Abstract
Ameloblastoma, One of the most Common and Frequently Encountered Odontogenic Epithelial Derived Tumours of the oral Cavity, are Reported to be Represented by Variable Number of Clinical, Radiological and Histological Types. Also, this Lesion has been Observed to be most Aggressive and has a Tendency to Recur in most Circumstances. The Histological Variants of Solid type of Ameloblastoma have also been Observed to Occur either in Isolation or in Combination with One or the Other Lesions. Hence, this case Report is One of those Combined Lesions Presenting with Little Clinical Presentation, but Histopathologically was Diagnosed to be Plexiform Ameloblastoma with Acanthomatous Changes. These Types of Lesions have been Scarcely Reported in Literature and should be Reported with Regular follow-up so as to not only Improve the Diagnostic Criteria, but also to Improve Surgical Outcomes, Making the Patients Prone to less Morbid Outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Odontogenic tumours can be variably defined as tumours or tumour-like growth that have their origin from odontogenic tissues, the heterogeneity amongst them being present as a result of varying induction that occurs between developing embryonic components which under normal conditions, would lead to the formation a normal tooth germ [1]. One such lesion is Ameloblastoma, which is the most common odontogenic tumours encountered in the jaws (48.9%) and represents 9% of all the odontogenic epithelial lesions found in the jaws, which itself causes minimal inductive changes in the connective tissue. It is a true neoplasm of enamel organ with certain peculiarities such as persistent local growth, high loco-regional invasion, non- encapsulated in nature and rarely metastasizing which does not undergo differentiation till the point it is capable of forming hard tissues(enamel). It was first coined as adamantinoma by Broca in 1868 and then defined by Malassez in 1885, who suggested that it may arise as a result of remnants of dental lamina [2]. It was then described by Robinson in 1937 as a benign tumour that is ―usually unicentric, non-functional, intermittent in growth, anatomically benign and clinically persistent. The World Health Organization (1991) defined ameloblastoma as a benign but locally aggressive tumour with a high tendency to recur, consisting of proliferating odontogenic epithelium lying in a fibrous stroma [3]. In 2005 WHO, had categorized ameloblastoma into (1) peripheral, which comprises an extraosseous counterpart and shows continuity with the oral mucosal stratified squamous epithelium, (2) unicystic, consisting of single cystic intraosseous growth pattern (3) solid/multicystic, characterized by invasive tumour which penetrates bone marrow spaces and may show multicystic foci (4) desmoplastic, comprising of an infiltrative intraosseous tumour dominated by the stromal component, radiographically reminiscent of a fibro-osseous lesion [4]. However, desmoplastic ameloblastoma was re-included only as a histological subtype in the 2017 WHO classification [5]. The tumour most commonly is found in jaw bones and has the potential to erode through the cancellous bone and it has been thought to arise through one of the following sources: - (1) Cell rests of the enamel organ, (2) epithelium of the odontogenic cysts, (3) disturbances of the developing enamel organ, (4) basal cells of the surface epithelium and (5) heterotrophic epithelium in other parts of the body [6]. It has variable clinical, radiological and histological characteristics, with a tendency to recur, if not excised in toto in a single go. The aetiology is unknown, but many associated factors have been proposed including nonspecific nonirritating factors such as extraction, caries, trauma, infection during tooth eruption or viral pathogenesis [7]. The lesion has most common tendency to occur in the mandibular molar-ramus region and is most often asymptomatic in its presentation [8]. It can occur in any decade of life, but most commonly presents in third to fourth decade, and may present clinically as swelling, loosening of teeth, malocclusion and sometimes pain [9]. The radiographic features are variable, ranging from multilocular radiolucency with scalloped cortical margins resulting in “soap-bubble appearance” to either expansion or resorption of cortical plate resulting in displacement, root resorption and loss of the teeth in the associated region [10]. Histologically, the variants of multicystic/ intraosseous ameloblastoma have been categorized as Follicular, Plexiform, Granular, Acanthomatous, Basaloid and Desmoplastic Ameloblastoma, occurring alone or in combination with one another [11]. The diagnostic criteria for identification of ameloblastoma was given by Vicker’s and Gorlin in 1970, which included: - hyperchromatism of basal cell nuclei, basal cell palisading with polarization which is referred to as reversal of polarity and cytoplasmic vacuolization with intercellular spacing of lining epithelium [12]. Management of ameloblastoma poses a challenge for all of those practitioners involved in the field of head and neck surgery because successful treatment requires not only adequate resection but also the functional and aesthetically acceptable reconstruction of the residual defect. Resection with wide margins and reconstruction in the same sitting is currently accepted as the treatment of choice in most cases. Idea of conservative surgery is no longer entertained since it is associated with higher recurrence rate [13].
The following study focuses on a case report which has reported to the department with only a complaint of swelling in the left posterior mandible with no associated symptoms which was then diagnosed to be Plexiform Ameloblastoma with Acanthomatous changes, which has been rarely reported in Literature.
Case Perspective
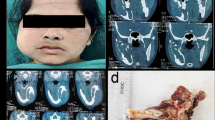
A patient reported to the department with the chief complaint of swelling in left lower back region of the jaw for 1 year. The swelling was gradual in onset, which slowly progressed to the size at the time patient reported. The swelling was not associated with any other symptoms of pain, induration or discharge from the affected region. Patient upon questioning further, did not revealed any history of substance abuse. Patient had a history of being diagnosed with Diabetes Mellitus in the last 2 years and is currently not on medication for the same, also had falling off the teeth in the region of swelling without any sort of intervention. Upon extraoral clinical examination, no gross facial asymmetry was noted. On intraoral clinical examination, hard, bony, painless swelling was noted extending from distal aspect of 35 without any extension into the soft tissues or extruding to the mucobuccal fold, being completely localised in the alveolar bone, and extended till the retromolar trigone region. Tooth corresponding to the same site viz., 36, 37, 38 were noted to be missing. Palpation confirmed the clinical findings. After the clinical examination, patient was sent for Cone- beam Computed tomography imaging. The imaging revealed a well demarcated, multilocular predominantly radiolucent lesion seen extending from the left side of the mandibular body region till the ramal region (Fig. 1). Then the patient was sent for haematological examination which revealed the fluid proteins level to be in higher range (987.50 mg/ dl: Normal range − 150–450 mg/dl). The provisional diagnosis of Odontogenic Keratocyst was given. Patient underwent complete surgical excision of the lesion and it was the fixed in Formalin and sent for histopathological examination. (Fig. 2).
Tissue underwent routine processing and then was stained with Haematoxylin and Eosin and the slides obtained were examined under examination. The examination revealed odontogenic islands arranged in the form of anastomosing pattern bounded by tall columnar cells with hyperchromatic nucleus in a palisaded arrangement showing reversal of polarity and subnuclear vacuolization. The central core of the section revealed loosely arranged stellate reticulum like areas with evidence of cystic degeneration and squamous differentiation. The histopathological features confirmed the diagnosis of Plexiform Ameloblastoma with Acanthomatous changes (Figs. 3 and 4).
Patient has been put on regular follow-up after surgical excision and reported no signs of recurrence after 6 months of excision.
Discussion
Plexiform ameloblastoma most commonly occurs during fifth to sixth decade of life. Most common site of occurrence is the posterior mandible. Plexiform Ameloblastoma has been classified histopathologically to be composed of cells arranged in interconnecting strands and cords with cuboidal or columnar basal cells exhibiting hyperchromatic nuclei, nuclear palisading with polarization and central stellate reticulumlike cells [14]. Acanthomatous ameloblastoma most common occurs during seventh decade of life [15]. The most common site of occurrence is the posterior mandible (80% of the cases). Histopathologically, acanthomatous type shows central squamous cell differential with keratin formation as seen in the present case. Some authors stated that formation of squamous metaplasia may be due to chronic irritation of calculus and oral sepsis [16]. Waldron and El-Mofty discovered a rare variant of ameloblastoma composed histologically of areas of the classic follicular or plexiform ameloblastoma and areas of desmoplastic ameloblastoma. This was named hybrid ameloblastoma (HA). Till 2016, > 30 cases with hybrid ameloblastoma have been reported in literature till date [17]. Hybrid ameloblastoma has a variable clinical, radiological, and histopathological presentation. They contain two or more different histologic types and their biologic comportment is still arguable. Mandible is the most common site for involvement of hybrid ameloblastomas as compared to the maxilla [18]. Radiographically, it mimics fibro-osseous diseases and odontogenic cysts and tumours with mixed radiolucent-radiopaque internal structure such as ossifying fibromas, fibrous dysplasia, osteoblastomas, osteosarcomas, calcifying epithelial odontogenic tumours, and calcifying odontogenic cysts [19]. With limited understanding of its behaviour and prognosis, the proper treatment strategies for hybrid ameloblastoma are not entirely defined so far. Based on the present knowledge, the WHO recommends to apply the same treatment modality as for solid ameloblastoma which includes complete resection as enucleation or curettage might result in its recurrence. However, small lesions can easily be enucleated in toto [20]. This kind of hybrid lesions is first amongst of its kind to be reported in the literature.
Conclusion
Hybrid ameloblastoma has a variable clinical, radiological, and histopathological presentation. The biologic comportment of the lesion is still arguable. Immunohistochemical markers may act as an adjunct in the accurate diagnosis of this lesion. Thus, many more clinical, radiological, and histopathological data are required to clearly demonstrate this pathologic entity. For this to take place, many case reports having such hybrid features should be increasingly reported so as to work out on all the arenas surrounding these lesions. The lesion reported in this article is Plexiform Ameloblastoma with Acanthomatous changes which has scarcely been reported in literature till date. So, a greater number of cases are required to form a basic sound literature proof.
References
Rastogi S, Nijhawan S, Modi M, Kumar A, Aslam N, Latheef F (2010) A large mixed radiolucent–radiopaque lesion in the mandible: a novel diagnostic approach. J Clin Diagn Res 4:2300–2307
Bansal M, Chaturvedi TP, Bansal R, kumar M (2010) Acanthomatous ameloblastoma of anterior maxilla. J Indian Soc Pedod prev Dent 28(3):209–211
Muddana K, Pasupula PA, Dorankula SP, Thokala MR, Muppallai JN (2014) Paediatric Odontogenic Tumour of the Jaw–A Case Report. J Clin Diagn Res 8(2):250–256
Barnes L, Eveson JW, Reichart P, Sidransky D (2005) WHO classification of Tumours: Pathology &Genetics, Head and Neck Tumours, vol 9. IARC, Lyon
Takata T, Slootweg PJ (2017) Odontogenic and maxillofacial bone tumours. In: El-Naggar AK, Chan JK, Grandis JR, Takata T, Slootweg PJ (eds) WHO classification of Head and Neck Tumours, 4th edn. IARC, Lyon
Adebiyi KE, Ugboko VI, Omoniyi-Esan GO, Ndukwe KC, Oginni FO (2006) Clinicopathological analysis of histological variants of ameloblastoma in a suburban Nigerian population. Head Face Med 24(242):171
Siar CH, Lau SH, Ng KH (2012) Ameloblastoma of the jaws: a retrospective analysis of 340 cases in a Malaysian population. J Oral Maxillofac Surg 70:608–615
Zemann W, Feichtinger M, Kowatsch E, Kärcher H (2007) Extensive ameloblastoma of the jaws: surgical management and immediate reconstruction using microvascular flaps. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103(2):190–196
Olaitan AA, Adeola DS, Adekeye EO (1993) Ameloblastoma: clinical features and management of 315 cases from Kaduna, Nigeria. J Craniomaxillofac Surg 21:351–355
McIvor J (1974) The radiological features of ameloblastoma. Clin Radiol 25(2):237–242
Reichart PA, Philipsen HP (2004) Odontogenic tumours and Allied lesions. Quintessence Pub: 189–197
Vickers RA, Gorlin RJ, Ameloblastoma (1970) Delineation of early histopathologic features of neoplasia. Cancer 3:699–710
Recurrence rate following treatment for primary multicystic ameloblastoma, Almeida RA, Andrade ES, Barbalho JC, Vajgel A, Vasconcelos BC (2016) Systematic review and meta-analysis. Int J Oral Maxillofac Surg 45:359–367
Deore SS, Dandekar RC, Mahajan AM, Patil R, Prakash N (2014) Plexiform unicystic ameloblastoma: A rare variant of ameloblastoma. Case Rep Dent; 2014:146989
Arkhede A, Tupkari JV, Mandale MS, Sarda M (2010) Plexiform ameloblastoma of mandible: Case report. J Clin Exp Dent 2:e146–e148
Bansal M, Chaturvedi TP, Bansal R, Kumar M (2010) Acanthomatous ameloblastoma of anterior maxilla. J Indian Soc Pedod Prev Dent 28:209–211
Waldron CA, el-Mofty SK (1987) A histopathologic study of 116 ameloblastomas with special reference to the desmoplastic variant. Oral Surg Oral Med Oral Pathol 63:441–451
Takata T, Miyauchi M, Ogawa I, Zhao M, Kudo Y, Sato S et al (1999) So-called ‘hybrid’ lesion of desmoplastic and conventional ameloblastoma: report of a case and review of the literature. Pathol Int 49:1014–1018
Madiyal A, Babu GS, Ajila V, Madi M, Castelino R, Rao K (2017) Desmoplastic ameloblastoma masquerading as a fibro-osseous lesion. Cukurova Med J 42:575–578
Hirota M, Aoki S, Kawabe R, Fujita K (2005) Desmoplastic ameloblastoma featuring basal cell ameloblastoma: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 99:160–164
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tomar, A. Plexiform Ameloblastoma with Acanthomatous Changes: A Rare Case Report. Indian J Otolaryngol Head Neck Surg (2024). https://doi.org/10.1007/s12070-024-05068-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12070-024-05068-x