Abstract
Maple syrup urine disease (MSUD), or branched-chain α-keto aciduria, is an inherited disorder that is caused by a deficiency in branched-chain α-keto acid dehydrogenase complex (BCKAD) activity. Blockade of this pathway leads to the accumulation of the branched-chain amino acids (BCAAs), leucine, isoleucine, and valine, and their respective ketoacids in tissues. The main clinical symptoms presented by MSUD patients include ketoacidosis, hypoglycemia, opisthotonos, poor feeding, apnea, ataxia, convulsions, coma, psychomotor delay, and mental retardation. Although increasing evidence indicates that oxidative stress is involved in the pathophysiology of this disease, the mechanisms of the brain damage caused by this disorder remain poorly understood. In the present study, we investigated the effect of BCAAs on some oxidative stress parameters and evaluated the efficacy of L-carnitine (L-car), an efficient antioxidant that may be involved in the reduction of oxidative damage observed in some inherited neurometabolic diseases, against these possible pro-oxidant effects of a chronic MSUD model in the cerebral cortex and cerebellum of rats. Our results showed that chronic BCAA administration was able to promote both lipid and protein oxidation, impair brain antioxidant defenses, and increase reactive species production, particularly in the cerebral cortex, and that L-car was able to prevent these effects. Taken together, the present data indicate that chronic BCAA administration significantly increased oxidative damage in the brains of rats subjected to a chronic model of MSUD and that L-car may be an efficient antioxidant in this disorder.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Maple syrup urine disease (MSUD) is an inborn error of metabolism associated with acute and chronic brain dysfunction that is caused by severe deficiency in the activity of the branched-chain α-keto acid dehydrogenase complex (E.C. 1.2.4.4), a mitochondrial enzyme involved in the branched-chain amino acid (BCAA) degradation pathway. Due to this blockage, high concentrations of the BCAAs leucine (Leu), valine (Val), and isoleucine (Ile) as well as the respective branched-chain α-keto acids (BCKAs) accumulate in patients when on an unrestricted diet and during episodes of metabolic decompensation during intercurrent illness [1, 2].
MSUD usually presents with a heterogeneous clinical phenotype, ranging from the severe classical form to mild variants, possibly due to distinct residual enzyme activity. Patients affected by the classical form of this disorder present encephalopathy characterized by episodes of ketoacidosis, hypoglycemia, apnea, convulsions, and coma. The chronic clinical features include failure to thrive, poor feeding, ataxia, psychomotor delay, and mental retardation [3]. Newborns with classic MSUD are asymptomatic at birth but may develop lethargy and poor feeding within days. Untreated patients fall into a coma within the first 10 days of life [4]. Alterations in magnetic resonance imaging show, in addition to generalized cerebral edema, a characteristic pattern of localized intense edema involving the cerebellar white matter (hypomyelination), the dorsal part of the brainstem, the cerebral peduncles, the posterior limb of the internal capsule, and the posterior aspect of the centrum semiovale, areas which are already myelinated at birth [3, 5].
In spite of the predominance of severe neurological sequelae in MSUD, the mechanisms underlying the brain damage are still poorly understood. In addition, metabolite accumulation in MSUD has been demonstrated to affect brain uptake of essential amino acids [6], brain energy metabolism [7, 8], the induction of apoptosis [9], and demyelination [10], which also contribute to brain injury. Indeed, oxidative stress has been demonstrated to be an underlying pathophysiological process in animal models and in MSUD patients [11–16], which makes it attractive for the study of antioxidants as an additional therapeutic approach to those currently employed for MSUD patients.
Therapy for MSUD consists of a protein-restricted diet with a low BCAAs content, supplemented with a BCAA-free amino acid mixture enriched with vitamins and minerals [1]. Although the benefits of dietary treatment for MSUD patients are undeniable, natural protein restriction may increase the risk of nutritional deficiencies and may result in a low total antioxidant status that can predispose and/or contribute to oxidative stress [12, 17, 18]. In this context, treated MSUD patients were recently observed to have reduced levels of L-carnitine (L-car), a quaternary amine that is primarily supplied by the diet, particularly by red meat and milk, and is indispensable for the transport of fatty acids across the inner mitochondrial membrane for subsequent β-oxidation [19, 20]. Furthermore, studies have reported that L-car may protect cells against oxidative damage in important neurodegenerative disorders, such as Alzheimer’s disease and some inherited neurometabolic disorders [21–23]. Moreover, Mescka et al. [24] showed that acute intraperitoneal injection of L-car reduces lipid and protein oxidation and increases the activity of antioxidant enzymes in the cerebral cortex in chemically induced MSUD rats. Therefore, in the present study, we extended this work, evaluating the possible neuroprotective effects of L-car, an efficient antioxidant that may be involved in the reduction of oxidative damage observed in some inherited neurometabolic diseases, against the pro-oxidative effects of BCAA in the cerebral cortex and cerebellum of rats in a chemically induced chronic model of MSUD to examine whether these compounds could be involved in the oxidative stress present in this disorder. So, we evaluated thiobarbituric acid-reactive substances to assess lipid oxidation, protein oxidative damage (evaluated by protein carbonyl content), and reduced glutathione content in order to estimate non-enzymatic antioxidant defenses, reactive species production (measured by 2′7′-dichlorofluorescein oxidation assay), and enzymatic antioxidant defenses, analyzed by catalase, superoxide dismutase, glutathione peroxidase, and glucose 6-phosphate dehydrogenase activities.
Materials and Methods
Materials and Equipment
All of the chemicals were purchased from Sigma (St. Louis, MO, USA). A spectrofluorometer (SpectraMax Gemini XPS; Molecular Devices) and a Wallac 1409 Scintillation Counter were used for the measurements. An Eppendorf 5417R and Eppendorf 5403 were used for centrifugation procedures.
Animals
Five-day-old Wistar rats bred in the Central Animal House of the Department of Biochemistry, ICBS, UFRGS, were used. Rats were kept with dams until they were sacrificed. The dams had free access to water and to a 20 % (w/w) protein commercial chow (Supra, Porto Alegre, RS, Brazil). They were maintained on a 12:12 h light/dark cycle (lights on 0700–1900 hours) in an air-conditioned colony room maintained at a constant temperature (22 ± 1 °C). The “Principles of Laboratory Animal Care” (NIH publication number 80–23, revised 1996) were followed throughout the experiments.
Chronic Administration of BCAA Pool With or Without L-car Treatment
A chemically induced chronic model of MSUD was adapted according to Bridi et al. [25]. Five-day-old Wistar rats received three subcutaneous administrations (at 1 h intervals from each other) of BCAA pool (15.8 μL/g body weight) containing 190 mmol/L Leu, 59 mmol/L Ile, and 69 mmol/L of Val for a period of 15 days. On the day of the experiment, the BCAA solution was prepared in saline solution (0.85 % NaCl) and 20 mM sodium phosphate buffer, pH 7.4, containing 140 mM KCl. L-car was administered intraperitoneally (100 mg/kg body weight) concomitantly until the last injection of the BCAA pool. Animals were divided into four groups (n = 7–12 per group): a control group (saline solution), MSUD group (BCAA pool), L-car group (L-car), and MSUD + L-car group (L-car and BCAA pool).
Tissue Preparation
Sixty minutes after the last injection, the rats were killed by decapitation without anesthesia, and the brain was rapidly removed and kept on an ice plate. The olfactory bulb, pons, and medulla were discarded, and the cerebral cortex and cerebellum were dissected, weighed, and kept chilled until homogenization. These procedures lasted up to 3 min. The cerebral cortex and cerebellum were homogenized in ten volumes (1:10, w/v) of 20 mM sodium phosphate buffer, pH 7.4, containing 140 mM KCl. Homogenates were centrifuged at 750×g for 10 min at 4 °C to discard nuclei and cell debris. The pellet was discarded, and the supernatant was immediately separated and used for the measurements.
Thiobarbituric Acid-Reactive Substances (TBA-RS)
TBA-RS were measured according to Ohkawa et al. [26]. Briefly, samples and reagents were added to glass tubes in the following order: 500 μL of tissue supernatant; 50 μL of 8.1 % SDS; 1,500 μL of 20 % acetic acid in aqueous solution (v/v), pH 3.5; 1,500 μL of 0.8 % thiobarbituric acid; and 700 μL of distilled water. The mixture was vortexed, and the reaction was carried out in a boiling water bath for 1 h. After cooling, the mixture was centrifuged at 1,000×g for 10 min. The resulting pink-stained TBA-RS were quantified in a spectrophotometer at 532 nm. The results are presented as nmol of TBA-RS per milligram protein.
Protein Carbonyl Content
Protein carbonyl formation, a marker of protein oxidative damage, was measured spectrophotometrically according to Reznick and Packer [27]. Two hundred microliters of the aliquots of the pre-treated supernatants (containing approximately 0.3 mg of protein) was treated with 400 μL of 10 mM 2,4-dinitrophenylhydrazine (DNPH) dissolved in 2 M HCl, left in the dark for 1 h, and vortexed every 15 min. Samples were then precipitated with 500 μL 20 % trichloroacetic acid and centrifuged at 20,000×g for 3 min. The supernatant was discarded, and the pellet was re-suspended in 600 μL of 6 M guanidine (prepared in a 20 mM potassium phosphate solution, pH 2.3). The sample was vortexed and incubated at 60 °C for 15 min. Subsequently, it was centrifuged at 20,000×g for 3 min, and the absorbance was measured at 370 nm (UV) in a quartz cuvette using a Hitachi U-2001 double-beam spectrophotometer with temperature control (Hitachi High Technologies America, Inc., Life Sciences Division, Pleasanton, CA, USA). The results are presented as protein carbonyl content (nanomoles per milligram protein).
Reduced Glutathione (GSH) Content
This method is based on the reaction of GSH with the fluorophore o-phthalaldehyde (OPT) after deproteinizing the samples, and GSH levels were measured according to Browne and Armstrong [28]. Initially, metaphosphoric acid was used to deproteinize the samples, which were then centrifuged at 1,000×g for 10 min. Briefly, 2 mL of sodium phosphate buffer (pH 8.0) and 100 μL 1 mg/mL OPT (prepared in methanol) were added to 100 μL of each supernatant. The mixture was vortexed and allowed to stand in the dark for exactly 15 min. After that, the fluorescence was measured at emission = 420 nm and excitation = 350 nm using an F-2500 Hitachi (Hitachi High Technologies America, Inc., Life Sciences Division, Pleasanton, CA, USA). A calibration curve was also performed with a commercial GSH solution, and the results are expressed as micromoles GSH per milligram protein.
2′7′-dichlorofluorescein Oxidation Assay (DCF)
Reactive oxygen/nitrogen species production was measured following the method of Lebel et al. [29] based on 2′7′-dichlorofluorescein (H2DCF) oxidation. Samples (30 μL) were incubated with 30 μL of 20 mM sodium phosphate buffer (pH 7.4 with 140 mM KCl) and 240 μL of 100 μM 2′7′-dichlorofluorescein diacetate (H2DCF-DA) solution in a 96-well plate for 30 min at 37 °C in the dark. H2DCF-DA is cleaved by cellular esterases, and the H2DCF formed is eventually oxidized by reactive species present in the samples. The last reaction produces the fluorescent compound DCF, which was measured at 488 nm excitation and 525 nm emission. The results are presented as nanomoles DCF per milligram protein.
Catalase (CAT) Activity
CAT activity was assayed using a SpectraMax M5/M5 Microplate Reader (Molecular Devices, MDS Analytical Technologies, Sunnyvale, CA, USA). The method used is based on the disappearance of H2O2 at 240 nm in a reaction medium containing 20 mM H2O2, 0.1 % Triton X-100, 10 mM potassium phosphate buffer (pH 7.0), and 0.1–0.3 mg protein/mL [30]. One CAT unit is defined as 1 μmol of H2O2 consumed per minute, and the specific activity is calculated as CAT units per milligram protein.
Superoxide Dismutase (SOD) Activity
SOD activity was assayed according to the method of Marklund [31], which is based on the capacity of pyrogallol to auto-oxidize, a process highly dependent on superoxide radical. Inhibition of the autoxidation of this compound occurs in the presence of SOD, the activity of which can be then indirectly assayed spectrophotometrically at 420 nm using a SpectraMax M5/M5 Microplate Reader (Molecular Devices, MDS Analytical Technologies, Sunnyvale, CA, USA). The reaction medium contained 50 mM Tris buffer/1 mM EDTA (pH 8.2), 80 U/mL catalase, 0.38 mM pyrogallol, and approximately 1 μg of protein. A calibration curve was performed with purified SOD as the standard to calculate the activity of SOD present in the samples. The results were calculated as units per milligram protein.
Glutathione Peroxidase (GPx) Activity
GPx activity was measured according to Wendel [32] using tert-butylhydroperoxide as the substrate. The enzyme activity was determined by monitoring the disappearance of NADPH at 340 nm in a medium containing 100 mM potassium phosphate buffer/1 mM ethylenediaminetetraacetic acid (pH 7.7), 2 mM GSH, 0.1 U/mL GR, 0.4 mM azide, 0.5 mM tert-butyl-hydroperoxide, and 0.1 mM NADPH using a SpectraMax M5/M5 Microplate Reader (Molecular Devices, MDS Analytical Technologies, Sunnyvale, CA, USA). One GPx unit (U) is defined as 1 μmol of NADPH consumed per minute. The specific activity was calculated as units per milligram protein.
Glucose 6-phosphate Dehydrogenase (G6PD) Assay
G6PD activity was measured according to Leong and Clark [33] using a SpectraMax M5/ M5 Microplate Reader (Molecular Devices, MDS Analytical Technologies, Sunnyvale, CA, USA). The method is based on the formation of NADPH at 340 nm in a reaction medium containing 100 mM Tris–HCl buffer (pH 7.5), 10 mM magnesium chloride, 0.1 % Triton X-100, 0.5 mM NADPH, 1 mM glucose 6-phosphate, and 0.1–0.3 mg protein/mL. One G6PD unit is defined as 1 μmol of NADPH produced per minute, and the specific activity is expressed as G6PD units/mg protein.
BCAA Quantification
The concentrations of BCAAs in plasma and in the cerebral cortex and cerebellum were determined by HPLC according to the method of Joseph and Marsden [34]. The analysis was performed using a reverse-phase column (ODS 25 cm × 4.6 mm × 5 μm) and fluorescent detection after pre-column derivatization with OPA (5.4 mg OPA in 1 mL 0.2 M sodium borate, pH 9.5) plus 4 % mercaptoethanol. The flow rate was adjusted to 1.4 mL/min in a gradient of the mobile phase of methanol and 0.5 M sodium phosphate buffer, pH 5.5 (buffer A, 80 % methanol; buffer B, 20 % methanol). Each sample run lasted 45 min. Amino acids were identified by their retention time and were quantitatively determined by correlating their chromatographic peak area with the peak area of the internal standard (homocysteic acid). A known amino acid standard mixture was used for calibration.
L-car Quantification
Cerebral cortex and cerebellum free L-car levels were determined based on the method of De Sousa et al. [35]. Initially, 50 μL of potassium hydroxide 0.20 mol/L was added to 50 μL of sample, and the mixture was incubated at 37 °C for 45 min. The solution to be assayed was added to 50 μL of HEPES 0.5 mol/L, 20 μL of N-ethylmaleimide 40 mmol/L, and 100 μL of [1–14C] acetyl coenzyme A 10 μmol/L. Then, 30 μL of L-carnitine acyltransferase (0.5 mg/ml) was added, and the mixture was passed down through a column of Dowex. The total column effluent was collected, the scintillation fluid was added, and the isotope content was determined using a liquid scintillation counter. Free L-car was determined by the same protocol, but without incubation with potassium hydroxide. Results were expressed as micromoles per liter.
Protein Determination
Protein concentration was determined in the cerebral cortex and cerebellum supernatants using bovine serum albumin as a standard [36].
Statistical Analysis
The results are presented as the mean ± standard deviation. Assays were performed in duplicate, and the mean was used for statistical analysis. Data were analyzed using one-way analysis of variance (ANOVA), followed by Tukey’s post hoc test for multiple comparisons when the F value was significant. A value of P < 0.05 was considered to be significant. All of the analyses were performed using the Statistical Package for the Social Sciences (SPSS) software on a PC-compatible computer.
Results
Initially, we measured plasma and cortical levels of BCAA after subcutaneous injection of BCAA pool (15.8 μL/g body weight) for a period of 15 days. Average BCAA levels (reported for plasma and brain, respectively) determined by HPLC were 592 and 135 μmol/L for Leu, 235 and 78 μmol/L for Ile, and 378 and 96 μmol/L for Val, data of five animals. Control Wistar rats that received an equal volume of saline showed plasma levels of 111 μmol/L Leu, 65 μmol/L Ile, and 109 μmol/L Val, whereas concentrations in the brain were 62 μmol/L Leu, 45 μmol/L Ile, and 57 μmol/L Val.
Table 1 lists the free L-car concentrations in the cerebral cortex and cerebellum supernatants of the four studied groups: the control group (saline solution), MSUD group (BCAA pool), L-car group (L-car), and MSUD + L-car group (L-car and BCAA pool). The results show that L-car levels were significantly higher in the L-car group and MSUD + L-car group compared with the control and MSUD groups, indicating that after intraperitoneal injection, L-carnitine was able to cross the blood–brain barrier for subsequent analysis of its action in the central nervous tissue.
Figure 1 (a, b) shows that chronic administration of BCAA pool significantly increased TBA-RS levels in the cerebral cortex and cerebellum compared with the controls and that these effects were prevented by L-car treatment ([F(3,27) = 8136; P = 0.0005] and [F(3,25) = 27.82; P < 0.0001] for the cerebral cortex and cerebellum, respectively). It was not observed protein damage induction by chronic administration of BCAA in the cerebral cortex, as shown by the absence of significant alterations in carbonyl content (Fig. 1c) [F (3,39) = 1.837; P = 0.1564]. However, this treatment significantly increased carbonyl levels in the cerebellum (Fig. 1d) of MSUD rats, and these levels were significantly decreased by L-car injections [F(3,29) = 11.32; P < 0.0001]. Next, our results showed that L-car treatment also prevented the decrease of GSH content caused by BCAA accumulation in the cerebral cortex [F(3,29) = 11.68; P < 0.0001] (Fig. 1e), and no changes were observed in GSH content in the cerebellum in any of the tested groups (Fig. 1f) [F(3,28) = 2.92; P = 0.0518]. Compared to control group, DCF production in the cerebral cortex (Fig. 1g) was also increased by BCAA administration [F(3,24) = 30.48, P < 0.0001], and L-car was able to reduce the reactive species produced by the MSUD model back to the control level. However, no effect was observed in the cerebellum using this assay (Fig. 1h) [F(3,28) = 1.74; P = 0.1809].
Effect of the chronic administration of BCAA pool (MSUD), with or without L-carnitine (L-car) treatment, on thiobarbituric acid-reactive species (TBA-RS; a, b), carbonyl content (c, d), reduced glutathione (e, f), and DCF oxidation (g, h). The results are the mean ± SD (n = 7–12) of independent experiments performed in duplicate. *P < 0.05 compared with control; # compared with the MSUD group; § compared with the L-car group (Tukey’s multiple-range test)
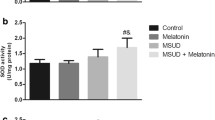
Last, we studied the effect of chronic BCAA administration on enzymatic antioxidant defenses in the brain. The activity of the antioxidant enzymes CAT, SOD, and GPx were assayed, as well as the activity of G6PD. The chronic chemical induction of MSUD significantly increased the activity of CAT in the cerebral cortex (Fig. 2a), and L-car prevented the enhancement of CAT activity due to BCAA administration [F(3,32) = 39.07; P < 0.0001]. However, it was not observed effect on the activity of this enzyme in the cerebellum by the MSUD induction [F(3,33) = 1.970; P > 0.1376] (Fig. 2b). In the cerebral cortex, L-car also prevented the inhibition of SOD activity caused by the chronic model of MSUD (Fig. 2c) [F(3,32) = 8.09; P = 0.0004]; however, it was not verified alterations on this activity in the cerebellum [F(3,27) = 0.96; P = 0.4253] (Fig. 2d). Likewise, the activity of GPx (Fig. 2e) was also inhibited by BCAA and restored by L-car in the cerebral cortex [F(3,35) = 4.88; P = 0.0061], but it was not detected changes in the cerebellum (Fig. 2f) [F(3,29) = 1.12; P = 0.3560]. The activity of G6PD was inhibited in the MSUD model only in the cerebral cortex, and this effect was prevented by L-car administration [F(3,34) = 3.26; P = 0.0333] (Fig. 2g). No alterations were observed in the cerebellum [F(3,32) = 0.26; P = 0.8519] (Fig. 2h).
Effect of the chronic administration of BCAA pool (MSUD), with or without L-carnitine (L-car) treatment, on catalase (CAT) activity (a, b), superoxide dismutase (SOD) activity (c, d), glutathione peroxidase (GPx) activity (e, f), and glucose 6-phosphate dehydrogenase (G6PD) activity (g, h). The results are the mean ± SD (n = 7–12) of independent experiments performed in duplicate. *P < 0.05 compared with the control group; # compared with the MSUD group (Tukey’s multiple-range test)
Discussion
The pathophysiology of the neurological symptoms and brain damage of MSUD patients seems to involve multiple mechanisms and remains poorly known, but it has been postulated that high concentrations of Leu and its transamination product (α-ketoisocaproic acid) produce direct and/or indirect effects and seem to be the main neurotoxic metabolites in the disease [1, 37]. Furthermore, several studies have demonstrated that oxidative stress contributes to this damage, showing that the main metabolites accumulated in the disease induce morphological alterations in glial cells through the generation of reactive species [38, 39]. Additionally, markers of lipid, protein, and DNA oxidative damage and reduced antioxidant status have been reported in experimental models and patients with MSUD [11, 12, 14, 15, 40, 41], probably secondary to the high production of free radicals. In addition, the protein-restricted diet used to treat MSUD has been postulated to possibly contribute to the compromised antioxidant status of these patients [11, 20, 40], thereby, highlighting the need for concomitant antioxidant strategies in addition to the restricted dietary treatment.
In this respect, Mescka et al. [24] showed that L-car may be an efficient antioxidant, protecting against the oxidative stress promoted by BCAAs in acute, chemically induced models of MSUD. To continue the work already underway, in this study, we evaluated the possible protective role of L-car against the chronic toxicity of BCAAs by analyzing a wide range of oxidative stress parameters in the cerebral cortex and cerebellum of rats, to evaluate L-car efficacy against BCAA pro-oxidative effects in the central nervous system.
We first observed that a chemically induced chronic model of MSUD significantly increased plasma and brain Leu, Ile, and Val concentrations compared with the controls and that these levels were similar to the concentrations reported in MSUD patients in the literature [1, 42], ensuring that our chronic model could be further used to study the long-term effects of BCAAs on oxidative stress parameters. Additionally, it is well known that L-car is actively transported through the blood–brain barrier by the organic cation transporter OCTN2 and accumulates in neural cells, especially as acetyl-L-carnitine [23]. Further, as shown in Table 1, we observed that the L-car intraperitoneal injections were effective in significantly increasing the concentration of this compound in the rat brain.
Subsequently, the influence of BCAA pool chronic administration on lipid peroxidation in cerebral cortex and cerebellum of rats was investigated. Considering that TBA-RS reflects mainly the content of malondialdehyde formation, an end product of membrane fatty acid peroxidation [26], we observed that BCAA administration significantly enhanced TBA-RS levels in cerebral cortex and cerebellum compared with the control group, indicating that BCAA pool promotes lipid oxidative damage in these tissues in the MSUD chronic model and that L-car treatment prevented the lipid peroxidation elicited by these metabolites. These results corroborate with previous findings showing that BCAA increases TBA-RS levels in the brains of rats [13–16] and in the plasma of MSUD patients [11, 12]. In our experiment, the generation of non-specific reactive species was measured by DCF oxidation assay. DCF levels in the cerebral cortex were significantly increased in the MSUD group compared with the controls, and chronic L-car treatment decreased these levels. In addition, DCF levels in the cerebellum did not differ significantly between the studied groups. Furthermore, previous studies have shown that L-car supplementation causes a dramatic reduction in malondialdehyde formation and increases overall antioxidant enzyme status, thus, decreasing the levels of free radicals available for lipid peroxidation in the brains of old rats [43]. Additionally, L-car directly scavenges free radicals and chelates metal ions that participate in reactive species reactions [19, 23]; therefore, it is plausible that L-car can inhibit the lipid peroxidation and DCF oxidation that are triggered by reactive species.
Therefore, the level of protein oxidation expressed as carbonyl content was determined in the brain areas studied. Interestingly, BCAA administration did not significantly alter cerebral cortex carbonyl content, but increased the measurement of this parameter in the cerebellum; L-car was not able to prevent this damage. These results corroborate with previous findings in the plasma of MSUD patients, as carbonyl content was significantly enhanced in MSUD patients, and the treatment with L-car was not able to change carbonyl content [20]. Carbonyl groups are mainly produced by the oxidation of protein side chains (Pro, Arg, Lys, and Thr) by the oxidative cleavage of proteins. Carbonyl groups can also be produced from the reduction of sugars or their oxidation products with lysine residues in proteins [44, 45]. Although protein carbonyls are usually caused by ROS-mediated protein damage, we also cannot exclude the possibility that aldehydes resulting from lipid peroxidation may also induce carbonyl generation [44, 45]. Although the exact mechanisms by which BCAAs cause protein oxidative damage are currently unknown, it is reasonable to speculate that these metabolite-induced reactive species may interact directly or indirectly with protein groups, leading to protein oxidation in the cerebellum.
GSH, the major non-enzymatic antioxidant defense in organisms, was also evaluated. Statistically significant differences in GSH levels were not observed in the cerebellar tissue; however, the chronic administration of BCAAs reduced GSH levels in the cerebral cortex, suggesting that this powerful antioxidant was used in the scavenging of the increased production of free radicals elicited by the high levels of DCFH oxidation in the MSUD group. The prevention of the decrease of GSH by the co-administration of L-car plus BCAA pool reinforces this interpretation. The reduction of GSH levels may compromise reactive species detoxification and may exacerbate the inhibition of GPx activity by BCAAs because this enzyme uses GSH as a cofactor [37].
We also evaluated the activity of the antioxidant enzymes CAT, SOD and GPx. In the cerebral cortex, CAT activity increased after BCAA administration, possibly as a consequence of increased production of H2O2 [46, 47]. On the other hand, SOD and GPx activities were inhibited, possibly caused by H2O2 accumulation [46, 48]. H2O2 accumulation and SOD inhibition can favor the Fenton/Haber–Weiss reaction, which generates hydroxyl radical (OH●), the most toxic reactive species [49]. In this context, it should be emphasized that hydroxyl radical readily initiate the process of lipid peroxidation [50]. Therefore, it may be presumed that the increased levels of superoxide, H2O2 and other reactive species caused by BCAA-mediated SOD and GPx inhibition could lead to the lipid peroxidation and GSH reduction found in the cerebral cortex in the MSUD group. However, further experiments should be carried out to clarify this matter. Previous results have already shown that BCAAs inhibit GPx [24] and that erythrocyte GPx activity is reduced in MSUD patients during treatment [18]. In addition, investigators have demonstrated that L-car has the ability to increase the levels of GSH [21], which is an essential cofactor of GPx. On the other hand, because MSUD patients under treatment may present selenium deficiency [18], it may be presumed that the restoration of GPx activity by L-car may be very important for their treatment. We demonstrated that chronic L-car administration restores CAT, SOD and GPx activity to the levels found in the control group, and these results agree with previous data from our research group [24]. It has been shown that L-car is an effective scavenger of reactive species such as H2O2 and superoxide anion [51, 52], which could help return the activity of these enzymes to normal levels. On the other hand, we did not observe alterations in the activity of these enzymes in the cerebellum in any of the tested groups.
The last antioxidant enzyme evaluated in the cerebral cortex and cerebellum supernatants from rats subjected to the chronic administration of BCAAs in this study was G6PD. We observed that chronic BCAA administration was able to inhibit G6PD activity in the cerebral cortex of MSUD rats, which could promote impairment of the production of NADPH and a disruption of the cellular redox balance. This observation is likely in line with the observed inhibition of activity because the activity of GPx depends on the regeneration of GSH by glutathione reductase, which in turn relies on NADPH, which is dependent on normal G6PD activity [53, 54]. It has also been reported that G6PD is strongly inactivated by 4-hydroxy-2-nonenal, a toxic product of membrane lipid peroxidation [55]. We also demonstrated that L-car treatment was able to return G6PD activity to normal levels. Therefore, the preservation of G6PD activity by L-car may be an important factor in the maintenance of proper enzymatic and non-enzymatic functioning of the GSH antioxidant system. Moreover, the reduction of G6PD activity in the MSUD group could elicit a deficit in the production of NADPH, which is used to produce GSH from GSSG.
The present study showed more important alterations of oxidative stress parameters in the cerebral cortex than in the cerebellum, suggesting that the cerebral cortex may be more susceptible to oxidative stress. This hypothesis is strengthened by reports showing higher reductive potential (calculated as NADPH/NADP+ and GSH/GSSG ratios) [56] and greater antioxidant enzyme activity [57] in the cerebellum compared with the cerebral cortex, which suggests a greater resistance of the cerebellum to oxidative stress [54]. Oxidant factors that directly or indirectly induce reactive species generation also differ among brain structures. For instance, the levels of iron, which catalyzes OH● formation from H2O2 through the Fenton reaction, are higher in the cerebral cortex than in the cerebellum [58]. Therefore, the higher iron levels along with increased H2O2 content may contribute to the higher susceptibility of the cerebral cortex to the oxidative stress promoted by BCAAs.
L-car and acylcarnitine supplementation have resulted in beneficial effects in the treatment of various neurological diseases. Recent data indicate new, multifactorial roles for L-car and acylcarnitine in neuroprotection. Brain carnitines can function in the synthesis of lipids, by altering and stabilizing membrane composition, by modulating genes and proteins, by improving mitochondrial function, by increasing antioxidant activity, and by enhancing cholinergic neurotransmission. In summary, L-car is not merely a cofactor in β-oxidation; rather, it has many known and yet-to-be-discovered functions in physiology [59].
The chemically induced chronic model of MSUD used in this study demonstrated that BCAAs induce oxidative stress in the brains of Wistar rats, corroborating previous reports of an involvement of oxidative damage in the neuropathophysiology of this disease. Because treatment with L-car was effective in improving the activity of antioxidant enzymes, increasing the non-enzymatic antioxidant defenses, and diminishing the lipid and protein damage and reactive species production (Fig. 3), an antioxidant treatment might be useful in avoiding the oxidative stress promoted by the main metabolites that accumulate in this disease. Considering that the current treatment of MSUD involves a BCAA-restricted diet, which is low in antioxidants and L-car [18, 20, 60], supplementation with antioxidants, especially L-car, may be considered a suitable adjuvant therapy for these patients because it can improve their redox homeostasis.
In vivo effects of L-carnitine on oxidative stress parameters (upward arrow increase, downward arrow decrease) induced by chronic administration of BCAA pool in a cerebellum and b cerebral cortex of rats subjected to a chemically induced chronic model of MSUD. SOD superoxide dismutase, CAT catalase, GPX glutathione peroxidase, G6PD glucose-6-phosphate dehydrogenase, GSH reduced glutathione. The figure was produced using Servier Medical Art (www.servier.com)
References
Chuang DT, Shih VE (2001) Maple syrup urine disease (branched chain ketoaciduria). In: Scriver CR, Beaudt AL, Sly WL, Valle D (eds) The metabolic and molecular bases of inherited disease. McGraw-Hill, New York, pp 1971–2005
Chuang DT, Chuang JL, Wynn RM (2006) Lessons from genetic disorders of branched-chain amino acid metabolism. J Nutr 136:243S–249S
Schönberger S, Schweiger B, Schwahn B, Schwarz M, Wendel U (2004) Dysmyelination in the brain of adolescents and young adults with maple syrup urine disease. Mol Genet Metab 82:69–75
Hoffmann B, Helbling C, Schadewaldt P, Wendel U (2006) Impact of longitudinal plasma leucine levels on the intellectual outcome in patients with classic MSUD. Pediatr Res 59:17–20
Klee D, Thimm E, Wittsack HJ, Schubert D, Primke R, Pentang G, Schaper J, Mödder U et al (2013) Structural white matter changes in adolescents and young adults with maple syrup urine disease. J Inherit Metab Dis 36:945–953
Araújo P, Wassermann GF, Tallini K, Furlanetto V, Vargas CR, Wannmacher CMD, Dutra-Filho CS, Wyse ATS et al (2001) Reduction of large neutral amino acid level in plasma and brain of hyperleucinemic rats. Neurochem Int 38:529–537
Pilla C, Cardozo RFD, Dutra CS, Wyze ATS, Wajner M, Wannmacher CMD (2003) Effect of leucine administration on creatine kinase activity in rat brain. Metab Brain Dis 18:17–25
Ribeiro CA, Sgaravatti AM, Rosa RB, Schuck PF, Grando V, Schmidt AL, Ferreira GC, Perry MLS et al (2008) Inhibition of brain energy metabolism by the branched-chain amino acids accumulating in maple syrup urine disease. Neurochem Int 33:114–124
Jouvet P, Rustin P, Taylor DL, Pocock JM, Felderhoff-Mueser U, Mazarakis ND, Sarraf C, Joashi U et al (2000) Branched chain amino acids induce apoptosis in neural cells without mitochondrial membrane despolarization or cytochrome c release: implications for neurological impairment associated with maple syrup urine disease. Mol Biol Cell 11:1919–1932
Treacy E, Clow CL, Reade TR, Chitayat D, Mamer OA, Scriver CR (1992) Maple syrup urine disease: interrelationship between branched chain amino-, oxo- and hydroxylacids implications for treatment association with CNS dysmyelination. J Inherit Metab Dis 15:121–135
Barschak AG, Sitta A, Deon M, Oliveira MH, Haeser A, Dutra-Filho CS, Wajner M, Vargas CR (2006) Evidence that oxidative stress is increased in plasma from patients with maple syrup urine disease. Metab Brain Dis 21:279–286
Barschak AG, Sitta A, Deon M, Barden AT, Dutra-Filho CS, Wajner M, Vargas CR (2008) Oxidative stress in plasma from maple syrup urine disease patients during treatment. Metab Brain Dis 23:71–80
Bridi R, Araldi J, Sgarbi MB, Testa CG, Durigon K, Wajner M, Dutra-Filho CS (2003) Induction of oxidative stress in rat brain by the metabolites accumulating in maple syrup urine disease. Int J Dev Neurosci 21:327–332
Bridi R, Braum CA, Zorzi GK, Wannmacher CM, Wajner M, Lissi EG, Dutra-Filho CS (2005) Alpha-keto acids accumulating in maple syrup urine disease stimulate lipid peroxidation and reduce antioxidant defenses in cerebral cortex from young rats. Metab Brain Dis 20:155–167
Bridi R, Latini A, Braum CA, Zorzi GK, Moacir W, Lissi E, Dutra-Filho CS (2005) Evaluation of the mechanism involved in leucine-induced oxidative damage in cerebral cortex of young rats. Free Radic Res 39:71–79
Fontella FU, Gassen E, Pulrolnik V, Wannmacher CMD, Klein AB, Wajner M, Dutra CS (2002) Stimulation of lipid peroxidation in vitro in rat brain by metabolites accumulating in maple syrup urine disease. Metab Brain Dis 17:47–54
Frazier DM, Allgeier C, Homer C, Marriage BJ, Ogata B, Rohr F, Splett PL, Stembridge A et al (2014) Nutrition management guideline for maple syrup urine disease: an evidence- and consensus-based approach. Mol Genet Metab 112:210–217
Barschak AG, Sitta A, Deon M, Barden AT, Schmitt GO, Dutra-Filho CS, Wajner M, Vargas CR (2007) Erythrocyte glutathione peroxidase activity and plasma selenium concentration are reduced in maple syrup urine disease patients during treatment. Int J Dev Neurosci 25:335–338
Gulcin I (2006) Antioxidant and antiradical activities of L-carnitine. Life Sci 78:803–811
Mescka CP, Wayhs CA, Vanzin CS, Biancini GB, Guerreiro G, Manfredini V, Souza C, Wajner M et al (2013) Protein and lipid damage in maple syrup urine disease patients: L-carnitine effect. Int J Dev Neurosci 31:21–24
Abdul HM, Butterfield DA (2007) Involvement of PI3K/PKG/ERK1/2 signaling pathways in cortical neurons to trigger protection by cotreatment of acetyl-L-carnitine and alpha-lipoic acid against HNE-mediated oxidative stress and neurotoxicity: implications for Alzheimer’s disease. Free Radic Biol Med 42:371–384
Uttara B, Singh AV, Zamboni P, Mahajan RT (2009) Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. Curr Neuropharmacol 7:65–74
Ribas GS, Vargas CR, Wajner M (2014) L-carnitine supplementation as a potential antioxidant therapy for inherited neurometabolic disorders. Gene 533:469–476
Mescka C, Moraes T, Rosa A, Mazzola P, Piccoli B, Jacques C, Dalazen G, Coelho J et al (2011) In vivo neuroprotective effect of L-carnitine against oxidative stress in maple syrup urine disease. Metab Brain Dis 26:21–28
Bridi R, Fontella FU, Pulrolnik V, Braun C, Zorzi GK, Coelho D, Wajner M, Vargas CR et al (2006) A chemically induced acute model of maple syrup urine disease in rats for neurochemical studies. J Neurosci Methods 155:224–230
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95:351–358
Reznick AZ, Packer L (1994) Oxidative damage to proteins: spectrophotometric method for carbonyl assay. Methods Enzymol 233:357–363
Browne RW, Armstrong D (1998) Reduced glutathione and glutathione disulfide. Methods Enzymol 108:347–352
Lebel CP, Ischiropoulos H, Bondy SC (1992) Evaluation of the probe 2′,7′-dichlorofluorescin as an indicator of reactive oxygen species formation and oxidative stress. Chem Res Toxicol 5:227–231
Aebi H (1984) Catalase in vitro. Methods Enzymol 105:121–126
Marklund SL (1985) Pyrogallol autoxidation. In: Greenwald RA (ed) Handbook of methods for oxygen radical research. CRC Press, Boca Raton, pp 243–247
Wendel A (1981) Glutathione peroxidase. Methods Enzymol 77:325–333
Leong SF, Clark JB (1984) Regional enzyme development in rat brain. Enzymes associated with glucose utilization. Biochem J 218:131–138
Joseph MH, Marsden CA (1986) Amino acids and small peptides. In: Lim CF (ed) HPLC of small peptides. IRL Press, Oxford, pp 13–27
De Sousa C, English NR, Stacey TE, Chalmers RA (1990) Measurement of L-carnitine and acylcarnitines in body fluids and tissues in children and in adults. Clin Chim Acta 187:317–328
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Danner DJ, Elsas JL (1989) Disorders of branched chain amino acid and keto acid metabolism. In: Scriver CR, Beaudt AL, Sly WL, Valle D (eds) The metabolic and molecular bases of inherited disease. McGraw-Hill, New York, pp 671–692
Funchal C, Latini A, Jacques-Silva MC, Dos Santos AQ, Buzin L, Gottfried C, Wajner M, Pessoa-Pureur R (2006) Morphological alterations and induction of oxidative stress in glial cells caused by branched-chain alpha-keto acids accumulating in maple syrup urine disease. Neurochem Int 49:640–650
de Lima PP, Funchal C, Loureiro SO, Heimfarth L, Zamoner A, Gottfried C, Latini A, Wajner M et al (2007) Branched-chain amino acids accumulating in maple syrup urine disease induce morphological alterations in C6 glioma cells probably through reactive species. Int J Dev Neurosci 25:181–189
Sitta A, Ribas GS, Mescka CP, Barschak AG, Wajner M, Vargas CR (2014) Neurological damage in MSUD: the role of oxidative stress. Cell Mol Neurobiol 34:157–165
Mescka CP, Wayhs CA, Guerreiro G, Manfredini V, Dutra-Filho CS, Vargas CR (2014) Prevention of DNA damage by L-carnitine induced by metabolites accumulated in maple syrup urine disease in human peripheral leukocytes in vitro. Gene 548:294–298
Morton DH, Strauss KA, Robinson DL, Puffenberger EG, Kelley RI (2002) Diagnosis and treatment of maple syrup disease: a study of 36 patients. Pediatrics 109:999–1008
Rani PJ, Panneerselvam C (2002) Effect of L-carnitine on brain lipid peroxidation and antioxidant enzymes in old rats. J Gerontol A Biol Sci Med Sci 57:B134–B137
Dalle-Donne I, Giustarini D, Colombo R, Rossi R, Milzani A (2003) Protein carbonylation in human diseases. Trends Mol Med 9:169–176
Dalle-Donne I, Aldini G, Carini M, Colombo R, Rossi R, Milzani A (2006) Protein carbonylation, cellular dysfunction, and disease progression. J Cell Mol Med 10:389–406
Gemelli T, de Andrade RB, Rojas DB, Bonorino NF, Mazzola PN, Tortorelli LS, Funchal C, Filho CS et al (2013) Effects of β-alanine administration on selected parameters of oxidative stress and phosphoryltransfer network in cerebral cortex and cerebellum of rats. Mol Cell Biochem 380:161–170
Rojas DB, Gemelli T, de Andrade RB, Campos AG, Dutra-Filho CS, Wannmacher CM (2012) Administration of histidine to female rats induces changes in oxidative status in cortex and hippocampus of the offspring. Neurochem Res 37:1031–1036
Moraes TB, Zanin F, da Rosa A, de Oliveira A, Coelho J, Petrillo F, Wajner M, Dutra-Filho CS (2010) Lipoic acid prevents oxidative stress in vitro and in vivo by an acute hyperphenylalaninemia chemically-induced in rat brain. J Neurol Sci 292:89–95
Lushchak VI (2014) Free radicals, reactive oxygen species, oxidative stress and its classification. Chem Biol Interact 224C:164–175
Lipinski B (2012) Hydroxyl radical and its scavengers in health and disease. Oxidative Med Cell Longev 2012:809696
Li JL, Wang QY, Luan HY, Kang ZC, Wang CB (2012) Effects of L-carnitine against oxidative stress in human hepatocytes: involvement of peroxisome proliferator-activated receptor alpha. J Biomed Sci 21:19–32
Ye J, Li J, Yu Y, Wei Q, Deng W, Yu L (2010) L-carnitine attenuates oxidant injury in HK-2 cells via ROS-mitochondria pathway. Regul Pept 161:58–66
Ho HY, Cheng ML, Chiu DT (2007) Glucose-6-phosphate dehydrogenase-from oxidative stress to cellular functions and degenerative diseases. Redox Rep 12:109–118
Pederzolli CD, Mescka CP, Zandoná BR, de Moura CD, Sgaravatti AM, Sgarbi MB, de Souza Wyse AT, Duval Wannmacher CM et al (2010) Acute administration of 5-oxoproline induces oxidative damage to lipids and proteins and impairs antioxidant defenses in cerebral cortex and cerebellum of young rats. Metab Brain 25:145–154
Ninfali P, Ditroilo M, Capellacci S, Biagiotti E (2001) Rabbit brain glucose-6-phosphate dehydrogenase: biochemical properties and inactivation by free radicals and 4-hydroxy-2-nonenal. Neuroreport 12:4149–4153
Yang MS, Chan HW, Yu LC (2006) Glutathione peroxidase and glutathione reductase activities are partially responsible for determining the susceptibility of cells to oxidative stress. Toxicology 226:126–130
Campese VM, Sindhu RK, Ye S, Bay Y, Vaziri ND, Jabbari B (2007) Regional expression of NO synthase, NAD(P)H oxidase and superoxide dismutase in the rat brain. Brain Res 1134:27–32
Beard JL, Connor JR, Jones BC (1993) Iron in the brain. Nutr Rev 51:157–170
Jones LL, McDonald DA, Borum PR (2010) Acylcarnitines: role in brain. Prog Lipid Res 49:61–75
Mc Guire PJ, Parikh A, Diaz GA (2009) Profiling of oxidative stress in patients with inborn errors of metabolism. Mol Genet Metab 98:173–180
Acknowledgments
This work was supported by research grants from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), and Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul (FAPERGS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Mescka, C.P., Rosa, A.P., Schirmbeck, G. et al. L-carnitine Prevents Oxidative Stress in the Brains of Rats Subjected to a Chemically Induced Chronic Model of MSUD. Mol Neurobiol 53, 6007–6017 (2016). https://doi.org/10.1007/s12035-015-9500-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9500-z