davidson RS, Dormans JP. Prophylactic bypass grafting and long-term bracing in the management of anterolateral bowing of the tibia and neurofibromatosis-1. J Bone Joint Surg Am. 2008;90(10):2126–34. https://doi.org/10.2106/jbjs.g.00272.
Boero S, Catagni M, Donzelli O, Facchini R, Frediani PV. Congenital pseudarthrosis of the tibia associated with neurofibromatosis-1: treatment with Ilizarov’s device. J Pediatr Orthop. 1997;17(5):675–84.
Van Royen K, Brems H, Legius E, Lammens J, Laumen A. Prevalence of neurofibromatosis type 1 in congenital pseudarthrosis of the tibia. Eur J Pediatr. 2016;175(9):1193–8. https://doi.org/10.1007/s00431-016-2757-z.
Tudisco C, Bollini G, Dungl P, Fixen J, Grill F, Hefti F, et al. Functional results at the end of skeletal growth in 30 patients affected by congenital pseudoarthrosis of the tibia. J Pediatr Orthop B. 2000;9(2):94–102.
Keret D, Bollini G, Dungl P, Fixsen J, Grill F, Hefti F, et al. The fibula in congenital pseudoarthrosis of the tibia: the EPOS multicenter study. European Paediatric Orthopaedic Society (EPOS). J Pediatr Orthop B. 2000;9(2):69–74.
Andersen KS. Congenital pseudarthrosis of the leg. Late results. J Bone Joint Surg Am. 1976;58(5):657–62.
Bassett CA, Caulo N, Kort J. Congenital “pseudarthroses” of the tibia: treatment with pulsing electromagnetic fields. Clin Orthop Relat Res. 1981;(154):136–48.
McFarland B. Pseudarthrosis of the tibia in childhood. J Bone Joint Surg Br Vol. 1951;33-b(1):36–46.
Dobbs MB, Rich MM, Gordon JE, Szymanski DA, Schoenecker PL. Use of an intramedullary rod for treatment of congenital pseudarthrosis of the tibia. A long-term follow-up study. J Bone Joint Surg Am. 2004;86-a(6):1186–97.
• Johnston CE 2nd. Congenital pseudarthrosis of the tibia: results of technical variations in the charnley-williams procedure. J Bone Joint Surg Am. 2002;84-a(10):1799–810 Examining the potenial benefits of rhBMP-2, this study contributes to the literature by evaluating the complication rates of patients treated with rhBMP-2 and patients' time to radiographic union.
Richards BS, Anderson TD. rhBMP-2 and intramedullary fixation in congenital pseudarthrosis of the tibia. J Pediatr Orthop. 2018;38(4):230–8. https://doi.org/10.1097/bpo.0000000000000789.
Richards BS, Oetgen ME, Johnston CE. The use of rhBMP-2 for the treatment of congenital pseudarthrosis of the tibia: a case series. J Bone Joint Surg Am. 2010;92(1):177–85. https://doi.org/10.2106/jbjs.h.01667.
Vanderstappen J, Lammens J, Berger P, Laumen A. Ilizarov bone transport as a treatment of congenital pseudarthrosis of the tibia: a long-term follow-up study. J Child Orthop. 2015;9(4):319–24. https://doi.org/10.1007/s11832-015-0675-7.
Anderson DJ, Schoenecker PL, Sheridan JJ, Rich MM. Use of an intramedullary rod for the treatment of congenital pseudoarthrosis of the tibia. J Bone Joint Surg. 1992;74(161):161–8.
McFarland B. Birth fracture of the tibia. Br J Surg. 1939;27:706–12.
Charnley J. Congenital pseudarthrosis of the tibia treated by intramedullary nail. J Bone Joint Surg Am. 1956;38-a(2):283–90.
Umber JS, Moss SW, Coleman SS. Surgical treatment of congenital pseudoarthrosis of the tibia. Clin Orthop Relat Res. 1982;28(166):28–33.
• Seo SG, Lee DY, Kim YS, Yoo WJ, Cho TJ, Choi IH. Foot and ankle function at maturity after Ilizarov treatment for atrophic-type congenital pseudarthrosis of the tibia: a comprehensive outcome comparison with normal controls. J Bone Joint Surg Am. 2016;98(6):490–8. https://doi.org/10.2106/jbjs.15.00964.
Stevenson DA, Little D, Armstrong L, Crawford AH, Eastwood D, Friedman JM, et al. Approaches to treating NF1 tibial pseudarthrosis: consensus from the Children’s Tumor Foundation NF1 bone abnormalities consortium. J Pediatr Orthop. 2013;33(3):269–75. https://doi.org/10.1097/BPO.0b013e31828121b8.
Mathieu L, Vialle R, Thevenin-Lemoine C, Mary P, Damsin JP. Association of Ilizarov’s technique and intramedullary rodding in the treatment of congenital pseudarthrosis of the tibia. J Child Orthop. 2008;2(6):449–55. https://doi.org/10.1007/s11832-008-0139-4.
Song MH, Park MS, Yoo WJ, Cho TJ, Choi IH. Femoral overgrowth in children with congenital pseudarthrosis of the tibia. BMC Musculoskelet Disord. 2016;17:274. https://doi.org/10.1186/s12891-016-1157-x.
Cho TJ, Choi IH, Lee SM, Chung CY, Yoo WJ, Lee DY, et al. Refracture after Ilizarov osteosynthesis in atrophic-type congenital pseudarthrosis of the tibia. J Bone Joint Surg Br Vol. 2008;90(4):488–93. https://doi.org/10.1302/0301-620x.90b4.20153.
• Zhu GH, Mei HB, He RG, Liu YX, Liu K, Tang J, et al. Combination of intramedullary rod, wrapping bone grafting and Ilizarov’s fixator for the treatment of Crawford type IV congenital pseudarthrosis of the tibia: mid-term follow up of 56 cases. BMC Musculoskelet Disord. 2016;17(1):443. https://doi.org/10.1186/s12891-016-1295-1 By contributing a large number of CPT cases to the published literature, this study significantly enhances our understanding of outcomes following Ilizarov treatment and bone grafting.
Taylor GI, Miller GD, Ham FJ. The free vascularized bone graft. A clinical extension of microvascular techniques. Plast Reconstr Surg. 1975;55(5):533–44.
Hagan KF, Buncke HJ. Treatment of congenital pseudarthrosis of the tibia with free vascularized bone graft. Clin Orthop Relat Res. 1982;(166):34–44.
Weiland AJ, Weiss AP, Moore JR, Tolo VT. Vascularized fibular grafts in the treatment of congenital pseudarthrosis of the tibia. J Bone Joint Surg Am. 1990;72(5):654–62.
Dormans JP, Krajbich JI, Zuker R, Demuynk M. Congenital pseudarthrosis of the tibia: treatment with free vascularized fibular grafts. J Pediatr Orthop. 1990;10(5):623–8.
Tan JS, Roach JW, Wang AA. Transfer of ipsilateral fibula on vascular pedicle for treatment of congenital pseudarthrosis of the tibia. J Pediatr Orthop. 2011;31(1):72–8. https://doi.org/10.1097/BPO.0b013e318202c243.
Pho RWH, Levack B, Satku K, Patradul A. Free vascularized fibular graft in the treatment of congenital pseudoarthrosis of the tibia. J Bone Joint Surg Br. 1985;67(1):64–70.
Vander Have KL, Hensinger RN, Caird M, Johnston C, Farley FA. Congenital pseudarthrosis of the tibia. J Am Acad Orthop Surg. 2008;16(4):228–36.
McCarthy RE. Amputation for congenital pseudarthrosis of the tibia. Indications and techniques. Clin Orthop Relat Res. 1982;(166):58–61.
Jacobsen ST, Crawford AH, Millar EA, Steel HH. The Syme amputation in patients with congenital pseudarthrosis of the tibia. J Bone Joint Surg Am. 1983;65(4):533–7.
Shabtai L, Ezra E, Wientroub S, Segev E. Congenital tibial pseudarthrosis, changes in treatment protocol. J Pediatr Orthop B. 2015;24(5):444–9. https://doi.org/10.1097/bpb.0000000000000191.
Shah H, Doddabasappa SN, Joseph B. Congenital pseudarthrosis of the tibia treated with intramedullary rodding and cortical bone grafting: a follow-up study at skeletal maturity. J Pediatr Orthop. 2011;31(1):79–88. https://doi.org/10.1097/BPO.0b013e318202c45d.
• Westberry DE, Carpenter AM, Tisch J, Wack LI. Amputation outcomes in congenital pseudarthrosis of the tibia. J Pediatr Orthop. 2018;38(8):e475–e81. https://doi.org/10.1097/bpo.0000000000001211 Focusing on the long-term outcomes of CPT patients who have undergone amputation, this retrospective study adds to the literature by describing pseudoarthrotic union rates post-amputation.
Edvardsen P. Resection osteosynthesis and Boyd amputation for congenital pseudarthrosis of the tibia. J Bone Joint Surg Br Vol. 1973;55(1):179–82.
Eilert RE, Jayakumar SS. Boyd and Syme ankle amputations in children. J Bone Joint Surg Am. 1976;58(8):1138–41.
Westberry DE, Davids JR, Pugh LI. The Boyd amputation in children: indications and outcomes. J Pediatr Orthop. 2014;34(1):86–91. https://doi.org/10.1097/BPO.0b013e3182a007a0.
DiGiovanni CW, Ehrlich MG. Treatment of congenital pseudarthrosis of the fibula with interposition allograft. Orthopedics. 1998;21(11):1225–8.
Tachdjian MO. Tachdjian’s pediatric orthopaedics : from the Texas Scottish rite hospital for children. 5th ed. Philadelphia: Elsevier Saunders; 2014.
Tachdjian MO. Pediatric orthopedics. Philadelphia: Saunders; 1990.
Cho TJ, Choi IH, Chung CY, Yoo WJ, Lee SH, Lee SH, et al. Isolated congenital pseudarthrosis of the fibula: clinical course and optimal treatment. J Pediatr Orthop. 2006;26(4):449–54. https://doi.org/10.1097/01.bpo.0000226273.85953.dd.
Dal Monte A, Donzelli O, Sudanese A, Baldini N. Congenital pseudarthrosis of the fibula. J Pediatr Orthop. 1987;7(1):14–8.
Goh JC, Mech AM, Lee EH, Ang EJ, Bayon P, Pho RW. Biomechanical study on the load-bearing characteristics of the fibula and the effects of fibular resection. Clin Orthop Relat Res. 1992;(279):223–8.
Lambert KL. The weight-bearing function of the fibula. A strain gauge study. J Bone Joint Surg Am. 1971;53(3):507–13.
Dooley BJ, Menelaus MB, Paterson DC. Congenital pseudarthrosis and bowing of the fibula. J Bone Joint Surg Br Vol. 1974;56-b(4):739–43.
Martus JE, Johnston CE 2nd. Isolated congenital pseudoarthrosis of the fibula: a comparison of fibular osteosynthesis with distal tibiofibular synostosis. J Pediatr Orthop. 2008;28(8):825–30. https://doi.org/10.1097/BPO.0b013e31818e192d.
Langenskiold A. Pseudarthrosis of the fibula and progressive valgus defformity of the ankle in children: treatment by fusion of the distal tibial and fibular metaphyses. Review of three cases. J Bone Joint Surg Am. 1967;49(3):463–70.
Merkel KD, Peterson HA. Isolated congenital pseudarthrosis of the fibula: report of a case and review of the literature. J Pediatr Orthop. 1984;4(1):100–4.
Makin M. Tibio-fibular relationship in paralysed limbs. J Bone Joint Surg Br Vol. 1965;47:500–6.
Paluska DJ, Blount WP. Ankle valgus after the Grice subtalar stabilization: the late evaluation of a personal series with a modified technic. Clin Orthop Relat Res. 1968;59:137–46.
Hsu LC, O'Brien JP, Yau AC, Hodgson AR. Valgus deformity of the ankle in children with fibular pseudarthrosis. Results of treatment by bone-grafting of the fibula. J Bone Joint Surg Am. 1974;56(3):503–10.
Wiltse LL. Valgus deformity of the ankle: a sequel to acquired or congenital abnormalities of the fibula. J Bone Joint Surg Am. 1972;54(3):595–606.
Yang KY, Lee EH. Isolated congenital pseudoarthrosis of the fibula. J Pediatr Orthop B. 2002;11(4):298–301.
Narasimhan RR, Banta JV. Congenital pseudarthrosis of the fibula. Orthopedics. 2001;24(5):499–500.
Rathjen KE, Birch JG. Rockwood and Wilkins’ fractures in children. In: Beaty JH, editor. Rockwood and Wilkins' fractures in children. 7th ed. Philadelphia: Wolters Kluwer/Lippincott, Williams & Wilkins; 2010. p. 92–119.
Ng BK, Saleh M. Fibula pseudarthrosis revisited treatment with Ilizarov apparatus: case report and review of the literature. J Pediatr Orthop B. 2001;10(3):234–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Katherine Eisenberg declares that she has no conflict of interest.
Carley Vuillermin declares that she has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pediatric Orthopedics
Rights and permissions
About this article
Cite this article
Eisenberg, K.A., Vuillermin, C.B. Management of Congenital Pseudoarthrosis of the Tibia and Fibula. Curr Rev Musculoskelet Med 12, 356–368 (2019). https://doi.org/10.1007/s12178-019-09566-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12178-019-09566-2