Abstract
To evaluate the outcome and initial hurdles of transaxillary robotic thyroidectomy in the Indian subcontinent. A total of seven (n = 7) patients were operated from August 2016 to February 2017. Ultrasonography was used as a tool to decide the size of thyroid lobe and fine needle aspiration cytology for the type of lesion. All patients underwent ipsilateral brachial plexus nerve conduction studies preoperatively. Two arm positions were evaluated. The robot was docked at the contralateral side of the surgical field. Before discharge from hospital, all patients were given a questionnaire evaluate outcome. Set 1 was answered on the day of discharge and Set 2 at one-month follow up. The most common pathology in our case series was colloid goiter (n = 4) followed by follicular lesion (n = 3). The mean console time was 167 min, with initial two cases taking more than 200 min. The maximum and minimum length of the axillary tunnel was 16 and 27 cm respectively. There was no difference with regard to complication rate with either arm position. None of the patients developed brachial plexus injury and was confirmed by normal nerve conduction study done on postoperative day three. In our experience with transaxillary robotic thyroidectomy, the problems we faced in our population were unique considering the varied physical parameters. Use of malleable retractors comes handy in these situation and we recommend the use of these over the rigid ones. Though both the arm positions had similar outcomes, the one with sideways position was more favorable.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
From the time of Leonardo da Vinci to the current era, robot has evolved from our imagination to a practical reality. The continuous endeavors of physicists, engineers and surgeons have lead to the development of this novel technique of robotic surgery. Since the original description of thyroid surgery by Sir Theodor Kocher, the ultimate goal of this surgery has remained unchanged. However the incision has shifted from neck to the axilla, retro auricular area or oral cavity keeping in mind the cosmetics. In 2011, the first series on trans axillary thyroidectomy was presented by South Korean team of surgeons lead Chung and in North America by Kupersmith and Holsinger [1].
India is a land of unity in diversity. Not only our language and food varies from region to region, our physical characteristic also varies unlike that of Korean and North American population. Our center caters to patients from various regions of India, who present with varied physical profile that poses a unique surgical challenge.
Chung et al. described the initial trans axillary gasless thyroidectomy using “four arm and two incision” technique, whereas we used the “three arm single incision” technique [2, 3]. As this surgical technique was new to all operation room staffs, there were initial hiccups, but as we gained experience the procedure became a delight for both the chief surgeon and our team.
Materials and Methods
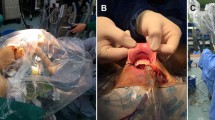
A total of seven (n = 7) patients were operated from August 2016 to February 2017. Inclusion criteria being benign thyroid lesion with unilateral lobe involvement with size was less than 5 cm. Ultrasonography was used as a tool to decide the size of thyroid lobe and fine needle aspiration cytology for the type of lesion. Exclusion criteria included patients with previous neck surgery or irradiation, any limb or shoulder joint injury or surgery and posteriorly located thyroid nodules. Informed consent about the nature of the surgery and what we hope to achieve at the end of it was explained thoroughly. All patients underwent ipsilateral brachial plexus nerve conduction studies preoperatively. Patients were taken up for surgery under general anesthesia after ensuring complete surgical safety check. All patients were intubated orally and a single shot intravenous antibiotic given at the time of induction, as per our departmental protocol. Supine position with neck extension was used and head stabilized with a head ring. For the first four cases, ipsilateral upper limb was positioned and fixed over the forehead. In the next three cases, ipsilateral arm was positioned to the side of the head in overhead abduction and elbow flexion, stabilized with a table-mounted armrest (Fig. 1). A 5-cm incision was marked over ipsilateral anterior axillary fold. Two parallel lines denoting the subcutaneous and subplatysmal tunnel were marked, with superior line joining upper end of axillary incision with hyoid and inferior line joining lower end of axillary incision to a point 1 cm above the suprasternal notch (Fig. 2). Surgical site was painted with 10% povidone iodine solution and sterile drapes were applied. Axillary incision was made and deepened to the deep fascia along the outer border of pectoralis major and subcutaneous tunnel was created up to the clavicle. Sharp dissection was done superior to the level of clavicle and subplatysmal tunnel was elevated till midline, identifying both the heads of ipsilateral sternocleidomastoid and strap muscles. The strap muscles were retracted using table mounted self-retaining malleable retractors passed through the tunnel and ipsilateral thyroid lobe was visualized (Fig. 3). The chief surgeon now switched over to the surgeons console. The robot was docked at the contralateral side of the surgical field. For right thyroid swelling the robot was docked to the left side and draped robotic arms were brought over the patient to enter the axillary tunnel and vice versa. On arm 2 (central arm), 0° and 30° endoscopes were used according to the need, while on arm 1 (cranial arm), Maryland forceps and on arm 3 (caudal arm), harmonic scalpel were mounted and interchanged as needed. Procedure started with identification of superior thyroid vessels that was cauterized and cut using harmonic scalpel (Fig. 4). Staying close to the gland we tried to preserve the superior laryngeal nerve. Next, the thyroid lobe was dissected from the Para-carotid tunnel and after cauterizing the middle thyroid vein dissection was continued towards the lower lobe. Here arm 1 and 3 were switched over. After identifying the parathyroid and inferior thyroid vessels, the lower pole was dissected taking care not to injure the recurrent laryngeal nerve. Here, we used neuropatties with thread tied to them for hemostasis and lifting the gland up from the bed. Dividing the isthmus and separating the gland from trachea and berry’s ligament was a critical step. Staying in midline and meticulous dissection using harmonic scalpel prevented injury to trachea (Fig. 5). At the end of the procedure, specimen was delivered through the axilla and hemostasis was achieved. Robotic arms were withdrawn and wound was closed over a negative suction drain. Vocal cord movements were checked during extubation using video laryngoscope. Suction drain was usually removed on postoperative day 2 and patient was discharged on day 3 after repeating nerve conduction studies. Before discharge from hospital, all patients were given a questionnaire to evaluate the postoperative comfort and the effect of procedure on the their social life, self confidence and general well being. The questionnaire consisted of 10 questions in their native languages and English, which were divided into two sets. Set 1 was answered on the day of discharge (Table 1) and Set 2 at one-month follow up (Table 2). Questions in set 1 were scored from 0 to 10 while responses in Set 2 were marked as yes, no or not sure.
Results
Out of the seven patients in our study there were two male and five female. All patients were in an age group of 20–50 years with a mean age of 36 ± 12 years. The most common pathology in our case series was colloid goiter (n = 4) followed by follicular lesion (n = 3). Six patients were having lesion on the right side while one had on the left. All patients underwent hemi thyroidectomy. The largest size of thyroid lobe operated was 6 cm and the smallest was 3 cm in the greatest dimension. The mean docking time was 21 ± 11 min while for the last two cases it was less then 10 min. The mean console time was 167 min, with initial two cases taking more than 200 min. The longest operative duration was 250 min and shortest was 135 min (Fig. 6). The mean blood loss in our series was 57 ml. In one of the case there was diffuse bleeding from the thyroid bed, which required the use of Surgicel ® (ETHICON, INC. © 2009) to achieve hemostasis. Only one patient in our study had ipsilateral vocal cord paresis noted on postoperative day one. The maximum and minimum length of the axillary tunnel was 16 and 27 cm respectively. The patient with the longest axillary tunnel had flap congestion postoperatively, which recovered by day 10 of follow up. None of the patients developed brachial plexus injury and was confirmed by normal nerve conduction study done on postoperative day 3. External approach to complete the procedure or to achieve the hemostasis was not required in any of the cases. All the patients answered a custom made questionnaire at discharge from hospital and at one-month follow up. Three out of seven patients complained of pain postoperatively, which was moderate (4–6). Only One patient with sideways arm position complained of shoulder joint discomfort that persisted even 1 month after surgery. However there were no restrictions of any movement at the joint. Five of the seven patients neither had any body image issues nor their social life activities were hampered. Four patients opted to chose the same procedure if they required it on the other side, while all seven patients were unanimous to recommend the procedure to other people. Three out of seven patients rated this procedure to be expensive but all patients rated the procedure to be highly satisfying (Table 3).
Discussion
Joseph Capek first used the term “robota” in Czechkoslavian literature meaning “serf” or “laborer” that eventually rose up against their human inventors [4]. The first use of robotics in human was in 1985 when PUMA 560 was used for Computed tomography guided brain biopsy with 0.05 mm accuracy. In the year 1994, AESOP became the first robotic camera holder approved by FDA. In 1999, Intuitive Surgical ® developed Da Vinci 2000, which had unique characteristics of binocular endoscopic 3D vision and instruments that closely mimicked human hand. In 2000 FDA approved it for laparoscopic procedures [5]. The Da Vinci surgical system consists of a console and a robot with four arms. The surgeon’s console provides a unique 3 D view and has control grips that allows for precise arm, wrist, and pincer movement [4]. The hand commands from the console are processed, tremors are filtered and data is transferred to the robotic arm, which provides the desired accurate movements with precision. The robotic system provide more degrees of freedom compared to endoscopic approaches and provide surgeons with more comfortable position to operate and also reduces the physiological tremors thus increasing the accuracy [6]. The human hand has seven degrees of freedom and with endoscope in hand this degree of freedom reduces to four, however the Da Vinci system has seven degrees of freedom, with six providing position at the level of surgical instruments [7]. Thus, the Da Vinci system is ergonomically better and has a better accuracy than human hand. Though this system was being used in other specialties from a long time, arrival of robotic system to the field of otolaryngology was delayed. It was in year 1995 that Brett et al. proposed the use of robotic drill in stapedotomy [6]. In year 2003, Federspil et al. described the robotic drilling of temporal bone and Haus et al. used the Da Vinci system for endoscopic neck surgery in porcine models [7]. In 1996, Gagner et al. described the endoscopic approaches to the neck. Earlier attempts at endoscopic thyroidectomy used an endoscope and several 5-mm trocars in the neck with insufflation, but an incision was still required to remove the specimen [8]. With time, extra cervical approaches to the thyroid gland started to appear in literature, with surgeons describing approaches to the thyroid gland via axillary approach, face-lift and even through the floor of mouth [9]. Out of all the approaches, the trans axillary approach popularized by South Koreans, gained the most appraisal. They first used the Da Vinci system to take out thyroid by trans axillary route without gas insufflation. The original trans axillary approach described by South Koreans used one axillary incision and a small anterior chest incision for the fourth arm, which grasps the gland and provides the counter traction. Wilson et al. who used the fourth arm just below the axillary incision through a separate chest port and modified this technique. However this technique became cumbersome in patients with high Basal Metabolic Index [2]. We used the technique described by Aliyev et al. where only three arms are used through the axillary incision [3]. Although Aliyev et al. did total thyroidectomy using 30° endoscope through the unilateral axillary incision, our patients had unilateral lesion and only underwent a hemi-thyroidectomy. Barring the first few cases, we could perform the procedures with the help of two instruments. The bedside assistant surgeon plays an important role in retracting the sternocleidomastoid and internal jugular vein using non-traumatic curved metallic malleable retractors. Care was taken while elevating subplatysmal flap over the sternocleidomastoid muscle to avoid inadvertent injury to internal jugular vein. Bleeding at this level can cause torrential bleeding mandating abandoning of the robotic procedure as securing hemostasis from the internal jugular vein via axillary approach is very difficult and requires head on approach. Therefore it is important to take a preoperative- consent for open surgery in all the patients undergoing trans axillary robotic surgery. We also used neuropatties tied with threads to push under the dissected thyroid gland so that we can lift the gland up and it helped in hemostasis and give us proper plane for dissection.
The mean diameter of tumor in study of Kang et al. was 0.80 ± 0.53 cm and in study of Landry et al. [10] maximum and minimum diameters was 4.7 and 2.1 cm. The maximum diameter of tumor we operated was 6 cm and smallest being 3 cm in the greatest dimension. The large variations in the tunnel length in our patients indicate the heterogeneity of the population we deal with and the reason why we recommend using malleable self-retaining retractors.
The majority of lesion in the study of Kang et al. was malignant while in Landry et al. and in our study all lesions were having benign pathology. Most of our cases were colloid goiter, as our centre caters to the population of Himalayan goiter belt. We did not include any patients with malignant thyroid lesion and neither did we encounter any histopathological surprises. We intend to operate low risk differentiated thyroid carcinoma as we gather more experience. The completeness of surgery and oncological outcomes have been reviewed by Lang et al. [11] and they have concluded that for low risk differentiated thyroid carcinoma robotic surgeries are unlikely to compromise any oncological outcome.
Trans axillary thyroidectomy poses the risk of brachial plexus injury due to arm position, thus in our case series we compared two arm positions. For the first four cases we used overhead arm position and for the last three cases we fixed the arm at 90° as used by Rodriguez et al. [12]. In their case series of 338 patients Kang et al. reported one case of brachial plexus injury and Landry et al. [13] in their case series of 14 patients reported 2 patients with brachial plexus injury. The most common postoperative complication was pain and limitation of movement of ipsilateral shoulder joint [14]. We did not encounter any brachial plexus injury in any of our patients with either arm position. In our experience, we found arm position used by Rodriguez et al.; to be more favorable in creating tunnel and applying the table mounted retractors. Brachial plexus injury is a devastating complication and it is recommended to have intraoperative nerve monitoring in all the case and there is always an option of facelift approach that does not put brachial plexus at risk [13]. Kim et al. [15] described a case of axillary web syndrome in one patient who underwent trans axillary robotic thyroidectomy.
In our case series we had only one patient with postoperative vocal cord paresis noted on day one, which improved at one month follow up with tapering dose of steroids. This patient had the longest tunnel length and had maximum intraoperative bleed that could possibly explain the paresis. None of our patients had hypocalcaemia, and this is attributed to the fact that we did hemi thyroidectomy and also it is easy to identify RLN and parathyroid gland with 10X magnification compared to open thyroidectomy [16]. In terms of patient satisfaction the procedure provided excellent cosmetics with minimal morbidity. All the patients including the ones with post operative shoulder discomfort and vocal cord paresis rated this procedure to be highly satisfying.
Despite so many advantages, economic feasibility remains the core issue as both acquiring and maintaining the equipment and in addition to it the cost of learning is high. The average cost of robotic thyroidectomy at our institution is around INR 35,000 ($540) as against INR 15,000 ($231) for the open procedure. Our institution being a non-profitable organization offers services at the least possible rate and further subsidizes for economically backward patients. Three patients who rated the procedure as expensive were from the lower economic class. The cost of robotic procedure were not completely waived off for these patients, in spite of these cost concerns patients preferred this technique to open procedure.
Conclusions
Every activity worth doing has a learning curve. As we gained experience our surgical time and comfort level improved which drives us to expand our limits. In our experience with transaxillary robotic thyroidectomy, the problems we faced in our population was unique considering the varied physical parameters. Use of malleable retractors comes handy in these situation and we recommend the use of these over the rigid ones. Though both the arm positions had similar outcomes, the one with sideways position was more favorable. In spite of the cost factors we believe that quality of health care should not be determined by the economic status.
References
Rabinovics N, Aidan P (2015) Robotic transaxillary thyroid surgery. Gland Surg 4(5):397–402
Wilson MN (2014) Modification of two-incision trans-axillary robotic thyroidectomy. J Robot Surg 8:325–327
Aliyev S, Taskin HE, Agcaoglu O, Aksoy E, Milas M, Siperstein A, Berber E (2013) Robotictransaxillary total thyroidectomy through a single axillary incision. Surgery 153(5):705–710
Hockstein NG, Gourin CG, Faust RA, Terris DJ (2007) A history of robots: from science fiction to surgical robots. J Robot Surg 1(2):113–118
Kalan S, Chauhan S, Coelho RF, Orvieto MA, Camacho IR, Palmer KJ, Patel VR (2010) History of robotic surgery. J Robot Surg 4(3):141–147
Kang SW, Lee SC, Lee SH, Lee KY, Jeong JJ, Lee YS, Nam KH, Chang HS, Chung WY, Park CS (2009) Robotic thyroid surgery using a gasless, transaxillary approach and the da Vinci S system: the operative outcomes of 338 consecutive patients. Surgery 146(6):1048–1055
Maan ZN, Gibbins N, Al-Jabri T, D’Souza AR (2012) The use of robotics in otolaryngology-head and neck surgery: a systematic review. Am J Otolaryngol 33(1):137–146
Duh QY (2011) Robot-assisted endoscopic thyroidectomy: has the time come to abandon neck incisions? Ann Surg 253(6):1067–1068
Kandil E, Abdelghani S, Noureldine SI, Friedlander P, Abdel Khalek M, Bellows CF, Slakey D (2012) Transaxillary gasless robotic thyroidectomy: a single surgeon’s experience in North America. Arch Otolaryngol Head Neck Surg 138(2):113–117
Landry CS, Grubbs EG, Morris GS, Turner NS, Holsinger FC, Lee JE, Perrier ND (2011) Robot assisted transaxillary surgery (RATS) for the removal of thyroid and parathyroid glands. Surgery 149(4):549–555
Lang BH, Wong CK, Tsang JS, Wong KP, Wan KY (2015) A systematic review and meta-analysis evaluating completeness and outcomes of robotic thyroidectomy. Laryngoscope 125(2):509–518
Rodriguez FN, Low RA, Singer JA, Bornstein AM, Bradford Doxey J, Hashimoto LA, Rassadi R, Dolce CJ, Hollingworth A, Hayes C 3rd, Shively CJ (2011) A new technique for robotic thyroidectomy: “the DaVinci gasless single-incision axillary approach”. J Robot Surg 5(3):157–162
Luginbuhl A, Schwartz DM, Sestokas AK, Cognetti D, Pribitkin E (2012) Detection of evolving injury to the brachial plexus during transaxillary robotic thyroidectomy. Laryngoscope 122(1):110–115
Alkan U, Zarchi O, Rabinovics N, Nachalon Y, Feinmesser R, Bachar G (2016) The cause of brachial plexopathy in robot-assisted transaxillary thyroidectomy—a neurophysiological investigation. Laryngoscope 126(9):2187–2193
Kim JH, Park JW, Gong HS (2014) Axillary web syndrome after transaxillary robotic thyroidectomy. J Robot Surg 8(3):281–283
Tae K, Song CM, Ji YB, Kim KR, Kim JY, Choi YY (2014) Comparison of surgical completeness between robotic total thyroidectomy versus open thyroidectomy. Laryngoscope 124(4):1042–1047
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest between authors and there was no funding agency/source involved in this study.
Informed consent
An informed consent was obtained before including the patients in the study.
Ethical approval
The Departmental Ethical Committee gave ethical clearance for the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gupta, A.K., Kumar, A., Singh, A. et al. Robot Assisted Trans Axillary Thyroidectomy: A Subcontinent Experience. Indian J Otolaryngol Head Neck Surg 70, 366–373 (2018). https://doi.org/10.1007/s12070-018-1357-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-018-1357-9