Abstract
Astrocytes are dynamic cells that maintain brain homeostasis, regulate neurotransmitter systems, and process synaptic information, energy metabolism, antioxidant defenses, and inflammatory response. Aging is a biological process that is closely associated with hippocampal astrocyte dysfunction. In this sense, we demonstrated that hippocampal astrocytes from adult and aged Wistar rats reproduce the glial functionality alterations observed in aging by evaluating several senescence, glutamatergic, oxidative and inflammatory parameters commonly associated with the aging process. Here, we show that the p21 senescence-associated gene and classical astrocyte markers, such as glial fibrillary acidic protein (GFAP), vimentin, and actin, changed their expressions in adult and aged astrocytes. Age-dependent changes were also observed in glutamate transporters (glutamate aspartate transporter (GLAST) and glutamate transporter-1 (GLT-1)) and glutamine synthetase immunolabeling and activity. Additionally, according to in vivo aging, astrocytes from adult and aged rats showed an increase in oxidative/nitrosative stress with mitochondrial dysfunction, an increase in RNA oxidation, NADPH oxidase (NOX) activity, superoxide levels, and inducible nitric oxide synthase (iNOS) expression levels. Changes in antioxidant defenses were also observed. Hippocampal astrocytes also displayed age-dependent inflammatory response with augmentation of proinflammatory cytokine levels, such as TNF-α, IL-1β, IL-6, IL-18, and messenger RNA (mRNA) levels of cyclo-oxygenase 2 (COX-2). Furthermore, these cells secrete neurotrophic factors, including glia-derived neurotrophic factor (GDNF), brain-derived neurotrophic factor (BDNF), S100 calcium-binding protein B (S100B) protein, and transforming growth factor-β (TGF-β), which changed in an age-dependent manner. Classical signaling pathways associated with aging, such as nuclear factor erythroid-derived 2-like 2 (Nrf2), nuclear factor kappa B (NFκB), heme oxygenase-1 (HO-1), and p38 mitogen-activated protein kinase (MAPK), were also changed in adult and aged astrocytes and are probably related to the changes observed in senescence marker, glutamatergic metabolism, mitochondrial dysfunction, oxidative/nitrosative stress, antioxidant defenses, inflammatory response, and trophic factors release. Together, our results reinforce the role of hippocampal astrocytes as a target for understanding the mechanisms involved in aging and provide an innovative tool for studies of astrocyte roles in physiological and pathological aging brain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Astrocytes are dynamic cells that participate in a diverse range of central nervous system (CNS) functions, including the regulation of neurotransmitter systems, synaptic information processing (as part of the tripartite synapse), ionic homeostasis, the development and maintenance of the blood–brain barrier, brain cholesterol levels, energy metabolism, antioxidant defenses, and inflammatory response [1–6]. These cells release anti- and proinflammatory cytokines in regenerative or protective processes and secrete an enormous array of neurotrophic factors, such as glia-derived neurotrophic factor (GDNF), brain-derived neurotrophic factor (BDNF), S100 calcium-binding protein B (S100B) protein, and transforming growth factor-β (TGF-β) [4, 7, 8]. In accordance with this, the pathophysiological roles of astrocytes have become a primary focus in the investigation of numerous diseases and have emerged as a target for preventive/therapeutic strategies for these diseases [9].
Although astrocytes have an essential role for brain functionality, their neuroprotective capacity decreases during aging, playing critical roles in age-related neurological disorders [9–11]. Aging is a biological process associated with gradual and spontaneous biochemical, cellular, and molecular changes, which increase susceptibility to diseases. Changes in glial functions, such as redox homeostasis and inflammatory response, are hallmarks of the brain aging [11–13]. Astrocytes sense and amplify inflammatory signals from microglia and/or initiate the release of inflammatory mediators that are closely associated to transcription factors, such as nuclear factor erythroid-derived 2-like 2 (Nrf2) and nuclear factor kappa B (NFκB), which are also the master regulators of the redox state [1, 14, 15]. In this sense, Nrf2 controls the biosynthesis of antioxidant systems, such as glutathione (GSH) and heme oxygenase-1 (HO-1), and cell cycle regulatory genes such as p21. Nrf2 also regulates the transcriptional activity of NFκB, which stimulates proinflammatory cytokine release, oxidative/nitrosative stress and the expressions of inducible nitric oxide synthase (iNOS) and cyclo-oxygenase 2 (COX-2) [16, 17]. Furthermore, the translocation of NFκB into the nucleus requires the activation of the p38 mitogen-activated protein kinase (MAPK) signaling pathway [14].
The association between oxidative stress, inflammation, and aging is based on complex molecular and cellular changes that have only just begun to be understood [9, 18, 19]. To understand, recognize, and manage these alterations before cognitive decline may be an important strategy to extend healthy lifespan. Thus, we choose Wistar rats from 90 (adult) to 180 days old (aged), which did not present any cognitive impairment, by Morris water maze evaluation. Moreover, age-related changes in astrocyte functions seem to be brain-region specific, and the hippocampus is one of the structures more closely related to behavioral, neurochemical, and cellular alterations during aging [12].
Considering the essential role of astrocytes to brain health and disease as well as the differences between immature and aging brain, the aim of this study was to demonstrate that hippocampal astrocyte cultures from adult and aged Wistar rats reproduce changes in glial functionality observed in the aging brain. In line with this, we expected that mature astrocytes present changes in senescence, glutamatergic, oxidative/nitrosative, inflammatory, and neurotrophic markers, when compared to astrocytes from immature brain (1–2 days old), since these parameters are generally affected with aging. We also projected that the expression of signaling pathways, such as Nrf2, NFκB, HO-1, and p38 MAPK, are associated with these changes. Therefore we evaluated the following: (i) behavioral performance; (ii) cytoskeleton proteins, such as glial fibrillary acidic protein (GFAP), vimentin, and actin; (iii) glutamate transporters (glutamate aspartate transporter (GLAST) and glutamate type I (GLT-1)) and glutamine synthetase (GS) expression protein and activity; (iv) p21 senescence gene expression; (v) signaling pathways classically associated with the aging process, like Nrf2, NFκB, HO-1, and p38 MAPK; (vi) reactive oxygen species (ROS) generation, RNA oxidation, mitochondrial functionality, NADPH oxidase (NOX) activity, superoxide levels, iNOS expression, and enzymatic and non-enzymatic antioxidant defenses; (vii) pro- and anti-inflammatory cytokines release; and (viii) BDNF, GDNF, S100B, and TGF-β levels. In conclusion, hippocampal astrocyte cultures from mature rats represent a powerful tool for the mechanistic investigation of astrocytes in the brain aging. In addition, it opens the exciting possibility to perform in vivo interventions and then evaluate what is the specific role of astrocyte in response to that.
Materials and Methods
Reagents
DNase, 2′-7′-dichorofluorescein diacetate (DCFH-DA), propidium iodide, γ-glutamyl hydroxamate, GSH standard, o-phthaldialdehyde, NADP/NADPH, lucigenin, superoxide anion assay kit, anti-GS and anti-vimentin, anti-β-tubulin III, peroxidase-conjugated anti-rabbit immunoglobulin (IgG), and anti-phospho-p38 MAPK were obtained from Sigma-Aldrich (St. Louis, MO, USA). JC-1, monoclonal anti-CD11, ELISA kit for monocyte chemoattractant protein-1 (MCP-1) and NFκB p65, TRIzol reagent, SYBR green PCR master mix, Dulbecco’s modified Eagle’s Medium/F12 (DMEM/F12), and other materials for cell cultures were purchased from Gibco/Invitrogen (Carlsbad, CA, USA). Polyclonal anti-GFAP was purchased from Dako (Carpinteria, CA, USA). Monoclonal anti-glyceraldehyde 3-phosphate dehydrogenase (GAPDH), anti-NeuN and 4ʹ,6ʹ-diamino-2-phenylindole (DAPI) were purchased from Millipore (Billerica, MA, USA). Anti-GLAST and anti-GLT-1 were obtained from Alpha Diagnostic (San Antonio, TX, USA). Anti-HO-1 antibody was purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Alexa Fluor® 488 (A max = 493; E max = 519) or 594 (A max = 591; E max = 614)-conjugated AffiniPure antibodies were purchase from Jackson ImmunoResearch (West Grove, PA, USA). Nitrocellulose membranes and enhanced chemiluminescence kits were purchased from Amersham (Buckinghamshire, UK). GDNF and BDNF ELISA kits were purchased from Promega (Madison, WI, USA). S100B and TGF-β ELISA kits were purchased from R&D Systems (Minneapolis, MN, USA). RANSOD and RANSEL were purchased from Randox (Autrim, UK). ELISA kit for TNF-α was purchased from PeproTech (Rocky Hill, NJ, USA). ELISA kits for interleukins were purchase from eBioscience (San Diego, CA, USA). All other chemicals were purchased from common commercial suppliers.
Animals
Male Wistar rats (1, 90, and 180 days old) were obtained from our breeding colony (Department of Biochemistry, UFRGS, Porto Alegre, Brazil), maintained under controlled environment (12-h light/12-h dark cycle; 22 ± 1 °C; ad libitum access to food and water). All animal experiments were performed in accordance with the National Institute of Health (NIH) Guide for the Care and Use of Laboratory Animals and Brazilian Society for Neuroscience and Behavior recommendations for animal care. The experimental protocols were approved by the Federal University of Rio Grande do Sul Animal Care and Use Committee (process number 27543).
Cognitive Evaluation
Wistar rats from 90 and 180 days old were submitted to training in the Morris water maze [20]. The apparatus consisted of a circular pool (180-cm diameter, 60-cm high) filled with water (30-cm depth; 24 ± 1 °C), placed in a room with consistently located spatial cues. An escape platform (10-cm diameter) was placed in the middle of one of the quadrants, 1.5 cm below the water surface, equidistant from the sidewall and the middle of the pool. The platform provided the only escape from the water and was located in the same quadrant every trial. Four different starting positions were equally spaced around the perimeter of the pool. During training, all four start positions were used once in a random sequence, i.e., four training trials per day. A trial began by placing the animal in the water facing the wall of the pool at one of the starting points. If the animal failed to escape within 60 s, it was gently guided to the platform by the experimenter. The rat was allowed to stay there for 20 s. The intertribal interval was 10 min. After each trial, the rats were dried and returned to their cages at the end of the session. Animals were trained for 5 days. Then, 24 h after the last training session, the rats were submitted to a test session. Before this session, the submerged platform was removed. The retention test consisted of placing the animals in the water for 1 min. The number of crossings over the original position of the platform and time spent in the target quadrant compared to the opposite quadrant were measured.
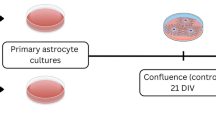
Hippocampal Primary Astrocyte Cultures from Newborn, Adult, and Aged Wistar Rats
Male Wistar rat groups (1, 90, and 180 days old) had their cerebral hippocampi aseptically dissected, on the same day, and meninges were removed. During the dissection, cerebral tissue was kept in Hank’s balanced salt solution (HBSS) containing 0.05 % trypsin and 0.003 % DNase and was kept at 37 °C for 8 min. The tissue was then mechanically dissociated for 7 min using a Pasteur pipette and centrifuged at 100g for 5 min. The pellet was resuspended in a solution of HBSS containing only 0.003 % DNase and again gently mechanically dissociated for 5 min with a Pasteur pipette and left for decantation for 20 min. The supernatant was collected and centrifuged for 7 min (400g). The cells from supernatant were resuspended in DMEM/F12 [10 % fetal bovine serum (FBS), 15 mM HEPES, 14.3 mM NaHCO3, and 0.04 % gentamicin], plated in 6- or 24-well plates pre-coated with poly-L-lysine and cultured at 37 °C in incubator with 5 % CO2. The cells were seeded at 3–5 × 105 cells/cm2. The first medium exchange occurred 24 h after obtaining a culture. During the first week, the medium change occurred once every 2 days and from the second week on, the medium change occurred once every 4 days. In cultures obtained from newborn rats, the cells reached confluence (the point that all cultures from all ages present the same number of adherent cells in culture plates) by approximately the second to third week. From the third week on, hippocampal astrocytes from 90- and 180-day-old rats received the culture medium supplemented with 20 % FBS. Around the third to fourth week, the cells reached confluence and were used for the experiments. The purity of the primary astrocyte cultures was assessed by immunocytochemistry for GFAP. OX-42 (CD11b/c) and NeuN were used as microglial and neuronal markers, respectively. Under these conditions, cell cultures were confirmed to be more than 98 % positive for GFAP, indicating the astrocytic phenotype. Furthermore, approximately 2 % of the astrocyte cell cultures stained positive for OX-42 [21].
Immunofluorescence Analysis
Immunofluorescence was performed as described previously by our group [21]. Cell cultures were fixed with 4 % paraformaldehyde for 20 min and permeabilized with 0.1 % Triton X-100 in PBS for 5 min at room temperature. After blocking overnight with 4 % albumin, the cells were incubated overnight with anti-GFAP (1:400), anti-vimentin (1:800), anti-GLT-1 (1:400), anti-GLAST (1:400), anti-GS (1:10,000), anti-NeuN (1:50), anti-β-tubulin III (1:500), or anti-CD11 (1:400) at 4 °C, followed by PBS washes and incubation with a specific secondary antibody conjugated with Alexa Fluor® 488 (green staining) or 594 (red staining) for 1 h at room temperature. For all the immunostaining-negative control reactions, the primary antibody was omitted. No reactivity was observed when the primary antibody was excluded. For actin-labeling analyses, the cells were incubated with 10 mg/ml rhodamine-labeled phalloidin in PBS for 45 min and two washes with PBS. Cell nuclei were stained with 0.2 mg/ml of 4ʹ,6ʹ-diamino-2-phenylindole (DAPI). Astrocytes were analyzed and photographed with a Nikon microscope and a TE-FM Epi-Fluorescence accessory.
Western Blot Analysis
Astrocytes were solubilized in lyses solution containing 4 % SDS, 2-mM EDTA and 50-mM Tris–HCl (pH 6.8). Samples were separated by SDS/PAGE (45 mg protein per sample), and transferred to nitrocellulose membranes, which were then incubated overnight (4 °C) with one of the following antibodies: anti-GFAP (1:1000), anti-vimentin (1:3000), anti-GLT-1 (1:200), anti-GLAST (1:2000), anti-GS (1:20,000), anti-HO-1 (1:1000), anti-phospho p38 (p-p38; 1:1000), or anti-GAPDH (1:3000). GAPDH was used as a loading control. Then, the membranes were incubated with a peroxidase-conjugated anti-rabbit immunoglobulin (IgG) or with peroxidase-conjugated anti-mouse (IgG) at a dilution of 1:3000 for 2 h. Chemiluminescence signals were detected in an Image Quant LAS4010 system (GE Healthcare) using an ECL kit [22]. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
GS Activity
The enzymatic assay was performed as described previously [21]. The cell lysate, suspended in 140 mM KCl, was added to the reaction mixture containing (in mM): 10 of MgCl2, 50 of L-glutamate, 100 of imidazole-HCl buffer (pH 7.4), 10 of 2-mercaptoethanol, 50 of hydroxylamine-HCl, and 10 of ATP, and incubated for 15 min at 37 °C. The reaction was stopped by the addition of a solution containing (in mM): 370 of ferric chloride, 670 of HCl and 200 of trichloroacetic acid. After centrifugation, the absorbance of the supernatant was measured at 530 nm and compared to the absorbance generated using standard quantities of γ-glutamyl hydroxamate treated with a ferric chloride reagent. The results are expressed in micromole per milligram protein per minute.
RNA Extraction and Quantitative RT-PCR
Total RNA was isolated from newborn, adult, and aged astrocyte cultures using TRIzol Reagent (Invitrogen, Carlsbad, CA). The concentration and purity of the RNA were determined spectrophotometrically at a ratio of 260:280. Then, 1 μg of total RNA was reverse transcribed using Applied Biosystems™ High-Capacity complementary DNA (cDNA) Reverse Transcription Kit (Applied Biosystems, Foster City, CA) in a 20 μL reaction according to manufacturer’s instructions. Quantitative RT-PCR was performed using a reaction mix containing cDNA (5 μL), primer pairs, and the Power SYBR Green PCR Master Mix (15 μl; Invitrogen) for amplification in duplicate using the Applied Biosystems 7500 Fast system. Primers used for quantitative RT-PCR analysis of p21, Nrf2, NFκB, iNOS, COX-2, and β-actin are listed on Table 1. No-template and no-reverse transcriptase controls were included in each assay, and these produced no detectable signal during the 40 cycles of amplification. Target messenger RNA (mRNA) levels were normalized to β-actin levels and expressed relative to the levels in newborn cultures using the 2-ΔΔCt method [23].
NFκB Levels
Levels of NFκB p65 in the nuclear fraction, which had been isolated from lysed cells by centrifugation, were measured using an ELISA commercial kit from Invitrogen (USA). The results are expressed as percentages relative to the control levels. The ELISA kit detects a minimum of 50.0 pg/ml.
Mitochondrial Membrane Potential-ΔΨm (JC-1 Assay)
To determine the ΔΨm, astrocytes were incubated for 30 min with JC-1 (5,5ʹ,6,6ʹ-tetrachloro-1,1ʹ,3,3ʹ-tetraethylbenzimidazolylcarbocyanine iodide, 2 μg/ml) [24]. Cells were then homogenized and centrifuged, washed once with HBSS, and transferred to a 96-well plate. Fluorescence was measured using an excitation wavelength of 485 nm and emission wavelengths of 540 and 590 nm. The ΔΨm was calculated using the ratio of 590 nm (red fluorescent J-aggregates) to 540 nm (green monomers). The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
DCFH Oxidation
Intracellular ROS production was detected using DCFH-DA [22]. DCFH-DA was added to the medium at a concentration of 10 μM and cells were incubated for 30 min at 37 °C. Following DCFH-DA exposure, the cells were scraped into phosphate-buffered saline with 0.2 % Triton X-100. The fluorescence was measured in a plate reader (Spectra Max GEMINI XPS, Molecular Devices, USA) with excitation at 485 nm and emission at 520 nm. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
RNA Oxidation
Total RNA was isolated from newborn, adult, and aged astrocyte cultures using TRIzol Reagent (Invitrogen, Carlsbad, CA). The concentration and purity of RNA were determined spectrophotometrically at a ratio of 260:280. The RNA oxidation levels were carried out using a rat ELISA kit from Cayman Chemical specific for 8-hydroxyguanosine. The results are expressed as fold relative to hippocampal primary astrocytes from newborn Wistar rats.
Superoxide Levels
Superoxide levels were determined using the superoxide anion assay kit from Sigma. The kit includes a superoxide anion producing system (xanthine/xanthine oxidase) for a positive control and the superoxide dismutase enzyme for the repression of the system, used as a negative control. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
NOX Activity
NADPH oxidase (NOX) activity was measured in cell lysate suspended in a sodium phosphate buffer with 140 mM KCl and protease mixture inhibitor using a modified assay [25]. This luminescence assay used lucigenin as the electron acceptor generated by the NADPH oxidase complex. NOX assay solution with 5 μM of lucigenin was used and the concentration of NADPH (1 μM to 1 mM) that used as the substrate, fell well within the linear range of the assay. The data were converted to relative light units per minute per milligram of protein, using a standard curve generated with xanthine/xanthine oxidase. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
Superoxide Dismutase Activity
Superoxide dismutase (SOD) activity was determined using the RANSOD kit from Randox (Autrim, UK). The SOD activity in lysed cells was assayed spectrophotometrically at 505 nm. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
Catalase Activity
Catalase (CAT) activity was assayed by the method described previously [25]. The decrease absorbance at 240 nm was measured in cell lysate suspended in a reaction medium containing 20 mM H2O2, 0.1 % Triton X-100, 10 mM potassium phosphate buffer, pH 7.0, and 50 μg protein. One unit (U) of enzyme activity is defined as 1 μmol of H2O2 consumed per minute. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
Glutathione Peroxidase Activity
Glutathione peroxidase (GPx) activity was measured using the RANSEL kit from Randox (Autrim, UK). The concentration of GPx in lysed cells is assessed by measuring the absorption of NADPH at 340 nm. The results are expressed as percentages relative to hippocampal primary astrocytes from newborn Wistar rats.
GSH Levels
GSH levels were assessed as described previously [21]. Cell lysate suspended in a sodium phosphate buffer with 140-mM KCl was diluted with a 100-mM sodium phosphate buffer (pH 8.0) containing 5-mM EDTA, and the protein was precipitated with 1.7 % meta-phosphoric acid. The supernatant was assayed with o-phthaldialdehyde (at a concentration of 1 mg/ml methanol) at 22 °C for 15 min. Fluorescence was measured using excitation and emission wavelengths of 350 and 420 nm, respectively. A calibration curve was performed with standard GSH solutions at concentrations ranging from 0 to 500 μM. The results are expressed in nanomole per milligram protein.
Inflammatory Response Measurement
The TNF-α levels were measured in an extracellular medium using a rat TNF-α ELISA kit from Peprotech. The levels of interleukins were measured in an extracellular medium using ELISA kits for IL-1β, IL-6, IL-10, and IL-18 from eBioscience and MCP-1 levels were measured using an ELISA kit from Invitrogen. The results are expressed in nanogram per milliliter. The average minimum sensitivity of the ELISA kit detection is 0.4 ng/ml of cytokines.
Trophic Factor Measurement
The GDNF, BDNF, S100B, and TGF-β levels were measured in an extracellular medium, using commercial ELISA kits from Promega for GDNF and BDNF, and kits from R&D Systems for S100B and TGF-β. The results are expressed in nanogram per milliliter or picogram per milliliter. The ELISA kits detect a minimum of 31.2 pg/ml for GDNF; 15.6 pg/ml for BDNF; 2.4 ng/ml for S100B, and 15.4 pg/ml for TGF-β.
Protein Determination
Protein content was measured using Lowry’s method with bovine serum albumin as a standard [26].
Statistical Analyses
All data are presented as the mean ± S.E.M. Comparisons between hippocampal astrocytes from newborn, adult, and aged Wistar rats were analyzed statistically using a one-way analysis of variance (ANOVA). Tukey’s test was employed for post hoc analysis. P values <0.05 were considered significant.
Results
Behavioral Effects
The Morris water maze task was used to evaluate reference memory, which is intimately associated with the hippocampal activity, in adult and aged Wistar rats. The time to find the platform (Fig. 1a), the time spent in the target quadrant (Fig. 1b), and the number of crossings over the platform location (Fig. 1c) did not decline with age.
Evaluation of the cognitive performance of adult and aged Wistar rats using Morris water maze. a Performance in the reference memory protocol, based on escape latency. Each line represents the mean ± S.E.M. (n = 10). b Memory in the probe trial of the reference memory, as measured by time spent (s) in the target quadrant. c Number of crossings over the platform position. The data represent the mean ± S.E.M. (n = 10). One-way ANOVA followed by Tukey’s test were used as statistical analysis
Astrocytes from Adult and Aged Rats Presented Classical Cytoskeleton Proteins
Typically, cultured rat astrocytes show a polygonal to fusiform and flat morphology, and these characteristics were also observed here in hippocampal astrocytes from adult and aged Wistar rats (Fig. 2a). Furthermore, actin cytoskeleton is the major determinant of the cell morphology, and our astrocyte cultures showed significant staining for actin with parallel arrangement of stress fiber organization at 7 days in vitro until confluence (Fig. 2a).
Cellular morphology and expression of classical cytoskeleton markers in hippocampal astrocytes. a Representative cell morphology and immunostaining for actin at 7 days in vitro and at confluence in adult and aged astrocytes. b Immunofluorescence analysis for GFAP (at 7 days in vitro and at confluence) and vimentin. c Representative immunoblots of GFAP and vimentin. The bar graph corresponds to the mean ± S.E.M. and represents the percentages relative to newborn astrocytes (adopted as control conditions). The data were generated in four independent experiments and analyzed statistically using a one-way ANOVA followed by Tukey’s test. Asterisk indicates significant differences from newborn astrocytes.*p < 0.05; **p < 0.01
To ensure that adult and aged hippocampal astrocytes serve as a model for studies of glial functionality in the aging brain, we performed several experimental paradigms comparing astrocyte cultures from newborn, adult, and aged Wistar rats. First, the purity of the astrocyte cultures was assessed using cytoskeletal protein GFAP. Immunocytochemical analysis showed an intense cytoplasmic immunolabeling for GFAP (Fig. 2b). Additionally, astrocytes, even with actin, were staining for GFAP from 7 days in vitro up to confluence (Fig. 2b). Moreover, in primary cultured astrocytes, vimentin is coexpressed with GFAP. Thus, Fig. 2b also illustrates that vimentin staining exhibited a meshwork extending across the cytoplasm. Immunoblotting analysis showed a decrease in the expression of GFAP and vimentin in astrocytes from adult and aged rats compared to newborn cultures (Fig. 2c).
Age-Related Changes in Glutamate Transporters and Glutamine Synthetase in Astrocytes
Astrocytes are responsible for clearing extracellular glutamate, due to their high-affinity glutamate transporters, GLAST and GLT-1 [27]. Thus, the immunocytochemistry labeling of astrocytes shows a high immunoreactivity for GLAST and GLT-1 (Fig. 3a). In addition, adult and aged astrocytes display an age-dependent decrease for GLAST expression levels (Fig. 3b). Otherwise, we did not observe changes in the expression of GTL-1 in astrocytes from adult rats; however, there was an increase in the GLT-1 expression in aged astrocytes (Fig. 3b).
Age-dependent changes in glutamate transporters and glutamine synthetase in astrocytes. a Representative immunofluorescences for GLAST, GLT-1, and GS. b Quantification of GLAST, GLT-1, and GS protein levels. c GS activity. For immunoblots and GS activity, the data are expressed as the mean ± S.E.M. and represents the percentages relative to newborn astrocytes (adopted as control conditions). The data were generated in four independent experiments and analyzed statistically using a one-way ANOVA followed by Tukey’s test. Asterisk indicates significant differences from newborn astrocytes.*p < 0.05; **p < 0.01
Once taken up by astrocytes, glutamate is converted into glutamine by GS, which is constitutively expressed by astrocytes. Figure 3a shows the immunofluorescence of GS for astrocytes. The western blotting analysis indicates that GS expression (Fig. 3b) and GS activity decreased with aging in astrocyte cultures (25 and 40 % decreases in adult and aged astrocytes, respectively, compared to newborn, Fig. 3c).
Adult and Aged Astrocytes Increased p21 Senescence-Associated Gene Transcription
The transcription of cell cycle inhibitory genes such as p21 is considered a biomarker for cellular senescence. In line with this, we observed a significant increase in the mRNA expression levels of p21 in adult (20 %) and aged (35 %) astrocytes (Fig. 4). The results suggest that our hippocampal astrocytes serve as a model for brain aging studies.
Changes in the p21 senescence-associated gene in astrocytes. Quantification of mRNA expression levels by RT-PCR. The data are expressed as the mean ± S.E.M. and represents the percentages relative to newborn astrocytes (adopted as control conditions). The data were generated in four independent experiments and analyzed statistically using a one-way ANOVA followed by Tukey’s test. Asterisk indicates significant differences from newborn astrocytes.*p < 0.05; **p < 0.01
Nrf2 and NFκB Pathways as Key Targets in Astrocytes Aging
To investigate signaling pathways associated with oxidative/nitrosative stress and inflammation in hippocampal astrocytes, we evaluated the transcriptional activity of Nrf2 and NFκB pathways. Quantitative RT-PCR revealed a decrease, in an age-dependent manner, in mRNA expression levels of Nrf2, an antioxidant transcription factor (Fig. 5a). Nrf2 regulates the transcription of HO-1, which may mediate neuroprotection against stressful conditions. The immunoblotting studies for HO-1 revealed a reduction of the expression levels in only aged astrocytes (Fig. 5b). Nrf2 is an upstream signal of NFκB, and there was a significantly increase, with age, in the mRNA expression levels of p65 NFκB as well as its transcriptional activity, as shown in Fig. 5c, d, respectively. p38 MAPK may control the transcriptional activity of NFκB in astrocytes [14]. Therefore, we evaluated whether p38 protein levels could be changed in hippocampal astrocytes and we also observed its increase with age (Fig. 5e).
Signaling pathways involved in age-dependent glial responses in astrocytes. RT-PCR quantification of mRNA expression levels of a Nrf2, c p65 NFκB, and d transcriptional activity of p65 NFκB. The mRNA levels are given relative to the newborn astrocytes (adopted as control conditions) and represent the mean ± S.E.M. of four independent experimental determinations, performed in triplicate. Immunolabeling of b HO-1 and e p-p38 MAPK protein levels. The data are expressed as percentages relative to newborn astrocytes and represent mean ± S.E.M. of four independent experiments, performed in triplicate. The data were analyzed statistically using a one-way ANOVA followed by a Tukey’s test. Asterisk indicates significant differences from newborn astrocytes. *p < 0.05; **p < 0.01
Oxidative Stress Increased with Age in Hippocampal Astrocytes
Mitochondria are the primary site of ROS production. Thus, we observed an age-dependent decrease in the ΔΨm in adult (15 %) and aged (25 %) astrocytes (Fig. 6a), as well as an increase in intracellular ROS production (25 and 35 %, respectively, for adult and aged astrocytes, Fig. 6b). Another potential consequence of ROS production is the oxidation of nucleic acids. Accordingly, we measured RNA oxidation, which is a highly sensitive biomarker for oxidative stress (Fig. 6c). There was a significant age-related increase in RNA oxidation levels in adult (32 %) and aged (45 %) astrocytes when compared to newborn cultures.
Characterization of the oxidative stress profile in cultured astrocytes. a The mitochondrial membrane potential (ΔΨm). b Intracellular ROS production. c RNA oxidation levels. d Superoxide levels. e NOX activity. f RT-PCR quantification of mRNA expression levels of iNOS. Determination of the activities of the antioxidant enzymes: g SOD, h CAT, and i GPx. j GSH content. The data are expressed relative to newborn astrocytes (adopted as control conditions) and represent mean ± S.E.M. of four independent experiments, performed in triplicate. The data were analyzed statistically using a one-way ANOVA followed by a Tukey’s test. Asterisk indicates significant differences from newborn astrocytes. *p < 0.05; **p < 0.01
Moreover, increasing evidence suggests that superoxide anion radicals produced via the superoxide-generating enzyme, NOX, might play a role in ROS production [28]. Thus, a substantial increase with age (adult 30 % and aged 40 %) in superoxide levels (Fig. 6d) and NOX activity (adult 45 % and aged 60 %, Fig. 6e) were observed in astrocytes. Additionally, nitric oxide (NO) can interact with superoxide anions, leading to the overproduction of peroxynitrite. iNOS catalyzes the synthesis of NO. Adult and aged astrocytes presented an age-dependent increase in the mRNA expression levels of iNOS (35 and 50 % for adult and aged astrocytes, respectively) (Fig. 6f).
Given that astrocytes may confer protection against age-related neurological diseases through antioxidant enzymatic and non-enzymatic defenses [29], we assessed the GSH content and the main enzymatic defenses, SOD, CAT, and GPx. SOD and CAT activities presented an age-dependent decrease in adult and aged astrocytes (Fig. 6g, h, respectively). However, Fig. 6i shows an age-related increase in GPx activity in adult and aged hippocampal astrocytes. Elevation of GPx activity may produce a reduction in GSH content. Thus, GSH levels decreased significantly with age, in adult and aged astrocytes (Fig. 6j).
Characterization of the Inflammatory Response and Release of Trophic Factors in Adult and Aged Astrocytes
Astrocytes actively participate in the inflammatory response releasing anti- and proinflammatory cytokines and chemokines [1]. To characterize the inflammatory response in astrocytes, classical anti- and proinflammatory cytokines were measured. As shown in Fig. 7, levels of TNF-α (7A), IL-1β (7B), IL-6 (7C), and IL-18 (7D) were significantly enhanced in an age-dependent manner in astrocytes. However, the anti-inflammatory IL-10 levels were not altered in different astrocyte-age cultures (Fig. 7e). Levels of chemokine MCP-1 were increased in adult and aged astrocytes (Fig. 7f). In addition, we evaluated the mRNA levels of the proinflammatory enzyme COX-2, which also increased in adult and aged astrocytes (Fig. 7g).
Characterization of inflammatory response in astrocytes. a TNF-α, b IL-1β, c IL-6, d IL-18, e IL-10, and f MCP-1 levels. g RT-PCR quantification of mRNA expression levels of COX-2. The data represent the mean ± S.E.M. of five independent experiments, performed in triplicate. The mRNA expression levels of COX-2 were performed in four independent experiments, in triplicate. The data were analyzed statistically using a one-way ANOVA followed by a Tukey’s test. Asterisk indicates significant differences from newborn astrocytes. *p < 0.05; **p < 0.01
Next, we investigated the protective role of astrocytes by releasing trophic factors, such as GDNF, BDNF, S100B protein, and TGF-β. In this instance, GDNF and BDNF levels decreased with age in astrocytes (Fig. 8a, b, respectively). Opposite trends were observed for S100B and TGF-β levels, which increased in an age-dependent manner (Fig. 8c, d, respectively).
Changes in trophic factors in cultured astrocytes. a GDNF, b BDNF, c S100B, and d TGF-β levels. The data represent the mean ± S.E.M. of five independent experiments, performed in triplicate, and analyzed statistically using a one-way ANOVA followed by a Tukey’s test. Asterisk indicates significant differences from newborn astrocytes. *p < 0.05; **p < 0.01
Discussion
Astrocytes are dynamic cells that maintain brain homeostasis regulating neural survival and development. Brain aging is accompanied by changes in astrocyte functionality, that are strongly associated with oxidative stress and inflammatory response [11, 12, 30, 31]. Moreover, the hippocampus is the most vulnerable cerebral structure to aging, suffering from a decline in synaptic function that can lead to dementia [32]. Thus, we have now generated a cell culture model of hippocampal astrocytes from adult and aged rats that reproduces the main glial changes observed in aging brain. Significant alterations in astrocyte marker proteins, redox homeostasis, inflammatory response, and signaling pathways were observed with aging. Our cell culture model might be an important step in better understanding the role of hippocampal astrocytes in brain aging under physiological and pathological conditions. In this way, astrocytes may emerge as a therapeutic target for age-related diseases.
Although p21 senescence-associated gene and classical astrocyte markers changed their expressions with age, there were no differences in cognitive function between adult and aged rats. Thus, our results may suggest that glial changes precede behavioral effects. Astrocyte senescence directly affects synaptic transmission, which is linked to age-related neurodegenerative diseases [33, 34]. Astrocytic GFAP expression profile is not a consensus for primary cultures [9, 18, 35, 36]. Here, we observed a decrease in GFAP expression that can reflect astroglial degeneration, which has been detected at the early stages of age-related neurodegenerative diseases [9, 19]. Our present data suggests that the oxidative and inflammatory phenotype observed in adult and aged rats may precede the increase of GFAP expression. Vimentin expression decreases with development, as it is progressively replaced by GFAP [36, 37]. However cultures co-express vimentin and GFAP [22, 37]. Adult and aged astrocytes showed decreased levels of vimentin expression, attesting to the utility our cell culture model for aging studies. Additionally, GFAP and vimentin appear to be involved in cell shape maintenance, CNS cytoarchitecture, mechanical stability, and synaptic function, properties that are strongly affected by aging [36].
Astrocytes perform the majority of glutamate uptake in the brain through the glutamate transporters GLAST and GLT-1, which are expressed almost exclusively in astrocytes [38]. Expression patterns vary during development with a predominance of GLAST expression at early stages, and progressively, more GLT-1 expression is observed with maturity [39–41]. The pathophysiology of age-related neurological disorders involves selective alterations in glutamate transporters expression, and significant decrease in GLT-1 content was observed in Alzheimer’s disease in vivo and in vitro models [42]. In line with this, our hippocampal astrocytes provide a means of assessing these influences.
Astrocytes also metabolize glutamate to glutamine via GS. In the CNS, GS is an enzyme expressed only in astrocytes and it is essential for maintaining the glutamate-glutamine cycle for glutamate/GABA-based neurotransmission [19, 43, 44]. The age-dependent decrease in GS expression and activity may affect both excitatory and inhibitory neurotransmission [9, 19]. Additionally, GS activity is very sensitive to oxidative and nitrosative stress, which was shown to increase with aging [9, 19]. Moreover, oxidative metabolism in aged astrocytes may limit the ability of astrocytes to supply neurons with metabolic substrates, and impairment in GS activity directly contributes to this condition [11].
The transcriptional factor Nrf2 mediates neuroprotection, allowing for adaptation and survival under stress conditions by regulating the gene expression of diverse networks of cytoprotective proteins, including antioxidant, anti-inflammatory and detoxification enzymes [45, 46]. Data from Nrf2 indicate that reduced translocation into the nucleus may be a primary response to changes in redox homeostasis and inflammation [47]. Our findings were corroborated by other reports, which show that Nrf2 transcriptional activity decreases with age. Nrf2 regulates the biosynthesis, utilization and regeneration of GSH, and thus controls the production of ROS by mitochondria and NOX [46, 48]. Nrf2 also controls the p21 senescence gene and HO-1 expression, a fundamental defense mechanism for cells exposed to oxidant challenges [17, 49]. HO-1 counteracts NO production by inhibiting iNOS activity [17]. Another important regulation of Nrf2 and HO-1 pathways is the control of NFκB.
NFκB is characteristically considered the major inflammatory mediator in the CNS because it regulates the release of proinflammatory cytokines and consequently participates in the pathology of neuroinflammatory disorders. There is ample evidence that NFκB increases with age, and the most identified signal for this activation is the elevation of NFκB p65 levels in the nucleus [11, 12, 50]. Ghosh et al. demonstrated that expression of NFκB induces astrocytic GLT-1-mediated transport activity, and this report corroborates our data since we observed an increase in GLT-1 expression in aged hippocampal astrocytes [39]. Moreover, NFκB activation may be a link between oxidative/nitrosative stress and inflammatory response, because its activation resulted in increased expression of iNOS, leading to elevated NO production and proinflammatory cytokine release. The MAPK pathway is also associated with oxidative/nitrosative stress and inflammatory response because p38 MAPK regulates NFκB translocation, which may be an early event for the activation [14]. In line with this, alterations in the mechanisms underlying Nrf2, HO-1, NFκB, and p38 pathways found in this study may explain the age-related changes in oxidative stress and inflammatory response in hippocampal astrocytes.
Oxidative stress is typically a major cause of brain aging, because it serves as a common feature associated with excitotoxicity and inflammation, both of which are processes linked to aging and neurodegenerative diseases [12, 51, 52]. Mitochondria and NOX are primarily involved in ROS production in the CNS, and there is increasing evidence supporting the association between mitochondrial dysfunction/NOX and aging [28]. Moreover, superoxide generated by NOX activation can lead to severe oxidative damage and neural death [28, 53, 54]. Furthermore, as shown in this study, adult and aged astrocytes induced RNA oxidation, which may affect gene expression and local protein synthesis and thereby provide another link between oxidative/nitrosative stress and brain aging. Additionally, inflammatory response may induce RNA oxidation [55], thus contributing to cellular senescence [56].
The oxidative damage induced during aging may be related to a decrease in antioxidant and repair systems. In this sense, enzymes such as SOD, CAT, and GPx, can determine the clearance of free radicals [57]. The age-dependent decrease in SOD and the CAT activities observed in hippocampal astrocytes may stimulate an overproduction of superoxide and H2O2, molecules which together with excessive NO production (via iNOS activity) cause severe cellular injury [10, 11, 57]. Moreover, SOD released from astrocytes is hypothesized to protect GSH by reducing the production of superoxide [58]. In addition, the increase in GPx activity may induce decreased levels of GSH, which may contribute to excitotoxicity because it may increase the vulnerability of glutamate transporters to oxidation [59]. GSH is the main antioxidant defense of the brain and depletion of its content induces an excessive inflammatory response in age-related neurodegenerative diseases [29]. Our data present divergent results from a previous report by Liddell et al., who demonstrated that astrocytes retain their antioxidant capacity into advanced old age as evinced by GSH content and GPx activity [60]. This fact might be due to differences in the rodent species and brain structures used in these studies, because they utilized the whole brain and we only utilized the hippocampus.
Oxidative/nitrosative stress also plays a critical role in inflammatory response, by increasing TNF-α levels. TNF-α induces astrocyte activation and is closely associated with increases in iNOS expression [61]. TNF-α is the first signal to enhance other proinflammatory cytokines, such as IL-1β, which act as acute inflammatory response. Moreover, TNF-α and IL-1β are essential for the production and release of IL-6 [62]. Furthermore, IL-18 (a member of the IL-1 superfamily) induces inflammatory processes and is strictly associated with neurodegenerative diseases [63]. The levels of TNF-α, IL-1β, IL-6, and IL-18 increase in the cerebral cortex and hippocampus during aging [64]. Moreover, the anti-inflammatory effect of IL-10 is related to the inhibition of TNF-α secretion and we did not observed a modification in IL-10 levels, indicating the possibility of an increase inflammatory response in hippocampal astrocytes [65]. IL-10 is also capable of exerting a rapid neuroprotection through delaying NFκB activation [64]. This pathway was also shown to increase chemokine MCP-1, which has a key role in the generation of chronic inflammation in the aging brain and in the pathology of Alzheimer’s disease [66, 67]. MCP-1 likewise activates the p38 MAPK pathway in the CNS. Additionally, proinflammatory cytokines up regulate COX-2 expression, which may be activated by NFκB. In turn, the increase in COX-2 activity potentiates the inflammatory response [68].
Trophic factors secreted by astrocytes are essential for the proliferation, survival, and maturation of neural cells [7]. Astrocytes may influence brain development via the release of trophic factors and adult astrocytes from the hippocampus are specific cells that can promote neurogenesis [69–71]. In this sense GDNF, BDNF, S100B, and TGF-β can play protective, reparative, or biomarker roles when secreted by astrocytes. Regarding GDNF and BDNF, their decrease with age may be associated with the pathophysiology of neurodegeneration [7], although their increased levels may protect neurons from metabolic and excitotoxic insults [72]. Additionally, the expressions of GDNF and BDNF in astrocytes may be modulated by HO-1 [73]. The S100B protein exerts both intracellular and extracellular functions [8]. As an extracellular factor, S100B may be a biomarker for Alzheimer’s disease and neuropsychiatric disorders [74]. Moreover, S100B via receptor for advanced glycation end products (RAGE) activates overproduction of ROS and inflammatory cytokines, triggering damaging and aging events [75]. Furthermore, GDNF and BDNF are able to increase S100B levels [75]. TGF-β signaling increases with age and mediates the initiation and regulation of CNS immune responses, participates in glial scar formation, and accelerates age-related neurological disorders [76, 77].
In conclusion, hippocampal astrocytes from adult and aged rats represent a new tool that reproduces the changes in glial functionality observed in the aging brain. NFκB, p38, Nrf2, and HO-1 pathways are probably linked to changes in the astrocyte-specific cytoskeleton, senescence markers, glutamate metabolism, mitochondrial function, oxidative/nitrosative stress, inflammatory response, and trophic factors. Our cell culture model provides a powerful in vitro tool for studying the cellular, biochemical, and molecular properties of hippocampal astrocytes, which can further be applied to study the role of astrocytes in in vivo and in vitro experimental models of neurotoxicity and neuroprotection. Through understanding these functions, astrocytes may emerge as a target for preventive/therapeutic strategies and astrocyte-specific drug discovery for age-related neurological diseases.
References
Farina C, Aloisi F, Meinl E (2007) Astrocytes are active players in cerebral innate immunity. Trends Immunol 28(3):138–145. doi:10.1016/j.it.2007.01.005
Hartline DK (2011) The evolutionary origins of glia. Glia 59(9):1215–1236. doi:10.1002/glia.21149
Kettenmann H, Verkhratsky A (2008) Neuroglia: the 150 years after. Trends Neurosci 31(12):653–659. doi:10.1016/j.tins.2008.09.003
Maragakis NJ, Rothstein JD (2006) Mechanisms of disease: astrocytes in neurodegenerative disease. Nat Clin Pract Neurol 2(12):679–689. doi:10.1038/ncpneuro0355
Wang DD, Bordey A (2008) The astrocyte odyssey. Prog Neurobiol 86(4):342–367. doi:10.1016/j.pneurobio.2008.09.015
Clarke LE, Barres BA (2013) Emerging roles of astrocytes in neural circuit development. Nat Rev Neurosci 14(5):311–321. doi:10.1038/nrn3484
Markiewicz I, Lukomska B (2006) The role of astrocytes in the physiology and pathology of the central nervous system. Acta Neurobiol Exp (Wars) 66(4):343–358
Donato R (2003) Intracellular and extracellular roles of S100 proteins. Microsc Res Tech 60(6):540–551. doi:10.1002/jemt.10296
Rodriguez-Arellano JJ, Parpura V, Zorec R, Verkhratsky A (2015) Astrocytes in physiological aging and Alzheimer’s disease. Neuroscience. doi:10.1016/j.neuroscience.2015.01.007
Alarcon-Aguilar A, Luna-Lopez A, Ventura-Gallegos JL, Lazzarini R, Galvan-Arzate S, Gonzalez-Puertos VY, Moran J, Santamaria A et al (2014) Primary cultured astrocytes from old rats are capable to activate the Nrf2 response against MPP+ toxicity after tBHQ pretreatment. Neurobiol Aging 35(8):1901–1912. doi:10.1016/j.neurobiolaging.2014.01.143
Jiang T, Cadenas E (2014) Astrocytic metabolic and inflammatory changes as a function of age. Aging Cell 13(6):1059–1067. doi:10.1111/acel.12268
Miller DB, O’Callaghan JP (2005) Aging, stress and the hippocampus. Ageing Res Rev 4(2):123–140. doi:10.1016/j.arr.2005.03.002
Niccoli T, Partridge L (2012) Ageing as a risk factor for disease. Curr Biol 22(17):R741–R752. doi:10.1016/j.cub.2012.07.024
Gorina R, Font-Nieves M, Marquez-Kisinousky L, Santalucia T, Planas AM (2011) Astrocyte TLR4 activation induces a proinflammatory environment through the interplay between MyD88-dependent NFkappaB signaling, MAPK, and Jak1/Stat1 pathways. Glia 59(2):242–255. doi:10.1002/glia.21094
Vargas MR, Johnson JA (2009) The Nrf2-ARE cytoprotective pathway in astrocytes. Expert Rev Mol Med 11:e17. doi:10.1017/S1462399409001094
Gorg B, Karababa A, Shafigullina A, Bidmon HJ, Haussinger D (2015) Ammonia-induced senescence in cultured rat astrocytes and in human cerebral cortex in hepatic encephalopathy. Glia 63(1):37–50. doi:10.1002/glia.22731
Wakabayashi N, Slocum SL, Skoko JJ, Shin S, Kensler TW (2010) When NRF2 talks, who’s listening? Antioxid Redox Signal. doi:10.1089/ars.2010.3216
Orre M, Kamphuis W, Osborn LM, Melief J, Kooijman L, Huitinga I, Klooster J, Bossers K et al (2014) Acute isolation and transcriptome characterization of cortical astrocytes and microglia from young and aged mice. Neurobiol Aging 35(1):1–14. doi:10.1016/j.neurobiolaging.2013.07.008
Rodriguez JJ, Yeh CY, Terzieva S, Olabarria M, Kulijewicz-Nawrot M, Verkhratsky A (2014) Complex and region-specific changes in astroglial markers in the aging brain. Neurobiol Aging 35(1):15–23. doi:10.1016/j.neurobiolaging.2013.07.002
Rodrigues L, Biasibetti R, Swarowsky A, Leite MC, Quincozes-Santos A, Quilfeldt JA, Achaval M, Goncalves CA (2009) Hippocampal alterations in rats submitted to streptozotocin-induced dementia model are prevented by aminoguanidine. J Alzheimers Dis 17(1):193–202. doi:10.3233/JAD-2009-1034
Bellaver B, Souza DG, Souza DO, Quincozes-Santos A (2014) Resveratrol increases antioxidant defenses and deceases proinflammatory cytokines in hippocampal astocyte cultures from newborn, adult and aged Wistar rats. Toxicol in Vitro 28:479–484. doi:10.1016/j.tiv.2014.01.006
Souza DG, Bellaver B, Souza DO, Quincozes-Santos A (2013) Characterization of adult rat astrocyte cutures. PLoS One 8:E60282. doi:10.1371/journal.pone.0060282
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−delta delta C(T)) method. Methods 25(4):402–408. doi:10.1006/meth.2001.1262
Bellaver B, Souza DG, Bobermin LD, Goncalves CA, Souza DO, Quincozes-Santos A (2015) Guanosine inhibits LPS-induced pro-inflammatory response and oxidative stress in hippocampal astrocytes through the heme oxygenase-1 pathway. Purinergic Signal. doi:10.1007/s11302-015-9475-2
Quincozes-Santos A, Bobermin LD, Souza DG, Bellaver B, Goncalves CA, Souza DO (2014) Guanosine protects C6 astroglial cells against azide-induced oxidative damage: a putative role of heme oxygenase 1. J Neurochem 130(1):61–74. doi:10.1111/jnc.12694
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193(1):265–275
Benarroch EE (2010) Glutamate transporters: diversity, function, and involvement in neurologic disease. Neurology 74(3):259–264. doi:10.1212/WNL.0b013e3181cc89e3
Brennan AM, Suh SW, Won SJ, Narasimhan P, Kauppinen TM, Lee H, Edling Y, Chan PH et al (2009) NADPH oxidase is the primary source of superoxide induced by NMDA receptor activation. Nat Neurosci 12(7):857–863. doi:10.1038/nn.2334
Lee M, Cho T, Jantaratnotai N, Wang YT, McGeer E, McGeer PL (2010) Depletion of GSH in glial cells induces neurotoxicity: relevance to aging and degenerative neurological diseases. FASEB J 24(7):2533–2545. doi:10.1096/fj.09-149997
Heneka MT, Kummer MP, Latz E (2014) Innate immune activation in neurodegenerative disease. Nat Rev Immunol 14(7):463–477. doi:10.1038/nri3705
Kohman RA, Rhodes JS (2013) Neurogenesis, inflammation and behavior. Brain Behav Immun 27(1):22–32. doi:10.1016/j.bbi.2012.09.003
Yankner BA, Lu T, Loerch P (2008) The aging brain. Annu Rev Pathol 3:41–66. doi:10.1146/annurev.pathmechdis.2.010506.092044
Bhat R, Crowe EP, Bitto A, Moh M, Katsetos CD, Garcia FU, Johnson FB, Trojanowski JQ et al (2012) Astrocyte senescence as a component of Alzheimer’s disease. PLoS One 7(9):e45069. doi:10.1371/journal.pone.0045069
Kawano H, Katsurabayashi S, Kakazu Y, Yamashita Y, Kubo N, Kubo M, Okuda H, Takasaki K et al (2012) Long-term culture of astrocytes attenuates the readily releasable pool of synaptic vesicles. PLoS One 7(10):e48034. doi:10.1371/journal.pone.0048034
Desclaux M, Teigell M, Amar L, Vogel R, Gimenez YRM, Privat A, Mallet J (2009) A novel and efficient gene transfer strategy reduces glial reactivity and improves neuronal survival and axonal growth in vitro. PLoS One 4(7):e6227. doi:10.1371/journal.pone.0006227
Menet V, Gimenez y Ribotta M, Chauvet N, Drian MJ, Lannoy J, Colucci-Guyon E, Privat A (2001) Inactivation of the glial fibrillary acidic protein gene, but not that of vimentin, improves neuronal survival and neurite growth by modifying adhesion molecule expression. J Neurosci 21(16):6147–6158
Pertusa M, Garcia-Matas S, Rodriguez-Farre E, Sanfeliu C, Cristofol R (2007) Astrocytes aged in vitro show a decreased neuroprotective capacity. J Neurochem 101(3):794–805. doi:10.1111/j.1471-4159.2006.04369.x
Danbolt NC (2001) Glutamate uptake. Prog Neurobiol 65(1):1–105. doi:10.1016/S0301-0082(00)00067-8
Ghosh M, Yang Y, Rothstein JD, Robinson MB (2011) Nuclear factor-kappaB contributes to neuron-dependent induction of glutamate transporter-1 expression in astrocytes. J Neurosci 31(25):9159–9169. doi:10.1523/jneurosci.0302-11.2011
Benediktsson AM, Marrs GS, Tu JC, Worley PF, Rothstein JD, Bergles DE, Dailey ME (2012) Neuronal activity regulates glutamate transporter dynamics in developing astrocytes. Glia 60(2):175–188. doi:10.1002/glia.21249
Anderson CM, Swanson RA (2000) Astrocyte glutamate transport: review of properties, regulation, and physiological functions. Glia 32(1):1–14. doi:10.1002/1098-1136(200010)32:1<1::AID-GLIA10>3.0.CO;2-W
Schallier A, Smolders I, Van Dam D, Loyens E, De Deyn PP, Michotte A, Michotte Y, Massie A (2011) Region- and age-specific changes in glutamate transport in the AbetaPP23 mouse model for Alzheimer’s disease. J Alzheimers Dis 24(2):287–300. doi:10.3233/JAD-2011-101005
Belanger M, Allaman I, Magistretti PJ (2011) Brain energy metabolism: focus on astrocyte-neuron metabolic cooperation. Cell Metab 14(6):724–738. doi:10.1016/j.cmet.2011.08.016
Hertz L, Zielke HR (2004) Astrocytic control of glutamatergic activity: astrocytes as stars of the show. Trends Neurosci 27(12):735–743. doi:10.1016/j.tins.2004.10.008
Johnson JA, Johnson DA, Kraft AD, Calkins MJ, Jakel RJ, Vargas MR, Chen PC (2008) The Nrf2-ARE pathway: an indicator and modulator of oxidative stress in neurodegeneration. Ann N Y Acad Sci 1147:61–69. doi:10.1196/annals.1427.036
Dinkova-Kostova AT, Abramov AY (2015) The emerging role of Nrf2 in mitochondrial function. Free Radic Biol Med. doi:10.1016/j.freeradbiomed.2015.04.036
Motohashi H, Yamamoto M (2004) Nrf2-Keap1 defines a physiologically important stress response mechanism. Trends Mol Med 10(11):549–557. doi:10.1016/j.molmed.2004.09.003
Kovac S, Angelova PR, Holmstrom KM, Zhang Y, Dinkova-Kostova AT, Abramov AY (2015) Nrf2 regulates ROS production by mitochondria and NADPH oxidase. Biochim Biophys Acta 1850(4):794–801. doi:10.1016/j.bbagen.2014.11.021
Volonte D, Liu Z, Musille PM, Stoppani E, Wakabayashi N, Di YP, Lisanti MP, Kensler TW et al (2013) Inhibition of nuclear factor-erythroid 2-related factor (Nrf2) by caveolin-1 promotes stress-induced premature senescence. Mol Biol Cell 24(12):1852–1862. doi:10.1091/mbc.E12-09-0666
Mattson MP, Camandola S (2001) NF-kappaB in neuronal plasticity and neurodegenerative disorders. J Clin Invest 107(3):247–254. doi:10.1172/jci11916
Ye B, Shen H, Zhang J, Zhu YG, Ransom BR, Chen XC, Ye ZC (2015) Dual pathways mediate beta-amyloid stimulated glutathione release from astrocytes. Glia 63(12):2208–2219. doi:10.1002/glia.22886
Webster SJ, Van Eldik LJ, Watterson DM (2015) Closed head injury in an age-related Alzheimer mouse model leads to an altered neuroinflammatory response and persistent cognitive impairment. J Neurosci 35(16):6554–6569. doi:10.1523/jneurosci.0291-15.2015
Suh SW, Shin BS, Ma H, Van Hoecke M, Brennan AM, Yenari MA, Swanson RA (2008) Glucose and NADPH oxidase drive neuronal superoxide formation in stroke. Ann Neurol 64(6):654–663. doi:10.1002/ana.21511
Suh SW, Hamby AM, Gum ET, Shin BS, Won SJ, Sheline CT, Chan PH, Swanson RA (2008) Sequential release of nitric oxide, zinc, and superoxide in hypoglycemic neuronal death. J Cereb Blood Flow Metab 28(10):1697–1706. doi:10.1038/jcbfm.2008.61
Gorg B, Qvartskhava N, Keitel V, Bidmon HJ, Selbach O, Schliess F, Haussinger D (2008) Ammonia induces RNA oxidation in cultured astrocytes and brain in vivo. Hepatology 48(2):567–579. doi:10.1002/hep.22345
Nunomura A, Hofer T, Moreira PI, Castellani RJ, Smith MA, Perry G (2009) RNA oxidation in Alzheimer disease and related neurodegenerative disorders. Acta Neuropathol 118(1):151–166. doi:10.1007/s00401-009-0508-1
Droge W (2002) Free radicals in the physiological control of cell function. Physiol Rev 82(1):47–95. doi:10.1152/physrev.00018.2001
Stewart VC, Stone R, Gegg ME, Sharpe MA, Hurst RD, Clark JB, Heales SJ (2002) Preservation of extracellular glutathione by an astrocyte derived factor with properties comparable to extracellular superoxide dismutase. J Neurochem 83(4):984–991. doi:10.1046/j.1471-4159.2002.01216.x
Trotti D, Danbolt NC, Volterra A (1998) Glutamate transporters are oxidant-vulnerable: a molecular link between oxidative and excitotoxic neurodegeneration? Trends Pharmacol Sci 19(8):328–334. doi:10.1016/S0165-6147(98)01230-9
Liddell JR, Robinson SR, Dringen R, Bishop GM (2010) Astrocytes retain their antioxidant capacity into advanced old age. Glia 58(12):1500–1509. doi:10.1002/glia.21024
Tanabe K, Kozawa O, Iida H (2011) Midazolam suppresses interleukin-1beta-induced interleukin-6 release from rat glial cells. J Neuroinflammation 8:68. doi:10.1186/1742-2094-8-68
de Rivero Vaccari JP, Dietrich WD, Keane RW (2014) Activation and regulation of cellular inflammasomes: gaps in our knowledge for central nervous system injury. J Cereb Blood Flow Metab 34(3):369–375. doi:10.1038/jcbfm.2013.227
Bossu P, Ciaramella A, Salani F, Vanni D, Palladino I, Caltagirone C, Scapigliati G (2010) Interleukin-18, from neuroinflammation to Alzheimer’s disease. Curr Pharm Des 16(38):4213–4224. doi:10.2174/138161210794519147
Xie Z, Morgan TE, Rozovsky I, Finch CE (2003) Aging and glial responses to lipopolysaccharide in vitro: greater induction of IL-1 and IL-6, but smaller induction of neurotoxicity. Exp Neurol 182(1):135–141. doi:10.1016/S0014-4886(03)00057-8
Tukhovskaya EA, Turovsky EA, Turovskaya MV, Levin SG, Murashev AN, Zinchenko VP, Godukhin OV (2014) Anti-inflammatory cytokine interleukin-10 increases resistance to brain ischemia through modulation of ischemia-induced intracellular Ca(2)(+) response. Neurosci Lett 571:55–60. doi:10.1016/j.neulet.2014.04.046
Sokolova A, Hill MD, Rahimi F, Warden LA, Halliday GM, Shepherd CE (2009) Monocyte chemoattractant protein-1 plays a dominant role in the chronic inflammation observed in Alzheimer’s disease. Brain Pathol 19(3):392–398. doi:10.1111/j.1750-3639.2008.00188.x
Kerschensteiner M, Meinl E, Hohlfeld R (2009) Neuro-immune crosstalk in CNS diseases. Neuroscience 158(3):1122–1132. doi:10.1016/j.neuroscience.2008.09.009
Bianchi R, Giambanco I, Donato R (2008) S100B/RAGE-dependent activation of microglia via NF-kappaB and AP-1 Co-regulation of COX-2 expression by S100B, IL-1beta and TNF-alpha. Neurobiol Aging 31(4):665–677. doi:10.1016/j.neurobiolaging.2008.05.017
Quesseveur G, David DJ, Gaillard MC, Pla P, Wu MV, Nguyen HT, Nicolas V, Auregan G et al (2013) BDNF overexpression in mouse hippocampal astrocytes promotes local neurogenesis and elicits anxiolytic-like activities. Translat Psychiatry 3:e253. doi:10.1038/tp.2013.30
Chen Y, Ai Y, Slevin JR, Maley BE, Gash DM (2005) Progenitor proliferation in the adult hippocampus and substantia nigra induced by glial cell line-derived neurotrophic factor. Exp Neurol 196(1):87–95. doi:10.1016/j.expneurol.2005.07.010
Kleindienst A, McGinn MJ, Harvey HB, Colello RJ, Hamm RJ, Bullock MR (2005) Enhanced hippocampal neurogenesis by intraventricular S100B infusion is associated with improved cognitive recovery after traumatic brain injury. J Neurotrauma 22(6):645–655. doi:10.1089/neu.2005.22.645
Davila D, Thibault K, Fiacco TA, Agulhon C (2013) Recent molecular approaches to understanding astrocyte function in vivo. Front Cell Neurosci 7:272. doi:10.3389/fncel.2013.00272
Hung SY, Liou HC, Fu WM (2010) The mechanism of heme oxygenase-1 action involved in the enhancement of neurotrophic factor expression. Neuropharmacology 58(2):321–329. doi:10.1016/j.neuropharm.2009.11.003
Mori T, Koyama N, Arendash GW, Horikoshi-Sakuraba Y, Tan J, Town T (2010) Overexpression of human S100B exacerbates cerebral amyloidosis and gliosis in the Tg2576 mouse model of Alzheimer’s disease. Glia 58(3):300–314. doi:10.1002/glia.20924
Donato R, Sorci G, Riuzzi F, Arcuri C, Bianchi R, Brozzi F, Tubaro C, Giambanco I (2009) S100B’s double life: intracellular regulator and extracellular signal. Biochim Biophys Acta 1793(6):1008–1022. doi:10.1016/j.bbamcr.2008.11.009
Teeling JL, Perry VH (2009) Systemic infection and inflammation in acute CNS injury and chronic neurodegeneration: underlying mechanisms. Neuroscience 158(3):1062–1073. doi:10.1016/j.neuroscience.2008.07.031
Doyle KP, Cekanaviciute E, Mamer LE, Buckwalter MS (2010) TGFbeta signaling in the brain increases with aging and signals to astrocytes and innate immune cells in the weeks after stroke. J Neuroinflammation 7:62. doi:10.1186/1742-2094-7-62
Acknowledgments
This work was supported by the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul (FAPERGS), Financiadora de Estudos e Projetos (FINEP) – IBN Net (Instituto Brasileiro de Neurociências) 01.06.0842-00, Federal University of Rio Grande do Sul (UFRGS), and Instituto Nacional de Ciência e Tecnologia para Excitotoxicidade e Neuroproteção (INCTEN/CNPq).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare there are no conflicts of interest.
Rights and permissions
About this article
Cite this article
Bellaver, B., Souza, D.G., Souza, D.O. et al. Hippocampal Astrocyte Cultures from Adult and Aged Rats Reproduce Changes in Glial Functionality Observed in the Aging Brain. Mol Neurobiol 54, 2969–2985 (2017). https://doi.org/10.1007/s12035-016-9880-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-9880-8