Abstract
Associative studies on a range of neurodevelopmental disorders have identified relationships between behavioral deficits and immune system function. The BTBR T+ Itpr3tf/J (BTBR) mouse strain displays aberrant characteristics in its social behavior and immune responses, providing a significant opportunity to examine the relationship between behavior and the immune system. This study investigated the influence of adenosine A2A receptor activity on C-C and C-X-C chemokine receptors involved in autism in the BTBR mouse model. A2A receptors have previously been targeted in clinical trials by potential therapeutics with neuroprotective, immunomodulatory, and analgesic properties. In this study, we examined the effects of A2A receptor antagonist SCH5826 (SCH) and A2A receptor agonist CGS21680 (CGS) on C-C and C-X-C chemokine receptors (CCR3, CCR4, CCR5, CCR6, CCR7, CXCR3, CXCR4, and CXCR5) on splenic CD8+ T cells in the BTBR autistic mouse model. We also assessed the C-C and C-X-C chemokine receptors mRNA levels in brain tissue. Our results showed that CCR3+, CCR4+, CCR5+, CCR6+, CCR7+, CXCR3+, CXCR4+, and CXCR5+ production in splenic CD8+ T cells decreased significantly in BTBR-CGS-treated mice in comparison with that in BTBR control and BTBR-SCH-treated mice. In addition, RT-PCR analysis revealed decreased gene expression levels for C-C and C-X-C chemokine receptors in the brain tissue of BTBR-CGS-treated mice, whereas these levels were significantly increased in BTBR control and BTBR-SCH-treated mice. Our results suggest that treating BTBR mice with CGS decreases C-C and C-X-C chemokine receptor signaling and might therefore provide a unique avenue for developing future therapies for autism and neuroimmunological disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Autism is a neurodevelopmental disorder characterized by stereotypical behaviors, including repetitive actions and impaired expressive communication that have been folded into the broader classification of autism spectrum disorders (ASD) [1]. An imbalance of immune cells associated with an autoimmune disorder plays a role in the pathogenesis of autism [2]. Several immune system abnormalities have been defined in the development of ASD as well as in some of the associated pathophysiologies [3]. A broad spectrum of immune abnormalities, including aberrant mucosal immunity, has been reported for autistic subjects [4]. Pro-inflammatory mediators such as cytokines, chemokines, and their receptors are associated with the progression and development of autism [5]. Evidence of immune dysfunction has been perceived in many individuals with autism, with marked activation of microglia, as well as increased pro-inflammatory cytokine and chemokine production [6]. Recently, we have observed that autism is also associated with the dysregulation of Th1, Th2, Th17, and T regulatory cell-related transcription factor signaling [7]. However, the exact cellular and molecular mechanisms of action underlying autistic disorder remain the subject of further detailed investigations.
Chemokine receptors play an essential role in inflammation, angiogenesis, and leukocyte trafficking in brain development [8, 9]. They are key potential therapeutic targets in many autoimmune and neurological disorders [9] and have been associated with numerous behavioral impairments in individuals diagnosed with autism [10, 11]. Various studies have confirmed that chemokine receptors are part of the altered immune environment noted in autism [12]. Chemokine receptors have been identified as functional mediators of neuroinflammatory disorders [13]. Various cell types in the brain have been revealed to possess chemokine receptors; these include CCR3, CCR5, CXCR1, CXCR2, CXCR3, and CXCR4, which are expressed in neurons, astrocytes, and microglia [14, 15]. Chemokine receptors were found to be more abundant in astrocytes, the anterior cingulate gyrus, the cerebellum, and autistic brain tissues [16]. The actual function of these receptors in the developed nervous system is not known. Chemokines and their receptors are involved in regulating neurodevelopment in the central nervous system (CNS) [15, 17]. Several studies have also reported elevated chemokine receptor expression in the brain tissue of ASD patients [10, 11]. Previous research showed that chemokine receptors are also implicated in neuroinflammation, neural damage, and astrocyte proliferation [18]. The expression levels of chemokine receptors were elevated in the temporal cortex of individuals with autism [5]. A significant focus of the immune imbalance has been on specific immune cell subsets, including helper cytotoxic CD8+ T cells [5, 19], which may behave differently in individuals with autism [20].
BTBR T+ Itpr3tf/J (BTBR) mice exhibit several immune abnormalities that are also observed in children with autism [21]. The BTBR mice showed highly replicable impairments in social interactions, including high levels of repetitive self-grooming and minimal vocalization in social settings [22, 23]. The BTBR mice have been recommended as a useful animal model for autism studies in comparison with C57BL/6 (B6) normal mice [22, 23]. An earlier study examined the expression of many inflammatory mediators in the whole brain and brain regions of BTBR mice [24]. BTBR mice have been shown to produce IL-6, IL-17, and TNF-α in greater amounts than B6 normal mice [25]. In our previous studies, we showed a distinct immune profile and higher levels of chemokine expression in BTBR mice [26]. Furthermore, we have also observed alterations in Th1, Th2, Th17, and T regulatory cell-related transcription factor signaling in the BTBR autistic model in comparison with that in the B6 normal mice [27].
There are four defined adenosine receptor subtypes: the Gi-protein-coupled A1 and A3 receptors, and Gs-protein-coupled A2A and A2B receptors [28, 29]. Adenosine A2A receptors (A2A receptors) are expressed in several types of cells that control physiological functions [30]. A2A receptors are expressed most highly on T cells [30, 31]. A2A receptors have been identified as significant inhibitors of inflammation and cell damage and have also been shown to decrease neutrophil cytotoxic function, as well as TNF-α and oxygen radical secretion [32, 33]. The selective A2A receptor agonist CGS decreases inflammatory mediators and suppresses the immune cell functions of T cells, granulocytes, dendritic cells, macrophages, and natural killer cells [30, 34]. The A2A receptors also decrease chemokine receptor, dendritic cells, and T cell expression levels [31, 35]. It has also been reported that A2A receptor treatment is for several disorders such as autoimmune inflammation, Parkinson’s disease, and experimental autoimmune encephalomyelitis [36, 37].
In our previous studies, we showed that A2A receptor antagonists and agonists effectively regulate the prominent repetitive behavior, reactions to painful sensory stimuli, Th17/RORγt transcription factor signaling, and Th1/Th2 cytokine balance in BTBR mice (manuscript submitted). Based on the abnormal immune alterations observed in autism, we herein elucidate the role of A2A receptors upon the chemokine receptor family and their association with the immune activation of autism. In this study, we tested the hypothesis that the activation of A2A receptors can trigger excessive chemokine receptor expression through its signaling pathways, which may be useful in treating autism. In the current study, we investigated several C-C (CCR3, CCR4, CCR5, CCR6, and CCR7) and C-X-C (CXCR3, CXCR4, and CXCR5) chemokine receptors in splenic cells. Furthermore, we also examined the gene expression levels of the C-C and C-X-C chemokine receptor families in brain tissue. We believe that this contribution achieves high relevance by elucidating molecular targets associated with therapeutic and etiological aspects of autism. It can also open new avenues for the prevention and/or treatment of this devastating neurodevelopmental disorder.
Methods
Chemicals and Antibodies
A2A receptor SCH 58261 (SCH) antagonist and RPMI medium were purchased from Sigma-Aldrich, USA. A2A receptor CGS 21680 (CGS) agonist was purchased from Santa Cruz Biotechnology, Inc., USA. Phycoerythrin (PE) and fluoroisothiocyanate (FITC)-labeled anti-mouse monoclonal antibodies CD8, CCR3, CCR4, CCR5, CCR6, CCR7, CXCR3, CXCR4, CXCR5, anti-CD3/CD28, and RBC buffers were purchased from Bio Legend and BD Biosciences, USA. FcR blocking reagent was obtained from Miltenyi Biotech, Germany. TRIzol reagent was purchased from Life Technologies, Grand Island, USA. SYBR® Green PCR master mix and high-capacity cDNA reverse transcription kits and primers were purchased from Applied Biosystems, UK and Genscript, USA.
Experimental Animals
The male adult BTBR T+ Itpr3tf/J (BTBR) mice 6–8 weeks old and male adult C57BL/6 (B6) normal mice aged 6–8 weeks old were purchased from (Jackson Laboratory, Bar Harbor, USA). The mice were housed in a specific pathogen-free environment maintained at 25 ± 2 °C with a 12-h light/dark cycle, and given standard rodent chow and water ad libitum. Institutional Animal Care and Use Committee, King Saud University, performed all procedures with approval.
Experimental Design
The mice were acclimatized for 2 to 3 weeks and divided into five groups of six mice each, as follows: BTBR control and B6 normal mice received 1% dimethyl sulfoxide (DMSO) in saline only, intraperitoneally (i.p.). A single dose of the SCH drug (0.03 mg/kg, i.p.) was administered to BTBR+SCH mice for 7 days. A single dose of the CGS drug (0.03 mg/kg, i.p.) was administered to BTBR+CGS mice for 7 days. A single dose of both SCH and CGS drugs (0.03 mg/kg, i.p.) was administered to SCH+CGS mice for seven consecutive days. The volume of drug administered to each mouse was based on its body weight. The doses of SCH and CGS were selected based on the results of the previous study [38].
Preparation of Spleen Cells
The mice were sacrificed on the eighth day, and spleens were removed aseptically. Briefly, the spleen cells were smashed with a stainless steel mesh and the cells were washed using RPMI-1640 medium (Sigma-Aldrich). The spleen cell suspension was collected by centrifugation and then resuspended in red blood cell (RBC) lysis buffer (BD Bioscience). After incubation at room temperature, the spleen cells were centrifuged and suspended in RPMI-1640 medium. One to two washes were performed with RPMI 1640 medium [39].
Flow Cytometric Analysis of CCR3, CCR4, CCR5, CCR6, CCR7, CXCR3, CXCR4, and CXCR5 on Splenic CD8 T Cells
Flow cytometric analysis was performed to evaluate CCR3, CCR4, CCR5, CCR6, CCR7, CXCR3, CXCR4, and CXCR5 production on splenic CD8 T cells. Briefly, splenocytes were cultured in 24-well plates (2 × 106 cells/mL) and activated with anti-CD3/CD28 (1 μg/mL, Bio Legend), and then incubated for 24 h. The cells were then collected, washed, and resuspended in staining buffer. The cells were incubated with monoclonal antibodies to the CD8 T cell surface receptor for 30 min at 4 °C. After washing with staining buffer, the cells were stained with CCR3, CCR4, CCR5, CCR6, CCR7, CXCR3, CXCR4, and CXCR5 monoclonal antibodies for 30 min at 4 °C. An FC500 Flow Cytometer (Beckman Coulter, USA) was used to acquire the 10,000 events, which were subsequently analyzed using CXP software [40].
RNA Isolation, cDNA Synthesis, and qPCR Analysis on Brain Tissue
The brain tissue was dissected and homogenized in TRIzol (Invitrogen). RNA was isolated and cDNA synthesized as described previously [41]. SYBR® Green reagent (Applied Biosystems), with 200 μM forward and reverse primer was used to amplify cDNA using the ABI 7500 system. The primers used in these assays were selected from PubMed and other databases. Primer sequences were as follows: GAPDH forward 5′-CCCAGCAAGGACACTGAGCAAG-3′, reverse 5′-GGTCTGGGATGGAAATTGTGAGGG-3′; CCR3 forward 5′-AACTTGCAAAACCTGAGAAGC-3′, reverse 5′-ACCATCATGTTGCCCAGGAG-3′; CCR4 forward 5′-GCCAACAGCCCTGTTTTCTG-3′, reverse 5′-ACACTGGATTTGAGGCTCCG-3′; CCR5 forward 5′-ACTGCTGCCTAAACCCTGTC-3′, reverse 5′-AGTGGTTCTTCCCTGTTGGC-3′; CCR6 forward 5′-CCCGTCTCTCAATGAGCACT-3′, reverse 5′-AACACGAGAACCACAGCGAT-3′; CCR7 forward 5′-GGGAAACCCAGGAAAAACGTG-3′, reverse 5′-CTTGCTGATGAGAAGCACGC-3′; CXCR3 forward 5′-TCAGCCAACTACGATCAGCG-3′, reverse 5′-CCTCTGGAGACCAGCAGAAC-3′; CXCR4 forward 5′-CATGGAACCGATCAGTGTGAG-3′, reverse 5′-TGAAGGCCAGGATGAGAACG-3′; and CXCR5 forward 5′-GCACGGAGATTCCCCTACAG-3′, reverse 5′-GCCAGTTGGGGAAAAGTTG-3′. The data are presented as the fold change in gene expression normalized to an endogenous reference gene (GAPDH) and relative to a calibrator [42].
Statistical Analysis
The results were firstly tested for homogeneity and normality of variance and then analyzed by employing a parametric test; comparisons between treatment groups were conducted using two-way repeated measure analysis of variation using GraphPad Prism. Each value indicates the mean ± SEM of six animals. The level of statistical significance was set at p < 0.05 and was considered significant.
Results
A2A Receptors Regulate CCR3, CCR4, CCR5, CCR6, and CCR7 Chemokine Receptors
To determine whether adenosine A2A receptors are involved in mediating C-C chemokine receptor expression, we examined the effects of specific SCH A2A receptor antagonists and CGS A2A agonists in BTBR mice. The A2A receptor antagonist and agonist were each used at a dose of 0.03 mg/kg, in accordance with a previous report [38]. We found that the number of CCR3+ cells and CD8+ T cells expressing CCR3+ increased in the BTBR control and BTBR-SCH-treated mice as compared to that in B6 normal mice (Fig. 1a). Treatment of the BTBR mice with CGS elicited a significant decrease in CCR3+ cells and CD8+ T cells expressing CCR3+ in the splenic cells in comparison with the BTBR control mice (Fig. 1a). To further clarify the mechanism of action of the A2A receptors, we used RT-PCR analysis to examine the alterations in CCR3 gene expression in brain tissues. The level of CCR3 mRNA was found to be elevated in the BTBR control and SCH-treated mice when compared with that in B6 normal mice. When BTBR mice were treated with CGS, the gene expression level of CCR3 in the brain tissue was decreased in comparison with that for the BTBR control and SCH-treated mice (Fig. 1b). These results showed that the A2A receptor agonist CGS may have a distinct capability of preventing the development of neuroimmunological disorders.
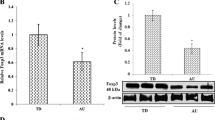
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CCR3+ and CD8+CCR3+ chemokine receptor production in the splenic cells. b CCR3 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CCR3 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
Furthermore, the production of CCR4+ cells and CD8+ T cells was significantly increased in the BTBR control mice relative to the B6 normal mice. We found that SCH treatment significant increased the number of CCR4+ positive cells and CD8+ T cells in BTBR mice in comparison with B6 normal mice (Fig. 2a). Additionally, we found that CGS treatment significantly reduced the percentage of CCR4+ cells and CD8+ expressing cells in BTBR-treated mice in comparison with the BTBR control mice in splenic cells (Fig. 2a). To understand the basis for the regulation of CCR4 production through A2A receptors, we further examined CCR4 mRNA expression using RT-PCR. The level of mRNA expression for CCR4 was clearly enhanced in the brain tissue of the BTBR control mice and SCH treated mice relative to the B6 normal mice (Fig. 2b). By contrast, treatment with CGS significantly decreased the level of CCR4 mRNA in the brain tissue of the BTBR mice (Fig. 2b). It has been shown that CGS A2A receptor agonist treatment decreases CCR4 expression levels, and these findings suggest that the A2A receptor may play an important role in autism and other neurological disorders.
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CCR4+ and CD8+CCR4+ chemokine receptors production in the splenic cells. b CCR4 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CCR4 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
Additionally, in comparison with the B6 normal mice, the BTBR control and BTBR-SCH-treated mice exhibited a significant increase in CCR5 production. The BTBR mice treated with SCH exhibited a significant increase in CD8+CCR5+ expressing cells as compared to the B6 normal mice (Fig. 3a). On the contrary, the treatment of BTBR mice with CGS significantly decreased the number of CCR5+ cells and CD8+ T cells expressing CCR5+ in comparison with that in the BTBR control and SCH-treated mice (Fig. 3a). As shown in Fig. 3b, there was also a significant increase in the CCR5 mRNA expression level in BTBR control mice and those treated with SCH, in comparison with that in the B6 normal mice. In the BTBR mice treated with CGS, CCR5 gene expression was significantly inhibited relative to that in the BTBR control and SCH-treated mice (Fig. 3b). Altogether, this result suggests that the A2A receptor agonist warrants further study as a potential therapeutic agent for the treatment of autism.
a, c Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CCR5+ and CCR6+ chemokine receptors produced in the splenic and by splenic CD8+ T cells. b, d CCR5 and CCR6 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
We further observed the effect of BTBR-SCH treatment on CCR6 production levels in BTBR-treated mice. We found that the numbers of CCR6+ cells and CD8+ T cells expressing CCR6+ in the splenic were increased in the BTBR control and SCH-treated mice as compared to B6 normal mice (Fig. 3c). Mice treated with CGS showed a significant decrease in CCR6+ and CD8+CCR6+ expressing splenic T cells as compared to the BTBR control mice (Fig. 3c). The CCR6 mRNA levels in the brain tissue of the BTBR control and SCH-treated mice were increased relative to that in the B6 normal mice. The BTBR mice treated with CGS exhibited a significant decrease in the gene expression level of CCR6 in the brain tissue compared with that in the BTBR control and SCH-treated mice (Fig. 3d). Our results demonstrated that the level of CCR6 was decreased in the splenic cells and brain through CGS treatment, indicating that the activation of the A2A receptor inhibits CCR6 chemokine receptor expression in the autistic mouse model.
Our results also showed that the percentage of T cells expressing CCR7+ and CD8+CCR7+ in the BTBR control and BTBR-SCH-treated mice significantly increased in comparison with that in the B6 normal mice. Treatment with CGS significantly decreased the number of T cells expressing CCR7+ and CD8+CCR7+ in the splenic in comparison with that in either BTBR- or SCH-treated mice (Fig. 4a). Moreover, the BTBR- and SCH-treated mice also showed a significant increase in CCR7 gene expression level relative to the B6 normal mice. Treatment with CGS decreased the mRNA expression of CCR7 levels in the brain tissue (Fig. 4b). The results from the current study recognize the important influence of an A2A receptor agonist on the C-C chemokine receptors family and deserve further study to offer a possible treatment for autism.
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CCR7+ chemokine receptors produced in the splenic and by splenic CD8+ T cells. b CCR7 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CCR7 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
A2A Receptor Activity Alters CXCR3, CXCR4, and CXCR5 Chemokine Receptor Expression
We further investigated the effects of SCH and CGS on C-X-C chemokine receptors in the BTBR mice. We found that the production of CXCR3+ and its expression on CD8+ splenic T cells were increased in the BTBR control mice relative to B6 normal mice (Fig. 5a). Treatment of BTBR mice with the A2A receptor antagonist SCH caused a significant increase in the percentage of CD8+ T cells secreting CXCR3+ in comparison with the B6 normal mice (Fig. 5a). In contrast, a decrease in CXCR3+ production was observed in splenic cells for BTBR mice treated with CGS in comparison with the BTBR- and SCH-treated mice (Fig. 5a). We further determined the changes in the gene expression level of CXCR3 in brain tissue. The mRNA expression level of CXCR3 was significantly increased in BTBR mice treated with SCH relative to B6 normal mice (Fig. 5b). Similarly, the inhibition of CXCR3 mRNA expression was observed in the brain tissue of BTBR mice treated with CGS as compared with both the BTBR control and SCH-treated mice (Fig. 5b). Our results showed that CXCR3 expression was significantly downregulated by A2A receptor agonist, suggesting that it could prevent neuroimmune dysfunctions or alterations.
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CXCR3+ chemokine receptors produced in the splenic and by splenic CD8+ T cells. b CXCR3 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CXCR3 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
The treatment of BTBR mice with SCH markedly increased the number of CD8+ T cells secreting CXCR4+ relative to the B6 normal mice. In contrast, the treatment of BTBR mice with CGS decreased the number of CXCR4+ secreting cells (Fig. 6a). The CXCR4 gene expression level was significantly increased following either BTBR or SCH treatment, but the expression level in brain tissue was lower in BTBR mice treated with CGS than in those treated with SCH (Fig. 6b). These data indicate that the suppressive effect exercised by CGS upon CXCR4 may play an important role in a future treatment of autistic disorder.
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CXCR4+ chemokine receptors produced in the splenic and by splenic CD8+ T cells. b CXCR4 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CXCR4 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
Flow cytometric staining was performed to evaluate CXCR5 production in the splenic CD8 T cells. As shown in Fig. 7a, BTBR control mice exhibited a significant increase in CXCR5+ and CD8+CXCR5+ production on splenic T cells. The treatment of BTBR mice with the A2A receptor antagonist SCH resulted in an increase in CXCR5+ and CD8+CXCR5+ production (Fig. 7a). On the contrary, treating BTBR mice with the A2A receptor agonist CGS reduced the production of CXCR5+ and CD8+CXCR5+ in splenic cells as compared with BTBR and SCH-treated mice (Fig. 7a). RT-PCR analysis was performed to detect the mRNA expression of CXCR5 in the brain tissue of the BTBR mice. The results revealed that the amount of CXCR5 mRNA was increased in the BTBR mice compared with the B6 normal mice; in addition, its expression was also upregulated in the brain of the SCH-treated mice (Fig. 7b). Correspondingly, the CXCR5 mRNA expression level was significantly decreased in the brain tissue of BTBR mice treated with CGS. Together, these findings suggest that targeting C-C and C-X-C chemokine receptors through A2A receptor agonist treatment may be of benefit in treating autism and neuroimmunological disorders. These results underline the requirement to further investigate A2A receptor agonists, as they may offer a therapeutic approach for the treatment of autism.
a Flow cytometric analysis indicates the influence of adenosine A2A receptor activity on the percentage of CXCR5+ chemokine receptors produced in the splenic and by splenic CD8+ T cells. b CXCR5 gene expression was measured by quantitative RT-PCR analysis in the brain tissue. c Dot plots represent the CXCR5 events of a mouse from each group. B6 normal mice received 1% DMSO in saline only [intraperitoneal (i.p.)], BTBR control mice received 1% DMSO in saline only (i.p.), BTBR mice treated with the A2A receptor antagonist SCH (0.03 mg/kg, i.p.), BTBR mice treated with the A2A receptor agonist CGS (0.03 mg/kg, i.p.), and BTBR mice treated with both SCH and CGS (0.03 mg/kg, i.p.). *P < 0.05 compared to the B6 normal mice; a P < 0.05 compared to BTBR control mice. All of the treatments were administered for 7 days
Discussion
There are significant indications that modulating A2A receptor activity is beneficial in neurological disorders. It has been recognized that the neuroprotective actions of A2A receptors and the mechanisms by which the A2A receptors affect the brain remain generally unknown. A2A receptors have been considered promising pharmacological modulators of neurodevelopmental and immune disorders [36]. The A2A receptors constitute a useful and important control mechanism that protects against neuroinflammation, EAE-induced brain damage, and human blood-brain barrier permeability [43, 44]. Earlier results revealed that A2A receptors have an significant role in mediating cytokine secretion, T lymphocyte activation, and the alteration of chemokine receptor expression levels [45–47]. Previous results also revealed the potency of the selective A2A receptor agonist CGS in decreasing cytokine production [48]. On the one hand, A2A receptor antagonists prevent the endogenous adenosine-mediated decrease in D2 receptor agonist affinity [49]. In our previous results, we showed that the A2A receptor regulates prominent repetitive behavior, Th1/Th2 cytokines balance, and Th17/RORγt transcription factors signaling pathways in the BTBR autistic model (manuscript submitted). The efficacy of A2A receptor signaling has uncovered novel and potentially therapeutic indications in the BTBR autistic mouse model. In the present study, we explored the effects of A2A receptors on C-C and C-X-C chemokine receptor expression on CD8 T cells involvement in the influence of chemokine receptors expression is still limited in autistic disorder particularly in the BTBR autistic mouse model.
Illuminating the mechanisms involved in neurodevelopmental disorders such as autism is essential in not only understanding the etiology of these disorders but also discovering early diagnostic markers and prophylactic treatments. Mouse models provide a distinctive opportunity to display causal links between immune and nervous system function and expose how changes in these systems alter behavioral profiles. BTBR mice show social deficits, high levels of repetitive self-grooming, and declined ultrasonic vocalizations in social settings [50]. Behavior rigidity and stereotypy are widely known as core and defining features of autistic disorder [51]. BTBR mice have revealed a number of immune abnormalities several of which observed in children with ASD [21]. The neuroimmune relation in the BTBR mice is characterized by higher pro-inflammatory signaling and diminished social interactions [52, 53]. BTBR mice showed the elevated expression levels of cytokines in the brain [24].
Although the mechanisms of autism are still unknown, chemokine receptors may play a critical role in the development of autism. We found an increase in CCR3+ production and CD8+ T cells in BTBR control mice compared with those of B6 normal mice. On the other hand, the treatment of BTBR mice with the A2A receptor agonist CGS significantly inhibited CCR3+ production and CD8+CCR3+. Moreover, BTBR control and BTBR-SCH-treated mice showed the CCR3 expression levels of splenic cells. These findings further demonstrate that CGS treatment suppresses CCR3 mRNA expression levels as compared with BTBR control and BTBR-SCH treated mice in brain tissue. CCR3 has been shown to play an important role in mediating neurological disorder. CCR3 expression has been detected on resident and inflammatory cells in the brain [54]. Neural progenitor cells from the brain were shown to express CCR3 highly [55]. Increased levels of CCR3 have been found in neurons of the hippocampus and brain regions [14, 15]. We showed for the first time that the A2A receptor agonist CGS has the effect of decreasing CCR3 expression. This study could lay the foundation for autism treatment with A2A receptor agonists in the future.
CCR4+ and CD8+CCR4+ production in CD8 T cells was significantly increased in BTBR mice treated with SCH, whereas CGS treatment significantly decreases CCR4+ expressed by CD8 positive cells in the splenic cells. Our results demonstrated that CGS significantly reduced the expression levels of CCR4 mRNA. CCR4 has a key pathogenic role in inflammatory conditions in allergies and autoimmune diseases [56, 57]. CCR4 exerts its immunomodulatory effects by modulating Th cell function, as well as reducing the induction of regulatory T cells and the elevation of the differentiation of Th17 cells [58]. Chemokine receptors might provide unique targets for future therapies in autism [10]. This may indicate that the elevation of CCR4 is closely linked to autism. We found that the lowering of CCR4 through CGS treatment may contribute to an improvement in autistic disorder.
We further examined the effect of A2A receptors on the production and expression levels of CCR5 and we found that treatment with CGS in BTBR mice resulted in a decrease in CCR5+ and CD8+ expressing T cells in the splenic of BTBR mice. In line with these observations, we further observed that treatment with CGS decreases the gene expression levels of CCR5 in brain tissue. The SCH treatment decreases the CCR5 mRNA expression level in BTBR mice. A CCR5 antagonist has been shown to lead to improved neurological outcomes, such as reduced neurological deficit [59]. CCR5 is highly recruited in astrocytes and leukocytes during brain development [60]. Hippocampal neurons have been shown to highly express CCR5 chemokine receptor [61]. Previous research also showed that CCR5 inhibition is neuroprotective against ischemia stroke and ischemic injury [62]. Our observations suggest the possible role of A2A receptor agonists in autism. Our data suggest that the A2A receptor agonist CGS might find application in controlling the chemokine receptor network underlying autistic disorder.
In the current study, we showed that the production of CCR6+ and CD8+CCR6+ T cells is increased in BTBR mice and provided evidence for the role of the A2A receptor agonist CGS in BTBR mice. The results demonstrated that the CGS decreases the expression level of CCR6 in brain tissue, whereas SCH had the effect of increasing this expression level in BTBR mice. These results indicate that CGS A2A receptor signaling can lead to a decrease in CCR6 levels in autistic neurological disorder. It has also been shown that CCR6 is upregulated in hippocampal neurons [63], while another recent study also suggested the CCR6 expressed in T helper cells is crucial to their migration into the CNS [64]. Our results clearly suggest that A2A receptor agonists have anti-neuroinflammatory effects and have the potential to be applied as treatments for autism. These effects support the hypothesis that an A2A receptor agonist could be a better therapeutic agent for autistic disorders than previously proposed treatments.
We have also observed for the first time that CCR7 expression is significantly increased in BTBR mice. Interestingly, we found that CGS treatment significantly decreased CCR7+ production and the number of splenic CD8+ T cells. Furthermore, we showed that the mRNA expression of CCR7 in brain tissue is decreased during treatment with CGS as compared with the A2A receptor antagonist SCH. These results clearly demonstrate that the neuroimmunological inhibition of CCR7 through the A2A receptor agonist CGS provides a therapeutic benefit in the BTBR autistic mouse model. CCR7 is a homeostatic chemokine receptor and induced during times of inflammation [65]. It has also been shown that CCR7 expression is upregulated in the CNS [66]. The expression level of CCR7 is found largely in the hippocampus [66]. Our results also deliver valuable information that CCR7 is found to be highly expressed in BTBR brain tissue. These observations indicate that CCR7 is a potential therapeutic target for neuroinflammatory diseases. These results demonstrate that the A2A receptor agonist CGS suppresses CCR7 and could be applied in treating several autism-like neuroimmuological disorders.
In this study, we further observed that the BTBR mice treated with SCH produced a substantial increase in CXCR3+ and CD8+CXCR3+ in the splenic T cells, which was decreased by CGS treatment. The gene expression level of CXCR3 was significantly decreased by the CGS treatment. Early studies pointed out the key role of CXCR3 in promoting the influx of activated T cells into the CNS [67]. Cerebrospinal fluid investigations have shown that a significant enrichment of T cells expressing CXCR3 correlates with CNS pathology [67]. CXCR3 expression has been reported on microglia and neurons and has been associated with the altered functionality of these cells [68]. Furthermore, CXCR3 is also implicated in the pathogenesis of many neuroinflammatory disorders [69]. Our results indicate that the A2A receptor agonist CGS can be a therapeutic treatment by downregulating the expression level of CXCR3 in autism. Decreasing the number of chemokine receptors may be an important potential therapeutic strategy in treating autism. Our study proposes that CXCR3 is a key component of the signaling pathways in autism disorder. In summary, these data suggest that this A2A receptor agonist effectively and directly suppresses CXCR3 expression.
In our study, CXCR4 expression was measured in splenic cells and brain tissue. There was a significant difference between the BTBR control, BTBR-SCH treatment, and BTBR-CGS treatment groups, suggesting that the CGS-treated mice showed a significant decrease in CXCR4+ and CD8+ T expressing cells. CXCR4 mRNA is expressed in the CNS [70]; we previously noticed that CGS treatment efficiently decreased the gene expression level of the CXCR4 in brain tissue as compared with that seen in the BTBR- and BTBR-SCH-treated mice. Hence, we suggested that decreased expression of CXCR4 transduction initiated through the A2A receptor agonist could contribute to improvements in neuroinflammation-related disorders. CXCR4 is also regulated in interneuron migration in the developing neocortex and broadly expressed in cells of both the immune and the CNS [70]. We have demonstrated the role of A2A receptor activity in modulating chemokine receptors in BTBR mice for the first time. These results may be important for designing strategies to reduce the signaling in chemokine receptor pathways to understand the mechanism and development of autistic disorder.
Importantly, we showed for the first time that the A2A receptor agonist CGS significantly downregulated CXCR5+ expression in CD8+ T cells in comparison with BTBR control and BTBR-SCH treated mice. The mRNA expression of CXCR5 was also increased in the brain tissue of BTBR control and BTBR-SCH treated mice, whereas it was decreased in BTBR-CGS treated mice. These results suggest that the increased CXCR5 expression is related to autism. CXCR5 is a potent chemokine receptor for the recruitment of neural precursor cells across brain endothelial cells [71]. In addition, neuroblastoma cells expressing CXCR5 chemokine receptors have been found to migrate toward CXCL13 [72]. Our results suggest that the A2A receptor agonist CGS corrects the neurodevelopmental dysregulation in autism through the downregulation of CXCR5. The possible use of an A2A receptor agonist as an agent for therapeutic intervention in neurological disorders might need to be considered in the context of its broader neurophysiological functions.
Conclusion
We have investigated the influence of adenosine A2A receptor signaling on C-C- and C-X-C chemokine receptors associated with the regulation of autistic disorder. Our findings lead us to hypothesize that increased C-C and C-X-C chemokine receptors may be associated in the pathophysiology of autism. Treatment with the A2A receptor agonist CGS had beneficial effect in BTBR autistic mice by reducing the number of C-C and C-X-C chemokine receptors. Our data suggest that the downregulation of C-C and C-X-C chemokine receptor expression using the A2A receptor agonist CGS may be a good strategy for treating autism and other immune-mediated neuroimmunological disorders. These findings serve as evidence that A2A receptor agonists may be important for the treatment of autistic disorder; however, more extensive therapeutic studies are required to investigate this possibility.
Abbreviations
- ASD:
-
Autism spectrum disorder
- CD4:
-
Cluster of differentiation 4
- Th cells:
-
T helper cells
- IL:
-
Interleukin
- PE:
-
Phycoerythrin
- FITC:
-
Fluoroisothiocyanate
- CXCR:
-
CXC chemokine receptor
- A2A receptors:
-
Adenosine A2A receptors
- SCH:
-
SCH 58261
- CGS:
-
CGS 21680
- CCR:
-
C-C chemokine receptor
- B6:
-
C57BL/6
- BTBR:
-
BTBR T+ Itpr3tf/J
- RORγt:
-
Retinoid-acid receptor-related orphan receptor gamma t
- STAT3:
-
Signal transducer and activator of transcription 3
- TNF-α:
-
Tumor necrosis factor-α
- RBC:
-
Red blood cell
- i.p.:
-
Intraperitoneally
- mRNA:
-
Messenger RNA
- RT-PCR:
-
Reverse transcription polymerase chain reaction
- CNS:
-
Central nervous system
- DMSO:
-
Dimethyl sulfoxide
References
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Association, Washington
Van Gent T, Heijnen CJ, TreVers PDA (1997) Autism and the immune system. J Child Psychol Psychiatry 38:337–349
Enstrom A, Onore C, Van de Water J, Ashwood P (2010) Differential monocyte responses to TLR ligands in children with autism spectrum disorders. Brain Behav Immun 24(1):64–71
Ashwood P, Wills S, Van de Water J (2006) The immune response in autism: a new frontier for autism research. J Leukoc Biol 80:1–15
Garbett K, Ebert PJ, Mitchell A, Lintas C, Manzi B, Mirnics K et al (2008) Immune transcriptome alterations in the temporal cortex of subjects with autism. Neurobiol Dis 30:303–311
Ashwood P, Enstrom A, Krakowiak P, Hertz-Picciotto I, Hansen RL, Croen LA et al (2008) Decreased transforming growth factor beta1 in autism: a potential link between immune dysregulation and impairment in clinical behavioral outcomes. J Neuroimmunol 204(1–2):149–153
Ahmad SF, Zoheir KM, Ansari MA, Nadeem A, Bakheet SA, Al-Ayadhi LY, Alzahrani MZ, Al-Shabanah OA, Al-Harbi MM, Attia SM (2016) Dysregulation of Th1, Th2, Th17, and T regulatory cell-related transcription factor signaling in children with autism. Mol. Neurobiol. http://dx.doi.org/10.1007/s12035-016-9977-0 (Epub ahead of print)
Moser B, Loetscher P (2001) Lymphocyte traffic control by chemokines. Nat Immunol 2:123–128
Tran PB, Miller RJ (2003) Chemokine receptors: signposts to brain development and disease. Nat Rev Neurosci 4:444–455
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Pessah IN, Van de Water J (2011) Associations of impaired behaviors with elevated plasma chemokines in autism spectrum disorders. J Neuroimmunol 232(1–2):196–199
Abdallah MW, Larsen N, Grove J, Nørgaard-Pedersen B, Thorsen P, Mortensen EL, Hougaard DM (2012) Amniotic fluid chemokines and autism spectrum disorders: an exploratory study utilizing a Danish Historic Birth Cohort. Brain Behav Immun 26(1):170–176
Depino AM (2013) Peripheral and central inflammation in autism spectrum disorders. Mol Cell Neurosci 53:69–76
Karpus WJ, Fife BT, Kennedy KJ (2003) Immunoneutralization of chemokines for the prevention and treatment of central nervous system autoimmune disease. Methods 29:362–368
Van der Meer P, Ulrich AM, Gonzalez-Scarano F, Lavi E (2000) Immunohistochemical analysis of CCR2, CCR3, CCR5, and CXCR4 in the human brain: potential mechanisms for HIV dementia. Exp Mol Pathol 69:192–201
Bajetto A, Bonavia R, Barbero S et al (2001) Chemokines and their receptors in the central nervous system. Front Neuroendocrinol 22:147–184
Vargas DL, Nascimbene C, Krishnan C, Zimmerman AW, Pardo CA (2005) Neuroglial activation and neuroinflammation in the brain of patients with autism. Ann Neurol 57(1):67–81
Rostène W, Dansereau MA, Godefroy D, Van Steenwinckel J, Reaux-Le Goazigo A et al (2011) Neurochemokines: a menage a trois providing new insights on the functions of chemokines in the central nervous system. J Neurochem 118(5):680–694
Louboutin JP, Chekmasova A, Marusich E, Agrawal L, Strayer DS (2011) Role of CCR5 and its ligands in the control of vascular inflammation and leukocyte recruitment required for acute excitotoxic seizure induction and neural damage. FASEB J 25:737–753
Gregg JP, Lit L, Baron CA, Hertz-Picciotto I, Walker W, Davis RA et al (2008) Gene expression changes in children with autism. Genomics 91:22–29
Gupta S, Aggarwal S, Rashanravan B, Lee T (1998) Th1- and Th2-like cytokines in CD4+ and CD8+ T cells in autism. J Neuroimmunol 85:106–109
Li X, Chauhan A, Sheikh AM, Patil S, Chauhan V, Li XM, Ji L, Brown T et al (2009) Elevated immune response in the brain of autistic patients. J Neuroimmunol 207(1–2):111–116
McFarlane HG, Kusek GK, Yang M, Phoenix JL, Bolivar VJ, Crawley JN (2008) Autism-like behavioral phenotypes in BTBR Tþtf/J mice. Genes Brain Behav 7:152–163
Silverman JL, Tolu SS, Barkan CL, Crawley JN (2010) Repetitive self-grooming behavior in the BTBR mouse model of autism is blocked by the mGluR5 antagonist MPEP. Neuropsychopharmacology 35:976–989
Heo Y, Zhang Y, Gao D, Miller VM, Lawrence DA (2011) Aberrant immune responses in a mouse with behavioral disorders. PLoS One e20912
Schwartzer JJ, Careaga M, Onore CE, Rushakoff JA, Berman RF, Ashwood P (2013) Maternal immune activation and strain specific interactions in the development of autism-like behaviors in mice. Transl Psychiatry 3:e240
Bakheet SA, Alzahrani MZ, Nadeem A, Ansari MA, Zoheir KM, Attia SM, Al-Ayadhi LY, Ahmad SF (2016) Resveratrol treatment attenuates chemokine receptor expression in the BTBR T+tf/J mouse model of autism. Mol Cell Neurosci 77:1–10
Bakheet SA, Alzahrani MZ, Ansari MA, Nadeem A, Zoheir KM, Attia SM, Al-Ayadhi LY, Ahmad SF (2016) Resveratrol ameliorates dysregulation of Th1, Th2, Th17, and T regulatory cell-related transcription factor signaling in a BTBR T + tf/J mouse model of autism. Mol Neurobiol. doi:10.1007/s12035-016-0066-1
Fredholm BB, IJzerman AP, Jacobson KA, Klotz KN, Linden J (2001) International Union of Pharmacology. XXV. Nomenclature and classification of adenosine receptors. Pharmacol Rev 53:527–552
Linden J (2001) Molecularapproach to adenosinereceptors: receptor-mediated mechanisms of tissue protection. Annu Rev Pharmacol Toxicol 41:775–787
Chen JF, Eltzschig HK, Fredholm BB (2013) Adenosine receptors as drug targets—what are the challenges? Nat. Rev. Drug Discov 12:265–286
Koshiba M, Rosin DL, Hayashi N, Linden J, Sitkovsky MV (1999) Patterns of A2A extracellular adenosine receptor expression in different functional subsets of human peripheral T cells. Flow cytometry studies with anti-A2A receptor monoclonal antibodies. Mol Pharmacol 55:614–624
Thiel M, Caldwell CC, Sitkovsky MV (2003) The critical role of adenosine A2A receptors in downregulation of inflammation and immunity in the pathogenesis of infectious diseases. Microbes Infect 5:515–526
Haskó G, Pacher P (2008) A2A receptors in inflammation and injury: lessons learned from transgenic animals. J Leukoc Biol 83:447–455
Mazzon E, Esposito E, Impellizzeri D, DI Paola R, Melani A, Bramanti P, Pedata F, Cuzzocrea S (2011) CGS 21680, an agonist of the adenosine (A2A) receptor, reduces progression of murine type II collagen-induced arthritis. J Rheumatol 38:2119–2129
Huang S, Apasov S, Koshiba M, Sitkovsky M (1997) Role of A2a extracellular adenosine receptor-mediated signaling in adenosine-mediated inhibition of T-cell activation and expansion. Blood 90:1600–1610
Ramlackhansingh AF, Bose SK, Ahmed I, Turkheimer FE, Pavese N, Brooks DJ (2011) Adenosine 2A receptor availability in dyskinetic and nondyskinetic patients with Parkinson disease. Neurology 76:1811–1816
Li N, Mu L, Wang J, Zhang J, Xie X et al (2012) Activation of the adenosine A2A receptor attenuates experimental autoimmune myasthenia gravis severity. Eur J Immunol 42(5):1140–1151
Kermanian F, Soleimani M, Ebrahimzadeh A, Haghir H, Mehdizadeh M (2013) Effects of adenosine A2a receptor agonist and antagonist on hippocampal nuclear factor-kB expression preceded by MDMA toxicity. Metab Brain Dis 28(1):45–52
Ahmad SF, Zoheir KM, Ansari MA, Nadeem A, Bakheet SA, Al-Hoshani AR, Al-Shabanah OA, Al-Harbi MM et al (2015) Histamine 4 receptor promotes expression of costimulatory B7.1/B7.2 molecules, CD28 signaling and cytokine production in stress-induced immune responses. J Neuroimmunol 15(289):30–42
Ahmad SF, Ansari MA, Nadeem A, Zoheir KM, Bakheet SA, Al-Shabanah OA, Al Rikabi AC, Attia SM (2016) The tyrosine kinase inhibitor tyrphostin AG126 reduces activation of inflammatory cells and increases Foxp3+ regulatory T cells during pathogenesis of rheumatoid arthritis. Mol Immunol 78:65–78
Fabrizius A, Andre D, Laufs T, Bicker A, Reuss S, Porto E, Burmester T, Hankeln T (2016) Critical re-evaluation of neuroglobin expression reveals conserved patterns among mammals. Neuroscience 337:339–354
Ahmad SF, Ansari MA, Nadeem A, Zoheir KM, Bakheet SA, Alsaad AM, Al-Shabanah OA, Attia SM (2017) STA-21, a STAT-3 inhibitor, attenuates the development and progression of inflammation in collagen antibody-induced arthritis. Immunobiology 222:206–217
Yao SQ, Li ZZ, Huang QY, Li F et al (2012) Genetic inactivation of the adenosine A(2A) receptor exacerbates brain damage in mice with experimental autoimmune encephalomyelitis. J Neurochem 123(1):100–112
Kim DG, Bynoe MS (2015) A2A adenosine receptor regulates the human blood-brain barrier permeability. Mol Neurobiol 52(1):664–678
Apasov SG, Chen JF, Smith PT, Schwarzschild MA, Fink JS, Sitkovsky MV (2000) Study of A(2A) adenosine receptor gene deficient mice reveals that adenosine analogue CGS 21680 possesses no A(2A) receptor-unrelated lymphotoxicity. Br J Pharmacol 131:43–50
Németh ZH, Lutz CS, Csóka B, Deitch EA, Leibovich SJ et al (2005) Adenosine augments IL-10 production by macrophages through an A2B receptor-mediated posttranscriptional mechanism. J Immunol 175(12):8260–8270
Williams AJ, Cronstein BN (2012) The effect of A(2A) adenosine receptor activation on C-C chemokine receptor 7 expression in human THP1 macrophages during inflammation. Inflammation 35:614–622
Haskó G, Kuhel DG, Chen JF, Schwarzschild MA, Deitch EA et al (2000) Adenosine inhibits IL-12 and TNF-alpha production via adenosine A2a receptor dependent and independent mechanisms. FASEB J 14:2065–2074
Pinna A (2009) Novel investigational adenosine A2A receptor antagonists for Parkinson's disease. Expert Opin Investig Drugs 18(11):1619–1631
Blanchard DC, Defensor EB, Meyza KZ, Pobbe RL, Pearson BL, Bolivar VJ, Blanchard RJ (2012) BTBR T+tf/J mice: autism-relevant behaviors and reduced fractone-associated heparan sulfate. Neurosci Biobehav Rev 36(10):2370
Baronio D, Castro K, Gonchoroski T, de Melo GM et al (2015) Effects of an H3R antagonist on the animal model of autism induced by prenatal exposure to valproic acid. PLoS One 10(1):e0116363
Careaga M, Schwartzer J, Ashwood P (2015) Inflammatory profiles in the BTBR mouse: how relevant are they to autism spectrum disorders? Brain Behav Immun 43:11–16
Onore CE, Careaga M, Babineau BA, Schwartzer JJ, Berman RF, Ashwood P (2013) Inflammatory macrophage phenotype in BTBR T+tf/J mice. Front Neurosci 7:158
Westmoreland SV, Rottman JB, Williams KC, Lackner AA, Sasseville VG (1998) Chemokine receptor expression on resident and inflammatory cells in the brains of m with simian immunodeficiency virus encephalitis. Am J Pathol 152:659–665
Krathwohl MD, Kaiser JL (2004) Chemokines promote quiescence and survival of human neural progenitor cells. Stem Cells 22(1):109–118
Galimberti D, Scalabrini D, Fenoglio C, De Riz M, Comi C, Venturelli E, Cortini F, Piola M et al (2008) Gender-specific influence of the chromosome 16 chemokine gene cluster on the susceptibility to multiple sclerosis. J Neurol Sci 267:86–90
Abelius MS, Ernerudh J, Berg G, Matthiesen L, Nilsson LJ, Jenmalm MC (2011) High cord blood levels of the T-helper 2-associated chemokines CCL17 and CCL22 precede allergy development during the first 6 years of life. Pediatr Res 70:495–500
Heiseke AF, Faul AC, Lehr HA, Förster I, Schmid RM, Krug AB, Reindl W (2012) CCL17 promotes intestinal inflammation in mice and counteracts regulatory T cell-mediated protection from colitis. Gastroenterology 142:335–345
Li L, Zhi D, Shen Y, Liu K, Li H, Chen J (2016) Effects of CC-chemokine receptor 5 on ROCK2 and P-MLC2 expression after focal cerebral ischaemia-reperfusion injury in rats. Brain Inj 30(4):468–473
Andjelkovic AV, Kerkovich D, Shanley J, Pulliam L, Pachter JS (1999) Expression of binding sites for chemokines on human astrocytes. Glia 28:225
Coughlan CM, McManus CM, Sharron M et al (2000) Expression of multiple functional chemokine receptors and monocyte chemoattractant protein-1 in human neurons. Neuroscience 97:591–600
Reichel CA, Khandoga A, Anders HJ, Schlondorff D, Luckow B, Krombach F (2006) Chemokine receptors Ccr1, Ccr2, and Ccr5 mediate neutrophil migration to postischemic tissue. J Leukoc Biol 79:114–122
Yamazaki T, Yang XO, Chung Y, Fukunaga A, Nurieva R, Pappu B, Martin-Orozco N, Kang HS et al (2008) CCR6 regulates the migration of inflammatory and regulatory T cells. J Immunol 181:8391–8401
Reboldi A, Coisne C, Baumjohann D, Benvenuto F, Bottinelli D, Lira S et al (2009) C-C chemokine receptor 6-regulated entry of TH-17 cells into the CNS through the choroid plexus is required for the initiation of EAE. Nat Immunol 10:514–523
Wilson EH, Harris TH, Mrass P, John B, Tait ED, Wu G, Pepper M, Wherry EJ et al (2009) Behavior of parasite-specific effector CD8+ T cells in the brain and visualization of a kinesis-associated system of reticular fibers. Immunity 30(2):300–311
Kivisakk P, Mahad DJ, Callahan MK et al (2004) Expression of CCR7 in multiple sclerosis: implications for CNS immunity. Ann Neurol 55:627–638
Balashov KE, Rottman JB, Weiner HL, Hancock WW (1999) CCR5(+) and CXCR3(+) T cells are increased in multiple sclerosis and their ligands MIP-1alpha and IP-10 are expressed in demyelinating brain lesions. Proc Natl Acad Sci U S A 96:6873–6878
Biber K, Dijkstra I, Trebst C, De Groot CJ, Ransohoff RM, Boddeke HW (2002) Functional expression of CXCR3 in cultured mouse and human astrocytes and microglia. Neuroscience 112:487–497
Sørensen TL, Trebst C, Kivisäkk P, Klaege KL, Majmudar A, Ravid R, Lassmann H, Olsen DB et al (2002) Multiple sclerosis: a study of CXCL10 and CXCR3 co-localization in the inflamed central nervous system. J Neuroimmunol 127:59–68
Stumm RK, Zhou C, Ara T, Lazarini F, Dubois-Dalcq M, Nagasawa T, Hollt V, Schulz S (2003) CXCR4 regulates interneuron migration in the developing neocortex. The Journal of neuroscience: the official journal of the Society for Neuroscience 23:5123–5130
Weiss N, Deboux C, Chaverot N, Miller F, Baron-Van Evercooren A, Couraud PO, Cazaubon S (2010) IL8 and CXCL13 are potent chemokines for the recruitment of human neural precursor cells across brain endothelial cells. J Neuroimmunol 223(1–2):131–134
Del Grosso F, Coco S, Scaruffi P, Stigliani S, Valdora F et al (2011) Role of CXCL13-CXCR5 crosstalk between malignant neuroblastoma cells and Schwannian stromal cells in neuroblastic tumors. Mol Cancer Res 9(7):815–823
Acknowledgments
The authors extend their appreciation to the Deanship of Scientific Research at King Saud University for funding the work through the research group project no. RGP-120.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Ahmad, S.F., Ansari, M.A., Nadeem, A. et al. Immune Alterations in CD8+ T Cells Are Associated with Neuronal C-C and C-X-C Chemokine Receptor Regulation Through Adenosine A2A Receptor Signaling in a BTBR T+ Itpr3tf/J Autistic Mouse Model. Mol Neurobiol 55, 2603–2616 (2018). https://doi.org/10.1007/s12035-017-0548-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-017-0548-9