Abstract
Radiation-induced skin damage (RID) is the most prevalent, significant side effect of radiotherapy (RT). Nearly 95% of patients experience moderate to severe skin reactions after receiving radiation therapy. However, criteria for acute radiation dermatitis (ARD) treatment remain unavailable. Topical agents with anti-inflammatory properties may protect the skin and facilitate tissue regeneration in patients with RID. Many of these topical agents function through nuclear factor kappa B pathway regulation. They either reduce the levels of inflammatory factors or elicit anti-inflammatory properties of their own, thus preventing oxidative stress and inflammatory responses and thus enabling RID prevention and management. Herein, we explore the 25 topical agents investigated for RID prevention and management thus far and evaluate their mechanisms of action. These agents include 11 natural agents, 3 miscellaneous agents, 9 topical nonsteroidal agents, and 2 topical corticosteroids.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
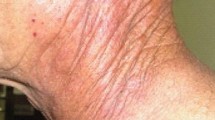
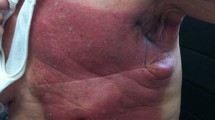
During radiotherapy (RT) for cancers, the skin is the first organ exposed to radiation and related damage; therefore, radiation-induced skin damage (RID) is the most common serious side effect of RT in patients with malignancies. Moderate-to-severe skin reactions occur in approximately 95% of patients with malignancies, most notably in those with head and neck cancer (HNC) and breast cancer [1, 2]. RID is characterized by consequences such as erythema, soreness, ulceration, scaling, distended, pruritus, and burning sensation. These consequences can be severe—requiring dose reduction or treatment interruption and worsening patients’ esthetic appeal and quality of life.
RID refers to inflammation of the skin caused by radiation therapy. The mechanism mainly involves primary damage to skin cells by radiation as well as secondary damage (Fig. 1). Radiation interacts directly with skin cells and with radiation energy with water molecules, causing damage to DNA and other cellular structures, leading to cell death and damage, triggering an inflammatory response. Primary damage refers to reactive oxygen species (ROS) and short-lived free radicals that trigger irreversible double-strand breaks in basal keratinocytes, hair follicle stem cells, and melanocytes DNA, inhibit the migration of basal cell division and keratinization, and induce RID in patients undergoing RT [3]. Transendothelial migration of leukocytes and other immune cells from circulation to irradiated skin is a hallmark of RID. Some studies have found that p53 plays a crucial role in radiation-induced apoptosis, apoptosis or programmed death dependent on p53 occurs within hours after irradiation [4]. The release of red flags during necrosis, as well as secondary necrosis following apoptosis, trigger proinflammatory cytokine production and immunostimulatory responses [4]. Necrosis can lead to the release of inflammatory cytokines such as IL-1, IL-6, IL-8 and TNF-α, as well as other inflammatory mediators, secondary to inflammation and injury. Research by Allam et al. has shown that radiation-induced mitochondrial apoptosis can lead to the release of oxidized mitochondrial DNA into the cytoplasm and binding to NLRP3 inflammasome in the cytoplasm, causing activation of NLRP3 inflammasomes, which promote the maturation and secretion of the inflammatory factors IL-1 β and IL-18 [5]. Free radicals cause upregulation of cyclooxygenase, nitric oxide synthase, and lipoxygenase, and their effects on mitochondrial function vary significantly [3]. NO is produced by macrophages stimulated by inflammation by the iNOS enzyme, while cyclooxygenase (COX) 2 can produce ROS indirectly. These factors are secondary to skin inflammation and injury.
In the Multinational Association for Supportive Cancer Care (MASCC) guidelines, the skin care recommendations during RT mainly include gentle skin care (eg., washing with moisturizing soap and water and wearing loose clothing). However, no consensus regarding the effectiveness or safety of topical prophylactic drugs for RID prevention has been reached thus far [6]. Moreover, although the MASCC guidelines recommend topical corticosteroids (commonly used anti-inflammatory drugs) for RID treatment [6], long-term topical corticosteroid use can lead to severe side effects [7]. Therefore, many studies have focused on identifying other topical drugs that may reduce RT-related skin damage with fewer adverse effects [7]. These topical drugs can be broadly divided into four categories: (i) natural agents, (ii) miscellaneous agents, (iii) topical nonsteroidal agents, and (iv) topical corticosteroids. In this review, we explore the effects of 25 topical agents in RID treatment and their underlying prevention mechanisms (Fig. 2).
D: Protective mechanism of topical drugs on skin tissue cells. The black lines represent the signaling pathway, the red lines represent the influence of traditional Chinese medicine on the signaling pathway, and the pink and green oval represent the cell signaling molecules activated and inhibited by traditional Chinese medicine. The numbers represent each type of topical drug. Topical agents: 1.Silymarin 2. Calendula 3.Phlorotannins 4. Chamomile 5.Nigella sativa 6. Turmeric 9. Honey 11. Aloe vera 12. Juango cream 13. Holoil 15. Doxepin 16. Hyaluronic acid 19. Epigallocatechin gallate 20. Allantoin 21. Sucralfate 22. Trolamine 23. Biafine emulsion. E: Mechanism of action of topical drugs on inflammatory cells. The black lines represent the signaling pathway, the red lines represent the influence of traditional Chinese medicine on the signaling pathway, and the pink and green oval represent the cell signaling molecules activated and inhibited by traditional Chinese medicine. The numbers represent each type of topical drug. Topical agents: 1.Silymarin 2. Calendula 3.Phlorotannins 4. Chamomile 5.Nigella sativa 6. Turmeric 7. Olive oil 9. Honey 10. Henna extract 11. Aloe vera 12. Juango cream 14. Vitamins 15. Doxepin 17. Statins 19. Epigallocatechin gallate 21. Sucralfate 24. Mometasone furoate 25.Betamethasone
Natural agents
Silymarin
Silymarin is a standardized extract of seeds and fruits of milk thistle (Silybum marianum), a member of the Asteraceae family. Silymarin gel may reduce RID severity and delay its occurrence after 5 weeks of application. A double-blind, randomized trial evaluated the RID-preventive effects of 1% silymarin gel in patients receiving RT [8]. During RT, compared with the placebo, silymarin led to the development of grade 1 RID; at the end of week 5, only 8 patients developed grade 2 RID and only 1 developed grade 3 RID [8].
Silymarin elicits a hepatoprotective effect because of its antioxidant activity: it enhances the free radical-scavenging activities of glutathione peroxidase and superoxide dismutase (SOD) [9]. In addition, silymarin demonstrates immunomodulatory properties by inhibiting COX-2 production; it also shows anti-inflammatory properties by blocking the nuclear factor kappa B (NF-κB) pathway and inhibits IL-1, IL-6, and TNF-α production [8]. In an in vitro model, silymarin inhibited lipopolysaccharide-induced microglial activation and reduced levels of inflammatory mediators (eg., nitric oxide [NO] and TNF-α), thereby blocking the cascade of inflammatory events [7].
Calendula
In 2008, the European Medicines Agency recognized calendula (Calendula officinalis) as a plant with anti-inflammatory, antioxidant, and other therapeutic effects when used for RID prevention and treatment [10]. Using calendula alone for RID prevention and treatment is effective and safe in breast cancer and HNC patients undergoing postoperative RT; however, this result has been reported by low-quality studies [11, 12]. Furthermore, calendula has been noted to be more effective in preventing and treating RID than triethanolamine; in particular, patients receiving calendula interrupted RT less frequently and had significantly lower levels of radiation-related pain [13].
C. officinalis contains many compounds, including flavonoids, triterpenoids, and carotenoids [14]. Triterpenoids have anti-inflammatory and antiedema effects by stimulating fibroblast proliferation and inhibiting COX-2, C3 invertase, and 5-lipoxygenase (5-LOX) activities [15]. Flavonoids demonstrate anti-inflammatory, antioxidant, and antiedema properties by inhibiting 5-LOX [16].
In summary, calendula mainly inhibits inflammatory cytokine (eg., IL-6, IL-1β, TNF-α, and interferon [IFN]-γ), COX-2, prostaglandin E2 (PGE2), inducible NO synthase (iNOS), and C-reactive protein production, thus exerting anti-inflammatory and antioxidant effects [14].
Phlorotannins
Cosmeceuticals containing phlorotannins (PTNs) can prevent or mitigate skin damage during or after RT [17]. Through histopathological and Western blot analyses, these cosmeceuticals have been confirmed to reduce epidermal and dermal thickness and alleviate acute skin inflammation in irradiated mice [17]. Of all tested PTNs, dieckol leads to the most prominent decrease in ultraviolet radiation-induced cell damage [17]. PTNs mitigate RID by disrupting the expression of nuclear factor erythroid 2-correlated factor (Nrf2), NF-κB, and their downstream targets.
PTNs also enhance the radiation-induced increase in the expression of heme oxygenase (HO) 1 and the downstream targets of Nrf2 and Nrf2 [17]. HO-1, an Nrf2-dependent enzyme, is a potent anti-inflammatory target. Under oxidative stress, HO-1 is released from its inhibitor (Kelch-like ECH-associated protein 1) and transferred from the cytoplasm to the nucleus, where it initiates the expression of many genes that protect cellular ROS damage and reduce the inflammatory response [18].
In summary, PTNs inhibit NF-κB pathway activation and IL-1β production in response to radiation. The NF-κB pathway is crucial in initiating and amplifying inflammation; PTNs can reduce radiation-induced tissue damage and related side effects by lowering IL-1β production [17].
Chamomile
Chamomile (Chamomilla recutita or Matricaria recutita), particularly its flowers, are widely and frequently used for their anti-inflammatory properties. Chamomile promotes wound healing at a faster rate than corticosteroids. The therapeutic properties of chamomile are attributable to its components, such as chamazurine, α-bisabolol, bisabolol oxide, spiroether, and flavonoids [16]. Applying chamomile gel to the skin not only delays the onset of dermatitis but also reduces the severity of itching, burning, and hyperpigmentation [19]. This finding is attributable to the anti-inflammatory effects of chamomile, facilitating inflammation alleviation and soothing sensation in the affected areas of the skin [13]. Although chamomile microparticles do not reduce or delay the onset of radiation dermatitis of any level significantly, they lead to a significant decrease in the incidence of grade 2 or higher radiation dermatitis; in addition, the onset of radiation dermatitis is delayed by 7 days [7]. Therefore, chamomile microparticles may delay the onset of severe symptoms (eg., excessive pain and itching), further confirming the potential of chamomile in RID prevention.
Chamomile may also inhibit the expression of the iNOS gene; this may be a mechanism underlying its anti-inflammatory properties [20, 21]. iNOS induces the production of NO, a key molecule involved in inflammatory disease development and progression. In addition, NF-κB initiates the production of proinflammatory molecules, including iNOS. Chamomile inhibits NF-κB activity by preventing the degradation and phosphorylation of its inhibitor protein, inhibitor kappa B (IκB). By preventing IκB degradation and phosphorylation, chamomile effectively inhibits NF-κB activation, reducing iNOS expression and NO production and thus preventing RID-related inflammatory response [20].
In summary, chamomile inhibits NO production and exhibits antioxidant effects by inhibiting ROS; it also exerts anti-inflammatory effects by activating macrophage lipopolysaccharides and reducing the expression of various inflammatory mediators, such as COX-2, 5-LOX, TNF-α, IL-6, and PGE2 [21].
Nigella sativa
Rafati et al. reported the effectiveness of an N. sativa gel in preventing ARD in patients with breast cancer. Compared with the placebo gel, the N. sativa gel prevented grade 2 and 3 of Radiation Therapy Oncology Group and the European Organization for Research and Treatment of Cancer toxicity, reduced wet desquamation severity, and increased time until the onset of related symptoms [22].
An N. sativa extract exerts anti-inflammatory effects by downregulating the expression of the inflammatory enzymes 5-LOX and COX-2, inhibiting cytokines TNF-α and IL-6, and reducing NO production but increasing the levels of the anti-inflammatory cytokine IL-10 [22, 23]. An N. sativa extract may exert anti-inflammatory and antioxidant properties by inhibiting the production of superoxides and enhancing the activities of antioxidant enzymes such as catalase, glutathione transferase, SOD, and quinone reductase, thus protecting skin cells from damage due to free radicals produced during RT [22, 24].
Thymoquinone, the main active component in N. sativa, has antioxidant, anti-inflammatory, and anticancer properties [24,25,26]. In patients with breast cancer, thymoquinone has been shown to scavenge free radicals in experimental studies [24], as well as aid in reducing ARD severity and delaying wet desquamation onset observed [22].
In summary, N. sativa and its active component, thymoquinone, might mitigate the side effects of RT on the skin.
Turmeric
Turmeric (Curcuma longa) is widely used to treat inflammation; one of its main components, curcumin, has been found to have anti-inflammatory, antioxidant, and antimicrobial properties [27]. Palatty et al. reported that an Ayurvedic cream containing turmeric and sandalwood oil reduces radiation dermatitis significantly [28]. Similarly, another study demonstrated that compared with the placebo, curcumin significantly reduces radiation dermatitis severity and wet desquamation [29]. In their randomized controlled trial, Ryan et al. noted no significant differences in RID severity at the end of RT between breast cancer patients treated with topical curcumin and control patients [30].
The precise mechanisms underlying the effects of curcumin on RID remain unclear. A possible mechanism is as follows: curcumin reduces skin tissue damage by downregulating COX-2, 5-LOX, and iNOS expression, thus inhibiting the production of inflammatory cytokines (TNF-α, IL-1, IL-6, IL-8, and IL-12) [31]; it also upregulates IL-10 expression, thus reducing TNF-α, IL-6, and ROS release [27]. Curcuminoid supplements have been noted to reduce serum IL-6 levels significantly [32]. Finally, curcumin can also block inflammatory gene expression by inhibiting NF-κB activity [33].
In summary, curcumin reduces inflammatory markers and thus may be a promising option for RID treatment. However, further research to clarify the mechanisms of action of curcumin, as well as its effectiveness and optimal dosage for RID treatment and prevention, are warranted.
Olive oil
Olive oil is considered the most effective option for preventing RID [6, 34]. In particular, the unique chemical and physiologic functions of olive oil make it a potent antioxidant and anti-inflammatory agent [35] and thus a potential RID-preventive agent [34,35,36,37]. In patients undergoing RT after hypofractionated mastectomy, the use of olive oil and calcium hydroxide emulsions led to better prophylaxis than the typical skin care regimens. These emulsions combination can delay skin toxicity, reduce acute RID severity, and improve the quality of life [36]. Chitapanarux et al. reported that compared with control treatment, olive oil use reduced skin reaction severity and led to better health-related quality of life; moreover, none of the patients who used olive oil experienced grade 3 skin reactions [36].
According to a systematic review and network meta-analysis, olive oil prevents RID effectively [34]; moreover, olive oil has promising therapeutic effects against RID. These observations may be attributable to linoleic acid in olive oil, which improves skin physiology and skin barrier function [35]. Linoleic acid—an important component of skin cell membranes and ceramides—is vital for maintaining skin barrier function [35]. The precise mechanism by which olive oil acts on RID remains unknown; nevertheless, extra virgin olive oil, believed to be rich in phenolic antioxidants, squalene, and oleic acid, may provide considerable protection against RID by inhibiting oxidative stress [38]. This oxidative stress is a main factor leading to the development of dermatitis caused by RT.
Cucumber cream
Cucumber cream facilitates irradiated skin recovery and regeneration. A study reported that none of the patients treated with a cucumber cream developed grade 1 or higher skin lesions over the month following RT [39]. Cucumber is added to various skin care products because it not only nourishes and soothes the skin but also reduces swelling and relieves pain caused by skin irritation or sunburns [40]. Copper oxide nanoparticles produced through green synthesis using cucumber extract demonstrate resistance to ultraviolet radiation and ROS inhibition without cytotoxicity. When incorporated into skin creams, the nanoparticles can repair the skin [41]. In general, cucumber cream leads to satisfactory RID treatment outcomes; however, its mechanism of action remains unclear.
Honey
Honey can prevent radiation-induced oral mucositis (OM), a common, painful side effect of RT in patients with HNC. A study reported that patients who received honey as an intervention demonstrated a considerable reduction in the severity of OM, particularly grade 3 and 4 OM [42]. Moreover, honey consumption significantly prolongs the time to OM onset in patients undergoing RT [43].
Honey can reduce severe mucositis incidence during RT in patients with OM and HNC. Moreover, using honey as a complementary treatment can aid in lowering OM-associated discomfort but without the effectiveness of RT in targeting and killing cancer cells [44]. In contrast, a Canadian double-blind clinical trial noted that their patients did not tolerate honey well; in addition, it did not relieve RT-induced OM significantly, even in the mouth [45].
Honey contains phenolic substances with anti-inflammatory properties; they inhibit the proinflammatory activity of COX-2, iNOS, or both [46]. Although their mechanisms of action remain unclear, these anti-inflammatory properties are essential for RI-induced OM prevention and treatment.
In summary, honey can inhibit the expression of inflammatory pathway markers, such as IL-1, IL-10, IL-6, COX-2, TNF-α, NF-κB, IκB, TGF-β, 5-LOX, NO, iNOS, and PGE2, and prevent OM by inhibiting the release of macrophages, monocytes, neutrophils, keratinocytes, and other leukocytes, thereby preventing ROS production [47].
Henna extract
Henna (Lawsonia inermis L.) extract and topical ointment α (containing natural henna) have been noted to prevent and reduce RID severity after RT in patients with breast cancer; it can also relieve discomfort related to burning and itching [7]. A study used henna-leaf decoctions to treat some skin problems, including skin inflammation [48]; its results indicated that henna has antioxidant properties, reducing lipid peroxidation rate, malondialdehyde levels, and RNA and DNA oxidation and thus inhibiting inflammatory responses and accelerating wound healing—thereby preventing and alleviating RID [7].
Aloe vera
Aloe vera is a medicinal plant traditionally used for the treatment of burns and scalds; it also has analgesic, antidiabetic, anti-inflammatory, antiproliferative, anticancer, anti-aging, and immunomodulatory properties [16, 49]. The use of aloe vera gel in combination with the typical skin care plan before RT initiation can significantly reduce the degree of burning sensation, as well as the incidence of skin erythema and wet desquamation, in HNC patients undergoing concurrent chemo-RT; however, it may not prevent RID [49].
Karbasizade et al [50] reported that an aloe vera solution prevented OM and reduced its severity. Sakhbujami et al. reported a similar result: aloe vera mouthwash reduced RT-induced OM severity effectively without any side effects; it may thus be used as an alternative option for OM treatment in patients with HNC [51]. A systematic review and cumulative analysis of randomized controlled trials reported that patients pretreated with aloe vera demonstrated significantly lower RID incidence (including the overall incidence and that of grade 2 to 4, grade 2, and grade 3 RID) and reduced RID risk by > 70%; among all RID grades, grade 3 RID demonstrated the lowest incidence after aloe vera treatment [52].
Aloe vera, particularly its active components, elicits a protective effect on the skin, promoting wound healing, reducing inflammation, and improving skin health through its antioxidant and anti-inflammatory mechanisms. In an animal model, topical application of aloe vera promoted wound healing, reduced inflammatory cell infiltration, and increased epidermal thickness and collagen deposition [53].
Aloe vera exerts anti-inflammatory effects by reducing IL-8 levels, ROS production, and DNA damage [54]. In addition, topical aloe vera increases antioxidant-enzyme activity and glutathione content but reduces ROS production, thereby preventing x-ray-induced damage [55]. Besides, aloin compounds, present in aloe vera, can promote cytokine and growth factor phosphorylation, leading to cell migration followed by wound healing acceleration [56].
Miscellaneous agents
Juango cream
Juango (containing Lithospermum Radix, Angelica Gigantis Radix, beeswax, and sesame oil) has anti-inflammatory properties, which may facilitate RID treatment. A study indicated that Juango cream reduced RID due to RT in patients with breast cancer without significant side effects. Similarly, several in vivo and in vitro studies have demonstrated the efficacy of Juango in dermatopathy [57]. Park et al [58] found that deoxyshikonin, the active component of Caryophyllum, activates extracellular signaling, which facilitates the regulation of kinases, including p38 mitogen-activated protein kinase, and thereby enhances human keratinocyte proliferation and migration and promotes skin healing. In patients with RID, Caryophyllum inhibits TNF-α release, NF-κB nuclear translocation, and proteasome activity in macrophages, whereas decursin (purified from angelica) exerts anti-inflammatory effects by inactivating inflammatory mediator expression in macrophages [59].
Holoil
Holoil—a medicinal mixture of Hypericum flower extract and neem oil—stimulates granulation tissue growth and effectively eliminates fibrin. Both Hypericum flower extract and neem oil have anti-inflammatory properties. In particular, Hypericum flower extract facilitates keratinocyte proliferation [60].
The effectiveness and safety of holoil have been validated for acute skin toxicity treatment in HNC patients undergoing chemo-RT [60]. Moreover, Franco et al. demonstrated that both Hypericum flower extract and neem oil may prevent wet desquamation and RID grade reduction [61].
Vitamins
Patients with severe OM are deficient in vitamins that inhibit proinflammatory pathways (eg., vitamins E, A, and D) [62].
Vitamin E, a potent antioxidant, alleviates OM in patients with HNC after RT [63,64,65]. It is a cofactor in an enzymatic antioxidant molecular complex that protects cells from damage [66] and reduces mucositis severity by exerting antioxidant effects, thus preventing skin and mucous membrane damage due to ROS [67].
Ascorbic acid (ie., vitamin C) is a potent antioxidant with free radical-scavenging properties; it maintains the intracellular redox balance by aiding the removal of free radicals such as ROS, NO, superoxide, and ozone, thus preventing oxidative damage [68]. However, topical ascorbic acid has not been shown to be effective in the management of RID [13, 69].
Topical nonsteroidal agents
Doxepin
Topical doxepin can alleviate OM pain [70]. Moreover, doxepin cream has been reported to be effective in preventing grade 2 or higher skin inflammation in patients undergoing RT for breast cancer postoperatively [71]. A randomized trial reported that doxepin improved acute cutaneous toxicity caused by breast intensity-modulated RT and significantly reduced dermatitis incidence rate and severity compared with the placebo [71].
Feng et al [72] explored the mechanism underlying the beneficial effects of doxepin; the authors reported that doxepin has anti-inflammatory properties: it blocks histamine H1 and H2 receptors and prevents histamine release. Animal studies further support these observations: doxepin administration leads to a decrease in the levels of various inflammatory cytokines (eg., IL-2, IL-12, IFN-γ, TNF-α, IL-6, and IL-1β) [73]. In summary, doxepin can suppress dermatitis symptoms and reduce inflammatory cytokine levels, making it a promising agent for RID prevention and treatment.
Hyaluronic acid
Hyaluronic acid (HA) is a natural biopolymer from the glycosaminoglycan family; it is widely employed as a key ingredient in irradiated skin care products. HA accelerates the healing process of wounds substantially by influencing the growth and activity of fibroblasts and fibrin [74]. Several studies have noted that HA gel does not prevent RID, reduce its severity, or provide protection against radiation [75, 76]. A meta-analysis demonstrated that HA has no significant effect on grade 2 RID occurrence or overall RID incidence [77]. However, in a study on RID treatment using HA gel (ie., Jalosome soothing gel), patients showed great satisfaction with RID-related pain reduction and resolution [78]. In their meta-analysis on randomized controlled trials, Lee et al. [79] indicated that compared to other topical drugs, HA demonstrates higher RID treatment efficacy and lower desquamation incidence, without major side effects, in patients with breast cancer; therefore, it may be a great alternative topical agent for RID treatment [79].
HA is believed to promote epidermal cell migration; it also has an occlusive effect, potentially allowing HA-containing cosmetics to persist in the skin layer and penetrate the epidermis more easily. In addition, HA can aid in maintaining skin firmness by eliciting a potential antioxidant effect; therefore, sunscreen products containing HA can protect the skin from ultraviolet radiation and reduce related damage [80]. Therefore, HA may have several RID-preventive and -treatment benefits in cancer patients undergoing RT.
Statins
Statins are a class of drugs mainly used to reduce cholesterol levels; they also have lipid-lowering, anti-inflammatory, immunomodulating, antioxidant, metabolic, and antibacterial properties. Statins have also been noted to reduce the severity of skin diseases satisfactorily [13].
Ghasemi et al. [81] investigated the effects of topical atorvastatin on radiation-induced breast site skin. The authors found that atorvastatin cream application significantly reduced swelling (measured as cup size increase), itching, and pain. In particular, the reduction in breast swelling, itching, and pain was nearly 1.8, 1.7, and 1.5 times higher in the atorvastatin group than in the control group, respectively [81].
D-Panthenol
D-Panthenol, also known as provitamin B5, is a common ingredient in commercially available skin care formulations indicated for use in individuals undergoing RT. D-Panthenol in these formulations mitigates the adverse effects of radiation on the skin.
Provitamin B5 deficiency can lead to dermatitis, whereas excessive provitamin B5 can promote epithelial regeneration and formation [13]. It is a polyhydroxy alcohol occurring naturally in human skin, hair, and nails.
The molecular structure of D-panthenol includes multiple hydroxyl groups; therefore, it promotes tissue regeneration and wound healing. When applied topically to the skin, D-panthenol effectively relieves all forms of irritation and redness, soothes burning sensations, and enhances epidermal lipid barrier integrity and function [74]. However, although creams containing D-panthenol significantly reduce epidermal flaking, they have no effect on grade 3 or 4 RID and a weak wet desquamation-preventive effect after RT [74].
Epigallocatechin gallate
Epigallocatechin gallate (EGCG) may be an innovative option for skin treatment for patients undergoing RT. In a study including patients undergoing adjuvant RT for breast cancer, a prophylactic EGCG solution significantly reduced RID incidence and severity by inhibiting oxidative stress induced by ultraviolet radiation [82]. In a single-arm study on the effects of EGCG in breast cancer, dermatitis severity regressed to grade 2 in 2 patients using EGCG [83]. The antioxidant activity of EGCG involves free radical scavenging; as such, it is being increasingly used for RID [84]. EGCG pretreatment significantly enhances skin cell viability after irradiation with x-ray and prevents x-ray-associated apoptosis incidence [85].
The beneficial effects of EGCG against RID may be attributable to a complex set of molecular mechanisms. EGCG effectively impedes NF-κB gene transcription, leading to a reduction in the expression of various inflammation-associated genes [86]. In particular, EGCG phosphorylates IκB and its upstream kinase inhibitor, κB kinase; this external stimulation activates macrophages, which in turn induces NF-κB activation [87]. This activation leads to inflammatory response modulation: it blocks the transcription of NF-κB, mainly through the induction of iNOS and COX-2, and reduces the levels of proinflammatory molecules, such as IL-1, TNF-α, and NO; furthermore, activation of antioxidant genes such as HO-1 mediated by Nrf2 inhibits NF-κB activation and thus the inflammatory response in macrophages [88].
Allantoin
Allantoin is a common ingredient in formulations recommended for treating skin care after exposure to ionizing radiation. A compound derived from heterocyclic urea, allantoin is widely used in skin care products to soothe, protect, condition, and moisturize the skin.
Allantoin affects skin regeneration by promoting cell reconstitution and exhibiting anti-inflammatory properties [74]; therefore, it may have therapeutic effects on RID. Allantoin significantly reduces mean skin toxicity levels after 3 weeks of RT; compared with that before RT initiation, allantoin-containing creams are much less effective at relieving inflammatory symptoms after 6 RT weeks or RT termination [89].
Sucralfate
Topical sucralfate exhibits excellent barrier ability, antibacterial activity, anti-inflammatory effects, and angiogenesis-promoting ability. Topical sucralfate also has therapeutic effects on mucocutaneous inflammatory diseases (including post-RT reactions) and mucocutaneous infectious diseases [90].
The results regarding the clinical efficacy of sucralfate in RID treatment are, however, mixed. Maiche et al. conducted a double-blind, randomized study on breast cancer patients undergoing electron beam therapy to assess the effectiveness of 7% micronized sucrose sucralfate cream. Their results revealed that sucralfate cream application significantly prevents acute radiation response in the skin. Delany et al [90] evaluated the effectiveness of topical 10% sucralfate cream in patients with wet desquamation due to RT. However, the authors noted that in these patients, 10% sucralfate cream does not lead to superior outcomes.
The potential mechanism through which sucralfate prevents or alleviates RID are as follows: (i) reduction in oxygen radical generation; (ii) modulation of macrophage activation and COX-2 activity and increase in PGE2 release; and (iii) enhancement of growth factor availability, promotion of blood flow and cell proliferation, and tissue repair through tissue growth factor binding.
Trolamine
Trolamine, a nonsteroidal anti-inflammatory molecule, is widely used as an oil-in-water emulsion in clinical practice for RID treatment in some European countries. Hamza et al. confirmed that trolamine emulsion considerably reduces ARD severity in head and neck squamous cell carcinoma patients receiving chemo-RT [91]. However, in a study, trolamine did not demonstrate superior RID treatment outcomes to those of supportive care or the placebo [13]. A study comparing calendula and trolamine for RID treatment indicated that trolamine might not be suitable as a standard alternative for RID prevention or treatment in patients with breast cancer or HNC [92]. Trolamine may resolve RID through a nonsteroidal anti-inflammatory process, where it may stimulate macrophage recruitment and promote granulation tissue growth [13].
Biafine emulsion
Biafine emulsion topical emulsion can accelerate wound healing by enhancing macrophage infiltration into the wound bed. In the early stages of healing, biafine emulsion use is associated with increased macrophage infiltration but reduced neutrophil infiltration [93].
A systematic review and meta-analysis suggested that biafine emulsion prevents RID development in patients with breast cancer; however, although it is less effective in preventing grade 1 and 2 RID or reducing RID incidence, it can reduce RID severity [77]. A study indicated that when used to treat grade 2 or 3 RID, the effects of biafine emulsion did not differ from those of Mabel ointment (comprising 0.25% b-sitosterol); in contrast, Mabel ointment significantly reduced toxic itching and local skin pain [94].
In summary, the application of biafine emulsion to RID may reduce inflammatory response by enhancing macrophage infiltration and lowering the neutrophil count. However, it may not be as effective as other topical nonsteroidal agents.
Topical corticosteroids
Mometasone furoate
Mometasone furoate, a synthetic corticosteroid, can prevent the development of severe RID. In particular, it induces proteins that inhibit phospholipase A2 and prevents arachidonic acid release from the phospholipid membrane, thus inhibiting the synthesis of specific inflammatory mediators effectively [95].
Recent studies on mometasone furoate cream have reported that it significantly alleviates ARD when applied topically. Mometasone furoate potentially inhibits the arachidonic acid pathway; it also significantly reduces leukotriene production and adhesion molecule expression and inhibits inflammatory cytokine and growth factor production [96]. Taken together, these effects lead to the inflammation-inhibition effect of mometasone furoate.
A clinical trial including 120 patients with breast cancer demonstrated that the patients using mometasone furoate cream experienced a significant reduction in RID incidence and an improvement in health-related quality of life [97]. In a randomized controlled trial including 41 head and neck squamous cell carcinoma patients undergoing radical RT, mometasone furoate cream application after high-dose RT (> 50 Gy) prevented ARD effectively, particularly when the radiation dose was < 6000 Gy [98].
In summary, many studies have examined topical corticosteroid use for ARD prevention. Current evidence consistently supports the efficacy of mometasone furoate in preventing ARD and the associated symptoms [99].
Betamethasone
Betamethasone, also a topical corticosteroid, can effectively prevent severe RID. Its mechanism of action inhibits the activation of NF-κB and the production of inflammatory cytokines (IL-6, IL-8, IL-1β, TNF-α), leading to its potent glucocorticoid activity [95].
Compared with mometasone furoate, betamethasone has a higher anti-RID potential because it more effectively prevents RID occurrence and progression in patients with cancer. Current evidence supports the use of topical corticosteroids to prevent ARD and its associated symptoms [99,100,101]. In breast cancer patients undergoing RT, daily topical application of betamethasone reduces ARD incidence [102]. In summary, betamethasone is more effective than mometasone furoate in preventing RID occurrence and progression in patients with cancer.
Conclusions
Many topical agents currently available on the market have RID treatment potential. These agents include natural agents (eg., silymarin, calendula, and PTNs), miscellaneous agents (eg., Juango cream, holoil, and vitamins), topical nonsteroidal agents (eg., EGCG, statins, and D-panthenol), and topical corticosteroids (eg., mometasone furoate and betamethasone). In experimental studies, silymarin, N. sativa gel, olive oil, Juango cream, doxepin, EGCG, and betamethasone have demonstrated positive RID treatment outcomes in breast cancer patients undergoing RT treatment; similarly, honey and holoil have demonstrated positive RID treatment outcomes in HNC patients undergoing RT. Moreover, calendula and mometasone furoate may be suitable for RID treatment in breast cancer patients undergoing chemotherapy, as well as in HNC patients after RT. In particular, MASCC guidelines recommend topical steroids and olive oil for RID prevention.
Most topical agents reviewed herein are used to prevent and manage RID by regulating oxidative stress and inflammatory responses; their mechanisms of action include regulation of the NF-κB pathway, promotion of antioxidant and anti-inflammatory activities, acceleration of wound healing, and formation of skin barriers. However, the mechanisms of action of some topical agents with promising preventive and therapeutic effects on RID remain unclear. Moreover, the applicability and efficacy of most of these topical agents for RID prevention and treatment in patients with different types of cancer vary widely. Therefore, whether these topical agents can be used for RID treatment or prevention, regardless of the cancer type, warrants further research.
All relevant studies reported thus far have several limitations. These studies have not classified patients based on the differences in their skin sensitivity to radiation; moreover, they have used small patient samples, employed different study designs and intervention types, and reported different assessment results. As such, the currently available evidence regarding the use of topical agents for RID prevention and management is of low quality. Furthermore, relevant trials have reported conflicting findings, with most of them not recommending the assessed topical agents for use in RID prevention and management.
RT is typically indicated for weak patients undergoing multiple treatments.
Patients typically become debilitated by multiple radiation treatments. In these patients, topical agents are the most convenient, inexpensive, and safest options for RID prevention and treatment. Future studies should focus on developing criteria for RID prevention and treatment using topical agents.
Data availability
Data sharing is not applicable to this article as no new data were created or analyzed in this study.
References
Fuzissaki MA, Paiva CE, Oliveira MA, Lajolo Canto PP, Paiva Maia YC. The impact of radiodermatitis on breast cancer patients’ quality of life during radiotherapy: a prospective cohort study. J Pain Symptom Manage. 2019. https://doi.org/10.1016/j.jpainsymman.2019.03.017.
Yokota T, Zenda S, Ota I, Yamazaki T, Yamaguchi T, Ogawa T, et al. Phase 3 randomized trial of topical steroid versus placebo for prevention of radiation dermatitis in patients with head and neck cancer receiving chemoradiation. Int J Radiat Oncol Biol Phys. 2021;111(3):794–803. https://doi.org/10.1016/j.ijrobp.2021.05.133.
Yang X, Ren H, Guo X, Hu C, Fu J. Radiation-induced skin injury: pathogenesis, treatment, and management. Aging (Albany NY). 2020. https://doi.org/10.18632/aging.103932.
Najafi M, Motevaseli E, Shirazi A, Geraily G, Rezaeyan A, Norouzi F, et al. Mechanisms of inflammatory responses to radiation and normal tissues toxicity: clinical implications. Int J Radiat Biol. 2018;94(4):335–56. https://doi.org/10.1080/09553002.2018.1440092.
Wei J, Meng L, Hou X, Qu C, Wang B, Xin Y, et al. Radiation-induced skin reactions: mechanism and treatment. Cancer Manag Res. 2019. https://doi.org/10.2147/CMAR.S188655.
Behroozian T, Bonomo P, Patel P, Kanee L, Finkelstein S, van den Hurk C, et al. Multinational association of supportive care in cancer (MASCC) clinical practice guidelines for the prevention and management of acute radiation dermatitis: international delphi consensus-based recommendations. Lancet Oncol. 2023;24(4):e172–85. https://doi.org/10.1016/S1470-2045(23)00067-0.
Baharara H, Rahsepar S, Emami SA, Elyasi S, Mohammadpour AH, Ghavami V, et al. The efficacy of medicinal plant preparations in the alleviation of radiodermatitis in patients with breast cancer: a systematic review of clinical trials. Phytother Res. 2023. https://doi.org/10.1002/ptr.7894.
Karbasforooshan H, Hosseini S, Elyasi S, Fani Pakdel A, Karimi G. Topical silymarin administration for prevention of acute radiodermatitis in breast cancer patients: a randomized, double-blind, placebo-controlled clinical trial. Phytother Res. 2019;33(2):379–86. https://doi.org/10.1002/ptr.6231.
Gillessen A, Schmidt HH. Silymarin as supportive treatment in liver diseases: a narrative review. Adv Ther. 2020;37(4):1279–301. https://doi.org/10.1007/s12325-020-01251-y.
Cruceriu D, Balacescu O, Rakosy E. Calendula officinalis: potential roles in cancer treatment and palliative care. Integr Cancer Ther. 2018;17(4):1068–78. https://doi.org/10.1177/1534735418803766.
Koukourakis G, Pissakas G, Ganos CG, Sivolapenko G, Kardamakis D. Effectiveness and tolerability of natural herbal formulations in the prevention of radiation-Induced skin toxicity in patients undergoing radiotherapy. Int J Low Extrem Wounds. 2022;21(1):75–86. https://doi.org/10.1177/1534734620923912.
Kole AJ, Kole L, Moran MS. Acute radiation dermatitis in breast cancer patients: challenges and solutions. Breast Cancer (Dove Med Press). 2017. https://doi.org/10.2147/BCTT.S109763.
Rosenthal A, Israilevich R, Moy R. Management of acute radiation dermatitis: A review of the literature and proposal for treatment algorithm. J Am Acad Dermatol. 2019;81(2):558–67. https://doi.org/10.1016/j.jaad.2019.02.047.
Shahane K, Kshirsagar M, Tambe S, Jain D, Rout S, Ferreira MKM, et al. An updated review on the multifaceted therapeutic potential ofcalendula officinalis L. Pharmaceuticals (Basel). 2023;16(4):611. https://doi.org/10.3390/ph16040611.
Givol O, Kornhaber R, Visentin D, Cleary M, Haik J, Harats M. A systematic review of calendula officinalis extract for wound healing. Wound Repair Regen. 2019;27(5):548–61. https://doi.org/10.1111/wrr.12737.
Ferreira AS, Macedo C, Silva AM, Delerue-Matos C, Costa P, Rodrigues F. Natural products for the prevention and treatment of oral mucositis-a review. Int J Mol Sci. 2022;23(8):4385. https://doi.org/10.3390/ijms23084385.
Yang K, Kim SY, Park JH, Ahn WG, Jung SH, Oh D, et al. Topical application of phlorotannins from brown seaweed mitigates radiation dermatitis in a mouse model. Mar Drugs. 2020;18(8):377. https://doi.org/10.3390/md18080377.
Besednova NN, Andryukov BG, Zaporozhets TS, Kuznetsova TA, Kryzhanovsky SP, Ermakova SP, et al. Molecular targets of brown algae phlorotannins for the therapy of inflammatory processes of various origins. Mar Drugs. 2022;20(4):243. https://doi.org/10.3390/md20040243.
Maleki M, Mardani A, Manouchehri M, Ashghali Farahani M, Vaismoradi M, Glarcher M. Effect of chamomile on the complications of cancer: a systematic review. Integr Cancer Ther. 2023. https://doi.org/10.1177/15347354231164600.
Bhaskaran N, Shukla S, Srivastava JK, Gupta S. Chamomile: an anti-inflammatory agent inhibits inducible nitric oxide synthase expression by blocking RelA/p65 activity. Int J Mol Med. 2010;26(6):935–40. https://doi.org/10.3892/ijmm_00000545.
Sah A, Naseef PP, Kuruniyan MS, Jain GK, Zakir F, Aggarwal G. A comprehensive study of therapeutic applications of chamomile. Pharmaceuticals (Basel). 2022;15(10):1284. https://doi.org/10.3390/ph15101284.
Rafati M, Ghasemi A, Saeedi M, Habibi E, Salehifar E, Mosazadeh M, et al. Nigella sativa L. for prevention of acute radiation dermatitis in breast cancer: a randomized, double-blind, placebo-controlled, clinical trial. Complement Ther Med. 2019. https://doi.org/10.1016/j.ctim.2019.102205.
Nasiri N, Ilaghi Nezhad M, Sharififar F, Khazaneha M, Najafzadeh MJ, Mohamadi N. The therapeutic effects of nigella sativa on skin disease: A systematic review and meta-analysis of randomized controlled trials. Evid Based Complement Alternat Med. 2022. https://doi.org/10.1155/2022/7993579.
Majdalawieh AF, Fayyad MW, Nasrallah GK. Anti-cancer properties and mechanisms of action of thymoquinone, the major active ingredient of Nigella sativa. Crit Rev Food Sci Nutr. 2017;57(18):3911–28. https://doi.org/10.1080/10408398.2016.1277971.
Hossen MJ, Yang WS, Kim D, Aravinthan A, Kim JH, Cho JY. Thymoquinone: An IRAK1 inhibitor with in vivo and in vitro anti-inflammatory activities. Sci Rep. 2017. https://doi.org/10.1038/srep42995.
Talebi M, Farkhondeh T, Samarghandian S. Biological and therapeutic activities of thymoquinone: Focus on the Nrf2 signaling pathway. Phytother Res. 2021;35(4):1739–53. https://doi.org/10.1002/ptr.6905.
Memarzia A, Khazdair MR, Behrouz S, Gholamnezhad Z, Jafarnezhad M, Saadat S, et al. Experimental and clinical reports on anti-inflammatory, antioxidant, and immunomodulatory effects of Curcuma longa and curcumin, an updated and comprehensive review. BioFactors. 2021;47(3):311–50. https://doi.org/10.1002/biof.1716.
Palatty PL, Azmidah A, Rao S, Jayachander D, Thilakchand KR, Rai MP, et al. Topical application of a sandal wood oil and turmeric based cream prevents radiodermatitis in head and neck cancer patients undergoing external beam radiotherapy: a pilot study. Br J Radiol. 2014;87(1038):20130490. https://doi.org/10.1259/bjr.20130490.
Ryan JL, Heckler CE, Ling M, Katz A, Williams JP, Pentland AP, et al. Curcumin for radiation dermatitis: a randomized, double-blind, placebo-controlled clinical trial of thirty breast cancer patients. Radiat Res. 2013;180(1):34–43. https://doi.org/10.1667/RR3255.1.
Ryan Wolf J, Gewandter JS, Bautista J, Heckler CE, Strasser J, Dyk P, et al. Utility of topical agents for radiation dermatitis and pain: a randomized clinical trial. Support Care Cancer. 2020;28(7):3303–11. https://doi.org/10.1007/s00520-019-05166-5.
Akbari S, Kariznavi E, Jannati M, Elyasi S, Tayarani-Najaran Z. Curcumin as a preventive or therapeutic measure for chemotherapy and radiotherapy induced adverse reaction: a comprehensive review. Food Chem Toxicol. 2020. https://doi.org/10.1016/j.fct.2020.111699.
Derosa G, Maffioli P, Simental-Mendia LE, Bo S, Sahebkar A. Effect of curcumin on circulating interleukin-6 concentrations: A systematic review and meta-analysis of randomized controlled trials. Pharmacol Res. 2016. https://doi.org/10.1016/j.phrs.2016.07.004.
Han S, Xu J, Guo X, Huang M. Curcumin ameliorates severe influenza pneumonia via attenuating lung injury and regulating macrophage cytokines production. Clin Exp Pharmacol Physiol. 2018;45(1):84–93. https://doi.org/10.1111/1440-1681.12848.
Kao YS, Ma KS, Wu MY, Wu YC, Tu YK, Hung CH. Topical prevention of radiation dermatitis in head and neck cancer patients: a network meta-analysis. In Vivo. 2022. https://doi.org/10.21873/invivo.12851.
Cui Z, Xin M, Yin H, Zhang J, Han F. Topical use of olive oil preparation to prevent radiodermatitis: results of a prospective study in nasopharyngeal carcinoma patients. Int J Clin Exp Med. 2015;8(7):11000–6.
Chitapanarux I, Tovanabutra N, Chiewchanvit S, Sripan P, Chumachote A, Nobnop W, et al. Emulsion of olive oil and calcium hydroxide for the prevention of radiation dermatitis in hypofractionation post-mastectomy padiotherapy: a randomized controlled trial. Breast Care (Basel). 2019;14(6):394–400. https://doi.org/10.1159/000496062.
Robijns J, Becherini C, Caini S, Wolf JR, van den Hurk C, Beveridge M, et al. Natural and miscellaneous agents for the prevention of acute radiation dermatitis: a systematic review and meta-analysis. Support Care Cancer. 2023;31(3):195. https://doi.org/10.1007/s00520-023-07656-z.
Hendawy OM, Al-Sanea MM, Elbargisy RM, Rahman HU, Mohamed AAB, Kamal I, et al. Phenylboronic acid-grafted chitosan nanocapsules for effective delivery and controllable release of natural antioxidants: Olive oil and hydroxytyrosol. Pharmaceutics. 2022. https://doi.org/10.3390/pharmaceutics15010081.
Thanthong S, Nanthong R, Kongwattanakul S, Laebua K, Trirussapanich P, Pitiporn S, et al. Prophylaxis of radiation-induced dermatitis in patients with breast cancer using herbal creams: a prospective randomized controlled trial. Integr Cancer Ther. 2020. https://doi.org/10.1177/1534735420920714.
Mukherjee PK, Nema NK, Maity N, Sarkar BK. Phytochemical and therapeutic potential of cucumber. Fitoterapia. 2013. https://doi.org/10.1016/j.fitote.2012.10.003.
Vats M, Bhardwaj S, Chhabra A. Green synthesis of copper oxide nanoparticles using Cucumis sativus (cucumber) extracts and their bio-physical and biochemical characterization for cosmetic and dermatologic applications. Endocr Metab Immune Disord Drug Targets. 2021;21(4):726–33. https://doi.org/10.2174/1871530320666200705212107.
Charalambous M, Raftopoulos V, Paikousis L, Katodritis N, Lambrinou E, Vomvas D, et al. The effect of the use of thyme honey in minimizing radiation - induced oral mucositis in head and neck cancer patients: A randomized controlled trial. Eur J Oncol Nurs. 2018. https://doi.org/10.1016/j.ejon.2018.04.003.
Yang C, Gong G, Jin E, Han X, Zhuo Y, Yang S, et al. Topical application of honey in the management of chemo/radiotherapy-induced oral mucositis: A systematic review and network meta-analysis. Int J Nurs Stud. 2019. https://doi.org/10.1016/j.ijnurstu.2018.08.007.
Rao S, Hegde SK, Rao P, Dinkar C, Thilakchand KR, George T, et al. Honey mitigates radiation-induced oral mucositis in head and neck cancer patients without affecting the tumor response. Foods. 2017;6(9):77. https://doi.org/10.3390/foods6090077.
Hawley P, Hovan A, McGahan CE, Saunders D. A randomized placebo-controlled trial of manuka honey for radiation-induced oral mucositis. Support Care Cancer. 2014;22(3):751–61. https://doi.org/10.1007/s00520-013-2031-0.
Samarghandian S, Farkhondeh T, Samini F. Honey and health: a review of recent clinical research. Pharmacognosy Res. 2017;9(2):121–7. https://doi.org/10.4103/0974-8490.204647.
Ahmed S, Sulaiman SA, Baig AA, Ibrahim M, Liaqat S, Fatima S, et al. Honey as a potential natural antioxidant medicine: An insight into its molecular mechanisms of action. Oxid Med Cell Longev. 2018. https://doi.org/10.1155/2018/8367846.
Rekik DM, Ben Khedir S, Daoud A, Ksouda Moalla K, Rebai T, Sahnoun Z. Wound healing effect of lawsonia inermis. Skin Pharmacol Physiol. 2019;32(6):295–306. https://doi.org/10.1159/000501730.
Tungkasamit T, Chakrabandhu S, Samakgarn V, Kunawongkrit N, Jirawatwarakul N, Chumachote A, et al. Reduction in severity of radiation-induced dermatitis in head and neck cancer patients treated with topical aloe vera gel: a randomized multicenter double-blind placebo-controlled trial. Eur J Oncol Nurs. 2022. https://doi.org/10.1016/j.ejon.2022.102164.
Karbasizade S, Ghorbani F, Ghasemi Darestani N, Mansouri-Tehrani MM, Kazemi AH. Comparison of therapeutic effects of statins and aloe vera mouthwash on chemotherapy induced oral mucositis. Int J Physiol Pathophysiol Pharmacol. 2021;13(4):110–6.
Sahebjamee M, Mansourian A, Hajimirzamohammad M, Zadeh MT, Bekhradi R, Kazemian A, et al. Comparative efficacy of Aloe vera and benzydamine mouthwashes on radiation-induced oral mucositis: a triple-blind, randomised, controlled clinical trial. Oral Health Prev Dent. 2015;13(4):309–15. https://doi.org/10.3290/j.ohpd.a33091.
Wang T, Liao J, Zheng L, Zhou Y, Jin Q, Wu Y. Aloe vera for prevention of radiation-induced dermatitis: A systematic review and cumulative analysis of randomized controlled trials. Front Pharmacol. 2022. https://doi.org/10.3389/fphar.2022.976698.
Sanchez M, Gonzalez-Burgos E, Iglesias I, Gomez-Serranillos MP. Pharmacological update properties of aloe vera and its major active constituents. Molecules. 2020. https://doi.org/10.3390/molecules25061324.
Liu FW, Liu FC, Wang YR, Tsai HI, Yu HP. Aloin protects skin fibroblasts from heat stress-induced oxidative stress damage by regulating the oxidative defense system. PLoS ONE. 2015;10(12): e0143528. https://doi.org/10.1371/journal.pone.0143528.
Bala S, Chugh NA, Bansal SC, Garg ML, Koul A. Radiomodulatory effects of Aloe vera on hepatic and renal tissues of X-ray irradiated mice. Mutat Res. 2018. https://doi.org/10.1016/j.mrfmmm.2018.07.001.
Wahedi HM, Jeong M, Chae JK, Do SG, Yoon H, Kim SY. Aloesin from Aloe vera accelerates skin wound healing by modulating MAPK/Rho and Smad signaling pathways in vitro and in vivo. Phytomedicine. 2017. https://doi.org/10.1016/j.phymed.2017.02.005.
Kong M, Hwang DS, Lee JY, Yoon SW. The efficacy and safety of Jaungo, a traditional medicinal ointment, in preventing radiation dermatitis in patients with breast cancer: a prospective, single-Blinded, randomized pilot study. Evid Based Complement Alternat Med. 2016. https://doi.org/10.1155/2016/9481413.
Park JY, Kwak JH, Kang KS, Jung EB, Lee DS, Lee S, et al. Wound healing effects of deoxyshikonin isolated from Jawoongo: In vitro and in vivo studies. J Ethnopharmacol. 2017. https://doi.org/10.1016/j.jep.2016.10.031.
Kim EH, Kim W. Post treatment application of Jaungo after a combined therapy of carbon dioxide laser and trichloroacetic acid in a case of vulvar syringoma. J Pharmacopuncture. 2019;22(3):200–3. https://doi.org/10.3831/KPI.2019.22.027.
Franco P, Rampino M, Ostellino O, Schena M, Pecorari G, Garzino Demo P, et al. Management of acute skin toxicity with Hypericum perforatum and neem oil during platinum-based concurrent chemo-radiation in head and neck cancer patients. Med Oncol. 2017;34(2):30. https://doi.org/10.1007/s12032-017-0886-5.
Franco P, Potenza I, Moretto F, Segantin M, Grosso M, Lombardo A, et al. Hypericum perforatum and neem oil for the management of acute skin toxicity in head and neck cancer patients undergoing radiation or chemo-radiation: a single-arm prospective observational study. Radiat Oncol. 2014. https://doi.org/10.1186/s13014-014-0297-0.
Anderson PM, Lalla RV. Glutamine for amelioration of radiation and chemotherapy associated mucositis during cancer therapy. Nutrients. 2020. https://doi.org/10.3390/nu12061675.
de Sousa MA, de Lima Dantas JB, Medrado A, Lima HR, Martins GB, Carrera M. Nutritional supplements in the management of oral mucositis in patients with head and neck cancer: narrative literary review. Clin Nutr ESPEN. 2021. https://doi.org/10.1016/j.clnesp.2021.03.030.
Yarom N, Hovan A, Bossi P, Ariyawardana A, Jensen SB, Gobbo M, et al. Correction to: Systematic review of natural and miscellaneous agents, for the management of oral mucositis in cancer patients and clinical practice guidelines–part 1: vitamins, minerals and nutritional supplements. Support Care Cancer. 2021;29(7):4175–6. https://doi.org/10.1007/s00520-021-06141-9.
Konuk Sener D, Aydin M, Cangur S, Guven E. The effect of oral care with chlorhexidine, vitamin E and honey on mucositis in pediatric intensive care patients: A randomized controlled trial. J Pediatr Nurs. 2019. https://doi.org/10.1016/j.pedn.2019.02.001.
Pessoa AF, Florim JC, Rodrigues HG, Andrade-Oliveira V, Teixeira SA, Vitzel KF, et al. Oral administration of antioxidants improves skin wound healing in diabetic mice. Wound Repair Regen. 2016;24(6):981–93. https://doi.org/10.1111/wrr.12486.
Cinausero M, Aprile G, Ermacora P, Basile D, Vitale MG, Fanotto V, et al. New frontiers in the pathobiology and treatment of cancer regimen-related mucosal injury. Front Pharmacol. 2017. https://doi.org/10.3389/fphar.2017.00354.
Higgins MR, Izadi A, Kaviani M. Antioxidants and exercise performance: With a focus on vitamin E and C supplementation. Int J Environ Res Public Health. 2020;17(22):8452. https://doi.org/10.3390/ijerph17228452.
Jacobs C, Hutton B, Ng T, Shorr R, Clemons M. Is there a role for oral or intravenous ascorbate (vitamin C) in treating patients with cancer? A systematic review. Oncologist. 2015;20(2):210–23. https://doi.org/10.1634/theoncologist.2014-0381.
Sio TT, Le-Rademacher JG, Leenstra JL, Loprinzi CL, Rine G, Curtis A, et al. Effect of doxepin mouthwash or diphenhydramine-lidocaine-antacid mouthwash vs placebo on radiotherapy-related oral mucositis pain: The alliance a221304 randomized clinical trial. JAMA. 2019;321(15):1481–90. https://doi.org/10.1001/jama.2019.3504.
Shariati L, Amouheidari A, Naji Esfahani H, Abed A, Haghjooy Javanmard S, Laher I, et al. Protective effects of doxepin cream on radiation dermatitis in breast cancer: A single arm double-blind randomized clinical trial. Br J Clin Pharmacol. 2020;86(9):1875–81. https://doi.org/10.1111/bcp.14238.
Tao F, Zhu J, Duan L, Wu J, Zhang J, Yao K, et al. Anti-inflammatory effects of doxepin hydrochloride against LPS-induced C6-glioma cell inflammatory reaction by PI3K-mediated Akt signaling. J Biochem Mol Toxicol. 2020;34(2): e22424. https://doi.org/10.1002/jbt.22424.
Zabihi M, Hajhashemi V, Minaiyan M, Talebi A. Evaluation of the central and peripheral effects of doxepin on carrageenan-induced inflammatory paw edema in rat. Res Pharm Sci. 2017;12(4):337–45. https://doi.org/10.4103/1735-5362.212052.
Kondziołka J, Wilczyński S. Overview of the activei ingredients in cosmetic products for the care of skin that has been exposed to ionizing radiation - Analysis of their effectiveness in breast cancer radiotherapy. Clin Cosmet Investig Dermatol. 2021. https://doi.org/10.2147/ccid.s322228.
Pinnix C, Perkins GH, Strom EA, Tereffe W, Woodward W, Oh JL, et al. Topical hyaluronic acid vs. standard of care for the prevention of radiation dermatitis after adjuvant radiotherapy for breast cancer: single-blind randomized phase III clinical trial. Int J Radiat Oncol Biol Phys. 2012. https://doi.org/10.1016/j.ijrobp.2011.09.021.
Rahimi A, Mohamad O, Albuquerque K, Kim DWN, Chen D, Thomas K, et al. Novel hyaluronan formulation for preventing acute skin reactions in breast during radiotherapy: a randomized clinical trial. Support Care Cancer. 2020;28(3):1481–9. https://doi.org/10.1007/s00520-019-04957-0.
Fatima S, Hirakawa S, Marta GN, Caini S, Beveridge M, Bonomo P, et al. Topical non-steroidal agents for the prevention of radiation dermatitis: a systematic review and meta-analysis. Support Care Cancer. 2023;31(4):217. https://doi.org/10.1007/s00520-023-07677-8.
Presta G, Puliatti A, Bonetti L, Tolotti A, Sari D, Valcarenghi D. Effectiveness of hyaluronic acid gel (Jalosome soothing gel) for the treatment of radiodermatitis in a patient receiving head and neck radiotherapy associated with cetuximab: a case report and review. Int Wound J. 2019;16(6):1433–9. https://doi.org/10.1111/iwj.13210.
Lee CJ, Fang HF, Wang CY, Chou KR, Huang TW. Effect of hyaluronic acid on radiodermatitis in patients with breast cancer: a meta-analysis of randomized controlled trials. Support Care Cancer. 2022;30(5):3965–75. https://doi.org/10.1007/s00520-022-06828-7.
Juncan AM, Moisa DG, Santini A, Morgovan C, Rus LL, Vonica-Tincu AL, et al. Advantages of hyaluronic acid and its combination with other bioactive ingredients in cosmeceuticals. Molecules. 2021;26(15):4429. https://doi.org/10.3390/molecules26154429.
Ghasemi A, Ghashghai Z, Akbari J, Yazdani-Charati J, Salehifar E, Hosseinimehr SJ. Topical atorvastatin 1% for prevention of skin toxicity in patients receiving radiation therapy for breast cancer: a randomized, double-blind, placebo-controlled trial. Eur J Clin Pharmacol. 2019;75(2):171–8. https://doi.org/10.1007/s00228-018-2570-x.
Zhao H, Zhu W, Zhao X, Li X, Zhou Z, Zheng M, et al. Efficacy of Epigallocatechin-3-Gallate in preventing dermatitis in patients with breast cancer receiving postoperative radiotherapy: a double-blind, placebo-controlled, phase 2 randomized clinical trial. JAMA Dermatol. 2022;158(7):779–86. https://doi.org/10.1001/jamadermatol.2022.1736.
Zhao H, Zhu W, Jia L, Sun X, Chen G, Zhao X, et al. Phase I study of topical epigallocatechin-3-gallate (EGCG) in patients with breast cancer receiving adjuvant radiotherapy. Br J Radiol. 2016;89(1058):20150665. https://doi.org/10.1259/bjr.20150665.
Kim SR, Seong KJ, Kim WJ, Jung JY. Epigallocatechin gallate protects against hypoxia-induced inflammation in microglia via NF-kappaB suppression and Nrf-2/HO-1 activation. Int J Mol Sci. 2022;23(7):4004. https://doi.org/10.3390/ijms23074004.
Zhu W, Xu J, Ge Y, Cao H, Ge X, Luo J, et al. Epigallocatechin-3-gallate (EGCG) protects skin cells from ionizing radiation via heme oxygenase-1 (HO-1) overexpression. J Radiat Res. 2014;55(6):1056–65. https://doi.org/10.1093/jrr/rru047.
Musial C, Kuban-Jankowska A, Gorska-Ponikowska M. Beneficial properties of green tea catechins. Int J Mol Sci. 2020;21(5):1744. https://doi.org/10.3390/ijms21051744.
Yang HL, Lin MW, Korivi M, Wu JJ, Liao CH, Chang CT, et al. Coenzyme Q0 regulates NFkappaB/AP-1 activation and enhances Nrf2 stabilization in attenuation of LPS-induced inflammation and redox imbalance: Evidence from in vitro and in vivo studies. Biochim Biophys Acta. 2016;1859(2):246–61. https://doi.org/10.1016/j.bbagrm.2015.11.001.
Ronchetti D, Impagnatiello F, Guzzetta M, Gasparini L, Borgatti M, Gambari R, et al. Modulation of iNOS expression by a nitric oxide-releasing derivative of the natural antioxidant ferulic acid in activated RAW 264.7 macrophages. Eur J Pharmacol. 2006. https://doi.org/10.1016/j.ejphar.2005.12.034.
Chan RJ, Mann J, Tripcony L, Keller J, Cheuk R, Blades R, et al. Natural oil-based emulsion containing allantoin versus aqueous cream for managing radiation-induced skin reactions in patients with cancer: a phase 3, double-blind, randomized, controlled trial. Int J Radiat Oncol Biol Phys. 2014;90(4):756–64. https://doi.org/10.1016/j.ijrobp.2014.06.034.
Abtahi-Naeini B, Saffaei A, Sabzghabaee AM, Amiri R, Hosseini NS, Niknami E, et al. Topical sucralfate for treatment of mucocutaneous conditions: A systematic review on clinical evidences. Dermatol Ther. 2022;35(4): e15334. https://doi.org/10.1111/dth.15334.
Abbas H, Bensadoun RJ. Trolamine emulsion for the prevention of radiation dermatitis in patients with squamous cell carcinoma of the head and neck. Support Care Cancer. 2012;20(1):185–90. https://doi.org/10.1007/s00520-011-1110-3.
Simões FV, Santos VO, Silva RND, Silva RCD. Effectiveness of skin protectors and calendula officinalis for prevention and treatment of radiodermatitis: an integrative review. Rev Bras Enferm. 2020;73(suppl 5): e20190815. https://doi.org/10.1590/0034-7167-2019-0815.
Krausz AE, Adler BL, Landriscina A, Rosen JM, Musaev T, Nosanchuk JD, et al. Biafine topical emulsion accelerates excisional and burn wound healing in mice. Arch Dermatol Res. 2015;307(7):583–94. https://doi.org/10.1007/s00403-015-1559-x.
Geara FB, Eid T, Zouain N, Thebian R, Andraos T, Chehab C, et al. Randomized, prospective, open-label phase III trial comparing mebo ointment with biafine cream for the management of acute dermatitis during radiotherapy for breast cancer. Am J Clin Oncol. 2018;41(12):1257–62. https://doi.org/10.1097/COC.0000000000000460.
Tam S, Zhou G, Trombetta M, Caini S, Ryan Wolf J, van den Hurk C, et al. Topical corticosteroids for the prevention of severe radiation dermatitis: a systematic review and meta-analysis. Support Care Cancer. 2023;31(7):382. https://doi.org/10.1007/s00520-023-07820-5.
Spada F, Barnes TM, Greive KA. Comparative safety and efficacy of topical mometasone furoate with other topical corticosteroids. Australas J Dermatol. 2018;59(3):e168–74. https://doi.org/10.1111/ajd.12762.
Holmes CJ, Plichta JK, Gamelli RL, Radek KA. Burn injury alters epidermal cholinergic mediators and increases HMGB1 and Caspase 3 in autologous donor skin and burn margin. Shock. 2017;47(2):175–83. https://doi.org/10.1097/SHK.0000000000000752.
Liao Y, Feng G, Dai T, Long F, Tang J, Pu Y, et al. Randomized, self-controlled, prospective assessment of the efficacy of mometasone furoate local application in reducing acute radiation dermatitis in patients with head and neck squamous cell carcinomas. Medicine (Baltimore). 2019;98(52): e18230. https://doi.org/10.1097/MD.0000000000018230.
Behroozian T, Goldshtein D, Ryan Wolf J, van den Hurk C, Finkelstein S, Lam H, et al. MASCC clinical practice guidelines for the prevention and management of acute radiation dermatitis: part 1 systematic review. Clin Med. 2023. https://doi.org/10.1016/j.eclinm.2023.101886.
Erridge SC, McCabe M, Porter MK, Simpson P, Stillie AL. Prospective audit showing improved patient-assessed skin toxicity with use of betamethasone cream for those at high risk of radiation dermatitis. Radiother Oncol. 2016;121(1):143–7. https://doi.org/10.1016/j.radonc.2016.07.005.
Menon A, Prem SS, Kumari R. Topical betamethasone valerate as a prophylactic agent to prevent acute radiation dermatitis in head and neck malignancies: A randomized, open-Label, phase 3 trial. Int J Radiat Oncol Biol Phys. 2021;109(1):151–60. https://doi.org/10.1016/j.ijrobp.2020.08.040.
Uysal B, Gamsiz H, Dincoglan F, Demiral S, Sager O, Dirican B, et al. Comparative evaluation of topical corticosteroid and moisturizer in the prevention of radiodermatitis in breast cancer radiotherapy. Indian J Dermatol. 2020;65(4):279–83. https://doi.org/10.4103/ijd.IJD_607_18.
Acknowledgements
We would like to thank the native English speaking scientists of Elixigen Company (Huntington Beach, California) for editing our manuscript.
Funding
This work was supported by a grant from the Funding for Chinese Medicine Service System and Capacity Building (Key Project with Chinese Medicine Characteristics and Advantages, Ruikang Hospital, 2023).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that there are no conflicts of interest.
Ethical approval and informed consent statements
As this article is a review, there is no need for ethical approval and informed consent statements.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guangmei, D., Weishan, H., Wenya, L. et al. Evolution of radiation-induced dermatitis treatment. Clin Transl Oncol 26, 2142–2155 (2024). https://doi.org/10.1007/s12094-024-03460-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-024-03460-1