Abstract
Since the introduction of the single-port (SP) robotic system, SP trans-axillary robot-assisted thyroidectomy (SP-TART) has been performed. We aimed to evaluate the safety and surgical outcomes of SP-TART in a consecutive series of 300 cases. We analyzed 300 patients with thyroid disease who underwent SP-TART from October 2021 to May 2023 in St. Mary’s Hospital in Seoul, Korea. We analyzed the patients’ clinicopathological characteristics and perioperative outcomes according to surgical extent. Of the 300 cases analyzed, 250 patients underwent less than total thyroidectomy (LTT), 31 patients underwent total thyroidectomy (TT), and 19 patients underwent TT with modified radical neck dissection (TT c mRND). The mean operative times for LTT, TT, and for TT c mRND were 69.8 ± 23.6, 104.2 ± 30.7, and 223.7 ± 72.4 min, respectively. Complications, including postoperative bleeding, transient hypoparathyroidism, and vocal cord palsy, were observed in nine, six, and six LTT, TT, and TT c mRND cases. The SP-TART method is a safe and feasible surgical option with a short operative time, good surgical outcome, and excellent cosmetic results.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Thyroid surgery is the established treatment for thyroid cancer or suspected nodules [1], which has been continually advancing over time. Conventional open thyroidectomy (COT), which is the standard approach of thyroid surgery, is performed by making an incision through the anterior portion of the neck. For this reason, the wound scar is easily visible. Since the majority of thyroid cancer patients are women in their 30s and 60s [2], not only is hypertrophic or keloid scarring a concern, but also the surgical wound itself is an important problem to young female patients [3].
To minimize surgical incisions, various types of minimally invasive surgeries have been introduced [4]. With advancements in endoscopy and robotic systems, these minimally invasive techniques, including trans-axillary, bilateral axillary breast, retro-auricular, and transoral approaches, have also been gaining popularity in thyroid surgery [5]. These surgical methods are designed to eliminate the need for incisions in the anterior neck and minimize incision length, ensuring better cosmetic outcomes [6].
Trans-axillary robotic surgery, which is among the minimally invasive surgeries, has favorable surgical outcomes and feasibility [7, 8]. The da Vinci single-port (SP) ® Surgical System (Intuitive Surgical, Sunnyvale, CA, USA) is the latest version of robotic system. The SP system comprises one camera and three robotic arms that enter through a cannula in one port, and this approach allows access narrower and deeper portions as compared to previous robotic systems. Therefore, it allows the operator to easily perform thyroidectomy and has the advantage of a shorter incision length.
However, research on the safety and surgical outcomes of SP trans-axillary robotic thyroid surgery (SP-TART) is lacking. Therefore, in this study, we aimed to evaluate the safety and surgical outcomes of SP-TART in a consecutive series of 300 cases.
Materials and methods
Patients
This retrospective study analyzed a total of 300 consecutive patients with thyroid disease who underwent SP-TART at St. Mary’s Hospital in Seoul, Korea from October 2021 to May 2023. The medical charts and pathology reports of all patients were reviewed. Preoperatively, all patients underwent ultrasonography of the thyroid; in case of thyroid cancer or if needed, an computed tomography scan was performed to confirm the clinical stage and surgical extent. The extent of surgery was decided based on the American Thyroid Association 2015 guidelines [1]. In terms of surgical extent, less than total thyroidectomy (LTT) includes isthmusectomy and lobectomy. LTT was performed when preoperative evaluation revealed no evidence of metastasis in the central or lateral lymph node (LN), no gross extrathyroidal extension (ETE), and a mass limited to a unilateral lobe. When lateral neck LN metastasis was proven by fine-needle aspiration cytology, mRND was performed. Vocal cord palsy (VCP) was confirmed by postoperative stroboscopy and otolaryngology consultation. Transient hypoparathyroidism is defined as a clinicopathological state requiring exogenous calcium supplements, which subsequently normalize within 6 months postoperatively [9]. The pathologic stage was classified according to the 8th edition of the American Joint Committee on Cancer/Union for International Cancer Control (AJCC/UICC) tumor-node-metastasis (TNM) staging system [10].
Surgical procedure of less than total thyroidectomy
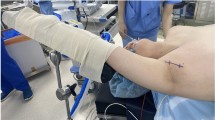
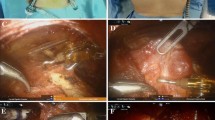
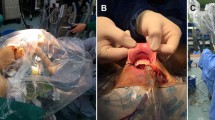
Under general anesthesia, the patient is placed in a supine position with a pillow placed under the shoulders to keep the neck slightly extended. The arm on the side of the lesion above the head was elevated (Fig. 1A). After making a 3.5–4 cm skin incision in the axilla, the pectoralis major muscle can be dissected along the anterior fascia, extending from the axilla to the clavicle. After exposure of the sternocleidomastoid (SCM) muscle, the avascular space between the sternal and clavicular head can be accessed, and the omohyoid muscle is identified and drawn. Dissecting beneath the strap muscle and lifting it upward are carefully done to prevent injury from the internal jugular vein (IJV). After exposing the ipsilateral thyroid lobe and lower part of the contralateral thyroid lobe, a rectractor blade is inserted through the skin incision and raised to maintain a working space (Fig. 2A).
(A) Patient positioning of LTT, TT: The arm on the side of the lesion above the head was elevated. (B) Patient positioning of mRND: The arm on the side where the mRND is is extended outward parallel. (C) Re-docking for level II dissection: external retractor blade is rotated toward the patient’s submandibular gland
The robotic system is approached from the patient’s contralateral side, and the central column of the robot is aligned in a straight direction with the retractor blade that lifts the flap. After fixing the cannula to the skin incision (Fig. 2B), the camera is placed at the bottom, the Maryland dissecting forceps are placed on both sides, and the Cadiere forceps on top (Fig. 2C). The operator uses Cadiere forceps to pull the thyroid in the caudal direction of the patient, and then uses Maryland forceps to dissect the upper pole of the thyroid. At this stage, the superior thyroid artery should be ligated by attaching it to the thyroid to minimize damage to the external branch of the superior laryngeal nerve. After confirming the location of the parathyroid glands, they are preserved, and Cadiere forceps were used to pull the thyroid superiorly, exposing the course of the recurrent laryngeal nerve (RLN). Following the excision of the adjacent soft tissue surrounding the thyroid gland to avoid damage to the RLN, dissection and extraction of the thyroid along the trachea are then performed. The surgical specimen is taken out through the skin incision by an assistant using laparoscopic forceps. In all cases, we performed neuromonitoring to ensure RLN preservation. The closed suction drain was inserted through the skin incision, and the wound is closed.
Surgical procedure of total thyroidectomy
The skin incision is the same as that for LTT, with a length of 3.5–4 cm, and the tumor location and the patient’s handedness are considered when deciding which side to approach. The flap creation method is the same as that for LTT, but the flap extent is extended beyond the isthmus to fully expose the contralateral thyroid lobe.
Thyroidectomy is performed from the ipsilateral thyroid lobe and the method is the same as that for LTT. After removing the ipsilateral thyroid specimen, dissection is started from the isthmic portion, followed by the contralateral thyroid upper pole. In contralateral thyroidectomy, the upper pole is mobilized first, followed by the lower pole, and dissection is performed in a medial-to-lateral direction through a subcapsular plane. Total thyroidectomy (TT) is then performed, ensuring that the course of the RLN and the position of the parathyroid glands are checked. A closed suction drain is placed and the wound is closed.
Surgical procedure of total thyroidectomy c modified radical neck dissection
While under general anesthesia, the patient is placed in a supine position with a cushion placed under their shoulders, and their neck is slightly extended. Unlike the position during LTT or TT, the arm on the side where the modified radical neck dissection (mRND) will be performed is extended outward parallel to the operating bed (Fig. 1B), and the patient’s head is turned to the opposite side to maximize exposure of the axilla and lateral neck [11]. The skin incision is made 7–8 cm along the anterior axillary fold. For patients undergoing bilateral mRND, the approach was made from both axilla. The mRND flap is dissected medially to the anterior boundary of the SCM muscle, inferiorly to the substernal notch, superiorly to the submandibular gland, and laterally to expose the anterior border of the trapezius muscle.
After TT, the mRND of the lateral neck is performed; the method is the same as the open conventional procedure, but docking is performed in two stages. Initially, LN dissection in levels III, IV, and V is carried out while the robot is docked in the same position as during the thyroidectomy. The LN dissection begins with levels III and IV, targeting the anterior and posterior portions of the IJV until the common carotid artery and vagus nerves are exposed. Once LN dissection is completed for each compartment, the assistant removes the LN specimen through a skin incision using endoscopic forceps. The inferior portion of the IJV is dissected until it reaches the subclavian vein. Continuing the dissection in a lateral direction along the subclavian vein, caution is needed to avoid damaging the transverse cervical artery and phrenic nerve. Subsequently, a level V dissection until the anterior border of the trapezius muscle is performed.
To initiate the level II dissection, the external retractor blade is removed and rotated toward the patient’s submandibular gland (Fig. 1C). It is then repositioned and re-docked to ensure sufficient visibility for level II dissection. A level II dissection is conducted along the anterior surface of the carotid artery and IJV, until reaching the submandibular gland, and posterior belly of the digastric muscle. Finally, a drain is inserted, and the wound is closed.
The details of all surgical procedures and techniques for SP-TART have been described in our previous study [11, 12].
Results
Baseline clinicopathological characteristics of the study patients
Table 1 shows the patients’ baseline clinicopathological characteristics. The median age was 42.87 ± 12.4 (range, 17–73) years, and the median body mass index (BMI) was 23.41 ± 3.61 (range, 15.62–40.28) kg/m2. Of the 300 cases analyzed, 262 (87.3%) were female and 38 (12.7%) were male. Altogether, 250 (83.4%) cases underwent LTT, which included lobectomy, isthmusectomy, and subtotal thyroidectomy. Additionally, 31 (10.4%) and 19 (6.4%) cases underwent TT and TT c mRND, respectively. The most common pathologic subtype was papillary thyroid cancer (PTC) [257 (85.7%) cases] and the second was follicular adenoma [19 (6.3%) cases]. The pathologic tumor size was measured based on the largest tumor when the multifocal tumors were observed, with a mean size of 1.28 ± 1.21 (range, 0.1–7.5) cm. Pathology confirmed thyroiditis in 116 (38.7%) cases.
Perioperative outcomes
Perioperative outcomes according to the surgical extent are summarized in Table 2. Three cases in the TT c mRND group underwent bilateral mRND. The mean operative times for LTT, TT, and TT c mRND were 69.8 ± 23.6, 104.2 ± 30.7, and 223.7 ± 72.4 min, respectively. The docking times were 1.9 ± 0.8, 2.6 ± 0.7, and 5.3 ± 2.0 min for LTT, TT, and TT c mRND, respectively. The measured blood loss in LTT, TT, and TT c mRND was 16.2 ± 26.8, 22.8 ± 36.4, and 39.5 ± 45.7 mL. The hospital stay was 2.0 ± 0.3, 2.1 ± 0.3, and 3.1 ± 0.8 days for the LTT, TT, and TT c mRND groups, respectively.
Postoperative complications
Table 3 shows the postoperative complications according to surgical extent. In the LTT group, nine (3.6%) cases had complications, including one (0.4%) case of chyle leak, two (0.8%) cases of postoperative bleeding, two (0.8%) cases of surgical site infection, and four (1.6%) cases of VCP. One LTT case required re-operation due to postoperative flap bleeding. In the TT group, six patients (18.2%) had complications, including five (15.2%) transient hypoparathyroidism and one (3.0%) VCP cases. In the TT c mRND group, there were six (31.6%) complications. One patient developed chyle leakage and transient hypoparathyroidism simultaneously, and all the others had transient hypoparathyroidism.
Clinicopathological characteristics of the patients with cancer
Table 4 summarizes the clinicopathological characteristics of the patients with cancer. Among the 300 cases, 262 (87.3%) were cancer. 214 (82.0%), 28 (10.7%), and 19 (7.3%) underwent LTT, TT, and TT c mRND, respectively. Regarding the pathologic subtype, PTC, follicular thyroid carcinoma (FTC), and poorly differentiated thyroid carcinoma were observed in 257 (98.1%), 3 (1.1%), and 2 (0.8%) cases, respectively. 175 (58.3%) cases had ETE, of which 18 (6.9%) had gross ETE. The mean harvested LN and positive LN counts were 8.43 ± 12.12 (range, 0–108) and 2.75 ± 5.39 (range, 0–44), respectively. The majority of patients (n = 228, 87.0%) had T1 stage disease, followed by 16 (6.1%) patients with T3b stage. For the N stage, the majority of cases had N0 (128 cases, 48.9%) and N1a (114 cases, 43.5%) diseases. According to the 8th version of the AJCC/UICC TNM stage, 240 (91.6%) and 22 (8.4%) patients had pathologic stage I and II diseases, respectively.
Discussion
During the initial phases of thyroid surgery, the main goal was to achieve complete excision of the thyroid tumor while ensuring RLN and parathyroid gland preservation. Nevertheless, with advancements in anatomical knowledge and surgical techniques, the focus has expanded to include the patients’ postoperative quality of life. Notably, the cosmetic aspect of postoperative scar formation has emerged as a significant concern, especially among thyroid cancer patients [3]. This concern is particularly relevant given the high survival rate associated with thyroid cancer and its relatively higher incidence among female patients [2].
COT is performed through the anterior neck, resulting in a highly visible surgical site. Surgical scarring has been a significant concern, prompting the introduction of minimally invasive surgical methods. The trans-axillary approach, first introduced by Ikeda et al. in 1999, is widely practiced and preferred [13]. This approach offers several advantages, including easy access to the upper and lower poles of the thyroid gland and enhanced identification of the RLN and parathyroid glands [14, 15]. Moreover, the skin incision made through the armpit area contributes to improved patient satisfaction, as the scar remains inconspicuous when the patient adducts their arm [16]. Furthermore, compared to COT, the trans-axillary approach involves lesser dissection of subcutaneous tissues in the anterior region. As a result, patients experienced less pain, numbness, and dysphagia [14].
However, the effectiveness of endoscopic surgery can be limited owing to the assistant operator’s ability to handle the camera. Moreover, achieving delicate maneuvering in curved areas can be challenging due to the use of straight instruments [17, 18]. To overcome these limitations, the da Vinci robotic system was introduced, featuring a 3D camera, articulated arm, and stabilized hand motion [4]. The first trans-axillary robotic surgery in the thyroid field was performed by Chung et al. in 2007 [18]. Subsequently, there has been a increase in the number of trans-axillary robotic surgical cases, with evidence demonstrating superior postoperative recovery rates for pain and paresthesia as compared to COT [19]. Robotic surgery is particularly superior in terms of cosmetic aspects, and it has been confirmed that it has similar or better results compared to COT in terms of postoperative voice changes and dysphagia [6, 8].
The SP system is the newest version of da Vinci systems, equipped with three instruments, each with two joints, and a three-dimensional high definition camera with articulation that facilitates visibility and control in narrow surgical spaces. Its enhanced operability in narrower and deeper flaps, as compared to the previous Xi system, allows for a reduction in the size of the skin incision, and the robotic arm experiences less resistance during the operation. Moreover, the SP system has the advantage of easy docking and de-docking [20], which is particularly advantageous during mRND where docking is performed in two stages. This results in a shortened docking time and added convenience during surgery. In this study, the docking times were 1.9 ± 0.8, 2.6 ± 0.7, and 5.3 ± 2.0 min for LTT, TT, and TT c mRND, respectively. It is much shorter than the docking time of a previous robot system (Si or Xi) [21,22,23].
In our study, the operative times were 69.8 ± 23.6, 104.2 ± 30.7, and 223.7 ± 72.4 min for LTT, TT, and TT c mRND, respectively. Each operative time is comparable with those reported in previous studies on robotic thyroidectomy, indicating that the trans-axillary approach is also efficient in terms of operative time [6, 24, 25]. Moreover, most of the patients were discharged from the hospital on postoperative day (POD) 2 for LTT or TT and POD 3 for TT c mRND. This implies that our surgical procedure does not lead to longer hospital stays as compared to other types of minimally invasive surgeries [6].
Altogether, 200 patients who underwent LTT had a mean harvested LN count of 4.95 ± 3.42 (range: 0–21), with a mean positive LN count of 1.40 ± 2.13 (range: 0–15). In TT, LN dissection was performed in 28 cases, resulting in mean harvested LN and positive LN counts of 9.14 ± 5.16 (range: 1–26) and 2.57 ± 3.76 (range: 0–12), respectively. mRND was performed in 19 patients, resulting in mean harvested LN and positive LN counts of 43.95 ± 19.29 (range: 23–108) and 17.11 ± 9.37 (range: 6–44), respectively. The LN yield serves as an indicator not only for evaluating the completion of neck dissection but also as a factor in assessing the risk of thyroid cancer [26]. Particularly, several studies have revealed an association between increased central or lateral LN yield and reduced recurrence of PTC [27,28,29]. Our results show that the number of harvested LN is consistent with those reported in previous studies [7, 30, 31], indicating that LN dissection using SP-TART is efficient. Reaching the deepest region in level IV dissection might be challenging due to the prominence of the clavicle, particularly in right-sided mRND using the Xi system [32]. However, the SP system minimizes this difficulty by utilizing three multi-jointed robotic arms [33].
In this study, the patients’ BMI ranged from 15.62 to 40.28 kg/m2. For patients with lower BMI, the skin’s thinness has a potential risk for skin injury, particularly when traversing the clavicular region. Conversely, in obese patients, challenges related to poor visibility were encountered during flap creation [34]. Fatty tissues are more susceptible to bleeding and challenging to handle, resulting in the need for more time to control bleeding and perform dissection. Additionally, excessive fatty tissues can also make it difficult to identify the platysma muscle when approaching the thyroid along the subplatysmal plane [35]. This is particularly problematic in young men with a good physique, as the distance from the skin incision to the anterior aspect may be longer, and the muscle tension may make it difficult to perform retraction during flap creation. This can serve as factor contributing to prolonged operative time or an increased bleeding risk [36]. In this study, one case underwent re-operation the day after surgery due to flap bleeding. The patient was a young man with a BMI of 25.9 kg/m2, and the bleeding focus was lower portion of the pectoralis major muscle. There were no case of conversion to open surgery.
The incidence of transient VCP was reported to be 3–8%, whereas permanent palsy occurs in approximately 0.3–3% of cases [37,38,39,40]. In this study, there were four cases of VCP as a complication of LTT surgery, and two of these cases had tumor sizes of 3.0 or 5.3 cm. Owing to the tumor size, it was difficult to identify the RLN course. In the other two cases, RLN invasion was present and RLN shaving had to be performed. In the TT group, there was one case of VCP, in which a patient with both thyroid cancer underwent a Lt. axillary approach, resulting in Rt. VCP. The dissection of the contralateral thyroid lobe and RLN in SP-TART with a unilateral approach is acknowledged as a challenging procedure [4]. Owing to the nature of trans-axillary surgery, it is challenging to identify the RLN course contralateral to the incision.
The incidence of hypoparathyroidism after thyroidectomy varies, with reports ranging from 1.5 to 22.8% for transient hypoparathyroidism and from 0 to 17.4% for permanent hypoparathyroidism [41,42,43,44]. In this study, transient hypoparathyroidism occurred in five (15.2%) TT and three (31.6%) TT c mRND cases, but no case of permanent hypoparathyroidism was found. In the TT c mRND surgery of this study, the number of transient hypoparathyroidism cases was relatively higher than that of a previous study [45]. This may be attributed to the challenge of visualizing the lateral portion on the contralateral side of the thyroid, leading to difficulties in preserving the parathyroid glands. Nevertheless, it is essential to highlight that no case of permanent hypoparathyroidism was observed in this study. This observation could be associated with the benefits of using a lateral view for the operative field and the articulation of the SP system robotic arm, allowing for delicate maneuvers that may have assisted in the preservation of the ipsilateral side parathyroid glands.
The SP system offers several advantages, including ease of docking, as compared to previous robotic systems, requiring only the movement of a single cannula instead of multiple robotic arms and a trocar [20]. The SP-TART provides a surgical view similar to that of a COT with a lateral view, making it easier for operators to adapt to the field [11]. In trans-axillary surgery, the SP-TART allows for a relatively small incision, ranging from 3.5 to 4 cm for LTT or TT procedures, and 7–8 cm for mRND, without compromising cosmetic satisfaction. Additionally, the SP system requires narrower flap dissection, reducing the risk of sensory nerve damage and minimizing paresthesia in the supra- and infra-clavicular regions [5].
The present study has some limitations. First, it is a retrospective study. Second, there is no data available regarding patient satisfaction and pain. We plan to conduct a satisfaction survey in the future. Third, since robotic surgery is not covered by insurance in South Korea, some patients were unable to undergo surgery due to cost problems. As a result, there might be differences in the socio-economic status between the groups of patients who underwent robotic surgery and those who underwent COT, leading to a selection bias. Lastly, the follow-up period was relatively short. Therefore, further research is needed to investigate the surgical outcomes through long-term follow-up.
Conclusions
Among the 300 cases of SP-TART performed, favorable operative time and hospital stay duration, as well as a relatively low complication rate were observed, indicating positive surgical outcomes. These results suggest that SP-TART is a safe and feasible procedure. However, further prospective studies are needed to substantiate the surgical outcomes and technical stability of SP-TART.
Data availability statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, Pacini F, Randolph GW, Sawka AM, Schlumberger M, Schuff KG (2016) 2015 American thyroid association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American thyroid association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26(1):1–133
LeClair K, Bell KJ, Furuya-Kanamori L, Doi SA, Francis DO, Davies L (2021) Evaluation of gender inequity in thyroid cancer diagnosis: differences by sex in US thyroid cancer incidence compared with a meta-analysis of subclinical thyroid cancer rates at autopsy. JAMA Int Med 181(10):1351–1358
Choi Y, Lee JH, Kim YH, Lee YS, Chang HS, Park CS, Roh MR (2014) Impact of postthyroidectomy scar on the quality of life of thyroid cancer patients. Ann Dermatol 26(6):693–699
Tae K, Ji YB, Song CM, Ryu J (2019) Robotic and endoscopic thyroid surgery: evolution and advances. Clin Exp Otorhinolaryngol 12(1):1
Chang EH, Kim HY, Koh YW, Chung WY (2017) Overview of robotic thyroidectomy. Gland Surg 6(3):218
de Vries LH, Aykan D, Lodewijk L, Damen JA, Borel Rinkes IH, Vriens MR (2021) Outcomes of minimally invasive thyroid surgery—a systematic review and meta-analysis. Front Endocrinol 12:719397
Pan JH, Zhou H, Zhao XX, Ding H, Wei L, Qin L, Pan YL (2017) Robotic thyroidectomy versus conventional open thyroidectomy for thyroid cancer: a systematic review and meta-analysis. Surg Endosc 31(10):3985–4001
Sun GH, Peress L, Pynnonen MA (2014) Systematic review and meta-analysis of robotic vs conventional thyroidectomy approaches for thyroid disease. Otolaryngol Head Neck Surg 150(4):520–32
Bhettani MK, Rehman M, Ahmed M, Altaf HN, Choudry UK, Khan KH (2019) Role of pre-operative vitamin D supplementation to reduce post-thyroidectomy hypocalcemia; Cohort study. Int J Surg (London, England) 71:85–90
Amin MB, Edge S, Greene F, Byrd DR, Brookland RK, Washington MK, Gershenwald JE, Compton CC, Hess KR, Sullivan DC, Jessup JM, Brierley JD, Gaspar LE, Schilsky RL, Balch CM, Winchester DP, Asare EA, Madera M, Gress DM, Meyer LR (2017) AJCC cancer staging manual, 8th edn. Springer, New York
Kang IK, Park J, Bae JS, Kim JS, Kim K (2022) Safety and feasibility of single-port trans-axillary robotic thyroidectomy: experience through consecutive 100 cases. Medicina (Kaunas, Lithuania) 58(10):1485
Park J, Kang LK, Kim K, Bae JS, Kim JS (2023) The learning curve for single-port transaxillary robotic thyroidectomy (SP-TART): experience through initial 50 cases of lobectomy. Updates Surg 75(3):691–700
Ikeda Y, Takami H, Sasaki Y, Kan S, Niimi M (2000) Endoscopic neck surgery by the axillary approach. J Am College Surg 191(3):336–340
Kang SW, Jeong JJ, Yun JS, Sung TY, Lee SC, Lee YS, Nam KH, Chang HS, Chung WY, Park CS (2009) Gasless endoscopic thyroidectomy using trans-axillary approach; surgical outcome of 581 patients. Endocr J 56(3):361–369
Lombardi CP, Raffaelli M, Princi P, De Crea C, Bellantone R (2006) Video-assisted thyroidectomy: report on the experience of a single center in more than four hundred cases. World J Surg 30(5):794–800
Li T, Zhang Z, Chen W, Yu S, Sun B, Deng X, Ge J, Wei Z, Lei S, Li G (2022) Comparison of quality of life and cosmetic result between open and transaxillary endoscopic thyroid lobectomy for papillary thyroid microcarcinoma survivors: a single-center prospective cohort study. Cancer Med 11(22):4146–4156
Lobe TE, Wright SK, Irish MS (2005) Novel uses of surgical robotics in head and neck surgery. J Laparoendosc Adv Surg Tech A 15(6):647–652
Kang SW, Jeong JJ, Yun JS, Sung TY, Lee SC, Lee YS, Nam KH, Chang HS, Chung WY, Park CS (2009) Robot-assisted endoscopic surgery for thyroid cancer: experience with the first 100 patients. Surg Endosc 23(11):2399–2406
Lee J, Nah KY, Kim RM, Ahn YH, Soh EY, Chung WY (2010) Differences in postoperative outcomes, function, and cosmesis: open versus robotic thyroidectomy. Surg Endosc 24(12):3186–3194
Kim JK, Choi SH, Choi SM, Choi HR, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2022) Single-port transaxillary robotic thyroidectomy (START): 200-cases with two-step retraction method. Surg Endosc 36(4):2688–2696
Chang YW, Lee HY, Kim WY, Kim HY, Lee JB, Son GS (2021) Detailed comparison of the da Vinci Xi and S surgical systems for transaxillary thyroidectomy. Medicine 100(3)
Piccoli M, Mullineris B, Gozzo D, Colli G, Pecchini F, Nigro C, Rochira V (2019) Evolution strategies in transaxillary robotic thyroidectomy: considerations on the first 449 cases performed. J Laparoendosc Adv Surg Tech A 29(4):433–440
Ban EJ, Yoo JY, Kim WW, Son HY, Park S, Lee SH, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2014) Surgical complications after robotic thyroidectomy for thyroid carcinoma: a single center experience with 3,000 patients. Surg Endosc 28(9):2555–2563
Lee J, Kwon IS, Bae EH, Chung WY (2013) Comparative analysis of oncological outcomes and quality of life after robotic versus conventional open thyroidectomy with modified radical neck dissection in patients with papillary thyroid carcinoma and lateral neck node metastases. J Clin Endocrinol Metab 98(7):2701–2708
Noureldine SI, Jackson NR, Tufano RP, Kandil E (2013) A comparative North American experience of robotic thyroidectomy in a thyroid cancer population. Langenbeck’s Arch Surg 398(8):1069–1074
Ji KS, Oyekunle TO, Thomas SM, Scheri R, Stang M, Roman SA, Sosa JA (2019) Adequacy of lymph node yield for papillary thyroid cancer: an analysis of 23,131 patients. J Surg Res 244:566–573
Beal SH, Chen SL, Schneider PD, Martinez SR (2010) An evaluation of lymph node yield and lymph node ratio in well-differentiated thyroid carcinoma. Am Surg 76(1):28–32
Yu ST, Ge JN, Sun BH, Wei ZG, Xiao ZZ, Zhang ZC, Chen WS, Li TT, Lei ST (2021) Lymph node yield in the initial central neck dissection (CND) associated with the risk of recurrence in papillary thyroid cancer: a reoperative CND cohort study. Oral Oncol 123:105567
Issa K, Stevens MN, Sun Y, Thomas S, Collins A, Cohen J, Esclamado RM, Rocke DJ (2022) A retrospective study of lymph node yield in lateral neck dissection for papillary thyroid carcinoma. Ear Nose Throat J 101(7):456–462
Chung EJ, Cho SJ, Park MW, Rho YS (2019) The impact of the number of harvested central lymph nodes on the lymph node ratio. Auris Nasus Larynx 46(2):267–271
Feng JW, Yang XH, Wu BQ, Sun DL, Jiang Y, Qu Z (2019) Predictive factors for central lymph node and lateral cervical lymph node metastases in papillary thyroid carcinoma. Clin Transl Oncol 21(11):1483–1491
Kang SW, Kim MJ, Chung WY (2018) Gasless, transaxillary robotic neck dissection: the technique and evidence. Gland Surg 7(5):466
Ho J, Kim D, Lee JE, Kim JK, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2023) Single-port transaxillary robotic modified radical neck dissection (STAR-RND): initial experiences. Laryngosc 133(3):709–7014
Holsinger FC, Chung WY (2014) Robotic thyroidectomy. Otolaryngol Clin N Am 47(3):373–378
Yap Z, Kim WW, Kang SW, Lee CR, Lee J, Jeong JJ, Nam KH, Chung WY (2019) Impact of body mass index on robotic transaxillary thyroidectomy. Sci Rep 9(1):8955
Stevenson CE, Gardner DF, Grover AC (2012) Patient factors affecting operative times for single-incision trans-axillary robotic-assisted (STAR) thyroid lobectomy: does size matter? Ann Surg Oncol 19(5):1460–1465
Steurer M, Passler C, Denk DM, Schneider B, Niederle B, Bigenzahn W (2002) Advantages of recurrent laryngeal nerve identification in thyroidectomy and parathyroidectomy and the importance of preoperative and postoperative laryngoscopic examination in more than 1000 nerves at risk. Laryngosc 112(1):124–133
Jeannon JP, Orabi AA, Bruch GA, Abdalsalam HA, Simo R (2009) Diagnosis of recurrent laryngeal nerve palsy after thyroidectomy: a systematic review. Int J Clin Practic 63(4):624–629
Lo CY, Kwok KF, Yuen PW (2000) A prospective evaluation of recurrent laryngeal nerve paralysis during thyroidectomy. Arch Surg (Chicago, IL: 1960) 135(2):204–207
Hayward NJ, Grodski S, Yeung M, Johnson WR, Serpell J (2013) Recurrent laryngeal nerve injury in thyroid surgery: a review. ANZ J Surg 83(1–2):15–21
Merchavy S, Marom T, Forest VI, Hier M, Mlynarek A, McHugh T, Payne R (2015) Comparison of the incidence of postoperative hypocalcemia following total thyroidectomy vs completion thyroidectomy. Otolaryngol Head Neck Surg 152(1):53–56
Bergenfelz A, Jansson S, Kristoffersson A, Mårtensson H, Reihnér E, Wallin G, Lausen I (2008) Complications to thyroid surgery: results as reported in a database from a multicenter audit comprising 3,660 patients. Langenbeck’s Arch Surg 393(5):667–673
Hundahl SA, Cady B, Cunningham MP, Mazzaferri E, McKee RF, Rosai J, Shah JP, Fremgen AM, Stewart AK, Hölzer S, US and German Thyroid Cancer Study Group (2000) Initial results from a prospective cohort study of 5583 cases of thyroid carcinoma treated in the united states during 1996. U.S. and German Thyroid Cancer Study Group. An American College of Surgeons Commission on Cancer Patient Care Evaluation study. Cancer 89(1):202–217
Jensen PV, Jelstrup SM, Homøe P (2015) Long-term outcomes after total thyroidectomy. Dan Med J 62(11):A5156
Rocke DJ, Mulder H, Cyr D, Kahmke R, Lee WT, Puscas L, Schulz K, Witsell DL (2020) The effect of lateral neck dissection on complication rate for total thyroidectomy. Am J Otolaryngol 41(3):102421
Acknowledgements
The authors wish to acknowledge the financial support of the Catholic Medical Center Research Foundation made in the program year of 2022.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by SA and KSK The first draft of the manuscript was written by SA and all authors commented on previous versions of the manuscript and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of Seoul St. Mary’s Hospital, the Catholic University of Korea (approval No.: KC23RASI0236, Date: April 21, 2023).
Consent to participate & consent to publish
This study waived the requirement for informed consent due to the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
An, S., Park, J., Kim, K. et al. Safety and surgical outcomes of single-port trans-axillary robot-assisted thyroidectomy: Experience from a consecutive series of 300 patients. J Robotic Surg 18, 13 (2024). https://doi.org/10.1007/s11701-023-01810-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-023-01810-9