Abstract
METTL3 is an important methyltransferase in N(6)-methyladenosine (m6A) modification. Recently, METTL3 mediates methylation of pri-microRNA (miRNA) to accelerate miRNA maturation, regulating tumor development. This study explored whether METTL3 mediated miR-99a-5p to influence oral squamous cell carcinoma (OSCC) cell metastasis. MiR-99a-5p, ZBTB7A, and MATTL3 expression was measured using quantitative real-time PCR. Biological behaviors were assessed using cell counting kit-8, flow cytometry, Transwell assay, as well as western blot. Luciferase reporter assay evaluated the interaction between miR-99a-5p and ZBTB7A. METTL3-regulated pri-miR-99a-5p processing was determined by RNA binding protein immunoprecipitation (RIP) and methylated RNA immunoprecipitation (MeRIP) assays. The consequences clarified that miR-99a-5p was upregulated in OSCC cells. Downregulation of miR-99a-5p suppressed cellular viability, migration, invasion, and epithelial-mesenchymal transition (EMT), and induced apoptosis. ZBTB7A acted as a miR-99a-5p target and reversed the effects on cellular behaviors induced by miR-99a-5p inhibitor. m6A content and METTL3 expression were increased in OSCC cells. METTL3 promoted the m6A modification of pri-miR-99a-5p and thereby facilitated miR-99a-5p processing. Moreover, knockdown of METTL3 inhibited OSCC metastasis by downregulating miR-99a-5p. Taken together, METTL3 promoted miR-99a-5p maturation in an m6A-dependent manner, which further targets ZBTB7A to accelerate the progression of OSCC. These findings suggest potential targets for OSCC therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral cancer is a malignant tumor occurring in the oral cavity, ranking 18th in incidence and 16th in mortality among all cancers [1]. More than 90% of oral cancers are squamous cell-based, known as oral squamous cell carcinoma (OSCC). It is the most malignant and harmful tumor type of head and neck cancer [2]. Genetic factors, tobacco, alcohol, and human papillomavirus are the main causes of OSCC [3]. At present, the clinical outcomes of OSCC have been obviously enhanced along with the continuous development of diagnosis and treatment. However, the prognosis for patients with advanced OSCC remains unsatisfactory [4, 5]. Surgery combined with chemoradiotherapy is the primary treatment for locally advanced OSCC [6, 7]. However, most advanced OSCCs occur in distal metastases, leading to poor therapeutic effects and poor prognosis. Therefore, control of distant metastasis of OSCC contributes to improving survival rates [8].
The dysregulation of microRNAs (miRNAs) is a cause of tumorigenesis, which makes miRNAs the new targets for tumor therapy [9]. MiRNAs are critical to tumorigenesis and cancer development, functioning as tumor promoters or suppressors [10]. Dysregulation of miRNAs is linked to OSCC recurrence and prognosis [11]. In addition, miRNAs are epigenetic molecular markers associated with OSCC metastasis, such as miR-21. miR-34a, miR-196a, and miR-137 [12]. Recently, the biogenesis of miRNAs has been identified: Drosha and DGCR8 complex convert pri-miRNAs to pre-miRNAs post-transcription [13]. Then, pre-miRNAs are cleaved by Dicer to form mature miRNAs [14]. MiR-99a-5p is downregulated in OSCC and inhibited cell proliferation, migration, and invasion [15, 16]. Therefore, understanding the mechanisms of miR-99a-5p maturation in OSCC has not been elucidated.
N6-methyladenosine (m6A) methylation is an RNA modification that regulates RNA structure, transcription, processing, splicing, stability, degradation, and translation [17]. The alteration of m6A methylation affects tumor progression by regulating growth, differentiation, metastasis, and cell death [18]. M6A methylation is a key regulator of miRNA biosynthesis, promoting pri-miRNAs to be specifically recognized by DGCR8 and thus making miRNAs maturation [19, 20]. Methyltransferase-like 3 (METTL3) is a methyltransferase involved in methylation modification that accelerates or decelerates tumor progression [21]. Several studies have revealed that METTL3 promotes the processing of pri-miRNAs, such as pri-miR-19a and pri-miR221/222 [22, 23]. However, whether METTL3 could regulate miR-99a-5p maturation in OSCC remains unclear.
Here, we aimed to investigate the functional role of miR-99a-5p and METTL3 in OSCC. Moreover, we identified the effects of METTL3 on the processing and maturation of pri-miR-99a-5p processing. We found that METTL3 promoted OSCC progression by modulating pri-miR-99a-5p maturation in an m6A-dependent manner via targeting ZBTB7A. These findings imply that METTL3 is a potential therapeutic target for OSCC.
Materials and Methods
Cell Culture
HOK (human oral keratinocyte) cells were purchased from Tongpai Biotechnology (Shanghai, China). CAL27, SCC9 SCC15, and UM2 cell lines were purchased from ATCC (Manassas, USA). All cells were maintained in DMEM containing 10% FBS (Hyclone, South Logan, USA) and 1% penicillin and streptomycin (Invitrogen, Carlsbad, USA) at 37 °C with 5% CO2.
Cell Transfection
MiR-99a-5p mimic (5’-AACCCGUAGAUCCGAUCUUGUG-3’), miR-99a-5p inhibitor (5’-CACAAGAUCGGAUCUACGGGUU-3’), mimic negative control (nc) and inhibitor nc were acquired from Ribobio (Guangzhou, China). Short hairpin RNA (sh-nc), sh-ZBTB7A, METTL3 overexpression vector (oe-METTL3), empty vector, and sh-METTL3 were obtained from Genepharma (Shanghai, China). CAL27 and SCC9 cells were seeded into 6-well plates until 80% confluence. Lipofectamine 3000 (Invitrogen) was used for transient transfection for 48 h.
Quantitative Real-Time PCR (qRT-PCR)
Total RNA was isolated using TRIzol reagent (Invitrogen). Following detecting RNA purity at A260/A280 ratio using an ultraviolet spectrophotometer (METTLER Toledo), a ReverTra Ace qPCR RT kit (TOYOBO, Osaka) was used for reverse transcription. Real-time PCR was conducted using THUNDERBIRD qPCR Mix (TOYOBO, Osaka, Japan) in a Step One Plus Real-time PCR system (Applied Biosystems, Foster, USA). U6 was the internal control of miR-99a-5p, and GAPDH was the normalization control of mRNAs. The relative quantity of expression was determined with the 2−ΔΔCt method.
Cell Counting Kit-8 (CCK-8)
Cell viability was analyzed using CCK-8. CAL27 and SCC9 cells (2000 cells/well) plated in 96-well plates were incubated for one day and subsequently incubated with 10 µL of CCK-8 solution (Dojindo, Tokyo, Japan) for 2 h. The transmittance (A) value was detected at 450 nm using a microplate reader (Bio-Tek, Biotek Winooski, USA).
Flow Cytometry
Cell apoptosis was analyzed using flow cytometry. Transfected cells were centrifugated, washed, and resuspended using a binding buffer. Annexin-V-PE (5 µL) and 7-AAD (5 µL) from Annexin V-PE/7-AAD apoptosis kit (Elabscience, Wuhan, China) were incubated with cell suspension for 20 min in the dark. Apoptosis was assessed by a flow cytometer (Beckman Coulter, Miami, USA).
Transwell Assay
Transfected cells were suspended in medium without serum and added to the top Transwell chambers for invasion or migration analysis with or without Matrigel. The lower chambers were filled with the medium with FBS. One day later, unmigrated or uninvaded cells were removed. Paraformaldehyde (4%) was used to fix the migrated or invaded cells, which were subsequently stained with crystal violet. The results were imaged under a microscope (Olympus, Tokyo, Japan).
Western Blotting
Harvested OSCC cells were lysed using RIPA buffer and a BCA kit (Beyotime, Shanghai) was used to examine protein concentration. Equal amounts of proteins were separated on 10% SDS-PAGE and transferred to PVDF membranes (Millipore, Billerica, USA). Primary antibodies (Abcam, Cambridge, USA) were diluted and incubated with the membranes at 4 °C overnight, which were further incubated with secondary antibody (Abcam) at room temperature for 1 h. A Clarity Western ECL Subs (Bio-Rad, Hercules, USA) was used to visualize protein bands. The antibodies are shown as follows: anti-E-cadherin (ab98952, 1:1000), anti-N-cadherin (ab98952, 1:1000), anti-Vimentin (ab8978, 1:1000), anti-ZBTB7A (ab70208, 1:2000), anti-GAPDH (ab8245, 1:2000), HRP-conjugated goat anti-mouse IgG (ab205719, 1:3000) and HRP-conjugated goat anti-rabbit IgG (ab6721, 1:3000).
Bioinformatic Analysis
The targets of miR-99a-5p were predicted using the TargetScan (https://www.targetscan.org/vert_80/), miRDB (http://www.mirdb.org/), and starBase (http://starbase.sysu.edu.cn/) datasets. The entered miRNA name was “miR-99a-5p”. “Human” was the specie.
Luciferase Reporter Assay
Wild-type and mutant ZBTB7A (ZBTB7A-WT, ZBTB7A-MUT) sequences were inserted into the pGL3 plasmids (Promega, Madison). CAL27 and SCC9 cells were co-transfected with ZBTB7A-WT or ZBTB7A-MUT and mimic or mimic nc using lipofectamine 3000. Two days later, the Dual-Luciferase Reporter Assay System (Promega) was used to detect the luciferase activity.
Detection of m6A Content
An m6A RNA methylation quantification kit (Abcam) was used to detect m6A content. Briefly, total RNA was incubated with 2 µl m6A negative control or positive control solution for 1.5 h at 37 °C. m6A RNA was captured using a capture antibody and detection antibody at room temperature for 1 h. After adding the developer solution, the samples were incubated until they turned blue in the dark. The stop solution was added, and the absorbance was detected using a microplate reader at 450 nm.
RNA Binding Protein Immunoprecipitation (RIP)
A RIP kit was acquired from Geneseed (Guangzhou, China) to analyze the binding relationship between DGCR8 and pri-miR-99a-5p. Cells were lysed on ice for 10 min. After centrifugation, 100 µL supernatant was collected as the input group. Protein A/G beads were connected to anti-DGCR8 (ab191875, 1:50, Abcam) and anti-IgG (ab172730, 1:50, Abcam) at 4 °C for 2 h. The other supernatant (900 µL) was cultured with the beads-antibody complex at 4 °C for 3 h. The pri-miR-99a-5p expression was detected by qRT-PCR.
Methylated RNA Immunoprecipitation (MeRIP)
The transfected cells were digested using DNase I to disrupt RNA. Fragmented RNA was collected as the input group. The magnetic beads A/G were incubated with anti-m6A (ab208577, 1:50, Abcam) and anti-IgG (ab18443, 1:50, Abcam) for 1 h. The other fragmented RNA was incubated with RNase inhibitor, immunoprecipitation (IP) buffer, and the beads-antibody complex at 4 °C for 2 h. Then, the pri-miR-99a-5p expression was detected using qRT-PCR.
Statistical Analysis
Each experiment was repeated at least 3 times. The data were assessed using the GraphPad Prism 7 software and presented as mean ± standard deviation. The significance of value differences was evaluated using Student’s t-test or one-way ANOVA. P < 0.05 indicates a statistically significant difference.
Results
The Upregulation of miR-99a-5p is Identified in OSCC
A previous study has reported that the expression of miR-21-5p, miR-31-5p, and miR-155-5p is increased, whereas miR-99a-5p expression is decreased in OSCC [15]. To confirm the results, we detected their expression in OSCC cells and normal HOK cells. We found that the levels of these four miRNAs were all significantly higher in OSCC cells including CAL27, SCC9, SCC15, and UM2 than that in HOK cells (Fig. 1A-D). The results indicated that only miR-99a-5p expression was inconsistent with the results of the previous study, suggesting the role of miR-99a-5p in OSCC may be contradictory. Therefore, it is of great significance to study its role in OSCC.
MiR-99a-5p Downregulation Suppresses Malignant Advancement of OSCC
Following inhibitor and inhibitor nc transfection, miR-99a-5p levels were markedly reduced in CAL27 and SCC9 cells (Fig. 2A). Inhibition of miR-99a-5p inhibited cellular viability (Fig. 2B). Conversely, inhibition of miR-99a-5p induced apoptosis of OSCC cells (Fig. 2C and D). Cell migration was suppressed by inhibition of miR-99a-5p, compared with inhibitor nc (Fig. 2E and F). Cell invasion was also inhibited by a miR-99a-5p inhibitor (Fig. 2G and H). Downregulation of miR-99a-5p elevated the protein levels of E-cadherin and reduced of N-cadherin and Vimentin levels (Fig. 2I). However, overexpression of miR-99a-5p did not affect cell viability, migration, and invasion of HOK cells (Supplementary Fig. S1). Taken together, downregulation of miR-99a-5p inhibits cell viability, migration, invasion, and epithelial-mesenchymal transition (EMT), and induces apoptosis of OSCC cells. MiR-99a-5p could not induce tumor features of HOK cells.
Downregulated miR-99a-5p suppresses the malignant advancement of OSCC cells. (A) qRT-PCR measured miR-99a-5p expression after transfection with inhibitor or nc. Following transfection, (B) cellular viability was analyzed using CCK-8; (C,D) flow cytometry was performed to analyze OSCC cell apoptosis; (E,F) the migration and (G,H) invasion were evaluated using Transwell assay; and (I) EMT was assessed by detecting E-cadherin, N-cadherin, and Vimentin protein levels using western blotting. ***P < 0.001 vs. the inhibitor nc group
MiR-99a-5p Targets ZBTB7A
To explore the molecular mechanism, the targets of miR-99a-5p were predicted using the TargetScan, miRDB, and starbase online databases (Fig. 3A). The levels of the top five possibly targets of miR-99a-5p that could be predicted by all these databases were detected. The results illustrated that downregulation of miR-99a-5p significantly upregulated ZBTB7A expression, but not affected the levels of HOXA1, EPDR1, FGFR3, and FZD8 (Fig. 3B and C). The protein levels of ZBTB7A were elevated by miR-99a-5p downregulation (Fig. 3D). The bioinformatic analysis data showed that 3’-UTR of ZBTB7A has binding sites of miR-99a-5p (Fig. 3E). ZBTB7A expression was lower in CAL27, SCC9, SCC15, and UM2 cells than that in HOK cells (Fig. 3F). As compared to nc, miR-99a-5p mimic reduced the luciferase activity co-transfected with ZBTB7A-WT plasmid, whereas did not affect the luciferase activity in ZBTB7A-MUT vector co-transfection group (Fig. 3G and H). The results demonstrate that ZBTB7A is a target of miR-99a-5p that is downregulated in OSCC.
MiR-99a-5p targets ZBTB7A. (A) The targets of miR-99a-5p predicted by TargetScan, miRDB, and starBase databases were shown using the Venn diagram. (B,C) qRT-PCR was carried out to measure the top five targets (HOXA1, EPDR1, FGFR3, ZBTB7A, and FZD8) expression after miR-99a-5p inhibitor and inhibitor nc transfection. (D) Effect of miR-99a-5p inhibitor on the protein levels of ZBTB7A was measured using western blot. (E) The binding position of miR-99a-5p in ZBTB7A at the 3’-UTR regions. (F) ZBTB7A expression in HOK, CAL27, SCC9, SCC15, and UM2 cells was measured using qRT-PCR. (G,H) Luciferase reporter assay was conducted to analyze the combination of miR-99a-5p and ZBTB7A. ***P < 0.001 vs. the inhibitor nc group in (B and C). ***P < 0.001 vs. the HOK group in (D) **P < 0.01 and ***P < 0.001 vs. the mimic nc group in (F and G)
MiR-99a-5p Downregulation Suppresses Malignant Advancement of OSCC Via Targeting ZBTB7A
After sh-ZBTB7A transfection, the levels of ZBTB7A were downregulated, compared with sh-NC transfection (Fig. 4A). Downregulated miR-99a-5p inhibited cell viability, and ZBTB7A knockdown abrogated the inhibition of viability (Fig. 4B). MiR-99a-5p inhibitor facilitated apoptosis, while ZBTB7A knockdown counteracted cell apoptosis (Fig. 4C and D). Additionally, inhibiting miR-99a-5p impeded cell migration and invasion, which was rescued by knockdown of ZBTB7A (Fig. 4E-H). MiR-99a-5p elevated E-cadherin levels and decreased N-cadherin and Vimentin levels, which were counteracted by ZBTB7A knockdown (Fig. 4I). To sum up, downregulation of miR-99a-5p inhibits OSCC cell viability, migration, and invasion, and promotes apoptosis by targeting ZBTB7A.
MiR-99a-5p suppresses the malignant advancement of OSCC cells via targeting ZBTB7A. (A) qRT-PCR measured ZBTB7A expression following sh-NC and sh- ZBTB7A transfection. Following transfection, (B) cellular viability was analyzed by CCK-8; (C,D) flow cytometry was performed to analyze cell apoptosis; (E,F) the migration and (G,H) invasion were evaluated by Transwell assay; and (I) EMT was assessed by detecting E-cadherin, N-cadherin, and Vimentin levels using western blotting. ***P < 0.001 vs. the sh-nc group in (A). ***P < 0.001 vs. inhibitor nc group in (B-H). ### P < 0.001 vs. inhibitor group
METTL3 Facilitates Pri-MiR-99a-5p Processing in a DGCR8-Dependent Manner
Subsequently, m6A levels in OSCC cells were measured. The results showed that m6A content was increased in CAL27, SCC9, SCC15, and UM2 cells, particularly in CAL27 and UM2 cells, compared with HOK cells (Fig. 5A), suggesting that m6A modification occurs in OSCC cells. Then, the expression of m6A “writers” was measured. METTL3 was identified to be highly expressed in CAL27 and SCC9 cells, whereas FTO, ALKBH5, and WTAP levels in OSCC and HOK cells were no significant difference (Fig. 5B). METTL14 expression was increased in SCC9 cells, but did not change in CAL27 cells, compared with HOK cells (Fig. 5B). The data illustrated that transfection with oe-METTL3 increased METTL3 levels, whereas transfected with sh-METTL3 reduced METTL3 levels (Fig. 5C). Overexpression of METTL3 upregulated, whereas knockdown of METTL3 downregulated the levels of miR-99a-5p (Fig. 5D). Pri-miR-99a-5p binding by DGCR8 immunoprecipitated was increased in oe-METTL3-transfected cells and was reduced after sh-METTL3 transfection (Fig. 5E and F). The Me-RIP data showed that overexpressing METTL3 promoted the m6A modification of pri-miR-99a-5p, while knockdown of METTL3 decreased m6A modification of pri-miR-99a-5p (Fig. 5G and H). In summary, METTL3 promotes the processing and maturation of pri-miR-99a-5p.
METTL3 facilitates the processing of pri-miR-99a-5p in a DGCR8-dependent manner. (A) The m6A content was detected in HOK, CAL27, SCC9, SCC15, and UM2 cells. (B) The expression of m6A ‘writers” including FTO, ALKBH5, WTAP, METTL3, and METTL14 was measured using qRT-PCR in HOK, CAL27, and SCC9 cell lines. (C) The efficiency evaluated using qRT-PCR after oe-nc, oe-METTL3, sh-nc, and sh-METTL3 transfection. (D) Effects of METTL3 overexpression or knockdown on miR-99a-5p expression was examined by qRT-PCR. (E,F) RIP was performed to determine DGCR8-dependent processing of pri-miR-99a-5p. (G,H) Me-RIP determined the m6A modification of pri-miR-99a-5p following METTL3 overexpressing or knockdown. *P < 0.05, **P < 0.01 and ***P < 0.001 vs. the HOK group in (A and B). **P < 0.01 and ***P < 0.001 vs. the oe-nc group in (C-H). ##P < 0.01 and ###P < 0.001 vs. the sh-nc group in (C-H).
Depletion of METTL3 Suppresses Malignant Advancement of OSCC by Downregulating miR-99a-5p
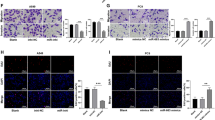
MiR-99a-5p expression was notably elevated following mimic transfection (Fig. 6A). METTL3 knockdown decreased miR-99a-5p levels, whereas mimic transfection reversed the decrease of METTL3 levels (Fig. 6B). Cell viability was inhibited by METTL3 silencing, and was abrogated by overexpressing miR-99a-5p (Fig. 6C). Apoptosis was facilitated by METTL3 knockdown, which was counteracted by miR-99a-5p (Fig. 6D and E). Knockdown of METTL3 inhibited cell migration and invasion, whereas enforced miR-99a-5p partly abolished the inhibition (Fig. 6F-I). In addition, silencing of METTL3 inhibited EMT, whereas miR-99a-5p overexpression rescued the effects induced by METTL3 loss (Fig. 6J). Taken together, silencing of METTL3 suppresses OSCC cell viability, migration, invasion, and EMT, and facilitating apoptosis by regulating miR-99a-5p.
Knockdown of METTL3 suppresses the malignant advancement of OSCC cells by downregulating miR-99a-5p. (A) qRT-PCR was used to measure miR-99a-5p expression after miR-99a-5p mimic and mimic nc transfection. (B) Effects of METTL3 knockdown and miR-99a-5p overexpression on miR-99a-5p expression was examined using qRT-PCR. Following transfection, (C) cell viability was analyzed by CCK-8; (D,E) flow cytometry analyzed apoptosis; (F,G) migration and (H,I) invasion were both evaluated by Transwell assay; and (J) EMT was assessed through western blotting by detecting E-cadherin, N-cadherin, and Vimentin levels. ***P < 0.001 vs. mimic nc group in (A). ***P < 0.001 vs. sh-nc group in (B-I). ## P < 0.01 vs. sh-METTL3 + mimic nc group in (B). ###P < 0.001 vs. the sh-METTL3 group in (C-I).
Discussion
Herein, we explored the functions of METTL3 in OSCC and its regulation of miR-99a-5p processing. This study revealed that downregulated miR-99a-5p targeted ZBTB7A to inhibit the progression of OSCC, and METTL3 promoted the maturation of pri-miR-99a-5p in an m6A-dependent manner.
MiRNAs are highly conserved and maintain cell homeostasis by negatively regulated mRNAs. Dysregulation of miRNAs has the potential for diagnosis, prognosis, and therapy of malignancy [24]. MiR-99a-5p is revealed to be upregulated in gastric cancer [25], epithelial ovarian cancer [26], and breast cancer [27]. Aberrantly expressed miR-99a-5p in serum of patients with OSCC is identified as a biomarker for prognosis [28]. Herein, the involvement of miR-99a-5p in OSCC was explored. In this study, we found that miR-21-5p, miR-31-5p, miR-99a-5p, and miR-155-5p were upregulated in OSCC cells. Only the miR-99a-5p expression was inconsistent with the results of Jakob et al. and Cui et al. studies, which showed that miR-99a-5p expression was decreased in OSCC [15, 29]. The interesting finding illustrates miR-99a-5p plays a paradoxical role in OSCC. Moreover, inhibiting miR-99a-5p expression impeded OSCC cell proliferation and metastasis, and facilitated apoptosis, which further demonstrated that miR-99a-5p has an oncogenic influence on OSCC.
ZBTB7A, a member of the POK family, is a transcriptionally regulated target gene by binding to short DNA recognition sites. It plays a crucial role in cancers by controlling tumor growth, differentiation, metastasis, and death [30]. ZBTB7A is commonly described as a powerful oncogene, whereas recent studies showed that it also has tumor-suppressing effects. For example, ZBTB7A induces cell senescence in PTEN loss of prostate cancer [31]. Downregulation of ZBTB7A is related to the poor outcomes of colon cancer and promotes tumor cell glycolysis [32]. ZBTB7A is usually downregulated in head and neck cancers, including OSCC. ZBTB7A, a target of miR-372, is related to tumorigenesis and drug resistance of OSCC [33]. However, whether ZBTB7A was regulated by miR-99a-5p and its effects on cell metastasis remain not understood. In this study, ZBTB7A was downregulated in OSCC cells and acted as a miR-99a-5p target. Downregulated miR-99a-5p attenuated OSCC progression via targeting ZBTB7A. These data suggest that ZBTB7A acts as a tumor-suppressor in OSCC.
METTL3 is a best-known m6A “writer” during m6A methylation modification. It is involved in multiple cellular processes, including differentiation, cell cycle, proliferation, invasion, inflammation, and death [34]. Moreover, METTL3 performs m6A-dependent modifications on miRNAs associated with cancer progression [35]. DGCR8 recognizes and cleaves pri-miRNAs in miRNA maturation, and METTL3 is required during this process [36]. Growing evidence has shown that METTL3 promotes the maturation of multiple miRNAs in malignancies, such as miR-126-5p, miR221/222, and miR-1246 [23, 37, 38]. However, whether METTL3 is related to miR-99a-5p maturation remains unknown. In the current study, METTL3 was upregulated in OSCC. Knockdown of METTL3 suppressed cell proliferation, metastasis, and facilitated apoptosis, consistent with the previous studies [39, 40]. However, the regulation of METTL3 on miR-99a-5p maturation has not been studied. We found overexpression of METTL3 accelerated miR-99a-5p maturation through m6A modification of pri-miR-99a-5p in a DGCR8-dependent manner. MiR-99a-5p rescued the influences of METTL3 silence on cellular processes and tumor growth. The data suggest that METTL3 accelerated OSCC progression by mediating miR-99a-5p maturation, providing a novel mechanism of METTL3 in OSCC.
However, limitations are existed in this study. The role of METTL3, miR-99a-5p, and ZBTB7A in vivo need to be explored. Moreover, whether they can be used in clinical treatments for OSCC needs much research.
Conclusions
In short, METTL3 plays a tumor promoting role in OSCC. Moreover, the METTL3/miR-99a-5p/ZBTB7A axis is crucial for the progression of OSCC, suggesting the potential to be therapeutic targets for the treatment of OSCC.
References
Sung, H., Ferlay, J., Siegel, R. L., Laversanne, M., Soerjomataram, I., Jemal, A., & Bray, F. (2021 May). Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and Mortality Worldwide for 36 cancers in 185 countries. C Ca: A Cancer Journal For Clinicians, 71(3), 209–249. https://doi.org/10.3322/caac.21660.
Vitório, J. G., Duarte-Andrade, F. F., Dos Santos Fontes Pereira, T., Fonseca, F. P., Amorim, L. S. D., Martins-Chaves, R. R., Gomes, C. C., Canuto, G. A. B., & Gomez, R. S. Metabolic landscape of oral squamous cell carcinoma. Metabolomics 2020 Sep 30;16(10):105. https://doi.org/10.1007/s11306-020-01727-6.
Chamoli, A., Gosavi, A. S., Shirwadkar, U. P., Wangdale, K. V., Behera, S. K., Kurrey, N. K., Kalia, K., & Mandoli, A. (2021 Oct). Overview of oral cavity squamous cell carcinoma: Risk factors, mechanisms, and diagnostics. Oral Oncology, 121, 105451. https://doi.org/10.1016/j.oraloncology.2021.105451.
Abdelmeguid, A. S., Silver, N. L., Boonsripitayanon, M., Glisson, B. S., Ferrarotto, R., Gunn, G. B., Phan, J., Gillenwater, A. M., & Hanna, E. Y. Role of induction chemotherapy for oral cavity squamous cell carcinoma. Cancer. 2021 Sep 1;127(17):3107–3112. https://doi.org/10.1002/cncr.33616.
Howard, A., Agrawal, N., & Gooi, Z. (2021 Oct). Lip and oral cavity squamous cell carcinoma. Hematol Oncol Clin North Am, 35(5), 895–911. https://doi.org/10.1016/j.hoc.2021.05.003.
Yao, C. M. K. L., Chang, E. I., & Lai, S. Y. Contemporary Approach to Locally Advanced Oral Cavity Squamous Cell Carcinoma. Curr Oncol Rep. 2019 Nov 7;21(11):99. https://doi.org/10.1007/s11912-019-0845-8.
Montagnani, F., Fornaro, L., Frumento, P., Vivaldi, C., Falcone, A., & Fioretto, L. (2017 Jun). Multimodality treatment of locally advanced squamous cell carcinoma of the oesophagus: A comprehensive review and network meta-analysis. Critical Reviews In Oncology Hematology, 114, 24–32. https://doi.org/10.1016/j.critrevonc.2017.03.024.
Tomioka, H., Yamagata, Y., Oikawa, Y., Ohsako, T., Kugimoto, T., Kuroshima, T., Hirai, H., Shimamoto, H., & Harada, H. Risk factors for distant metastasis in locoregionally controlled oral squamous cell carcinoma: A retrospective study. Sci Rep 2021 Mar 4;11(1):5213. https://doi.org/10.1038/s41598-021-84704-w.
Rupaimoole, R., & Slack, F. J. (2017 Mar). MicroRNA therapeutics: Towards a new era for the management of cancer and other diseases. Nature Reviews. Drug Discovery, 16(3), 203–222. https://doi.org/10.1038/nrd.2016.246.
Hill, M., & Tran, N. miRNA interplay: mechanisms and consequences in cancer. Dis Model Mech. 2021 Apr 1;14(4):dmm047662. https://doi.org/10.1242/dmm.047662.
Rajan, C., Roshan, V. G. D., Khan, I., Manasa, V. G., Himal, I., Kattoor, J., Thomas, S., Kondaiah, P., & Kannan, S. MiRNA expression profiling and emergence of new prognostic signature for oral squamous cell carcinoma. Sci Rep. 2021 Mar 31;11(1):7298. https://doi.org/10.1038/s41598-021-86316-w.
Jadhav, K. B., Nagraj, S. K., & Arora, S. (2021 Apr). miRNA for the assessment of lymph node metastasis in patients with oral squamous cell carcinoma: Systematic review and metanalysis. Journal Of Oral Pathology And Medicine, 50(4), 345–352. https://doi.org/10.1111/jop.13134.
Gregory, R. I., Yan, K. P., Amuthan, G., Chendrimada, T., Doratotaj, B., Cooch, N., & Shiekhattar, R. The Microprocessor complex mediates the genesis of microRNAs. Nature. 2004 Nov 11;432(7014):235 – 40. https://doi.org/10.1038/nature03120.
Bernstein, E., Caudy, A. A., Hammond, S. M., & Hannon, G. J. Role for a bidentate ribonuclease in the initiation step of RNA interference. Nature. 2001 Jan 18;409(6818):363-6. https://doi.org/10.1038/35053110.
Jakob, M., Mattes, L. M., Küffer, S., Unger, K., Hess, J., Bertlich, M., Haubner, F., Ihler, F., Canis, M., Weiss, B. G., & Kitz, J. (2019 Oct). MicroRNA expression patterns in oral squamous cell carcinoma: Hsa-mir-99b-3p and hsa-mir-100-5p as novel prognostic markers for oral cancer. Head And Neck, 41(10), 3499–3515. https://doi.org/10.1002/hed.25866.
Sun, X., & Yan, H. (2021 May). MicroRNA-99a-5p suppresses cell proliferation, migration, and invasion by targeting isoprenylcysteine carboxylmethyltransferase in oral squamous cell carcinoma. Journal Of International Medical Research, 49(5), 300060520939031. https://doi.org/10.1177/0300060520939031.
Liu, Z., & Zhang, J. Human C-to-U Coding RNA Editing Is Largely Nonadaptive. Mol Biol Evol. 2018 Jul 1;35(7):1821. https://doi.org/10.1093/molbev/msy011.
Liu, Z. X., Li, L. M., Sun, H. L., & Liu, S. M. Link between m6A modification and cancers. Front Bioeng Biotechnol 2018 Jul 13;6:89. https://doi.org/10.3389/fbioe.2018.00089.
Han, X., Guo, J., & Fan, Z. Interactions between m6A modification and miRNAs in malignant tumors. Cell Death Dis. 2021 Jun 9;12(6):598. https://doi.org/10.1038/s41419-021-03868-5.
Alarcón, C. R., Lee, H., Goodarzi, H., Halberg, N., & Tavazoie, S. F. N6-methyladenosine marks primary microRNAs for processing. Nature 2015 Mar 26;519(7544):482–5. https://doi.org/10.1038/nature14281.
Zeng, C., Huang, W., Li, Y., & Weng, H. Roles of METTL3 in cancer: Mechanisms and therapeutic targeting. J Hematol Oncol 2020 Aug 27;13(1):117. https://doi.org/10.1186/s13045-020-00951-w.
Gong, Y., Jiang, Q., Liu, L., Liao, Q., Yu, J., Xiang, Z., & Luo, X. (2022). METTL3-mediated m6A modification promotes processing and maturation of pri-miRNA-19a to facilitate nasopharyngeal carcinoma cell proliferation and invasion. Physiol Genomics. Sep 1;54(9):337–349. https://doi.org/10.1152/physiolgenomics.00007.2022.
Han, J., Wang, J. Z., Yang, X., Yu, H., Zhou, R., Lu, H. C., Yuan, W. B., Lu, J. C., Zhou, Z. J., Lu, Q., Wei, J. F., & Yang, H. METTL3 promote tumor proliferation of bladder cancer by accelerating pri-miR221/222 maturation in m6A-dependent manner. Mol Cancer 2019 Jun 22;18(1):110. https://doi.org/10.1186/s12943-019-1036-9.
Mishra, S., Yadav, T., & Rani, V. (2016 Feb). Exploring miRNA based approaches in cancer diagnostics and therapeutics. Critical Reviews In Oncology Hematology, 98, 12–23. https://doi.org/10.1016/j.critrevonc.2015.10.003.
Li, Y., Yan, J., Wang, Y., Wang, C., Zhang, C., & Li, G. (2020 Dec). LINC00240 promotes gastric cancer cell proliferation, migration and EMT via the miR-124-3p / DNMT3B axis. Cell Biochemistry And Function, 38(8), 1079–1088. https://doi.org/10.1002/cbf.3551.
Yoshimura, A., Sawada, K., Nakamura, K., Kinose, Y., Nakatsuka, E., Kobayashi, M., Miyamoto, M., Ishida, K., Matsumoto, Y., Kodama, M., Hashimoto, K., Mabuchi, S., & Kimura, T. Exosomal miR-99a-5p is elevated in sera of ovarian cancer patients and promotes cancer cell invasion by increasing fibronectin and vitronectin expression in neighboring peritoneal mesothelial cells. BMC Cancer 2018 Nov 5;18(1):1065. https://doi.org/10.1186/s12885-018-4974-5.
Garrido-Cano, I., Constâncio, V., Adam-Artigues, A., Lameirinhas, A., Simón, S., Ortega, B., Martínez, M. T., Hernando, C., Bermejo, B., Lluch, A., Lopes, P., Henrique, R., Jerónimo, C., Cejalvo, J. M., & Eroles, P. Circulating miR-99a-5p Expression in Plasma: A Potential Biomarker for Early Diagnosis of Breast Cancer. Int J Mol Sci. 2020 Oct 8;21(19):7427. https://doi.org/10.3390/ijms21197427.
Shi, J., Bao, X., Liu, Z., Zhang, Z., Chen, W., & Xu, Q. Serum miR-99a-5p and miR-5100 are Promising Prognosis Predictors for Oral Squamous Cell Carcinoma. Theranostics. 2019 Jan 25;9(4):920–931. https://doi.org/10.7150/thno.30339.
Cui, S. H., Hu, X. D., & Yan, Y. (2021 Nov). Wnt/β-catenin signaling pathway participates in the effect of miR-99a-5p on oral squamous cell carcinoma by targeting RASSF4. Journal Of Oral Pathology And Medicine, 50(10), 1005–1017. https://doi.org/10.1111/jop.13216.
Singh, A. K., Verma, S., Kushwaha, P. P., Prajapati, K. S., Shuaib, M., Kumar, S., & Gupta, S. Role of ZBTB7A zinc finger in tumorigenesis and metastasis. Mol Biol Rep 2021 May;48(5):4703–4719. https://doi.org/10.1007/s11033-021-06405-x.
Wang, G., Lunardi, A., Zhang, J., Chen, Z., Ala, U., Webster, K. A., Tay, Y., Gonzalez-Billalabeitia, E., Egia, A., Shaffer, D. R., Carver, B., Liu, X. S., Taulli, R., Kuo, W. P., Nardella, C., Signoretti, S., Cordon-Cardo, C., Gerald, W. L., & Pandolfi, P. P. (2013 Jul). Zbtb7a suppresses prostate cancer through repression of a Sox9-dependent pathway for cellular senescence bypass and tumor invasion. Nature Genetics, 45(7), 739–746. https://doi.org/10.1038/ng.2654.
Liu, X. S., Haines, J. E., Mehanna, E. K., Genet, M. D., Ben-Sahra, I., Asara, J. M., Manning, B. D., & Yuan, Z. M. ZBTB7A acts as a tumor suppressor through the transcriptional repression of glycolysis. Genes Dev. 2014 Sep 1;28(17):1917-28. https://doi.org/10.1101/gad.245910.114.
Yeh, L. Y., Yang, C. C., Wu, H. L., Kao, S. Y., Liu, C. J., Chen, Y. F., Lin, S. C., & Chang, K. W. The miR-372-ZBTB7A Oncogenic Axis suppresses TRAIL-R2 Associated Drug Sensitivity in oral carcinoma. Front Oncol 2020 Jan 31;10:47. https://doi.org/10.3389/fonc.2020.00047.
Liu, S., Zhuo, L., Wang, J., Zhang, Q., Li, Q., Li, G., Yan, L., Jin, T., Pan, T., Sui, X., Lv, Q., & Xie, T. METTL3 plays multiple functions in biological processes. Am J Cancer Res. 2020 Jun 1;10(6):1631–1646.
Yi, Y. C., Chen, X. Y., Zhang, J., & Zhu, J. S. Novel insights into the interplay between m6A modification and noncoding RNAs in cancer. Mol Cancer. 2020 Aug 7;19(1):121. https://doi.org/10.1186/s12943-020-01233-2.
Nogami, M., Miyamoto, K., Hayakawa-Yano, Y., Nakanishi, A., Yano, M., & Okano, H. DGCR8-dependent efficient pri-miRNA processing of human pri-miR-9-2. J Biol Chem 2021 Jan-Jun;296:100409. https://doi.org/10.1016/j.jbc.2021.100409.
Bi, X., Lv, X., Liu, D., Guo, H., Yao, G., Wang, L., Liang, X., & Yang, Y. METTL3-mediated maturation of mir-126-5p promotes ovarian cancer progression via PTEN-mediated PI3K/Akt/mTOR pathway. Cancer Gene Ther 2021 Apr;28(3–4):335–349. https://doi.org/10.1038/s41417-020-00222-3.
Peng, W., Li, J., Chen, R., Gu, Q., Yang, P., Qian, W., Ji, D., Wang, Q., Zhang, Z., Tang, J., & Sun, Y. Upregulated METTL3 promotes metastasis of colorectal Cancer via miR-1246/SPRED2/MAPK signaling pathway. J Exp Clin Cancer Res. 2019 Sep 6;38(1):393. https://doi.org/10.1186/s13046-019-1408-4.
Liu, L., Wu, Y., Li, Q., Liang, J., He, Q., Zhao, L., Chen, J., Cheng, M., Huang, Z., Ren, H., Chen, J., Peng, L., Gao, F., Chen, D., & Wang, A. METTL3 Promotes Tumorigenesis and Metastasis through BMI1 m6A Methylation in Oral Squamous Cell Carcinoma. Mol Ther. 2020 Oct 7;28(10):2177–2190. https://doi.org/10.1016/j.ymthe.2020.06.024.
Zhao, W., Cui, Y., Liu, L., Ma, X., Qi, X., Wang, Y., Liu, Z., Ma, S., Liu, J., & Wu, J. METTL3 facilitates oral squamous cell Carcinoma Tumorigenesis by enhancing c-Myc Stability via YTHDF1-Mediated m6A modification. Mol Ther Nucleic Acids 2020 Jun 5;20:1–12. https://doi.org/10.1016/j.omtn.2020.01.033.
Funding
This study was supported by Research Project of TCM Bureau of Guangdong Province(Project name: Study on the mechanism of inhibiting invasion and metastasis of oral squamous cell carcinoma by reducing the m6A modification level of miR-99a-5p by downregulating METTL3, Project number: 20222084).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
12033_2023_815_MOESM4_ESM.jpg
Supplementary Material 4: Supplementary Figure S1. Effects of miR-99a-5p on the biological functions of HOK cells. After HOK cells were transfected with miR-99a-5p mimic and mimic nc, (A) cell viability was evaluated using CCK-8; (B,C) cell migration and (D,E) invasion were evaluated by Transwell assay.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, Y., Guan, Y. & Zhang, X. METTL3-Mediated Maturation of miR-99a-5p Promotes Cell Migration and Invasion in Oral Squamous Cell Carcinoma by Targeting ZBTB7A. Mol Biotechnol 66, 1942–1953 (2024). https://doi.org/10.1007/s12033-023-00815-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12033-023-00815-x