Abstract
The prevalence of comorbid depression and anxiety has increased significantly over the last three years. Herein, we used network analysis to identify core symptoms and comorbid pathways between the two disorders, and reveal temporal changes in symptoms that traditional assessment tools fail to capture. Data was collected from 787 clinically comorbid patients (mean age: 31.8 years, 67.1% female) who completed the Zung Self-Rating Depression Scale (SDS) and Self-Rating Anxiety Scale (SAS) before and after treatment (T1 → T2) from 2019 to 2022. Node and bridge strengths were calculated, and the Network Comparison Test (NCT) was used to explore network differences from T1 to T2 and across gender groups. Results indicate that emptiness exhibited the highest strength centrality, particularly among adolescents. The strongest bridge nodes were found in the emotional, physical, and psychological symptoms communities of the two disorders. Although the total score of the assessment tools decreased during treatment, NCT confirmed a significant increase in the overall strength of the network (p = .03). Notably, mental agitation exhibited higher strength within the male network. In conclusion, our findings provide further insights into the mechanisms of comorbid symptomatology and its evolution during treatment, offering valuable targets for intervention. Thus, suggesting the inclusion of network analysis in existing diagnostic, treatment, and follow-up processes facilitates personalized interventions and enhances patient recovery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
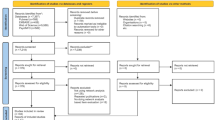
During the three-year COVID-19 pandemic, there has been a significant increase in the prevalence of depression and anxiety disorders (World Health Organization, 2022). These disorders exhibit high a rate of comorbidity (Chen, 2022; Saha et al., 2021). This may be attributed to common neurobiological mechanisms and psychological factors (Tafet & Nemeroff, 2020), and overlapping symptoms between two disorders (Cramer et al., 2010; Yapan et al., 2022). Compared to independent depression or anxiety, comorbidity leads to higher functional impairment (Melton et al., 2016), poorer treatment outcomes (Furukawa et al., 2018), and poorer prognoses (Melton et al., 2016). These issues have been further highlighted during the COVID-19 pandemic. For example, at a national-level psychiatric hospital in Northwest China, the remission and recovery rates among outpatient patients reached 76%. However, follow-up results on a randomly selected sample of 1,840 comorbid patients between November 2019 and November 2022 revealed contrasting information. From the same sample, 451 patients reported no improvement or recurrence after treatment, 778 indicated overall improvement but with lingering or new symptoms, 239 provided neutral evaluations, and 372 expressed satisfaction. Thus, comorbidity represents a widespread and severe issue; there is an urgent need to investigate the mechanisms involved in this condition. Currently, the dominant approach used to investigate mental disorders focuses on identifying the underlying common causes, whereby a hypothetical disease entity determines a range of symptoms (McNally, 2021). Within this framework, mental disorders are conceptualized as a foundation of symptom clusters, and comorbidity is often conceptualized as a relationship between two disorders (Cramer et al., 2010).
However, the common cause model may obscure the true characteristics of comorbidity. First, research often focuses on diagnosing disorders (Cramer et al., 2010). This may overlook the intricate relationships between symptoms. For example, according to the ICD-10, decreased interest and reduced activity are symptoms of a depressive episode. In the common cause model, the strong positive correlation between these symptoms is solely attributed to the shared influence of depression. However, one might question if there is a direct causal relationship between the symptoms, such as decreased interest leading to reduced activity. Secondly, the analysis of psychopathological data relies heavily on the latent variable model (Borsboom & Cramer, 2013). In these models, observed variables (i.e., symptoms or scale items) are treated as measurements of underlying variables (i.e., disorders), and symptoms are aggregated into a total score to reflect the severity of the disorder (Borsboom, 2008). However, this unweighted total score implies that all symptoms are considered equal (Cramer et al., 2010), potentially obscuring real changes in the condition. For example, two patients with identical total scores may present with different symptoms. One individual may score higher with regards to depressive mood but lower with regards to somatic symptoms; another individual’s situation might be the reverse. However, it is evident that the former may have a more severe condition. Although diagnostic criteria (e.g., the DSM-5) emphasize the importance of core symptoms, the common cause model of comorbidity research fails to focus on individual symptoms or symptom clusters (Cramer et al., 2010). This may overlook individual heterogeneity and heterogeneity within disorders, leading to indiscriminate treatment approaches. For example, current treatments for depression are also generally effective for most other internalizing disorders such as anxiety (Junghänel et al., 2023).
A new perspective, network analysis, offers a better explanation for the intricate organization of psychiatric conditions (Borsboom & Cramer, 2013; Cramer et al., 2010; McNally, 2021). This approach highlights causal relationships between symptoms, rather than being influenced by latent common causes (Borsboom, 2008). These causal relationships are real, encompassing direct associations between symptoms or mediated by other symptoms or processes (Cramer et al., 2010). For instance, in the case of GAD (Generalized Anxiety Disorder), insomnia may lead to attentional deficits through fatigue. This approach introduces an entirely different notion of comorbidity, thus emphasizing the direct relationships between symptoms across two disorders and aligning naturally with clinical practice (Kim & Ahn, 2002; McNally, 2021). Consequently, when constructing comorbidity models, we no longer assume direct relationships between two disorders. Instead, we combine symptoms together and model comorbidity with a direct relationship between a set of symptoms. The advancement of network analysis has enriched the study of comorbidity between depression and anxiety disorders. For example, overlapping symptoms (e.g., insomnia and fatigue) serve as connecting points in comorbidity (Cramer et al., 2010); core symptoms, such as depressed and anxious moods play a crucial role in the onset and maintenance of mental disorders (Beard et al., 2016). Bridges between depression and anxiety transmit information and contribute to their high comorbidity rate (Fried, 2015). In another study, Jones et al. (Jones et al., 2021) further developed bridge centrality indices to identify bridge symptoms that facilitate the spread of comorbidity. Moreover, networks can be compared across groups or time periods (van Borkulo et al., 2022).
However, previous research yielded inconsistent or contradictory results. For instance, Beard et al. (2016)) reported increased connectivity among symptoms after treatment, whereas Kaiser et al. (Kaiser et al., 2021) challenged this result. Possible reasons for such discrepancies may be related to variations in study populations, assessment tools, and selected network analysis methods (Robinaugh et al., 2020). In addition, the cultural (Yang et al., 2022), social environments of participants (Kim et al., 2023; Leong et al., 2021) and economic status (Jing et al., 2023) can also influence study outcomes.
Therefore, in the present study, we aimed to investigate the network characteristics of comorbidity between depression and anxiety, identify core symptoms and comorbid pathways, and explore symptom changes that cannot be captured by existing assessment tools by comparing networks before (T1) and after treatment (T2). In addition, we conducted a comparative analysis of networks among different genders; this part of the research was carried out for three main reasons: first, the heightened susceptibility of women to the impact on mental health caused by the recent pandemic (World Health Organization, 2022); second, previous research relating to the nature of this disease obtained from network variations between females and males (Borsboom & Cramer, 2013), and third, the enhanced reliability and applicability of the study across different groups.
Methods
Participants
Between December 2019 and November 2022, participants with symptoms of depression and anxiety were diagnosed by clinical interviews based on the International Classification of Diseases, 10th Revision (World Health Organization, 1992). The patients received treatment as outpatients at a public psychiatric hospital. The inclusion criteria were as follows: a primary diagnosis of depression (ICD codes F32 or F33) or anxiety (F40 or F41) disorders, with the presence of the other as a secondary diagnosis (see Supplementary Table S1). Assessments were conducted pre- and post-treatment. The study was approved by the Ethics Review Committee of Ningxia Mental Health Center and all participants provided written informed consent, either in paper or electronic format. Table 1 lists demographic data.
Measures
The self-rating anxiety scale (SAS) and self-rating depression scale (SDS), developed by Zung (1965, 1971), each consist of 20 items scored from 1 to 4. The scores of the 20 items are then summated to obtain a raw score which is then multiplied by 1.25 and rounded to the nearest whole number to derive the standard score. A higher total score indicates a greater tendency towards anxiety or depression. The SAS scale covers psychological and somatic symptoms (Zung, 1971) while the SDS scale includes affective, physiological, psychomotor, and psychological symptoms (Zung, 1965). Figure 1 shows the items that are included in each dimension of the scale. These scales have been standardized and shown to be effective in China (Wang et al., 1999, pp. 468–471, 388–391). In this study, the internal consistency of the scales was as follows: SAS at T1 (Cronbach's α = 0.908; McDonald's ω = 0.912) and T2 (Cronbach's α = 0.929; McDonald's ω = 0.932); SDS at T1 (Cronbach's α = 0.907; McDonald's ω = 0.909) and T2 (Cronbach's α = 0.933; McDonald's ω = 0.934). Further details regarding the item codes, the complete item content, the assessed symptoms, and the Chinese version, are shown in Supplementary Material Table S2. Reverse-scored items were adjusted appropriately.
Data analysis
Descriptive statistics and missing data handling
SPSS version 25.0 was used to calculate descriptive statistics. We excluded ten samples because of missing data and data anomalies. For samples that were missing < 0.5% of item data, missing values were replaced with the mean. The final sample comprised 787 participants; data from these patients were then used for network analysis.
Network estimation
Network analysis was conducted using R software (version 4.2.2). Analysis involved nodes and edges with each symptom treated as a node and the partial correlation between symptoms as an edge (van Borkulo et al., 2015). First, we estimated an extended Bayesian information criterion (EBIC) graphical least absolute shrinkage and selection operator (LASSO) network model encompassing all items (Jankova & van de Geer, 2018). After controlling for all other symptoms in the network, we calculated the association between each pair of symptoms using partial correlation. LASSO was then employed to shrink small correlations to zero, with the tuning parameter set by the EBIC. Importantly, we ensured that non-zero correlations were conditionally dependent, thus eliminating spurious relationships with other network variables. This resulted in a sparser and more interpretable network. Blue edges indicated positive correlations, while red edges represented negative correlations. Secondly, to optimize the visualization of the networks and minimize potential overlaps between edges and nodes, we utilized the Average Layout Function. This function enabled us to fix the average layout of both networks. For analysis we used two R packages: qgraph version 1.9.4 and bootnet version 1.5 (Epskamp et al., 2018). Thirdly, we assessed network properties using the centrality plot function from the qgraph package in R. Specifically, we focused on strength centrality, which was computed by summating the absolute edge weights of all nodes directly connected to a given node (Bringmann et al., 2019). Finally, we considered the bridge nodes and estimated the bridge strength; this parameter indicates the total connectivity of each node with the nodes of other communities with which it is directly related by summating the weights of the edges that connect the node with nodes of other communities considering absolute values (Jones et al., 2021). A blind cut-off point at the 80th percentile (a cut-off that is considered to provide an acceptable balance between sensitivity and specificity) of bridge strength was applied to identify bridge nodes (Jones et al., 2021).
Comparison of networks
To compare the global connection and local differences between networks, we utilized the R package Network Comparison Test (van Borkulo et al., 2022). This involved analyzing invariant global strength and invariant edge weights using permutation tests with 1000 iterations. Participants were randomly assigned to different groups (e.g., T1 and T2, female and male). Networks were then constructed, estimated, and compared using a bootstrap resampling method repeated 1000 times to generate the null distribution of network differences under the null hypothesis. The significance level was set at 0.05. Global strength, the weighted sum of all edges, was used to assess overall differences in strength (Opsahl et al., 2010). Furthermore, invariant edge weights were examined to identify any differing edges between networks. Local network properties were evaluated by assessing strength invariance, thus reflecting variations in node strength (van Borkulo et al., 2022).
Network robustness
To confirm the robustness of the results, we employed the R package bootnet (version 1.4.3) to evaluate the stability and accuracy of the network. Node stability was assessed by a case-dropping bootstrap procedure and quantified using the correlation stability coefficient (CS-C). The accuracy of the edge weights was estimated using a non-parametric bootstrap method to calculate 95% confidence intervals (CIs). Finally, we conducted bootstrapped difference tests to identify differences in network properties, relying on 95% confidence intervals (CIs) to determine significance (Epskamp et al., 2018).
Results
Descriptive statistics
Item-codes, symptom abbreviations, scores, and data distribution are shown in Table 2. Comparisons were made between T1 and T2 to assess the severity of each disorder. Following treatment, a significant reduction in anxiety and depression levels was detected among patients (tSAS(786) = 11.12, p < 0.001, d = 0.41; tSDS(786) = 11.12, p < 0.001, d = 0.45). Similar findings emerged when evaluating gender-specific groups before and after treatment. However, t-tests conducted between male and female groups during the same period did not yield any significant differences (for more details, see Supplementary Table S3).
Network at T1
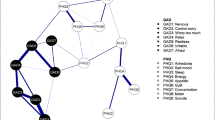
The network plot in Fig. 1 shows the densest connections between depressive and anxiety symptoms in the upper right quadrant. Symptoms such as SDS1 (depressed), SDS3 (crying spells), SDS13 (agitation), SDS15 (irritability), SDS4 (sleep difficulty), as well as anxiety-related psychological symptoms, including SAS1 (anxiousness), SAS2 (fear) and SAS3 (panic), SAS4 (mental disintegration) and SAS19 (insomnia) were shown to be directly interconnected or linked through intermediate nodes. The network analysis highlighted the strongest edges between the overlapping symptoms of anxiety and depression, such as SDS9 (tachycardia) and SAS10 (palpitation), SDS10 (fatigue) and SAS8 (easy fatiguability), and sleep difficulty and insomnia. The symptom with the highest strength was SDS18 (emptiness), followed by palpitations, panic, anxiousness, SDS14 (hopelessness), fatigue, SDS17 (personal devaluation) and depressed.
Based on the values of bridge strength presented in Table 3, Figs. 1 and 2 illustrates the symptoms that function as bridge nodes. These nodes, which scored in the top 20% for bridge strength, included fatigue, depressed, agitation, sleep difficulty, tachycardia, crying spells, insomnia and irritability. Edge investigation showed that the connections between anxiety and depression symptoms primarily occurred via these bridge nodes. Notably, most of these bridge nodes corresponded to the affective, physiological, and psychological symptom domains of the SDS. The only exception was insomnia, which fell under the somatic symptom domain of the SAS.
Network comparisons
Comparing the T1 and T2 networks, no significant differences were found in terms of the distribution of edge weights (p = 0.64). However, there was a significant increase in global strength (p = 0.03). Further analysis of local strength invariance revealed that the greatest differences occurred in panic, SAS15 (nausea and vomiting), along with insomnia, tachycardia and SDS11 (confusion), as shown in Table 3. With regards to the T1 network, there were no gender differences in edge weights (p = 0.14) or overall strength (p = 0.12). However, when analyzing local strength, we found that hopelessness was significantly reduced in strength in the male network, while mental disintegration was increased in strength (ranking fifth). The network analysis plots and strength centrality for different gender groups are shown in Supplementary Figures S1 and S2.
Network stability and accuracy
Case-dropping bootstrap analysis revealed a highly stable network with consistent values for strength and bridge strength even when reducing the sample size by 75%. The CS-C values for both strength and bridge strength were 0.75 (r = 0.7), thus indicating minimal changes in the findings. The non-parametric bootstrap method confirmed the stability of the edge weights, as they remained identical in the bootstrapped sample. The calculated CIs for edge weights reflected a reliable network, with narrower intervals indicating greater reliability. In addition, bootstrapped difference tests revealed statistically significant comparisons between edge weights and node strength, further supporting the robustness of the network analysis. (See Supplementary Figures S3-S7 for details).
Discussion
This study describes the first exploration of comorbidity in depression and anxiety using network analysis in a large clinical sample in China. Analysis identified core symptoms, bridge symptoms and comorbidity pathways. In addition, we investigated symptom changes during treatment and differences between gender. Importantly, the network demonstrated robustness, thus enhancing confidence in the conclusions drawn from this research.
Central symptoms
Our analysis found that emptiness was the most central symptom closely associated with depressive mood, hopelessness, self-deprecation, and loss-of-interest; furthermore, via bridge nodes, such as depression and fatigue, emptiness was also linked to psychological and physiological symptoms of anxiety. In addition, in the T2 network, emptiness continued to hold a central position. Further variance analysis revealed that students (66% of whom were secondary school students) scored the highest in terms of feelings of emptiness (see Supplementary Table S4). This aligns with the definition of emptiness, a negative emotional state involving physiological aspects, loneliness, social disconnection, dissatisfaction or a lack of goals (D’Agostino et al., 2020). However, our understanding of emptiness is limited, primarily due to its correlation or overlap with similar psychological states such as loneliness, or the difficulty in determining its importance in diagnosing mood disorders (Konjusha et al., 2021). As the strongest node in the network, the presence of emptiness indicates a higher probability of activating other symptoms and increasing overall functional impairment. This may be more important than first thought.
This finding aligns with the concept of “hollow mind disorder”. This disorder was initially proposed by Xu Kaiwen, a professor of clinical psychology at Peking University, in response to the cultural background and educational situation in China. This disorder specifically refers to students who feel spiritually empty, lacking value and meaning in life, despite having superior material conditions and no apparent trauma. This state is accompanied by the emergence of depressive symptoms, including low mood, diminished interest, helplessness, despair, anxiety as well as addictive, self-harming and suicidal behaviors (Casaleet al., 2023; Gineret al., 2016; Xu, 2016). Chinese traditional culture emphasizes that children are the only hope of prosperity for the family; moreover, the children should strive wholeheartedly for the future of the family. Good exam grades and prestigious universities are considered the best way to achieve this, as reflected in the Chinese proverb “of all things, reading alone is the highest”. This has led to a utilitarian exam-oriented educational system and widespread educational anxiety in society. In this context, students face immense academic pressure, leaving little time for social interaction and the self-exploration of personal interests. Moreover, students tend to internalize their academic performance as a vital component of their self-worth. Students lacking values, meaning in life, and goals are more vulnerable to feelings of emptiness, helplessness, depressive mood, and anxiety (D’Agostino et al., 2020). The COVID-19 pandemic disrupted their activities, reduced autonomy in learning, and increased reliance on the internet, thus intensifying feelings of emptiness and triggering the occurrence and exacerbation of depressive and anxiety symptoms (Zerach, 2021).
Moreover, hollow mind disorder is not limited to China; this condition has also been observed in Western culture (e.g., the poem “The Hollow Men” by T.S. Eliot; D’Agostino et al., 2020). Further research can provide cross-cultural evidence to corroborate this finding.
Bridge symptoms and comorbid pathways
We found that the comorbid pathways involved most dimensions of both disorders, thus enriching previous research (e.g., Dobson et al., 2021; Fan et al., 2023; Groen et al., 2020). Interconnections between the two diseases extend beyond emotional symptoms and may involve relationships between physical and psychological symptoms. This implies that once these nodes are activated, comorbidity between patients may be more likely to occur. For instance, sleep difficulties, palpitations, and the fatigue associated with depression, may trigger clusters of physical symptoms related to anxiety. Similarly, psychological symptoms associated with depression, such as anxiety and irritability, may trigger psychological symptoms related to anxiety, and vice versa. Alternatively, these bridging nodes may themselves be activated, simultaneously triggering both anxiety-related and depression-related symptoms. This suggests the need to consider the interconnections between multiple dimensions in interventions to disrupt the comorbid pathways. Given the lack of long-term and multiple time-point data (three or more), caution is warranted when interpreting the directional explanations of the bridging pathways in this study.
Assessment of treatment outcomes
Our NCT findings confirmed that during treatment, there is a significant increase in overall network strength. However, a difference test of total scores indicated a marked improvement in comorbid symptoms following treatment. These results align with previous work that reported enhanced connectivity among symptoms during the therapeutic period (Beard et al., 2016). In another paper, Fried et al. (2016) postulated that this may be attributed to spurious effects caused by measurement artifacts. However, such an explanation does not apply to the study conducted by Beard et al. (2016) or the present findings, as both pre- and post-treatment total scores exhibited a relatively normal distribution without any apparent floor or ceiling effects (see Table 2). As highlighted by Fried and Nesse (2015), commonly used total scores may mask the interactions between symptoms. Node strength invariance support this inference, with the majority of nodes showing significant differences, thus playing crucial roles in the network. For instance, anxiety serves as a central node, while insomnia and tachycardia act as pivotal bridge nodes. The enhancement of connections with these symptoms or symptom clusters during treatment is likely to be the primary factor contributing to the overall increase in connectivity observed in this study. This suggests that our current assessment tools may be inadequate and lead to inconsistencies between clinical assessments and patient feedback.
Gender differences
Mental disintegration is more prominent in males compared to females, correlating strongly with fear, panic, irritability, and crying spells. In the Chinese version of the SAS, mental disintegration is described as a feeling of going mad. Chinese society exhibits strong gender role norms (Qing, 2020; Xu & Meier, 2022) in which males are traditionally expected to be breadwinners. Despite the narrowing of gender differences in occupational division over time, the traditional notion of "men should be breadwinners and women homemakers" remains prevalent. Males who face career difficulties may be labeled as lacking competence or ambition. Even among student populations, boys are burdened with higher expectations (Xu & Meier, 2022). Influenced by traditional culture, such as "men don't easily shed tears", males tend to suppress negative emotions, or handle them in a more rational manner (Coutlee & Huettel, 2012) to uphold their Mianzi, a concept embedded in Chinese culture that represents social recognition of an individual's status and the maintenance of personal dignity and prestige (Buckley et al., 2010). Consequently, denial, concealment, and emotional diversion through substances (such as tobacco and alcohol) become common defense mechanisms for males. When faced with a series of negative events (e.g., reduced social interactions, declining income, unemployment, and indebtedness during the COVID-19 pandemic) that they are unable to resolve, their previous defense mechanisms are shattered, potentially leading to a sense of detachment from society (Anderson et al., 2012), the fear of abandonment, and the fear of lacking family and social status (Morrison, 1989). These heightened anxiety experiences can trigger panic, resulting in mental disintegration, rage, and extreme feelings of helplessness (Taffler et al., 2017).
It is worth noting that gender differences in emotional expression are also prevalent in Western societies (Chaplin, 2015). Thus, the characteristic of mental disintegration as a core symptom in male comorbidity may potentially exhibit cross-cultural universality when confronted with negative events.
Limitations
Although this study revealed temporal changes in symptom networks, caution is warranted in providing directional explanations for causal relationships among symptoms. Such interpretations may necessitate the inclusion of data from three or more time points, the implementation of cross-lagged panel network analysis (CLPN), and the differentiation between internal and external influences to confidently elucidate the directional aspects of causal relationships among symptoms. We aim to target this objective in our future research.
Conclusion
This study provides further insights into the mechanisms of comorbid symptomatology and its evolution during treatment, offering valuable clinical implications. First, emptiness can serve as a critical focal point for interventions, particularly among secondary school students. Given the primarily pharmacological treatment approach employed in this study (see Table 1), targeted interventions such as psychotherapy may yield better outcomes. Family therapy can alleviate parental anxiety and stress while improving parent–child relationships. Client-centered therapy can establish a safe therapeutic alliance, thus providing unconditional acceptance to students. Cognitive-behavioral therapy encourages the exploration of personal interests, fostering improved relationships and greater psychological resources. To tackle the core symptom of emptiness in secondary school students, Existential Group Therapy offers a targeted strategy (Peteet, 2011). This therapeutic approach employs artistic and creative activities, such as constructing a "Tree of Life" and participating in psychodrama sessions (Moon, 2009), along with group characteristics (e.g., mutual support, mutual assistance, and the cultivation of hope) to progressively explore various sub-themes (e.g., loneliness and emptiness, self, existential anxiety, fear of death, purpose in life, voluntary selection and assuming responsibility). Ultimately, Existential Group Therapy aims to assist group members in achieving self-identification, strengthening the sense of meaning in life, thereby alleviating existential anxiety, the fear of death and depression (Ding et al., 2022; Tomaszek & Muchacka-Cymerman, 2020). Moreover, existing assessment tools reveal limitations in capturing true symptom changes, prompting the integration of network analysis in clinical practice. We have started integrating the reshape2 package in the R language with the hospital's existing information system (HIS) for data extraction and analysis, thus enhancing technical feasibility and clinical convenience. This approach enables clinicians to access additional symptom network characteristics. Finally, the heightened centrality of mental disintegration in the male network may be attributed to gender role norms and differences in emotional expression, thus emphasizing the importance of adapting emotional regulation and stress coping strategies among males.
In conclusion, network analysis provides additional insights at the symptom level, thus suggesting the inclusion of network analysis in existing diagnostic, treatment, and follow-up processes to develop more personalized treatment plans and expedite recovery in comorbid populations.
Data availability
The datasets analysed during the current study are available in the OSF (https://osf.io/75eur/).
References
Anderson, J., Hurst, M., Marques, A., Millar, D., Moya, S., Pover, L., & Stewart, S. (2012). Understanding suicidal behaviour in young people referred to specialist CAMHS: A qualitative psychoanalytic clinical research project. Journal of Child Psychotherapy, 38(2), 130–153. https://doi.org/10.1080/0075417X.2012.684484
Beard, C., Millner, A. J., Forgeard, M. J. C., Fried, E. I., Hsu, K. J., Treadway, M. T., Leonard, C. V., Kertz, S. J., & Björgvinsson, T. (2016). Network analysis of depression and anxiety symptom relationships in a psychiatric sample. Psychological Medicine, 46(16), 3359–3369. https://doi.org/10.1017/S0033291716002300
Borsboom, D. (2008). Psychometric perspectives on diagnostic systems. Journal of Clinical Psychology, 64(9), 1089–1108. https://doi.org/10.1002/jclp.20503
Borsboom, D., & Cramer, A. O. J. (2013). Network Analysis: An Integrative Approach to the Structure of Psychopathology. Annual Review of Clinical Psychology, 9(1), 91–121. https://doi.org/10.1146/annurev-clinpsy-050212-185608
Bringmann, L. F., Elmer, T., Epskamp, S., Krause, R. W., Schoch, D., Wichers, M., Wigman, J. T. W., & Snippe, E. (2019). What do centrality measures measure in psychological networks? Journal of Abnormal Psychology, 128(8), 892–903. https://doi.org/10.1037/abn0000446
Moon, B. L. (2009). Existential Art Therapy: The Canvas Mirror (Third version). Published LTD.
Buckley, P.J., Clegg, J., Tan, H. (2010). Cultural Awareness in Knowledge Transfer to China — The Role of Guanxi and Mianzi. Foreign Direct Investment, China and the World Economy (pp. 165–191). Palgrave Macmillan. https://doi.org/10.1057/9780230248328_8
Casale, S., Musicò, A., Gualtieri, N., & Fioravanti, G. (2023). Developing an intense player-avatar relationship and feeling disconnected by the physical body: A pathway towards internet gaming disorder for people reporting empty feelings? Current Psychology, 42(24), 20748–20756. https://doi.org/10.1007/s12144-022-03186-9
Chaplin, T. M. (2015). Gender and Emotion Expression: A Developmental Contextual Perspective. Emotion Review, 7(1), 14–21. https://doi.org/10.1177/1754073914544408
Chen, C. (2022). Recent advances in the study of the comorbidity of depressive and anxiety disorders. Advances in Clinical and Experimental Medicine, 31(4), 355–358. https://doi.org/10.17219/acem/147441
Coutlee, C. G., & Huettel, S. A. (2012). The functional neuroanatomy of decision making: Prefrontal control of thought and action. Brain Research, 1428, 3–12. https://doi.org/10.1016/j.brainres.2011.05.053
Cramer, A. O. J., Waldorp, L. J., van der Maas, H. L. J., & Borsboom, D. (2010). Comorbidity: A network perspective. Behavioral and Brain Sciences, 33(2–3), 178–193. https://doi.org/10.1017/S0140525X09991567
D’Agostino, A., Pepi, R., Monti, M. R., & Starcevic, V. (2020). The feeling of emptiness: A review of a complex subjective experience. Harvard Review of Psychiatry, 28(5), 287–295. https://doi.org/10.1097/HRP.0000000000000269
Ding, F. Q., Tian, X. Y., Chen, L., & Wang, X. F. (2022). The relationship between physical health and fear of death in rural residents: The mediation effect of meaning in life and mental health. Death Studies, 46(1), 148–156. https://doi.org/10.1080/07481187.2020.1723741
Dobson, E. T., Croarkin, P. E., Schroeder, H. K., Varney, S. T., Mossman, S. A., Cecil, K., & Strawn, J. R. (2021). Bridging Anxiety and Depression: A Network Approach in Anxious Adolescents. Journal of Affective Disorders, 280, 305–314. https://doi.org/10.1016/j.jad.2020.11.027
Epskamp, S., Borsboom, D., & Fried, E. I. (2018). Estimating psychological networks and their accuracy: A tutorial paper. Behavior Research Methods, 50(1), 195–212. https://doi.org/10.3758/s13428-017-0862-1
Fan, P., Wang, T., Wang, J., & Wang, J. (2023). Network analysis of comorbid depression and anxiety and their associations with response style among adolescents with subthreshold depression. Current Psychology. https://doi.org/10.1007/s12144-023-04992-5
Fried, E. I. (2015). Problematic assumptions have slowed down depression research: Why symptoms, not syndromes are the way forward. Frontiers in Psychology, 6. https://doi.org/10.3389/fpsyg.2015.00309
Fried, E. I., & Nesse, R. M. (2015). Depression sum-scores don’t add up: Why analyzing specific depression symptoms is essential. BMC Medicine, 13(1), 72. https://doi.org/10.1186/s12916-015-0325-4
Fried, E. I., Epskamp, S., Nesse, R. M., Tuerlinckx, F., & Borsboom, D. (2016). What are 《good》 depression symptoms? Comparing the centrality of DSM and non-DSM symptoms of depression in a network analysis. Journal of Affective Disorders, 189, 314–320. https://doi.org/10.1016/j.jad.2015.09.005
Furukawa, T. A., Efthimiou, O., Weitz, E. S., Cipriani, A., Keller, M. B., Kocsis, J. H., Klein, D. N., Michalak, J., Salanti, G., Cuijpers, P., & Schramm, E. (2018). Cognitive-Behavioral Analysis System of Psychotherapy, Drug, or Their Combination for Persistent Depressive Disorder: Personalizing the Treatment Choice Using Individual Participant Data Network Metaregression. Psychotherapy and Psychosomatics, 87(3), 140–153. https://doi.org/10.1159/000489227
Giner, L., Blasco-Fontecilla, H., De La Vega, D., & Courtet, P. (2016). Cognitive, Emotional, Temperament, and Personality Trait Correlates of Suicidal Behavior. Current Psychiatry Reports, 18(11), 102. https://doi.org/10.1007/s11920-016-0742-x
Groen, R. N., Ryan, O., Wigman, J. T. W., Riese, H., Penninx, B. W. J. H., Giltay, E. J., Wichers, M., & Hartman, C. A. (2020). Comorbidity between depression and anxiety: Assessing the role of bridge mental states in dynamic psychological networks. BMC Medicine, 18(1), 308. https://doi.org/10.1186/s12916-020-01738-z
Janková, J., & van de Geer, S. (2018). Inference in high-dimensional graphical models. In M. Drton, M. Maathuis, S. Lauritzen, & M. Wainwright (Eds.), Handbook of graphical models. CRC Press.
Jing, Z., Ding, F., Sun, Y., Zhang, S., & Li, N. (2023). Comparing Depression Prevalence and Associated Symptoms with Intolerance of Uncertainty among Chinese Urban and Rural Adolescents: A Network Analysis. Behavioral Sciences, 13(8), 662. https://doi.org/10.3390/bs13080662
Jones, P. J., Ma, R., & McNally, R. J. (2021). Bridge Centrality: A Network Approach to Understanding Comorbidity. Multivariate Behavioral Research, 56(2), 353–367. https://doi.org/10.1080/00273171.2019.1614898
Junghänel, M., Thöne, A.-K., Dose, C., Breuer, D., Görtz-Dorten, A., & Döpfner, M. (2023). Conceptualizing anxiety and depression in children and adolescents: A latent factor and network analysis. Current Psychology. https://doi.org/10.1007/s12144-023-04321-w
Kaiser, T., Herzog, P., Voderholzer, U., & Brakemeier, E. (2021). Unraveling the comorbidity of depression and anxiety in a large inpatient sample: Network analysis to examine bridge symptoms. Depression and Anxiety, 38(3), 307–317. https://doi.org/10.1002/da.23136
Kim, N. S., & Ahn, W. (2002). Clinical psychologists’ theory-based representations of mental disorders predict their diagnostic reasoning and memory. Journal of Experimental Psychology: General, 131(4), 451–476. https://doi.org/10.1037/0096-3445.131.4.451
Kim, S. T., Seo, J. H., Park, C. I., Kim, S. J., & Kang, J. I. (2023). COVID-19 pandemic’s impact on networks of depression and anxiety in naturalistic transdiagnostic sample of outpatients with non-psychotic mental illness. Frontiers in Psychiatry, 14, 1118942. https://doi.org/10.3389/fpsyt.2023.1118942
Konjusha, A., Hopwood, C. J., Price, A. L., Masuhr, O., & Zimmermann, J. (2021). Investigating the Transdiagnostic Value of Subjective Emptiness. Journal of Personality Disorders, 35(5), 788–800. https://doi.org/10.1521/pedi_2021_35_510
Leong, Bin Abdullah M. F. I., Ahmad, Yusof H., Mohd, Shariff N., Hami, R., Nisman, N. F., Law, K. S. (2012). Depression and anxiety in the Malaysian urban population and their association with demographic characteristics, quality of life, and the emergence of the COVID-19 pandemic. Current Psychology, 40(12), 6259–6270. https://doi.org/10.1007/s12144-021-01492-2
McNally, R. J. (2021). Network Analysis of Psychopathology: Controversies and Challenges. Annual Review of Clinical Psychology, 17(1), 31–53. https://doi.org/10.1146/annurev-clinpsy-081219-092850
Melton, T. H., Croarkin, P. E., Strawn, J. R., & Mcclintock, S. M. (2016). Comorbid Anxiety and Depressive Symptoms in Children and Adolescents: A Systematic Review and Analysis. Journal of Psychiatric Practice, 22(2), 84–98. https://doi.org/10.1097/PRA.0000000000000132
Morrison, A. P. (1989). Shame: The underside of narcissism. Analytic Press.
Opsahl, T., Agneessens, F., & Skvoretz, J. (2010). Node centrality in weighted networks: Generalizing degree and shortest paths. Social Networks, 32(3), 245–251. https://doi.org/10.1016/j.socnet.2010.03.006
Peteet, J. R. (2011). Approaching Emptiness: Subjective, Objective and Existential Dimensions. Journal of Religion and Health, 50(3), 558–563. https://doi.org/10.1007/s10943-010-9443-7
Qing, S. (2020). Gender role attitudes and male-female income differences in China. The Journal of Chinese Sociology, 7(1), 12. https://doi.org/10.1186/s40711-020-00123-w
Robinaugh, D. J., Hoekstra, R. H. A., Toner, E. R., & Borsboom, D. (2020). The network approach to psychopathology: A review of the literature 2008–2018 and an agenda for future research. Psychological Medicine, 50(3), 353–366. https://doi.org/10.1017/S0033291719003404
Saha, S., Lim, C. C. W., Cannon, D. L., Burton, L., Bremner, M., Cosgrove, P., Huo, Y., & McGrath, J. (2021). Co-morbidity between mood and anxiety disorders: A systematic review and meta-analysis. Depression and Anxiety, 38(3), 286–306. https://doi.org/10.1002/da.23113
Tafet, G. E., & Nemeroff, C. B. (2020). Pharmacological Treatment of Anxiety Disorders: The Role of the HPA Axis. Frontiers in Psychiatry, 11. https://doi.org/10.3389/fpsyt.2020.00443
Taffler, R. J., Spence, C., & Eshraghi, A. (2017). Emotional economic man: Calculation and anxiety in fund management. Accounting, Organizations and Society, 61, 53–67. https://doi.org/10.1016/j.aos.2017.07.003
Tomaszek, K., & Muchacka-Cymerman, A. (2020). Thinking about My Existence during COVID-19, I Feel Anxiety and Awe — The Mediating Role of Existential Anxiety and Life Satisfaction on the Relationship between PTSD Symptoms and Post-Traumatic Growth. International Journal of Environmental Research and Public Health, 17(19), Article 19. https://doi.org/10.3390/ijerph17197062
van Borkulo, C., Boschloo, L., Borsboom, D., Penninx, B. W. J. H., Waldorp, L. J., & Schoevers, R. A. (2015). Association of Symptom Network Structure With the Course of Depression. JAMA Psychiatry, 72(12), 1219. https://doi.org/10.1001/jamapsychiatry.2015.2079
van Borkulo, C. D., van Bork, R., Boschloo, L., Kossakowski, J. J., Tio, P., Schoevers, R. A., Borsboom, D., & Waldorp, L. J. (2022). Comparing network structures on three aspects: A permutation test. Psychological Methods. https://doi.org/10.1037/met0000476
Wang, X. D., Wang, X. L., & Ma, H. (1999). Handbook of mental health assessment scale. (5th ed, pp. 468–471, 388–391). Chinese Mental Health Journal.
World Health Organization. (1992). The ICD-10 Classification of Mental and Behavioural Disorders: Clinical descriptions and diagnostic guidelines. World Health Organization Geneva.
World Health Organization. (2022). COVID-19 pandemic triggers 25% increase in prevalence of anxiety and depression worldwide. Retrieved November 6, 2023, from https://www.who.int/news/item/02-03-2022-covid-19-pandemic-triggers-25-increase-in-prevalence-of-anxiety-and-depression-worldwide
Xu, K. (2016). Interpretation of the hollow mind disorder. Shaanxi Education Press (comprehensive edition), 58–60.
Xu, X., & Meier, K. J. (2022). Separating symbolic and active representation: A mixed methods study of gender and education in China. Public Management Review, 24(9), 1429–1451. https://doi.org/10.1080/14719037.2021.1900352
Yang, Y., Zhang, S.-F., Yang, B. X., Li, W., Sha, S., Jia, F.-J., Cheung, T., Zhang, D.-X., Ng, C. H., & Xiang, Y.-T. (2022). Mapping Network Connectivity Among Symptoms of Depression and Pain in Wuhan Residents During the Late-Stage of the COVID-19 Pandemic. Frontiers in Psychiatry, 13, 814790. https://doi.org/10.3389/fpsyt.2022.814790
Yapan, S., Türkçapar, M. H., & Boysan, M. (2022). Rumination, automatic thoughts, dysfunctional attitudes, and thought suppression as transdiagnostic factors in depression and anxiety. Current Psychology, 41(9), 5896–5912. https://doi.org/10.1007/s12144-020-01086-4
Zerach, G. (2021). Emptiness Mediates the Association Between Pathological Narcissism and Problematic Smartphone Use. Psychiatric Quarterly, 92(1), 363–373. https://doi.org/10.1007/s11126-020-09803-9
Zung, W. W. K. (1965). A Self-Rating Depression Scale. Archives of General Psychiatry, 12(1), 63. https://doi.org/10.1001/archpsyc.1965.01720310065008
Zung, W. W. K. (1971). A Rating Instrument For Anxiety Disorders. Psychosomatics, 12(6), 371–379. https://doi.org/10.1016/S0033-3182(71)71479-0
Acknowledgements
We appreciate the hard work and critical comments of the editors and reviewers. Additionally, we thank all clinical participants for their understanding and selfless support.
Funding
Financial support was received from the National Natural Science Foundation of China (ID: 32360206) is gratefully appreciated.
Author information
Authors and Affiliations
Contributions
Study design and hypothesis proposion: Fengqin Ding; Methodology and data analysis: Ning Li and Sensen Zhang; Data collection: Ning Li, Zhi Jing and Yumeng Zhao; Writing—original draft preparation: Fengqin Ding and Ning Li; Writing—review and editing: Fengqin Ding, Ning Li and Jia Li.
Corresponding author
Ethics declarations
Competing interest
All authors approved the submitted version. And On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethics approval and consent to participate
This study was performed in line with the principles of the Declaration of Helsinki.Approval was granted by the Ethics Committee of Ningxia Mental Health Center (Ningan Hospital) in China (2023-WS-007).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ding, F., Li, N., Zhang, S. et al. Network comparison analysis of comorbid depression and anxiety disorder in a large clinical sample before and after treatment. Curr Psychol 43, 13267–13278 (2024). https://doi.org/10.1007/s12144-023-05308-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-023-05308-3